Pathogen Evasion Mechanisms: Serotypes, Antigenic Drift, and Immune System Strategies
1/12
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
13 Terms
What are serotypes and how does this relate to pathogen evasion?
-Each serotype has a unique surface structure (like a different “coat”) that the immune system recognizes as foreign.
-The body produces specific antibodies against those surface antigens.
Immunity to one serotype does not protect against others.
-By having many serotypes (like Streptococcus pneumoniae’s 100+), the pathogen can dodge immune memory — an antibody that recognizes serotype A won’t recognize serotype B.
serotypes are like the "types" of pathogen
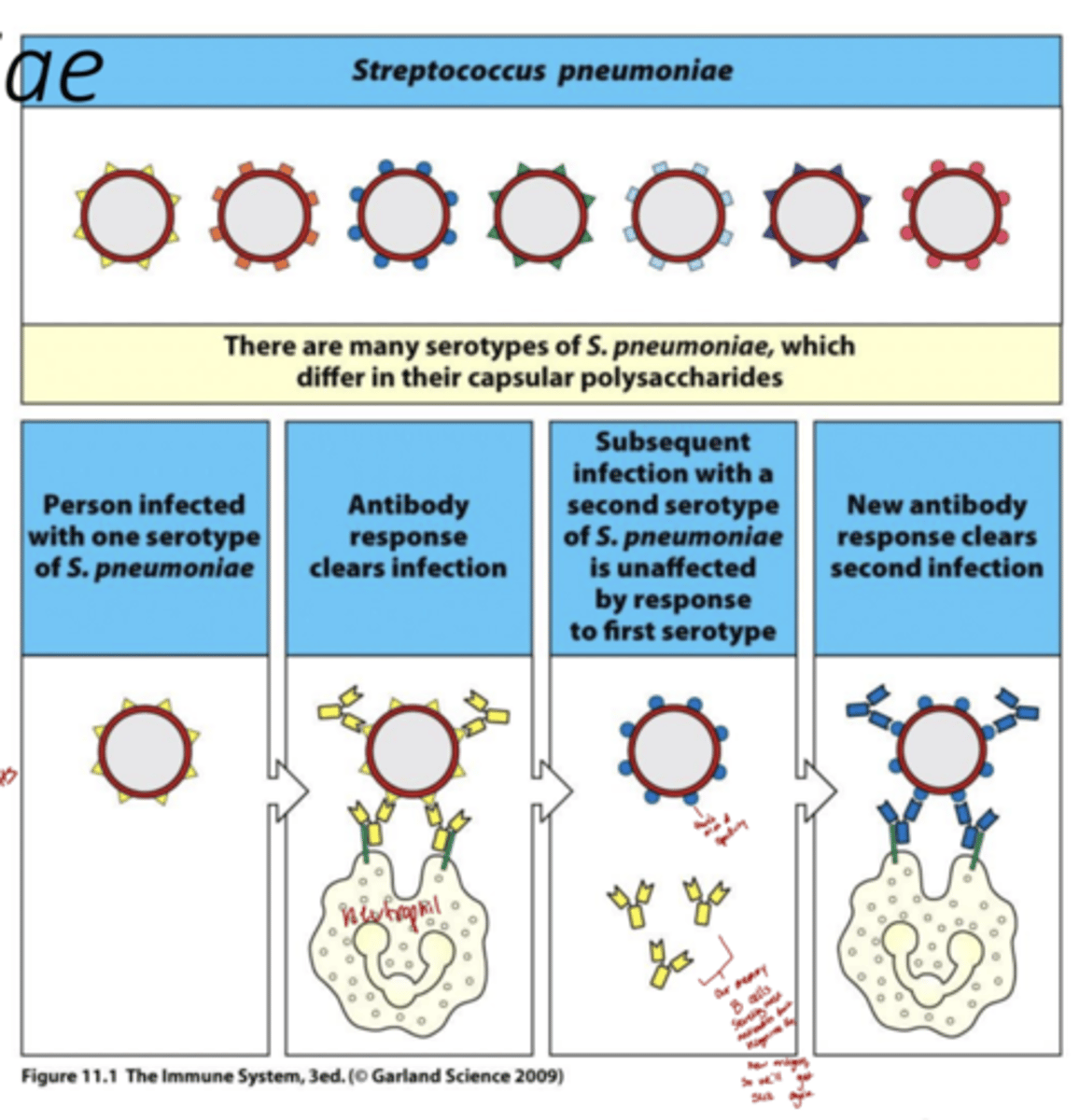
How do serotypes affect vaccine production?
-This makes it hard to create broad, lasting vaccines, since immunity is serotype-specific.
The pathogen can continue circulating in the population by switching serotypes that are not covered by vaccines or prior infections.
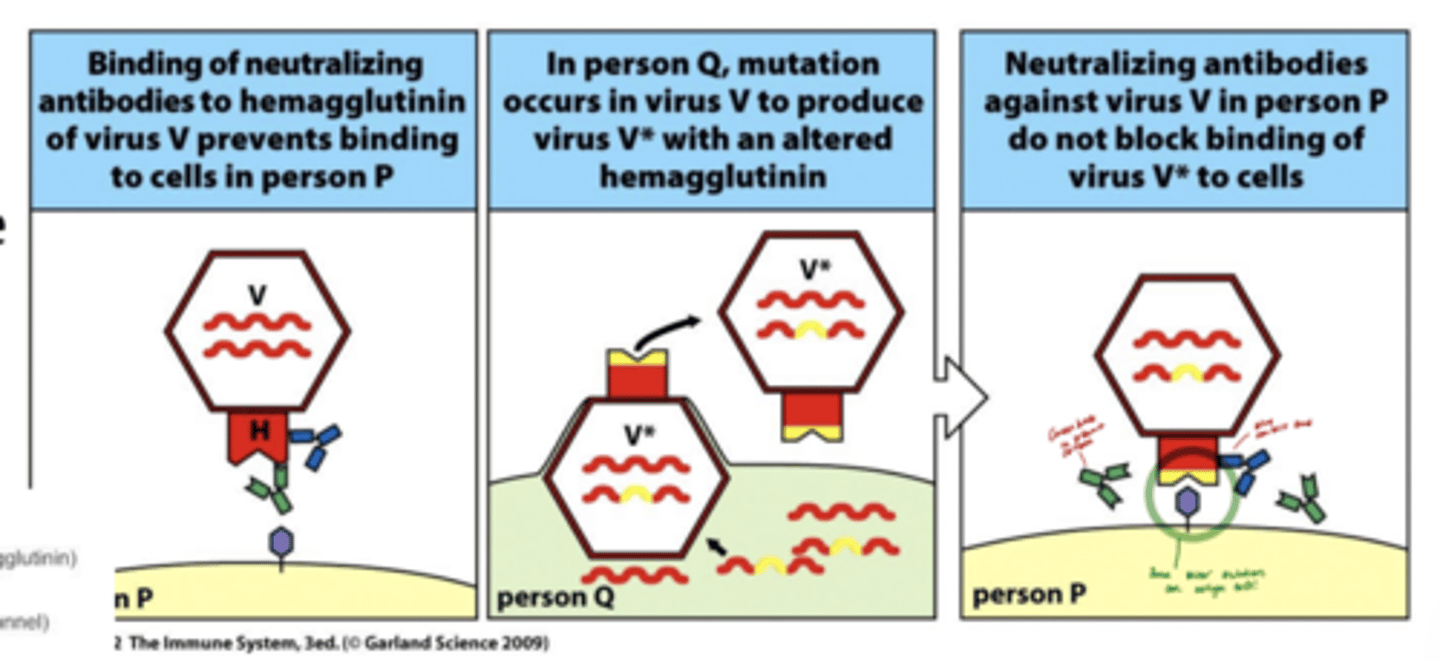
how does antigenic drift relate to pathogen evasion
-Pathogens can change their DNA,Antigenic drift = slow, continuous changes in antigen structure due to random mutations.Over time, the altered antigens are no longer well-recognized by pre-existing antibodies.
-Antigenic drift helps pathogens evade immunity by making small, gradual changes to their surface antigens — allowing them to “stay one step ahead” of the immune system.
in the picture notice how the pathogen mutates to have the yellow piece which prevents antibodies from neutralizing it
another example is how viruses can trasmit to other species, mutate, then come back to the original species and the host will not have the antibodies to defend itself.
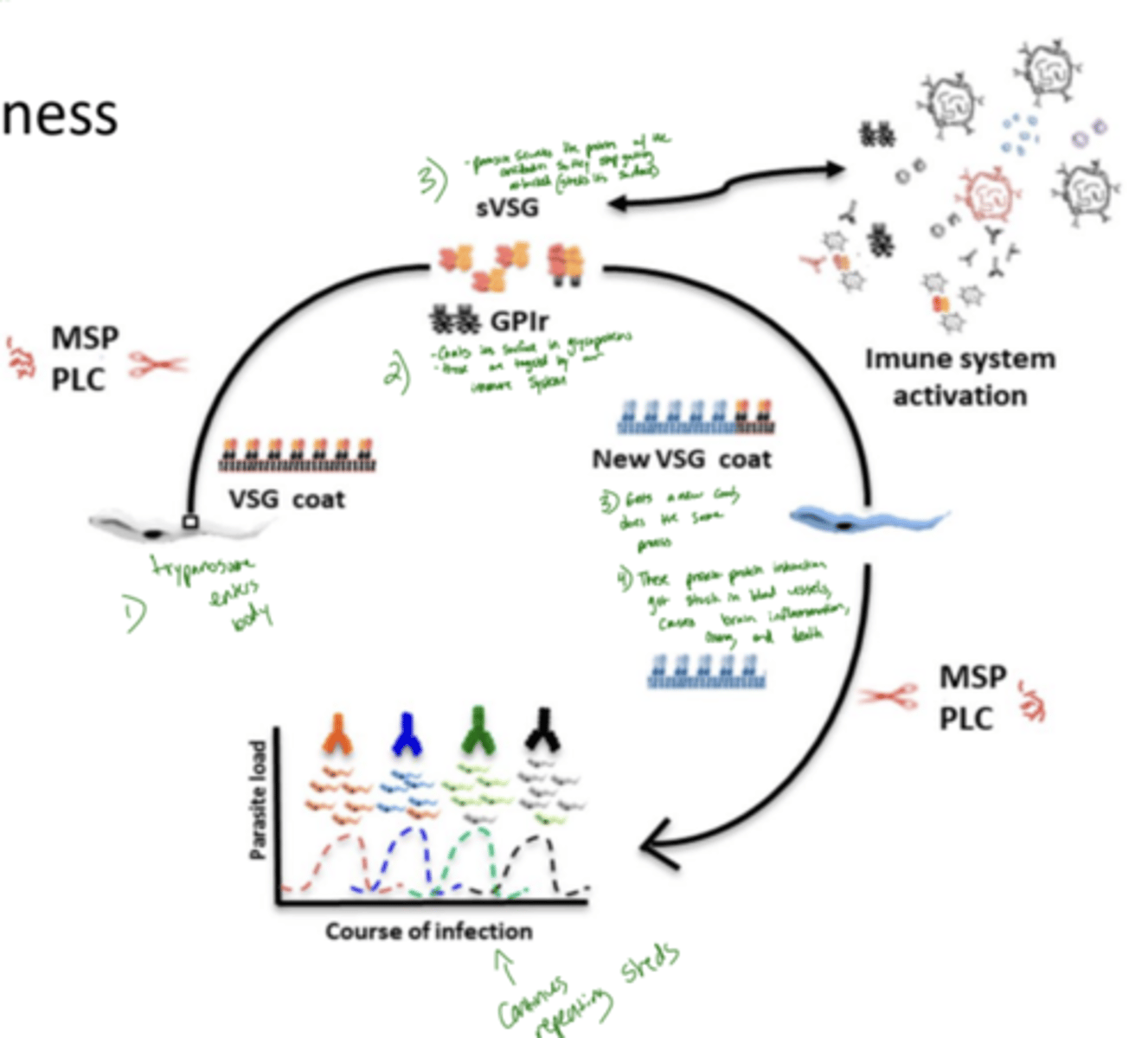
what is Gene rearrangement in Trypanosomes and how does it relate to pathogen evasion
The organism changes which gene is turned on so it can make a different surface protein and trick the immune system.
It’s like the parasite keeps changing its outfit every time the immune system starts recognizing it — ensuring it can survive and continue infecting the host.
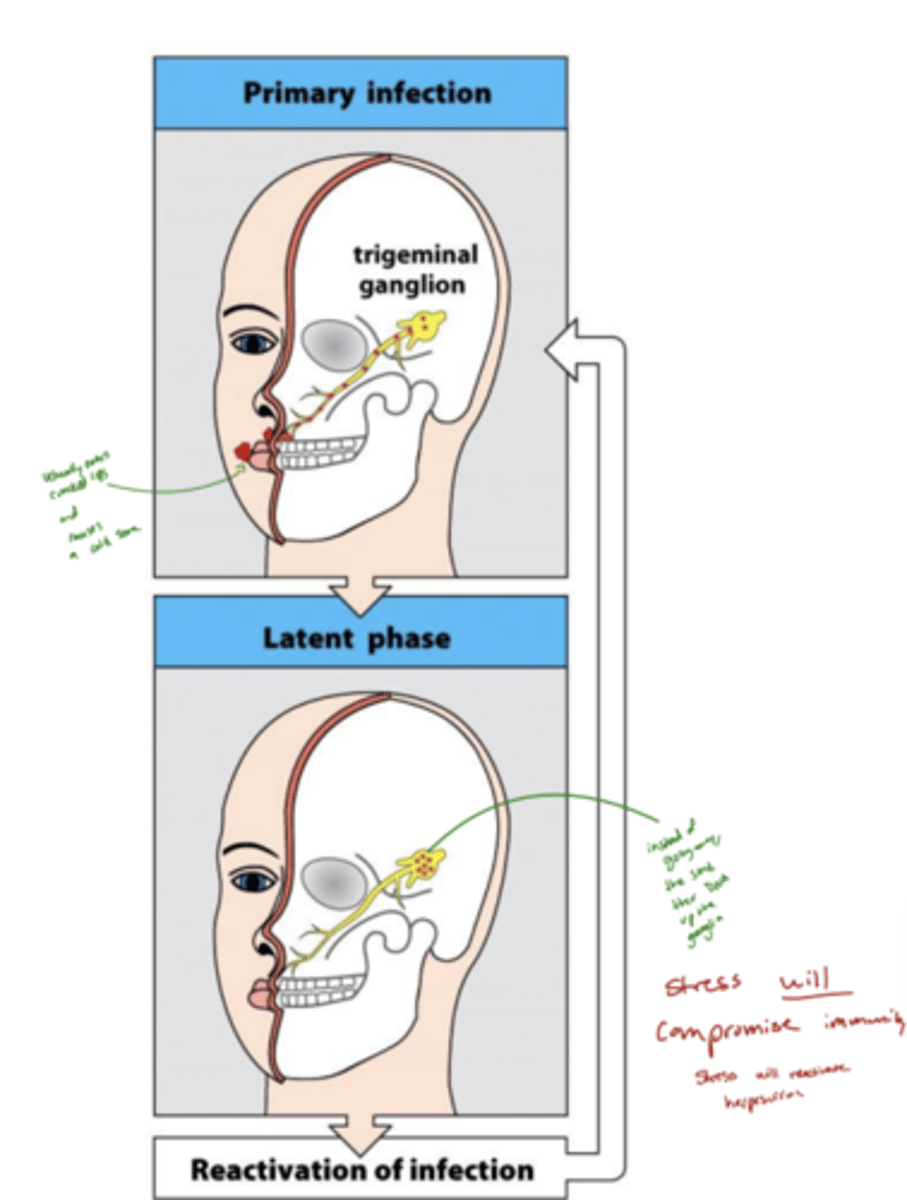
what is latency in herpes virus and how does it relate to pathogen evasion
After the first infection, the herpes virus doesn’t get completely removed by your immune system.
Instead, it hides inside certain cells (like nerve cells) where the immune system can’t easily detect it.
While it’s hiding, the virus stops making most of its proteins, so the immune system has nothing to recognize or attack.
Later, the virus can “wake up” (reactivate) due to stress, illness, sunlight, or a weak immune system.
It then starts replicating again and causes cold sores, genital sores, or other symptoms — depending on the type of herpes virus.
why do we need Th1 cells for pathogens like mycobacterium tuberculosis
Th1 cells are essential for fighting TB because they activate macrophages with IFN-γ, helping contain and kill the bacteria that hide inside those very cells.
in the first pic, the bacteria hides in the mac and destroys the phagolysosome so it kills the mac
see how in the second pic the bacteria is hiding inside the mac, and the Th1 binds to make ROR and Nitric oxide to promote phagocytosis
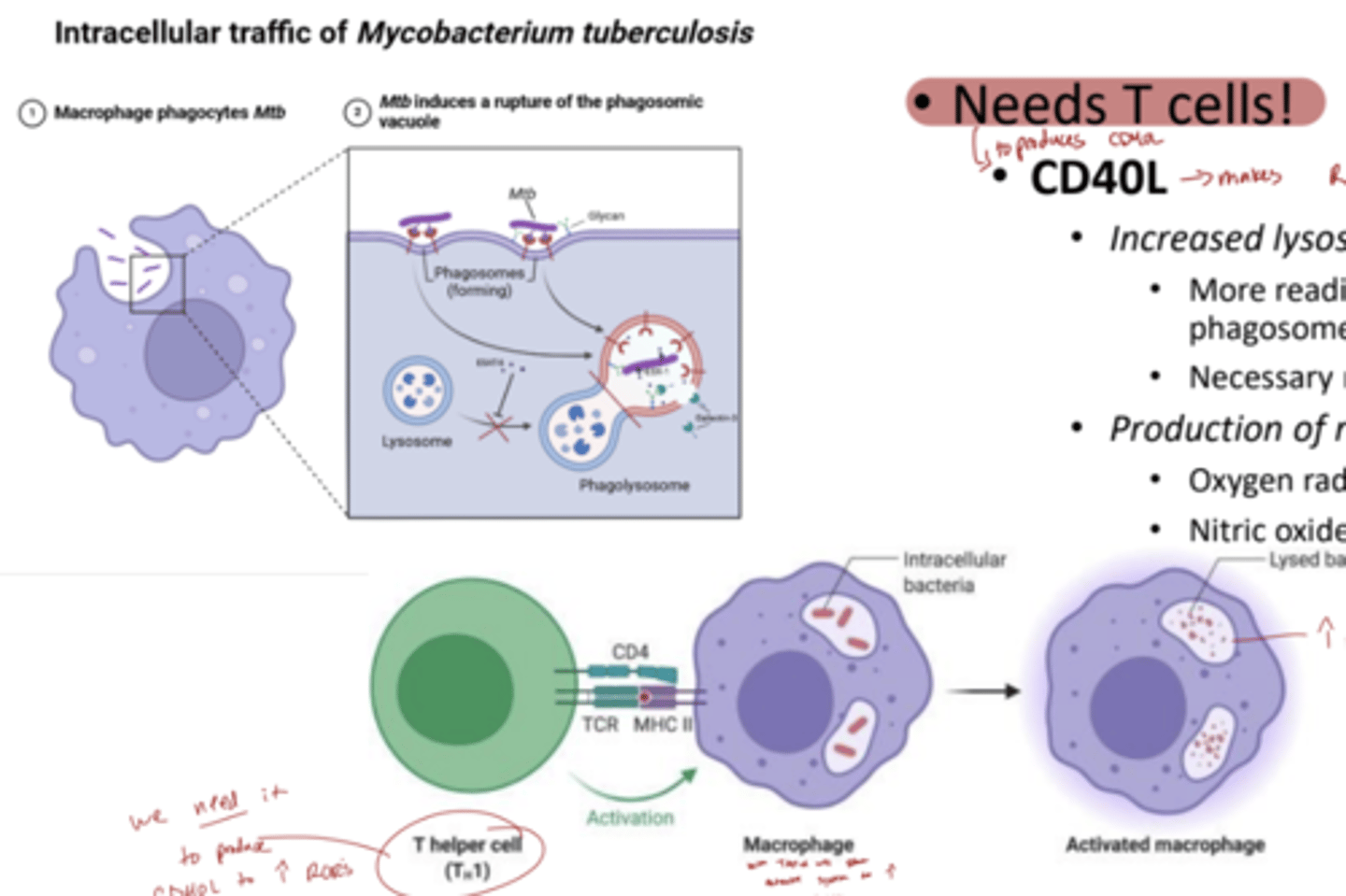
what do Th1 cells do?
the produce Cd40L which makes ROS and nitric oxide to kill (phagocytose)
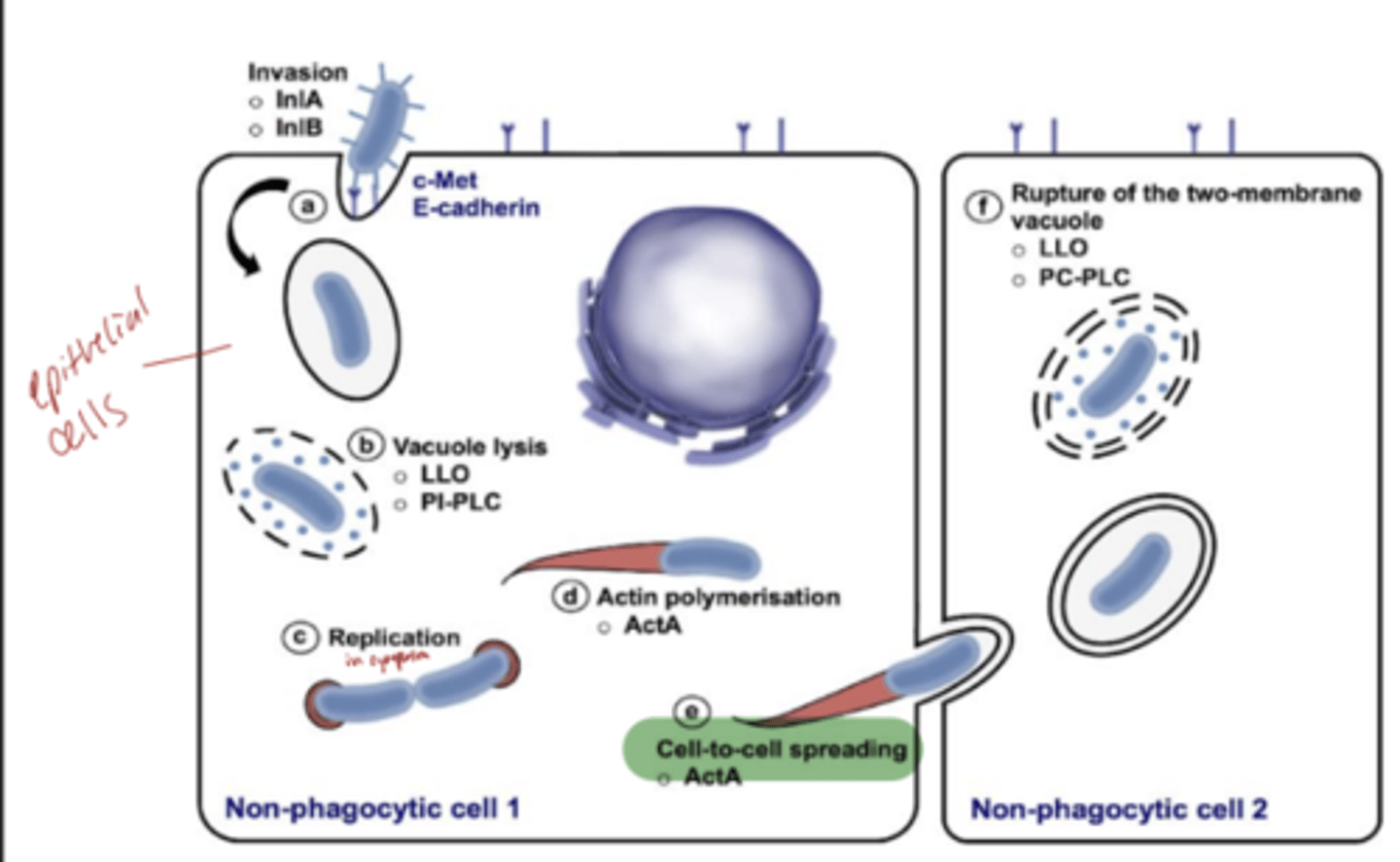
how does Listeria monocytogenes relate to pathogen invasion, include TH1 early and CTL late and what that means
Listeria is a bacterium that invades host cells, especially macrophages and epithelial cells.
It escapes the phagosome (the vesicle that would normally digest it) and lives in the cytoplasm.
By hiding in the cytoplasm, it avoids antibodies, which mainly attack extracellular pathogens.
This makes cell-mediated immunity crucial.
Listeria evades humoral immunity (antibodies) by hiding inside cells.
Th1 cells activate macrophages before the bacteria spread.
CTLs are needed later to kill cells already infected, because the bacteria are invisible to antibodies.
The combination of Th1 early + CTL late ensures the immune system can both contain and eliminate intracellular bacteria.
what are virokines and how do they relate to pathogen evasion
Virokines = viral “fake signals” that trick the immune system.
what are virorecpetors and how do they relate to pathogen evasion
Viroreceptors = viral “signal blockers” that stop the immune system from acting.
what are superantigens and how do they relate to pathogen evasion
Superantigens (SAgs) are bacterial proteins, such as staphylococcal enterotoxins (SEs), toxic shock syndrome toxin (TSST), and streptococcal pyrogenic exotoxins (SPEs), that hyperactivate the immune system. They work by binding MHC class II molecules on antigen-presenting cells and T cell receptors (TCRs) simultaneously, bypassing normal antigen specificity and activating a large proportion of T cells (~20% vs normal <0.01%). This causes T cells to divide rapidly and differentiate, resulting in a massive cytokine release (“cytokine storm”) that can lead to fever, inflammation, and potentially toxic systemic effects. In short, superantigens force T cells to overreact, overwhelming the immune system.
what is HIV and how do they relate to pathogen evasion
HIV targets CD4+ cells, (T helper cells)
CD4⁺ cells normally coordinate immune responses, helping B cells make antibodies and activating cytotoxic T lymphocytes (CTLs).
HIV can replicate and persist because the immune system can't mount a coordinated response.
Targeting the very cells that orchestrate immunity is a sophisticated form of pathogen evasion.
This strategy leads to chronic infection and eventual AIDS if untreated.
what are AIDS and how do they relate to pathogen evasion
Untreated HIV gradually destroys the immune system, and when the damage becomes severe, it progresses to AIDS, leaving the body vulnerable to infections and cancers.
T cell death drives AIDS. HIV kills CD4⁺ T cells, crippling immune coordination, which eventually allows opportunistic infections and cancers to take over.