Liver & biliary system pathology 3
1/68
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
69 Terms
What are the usual features of a acute bacterial hepatitis?
Degen / necrosis of hepatocytes → inflam
Perioportal inflammation —> bacterial infection from GI tract
septicaemia
Neutrophil dominated
Where is acute hepatitis located in the case of septicaemia?
Inflam in sinusoids
What are the features of an acute hepatitis caused by a viral infection?
Lymphocytic & plasmacytic
Random pattern
What is the most common cause centrolobular hepatitis?
Hypoxia/ischaemia
If no blood supply you won't get inflam
What is being shown in this image
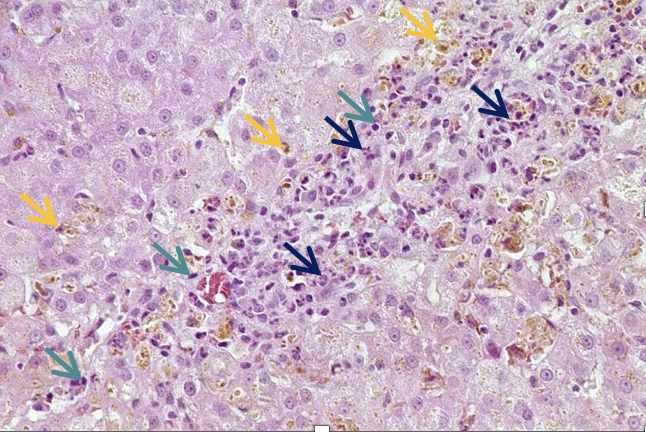
Acute hepatitis
Neutrophils dom = blue arrows
Mononuclear cells
Pigment = bile —> extracellular
bile stasis in caniculi
Lymphos & macros also
What is being shown in this image
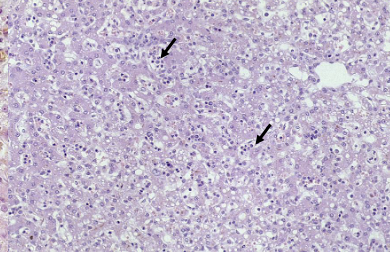
Necrosis during acute hepatitis
Increased leukocytes in sinusoids (diffuse)
What is being shown here?
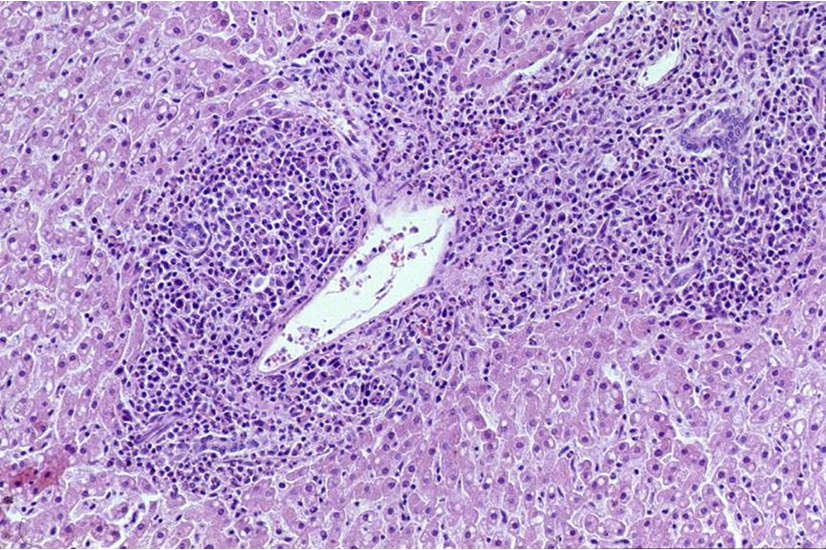
Perioportal inflammation —> in acute hepatitis
leads to restriction of perioportal system
What are the general features of a chronic hepatitis?
Predom. periportal infiltration by lymphocytes and plasma cells
hepatocyte apoptosis/necrosis & some evidence of regen
progressive periportal fibrosis bridging fibrosis
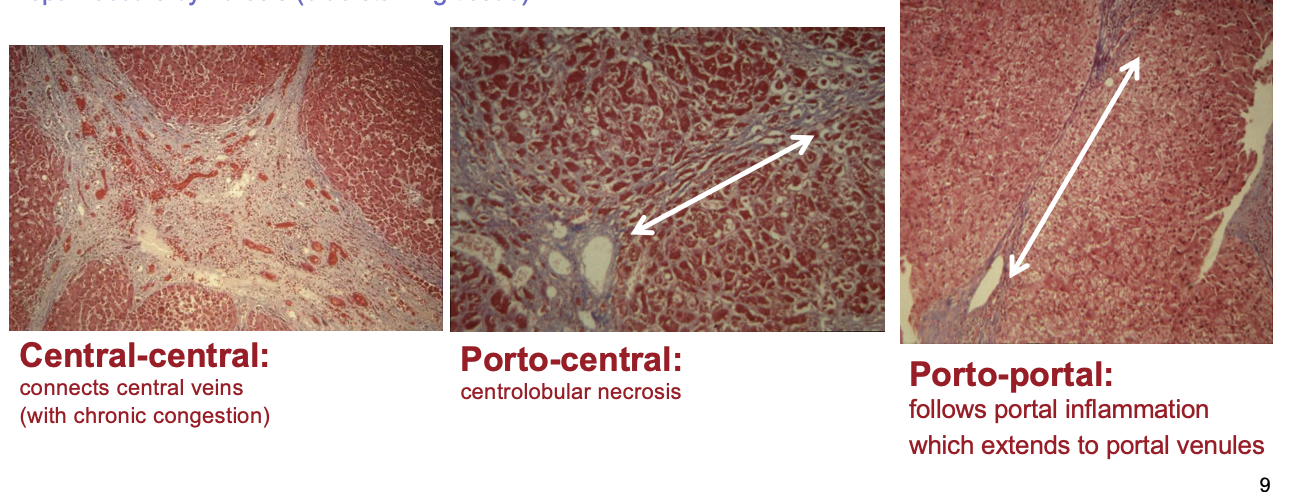
chronic active hepatitis → cirrhosis
necrosis → loss of architecture (reticulin frameworm), fibrosis (blue-staining tissue) & repair
What is chronic active hepatitis?
Seen in certain breeds —> idiopathic not well understood
Doberman hepatitis
Cu accumulation in Bedlington terrier
Determined by quantitiy of inflam & extent of hepatocellular death
More severe maybe
May see neutrophils as well
Can progress to cirrhosis (end stage)
How does chronic hepatitis present histologically?
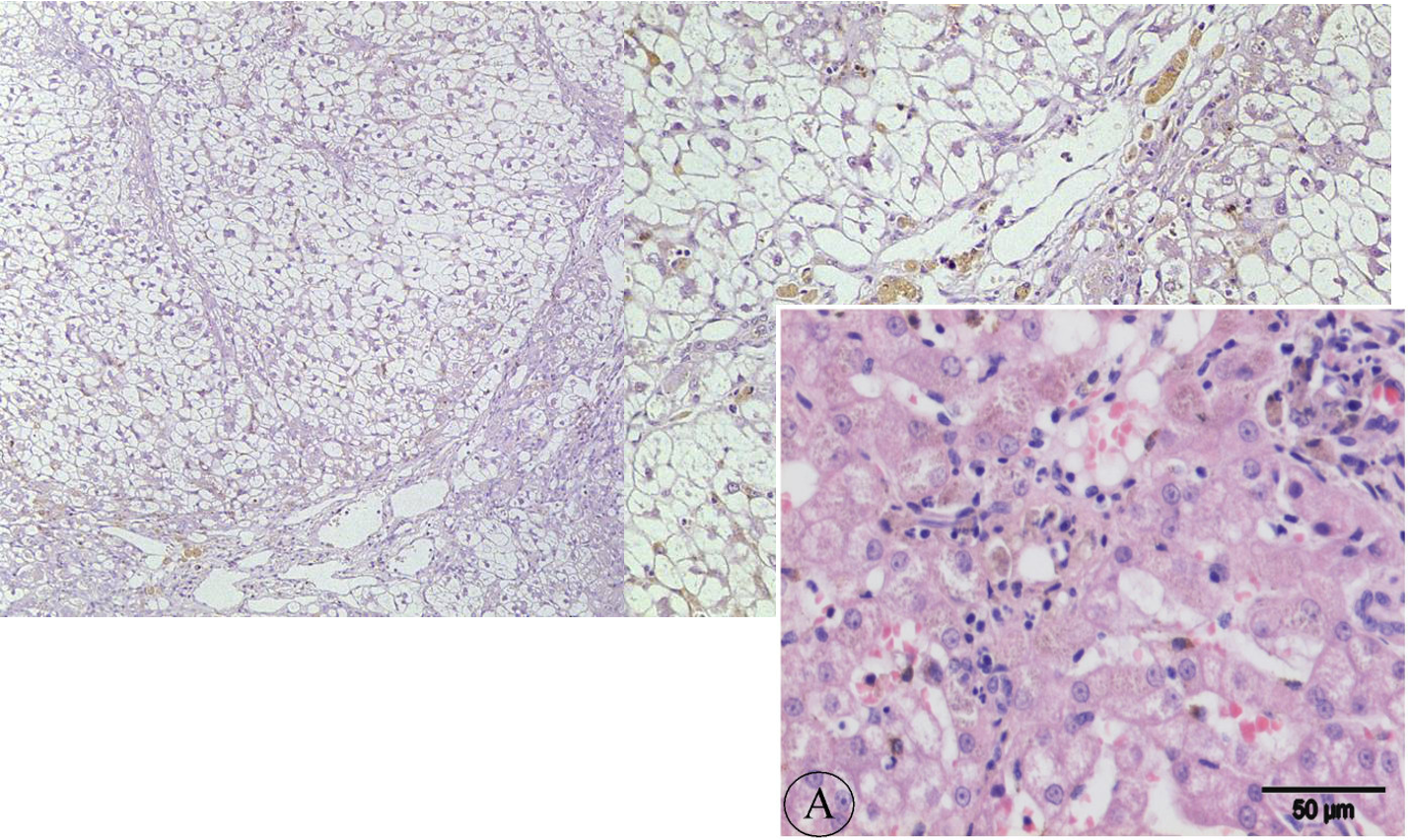
Areas of fibrosis
Marked degen of hepatocytes
Pigment accumulation
Hydropic degeneration = entry of fluid into hepatocytes
Mononuclear infiltration
What is being shown here?
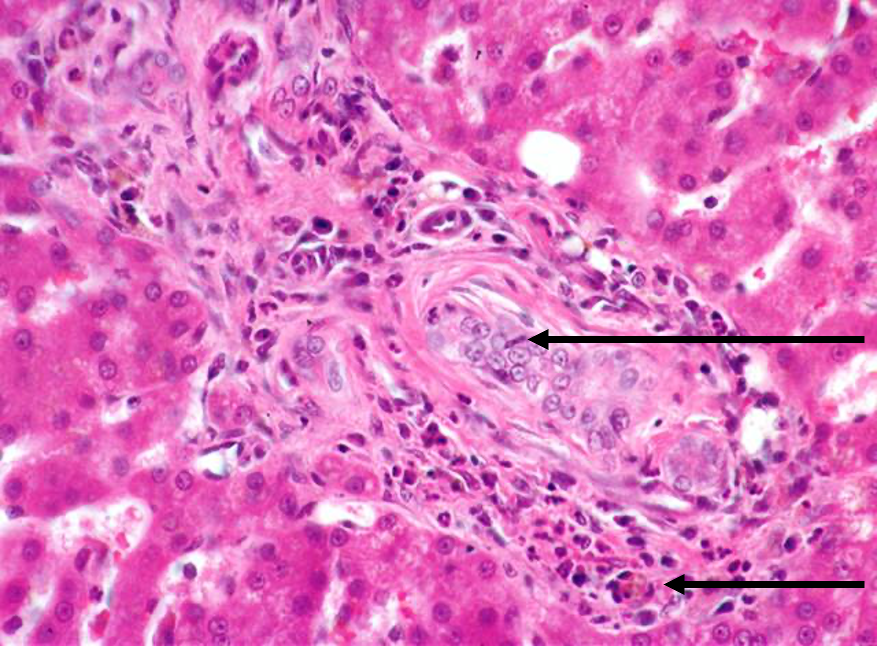
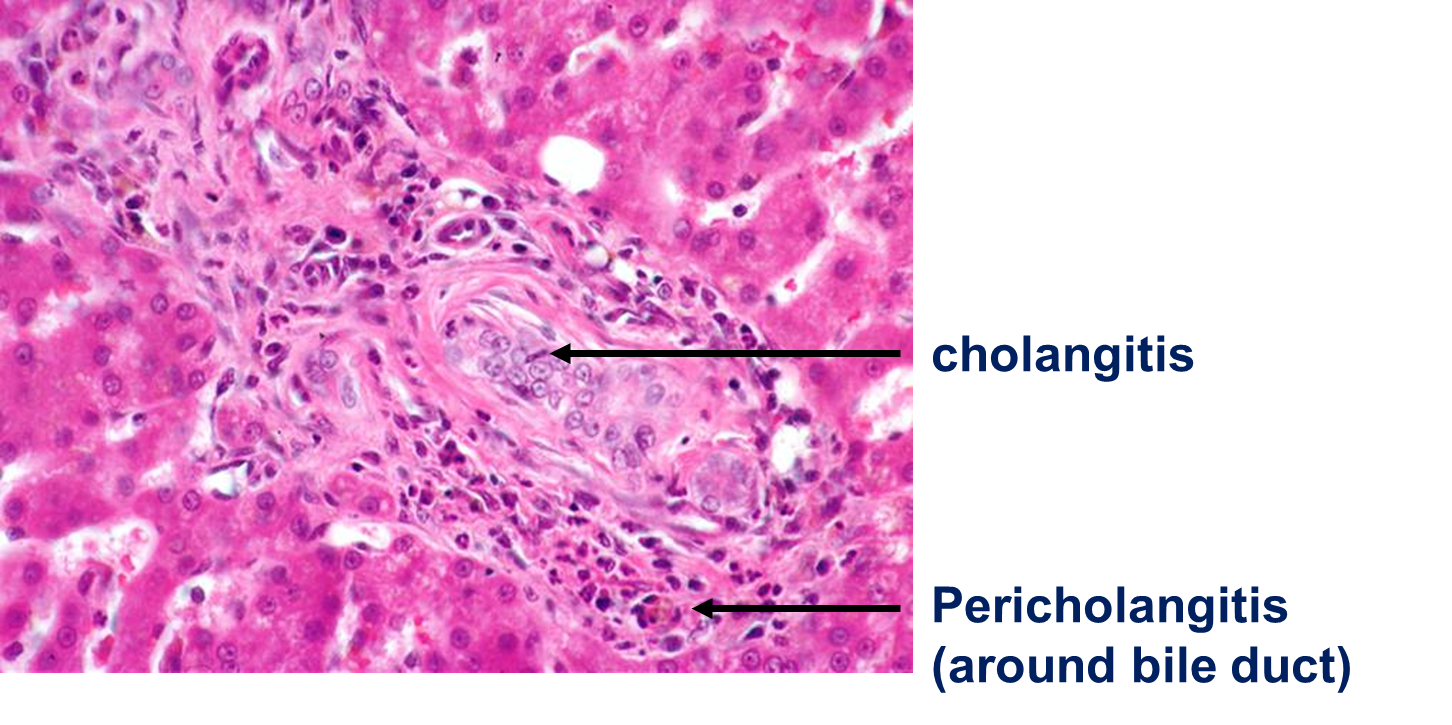
Cholangiitis / cholangiohepatitis = inflam originating from biliary tree
What is cholangiohepatitis?
Inflam originating from the biliary tree AND liver
When may you see cholangitis/cholangiohepatitis?
Chronic fascioliasis
Eimeria in rabbits
Biliary mucocoele (change in gall bladder of dog causing bile stasis)
Feline “triaditis”
What is feline triaditis?
Associated with three inflammation
IBD
Chronic pancreatitis
Feline cholangitis (inflam of bile duct system)
What are the clinical findings associated with feline cholangitis?
ascites, jaundice, polyphagia, weight loss
What are the three characteristic histological stages of feline cholangitis?
Suppurative cholangitis / cholangiohepatitis
Lymphocytic and plasmacytic periportal infiltration (1) bile duct hyperplasia and periportal fibrosis (2)
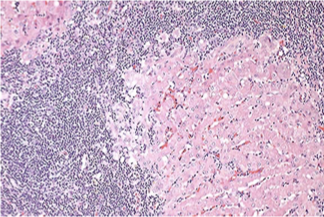
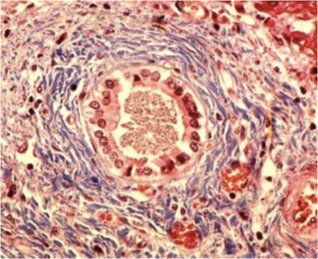
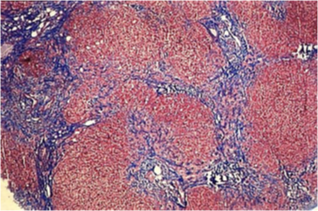
Biliary cirrhosis (2) [= end stage] (severe porto-portal fibrosis, bile duct hyperplasia (1), nodular hepatic hyperplasia)
List some examples of viral hepatitis
Infectious canine hepatitis [CAV-1; adenovirus]
Equine herpesvirus infection [EHV-1]
Canine herpesvirus infection [CaHV-1]
Rabbit haemorrhagic disease [RHDV-1 and -2; calicivirus]
Feline calicivirus (FCV)
Feline infectious peritonitis [FCoV; coronavirus]
any virus causing viraemia can affect the liver these are just specific
What aetiological agent causes canine hepatitis?
canine adenovirus type 1 [CAV-1]
Describe the pathogenesis of canine hepatitis
oronasal infection —> tonsils, regional lymph nodes, lymphatics, thoracic duct
blood (viraemia)
liver (hepatocytes, Kupffer cells)
eye (corneal epithelium)
kidney (glomerular endothelium)
blood vessels (endothelium)
(vacc against)
What are the different outcomes of canine hepatitis?
high titre = acute (necrotising) hepatitis —> if survives liver can regenerate
low titre = chronic, fibrosis, perrsistent infection
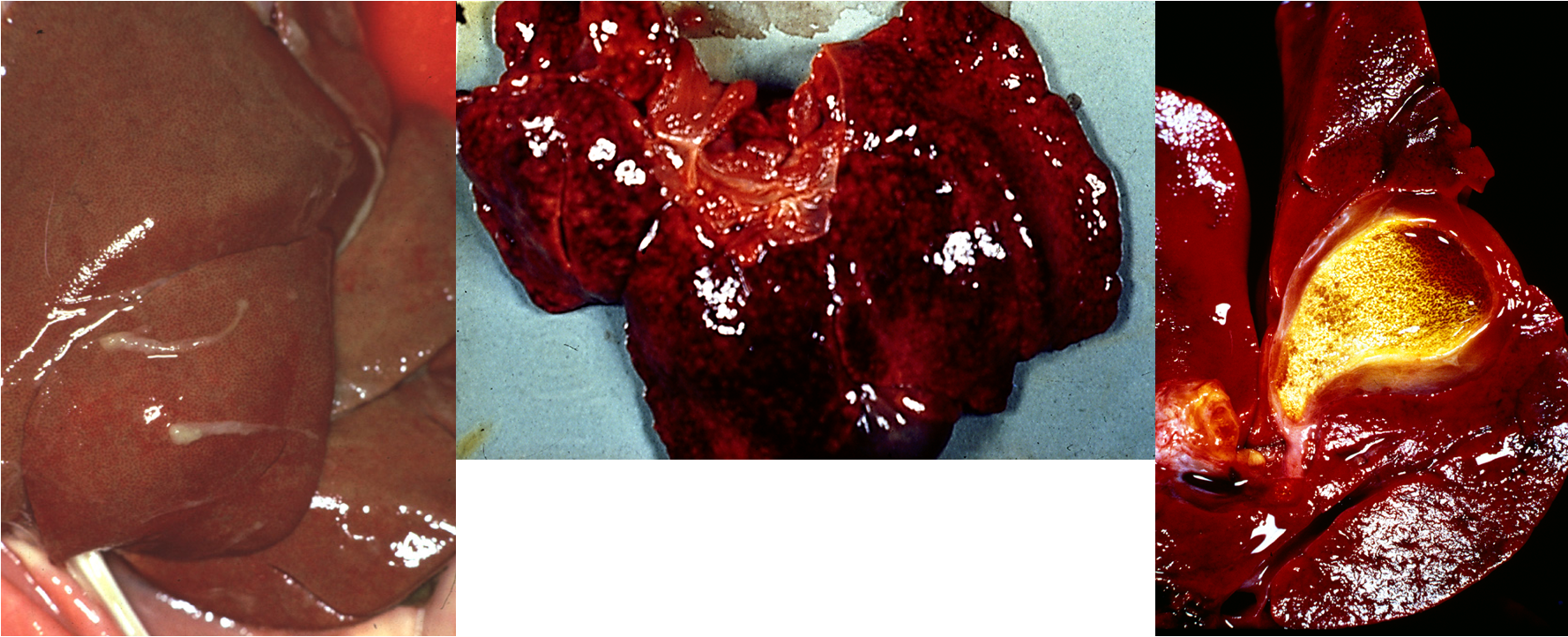
What gross lesions are associated with canine hepatitis?
multifocal haemorrhage (tropism for endothelium → damage)
fibrin deposition
oedema of gall bladder
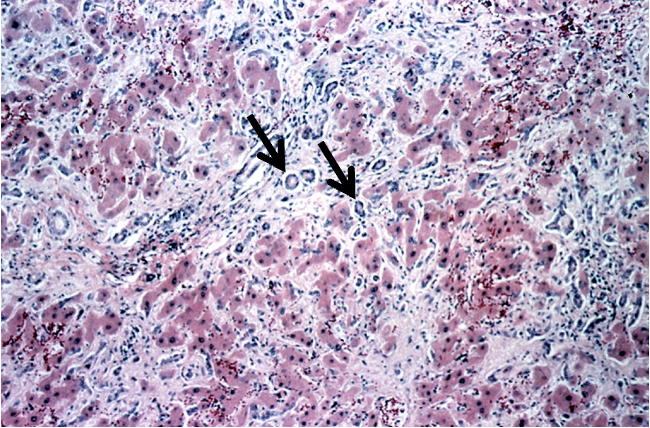
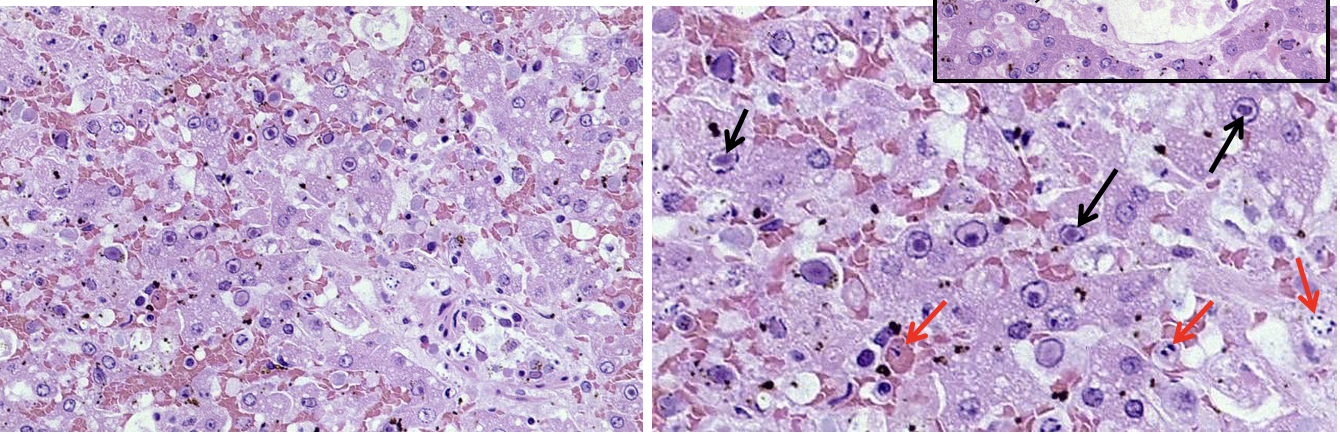
What histological lesions are associated with canine hepatitis?
Necrotic hepatocytes (red arrows)
Centrilobular
Intranuclear inclusion bodies (black arrows) (can get them in both hepatocytes & endothelial cells) —> chromatin in nucleus pushed to edge
seen in periphery of necrosis
What aetiological agent causes equine herpesvirus infection?
Equine herpesvirus 1 [EHV-1], rarely EHV-4
What is the pathogenesis of equine herpesvirus?
transplacental infection
uterus (endothelial cells),
(peri)vasculitis, thrombi → placental detachment → late abortion (7th month)
What organs does equine herpesvirus affect in the fetus?
Liver
Lungs
Thymus
Spleen (follicles)
Brain
Adrenal gland
What gross and histological lesions are associated with equine herpesvirus in the liver?
Disseminated multifocal necrosis
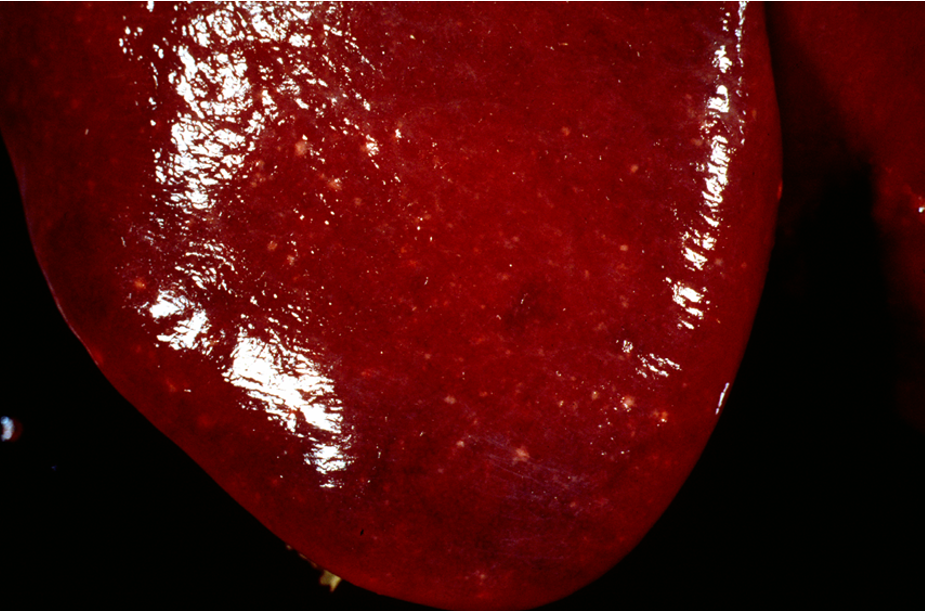
Disseminated multifocal necrosis, inflammation and intranuclear inclusion bodies (eosinophilic) (less frequent + smaller in herpesvirus than in adenovirus
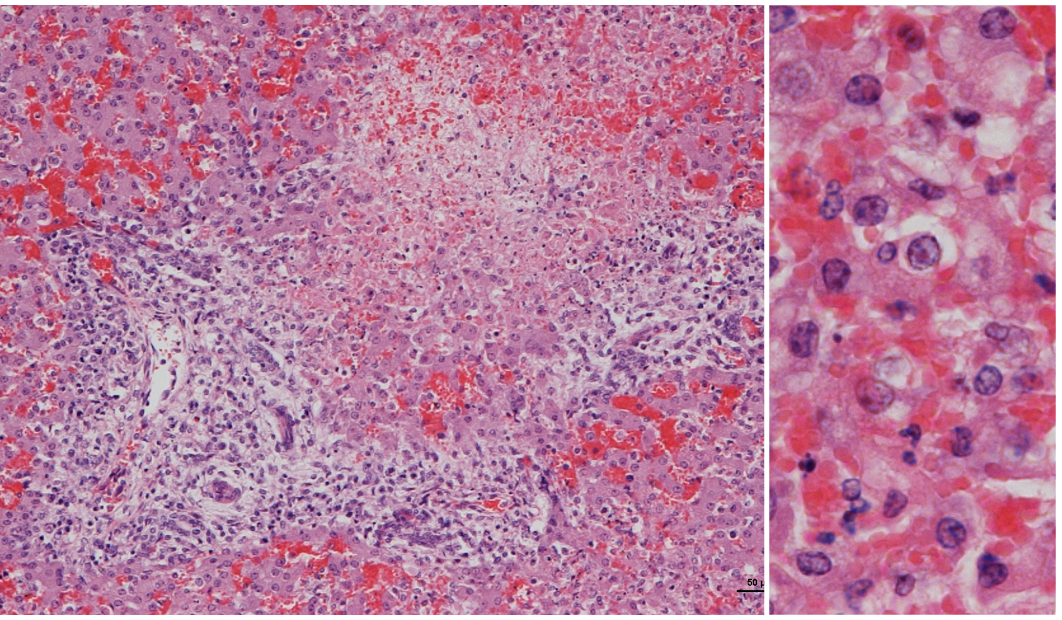
DO PCR TO CONFIRM
What different ages can be infected by canine herpes and how does this impact the pathogenesis of the viral?
In utero
Usually generalised infection fatal before or after birth
Neonate —> from ingestion, inhalation material in birth canal
<1 week generalised infection (viraemia due to not well developed immune system)
>2 weeks localised infection and replication —> latency and recrudescence
Adult (less common)
Localised infection and replication —> latency and recrudescence if stressed, immunosuppressed, pregnant…
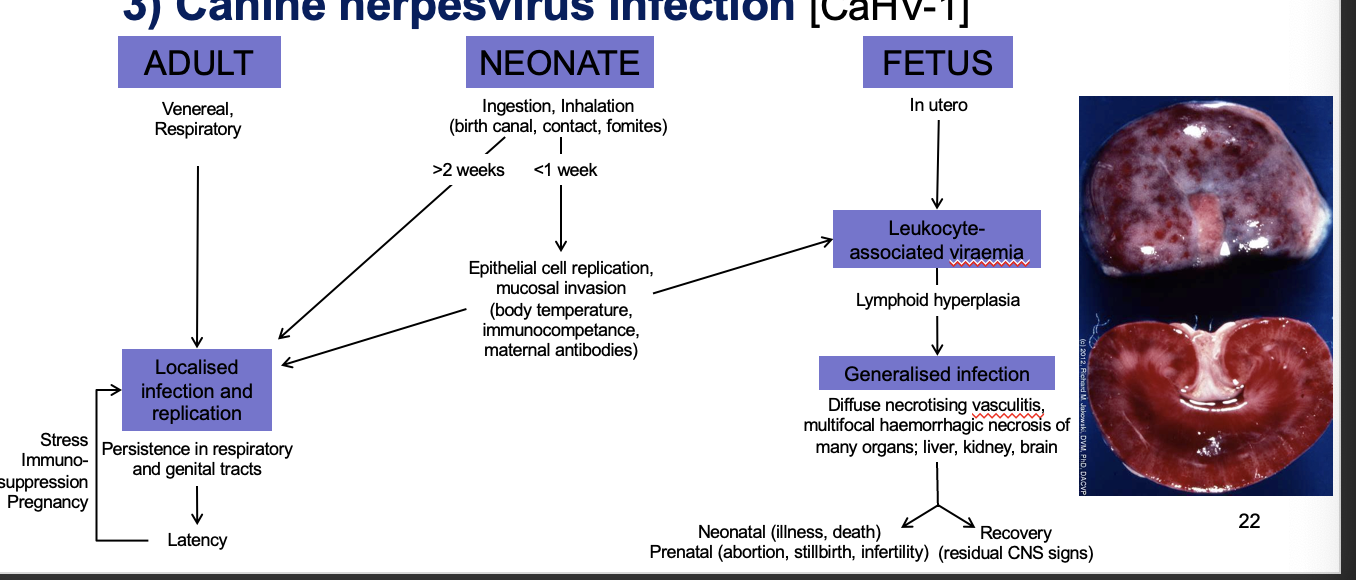
(can vacc against but not standard vacc)
What aetiological agent causes rabbit haemorrhagic disease?
calicivirus (RHDV-1, RHDV-2)
(can vacc against)
What is the pathogenesis of rabbit haemorrhagic disease?
faecal-oral infection (highly contagious —> transmitted on fomites)
(per)acute dx w/ massive necrosis of hepatocytes (virus infects hepatocytes) → sudden death
DIC in multiple organs (microthrombi e.g. in lung capillaries and renal glomeruli) —> haemorrhage due to reduction in clotting factor production
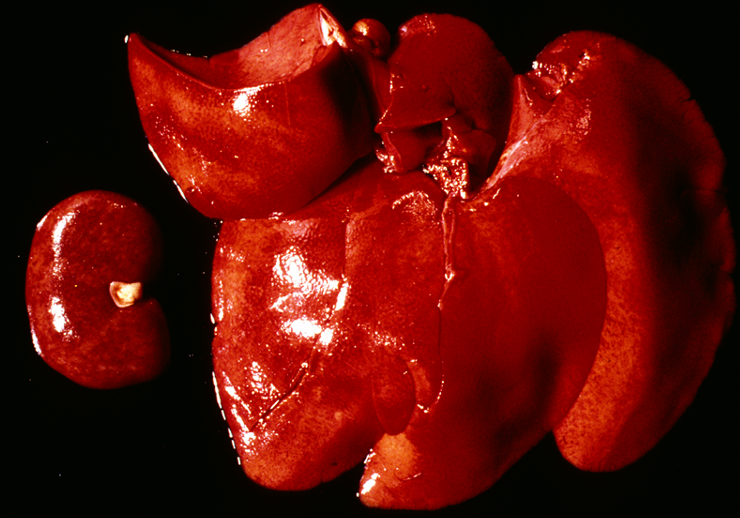
How does rabbit haemorrhagic disease present grossly?
Multifocal disseminated hepatic necrosis, glomerular hyperaemia
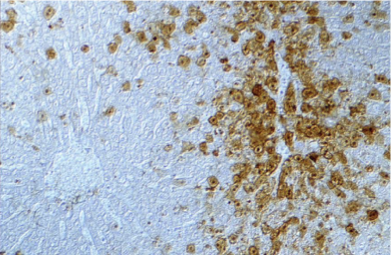
How does rabbit haemorrhagic disease present histologically?
Hepatic necrosis & calicivirus antigen
How does feline systemic calicivirus present histologically in the liver?
Hepatitis
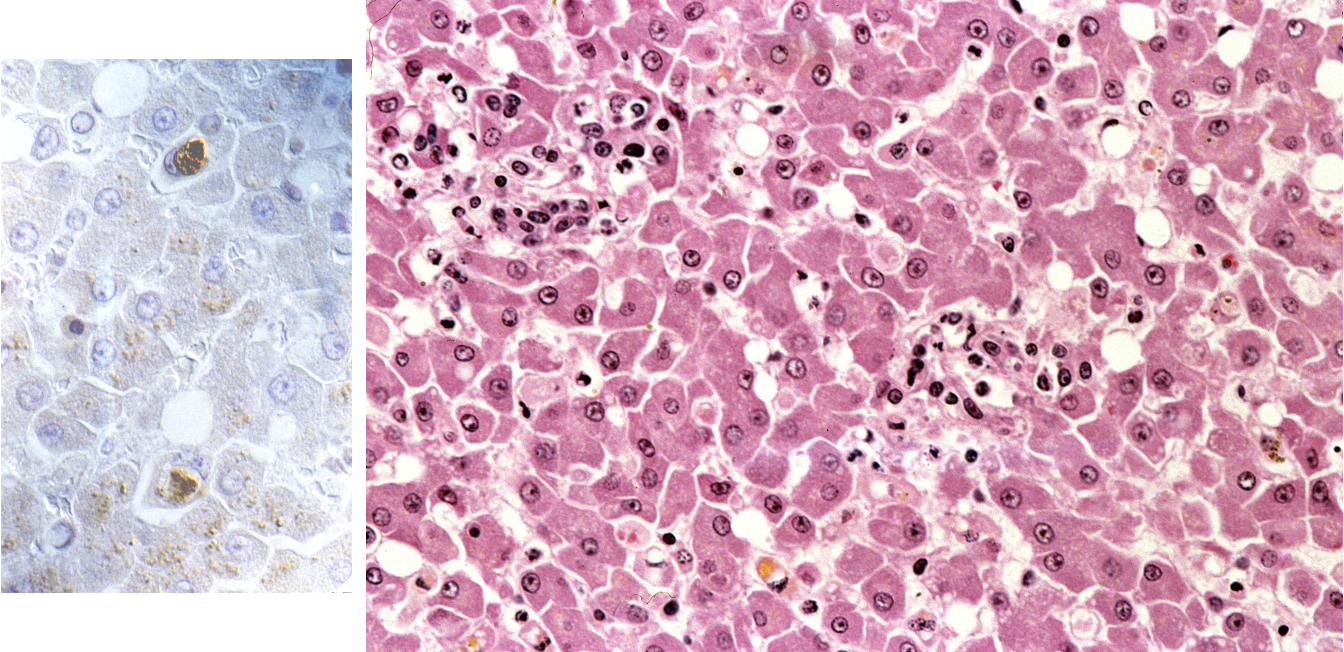
stain = virus present
What aetioloigcal agent causes feline infectious peritonitis?
Feline coronavirus (FCoV)
Describe the pathogenesis of feline infectious peritonitis
oral infection
infection of enterocytes
monocyte-associated viraemia
granulomatous (peri)phlebitis / serositis / hepatitis etc.
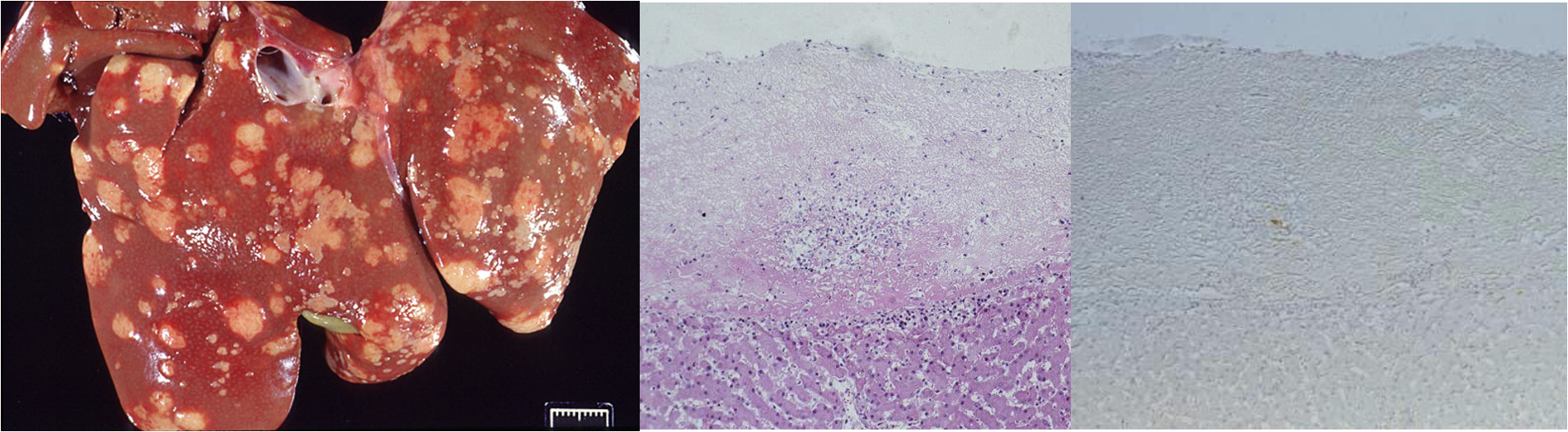
How does feline infectious peritonitis present grossly and histoloigcally?
multifocal granulomatous inflam (in any tissue)
Perivasculitis
What are the routes of entry of bacteria causing hepatitis?
the portal vein
umbilical veins in neonates
hepatic artery (generalised bacteraemia)
ascending infection via bile duct / system
parasitic migration
direct extension of infection from an adjacent tissue
List examples of bacteria causing bacterial hepatitis
Enteric bacteria
Francisella tularensis (tularaemia)
Nocardia asteroides
Actinobacillus spp.
Mycobacterium spp. (tuberculosis)
Fusobacterium necrophorum (necrobacillosis)
What aetiological agent causes necrobacillosis?
Fusobacterium necrophorum
[filamentous, gram-negative, anaerobe, commensal in digestive tract]
What is the pathogenesis of necrobacillosis in ruminants?
rumenitis-liver abscess syndrome
carbohydrate-rich diet → ruminal acidosis
change in rumen microflora and defects in ruminal mucosa
access of bacteria to blood vessels and portal vein
liver —> multifocal necrosis, abscess formation
What is this showing?
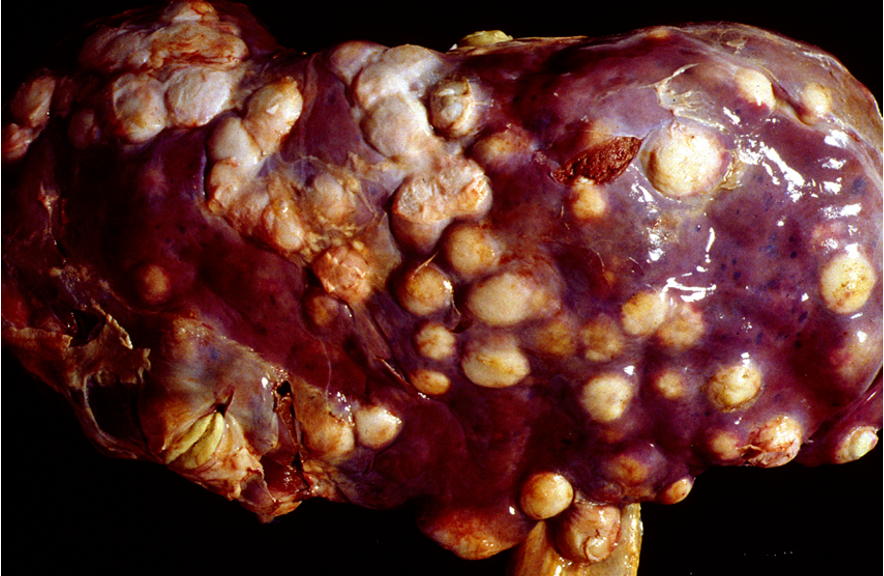
Necrobacillosis
Multiple abscesses
This indicated blood borne infection because of how spread out it is
What aetiological agent causes tularaemia?
Francisella tularensis
[ZOONOSIS] [pleomorphic, gram-negative, non-spore forming bacillus]
How is francisella tularensis spread?
Ticks
What is the pathogenesis of tularaemia?
inoculation site (skin lesions, tick bite, prey animals: intestine)
localised infection & regional lymphadenitis
bacteraemia, dissemination
What pathology is assocaited with tularaemia?
ulceration of lymph nodes (or Peyer`s patches with enteric infection),
necrotising lymphadenitis,
hepatitis

splenitis
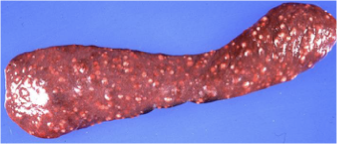
What is being shown here?
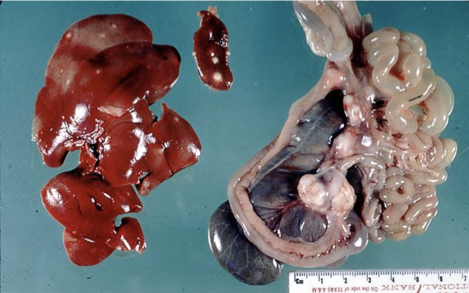
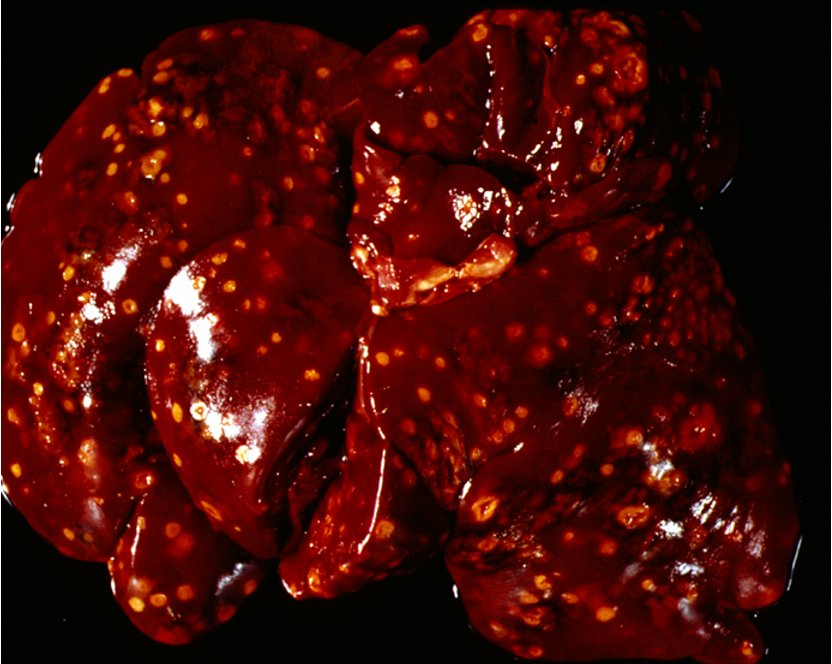
Yersiniosis
Microabscesses (disseminated, multifocal) in mesenteric LNs, spleen & liver
What aetioloigcal agents causes yersiniosis?
Y. pseudotuberculosis
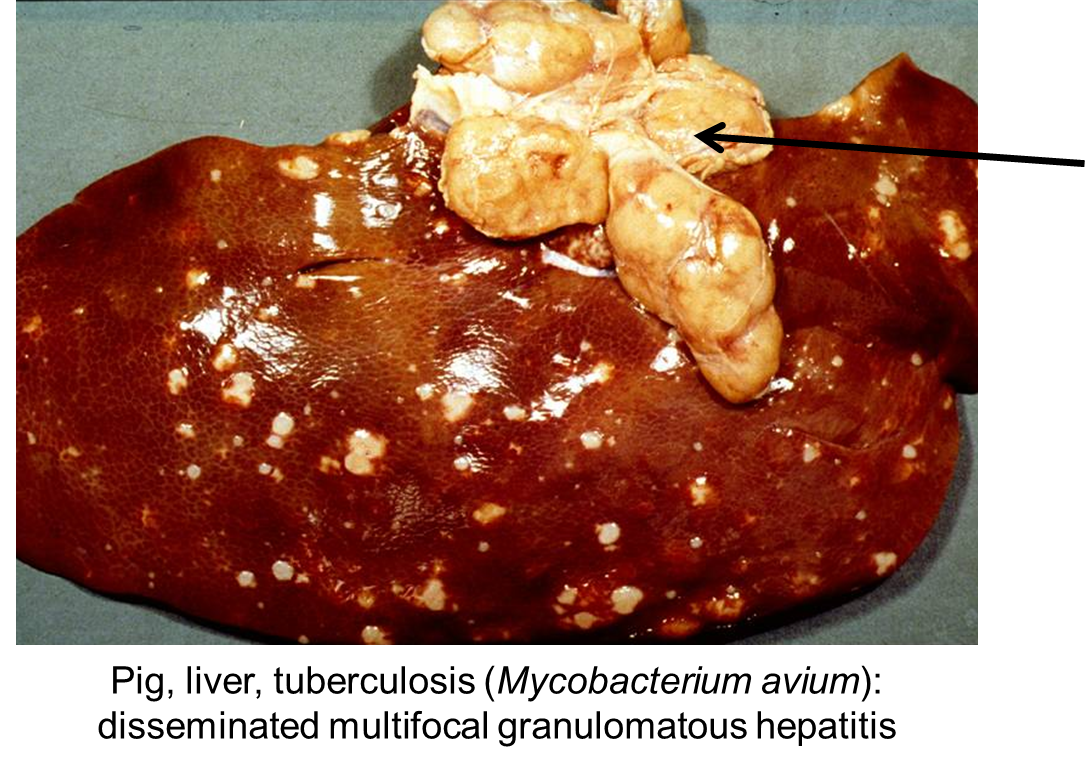
What has caused this lesion?
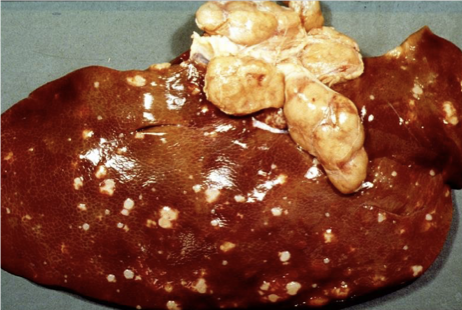
Tuberculosis (M.bovis / M. tuberculosis / M. avium)
Disseminated multifocal granulomatous hepatitis
What aetiological agents cause leptospirosis?
Leptospira canicola, L., icterohaemorrhagica, L.grippotyphosa
[motile, filamentous, spiral-shaped (spirochaetes)]
Zoonosis
(can vacc against certain strains in dogs)
What is the pathogenesis of leptospirosis?
Penetration of MM/abraded skin
Replication in blood
kidneys, liver, spleen, brain, eyes, genital tract
serum abs clear spirochaetes from organs, but persistence in renal tubular epithelium can occur
Transmission via contam water, soil, dirty bedding —> excreted in urine
How does leptospirosis affect the liver in dogs?
Dysfunction due to cell damage by leptospiral toxins (hepatocellular necrosis);
Periportal inflammation and necrosis
Intracanalicular bile plugs —> jaundice
Intravascular haemolysis-> jaundice->centrolobular necrosis (hypoxia)
Can develop to chronic active hepatitis
How does leptospirosis affect the kidneys in dogs?
Tubular necrosis (esp. L. grippotyphosa, L. canicola)
What is causing these lesions?
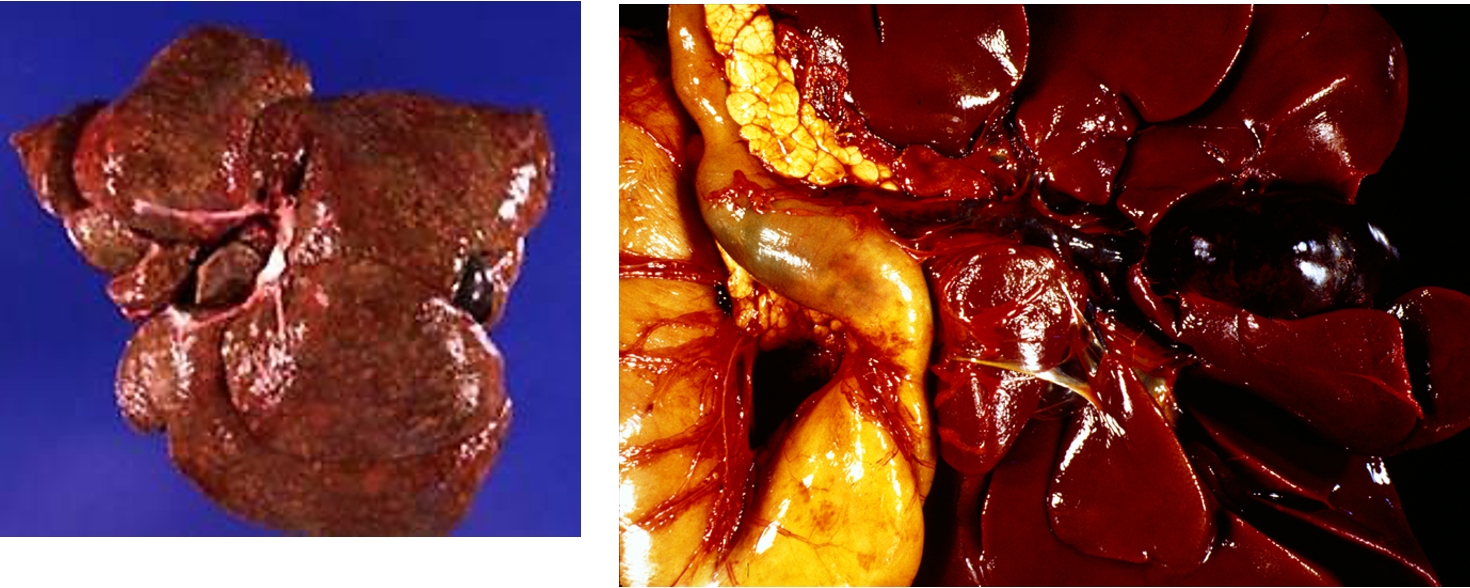
Leptospirosis
mottled appearance due to haemorrhage and necrosis
Jaundice
Due to intravascular haemolysis and/or bile stasis
Can also get anaemia cuasing centrolobular necrosis in liver 2° to ischaemia and hypoxia
Gallbladder and bile ducts filled with blood
What are the histological features of leptospirosis?
Hepatocellular dissociation (loss of tight junctions between hepatocytes)
Causes loss of pressure between cells which induces mitosis → Mitotic figures (arrows)
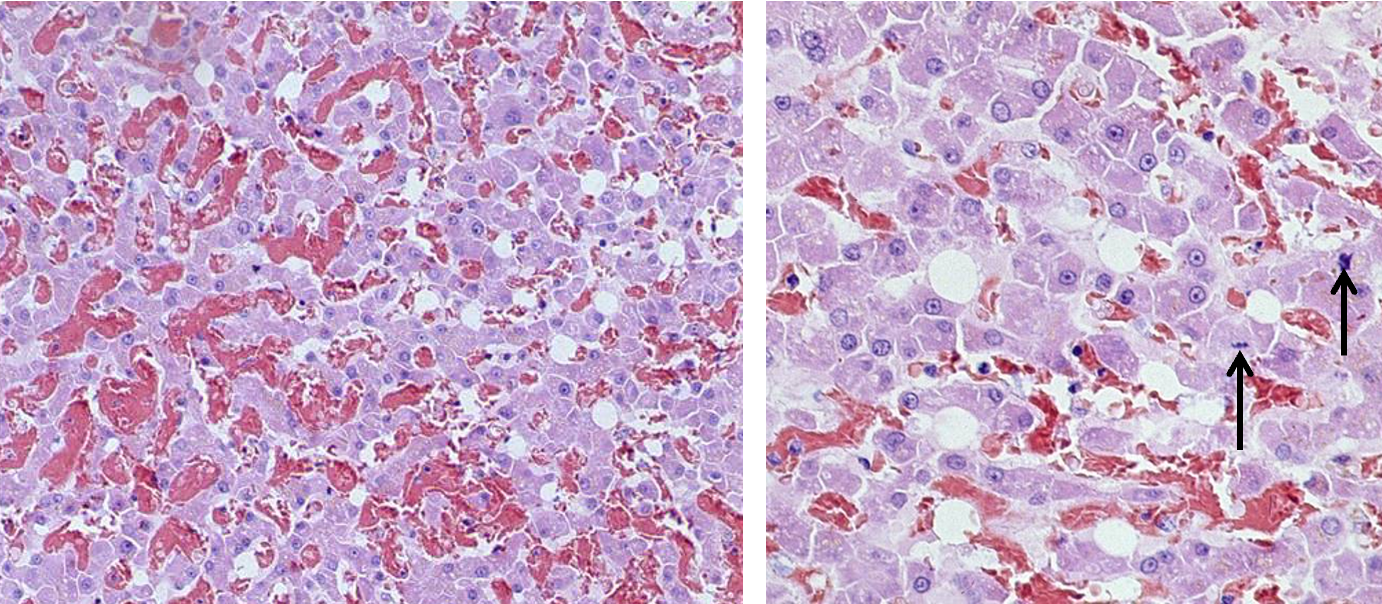
Rounded cells
Eosinophilic granular cytoplasm
Dark shrunken basophilic nuclei
Loss of cords/plates (dissociation)
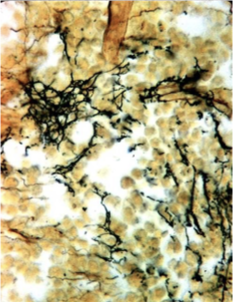
^^^ Leptospira with Warthin Starry (silver stain) highlights bacteria
What aetiological agent causes Tyzzer's disease?
Clostridium piliforme
[ZOONOSIS]
[motile, spore-forming, gram-negative, obligate intracellular, commensal in gastrointestinal tract of small rodents —> faecal contam]
What animals does Tyzzer's disease affect?
laboratory rodents, guinea pigs, foals, dogs, cats
young or immunocompromised animals
What is the pathogenesis of Tyzzer's disease?
contact with rodent (prey) faeces
prolif in intestinal epithelial cells (ulcerative, necrotising colitis and typhlitis) with immunosuppression (?)
spread to liver
necrosis
foals —> infectious route not known
What has caused these lesions?
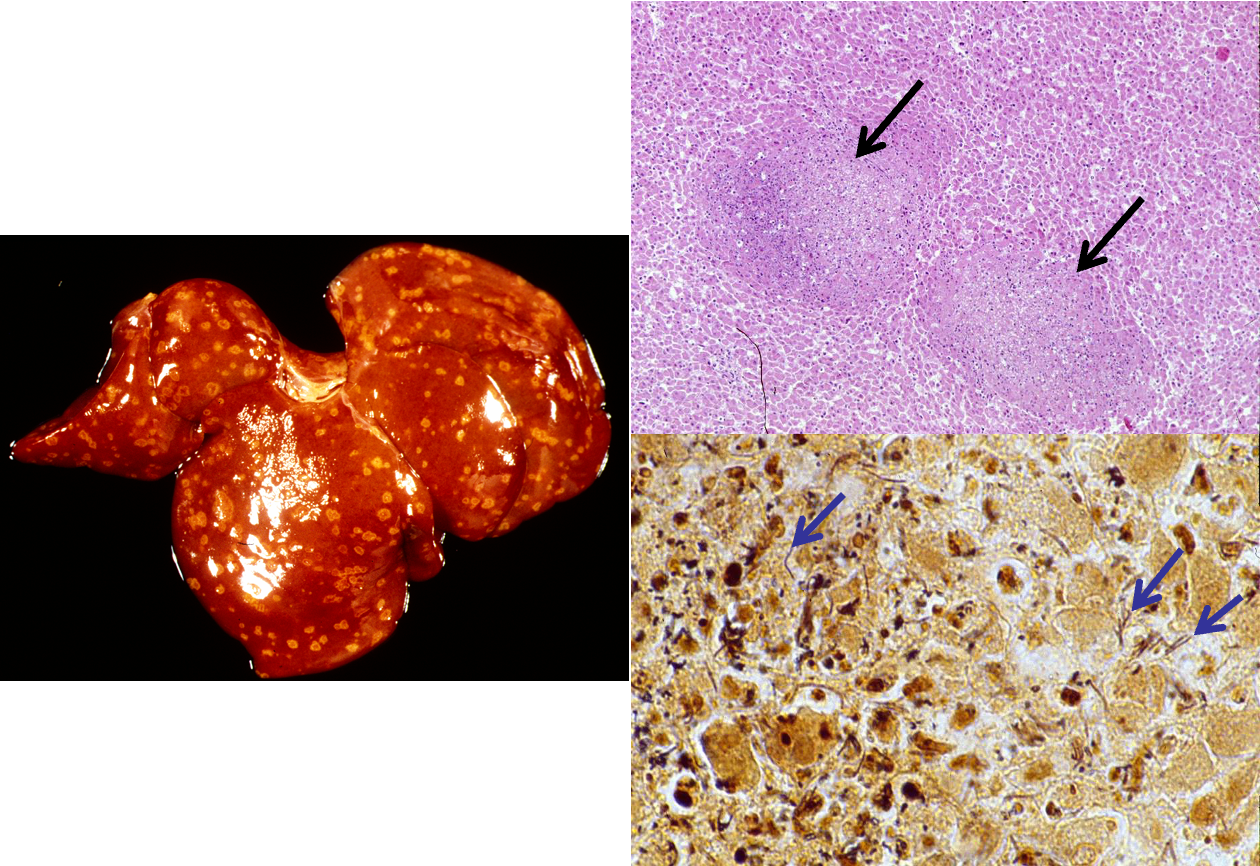
Tyzzer's diseass
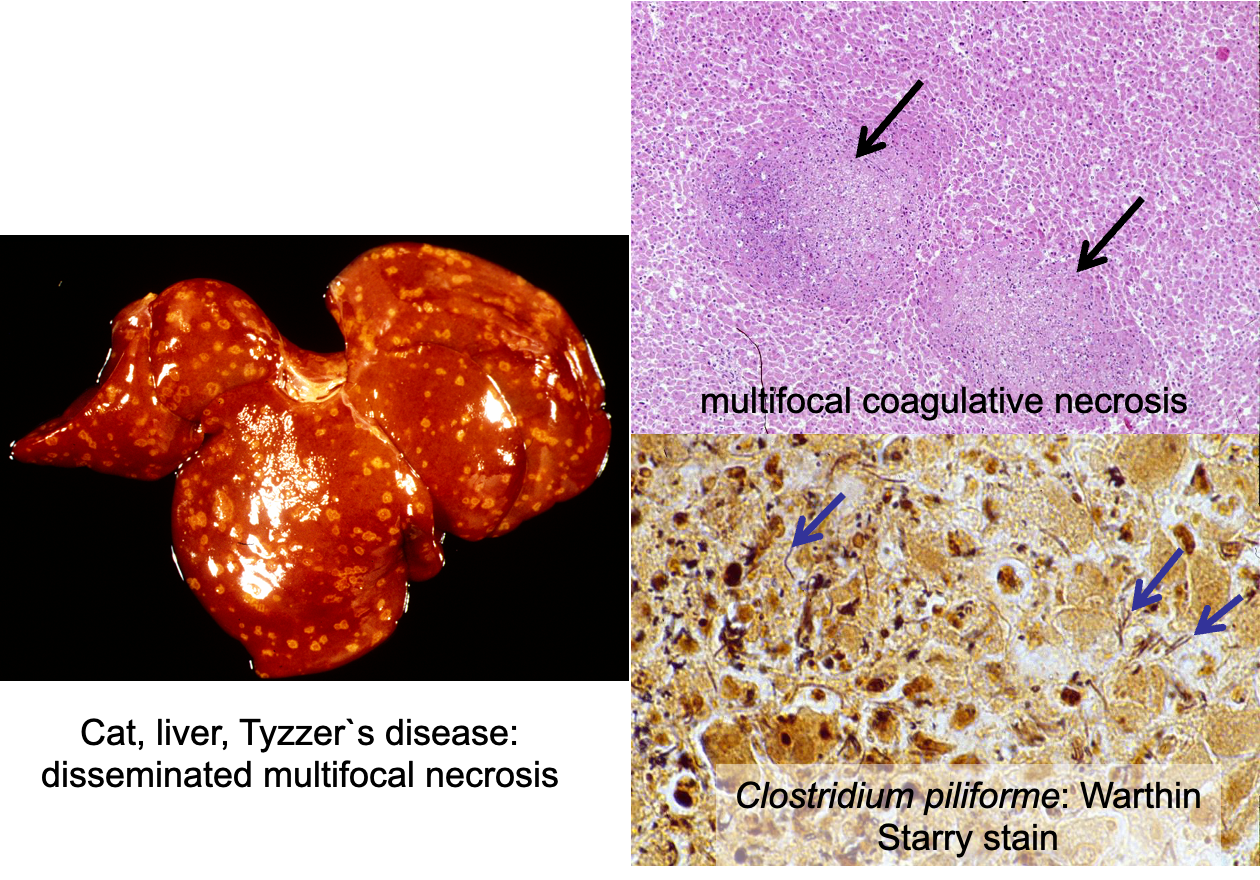
What protozoan infections cause parasitic hepatitis? What are their features
Toxoplasmosis (toxoplasma gondii, zoonosis)
Can see tachyzoites in hepatocytes
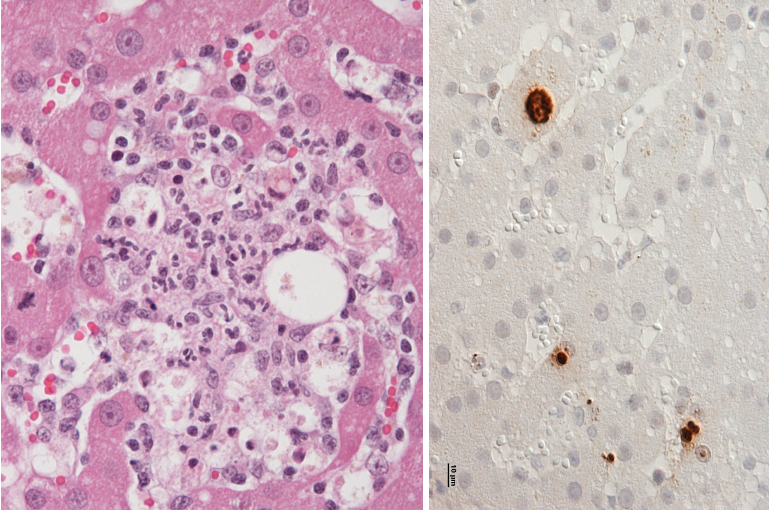
Leishmaniasis
Biting inseccts → generalised, chronic infection
Infection of macros → replication → rupture of cells → release
Typically chronic infection
Granulomatous hepatitis
Amastigotes in macrophages
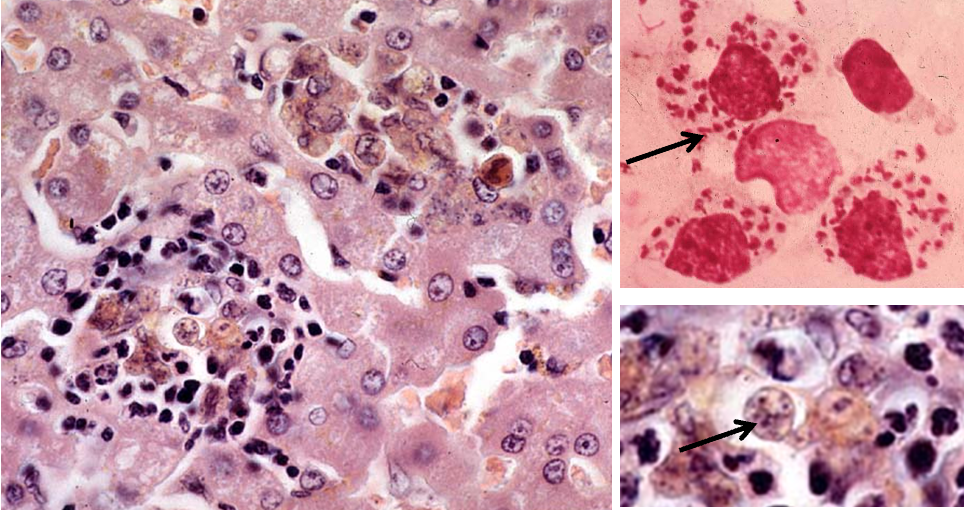
What coccidiosis can affect the liver?
Eimeria stiedai in hares and rabbits
What are the features of Eimeria stiedai?
replication in bile duct epithelium —> induction of
proliferation of bile duct epithelium
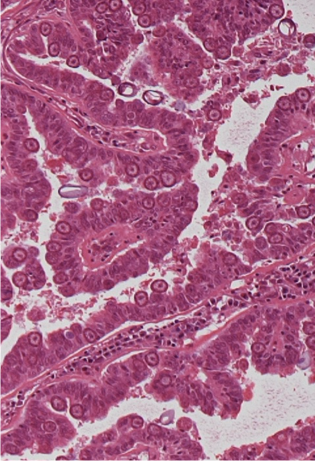
proliferation (sporo- and gammogonia in bile duct epithelium) and induction of papillary proliferation of bile duct epithelium
Chronic hyperplastic cholangitis
What metazoan infections can cause parasitic hepatitis?
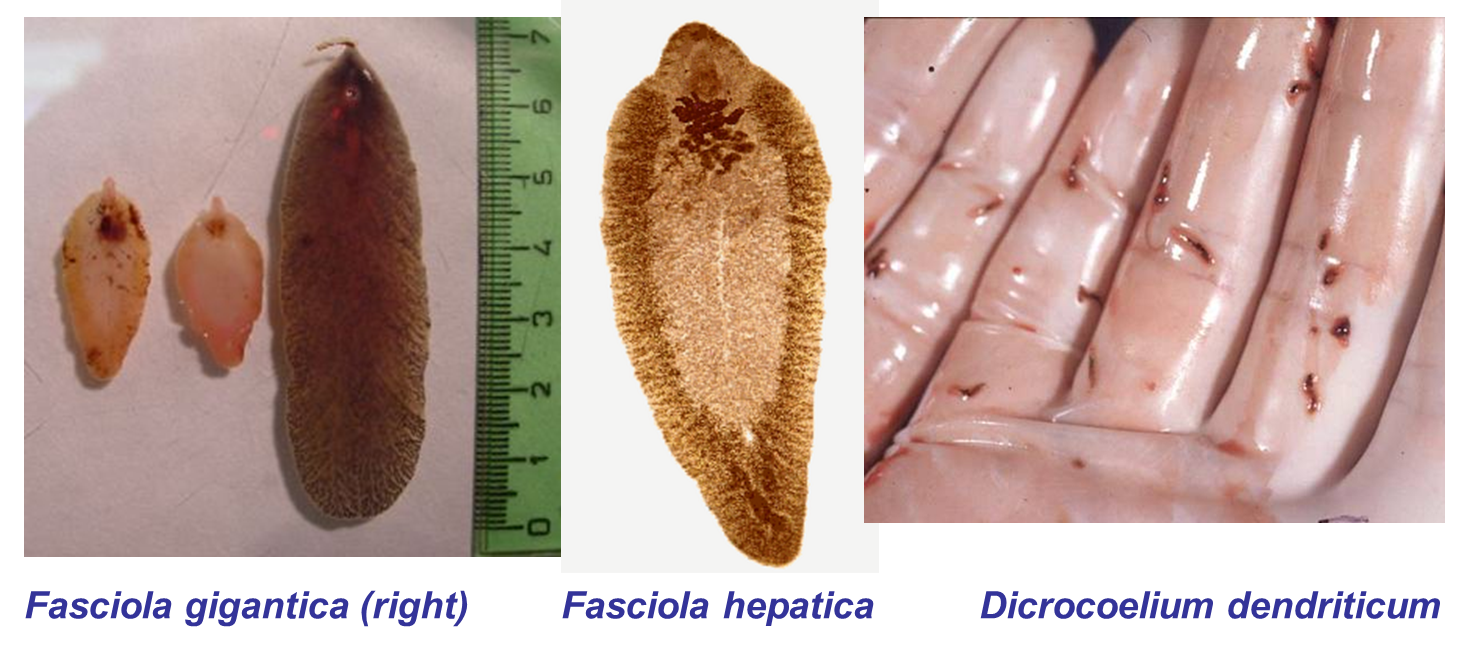
Trematodes
Liver flukes —> Fasciola hepatica, Dicrocoelium dendriticum
Cestodes - hydatid cysts
Echinococcus granulosus
Echinococcus multiocularis
Cysticercus tenuicollis
Taenia hydatigena
Nematodes
What are the two forms of Fascioliasis?
Acute fascioliasis —> due to larval migration
Chronic fascioliasis —> due to mature fluke in bile ducts
How does acute fascioliasis present grossly and histologically?
haemorrhage & necrosis with eosinophils and granulomatousinflammation
Acute but granulomatous inflam
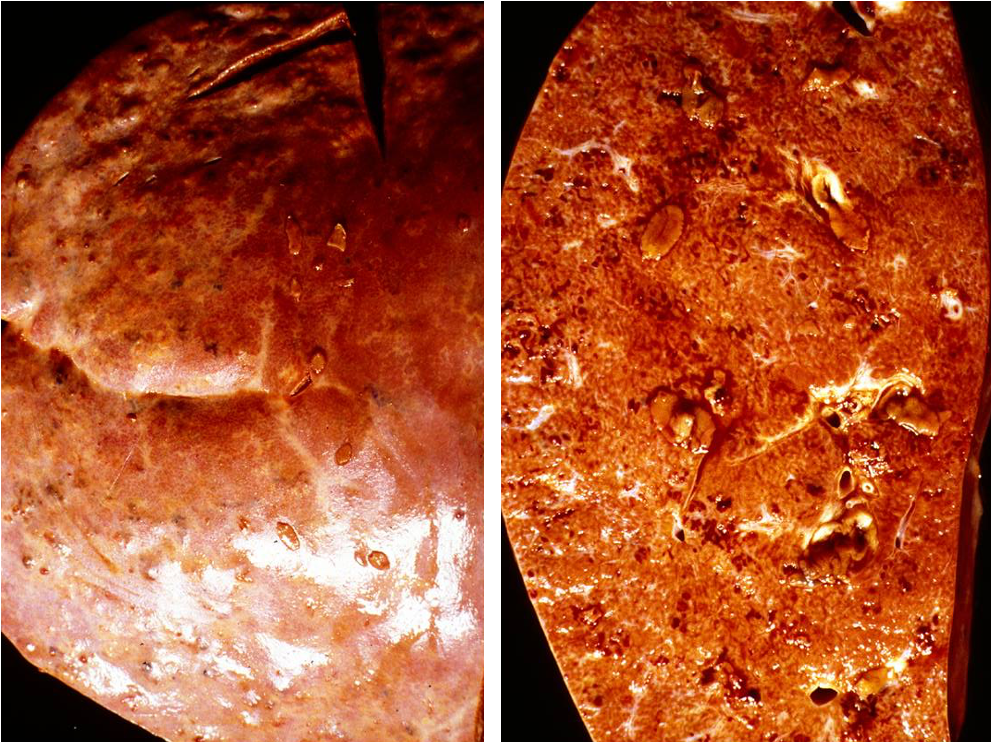
What are the possible consequences adn outcomes of acute fascioliasis?
Consequences:
hepatic dysfunction, anaemia
Outcome:
1) healing —> granulations tissue → residual scarring → diffuse fibrosis
2) Black disease (Clostridium novyi) —> spores latent in macrophages (liver), & proliferate in anaerobic (necrotic) areas
3) chronic fascioliasis
What lesions does chronic fascioliasis cause?
chronic hyperplastic cholangitis
peribiliary fibrosis +/- calcification due to mechanical irritation, bile stasis, excretions
'Pipe stem appearance'

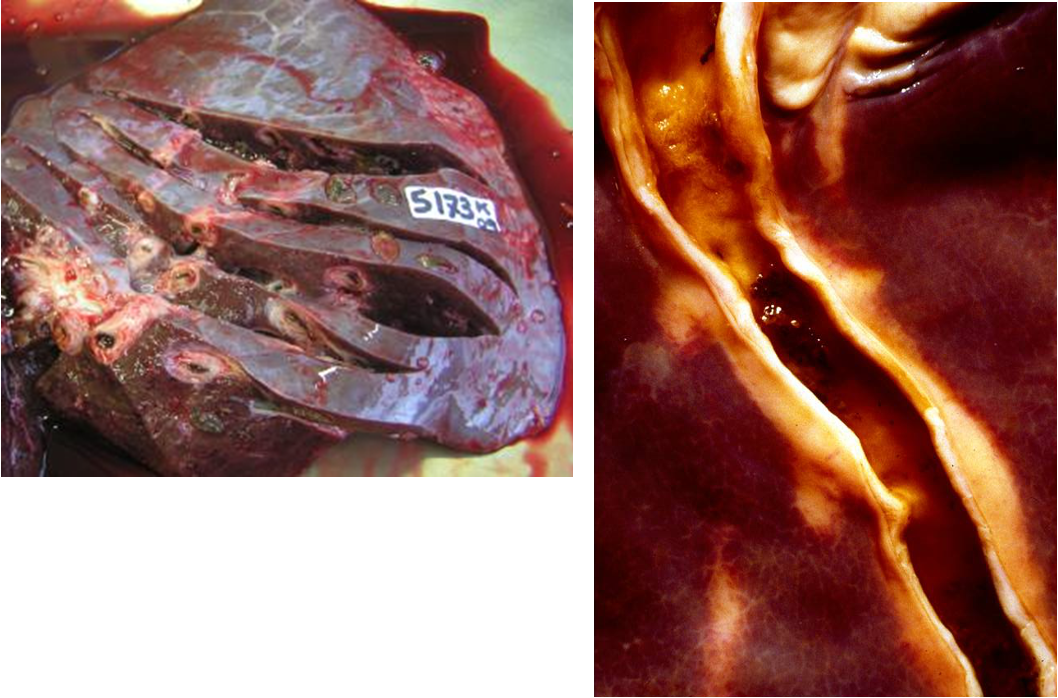
What are the possible consequences of chronic fasciolosis?
anaemia
hypoproteinaemia
chronic debilitation
death (sheep)
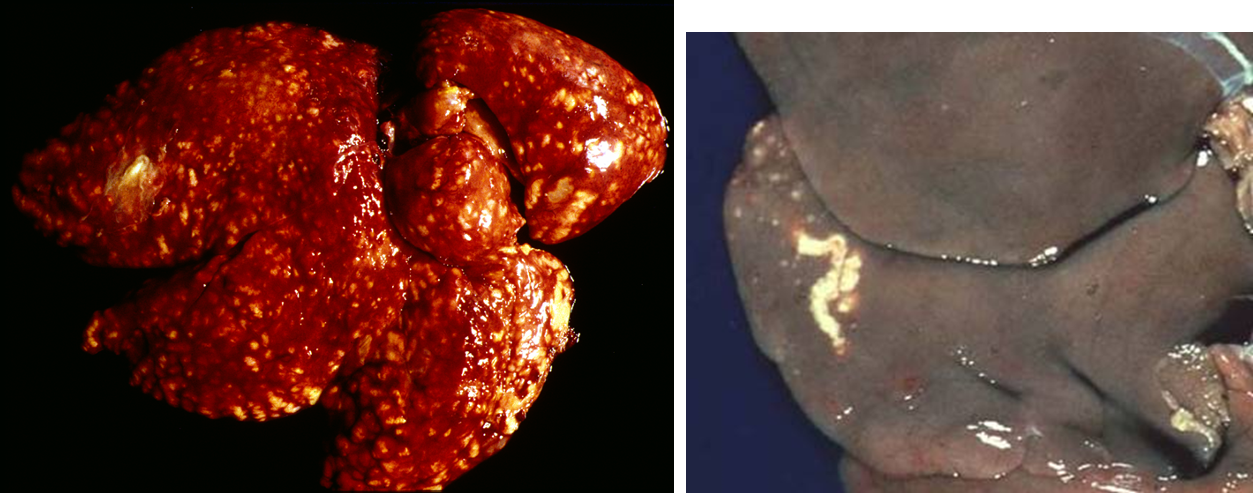
What are these lesions assocaited with?
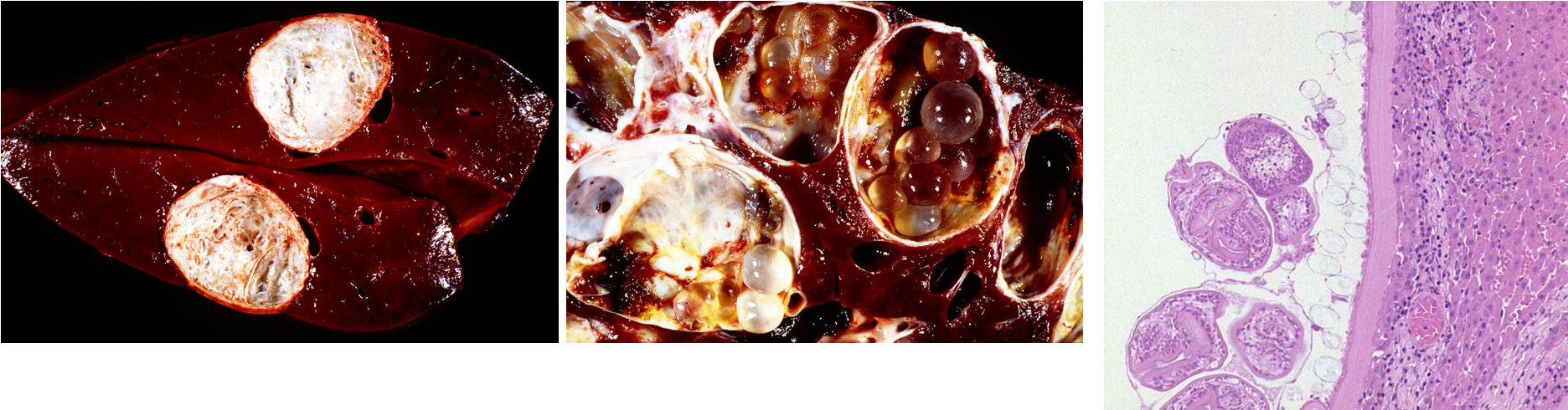
Cestodes —> “hepatophilic”
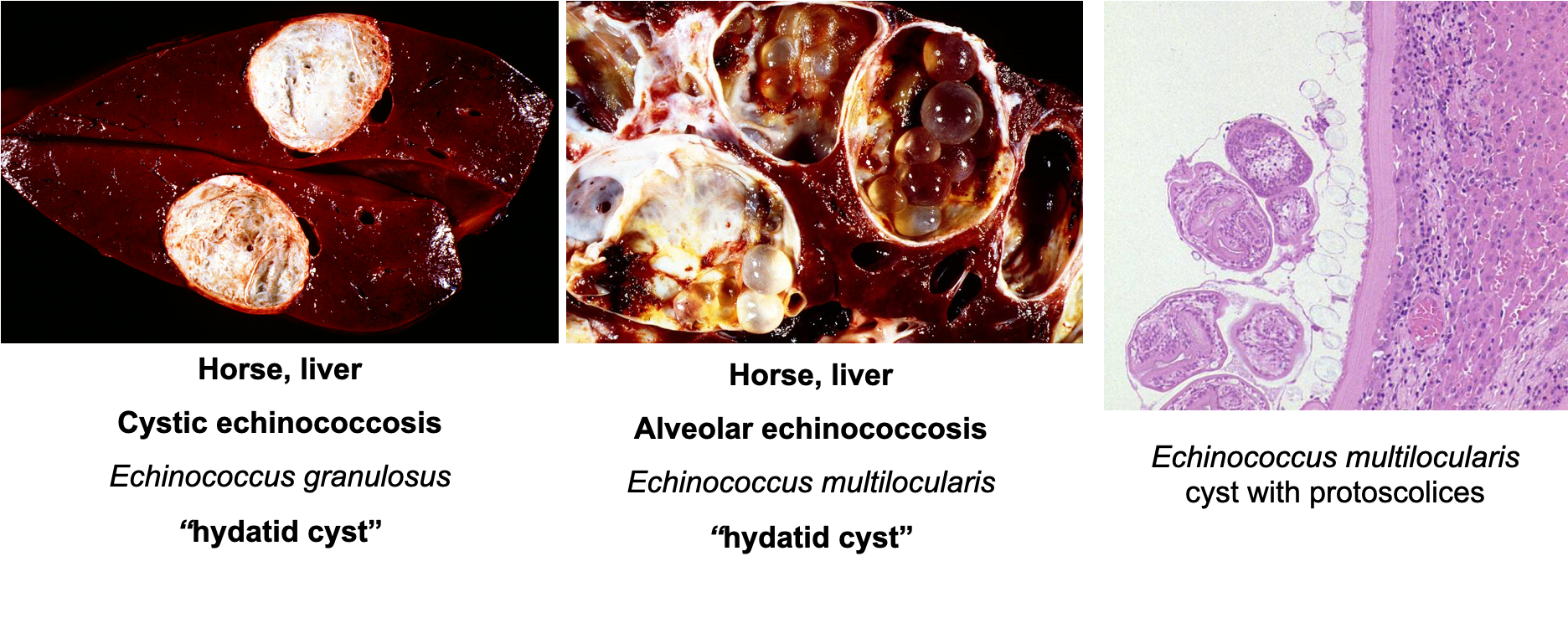
What are these lesions assocaited with?
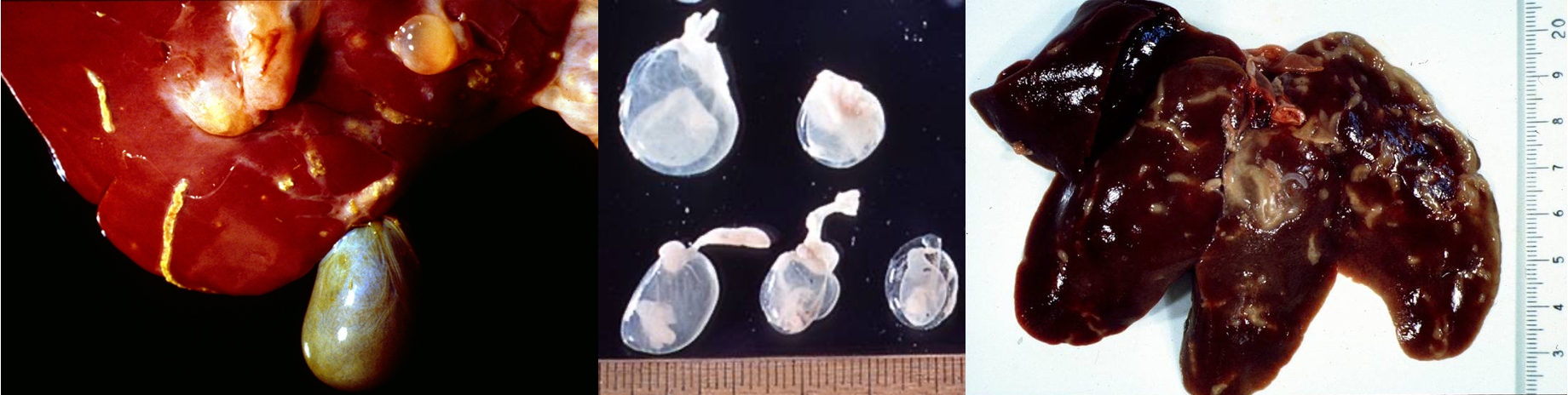
Cestodes —> “serosophilic”
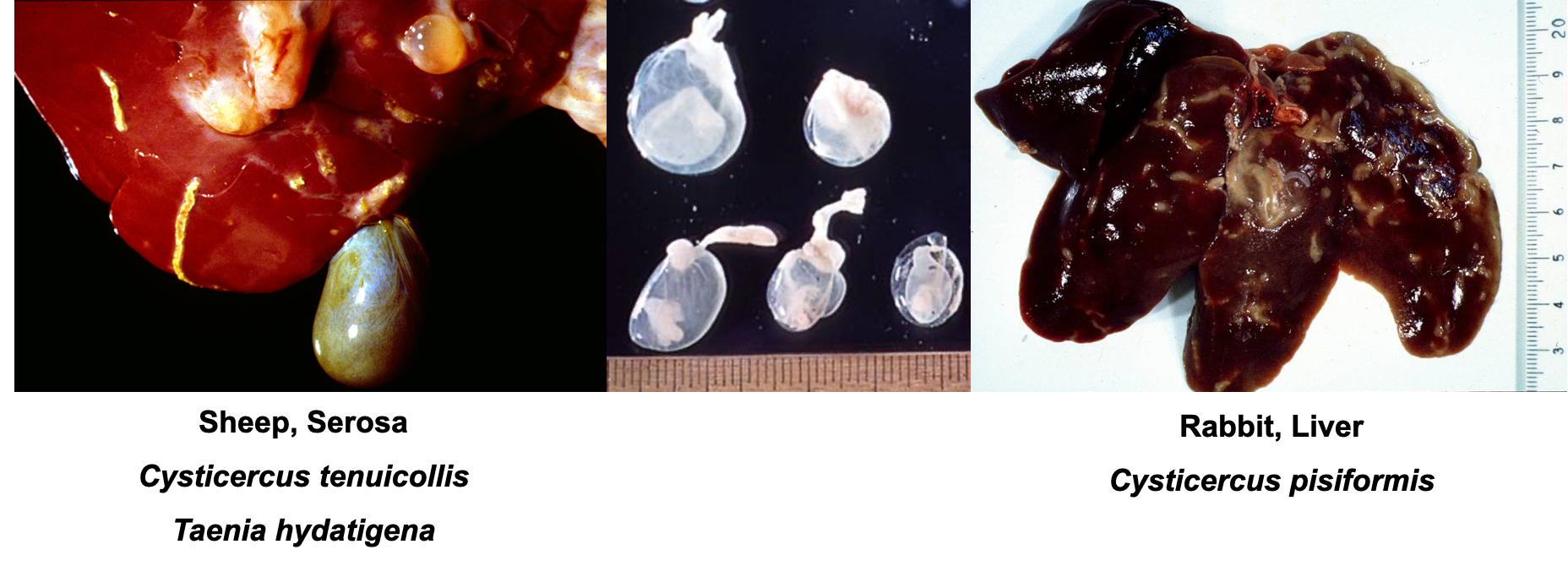
What is this lesion associated with?
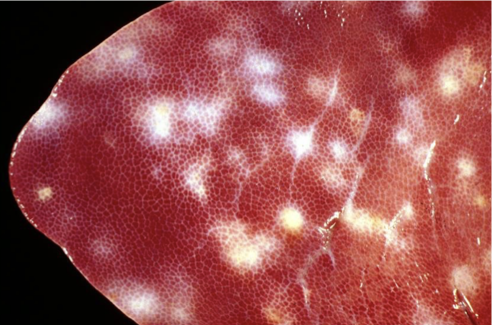
'Milk spot liver' —> fibrosis & hepatitis due to migration through liver parenchyma + eosinophil-dom inflam
Ascaris suum (pig) (also toxocara canis, and t. mystax)
Multifocal interstitial hepatitis
Chronic eosinophil dominated periportal infiltration