Chapter 15 Physiology
1/147
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
148 Terms
Blood vessels operate under a _ system
closed
(this means blood does not leave the heart or vessels)
Vessels get progressively _ layers as they progress
less
(arteries have more layers than arterioles, and arterioles have more layers than capillaries, etc)
Layers in the capillary
endothelium
basement membrane
Layers in the arteriole
endothelium
basement membrane
high levels of smooth muscle
Layers in the venule
endothelium
basement membrane
moderate levels of smooth muscle
Layers in the muscular artery
endothelium
basement membrane
high levels of smooth muscle
Elastic connective tissue
All vessels, instead of capillaries, have some amount of _ in them. Muscular arteries and arterioles have a lot of it.
smooth muscle
endothelium
innermost
thin layer of cells
nonstick
do much more than just letting the blood flow
smooth muscle regulates
blood vessel diameter
how does smooth muscle regulate diameter?
vasodilation, if the blood vessel increases in diameter,
vasoconstriction, if it narrows down in diameter.
connective tissue; two types
Elastic
Fibrous
Elastic artery function
also they are also called pressure reservoirs
stretch aorta in response to pressure
arterioles feed blood to the capillaries and are known as resistance vessels because
they have the most smooth muscle and can alter diameter the most
Vasoconstriction _ the resistance by the tube narrowing down and therefore blood pressure _.
increases; increases
Vasodilation _ the resistance and blood pressure because now the tube is wider.
decreases
Capillaries are fit to exchange nutrients for two reasons:
Capillary walls are thin (single cell layer thick)
Capillary walls contain pores
Capillaries form _ at tissue
beds
Flow of blood in capillaries is controlled in two ways:
using the metarteriole and the capillary sphincters.
Microcirculation refers to which vessels?
The arterioles, capillaries, and venules
Metarterioles structure (see image)
branch off of arterioles, ends at the venule
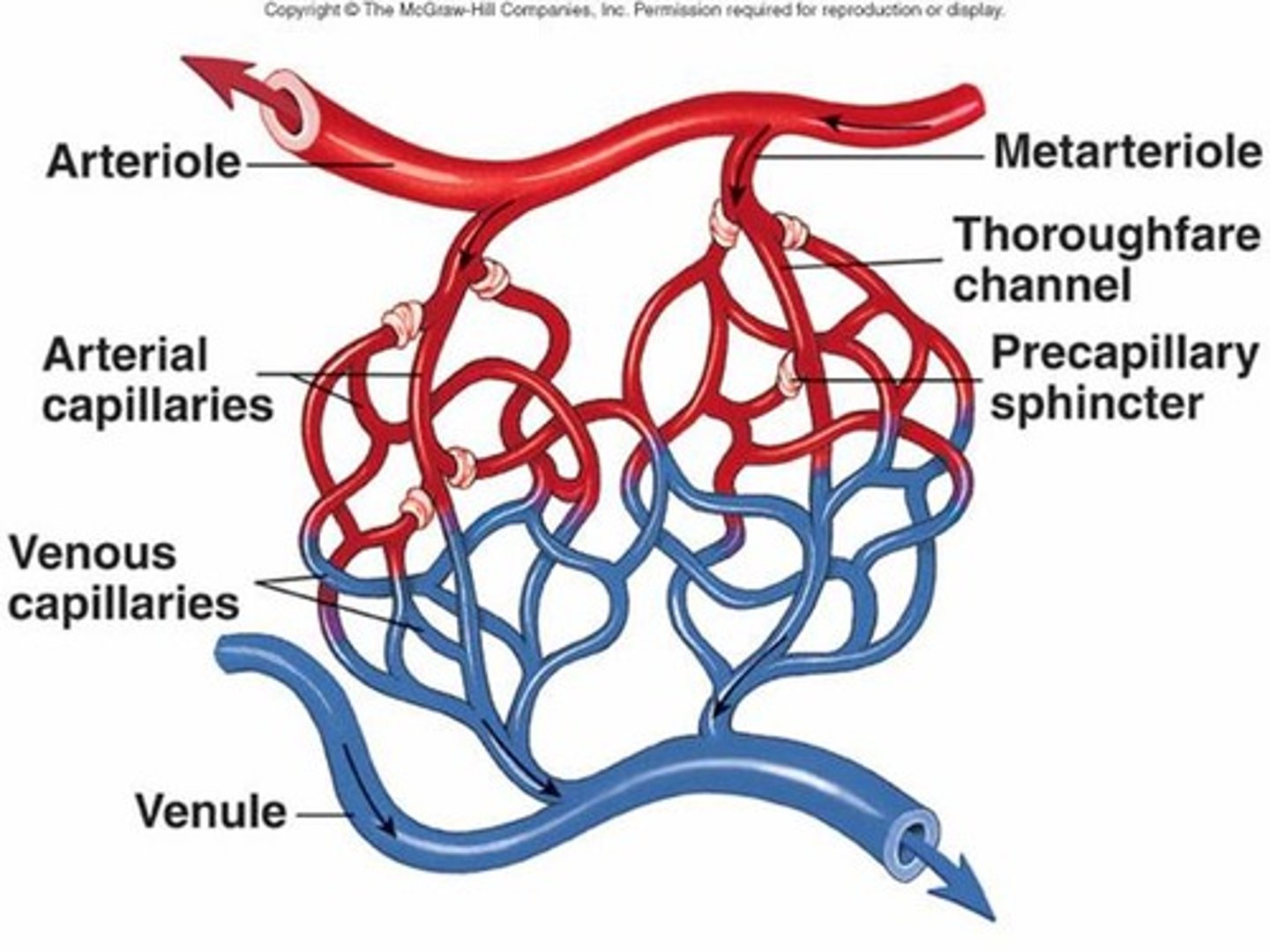
Metarteriole blood flow is controlled by
precapillary sphincters
precapillary sphincters can relax or contract. When they are relaxed,
blood will flow to the capillary bed, where nutrients can be exchanged
(then to the venule, then back to the heart)
When precapillary sphincters are contracted, blood
cannot go to the capillary bed, it passes on through directly to the venule
(in the image, the white part indicates NO blood flow)
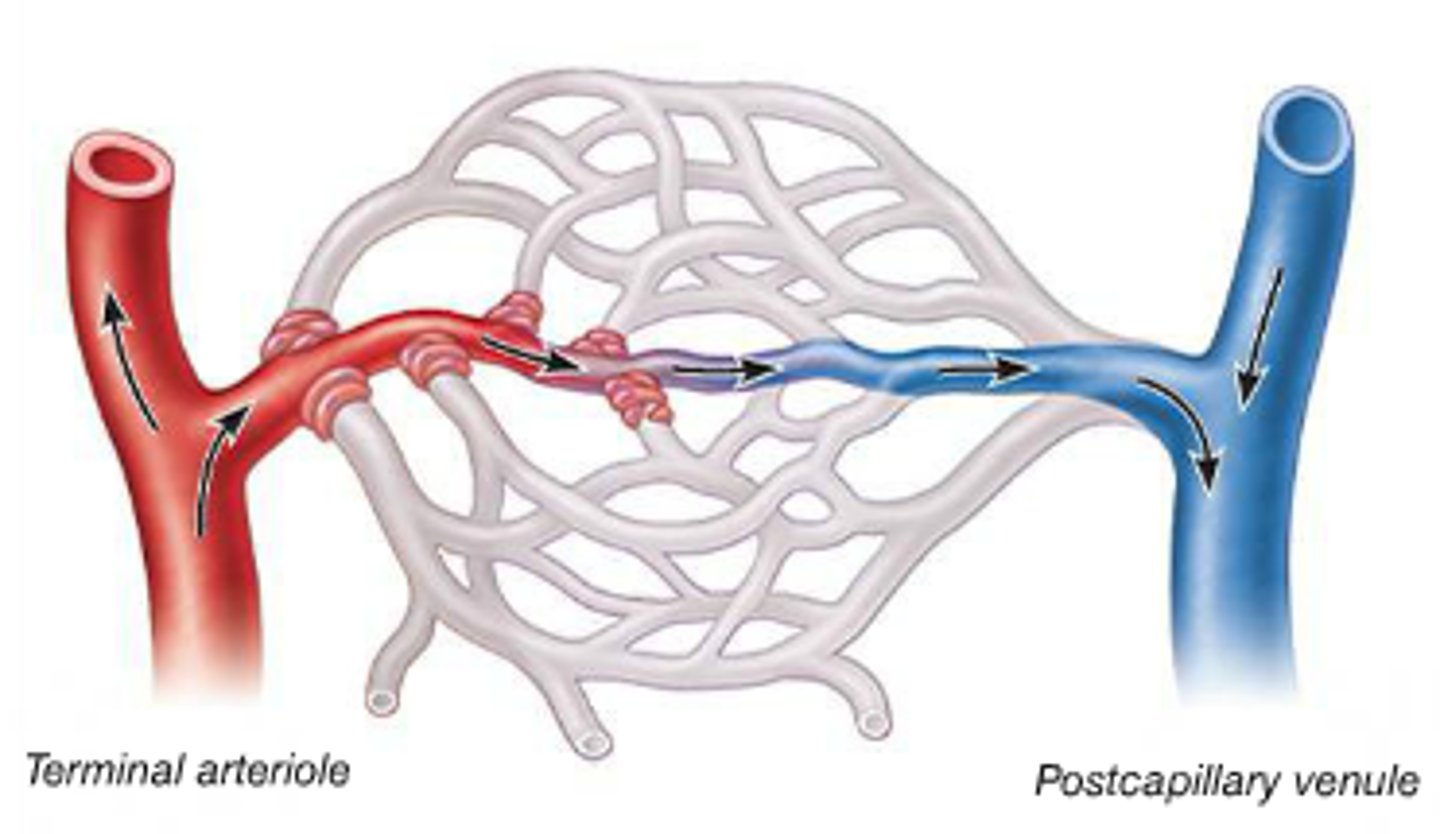
Example of precapillary sphincters contracting and relaxing (teacher example)
Let's take the skeletal muscle contracting. Now, during exercise, the requirement for glucose, oxygen, etc. is increased in the skeletal muscle. So, what happens in the skeletal muscle is the precapillary sphincter is relaxed and the muscle tissue is able to get a lot of blood supply. Now, because the amount of blood that is in the body is fixed, you need to remove blood from some other organ system, and bypass or shunted to the skeletal muscle. So the precapillary sphincters in the digestive system in this case will be contracted. That is why the blood bypasses the GI tract and gets straight back to the heart and feeding that muscle that is requiring extra supply.
Three types of capillaries
Continuous
Fenestrated
Sinusoids
the primary difference in the Three types of capillaries is that they have different
permeabilities
in Continuous capillaries, cells form a _ and are interrupted by some _
continuous layer; intercellular clefts
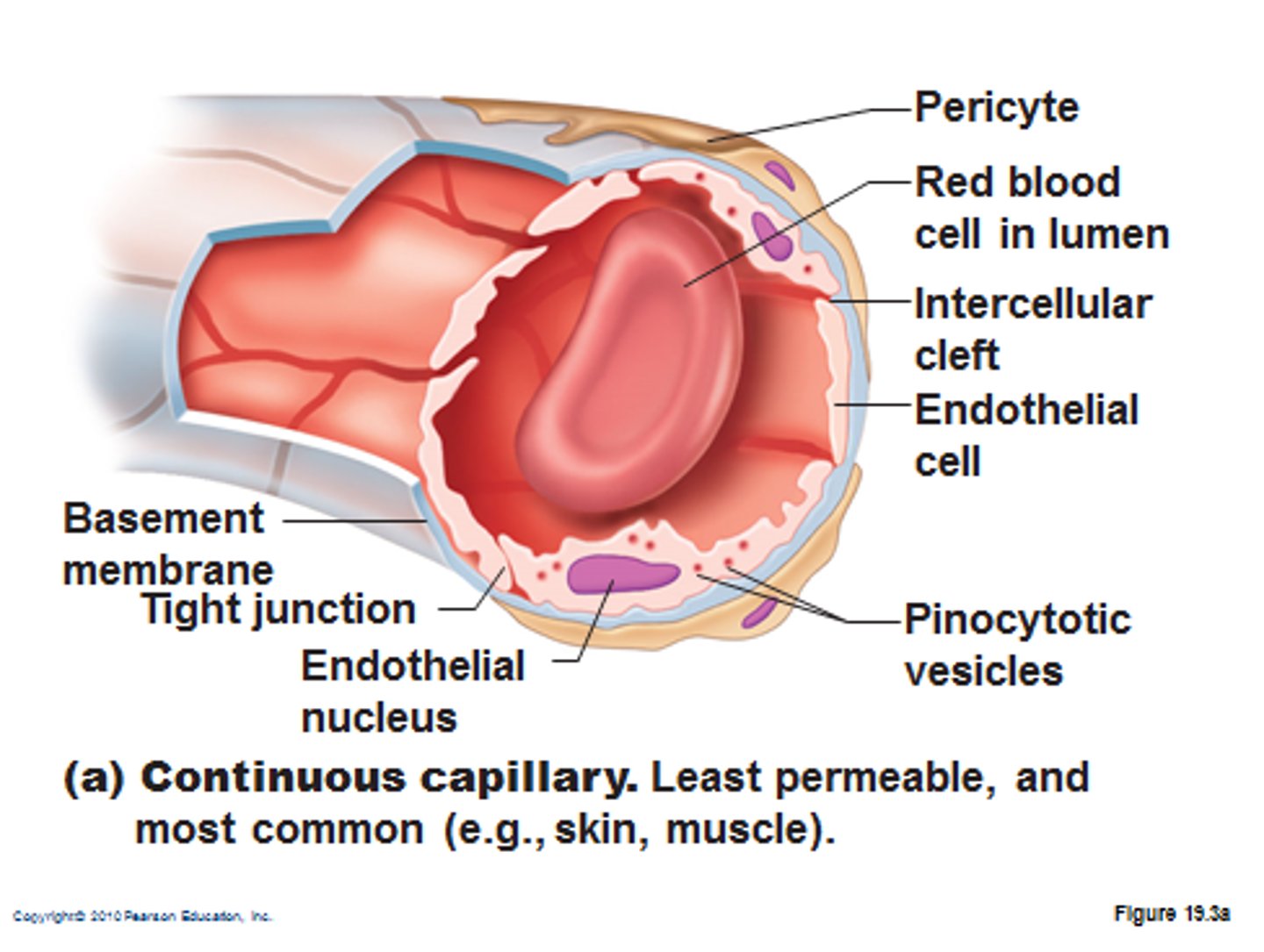
Fenestrated capillaries contain
pores called fenestrations
Fenestrated capillaries have _ than continuous
higher permeability
Fenestrated capillaries main locations
kidneys, small intestine, endocrine organs
Sinusoids structure
wider and more winding
Sinusoids have unusually large
fenestrations
Sinusoids location
bone marrow, spleen, liver
Sinusoids are permeable to
proteins and cells
Veins are helped by a system of
valves and pumps
veins and venules are termed as _ because about _ of the blood when a person is at rest
blood reservoirs; 65%
REVIEW:
arteries are called as _, arterioles are called as _, and venules and veins are called as _.
pressure reservoirs; resistance vessels; blood reservoirs
Which blood vessels drain blood from capillaries
venules
Primary method of capillary exchange
diffusion
diffusion does not need
energy
Substances that are easily exchanged in diffusion
Gases
fluids
nutrients (such as glucose)
Larger substances in capillaries are transported via
transcytosis
Bulk flow is a _ process
passive
bulk flow moves large volumes of solutes and fluid moved in the
same direction
For filtration and absorption, the reference point is the
capillary
Bulk movement from capillaries into interstitial fluid is
Filtration
Bulk movement from interstitial fluid into capillaries is
Absorption
Starling forces determine the
direction of flow
starling forces include
capillary hydrostatic pressure,
interstitial fluid hydrostatic pressure,
plasma colloid osmotic pressure, and
interstitial fluid colloid osmotic pressure
starling forces
Main Function of the lymphatic system
picks up EXCESS FLUID filtered by the capillaries
Misc functions of the lymphatic system
Returns filtered plasma proteins back to the blood
Carries out immune responses
transporting dietary lipids
fluid inside the lymphatic vessels is referred to as
lymph
lymphatic vessels will begin as
capillaries
NOT BLOOD CAPILLARIES; they start as lymphatic capillaries
lymphatic capillaries are closed
at one end
(contrast this to blood capillaries, which have two ends)
Lymph drainage is done through a _ network that runs excess fluid back to the cardiovascular system
parallel
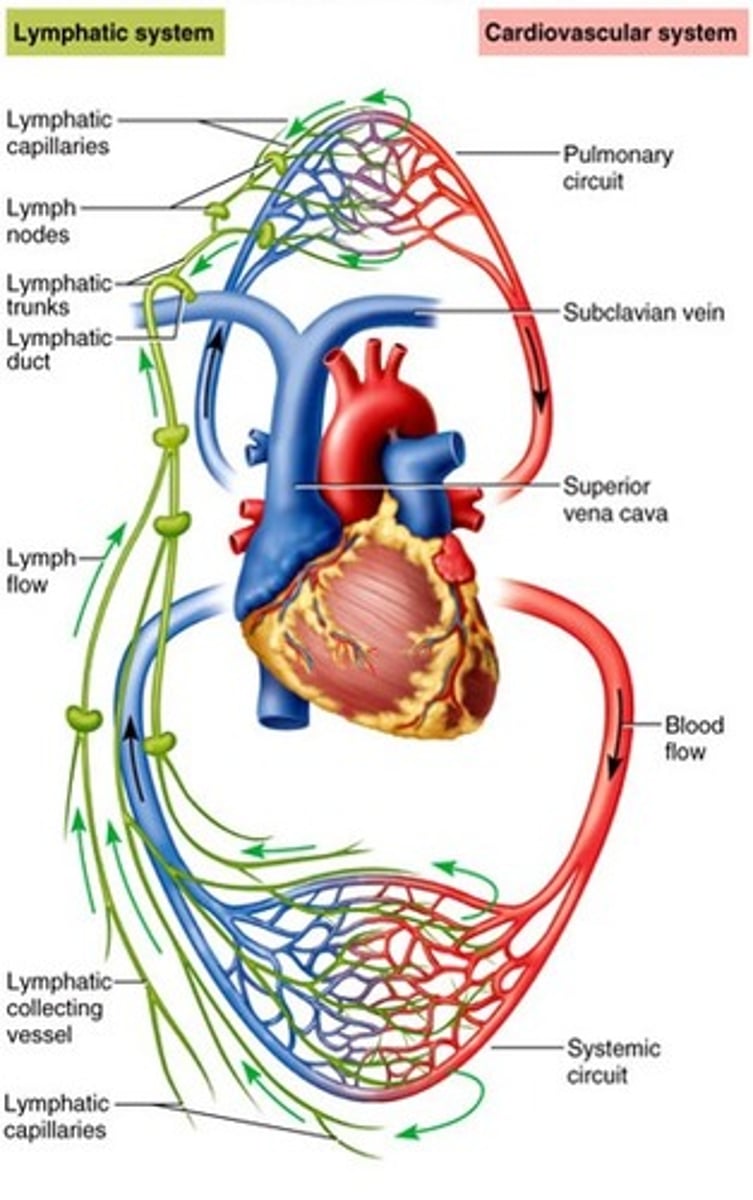
Definition of blood flow
volume of blood that flows through the tissue at any given time
two factors that will impact blood flow
pressure gradient
resistance
Blood flow equation
F = ΔP/R
F is blood flow
ΔP is pressure gradient
R is resistance to blood flow
Based off the blood flow equation, flow is directly proportional to the _ and inversely proportional to the _ offered.
pressure gradient; resistance
Resistance is the opposition to
blood flow
All of the resistances of the vessels is referred to as
total peripheral resistance (TPR)
total peripheral resistance (TPR) equation
Need to know equation so you know if, say, a certain value, like blood viscosity, increased, would TPR increase or decrease? By how much? Exponentially or not?

Laminar
No noise and the inner sides of the tubes are uniform and smooth
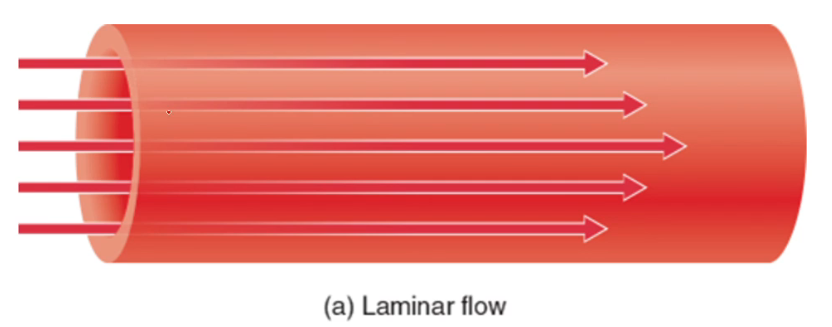
turbulent flow
creates sound, insides of the tube are not uniform, then it creates turbulence and it is called as turbulent flow.
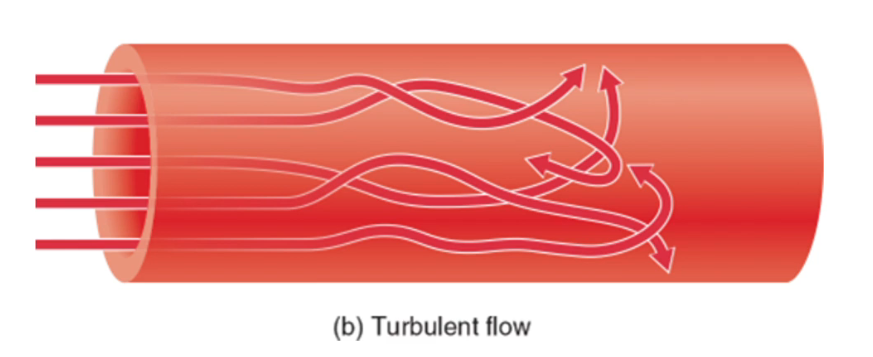
Which flow used to measure blood pressure
turbulent flow
(b/c it creates sound)

and is the _ measured pressure in the system
highest

and is the _ measured pressure in the system
lowest

MAP drives

Graph of MAP: See avg pressure, and how pressure changes depending on vessels
avg is 90 millimeters mercury pressure, pressure is highest in the aorta and decreases when going to arterioles, capillaries, venules, and veins
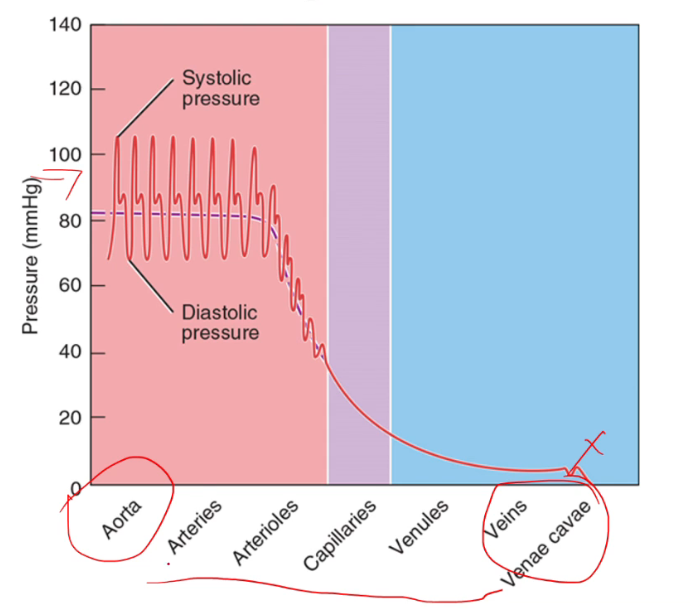
Maximum drop in blood pressure occurs in the
arterioles
(b/c of smooth muscle that controls the diameter; see last flashcard)
MAP =
Cardiac output (CO) * Total peripheral resistance (TPR)
Modified MAP equation
MAP = Heart rate * Stroke volume * TPR
Vessel compliance
measure of the ability for a hollow object to stretch
Vessel compliance equation

Veins have high compliance so they can _, whereas arteries have less compliance.
easily expand
Venous return (blood coming back to the heart) is largely determined by the
venous pressure gradient
mechanisms that are also responsible for venous return
(maybe not as prominent as the venous pressure gradient, but still need to know)
the valves in the veins, the skeletal muscle pump, vasoconstriction, and the respiratory pump
Blood flow is dependent on _

Blood flow from organ to organ _
varies
When flow of blood is parallel,
flow of blood to an organ does not affect flow of blood to other organs
(e.g. flow to the kidney does not affect flow of blood to the heart)
Baseline for constriction and dilation
Vascular tone
Vascular tone can be _ based off of _ or _ factors
changed; intrinsic; extrinsic
Examples of intrinsic factors

Examples of extrinsic factors

Metabolic control and hyperemia refers to
blood flow to a specific tissue is increased (hyperemia) to meet elevated metabolic demands or compensate for a temporary lack of oxygen
Definition of shock

4 types of shock

Hypovolemic shock
reduced volume of blood
Hypovolemic shock usually happens after a
hemorrhage
Cardiogenic shock
Heart is not able to pump
(therefore less delivery of blood to tissues)
in vascular shock, blood vessels undergo massive
vasodilation
massive vasodilation causes sudden drops of
pressure and delivery of materials is not possible
obstructive shock
something wrong obstructing the flow of blood
Homeostatic response to shock:
_ of the renin-angiotensin-aldosterone system
activation
Homeostatic response to shock:
Secretion of
antidiuretic hormone
Homeostatic response to shock:
activation of the _ division of the ANS
sympathetic
Homeostatic response to shock:
Release of
local vasodilators
Unlike arterioles in most tissues of the body, the arterioles in the heart and skeletal muscle have an abundance of
β2-adrenergic receptors (beta receptors)
Activation of the β2 receptors causes
arterioles to vasodilate