Gastrointestinal: BLOCK 1 Flashcards: The Exocrine Pancreas
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
describe the basic anatomy of the pancreas (4)
retroperitoneal
originates from the foregut
pancreas is split into the tail, body, head and Uncinate Process
has exocrine and endocrine portions
Describe the anatomy of the Exocrine Pancreas
exocrine pancreas has a bile duct which travels from the liver and runs through the pancreas
the pancreas has an auxiliary duct which empties into the duodenum
made up of Acinar Units
What units make up the endocrine pancreas?
islets of langerhans
Describe the innervation of the Pancreas:
has autonomic (sympathetic + parasympathetic) and visceral sensory fibers
Which nerve is responsible for parasympathetic innervation of the pancreas?
vagus nerve (these fibers reach the pancreas via the celiac plexus
What function does Parasympathetic Innervation have on the pancreas?
stimulates exocrine secretion (digestive enzymes)
promotes endocrine activity (insulin and glucagon release)
What nerves are responsible for sympathetic innervation of the pancreas?
nerve fibers originate from T5-T9 → travel via greater splanchnic nerves → synapse in celiac ganglia → postganglionic fibres supply pancreas through celiac plexus
What function does sympathetic innervation of the pancreas have?
inhibits pancreatic secretion
causes vasoconstriction of pancreatic blood vessels
What visceral innervation does the pancreas have?
pain fibers travel with sympathetic pathways back to spinal cord levels T5-T9
this explains referred pain from the pancreas to the epigastric region and sometimes the back
describe the celiac plexus
innervates the pancreas
integrates sympathetic and parasympathetic fibers
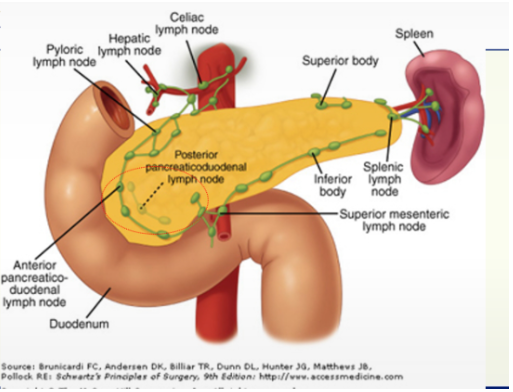
list the 7 lymph nodes found in the pancreas
superior mesenteric lymph node
splenic lymph node
pyloric lymph node
posterior pancreaticoduodenal lymph node
anterior pancreaticoduodenal lymph node
celiac
hepatic
What arteries supply the pancreas?
hepatic artery
splenic artery
superior pancreticoduodenal artery
inferior pancreaticoduodenal artery
describe the pathway of the superior pancreaticoduodenal arteries:
celiac trunk → gastroduodenal artery → superior pancreaticoduodenal arteries
where do the inferior pancreaticoduodenal arteries originate from?
branches of the superior mesenteric artery
which veins drain the pancreas?
splenic vein
hepatic portal vein
superior and inferior pancreatioduodenal veins
superior mesenteric vein
where do the Endocrine cells (islets of langerhans) of the pancreas originate from?
bud cells of the ‘trunk’ domain
endoderm
pancreatic epithelium → differentiation → islets cell clusters → islets of langerhans
where do the exocrine cells (acinar cells) originate from?
multipotent progenitor cells at the ‘tip’ domain
Describe the embryology of the pancreas:
arises from foregut (endodermal lining of duodenum) - around week 4-5
two buds form; dorsal develops first, then ventral
ventral bud rotates posteriorly around the duodenum and fuses with dorsal bud ~ week 7
duct systems also fuse
What structures arise from dorsal pancreatic bud?
upper part of head of pancreas
neck of pancreas
body
tail
What structures arise from ventral pancreatic bud/
associated with common bile duct
forms inferior part of pancreatic head
uncinate process
describe how Acinar cells are arranged in the exocrine pancreas:
acinar cells are arranged in grape-like clusters called acini
List 2 functions of ductal cells
ductal cells produce bicarbonate-rich fluid that neutralises stomach acid in the duodenum
they also deliver enzymes from acinar cells to the duodenum
where are ductal cells located?
lining the network of ducts within the exocrine pancreas
What receptors do Acinar cells have and why?
Acinar cells have CCK receptors
when CCK binds to these receptors → release of enzyme zymogens into small intestine
helps with digestion
What receptors do ductal cells have and why?
ductal cells have receptors for secretin
when secretin binds to receptors → increase in cAMP → activates protein kinases → pKA acts on Cl- channels
Cl- channels transport chloride out of cell
this gradient is used by another transporter → release of bicarbonate and water
What is the name for the chloride channels within ductal cells?
Cystic fibrosis transmembrane conductance regulator proteins
What function do CFTR proteins have in the pancreas?
regulate water balance and fluid secretion
ensures thin, non-viscous mucus
List 3 diseases of the exocrine pancreas:
chronic pancreatitis
acute pancreatitis
pancreatic cancer
What is Chronic Pancreatitis?
long-standing inflammatory disease of pancreas
irreversible structural damage; fibrosis and scarring
loss of exocrine and endocrine function
what is acute pancreatitis?
extreme inflammation of pancreatic cells → causes necrosis
endocrine failure → diabetes
exocrine failure → malabsorption of food
what is pancreatic cancer?
malignant tumor arising from the cells of the pancreas
most commonly from the exocrine ductal epithelium (at head of pancreas)
What causes pancreatitis on a cellular level?
Activation of trypsinogen into trypsin within the pancreas → caused by spike of calcium within Acinar cell
This causes cell damage, cytokine release, inflammation and necrosis → causes further trypsinogen proenzyme activation → active trypsin
explain exactly what happens when trypsinogen is activated to trypsin:
Release of calcium causes cathepsin B vesicles to join with the trypsinogen vesicles → activates trypsinogen to become trypsin → acute pancreatitis
What normally happens when this loop occurs in the pancreas in a healthy pancreas?
Body releases pancreatic enzyme inhibitors SPINK1/PSTI
This is a form of auto-regulation and inhibits trypsinogen from becoming activated and prevents the active trypsin from functioning.
I GET SMASHED:
I = idiopathic and hereditary
G = gallstones is the most common cause
E = ethanol (alcohol abuse)
T = trauma
S = steroids
M = mumps
A = autoimmune
S = scorpion stings
H = hyper - calcaemia, lippidaemia, thermia
E = ERCP
D = drugs
What happens in the exocrine pancreas in a patient with acute pancreatitis? (11)
increased CCK release
increased trypsinogen
decreased SPINK1
Acinar cell damage
decreased bicarbonate
decreased water
decreased pH
decreased flow
increased viscosity
proteolytic cleavage
protein plugs
What is the main cause of chronic pancreatitis?
alcohol
In what 2 ways can alcohol be metabolised and which one causes a calcium spike in Acinar cells?
oxidative metabolism
non oxidative metabolism; carboxylesterase converts alcohol to fatty acid ether esters → causes calcium spikes in pancreatic cells
what was the mortality rate of pancreatic cancer in 2000?
100%