252 exam 2
1/227
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
228 Terms
Functions of the Skeletal System
protection: skeleton protects vital organs such as the brain
mineral storage and acid base homeostasis: bone stores minerals such as calcium and phosphate which are necessary for electrolyte and acid base balance
blood cell formation: red bone marrow site of blood cell formation
fat storage: yellow bone marrow stores triglycerides
movement: muscles produce body movement via their attachment to bones
support
Which best describes why doctors recommend that women (XX genotyped individuals), who are prone to estrogen-dependent osteoporosis, take calcium supplements?
A. As women age, their ability to produce Ca2+ decreases and reduced Ca2+ causes the bone to shatter.
B. Women cannot make Ca2+, which is essential to maintaining the shape of bone
C. Estrogen prohibits Ca2+ production by the parathyroid gland, which causes bone to shatter
B. Women cannot make Ca2+, which is essential to maintaining the shape of bone
We can’t make Ca2+ we get it from our diets
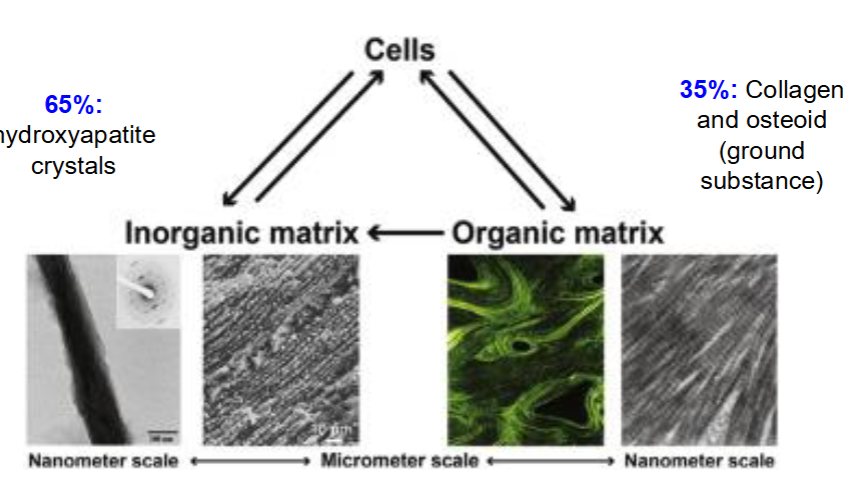
Types of Specialized Connective Tissue: Bone
65%: hydroxyapatite crystals
35%: collagen and osteoid (ground substance)
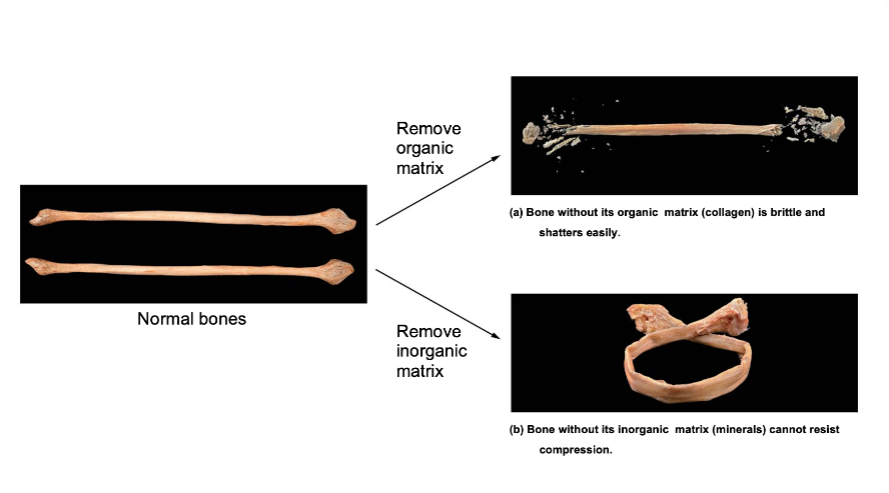
Organic and Inorganic matrices work together to promote bone structure and function
If you remove the organic matrix
collagen is brittle and the bone shatters easily
if you remove the inorganic matrix
minerals cannot resist compression bone will bend/curve
Which of the following statements is/are true?
A. Osteoblasts secrete enzymes that break down the extracellular matrix.
B. Osteocytes are derived from osteoblasts.
C. Both of the above are true statements
D. Neither of the above are true statements
B. Osteocytes are derived from osteoblasts.
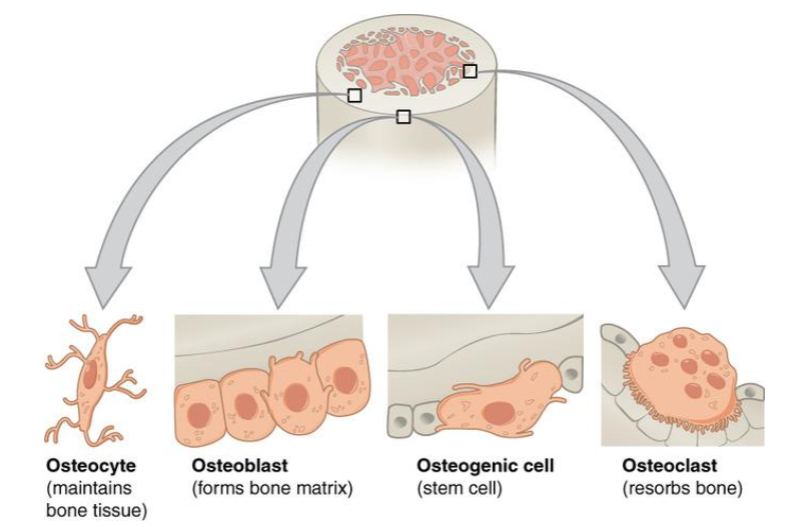
Bone Cells
Osteocyte
maintains bone tissue
Osteoblast
forms bone matrix
Osteogenic cell
stem cell
Osteoclast
resorbs bone
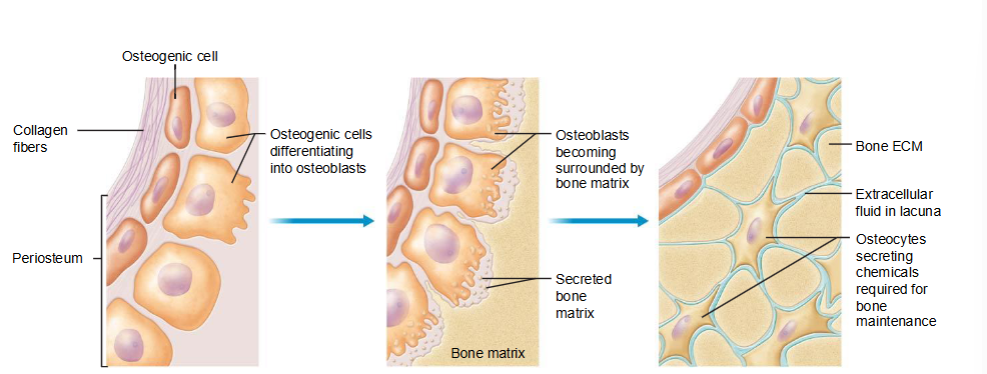
Osteoblasts and Osteocytes
osteogenic cells differentiate into osteoblasts
osteoblasts deposit bone until they are trapped and become osteocytes
osteocytes maintain the bone extracellular matrix (ECM)
Osteocyte
mature bone cells that are amitotic; derived from osteoblasts
thought to be mechanosensory cells that control activity of osteoblasts and osteoclasts
communicate with other osteocytes via gap junctions
Osteoclasts
sit on surface of bone
enzymes and H+ degrade the bone ECM, Components of the bone ECM enter the osteoclast (bone resorption)
Chondrocyte
cells of cartilage that initiate bone formation. They differentiate into osteogenic cells → osteoblasts
epiphyseal plate
Diaphyseal side
zone of ossification
osteoblasts and calcified cartilage
zone of calcification
dead chondrocytes
zone of hypertrophy and maturation
zone of proliferation
chondrocytes in lacunae
zone of reserve cartilage
epiphyseal plate
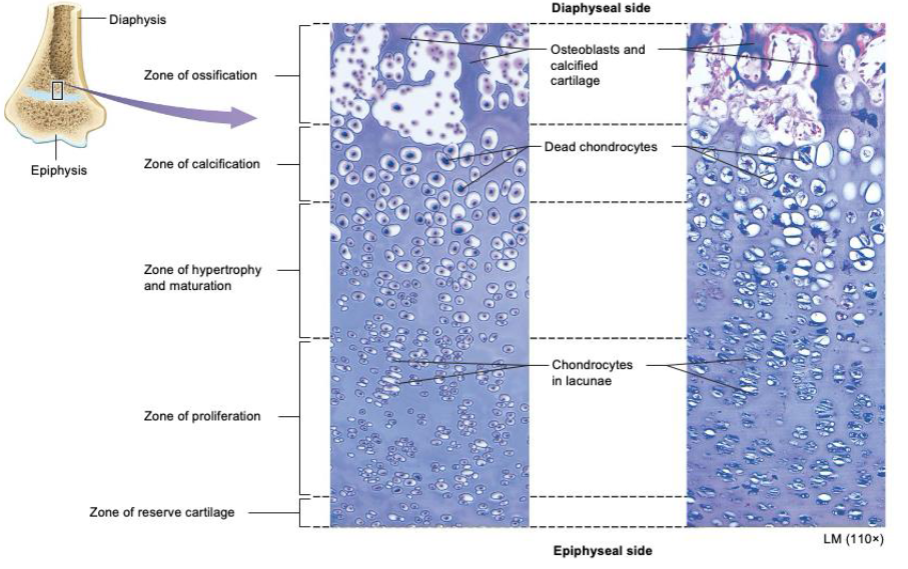
Which epiphyseal zone is closest to the diaphysis?
A. Zone of ossification
B. Zone of calcification
C. Zone of hypertrophy and maturation
D. Zone of proliferation
A. Zone of ossification
Longitudinal Bone Growth
Diaphysis
newly formed bone
bone is resorbed by osteoclasts and replaced with bone
zone of ossification
osteoblasts invade calcified cartilage and lay down bone
zone of calcification
chondrocytes die (far from blood supply) and ECM calcifies
zone of hypertrophy and maturation
chondrocytes enlarge, mature, and stop dividing
zone of proliferation
chondrocytes divide in the zone of proliferation
epiphyseal plate
Growth hormone induces longitudinal bone growth
longitudinal bone growth = bone grows in length
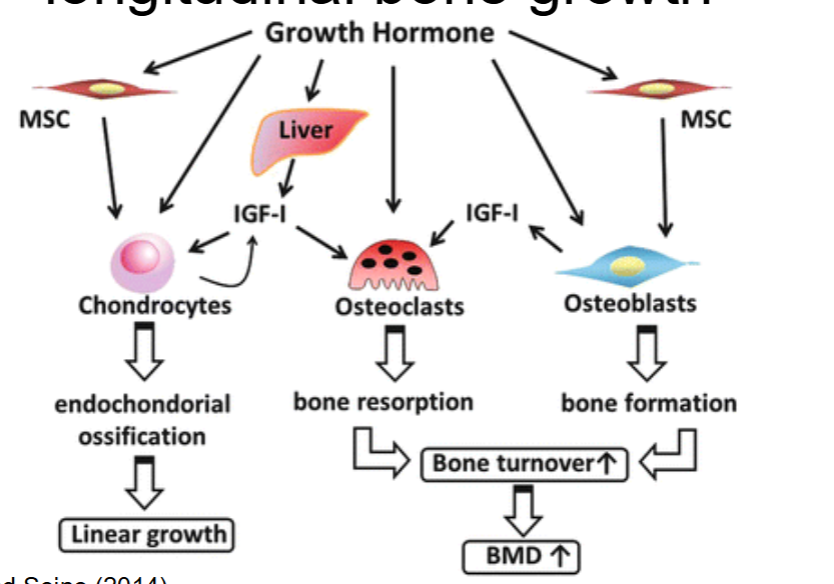
Testosterone and Estrogen also promote bone growth
appositional bone growth - growth in width (testosterone)
increases rate of mitosis and epiphyseal plate
can increase the closure of epiphyseal plates (estrogen is more potent than testosterone)
Testosterone and estrogen also prohibit the activity of osteoclasts
Estrogen activates osteoclast apoptosis and inhibits osteoclast activity
androgens like testosterone inhibit osteoclast activity and osteoblast apoptosis and activate osteoblast proliferation and differentiation
Bone terminology
bone remodeling: continuous formation and loss of bone
bone deposition: formation of new bone
bone resorption: destruction of old bone
Bone deposition is caused by increased osteoblast activity due to:
compressional load/exercise
tension on bone
testosterone
vitamin consumption
Bone deposition is caused by decreased osteoclast activity due to:
estrogen
calcitonin
increased blood calcium ion concentration
Bone resorption is caused by decreased osteoblast activity due to
inadequate exercise
inadequate vitamin consumption
bone resorption is caused by increased osteoclast activity due to
continuous pressure placed on bone
parathyroid hormone
decrease in blood calcium ion concentration
If there is imbalance in bone deposition and resorption what disease(s) could occur?
rheumatoid arthritis
Below is a graph with age starting at adulthood on the x-axis and bone
mineral content on the Y-axis.
• Draw a solid line for what we’d expect for individuals who regularly
perform cardio exercises (e.g., walking, running, swimming).
• Draw a dotted line for what we’d expect for individuals who regularly
weight train.
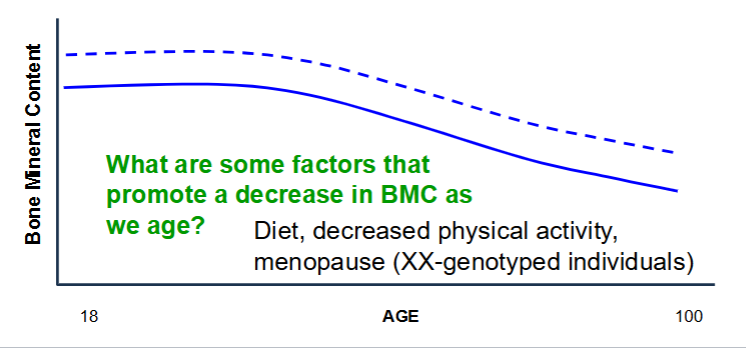
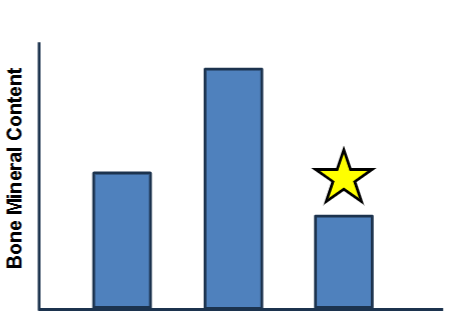
Below is a graph of XY-individuals (same age; no homeostatic imbalances) who regularly engage in different physical activities. The star likely represents:
A. Someone who swims for an hour, 4 times per week.
B. Someone who walks for an hour, 4 times per week while wearing a 12 lb vest.
C. Someone who spends 45 minutes in the gym lifting free weights 3 times per week.
A. Someone who swims for an hour, 4 times per week.
Why is eating oranges (rich in vitamin C) important to bone health?
A. Promotes Ca2+ deposition in bone
B. Promotes the synthesis of collagen
C. Both of the above
D. Neither of the above
Promotes the synthesis of collagen
True or False: when you drink or consume collagen, the collagen immediately goes to your bones / tissues.
FALSE
Factors Promoting bone remodeling
Hormones
Testosterone – bone deposition
Estrogen – inhibits osteoclast activity
Nutrition
Calcium
Parathyroid hormone increases Ca2+ release into blood stream
Calcitonin hormone promotes deposition of Ca2+ into bone
Vitamin D – promotes Ca2+ uptake in the intestines
Safe sun exposure or consumption of dairy products.
Vitamin C – required for synthesis of collagen
Vitamin K – glycoprotein production (bind Ca2+)
Protein – collagen synthesis
Blood Ca2+ homeostasis
Stimulus: blood calcium decreases below normal range
receptor: parathyroid gland cells detect a low blood Ca2+ level
control center: parathyroid gland cells release PTH int the blood
effector/response: osteoclasts resorb bone, kidneys retain Ca2+, intestines absorb Ca2+
in homeostatic range: as blood Ca2+ returns to normal, feedback stops effector responses
Properties of muscle cells
contractility - ability to contract (but not necessarily shorten)
excitability - responsive to stimuli
conductivity - electrical changes across the membrane
distensibility - stretch without damage
elasticity - stretch and retain shape
Which of the following are true (select all that apply)?
A. Striated cells are always multinucleated
B. Striated muscle tissue can be associated with voluntary and involuntary movements
C. Smooth muscle cells communicate with each other via gap junctions
D. Smooth muscle cells are only found in the heart
E. Striated muscle cells can have gap and tight junctions
B. Striated muscle tissue can be associated with voluntary and involuntary movements
C. Smooth muscle cells communicate with each other via gap junctions
E. Striated muscle cells can have gap and tight junctions
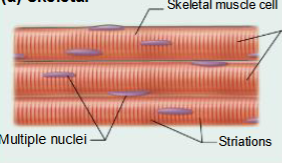
Skeletal Muscle Tissue
Structure
long, cylindrical striated muscle fibers; cells are multinucleated.
Location
mostly attached to skeleton
Voluntary
Function
produced movement of the body
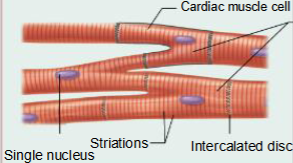
Cardiac Muscle Tissue
Structure
Short, wide, branching striated cardiac muscle cells with intercalated discs; cells have a single nucleus or two nuclei.
Location
heart
Involuntary
Function
produces beating of the heart
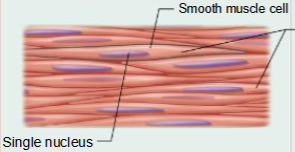
Smooth Muscle Tissue
Structure
thin, smooth muscle cells, generally joined by gap junctions; cells have a single nucleus
Location
walls of hollow organs, as well as in the skin, and the eyes
Involuntary
Function
changes diameter of hollow organs
causes hairs to stand erect
adjusts the shape of the lens and the size of the pupil of the eye
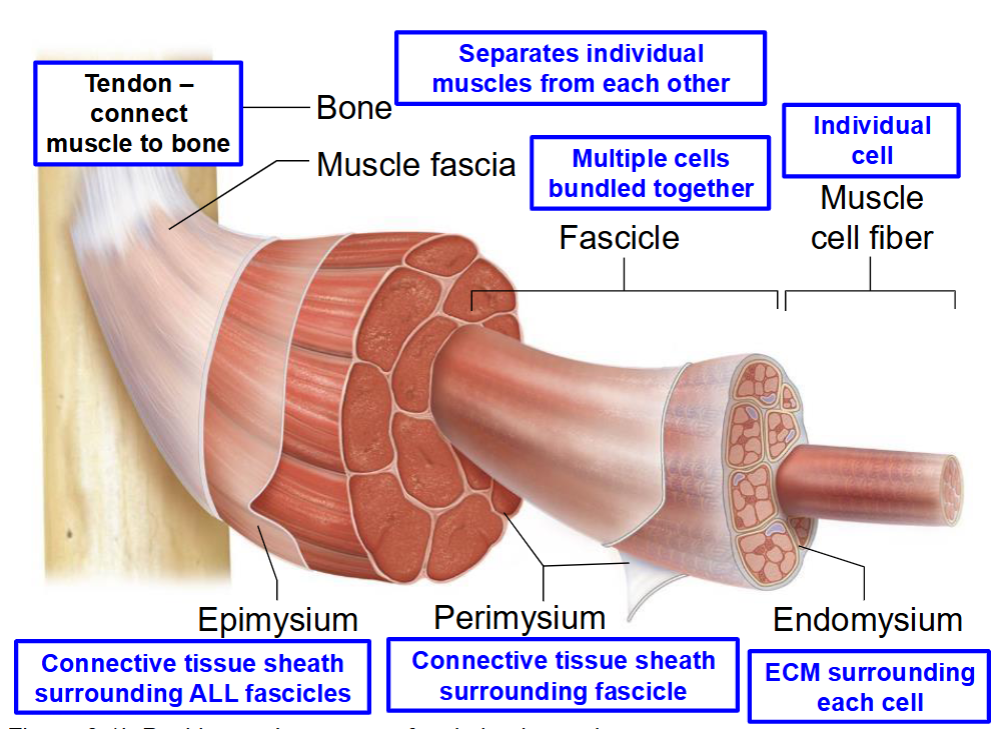
1. Extracellular matrix surrounding a single muscle fiber.
2. Connective tissue surrounding a cluster of many muscle fibers.
3. Connective tissue that connects muscle to bone
4. Connective tissue that surrounds numerous fascicles
A. Endomysium
B. Epimysium
C. Perimysium
D. Tendon
Function of Skeletal Muscles
Muscle tension - contraction to generate force
action = production of body movement
heat production
Muscle movement is a lever system
1. Lever
2. Load or object you are moving
3. Force (or effort) applied to the lever to move the object
4. Fulcrum – hinge point that allows lever to move
Features of skeletal muscle cells
• Long, thin cylinders
• Striated (striped)
• Multinucleated
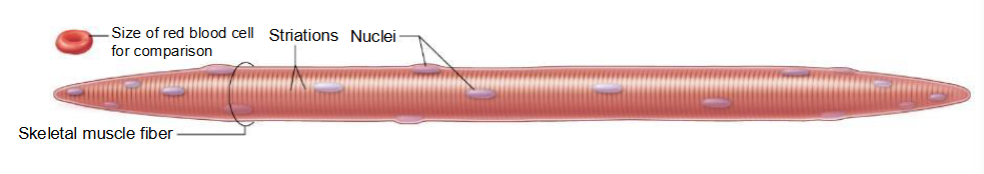
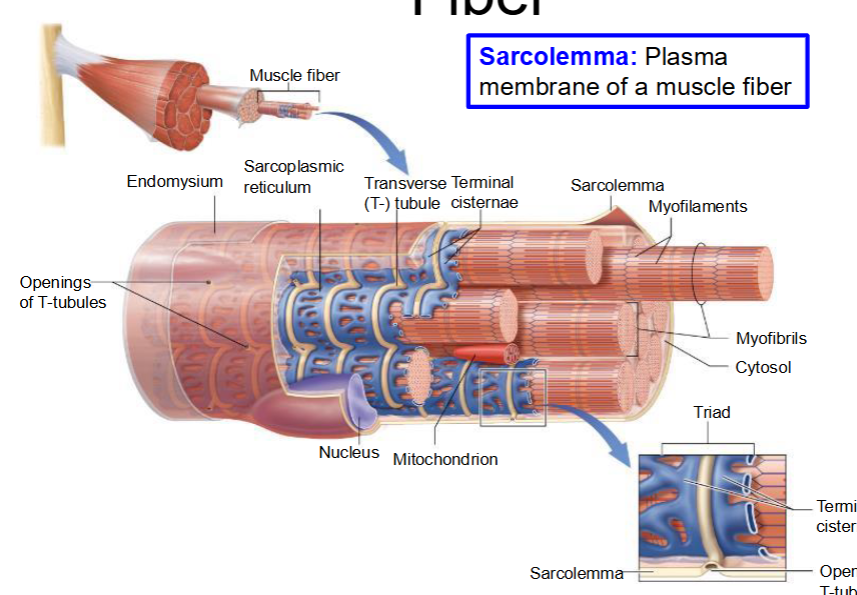
Structure of Skeletal Muscle Fiber
Sarcolemma: Plasma membrane of a muscle fiber
Myofibril – proteins involved in cell contraction
Sarcoplasmic reticulum – smooth endoplasmic reticulum that stores and releases Ca2+
Transverse tubules (T-tubules) – inward extensions of sarcolemma that form a tunnel-like network and filled with extracellular fluid.
Terminal cisternae – enlarged portions of the sarcoplasmic reticulum on either side of T- tubules
Which region within a sarcomere contains thick filaments only?
A. A band
B. H zone
C. I band
B. H zone
What are thick filaments?
MYOSIN!
Myofibril
Bundles of proteins (myofilaments)
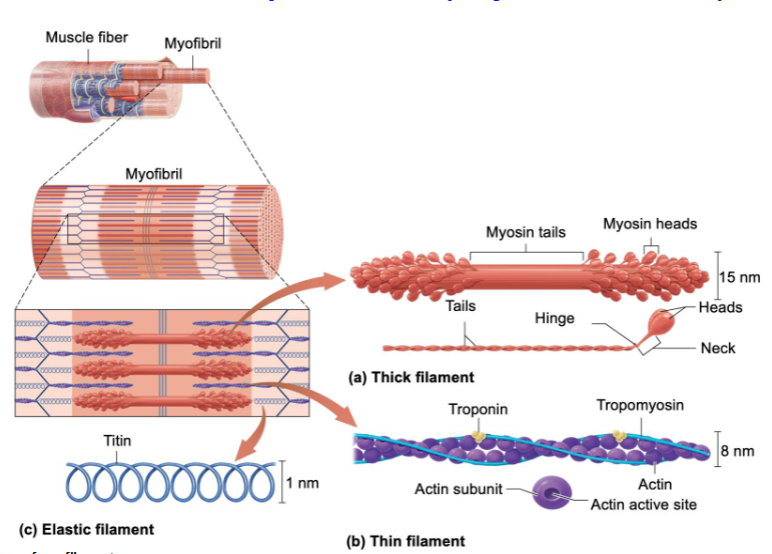
Structural proteins within a myofibril ensure that the myofilaments themselves are in their proper place and promote the structural stability of the myofibril within a muscle fiber. Based on this definition, which of the following proteins would serve as a myofibril structural protein?
A. Myosin
B. Actin
C. Troponin
D. Titin
D. Titin
Stabilizes the thick filament
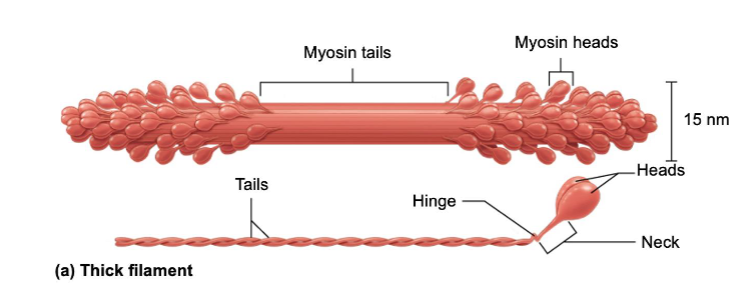
Thick Filaments
Myosin protein clusters – contractile
Head – where thin filaments bind
ATP dependent
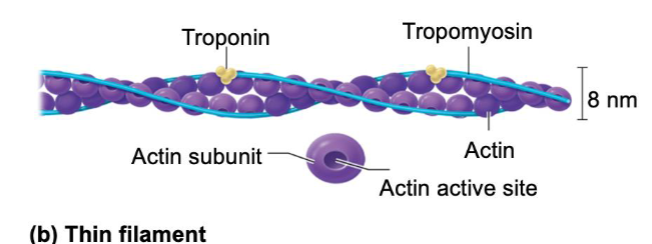
Thin filaments
Actin – subunits of contractile protein with an active site that binds myosin
Tropomyosin – ropelike protein that spirals around actin and covers active site at rest
Troponin – holds the tropomyosin in place
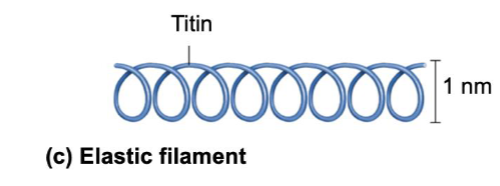
Elastic Filaments
Titin – thinnest filament shaped like a slinky
Holds thick filaments in place
Resist excessive stretching and provide elasticity
Myofilaments form sarcomeres
I band contains only thin filaments (light)
H zone contains only thick filaments
outer edge of A band - the zone of overlap - contains thick and thin filaments (dark)
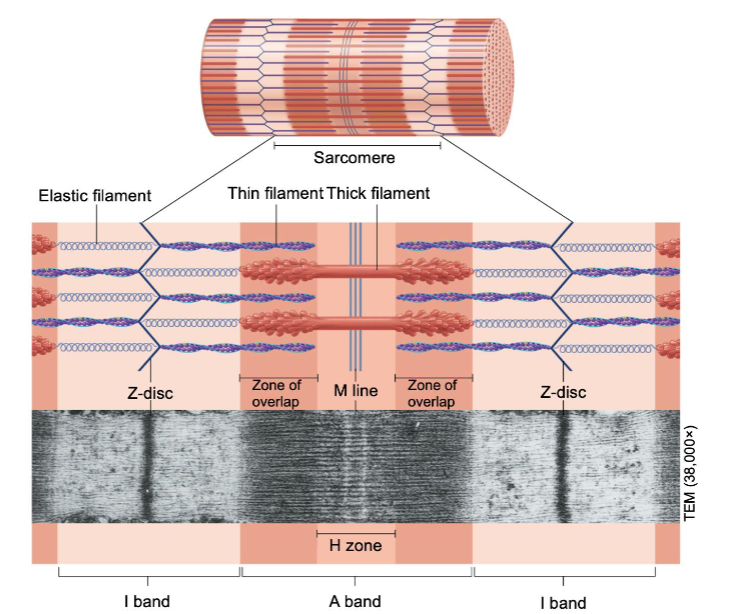
If a muscle fiber were excessively stretched to the extent that the thin and thick filaments did not overlap, the reaction of this fiber to a stimulus would be:
A. It will exert more tension than an unstretched muscle
B. It will exert less tension than an unstretched muscle
C. It will exert tension, but without changing the length of the muscle
D. It will not exert tension
D. It will not exert tension
For a muscle to exert tension, thick and thin filaments must overlap!
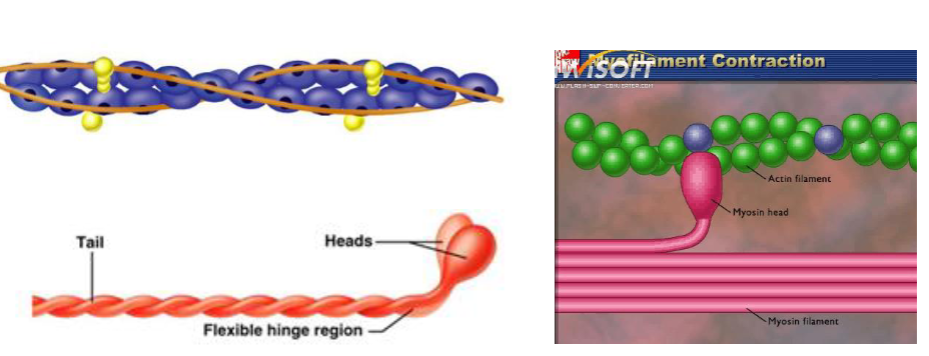
Actin has Myosin binding sites
Once bound, a change in the angle of the myosin head will pull the actin filaments
Sliding Filament Theory
Upon stimulation, myosin heads bind to actin and sliding begins
Thin filaments slide past the thick ones
when fully contraction shorter gap between z lines and reduction in H zone
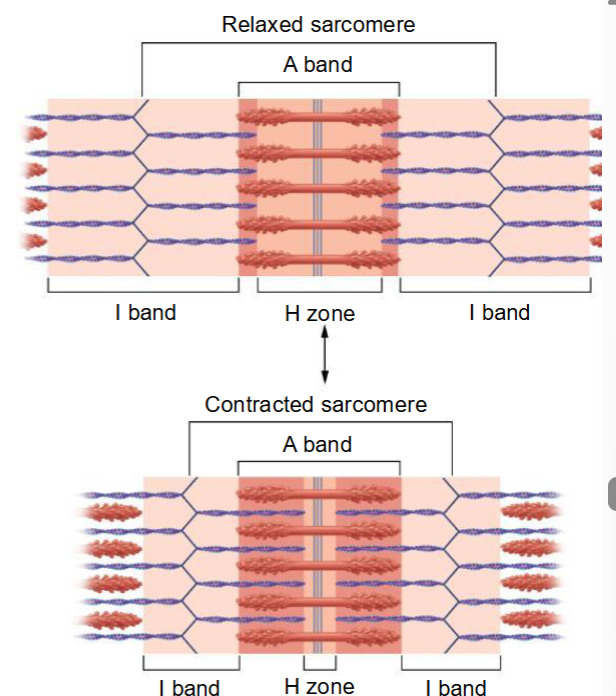
According to the sliding filament theory, which region of a sarcomere changes in length during a muscle contraction?
A. I band only
B. H band only
C. A band only
D. I band and H band
E. I band and A band
F. I band, H band, and A band
D. I band and H band
Sarcomeres and myofibrils
- We have many sarcomeres in one myofibril
- When all sarcomeres shorten, so does the myofibril
- We have many myofibrils in one muscle fiber
- When all myofibrils shorten, so does the muscle cell
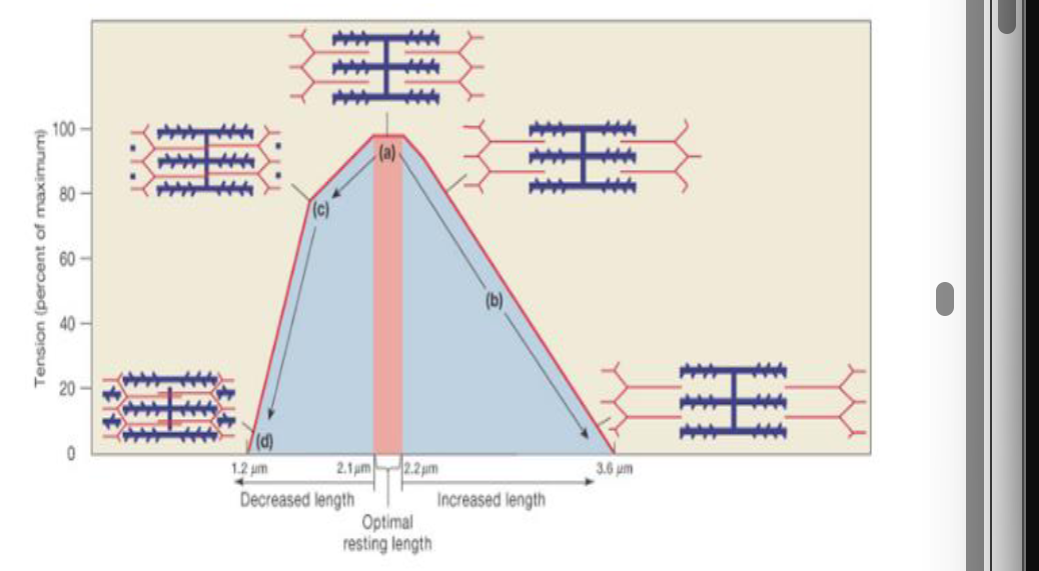
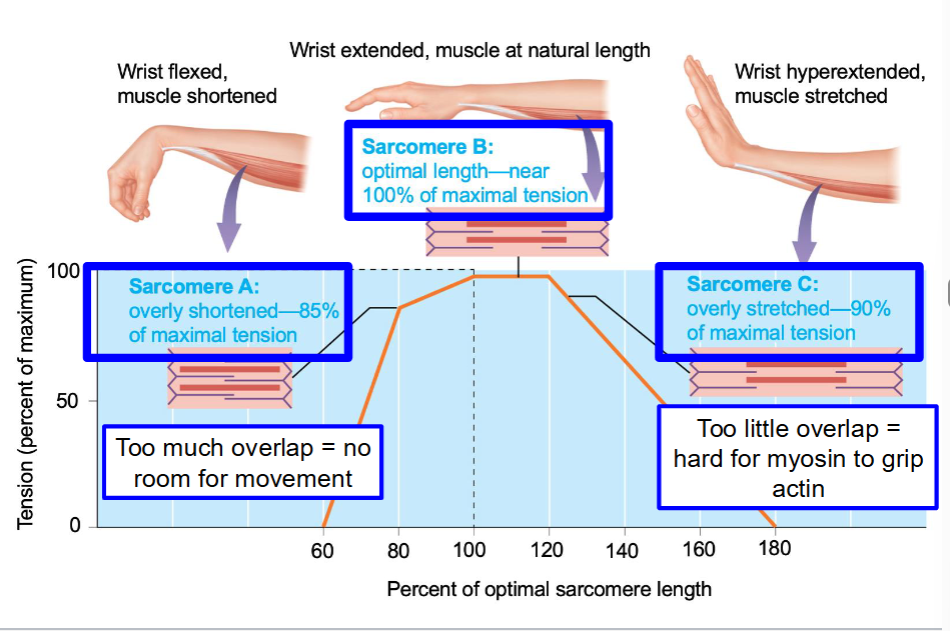
The graph below depicts the length of the sarcomere at rest (x-axis) vs. the tension generated (y-axis; percent of maximum). I
Optimal actin and myosin overlap will produce maximal contraction (tension)
How is myosin and actin interactions regulated?
In a resting state, tropomyosin prevents myosin from binding to actin
Acetylcholine causes muscle contractions when released at the neuromuscular junction. Muscle cells can also propagate action potentials. Therefore, which of the following are present in the membrane of a sarcolemma? (Select all that apply)
A. Voltage-gated K+ channels
B. Voltage-gated Na+ channels
C. K+ leak channels
D. Na+/K+ ATPase
A. Voltage-gated K+ channels
B. Voltage-gated Na+ channels
C. K+ leak channels
D. Na+/K+ ATPase
A and B: Action potentials!
C and D: RMP!
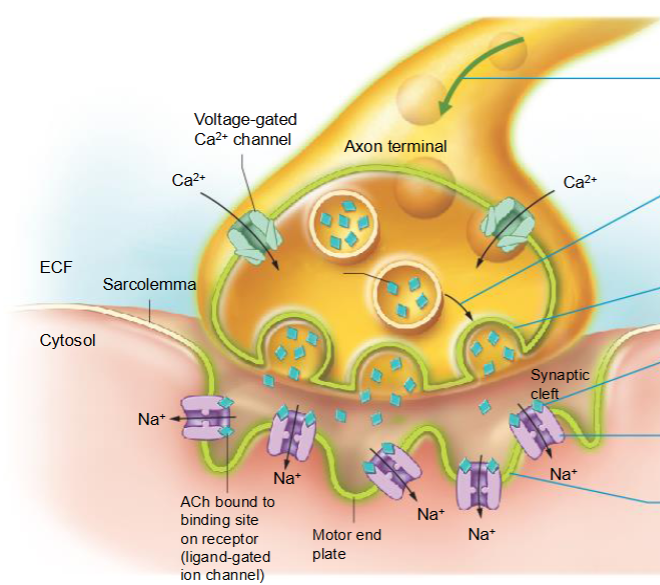
Skeletal muscle is innervated by motor neurons
Acetylcholine (ACh) is the major neurotransmitter that signals to skeletal muscle cells. acetylcholinesterase (AChE) is found in the synaptic cleft.
Motor end plate is region of sarcolemma that has “folded structure” that contains nicotinic cholinergic receptors (needed to induce skeletal muscle contraction)
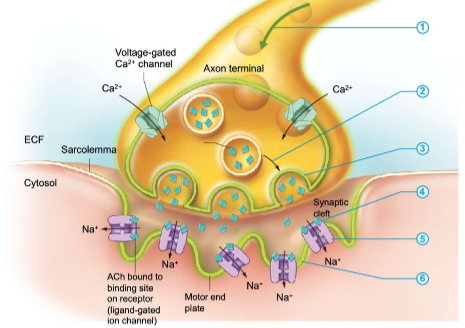
Muscle contraction
an action potential arrives at the axon terminal and triggers Ca2+ channels in the axon terminal to open
Ca2+ entry triggers exocytosis of synaptic vesicles
synaptic vesicles release ACh into the synaptic cleft
ACh binds to ligand gated ion channels in the motor end plate
ion channels open and Na+ enter the muscle fiber
entry of Na+ depolarizes the sarcolemma locally, producing an end plate potential
Neural signals stimulate release of calcium from the SR to the sarcoplasm
ECM in t-tubules
the end plate potential stimulates an action potential
the action potential is propagated down the t-tubules
t tubule depolarization leads to the opening of the Ca2+ channels in the Sr and Ca2+ enter the cytosol
Calcium binds to troponin, leading to release of tropomyosin from the myosin-binding sites
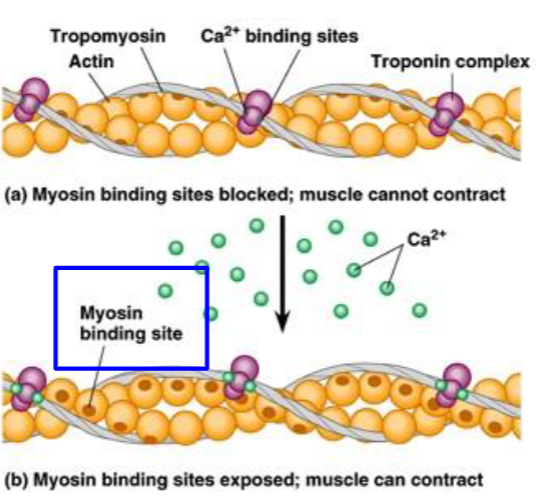
crossbridge cycle starting ATP hydrolysis
ATP hydrolysis “cocks” the myosin head
the myosin binds to actin
the power stroke occurs when the phosphate detaches from the myosin head and myosin pulls actin toward the center of the sarcomere; ADP leaves the myosin head at the end of the power stroke
ATP breaks the attachment of myosin to actin (cycle restarts)
crossbridge cycle is repeated to contract the sarcomere
How many ATP molecules are required for a single
crossbridge cycle during the contraction phase?
A. 1
B. 2
C. 3
D. 4
1
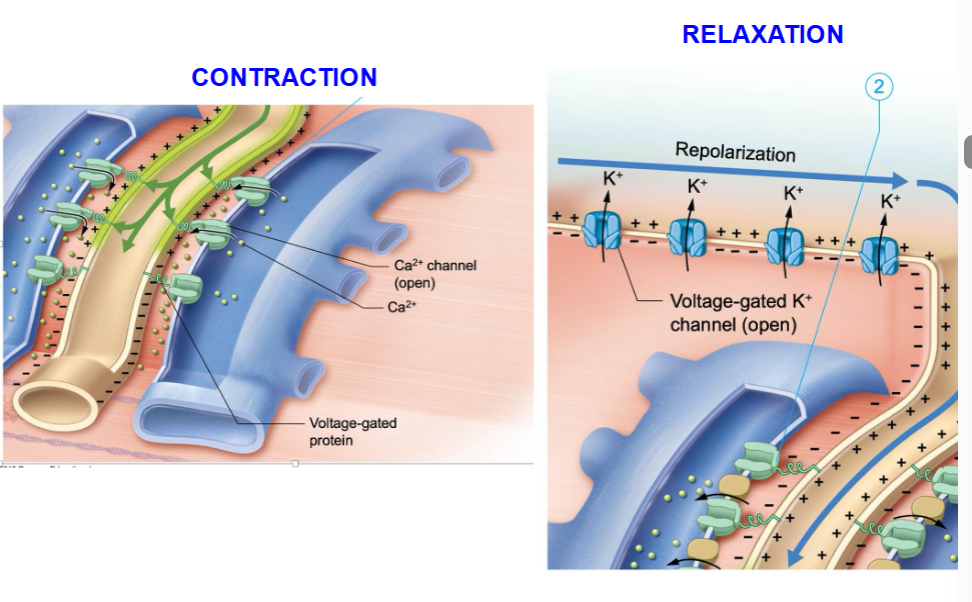
Muscle relaxation
acetylcholinesterase degrades the remaining ACh, and the final repolarization begins
the sarcolemma returns to its resting membrane potential (-90 mV) and the Ca2+ channels in the SR close
Ca2+ are pumped back into the SR returning the Ca2+ concentration in the cytosol to its resting level
troponin and tropomyosin block the active sites of actin, and the muscle relaxes
ATP is required for cells to relax T or F
True
Ca2+ and AChE work continuously to allow for muscle contraction
• Muscle that is unable to relax = spasm
• Rigor mortis – when muscles cannot relax after death (Ca2+ remains in the cytosol and stimulate contraction)
Muscle cells need a lot of ATP
Na+/K+ ATPase that maintains restingmembrane potential (-90 mV) of the sarcolemma
Muscle contraction – crossbridge cycle and actin / myosin interactions
Muscle relaxation – active transport of Ca2+ back into the sarcoplasmic reticulum
Muscle cells do not store high amounts of cytosolic ATP – they must have mechanisms to generate it quickly!
Creatine phosphate is the main immediate source of ATP in skeletal muscle cells during contraction.
True
False
True
Three mechanisms that skeletal muscles use to generate ATP
Immediate energy needs
creatine kinase
glycolytic catabolism
long-term energy needs
oxidative catabolism
Glycolytic Catabolism
1 glucose = 2 (net) ATP
Glucose source
Glucose from bloodstream
Glycogen stores in muscle cells
Oxygen dependent and independent
Aerobic – 2 pyruvate enter mitochondria and Citric Acid cycle
Anaerobic – 2 pyruvate converted to 2 lactate (lactic acid)
Short-term energy
Equation for short term energy needs via creatine kinase
ADP + creatine phosphate ←-> creatine + ATP
The Cori cycle
converts lactate into glucose
Oxidative respiration
Oxygen-dependent mechanism that generates ~32-38 ATP per glucose
Three stages:
Glycolysis (2 net ATP) – cytosol
Pyruvate oxidation and Citric Acid cycle (2 net ATP) -- mitochondria (CAC has 2 rounds)
Oxidative phosphorylation (~28-34 net ATP) – mitochondria
Long-term ATP
Oxygen dependence
Oxygen (non-polar) diffuses into the muscle cell from the bloodstream
Myoglobin – oxygen-carrying protein found in the cytosol of muscle cells
Releases O2 to be used in the mitochondria for oxidative catabolism
Contraction and Relaxation
Which type of wave summation would you expect to observe in a muscle fiber that is being used to lift something heavy for an extended period of time?
A. Unfused tetanus
B. Fused tetanus
B. Fused tetanus
Would need sustained to generate maximum tension in a muscle fiber to lift something heavy for an extended period of time – would therefore expect frequent action potentials.
Draw what the curve would look like for a fused and unfused tetanus.
Wave summation: the amount of tension produced depends on the frequency of stimulation
for an unfused tetanus we would expect more frequent stimuli for a fused tetanus we would expect less frequent stimuli
muscle fatigue is associated with a fused tetanus
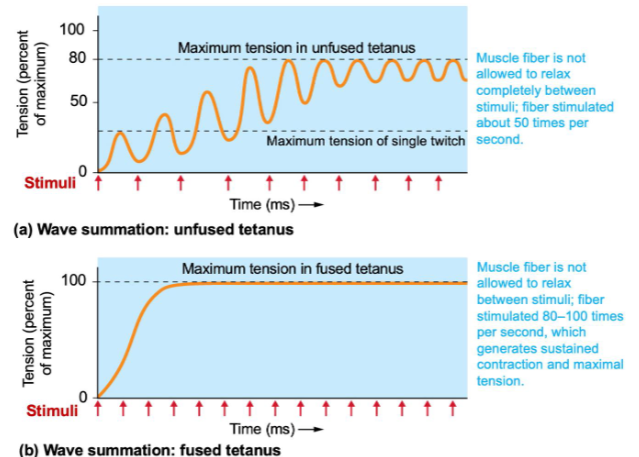
Increasing stimuli frequency = increasing tension
- New stimulus starts before the Ca++ is returns to the SR
- Fused tetanus will lead to muscle fatigue
Again with lifting something heavy for an extended period of time. Which type of sarcomere would be LEAST effective at generating the required tension to lift the object?
A. Sarcomere that is overly short
B. Sarcomere that is overly stretched
Sarcomere that is overly short
Length-Tension Relationship
too much overlap = no room for movement
too little overlap = hard for myosin to grip actin
Myosin ATPase
Regulates how quickly a muscle fiber proceeds through a twitch contraction
Twitch Fibers
Fast twitch fibers: high myosin ATPase activity.
Found in muscles that move body parts quickly (e.g., eyes).
Slow twitch fibers: low myosin ATPase activity.
Found in muscles that require slow and sustained contractions (e.g., back muscles that maintain posture)
Availability of ATP regulates the speed of the twitch contractions
In which type of muscle fiber are you most
likely going to generate lactate?
A. Type I
B. Type IIa
C. Type IIx
C. Type IIx
Fast twitching fibers and primarily generate ATP via glycolysis (anaerobic)
Differentiating between Twitch fibers
Type I:slow oxidative
small intermediate in diameter
require high ATP levels and maintain extended contractions
e.g. sitting in chair
Type II:
large in diameter and contract rapidly but fatigue quickly
rely on glycolytic energy and have reduced myoglobulin levels
IIa oxidative glycolytic: fast, precise e.g. handwriting notes
IIx glycolytic: fast anaerobic, buildup of lactic acid, greatest glycogen levels, e.g.sprinting to class
Dr. Ott is doing an endurance ride on her Peloton. Which type of skeletal muscle fibers helps her to be successful on her long distance, endurance ride?
A. Type I
B. Type IIa
C. Type IIx
B. Type IIa
The Motor Unit
Average motor unit = approx. 150 muscle fibers
Fine control = multiple small motor units
Large and powerful muscles = 2000 – 3000 muscle fibers / motor unit
Each motor unit consists of a single class of muscle fiber
Recruitment
The greater the force (tension) needed, the greater the motor units that are activated.
Slow motor units (type I fibers) are activated first, followed by fast motor units (type II fibers) if additional force is needed.
Muscle Tone
Involuntary activation of motor units to generate a small amount of tension of a muscle at rest
Hypotonia – low skeletal muscle tone
Hypertonia – abnormally high muscle tone
You are in the gym doing bicep curls. When you lower the dumbbell back to resting position, which type of muscle contraction are you performing?
A. Isotonic concentric
B. Isotonic eccentric
C. Isometric contraction
B. Isotonic eccentric
Isotonic Concentric Contraction
Muscle tissue shortens
Force generated by muscle is greater than the external load
Isotonic Eccentric Contraction
Muscle tissue lengthens
Force generated by muscle is less than the load
Elastic filaments (sarcomeres) stretch, although motor units are generating tension
Requires greatest amount of tension
Muscle is elongating while under tension from opposing force that is greater than force generated by the muscle – control reposition of the load (no tension = flop).
Isometric Contractions
Length of muscle does not change
During isometric contractions:
A. Myosin filaments exert tension on the thin filaments, but sarcomeres do not shorten
B. Myosin heads do NOT bind to actin filaments
C. There is no overlap between thick and thin filaments to begin with
D. The sarcomere shortens, but the muscle organ does not
D. The sarcomere shortens, but the muscle organ does not
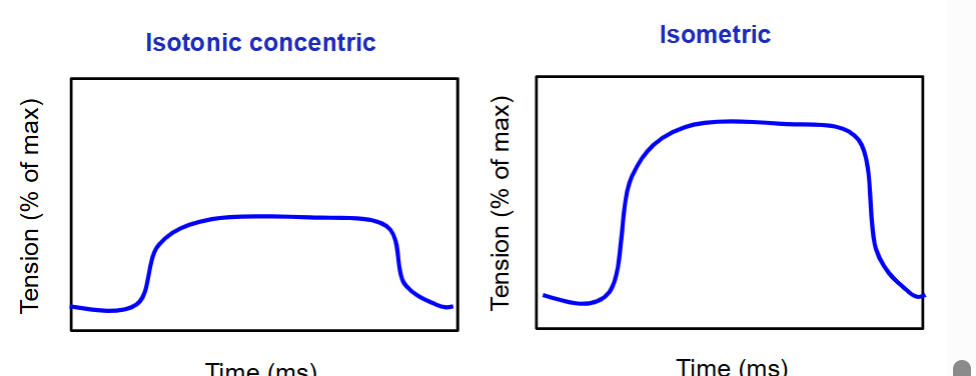
The graphs below depict time (x-axis) and tension (y-axis).
draw what the curves would look like for an isotonic concentric and isometric contraction.
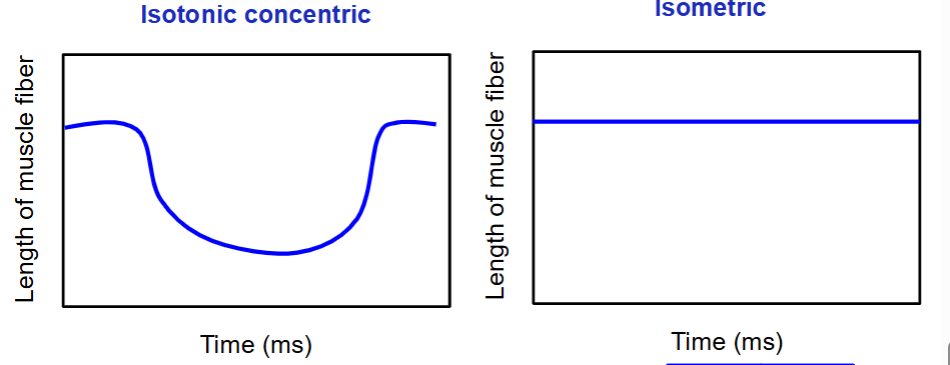
The graphs below now depict time (x-axis) and length of muscle fiber (y-axis). draw what the curves would look like for an isotonic concentric and isometric contraction.
Elastic components of the muscle organ
(tendons, connective tissues between fibers, elastic molecules in the cytoplasm)
Principle of Myoplasticity
Muscle will alter its structure to support its function
Kenneth “Flex” Wheeler is a world-famous body builder who has won countless championships. Which best describes the anatomy of Flex’s muscle fibers?
A. Flex’s muscle fibers are enriched with blood vessels
B. Flex’s muscle fibers are enriched with mitochondria
C. Flex’s muscle fibers are enriched with myofibrils
C. Flex’s muscle fibers are enriched with myofibrils
Endurance Training
More repetitions, lighter load (swimming, jogging, cycling)
Resistance Training
Fewer repetitions, higher load (Strength or resistance training)
Hypertrophy = Enlargement of an organ, tissue, or cell.
Sedentary Lifestyle
Physical inactivity
Atrophy = A decrease in the size of a cell or organ
Muscle Fatigue
The inability to maintain a level of intensity during exercise.
Depletion of metabolites (creatine phosphate, glycogen, blood glucose)
Reduced oxygen supply to muscle fibers (reduced O2 bound to myoglobin) and greater dependency on glycolysis
Accumulation of Ca2+, ADP, PO4-
Environment – high heat, high altitude
We continue to have elevated ventilation after our workouts to help us rid our muscle fibers of any lactic acid buildup.
A. True
B. False
False EPOC!!
Is homeostasis out of balance when we workout?
• Elevated body temperature – energy is lost during glycolysis and oxidative metabolism, raising our body temperature
• Ion concentrations are abnormal – abnormal [Na+] and [Ca2+] in the cytosol and [K+] in the extracellular fluid
• Correct blood pH – lactic acid and CO2 in the blood can reduce the blood pH
Excess Postexercise Oxygen Consumption (EPOC)
When the rate of ventilation remains high after our workout has concluded
EPOC restores homeostasis
• Elevated body temperature – sweating, an ATP-dependent process (active transport of Na+ out of cells), helps us to decrease our body temperature
• Ion concentrations are abnormal – Na+/K+ ATPase helps to restore ion gradients across a membrane (active transport – requires ATP)
• Correct blood pH – exhalation of CO2 helps to restore the slight alkalinity of blood (7.35-7.45)
Functions of blood
• Gas exchange – O2 in, CO2 out
• Distribute solutes – nutrients, ions, hormones, waste
• IMMUNE FUNCTION!!!!!!!!!
• Body temperature – distributes heat that is given off by metabolic reactions
• Clotting / wound healing
• Acid-base homeostasis (buffer)
• Blood pressure – volume of blood
Blood
We have ~5 liters (8% of body weight)
Connective tissue
Liquid (plasma) and formed elements (cells)