Cartilage Cheat Sheet
1/99
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
100 Terms
Cartilage basic characteristics (blood + nerves)
avascular and aneural (no blood vessels or nerves)
What surrounds cartilage?
perichondrium
Functions of perichondrium
provides nutrients via diffusion
Main cells of cartilage
chondrocytes
Space that holds chondrocytes
lacunae
Cartilage matrix composition
gel-like ground substance + fibers
Most abundant cartilage type
hyaline cartilage
Hyaline cartilage fibers
collagen fibers
Hyaline cartilage appearance
glassy/frosted
Hyaline cartilage locations
joints, ribs, nose, trachea
Elastic cartilage key feature
contains elastic fibers E
Elastic cartilage locations
ear and epiglottis ONLY
Strongest cartilage type
fibrocartilage
Fibrocartilage functions
resists compression and tension
Fibrocartilage locations
intervertebral discs, pubic symphysis, menisci
Two types of cartilage growth
appositional and interstitial
Appositional growth definition
growth from the outside
Interstitial growth definition
growth from within
Bone growth type
Appositional only
Cartilage vs. bone (blood supply)
cartilage = none, bone = present
Cartilage cells vs. bone cells
chondrocytes vs. osteocytes
7 functions of bone (SPAM BTH)
support, protection, anchorage, mineral storage, blood cell formation, triglyceride storage, hormone production
Where are minerals stored in bone?
bone matrix
What minerals are stored in bone?
calcium and phosphate
Where does hematopoiesis occur?
red bone marrow
What does red marrow produce?
RBC’s, WBC’s, platelets
What is stored in yellow bone marrow?
triglycerides (fat)
Hormone produced by bone
osteocalcin
Axial skeleton includes
skull, vertebral column, rib cage
Appendicular skeleton includes
limbs and girdles
Long bone structure parts
diaphysis, epiphyses, compact bone, spongy bone, medullary cavity
Diaphysis definition
shaft of long bone
Epiphysis definition
ends of long bone
Medullary cavity contains (adults)
yellow marrow
Short bones
•cube-shaped
•wrist and ankles
Flat bones
•protection + muscle attachment
sternum and ribs
Sesamoid
•patella
•reduce friction, change tendon pull
Irregular bone
•vertebrae and hip bones
Compact bone function
strength and protection S
Spongy bone structure and function
•provide structural support
•house red bone marrow for blood cell production
Periosteum functions
outer covering, growth, blood supply W
Why are fractures painful
periosteum has nerves
Endosteum location
inner bone surfaces
Bone cells
osteoprogenitor
osteoblast
osteocyte
lining cells
osteoclast
Osteoblast
build bone Os
Osteoclast
break down bone
Osteocyte
maintain bone
Osteon definition
structural unit of compact bone
Central (Haversian) canal contains
blood vessels and nerves
Lamellae
concentric rings of bone matric
Organic bone component
collagen (flexibility)
Inorganic component
hydroxyapatite (hardness(
Ossification definition
bone formation
Endochondral ossification
•hyaline cartilage → bone
•femur, humerus, tibia, vertebrae, pelvis, and base of skull
Intramembranous ossification
•fibrous membrane → bone
•frontal and parietal bone, mandible and maxilla, clavicle
Epiphyseal plate function
lengthwise bone growth
5 zones of epiphyseal plate (Royal Penguins Hate Cold Oceans)
resting
proliferation
hypertrophic
calcification
ossification
Resting zone
•small inactive cartilage
zone of reserve cartilage
Proliferation zone
•growth zone
•chondrocytes divide rapidly, stacking up like coins
•multiplying to create more cartilage
Hypertrophic zone
•maturation zone
•cartilage cells stop dividing and grow huge
•they take up more space
Calcification zone
•death zone
•cartilage matrix calcifies (hardens)
•enlarged cells die
Ossification zone
•deposition zone
•blood vessels enter
•bone replaced
PTH function
increases blood clacium W
olff’s law
bone adapts to stress
1st stage (fracture repair)
hematoma forms
2nd stage (fracture repair)
soft (fibrocartilaginous) callus forms
3rd stage (fracture repair)
hard (bony) callus forms
4th stage (fracture repair)
remodeling begins
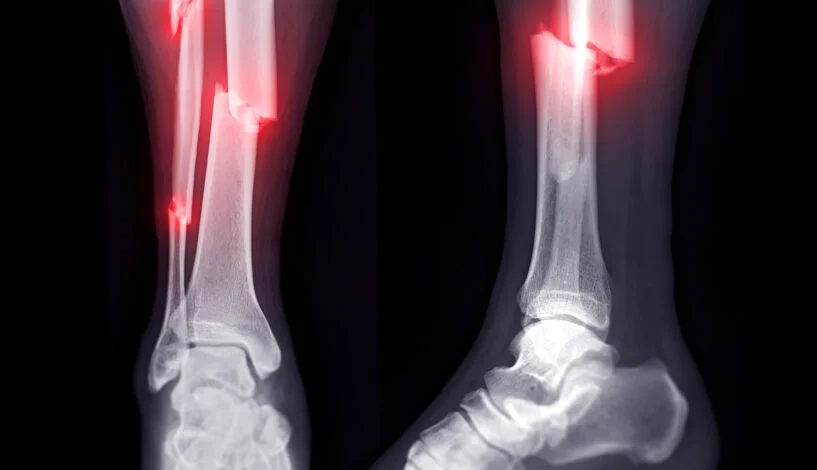
open (compound) fracture
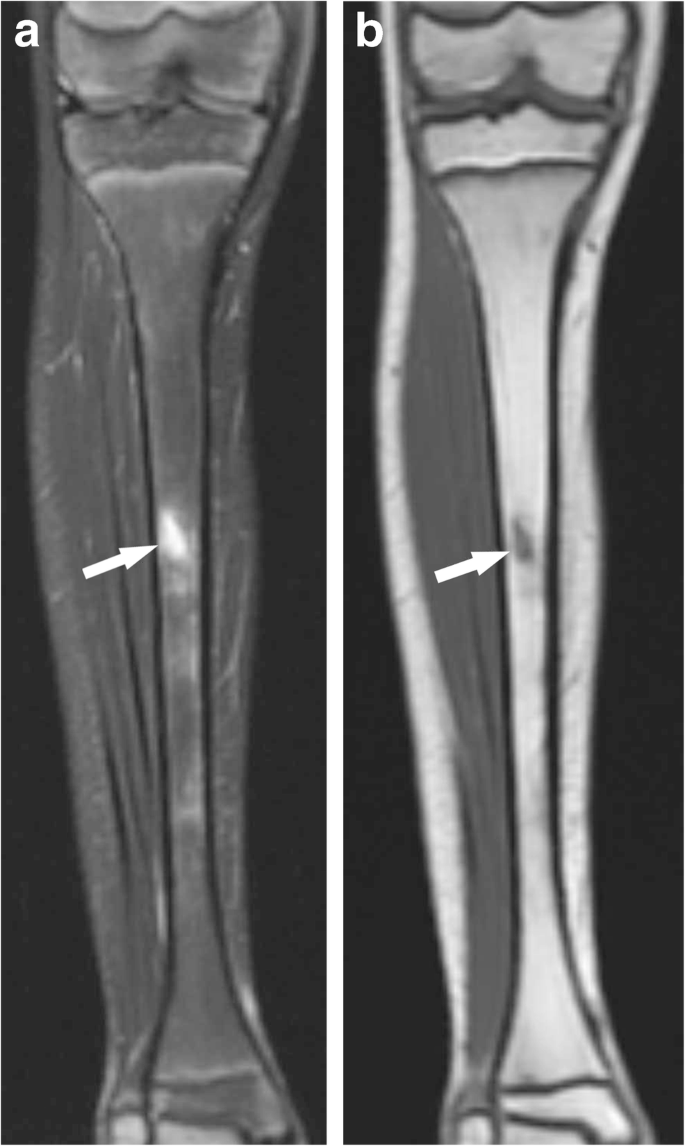
closed (simple) fracture
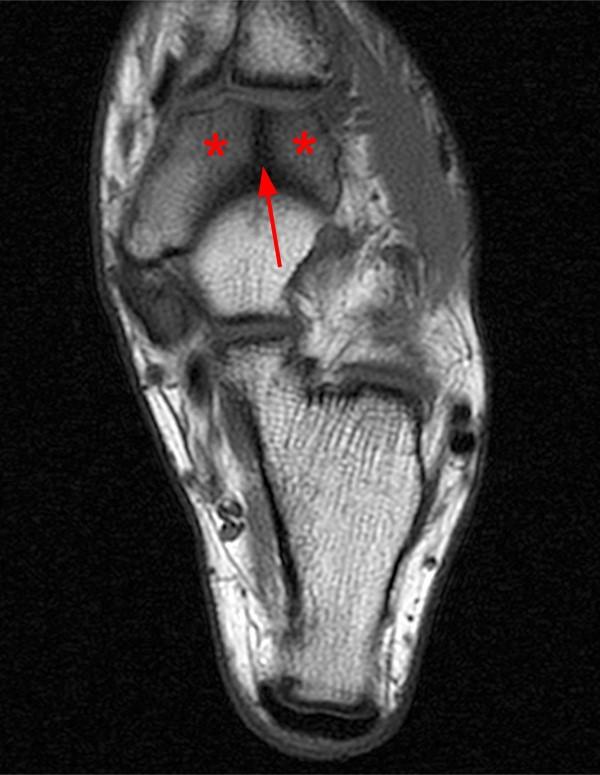
displaced fracture
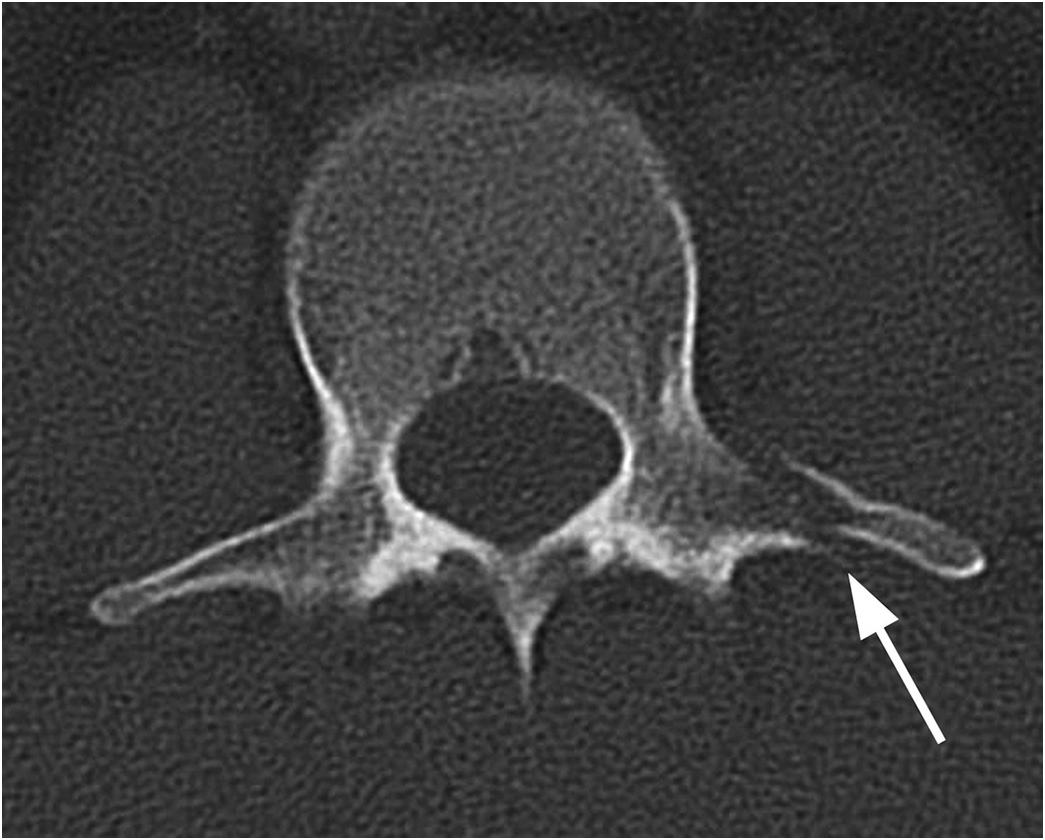
transverse fracture
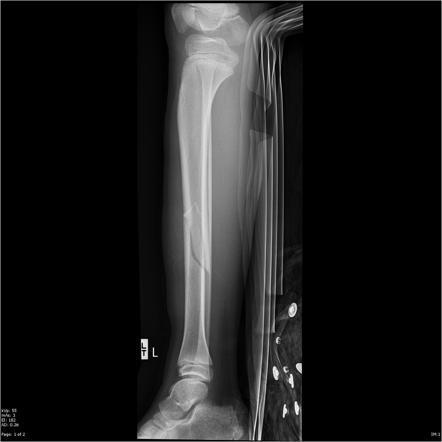
oblique fracture
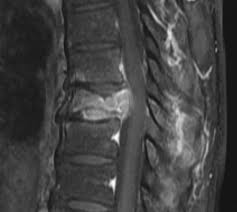
compression fracture
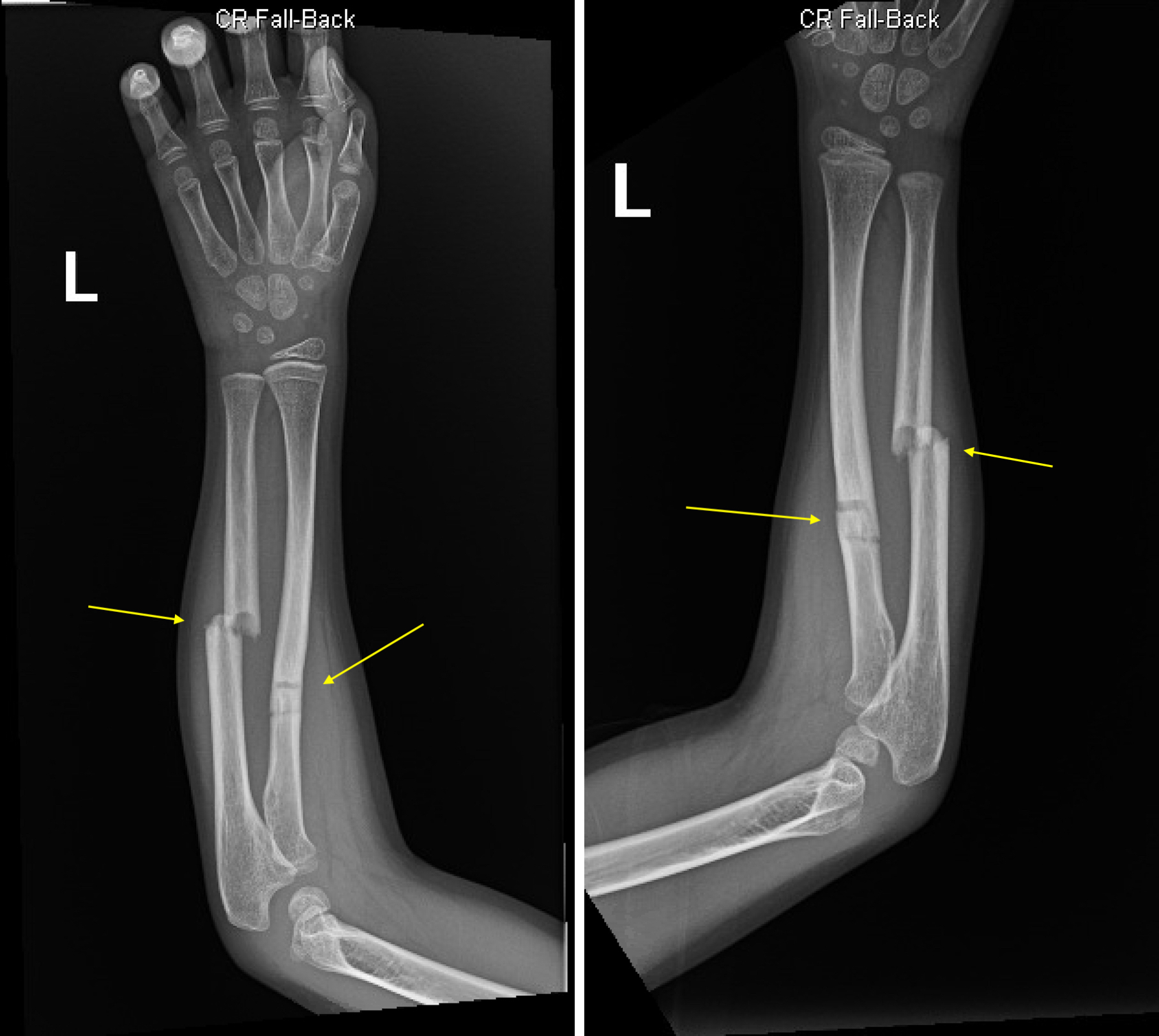
greenstick fracture
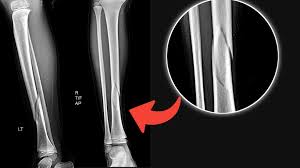
spiral
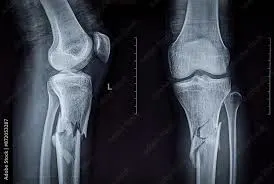
communiated fracture
Osteomalacia/Rickets
•poor mineralization (soft bones)
•lack of vitamin D
•osteomalacia = adults
•rickets = children
Osteoporosis
•too much bone resorption
•porous bones
•most common group: postmenopausal women
Paget’s disease problem
•disorganized bone remodeling
•messy bones
Tuberosity
•BIG BUMP
•large-rounded projection
Crest
•narrow ridge of bone
•ridge on a helmet
Trochanter
•very large, blunt irregularly shaped process
•TRUCK-sized bump
Line
•narrow ride of bone
•less prominent
•light line
Tubercle
•small-rounded projection or process
•tiny small bump
Epicondyle
•raised area on or above a condyle
•epi = above
Spine
•sharp and slender
•often projection
•sharp spine = OUCH
Process
•any bony prominence
•anything sticking out
Head
•bony expansion carried on a narrow neck
•ball head = rounded end
Facet
•smooth, nearly flat articular (joint) surface
•flat face
Condyle
•rounded articular projection; often articulates with a corresponding fossa
•rounded connector
Groove
•furrow
•slide; shallow trench
Fissure
•narrow-slit like opening
•fish-slit = narrow crack
Foramen
•round or oval opening through a bone
•”for a man to pass through”
Notch
indentation
Meatus
•canal-like passageway
•me-at-us = tunnel
Sinus
•cavity within a bone
•air space
Fossa
•shallow, basin-like depression in a bone, often serving as an articular surface
•fossil sits in
Cartilage (OVERVIEW)
•avascular
•chondrocytes
•matrix = flexible
•appositional and interstitial growth
Bone (OVERVIEW)
•blood
•osteocytes
•matrix = hard
•interstitial growth