NS 3310 Lecture 23
1/131
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
132 Terms
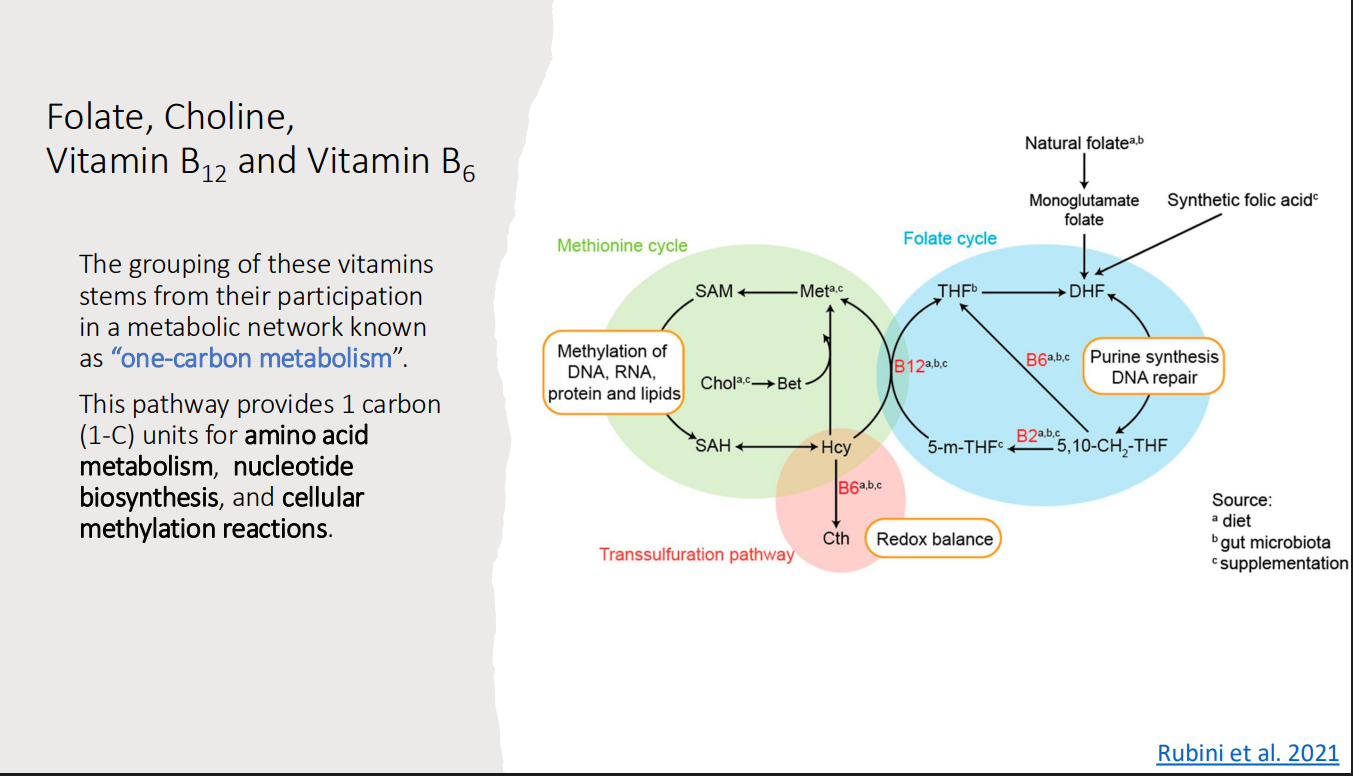
Folate, Choline, Vitamin B12 and Vitamin B6: The grouping of these vitamins stems from their participation in a metabolic network known as?
“one-carbon metabolism”
“One-carbon metabolism” is a pathway provides 1 carbon (1-C) units for what 3 things?
Amino acid metabolism
Nucleotide biosynthesis
Cellular methylation reactions
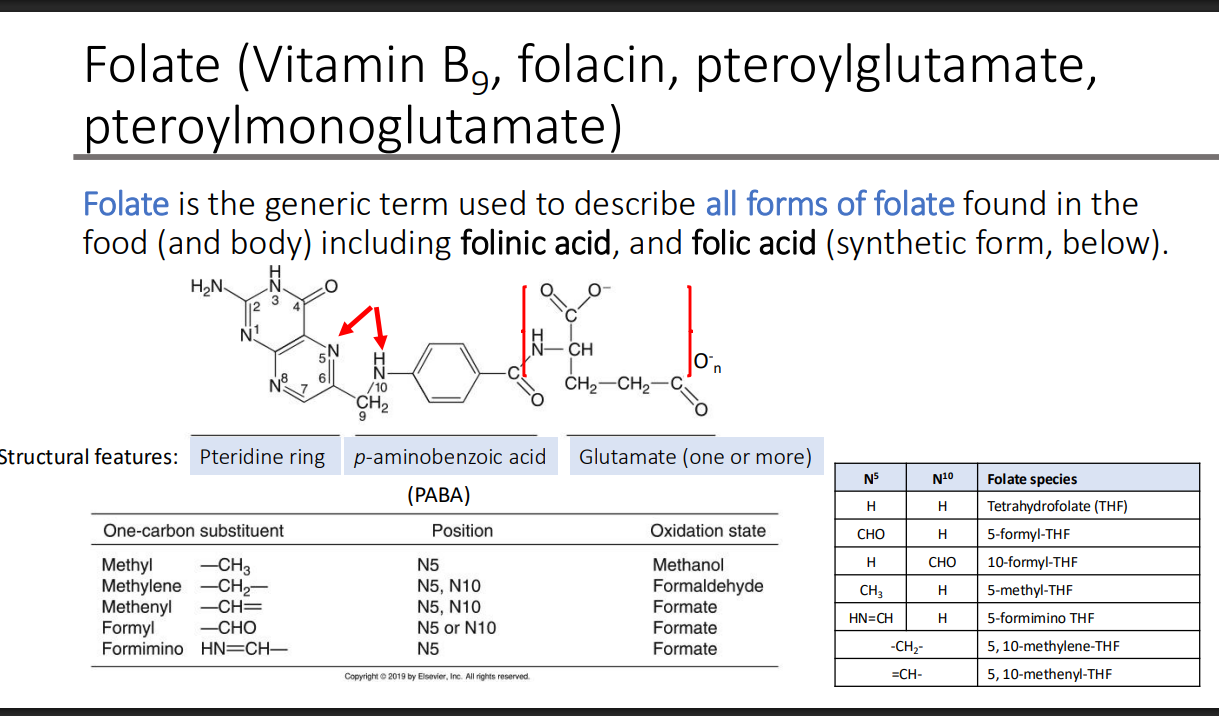
Folate (Vitamin B9 , folacin, pteroylglutamate, pteroylmonoglutamate): Folate is the generic term used to describe all forms of folate found in the food (and body) including what two things?
Folinic acid
Folic acid (synthetic form)
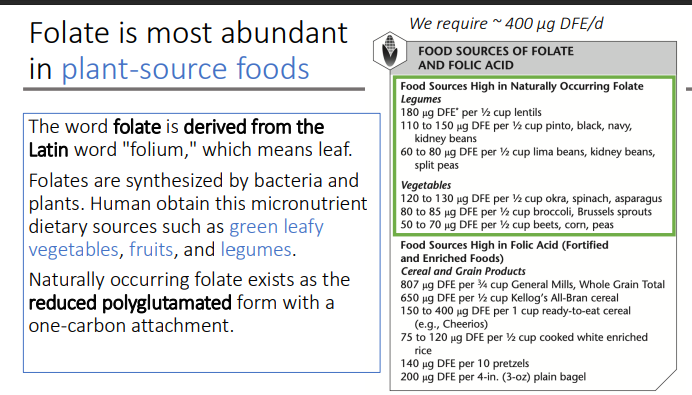
Folate is most abundant in what type of food?
plant source foods
The word folate is derived from the Latin word "folium," which means leaf.
Folates are synthesized by what two things?
bacteria and plants
Human obtain this micronutrient dietary sources such as what 3 things?
Green leafy vegetables
Fruits
Legumes
Naturally occurring folate exists as the reduced? with what attachment?
polyglutamated form with a one-carbon attachment.
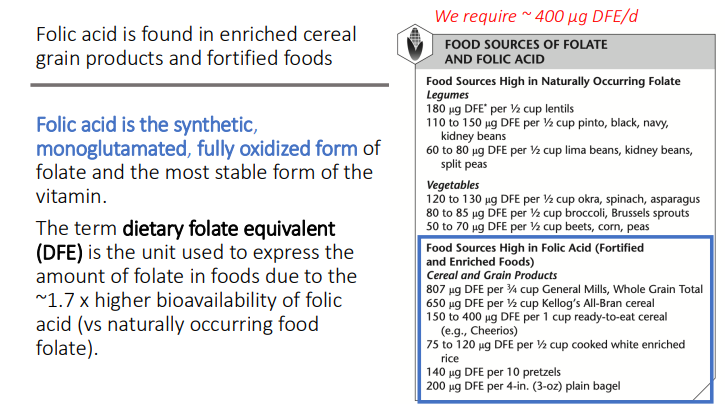
Folic acid is found in what two type of products?
Enriched cereal grain products
Fortified foods
Folic acid is the ____, _____, and fully ____ form of folate and the most?
Synthetic
Monoglutamated
oxidized
Most STABLE form of the vitamin
The term dietary folate equivalent (DFE) is the unit used to express the amount of folate in foods due to the?
~1.7 x higher bioavailability of folic acid (vs naturally occurring food folate).
We require how much DFE/d?
~ 400 µg DFE/d
Folate Bioavailability: Synthetic forms of folate are significantly more?
available than folates found naturally in foods.
Synthetic forms of folate are significantly more bioavailable than folates found naturally in foods. Because of the entrapment of naturally occurring food folate in the which two things?
Cellular structure
Insoluble matrix of certain foods
Synthetic forms of folate are significantly more bioavailable than folates found naturally in foods because of the destruction of?
THF during passage
Synthetic forms of folate are significantly more bioavailable than folates found naturally in foods because of the inhibition of intestinal deconjugation of?
polyglutamyl folates

Large losses of food folate can occur during food processing or preparation. What are the two examples?
Heating under oxidative conditions (e.g., cast iron)
Leaching of folate from food into the cooking water

Digestion, Absorption, and Intestinal Metabolism of Folate: Absorption of naturally occurring food folate requires cleavage of the? by what type of enzymes?
polyglutamate tail
brush border enzymes.
What are used for folate uptake and are present in the intestine and other tissues? What are two examples?
Folate transporters
proton-coupled folate transporter (PCFT)
Reduced folate carrier (RFC)
At high intake levels, folate can enter cells by?
passive diffusion
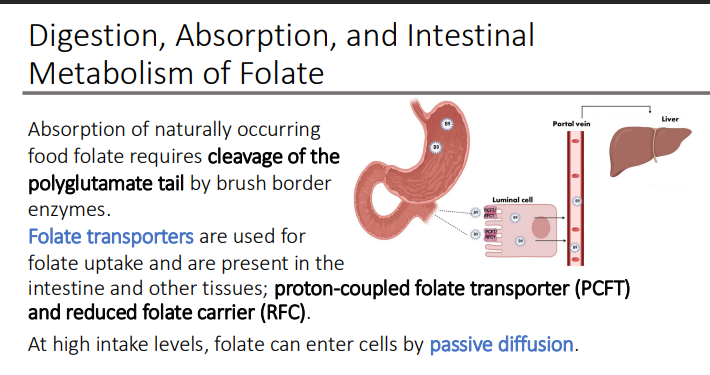
Digestion, absorption, and intestinal metabolism of folate: The majority of folate taken up by intestinal cells is converted to what?
Small amounts of what can also be present
5- methyl-THF, which is the major form found in circulation
folic acid
The liver exports excess folate into? where is it sent to?
bile that is then sent to the gallbladder and GI tract,
The liver exports excess folate into bile that is then sent to the gallbladder and GI tract, but this can be reabsorbed in the intestine via an?
enterohepatic circulation
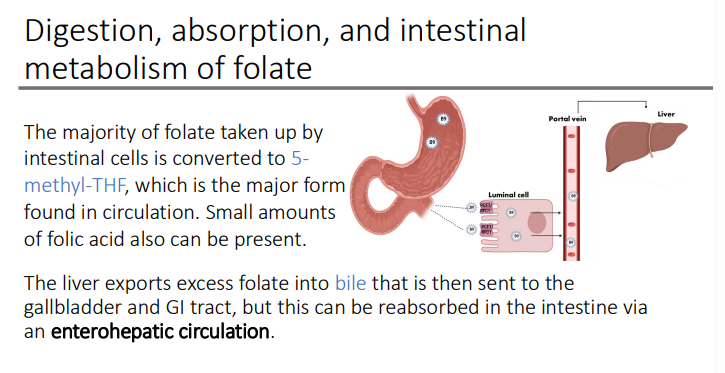
Folate requires conversion to what before it can function as a coenzyme?
THF
THF is the most abundant form in the human body. THF is the form that?
accepts/donates one-carbon groups
THF is ____ at positions 5, 6, 7, and 8 in the ___ ring?
reduced; pteridine
THF is?
Folic acid is reduced by what enzyme to become THF?
polyglutamated
Dihydrofolic reductase
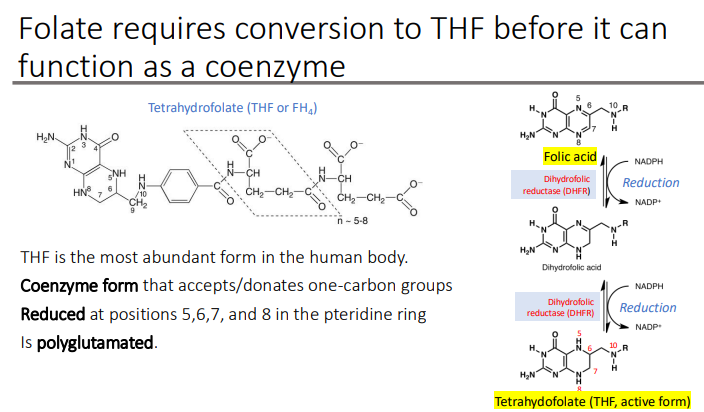
Metabolic differences between folic acid and folinic acid: Folic acid requires additional processing via what? Whereas FOLINIC acid bypasses this “Activation” step
DHFR to become active
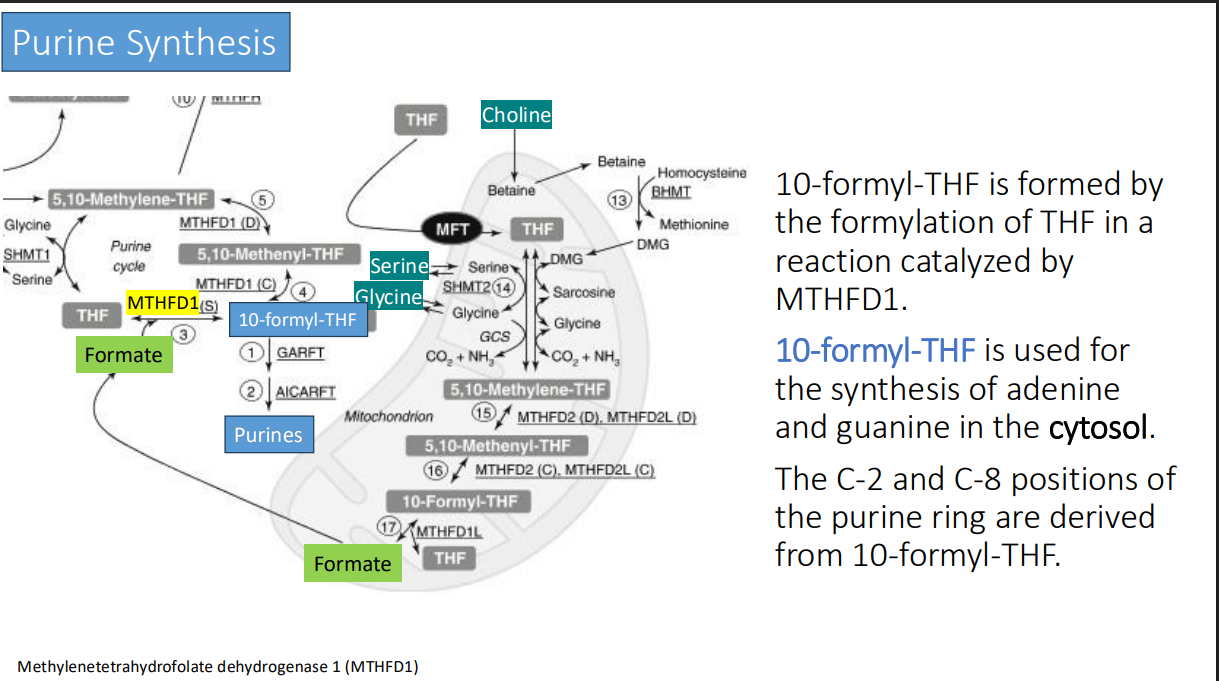
Sources of 1-C groups: One carbon units are obtained from what 5 sources?
Serine
Glycine
Histidine
formaldehyde
Formate
While these carbons are attached to THF (bound to N5 , N10, or both) they can be either?
reduced or oxidized (pteridine ring).
Folate can exist in a variety of forms. Once a carbon has been reduced to what level? it can’t be?
methyl; re-oxidized
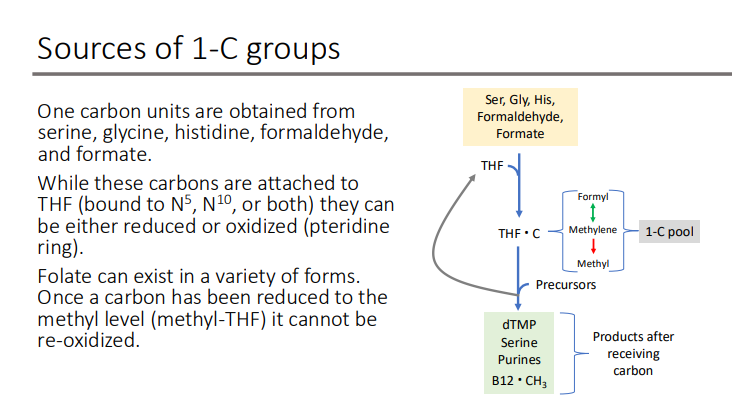
Role of THF inside the cell: Folate-dependent pathways are compartmentalized. What does this mean?
cytosol, nucleus and mitochondria
with each compartment carrying out specific one-carbon processes.
Role of THF inside the cell: Folate-dependent pathways are compartmentalized (cytosol, nucleus and mitochondria); each compartment is associated with a particular? and?
folate coenzyme and metabolic function.
Role of THF inside the cell: Folate coenzymes function as acceptors and donors of 1-C units in reactions involved in what 3 things?
Amino acid metabolism (ser, gly, met)
Nucleotide biosynthesis (purines and thymidylate, dTMP)
Methylation reactions (remethylation of Hcy)
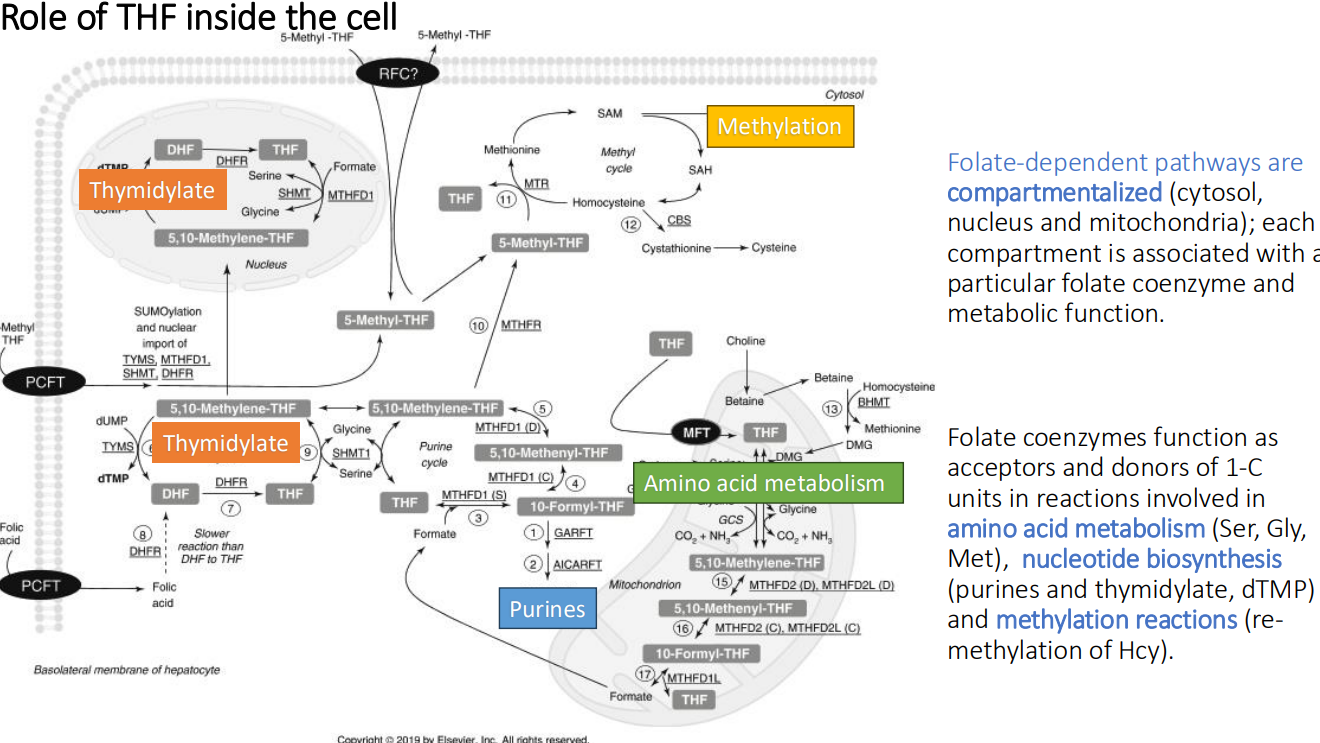
Purine synthesis: The mitochondria generates 1-C units in the form of formate through the catabolism of what 4 things?
Serine
Glycine
Dimethylglycine (DMG)
Sarcosine (methylglycine)
Purine Synthesis: DMG and sarcosine are derived from?
choline
Purine Synthesis: In the cytosol, what is a major source of 1-C units?
serine
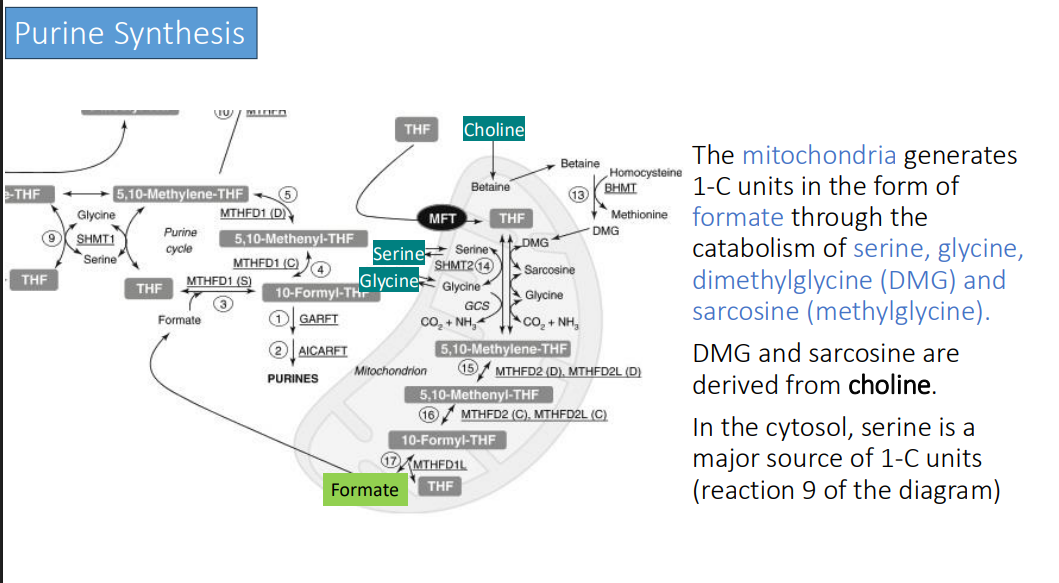
Purine Synthesis: 10-formyl-THF is formed by the formylation of? in a reaction catalyzed by?
THF
MTHFD1
10-formyl-THF is used for the synthesis of what two things in the cytosol?
adenine and guanine
The C-2 and C-8 positions of the purine ring are derived from?
10-formyl-THF
REVIEW: Purine synthesis requires glutamine, glycine, and aspartate
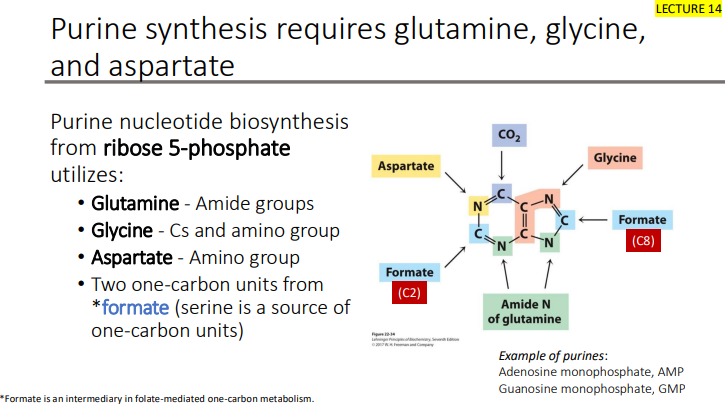
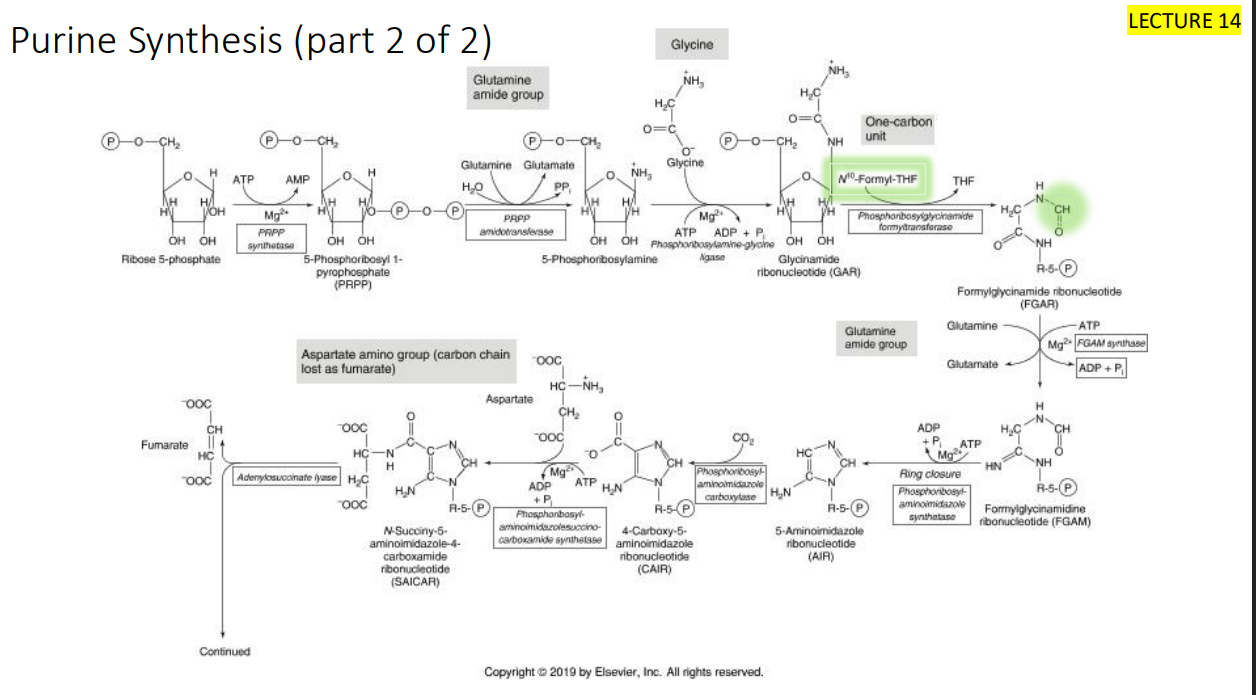
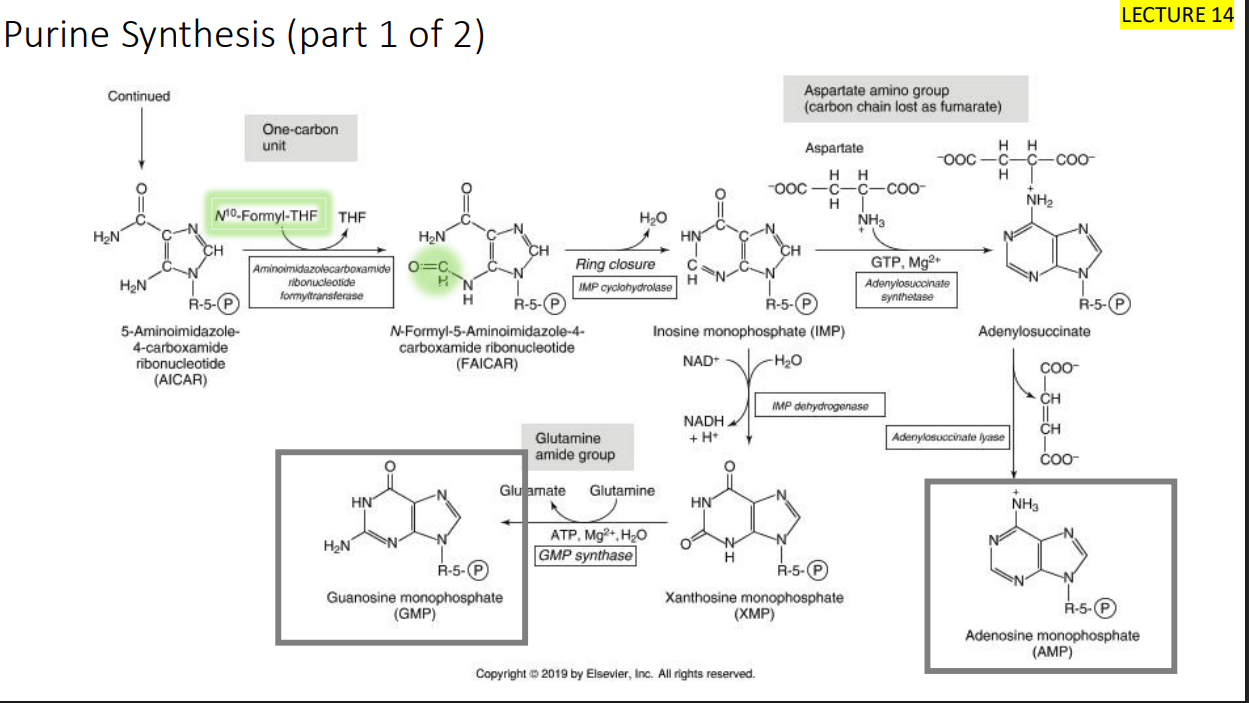
Purine synthesis review
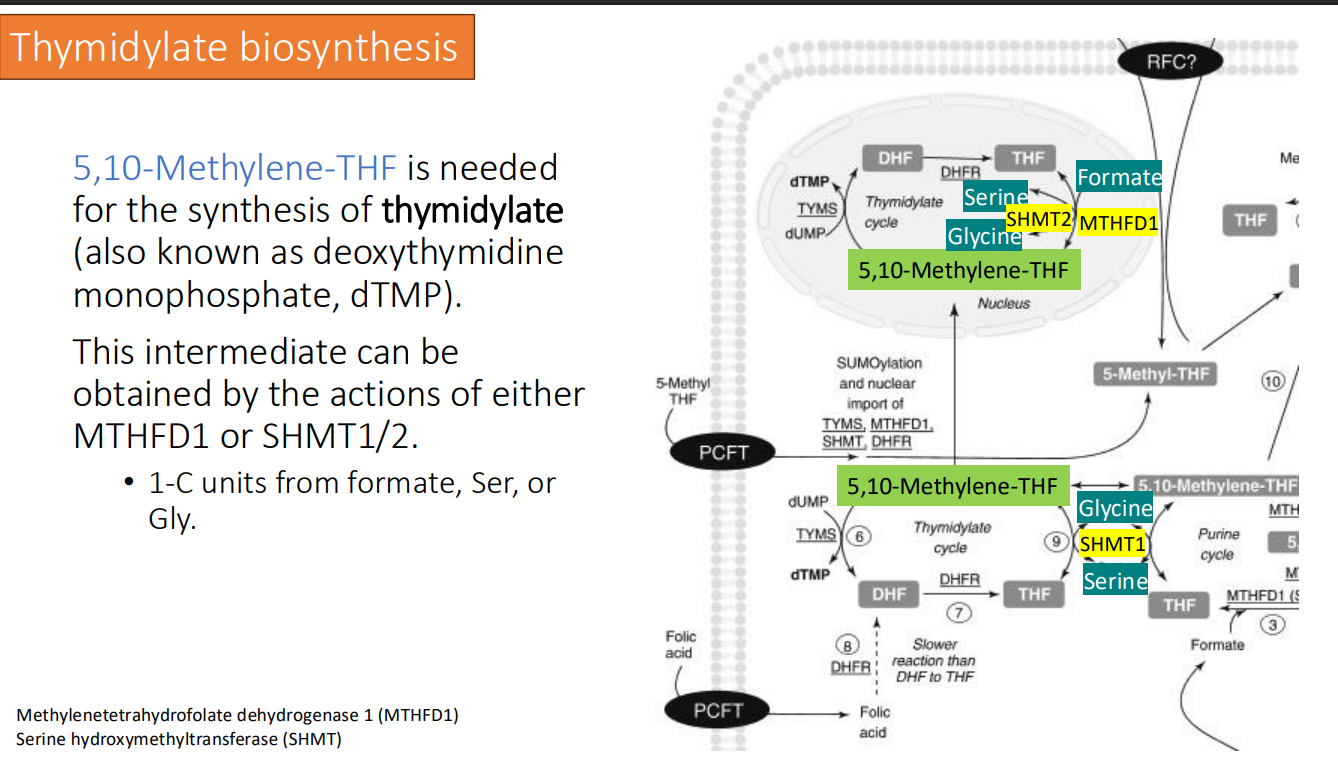
Thymidylate biosynthesis: What is needed for the synthesis of thymidylate (also known as deoxythymidine monophosphate, dTMP)?
5,10-Methylene-THF
5,10-Methylene-THF is needed for the synthesis of thymidylate (also known as deoxythymidine monophosphate, dTMP). This intermediate can be obtained by the actions of either what two things?
MTHFD1
SHMT1/2
1-C units from formate, Ser, or Gly.
Thymidylate biosynthesis: Most thymidylate synthesis occurs in the? Why?
nucleus
as pyrimidine is required for DNA synthesis, replication, and repair.
Thymidylate synthase (TYMS) transfers what to from 5,10-methylene-THF to deoxyuridine monophosphate (dUMP), which makes?
1- C to make dTMP
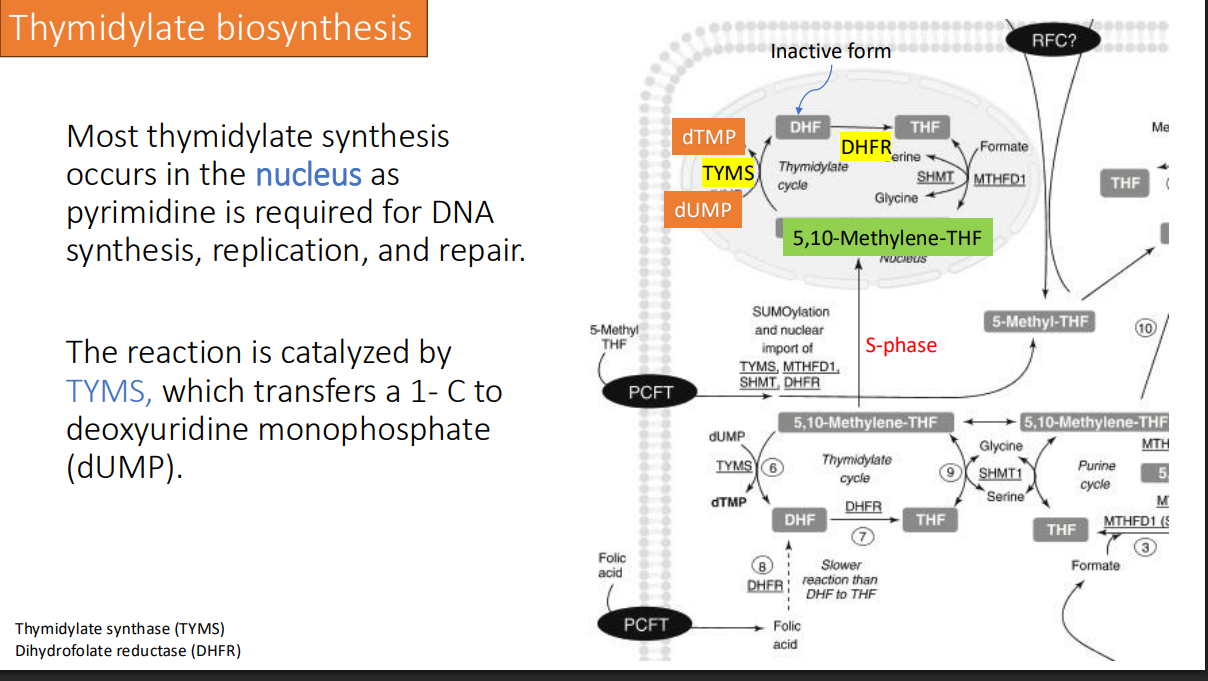
5-Methyl-THF is needed in what cycle? for the re-methylation of?
Where does this all occur in?
methionine cycle for the re-methylation of Hcy to Met (occurs in the cytosol)
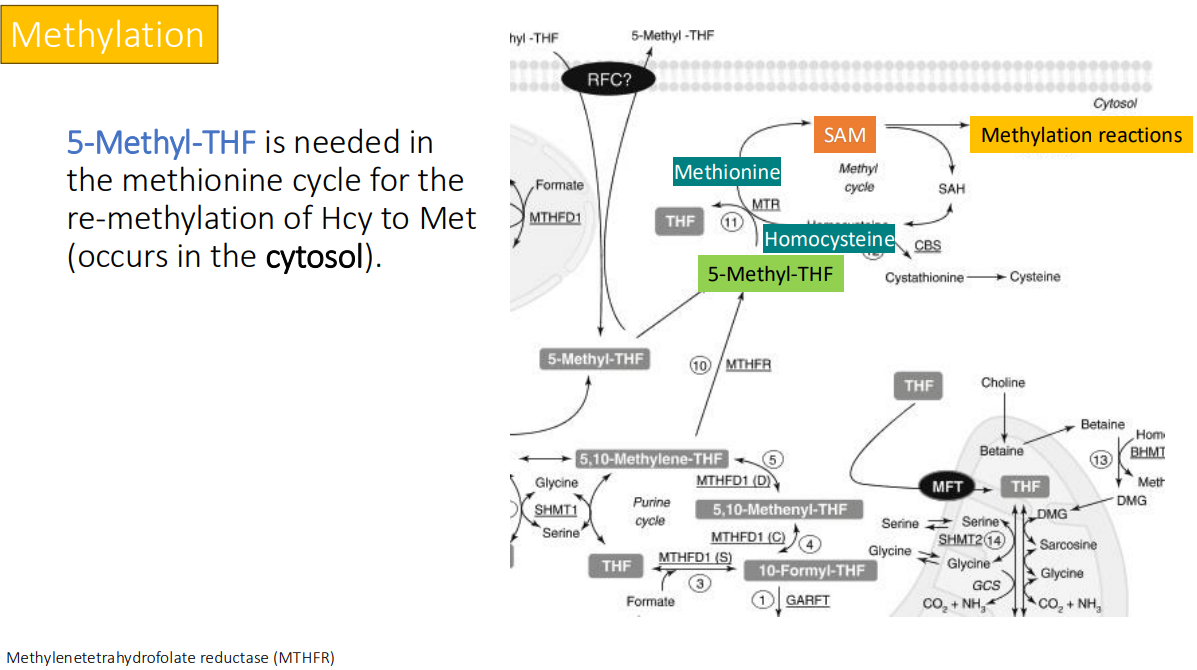
Methionine is used for SAM and cysteine synthesis: The methionine transmethylation pathway is responsible for the synthesis of Sadenosylmethionine (SAM). SAM is a universal? It participates in numerous synthetic pathways including the synthesis of what 4 things?
methyl donor in cells
Creatine
Carnitine
Epinephrine
Melatonin
Homocysteine can be remethylated to Met via what two pathways?
folate or choline/betaine-dependent pathways.
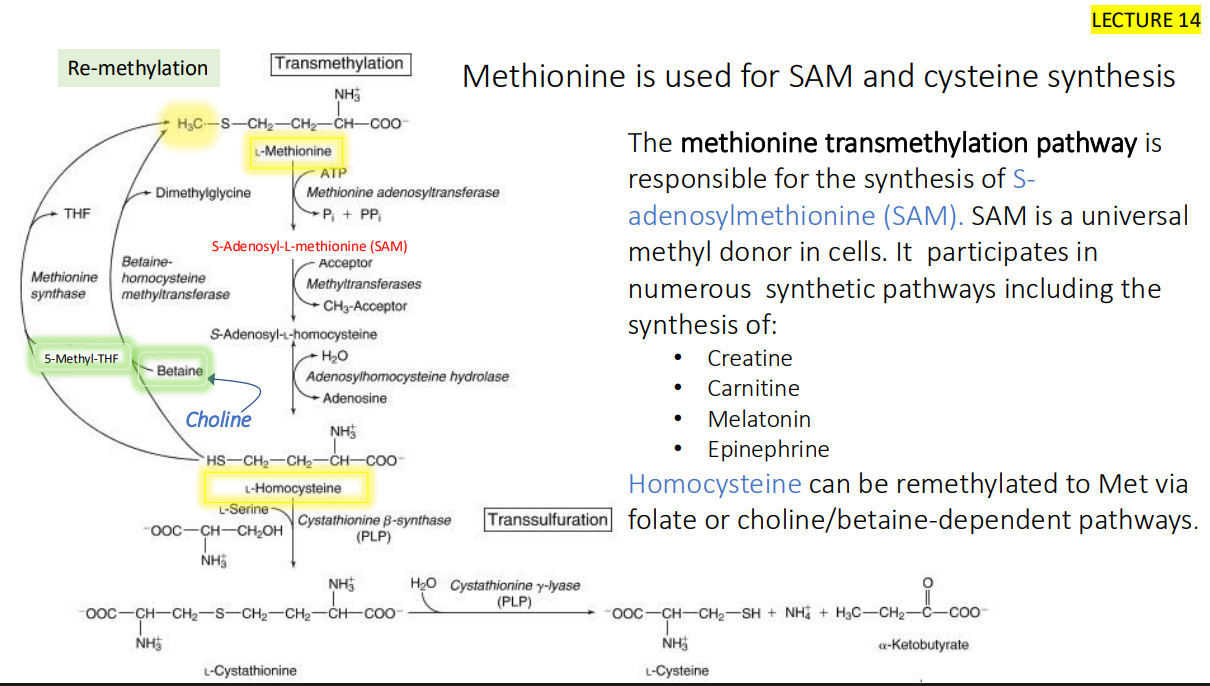
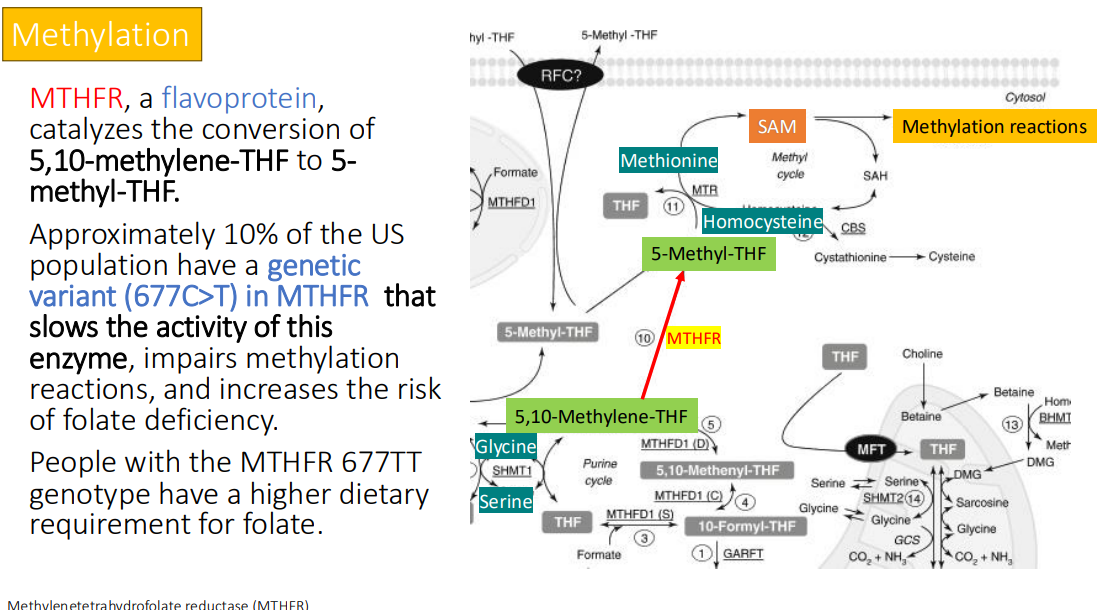
MTHFR, a flavoprotein, catalyzes the conversion of what to what?
5,10-methylene-THF to 5- methyl-THF
Approximately 10% of the US population have a genetic variant (677C>T) in MTHFR that? impairs? and increases the risk of?
slows the activity of this enzyme
Impairs methylation reactions,
increases the risk of folate deficiency
People with the MTHFR 677TT genotype have a higher?
dietary requirement for folate.
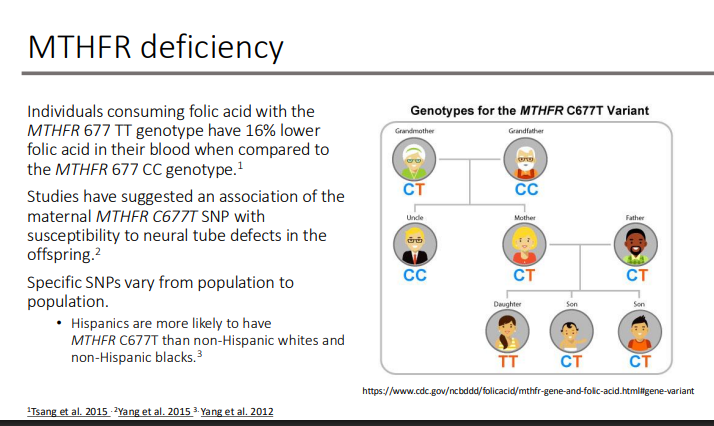
MTHFR deficiency: Individuals consuming folic acid with the MTHFR 677 TT genotype have 16% lower what in their blood when compared to MTHFR 677 CC genotype?
folic acid
Studies have suggested an association of the maternal MTHFR C677T SNP with what in offspring?
susceptibility to neural tube defects in the offspring
Specific SNPs vary from population to population. What ethnicity is more likely to have MTHFR C677T?
Hispanics are more likely to have MTHFR C677T than non-Hispanic whites and non-Hispanic blacks.
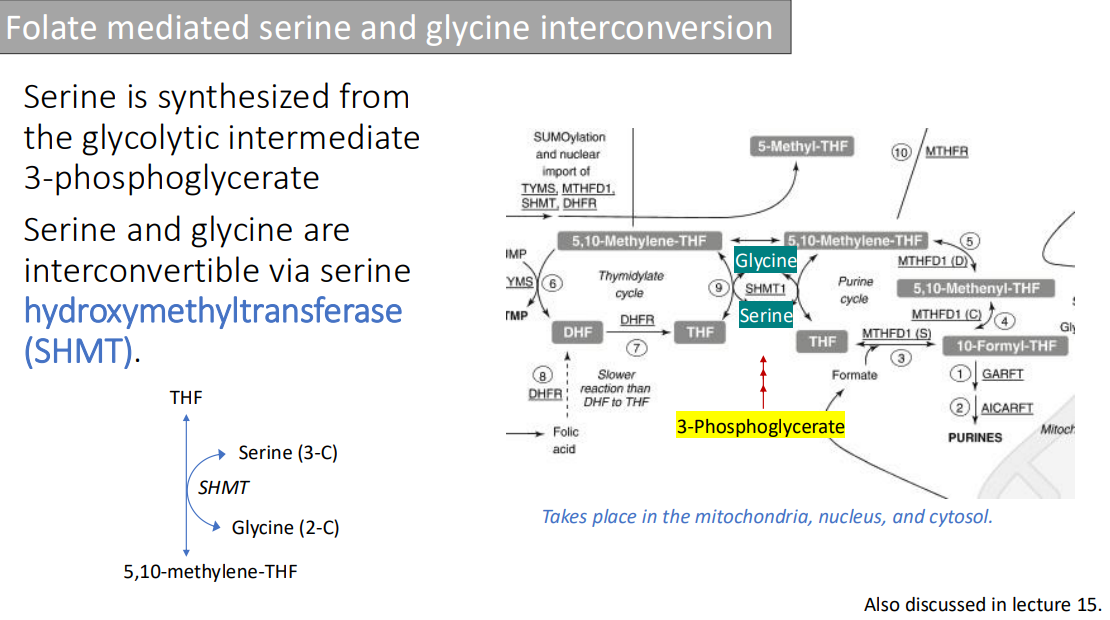
Folate mediated serine and glycine interconversion: Serine is synthesized from the glycolytic intermediate?
3-phosphoglycerate
Folate mediated serine and glycine interconversion: Serine and glycine are interconvertible via?
serine hydroxymethyltransferase (SHMT).
Folate mediated serine and glycine interconversion: This takes place in what three locations?
Mitochondria,
Nucleus
Cytosol

A loss-of-function variant of methylenetetrahydrofolate reductase (MTHFR) would:
A

Who is the universal methyl donor in cells?
S-adenosylmethionine (SAM)
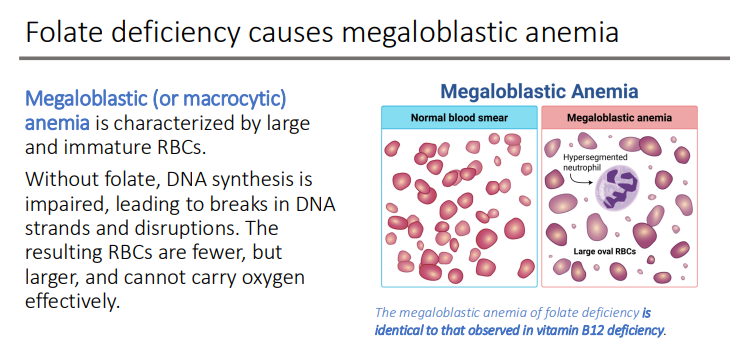
Folate deficiency causes what type of anemia?
megaloblastic (macrocytic) anemia
characterized by large and immature RBCs.
Without folate, DNA synthesis is ____, leading to breaks in ____ and disruptions. The resulting RBCs are fewer, but larger, and cannot carry ___effectively
impaired; DNA strands; oxygen
The megaloblastic anemia of folate deficiency is identical to that observed in what type of deficiency
Vit B12
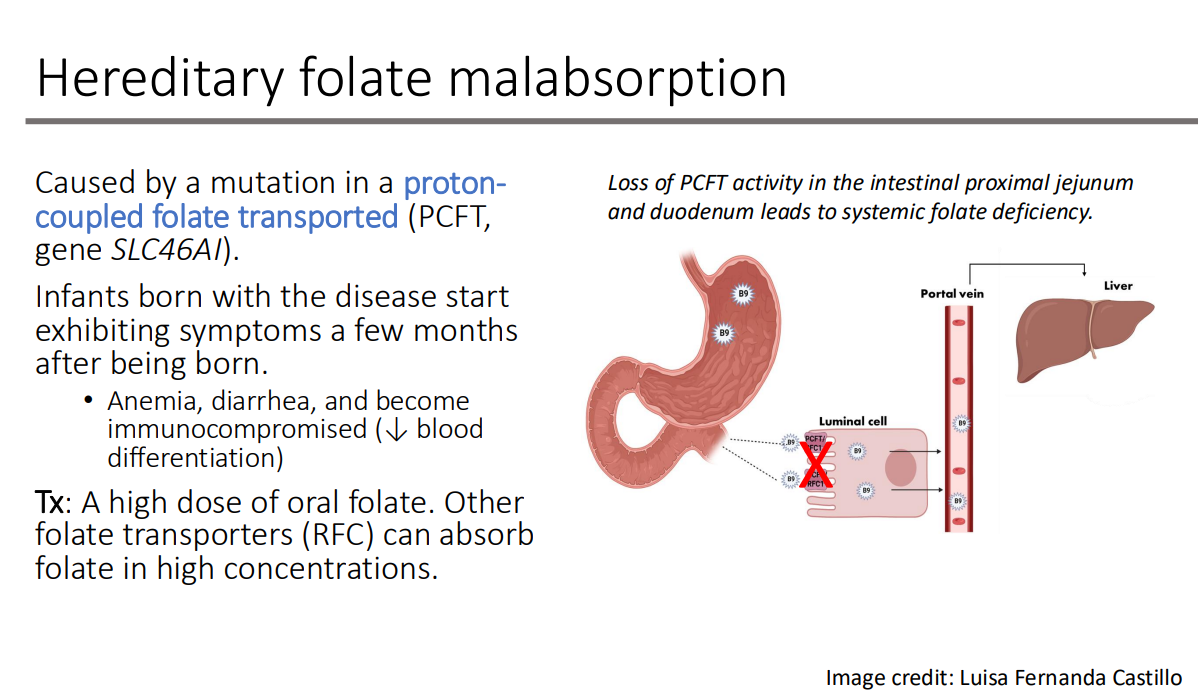
Hereditary folate malabsorption is caused by a mutation in what transporter?
proton coupled folate transporter (PCFT, gene SLC46AI).
Hereditary folate malabsorption: Loss of PCFT activity in what two areas leads to systemic folate deficiency
intestinal proximal jejunum and duodenum
Infants born with the disease start exhibiting symptoms a few months after being born. What are 3 symptoms?
Anemia
Diarrhea
Become immunocompromised (↓ blood differentiation
What is the treatment to Hereditary folate malabsorption?
A high dose of oral folate. Other folate transporters (RFC) can absorb folate in high concentrations.
Folic acid Fortification to Prevent Adverse Pregnancy Outcomes: Folic acid was added to the US food supply in 1998 to reduce a woman’s risk of having a baby with? What are two examples?
neural tube defects (NTDs)
including anencephaly and spina bifida.
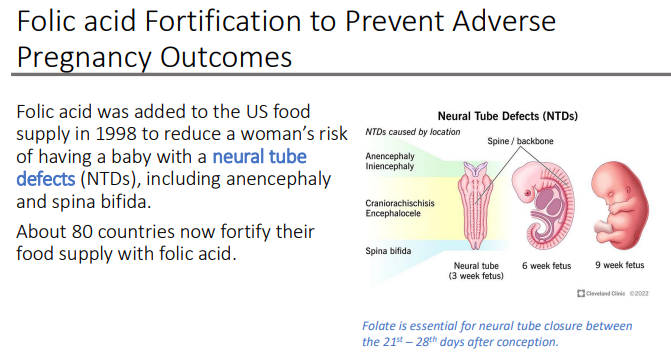
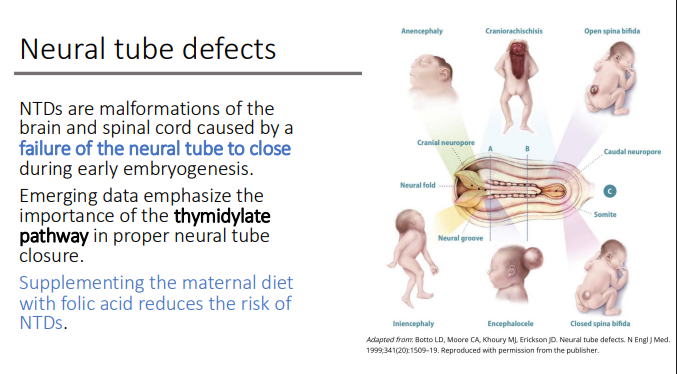
NTDs are malformations of the brain and spinal cord caused by a failure of? during?
the neural tube to close during early embryogenesis
Emerging data emphasize the importance of what pathway in proper neural tube closure?
the thymidylate pathway
Supplementing the maternal diet with what reduces the risk of NTDs?
folic acid
Folate intake and cancer risk: Inadequate intake of folate among adults is associated with increased risk for?
certain types of cancer (e.g., colon cancer) in epidemiological studies
Inadequate intake of folate among adults is associated with increased risk for certain types of cancer (e.g., colon cancer) in epidemiological studies. The underlying mechanism could involve?
uracil misincorporation arising from defective thymidylate synthesis.
This ultimately leads to DNA strand breaks / damage.
Excess intake Concerns have been raised over the potential for what promotion? with an overly abundant intake of folic acid due to folate’s role in supporting?
cancer promotion;
DNA synthesis/replication and cell division

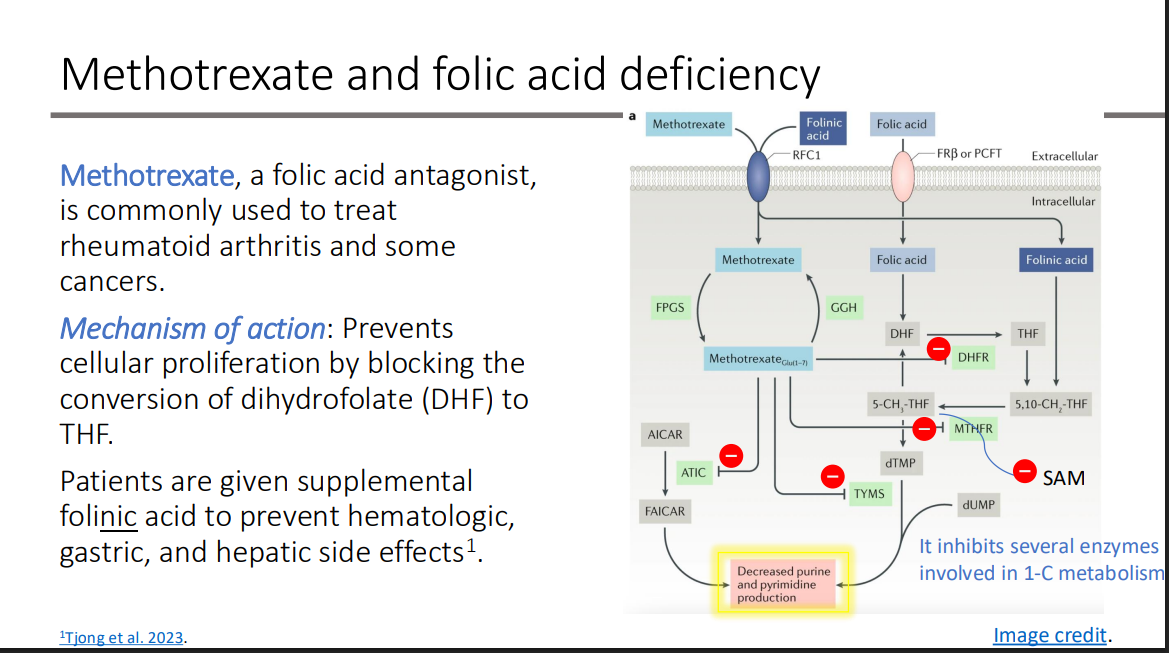
What is Methotrexate? what is it commonly used to treat?
a folic acid antagonist
is commonly used to treat rheumatoid arthritis and some cancers.
Mechanism of action of Methotrexate: Prevents cellular proliferation by blocking the conversion of what to what?
dihydrofolate (DHF) to THF
Patients are given supplemental what to prevent hematologic, gastric, and hepatic side effects.
folinic acid
Methotrexate inhibits several enzymes involved in?
1-C metabolism
Folate and vascular disease: Folate intake and status may modify the risk of vascular disease by affecting what levels in plasma?
homocysteine levels
Elevations in homocysteine are associated with an increased risk of?
CVD (via increased inflammation, and immunological responses)
Lowering homocysteine through treatment with folic acid and other B vitamins has NOT been proven to be effective in the? BUT appears to lower the risk of?
secondary prevention of a heart attack;
stroke

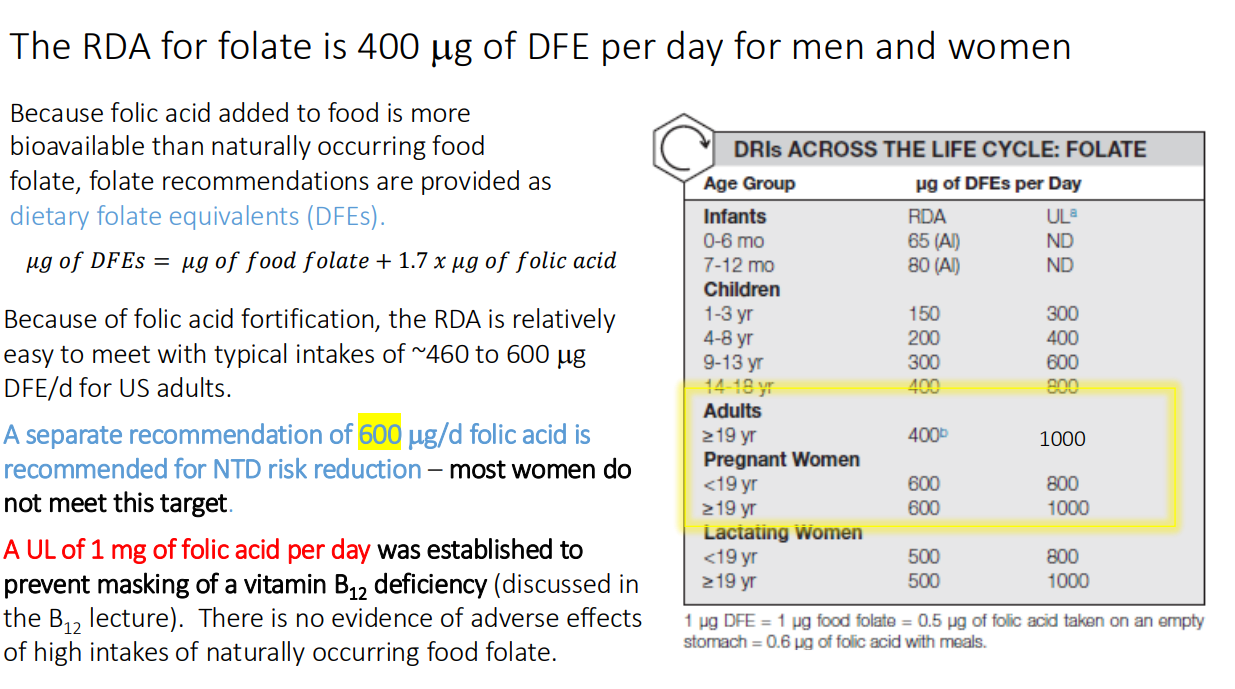
The RDA for folate is 400 ug of DFE per day for men and women: Because folic acid added to food is more bioavailable than naturally occurring food folate, folate recommendations are provided as?
dietary folate equivalents (DFEs).
𝜇𝑔 𝑜𝑓 𝐷𝐹𝐸𝑠 = 𝜇𝑔 𝑜𝑓 𝑓𝑜𝑜𝑑 𝑓𝑜𝑙𝑎𝑡𝑒 + 1.7 𝑥 𝜇𝑔 𝑜𝑓 𝑓𝑜𝑙𝑖𝑐 𝑎𝑐𝑖d
Because of folic acid fortification, the RDA is relatively easy to meet with typical intakes of ~460 to 600 ug DFE/d for US adults. A separate recommendation of what for NTD risk reduction?
600 ug/d folic acid is recommended for NTD risk reduction – most women do not meet this target
A UL of 1 mg of folic acid per day was established to prevent masking of
vitamin B12 deficiency
There is no evidence of adverse effects of high intakes of naturally occurring food folate

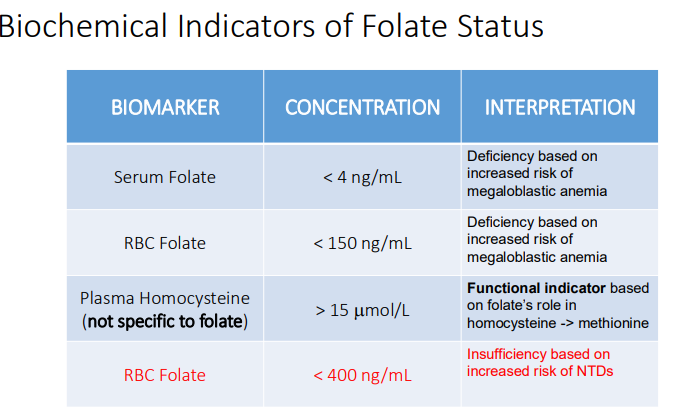
What are the 4 Biochemical Indicators of Folate Status?
Serum folate → Deficiency based on increased risk of megaloblastic anemia
RBC folate → Deficiency based on increased risk of megaloblastic anemia
Plasma homocysteine (not specific to folate) → Functional indicator based on folate’s role in homocysteine -> methionine
RBC Folate → Insufficiency based on increased risk of NTDs
The nutritional importance of choline was demonstrated in the early 1930s. Studies in animal models showed choline is essential for? and the prevention of?
lipid export from the liver
fatty liver
Dietary choline deficiency results in liver dysfunction
It wasn’t until the early 1990s that choline was recognized as an essential nutrient for humans. Dietary recommendations for choline were established in 1998. Choline is NOT recognized as a “vitamin” because, unlike most vitamins, choline does not function as a?
co-enzyme in metabolic reactions
Choline functions as a substrate and is used for the synthesis of what 3 things?
Acetylcholine
Betaine
Phospholipids

Structure and classification: Choline is a ___-containing compound with three labile ___ group
nitrogen; methyl
Structure and classification: The different forms of choline can be classified as?
water or lipid soluble
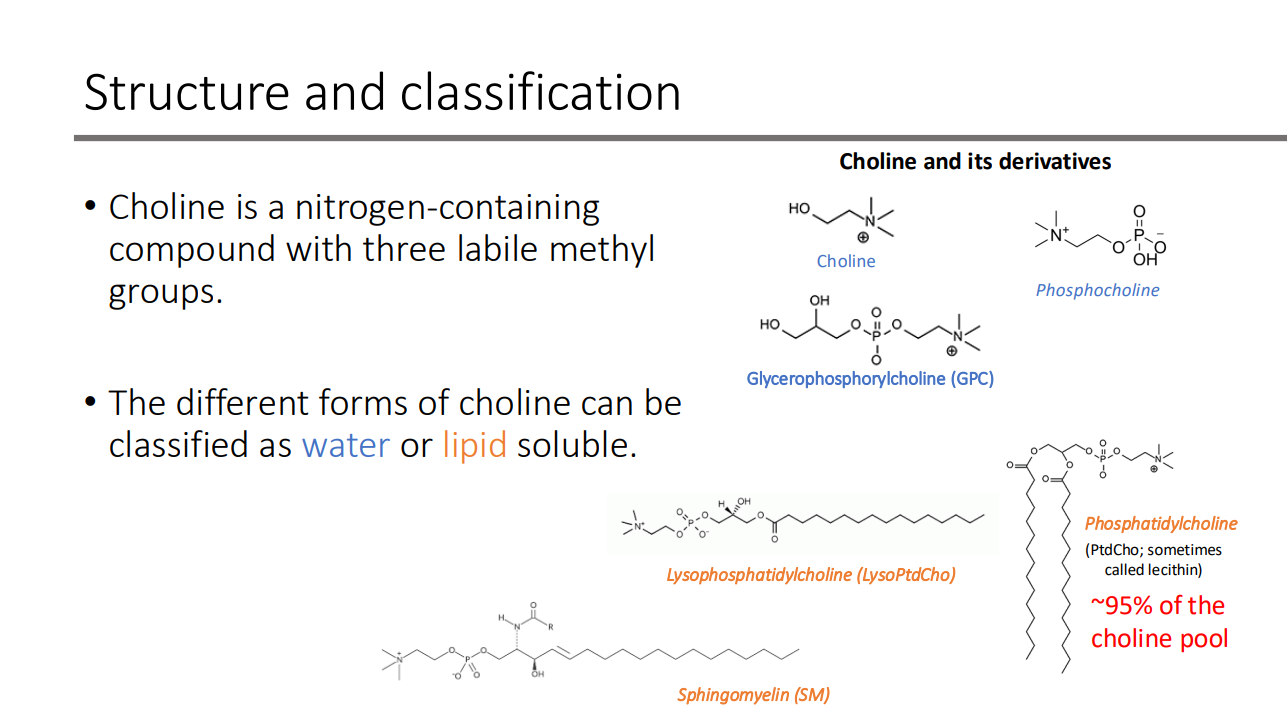
The body can produce a small amount of choline in the liver but is not enough to meet daily needs. Choline is present in both animal and plant sources, but which source have a higher choline content?
animal foods

The choline content of food is the sum of all forms of choline except what two things?
Acetylcholine → not present in food
Betaine → is not included in measurements of total dietary choline because cannot be converted back to choline in the body

Digestion and absorption of choline metabolites vary depending on their structure. Choline from water-soluble forms is taken up by intestinal cells (and other tissues) through?
sodium-independent carrier-mediated transporters.
Digestion and absorption of choline: Passive diffusion also occurs at?
high intake levels
Absorption is near complete except when intakes exceed the capacity of transporters, in which case, unabsorbed choline is acted on by? to generate?
gut microbes
trimethylamine (TMA)

Fat-soluble forms of choline (PtdCho, LysoPtdCho, SM) are incorporated into?
chylomicrons with other lipids
Absorption is somewhat less than observed with what type of form?
water-soluble forms

Except for betaine, all choline metabolites are?
interconvertible
The interconvertible forms comprise “total” choline intake.
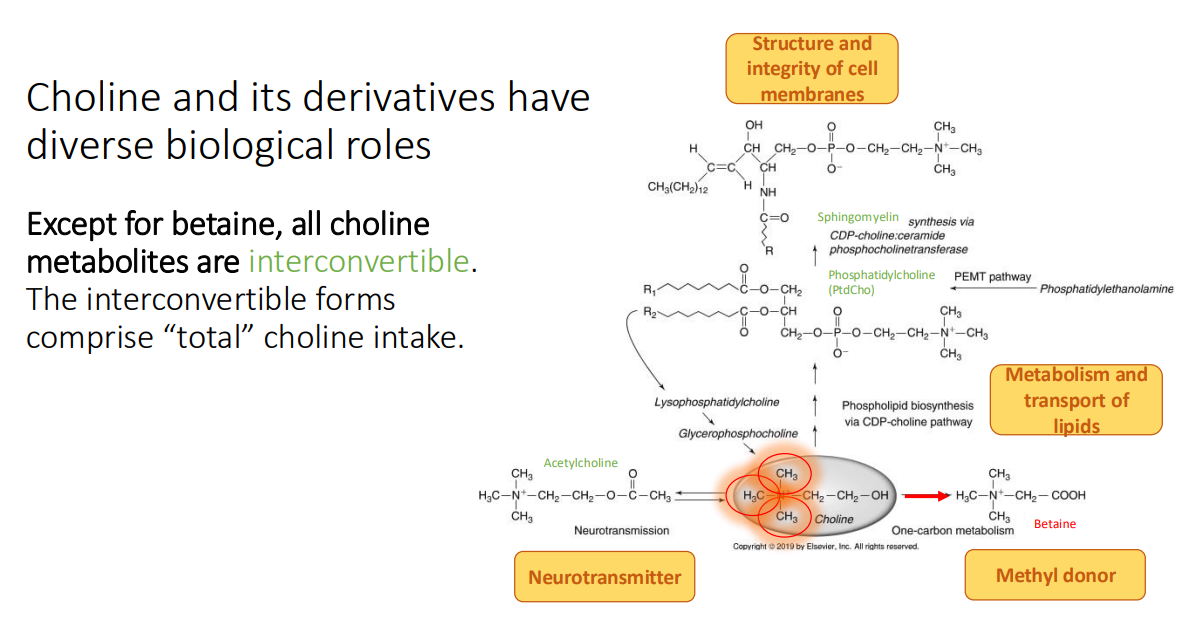
Metabolism of choline: Synthesis of PtdCho: What is the major site of choline metabolism?
Liver
Metabolism of choline: Synthesis of PtdCho: The liver is the major site of choline metabolism, wherein what biosynthesis takes place
phospholipid (e.g., PtdCho and SM)
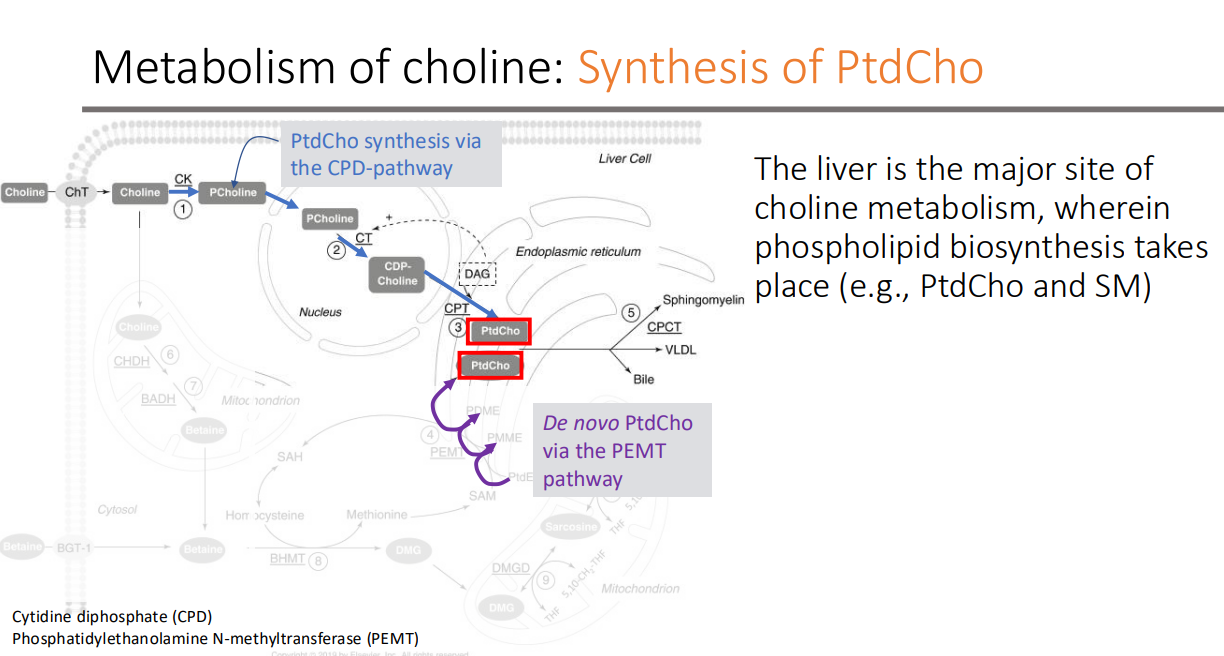
What pathway produces PtdCho from an existing choline molecule
The cytidine diphosphate (CPD)-choline pathway