Hematology (chapter 12)
1/19
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
20 Terms
Describe blood according to its tissue type and major functions.
Tissue Type: Liquid connective tissue.
Major Functions: 1) Transportation (gases, nutrients, hormones, wastes);
2) Regulation (maintaining body temp, pH, and fluid volume);
3) Protection (preventing blood loss via clotting and preventing infection via WBCs/antibodies).
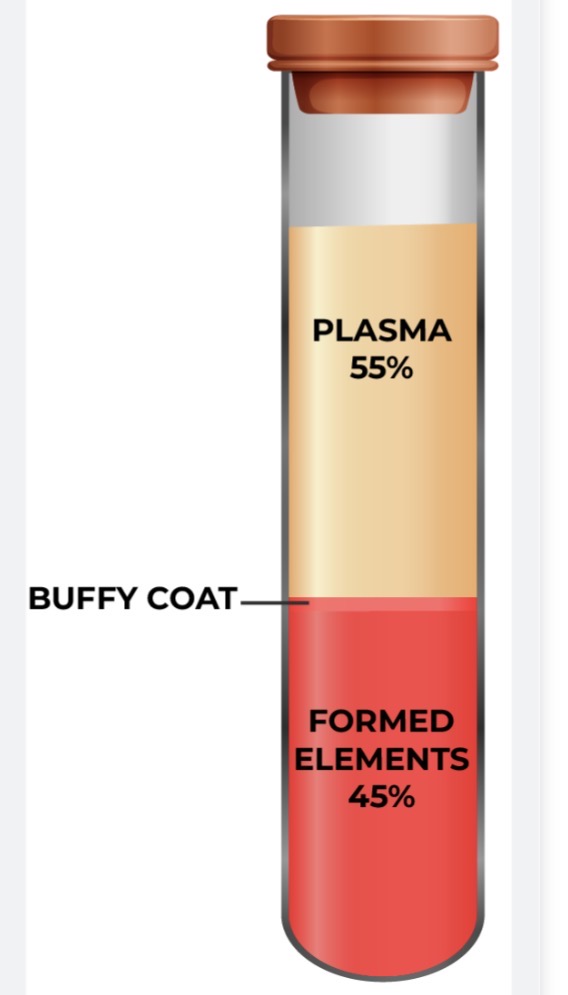
Name the two major components of blood and the percentage of each by weight.
1) Plasma (~55%): The liquid extracellular matrix.
2) Formed Elements (~45%): The cells and cell fragments (RBCs, WBCs, and platelets).
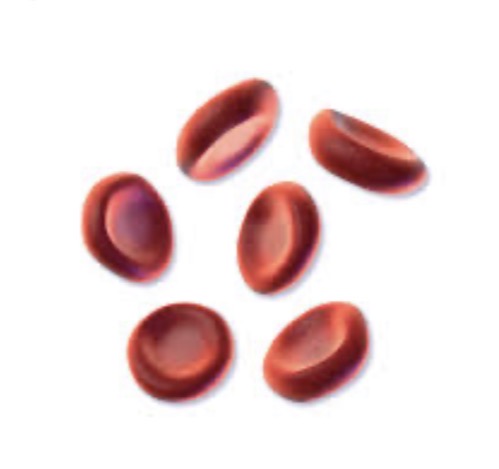
Give the common and scientific name for RBC, and describe its overall function and key characteristics.
Common Name: Red Blood Cell (RBC).
Scientific Name: Erythrocyte.
Function: Transport oxygen and carbon dioxide. Characteristics: Biconcave disc shape (increases surface area), enucleated (no nucleus), contains hemoglobin.
Give the common and scientific name for WBC, and describe its overall function and key characteristics.
Common Name: White Blood Cell (WBC).
Scientific Name: Leukocyte.
Function: Defense and immunity.
Characteristics: Complete cells with nuclei and organelles; far less numerous than RBCs.
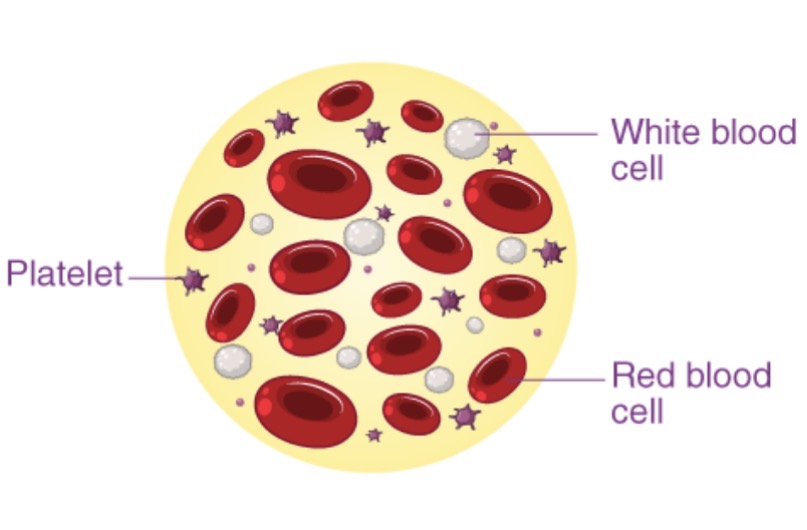
Give the common and scientific name for platelets, and describe its overall function and key characteristics.
Common Name: Platelets.
Scientific Name: Thrombocytes.
Function: Blood clotting (hemostasis). Characteristics:Cytoplasmic fragments of larger cells called megakaryocytes; no nucleus.
Explain why red blood cells have a relatively short life span.
Because they lack a nucleus and organelles, they cannot synthesize new proteins, grow, or repair damage. After ~120 days, they become rigid and fragile, eventually getting trapped and destroyed in the spleen or liver.
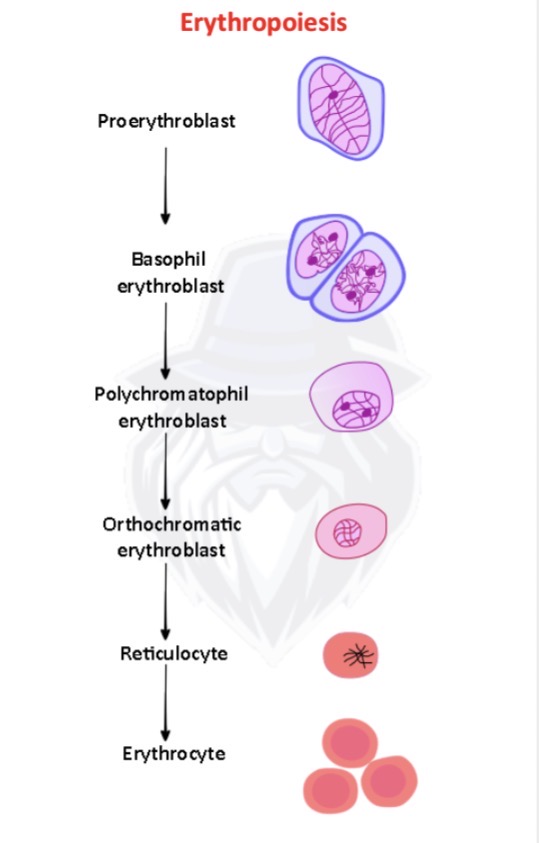
Discuss where erythropoiesis occurs in adults.
It occurs in Red Bone Marrow, specifically in the axial skeleton, girdles, and the proximal epiphyses of the humerus and femur.
What other factors are needed for red cell production?
Iron (for hemoglobin), Vitamin B12 and Folic Acid (for DNA synthesis), and Amino Acids (for globin chains).
Outline the negative feedback loop involving the hormone erythropoietin (EPO).
1) Stimulus: Hypoxia (low blood O2).
2) Sensor: Kidneys detect low O2 and release EPO.
3) Effector: EPO stimulates red bone marrow to increase RBC production.
4) Result: Increased RBC count raises blood O2 levels, which then shuts off EPO release.
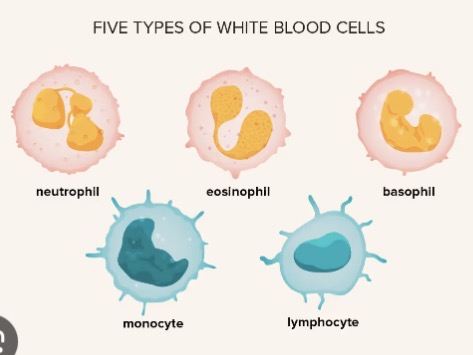
Distinguish between granulocytes and agranulocytes and name the leukocytes in each category.
Granulocytes: Contain visible cytoplasmic granules (Neutrophils, Eosinophils, Basophils). Agranulocytes: Lack visible cytoplasmic granules (Lymphocytes, Monocytes).
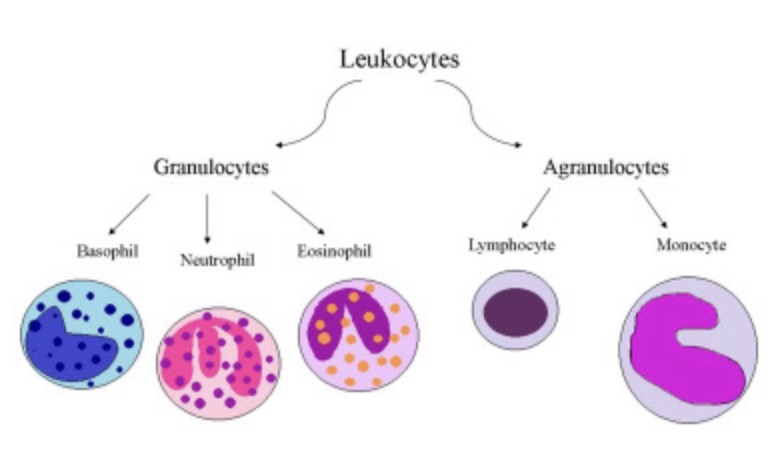
List the specific function for each leukocyte cell type (N.E.B.L.M.).
1) Neutrophils: Phagocytize bacteria.
2) Eosinophils: Kill parasitic worms; complex role in allergies.
3) Basophils:Release histamine (vasodilator) for inflammation.
4) Lymphocytes: Immune response via T-cells and B-cells (antibodies).
5) Monocytes: Turn into macrophages for long-term phagocytosis.
Outline and explain the three steps involved in hemostasis.
1) Vascular Spasm: Immediate vasoconstriction to reduce blood flow.
2) Platelet Plug Formation: Platelets stick to exposed collagen and each other to form a temporary seal.
3) Coagulation: Blood clotting; a cascade of factors results in a fibrin mesh that traps RBCs.
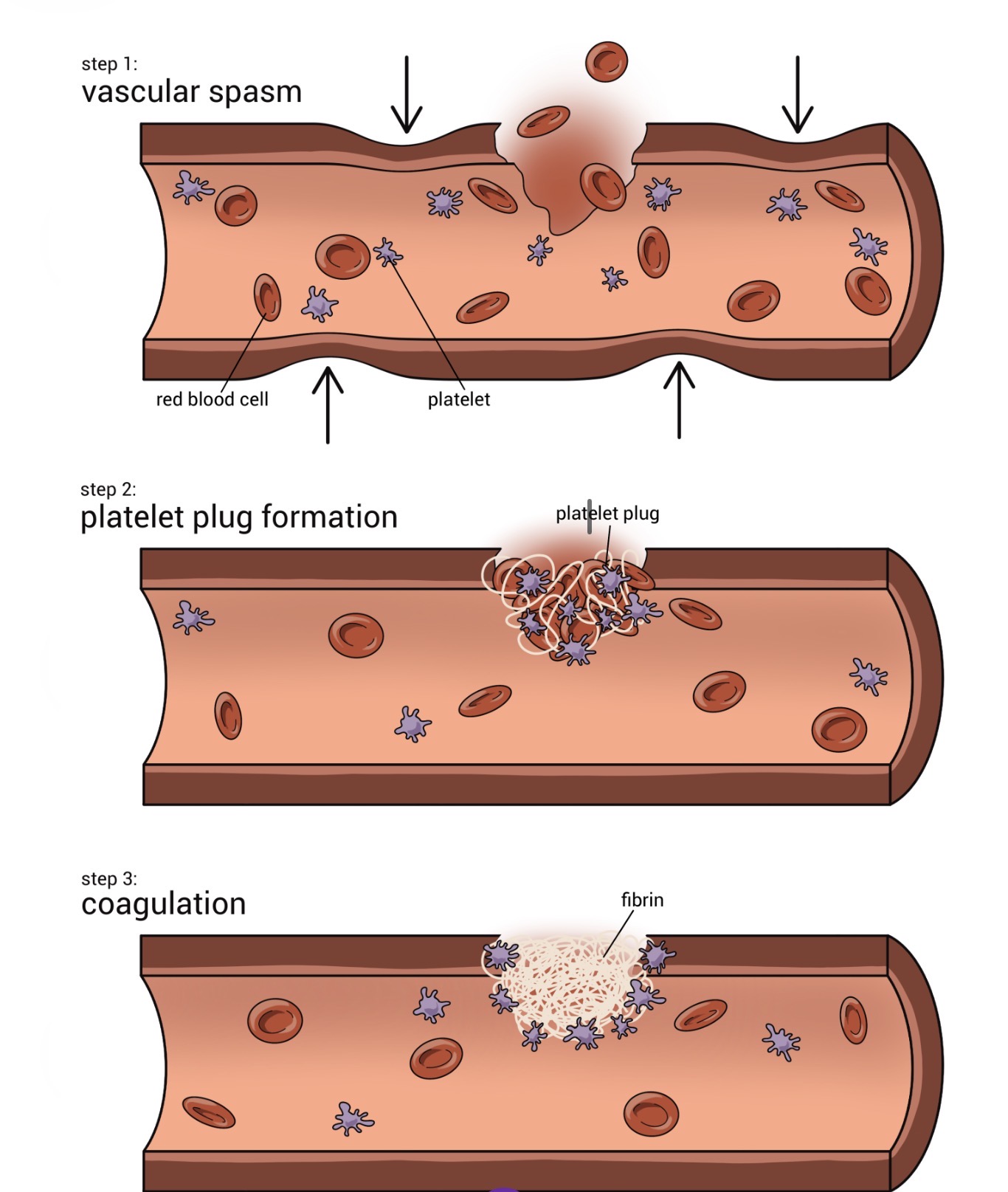
Name the 2 substances that platelets within a platelet plug release that causes further vasoconstriction of a vessel.
Serotonin and Thromboxane A2.
Describe the final step in blood coagulation.
Thrombin converts the soluble plasma protein Fibrinogen into insoluble Fibrin strands. These strands form a "net" that traps formed elements to create a solid clot.
Define the term agglutination.
The clumping of foreign cells (RBCs) induced by cross-linking of antigen-antibody complexes. Usually occurs during an incompatible blood transfusion.
Discuss blood typing (A, B, AB, O) in terms of antigens, antibodies, and compatibility.
Type A: A antigens / Anti-B antibodies / Compatible with A, O.
Type B: B antigens / Anti-A antibodies / Compatible with B, O.
Type AB: Both antigens / No antibodies / Compatible with A, B, AB, O.
Type O: No antigens / Both antibodies / Compatible with O only.
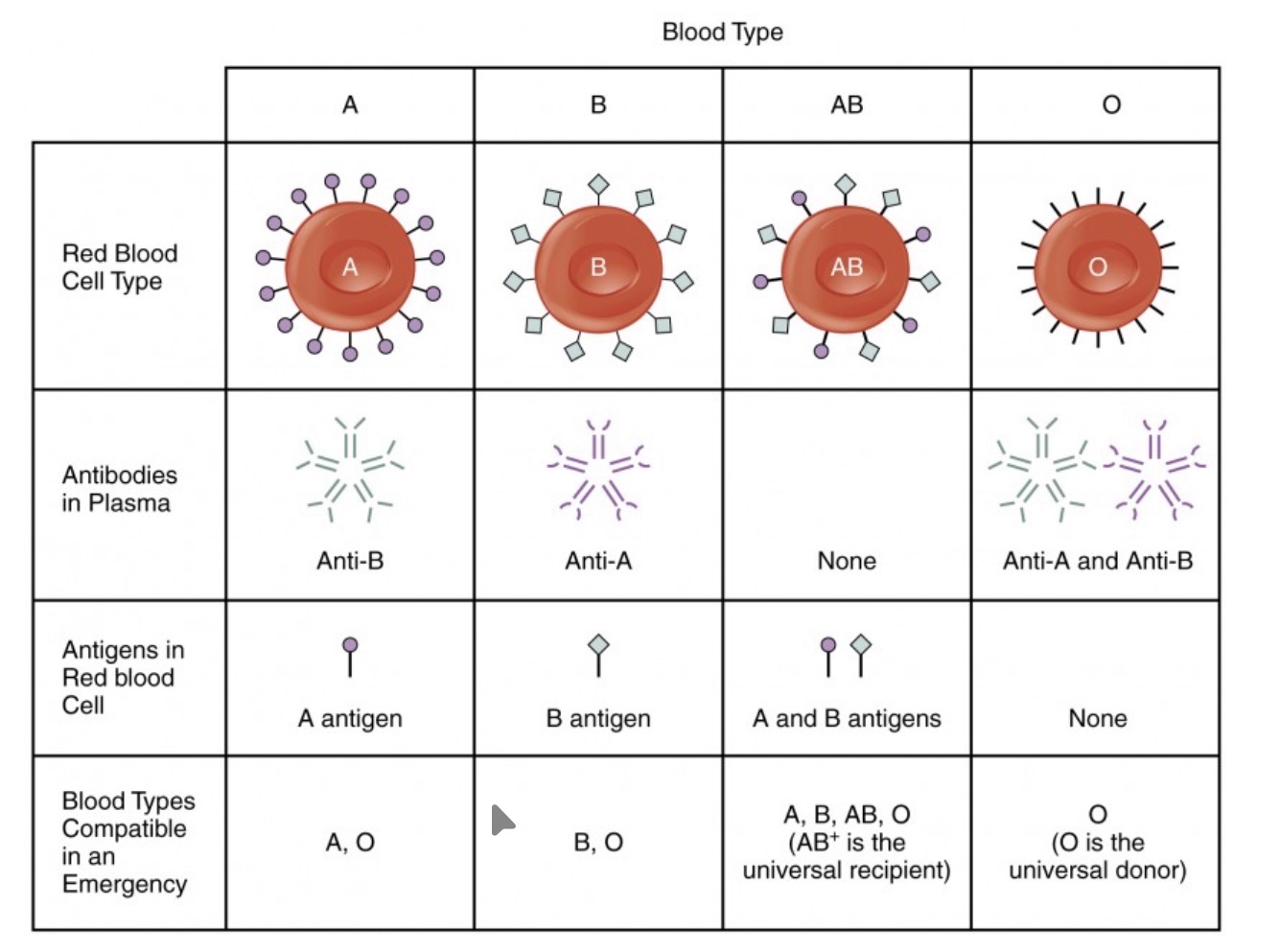
Identify the blood type considered the universal donor and the blood type considered the universal recipient.
Universal Donor: Type O (specifically O-), because it lacks A and B antigens. Universal Recipient: Type AB (specifically AB+), because it lacks Anti-A and Anti-B antibodies.