BIO 6.2 - SKELETAL MUSCLE & HOMEOSTASIS & BLOOD GLUCOSE & KIDNEYS
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
types of muscle
smooth muscle = found in internal organs and blood vessels
cardiac muscle = makes up the heart
skeletal muscle = attached to bone, enabling the movement of limbs. work as antagonistic pairs

structure of skeletal muscle
bundle of muscle cells → each muscle cell is called a muscle fibre → myofibril
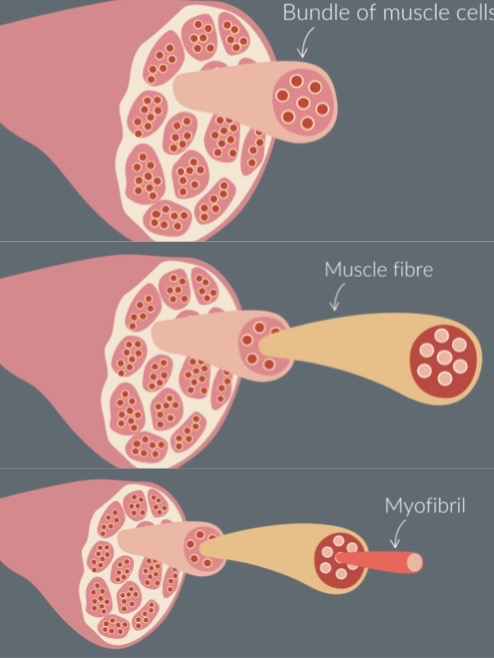
myofibril
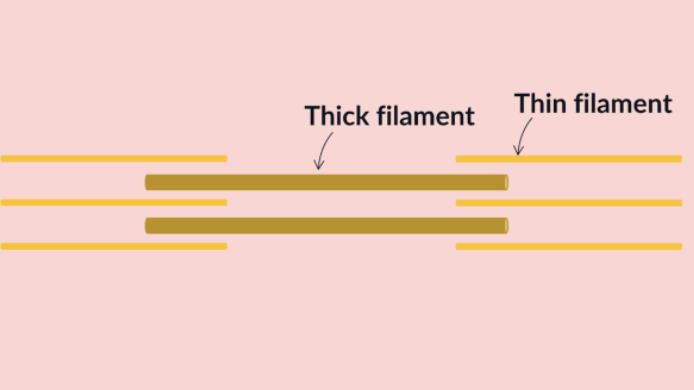
made up of protein filaments - thick and thin filaments
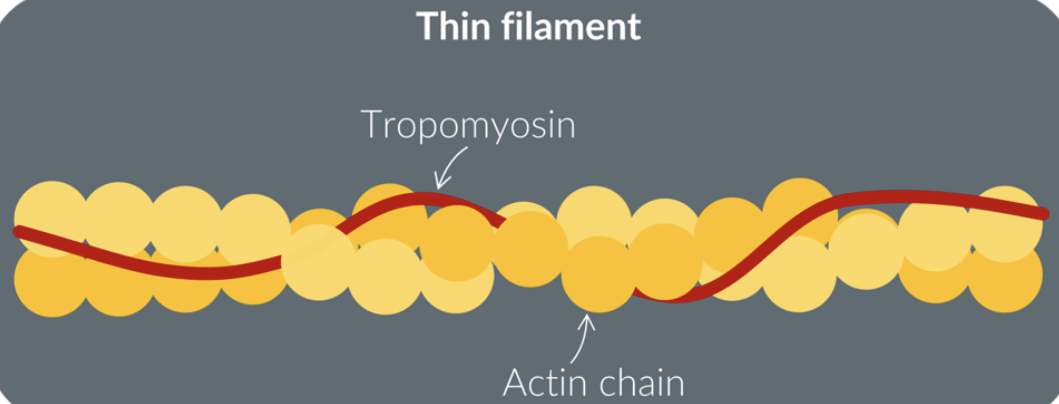
thin filament - myofibril
made up of 2 actin filaments wrapped around each other
has a protein chain wrapped around the actin filaments called tropomyosin
each individual circle in the actin chain is an actin protein
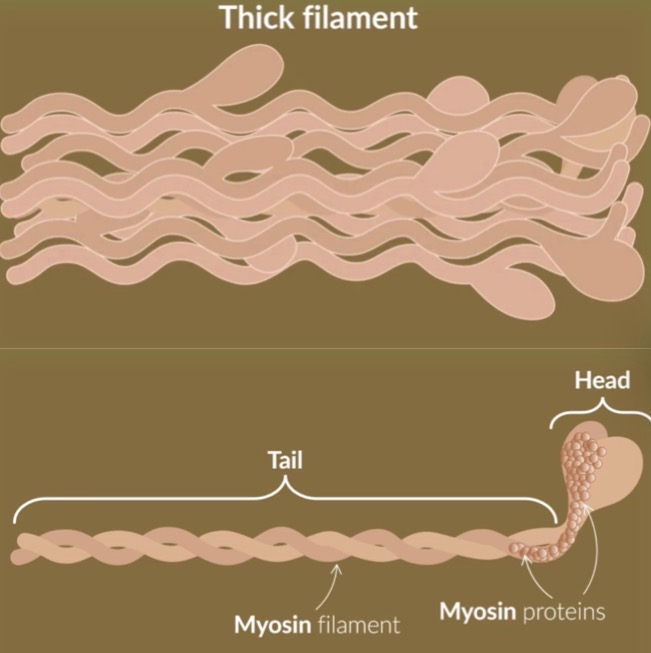
thick filament - myofibril
made up of a bundle of threads
each thread consists of 2 myosin filaments wrapped around each other
each myosin filament strand ends in a head structure
the tail and the head are made up of myosin proteins
sarcomere
a section inside a myofibril made up of a vertical stack of at least 4 thin filaments and 1 thick filament
a myofibril is made up of many repeating sarcomeres
structures of a sarcomere
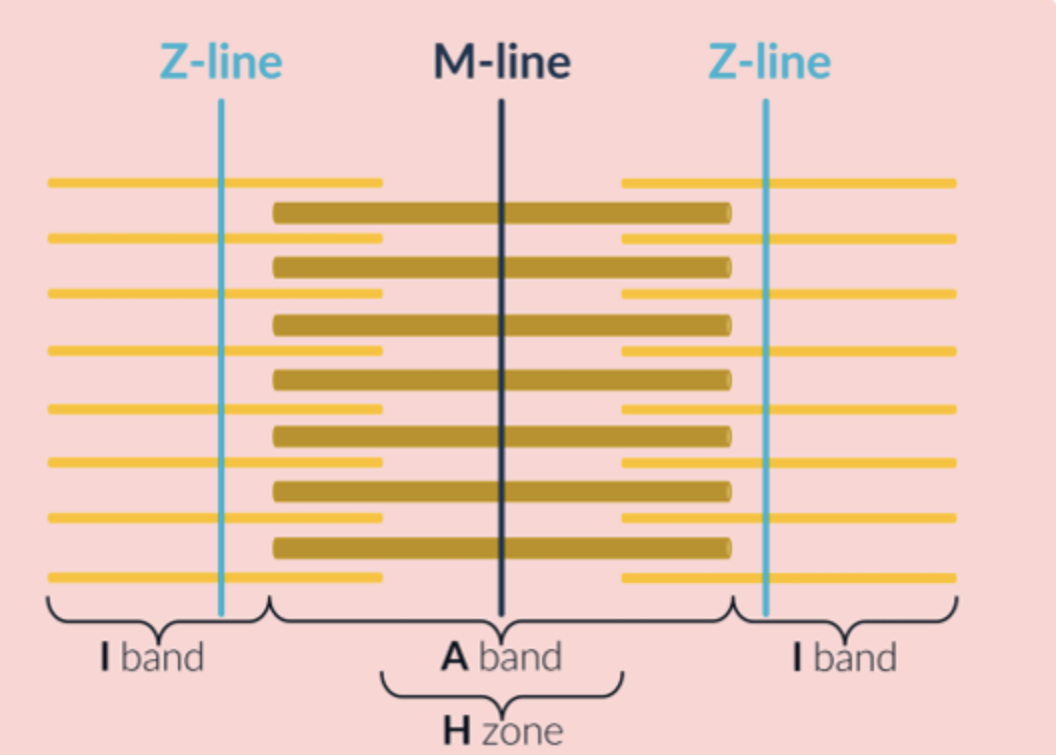
M line is found in the middle of the thick filaments
Z line is the mid point between two M lines found at the thin filaments
each individual sarcomere is made of 1 M line and 2 Z lines

structures of a sarcomere 2
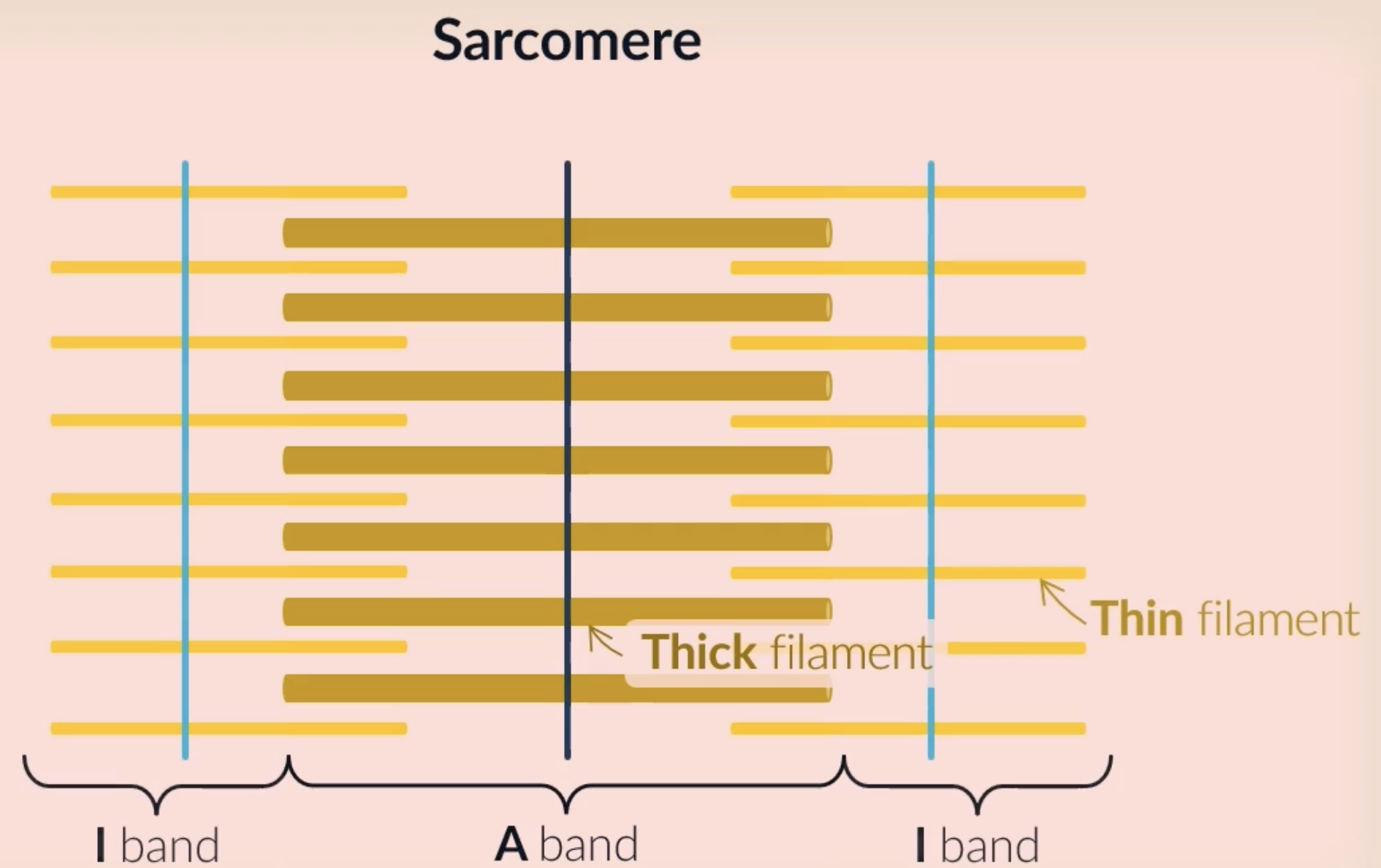
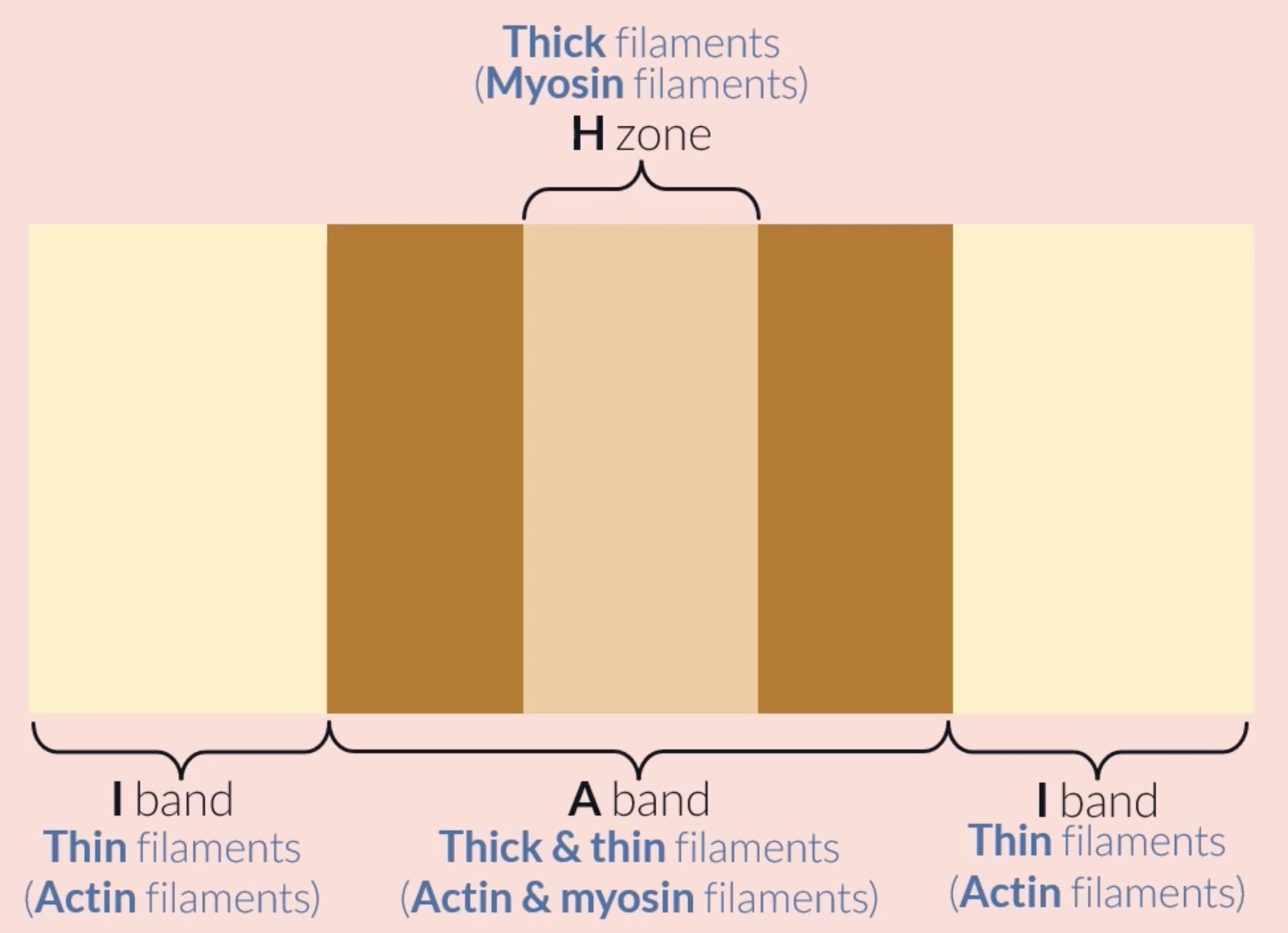
each sarcomere consists of a light and dark band: the light band is the area where just the thin filaments are which allows more light through, the dark band is the are where the thick filaments are which doesnt allow a lot of light through
I band is the whole area where only the thin filaments are found (light band)
A band is the whole area where the thick filaments are found (dark band)
(M line is found at the centre of the A band)
(Z line is found at the centre of the I band)
structures of a sarcomere 3
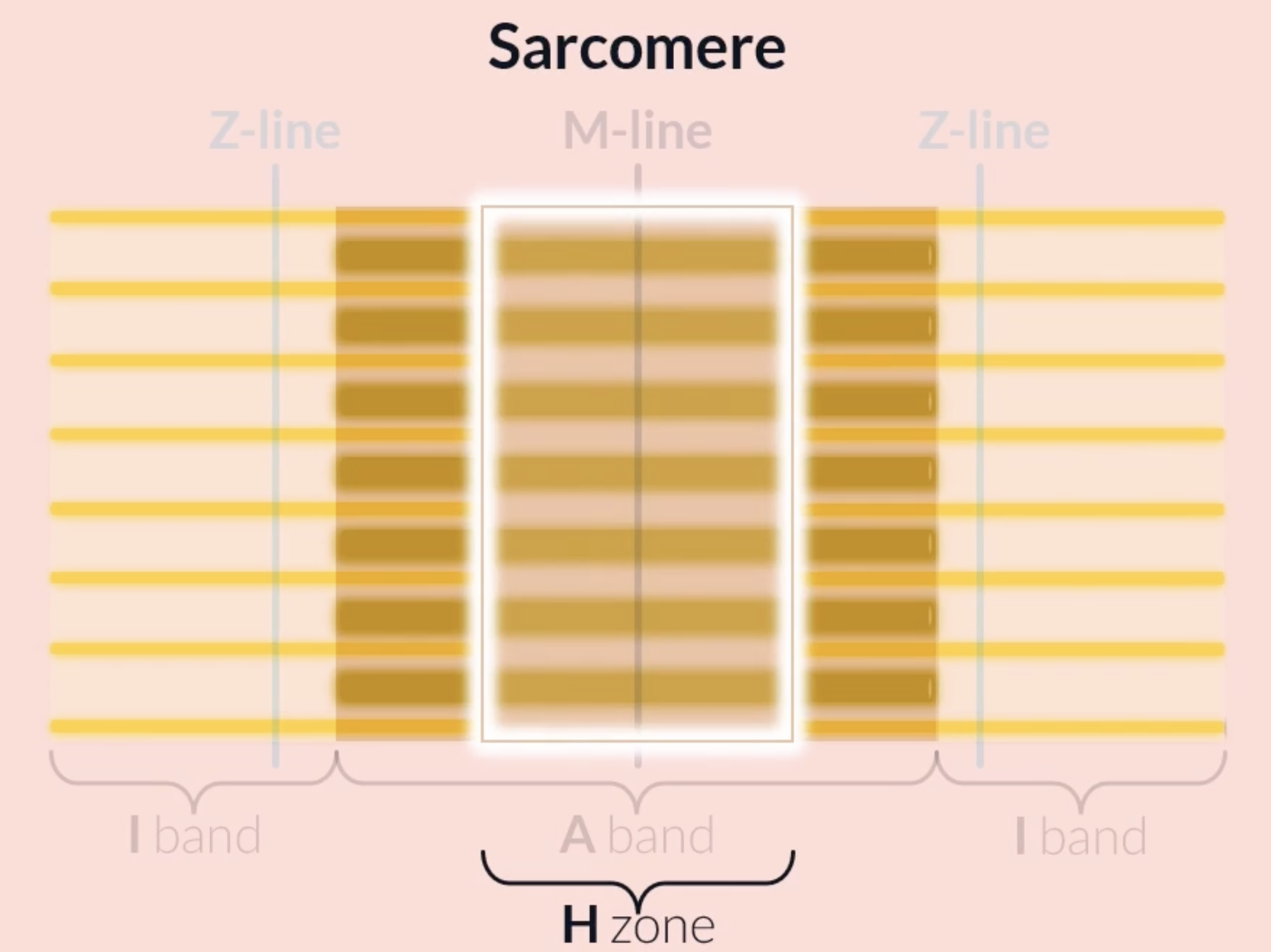
H zone is found at the middle of the A band, it consists of only thick filaments, appears lighter than the rest of the A band because it only consists of thick filaments whereas areas of the A band consist of thick and thin filaments
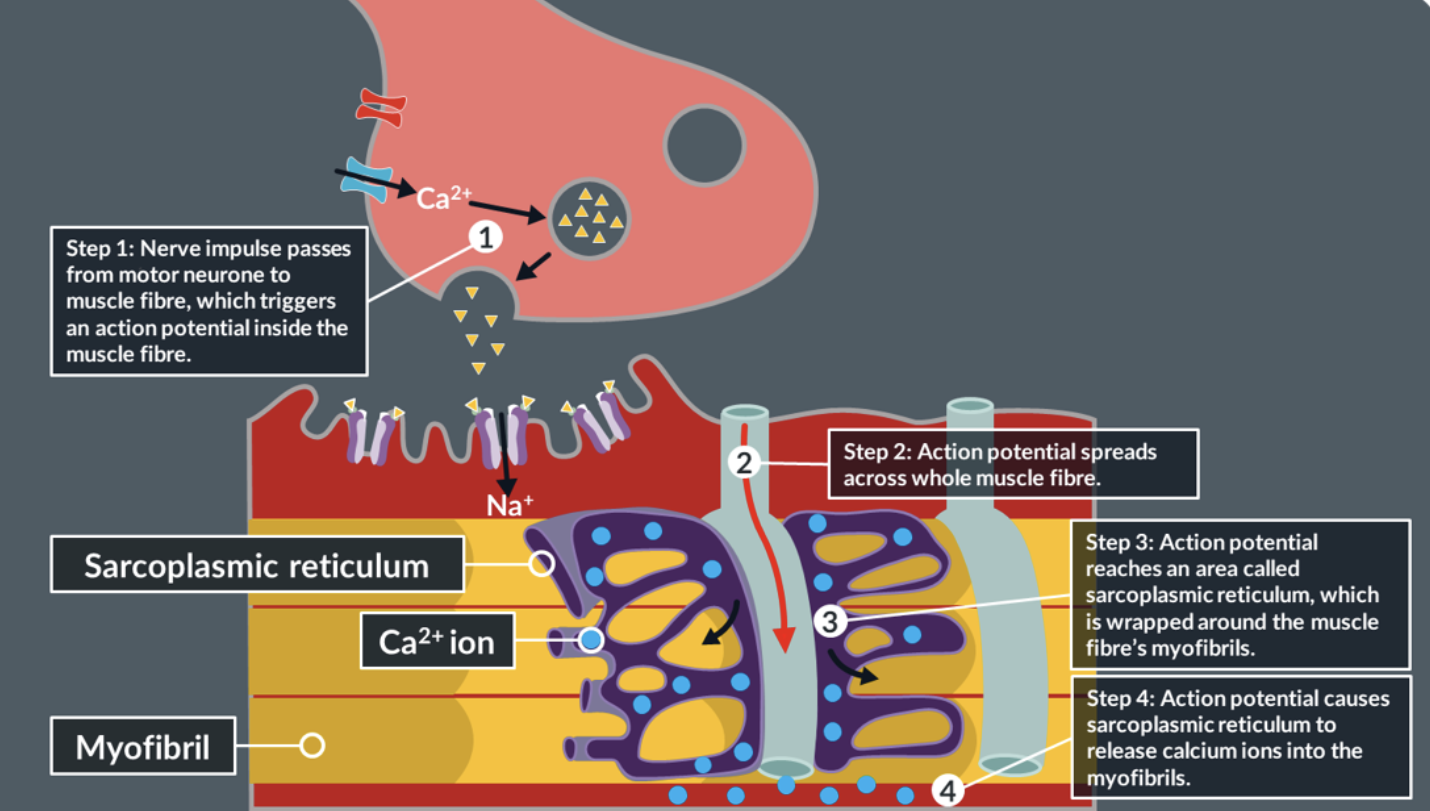
effect of an action potential at the muscle fibre
the movement of actin and myosin is the result of an action potential that is triggered inside a muscle fibre of a neuromuscular junction
zoom in on myosin filaments
the heads stick out towards the actin filaments

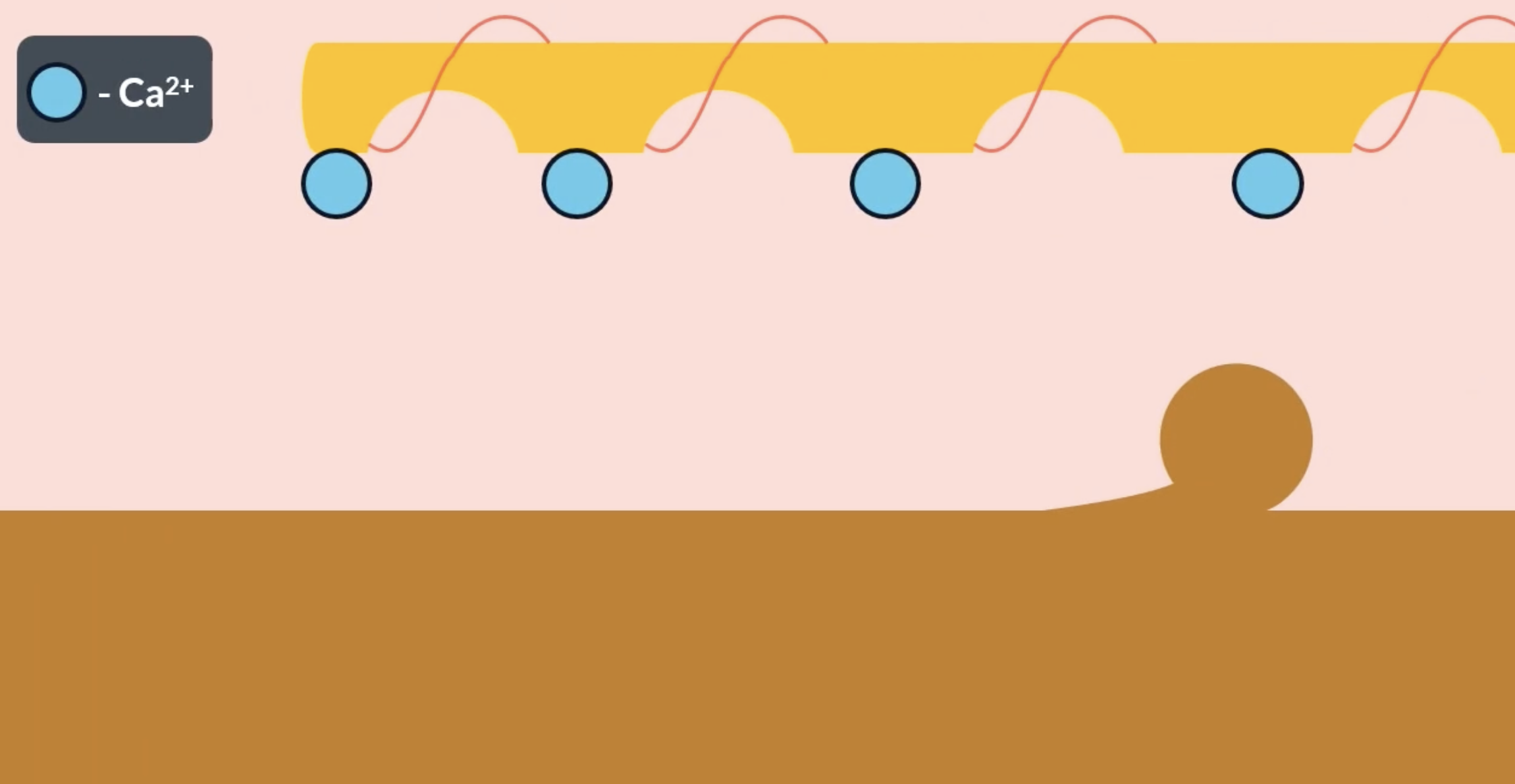
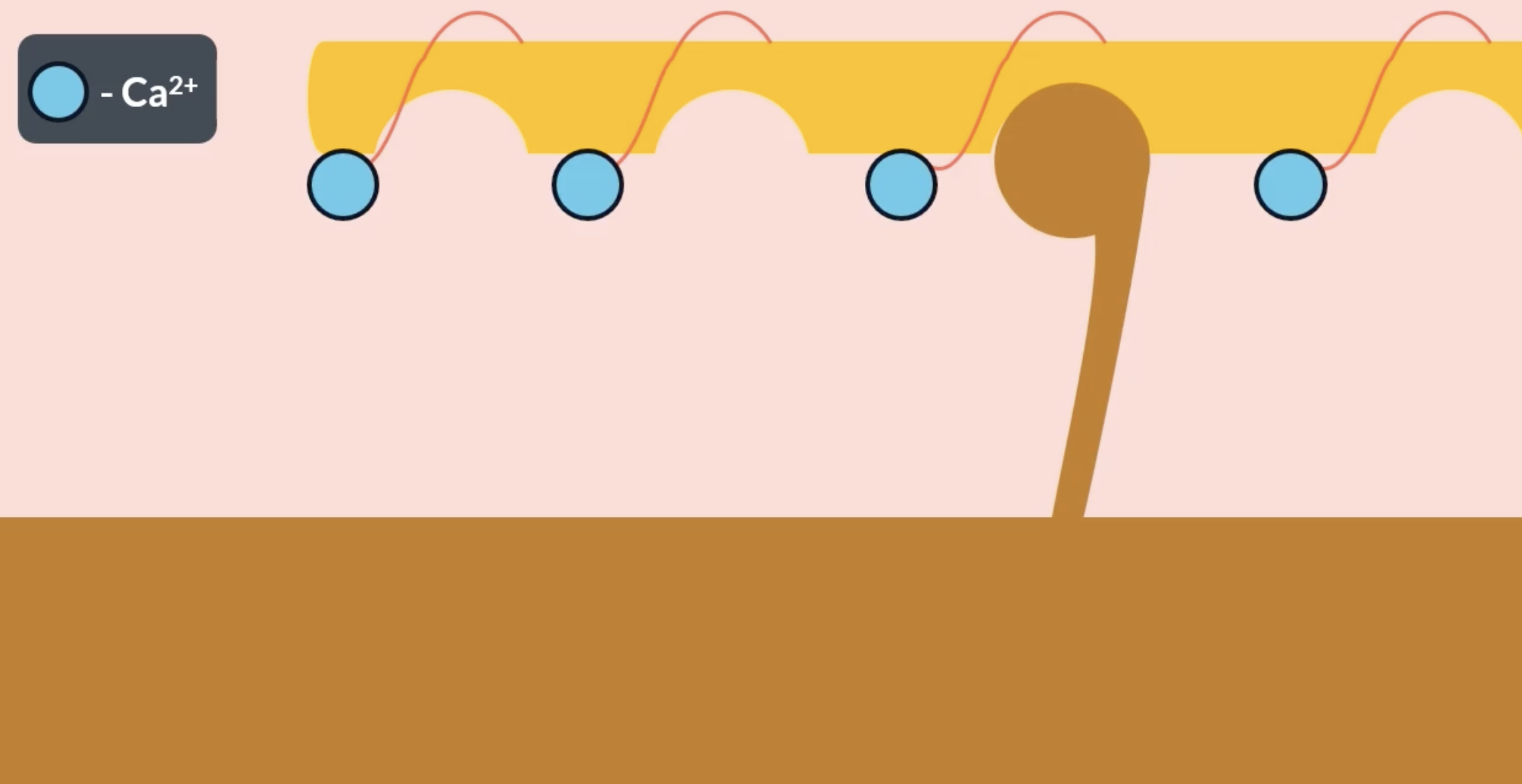
tropomyosin and calcium ions
actin has complementary binding sites for the myosin heads which are usually covered by the tropomyosin chain. as the result of an action potential, Ca2+ ions arrive at the actin and bind to troponin (found on the actin filament). the presence of the Ca2+ ions trigger tropomyosin to change shape and move away from the binding site, allowing the myosin head to attach
when the myosin head successfully binds to the actin binding site = actinomyosin bridge is formed
myosin head returning to starting position
for the myosin head to return back to its resting position, it has an active site where ATP can bind. ATP gets hydrolysed into ADP + Pi, which provides the energy needed for the myosin head to return back to its original resting position
the myosin heads catalyse this hydrolysis reaction, so the myosin heads are actually enzymes known as ATPase
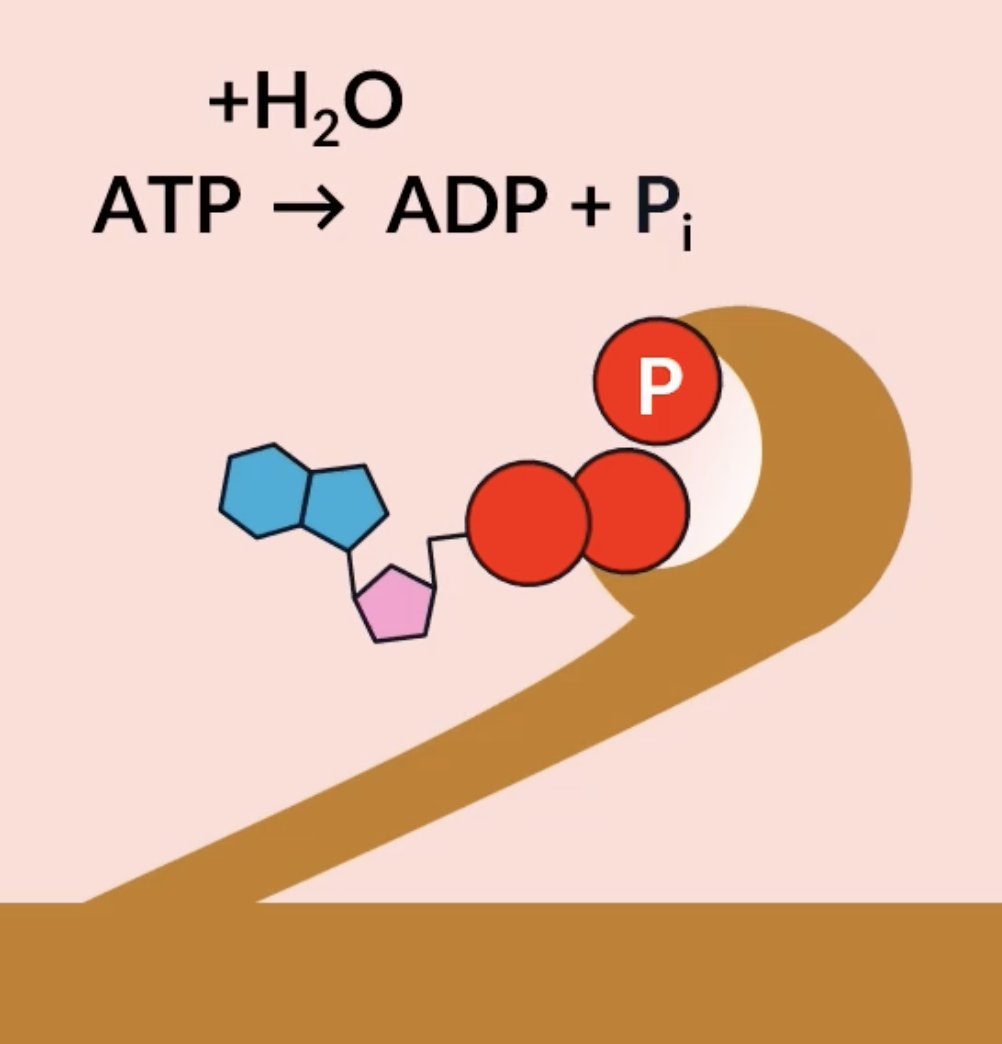
the sliding filament mechanism of muscle contraction
Ca2+ ions arrive, triggering tropomyosin to change shape and move away from the binding site on actin
myosin head attaches to the binding site on the actin, forming an actinomyosin bridge
the myosin head hydrolyses ATP into ADP and Pi and releases them, which provides the energy for myosin to change its angle and move the actin = power stroke
another ATP molecule binds to the myosin head active site and myosin detaches
ATP gets hydrolysed into ADP and Pi, providing the energy needed for the myosin head to return back to its resting position
myosin head can then repeat this process with the next actin binding site
in each sarcomere theres many myosin heads moving actin filaments, which causes the whole sarcomere to contract, moving the actin filaments closer to the M line → muscle contraction
evidence for the sliding filament mechanism
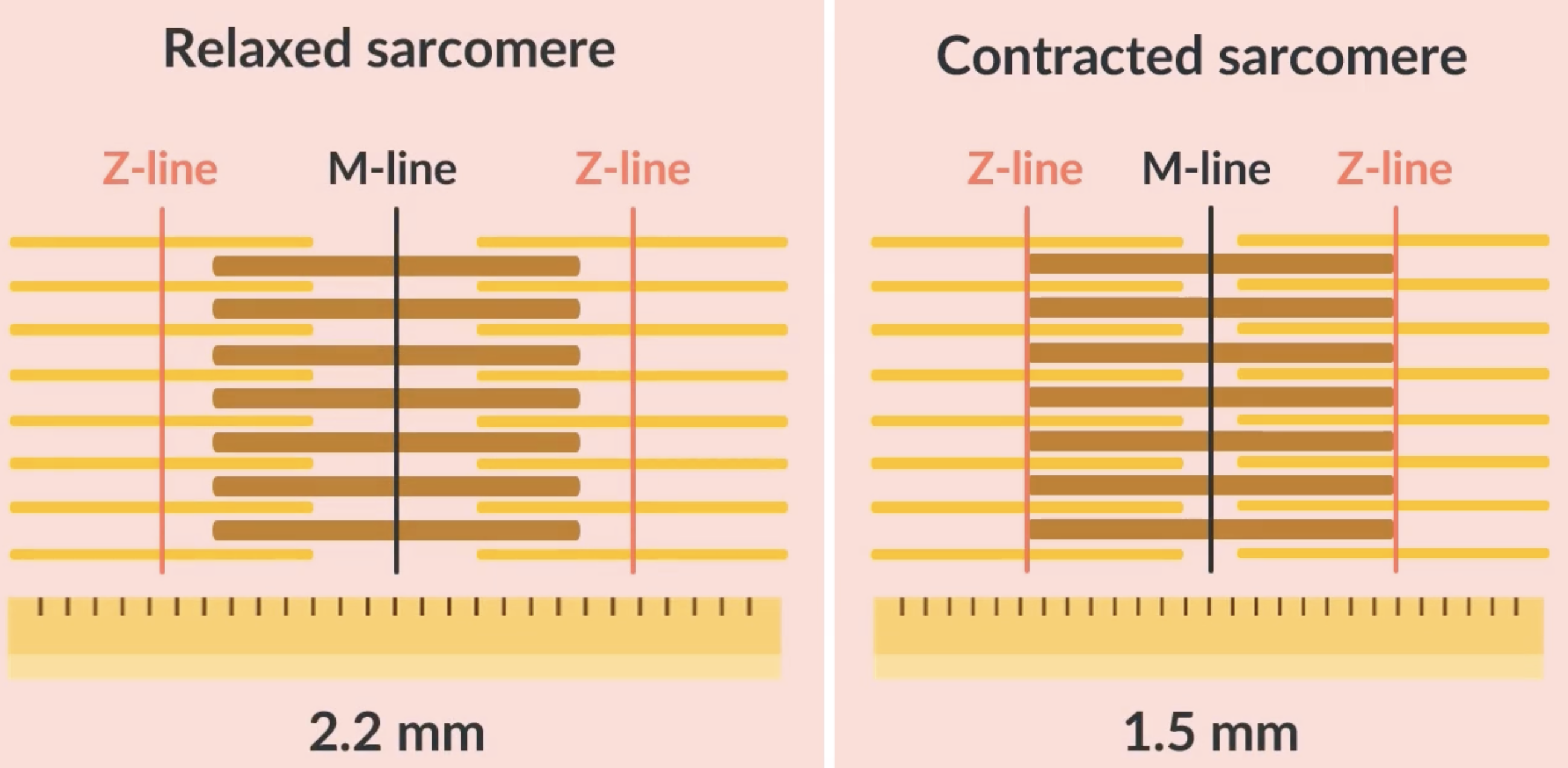
during contraction, the actin filaments slide along the myosin filaments, more of the actin and myosin filaments overlap, causing a darker section of the sarcomere
during contraction:
-length of the sarcomere shortens
-Z lines move more closely together
-I band becomes narrower
-A band stays the same
-H zone becomes narrower
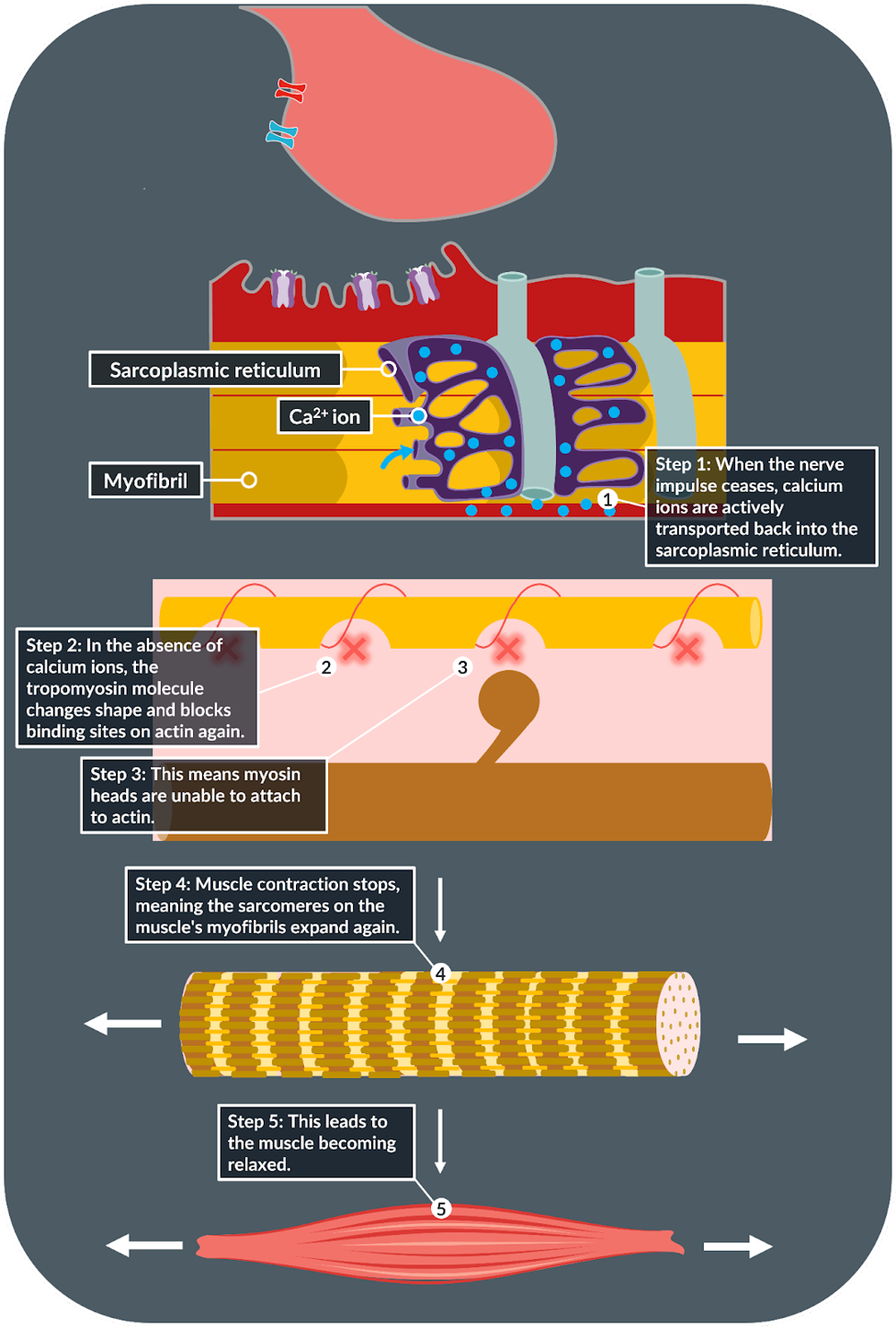
muscle relaxation
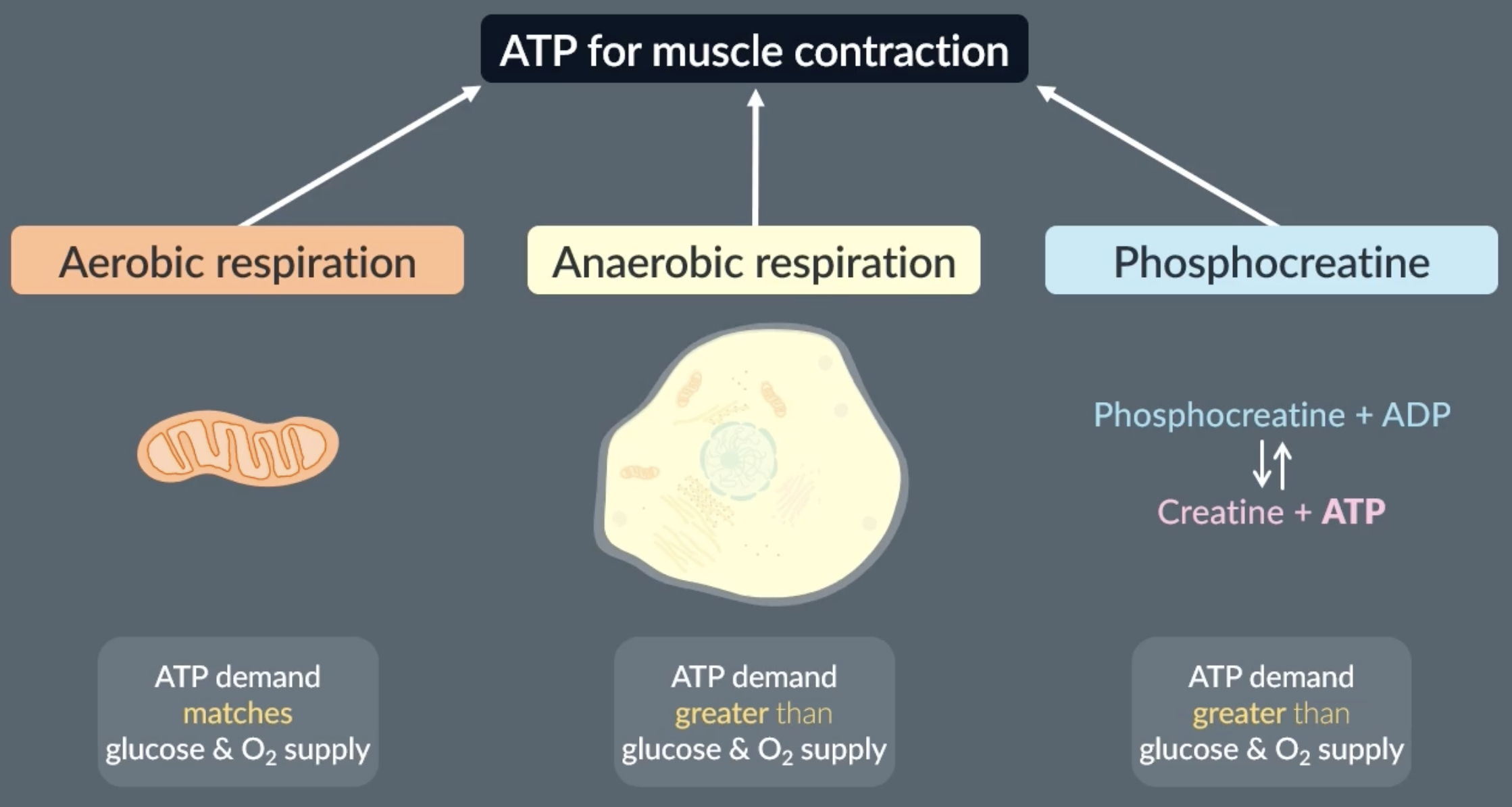
phosphocreatine
phosphocreatine acts as a rapid ATP source in muscle cells by donating a phosphate group to ADP to make ATP, ensuring ATP availability during short bursts of intense activity
phosphocreatine is a chemical that phosphorylates ADP to make ATP
sources of ATP in muscles
fast twitch fibres vs slow twitch fibres
fast twitch = fast, powerful, but tire quickly
slow twitch = slower, less powerful, but don’t tire easily
fast muscle fibres are specialised to provide quick, powerful contractions
slow muscle fibres are specialised to provide slower, weaker contractions
fast: found in arms and legs, use anaerobic and phosphocreatine, contain a lot of phosphocreatine and few mitochondria
slow: found in calfs and back, mainly aerobic respiration, contain many mitochondria
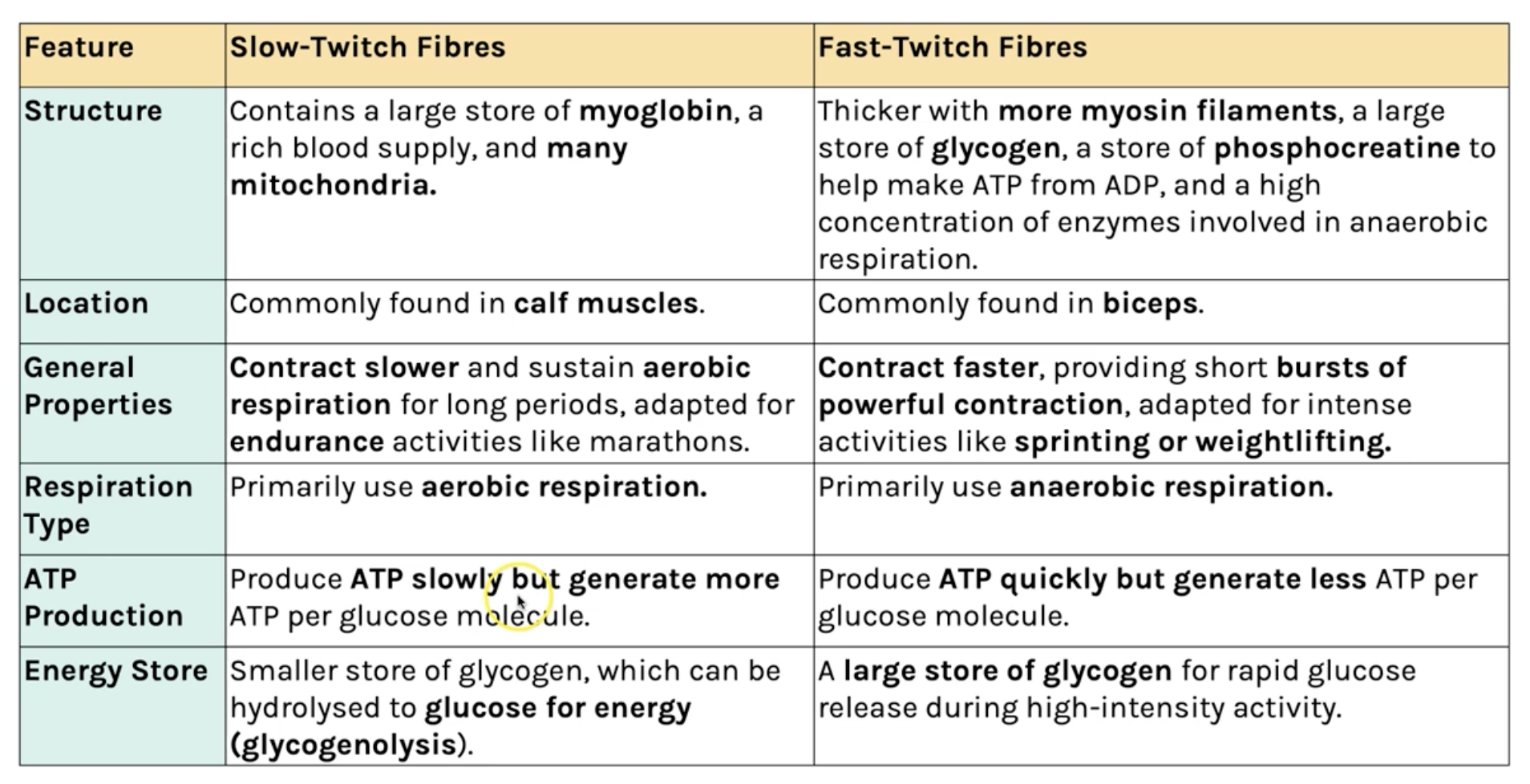
homeostasis
involves physiological control systems that maintain the internal environment within restricted limits
each physiological control system has these 3 features:
-receptor = detects deviation from optimum
-coordinator (eg. CNS) = transfers info
-effector = carries out a response
homeostasis ensures that blood has a stable pH and that the body has a stable core temperature, which is essential for enzyme activity in the body
the 2 feedback mechanisms involved in homeostasis
negative feedback: (most common) counteracts a change to restore the system to its original level. may have to repeat a few times to reach the original level
eg. body temperature rising
positive feedback: exaggerates a change, increasing a systems deviation from its original level
eg. stretched cervix during childbirth is detected, effector releases hormones to continue the stretching until baby is born
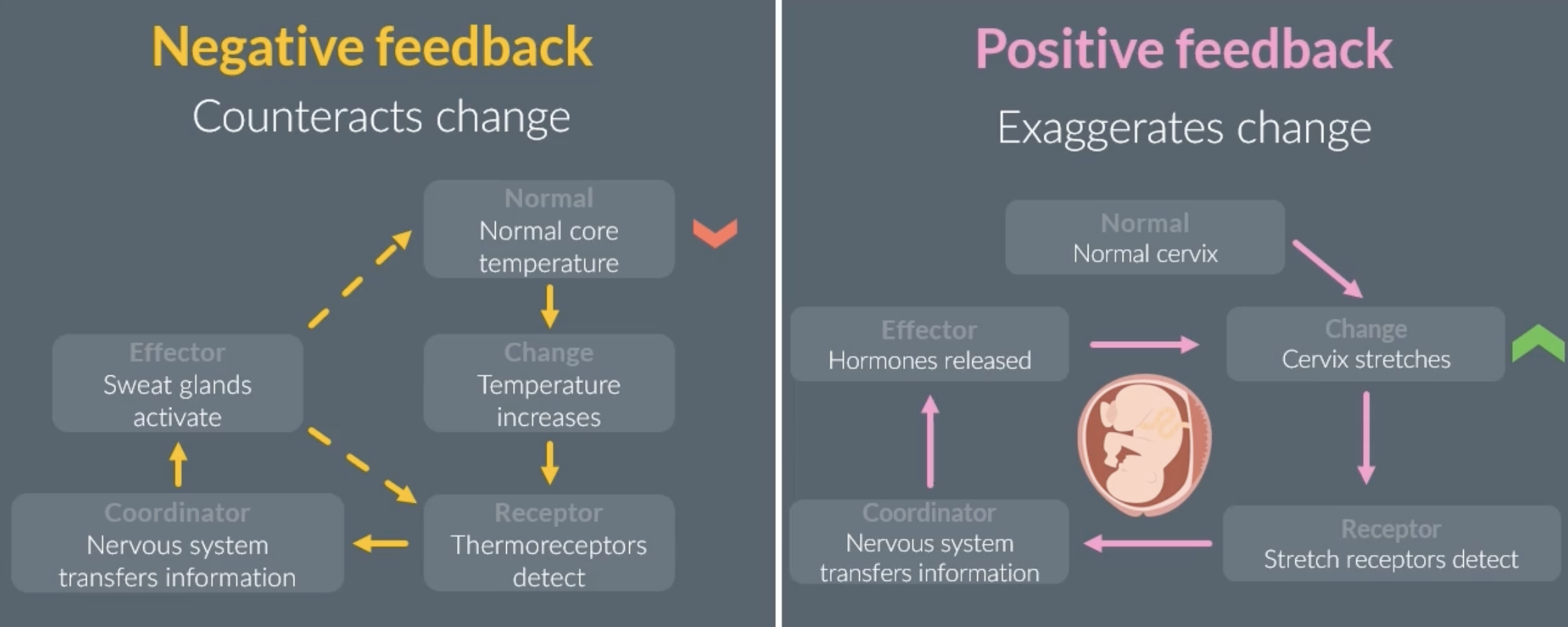
what happens when blood glucose concentration gets too low or too high?
the optimum blood glucose concentration is 5mmol dm-3
too low:
cells cannot carry out much respiration so cells can die
experience symptoms of hunger, headaches etc
too high:
water potential of blood decreases, so water moves from our cells into the blood by osmosis. our cells shrink and can die
experience symptoms of tiredness, can damage eyes, nerve cells etc
factors that influence blood glucose concentration
food
when we eat, our body digests the food and produces glucose. this causes our blood glucose concentration to increase
exercise
when we exercise, our cells respire more and use up more glucose. this causes our blood glucose concentration to decrease.
hormones regulating blood glucose concentration
pancreas detects changes in our blood glucose concentration and releases hormones
when blood glucose concentration gets too low, glucagon is released from the pancreas to increase it to optimum blood glucose concentration
when blood glucose concentration gets too high, insulin is released from the pancreas to decrease it to optimum blood glucose concentration
these are examples of negative feedback
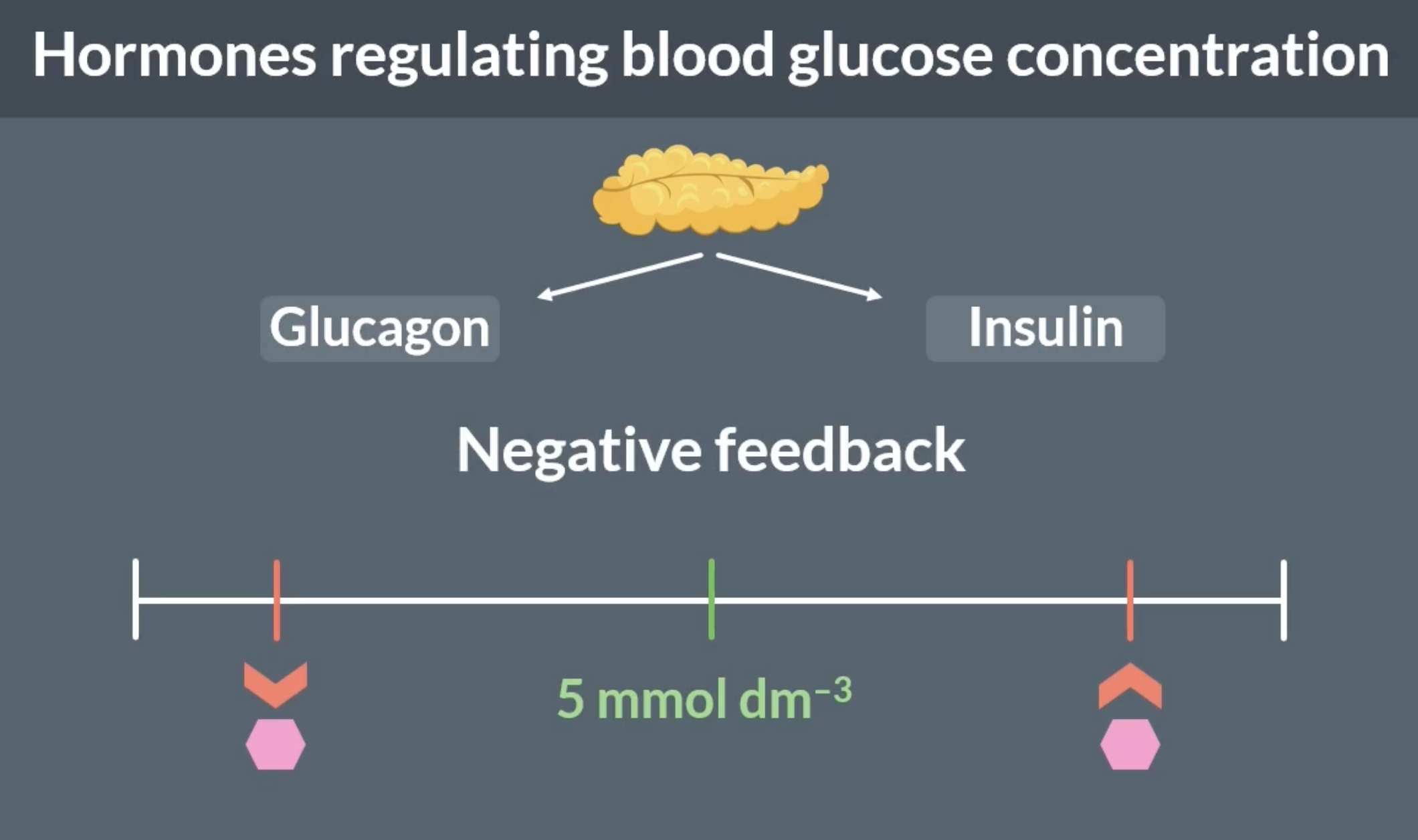
role of pancreas
pancreas contains a clump of cells called islet of langerhans.
islet of langerhans contains alpha and beta cells
-alpha cells: detect a decrease in blood glucose concentration and release glucagon. when blood glucose concentration returns to optimum alpha cells stop releasing glucagon
-beta cells: detect an increase in blood glucose concentration and release insulin. when blood glucose concentration returns to optimum beta cells stop releasing insulin
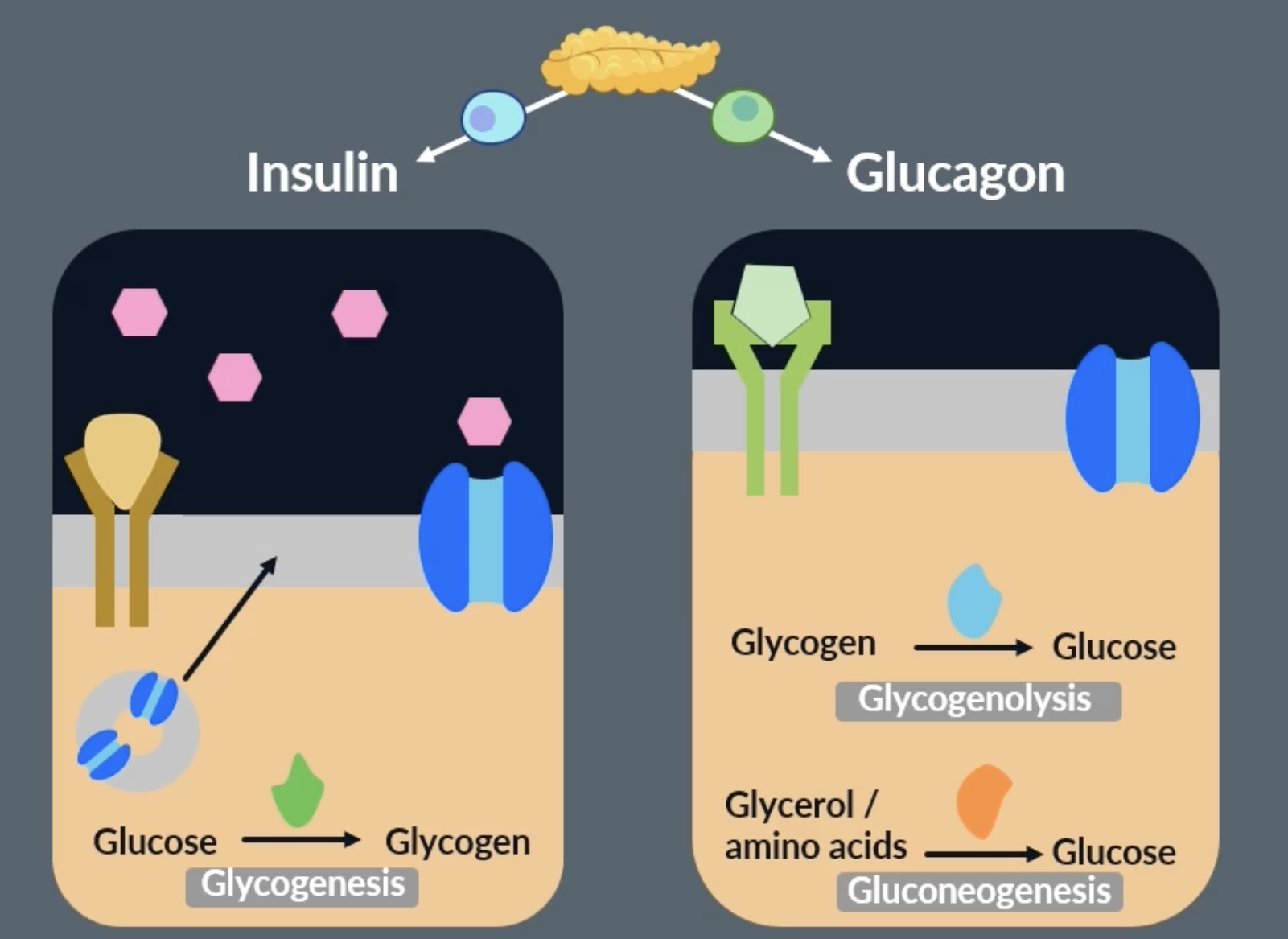
decreasing blood glucose concentration: insulin and channel proteins
our cells have glucose channel proteins which allows glucose into cells to be used in respiration
cells also have insulin receptors, when insulin binds to the insulin receptors, it triggers vesicles (which contain extra glucose channel proteins) to move to the cell membrane. these vesicles fuse with the cell membrane and the glucose channel proteins are added to the cell membrane. this increases the amount of glucose that can enter the cell, which decreases the blood glucose concentration. this glucose can then be used in respiration or to synthesise new molecules for the cell
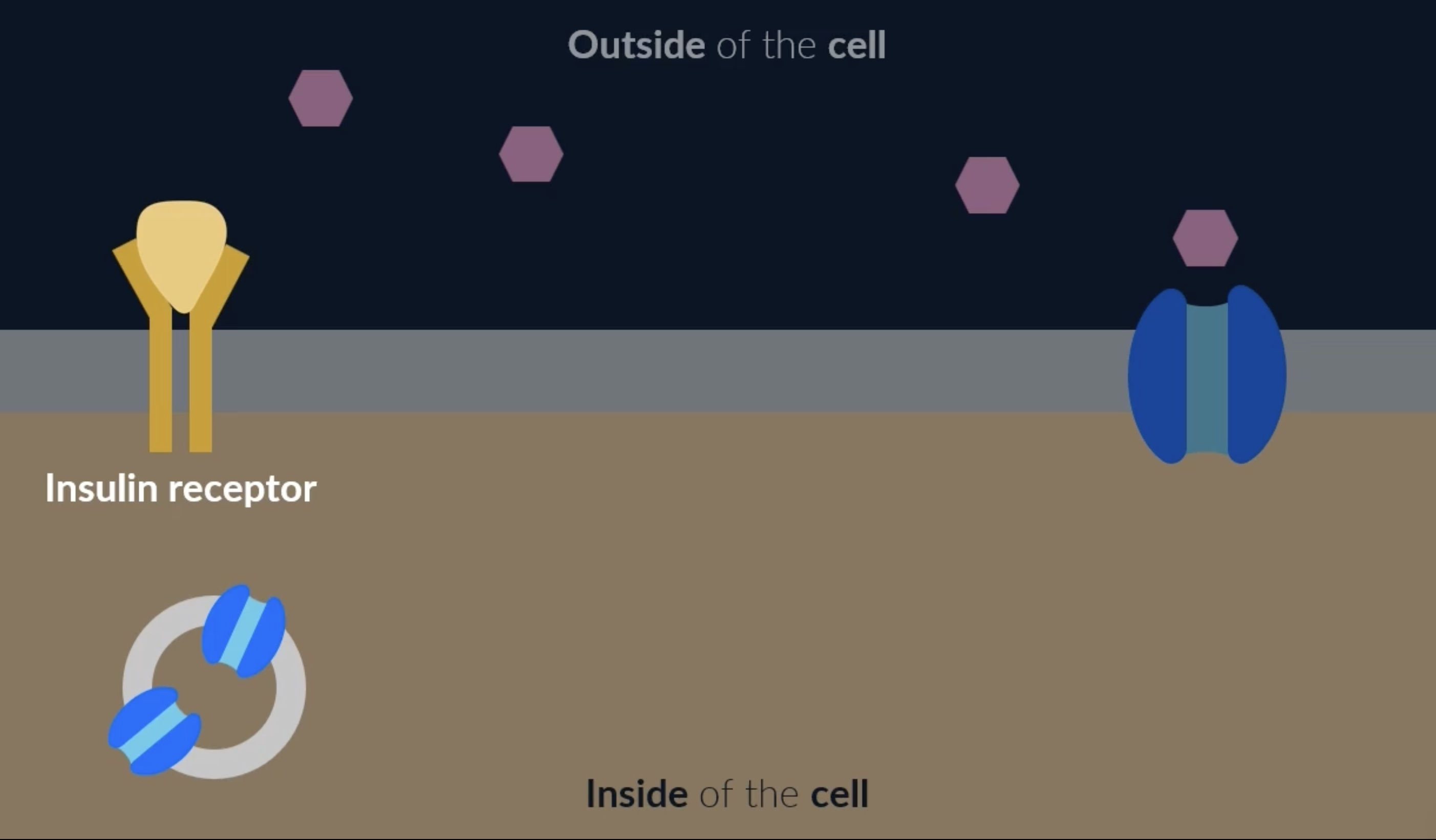
decreasing blood glucose concentration: glycogenesis
glycogenesis : conversion of glucose into glycogen
occurs in liver cells for the control of blood glucose concentration
when insulin binds to an insulin receptor on a liver cell, it activates enzymes inside the cell. these enzymes catalyse the conversion of glucose into glycogen. this is good because glycogen is a good store for glucose as its too big to escape the cell. it also reduces the concentration of glucose in the liver cells, which creates a concentration gradient for glucose to move out of the blood and into the liver cells = decreasing blood glucose concentration
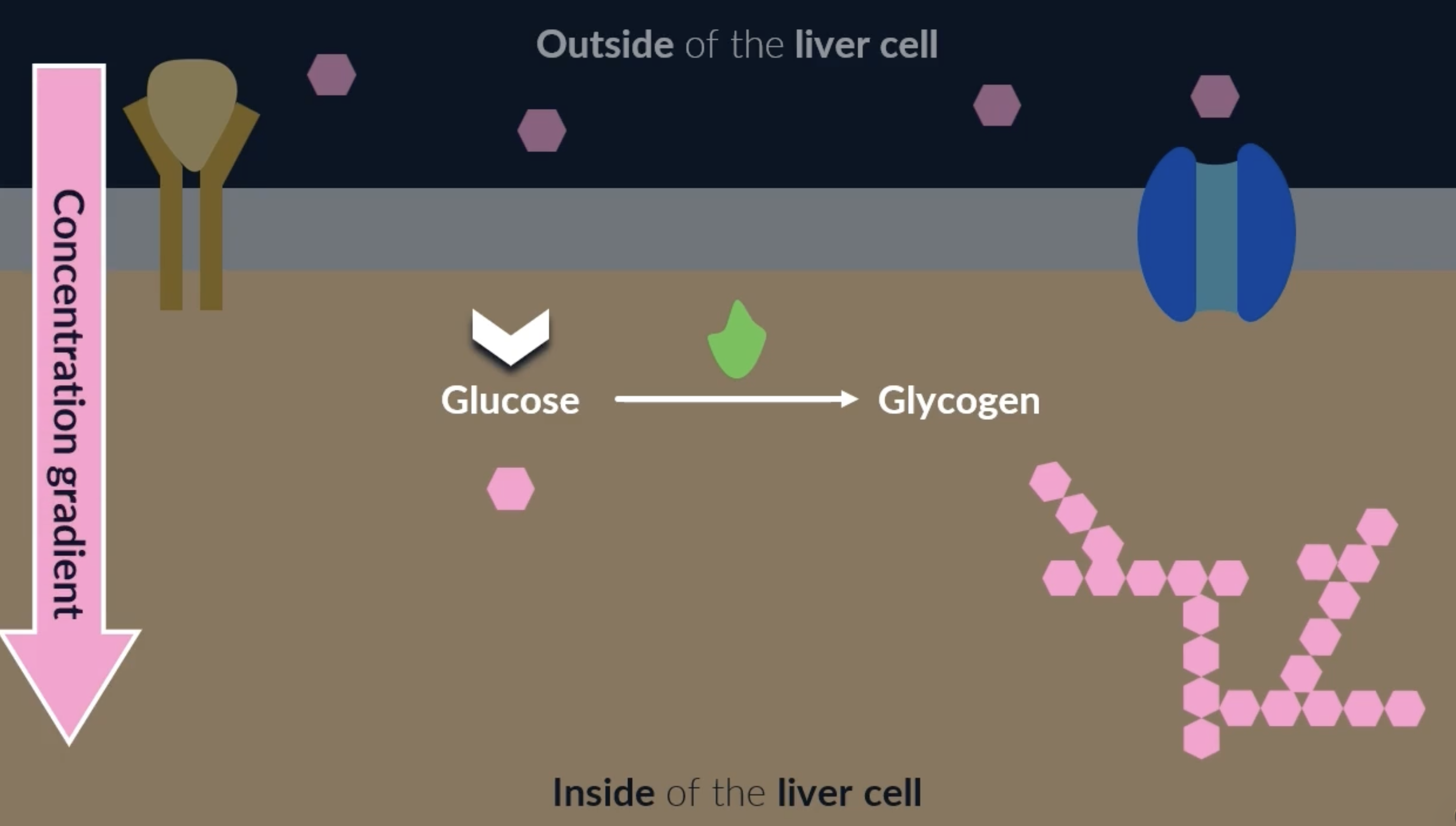
increasing blood glucose concentration: glucagon and channel proteins
glucagon receptors are usually only found on the cell membrane of liver cells
glycogenolysis : breakdown of glycogen into glucose
when glucagon binds to these receptors, it activates enzymes which catalyse the conversion of glycogen to glucose. the glucose can then leave the cell through the glucose channel proteins and increase the blood glucose concentration = glycogenolysis * secondary messenger pathway on flashcard 32
gluconeogensis : formation of glucose form non-carbohydrate sources (glycerol and amino acids)
when glucagon binds to its receptors, another enzyme is activated that can convert other molecules (such as glycerol and amino acids) into glucose = gluconeogenesis
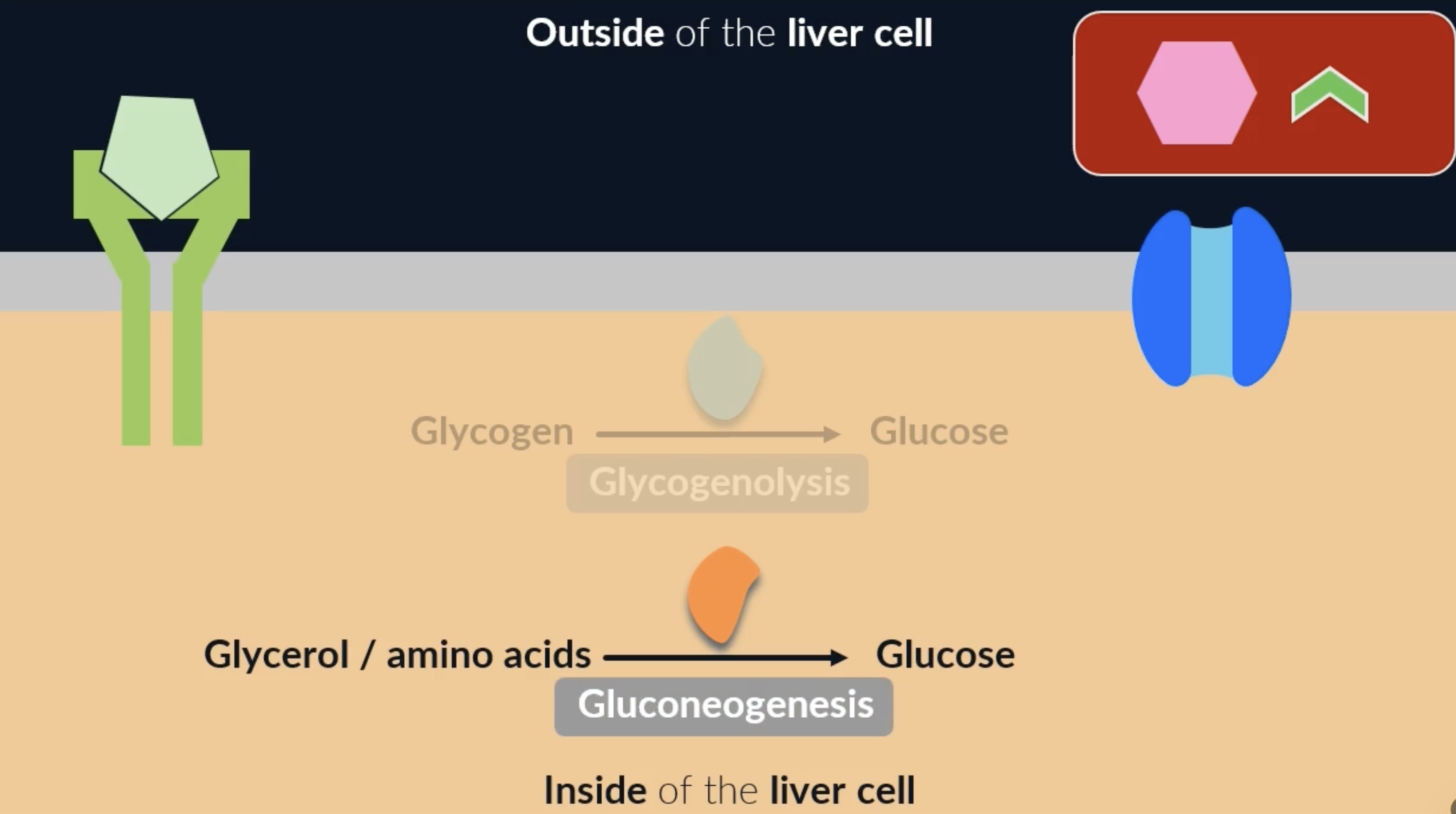
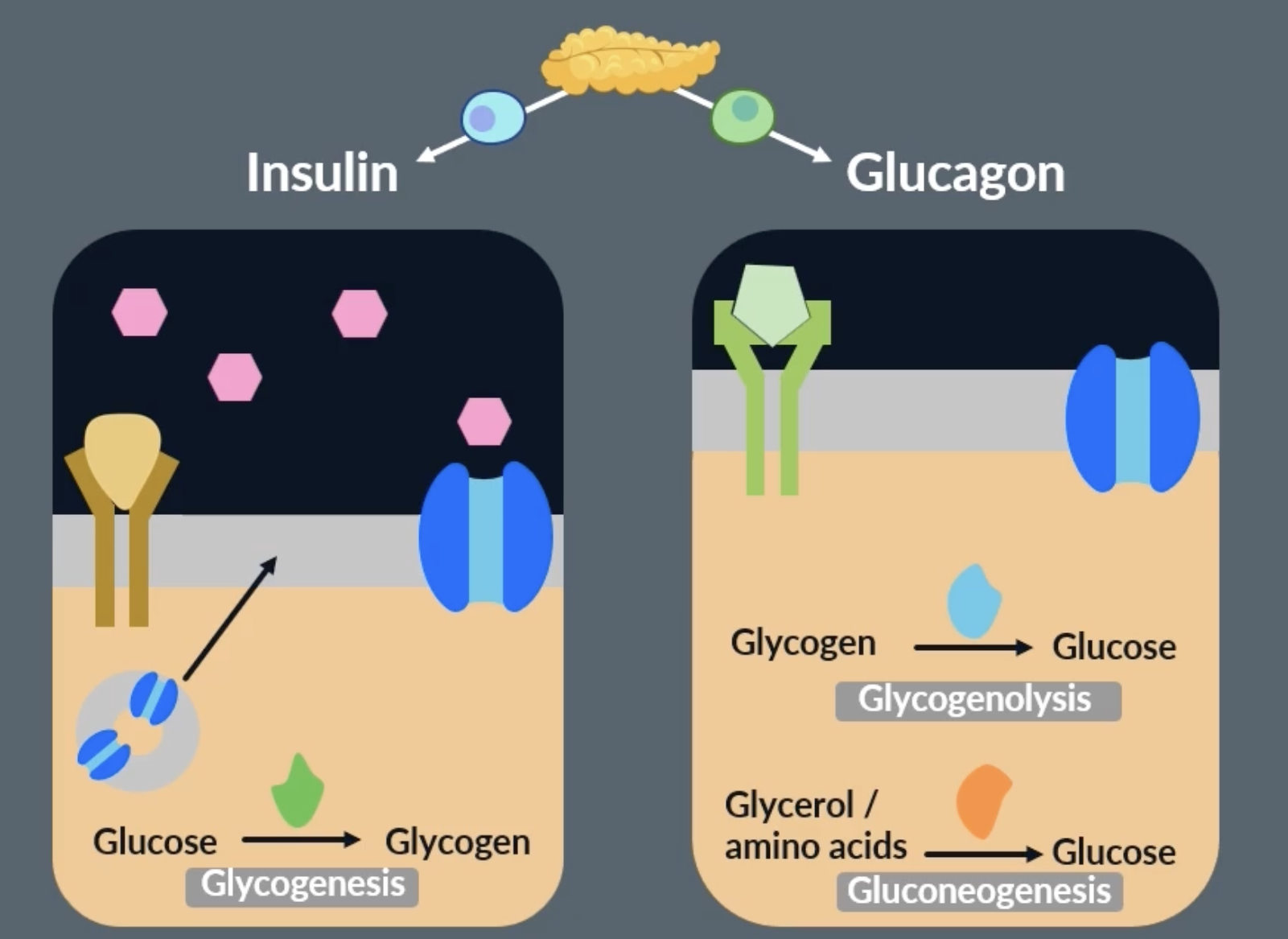
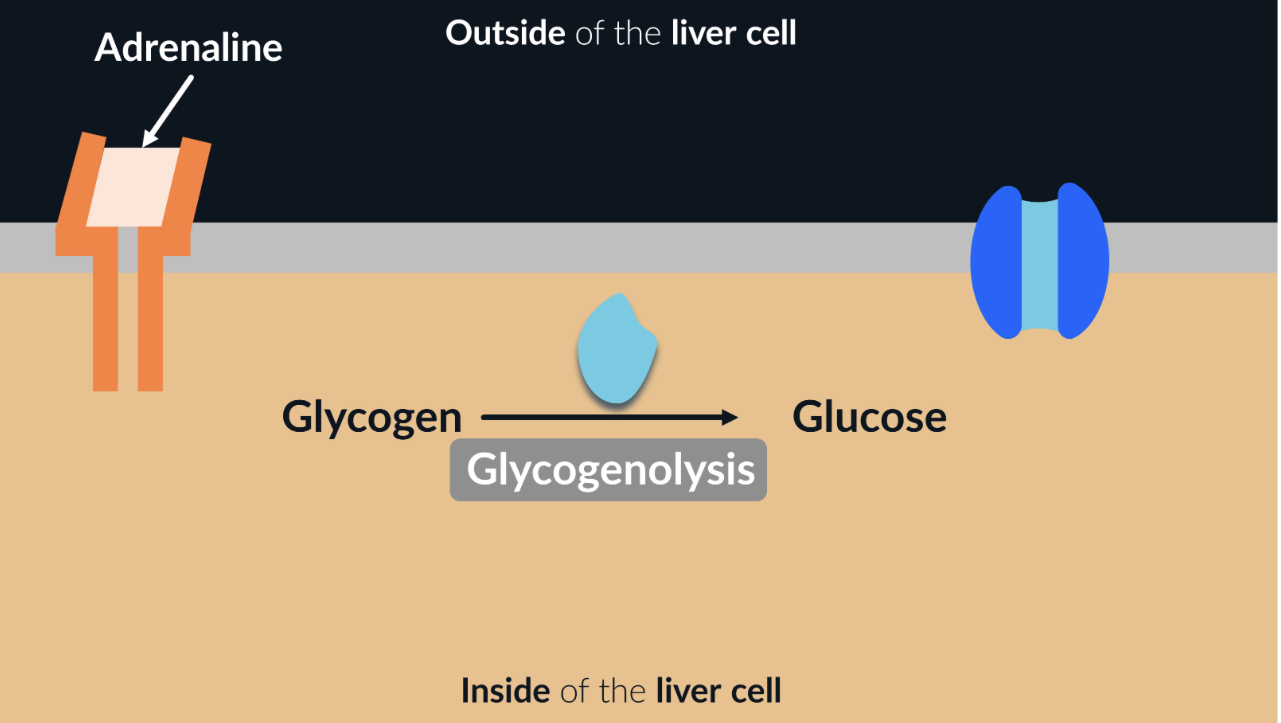
increasing blood glucose concentration: adrenaline
a third hormone that can affect our blood glucose levels is adrenaline. adrenaline is produced by our adrenal glands in response to stress
in the blood, adrenaline binds to complementary receptors in liver cells. once bound, it activates the enzymes that catalyse glycogenolysis: breakdown of glycogen into glucose
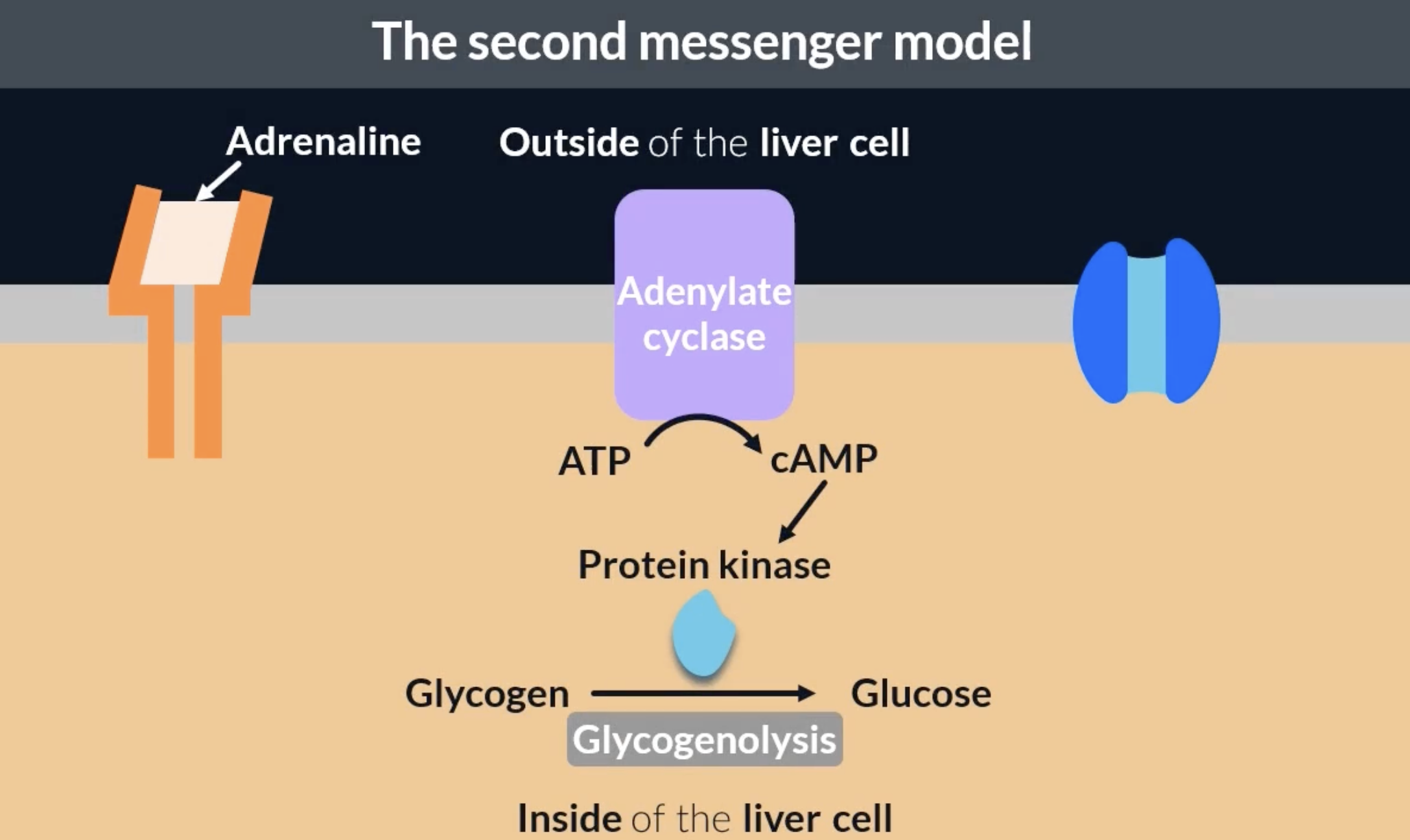
second messenger model: adrenaline and glucagon → glycogenolysis
protein kinase is the specific enzyme that catalyses glycogenolysis
when adrenaline or glucagon binds to complementary receptors, it activates an enzyme in the cell membrane called adenylate cyclase. this enzyme catalyses the conversion of ATP to cAMP. cAMP can bind to the enzyme protein kinase and activate it to carry out glycogenolysis
this process is called the second messenger model because it involves 2 messengers. the first messenger is the molecule that binds to receptors and signals a change = adrenaline or glucagon. the second messenger is the molecule that coordinates the response = cAMP activating protein kinase
diabetes
condition in which the body is unable to regulate blood glucose concentration
type 1 diabetes: begins in childhood. immune system attacks beta cells preventing them from producing insulin. can be treated with insulin injections and managing diet
type 2 diabetes: occurs usually after age 40. pancreas stops producing enough insulin or cell surface membranes loose sensitivity to insulin receptors (insulin can no longer bind to their receptors), preventing glycogenesis. controlled by managing diet and exercise (since exercise reduces blood glucose concentration)
kidneys
role of the kidneys:
-to filter blood and produce urine, which removes harmful waste products (eg. urea) from blood
-osmoregulation = process of regulating the water potential of the blood. if wp is too low, cells will shrink, if wp is too high, cells undergo lysis
structures of nephrons
nephrons are tubes that extend through the cortex and medulla of the kidney that filter the blood
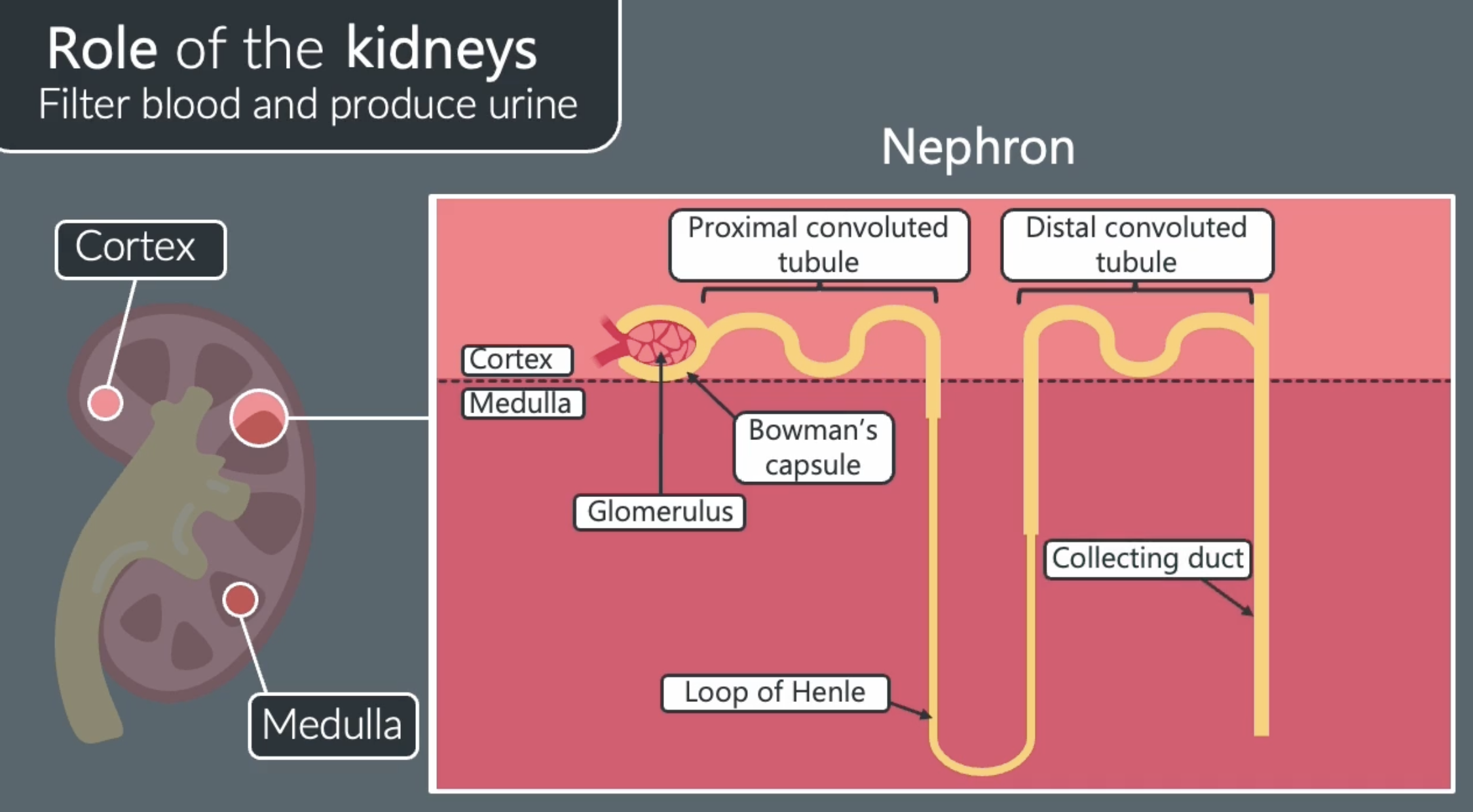
structures of nephrons 2
the glomerulus is a mass of blood capillaries found in the bowmans capsule, blood is supplied to the glomerulus by the afferent arteriole
the efferent arteriole carries blood away from the glomerulus to another network of capillaries in the rest of the nephron. ensures that theres a short diffusion pathway to the blood
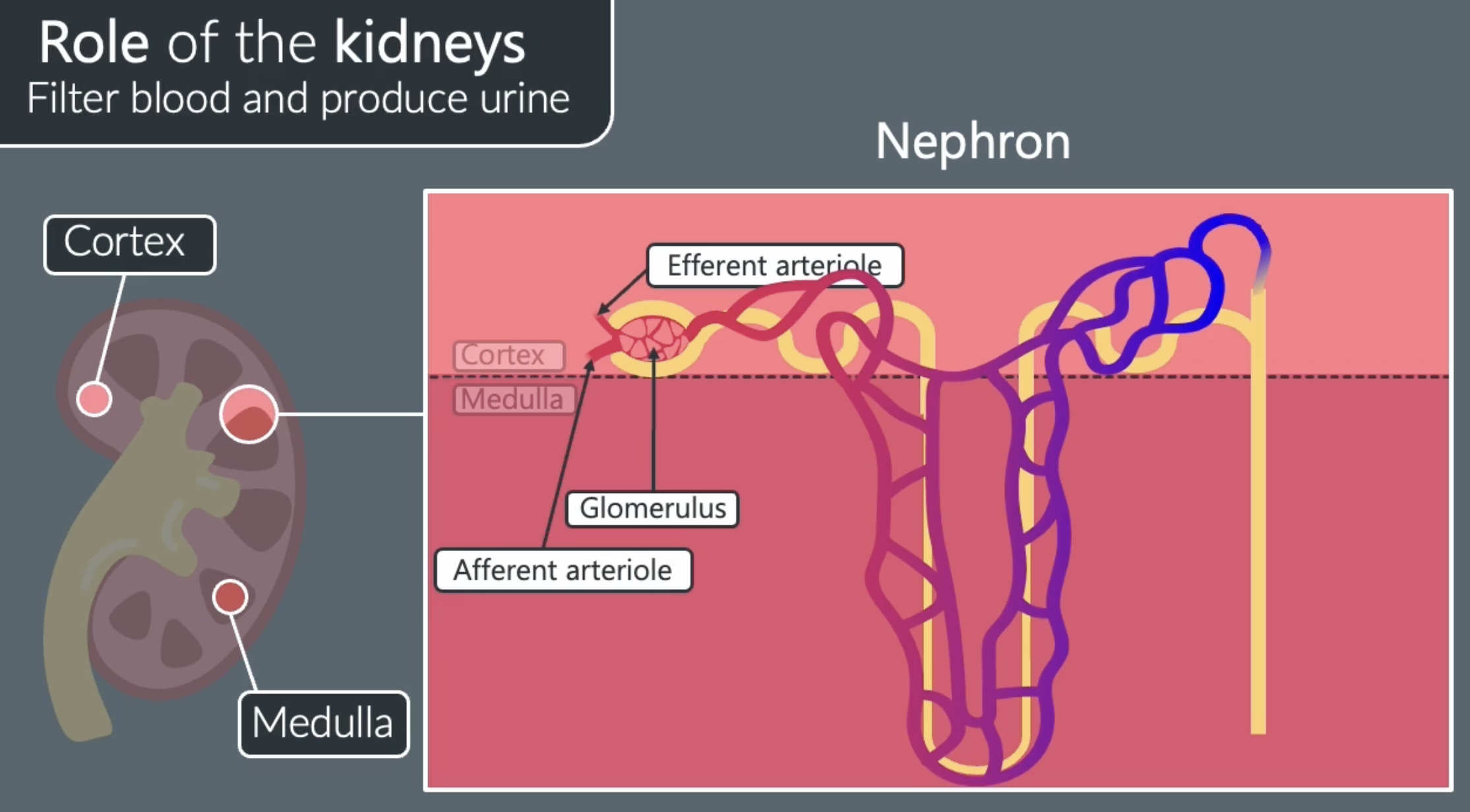
role of nephrons
urine is produced in nephrons
are responsible for filtering blood and producing urine
producing urine 1
the blood in the glomerulus has a high hydrostatic pressure because the afferent arteriole has a larger diameter than he efferent arteriole. this creates a pressure gradient between he glomerulus and bowmans capsule, causing substances to pass out of the glomerulus and into the bowmans capsule
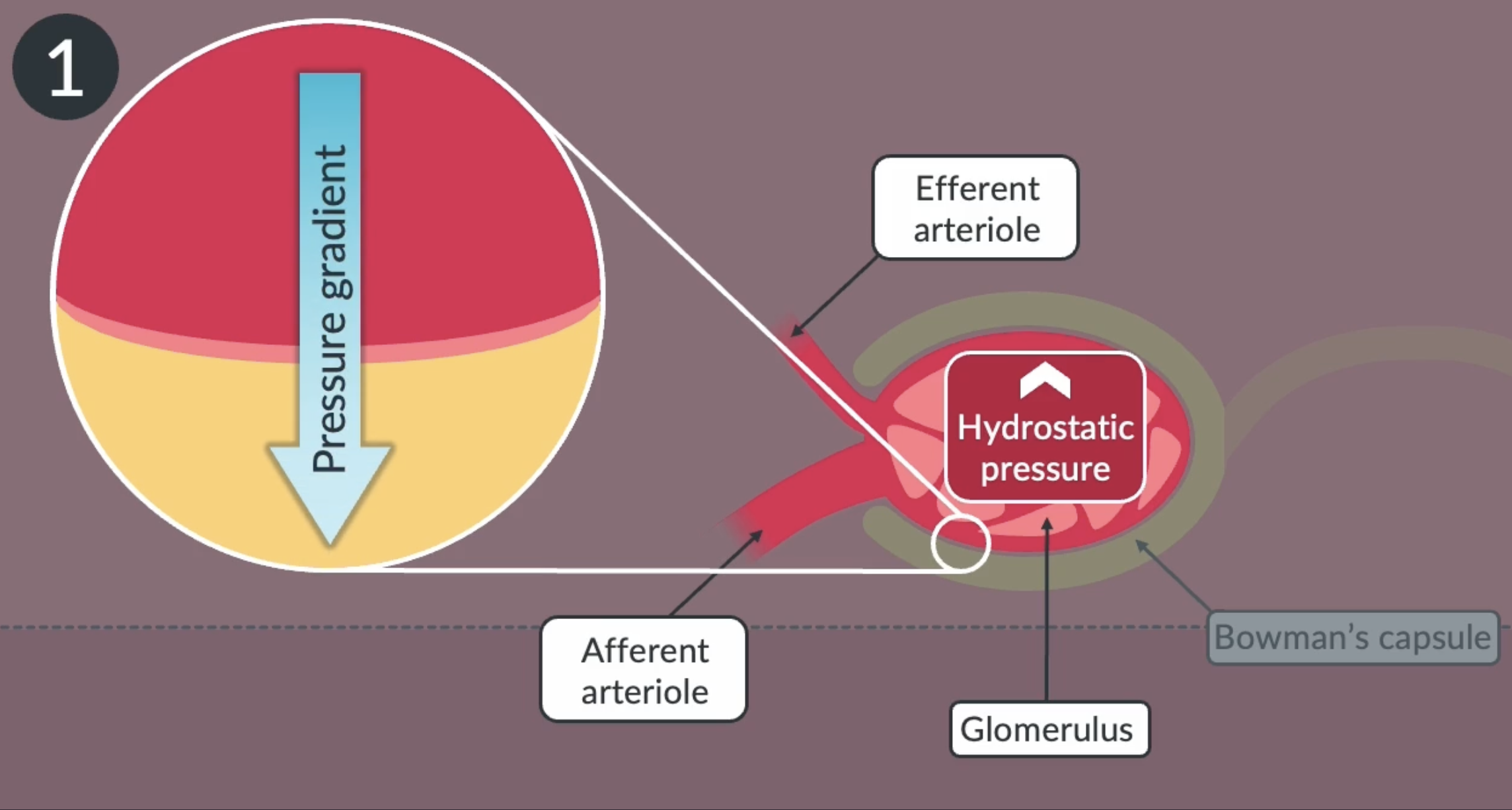
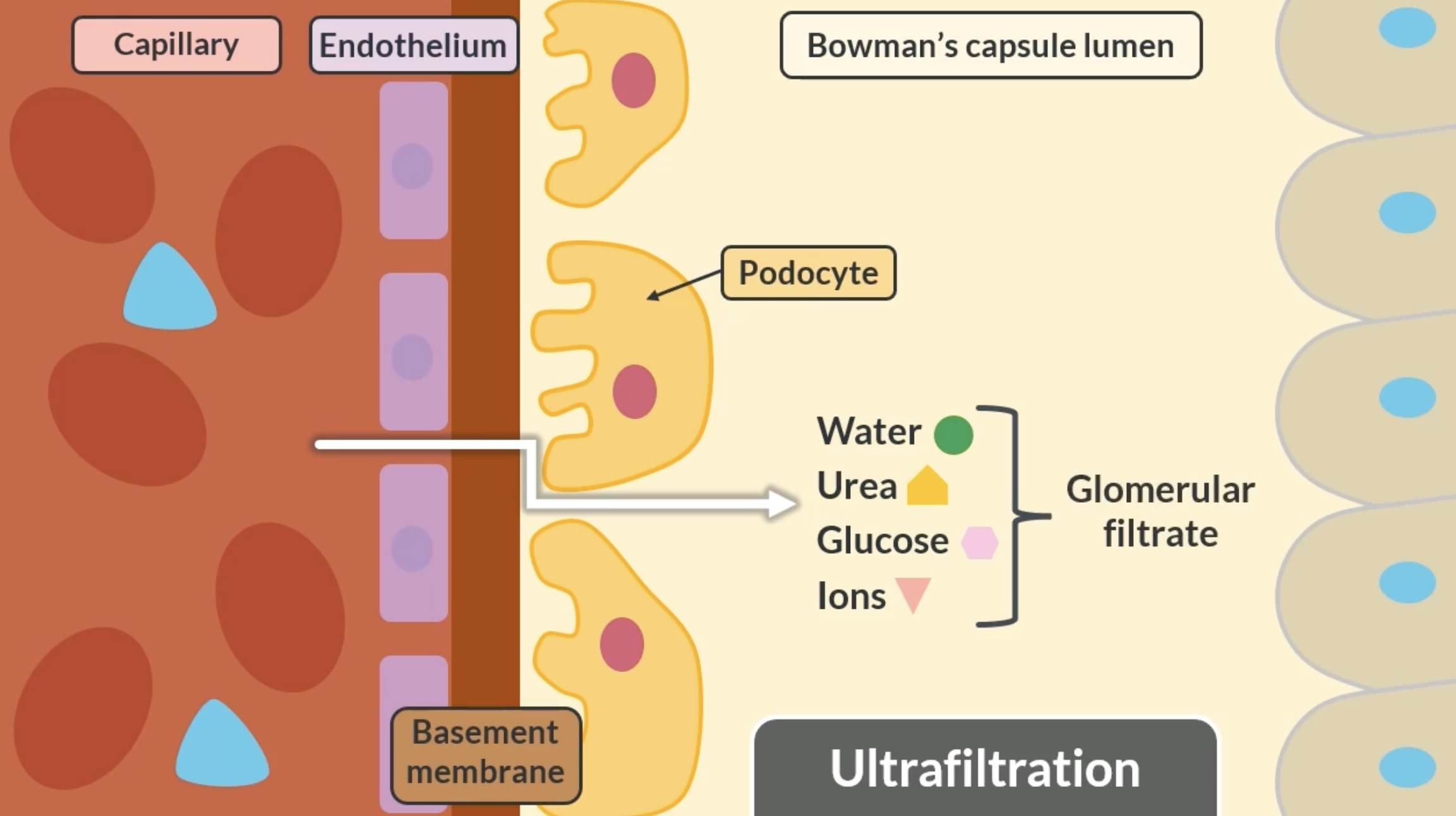
ultrafiltration
not all substances can move from the glomerulus into the bowmans capsule. this is due to a process called ultrafiltration. substances must pas through these 3 barriers:
-endothelium lining of the capillary
-basement membrane. contains pores that control the size of substances passing through
-podocytes = cells that line the bowman capsule. have gaps to control the movement of useful substances passing through
examples of substances that pass through: water, urea, glucose, ions = glomerular filtrate