PATH FINAL From review stuff
1/265
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
266 Terms
Atrophy
↓ cell SIZE — cells shrink due to decreased workload, ischemia, denervation, or loss of hormonal stimulation
Hypertrophy
↑ cell SIZE — cells grow larger in response to increased workload; common in non-dividing cells (e.g., cardiac muscle)
Hyperplasia
↑ cell NUMBER — occurs in cells capable of division; driven by growth factor signaling
Metaplasia
REVERSIBLE switch from one differentiated cell type to another; can progress to dysplasia if stimulus persists
Dysplasia
DISORDERED GROWTH — abnormal cell size, shape, and organization; NOT a normal adaptive response; pre-malignant
Hyperplasia vs. Hypertrophy
Hyperplasia = ↑ number (mitosis);
Hypertrophy = ↑ size (no new cells); can occur together (e.g., pregnant uterus)
Endometrial Hyperplasia
Caused by ↑ unopposed estrogen (e.g., anovulatory cycles); excess estrogen drives endometrial cell proliferation
BPH (Benign Prostatic Hyperplasia)
Driven by DHT (dihydrotestosterone); does NOT progress to prostate cancer
Barrett's Esophagus
Chronic acid reflux:
normal stratified squamous epithelium → non-ciliated columnar epithelium; ↑ risk of adenocarcinoma
Smoker's Metaplasia
Normal respiratory pseudostratified ciliated columnar →
stratified squamous epithelium;
caused by chronic irritation
Cervical Intraepithelial Neoplasia (CIN)
Classic dysplasia; caused by HPV 16 & 18; disordered/pre-malignant growth — NOT a normal adaptive response
Reversible Injury — ATP Depletion
Mild to moderate;
Na/K-ATPase fails → intracellular Na+ ↑ → water influx →
cell swelling (hydropic change)
Irreversible Injury — ATP Depletion
Severe and prolonged; ion pump failure becomes irreversible → membrane rupture → cell death
Reversible Injury — Cell Membrane
Integrity maintained; plasma membrane intact (blebs may form but no rupture)
Irreversible Injury — Cell Membrane
LOST — plasma membrane ruptures → contents leak → triggers inflammation
Reversible Injury — Mitochondria
Swelling only; outer membrane intact; cytochrome c NOT released
Irreversible Injury — Mitochondria
Severe damage + membrane rupture; cytochrome c released → triggers apoptosis cascade; large flocculent densities form
Reversible Injury — Nuclear Changes
No significant change to nucleus
Irreversible Injury — Nuclear Changes
3 patterns:
1. pyknosis: condensed/dark
2. karyorrhexis: fragmented
3. karyolysis: dissolved
Pyknosis
Nuclear shrinkage and increased basophilia (dark, shrunken nucleus);
first nuclear sign of irreversible injury
Karyorrhexis
Nuclear fragmentation — chromatin breaks into scattered pieces; seen in irreversible injury/necrosis
Karyolysis
Nuclear dissolution/fading — DNA digested by DNases; seen in late necrosis
Reversible Injury — Fatty Change
Seen especially in liver; reversible if insult removed before membrane rupture
Reversible Injury — Outcome
Full recovery possible if insult removed in time
Irreversible Injury — Outcome
Cell death — either necrosis or apoptosis depending on mechanism
Reversible Injury — ER
ER swelling; dispersion of ribosomes → ↓ protein synthesis
Reversible Injury — Lysosomes
Autophagy by lysosomes (recycling damaged organelles); no rupture yet
Irreversible Injury — Lysosomes
Rupture of lysosomes → autolysis (lysosomal enzymes digest cell from within)
Irreversible Injury — ER
Complete lysis of ER
Myelin Figure
Whorls of phospholipids from damaged cell membranes; seen in both reversible injury and early necrosis
Necrosis — Cause
Always PATHOLOGICAL; caused by external insult (ischemia, toxins, infection)
Apoptosis — Cause
May be PHYSIOLOGICAL (embryogenesis, immune deletion) OR pathological (DNA damage, viral infection)
Necrosis — Scope
Affects adjacent GROUPS of cells simultaneously
Apoptosis — Scope
Affects SINGLE cells; scattered pattern
Necrosis — Cell Size
INCREASED — cell swells due to ion pump failure and water influx
Apoptosis — Cell Size
SHRUNKEN — cytoplasm and nucleus condense
Necrosis — Process
PASSIVE — uncontrolled, energy-independent
Apoptosis — Process
ACTIVE — energy-dependent; requires ATP; executed by caspases
Necrosis — Inflammation
CAUSES inflammatory reaction — DAMPs released from ruptured membrane trigger innate immunity
Apoptosis — Inflammation
NO inflammatory reaction — apoptotic bodies cleanly phagocytosed; membrane stays intact
Necrosis — Plasma Membrane
DISRUPTED — membrane ruptures and contents spill
Apoptosis — Plasma Membrane
INTACT — blebs form but membrane stays sealed; contents packaged into apoptotic bodies
Apoptosis — Key Steps
Chromatin condensation → membrane blebbing → cellular fragmentation → apoptotic bodies → phagocytosis by macrophages
Coagulative Necrosis
Architecture PRESERVED (ghost outlines of dead cells); caused by ischemia to all solid organs EXCEPT CNS; also thermal injury
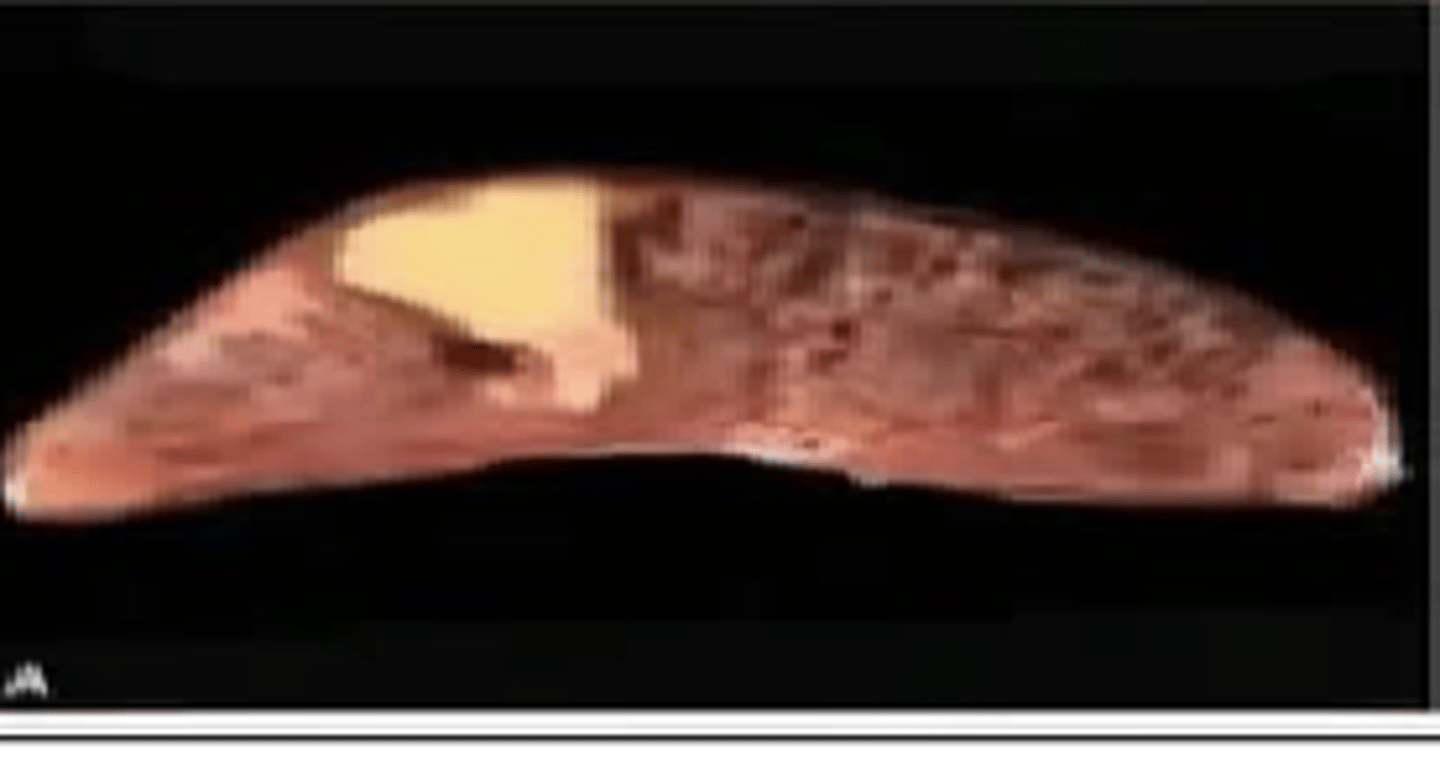
Zenker's Degeneration
Coagulative necrosis of the rectus abdominis muscle; seen in severe systemic infections (e.g., typhoid fever)
Liquefactive Necrosis
Tissue completely digested → liquid/pus; caused by ischemia to the BRAIN or bacterial infections (wet gangrene)
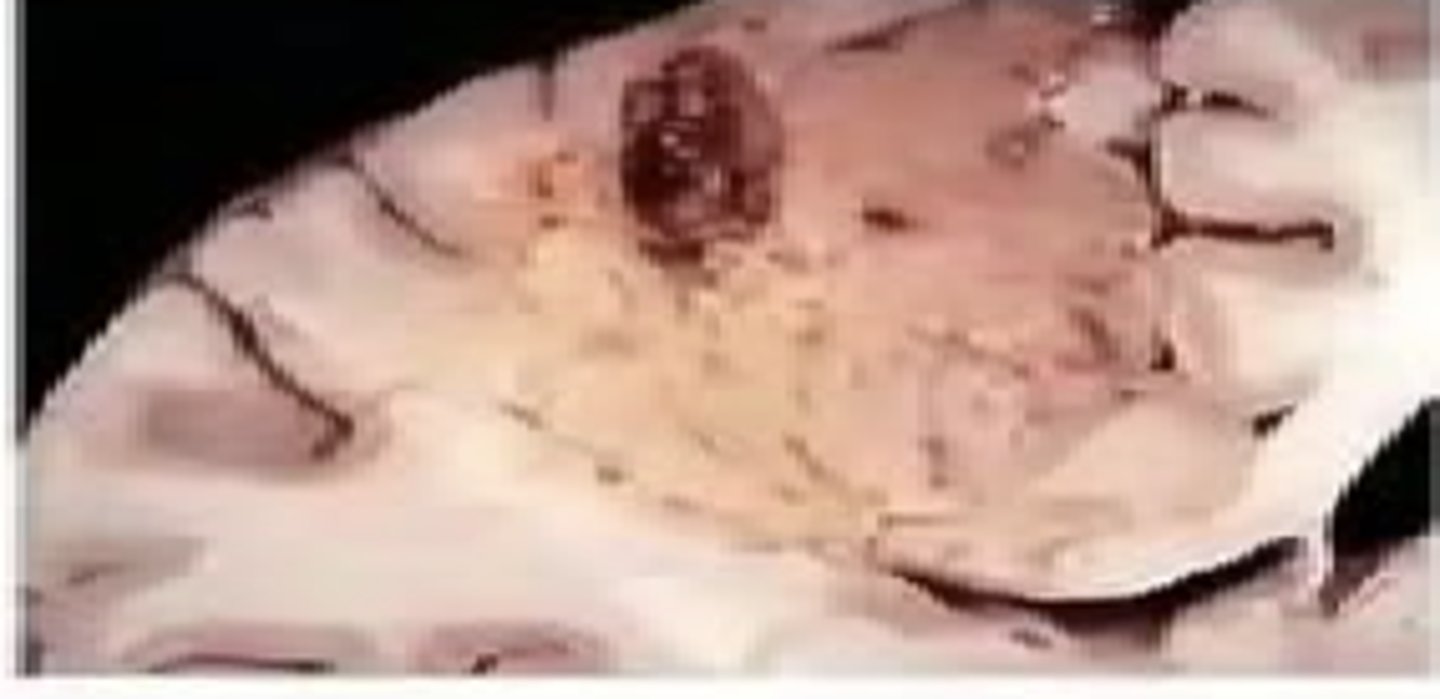
Liquefactive Necrosis — Brain Exception
Brain undergoes liquefactive (not coagulative) necrosis due to high lipid content and abundant hydrolytic enzymes
Caseous Necrosis
"Cheese-like" gross appearance; combo of coagulative + liquefactive; surrounded by granuloma; seen in TB, syphilis, histoplasmosis

Caseous Necrosis — Organisms
TB (Mycobacterium tuberculosis), Syphilis (Treponema pallidum), Histoplasma capsulatum
Fat Necrosis — Traumatic
Direct trauma to fat-containing tissue (breast, buttock, abdomen) → fat cell destruction
Fat Necrosis — Enzymatic
Pancreatitis → pancreatic lipases released → fatty acids + Ca²⁺ → calcium soaps (saponification); chalky-white deposits grossly

Fibrinoid Necrosis
Seen in VESSEL WALLS only; fibrin-like material deposited in walls; causes: vasculitis, malignant hypertension, immune complex deposition
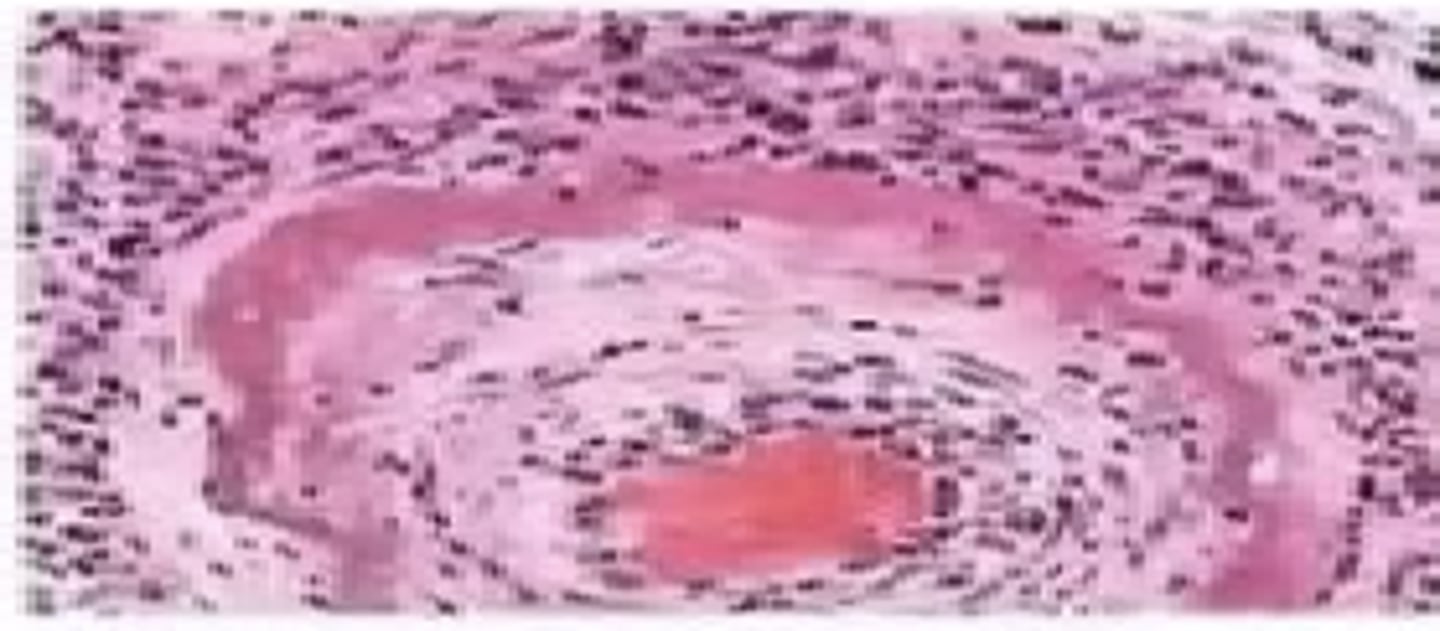
Coagulative vs. Liquefactive
Coagulative = architecture preserved, solid organs (not CNS);
Liquefactive = architecture destroyed, brain + bacterial infections
Caseous vs. Coagulative
Caseous = no architecture + "cheesy" + granuloma; Coagulative = ghost cells preserved, no granuloma
Transudate — Protein Content
Low (<2.5-3.0 g/dL); ultrafiltrate with little protein
Exudate — Protein Content
High (>2.5-3.0 g/dL); protein-rich due to ↑ vascular permeability
Transudate — Specific Gravity
<1.012
Exudate — Specific Gravity
>1.020
Transudate — LDH
Low
Exudate — LDH
High
Transudate — Appearance
Clear and watery
Exudate — Appearance
Cloudy/turbid; may be yellow or purulent
Transudate — Cellularity
Few cells; mostly mononuclear
Exudate — Cellularity
Many cells; neutrophils and macrophages predominate
Transudate — Mechanism
↑ Hydrostatic pressure OR ↓ oncotic pressure; no inflammation involved
Exudate — Mechanism
↑ Vascular permeability from inflammation → proteins and cells leak out
Transudate — Common Causes
CHF, nephrotic syndrome, liver cirrhosis
Exudate — Common Causes
Infection (e.g., pneumonia), inflammation, malignancy
Edema — Increased Hydrostatic Pressure
Impaired venous return: CHF, constrictive pericarditis, cirrhosis, venous thrombosis, external compression
Edema — Arteriolar Dilation
Heat or neurohumoral dysregulation → ↑ capillary pressure → fluid leaks out
Edema — Reduced Plasma Osmotic Pressure
Hypoproteinemia: nephrotic syndrome, liver cirrhosis, malnutrition, protein-losing gastroenteropathy
Edema — Lymphatic Obstruction
Blocked lymph drainage: inflammatory, neoplastic, postsurgical, or postirradiation causes
Edema — Sodium Retention
Excessive salt intake with renal insufficiency OR ↑ tubular reabsorption via RAAS activation
Edema — Inflammation
Acute/chronic inflammation → ↑ vascular permeability → fluid accumulates in tissue
Leukocyte Extravasation — Step 1: Margination & Rolling
Selectins (E-selectin, P-selectin on endothelium) bind sialyl-Lewis X on leukocytes; loose, reversible adhesion
Leukocyte Extravasation — Step 2: Adhesion
Integrins (CD18/LFA-1, Mac-1) on leukocytes bind ICAM-1/VCAM-1 on endothelium; firm, irreversible binding
Leukocyte Extravasation — Step 3: Diapedesis
Leukocytes squeeze through endothelium via PECAM-1 (CD31) at postcapillary venules
Leukocyte Extravasation — Step 4: Chemotaxis
Migration toward injury guided by C5a, IL-8, LTB4, and bacterial products
Selectins — Role
E-selectin and P-selectin on endothelium mediate rolling; rapidly expressed after TNF/IL-1 stimulation
Integrins — Role
CD18/LFA-1 and Mac-1 bind ICAM/VCAM; mediate firm adhesion (upregulated by TNF, IL-1)
PECAM-1 (CD31)
Mediates diapedesis — leukocytes transmigrate through interendothelial junctions at postcapillary venules
Chemotaxis — Key Mediators
C5a, IL-8 (CXCL8), LTB4, and bacterial products (e.g., fMLP)
Rubor (Redness)
Vasodilation → ↑ blood flow; mediators: Histamine, PGE₂, PGI₂, NO
Calor (Heat)
Vasodilation + ↑ blood flow → local temperature rise; mediators: Histamine, Prostaglandins, NO
Tumor (Swelling)
↑ Vascular permeability → exudate into tissue; mediators: Histamine, Bradykinin, LTC₄, LTD₄
Dolor (Pain)
Direct nerve stimulation; mediators: Bradykinin, PGE₂, IL-1, TNF-α
Functio Laesa (Loss of Function)
Combination of pain, swelling, and tissue damage; indirect result of all inflammatory mediators
Arachidonic Acid — Source
Released from cell membrane phospholipids by phospholipases; blocked upstream by corticosteroids
Arachidonic Acid — COX Pathway
Cyclooxygenase → PGG₂ → PGH₂ → PGI₂, TXA₂, PGD₂, PGE₂; blocked by aspirin/NSAIDs
Arachidonic Acid — 5-LOX Pathway
5-Lipoxygenase →
LTB4 (chemotaxis)
LTC₄, LTD₄, LTE₄ (bronchoconstriction, ↑ permeability)
Prostacyclin (PGI₂)
Vasodilation + inhibits platelet aggregation; produced by endothelium
Thromboxane A₂ (TXA₂)
Vasoconstriction + promotes platelet aggregation; produced by platelets
PGD₂ / PGE₂
Vasodilation, ↑ vascular permeability, leukocyte chemotaxis
LTB4
Potent neutrophil chemotactic agent; via 5-lipoxygenase pathway
LTC₄, LTD₄, LTE₄
Cysteinyl leukotrienes → bronchospasm + ↑ vascular permeability; blocked by montelukast
Lipoxins (LXA₄, LXB₄)
Via 12-lipoxygenase;
1. inhibit neutrophil adhesion
2. chemotaxis — pro-resolution mediators
Steroids — Mechanism
Inhibit phospholipases → block arachidonic acid release →
suppress both COX and LOX pathways
NSAIDs/Aspirin — Mechanism
Inhibit COX-1 and COX-2 → block prostaglandin/thromboxane synthesis;
do NOT block leukotriene pathway
Acute Inflammation — Key Features
Vascular changes, neutrophil recruitment, mediator release; caused by infarction, infection, toxins, trauma
Acute Inflammation — Resolution
Clearance of stimulus + mediators + inflammatory cells → injured cells replaced → normal function restored