The Motor System
1/82
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
83 Terms
Basal Ganglia
Initiation and execution of motor activity
Automatic stereotyped movement of a postural and reflex nature
The "Striatal Motor System"
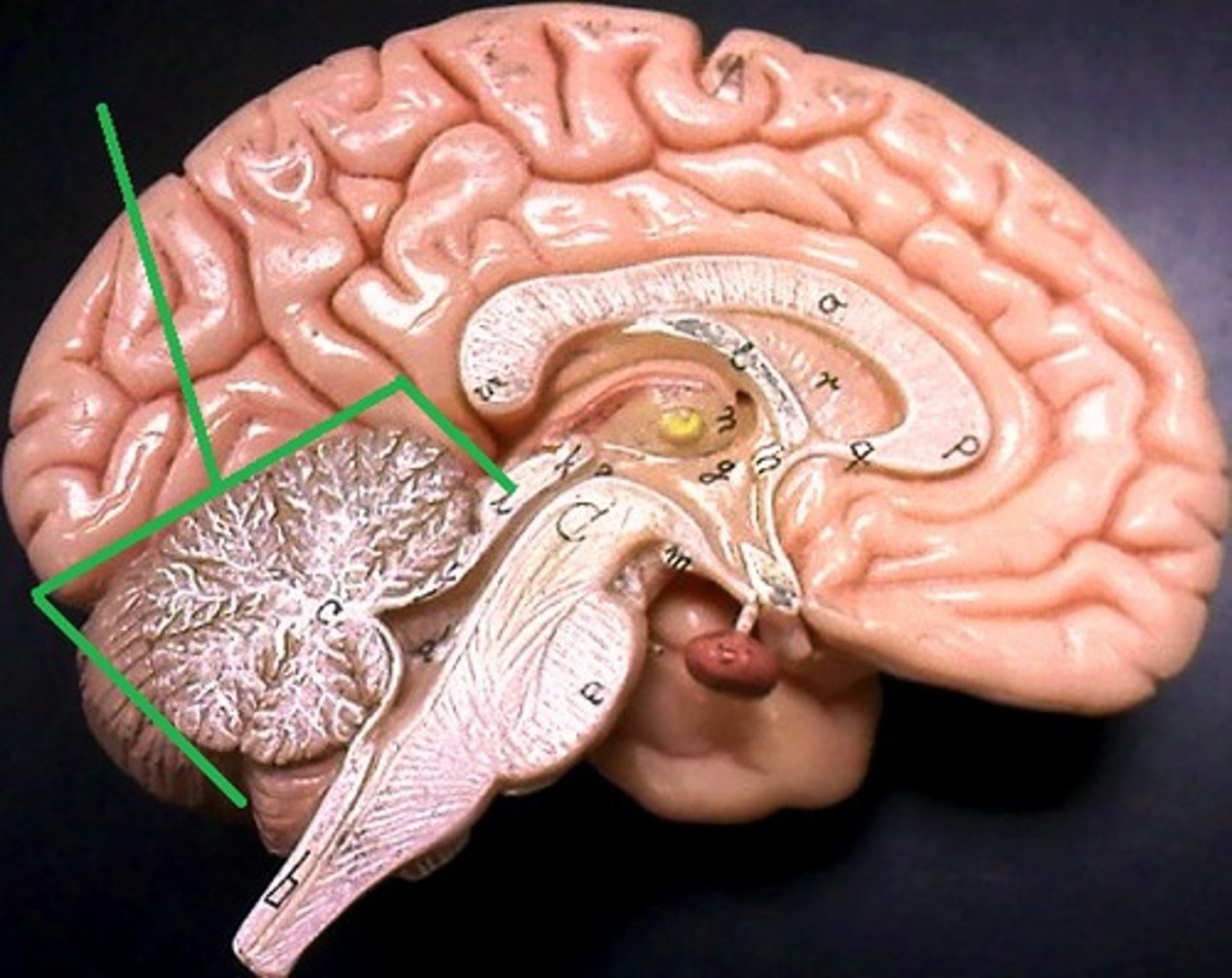
Cerebellum
Maintenance of posture, balance, and muscle tone
Coordination of voluntary motor activity
Lower Motor Neurons
Axons leave the CNS, extend through PNS to skeletal muscles. Cell bodies in anterior horns of spinal cord and in cranial nerve nuclei of brainstem
Damage = flaccid paralysis
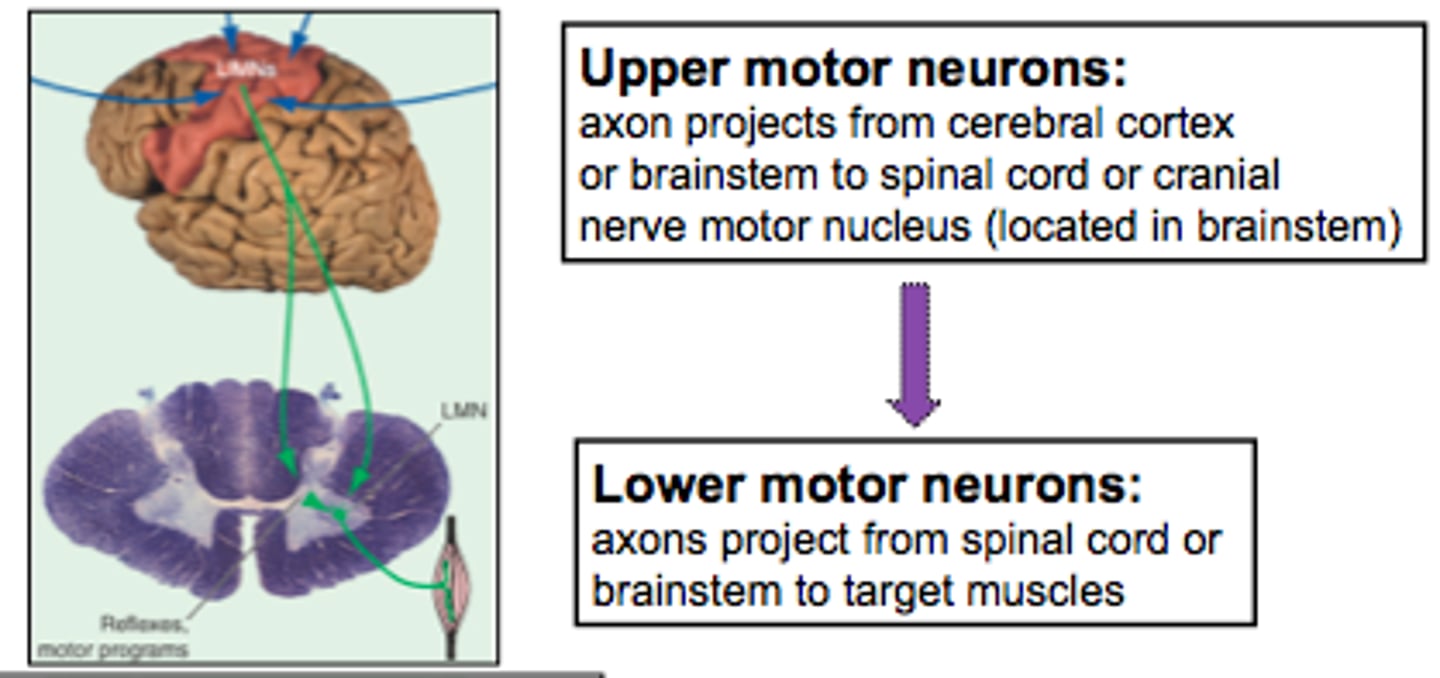
Upper Motor Neurons
Motor neurons in the central nervous system that control the lower motor neurons in the peripheral nervous system
Damage = partial paralysis with hyperflexia
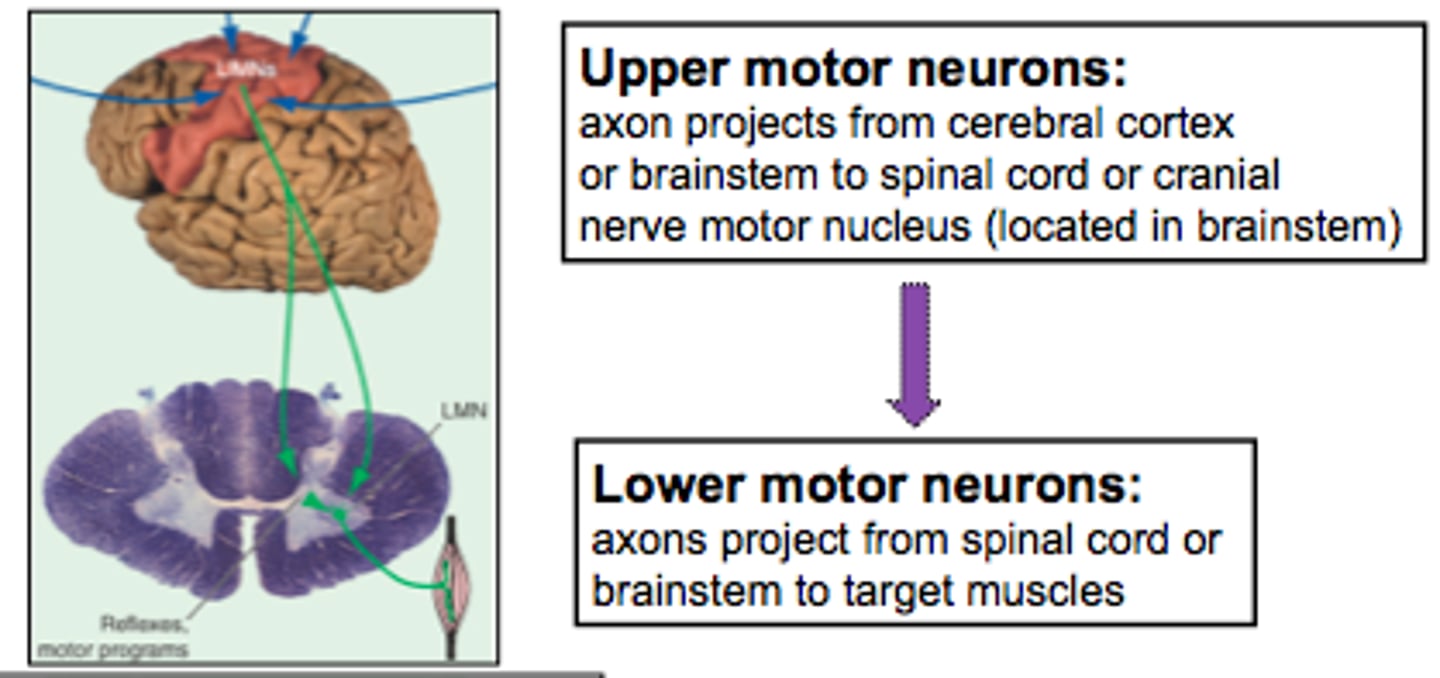
Pyramidal UMN
Projections from the cortex
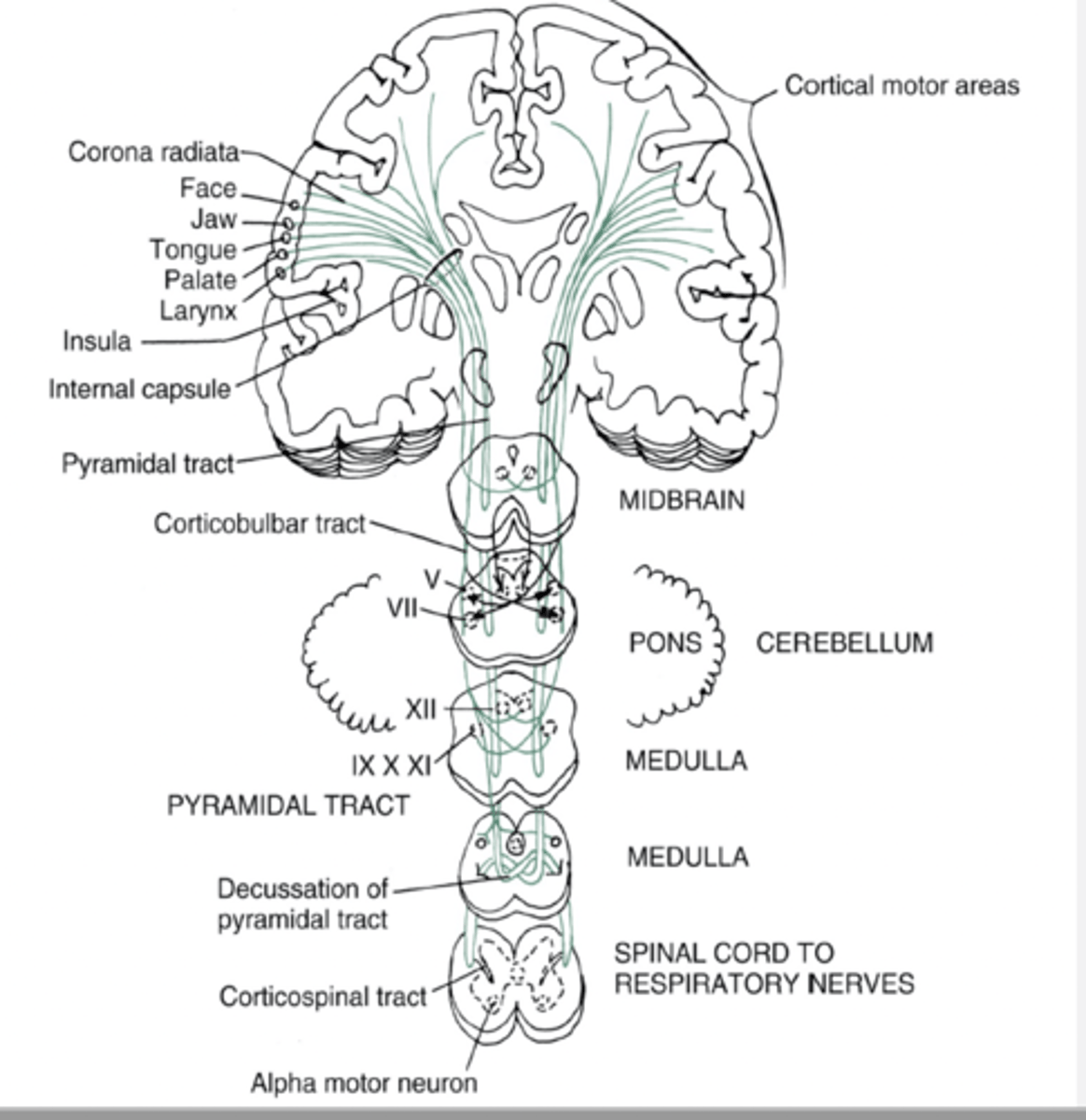
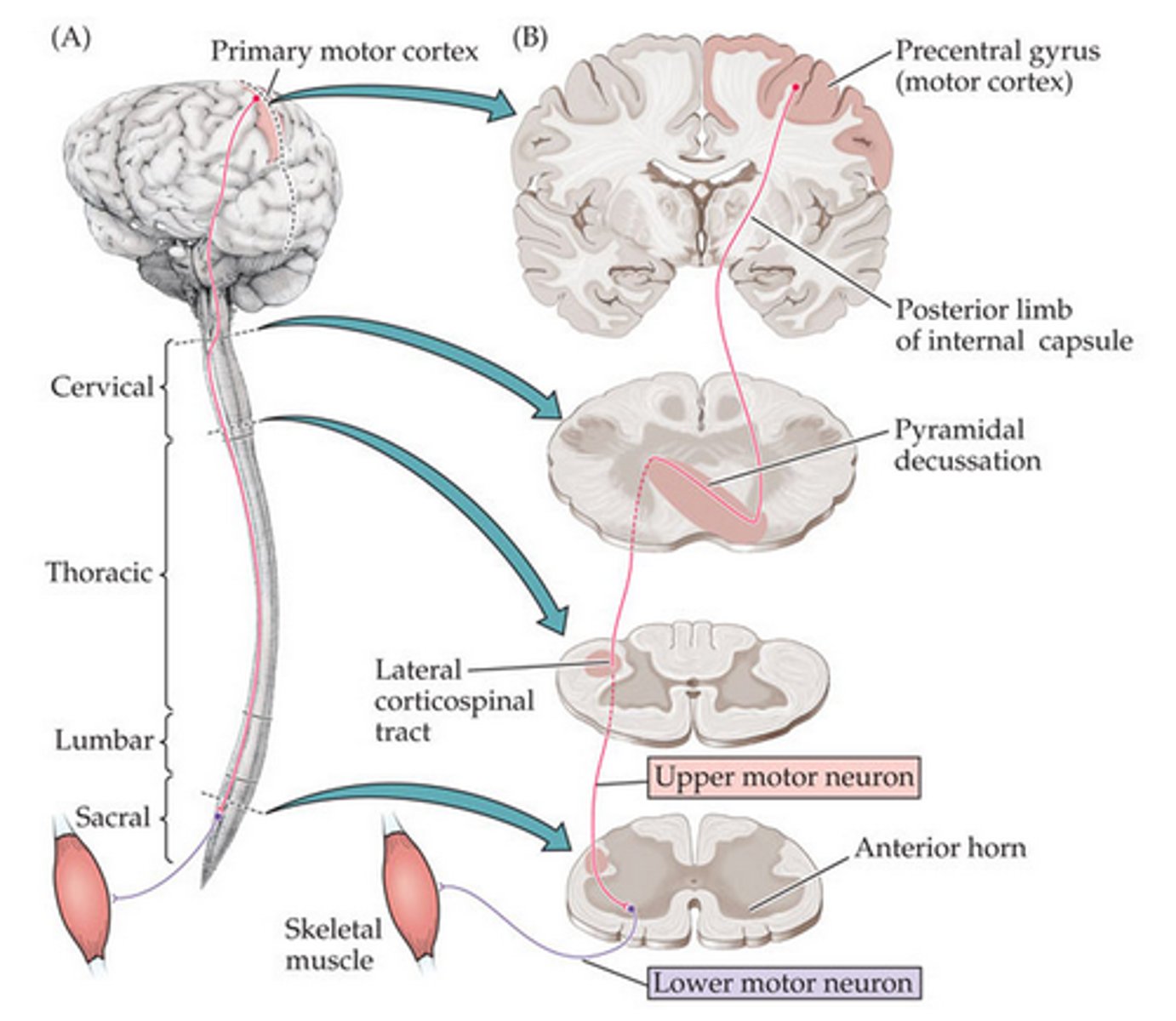
Corticospinal
Descending tract whose fibers conduct motor impulses to skeletal muscles
Synapse on LMN of the spinal cord
Lateral and ventral
Damage = contralateral hemiparesis of trunk and extremities
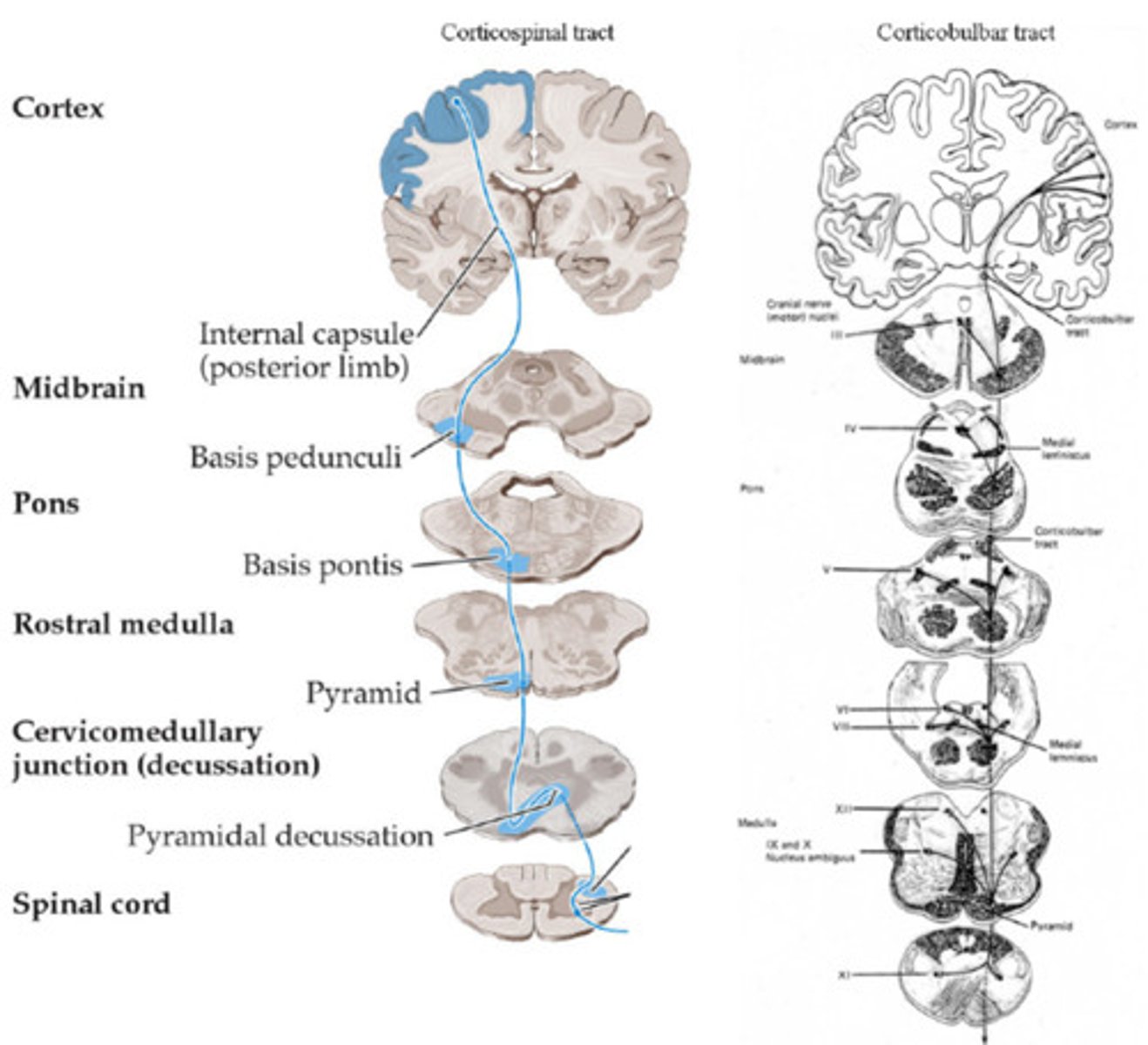
Corticobulbar
Direct control of movements in head and neck
Synapse on brainstem nuclei
Damage = contralateral weakness of lower face
Extrapyramidal UMN
Projections from the brainstem nuclei
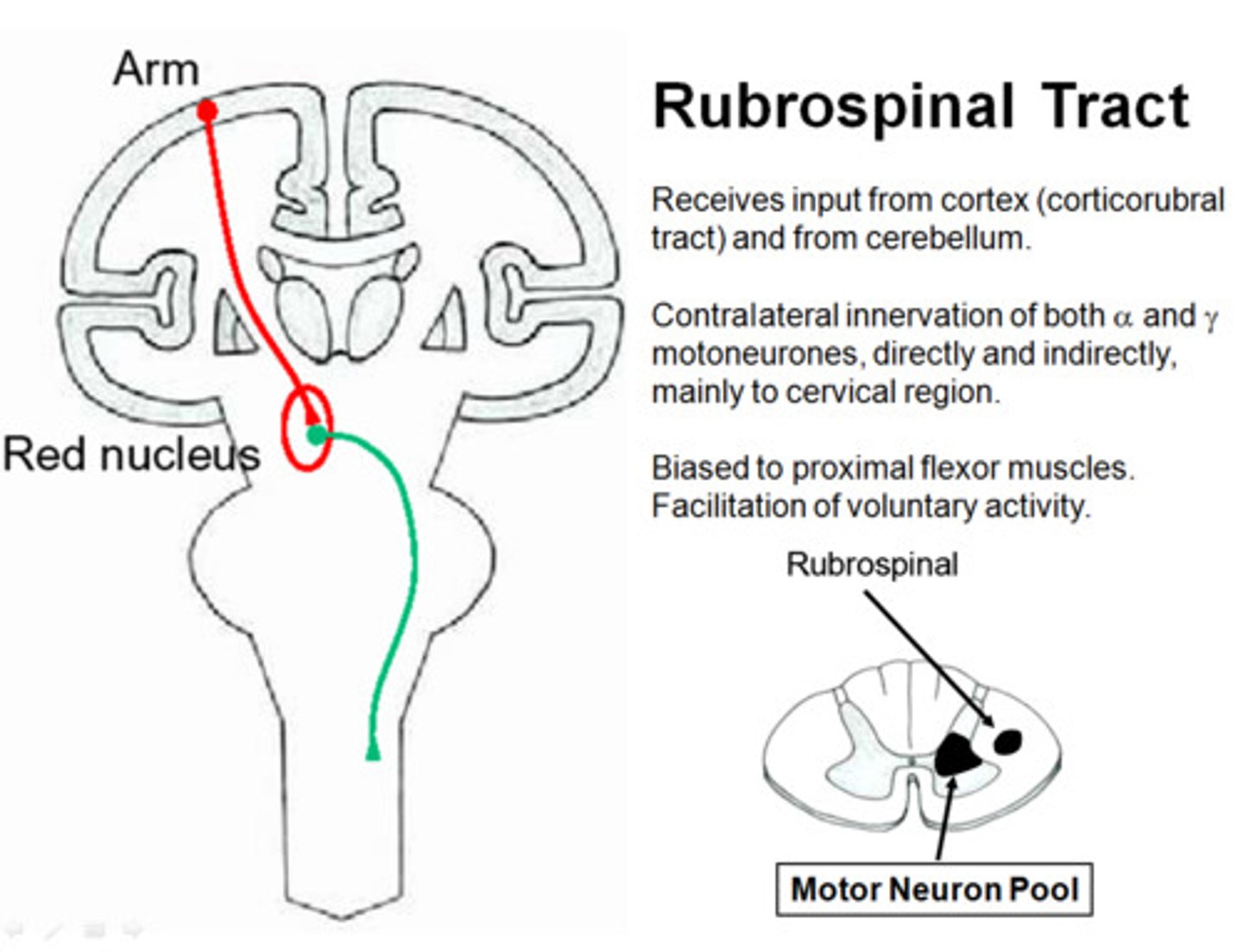
Rubrospinal
From the red nucleus to the spinal cord
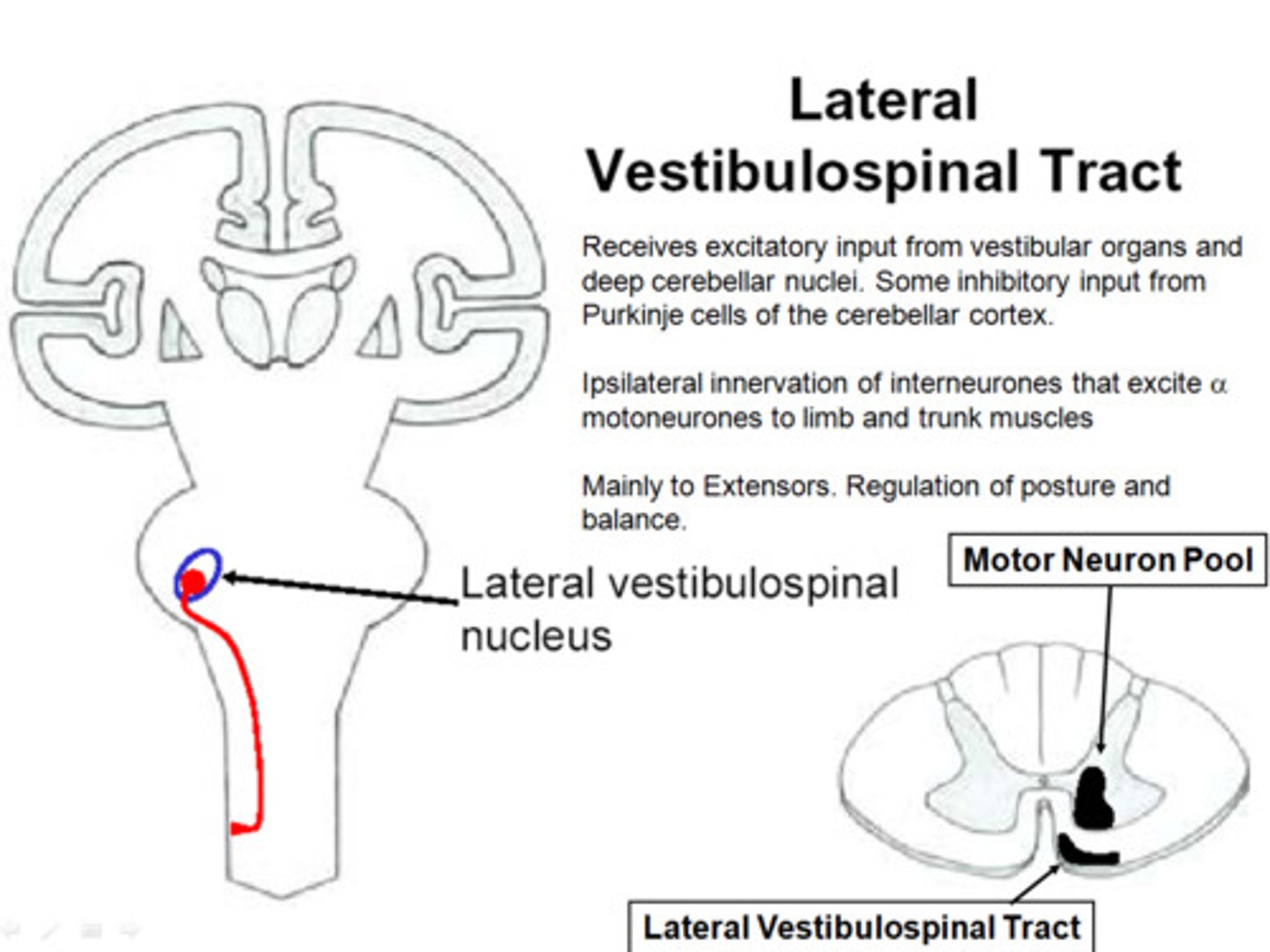
Vestibulospinal
From the vestibular nuclei to the spinal cord
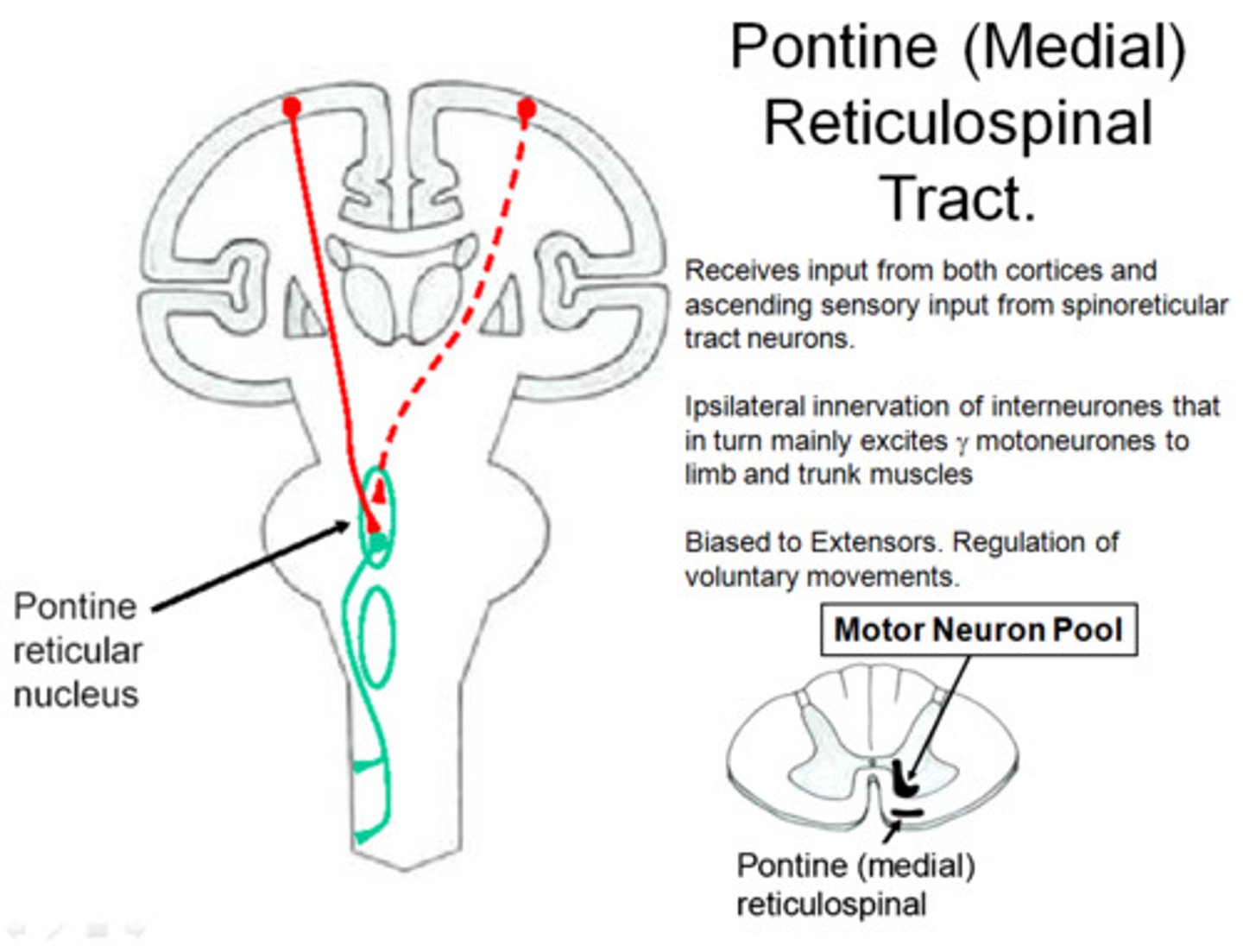
Reticulospinal
From the reticular nuclei to the spinal cord
Tectospinal
From the midbrain tectum to the spinal cord
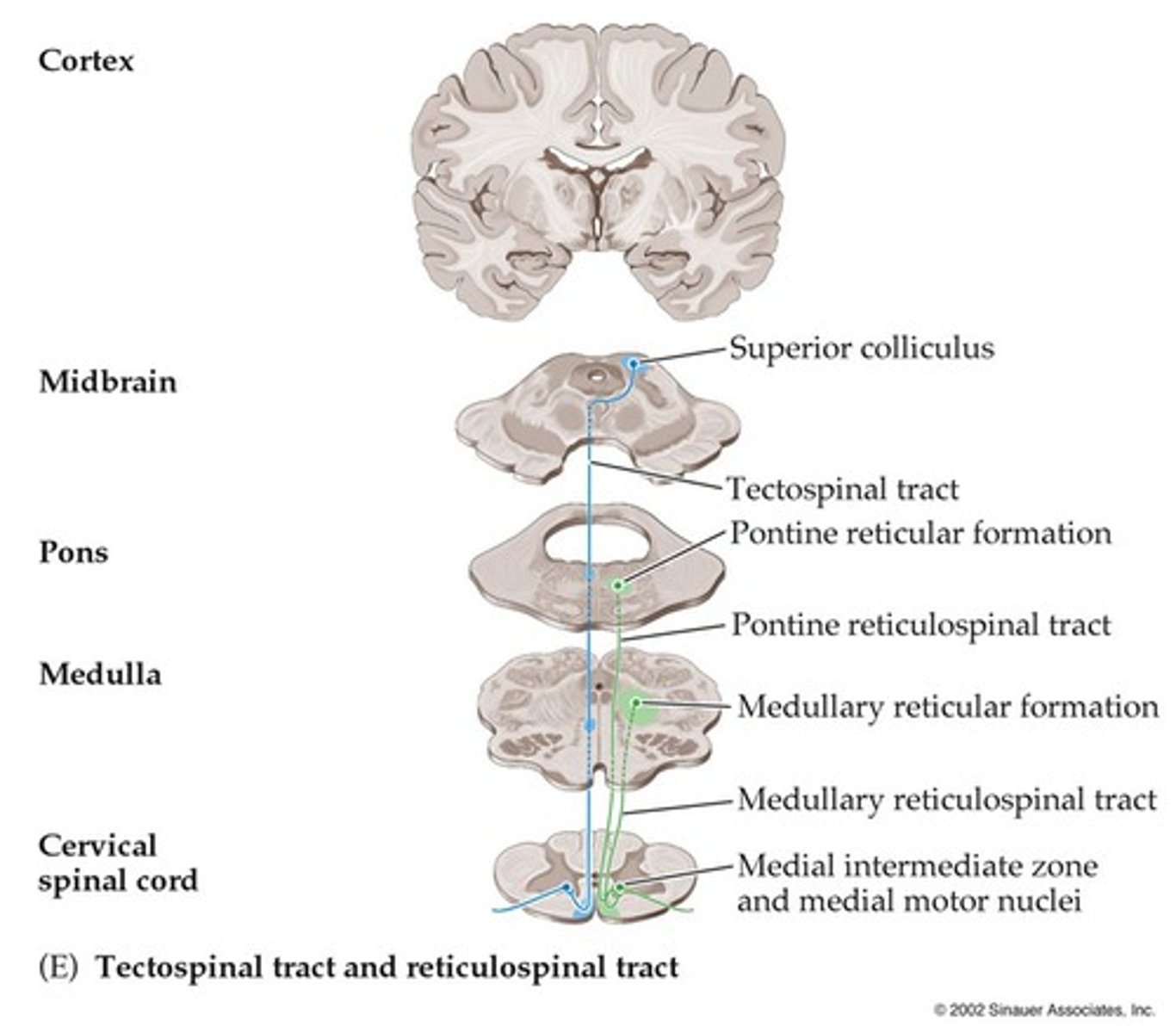
Lateral Corticospinal Tract
A set of axons from the primary motor cortex, surrounding areas, and midbrain area that is primarily responsible for controlling the peripheral muscles
85% cross in the caudal medulla
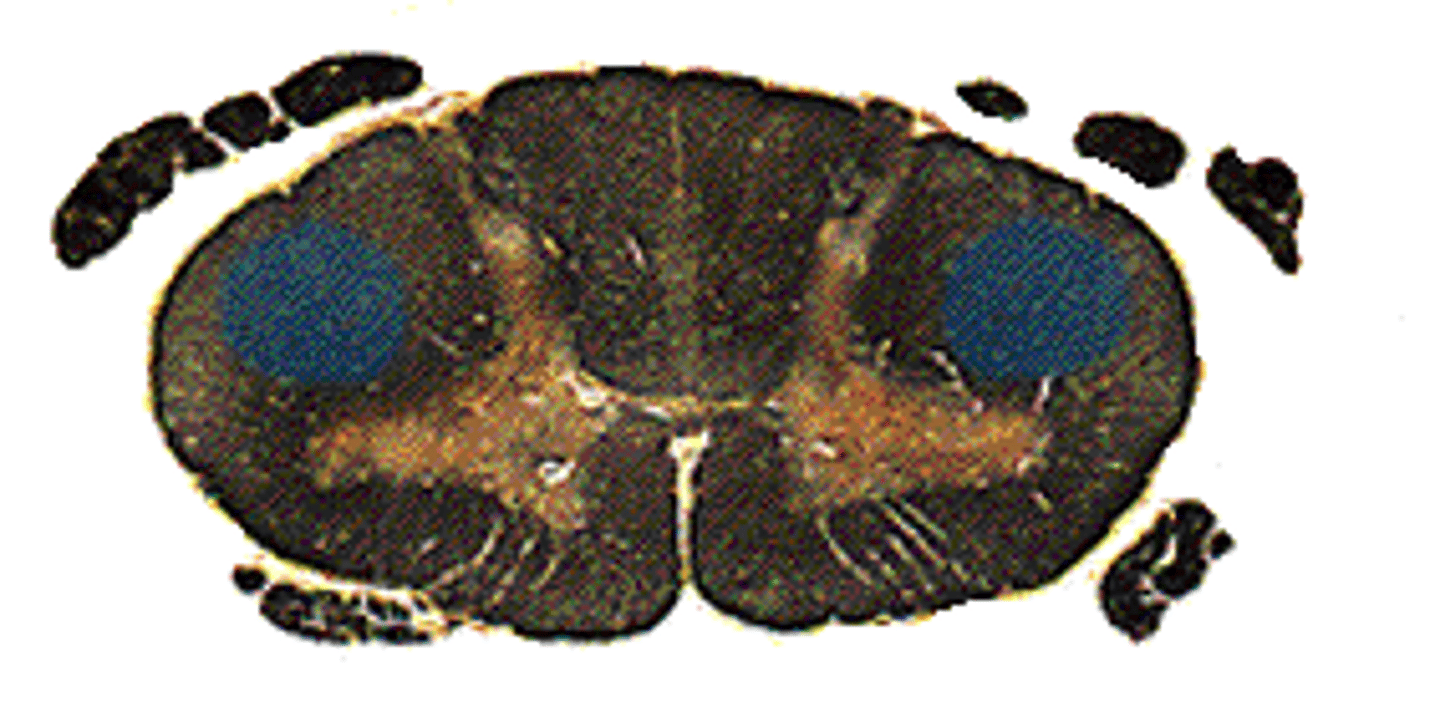
Ventral Corticospinal Tract
The system of axons that originates in the motor cortex and terminates in the ipsilateral ventral gray matter of the spinal cord; controls movements of the upper legs and trunk
Continues uncrossed
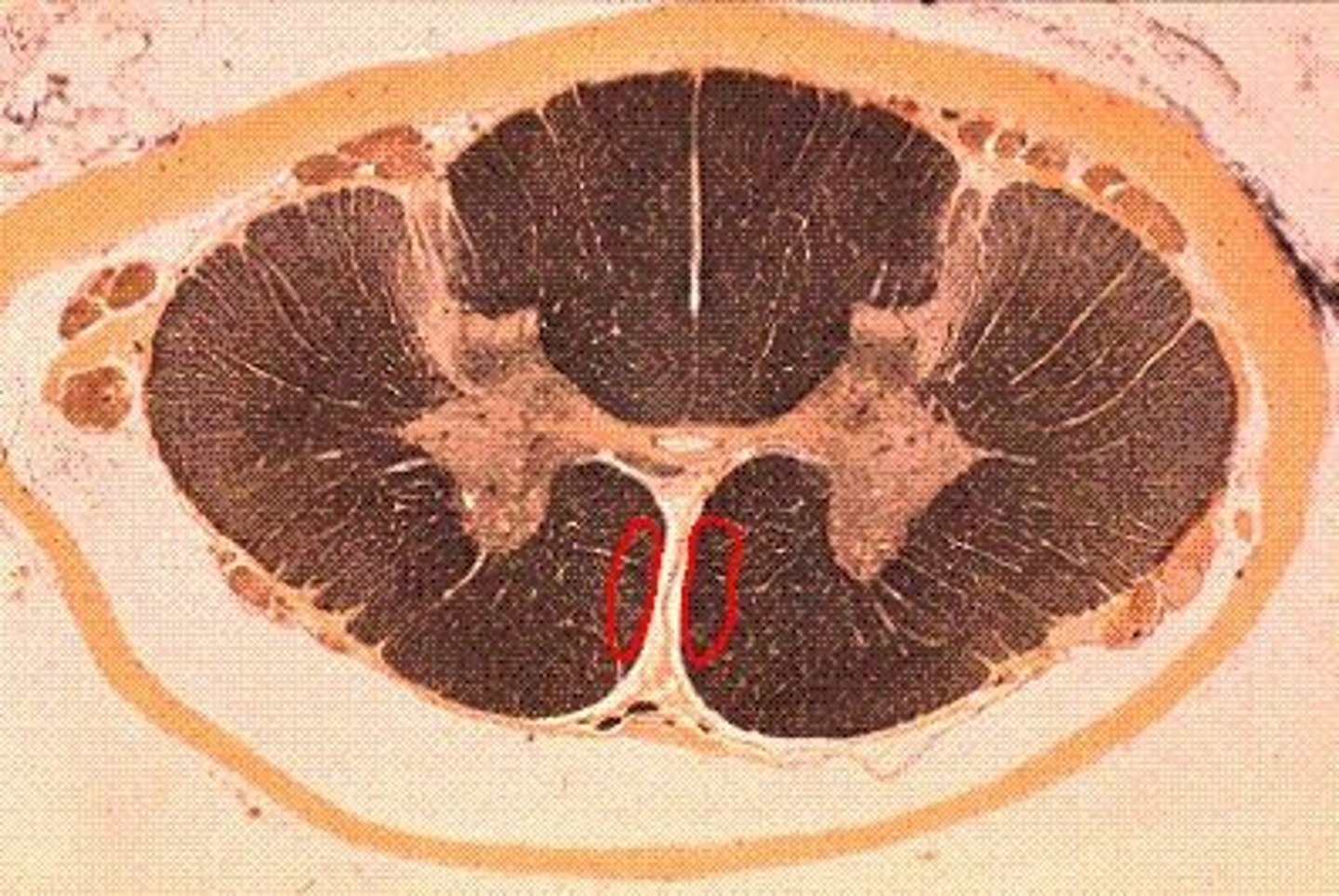
Pyramidal System
The motor system that includes neurons within the cerebral cortex and their axons, which form the pyramidal tract.
Originates from neurons in the primary motor cortex, premotor cortex, supplementary motor cortex, and somatosensory cortex
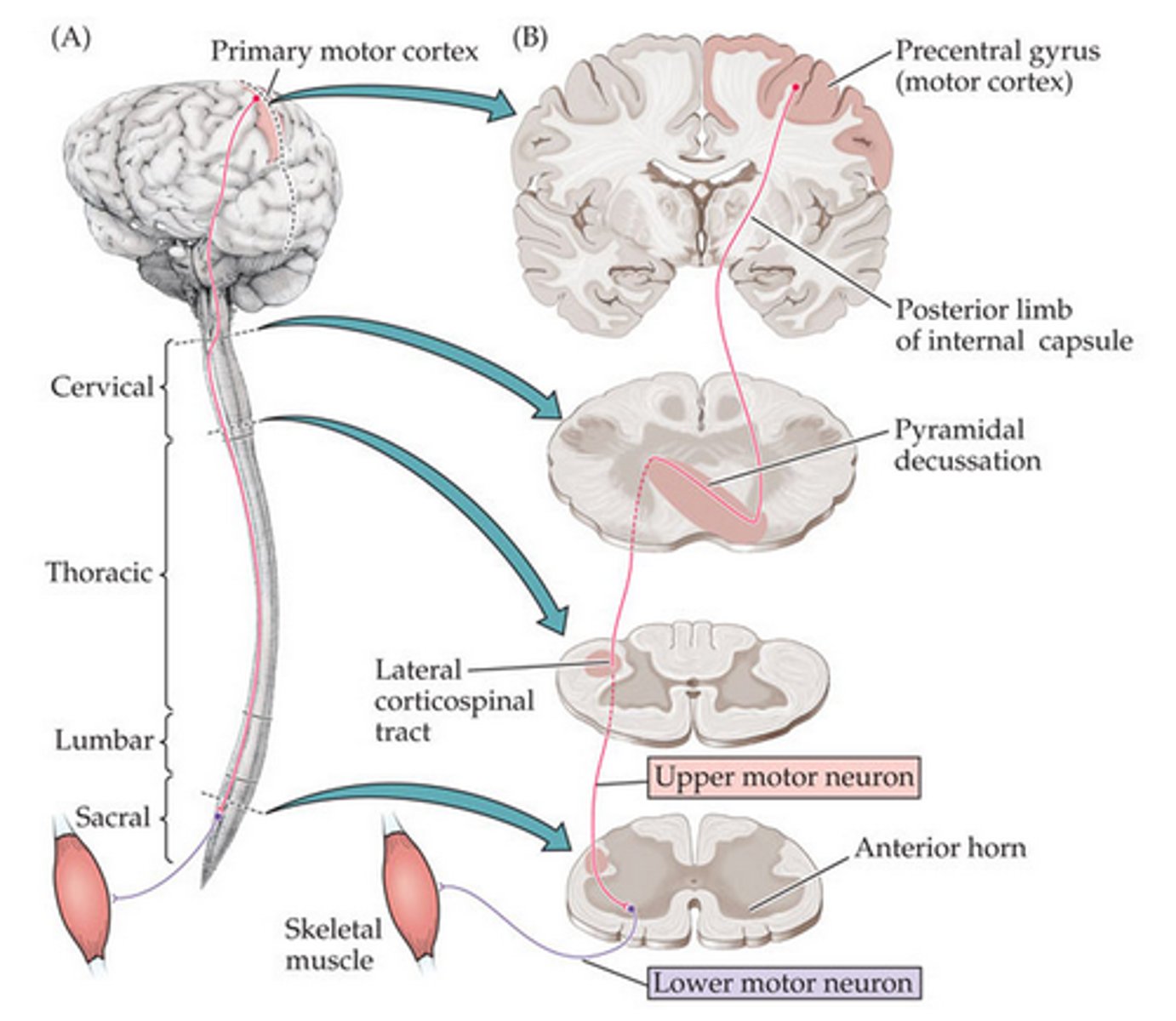
Internal Capsule
A large collection of axons that connects the telencephalon with the diencephalon
Pyramidal tracts, among other things, pass through here
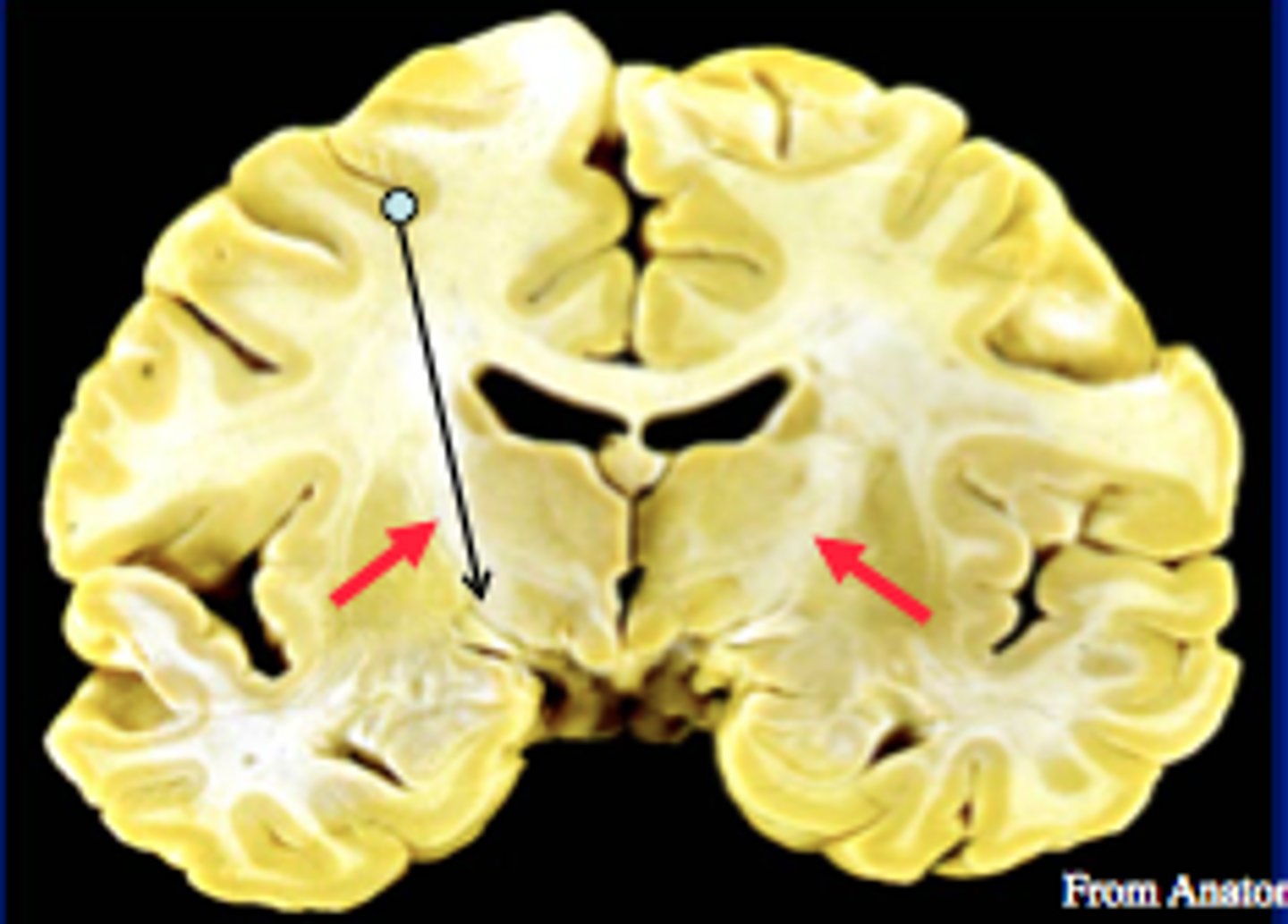
Corona Radiata
All the fibers connecting cortical and subcortical regions also pass through here
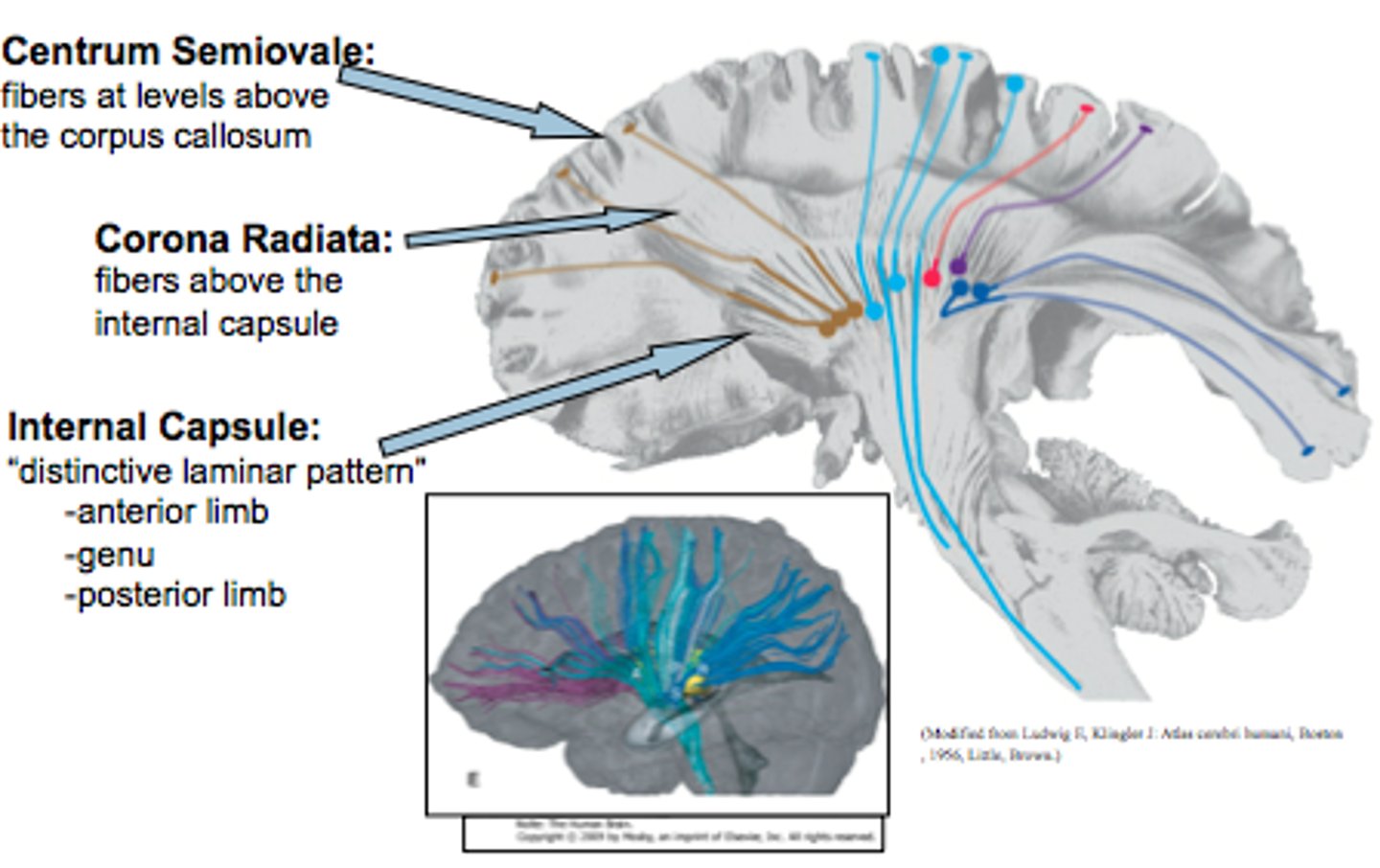
Motor Homunculus
Broad areas of primary motor cortex devoted to controlling movements of different body regions
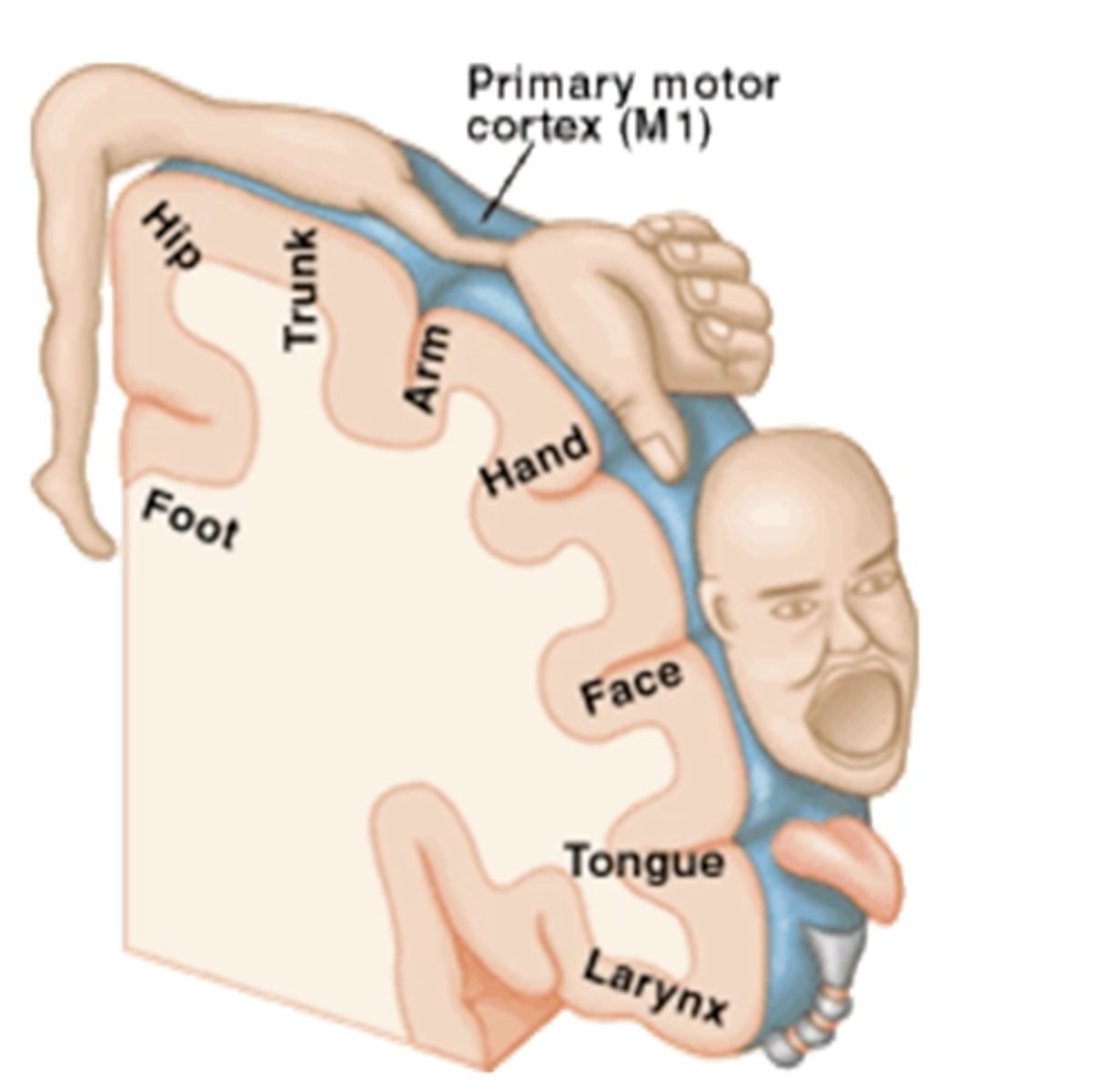
Descending UMN of the Extrapyramidal System
Fibers from various regions of the brainstem descend and synapse on LMN
More diffuse and multisynaptic than corticospinal tracts
Involved in non-skilled, voluntary movements
Influenced by cerebral cortex via descending fibers synapsing in the brainstem
Rubrospinal Tract
From red nucleus
Crosses in the midbrain
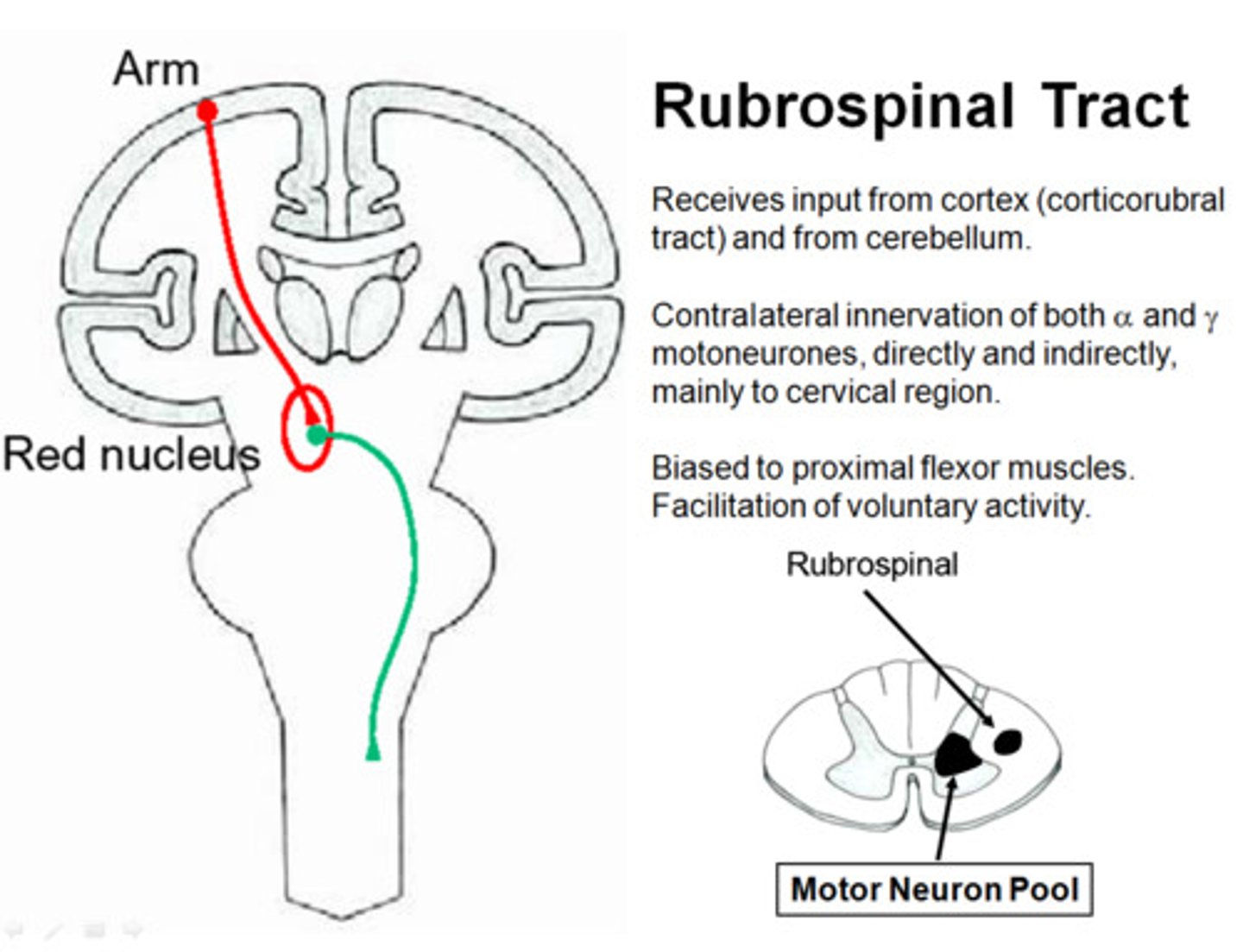
Pontine Reticulospinal Tract
A tract originating in the pontine reticular formation and terminating in the spinal cord, involved in the control of movement.
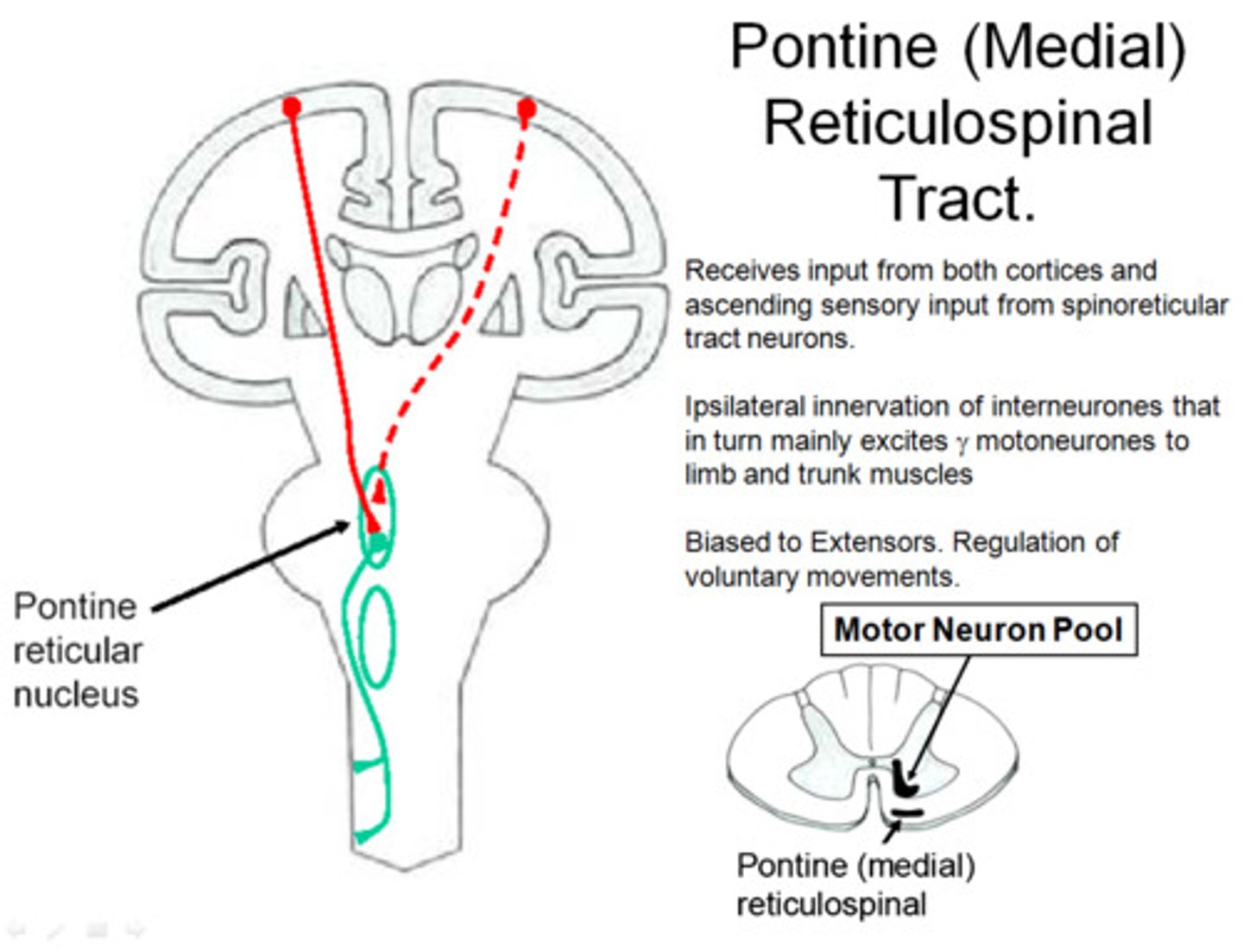
Medullary Reticulospinal Tract
A tract originating in the medullary reticular formation and terminating in the spinal cord; involved in the control of movement.
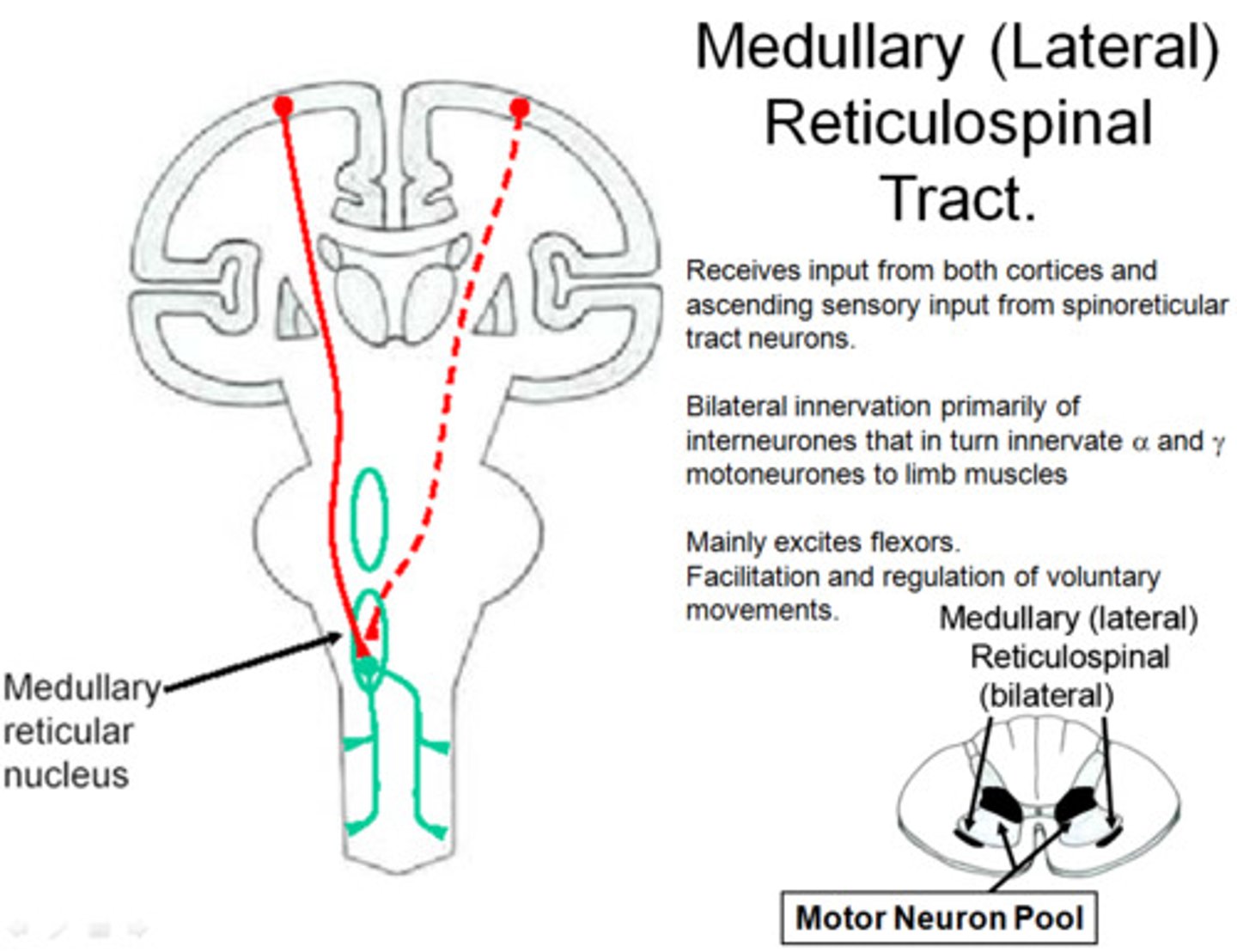
Lateral Vestibulospinal Tract
Axons arising in the lateral vestibular nucleus that project ipsilaterally to facilitate lower motor neurons to extensor muscles and simultaneously inhibit lower motor neurons to flexor muscles via interneurons.
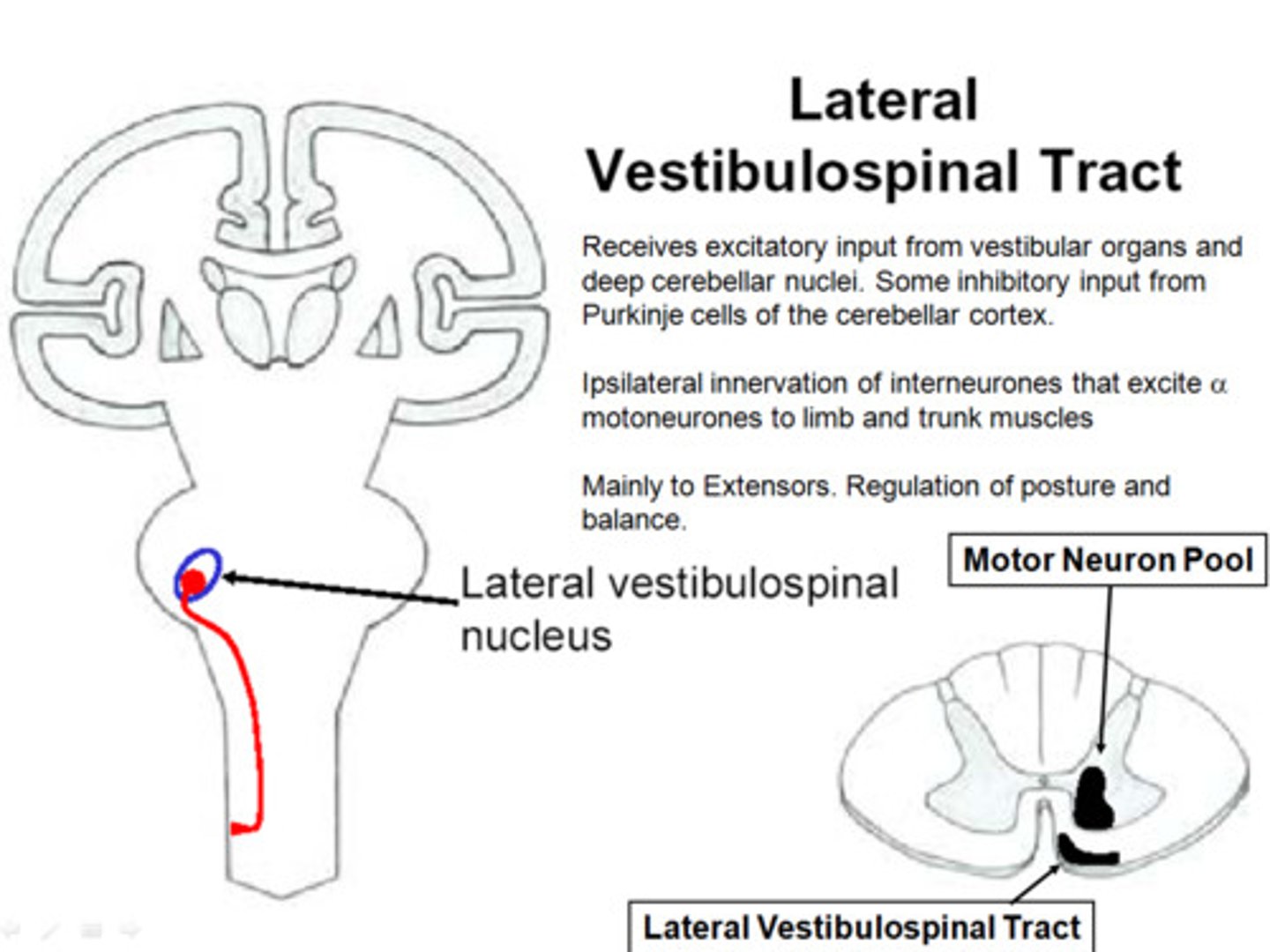
Medial Vestibulospinal Tract
Axons arising in the medial vestibular nucleus that project bilaterally to the cervical and thoracic spinal cord. Affects the activity of lower motor neurons that control the neck and upper back muscles.
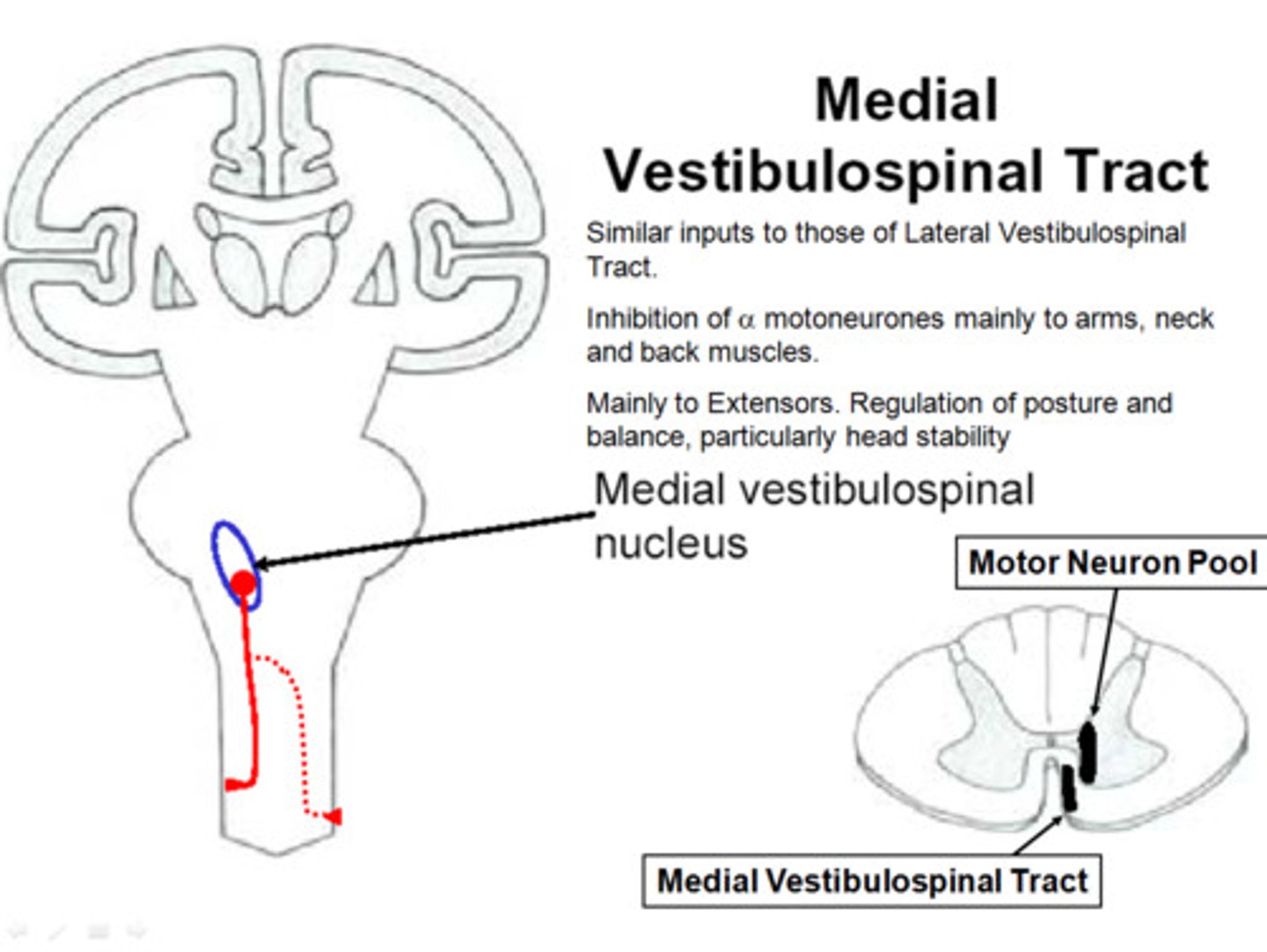
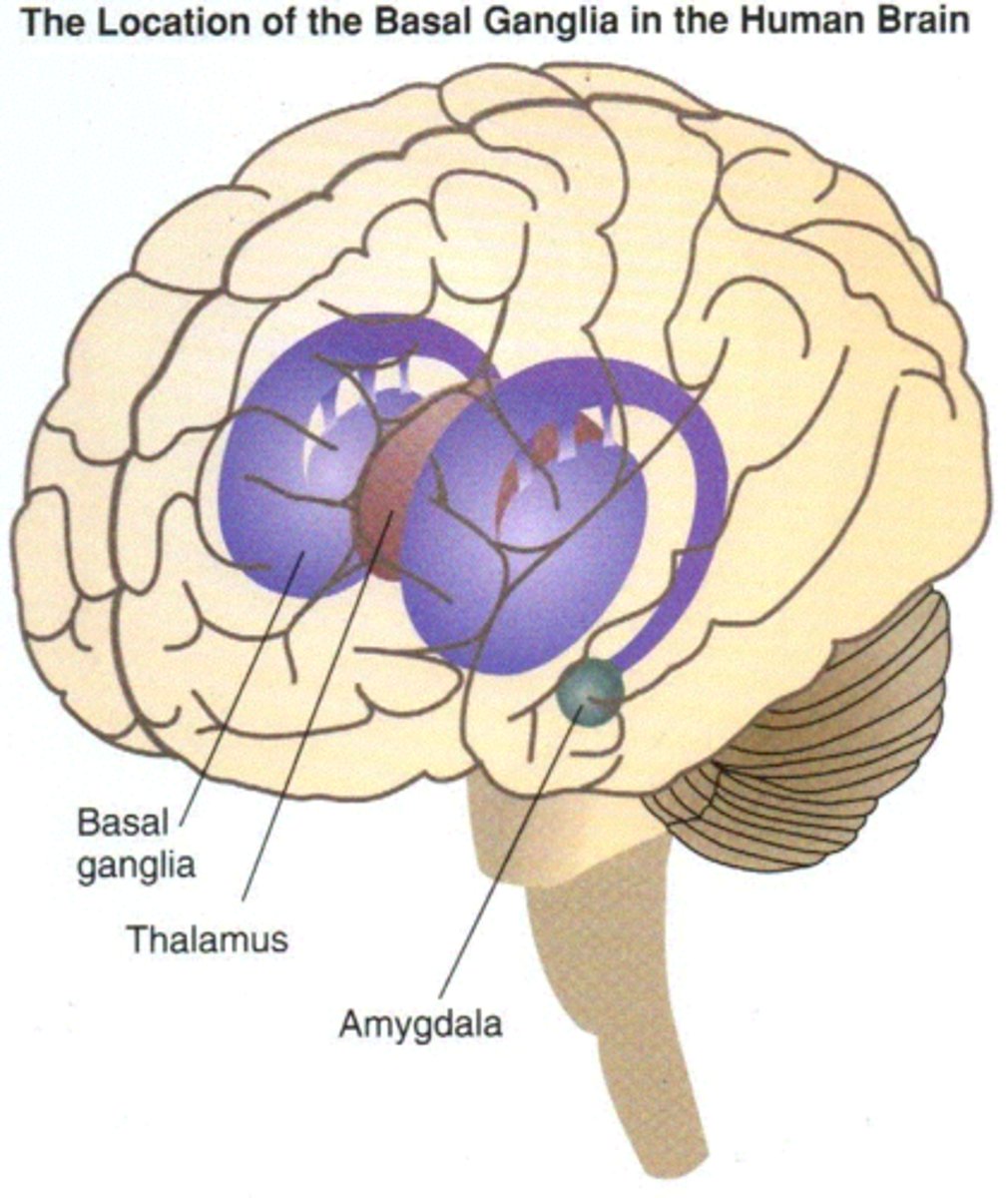
Components of the Basal Ganglia
Caudate nucleus
Putamen
Globus pallidus
Subthalamic nucleus (in diencephalon)
Substantia nigra (in midbrain)
Thalamus
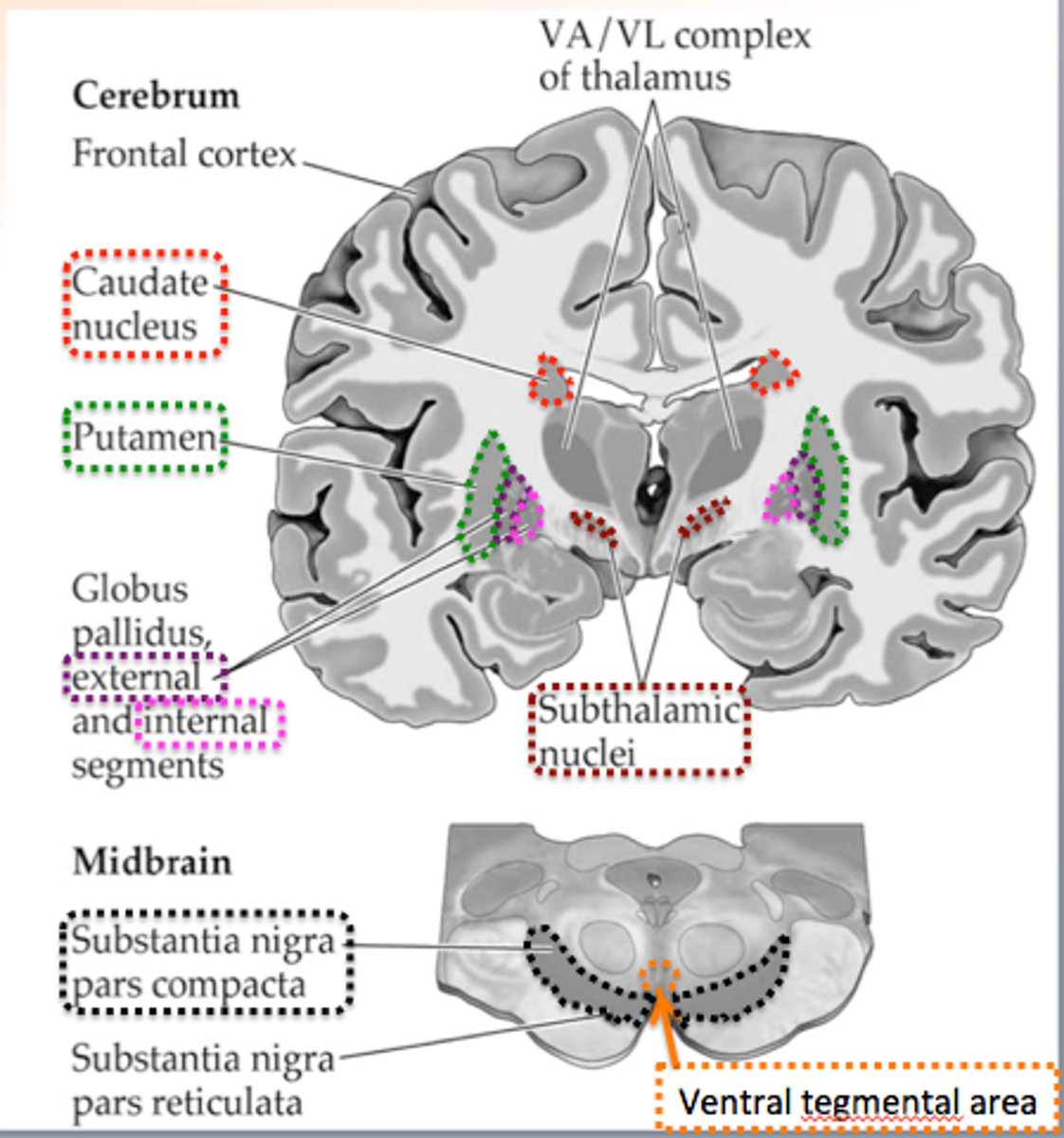
Lenticular Nucleus
Consists of the putamen and globus pallidus
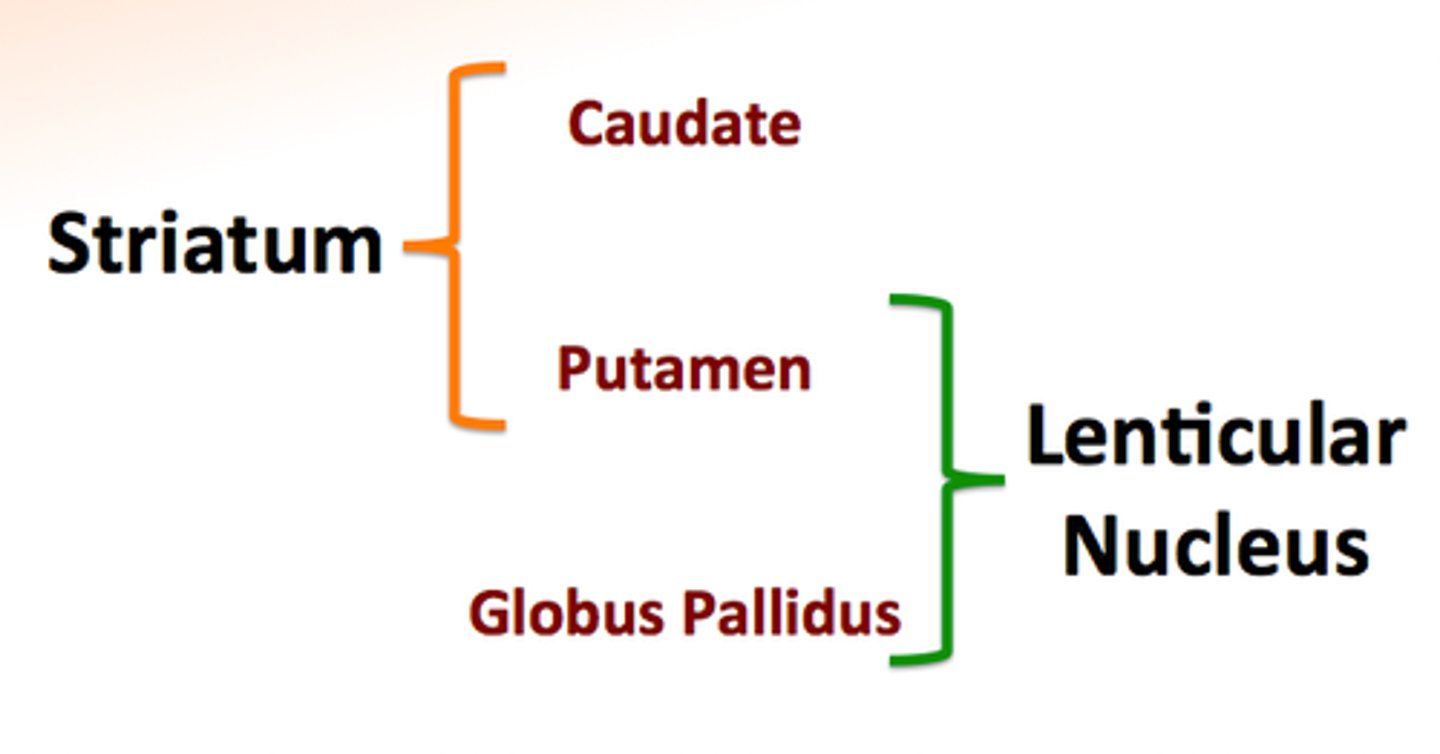
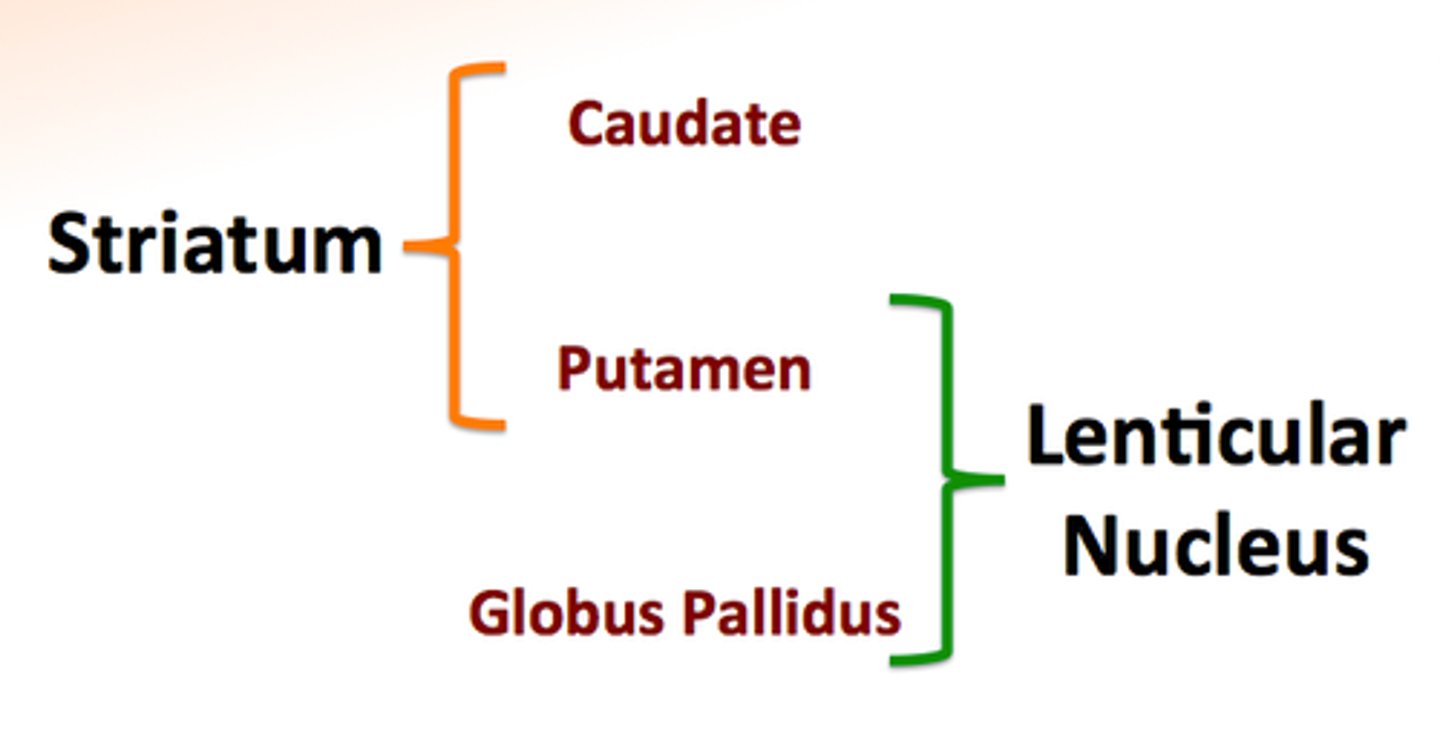
Striatum
Consists of the caudate nucleus and putamen
Substantia Nigra
An area of the midbrain that is involved in motor control and contains a large concentration of dopamine-producing neurons
Largest nucleus in the midbrain
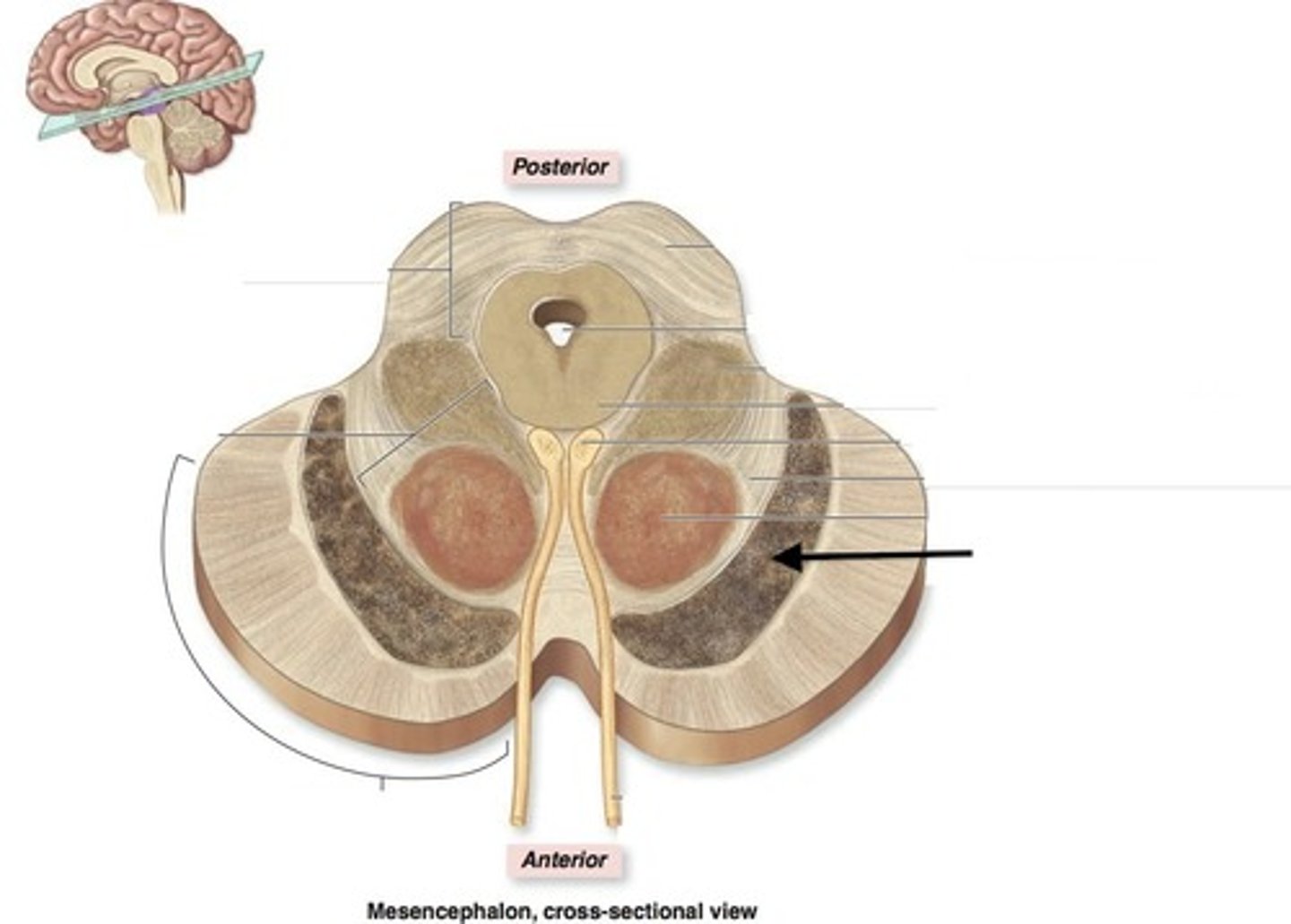
Substantia Nigra Degeneration
Parkinson's disease

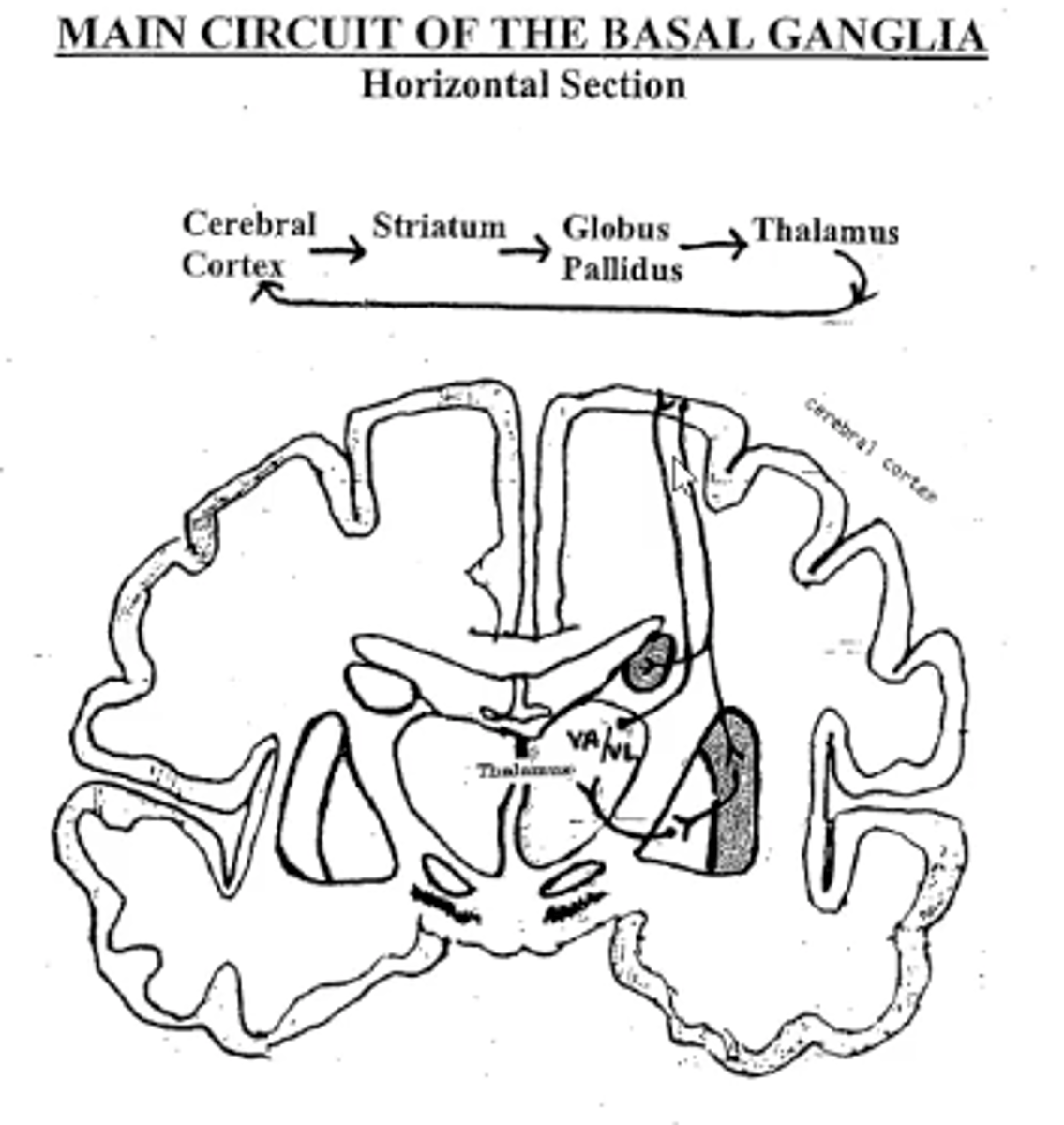
Main Circuit of the Basal Ganglia
Cerebral cortex -->
Striatum -->
Globus pallidus -->
Thalamus -->
Cerebral cortex
Subthalamus
Subthalamus: origin of neuroblasts that form the globus pallidus
A stroke in this region results in hemiballism
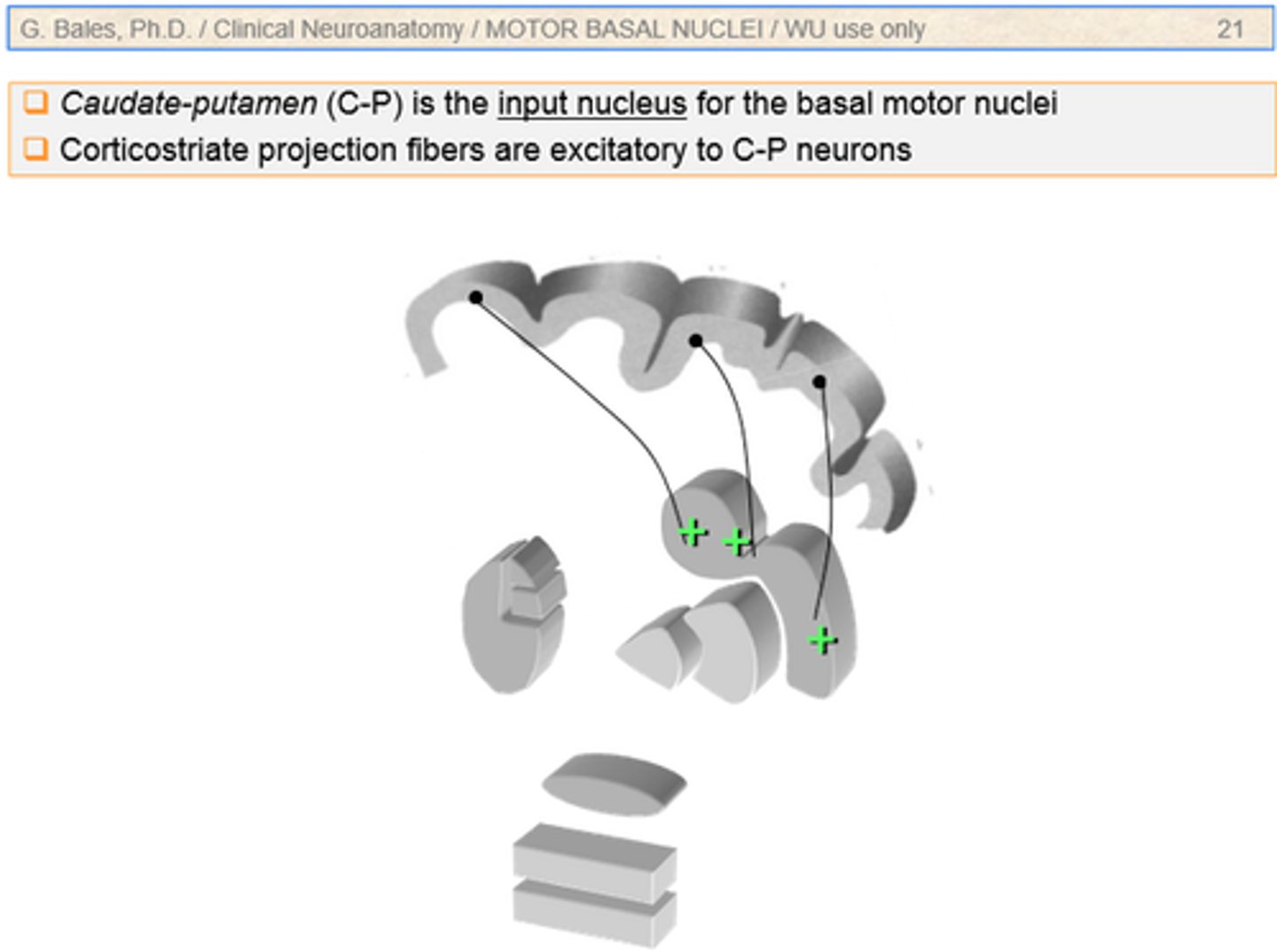
Corticostriate Fibers
Originate all 4 lobes
Terminate in striatum (caudate, putamen)
Basal Ganglia Ipsilateral Connections
Cerebral cortex
Thalamus
Basal Ganglia Contralateral Connections
Side of the body
Hypertonia
Increase in muscle tone
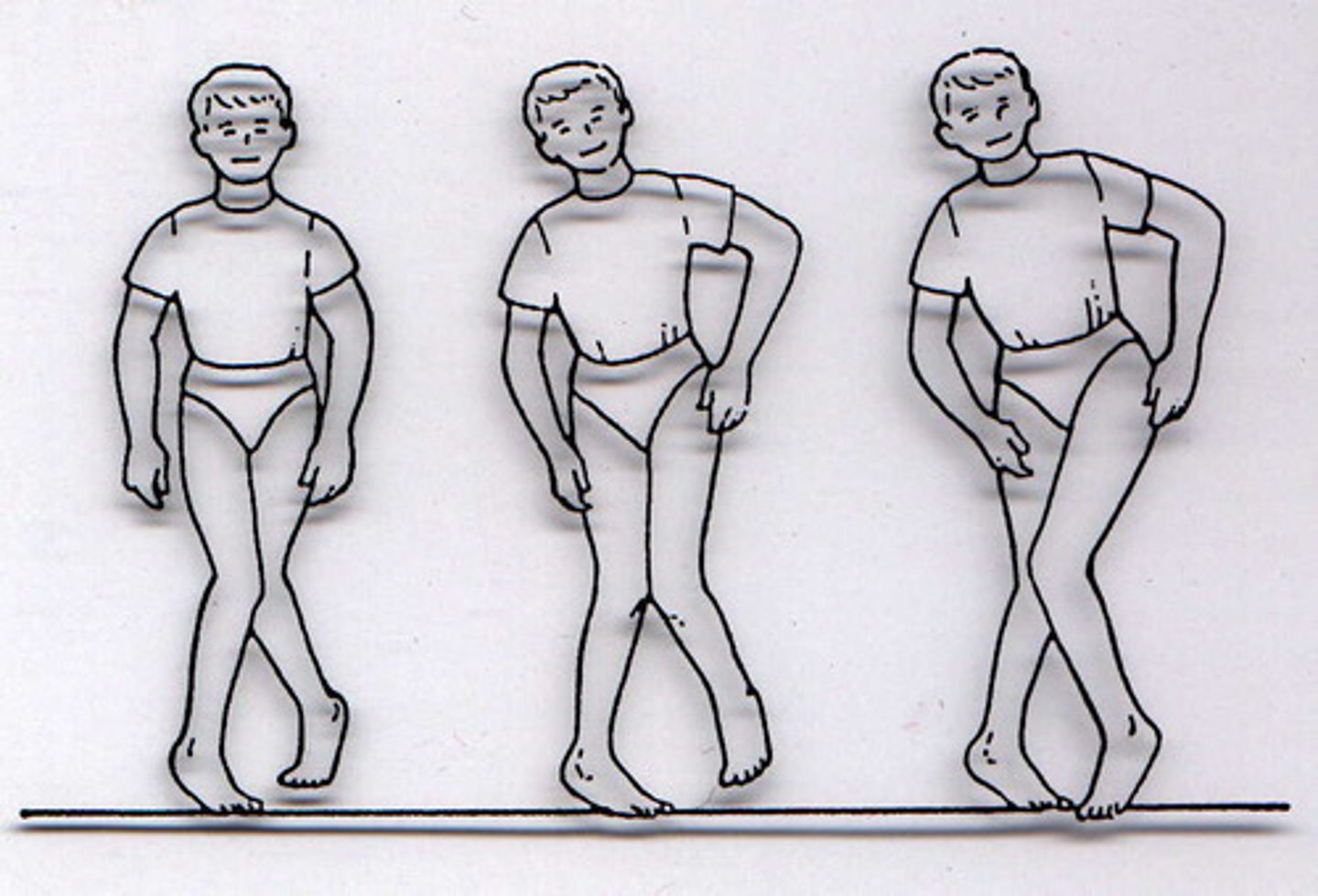
Hypotonia
Decrease in muscle tone
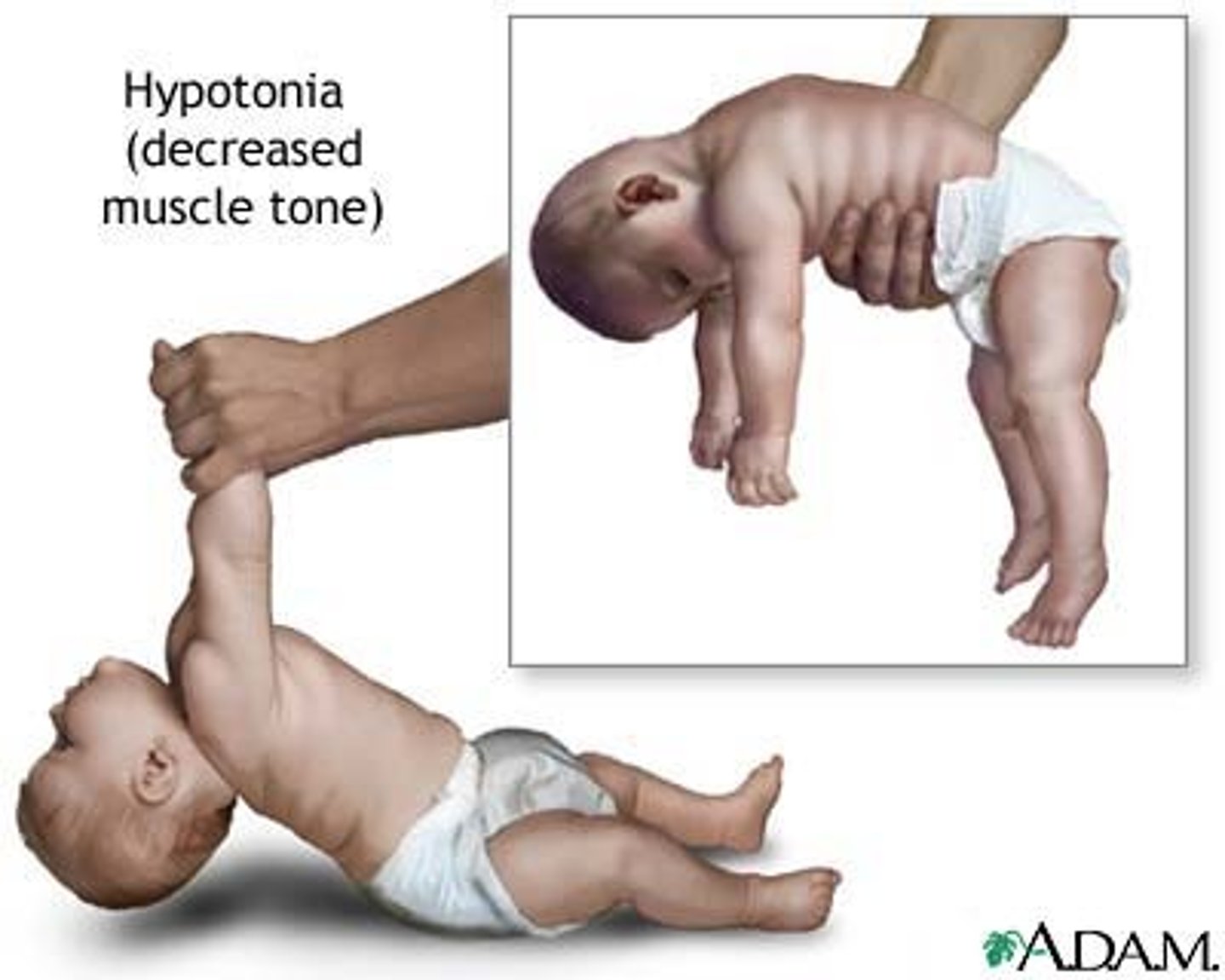
Dyskinesias
Movement disorders caused by lesions in the basal nuclei
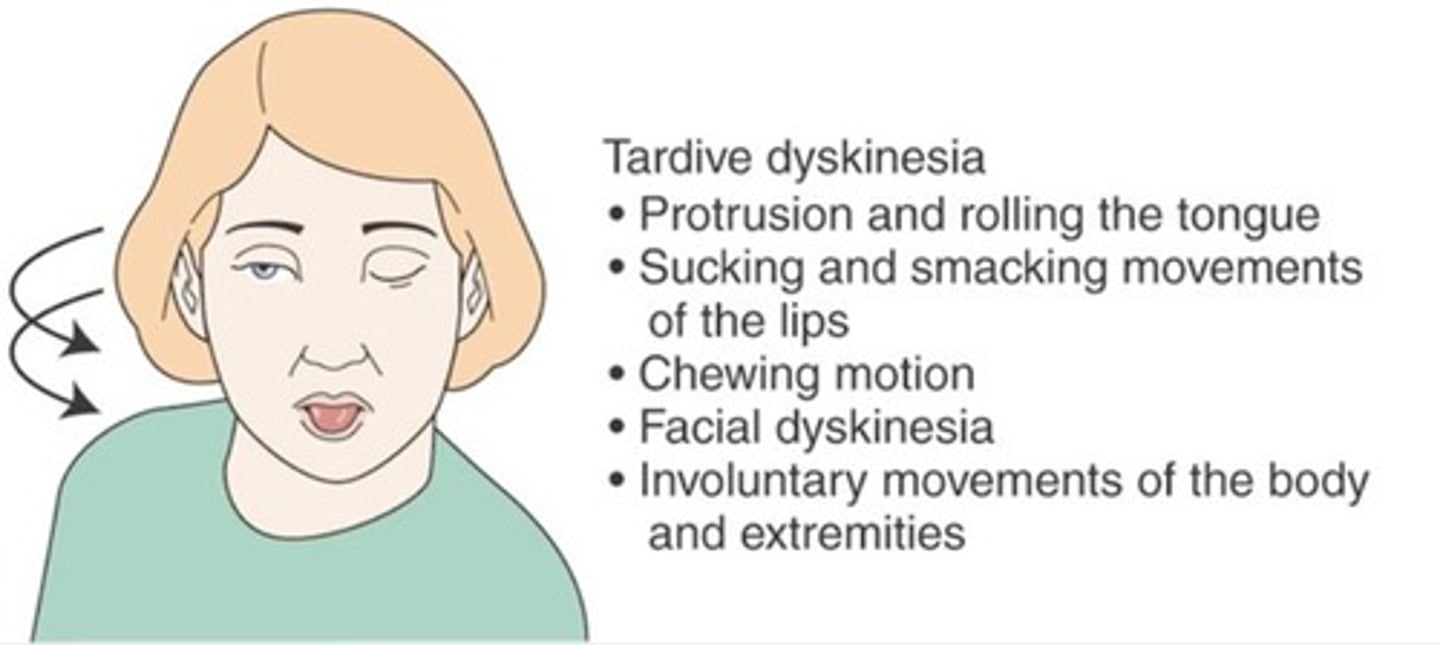
Resting Tremor
Rhythmic oscillations of the hand or head
Chorea
Sudden, rapid, jerky, purposeless movement involving limbs, trunk, or face

Athetosis
Bizarre, slow, twisting, writhing movement, resembling a snake or worm
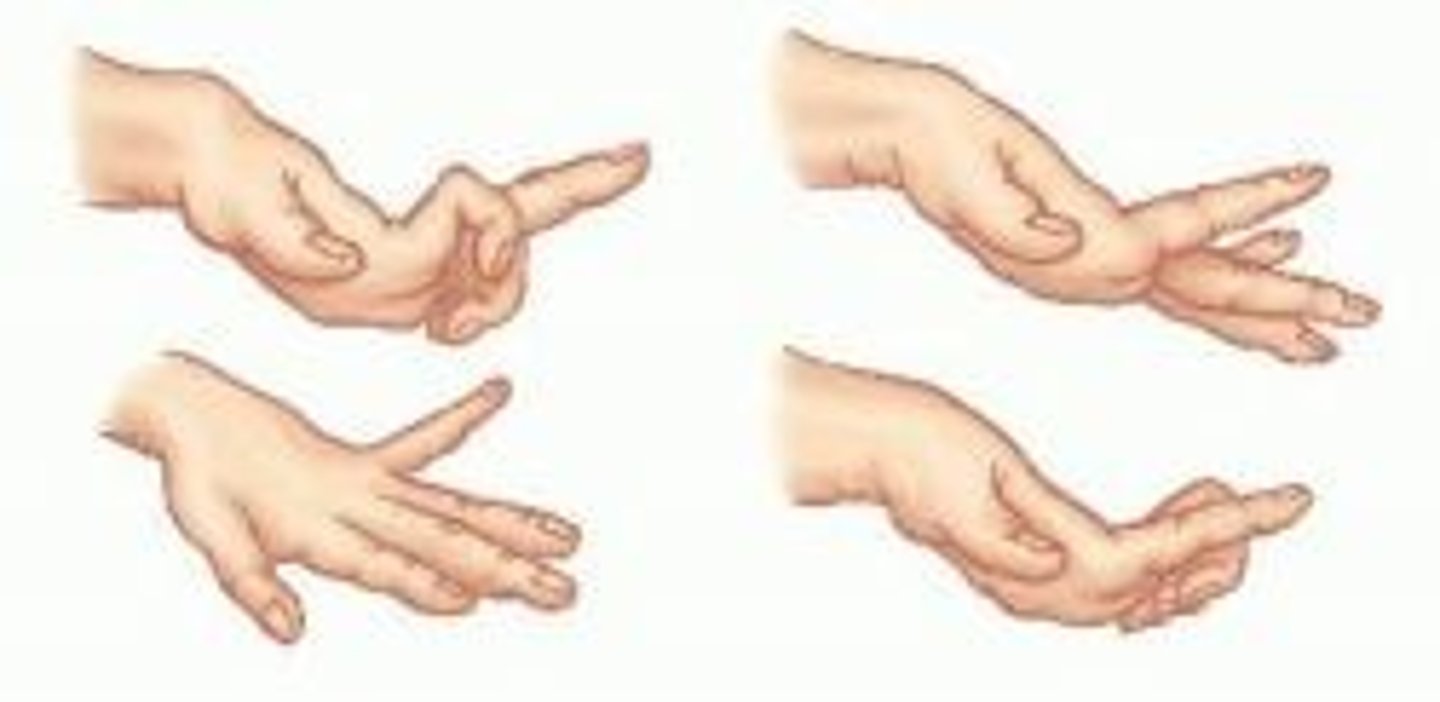
Dystonia
A condition of abnormal muscle tone that causes slow, sustained contractions of the head and trunk
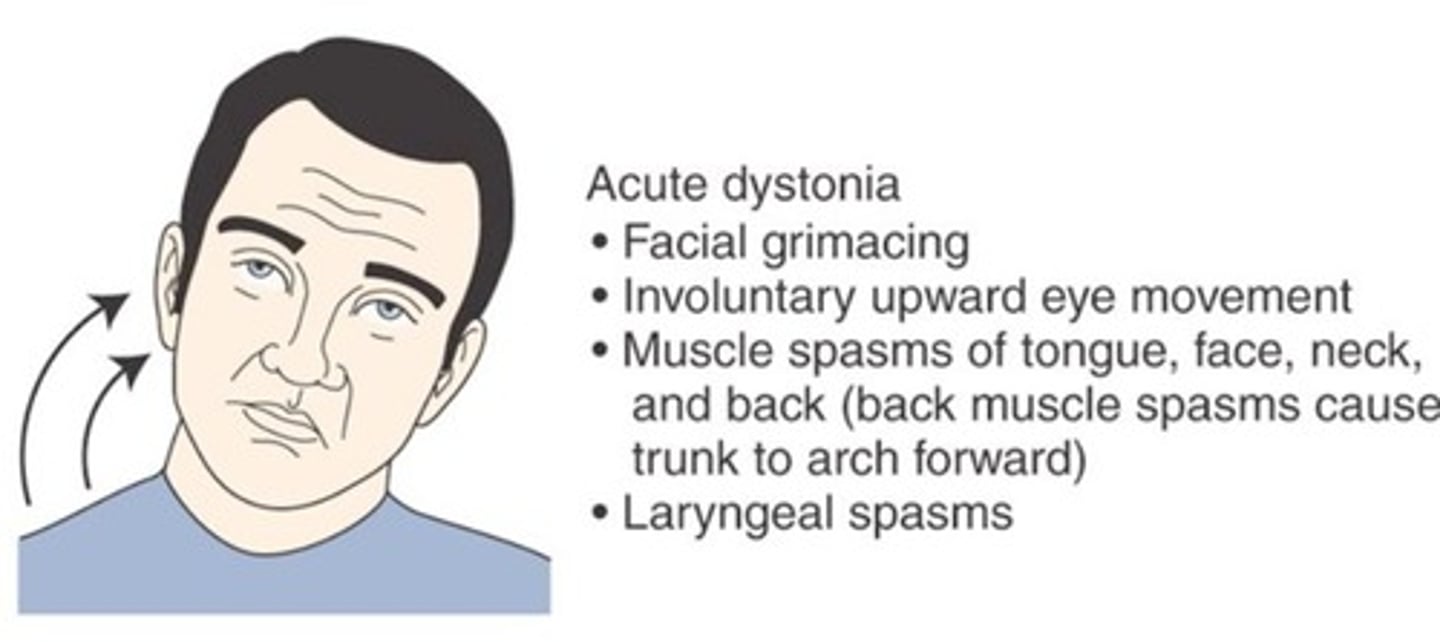
Ballism
A movement disorder caused by damage to the subthalamus, characterized by violent, flinging movements of the extremities.
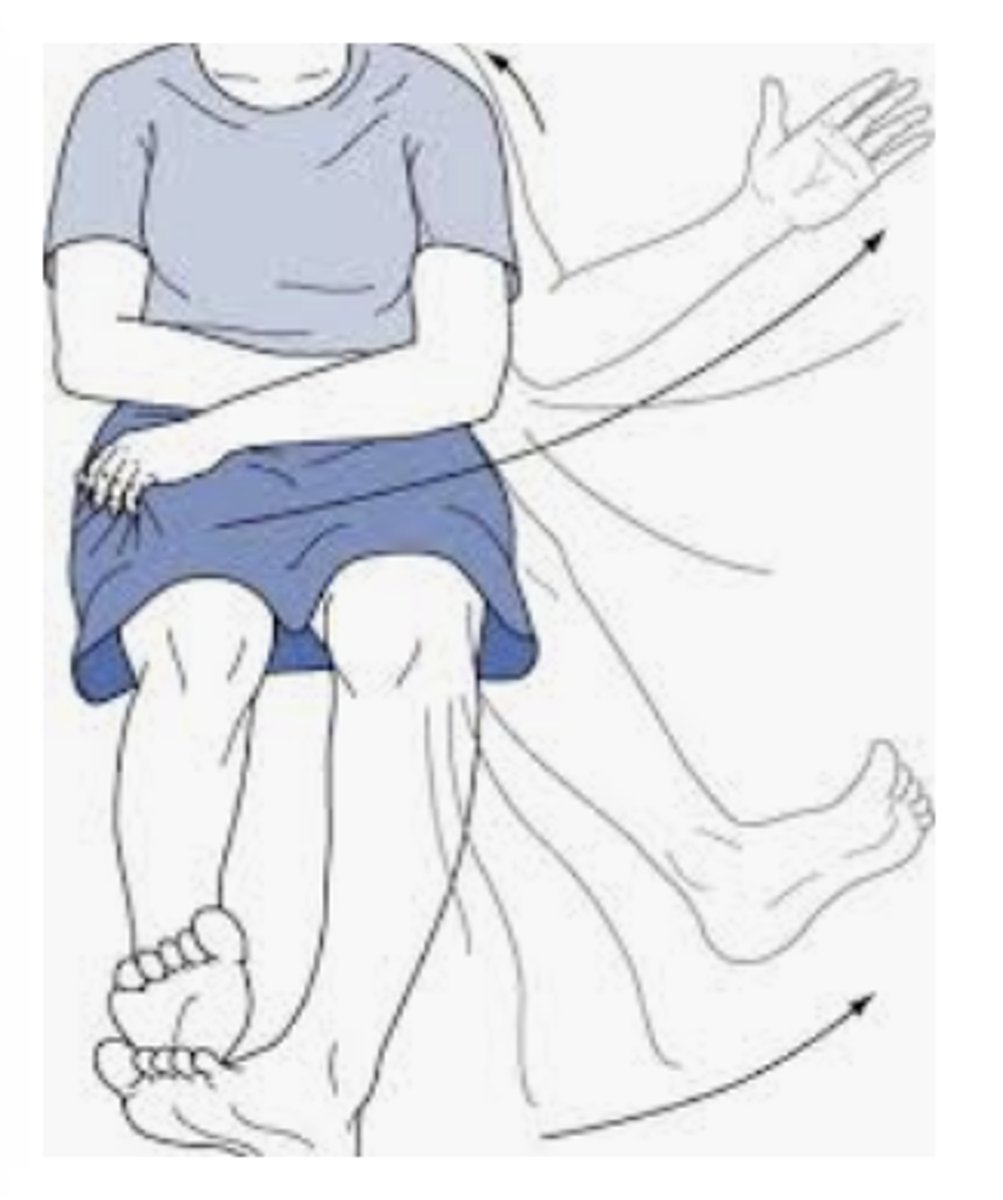
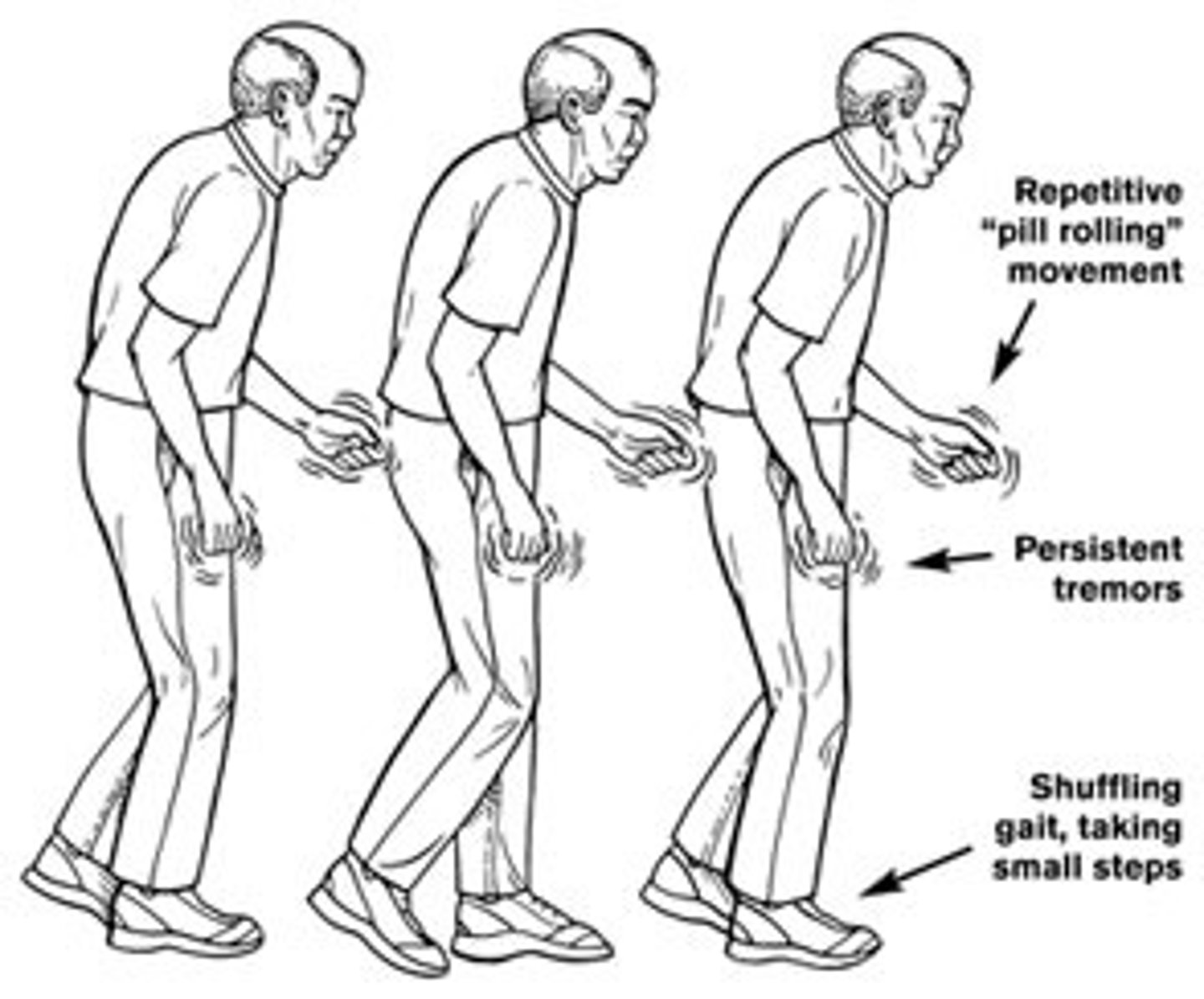
Parkinson's Disease
A slow, progressive neurological disease caused by degeneration of dopaminergic neurons in the substantia nigra - results in depletion of dopamine in the striatum
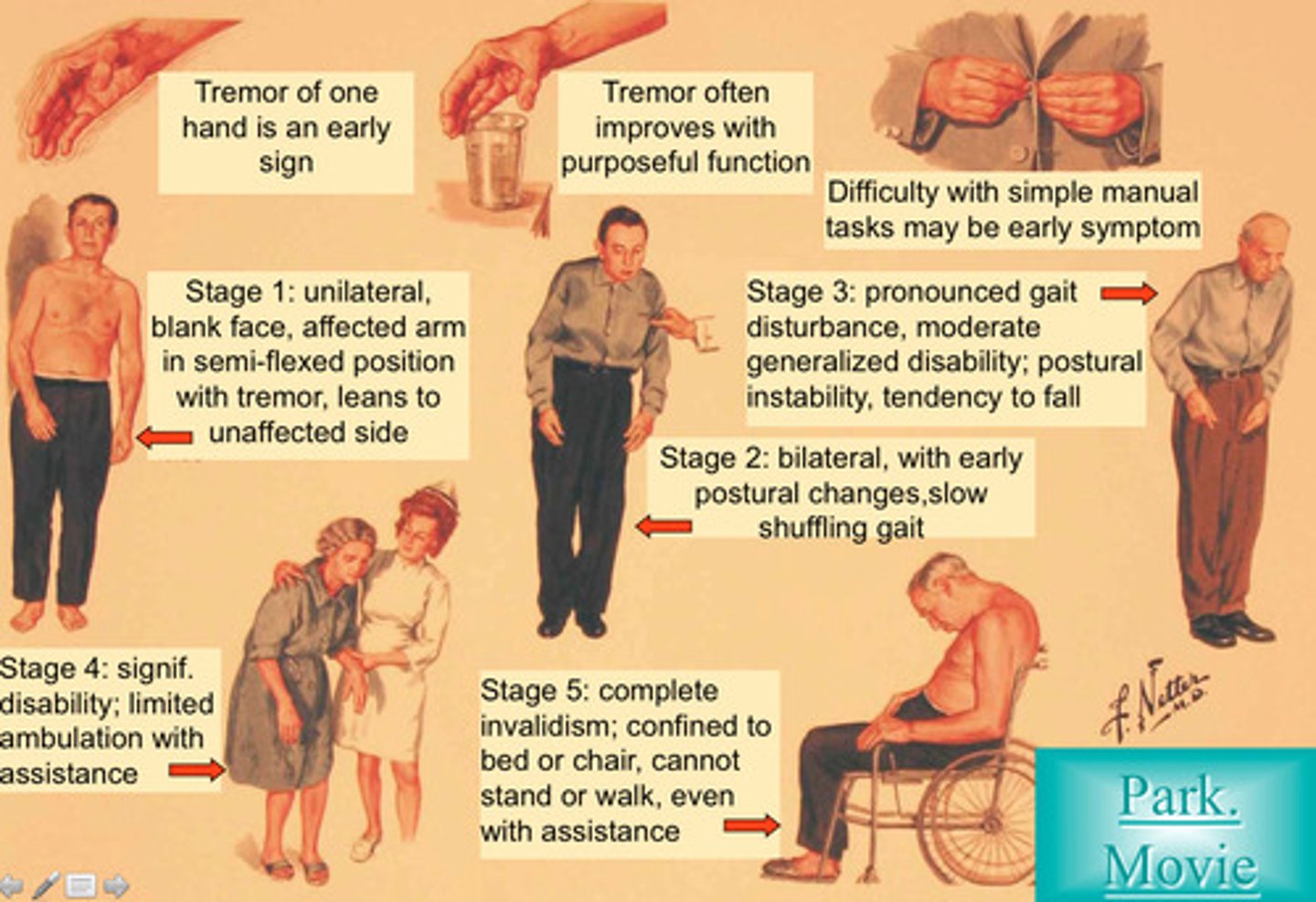
Symptoms of Parkinson's
Resting tremors (pill rolling)
Rigidity
Akinesia
Bradykinesia
Impaired postural reflexes
Masked face (I can move, but would prefer not to)
Parkinsonism
Parkinson's disease-like extrapyramidal symptoms that are adverse effects associated with particular drugs or brain injuries
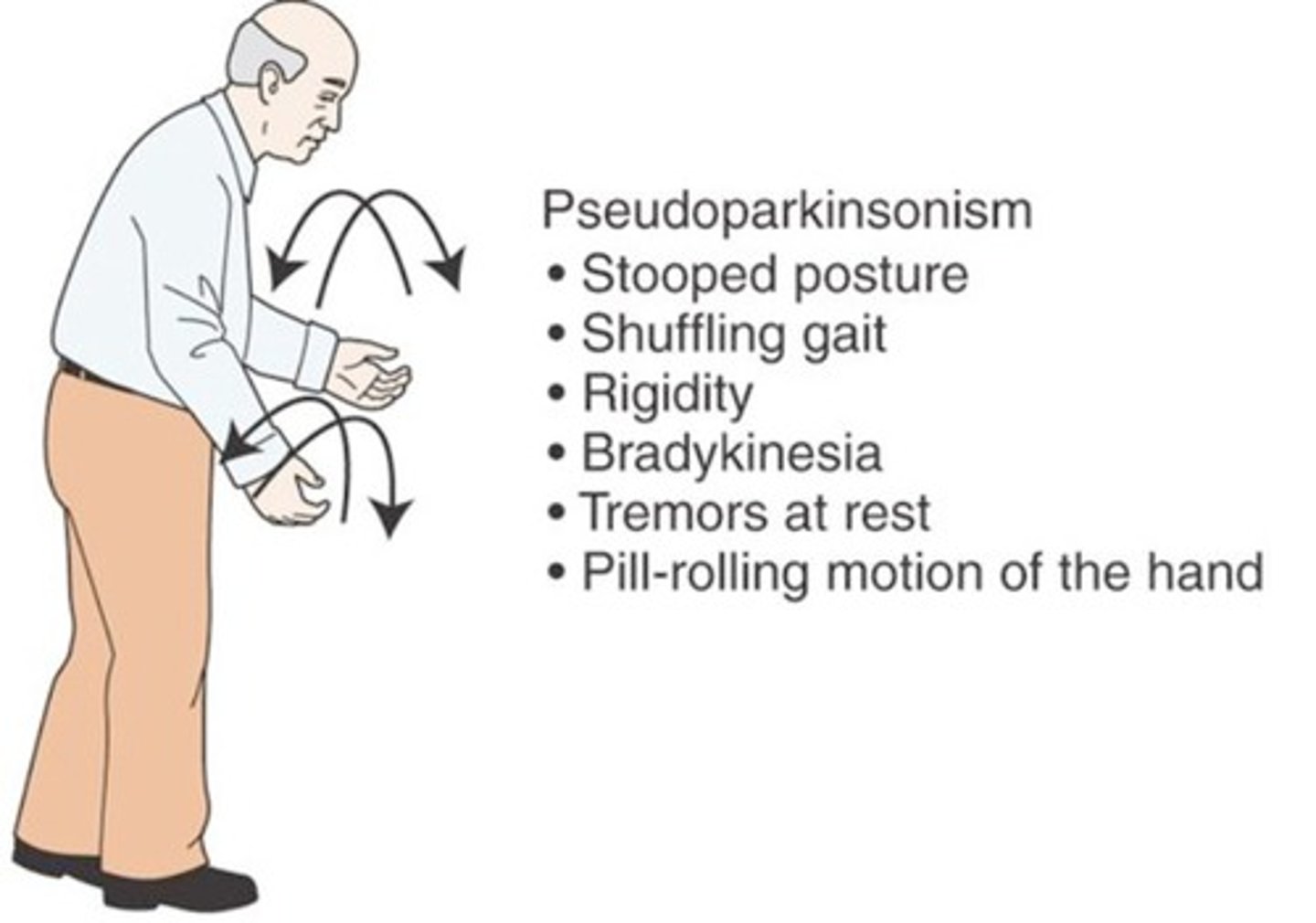
Progressive Supranuclear Palsy
Associated with Parkinson's and characterized by supranuclear ophthalmoplegia
Primarily downward gaze paresis, followed by paresis of other eye muscles
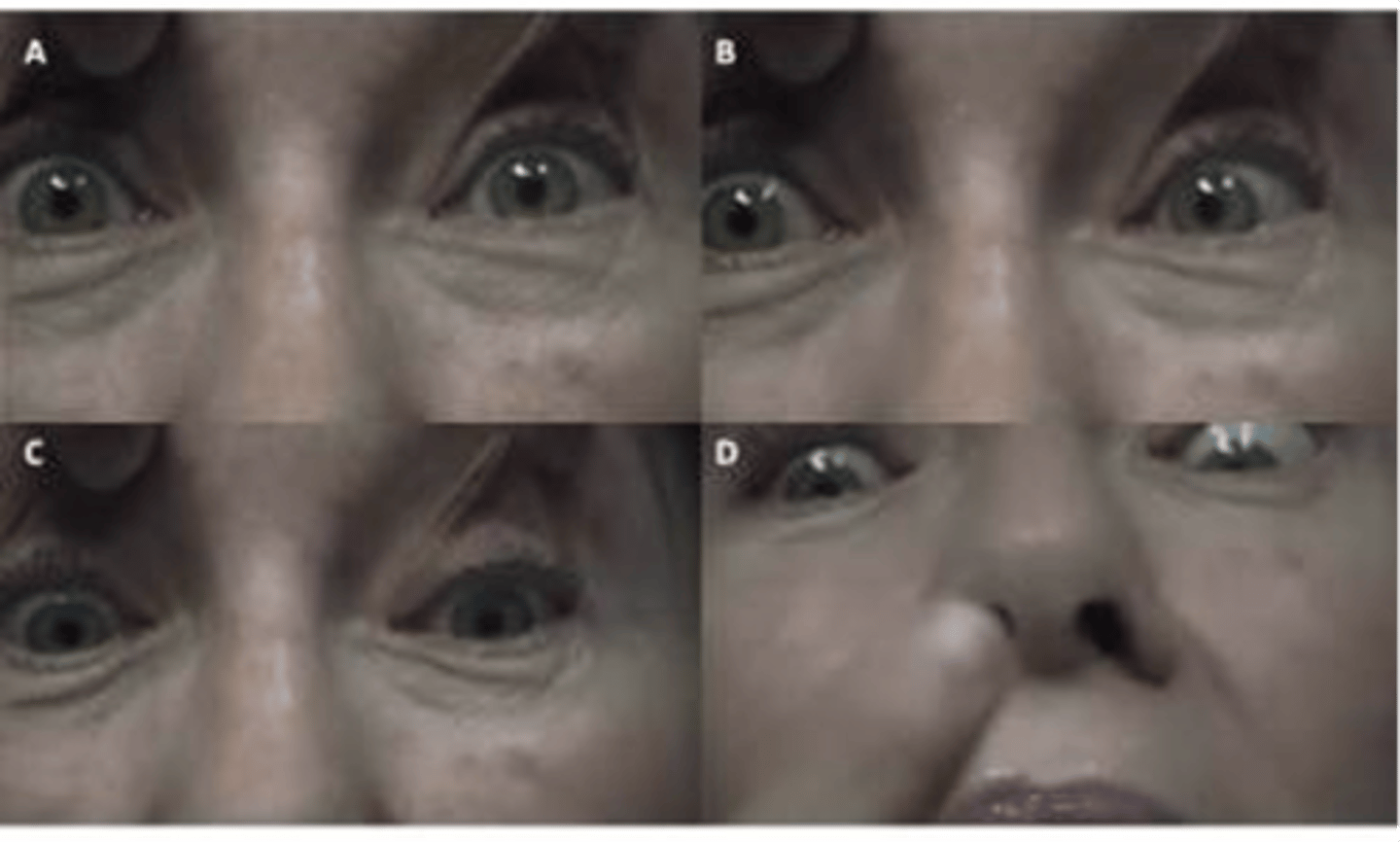
Huntington's Chorea
Autosomal dominant movement disorder, onset in mid-thirties
Localized to a single gene defect on chromosome 4
Symptoms: chorea, dementia, slowness of eye saccades, and inability to perform saccade without head movement

Wilson's Disease (Hepatolenticular Degeneration)
Autosomal recessive movement disorder localized on chromosome 13; caused by a defect in copper metabolism
Results in lesions in the liver and lentiform nucleus (putamen)
Symptoms: psychiatric problems, personality disorders, dementia tremor, rigidity, choreiform and athetotic movements
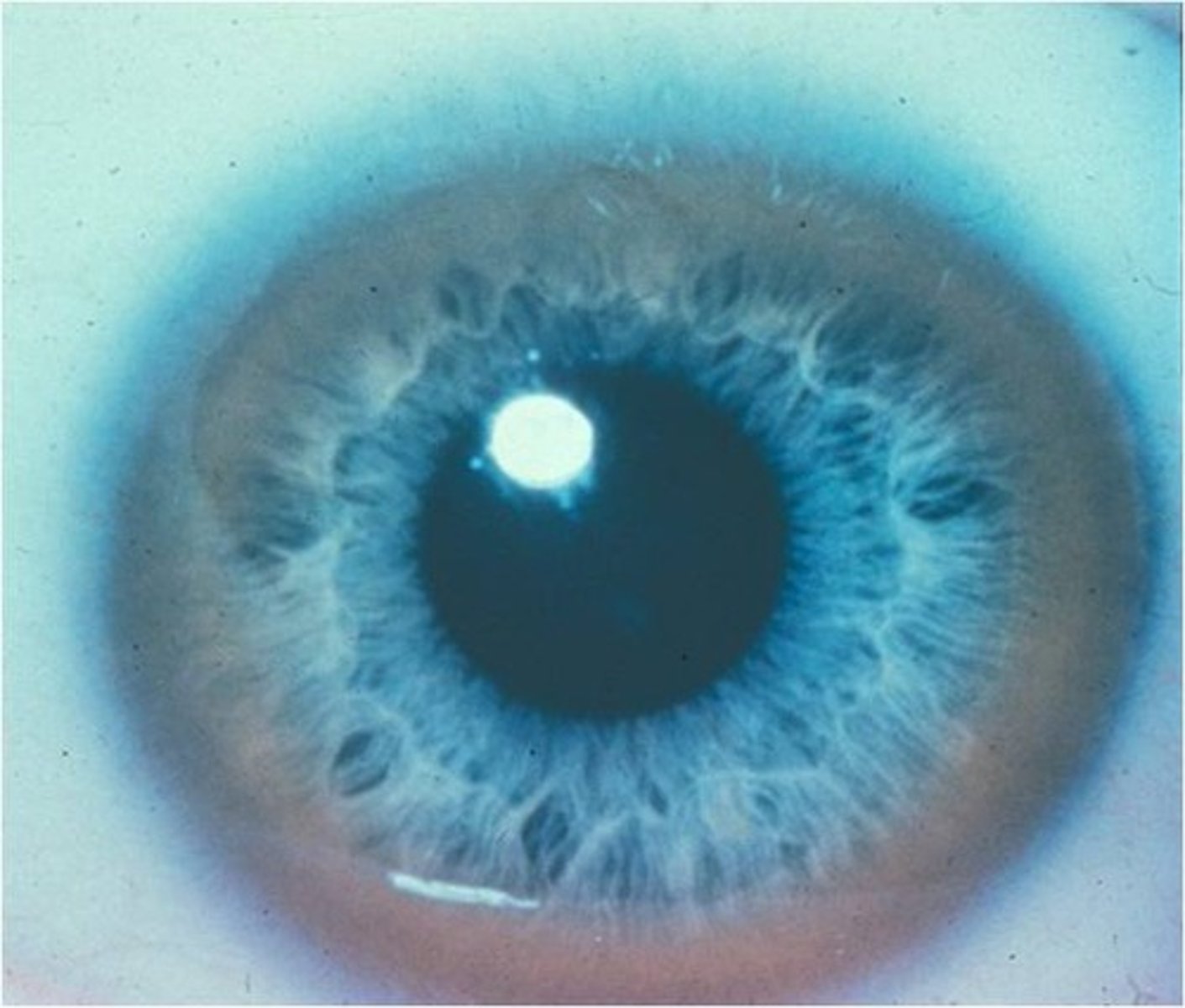
Kayser-Fleischer Ring
Gray/green or red/gold pigmented ring on the outer margin of the cornea
Used as a diagnostic sign of Wilson's disease
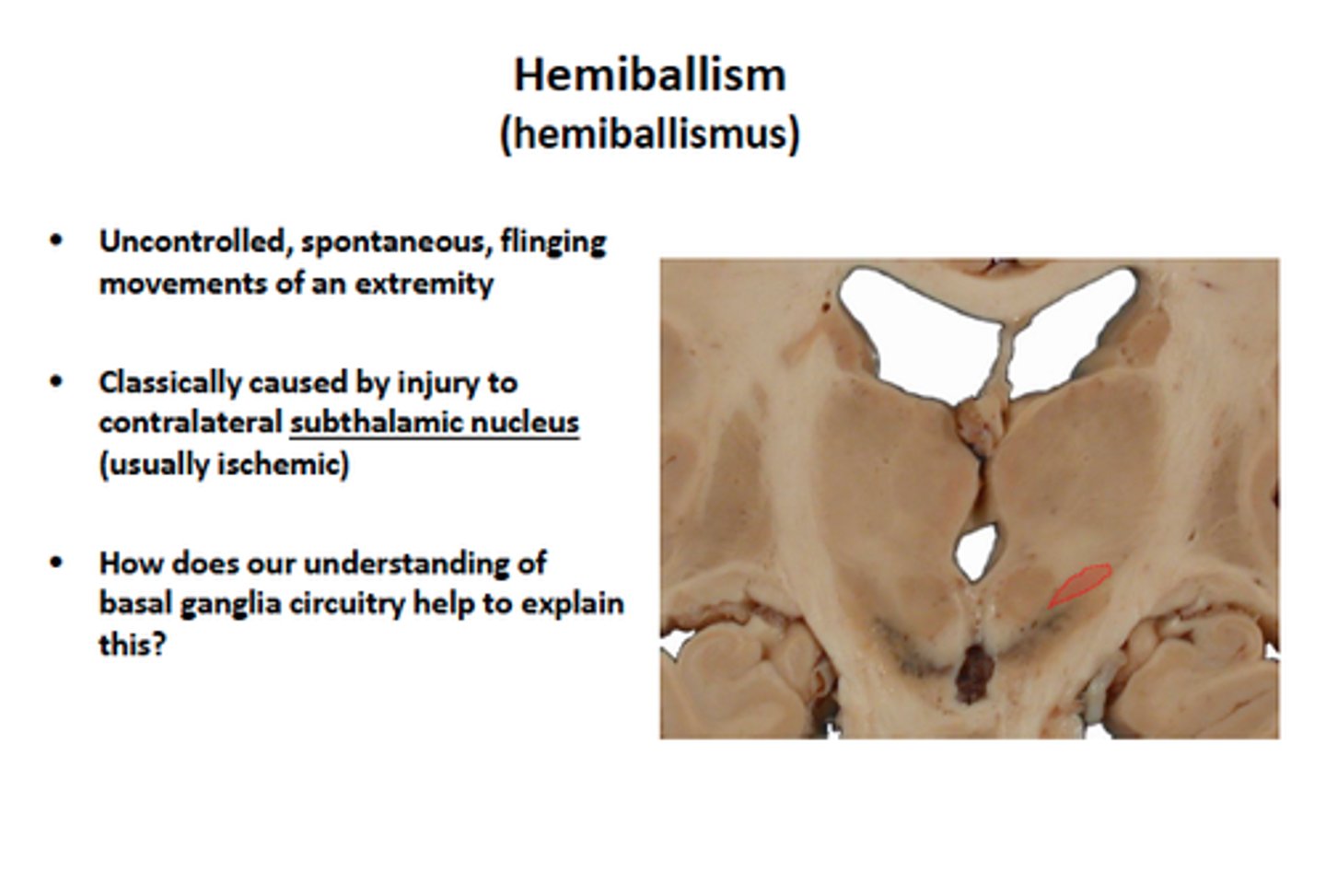
Hemiballism
An involuntary and violent movement of a large body part
Caused by a stroke in the subthalamus
Symptoms: violent, flinging movements of the contralateral arm and/or leg
Cerebral Palsy
A loss or deficiency of motor control with involuntary spasms caused by permanent brain damage present at birth due to oxygen deficiency
Symptoms: dystonia and athetosis
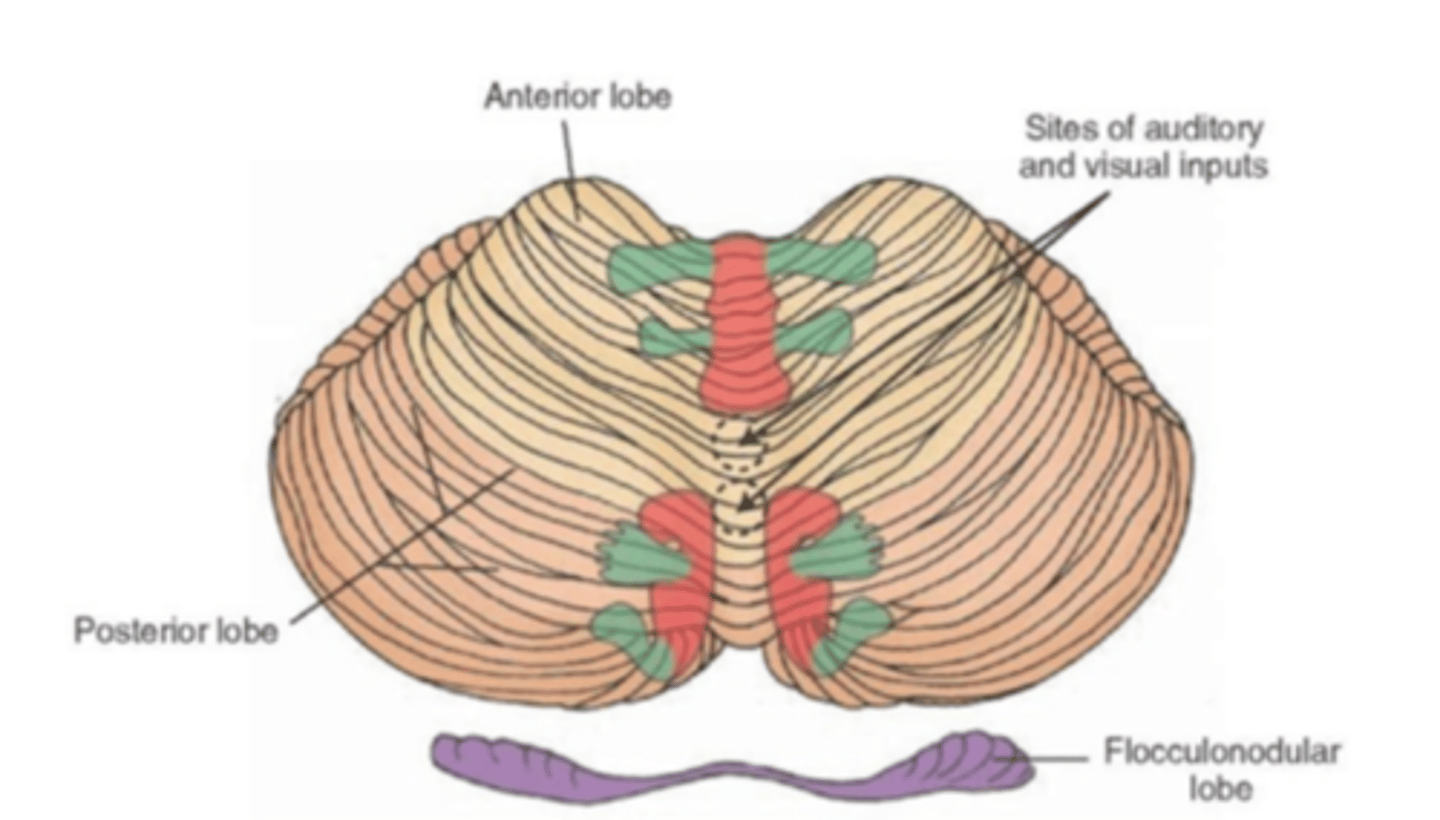
Flocculonodular Lobe
A region of the cerebellum; involved in control of postural reflexes
Associated with the thalamus
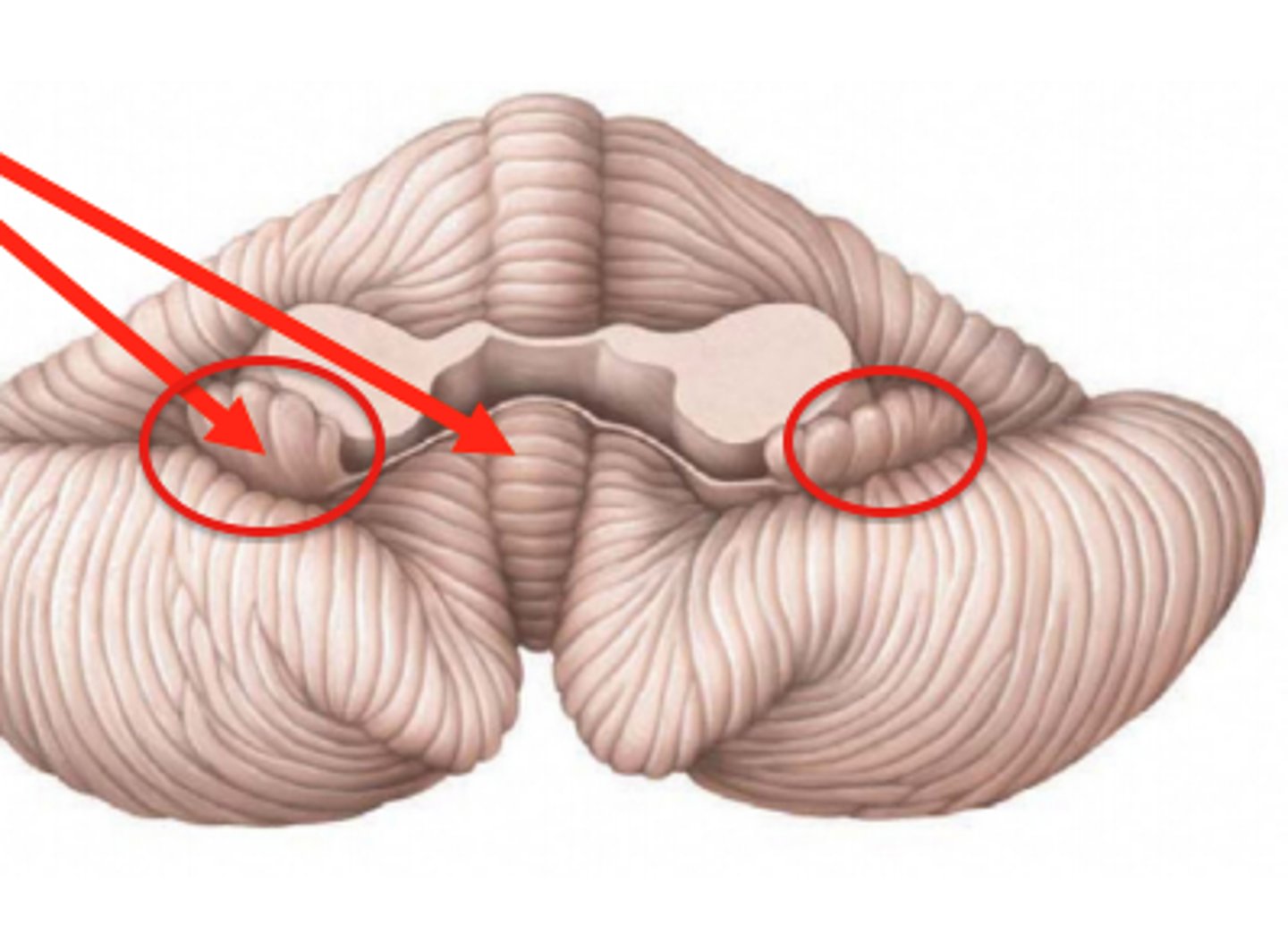
Flocculus
Small but dense lobe involved in eye movements and balance
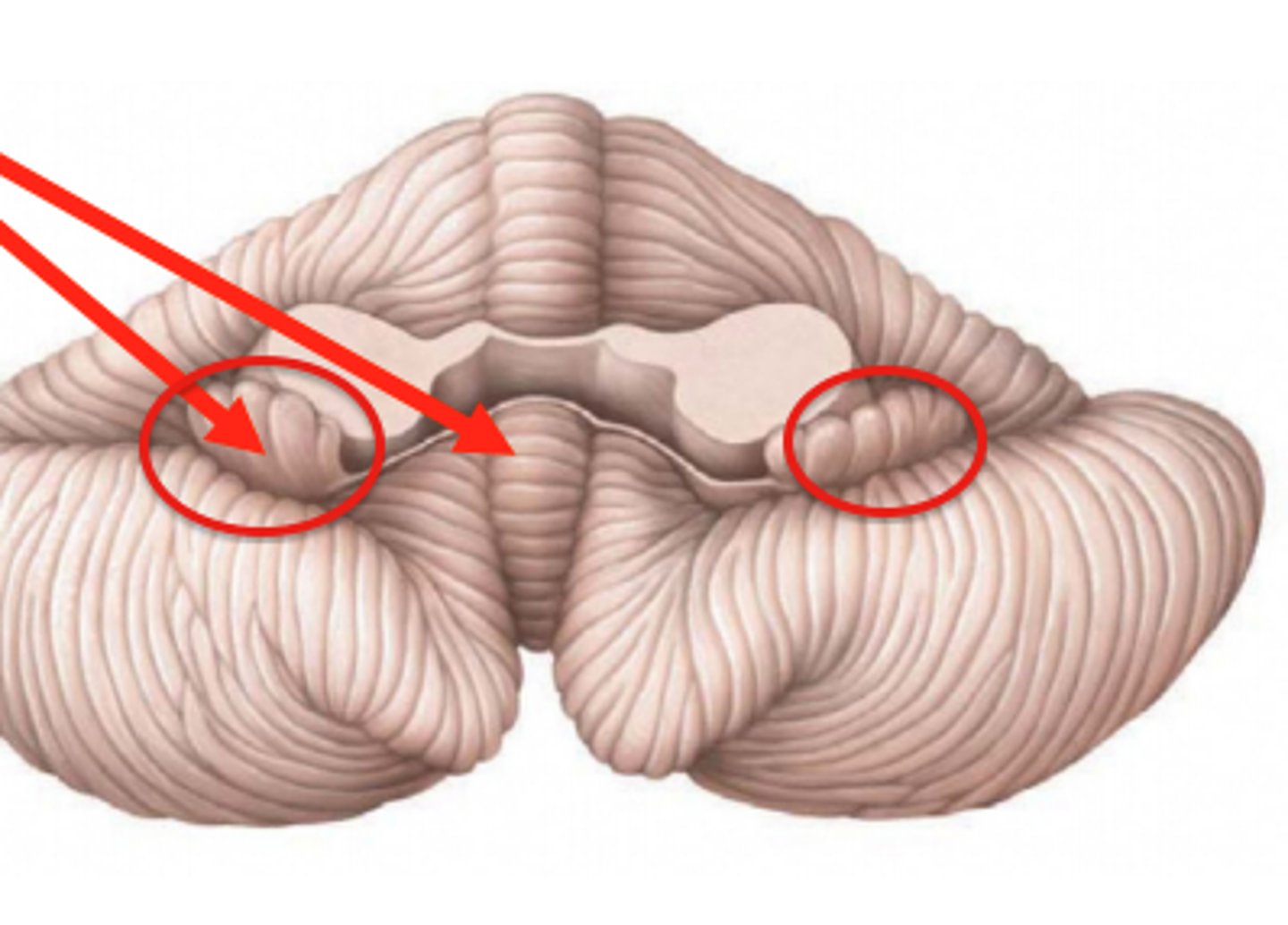
Nodule
Medial protrusion seen on the midsagittal view of the cerebellum; part of the vermis
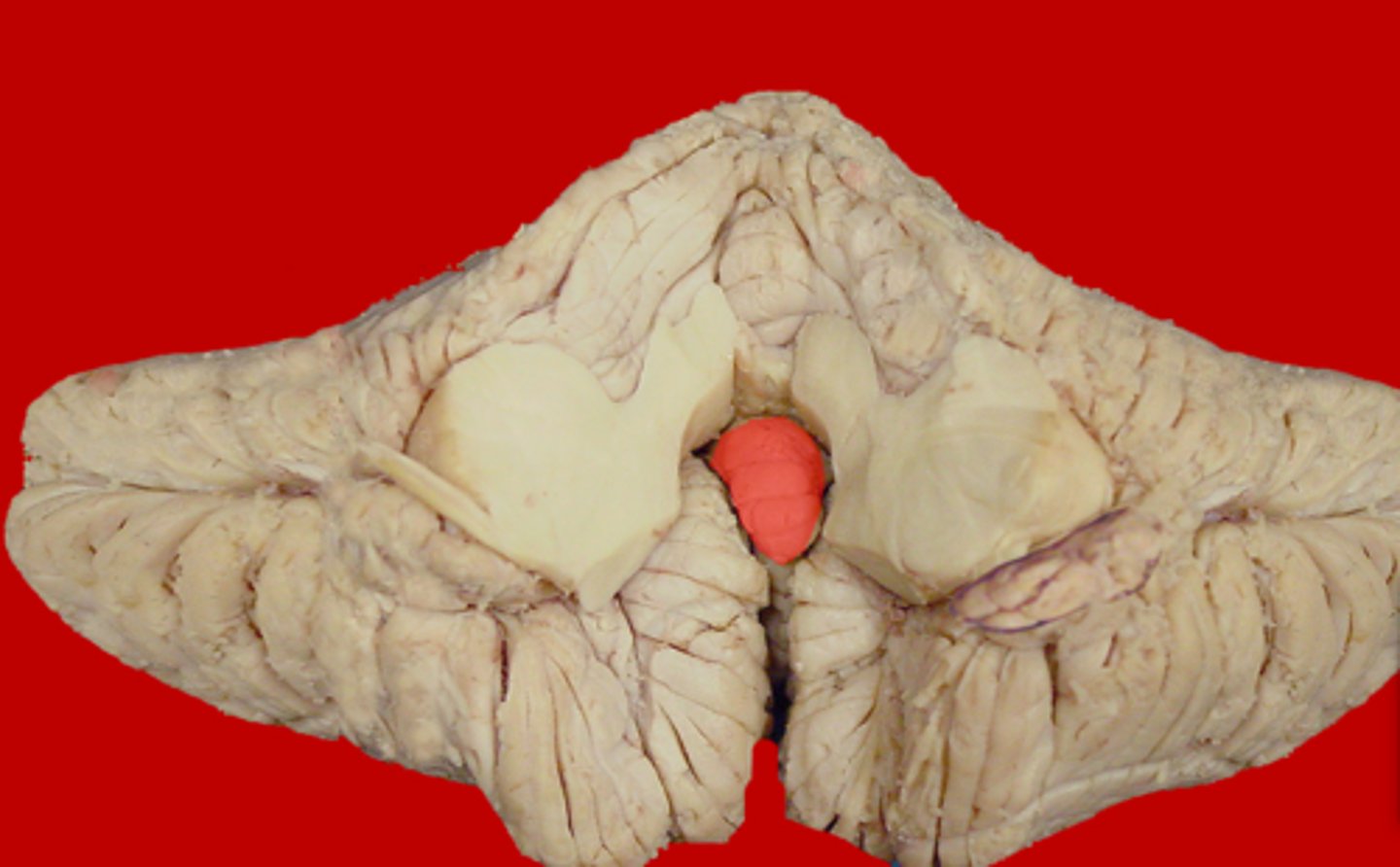
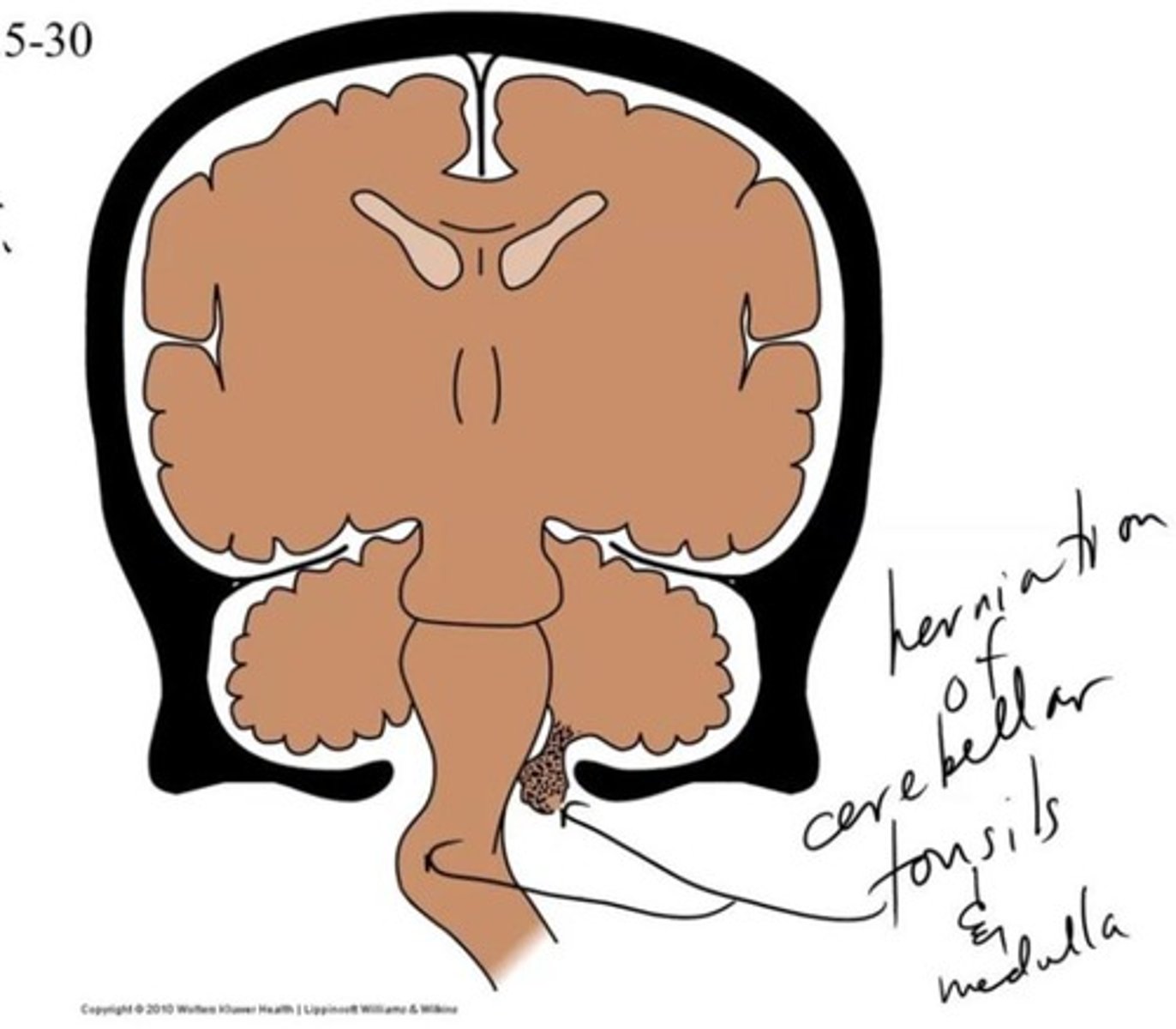
Tonsil of Cerebellum
Two elevated masses on inferior surface of hemispheral portion just nearby foramen magnum
Can herniate into the foramen magnum, exerting pressure on the medulla
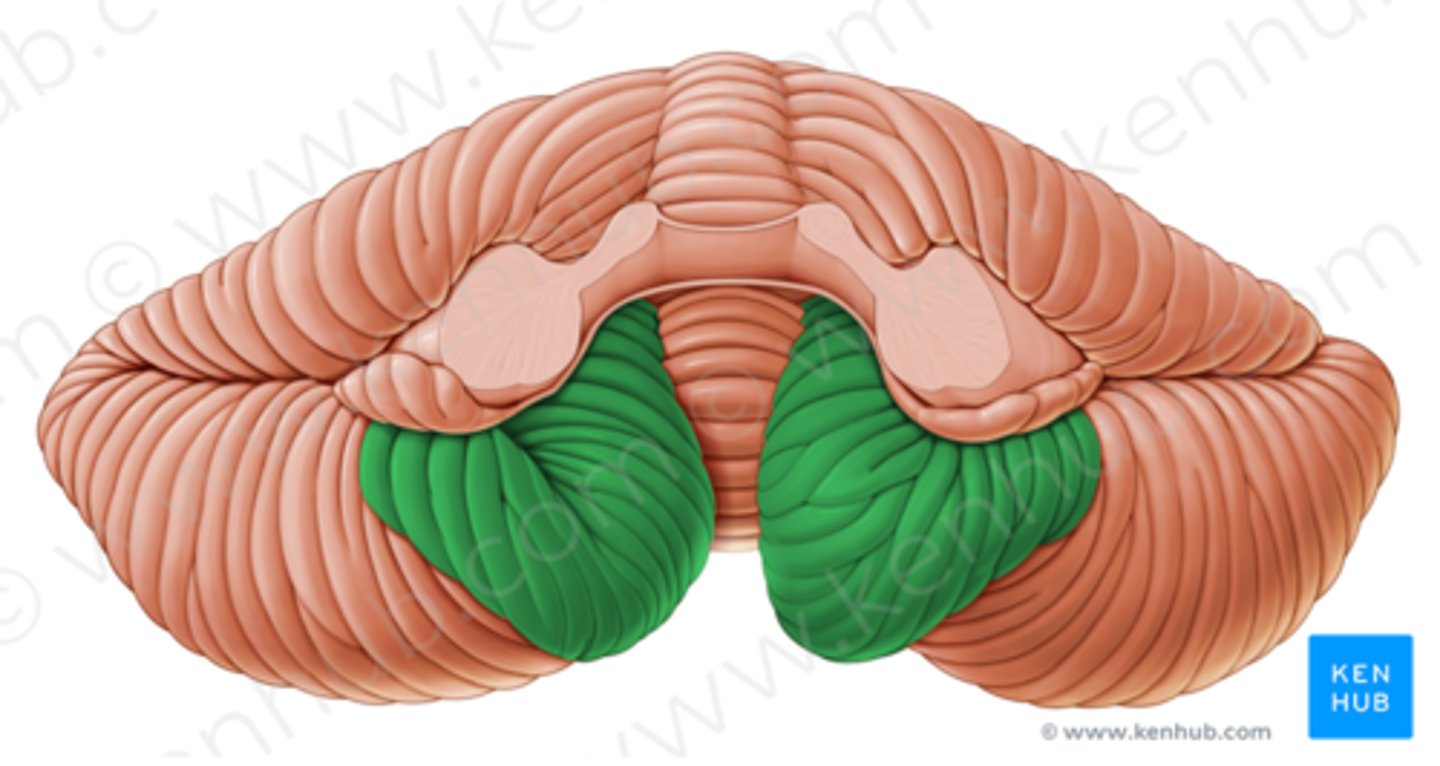
Cerebrocerebellum
Planning and initiation of voluntary activity
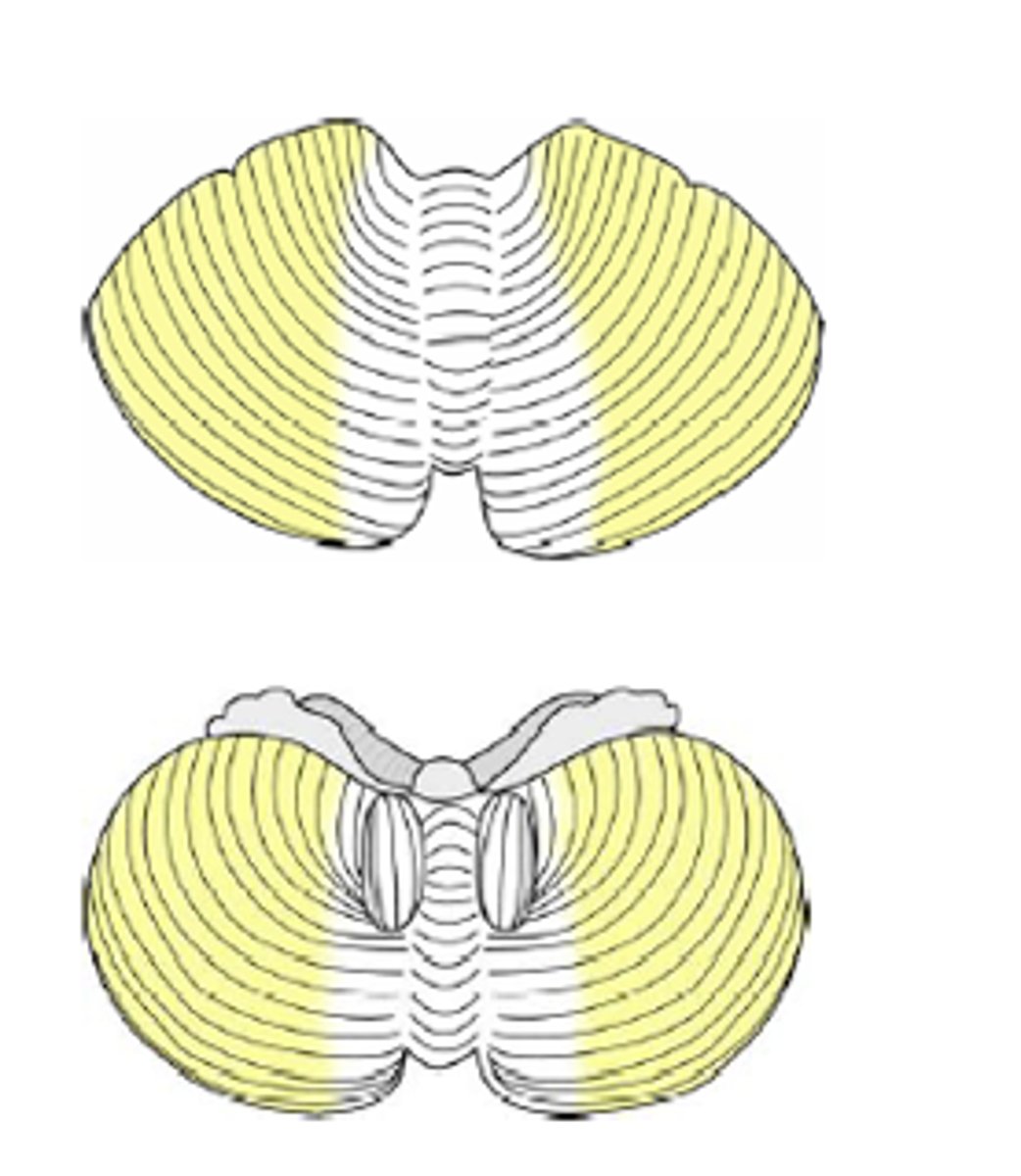
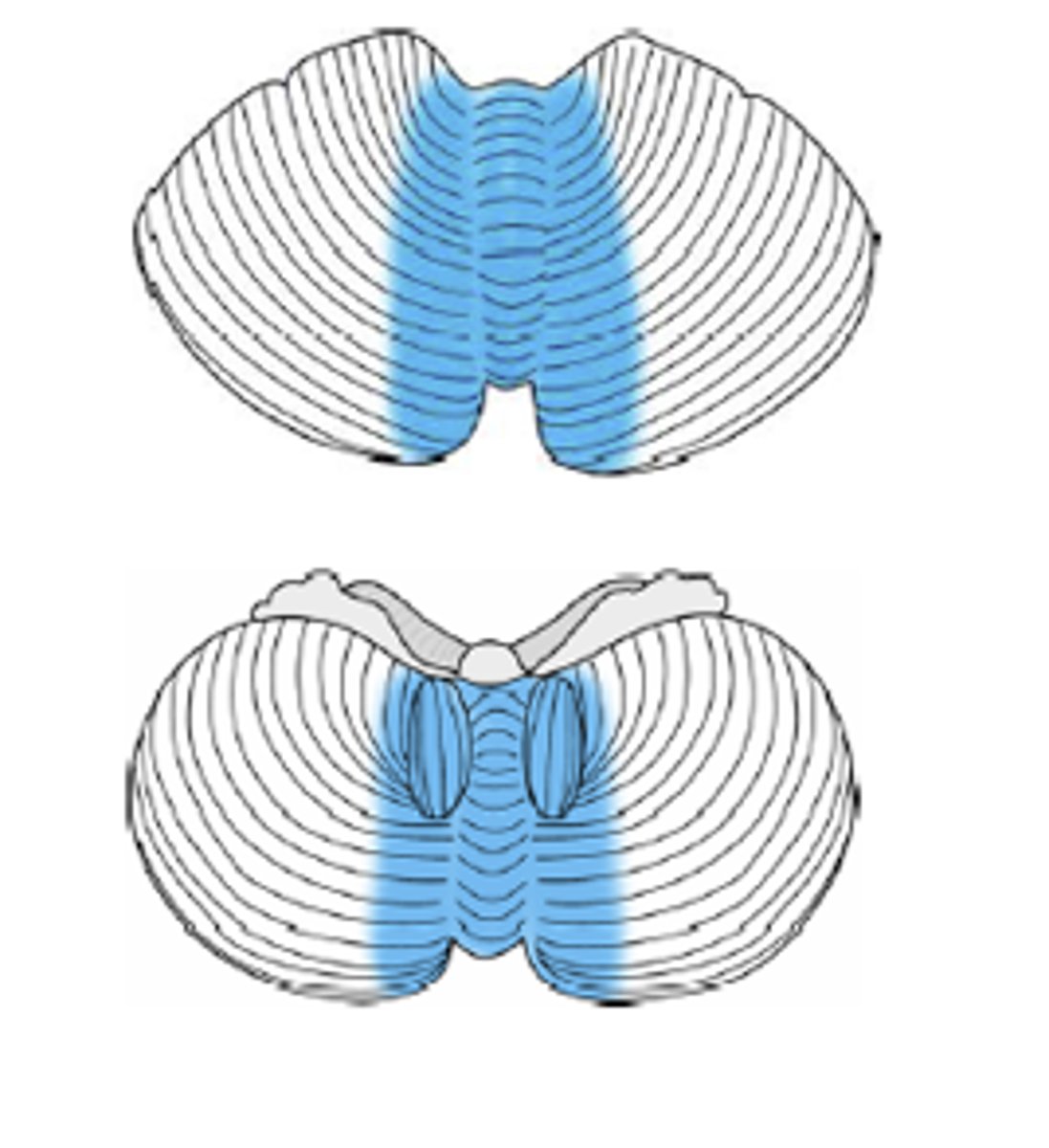
Vestibulocerebellum
Maintenance of balance, control of eye movements
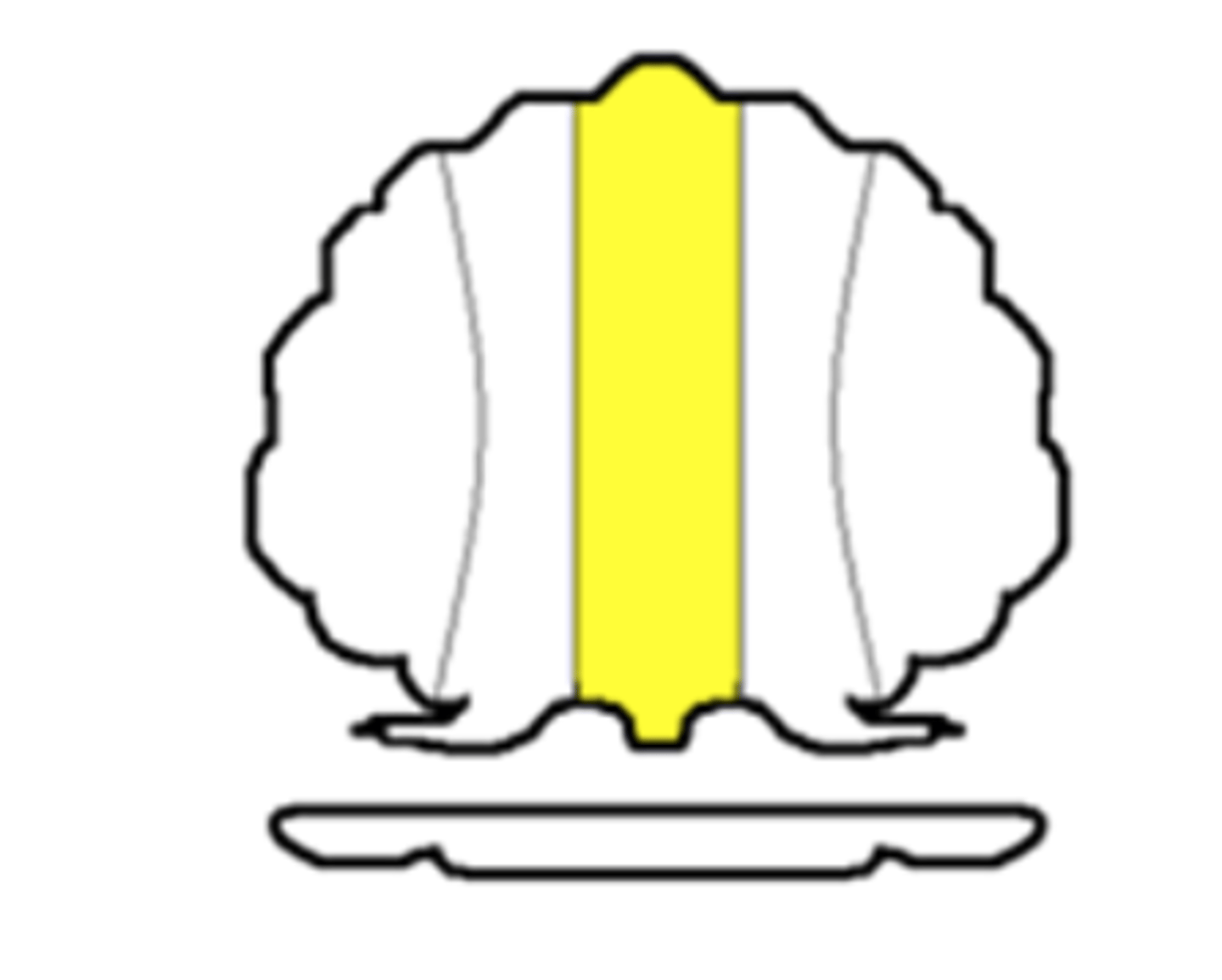
Vermal Zone
Composed of flocculonodular lobe
Controls eye movement and axial musculature related to balance and posture
Connects two hemispheres of cerebellum
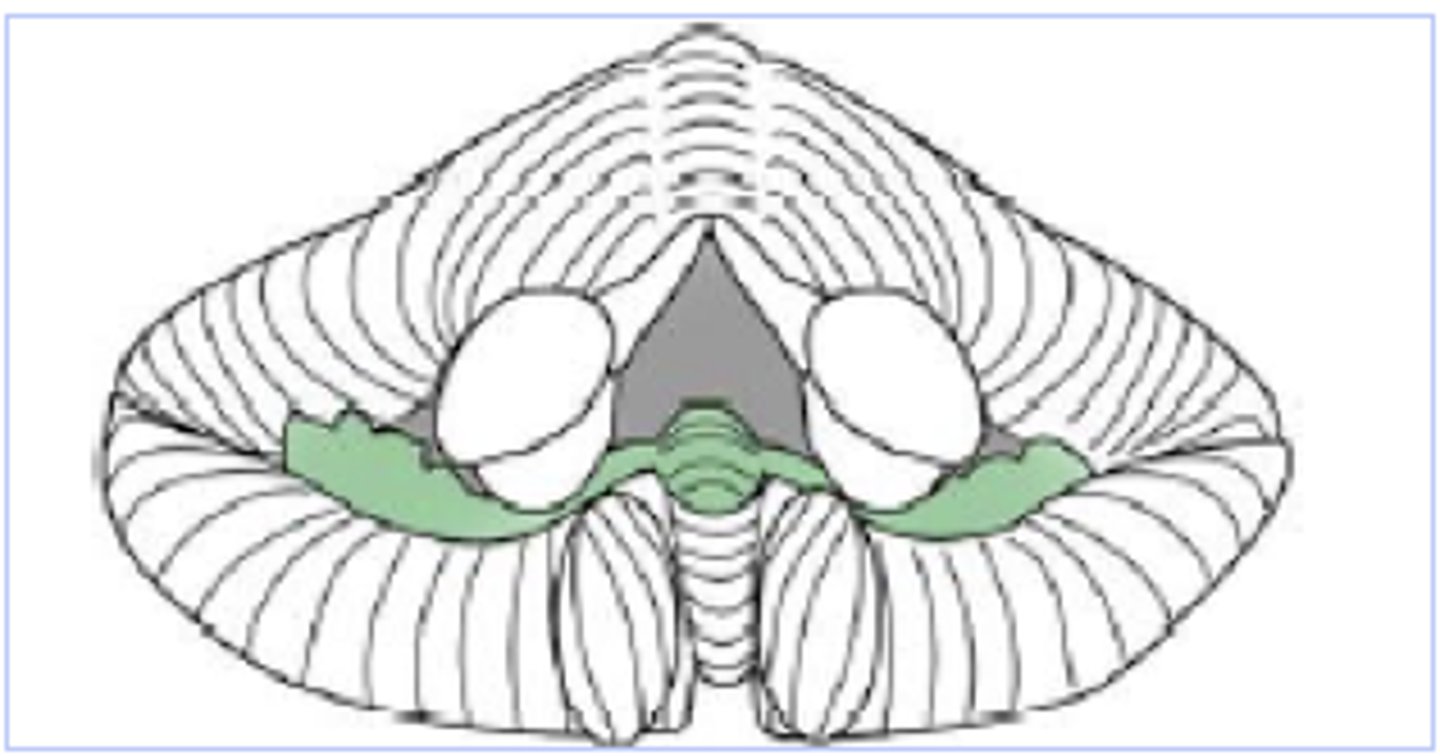
Spinocerebellum
Enhances muscle tone and coordinates skilled, voluntary movements
Fastigial, globose and emboliform nuclei
Input to the Cerebellar Cortex
Climbing fibers and mossy fibers
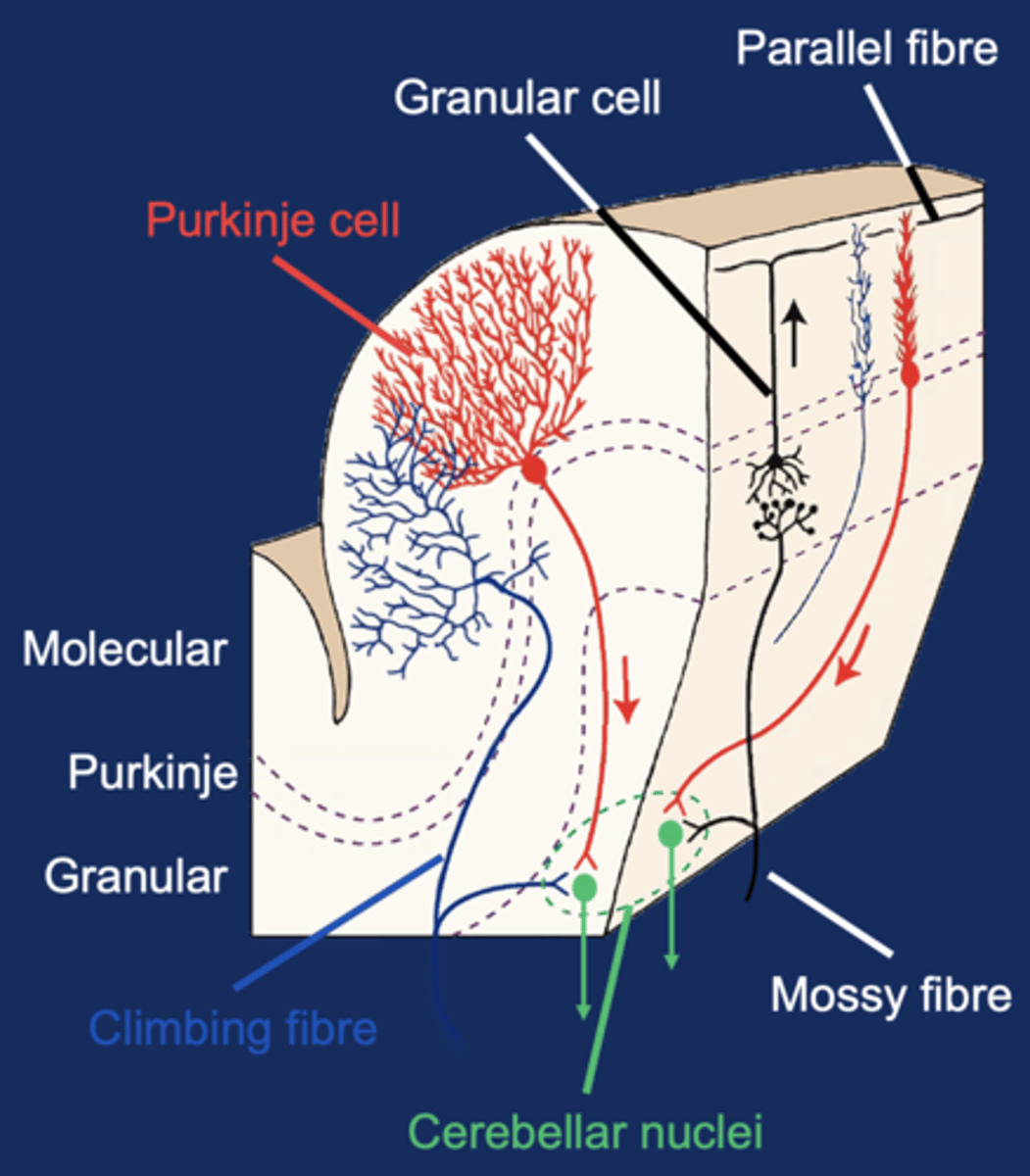
Output from the Cerebellar Cortex
Transmitted via GABAergic Purkinje cell fibers
Only output from cortex
Final Output from the Cerebellum
From the deep cerebellar nuclei
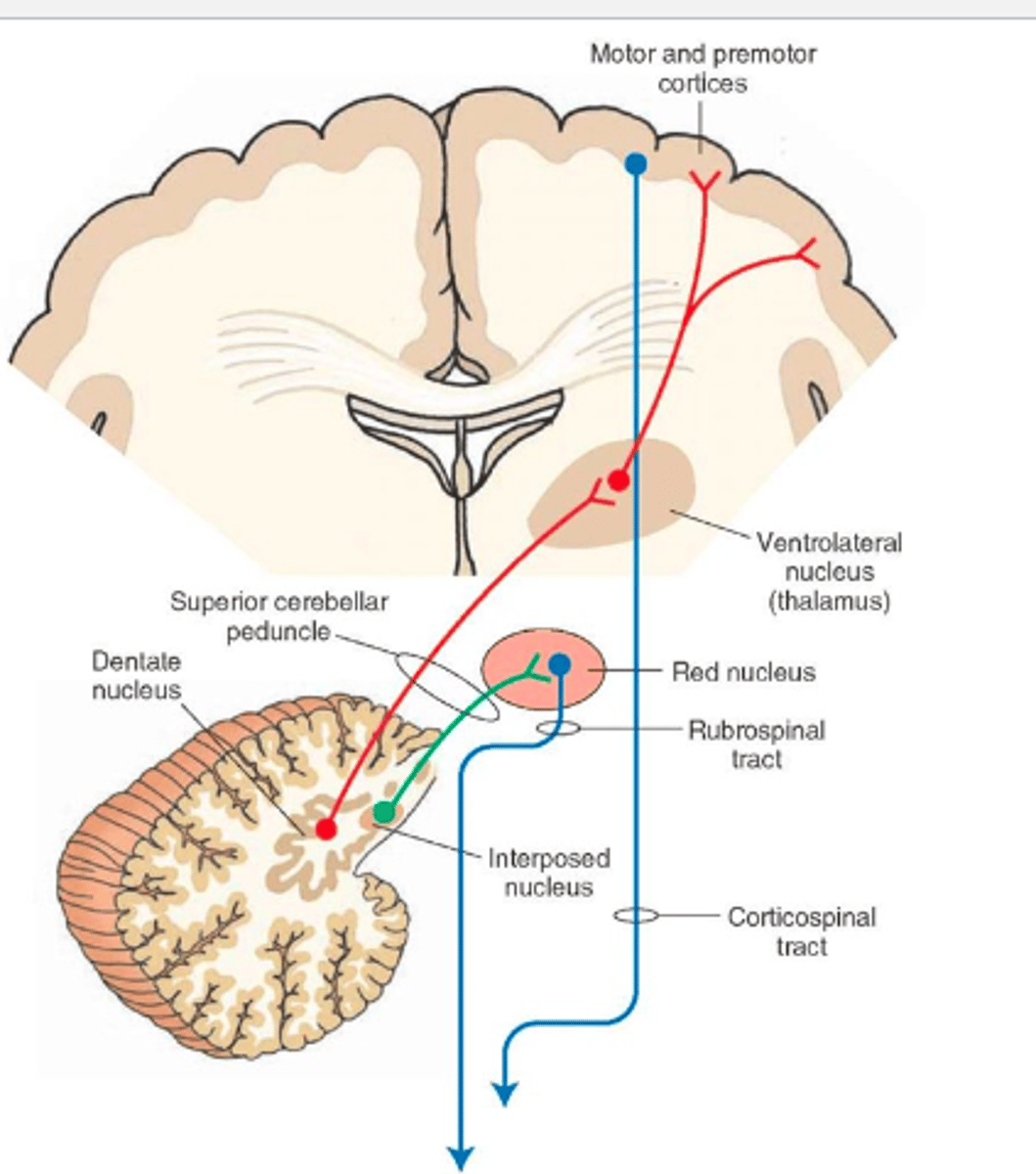
Path Through the Cerebellum
Fibers from spinal cord and brainstem enter and synapse in both cerebellar deep nuclei and cerebellar cortex
Purkinje cells in the cortex send axons to the deep nuclei, modulating the output of the nuclei
Deep nuclei send fibers out of the cerebellum to the brainstem and thalamus
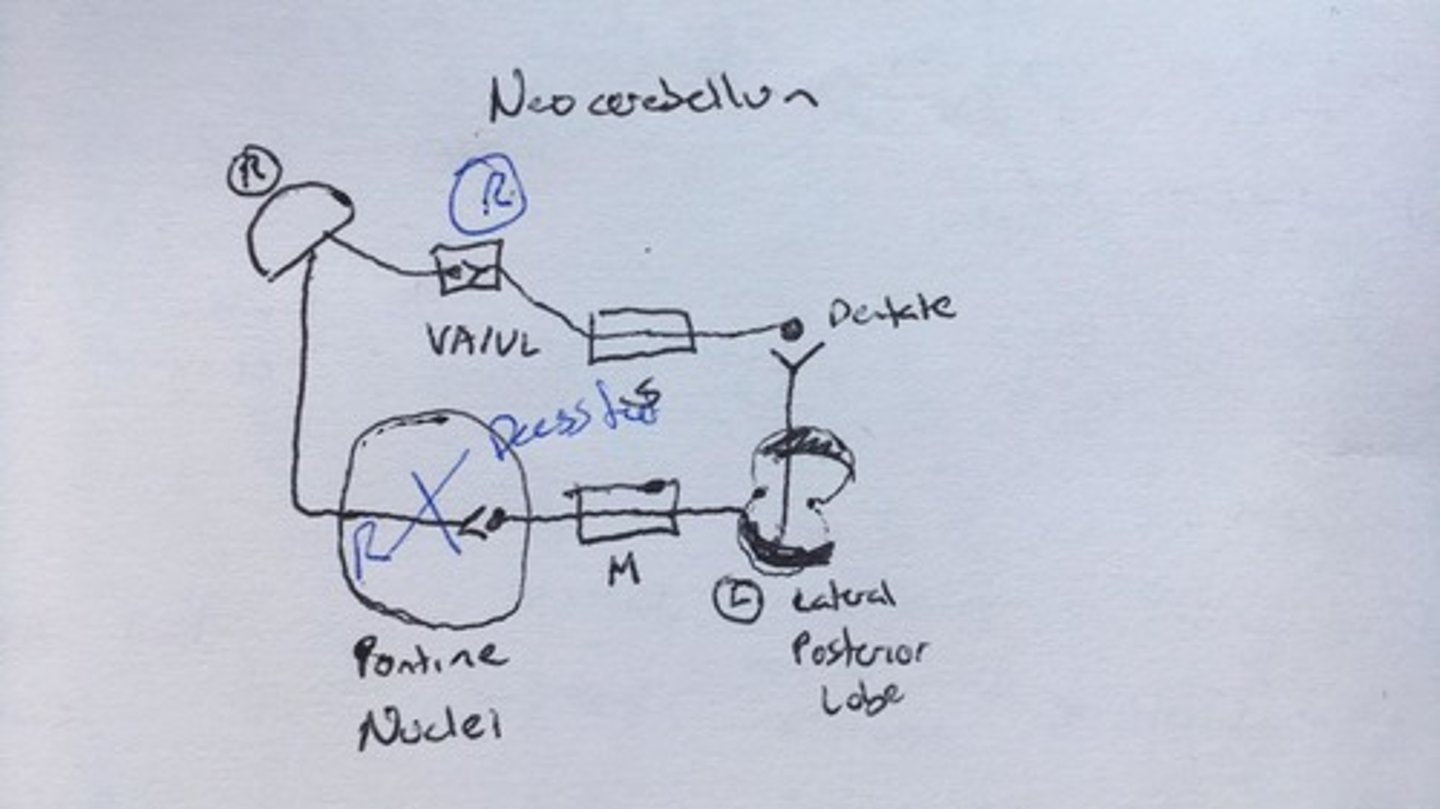
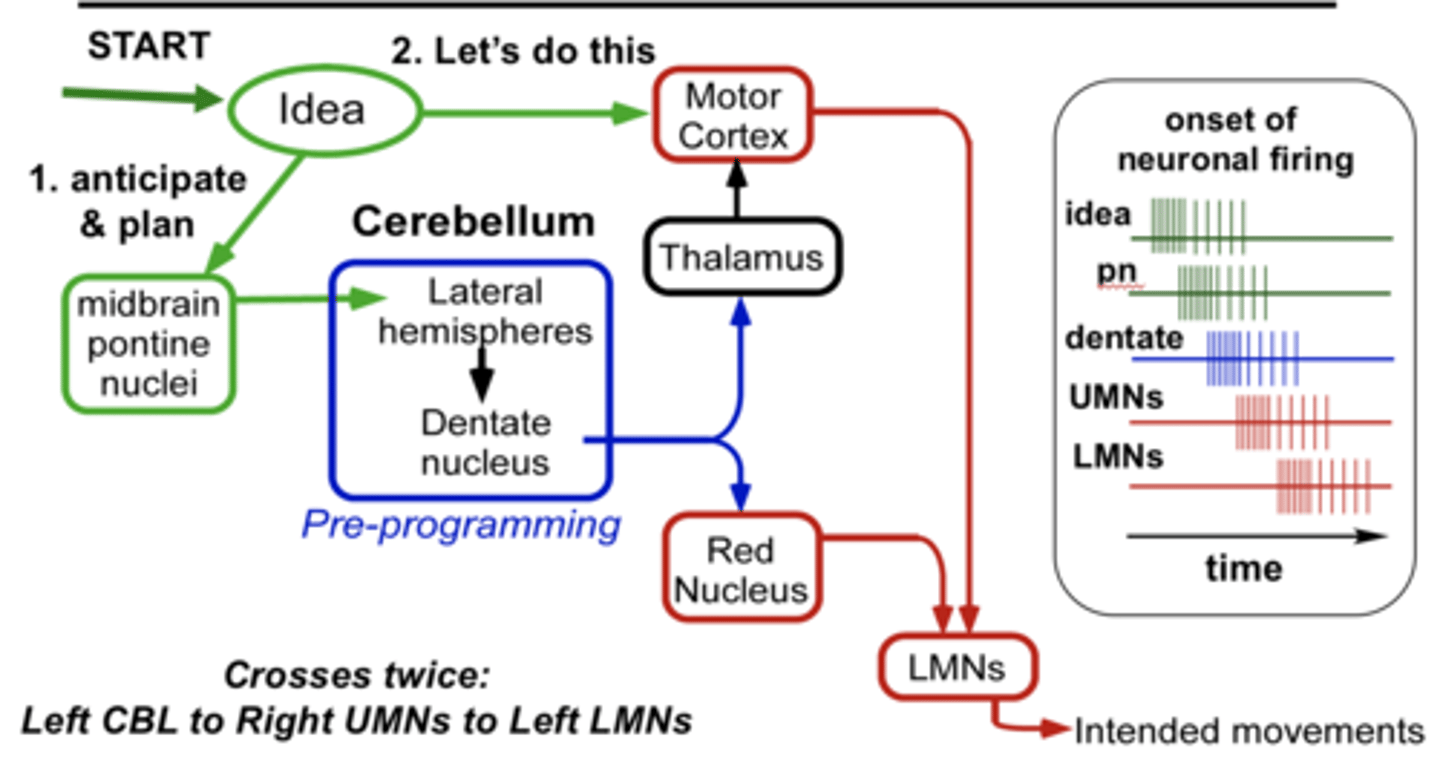
Cerebrocerebellum Circuitry
Input to contralateral cerebral cortex indirectly via the pons
Output to the contralateral red nucleus which projects to the thalamus (VL/VA) and contralateral thalamus relays info to the cortex
Lateral nuclei = dentate nuclei
Double crossing: the cerebellum talks to the initiating cerebral hemisphere
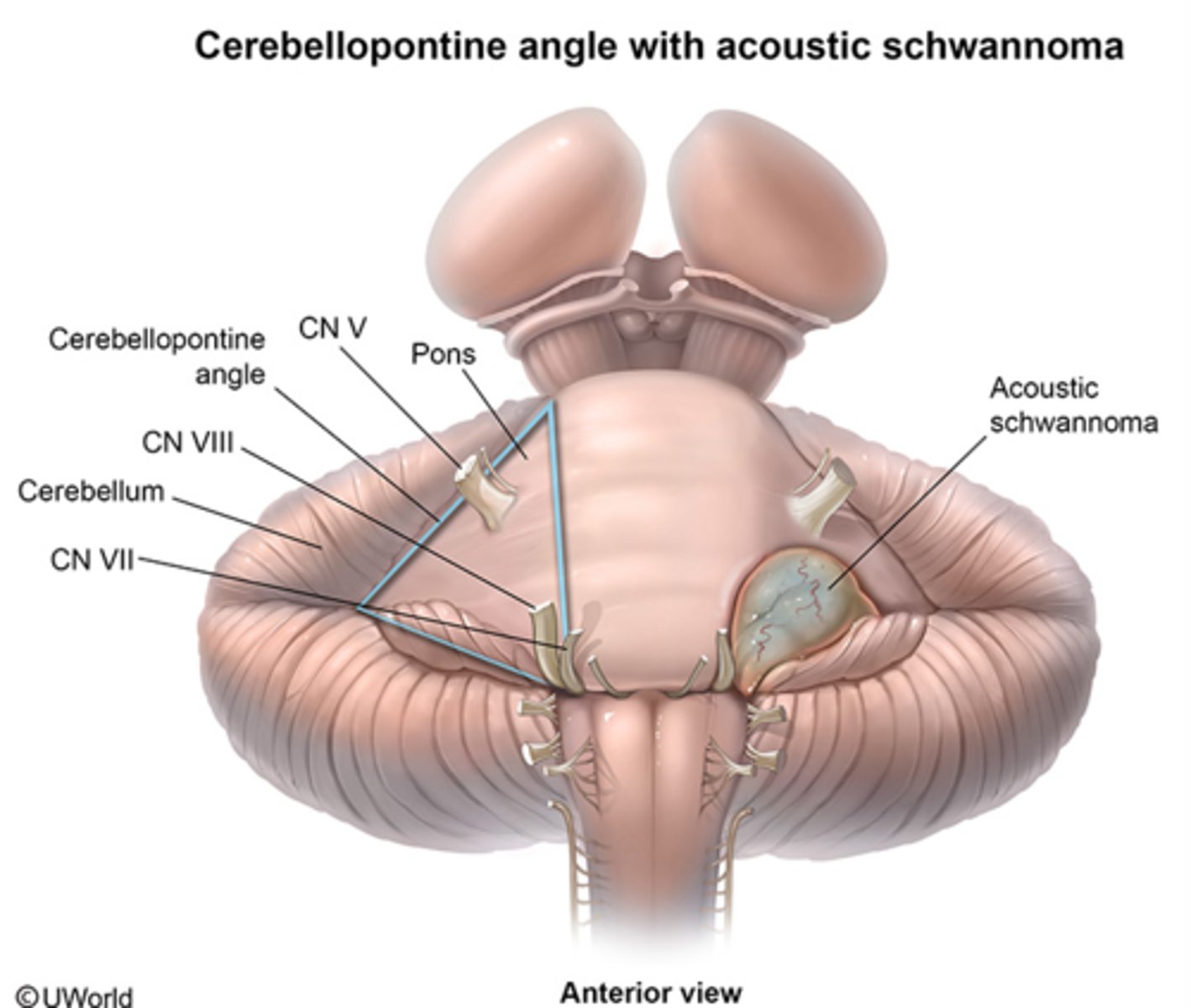
Cerebellopontine Angle
The junction at the base of the brain where the cerebellum, medulla, and pons communicate
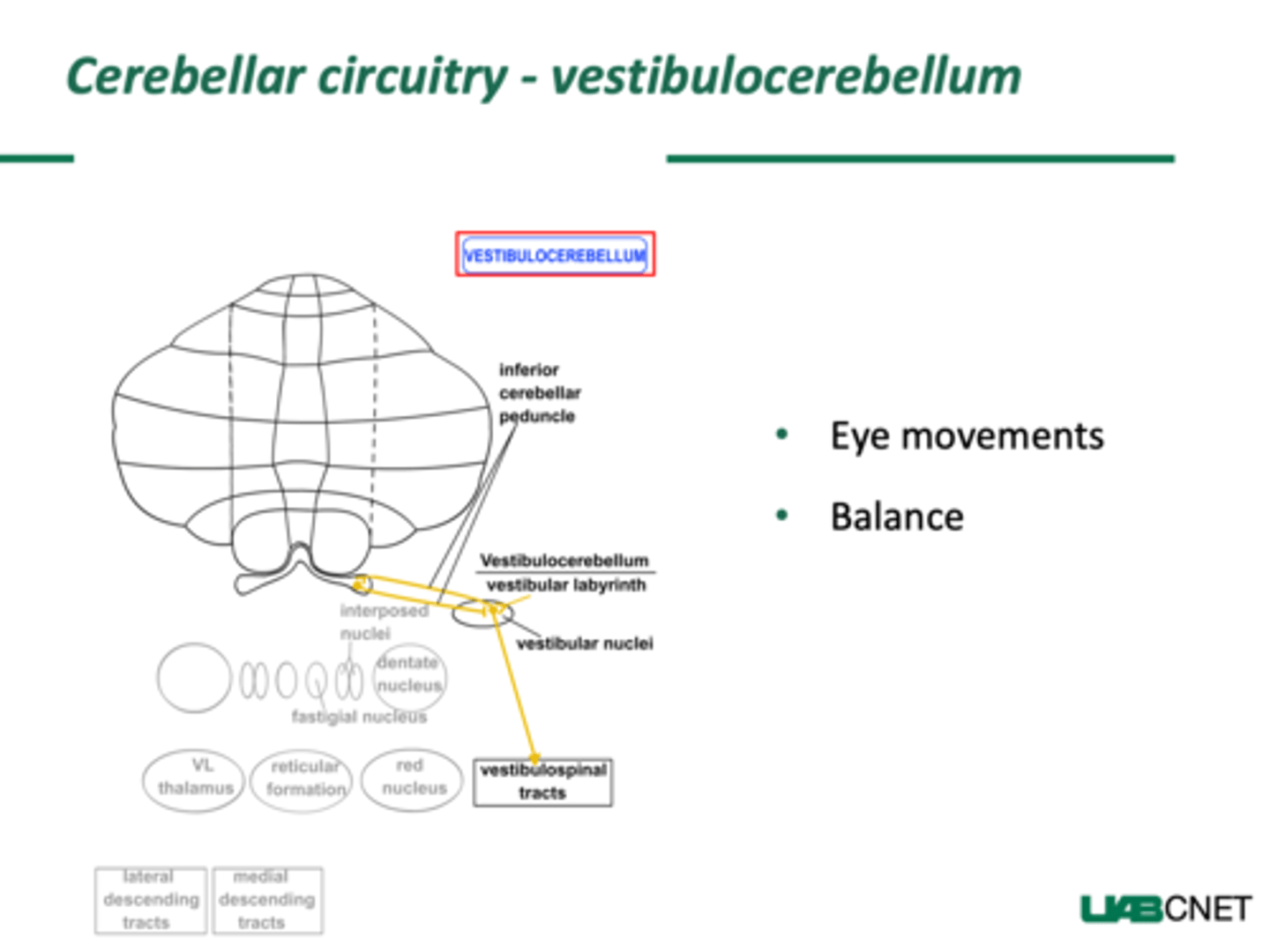
Vestibulocerebellum Circuitry
Input from the vestibular nuclei and nerve
Output to the vestibular nuclei, giving rise to the vestibulospinal tract and to the reticular nuclei, giving rise to the reticulospinal tract
Spinocerebellum Circuitry
Input from the cerebral cortex (program) and sensory inputs (environmental cues)
Output to the UMNs of the brainstem (red, reticular, vestibular) which communicate with LMNs through extrapyramidal pathways
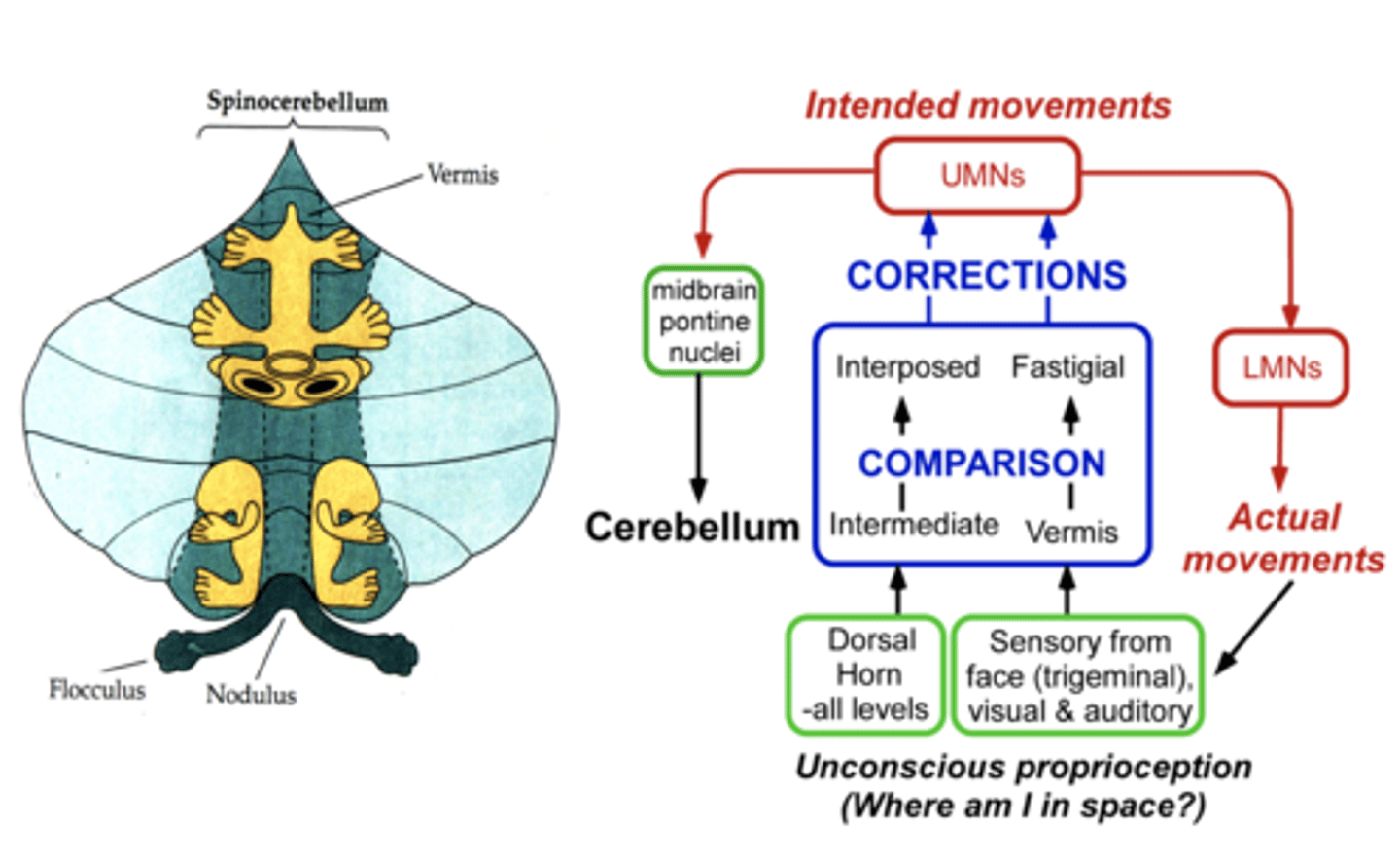
Somatotopic Map of the Cerebellum
The neuronal regions associated with regulation of the distal musculature are shown in green, and the regions associated with the axial musculature are shown in red
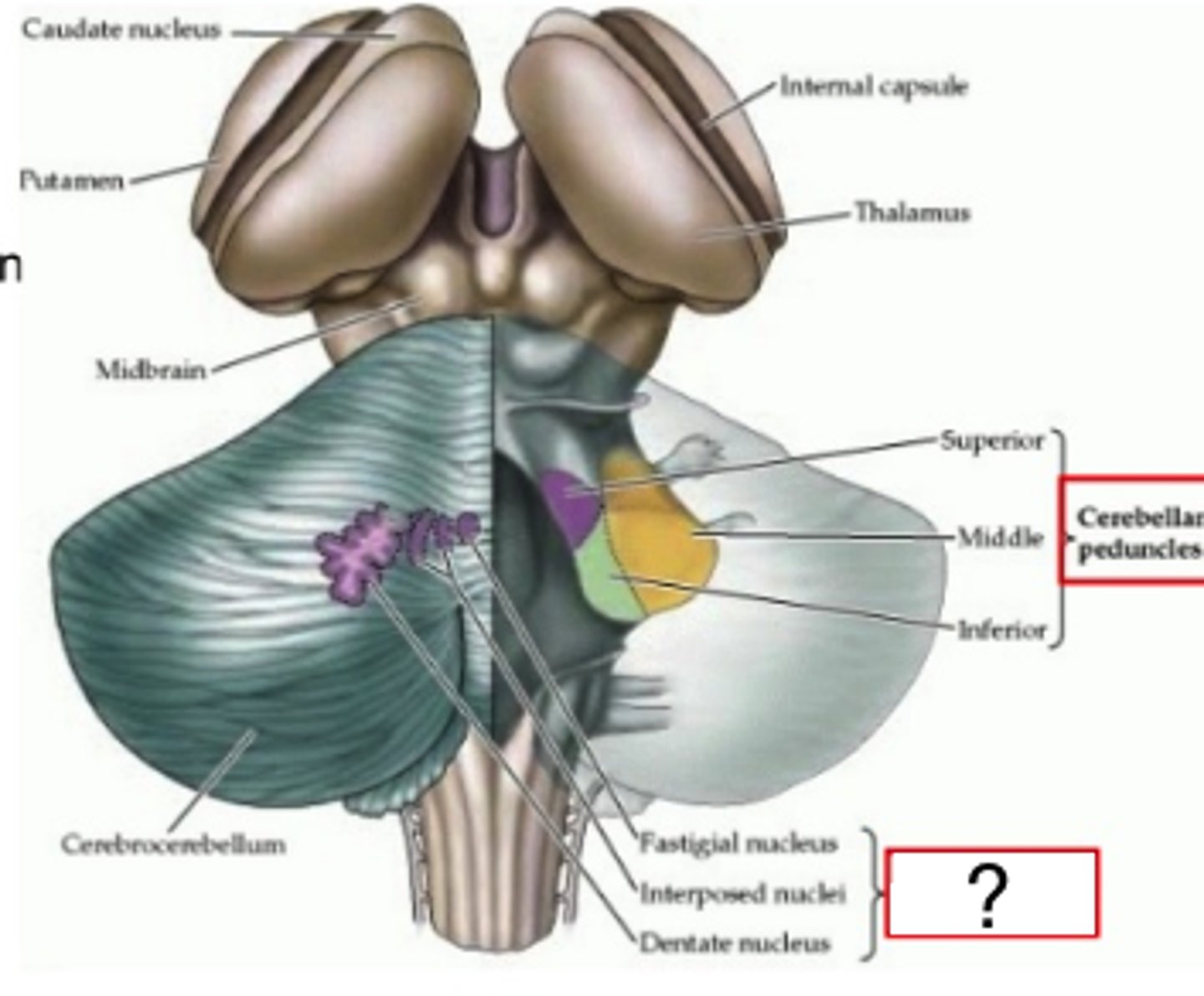
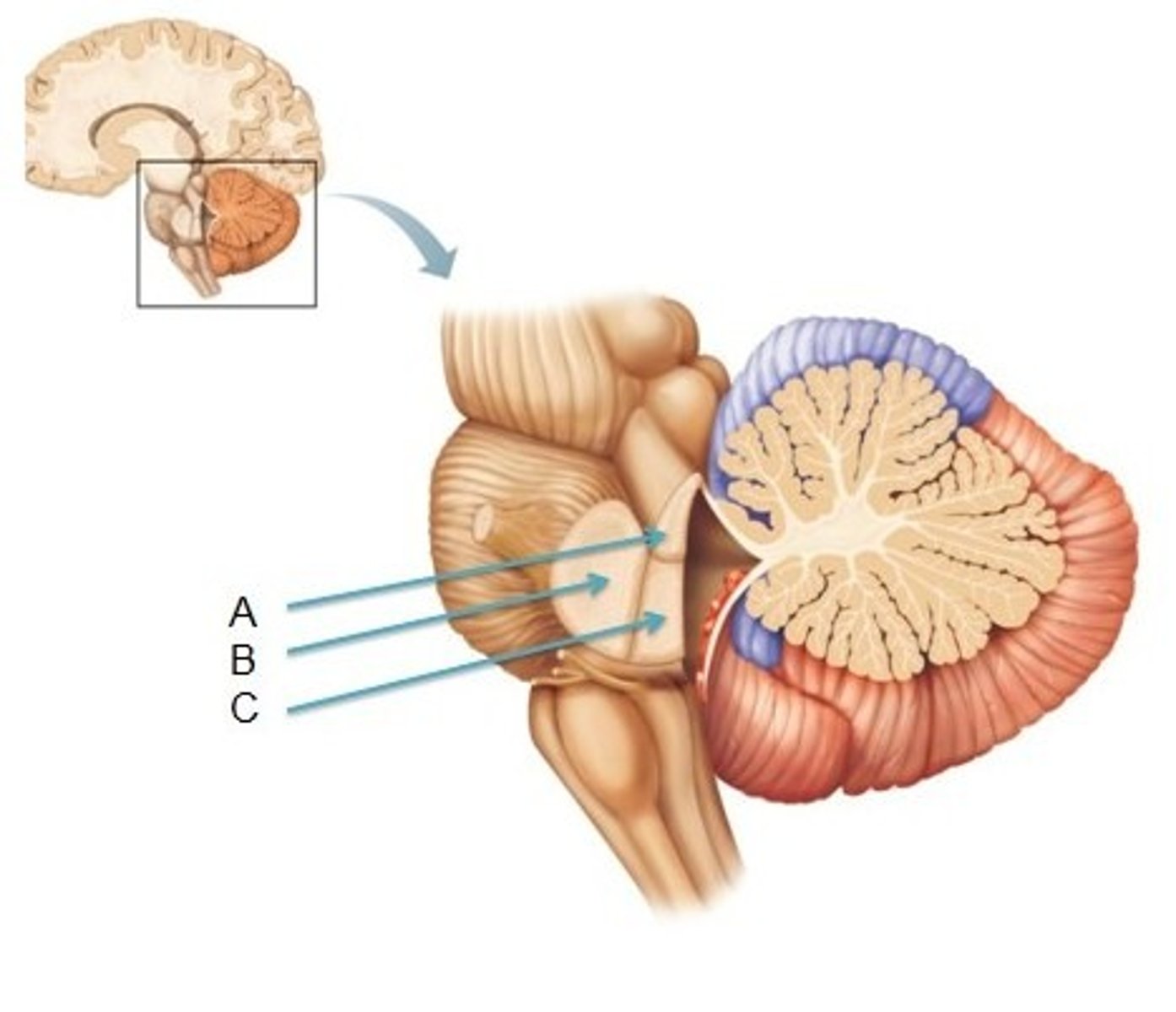
Superior Cerebellar Peduncles
Connects cerebellum to midbrain
Contains contralateral tracts that output to the red nucleus and thalamus
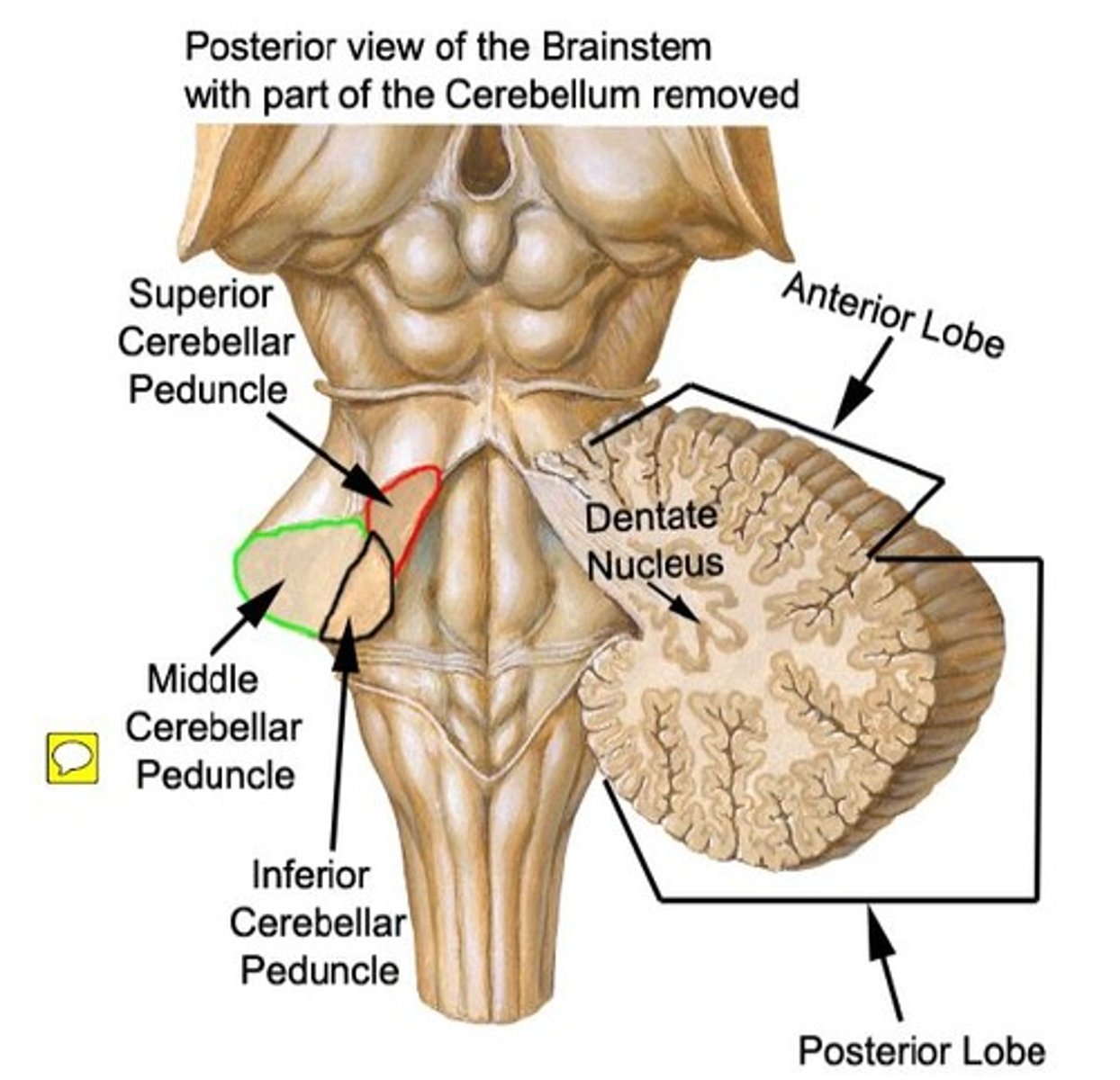
Middle Cerebellar Peduncles
Connect pons to cerebellum
Contain contralateral tracts that receive input from the pons - pontocerebellar
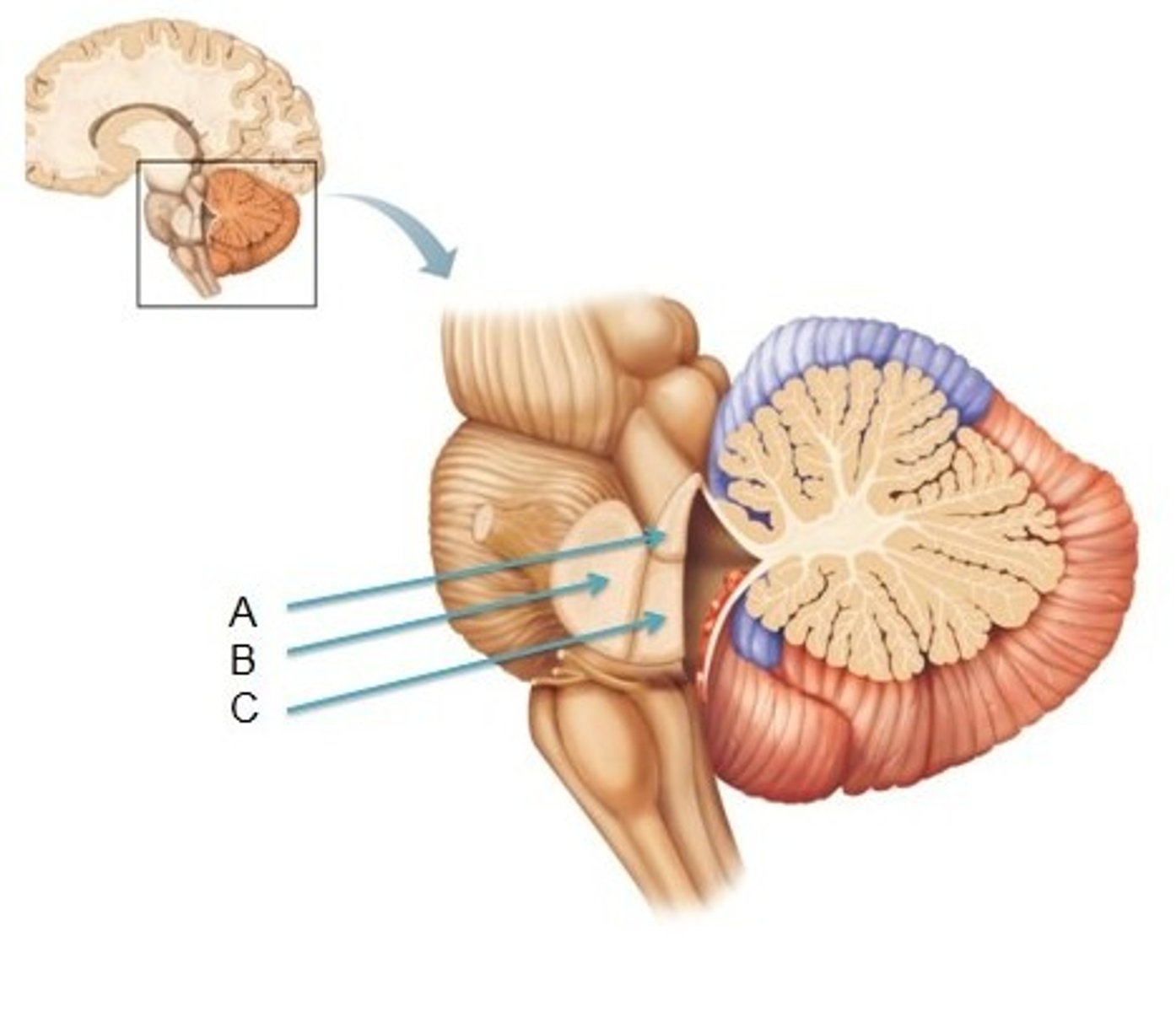
Inferior Cerebellar Peduncles
Connect medulla oblongata to cerebellum
Contains an ipsilateral tract that receives input from the spinal cord - dorsal spinocerebellar
Contains both ipsilateral and contralateral tracts connecting to the reticular and vestibular systems - vestibulospinal and reticulospinal
Contains a contralateral tract connecting to the inferior olivary nucleus - olivocerebellar
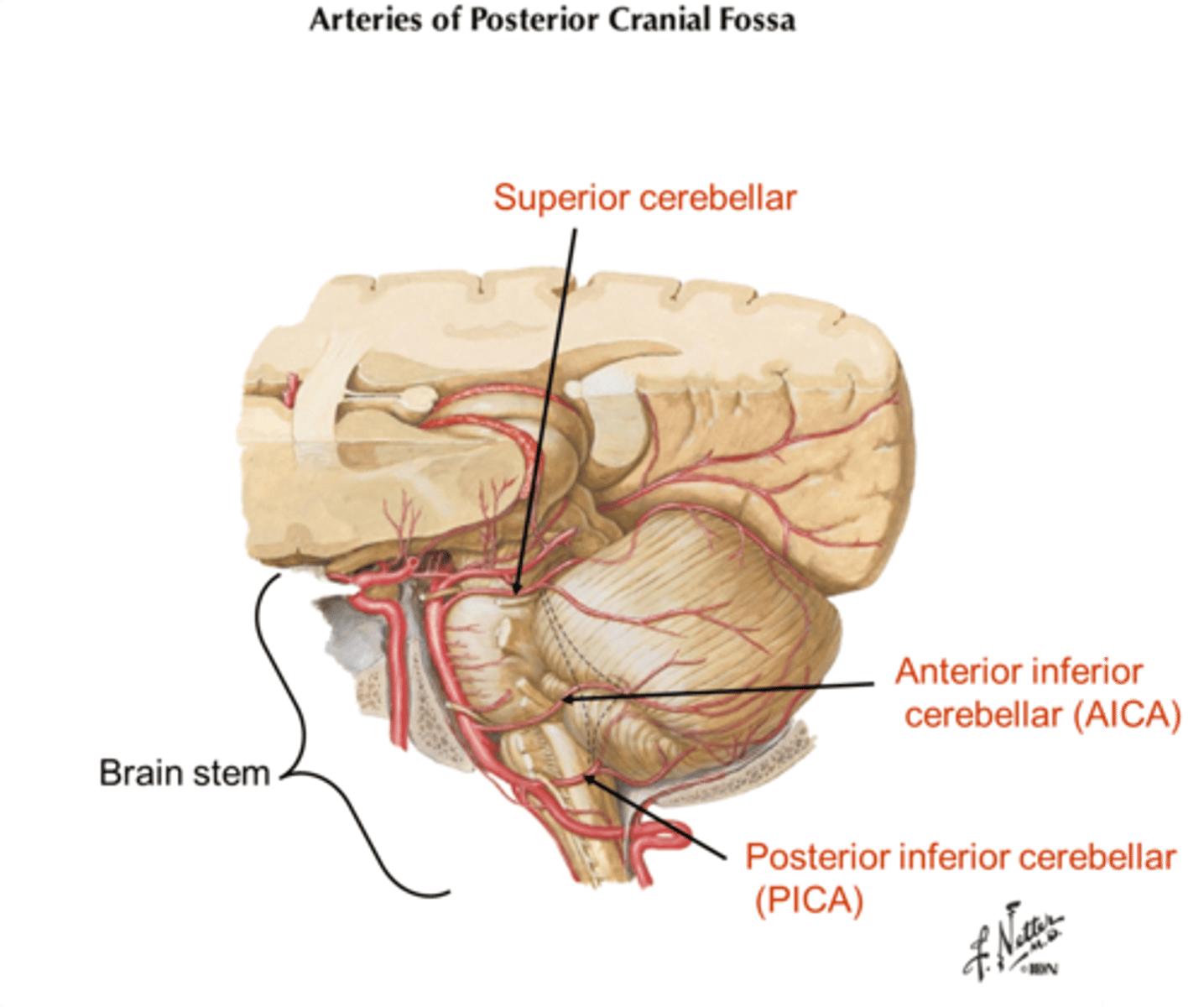
Blood Supply of the Cerebellum
Vertebral-basilar system branches: superior cerebellar, AICA, and PICA
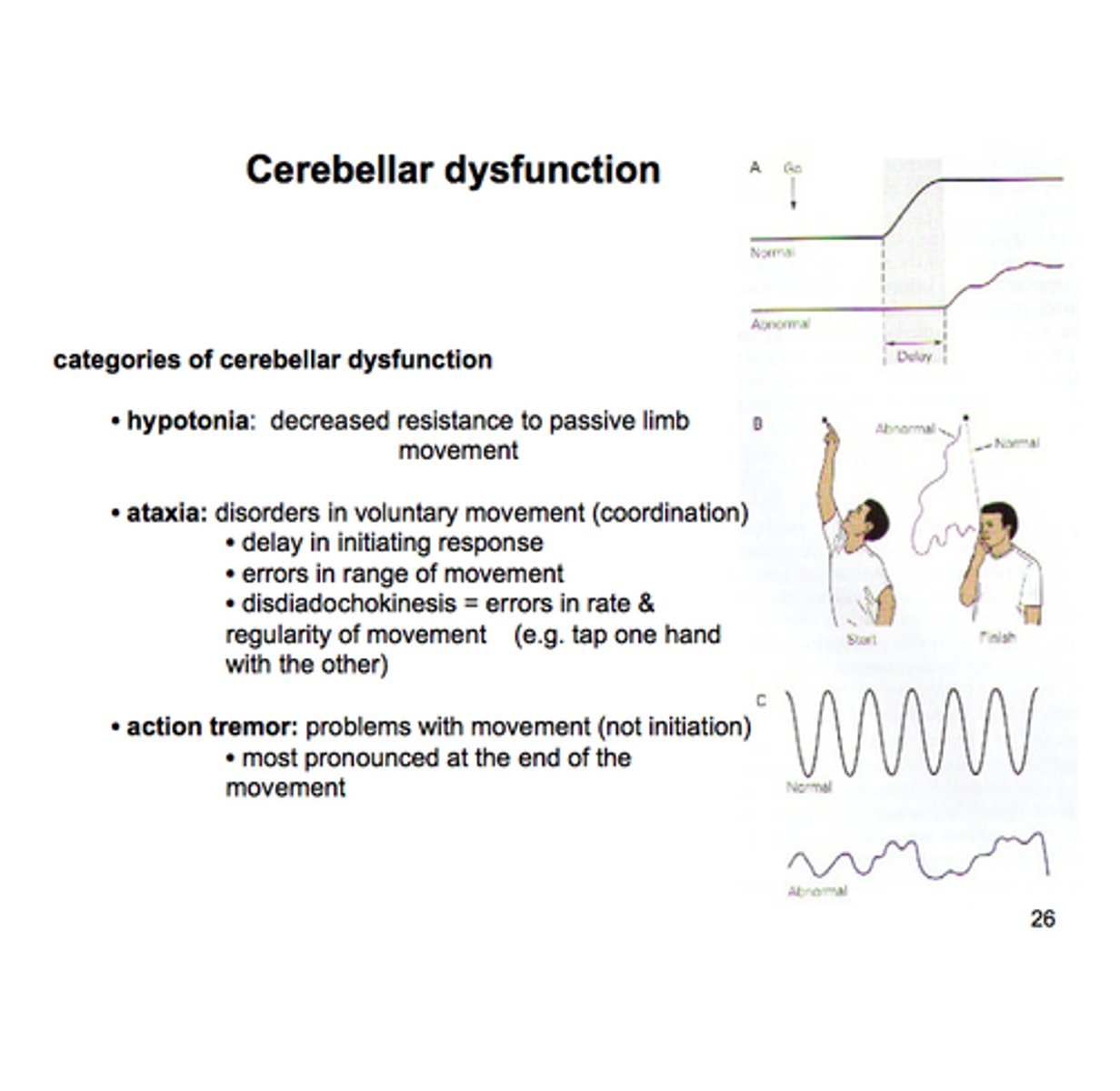
Cerebellar Dysfunction
Ipsilateral defects where the somatotopic organization is reflected
Lesions damaging the deep cerebellar nuclei produce more severe symptoms than lesions only damaging the cerebellar cortex
Signs and symptoms include hypotonia, disequilibrium, and dyssynergy
Dyssynergy
Lack of coordinated action of the muscle groups
Cerebellar Ataxia
Staggering, wide-based gait; difficulty with turns; uncoordinated movement with positive Romberg sign
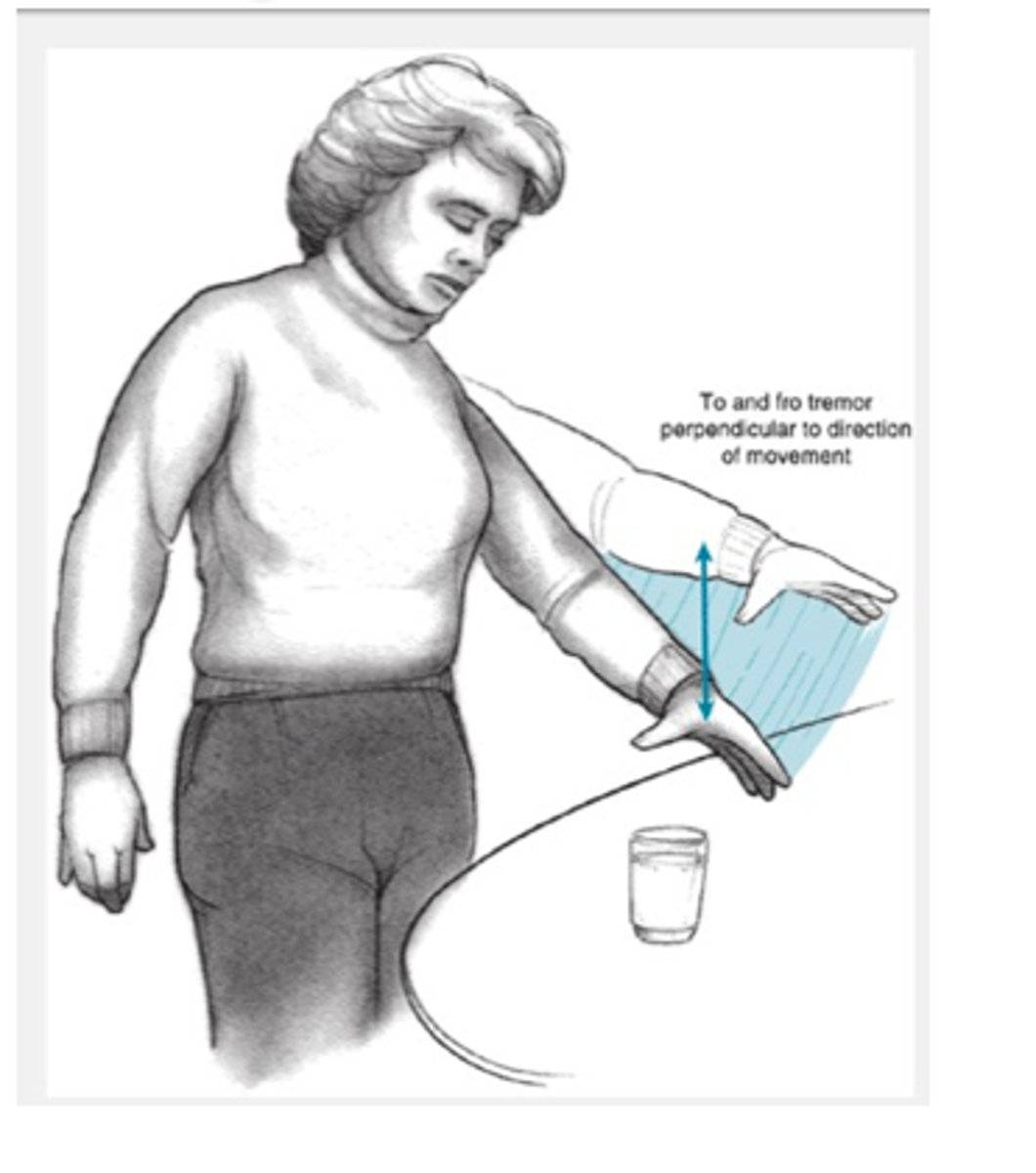
Intention Tremor
Involuntary trembling when an individual attempts a voluntary movement
Dysdiadochokinesia
Inability to perform rapid alternating movements
Dsyarthria
Difficulty speaking due to disruption of muscle control
Nystagmus
Involuntary, jerking movements of the eyes
Phenytoin Intoxication
Caused by use of the anti-epileptic drug, phenytoin
Symptoms: ataxia, nystagmus, gait disturbances, and dysarthria
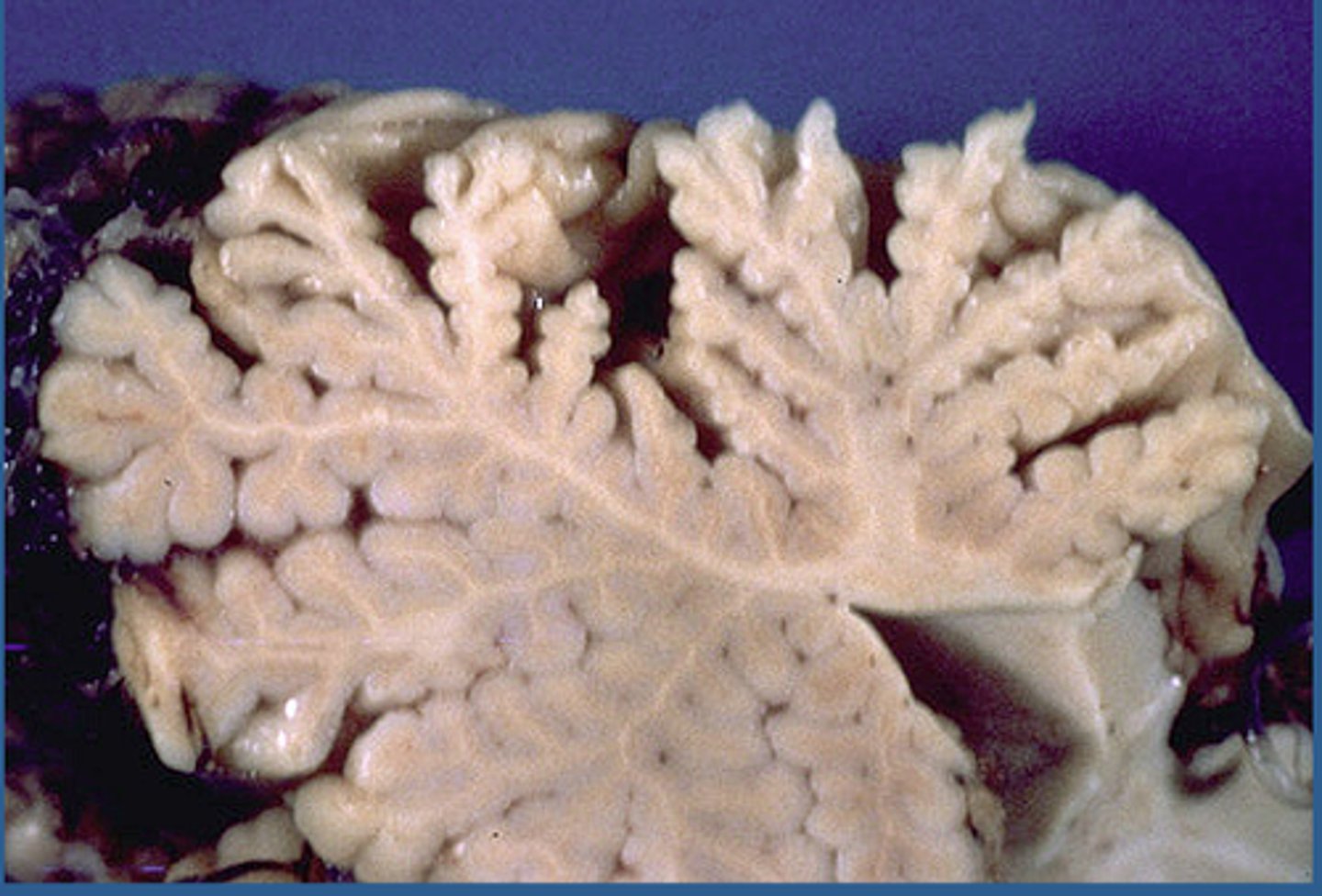
Cerebellar Atrophy
Caused by certain specific inherited disorders
Symptoms: gait ataxia, dysarthria, intention tremor
Tonsillar Herniation
Caused by the cerebellar tonsils herniating through the foramen magnum, resulting in blockage of CSF flow
Symptoms: related to pressure on the cerebellum and medulla, involvement of CNs IX, X, XI, and XII
Arnold-Chiari Phenomenon
Displacement of hindbrain downward through foramen
magnum to obstruct CSF flow
Associated with craniovertebral anomalies, such as spina bifada