Pharm ch. 14
1/108
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
109 Terms
Pharmacology of the CNS
: Study of drugs affecting the brain and spinal cord
CNS main functions
: Controls motor function, sensation, cognition, memory, emotions, and autonomic functions
Cerebrum function
: Motor control, interpretation, memory, feelings, reasoning
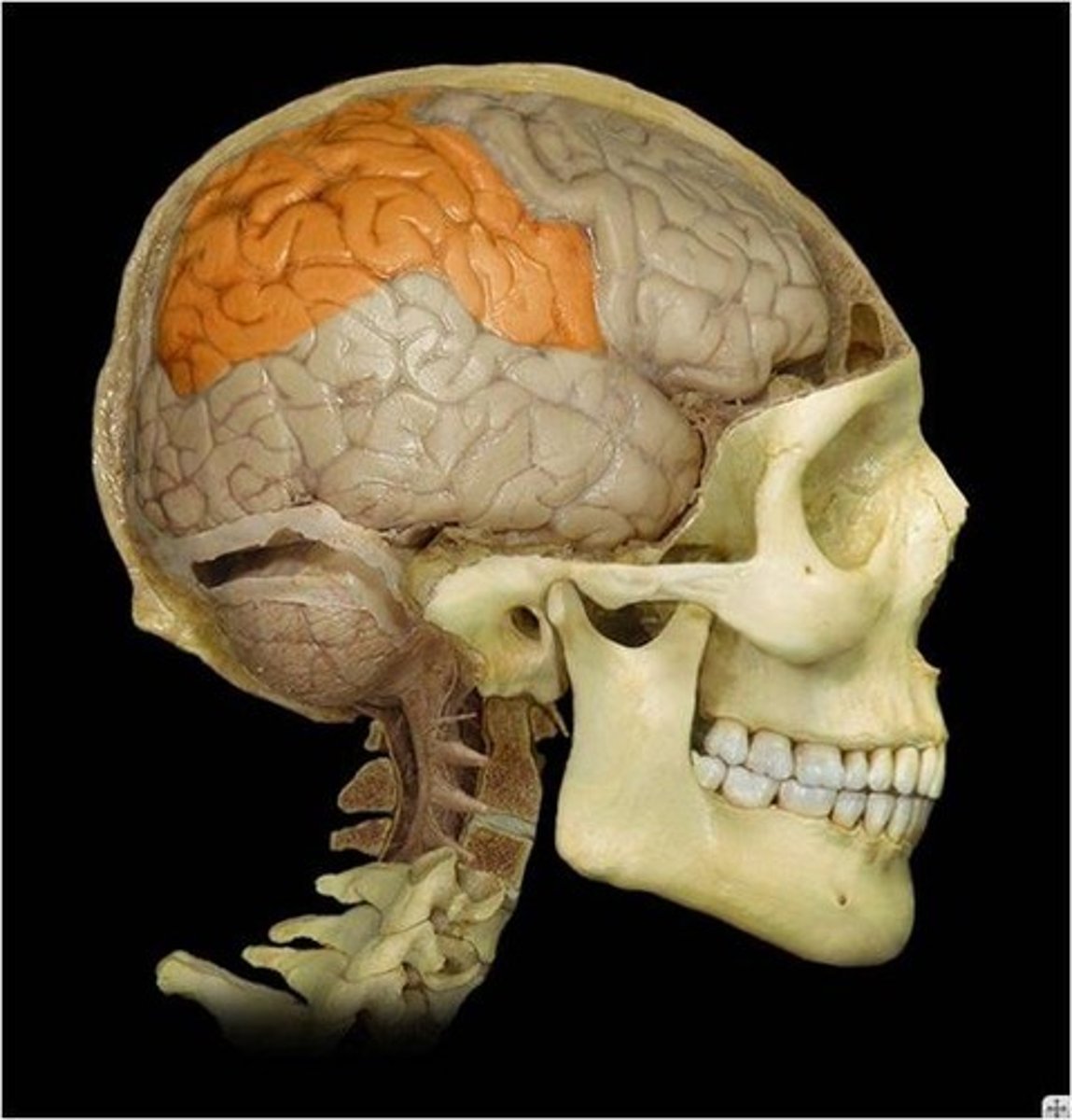
Diencephalon function
: Thalamus = sensory relay; Hypothalamus = homeostasis control
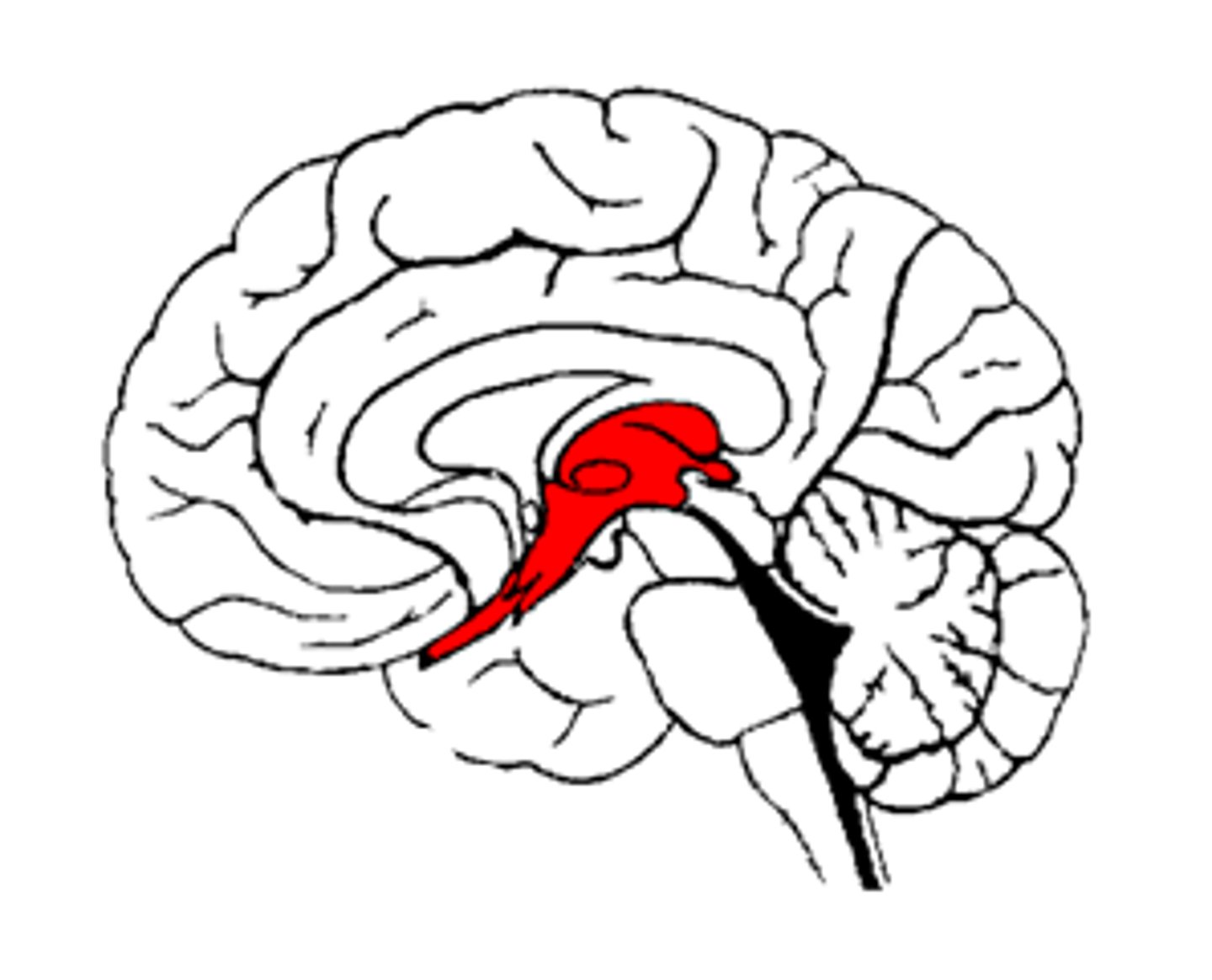
Midbrain function
: Eye movement, auditory and visual processing
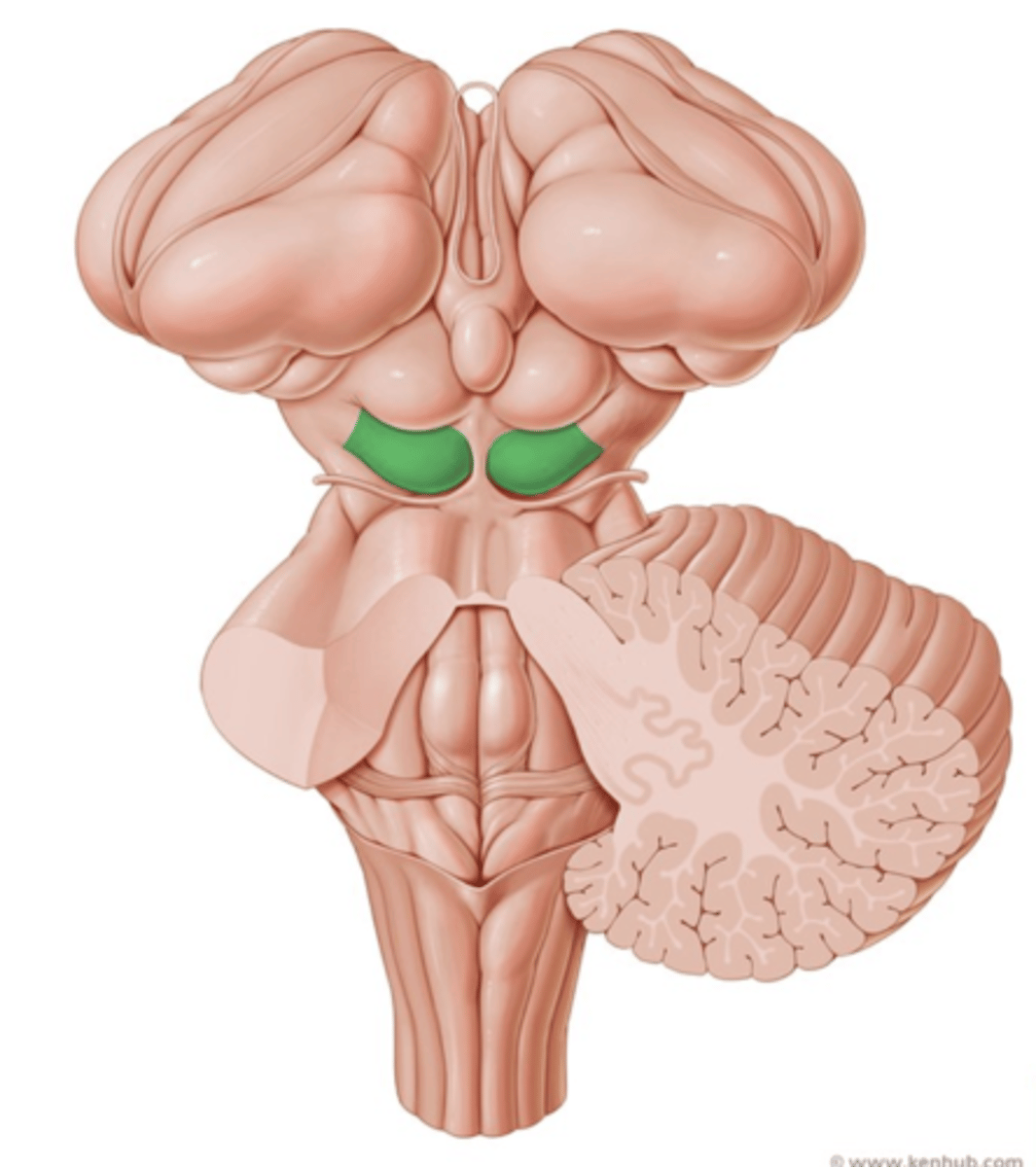
Pons function
: Sensory relay and respiratory rhythm control
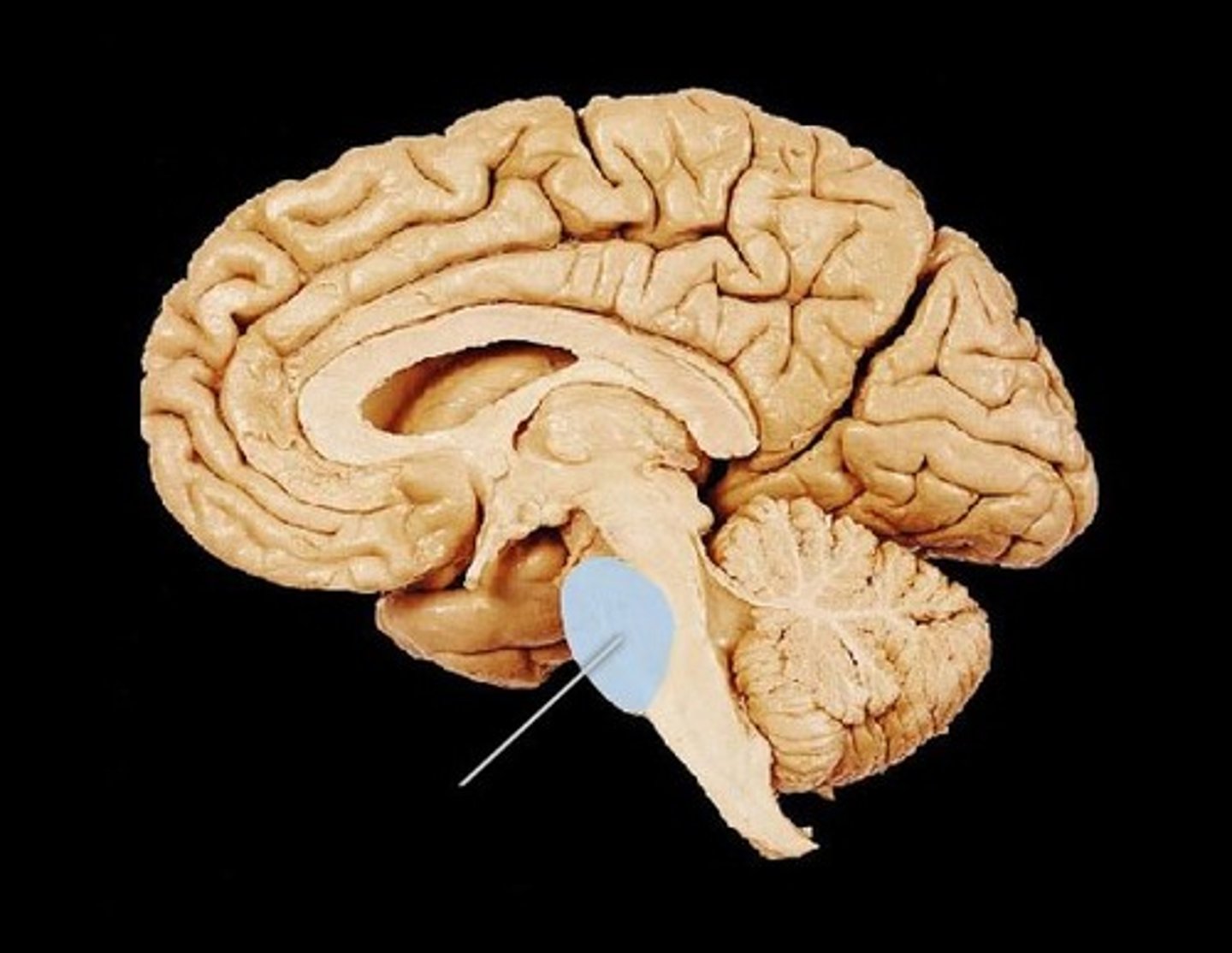
Medulla oblongata function
: Controls autonomic functions (breathing, heart rate)
Cerebellum function
: Coordinates movement and proprioception
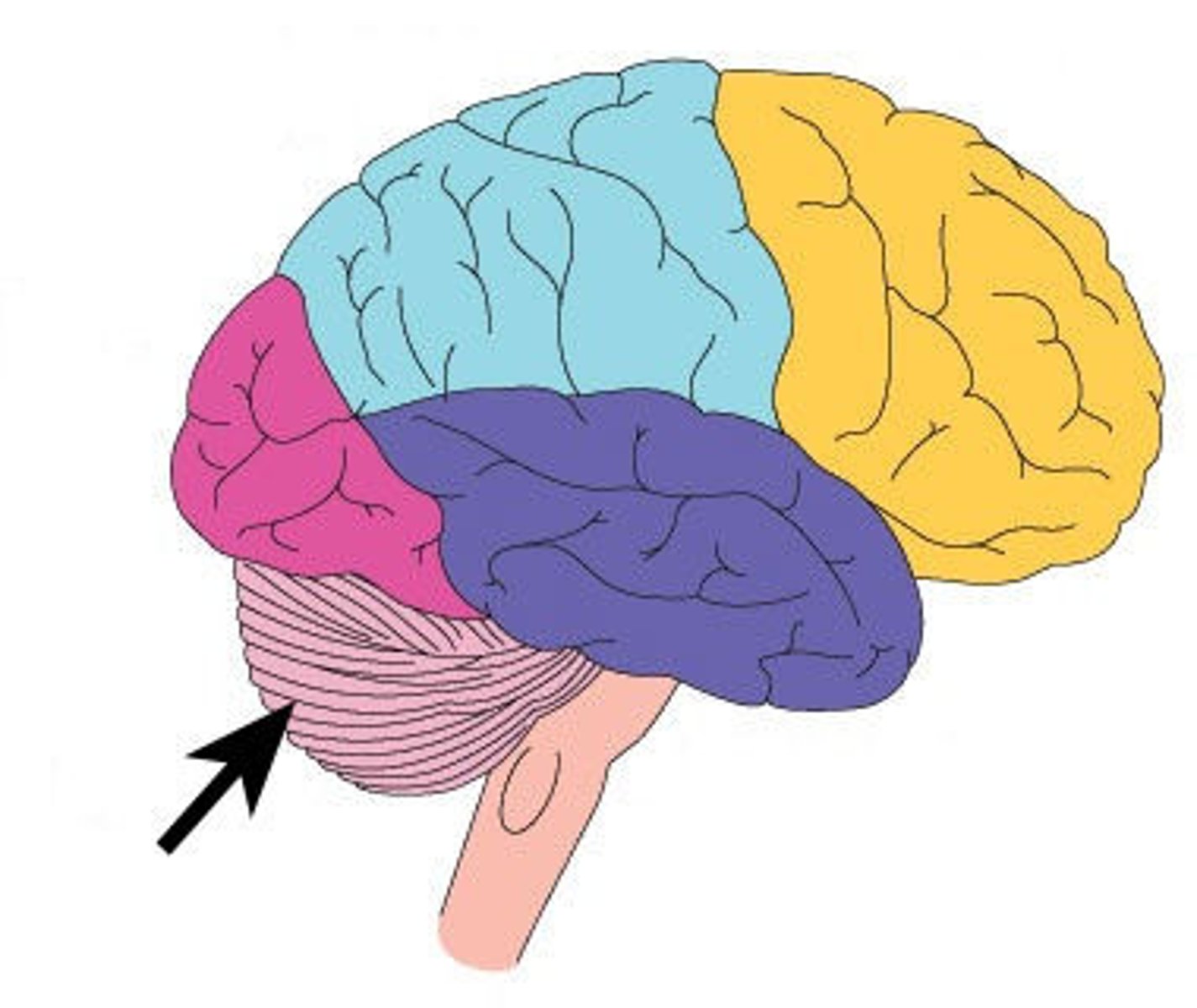
Why CNS knowledge matters in respiratory care
: Brainstem controls breathing, airway reflexes, and consciousness
Drug effects on CNS
: Enhance, prolong, or block neurotransmitters; alter synthesis/release
Analgesia
: Pain relief without loss of consciousness
Analgesic
: Drug that reduces or eliminates pain
Antidepressant
: Drug that treats depression by altering neurotransmitters
Antipsychotics
: Treat psychosis; affect dopamine; can cause movement disorders
Antipyretic
: Drug that reduces fever
Anxiolytic
: Drug that reduces anxiety
Conscious sedation
: Relaxed, responsive, maintains airway and breathing
Equianalgesic doses
: Equivalent pain-relief doses between drugs
Extrapyramidal symptoms (EPS)
: Tremor, rigidity, akathisia, dystonia
General anesthetic
: Causes complete loss of consciousness and reflexes
Hypnotic
: Drug that induces sleep
Sedative
: Calms patient, may cause drowsiness
Stimulant
: Increases CNS activity and alertness
Tardive dyskinesia
: Irreversible movement disorder from long-term antipsychotic use
Uricosuria
: Increased uric acid excretion in urine
Sedative effect
: Calming, decreased CNS activity
Hypnotic effect
: Promotes sleep
Anxiolytic effect
: Reduces anxiety
Barbiturates definition
: Powerful CNS depressants
Barbiturate uses
: Sedation, hypnosis, anesthesia induction, seizure treatment
Barbiturate mechanism
: Bind GABAA receptors → CNS depression
Barbiturate metabolism
: Liver
Barbiturate characteristic
: Redistribution
Benzodiazepines definition
: Common sedative-hypnotics and anxiolytics
Benzodiazepine advantages
: Safer, fewer side effects, less addiction than barbiturates
Benzodiazepine mechanism
: Enhance GABA effects
Common benzodiazepines
: Diazepam, lorazepam, midazolam, alprazolam, clonazepam, temazepam, triazolam, chlordiazepoxide
Alcohol mechanism
: Enhances GABA, inhibits excitatory neurotransmitters
Alcohol short-term effects
: Headache, nausea, confusion, thirst
Alcohol long-term effects
: Dementia, hepatitis, reflux
Psychopharmacology definition
: Use of drugs to treat mental disorders
Psychopharmacology conditions treated
: Schizophrenia, bipolar disorder, depression
Psychopharmacologic drug classes
: Antipsychotics, antidepressants, mood stabilizers, stimulants, anxiolytics
First-generation antipsychotics (FGAs)
: Treat psychosis but cause EPS and sedation
FGA mechanism
: D2 receptor antagonists
Examples of FGAs
: Haloperidol, chlorpromazine, fluphenazine, thioridazine, loxapine
Second-generation antipsychotics (SGAs)
: Fewer EPS, act on dopamine and serotonin
Examples of SGAs
: Clozapine, risperidone, olanzapine, quetiapine, ziprasidone, aripiprazole
Depression cause
: Changes in norepinephrine, serotonin, dopamine
Antidepressant classes
: SSRIs, SNRIs, TCAs, MAOIs
SSRI mechanism
: Block serotonin reuptake
SNRI mechanism
: Block serotonin and norepinephrine reuptake
Bupropion mechanism
: Blocks norepinephrine and dopamine reuptake
TCA mechanism
: Block norepinephrine and serotonin reuptake; affect other receptors
MAOI mechanism
: Inhibit monoamine oxidase → increase neurotransmitters
Antidepressant onset
: Initial 3 weeks, max 6 weeks
Lithium use
: Bipolar disorder
Lithium mechanism
: Increases serotonin and norepinephrine reuptake
Valproic acid mechanism
: Enhances GABA
Carbamazepine use
: Second-line bipolar treatment
CNS stimulants
: Increase norepinephrine and dopamine
Stimulant mechanisms
: Increase release, block reuptake, stimulate receptors
Stimulant use
: ADHD
Examples of stimulants
: Amphetamines, methylphenidate
Focal seizures
: Affect one area of brain
Generalized seizures
: Affect entire brain
Types of generalized seizures
: Absence, tonic-clonic, myoclonic, atonic
Antiepileptic drugs
: Phenytoin, carbamazepine, valproic acid, levetiracetam, phenobarbital, topiramate, ethosuximide, lacosamide
Opioid analgesics
: Treat moderate-to-severe pain
Non-opioid analgesics
: Treat mild-to-moderate pain
Pain scale
: 0-10 rating
Opioid mechanism
: Act on mu receptors
Opioid effects
: Pain relief and euphoria
Opioid adverse CNS effects
: Sedation, confusion, miosis
Opioid GI effects
: Nausea, vomiting, decreased motility
Opioid respiratory effects
: Decreased rate, tidal volume, respiratory arrest
Opioid cardiovascular effects
: Orthostatic hypotension
Opioid skin effects
: Itching, redness
Opioid GU effects
: Urinary retention, decreased libido
Opioid tolerance
: Need higher doses
Opioid dependence
: Withdrawal symptoms when stopped
Natural opioids
: Morphine, codeine
Semisynthetic opioids
: Hydrocodone, oxycodone, hydromorphone
Synthetic opioids
: Fentanyl, methadone, meperidine
Agonist-antagonist opioids
: Buprenorphine, nalbuphine, pentazocine
Opioid antagonists
: Naloxone, naltrexone
Naloxone use
: Reverses opioid overdose
Naloxone forms
: IV and intranasal
Non-opioid analgesics
: NSAIDs, acetaminophen, salicylates
NSAID mechanism
: Inhibit COX → decrease prostaglandins
NSAID effects
: Analgesic, anti-inflammatory, antipyretic
Common NSAIDs
: Ibuprofen, naproxen, aspirin, diclofenac, ketorolac
NSAID adverse effects
: GI upset, bleeding, renal dysfunction, hypertension
Acetaminophen use
: Pain and fever
Acetaminophen mechanism
: Weak COX inhibition
Acetaminophen advantage
: Fewer GI side effects
General anesthesia definition
: Loss of sensation and consciousness
General anesthetic mechanism
: Enhance GABA → CNS depression
Inhaled anesthetics
: Nitrous oxide, isoflurane, sevoflurane, desflurane
Inhaled anesthetic route
: Inhaled and absorbed into bloodstream/brain