4- Dilated cardiomyopathy.
1/20
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
21 Terms
What is the definition of cardiomyopathy
myocardial disorder in which the heart muscle is structurally and functionally abnormal
In the absence of what diseases can you CM be diagnosed
coronary artery disease
hypertension
valvular disease
congenital heart disease
or the degree is not sufficient to cause the observed myocardial abnormality
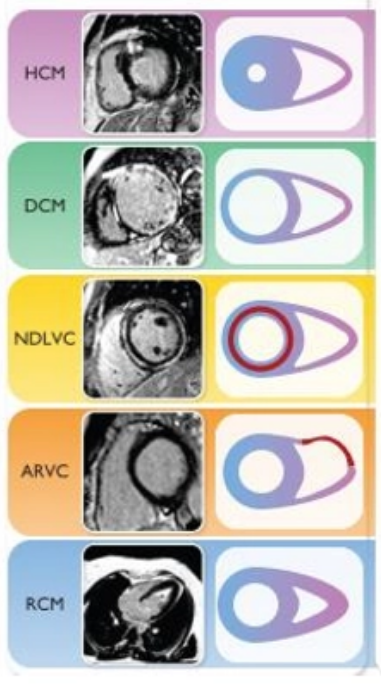
What is the classification of cardiomyopathies- ESC guidelines
hypertrophic
dilatative
non dilated left ventricular
arrhythmogenic
restrictive
un classified- non compaction, Tako-Tsubo
What are secondary causes of DCM
myocarditis
chronic alcohol disease
endocrine disorders
chronic tachyarrhythmia
What is DCM
characterised by cavity enlargement and impaired systolic function
What is the etiology of DCM
familial 30-40%- most commonly AD
idiopathic
secondary causes
infections- Coxsackie B virus myocarditis
chronic alcohol disease
endocrine disorders- eg hyperthyroidism
chronic tachycardia- eg A fib
What is the morphology of DCM
Reversible/ irreversible damage of the myocardium
increased interstitial fibrosis
decreased systolic function
dilated cavities
thin ventricular walls
What are the symptoms of DMC
progressive disease- asymptomatic in early stage
symptoms of HF- fatigue
progresses- all signs of L and R ventricular HF
What is the pathomechanism of DCM
Causative factors decrease the contractility of myocardium
compensatory Frank Starling law- to maintain CO
increased EDV- preload
myocardial remodeling
eccentric hypertrophy + dilation of ventricle
decreased myocardial contractility
systolic dysfunction and decreased EF → HF
decreased LV contractility due to dilation → LSHF then eventual RSHF
What do you do to diagnose DMC
ECG
Imaging- echo, CMR, coronary CT angiography
What is seen during a physical examination
decreased BP, increased JVP, narrow PP
possible signs of RSHF- peripheral oedema, ascites, hepatomegaly
displaced apex, murmurs
What are the signs of DMC on an ECG
conduction disturbances- LBBB
atrial fibrillation
ventricular arrhythmias
What is seen on an echo, CMR
Echo is GOLD STANDARD
dilated cavities
diffuse hypokinesis
functional mitral/ tricuspid regurgitation
What are the complications of DCM
arrhythmias-
incl A fib, malignant arrhythmias- v. tachycardia, v. fibrillation
progression of systolic and diastolic dysfunction
functional mitral/ tricuspid regurgitation
intracardiac thrombus- LV, LA appendage
progression of HF, decompensation
How do you treat the underlying causes of DCM
avoid cardiotoxic agents, abstain from alcohol
treat infection and endocrine disorders
What is the treatment of HF
ACEi, BB, diuretics, digoxin, aldosterone antagonists
anticoagulants
What is the surgical treatments for DCM
if LVEF <35% → ICD to prevent SCD caused by V fib
heart transplant
How do you prevent SCD
ICD is recommended
When do you do primary prevention
symptomatic HF and EF <35% after ≥3 months OMT
When do you do secondary prevention
haemodynamically not tolerated VT/VF without any reversible cause
What are the non dilated left ventricular cardiomyopathies
isolated left ventricular dysfunction
non ischemic left ventricular scar
fatty infiltration
left ventricular wall motion abnormalitie