Pain, Perception, Neuroanatomy, and Neurophysiology
1/34
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
35 Terms



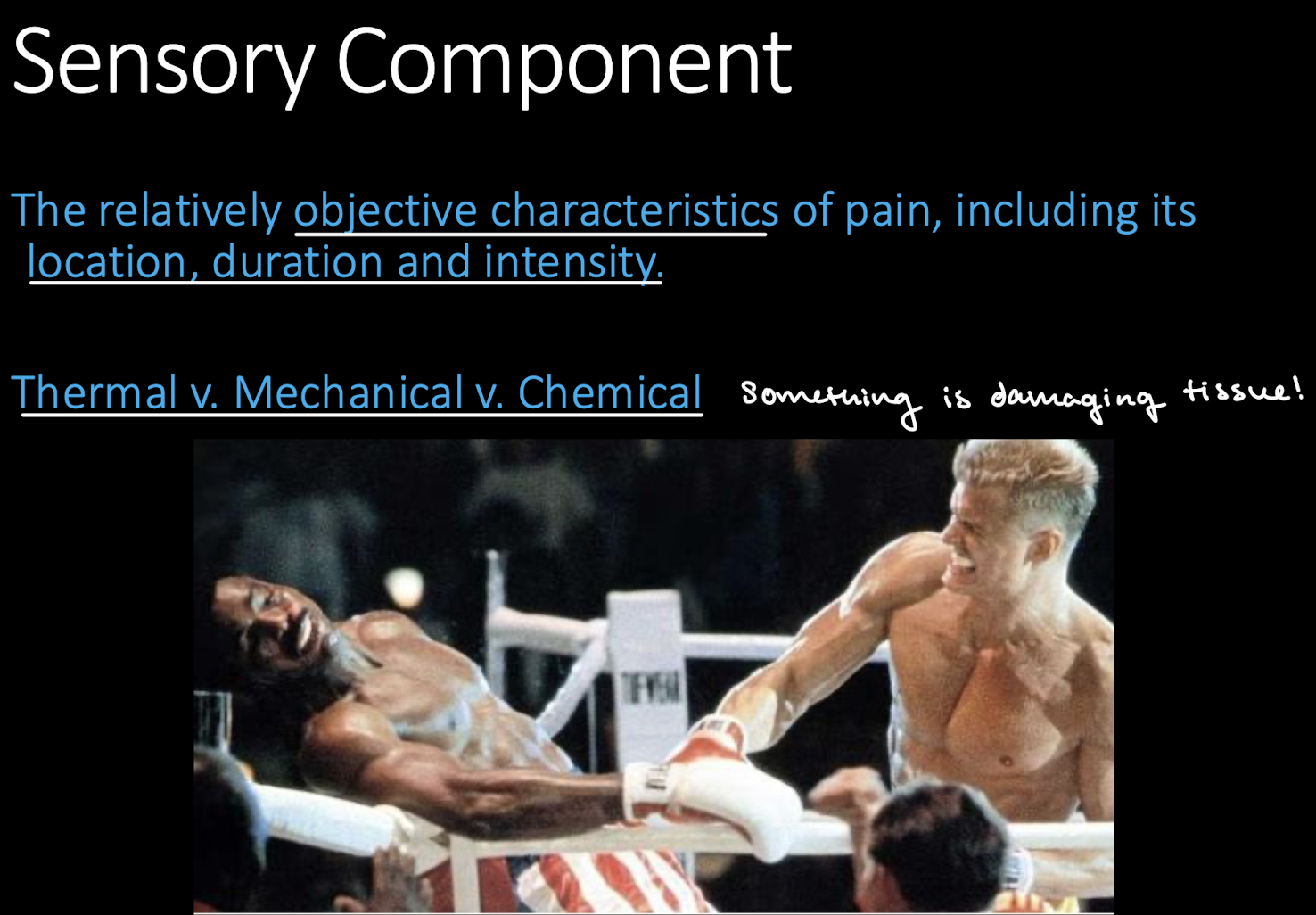


A drug that is used to decrease the sensation of pain

A dug that is used to abolish all sensation (blocking nociception is the primary goal)










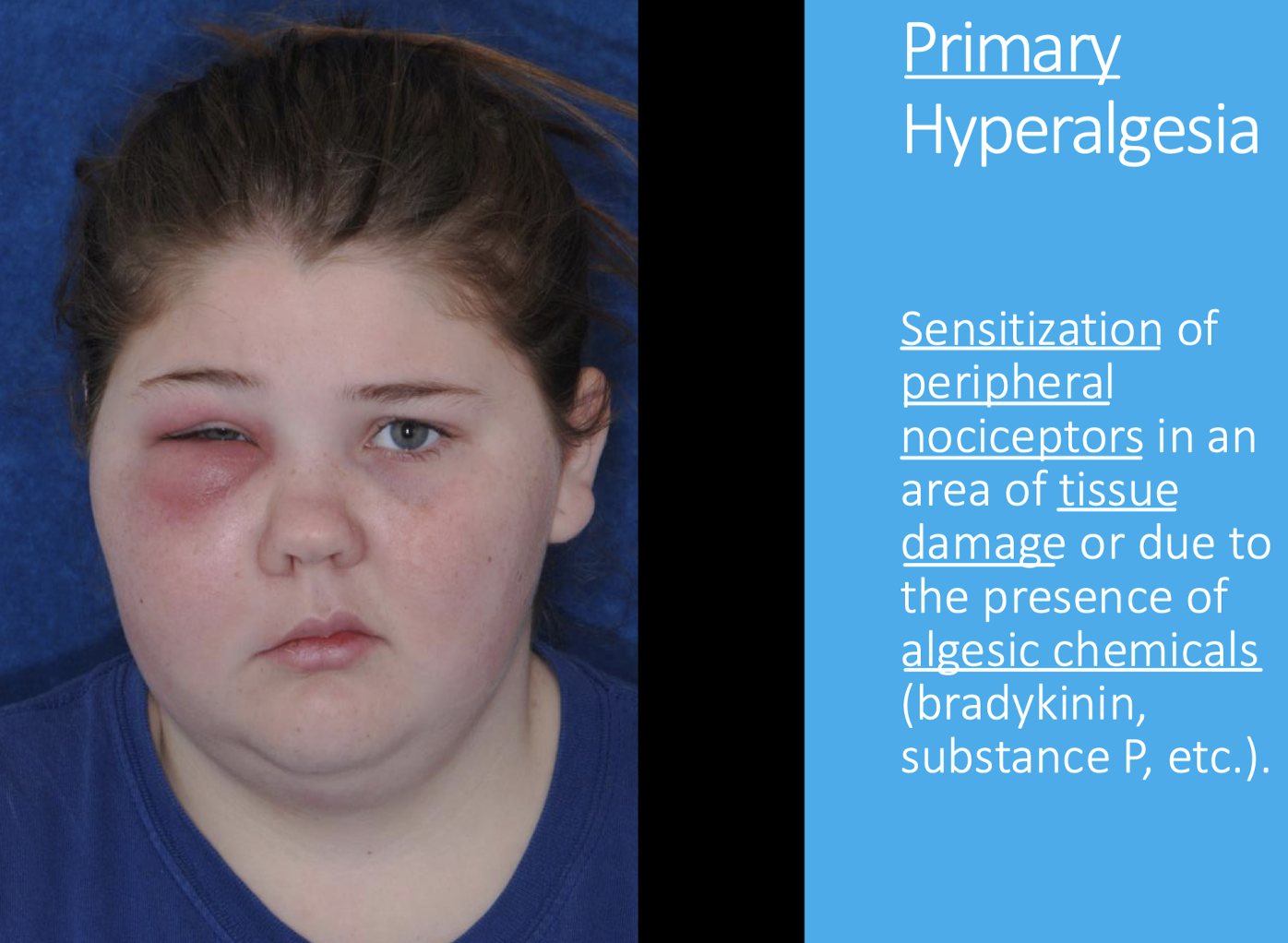


What is referred pain and convergence?
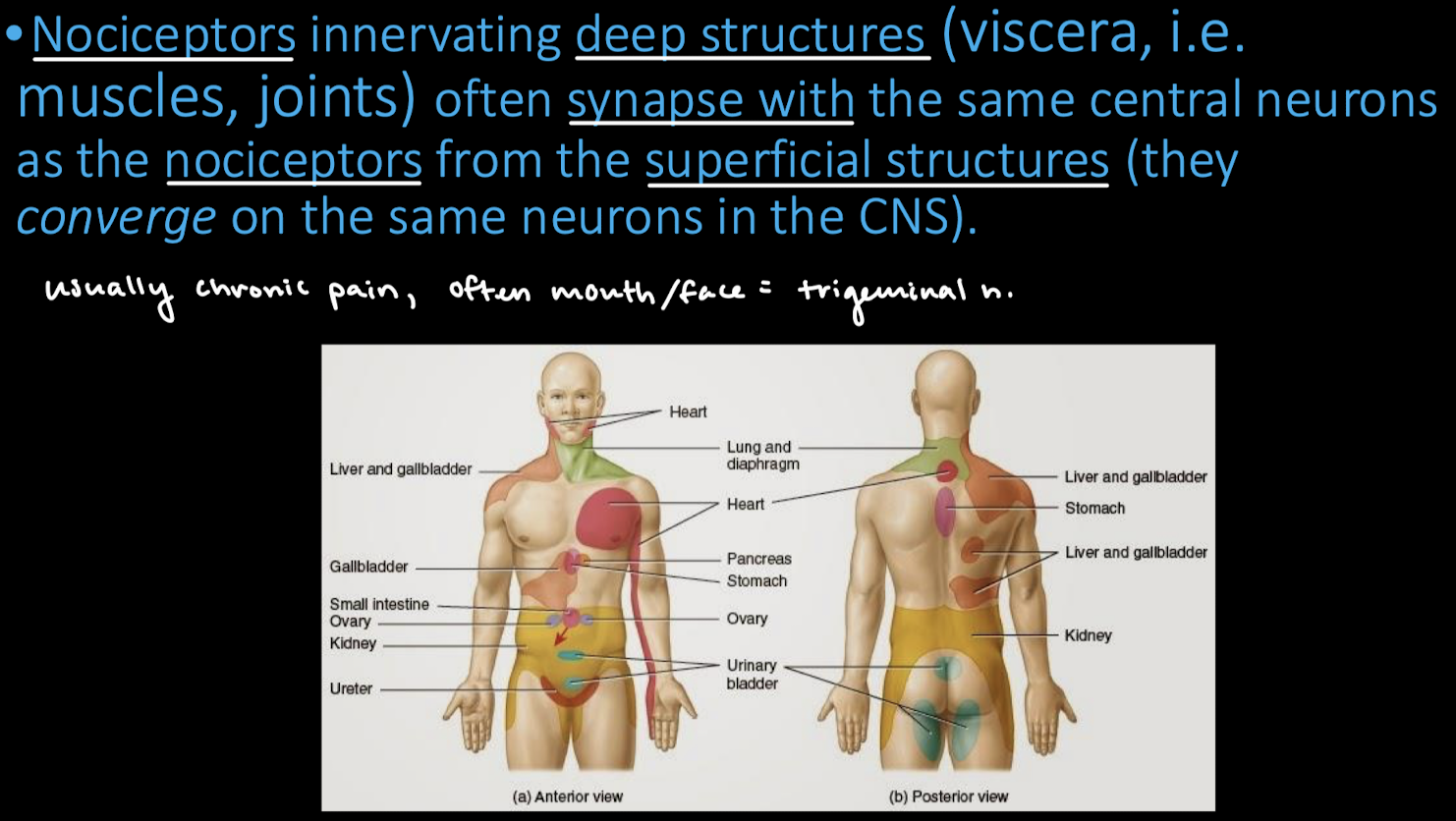


What is the part of the trigeminal nerve that receives pain fibers from oral cavity?
Pars oralis spinal trigeminal nucleus
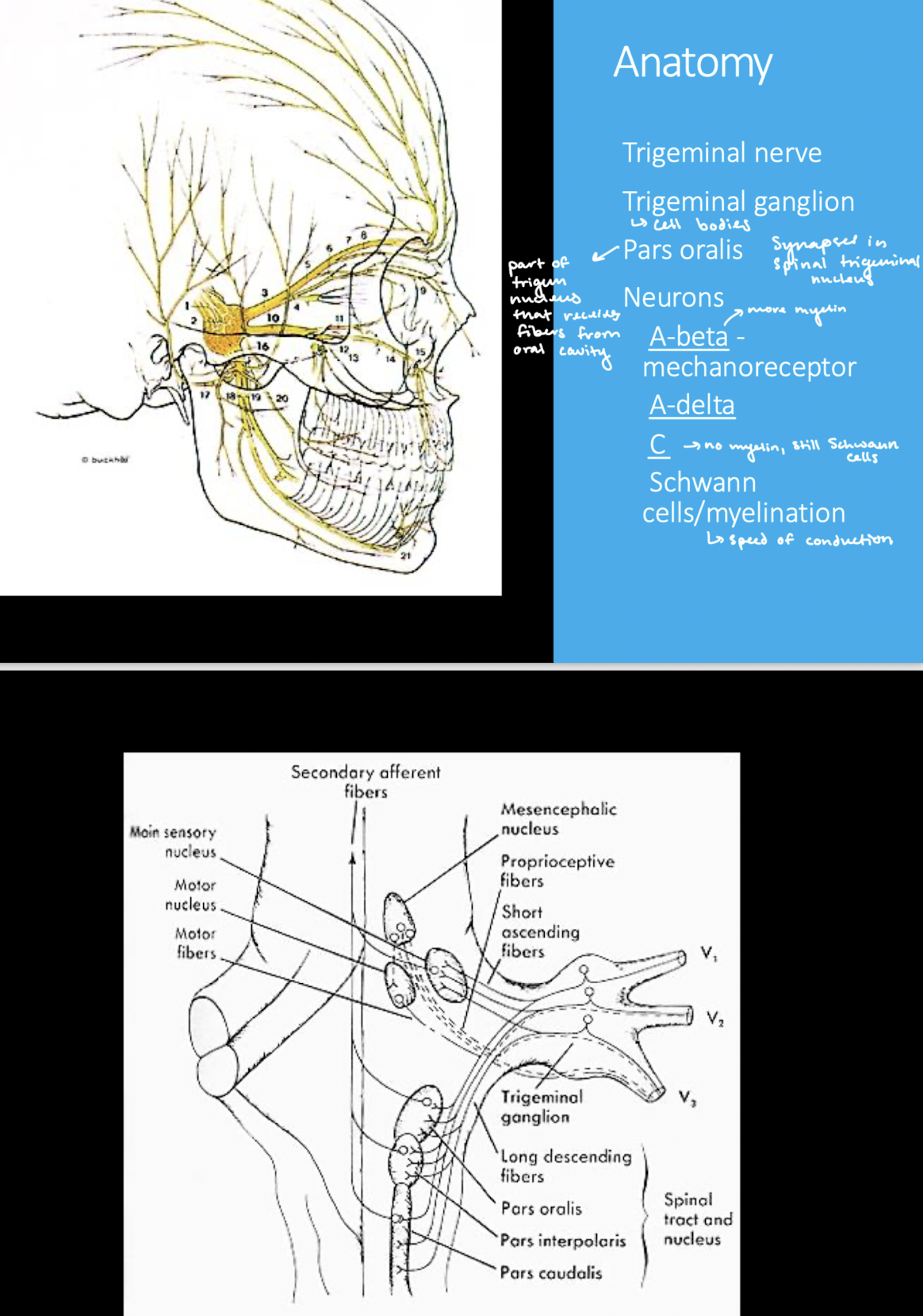
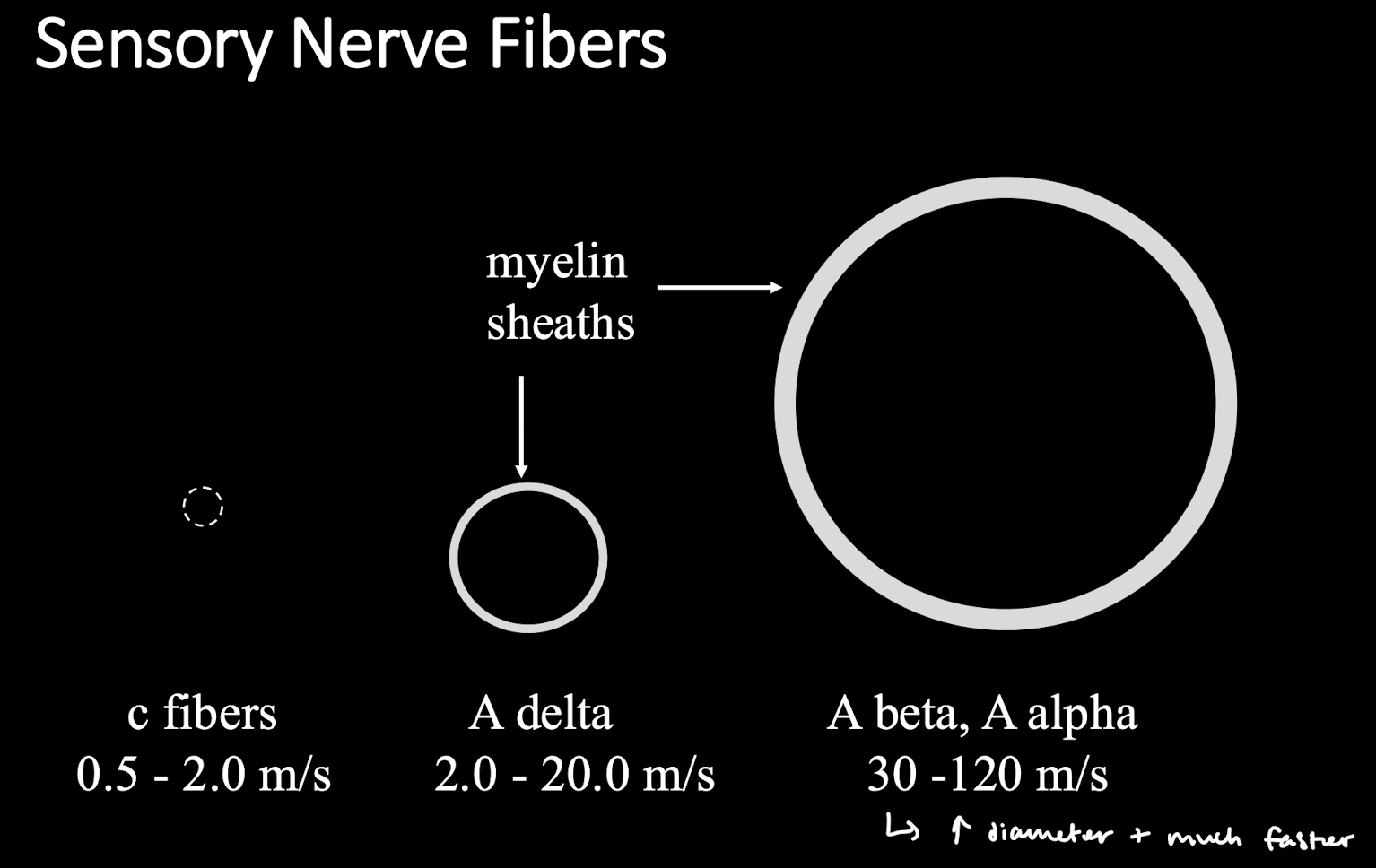
What are the different nerve fiber types? What does decreased diameter mean?

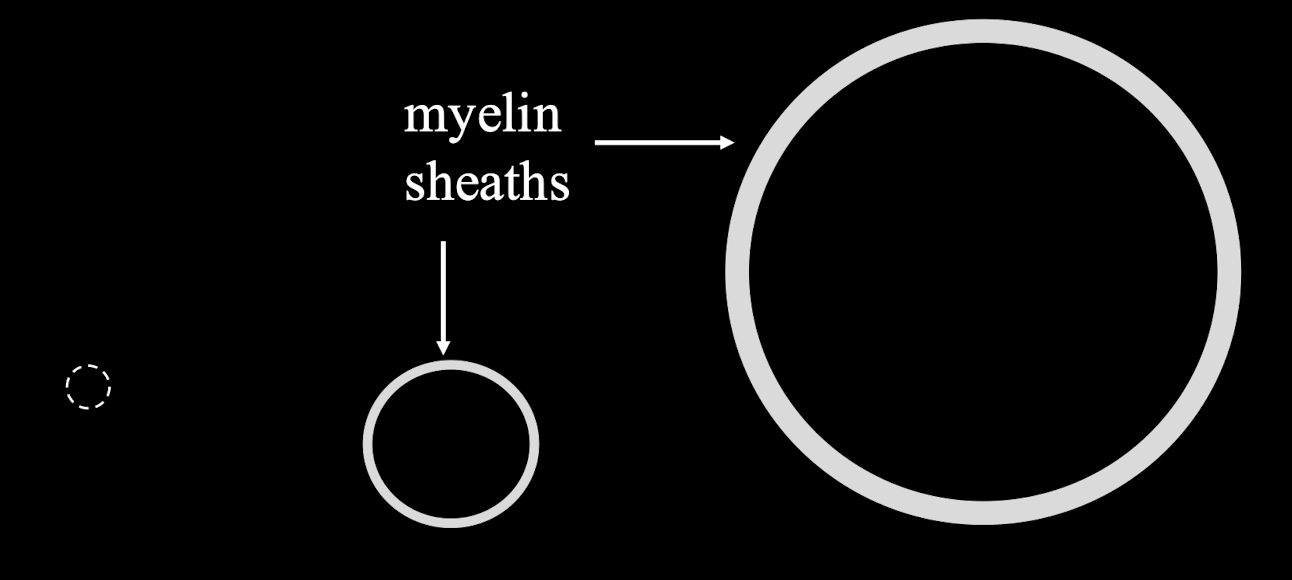
Label teh sensory nerve fiber types and know their general speeds/
Remember what impulse conduction entails.
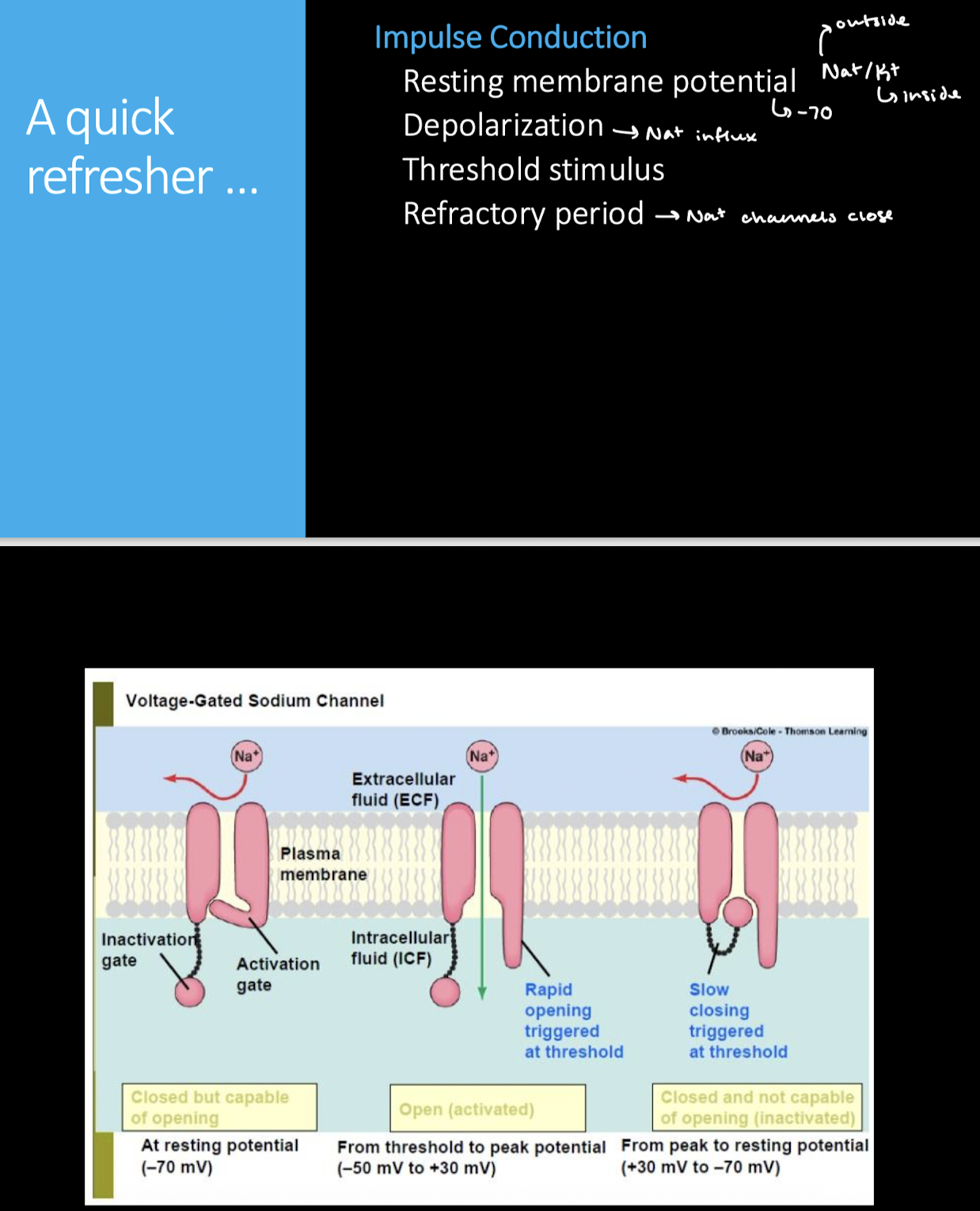
Immediately following an action potential, the neuron is unresponsive for a very brief period
Absolute refractory period
Absolute refractory period is followed by a period of time when a larger-than-normal depol is required to initiate a potential
relative refractory period
The equilibrium of a local anesthetic in solution depends on what two factors? What does this mean for time to effect?
The pKa of LA and pH of solution (H/H equation). Higher pKa takes longer to take effect

What is the mechanism of action of most LAs?
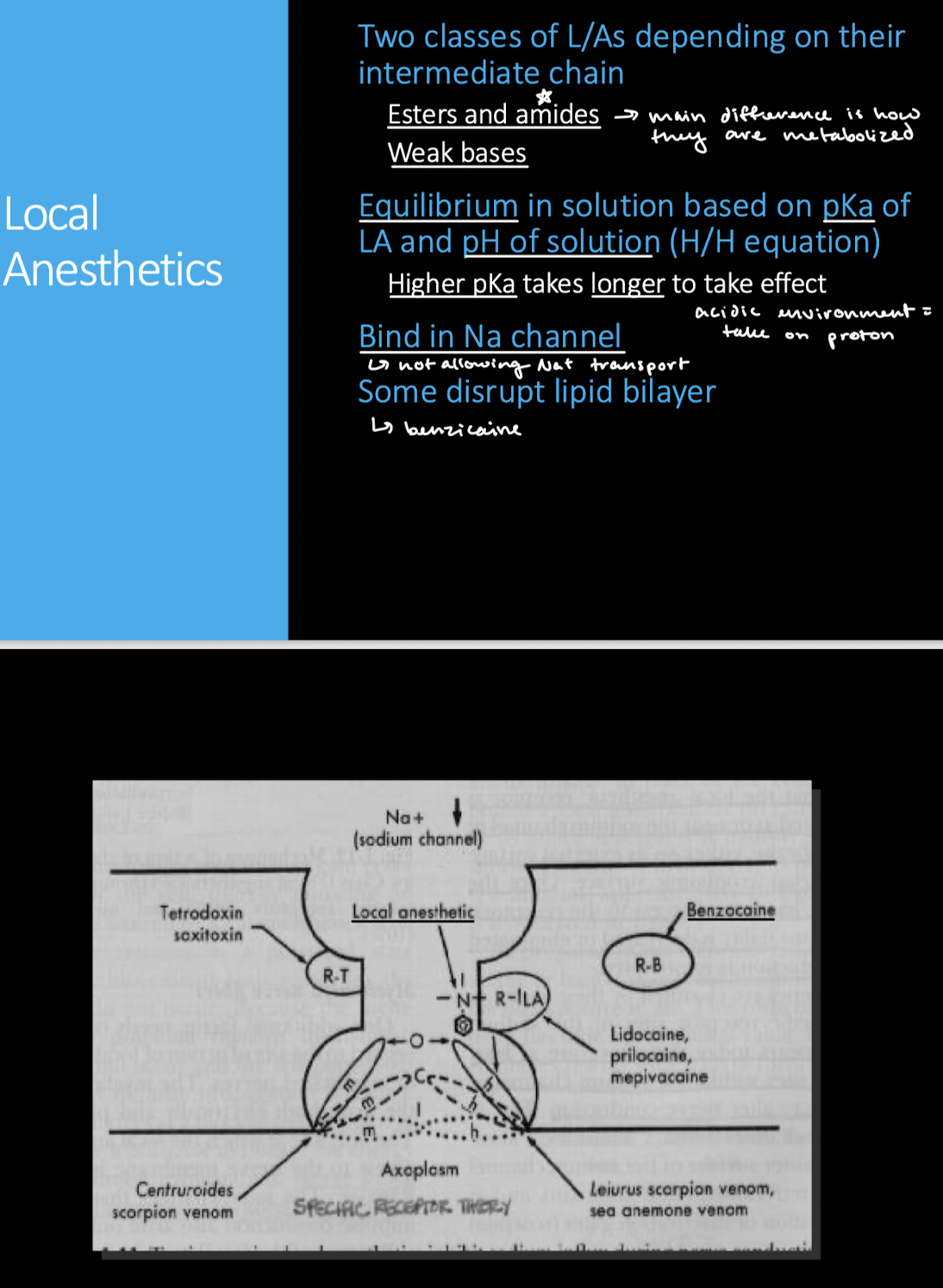
What forms of the LA are required for action?
Both uncharged and charged forms are required for action
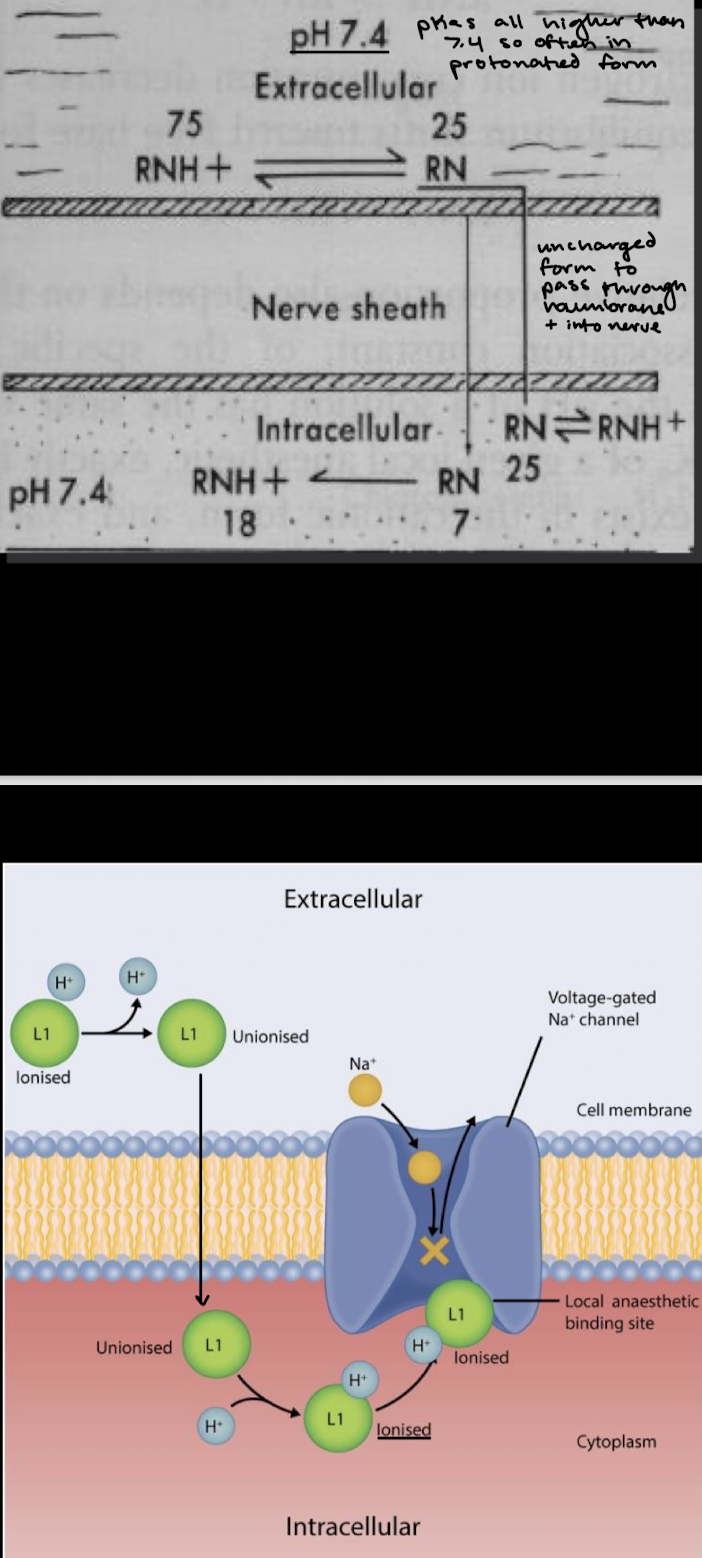
In an acidic environment, what is the main form of LA? What implications does this have clinically?
In an acidic environment, this pushes the LA toward its protonated form, so less uncharged LA will exist in that environment. This means that the LA can’t get intracellular/in the axon as easily, so the resulting blockade of APs (numbness) will be poor and possibly inadequate. This is often a problem when treating areas with infection.
What are the three main factors effecting LA action? What are the characteristics associated with these factors?

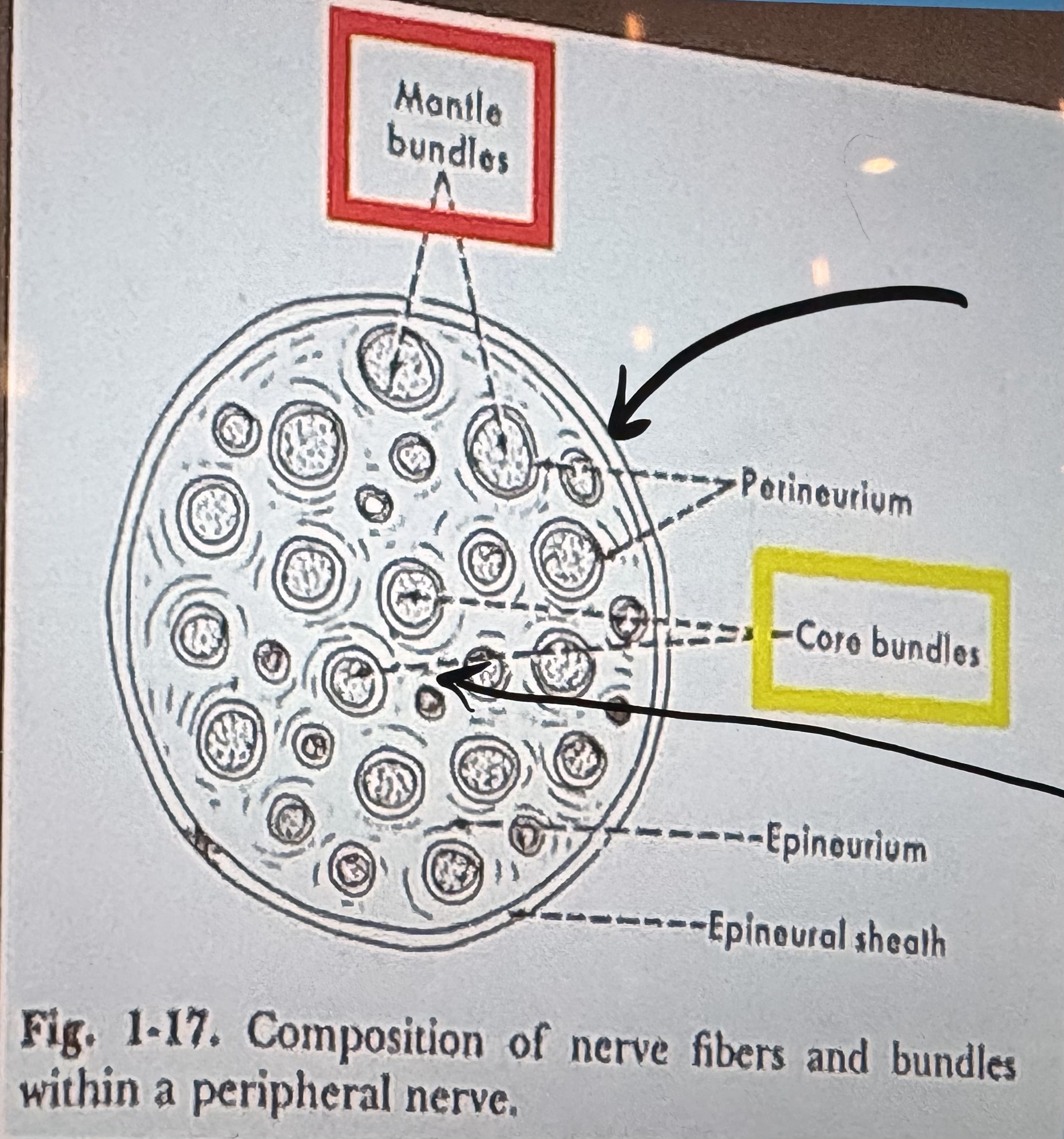
Definition 1: Some diffusion into surrounding tissues occurs.
Definition 2: Distributed throughout the body and can pass the BBB and placenta.

What are the ideal properties of LAs?

History of lOcal Anesthetics

What are the uses of local anesthetics?

How are ester LAs metabolized? What are some of the issues with esters?

How are amide LAs metabolized? Which can result in methemoglobinemia?
Prilocaine, articaine, and benzocaine for methemoglobinemia

What is methemoglobinemia?

What are the three ways to minimize the systemic actions on the CNS and CVS?

What are the initial signs of CNS effects from LAs and what is the ultimate outcome?

What are the effects of LAs on the CV system?

What are the best ways to avoid systemic toxicity?
