2.4 Cell recognition and the immune system
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
28 Terms
What is an antigen?
foreign molecule / protein / glycoprotein / glycolipid
that stimulates an immune response leading to production of antibody
How are cells identified by the immune system?
each type of cell has specific molecles on its surface (cell-surface membrane / cell wall) that identify it
often proteins → have a specific tertiary structure (or glycoproteins / glycolipids)
What types of cells and molecules can the immune system identify?
Pathogens (disease causing microorganisms) e.g. viruses, fungi, bacteria
cells from other organisms of the same species (e.g. organ transplants / blood transfusions)
abnormal body cells e.g. tumour cells or virus-infected cells
toxins (poisons) released by some bacteria
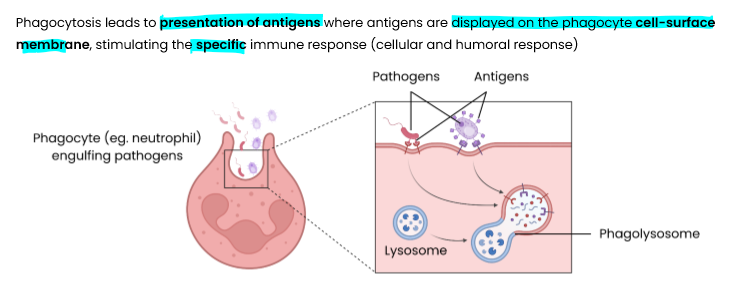
Describe phagocytosis of pathogens (non-specific immune response)
phagocyte attracted by chemicals/ recognises (foreign) antigen on pathogen
phagocyte engulfs pathogen by surrounding it with its cell membrane
pathogen contained in vesicle / phagosome in cytoplasm of phagocyte
lysosome fuses with phagosome and releases lysozymes (hydrolytic enzymes)
lysozymes hydrolyse / digest pathogen
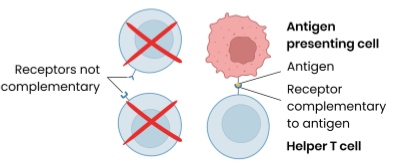
Describe the response of T lymphocytes to a foreign antigen (the cellular response)
T lymphocytes recognise (antigens on surface of) antigen presenting cells e.g. infected cells, phagocytes presenting antigens, transplanted cells, tumour cells etc
Specific helper T cells with complementary receptors (on cells surface) bind to antigen on antigen-presenting cell → activated and divide by mitosis to form clones which stimulate:
cytotoxic T cells → kill infected cells / tumour cells (by producing perforin)
specific B cells (humoral response)
phagocytes → engulf pathogens by phagocytosis
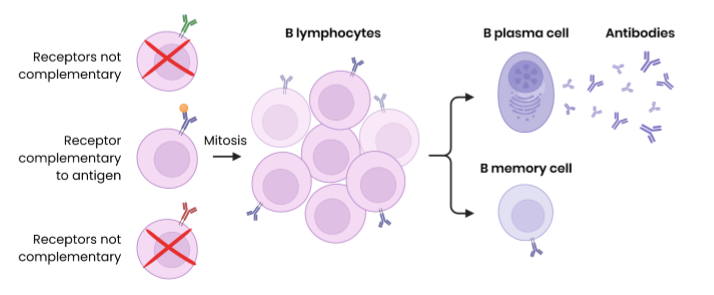
Describe the response of B lymphocytes to a foreign antigen (the humoral response)
B lymphocytes can recognise free antigens e.g. in blood or tissues, not just antigen presenting cells
Clonal selection:
specific B lymphocytes with complementary receptor (antibody on cell surface) binds to antigen
this is then stimulated by helper T cells (which releases cytokines)
so divides (rapidly) by mitosis to form clones
some differentiate into B plasma cells → secrete large amounts of (monoclonal) antibody
some differentiate into B memory cells → remain in blood for secondary immune response
NB - you must say that complementary receptors on B cell bind to antigen
What are antibodies?
quaternary structure proteins (4 polypeptide chains)
secreted by B lymphocytes e.g. plasma cells in response to specific antigens
bind specifically to antigens forming antigen-antibody complexes
Describe the structure of an antibody
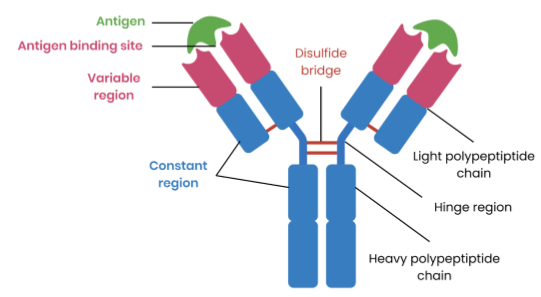
Explain how antibodies lead to the destruction of pathogens
antibodies bind to antigens on pathogens forming an antigen-antibody complex
→ specific tertiary structure so binding site / variable region binds to complementary region
each antibody binds to 2 pathogens at a time causing agglutination (clumping) of pathogens
antibodies attract phagocytes
phagocytes binds to the antibodies and phagocytose many pathogens at once
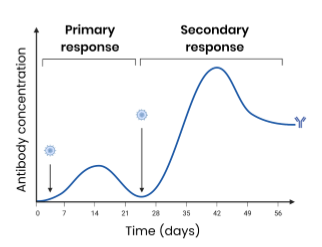
Explain the differences between the primary and secondary immune response
Primary - first exposure to antigen
antibodies produced slowly and at a lower concentration
takes time for specific B plasma cells to be stimulated to produce specific antibodies
memory cells produced
Secondary - second exposure to pathogen
antibodies produced faster and at a higher concentration
B memory cells rapidly undergo mitosis to produce many plasma cells which produce specific antibodies
What is a vaccine?
injection of antigens from attenuated (dead or weakened) pathogens
stimulating formation of memory cells
Explain how vaccines provide protection to individuals against disease
specific B lymphocyte with complementary receptor binds to antigen
specific T helper cell binds to antigen-presenting cell and stimulates B cell
B lymphocyte divides by mitosis to form clones
some differentiate into B plasma cells which release antibodies
some differentiate into B memory cells
on secondary exposure to the pathogen, B memory cells rapidly divide by mitosis to produce B plasma cells
these release antibodies faster and at a higher concentration
Explain how vaccines provide protections for populations against disease
herd immunity - large proportion of population vaccinated, reducing spread of pathogen
→ large proportion of population immune so do not become ill from infection
fewer infected people to pass pathogen on / unvaccinated people less likely to come into contact with someone with disease
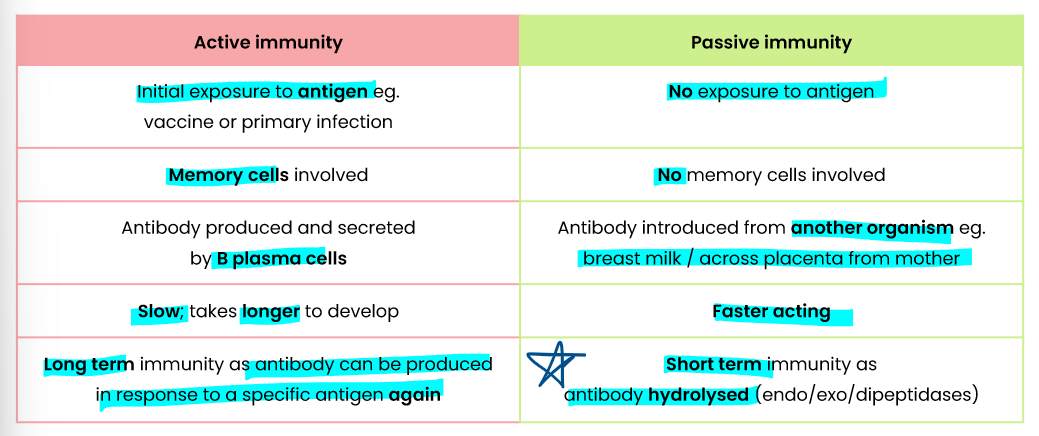
Describe the difference between active and passive immunity
Explain the effect of antigen variability on disease and disease prevention
antigens on pathogens change shape / tertiary structure due to gene mutations (creating new strains)
so no longer immune (from vaccine or prior infection)
→ B memory cell receptors cannot bind to / recognise changed antigen on secondary exposure
→ specific antibodies not complementary / cannot bind to changed antigen
(Example applications: yearly new flu vaccines developed, no vaccine for HIV, can catch a cold many times)
Describe the structure of a HIV particle
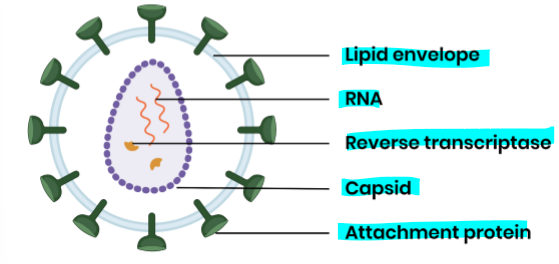
Describe the replication of HIV in helper T cells
HIV attachment proteins attach to receptors on helper T cells
lipid envelope fuses with cell-surface membrane, releasing capsid into cell
capsid uncoats, releasing RNA and reverse transcriptase
reverse transcriptase converts viral RNA to DNA
viral DNA inserted / incorporated into helper T cell DNA (may remain latent)
viral protein / capsid / enzymes are produced
a) DNA transcribed into HIV mRNA
b) HIV mRNA translated into new HIV proteins
virus particles assemble and released from cell (via budding)
Explain how HIV causes the symptoms of acquired immune deficiency syndrome (AIDS)
HIV infects and kills helper T cells (host cell) as it multiplies rapidly
→ so T helper cells can’t stimulate cytotoxic T cells, B cells and phagocytes
→ so B plasma cells can’t release as many antibodies for agglutination and destruction of pathogens
immune system deteriorates → more susceptible to (opportunistic) infections
pathogens reproduce, release toxins and damage cells
Explain why antibiotics are ineffective against viruses
Viruses do not have structures / processes that antibiotics inhibit:
viruses do not have metabolic processes (e.g. do not make protein) / ribosomes
viruses do not have bacterial enzymes / murein cell wall
What is a monoclonal antibody?
antibody produced from genetically identical / cloned B lymphocytes / plasma cells
so have same tertiary structure
Explain how monoclonal antibodies can be used in medical treatments
monoclonal antibody has a specific tertiary structure / binding site / variable region
complementary to specific receptor / protein / antigen associated with diagnosis
dye / stain / fluorescent marker attached to antibody
antibody binds to receptor / protein / antigen, forming antigen-antibody complex
In Specification:
targeting medication to specific cell types by attaching a therapeutic drug to an antibody
medical diagnosis
examples vary, e.g. pregnancy tests - you’ll need to interpret information in the question on how these work
Explain the use of antibodies in the ELISA (enzyme-linked immunosorbent assay) test to detect antigens
Example method 1 (direct ELISA):
attach sample with potential antigens to well
add complementary monoclonal antibodies with enzymes attached → bind to antigens in present
wash well → remove unbound antibodies (to prevent false positives)
add substrate → enzymes create products that cause a colour change (positive result)
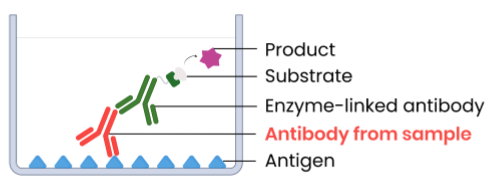
Example method 2 (sandwich ELISA):
attach specific monoclonal antibodies to well
add sample with potential antigens, then wash well
add complementary monoclonal antibodies with enzymes attached → bind to antigens if present
wash well → remove unbound antibodies (to prevent false positive)
add substrate → enzymes create products that cause a colour change (positive result)
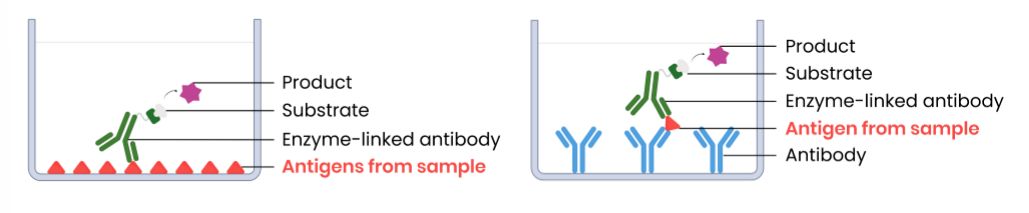
Explain the use of antibodies in the ELISA test to detect antibodies
Example method (indirect ELISA):
Attach specific anitgens to well
add sample with potential antibodies, wash well
add complementary monoclonal antibodies with enzymes attached → bind to antibodies if present
wash well → remove unbound antibodies
add substrate → enzymes create products that cause a colour change (positive result)
Suggest the purpose of a control well in the ELISA test
compare to test to show only enzyme causes colour change
compare to test to show all unbound antibodies have been washed away
Suggest why faiure to thoroughly wash the well can result in a flase positive in the ELISA test
antibody with enzyme remains / not washed out
so substrate converted into colour product
Discuss some general ethical issues associated with the use of vaccines and monoclonal antibodies
pre-clinical testing on / use of animals - potential stress / harm / mistreatment
→ but animals not killed and helps produce new drugs to reduce human suffering
clinical trials on humans → potential harm / side effects
vaccines - may continue high risk activities and still develop / pass on pathogen
use of drug - potentially dangerous side-effects
Suggest some points to consider when evaluating methodology relating to the use of vaccines and monoclonal antibodies
was the sample size large enough to be representative?
were participants diverse in terms of age, sex, ethnicity and health status?
were placebo / control groups used for comparison?
was the duration of the study long enough to show long-term effects?
was the trial double-blind (neither doctor / patient knew who was given drug or placebo) to reduce bias?
Suggest some points to consider when evaluating evidence and data relating to the use of vaccines and monoclonal antibodies
what side effects were observed, and how frequently did they occur?
was a statistical test used to see if there was a significant difference between start and final results?
was the standard deviation of final results large, showing some people did not benefit?
did standard deviation of start and final results overlap, showing there may not be a significant difference?
what dosage was optimum? does increasing dose increase effectiveness enough to justify extra cost?
was the cost of production and distribution low enough?