Physiology of the Upper GI tract
1/75
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
76 Terms
What are the main secretory regions of the stomach?
Oxyntic (parietal) - in fundus & body- secrete gastric juice
Pyloric- in pyloric antrum
What does the oxyntic area do?
-Oxyntic (parietal) cells - secrete acid and IF (needed for B12 absorption)
- Chief (peptic cells)- gastric pits- secrete pepsinogen
What does the pyloric area do?
Pyloric area- secretes hormones gastrin (G cells)
What does the stomach also contain?
ECL (enterochromaffin-like) cells which secrete histamine (stimulates the release of stomach acid)
D cells secrete somatostatin which do the opposite.
What is the composition of Gastric Juice?
Parietal juice- acid- released by oxyntic
Alkaline juice- release by mucous cells
-Both isotonic with plasma- conc vary. More flow of gastric juices- chyme becomes more acidic (pH2)
-This can be induced by histamine injection.
What stimulates gastric secretions?
Food
What happens when food stimulates secretion?
-The rate of acid secretion increases quickly
- Secretion of alkaline fluid is primarily is passive process
What is pentagastrin & what is it used for?
What is it- synthetic drug
What is it used for- test for stimulation of several hormones & diagnosis of calcitonin secreting tumours of the thyroid (as gastrin stimulates thyroid C cells)
What is intragastric pH monitoring used for?
To assess gastric function using a probe or remotely using a capsule
What is achlorhydria?
Absence of HCL secretion
When does Achlorhydria occur?
1. When gastric pits are destroyed
2. Occurs in certain autoimmune problems e.g. Sjogrens
3. Also occurs in Helicobacter pylori infection
What is Sjogren's?
Autoimmune destruction of the salivary glands
Why does Achlorhydria occur in Helicobacter pylori?
It releases ammonia to neutralise the HCl in the stomach
What is Achlorhydria associated with?
Pernicious anaemia- most people with achlorhydria have antibodies against the H+/K+ proton pumps of the oxyntic cells.
HCl is a reducing agent that reduces the iron to be absorbed. If HCl is not present=> less iron absorption
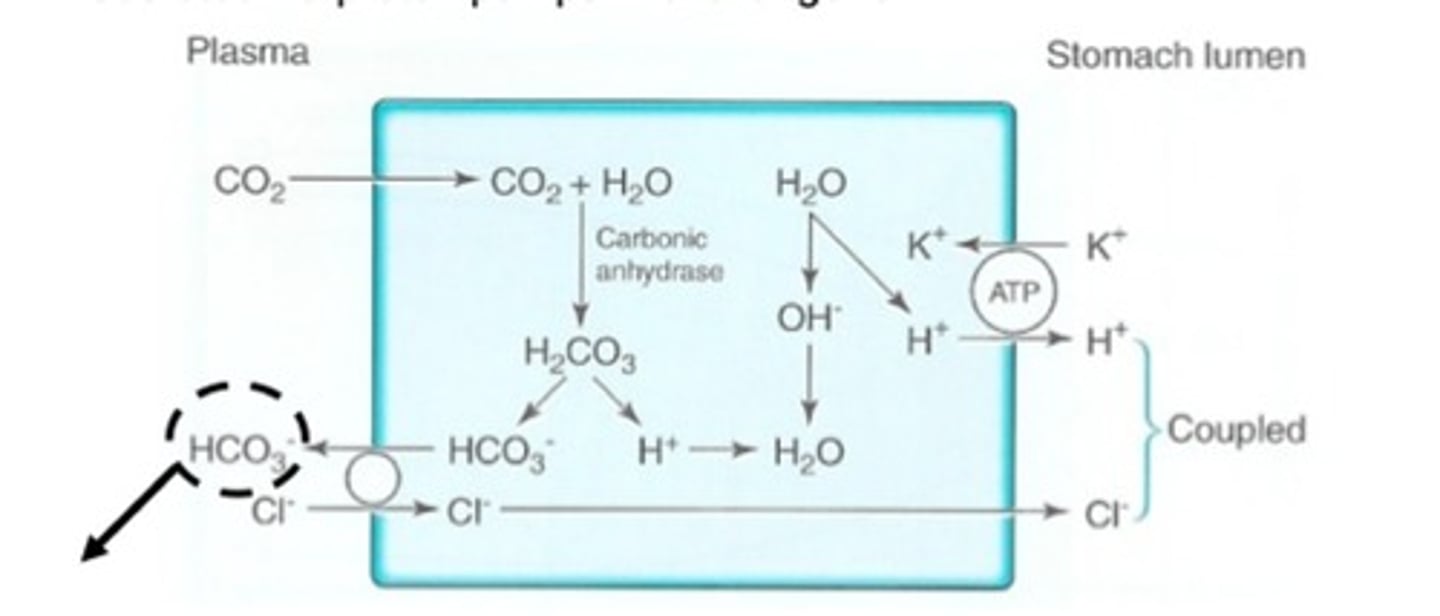
What is the cellular mechanism of secretion of HCL in the oxyntic cell? a) What happens to H+ ions. b) What happens to the Cl-
Look at the image in the lecture.
H+ & Cl- actively secreted against an high conc. gr
a)
- Co2 from the plasm enters the cell & reacts with water to form H2Co3. This dissociates into HCO3- & H+ .
- HCO3- leaves the cell (due to Cl-) back into the plasma- This causes plasma to be transiently alkaline ('alkaline tide')
- H20 forms OH- & H+. The OH- reacts with the H+ formed in the step above to make water.
- The H+ formed by H20 is secreted via proton pumps in exchange for K+ .
-At rest Cl- is also secreted against electrochemical grd.
-When the oxyntic cell is stimulated, the luminal surface potential becomes less negative
- Cl- enters at the serosal surface bound to transporter protein- in exchange for HCO3-
- Cl- is then actively pumped at mucosal surface via a chloride channel
What does the alkaline tide cause?
Metabolic alkalosis in persistent vomiting
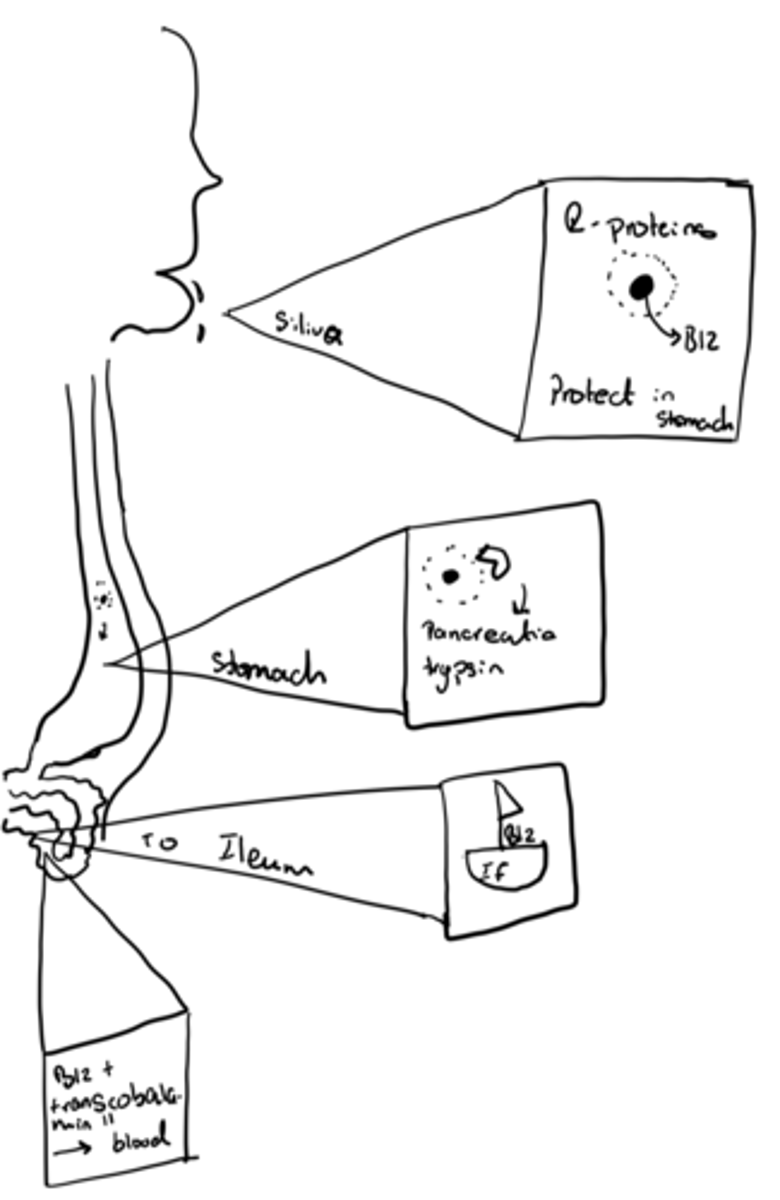
Why is Intrinsic Factor produced in the oxyntic cell?
-Dimerises & then the dimer binds to 2 molecules of B12
-R-proteins (Haptocorrin) in the saliva protect the B12- allows it through the stomach
-When it passes the stomach, the pancreatic trypsin releases B12 from the protein.
-IF transport B12 to ileum.
-Complex absorbed via a specialised absorption system in the ileum (B12 binds to transcobalamin II and then taken into blood stream)
Why is gastroferrin produced in the oxyntic cell?
-Complexes with Fe2+ to facilitate absorption
-Fe2+ is readily absorbed and not converted into Fe3+ due to the pH (since Fe3+ is not as readily absorbed).
What can antiacid use (H2 receptor antagonists & proton pump inhibitors) lead to?
Iron deficiency anaemia
What happens to Pepsinogen produced in the Chief cells?
Stored in granules & released by exocytosis
What are the two forms of pepsinogen & its precursors?
Pepsinogen 1 & 2=> pepsin 1 & 2
Where is Pepsinogen 1 secreted?
In the oxyntic area
Where is Pepsinogen 2 secreted?
Throughout the stomach
What activates pepsinogen & its reaction?
-Activated in the stomach lumen by hydrolysis.
-Pepsinogen is converted into pepsin & peptide using H+ & pepsin (enzyme).
-The optimum pH for this reaction is 3.5
Mucous cell- What is mucins?
Glycoproteins- a part of mucus
Mucous cell- What does the epithelial cells secrete?
Alkaline mucous (high HCO3-)- protects stomach lining
Mucous cell- what does the mucus cells secrete?
Clear mucus
Mucous cell- mucin tetramers form a gel. What happens when this gel is disrupted with dramatic changes in pH?
Cause precipitation of the mucus
How do ulcers form?
Due to action of acid & pepsin when the mucous layer is damaged
What are the causes of ulcers?
-Long term use of NSAIDS
-Infection with Helicobacter pylori
-Cancers of the pancreas/ duodenum
-Zollinger- Ellison syndrome (rare-when one or more tumors form)
What are the treatment options for Ulcers?
Omeprazole (Losec)- blocks protein pumps in the canaliculi (only works if pH is equal to/lower than 3)
What do H2 (histamine receptors) antagonists do? What is an example of this?
-Competitively inhibits actions of histamine receptors on oxyntic cells
-Ranitidine- not used anymore- due to presence of NDMA in manufacture
What can be absorbed by the stomach?
Aspirin- becomes lipid soluble at low pH
Alcohol- is lipid soluble
How can aspirin cause peptic ulcers?
Inhibits prostaglandin synthesis=> reduced inflammatory response to injury & reduced cell turnover (i.e. prevent repair)
What is the role of the stomach?
Responsible for churning the food & mixing it with gastric juice
What do the pacemaker cells in the longitudinal muscle of the greater curvature of the fundus do?
Depolarises in response to vagal stimulation/gastrin
Or
Hyperpolarises in response to adrenalin/CCK/Secretin
What is the basal rhythm?
spontaneous depolarisation and repolarisation of pacemaker cells in the smooth muscle of the stomach, small intestine, and large intestine
Is the basal rhythm lower in the stomach or duodenum?
Basal rhythm lower in the stomach than in the duodenum- because if it was the same, when the pyloric opens, all the content with acid would go into duodenum & will overwhelm the duodenum with acid
What happens in the stomach after a meal?
-First ½ hr- peristalsis causes weak ripples over the body of the stomach pushing food towards the antrum
-Contractions becomes more intense- eventually a large part of the muscle in the terminal antrum undergoes intense contraction- empties material into duodenum.
-Only a small spurt is emptied at one time- rest is forced back into stomach for further mixing. Pressure in duodenum helps close the pyloric sphincter
What does the control of stomach secretion involve?
1. Intrinsic and extrinsic nerves
2. Hormones and paracrine mediators
What has a similar structure gastrin?
CCK- competes for the same active site as gastrin
What are the 2 forms of gastrin?
G17 (17aa's)- half life of 6 mins
G34 (34(aa's)- half life of 36 mins
What does gastrin act on?
Oxyntic (parietal) cells (acid producing)
ECL
D cells
What is the neural control of gastric secretions?
- Intrinsic nerves of ENS (enteric nervous system)
- Extrinsic nerves in vagus and sympathetic system
In general, what do cholinergic fibres do?
Stimulate gastric secretion and motility
In general, what do adrenergic fibres do?
Inhibit secretion and motility
What do some fibres in the vagus nerve also contain?
GRP= gastrin- releasing peptide
What controls acid secretion?
Somatostatin
Prostaglandins
What does somatostatin do?
Inhibits gastrin secretion
It acts paracrine and hormonal
Where are prostaglandins synthesised?
In the gastric mucosa
What is the function of the prostaglandins?
- Protect deeper mucosal layers from damage by acid
-Inhibit acid secretion
When is mucus secreted?
In response to chemicals such as alcohol, and contract with roughage (indigestible material)
What are mucus neck cells stimulated by?
Gastrin
How is stomach motility controlled?
- By Pacemaker cells in the longitudinal muscles of the stomach in the greater curvature region of the fundus
- Spontaneously oscillating membrane potential generating action potentials in pacemaker cells
How is the activity of the pacemaker increased/ decreased?
- Activity can be increased or decreased in amplitude and frequency by factors that control electrical activity of the smooth muscle cell membranes.
- These changes are of different shape and amplitude in different regions of the stomach
What also controls stomach motility?
Normal muscle contraction:
Rapid depolarisation phase- entry of Ca2+ through voltage gated channels
Plateau phase- entry of both Na+ and ca2+ through slow voltage gated channels
Control of stomach motility-
What endogenous factors cause depolarisation in smooth muscle?
Stretch, ACh, Gastrin
Control of stomach motility - What endogenous factors cause hyperpolarisation in smooth muscle?
Adrenaline, ATP, CCK, secretin, VIP (Vasoconstrictive intestinal peptide), GIP (gastric inhibitory peptide)
Is the basal electrical rhythm of the duodenum faster or slower than of the stomach?
Faster- refer to slide 7
Why does the duodenal bulb contract irregularly?
It is due to the influence of both the stomach and duodenum
Is the activity of the antrum and duodenum coordinated?
Yes
What is the pyloric sphincter innervated by?
Parasympathetic (vagus) and sympathetic
What neurotransmitter is released by the sympathetic nerves and what does it do?
Noradrenaline- increases constriction of sphincter
What constricts the pyloric sphincter other than noradrenaline?
Excitatory vagus nerves- Cholinergic fibres of the vagus
CCK also constricts sphincter
What relaxes the pyloric sphincter?
Inhibitory vagus nerves- Inhibitory fibres release VIP (Vasoconstrictive intestinal peptide)
How is the motility of stomach partly controlled by blood glucose levels?
When blood glucose falls when fasted gastric smooth muscle is stimulated
Peristaltic contractile activity increases but gastric emptying does not (can be very strong "hunger pains")- impulse due to impulse in the vagus nerve which is sensitive to low blood glucose
What are the 3 stages of gastric function?
1. Cephalic phase
2. Gastric phase
3. Intestinal phase
Summary of the cephalic phase
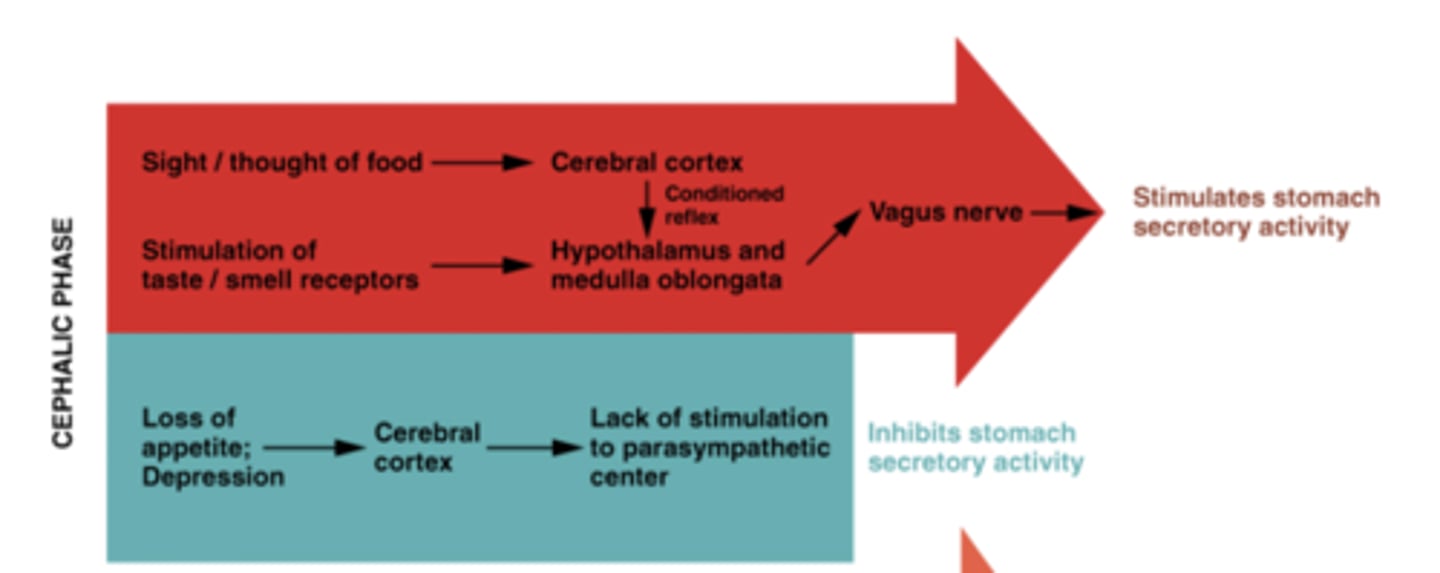
What occurs in cephalic secretion?
>Occurs before food reaches the stomach-
Response to smell, sight and touch of food
(Emotions also influence gastric secretion)
>Response to sight/smell is a conditioned response
>Response to taste and touch is a non-conditioned reflex
Effects are facilitated by the vagus nerve
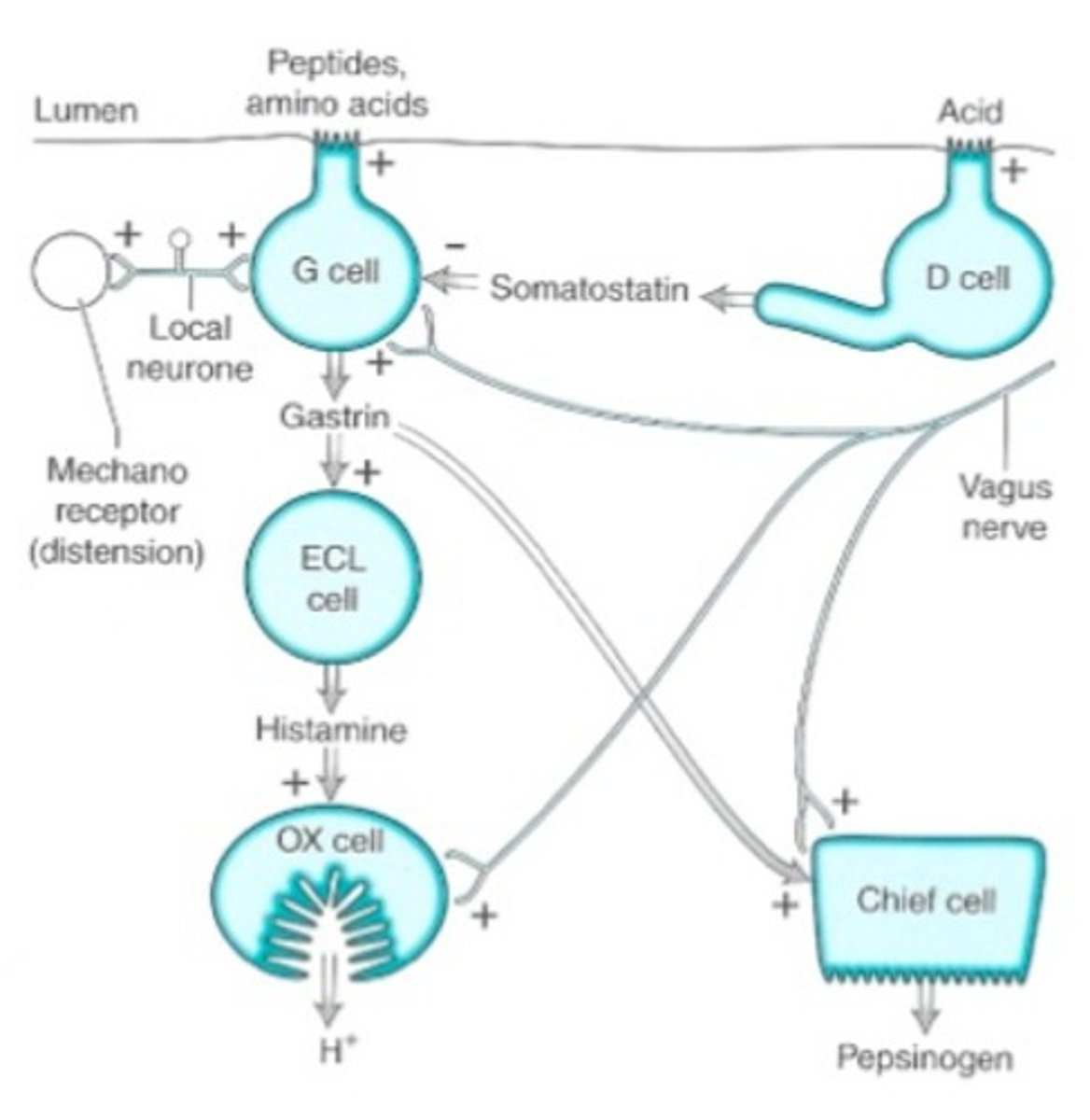
What affects cephalic motility?
- Sight, smell, taste and touch of food also inhibit gastric emptying
- Pain, depression, fear and sadness also inhibit
- Mechanism- probably via purinergic fibres in the vagus nerve
- Aggression and anger increase stomach motility (mechanisms no elucidated)
Summary of the gastric phase
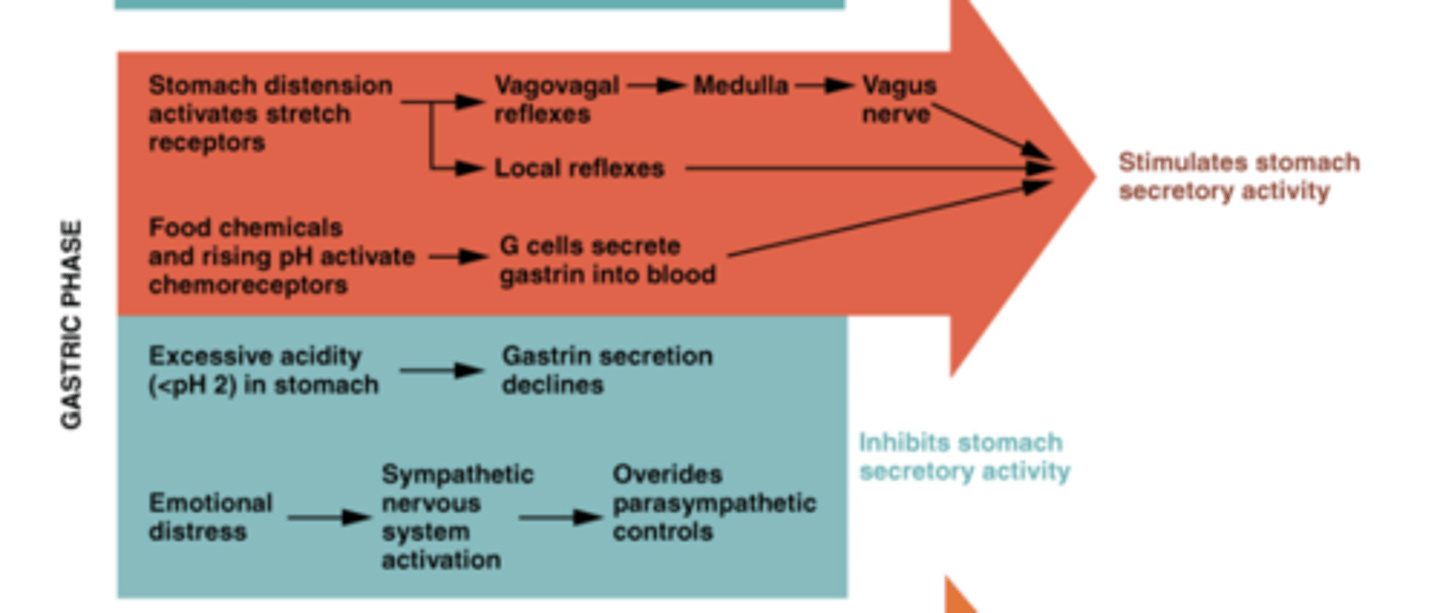
What happens/stimulates gastric phase secretion?
>Secretion stimulated by food directly
place in the stomach
>Amount of secretion depends on
chemical content of food and volume
(distension of wall-not as powerful a
stimulant as chemical)
>Products of protein digestion, caffeine
and alcohol stimulate gastric
secretion
>These chemical substances
(secretagogues)are sensed by APUD
cells (act like taste cells)
>G cells sense peptides and aa's-D
cells sense pH
>Gastric phase accounts for >50% of
acid secreted during a meal.
Summary of the intestinal phase
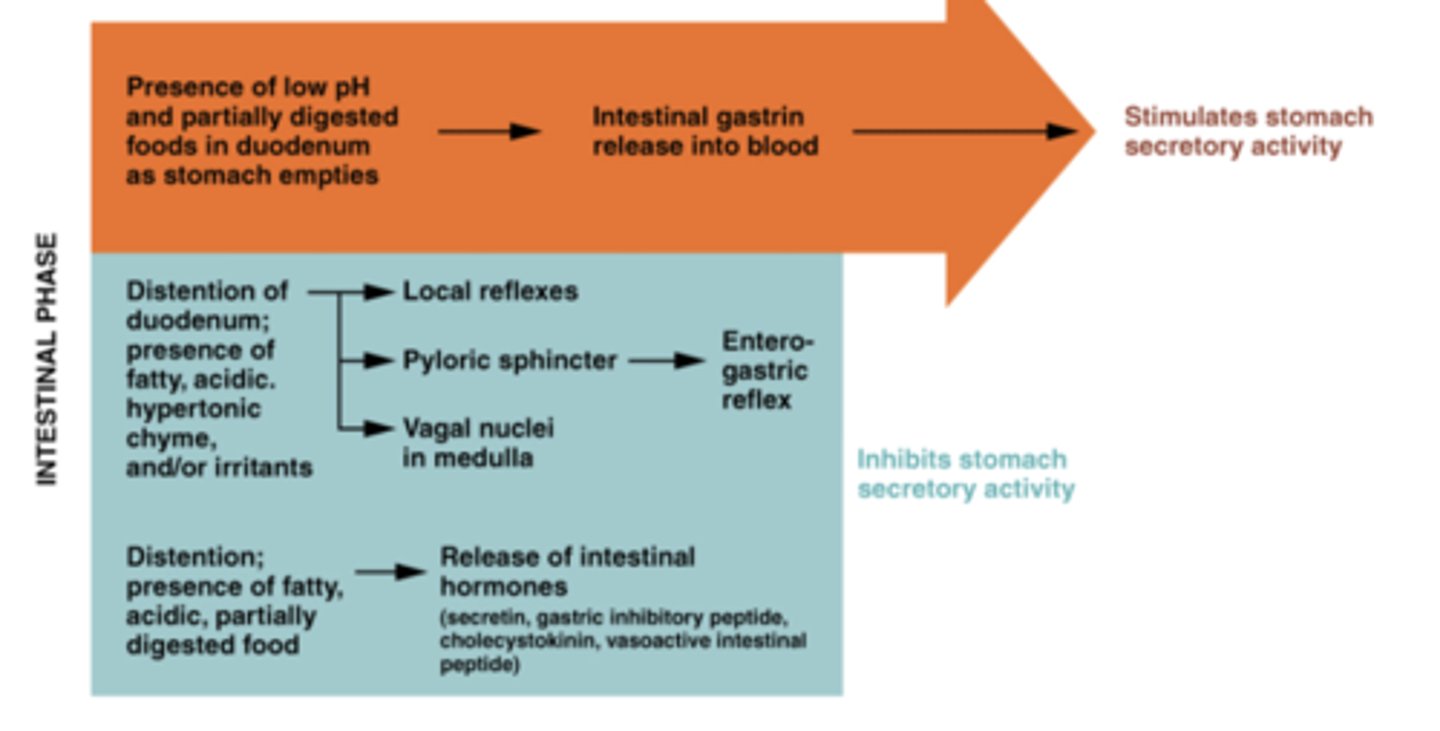
What happens/ stimulates gastric phase motility?
>At this stage the stomach empties at a rate proportional to
the volume of material within it
>Chyme stimulates pressure receptors in the wall of the
stomach which trigger impulses in the internal nerve plexi
>Probably also the direct effect of stretching the smooth
muscle ('stretch activation')
There is also a vagal mechanism involved in the response
to distension but unlike in the cephalic phase, vagal
impulses increase peristalsis and gastric emptying (in this
case cholinergic rather than purinergic fitres)
What happens/ stimulates intestinal phase secretion?
>Food in duodenum is largely inhibitory
>There is an early stimulatory phase in response to slight distension ofthe
duodenum (probably due to release of gastrin from the duodenum)
>Inhibitory stimuli= distension (dilation) of duodenum, fats, peptides, increased acidity and hypertonic solutions
> Stimuli cause APUD cells to release secretin into blood (inhibits secretion or
gastric juice) and CCK (inhibits acid and pepsinogen release in stomach)
>Important because:
1) Digestive enzymes in duodenum need neutral alkaline pH
2) Micelle formation (fats) needs neutral/alkaline pH
3) Duodenum common site for ulcer formation
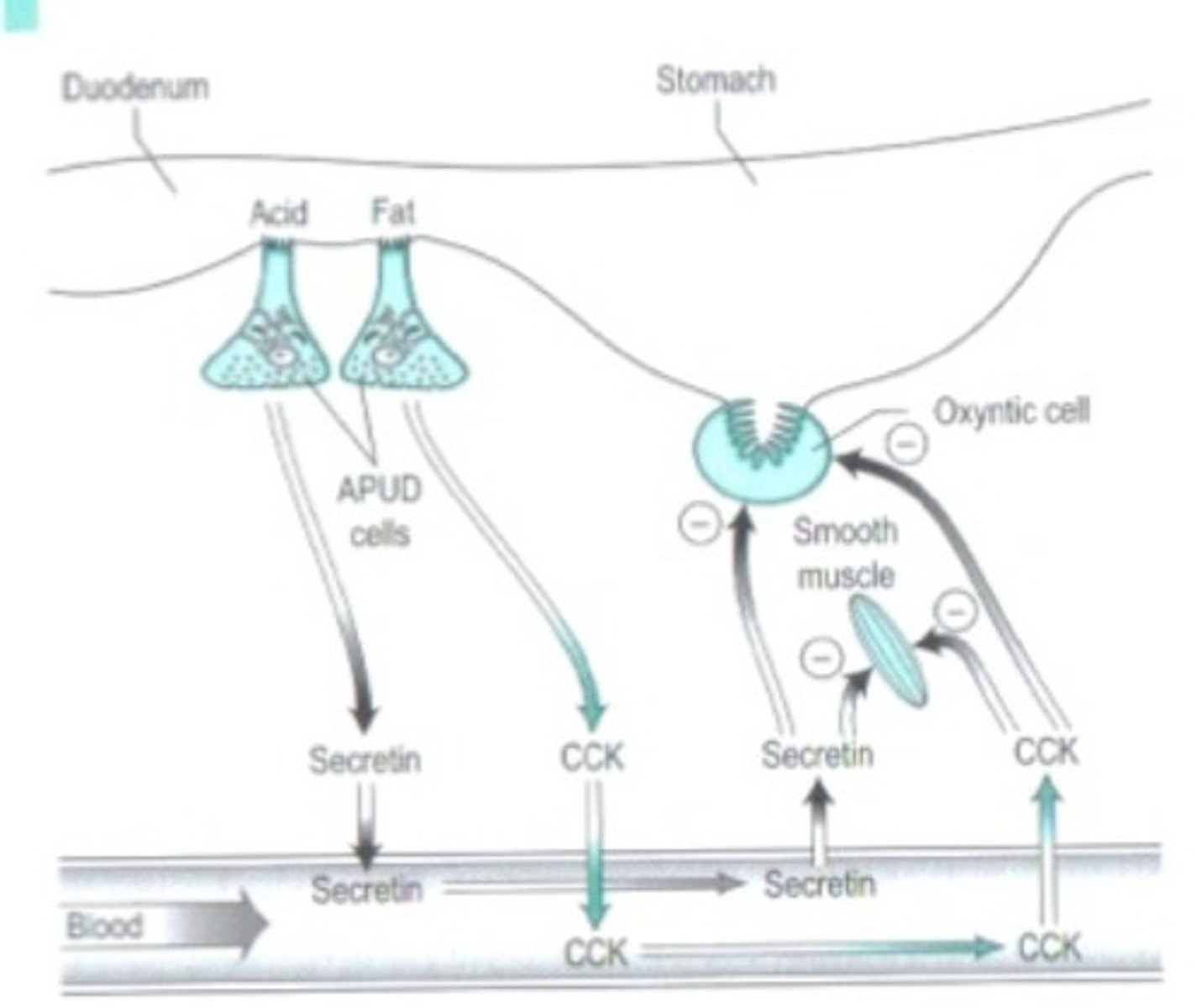
What happens/ stimulates intestinal phase motility?
>Distension of the duodenum inhibits gastric motility in two ways:
1) Enterogastric reflex (fast -nerve fibres in vagus)
2) Humoral mechanism (sow-hormones called 'enterogastrones' including CCK
and secretin)
>When food reaches the ileum emptying of the stomach is delayed (neural reflex)
>This 'ileogastric reflex' operates in both directions (ie., food entering stomach increase motility of ileum)
>Also a neural response when chyme enters colon-distension of colon delays gastric emptying