Module 2 Blood Lab Practice
1/67
Earn XP
Description and Tags
SDMMSGMDFMGMDFGDFMGMDFGMG
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
68 Terms
Blood
Liquid that carries nutrients, electrolytes, gases, and a number of chemicals as well as specialized cells. Capable of producing important reactions in stopping bleeding and fighting infection. Considered connective tissue. It includes specialized cells such as red and white blood cells, platelets (cell fragments), and plasma (a straw-colored liquid)
5
The volume of blood in the typical adult is approx. _ liters.
Plasma
The fluid portion of the blood. Contains vitamins, amino acids, proteins, carbohydrates, lipids, cellular wastes, and hormones.
45 55
If we were to separate the solid from the liquid portion of blood, we would see that it is about % cells, and % plasma by volume.
Hematocrit
the separation of the solid and liquid portions of the blood.
hemocytoblast
The cell of origin for all blood cells.
colony-stimulating factors
The hemocytoblast can differentiate into any of the mature blood cells by responding to factors called _______________ _______
Red blood cells
Also called erythrocytes, make up the largest percentage of the formed elements of the blood. Their primary function is to transport oxygen and carbon dioxide.
Hemoglobin
A protein molecule that makes up ⅓ of a red blood cells volume. Responsible for giving red blood cells their color. It is the transport molecule for oxygen and carbon dioxide.
Oxyhemoglobin
The bright red, functional form of hemoglobin bound with oxygen. Formed when oxygen combines with hemoglobin, and is used to transport oxygen throughout the body’s tissues.
Deoxyhemoglobin
Formed when oxygen is released from hemoglobin (hence the prefix). Compared to Hemoglobin, it is a dull red color, and looks bluish under the skin, as the skin filters out some light.
nucleus mitochondria
Since the main function of red blood cells is to transport gases, there is no need for a ______ or __________.
bone marrow
Red blood cells develop in the ____ ______.
Hematopoiesis
The process of blood cell formation.
Erythropoiesis
The process of red blood cell formation.
erythropoietin
Immature red blood cells called erythroblasts differentiate from hemocytoblasts in the presence of the hormone ___________, which is primarily released by the kidneys and liver in response to low oxygen concentration in the blood.
nucleus mitochondria
Erythroblasts still contain a _______ and _________ and produce hemoglobin. When they mature into erythrocytes, they shed them.
120
Red blood cells circulate in the bloodstream for ~___ days after development.
2.5
About ___ million red blood cells are produced each second to keep up with the number of cells being recycled.
capillary membranes
In the red blood cells’ lifetime, they slowly wear out from passing through ________ __________.
75,000
Each cell can travel through the body as many as _______ times
capillary membranes spleen liver hemoglobin
When red blood cells are 120 days old, they become worn enough to pass through _________ ________ in the _____ and _____. they are then broken down and phagocytized by macrophages, and the ________ is recycled/
Red Blood Cell Count
An indicator of the amount of red blood cells in the bloodstream.
globin heme iron biliverdin
Hemoglobin is broken down in the liver and spleen into 4 _____ molecules as well as 1 ___ molecule, which is then broken into ____ and ________
4,600,000-6,200,000
For males, RBC is:
4,200,000-5,400,000
For females, RBC is:
4,500,000-5,100,000
For children, RBC is:
Erythrocytosis
Also called erythema, is an increase in the red blood cell count. It can be casued by lung disease, poisoning, and dehydration. A temporary red blood cell increase can occur when people who live at sea level visit high-altitude environments.
Anemia
A decrease in the red blood cell count. Can be caused by a number of factors, such as vitamin B12 deficiency, blood loss, and iron deficiency.
Vitamin B12 folic acid iron intrinsic factor
What are the main components needed for red blood cell production?
vitamin B12
Damage to the stomach lining can decrease secretion of intrinsic factors and produce a _______ ___ deficiency.
Iron
What is needed for the production of hemoglobin?
Pernicious Anemia
A type of anemia that develops when there is a deficiency of vitamin B12. Cells are larger (macrocytic) because the larger hemocytoblast has not differentiated fully into a smaller erythrocyte.
Iron Deficiency Anemia
A type of anemia that results from an iron deficiency. Cells are smaller and contain less hemoglobin.
Leukocytes
White blood cells. They are found in the blood, but also work outside of the circulatory system in organs and tissues. There are two categories: Granulocytes, which have a granular cytoplasm, and agranulocytes, which do not.
Granulocytes
White blood cells that tend to be significantly larger than red blood cells. There are 3 types: neutrophils, basophils, and eosinophils. They have a shorter lifespan than red blood cells; hours compared to the 120 days that red blood cells have.
Neutrophils
Cells that are larger than red blood cells and contain a segmented nucleus. They account for the majority of leukocytes. They phagocytize bacteria and viruses, and are the first cells to arrive at an infection
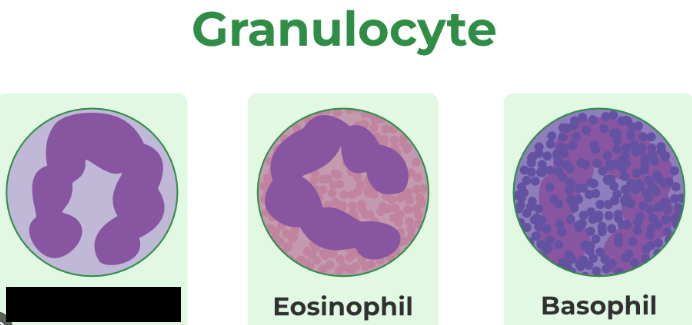
Eosinophils
Cells that have a bilobed nucleus and a granular cytoplasm. They are rare cells that make up ~1-3% of the leukocyte population, and they moderate allergic reactions and defend against parasites.
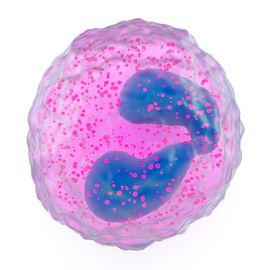
Basophils
Cells that have fewer and larger granules as eosinophils, but have the same size and shape of nuclei. The granules release histamine and heparin. They function in inflammation (heat, redness, pain, swelling). Histamine and heparin bring more blood to the inflamed area, producing the signs of inflammation. They are rare, only representing 1% of the leukocyte population.
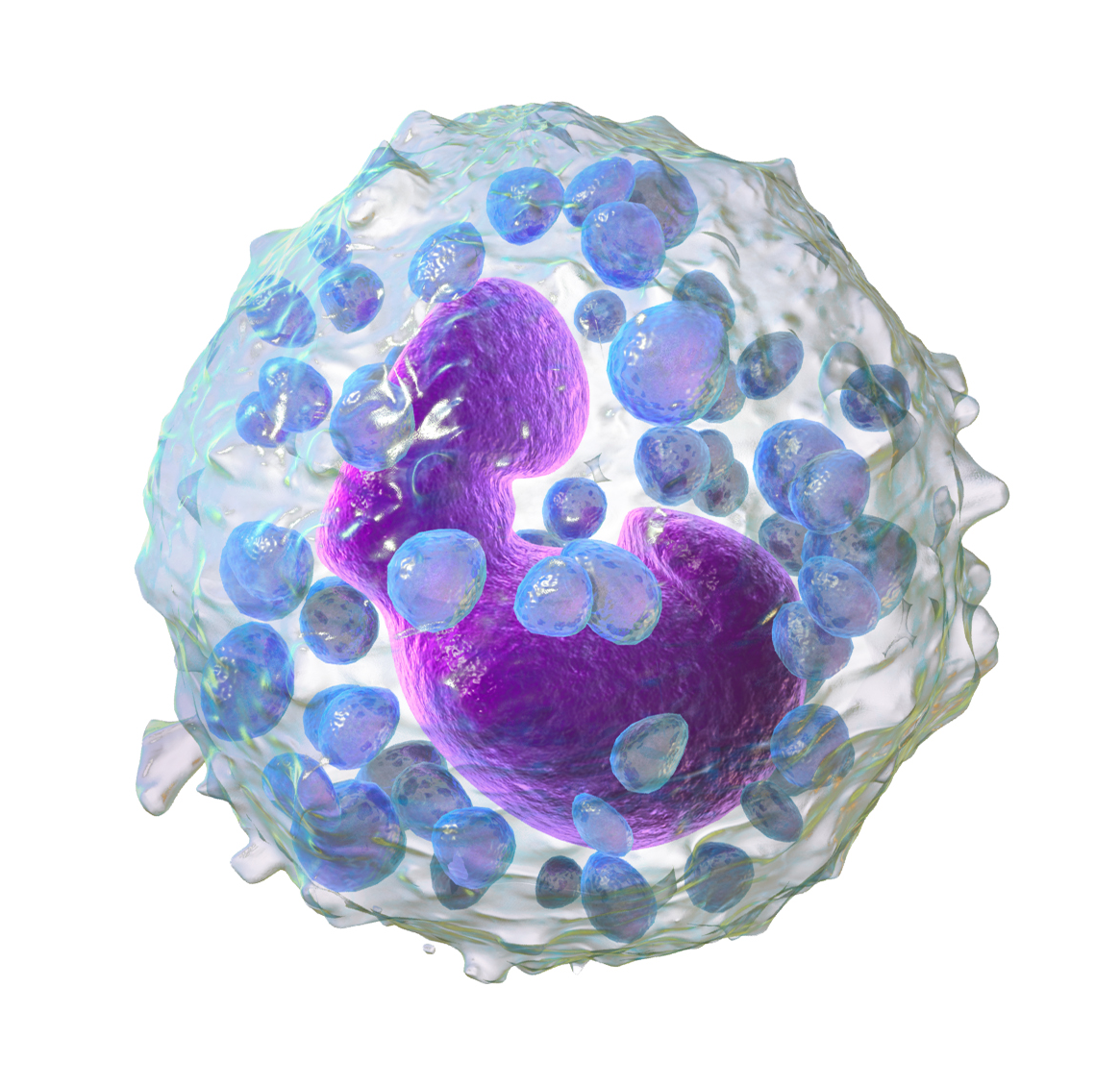
monocytes lymphocytes
There are two agranular leukocytes: ________ and __________.
Monocytes
The largest blood cells. They have spherical, kidney-shaped, oval, or lobed nuclei. They have a function very similar to neutrophils; they clean up debris and phagocytize bacteria. They constitute 3-9% of the leukocyte population.
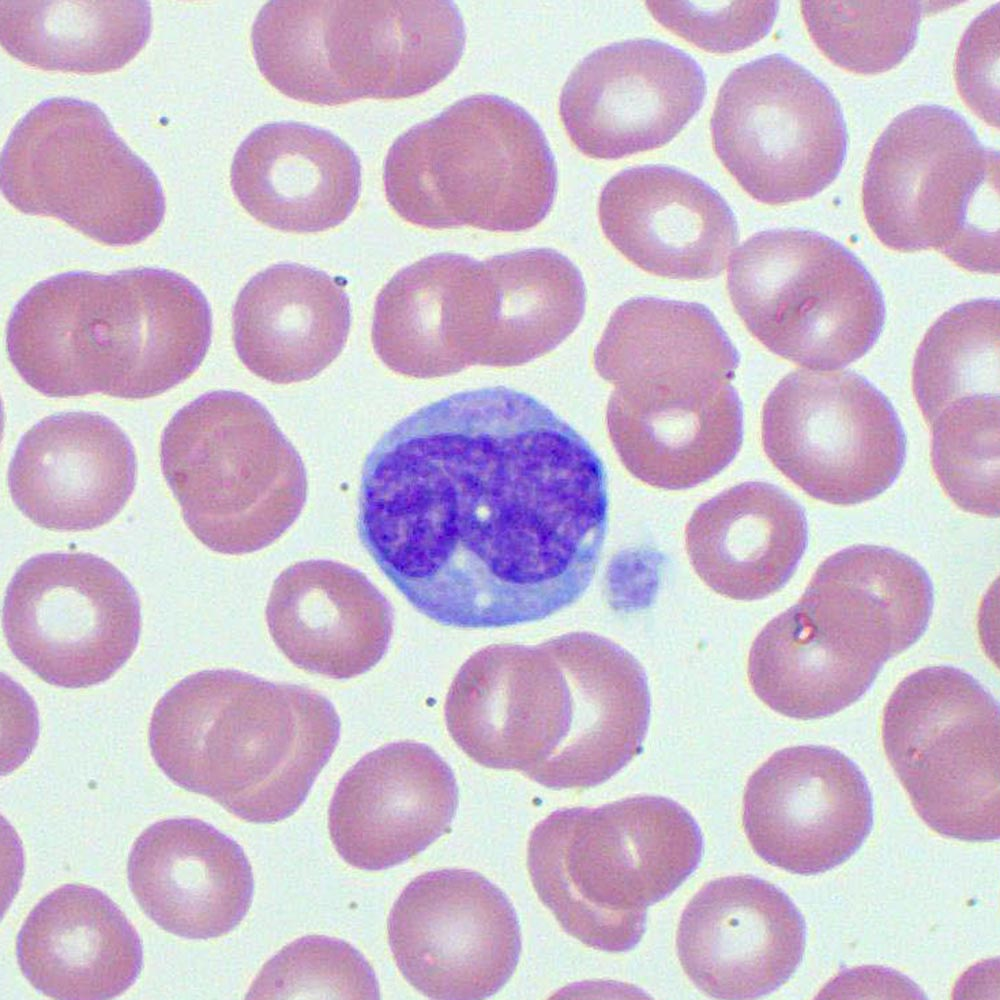
Lymphocytes
Constituting 25-30% of the leukocyte population, has 2 types of cells that function in immunity. T-__________ attack pathogens, while B-_________ produce antibodies that attack pathogens. They are about the same size as red blood cells.
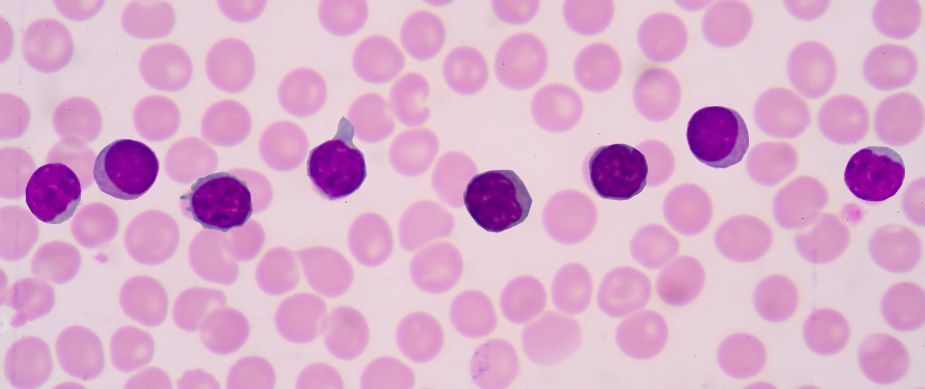
Diapedesis
The process of white blood cells moving between capillary walls and entering tissue. An appendage of the cell first moves to an area, followed by the remainder of the cell.
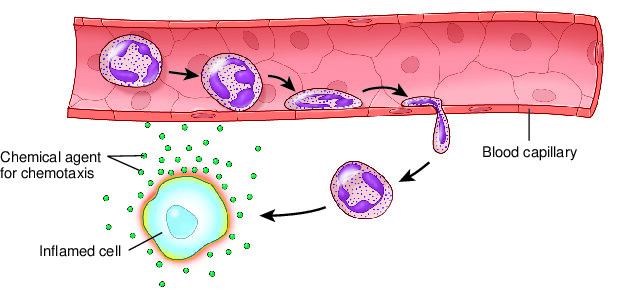
Chemotaxis
Substances secreted by damaged cells. Used by cells to attract white blood cells to an area, where they lyse bacteria and form pus.
5000-10000
The typical white blood cell count is about ____-_____ cells per cubic meter
Leukocytosis
A high white blood cell count, caused by infection, exercise, loss of body fluids, or emotional stress.
Leucopenia
A low white blood cell count, can be caused by viruses like influenza, measles, mumps, and chickenpox, or toxins such as lead.
Platelets
Cell fragments called thrombocytes. Hemocytoblasts (stem cells) differentiate into megakaryocytes that fragment into platelets. They are ~½ the size of red blood cells. There are 130,000-360,000 _______ per cubic millimeter of blood. They help stop bleeding by sticking together to form plugs and secrete the hormone serotonin, which acts to vasoconstrict the vessels.
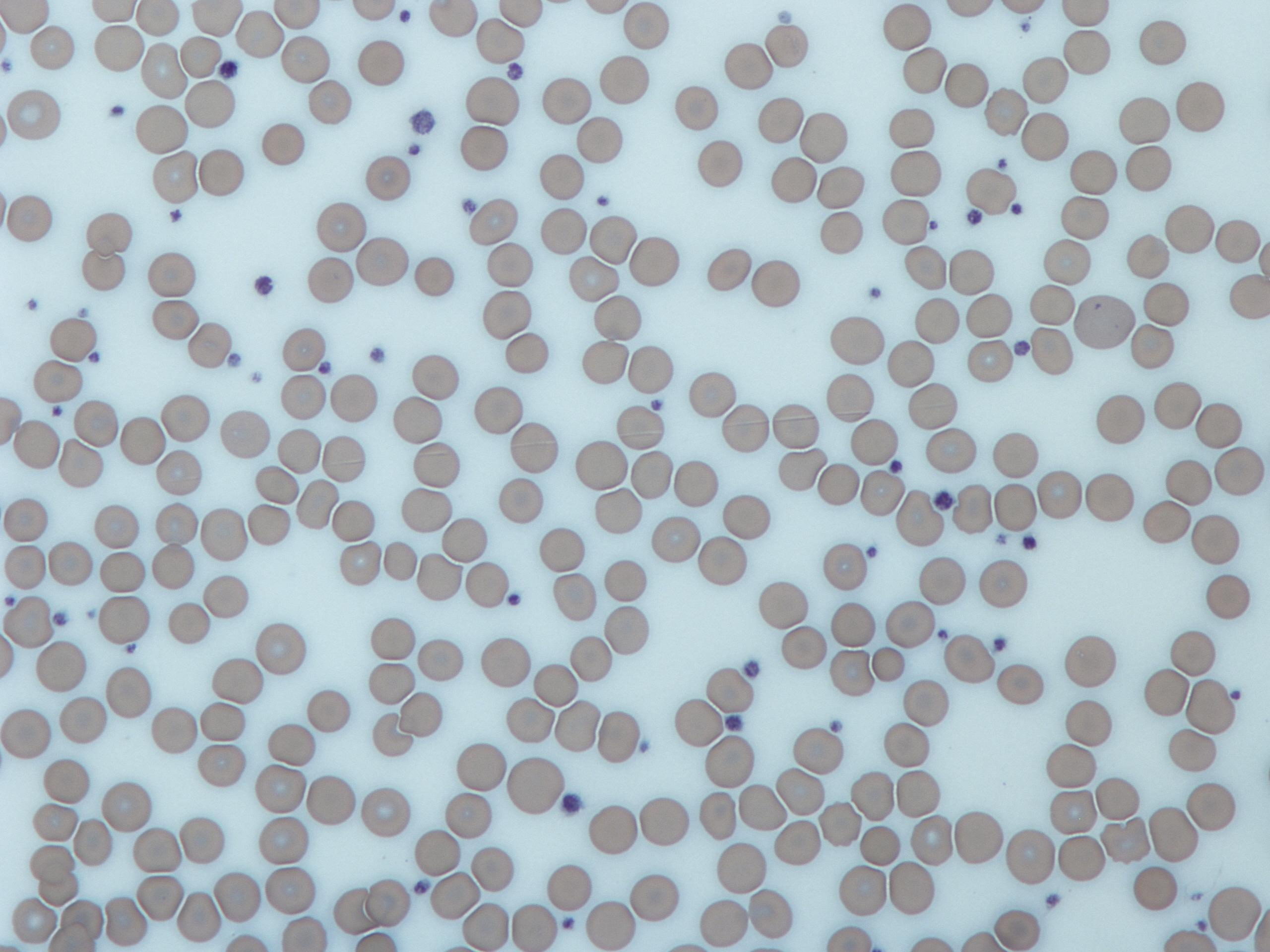
Blood Plasma
The fluid portion of the blood that carries the cells and platelets. Straw-colored (a pale yellow), clear, and contains water with other substances.
Contains proteins such as Fibrinogen, Globulins, and Albumin
Contains dissolved gases such as carbon dioxide and oxygen
Contains nutrients such as Carbohydrates, Amino acids, and lipids
very low-density lipoproteins Low-density lipoproteins high-density lipoproteins Chylomicrons
Lipids in the plasma are packaged in lipoproteins such as ____ ___-____ _________ (VLDL), ___-______ _________ (LDL), ____-_______ _________(HDL), and ____________
Hemostasis
The stopping of bleeding. There are three basic mechanisms: blood vessel spasms. Platelet plug formation, and clotting.
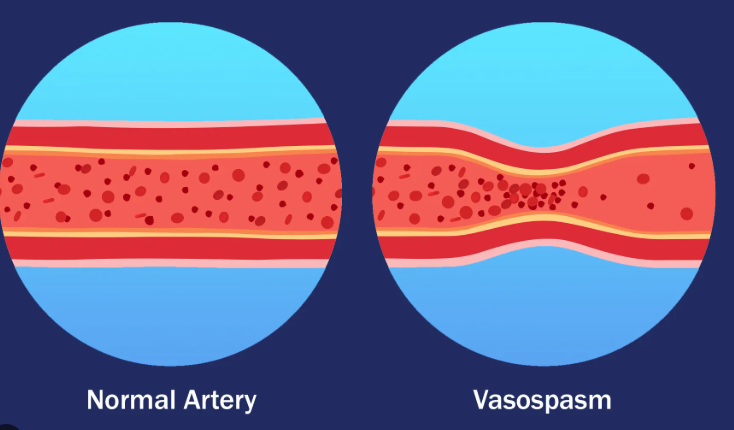
Blood Vessel Spasm
Occurs in response to a damaged vessel. Blood vessels have a smooth muscle layer that constricts when the vessel is damaged. Platelets release serotonin, which facilitates the construction of the vessel. This action helps to stop bleeding.
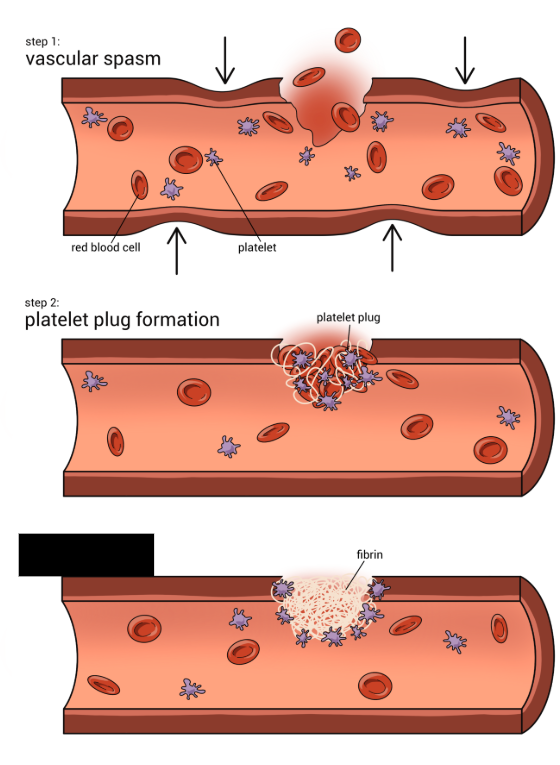
Platelet Plug Formation
When platelets contact damaged blood vessels and stick to one another to form a plug which fills in the small holes in vessels.
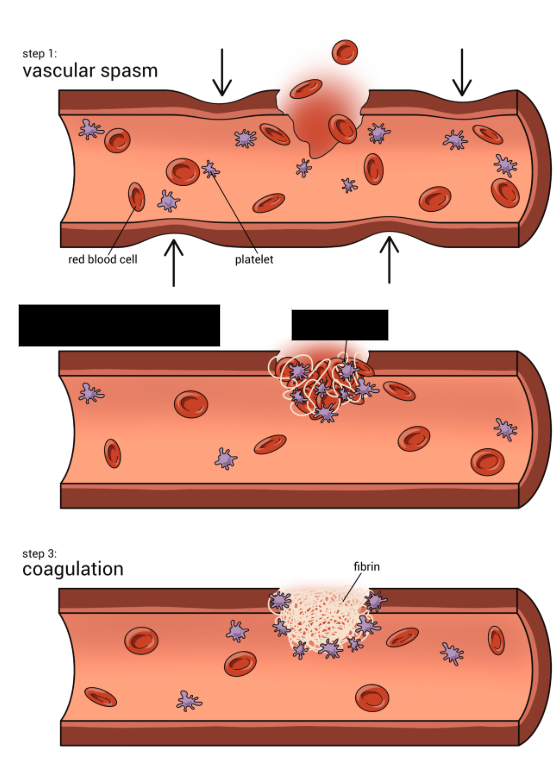
Clotting
The third mechanism of hemostasis. Includes 2 pathways consisting of a cascade of reactions involving molecules called ______ factors. The two pathways are the intrinsic and extrinsic pathways, which both converge at a common point to form a fibrin clot.
Extrinsic Pathway Clotting
Pathway of clotting triggered when blood leaves the damaged blood vessel. The clotting factor tissue thromboplastin (factor III) is triggered to begin the cascade of reactions. Thromboplastin activates factor VII, which activates Factor X. Factor X combines with factor V and calcium to activate prothrombin activator. Prothrombin activator allows prothrombin (factor II) to convert to thrombin. Thrombin allows for the conversion of Fibrinogen (factor I) to fibrin. Factor XIII stabilizes the fibrin clot.
Intrinsic Pathway Clotting
Pathway of clotting triggered when blood contacts damaged blood vessel walls, but does not leave the vessel. The Hagman factor (factor XII) activates factor XI, which activates factor IX. Factor IX combines with factor VIII to activate Factor X, which then combines with factor V and calcium to activate prothrombin activator. At this point, the pathway is the same as extrinsing pathway clotting.
atherosclerosis
Plaque buildup inside arterial walls. Can trigger Intrinsic pathway clotting.
Stasis
Slowing or pooling of blood. Can trigger Intrinsic pathway clotting.
Type A Blood
Blood that contains antigen A. Contains antibodies that are not compatible with antigen B. Compatible with itself and type O blood.
Type B Blood
Blood that contains antigen B. Contains antibodies that are incompatible with type A.
Type AB Blood
Blood that contains both antigens A and B. Contains no antibodies that will react with the type A or B antigens. Compatible with all of the blood types, and known as the universal blood acceptor.
Type O Blood
Blood that contains neither antigens A or B. Compatible only with itself. Known as the universal blood donor.
Agglutination
The coagulation of blood. Happens when antibodies in the recipients blood attack foreign antigens, such as when a type A acceptor receives type B blood, and their anti-B antibodies attack the foreign type B blood antigens.
positive negative
If the Rh antigen is present on the surface of a red blood cell, it is Rh _______, else it is Rh ______.
positive negative
Rh-positive blood is compatible with both Rh-________ and ______ blood.
negative
Rh-negative blood is only compatible with Rh-_______ blood.
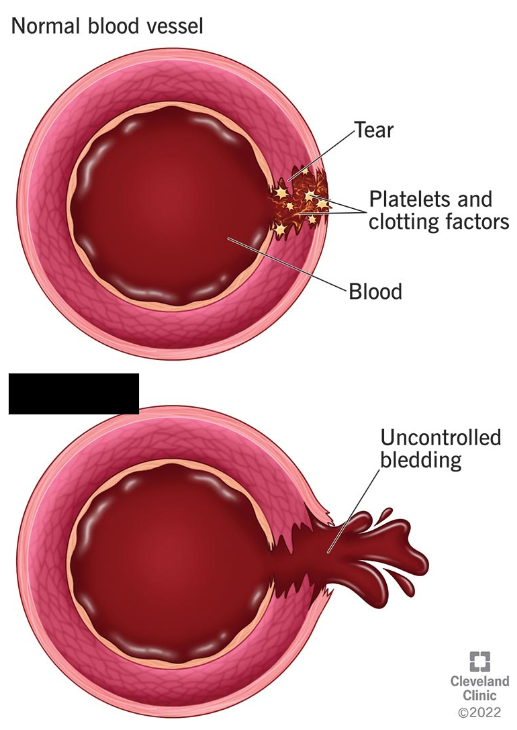
Hemophilia
A recessive genetic disorder that impairs the blood's ability to clot. This causes unexpected and prolonged bleeding, bruises, and pain in joints. There is no cure, but transfusions with healthy clotting factors can be administered.
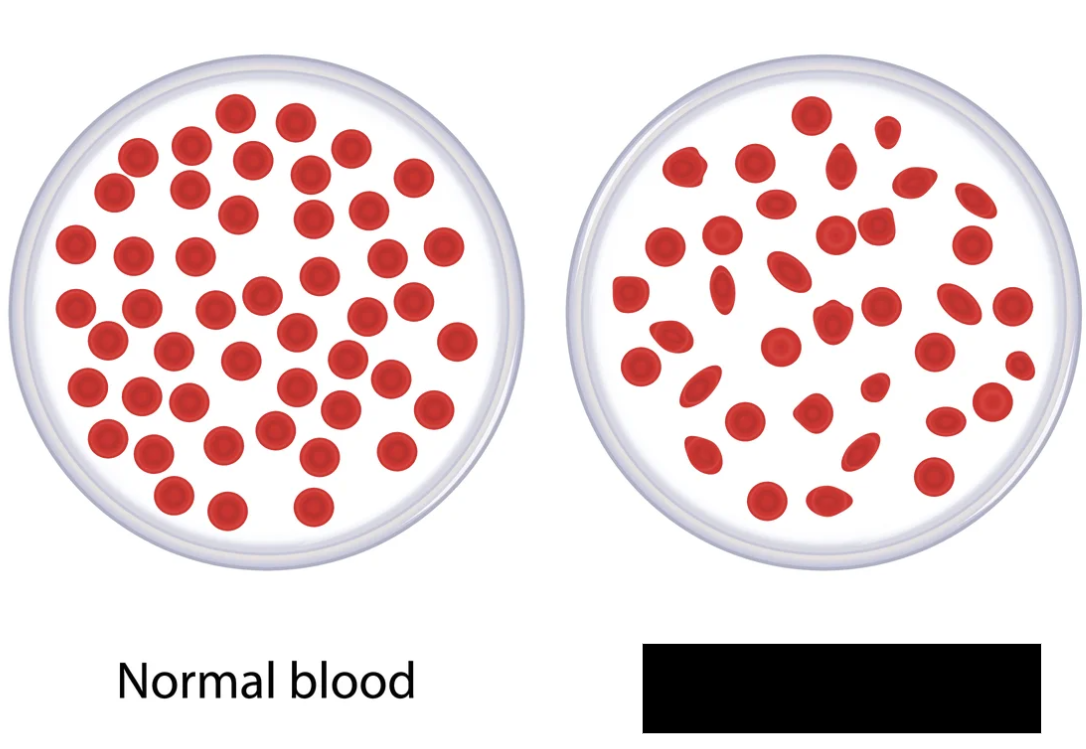
Thalassemia
A disease that affects hemoglobin, the oxygen-carrying molecule in the blood. Individuals with the disease may have red blood cells that differ in color and shape, therefore being less efficient in carrying gases. Unusual cell types include “target” cells, “teardrop” cells, microcytes, and red blood cells with nuclei. Causes fatigue, weakness, swelling of the abdomen, and jaundice. May require blood transfusions.