A&P chap 12 - Heart terms
1/59
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
60 Terms
Pericardium
Loosely fitting sac that separates the heart from surrounding tissue
Allows space for the heart to expand and contract
fibrous pericardium
outer layer of pericardium
Parietal layer of serous pericardium
Delicate membrane lining inner surface of fibrous pericardium
Forms the visceral layer of serous pericardium at the base
epicardium
Thin membrane that tightly adheres to surface of the heart
Pericardial cavity
Space between the parietal layer and visceral layer of serous pericardium
Filled with pericardial fluid, Reduces friction
Myocardium
Thick layer of cardiac muscle tissue
Provides force for contraction
Epicardium
Outer layer
Contains blood vessels that nourish the heart
Endocardium
Inner layer of simple squamous epithelium
Continuous with the inner lining of the blood vessels attached to heart
atria
Receive blood from veins
ventricles
Pump blood into arteries
Interatrial septum
thin wall separating the heart's right and left atria
Interventricular septum
thick wall separating the heart's left and right ventricles
Atrioventricular valves
Allow flow from atria to ventricles.
Prevents backflow when ventricles contract
Tricuspid valve
Between R atrium and R ventricle
Mitral valve
Between L atrium and L ventricle
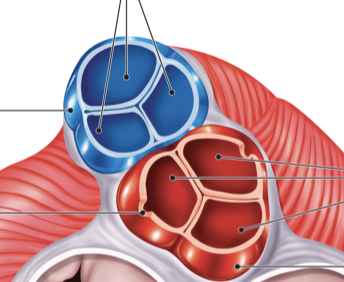
Semilunar valves
Located at bases of large arteries that carry blood from ventricles
Allow blood to flow from ventricles into blood vessels when ventricles contract
Prevent backflow from blood vessels when ventricles relax
AV valve structure
Originate from the fibrous skeleton of the heart
Provides valve support
Serves as electrical insulation between atria and ventricles
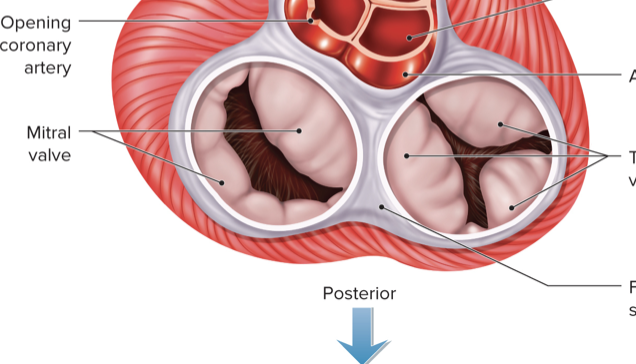
Semilunar valve structure
Three pocket-like cusps
Pulmonary circuit
Deoxygenated blood flows from R ventricle to lungs.
Oxygenated blood flows from lungs to L atrium.
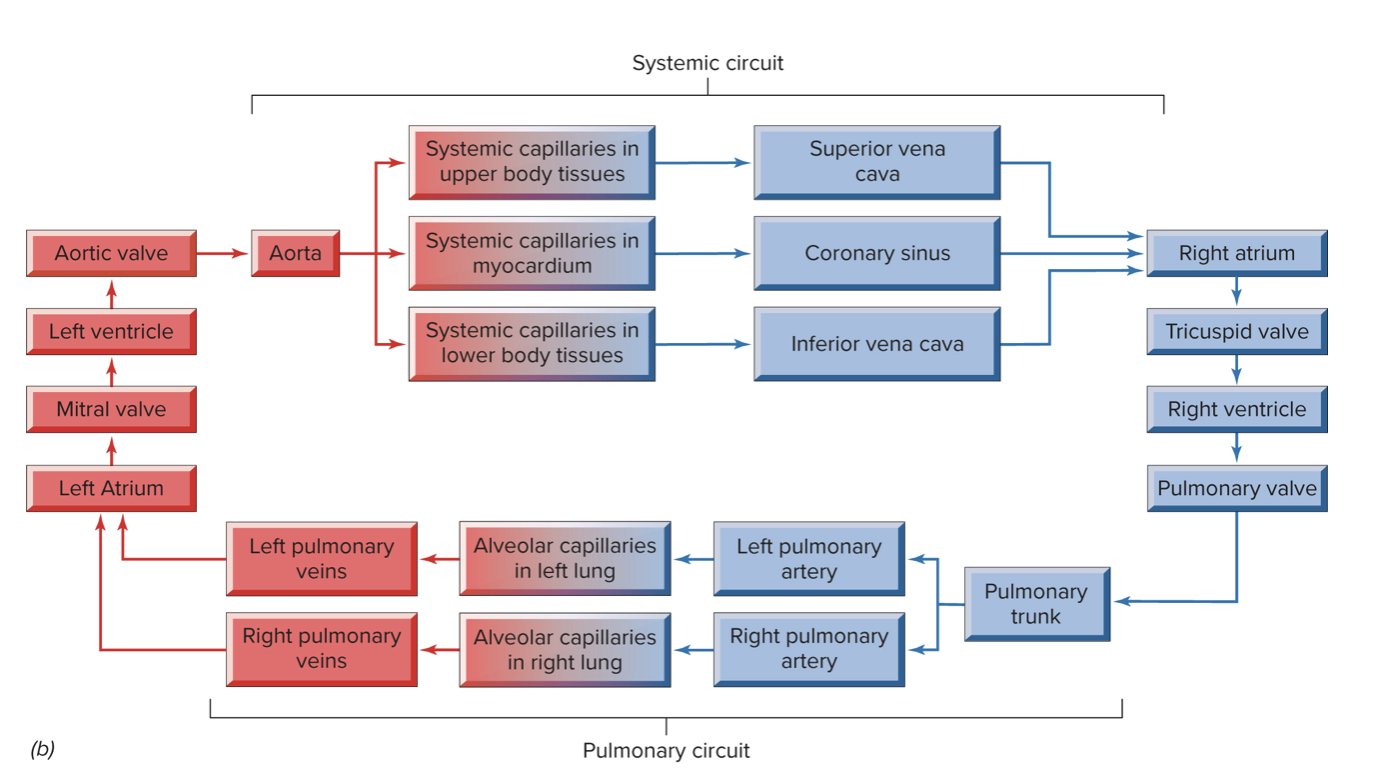
Systemic Circuit
Oxygenated blood flows L ventricle to body.
Deoxygenated blood flows from body to R atrium.
coronary arteries
Arise from the aorta just above the aortic valve
Supply myocardium with oxygenated blood
Cardiac veins
Lie next to coronary arteries
Return deoxygenated blood to the coronary sinus, which drains into the R atrium
Cardiac cycle
the sequence of events that occur during one heartbeat
Systole
Contraction phase
Increases blood pressure within a chamber
Diastole
Relaxation phase
Decreases blood pressure within a chamber
When ventricles contract, atria relax.
When atria contract, ventricles relax.
Lub
heart sound
closing of AV valves at the start of ventricular systole
dup
heart sound
closing of semilunar valves at the start of ventricular diastole
SA node
Located in right atrium near the SVC junction
Pacemaker of the heart
60–100 beats per minute
Rhythmically forms action potentials to initiate each heartbeat. Action potentials cause simultaneous contraction of atria.
AV Node
In right atrium near lower portion of interventricular septum
Receives action potentials from S A node
secondary pacemaker (40-60 bpm)
AV bundle
Divides into left and right bundle branches
Carry action potentials down ventricular septum and up lateral ventricle walls
Forms the subendocardial conducting network
Purkinje fibers
Carry action potentials to myocardium of ventricles
Contraction occurs from the apex upward
last resort pacemaker, (20-40) beats per minute.
P wave
Atrial depolarization
QRS complex
Ventricular depolarization
T wave
Ventricular repolarization
Electrocardiogram
Recording of the electrical current generated by the conducting system of the heart
Performed using an electrocardiograph
Cardiac output
the volume of blood pumped from each ventricle per minute.
Determined by, stoke volume and heart rate
CO = SV × HR
Stroke volume
volume of blood pumped out of each ventricle per heartbeat.
Heart rate
number of heartbeats per minute.
venous return
the rate of blood flow back to the heart's right atrium
medulla oblongata
Cardiac control center
Also affected by emotions created by the limbic system.
Baroreceptors
in the aortic arch and carotid sinuses.
Stimulated by changes in vessel wall stretching due to blood pressure changes.
Chemoreceptors
in aortic arch and carotid bodies.
Stimulated by low blood pH, high blood CO2, very low blood O2.
Sympathetic neurons
Axons exit thoracic region of spinal cord to innervate S A node (also A V node and parts of myocardium).
Secrete norepinephrine
Increases heart rate, Strengthens force of myocardial contraction
Parasympathetic neurons
Axons exit in the vagus nerve (C N X) to innervate the S A and A V nodes.
Secretes acetylcholine, Slows heart rate
Blood Vessels
closed system of tubes carrying blood from the heart to tissue cells and back to the heart.
Arteries, Capillaries, Veins
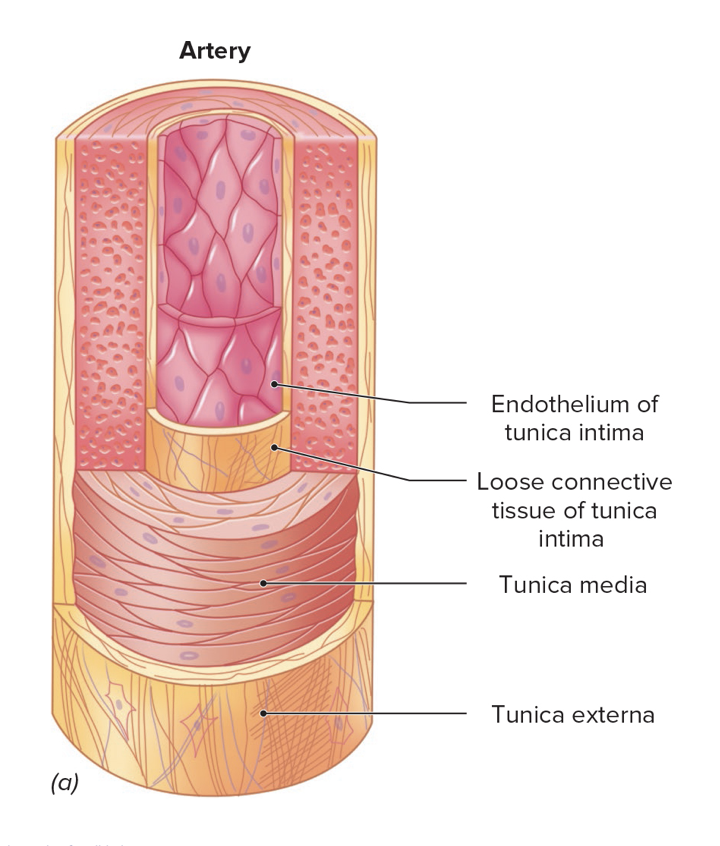
Tunica externa
Outermost layer
Dense irregular connective tissue
Provides support and elasticity
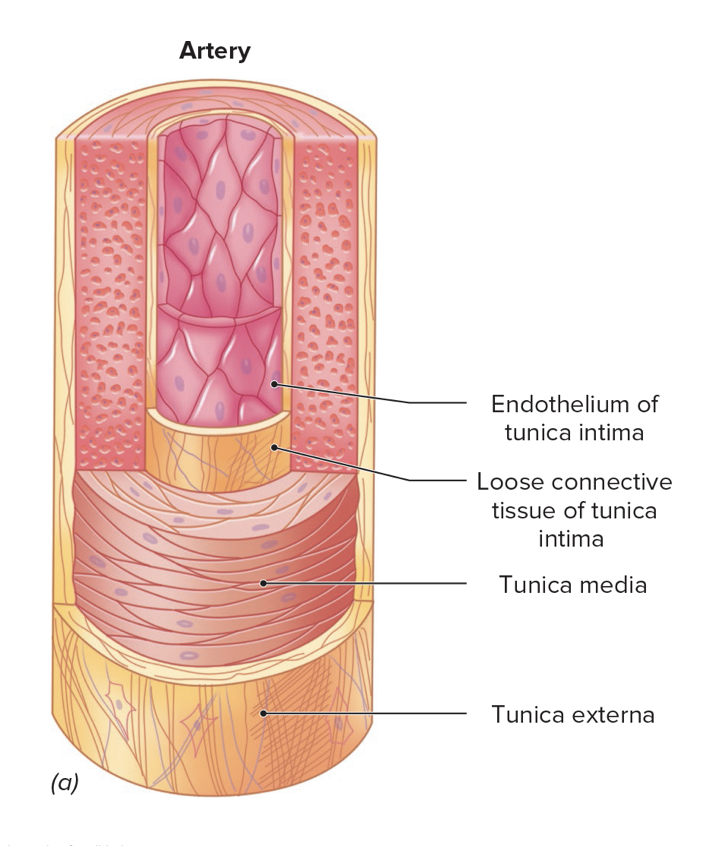
Tunica media
Middle layer
Smooth muscle fibers
Supports the vessel
Causes changes in blood vessel diameter
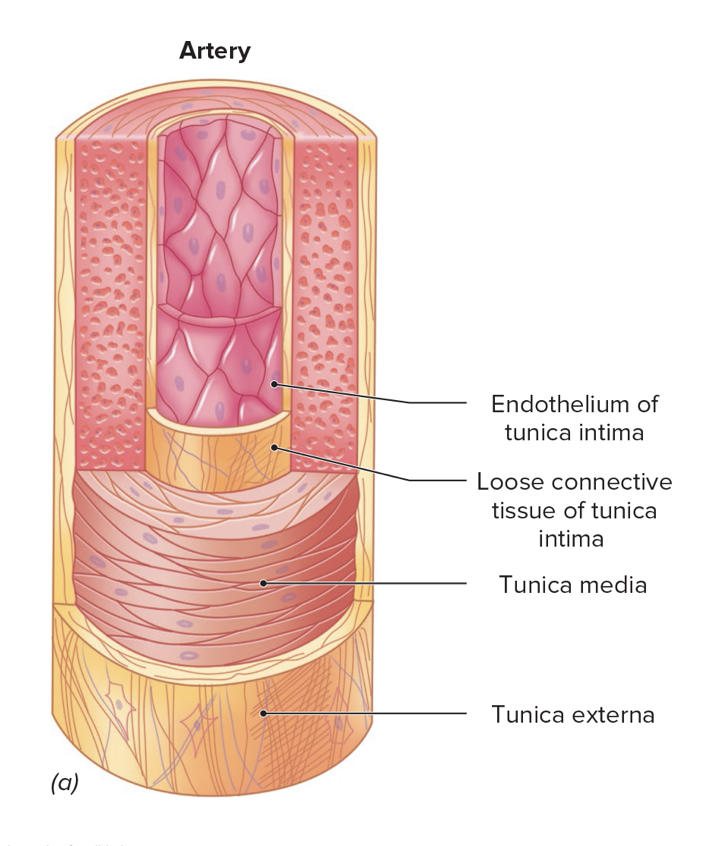
Tunica intima
Deepest layer
Internal lining of a blood vessel.
Consists of endothelium supported by areolar connective tissue
capillary
transfer oxygenated blood from arteries to veins
Most numerous and smallest vessels
Walls contain only tunica intima.
Precapillary sphincters
regulate blood flow into capillaries.
Sphincter contraction inhibits blood flow.
Sphincter relaxation allows blood flow.
Osmotic pressure
Due to plasma proteins in blood
Promotes reabsorption
“Pulls” fluid from interstitial fluid into blood by osmosis
Blood pressure
Promotes filtration
“Pushes” fluid out of blood capillaries and into interstitial fluid
Venules
unite to form larger veins, which in turn unite to form even larger veins.
vein
Reducing venous volume can compensate for blood loss or increase in muscle activity:
Sympathetic part sends action potentials that trigger contraction of venous smooth muscle.
Reduces venous volume
Increases blood volume and pressure in heart, arteries, and capillaries
Blood pressure
The force of blood against the wall of blood vessels
Usually refers to arterial blood pressure in the systemic circuit
Systolic blood pressure:
Highest pressure during ventricular systole
Diastolic blood pressure
Lowest pressure during ventricular diastole
Pulse pressure
the difference between systolic and diastolic blood pressures.
Causes the pulse
Expansion and contraction of arterial walls
vasoconstriction
An increase in the frequency of sympathetic action potentials
Increases resistance.
Increases blood pressure and blood velocity.
Accelerates O2 and CO2 transport rates.
vasodilation
A decrease in the frequency of sympathetic action potentials
Decreases resistance
Decreases blood pressure and velocity