Female Pelvis SG
1/75
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
76 Terms
Uterine positions
anteversion, anteflexion, anteversion/anteflexion, retroversion, retroflexion, retroflexed/retroverted, dextroversion, levoversion
Uterine Version =
vagina-cervix angle
Uterine Flexion =
cervix-body angle
Uterus is usually positioned:
Anteverted and anteflexed
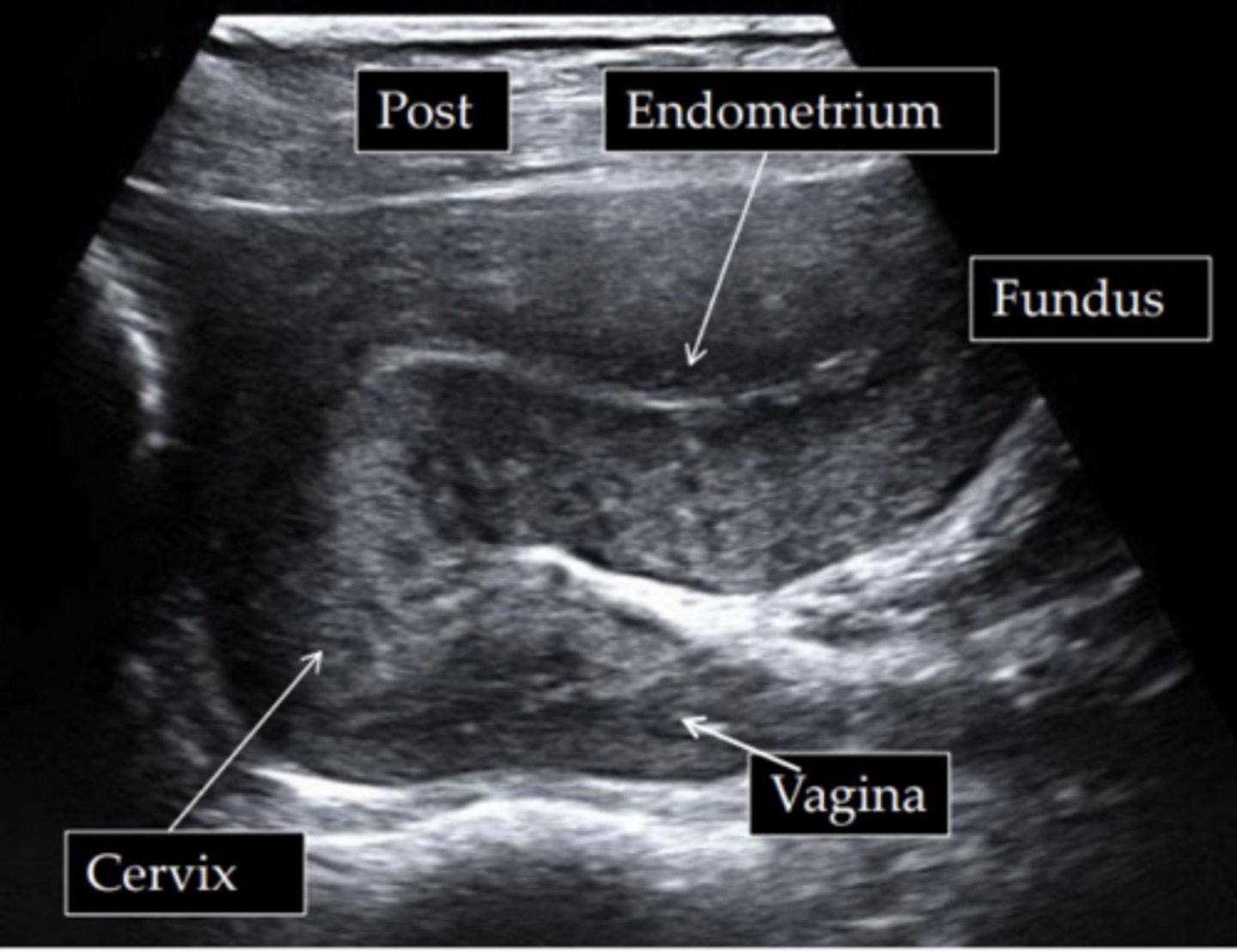
anteversion
the cervix forms a 90 degree or smaller anterior angle with the vaginal canal
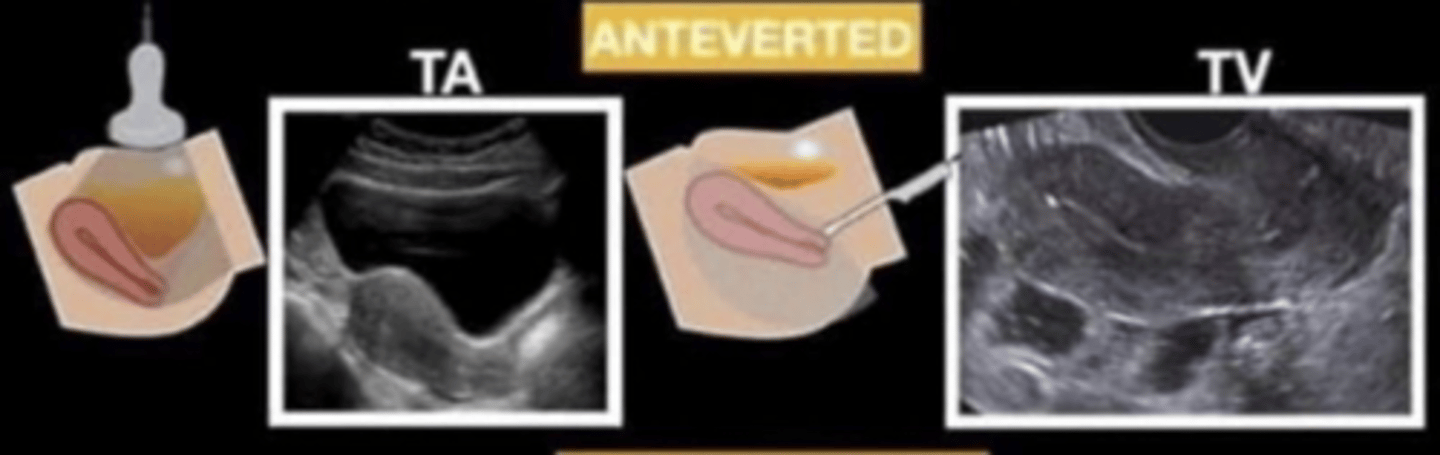
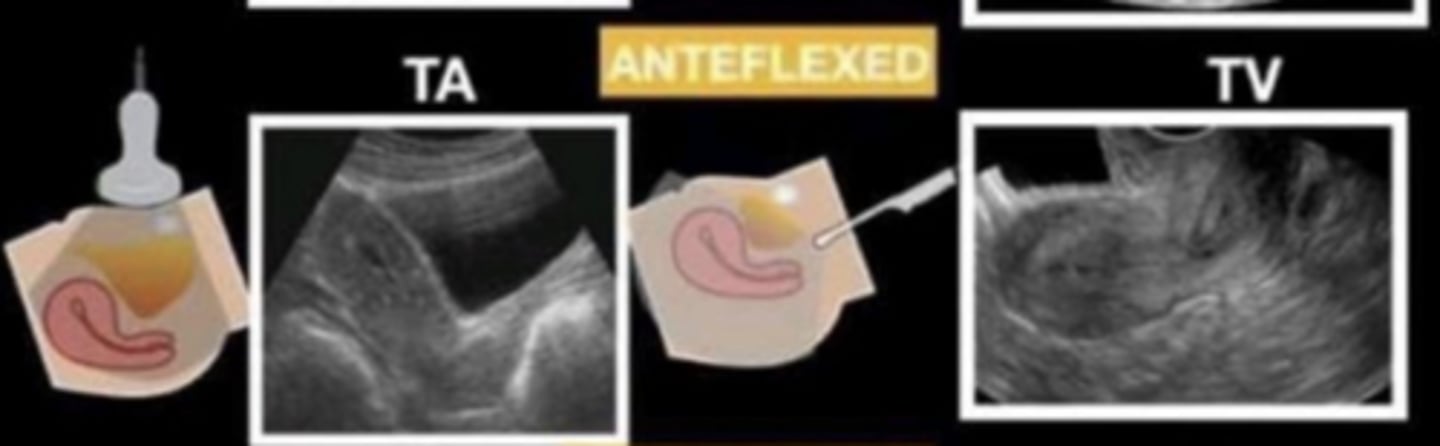
anteflexion
body and fundus only angle anteriorly
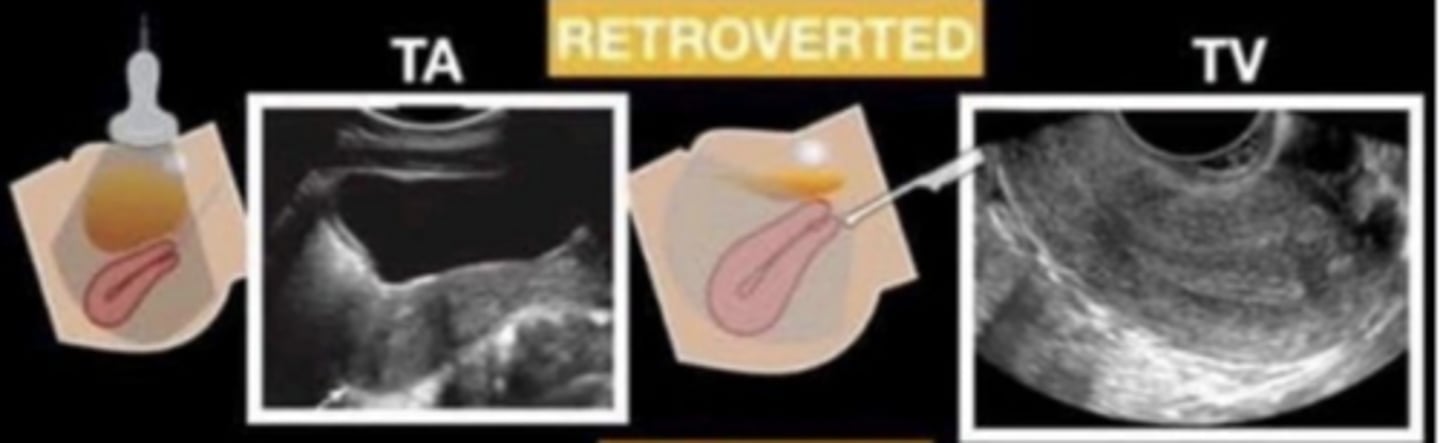
retroversion
the cervix forms an posterior angle of greater than 90 degrees to the vaginal canal
retroflexion
fundus and body bent posteriorly
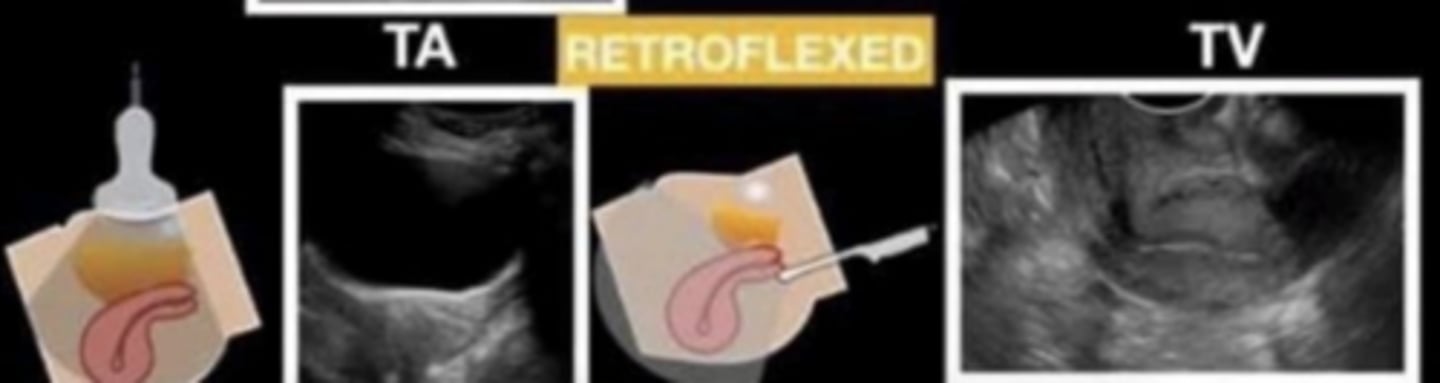
retroflexed/retroverted
entire uterus is angled posteriorly
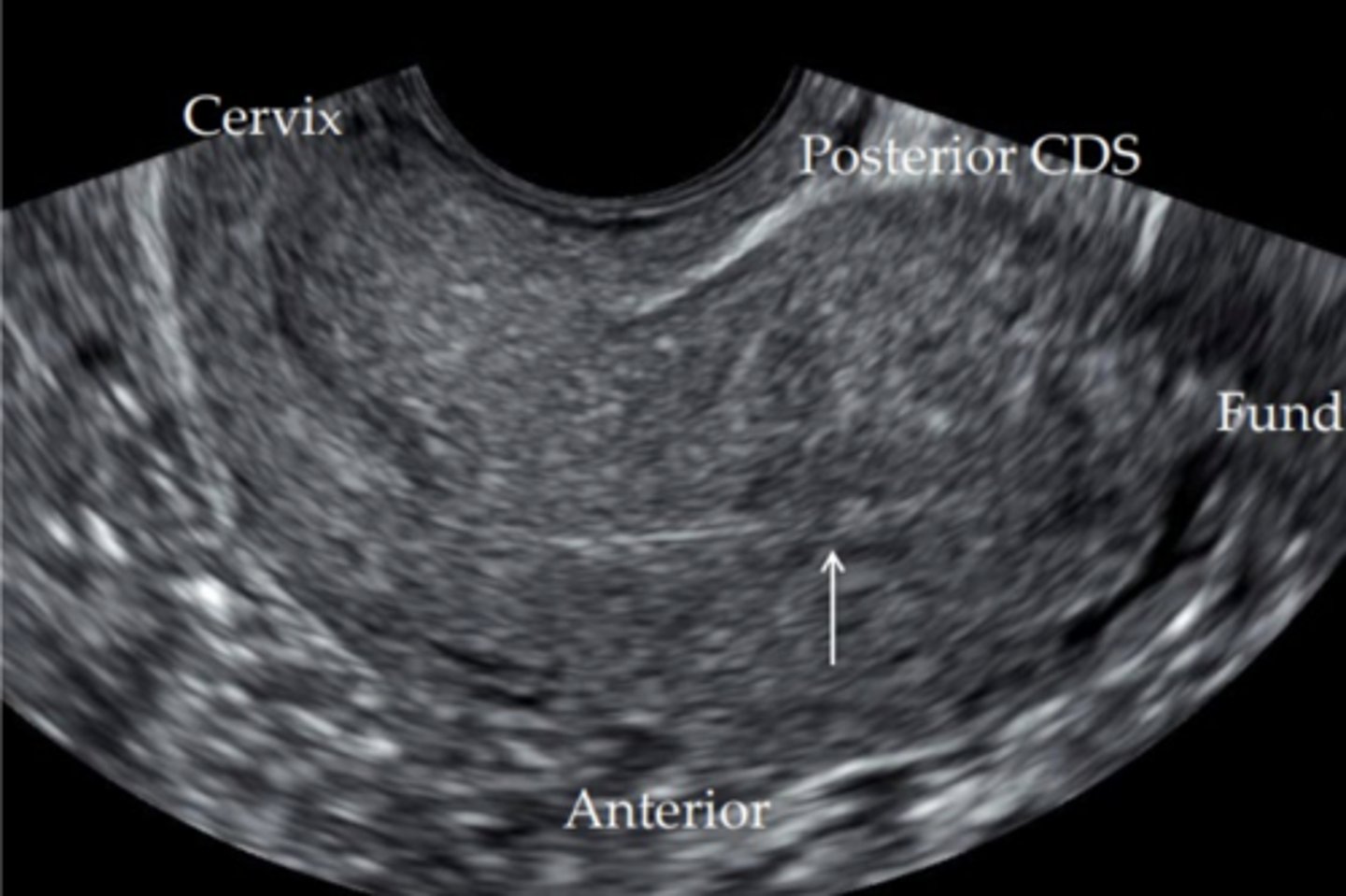
dextroversion
normal variant to the right in absence of pelvic masses
levoversion
normal variant to the left in absence of pelvic masses
Postmenopausal patients who are not on HRT (hormone replacement therapy) should have endometrial thickness of _____.
<5 mm
Postmenopausal patients on HRT or taking tamoxifen may demonstrate normal endometrial thicknesses up to _______.
8 mm
Postmenopausal patients with an endometrial thickness grater than 8mm, would be consider ____________.
hyperplasia
Echogenicity of ovaries
ovoid medium-level
What is LMP?
last menstrual period
What does the pituitary gland secrete?
Luteinizing Hormone (LH)
When does progesterone levels decline?
9-11 days after ovulation
What is GPA?
Gravida/para/abortus
Gravida in GPA is defined as:
the total number of times the patient has been pregnant
Para in GPA is defined as:
the number of live births (viable children) that the patient has had
Abortus in GPA is defined as:
the total number of miscarriages or elective abortions
What does the hypothalamus release?
gonadotropin-releasing hormone (GnRH)
Estrogen is secreted by
follicles
Progesterone secreted by
corpus luteum
Ovulation normally occurs on day ___
14
What triggers ovulation?
LH surge, accompanied by smaller FSH surge
Process of ovulation regulated by _________________ within the brain.
hypothalamus
What are the different stages of ovulation?
Follicular Phase (Preparation), Ovulatory Phase (Release), Luteal Phase (Post-Ovulation)
Follicular Phase
ovarian follicles grow, they fill with fluid (antrum) and secrete increasing amounts of estrogen
Ovulation Phase
ovum/egg released once a month from a ruptured Graafian follicle from one of two ovaries
Luteal Phase
cells in lining of ruptured ovarian follicle begin to multiply and create the corpus luteum, or yellow body
Luteinizing hormone level will typically increase rapidly ________hours before ovulation in process known as LH surge.
24 to 36
Mittelschmerz
lower pelvic pain during ovulation
Muscles of the pelvis major (false)
psoas major and iliacus muscles
Muscles of the pelvis minor (true)
piriformis muscles and obturator internus muscles
When is FSH released?
days 1 - 14
What does FSH do?
stimulates development of the follicle in the ovaries
Pelvic vasculature in descending order in size:
uterine, arcuate, radial, basal, spiral
The bony pelvis consists of four bones:
Right and Left Coxal, Sacrum, Coccyx
Where is the pelvis major (false pelvis) located?
superior to the iliopectineal line
Where is the pelvis minor (true pelvis) located?
inferior to caudal portion of parietal peritoneum
Uterus is derived from
embryonic mullerian ducts
What shaped does the uterus have?
pear shaped, hollow
Uterus is divided into
fundus, body, and cervix
Largest to smallest segments of the fallopian tube:
ampulla, isthmus, interstitial portion
What are the uterine ligaments?
broad, round, cardinal, uterosacral, suspensory, and ovarian
Broad ligament divides into:
Mesosalpinx, Mesovarium, and Mesometrium
mesosalpinx of broad ligament
upper fold of broad ligament; encloses fallopian tube
mesovarium of broad ligament
posterior fold of broad ligament; encloses ovary
mesometrium of broad ligament
between mesovarium and mesosalpinx
Round Ligament
Fundus to anterior pelvic sidewalls; holds uterus forward
Cardinal ligament
Extend across pelvic floor laterally; firmly supports cervix
Uterosacral ligament
Extend from uterine isthmus posteriorly, alongside rectum to sacrum; firmly supports cervix
Suspensory ligament
Extends from lateral aspect of ovary to pelvic sidewall
What are the three pouches?
vesicouterine pouch, rectouterine pouch, retropubic space
Where is the vesicouterine pouch located?
anterior to fundus, between uterus and bladder
Where is the rectouterine pouch located?
posterior to uterine, between uterus and rectum
Where is the retropubic space located?
space of retzius, between bladder and symphysis pubis
Menstrual status divided into 4:
premenarche, menarche, menstrual cycle, and menopause
Premenarche
prepuberty
Menarche
onset of menses
Menstrual cycle
menstruating approximately every 28 days
Menopause
cessation of menses
What is the name for endometrial regeneration?
proliferative phase
Graafian follicle
mature follicle
Corpus luteum
enlarged ovarian follicle that secretes progesterone after release of the egg cell
Layers of the uterus
perimetrium, myometrium, endometrium
Perimetrium
serous outer layer (serosa)
Myometrium
muscular middle layer
Endometrium
inner mucous (mucosal) membrane, glandular portion of uterine body
What are the 2 zones of the endometrium?
zona functionalis and zona basalis
Zona Functionalis
superficial layer of glands and stromas (shedding)
Zona Basalis
deep layer of endometrial glands (regenerates)
How should the bladder be for a transvaginal ultrasound?
empty bladder
How should the bladder be for a transabdominal ultrasound?
distended bladder