chapter 31: internal fluids
1/20
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
21 Terms
what is the general purpose of our circulatory and respiratory systems and what major process is involved in all of them?
general purpose is homeostasis
how we get and move oxygen
how organisms move nutrients plus move/get rid of metabolic wastes
major process in both: diffusion
contrast open and closed circulatory systems
open circulatory system
lack complete vessel networks
blood (or hemolymph) flows into a cavity (hemocoel), bathing organs directly at lower pressure
closed circulatory system
confine blood within vessels (veins, arteries, capillaries), allowing for fast, high-pressure circulation
all vertebrate systems are closed
list the components of vertebrate blood
plasma — water (90%)
some solids (proteins, hormones, and glucose)
gases — oxygen stored in red blood cell, CO2 transported in blood as ions
formed elements — blood cells and platelets
describe hemostasis (process of forming a clot)
hemostasis → how we decrease blood loss
platelets → other formed element in the blood, helps clotting occur
process of forming a clot:
damaged blood vessels — collagen fibers hanging inside smooth vessel
platelets bind to fibers to form a plug/clot
platelets and injured tissue release clotting factors
clotting factors to convert prothrombin to thrombin
thrombin converts fibrinogen to fibrin
fibrin meshwork is created and platelets contract to pull together
(clotting factors — >=13 identified)
distinguish between single vs double circulation and which vertebrate groups have single or double circulation (a.k.a. single and double circuit)
single circuit: blood travels from heart → goes to gills → gets O2 → goes to systemic system → back to heart
ex. fish → heart only receives blood once; deoxygenated blood (in fish)
heart has 2 chambers
double circuit:
pulmonary — heart → lungs → heart
systemic — heart → body → heart
mammals, birds, and crocodiles — 4 chamber heart (2 atria, 2 ventricle)
amphibians and most reptiles have 3 chamber heart (2 atrium, single ventricle)
some mixing in ventricle chamber
blood pressure can be different in two chambers in 2 chambers
describe the structure of the human heart, and how blood flows through the heart (chambers and valves)
structure: **take picture and modify on goodnotes**
blood flow:
blood comes from inferior vena cava (deoxygenated blood from lower body) or superior vena cava (deoxygenated blood from upper body) into superior right atrium
goes into right ventricle (contains papillary muscles) via tricuspid valve
goes into pulmonary semilunar valve → left pulmonary arteries (arteries going to the lungs (pulmonary))
blood is now oxygenated and comes back via pulmonary veins (veins coming from lungs) into the left atrium
goes into left ventricle via bicuspid valve
travels up through the aorta, which goes down and behind the heart, which then leads oxygenated blood to the lower body
how is cardiac rhythm is maintained?
excitation (maintains cardiac rhythm):
it starts with pacemaker cells → specialized myogenic (muscle cells) with leaky VGNaIC
does not require outside stimulus to open Na channels
heart can contract on its own without input from CNS or ANS — needs blood for nutrients Na, O2
found in 3 places: SA (sinoatrial node), AV (atrioventricular node), Bundle of His (purkinje fibers)
sinoatrial (SA) node → pacemaker cells here do not contract but rather initiate depolarization — continuous with fibers in atrial muscle
sends impulse through the right atrium and across to left atrium
impulse triggers AV node
AV node sends signal to Bundle of His
Bundle of His splits into left and right branches
Purkinje fibers — branch off nerves and extends through outer wall of ventricle
contraction:
atrium → contracts from top down (atrial systole)
ventricle → contracts from bottom up (ventricle systole)
both contract at the same time
describe heart contraction/heart sounds as it relates to the EKG (ECG)
ECG (electro-cardiogram) → measures heart electrical activity during atrial and ventricular systole (contraction)
heart contraction:
P — atrial depolarization, atria systole
QRS — ventricular depolarization, ventricular systole (atrial repolarization)
T — ventricular repolarization, ventricle relax
heart sounds:
lub → A-V valves Bicuspid (mitral) and Tricuspid closing
ventricles contract
dub → pulmonary and aortic semilunar closing
ventricles relax/atria contract
describe congestive heart failure (left and right side)
congestive heart failure → damage to heart
right side symptoms:
blood from body backs up (usually inferior vena cava) into legs
left side symptoms:
blood pools in lungs
shortness of breath (crackly breathing)
define blood pressure
blood pressure → the force of blood pushing against the walls of the arteries as the heart pumps the blood around the body
typical blood pressure measures systemic bp
ventricular systole and diastole
~120 mm Hg systolic b.p.
~80 mm Hg diastolic b.p.
systole → muscles contracted
when elasticity of the arteries declines with age, systolic bp increases (same amount of blood, smaller space, increased pressure)
diastole → muscles relaxed
when elasticity of the arteries declines with age, diastolic bp decreases (vessels stay wider longer, large vessel with less amounts of blood so pressure is less)
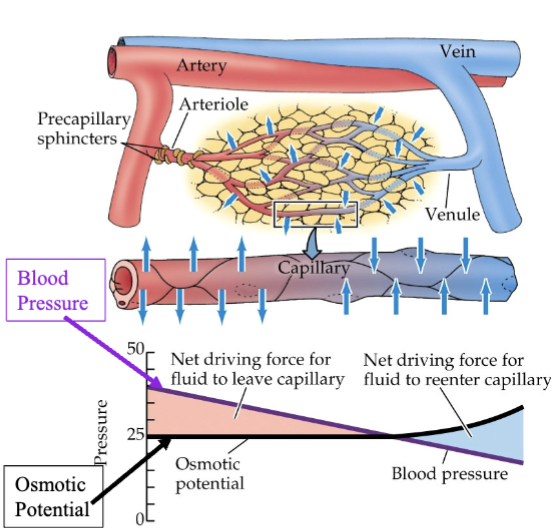
discuss the capillary exchange. what substances pass across the capillary wall and what’s the significance? what factors are involved in exchange of substances across capillaries in tissues? illustrate changes in the various pressures along the length of a capillary using a graph.
exchange → forcing out of arteries and into veins all due to hydrostatic pressure and osmotic potential
hydrostatic pressure (blood) → pressure exerted by a fluid at rest (static) due to gravity
drops over length of capillary because of frictional resistance to blood flow against vessel walls
osmotic pressure → minimum pressure needed to stop water (or other solvent) from flowing across a semipermeable membrane into a more concentrated solution
rises at the end of the capillary because water is filtered out of the plasma into the tissue space along the length of the capillary
substances that pass across capillary wall
oxygen, water, and nutrients (like glucose, amino acids, and lipids) moves into tissues
CO2, urea, and other metabolic wastes pass into blood
passes through primarily through diffusion
vital for maintaining homeostasis, provides essential nutrients and oxygen to tissues, while removing waste products like CO2 and urea
describe Kwashiorkor food deficiency and relate the swollen characteristic to exchange of fluids in capillaries
Kwashiorkor disease → severe form of malnutrition caused by inadequate protein intake
affects osmotic potential
more fluid leaves, less fluid returns
low blood protein reduces osmotic pressure, preventing fluid from returning to capillaries and forcing it into tissues
leads to edema
describe the function of the vertebrate lymphatic system
function → maintains fluid balance by draining excess fluid from tissues
recovers fluids that are not returned to venous capillaries (if not lymphatic)
lymph drains into veins of lower neck
lymph nodes (immune system)
areas of lymphatic tissue with immune cells
filters fluid and checks fluids for foreign objects, bacteria, viruses, etc.
describe the structures and functions of the human respiratory system (muscles associated with breathing, what drives our desire to breathe)
glottis → the part of the larynx consisting of the voice box
epiglottis → flexible, leaf-shaped flap of cartilage located behind the tongue at the top of the larynx (voice box)
human lung structure:
trachea
bronchus
bronchioles
alveoli
muscles associated with breathing → diaphragm and external intercostal muscles
inhale: diaphragm contracts → thoracic cavity volume increases thus expanding lung → pressure inside air space of lungs is negative, causing suction and drawing air in → lungs fill and rib cage expands
exhale: diaphragm muscles relax → pressure inside air space of lungs is higher, forcing air out
desire to breath comes from build up of CO2 lowering pH which stimulates desire to breath
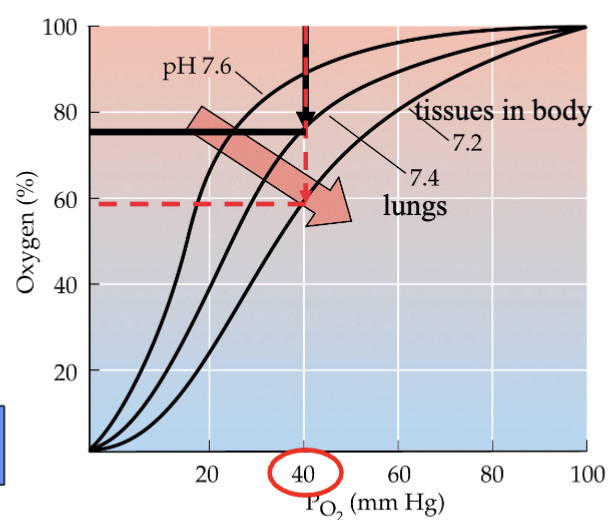
be able to determine the amount of oxygen delivered to the tissues using an oxygen saturation curve for hemoglobin. what is the Bohr effect and how does it affect the saturation curve?
oxygen saturation curve → shows how much oxygen is delivered
Bohr effect (CO2 effect) → decrease in pH causes hemoglobin to have reduced affinity (strength of binding interaction) for oxygen, tissues have a great affinity for O2
build up of CO2 in systemic tissues of body → decrease of pH in blood
decrease in pH → reduced attraction for O2 in blood
therefore, a greater % is delivered to tissues
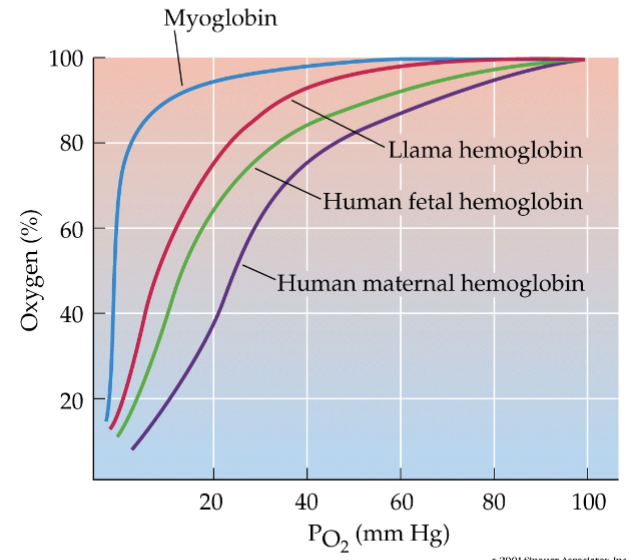
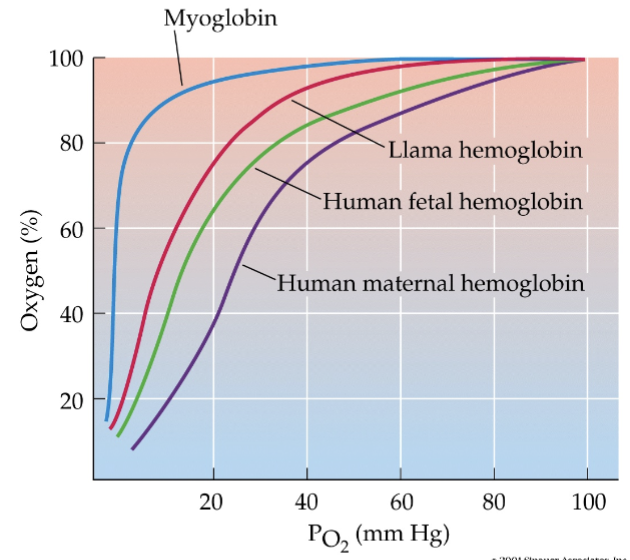
if given saturation curves for other pigments like myoglobin, etc., determine which has the highest affinity. also, be able to use the saturation curves of fetal and maternal hemoglobin to show why it is advantageous for the unborn child to have hemoglobin with a higher affinity for oxygen relative to the mother’s hemoglobin
myoglobin has the highest affinity — found in cardiac and skeletal muscle
hemoglobin is pigment found in the blood
as O2 is given up by bloodstream, muscles have stronger affinity to hold onto it to use it for muscles contraction
human fetal hemoglobin has higher attraction than human maternal hemoglobin
in placenta, capillaries get close and O2 and nutrients diffuse from maternal to fetal
list the 3 ways carbon dioxide is carried by blood. most of the CO2 is carried in the blood in what form?
some carried as carbaminohemoglobin (23-25%) — an amino acid
some in dissolved state (5-7%)
most converted as bicarbonate ion (~70%)
Fick’s law as it relates to various processes of diffusion
Q = DA (c1-c2)
L
Q = rate of diffusion
simple squamous epithelium maximizes diffusion by minimizing diffusion distance (L)
alveoli increases surface area (A)
compare arteries and veins with regard to structure, movement of blood, and the oxygen content of blood being carried
arteries → carries high-pressure, oxygen-rich blood away from the heart through thick, muscular, elastic walls
has more smooth muscle than veins
blood is under higher pressure
smooth muscles contract and relax, helping to maintain pressure
when left ventricle:
contracts → arteries expand
relaxes → arteries contract
veins → carries low-pressure, oxygen-poor blood towards the heart using thin walls and one-way valves to prevent backflow
has smooth muscle
not under a lot of pressure
usually carrying deoxygenated blood back to heart (systemic)
more superficial — closer to surface
define medical terms given in lecture associated with the circulatory system like embolus, etc.
thrombus → stationary clot
embolus → detached clot
acute coronary syndrome (ACS) → affects coronary arteries bringing O2 to the heart
ischemia → decreased blood flow to region of the body (due to embolus)
heart does not receive blood flow it needs
angina (pectoralis) → chest pain due to ischemia to the heart
myocardial infarction (heart attack) → a blockage of the coronary arteries that carry oxygenated blood to heart tissues
infarct → any tissue damage due to disruption of blood supply
circumflex redundancy → multiple arteries surround heart to maintain blood flow if blockage
balloon angioplasty → open up artery to increase blood flow
aneurysm → weakening and localized dilation in the wall of a blood vessel
stroke → blockage or hemorrhage of capillary in brain
brain aneurysm -- bursts = hemorrhagic stroke
the medical moments covered in lecture
jaundice → build-up of bilirubin in circulatory system
trauma of childbirth — broken vessels
hemoglobin needs broken down; UV light makes bilirubin more water soluble, breaks it down
adult — liver damage cannot remove bilirubin
bruise coloring
red → recent; red blood cells in bruised site
purple/blue → to 5 days; area with little oxygen due to damaged blood vessels
green → 5-7 days, biliverdin
yellow → >7 days, bilirubin