Female reproduction system
1/35
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
36 Terms
T/F: the parietal perineum does not reach the pelvic floor
True: it reflects onto the pelvic viscera, remaining separated from the pelvic viscera and the surrounding pelvic fascia
only the superior and superolateral surfaces of the pelvic viscera are covered with peritoneum
The _________ and __________ are the only structures that are fully surrounded by peritoneum
Ovaries and uterine tubes (fallopian tubes)
There is a small opening in the parietal peritoneum at the junction of the ________ and __________
Ovaries, uterine tubes
zygotes can implant outside of uterus = ectopic pregnancy
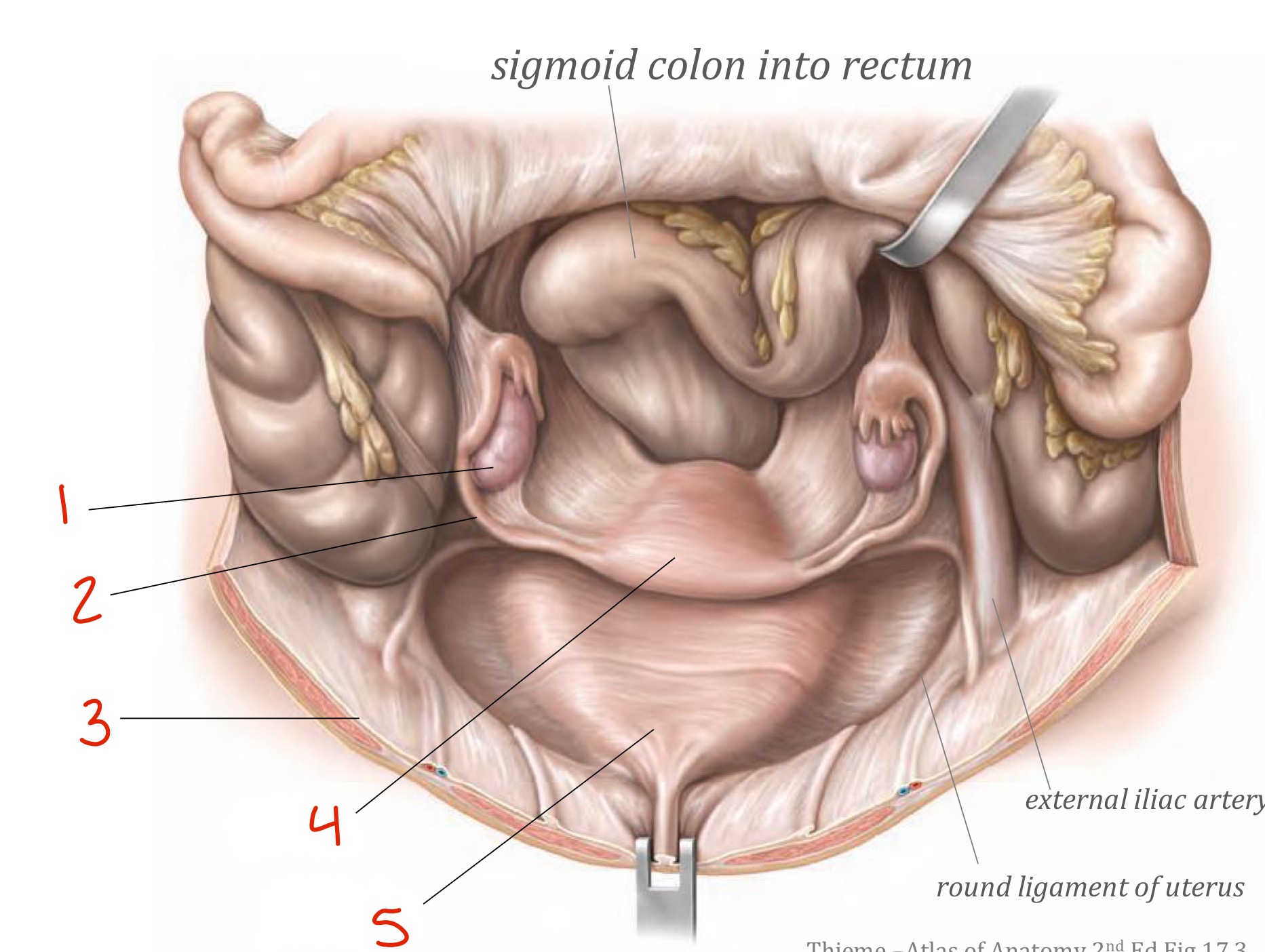
Identify
Ovary
Uterine tube
Parietal peritoneum
Uterus
Bladder
The parietal peritoneum forms two pouches between neighbouring pelvic viscera. What are they?
Vesico-uterine pouch: between bladder and uterus
Recto-uterine pouch: between rectum and uterus
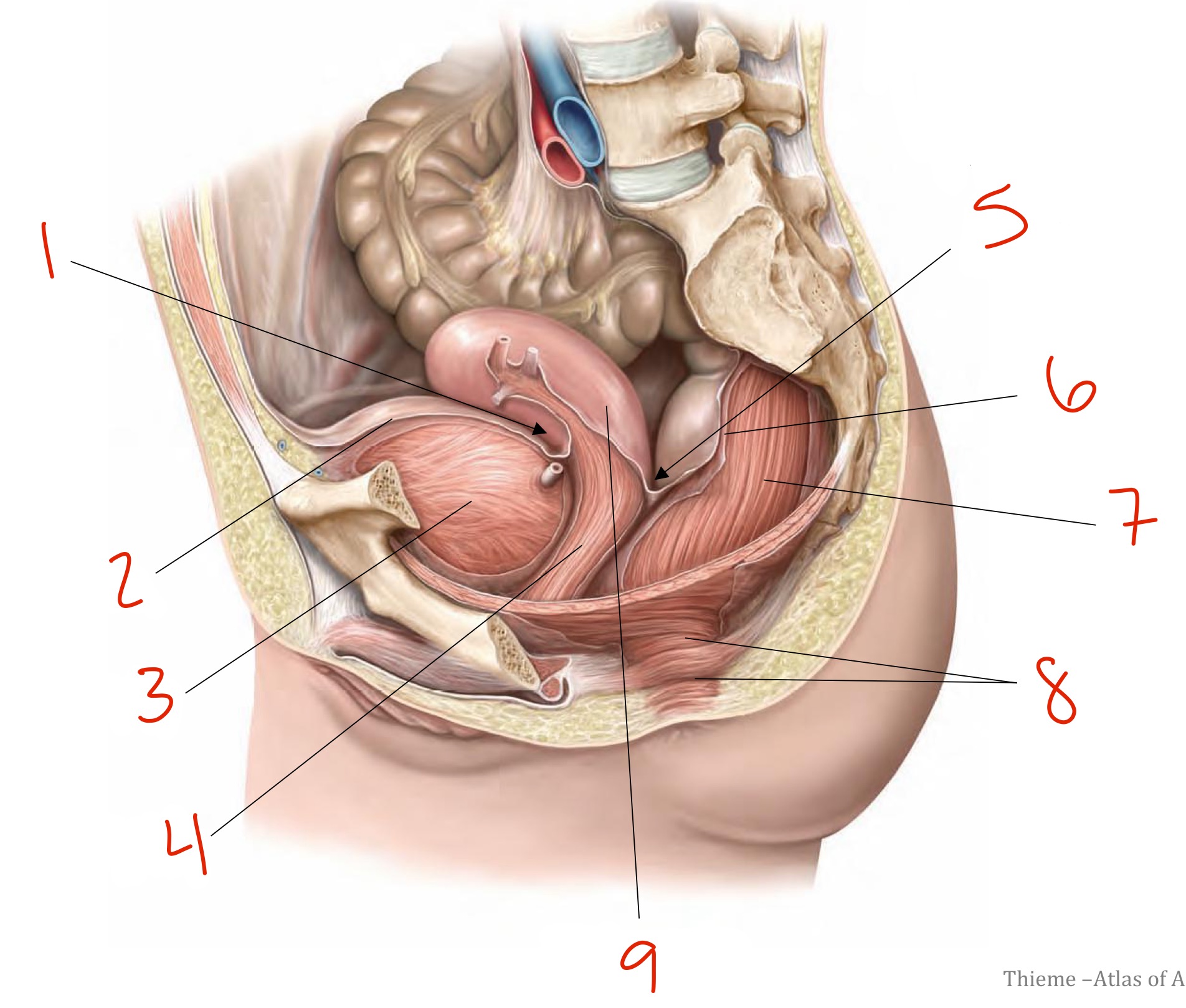
Identify
Vesico-uterine pouch
Parietal peritoneum
Bladder
Vagina
Recto-uterine pouch
Parietal peritoneum
Rectum
Anal canal
Uterus
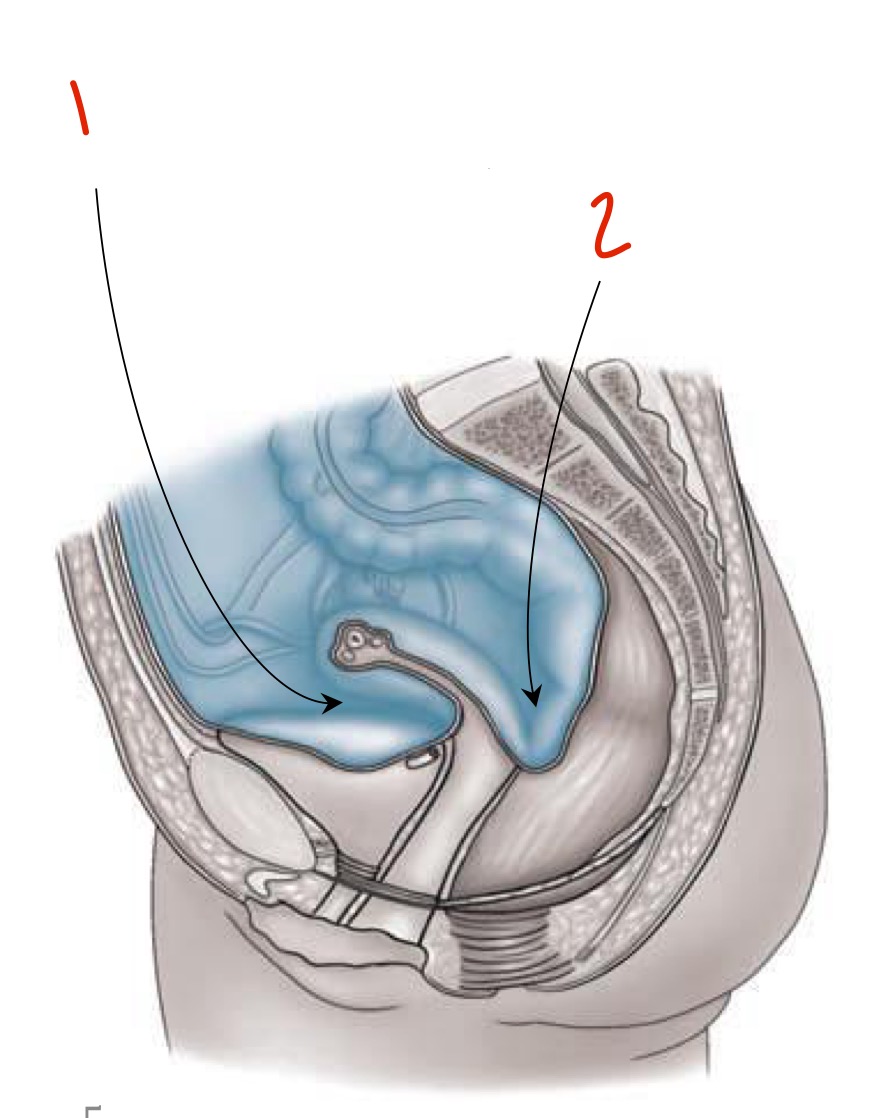
Identify
Vesico-uterine pouch
Recto-uterine pouch
What are the pelvic organs? Are they part of:
Lower GI tract
Lower urinary tract
Internal pelvic organs
External pelvic organs
Ureter - lower UT
Bladder - lower UT
Urethra - lower UT
Sigmoid colon - lower GI
Rectum - lower GI
Anal canal - lower GI
Ovary - internal pelvic
Uterine tube - internal pelvic
Uterus - internal pelvic
Vagina - internal pelvic
Vulva - external pelvic
Clitoris - external pelvic
The sigmoid colon becomes the _________ at the rectosigmoid junction (level of S3), which then becomes the ____________ at the anorectal flexure as it passes through the levator ani
Rectum, anal canal
What nerve and artery/vein are associated with the perineum?
Pudendal nerve
Internal pudendal artery and vein
Name and describe the different parts of the vulva
Mons pubis: the rounded, hair-bearing area of skin and adipose tissue over the pubic symphysis
Labia majora: two prominent, longitudinal folds of skin that extend back from the mons pubis to the perineum
Labia minora: two small cutaneous folds, devoid of fat, that lie between the labia majora
Glans of the clitoris: an erectile structure, partially enclosed by the anterior bifurcated ends of the labia minora
Vestibule: the cavity that lies between the labia minora; contains the following structures
Urethral orifices: open into the vestibule about 2.5cm below the clitorisa d above the vaginal opening
Vaginal orifice: external opening
Vestibular bulb: two elongated masses of erectile tissue, 3cm long, on each side of the vestibule (each covered posteriorly by bulbospongiosus)
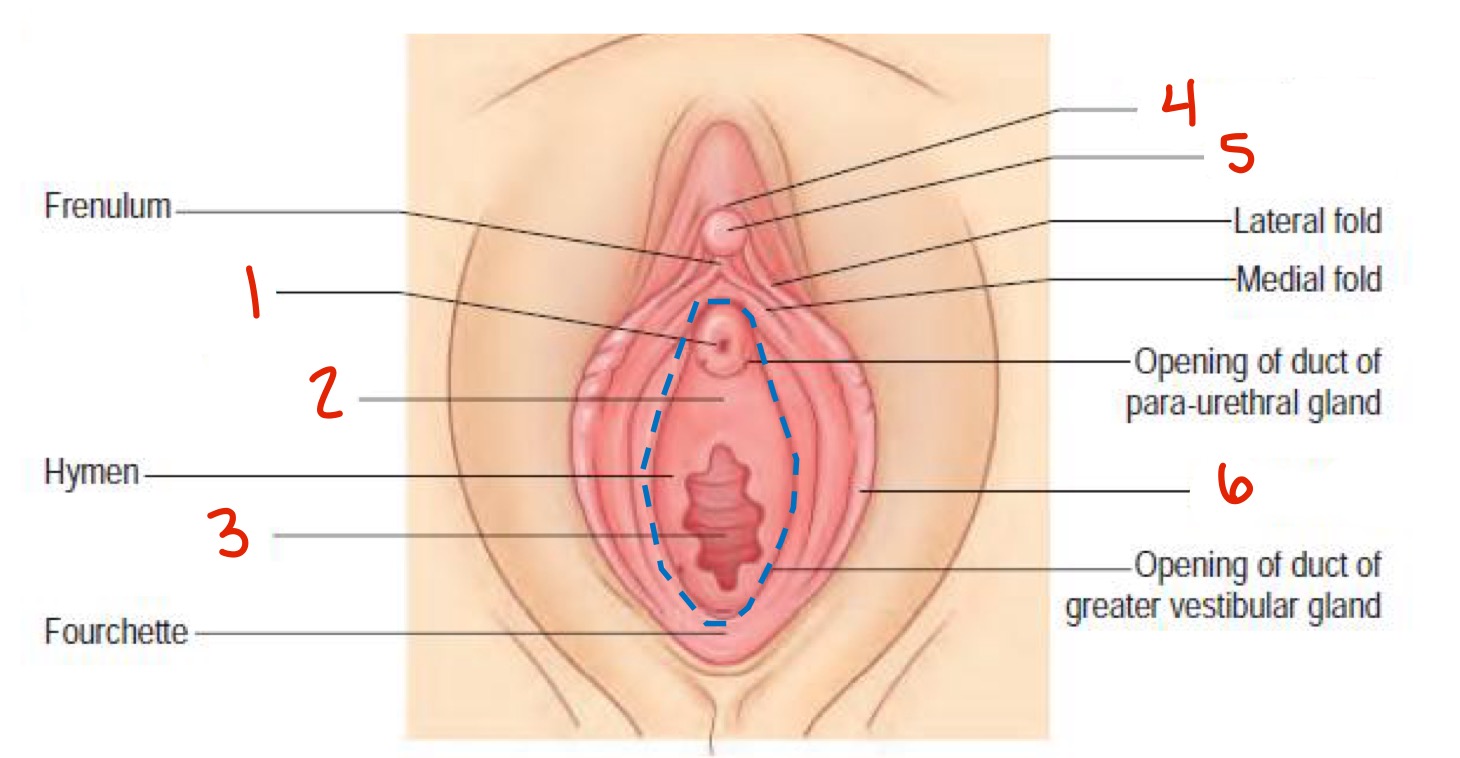
What’s the function of the clitoris?
It is the organ of sexual arousal
highly innervated (twice as much as penis)
Describe the external anatomy of the clitoris
Suspensory ligament: attached to pubic symphysis and clitoral hood
Clitoral hood: shaft skin from the clitoral body (also called prepuce)
Glans of clitoris: 0.5 to 2.5cm
Labia minora
Vestibule → urethral orifice and vaginal orifice
The deeper anatomy of the clitoris includes structures such as the clitoral body, crura, and greater vestibular glands (Bartholins gland). Describe them.
Clitoral body:
Internal structure similar to shaft of penis
Includes corpora cavernosa (erectile tissue that engorges with arousal)
Dorsal nerve of the clitoris
Crura:
split of the body composed of corpora cavernosa
Attach the corpora cavernosa to the ischiopubic ramus
Extend from root of the clitoris
Bartholin’s glands:
two pea-sized compound alveolar glands, located on either side of the vaginal opening, deep to the labia majora in the vulva
Produce mucus to lubricate the vagina and vulva
Innervated by the pudendal nerve (sensory and parasympathetic stimulation)
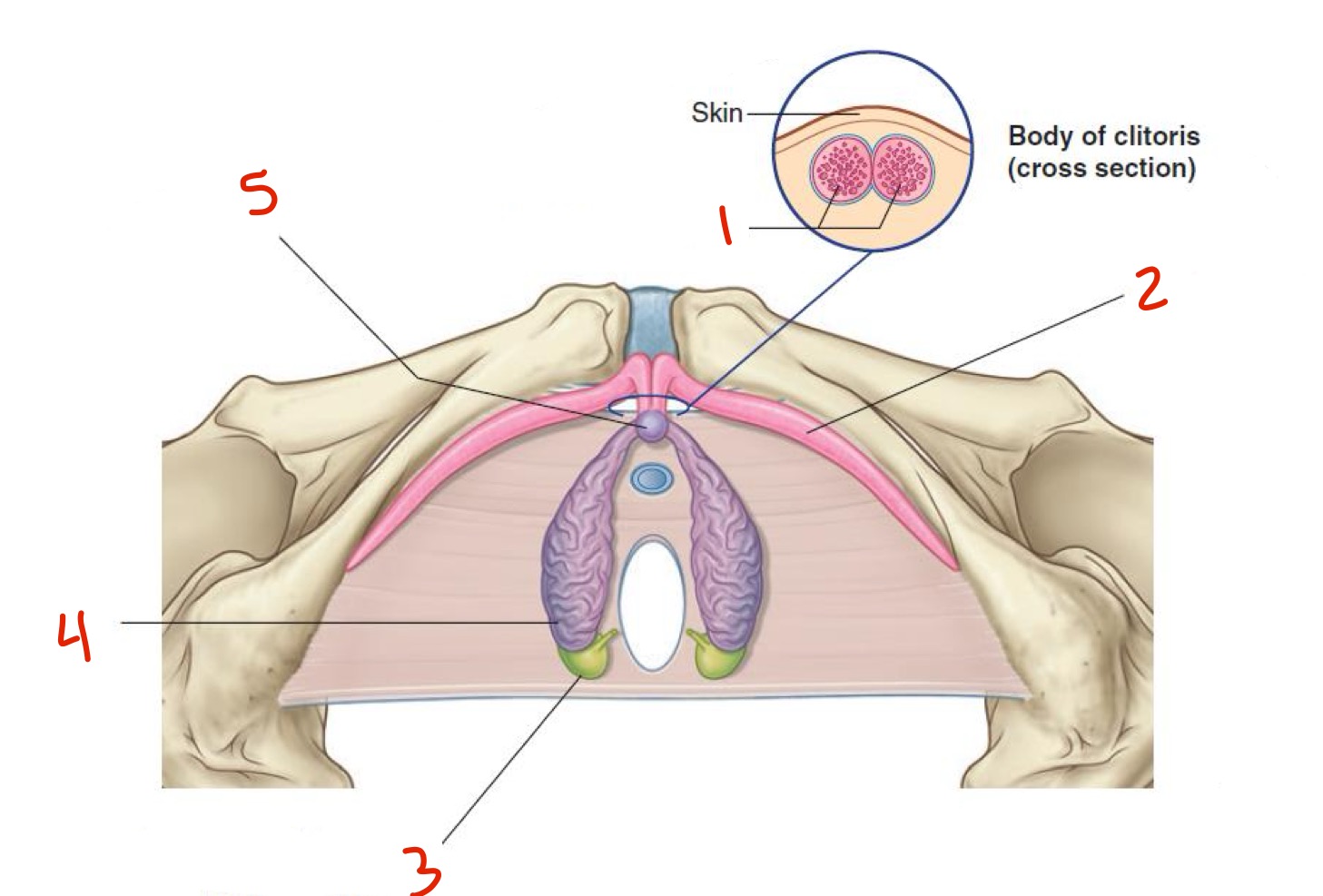
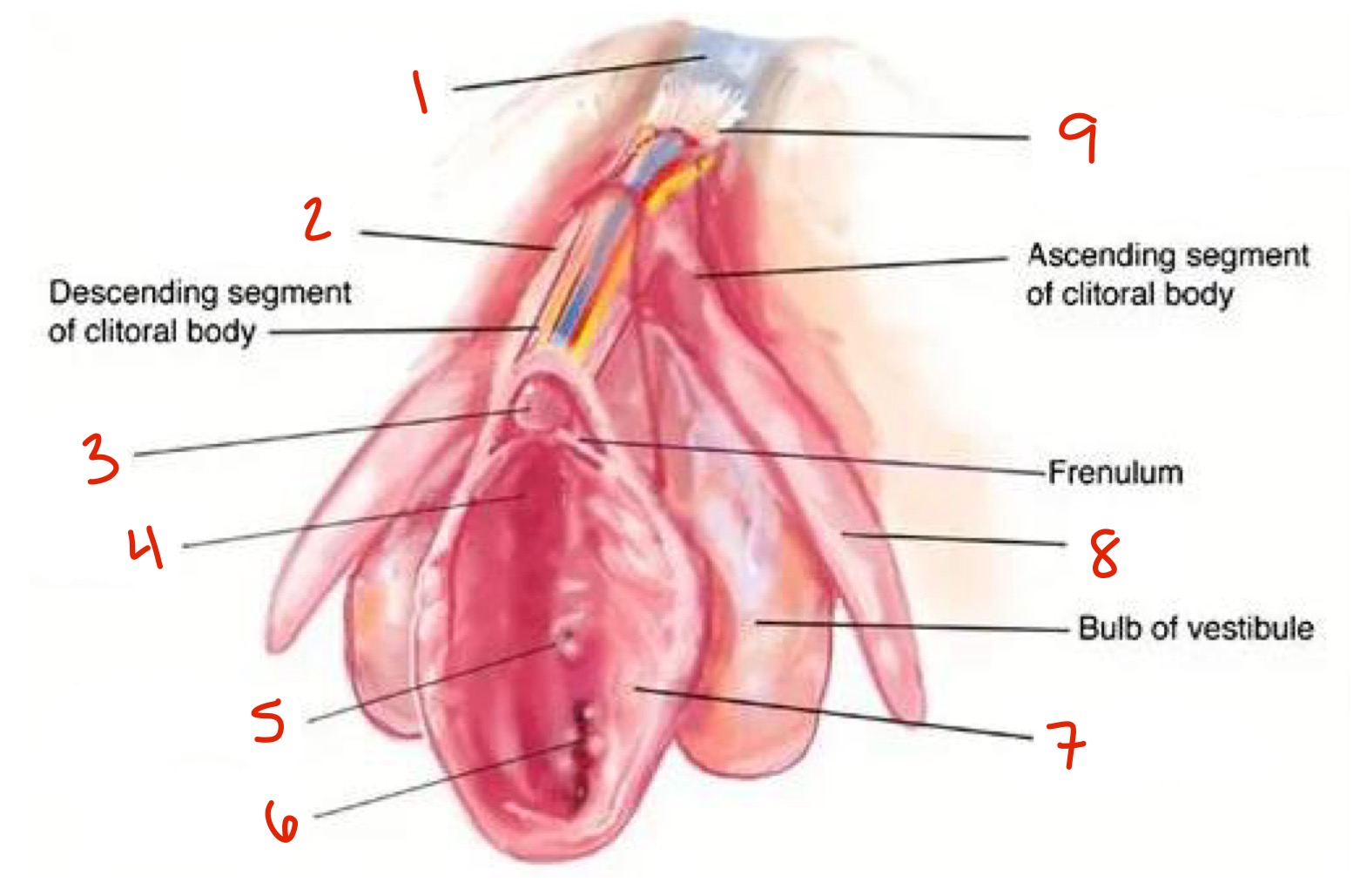
Identify
Pubic symphysis
Clitoral hood
Glans of clitoris
Vestibule
Urethral orifice
Vaginal orifice
Labia minora
Crus
Suspensory ligament of clitoris
What is the vagina?
A fibromuscular tube lined by non-keratinized stratified epithelium
Describe the anatomy of the vagina (not the muscles)
extends from the vestibule to the uterus
Vaginal canal is usually collapsed so that the anterior wall is in contact with the posterior wall
Vaginal vault: enlarged internal end of the canal
The urethra is embedded in the anterior wall
Recto-uterine pouch (pouch of Douglas) separates the posterior vagina from the rectum
Which muscles surround the vagina?
Levator ani: supports the upper part of the vagina laterally, together with the transverse cervical, pubocervical, and uterosacral ligaments
Pubovaginalis: provides a U-shaped muscular sling around the mid-vagina
Bulbospongiosus: surrounds the lower vagina
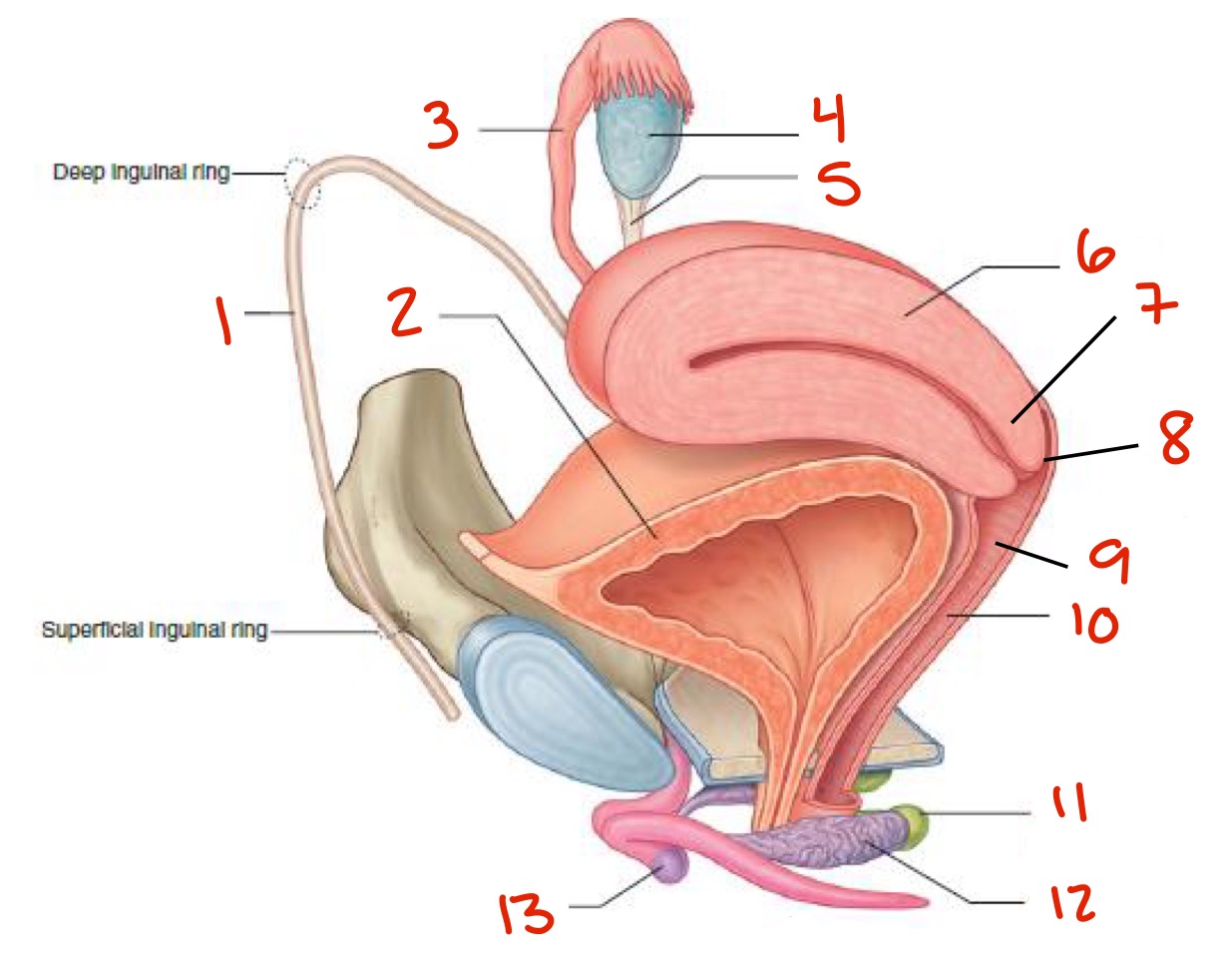
What is the uterus? What are its functions?
A thick-walled, muscular, pear-shaped organ in the midline between the bladder and rectum
It’s position varies with distension of the bladder and rectum
Functions: gestation, menstruation, labor and delivery
What does the uterus consist of?
Body: flattened anteroposteriorly, made up of:
Fundus: rounded superior end
Isthmus: inferior-posterior part of the uterus, on its cervical end where the uterine muscle is narrower and thinner
Cervix: the lower, cyndrical part
External os: opening between cervix and the vagina inferiorly
Normal cervix feels firm and smooth, and has a slight indentation in the middle
Where are the uterine tubes?
Connected to uterus; project laterally from the uterus and open into the peritoneal cavity immediately adjacent to the ovaries
The uterus has __ layers. What are they?
Three:
Perimetrium: the outer double-layered serous membrane of the uterus
Secretes a lubricating fluid that helps reduce friction
Also part of the peritoneum that covers some of the organs of the pelvis
Myometrium: the middle and thickest layer
made up mostly of smooth muscle
Cells undergo hypertrophy and hyperplasia during pregnancy
Endometrium: the inner layer that lines the uterus
Made up of glandular cells that make secretions
Site of implantation of a blastocyst
Sheds if pregnancy doesn’t happen
Subdivided into 2 parts (that I don’t need to know)
slide 14
What are the parts of the uterine tubes ?
Infundibulum: lateral, funnel-shaped portion
Fimbrae: pick up and carry the oocyte from the ovary after ovulation and transport it to the uterus over the course of 4-5 days
Ampulla: expanded portion medial to infundibulum
usual site for fertilization
Isthmus: narrow medial portion
visceral peritoneum, smooth muscle, ciliated epithelium
What’s the broad ligament?
A double-sheet of peritoneum (a mesentery) that supports and develops the ovaries, uterine tubes, and uterus
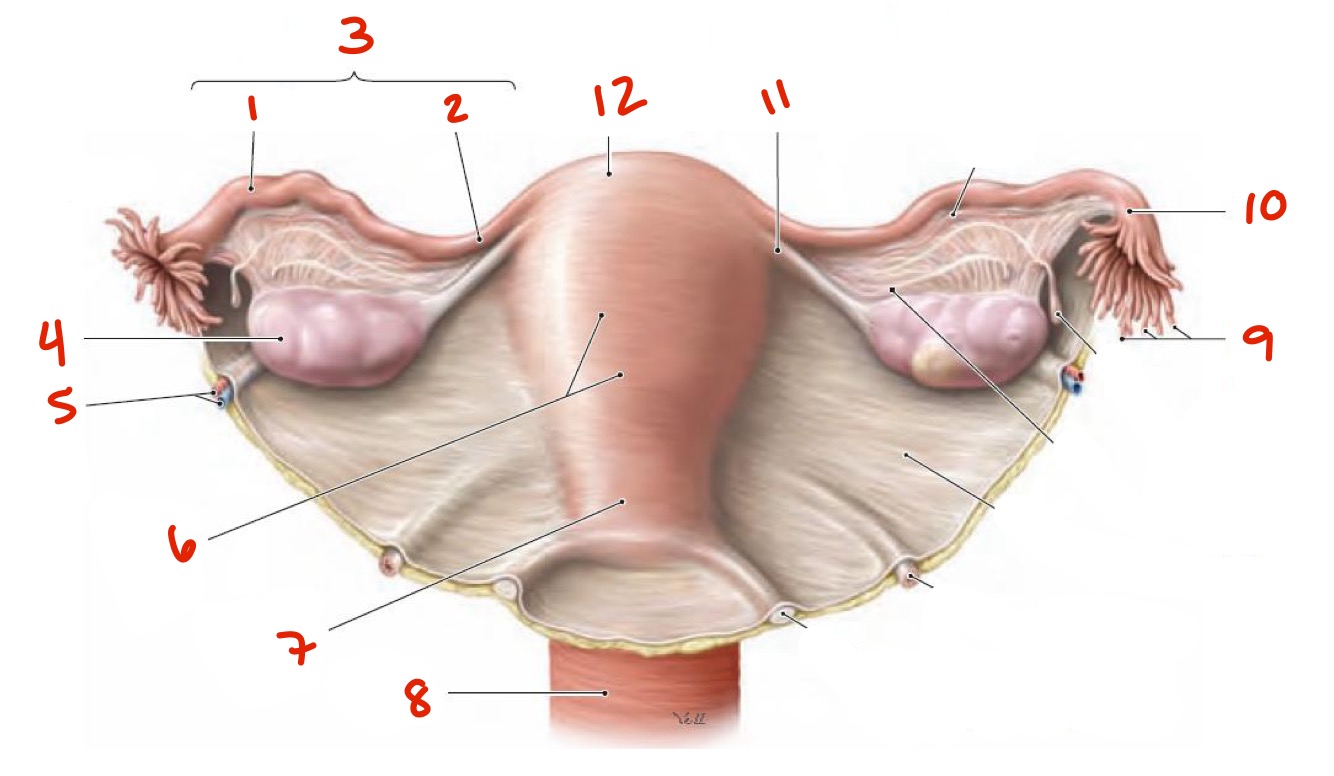
Identify
Ampulla
Isthmus
Uterine tube
Ovary
Ovarian artery and vein in suspensory ligament of ovary
Body of uterus
Cervix
Vagina
Fimbriae
Infundibulum
Ligament of ovary
Fundus of uterus
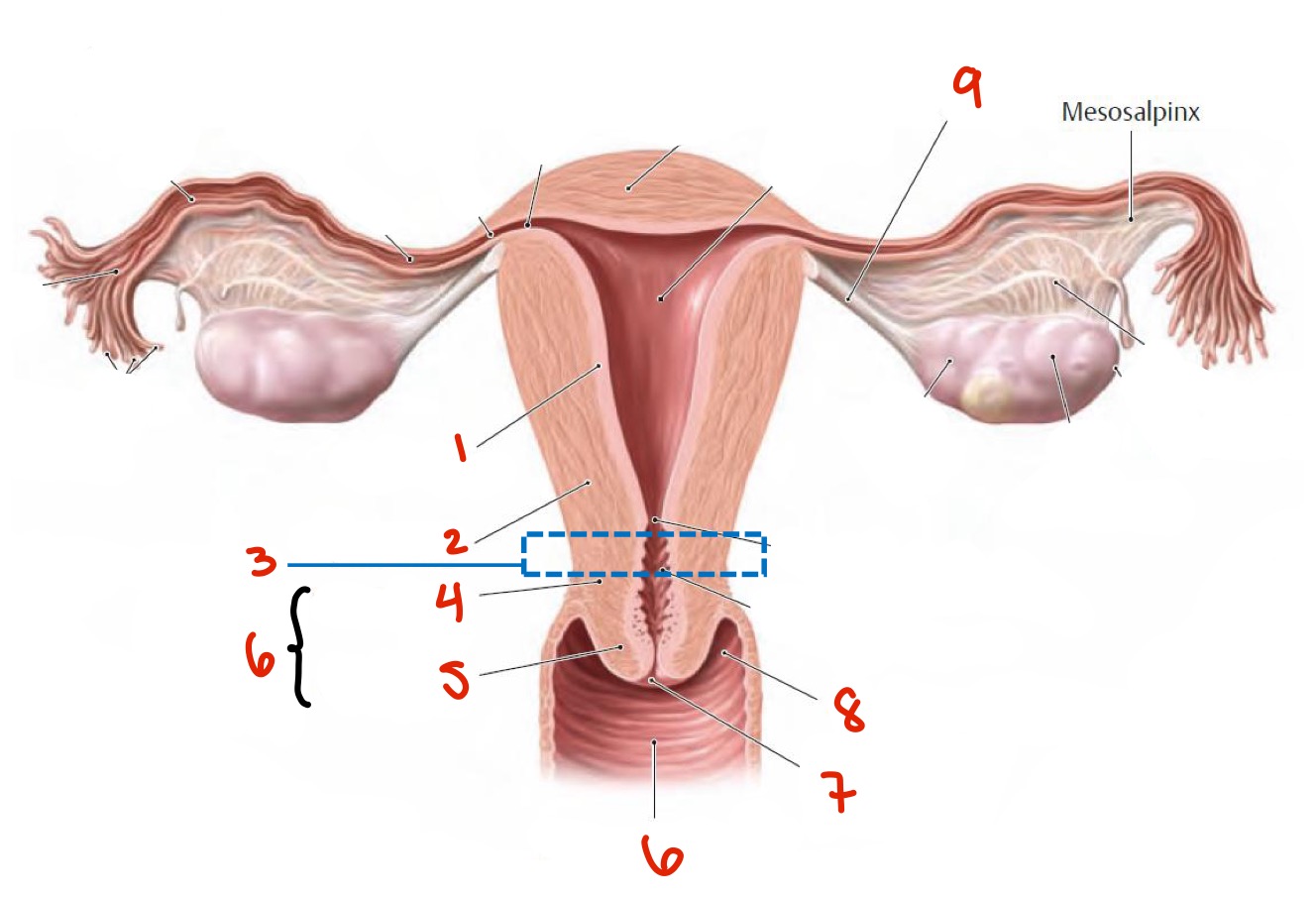
Identify
Endometrium
Myometrium
Isthmus
Supravaginal part of cervix
Vaginal part of cervix
Cervix — vagina (there are 2 6’s)
External os
Vaginal fornix
Ligament of ovary
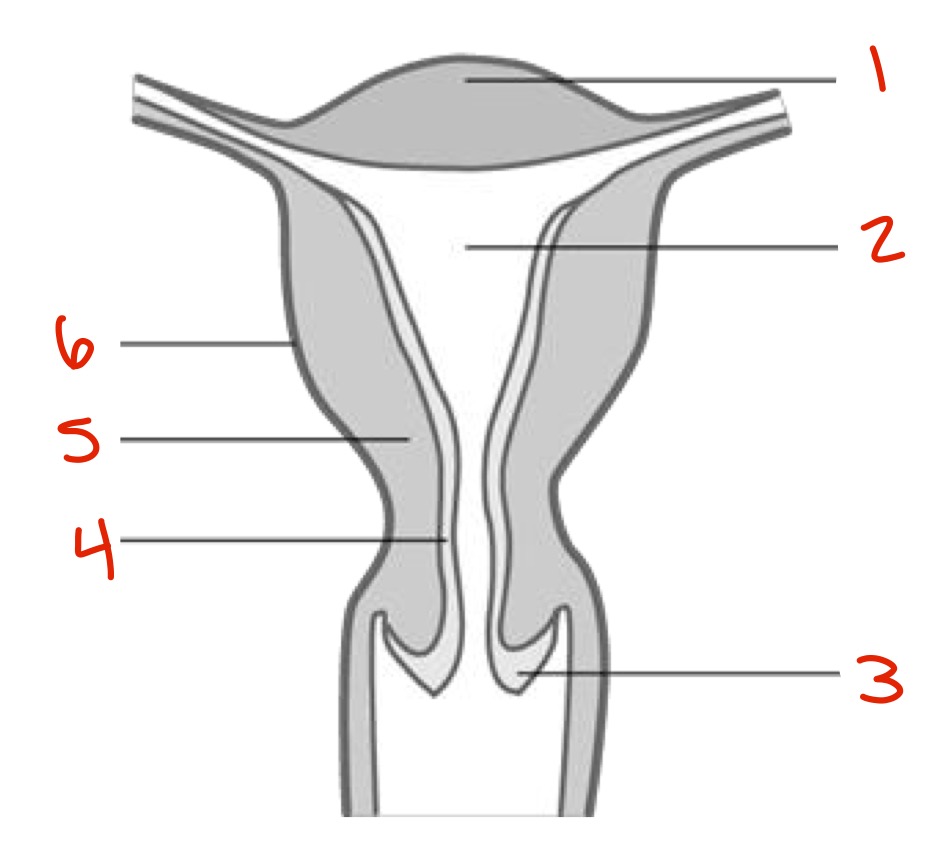
Identify
Fundus
Uterine cavity
Cervix
Endometrium
Myometrium
Perimetrium
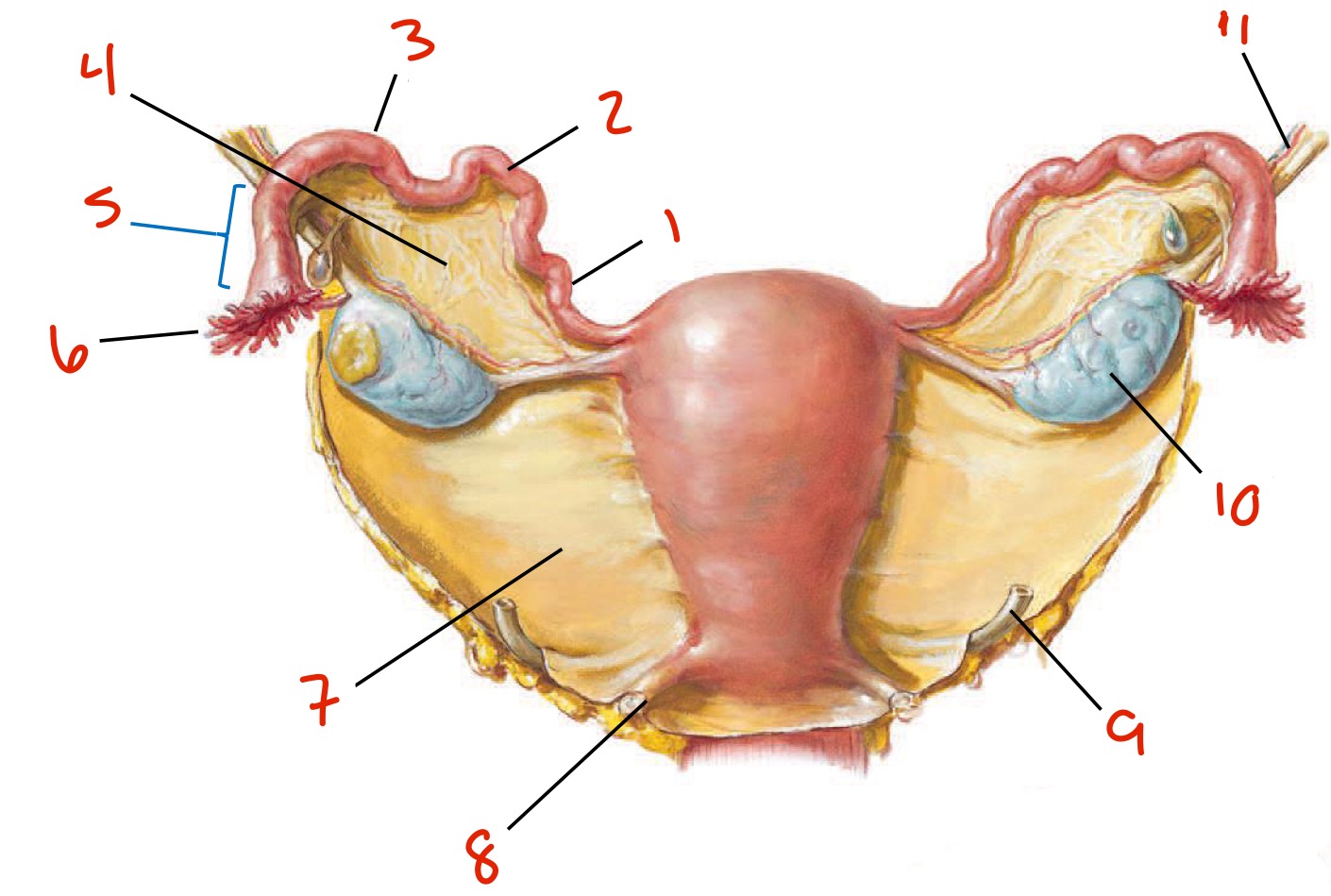
Identify
Isthmus
Uterine tubes
Ampulla
Broad ligament
Infundibulum
Fimbrae
Broad ligament again
Uterosacral ligament
Ureter
Ovary
Suspensory ligament of the ovary
Slide. 17
What artery supplies:
Uterus
Vagina
Ovaries
Uterine arteries (from internal iliac artery)
Vaginal arteries (from internal iliac)
Ovarian arteries (from aorta) and ovarian branches of the uterine arteries
The ovarian arteries are surrounded by the ______________
Suspensory ligament — a fold of peritoneum that extends from the upper pole of the ovary and uterine tube to the lateral pelvic wall
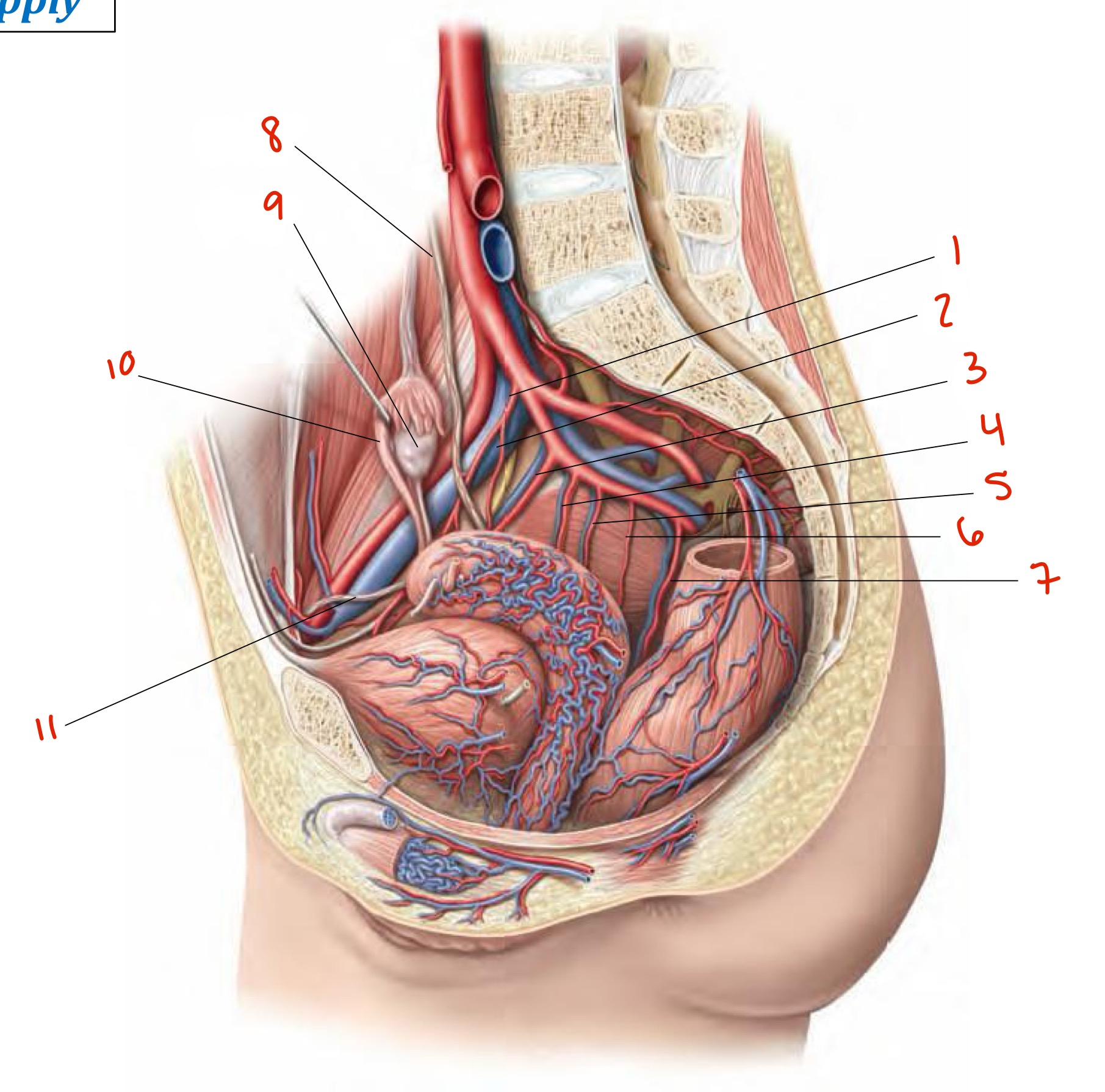
Umbilical a.
Superior vesical a.
Obturator a.
Uterine a.
Inferior vesical a.
Vaginal a.
Middle rectal a.
Ureter
Ovary
Uterine tube
Round ligament