quiz 8 (congenital heart defects)
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
Which of the following vessels return blood to the right ventricle?
I. Pulmonary vein
II. Inferior vena cava
III. Superior vena cava
IV. Coronary sinus
a. I and IV only
b. II and III only
c. I, II, and III only
d. II, III, and IV only
d. II, III, and IV only
At birth, what factor causes dilation of the pulmonary vascular bed and a decrease in the pulmonary vascular resistance?
a. Increased arterial partial pressure of oxygen (PaO2)
b. Decreased arterial partial pressure of carbon dioxide (PaCO2)
c. Lung inflation
d. Circulating indomethacin
a. Increased arterial partial pressure of oxygen (PaO2)
What factor is responsible for closure of the foramen ovale?
a. Increased PaO2
b. Increased pressure on the left side of the heart
c. Blood flowing through the lungs
d. High pulmonary vascular resistance
b. Increased pressure on the left side of the heart
For which of the following congenital cardiac defects may spontaneous closure of the ductus arteriosus be catastrophic?
I. Tetralogy of Fallot with pulmonary atresia
II. Atrial septal defect
III. Severe coarctation of the aorta
IV. Hypoplastic left heart syndrome
a. I and III only
b. III and IV only
c. I, II, and IV only
d. I, III, and IV only
d. I, III, and IV only
How should the therapist interpret a preductal-to-postductal PaO2 difference of 8 mm Hg in a neonate?
a. Unreliable data
b. Absence of ductal shunting
c. Presence of ductal shunting
d. Inconclusive data
b. Absence of ductal shunting
Which of the following methods is involved in the management of a PDA?
a. Increasing the circulating volume
b. Maintaining/optimizing the hematocrit at the low end of normal hemoglobin level
c. Administering indomethacin
d. Administering digoxin
c. Administering indomethacin
Which of the following clinical manifestations is consistent with an atrial septal defect (ASD)?
a. An ASD often causes congestive heart failure (because of decreased pulmonary blood flow).
b. The right ventricle may become hypertrophic (right ventricular hypertrophy).
c. Most patients with an ASD are symptomatic in the neonatal intensive care unit, presenting with right atrial enlargement.
d. Chest radiographs are usually abnormal.
b. The right ventricle may become hypertrophic (right ventricular hypertrophy).
Which of the following clinical pathophysiologic manifestations are consistent with a large ventricular septal defect (VSD)?
1. The majority of the blood flow is shunted from left right to right left.
2. Shunting typically occurs during ventricular diastole, which causes left atrial enlargement.
3. Chest radiography reveals an enlarged cardiac silhouette and increased pulmonary vascular markings, increasing pulmonary blood flow.
4. Thickening and fibrosing of the pulmonary veins develop, decreas
2 and 3
2. Shunting typically occurs during ventricular diastole, which causes left atrial enlargement.
3. Chest radiography reveals an enlarged cardiac silhouette and increased pulmonary
vascular markings, increasing pulmonary blood flow.
Why must supplemental oxygen be judiciously administered to patients with an atrioventricular canal defect?
a. To prevent the development of retinopathy of prematurity
b. To avoid oxygen-induced hypoventilation
c. To minimize pulmonary vascular dilation
d. To reduce oxidative stress
c. To minimize pulmonary vascular dilation
Which of the following clinical features characterize a critical aortic stenosis in a neonate?
a. Chest radiography reveals pleural effusion and pulmonary engorgement.
b. The neonate often has metabolic alkalosis.
c. The neonate presents in cardiogenic shock with hypotension.
d. These infants are rarely symptomatic during the first month of life.
c. The neonate presents in cardiogenic shock with hypotension.
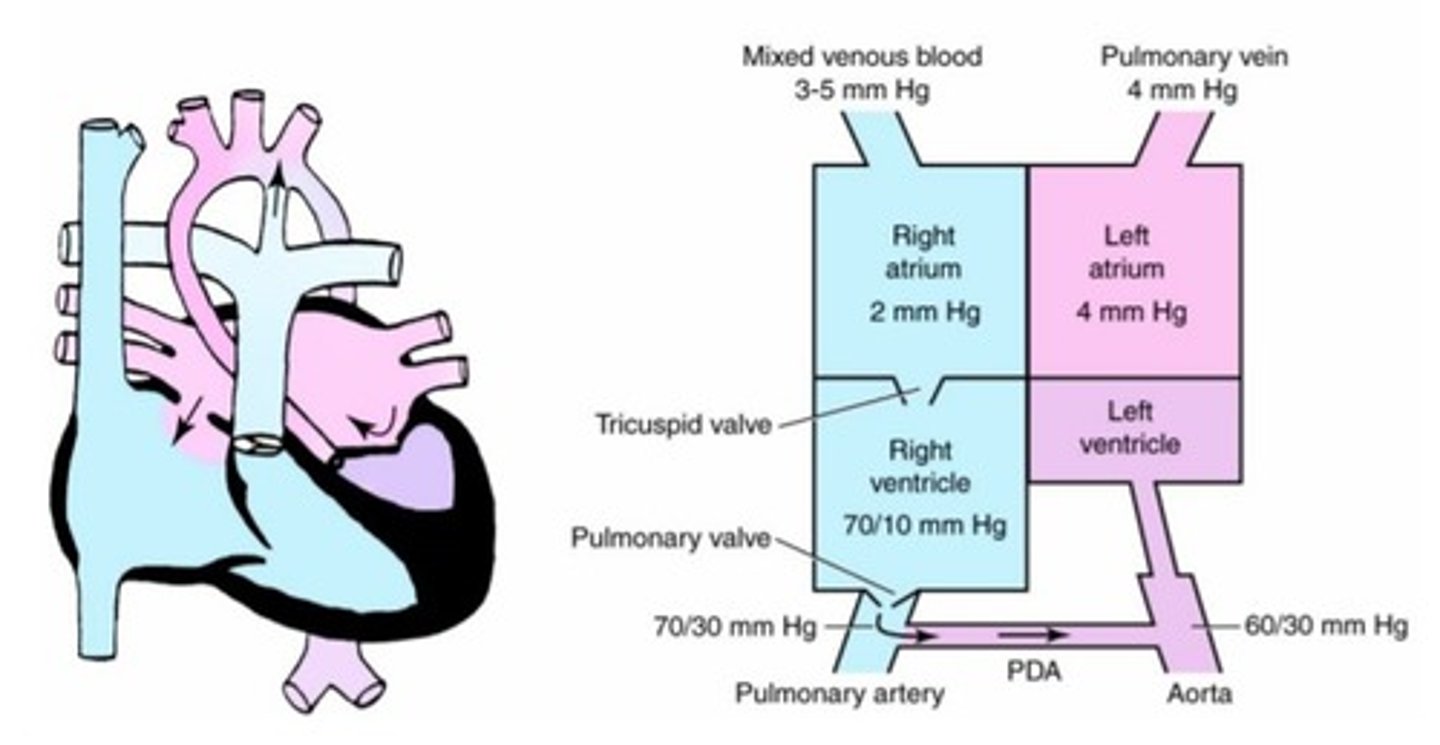
a. Atrial septal defect
b. Hypoplastic left ventricular syndrome
c. Hypoplastic right ventricular syndrome
d. Atrioventricular canal defect
b. Hypoplastic left ventricular syndrome
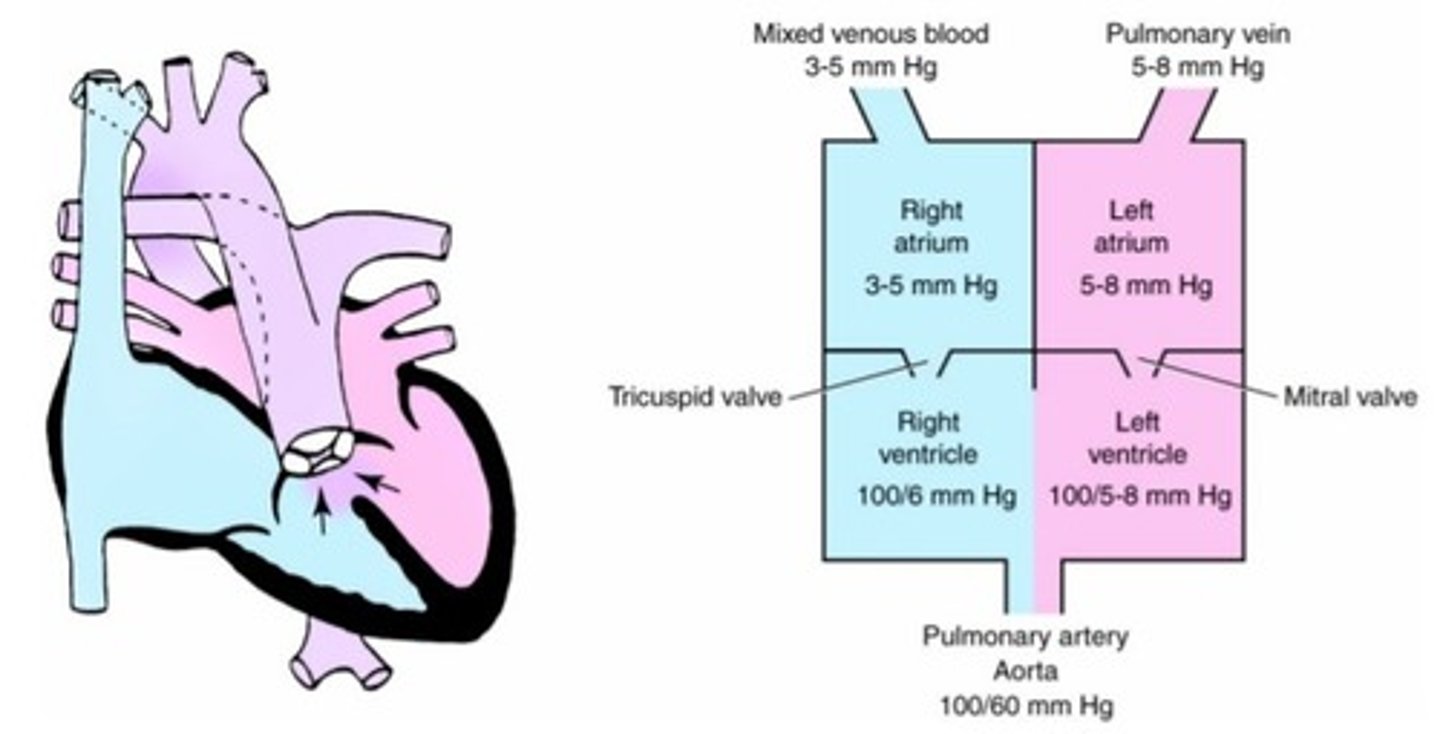
a. truncus arteriosus
b. hypoplastic left ventricle
c. transposition of the great vessels
d. ventricular septal defect
a. truncus arteriosus
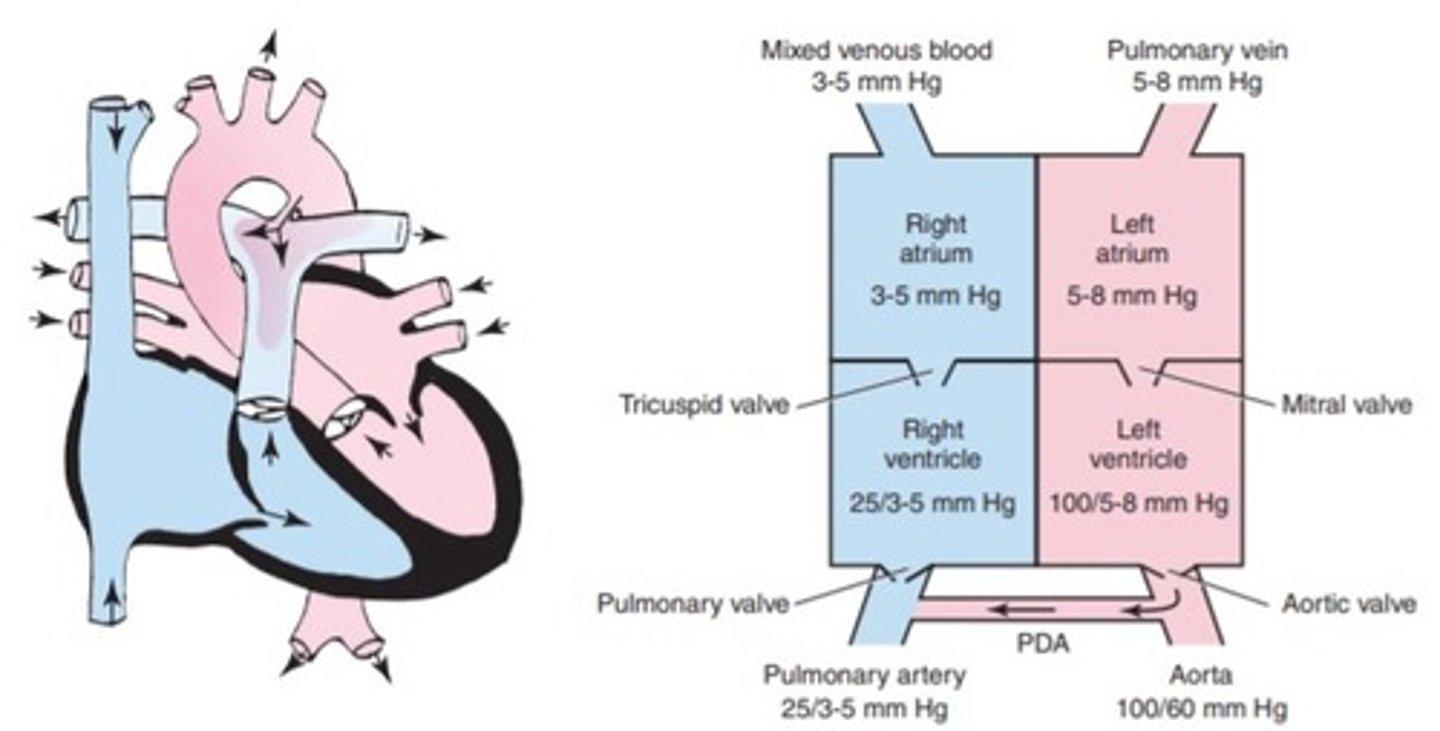
a. Atrial septal defect
b. Hypoplastic left ventricular syndrome
c. Patent ductus arteriosus
d. Atrioventricular canal defect
c. Patent ductus arteriosus
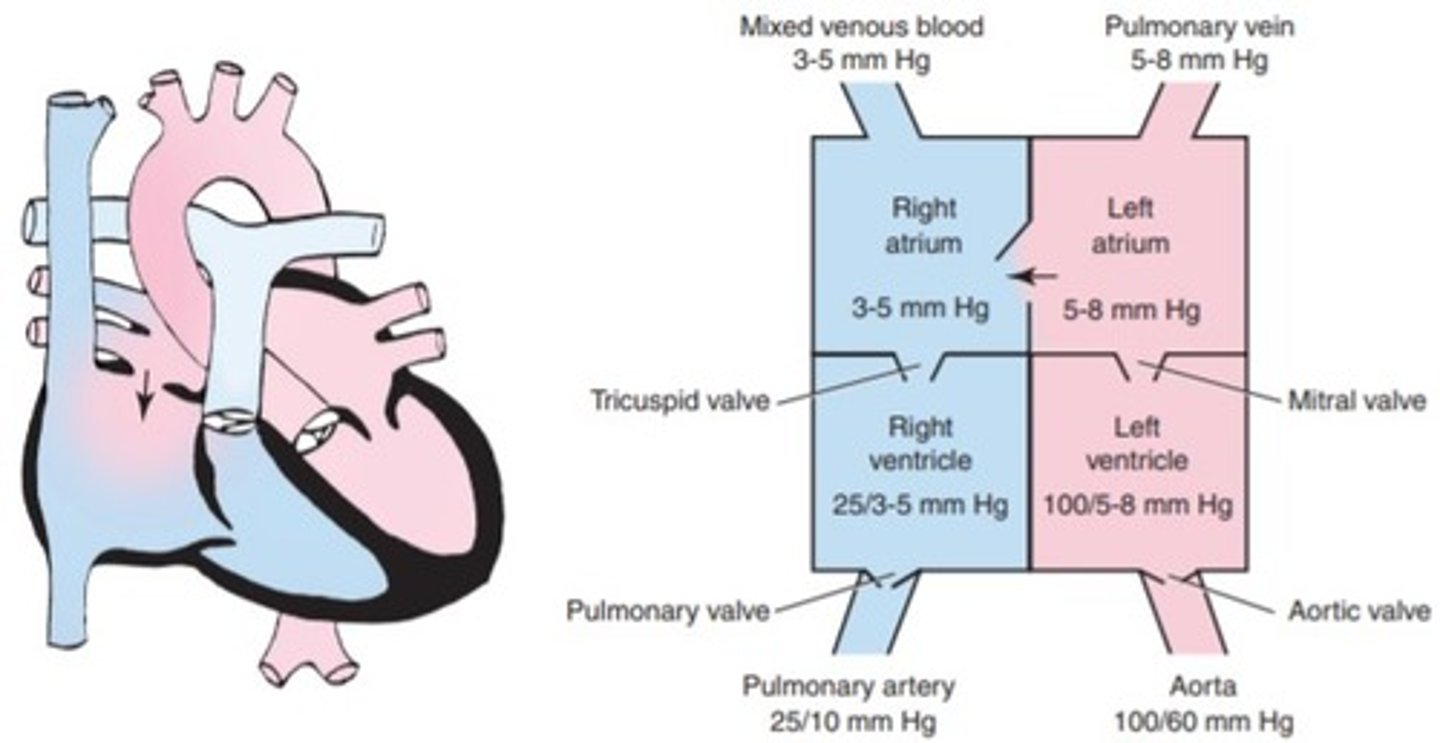
a. Atrial septal defect
b. Hypoplastic left ventricular syndrome
c. Patent ductus arteriosus
d. Atrioventricular canal defect
a. Atrial septal defect
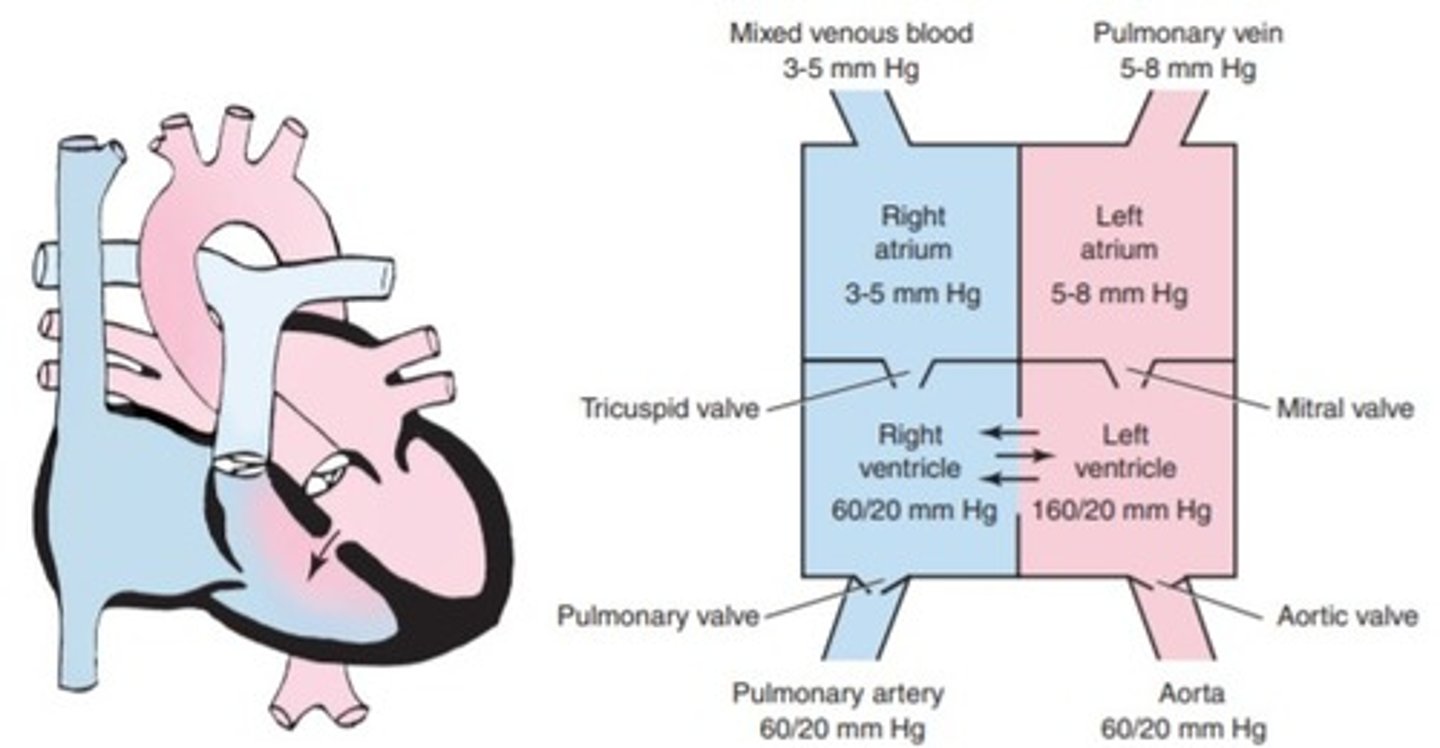
a. truncus arteriosus
b. hypoplastic left ventricle
c. transposition of the great vessels
d. ventricular septal defect
d. ventricular septal defect
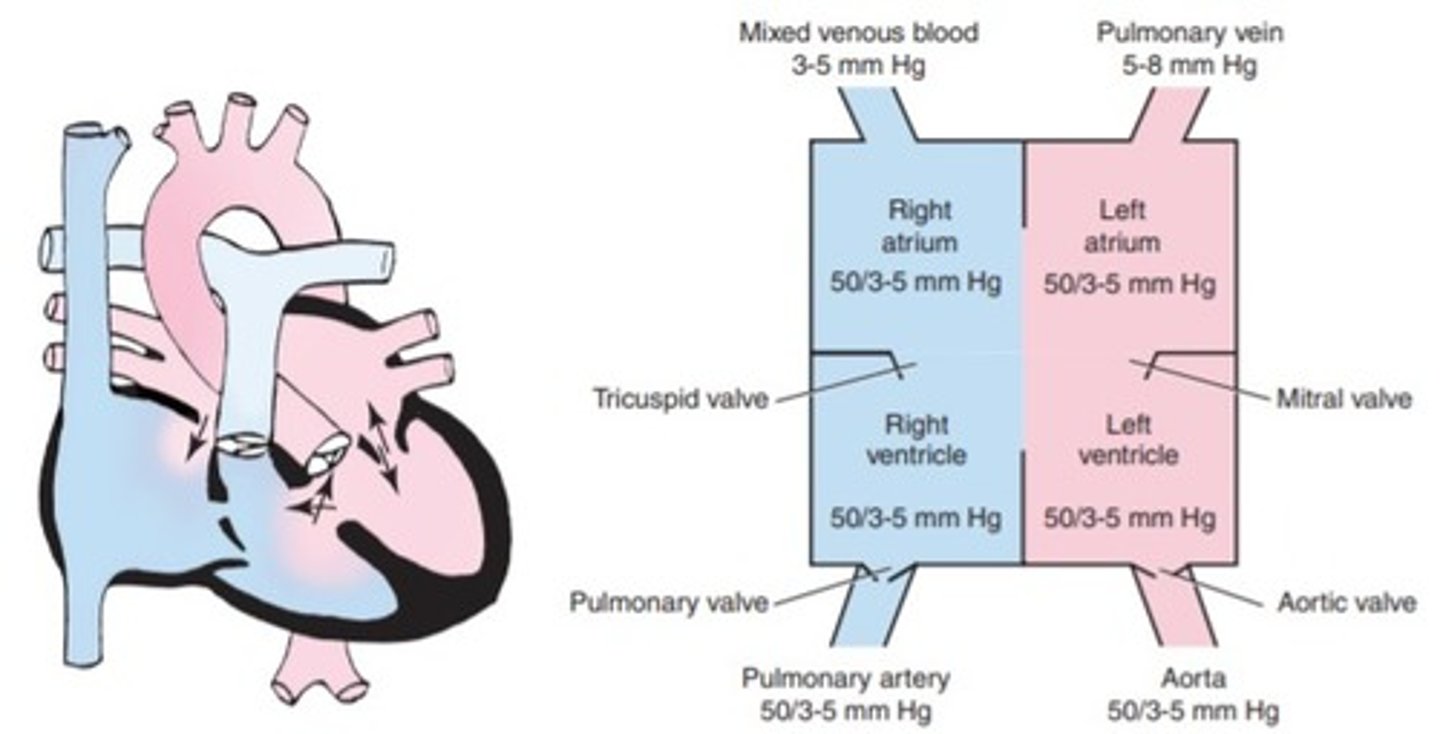
a. Atrial septal defect
b. Hypoplastic left ventricular syndrome
c. Patent ductus arteriosus
d. Atrioventricular canal defect
d. Atrioventricular canal defect
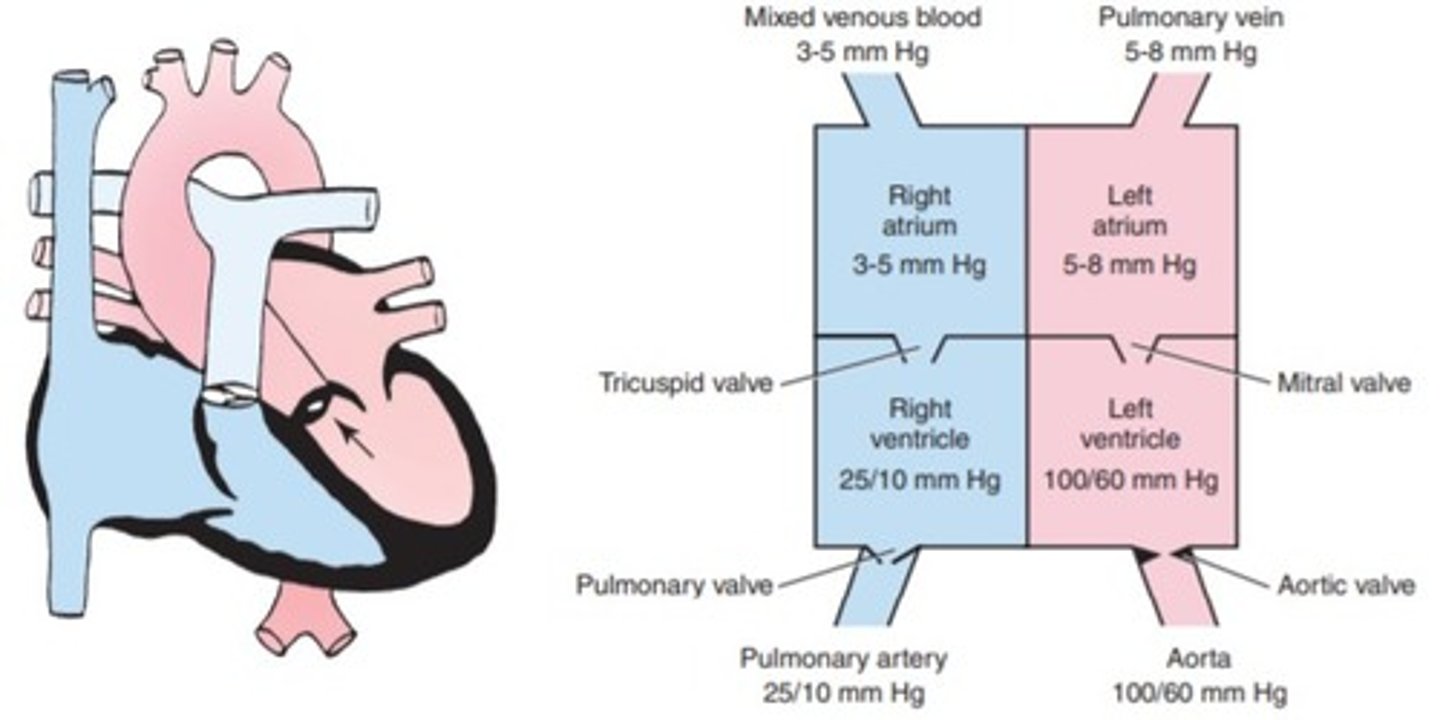
a. truncus arteriosus
b. aortic stenosis
c. transposition of the great vessels
d. ventricular septal defect
b. aortic stenosis
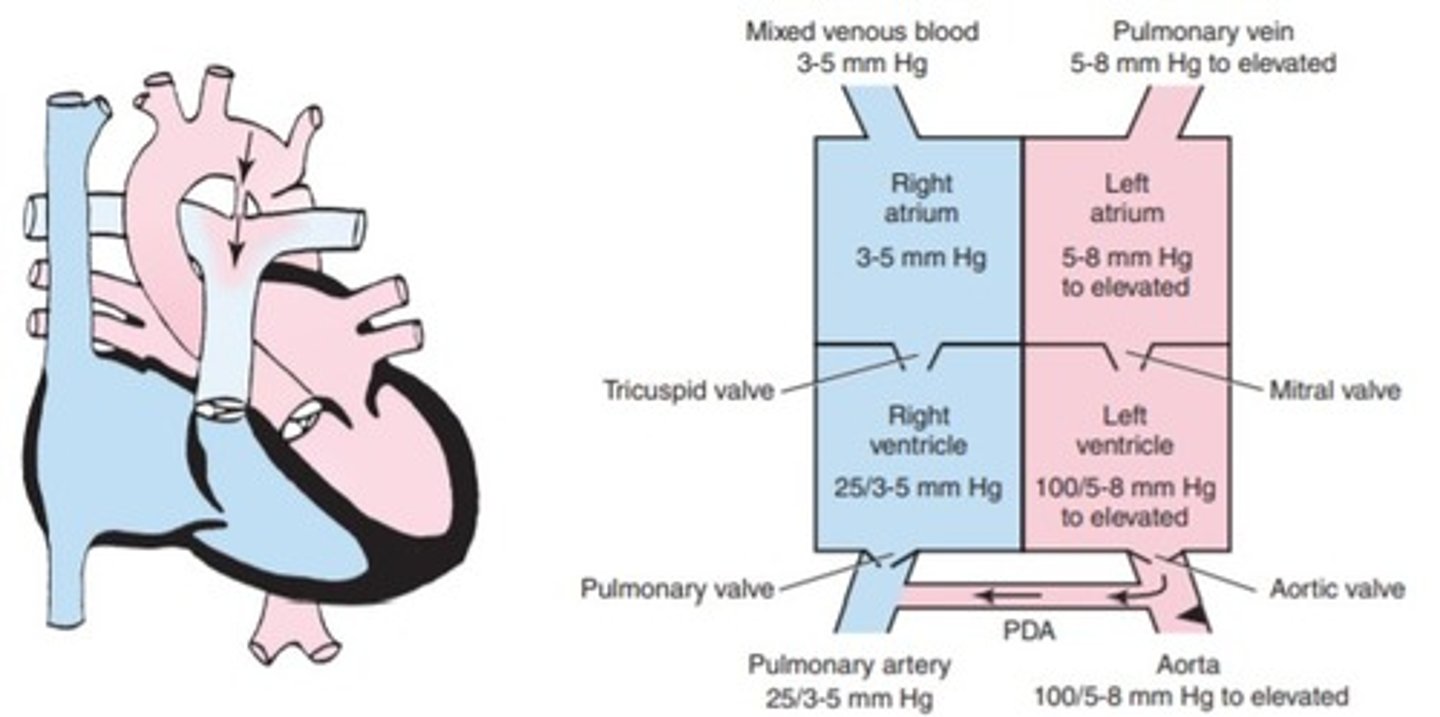
a. coarctation of the aorta
b. aortic stenosis
c. transposition of the great vessels
d. ventricular septal defect
a. coarctation of the aorta
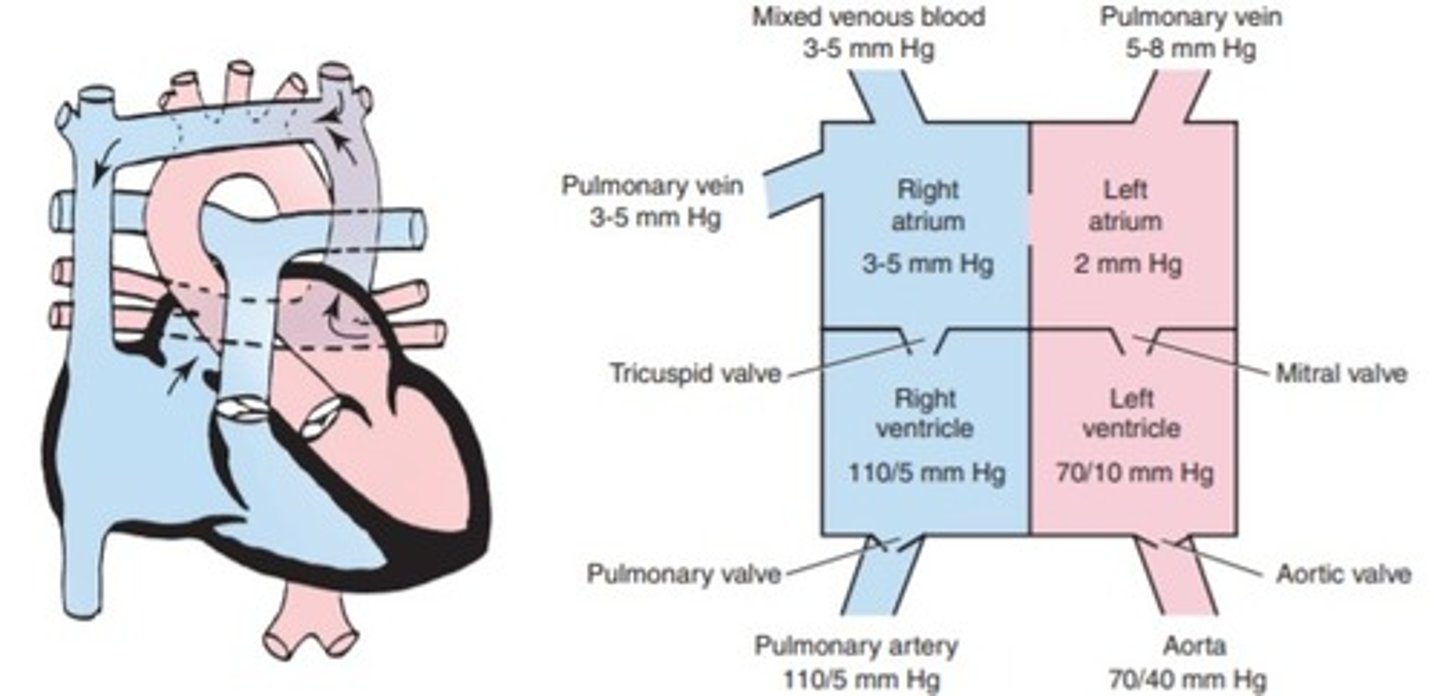
a. coarctation of the aorta
b. aortic stenosis
c. transposition of the great vessels
d. Total anomalous pulmonary venous return
d. Total anomalous pulmonary venous return
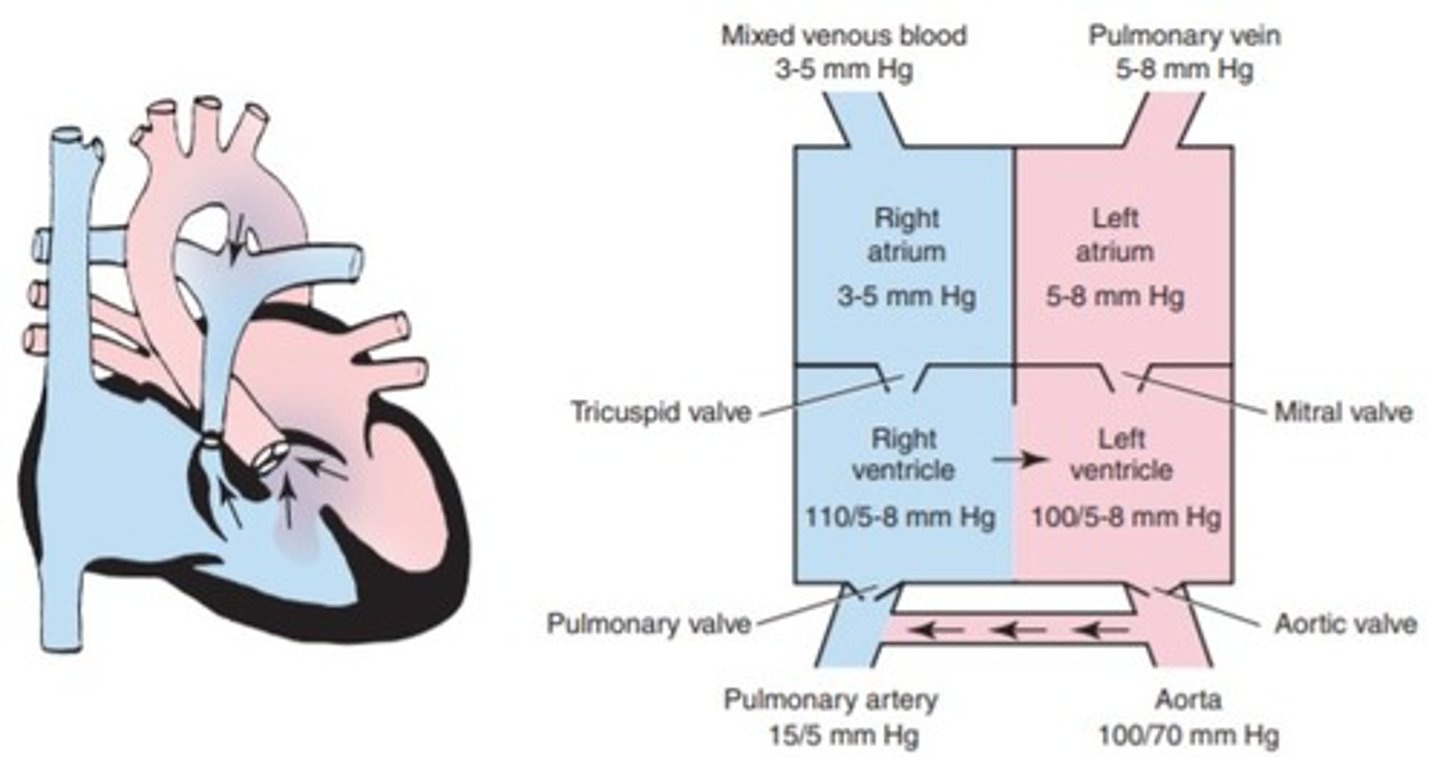
a. Atrial septal defect
b. Hypoplastic left ventricular syndrome
c. Patent ductus arteriosus
d. Tetrology of Fallot
d. Tetrology of Fallot
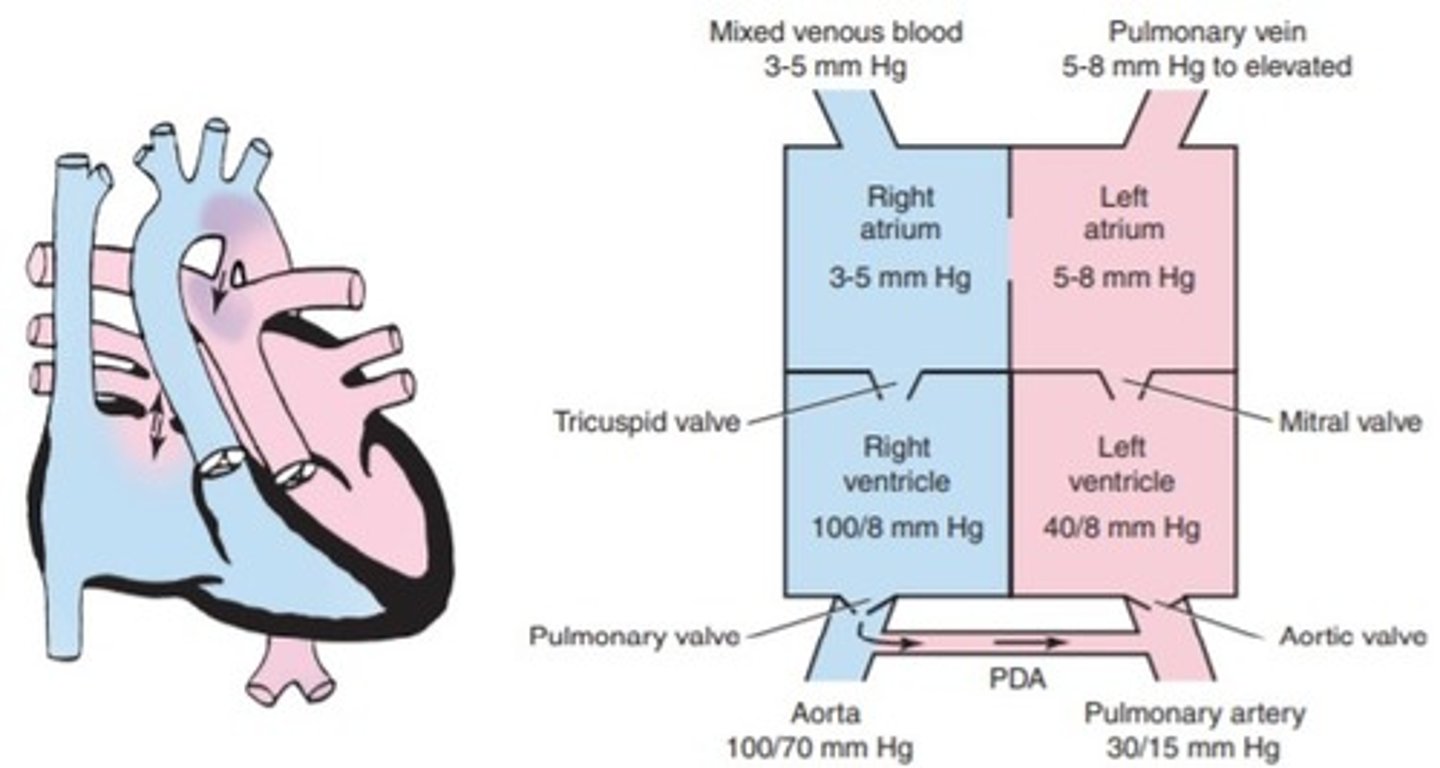
a. coarctation of the aorta
b. aortic stenosis
c. transposition of the great arteries
d. Total anomalous pulmonary venous return
c. transposition of the great arteries
Which of the following medications is the most common preoperative treatment to minimize preductal constriction until surgical correction of coarctation of the aorta can be achieved?
a. Indomethacin
b. Prostaglandin E1
c. Negative inotropes
d. Diuretics
b. Prostaglandin E1
Which of the following physiologic mechanisms need to be in place to ensure adequate systemic perfusion in infants with HLHS?
a. Presence of an ASD
b. Presence of a mitral regurgitation
c. Adequate left atrial function
d. Presence of a PDA
d. Presence of a PDA
Which of the following strategies can be used to increase PVR in infants with HLHS?
a. FiO2 < 0.21
b. Induce hypocapnia
c. Administer indomethacin
d. Close the PDA
a. FiO2 < 0.21
What should the therapist select as target gas exchange parameters after surgical intervention for infants with hypoplastic left ventricular syndrome HLHS?
a. pH < 7.35
b. PaO2 of 60 mm Hg and PaCO2 of 60 mm Hg
c. pH > 7.45
d. PaO2 of 40 mm Hg and PaCO2 of 40 mm Hg
d. PaO2 of 40 mm Hg and PaCO2 of 40 mm Hg
The therapist is treating a child with TOF who appears to be having a "tet" spell. What should the therapist suggest to treat this event?
I. Beta blockers
II. Knee-chest position to increase SVR
III. Morphine sulfate
IV. Oxygen
a. IV only
b. I and III only
c. I and IV only
d. I, II, III, and IV
d. I, II, III, and IV
Which of the following congenital cardiac anomalies is classified as conotruncal, associated with a "boot-shaped" appearance of the heart?
a. Tetralogy of Fallot
b. Transposition of the great vessels
c. Coarctation of the aorta
d. Atrioventricular canal defect
a. Tetralogy of Fallot
Which of the following statements describe truncus arteriosus?
I. It is a rare defect in which a single great artery arises from the ventricles of the heart
II. If PVR increases relative to systemic vascular resistance (SVR), more blood flows to the lungs through the truncus, decreasing systemic cardiac output.
III. Oxygen should be avoided in almost all circumstances in the preoperative setting
IV. Patients may undergo complete biventricular repair in the newborn period
I, III, IV
Which of the following blood flow patterns occurs in complete transposition of the great arteries?
a. The systemic venous blood passes through the right heart chambers.
b. The pulmonary venous blood traverses the left side of the heart and then returns to the systemic circulation.
c. When PVR increases relative to SVR, blood flow increases through the ductus arteriosus.
d. Systemic venous blood flows to the lungs after leaving the right ventricle.
a. The systemic venous blood passes through the right heart chambers.
The therapist is treating a child with a congenital heart defect who is unresponsive to oxygen therapy. Although the chest X-ray is relatively normal, the heart is described as "egg-shaped." Which of the following heart defects is more consistent with this description?
a. Complete transposition of the great arteries
b. Coarctation of the aorta
c. Truncus arteriosus
d. Tetralogy of Fallot
a. Complete transposition of the great arteries
The therapist is setting pulse oximetry to determine the presence of right-to-left shunt in an infant suspected of having a heart defect. Where should the therapist place the pulse ox probe to obtain the most accurate measure of preductal oxygen saturation?
a. Any finger of the right hand
b. Any finger of the left hand
c. Left earlobe
d. Lower extremities
a. Any finger of the right hand
A therapist monitoring an infant after a Blalock-Tausig shunt placement notices a significant drop in the end-tidal carbon dioxide (ETCO2) despite no changes in the infant's respiratory rate. How should the therapist interpret this change?
a. The infant has dramatically improved ventilation by breathing deeply.
b. The ETCO2 monitor is not accurate.
c. Loss of pulmonary blood flow through the shunt
d. Tricuspid regurgitation
c. Loss of pulmonary blood flow through the shunt
When using subambient oxygen therapy, what range of oxygen saturations should the therapist target?
a. >95% to 95%
b. 85% to 90%
c. 75% to 85%
d. 70% to 80%
c. 75% to 85%
Which of the following is a risk if PVR decreases in the first days of life in infants with HLHS?
a. Pulmonary edema
b. Induce hypocapnia
c. Development of a VSD
d. Development of an ASD
a. Pulmonary edema
A condition in which blood flow out of the right ventricle is obstructed because of atresia of the pulmonary valve is more consistent with which of the following defects?
a. Pulmonary atresia with intact ventricular septum
b. Coarctation of the aorta
c. Truncus arteriosus
d. Transposition of the great arteries
a. Pulmonary atresia with intact ventricular septum
In patients with HLHS, which of the following are consequences if premature closure of the PDA occurs?
a. Metabolic alkalosis
b. Respiratory alkalosis
c. Hypertension
d. Hypoperfusion
d. Hypoperfusion
Low signal strength on a plethysmogram may indicate which of the following?
a. Hyperperfusion
b. Increased stroke volume
c. Probe malposition
d. Decreased SVR
c. Probe malposition
The therapist is monitoring a patient in the CICU with a cardiac abnormality. They notice a narrowing pulse pressure. Which of the following could result?
I. A low stroke volume
II. Increased cardiac output
III. Poor ventricular function
IV. Impaired venous return
a. I, II. III, and IV
b. I, II, and III
c. I, III, and IV only
d. I and II only
c. I, III, and IV only
Which of the following is a correct statement regarding the path of blood as it travels through the heart?
a. During ventricular systole, blood is pumped from the RA into the right ventricle (RV) via the mitral valve (TV).
b. The coronary sinus drains venous blood supplying the heart muscle itself.
c. During ventricular diastole, blood passes through the tricuspid valve and into the left ventricle (LV).
d. During ventricular diastole, blood is ejected from the RV into the pulmonary arteries.
b. The coronary sinus drains venous blood supplying the heart muscle itself.