4- antibiotic resistance
1/13
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
14 Terms
How do bacteria become resistant to antibiotics?
Resistance first develops due to a mutation. Bacteria reproduce asexually, so all the offspring should be the same, but sometimes, at random, mutations occur when DNA is replicated. These mutations may have any effect (and most will be fatal), but occasionally a mutation occurs that makes the bacterium resistant to an antibiotic.
Give examples of how a mutation can cause antibiotic resistance.
A mutation could slightly alter an enzyme, changing its substrate specificity so that its active site will now bind penicillin. Some bacteria now have penicillinase enzymes that modify or break down penicillin, rendering the antibiotic useless. Antibiotics are often similar to normal bacterial metabolites, and a small mutation in an existing enzyme can modify its active site to fit and antibiotic.
A mutation could modify a transport protein so that the antibiotic is transported out of the bacterial cell, or not transported into the bacterial cell.
A mutation could slightly alter a ribosome so that antibiotics like tetracycline and streptomycin can no longer bind and inhibit protein synthesis.
These mutations are rare, but bacteria reproduce so rapidly, and there are so many bacterial cells, that new resistance mutations do occur at a significant rate.
This is a random event, and is not caused by the presence of the antibiotic.
What is vertical gene transfer?
It is the process of bacteria reproducing by binary fission which passes on their antibiotic resistant gene to all of its offspring, forming a new strain of bacteria.
If there is no antibiotic present this mutated strain may well die out due to competition with all the other bacteria, and the mutation will be lost again.
However, if the person is taking antibiotics, then the antibiotic will be present in the bacteria’s environment, the mutated cells are now at a selective advantage; the antibiotic kills all the normal bacterial cells, leaving only the mutated cells alive. These cells can then reproduce rapidly without competition and will colonise the whole environment.
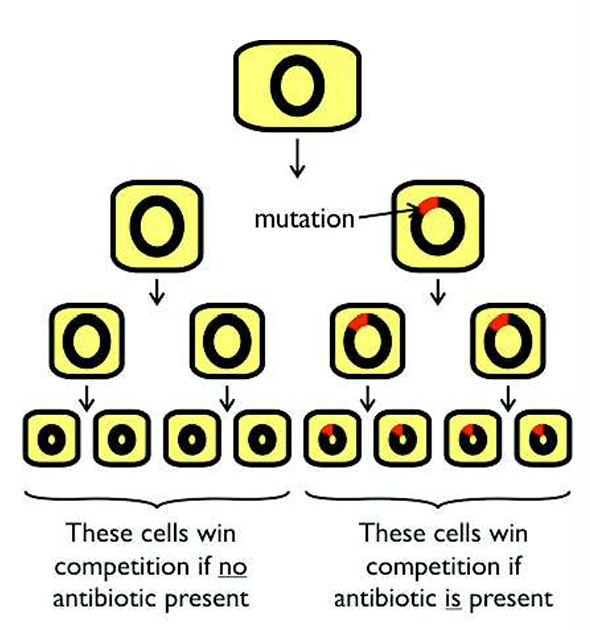
What is vertical gene transfer an example of?
Natural selection. The mutated cells have been selected by the environment and so the frequency of the resistant allele in the population increases.
What is horizontal gene transfer?
Bacteria can transfer genes between each other by conjugation. (no other organism can do this).
This is the transfer of DNA between bacterial cells via a conjugation tube or pilus. From time to time two bacterial cells can join together (conjugate), and DNA passes from one cell (the donor) to the other (the recipient). The transferred DNA is usually a plasmid but can be part of the chromosome.
Conjugation means a resistant gene can spread from the bacterium in which it arose to other, perhaps more dangerous species. It is also the cause of multiple resistance.
It is highly unlikely that a single strain will mutate twice to develop resistance to antibiotics, but it is likely that it could receive genes for resistance to different antibiotics by horizontal gene transfer. This has led to strains of bacteria that are resistant to many (or even all) antibiotic.
How else can antibiotic-resistant bacteria be spread (other than horizontal and vertical gene transfer)?
It can spread to other people by any of the normal methods of spreading an infection: through faeces, water, food, sneezing, infected instruments etc.
This is a common source of antibiotic resistant bacteria (and especially multiple-resistant bacteria) in hospitals. This is partly because hospitals have a high concentration of people with bacterial infections, but also because the use of antibiotics means any antibiotic-resistant strains can multiply in the absence of competition.
Give examples of antibiotic resistant bacteria.
Staphylococcus aureus, a bacterium responsible for a variety of diseases (including food poisoning and toxic shock syndrome). This species has been resistant to penicillin for years, due to the possession of the penicillinase enzyme. Methicillin is unaffected by penicillinase and so was effective against S. aureus. However, within a year of the introduction of methicillin, methicillin-resistant strains of S. aureus (MRSA) were found in hospitals where methicillin was in regular use. Infections by MRSA were very difficult to treat. In 1997 vancomycin- resistant, methicillin-resistant S. aureus appeared in Japan, these bacteria are effectively untreatable at present.
Mycobacterium tuberculosis, the bacterium that causes TB, has developed resistance to streptomycin. An extreme drug resistant TB strain (XDR-TB) has been found in South Africa that kills 98% of those infected within two weeks, and is resistant to most antibiotics. Resistant strains of M. tuberculosis can only be treated using a cocktail of four different antibiotics over a prolonged period of months, which is expensive and unlikely to be achieved in developing countries.
What are some of the different measures that are being taken to control the spread of antibiotic resistance?
Using a wide range of antibiotics
Prescribing fewer antibiotics
Stopping using antibiotics in animal feed
Improving hospital hygiene
Screening and isolating patients
How can using a wider range of antibiotics help control the spread of antibiotic resistance?
There is constantly industrial searches for new antibiotics which there is no resistance for. However, it is becoming more and more expensive to find truly new drugs and sooner or later the bacteria will develop resistance. So using a wider range of antibiotics can help reduce the spread of antibiotic resistance, but it is only a short-term solution.
How can prescribing fewer antibiotics help control the spread of antibiotic resistance?
This will reduce the selection pressure in favour of resistant strains. Most resistant strains are inferior to the ‘wild type’ strains in order respects (perhaps they reproduce more slowly), so in an antibiotic-free environment the mutants are generally out-competed and will die out. The antibiotic resistant genes will therefore disappear from the gene pool of that population. Unfortunately we are now in an ‘antibiotic culture’ where many doctors prescribe antibiotics routinely for common ailments such as the flu (even though they have no effect), simply to keep the patient happy. And in some countries antibiotics can be bought over the counter without a doctor’s prescription, so are impossible to control.
How can stopping using antibiotics in animal feed help control the spread of antibiotic resistance?
Many farmers routinely feed their livestock small concentrations of antibiotics to promote growth and as a prophylactic against possible infection. This agricultural use accounts for 90% of all antibiotic use worldwide, and provides very strong selection for antibiotic- resistant bacteria. This practise was made illegal in the EU in 2006, but this has had little effect and anyway few other countries have passed any laws, partly because the agriculture industry is a very powerful lobby.
How can improving hospital hygiene help control the spread of antibiotic resistance?
Transfer of bacteria between patients in hospitals is a major cause of spread of antibiotic resistance genes. Hand washing with antibacterial wash, using disposable gloves and aprons when handling patients, deep cleaning wards and all soft furnishings periodically all help to reduce spread. But these measures are expensive and rely on compliance of all staff and visitors.
How can using screening and isolating patients help control the spread of antibiotic resistance?
New patients can be tested for the presence of MRSA and other resistant ‘superbugs’ and then isolated in wards separate from uninfected patients. However, screening takes time (24h typically) and many hospitals don’t have space for isolation wards.
What happens if we cannot control the spread of antibiotic resistance?
Most antibiotics will become useless, and we will revert to the pre-antibiotic age where bacterial infections are effectively untreatable.