MALE Reproductive system - slides
1/44
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
45 Terms
Somatic cells
also known as diploid cells (2n)
23 chromosomes (homologous pairs-very similar)
22 autosomes & 1 pair of sex chromosomes
XX and XY
in males sex cells are not homologous
in females all homologous
Gametes
also known as haploid cells (n)
single set of chromosomes
produced by special type of division: meiosis
siter chromatids
are identical
Meiosis
sexual reproduction
reduce chromosome number by half ( 2n → n)
2 stages- Meiosis I and II
Diploid- 2N (homologous chromosomes(pair)
Haploid - N
DNA synthesis
occurs in S phase of interphase
During prophase I
synapsis of homologous chromosomes
cross over
During metaphase I
homologous chromosomes line up at the metaphase plate
During metaphase II
sister chromatids line up at the metaphase plate
Outcome of Meiosis
Four haploid cells at the end of meiosis II
Gonads
testes
System of ducts
epididymis
ductus deferens
ejaculatory duct
urethra
Accessory sex glands
seminal vesicles
prostate
bulbourethral glands
Supporting structures
scrotum
penis
Scrotum
support structure for testes
sac of loose skin, fascia & smooth muscle divided into 2 pouches by septum
Raphe a ridge running along the midline.
Scrotum muscles
cremaster (smooth muscle) and Dartos (smooth)
regulate position of testes and temperature for optimal sperm production.
cold/arousal: contract
hot: relax
testes are located outside of the body (regulate temp, external position keeps them 2-3 degrees lower than core body temp)
Testes
paired, oval glands in the scrotum
surrounded by two tunics
tunica albuginea (inner tough layer)
tunica vaginalis (outer)
Mediastinum testis (house rete testis- about 250 lobules)
Seminiferous tubules
¼ tubules per lobe
produce sperm
Seminiferous tubules
Site of sperm production
formed sperm are transferred to epididymis (where sperm matures) and sperm leaves epididymis during ejaculation via the ductus deferens
Cryptorchidism
one or both testes fail to descend normally
about 3% of full term babies
about 30% premature babies
Support cells of the seminiferous tubule
Sertoli cells (sustentacular)
Leydig cells (interstitial)
Sertoli (sustentacular) cells
Somatic cells
form blood-testis barrier (sperms are antigenic)
support, protect & nourish spermatogenic cells
produce fluids
control release of sperm into lumen
secrete inhibin (when sperm production is high)- regulate effects of FSH and testosterone
Leydig (interstitial) cells
arise from dividing stem cells
produce androgens (testosterone)
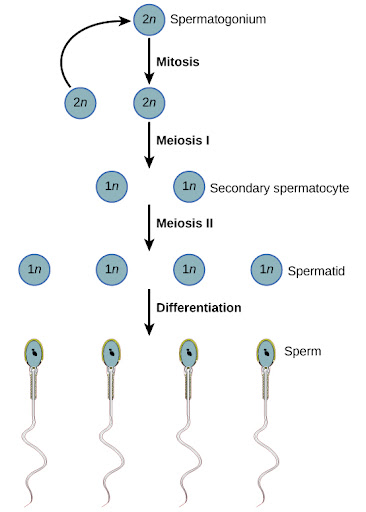
Spermatogenesis
begins at puberty
takes 2.5 months
Stimulated by FSH & LH
Spermatogonia(2n) → Primary Spermatocyte(2n) → Secondary spermatocyte(n) → spermatids(n) → spermatozoa/sperm(n)
Spermiogenesis
spermatids → sperm cells
Spermiation
the release of mature sperm cells from Sertoli cells into the seminiferous tubules
Sperm head
contain 23 chromosomes
DNA
acrosome (hyaluronidase & proteinase enzyme) pushes sperm out
Mid piece of sperm
mitochondria (does not enter egg cell)
Tail (flagellum) of sperm
movement (locomotion)
Sperm production and viability
about 100-300 million sperm produced each day
once ejaculated, sperm remain viable for up to 5 days within the female reproductive tract
Testosterone production
stimulate sperm production (spermatogenesis)
stimulate libido
sex characteristics
Regulation of Testosterone Production
Hypothalamus releases GnRH that stimulates the pituitary gland to release LH and FSH, which in turn promote testosterone production in the testes.
LH release → targets Leydig cells → testosterone release
FSH release → target Sertoli cells → inhibin release (in response to rising sperm count levels)which stops release of FSH → negative feedback of hypothalamus and pituitary → inhibits release of FSH, LH and GnRH
FSH release → target Sertoli cells → androgen binding protein release → testosterone release (ADP binds to testosterone keeping the latter at a high concentration)
Epididymis
store sperm until fully mature
Pathway of sperm flow through Ductus of Testis
seminiferous tubules
straight tubules
rete testis
efferent ducts
epididymis
ductus (vas) deferens
Spermatic cord
ductus deferens
testicular artery
plexus of testicular veins
autonomic nerves
lymphatic vessels
cremaster muscle
Seminal vesicles (accessory glands)
viscous, whitish-yellow, alkaline fluid
fructose, prostaglandins, clotting proteins, seminal plasmin
prostate (accessory gland)
slightly milky fluid, weakly acidic
citric acid, proteolytic enzymes
Bulbourethral or Cowper’s gland
clear, viscous mucin (alkaline)
Accessory glands
seminal vesicles, prostate, bulbourethral glands
Semen
made of sperm and seminal fluid
pH 7.2-7.7
coagulates & reliquefies on ejaculation (clotting factors and fibro myosin)
average ejaculate contains 50-150 million sperm/ml
Sperm analysis
motility
count (normal- 200-500 million sperm/ml)
shape
Penis
Forms external genitalia with scrotum
passageway for semen & urine(urethra)
root: bulb and crus, body, glans penis, prepuce
Body composed of 3 erectile tissue masses filled with blood sinuses
2 corpora cevernosa
1 corpus spongiosum
Erection
Parasympathetic fibers release & cause local production of NO (nitric oxide) → smooth muscle in arterioles to relax and dilate allowing large amounts of blood to enter penis
blood enters penis compressing drainage veins → blood being trapped (retards blood outflow and maintain engorgement)
erectile dysfunction = impotence
Ejaculation
Due to Sympathetic stimulation
muscle contractions close sphincter at base of bladder
move fluids through ductus deferens, seminal vesicle & ejaculatory ducts
contraction of muscles in ischiocavernosus & bulbospongiosus → completes ejaculation(the job)
Men with decreased testosterone levels in the 50s
due to decreased number of interstitial cells
decline more gradually than women’s hormone drop
most men with few symptoms
some with mood swings, decreased sex drive, hot flashes
Prostate enlargement
experienced by most men with age
can interfere with sexual and urinary functions
Erectile dysfunction
inability to achieve or maintain erection
associated with aging, other risk factors
MEN can reproduce until 80-90