9. Hemodynamic Parameters Measurements
1/64
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
65 Terms
Strain gauge transducer mounted catheters limitations
time delays for the pressure wave to travel from the measurement site to the transducer is likely and can cause delays
noise
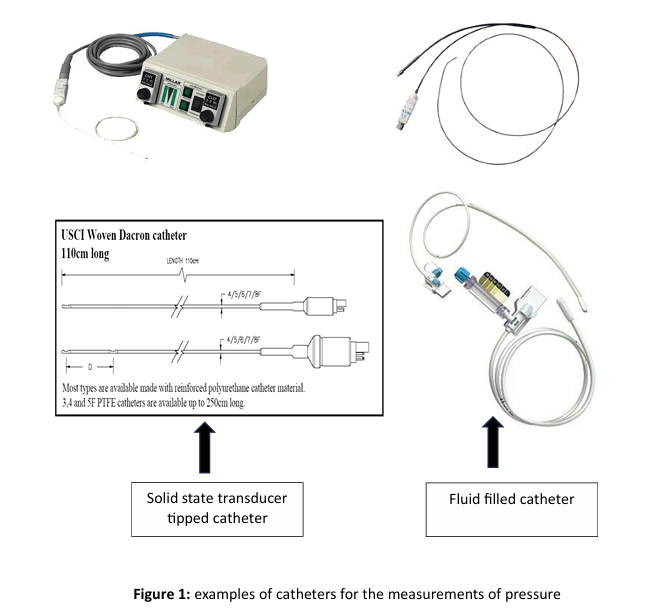
arterial tonometry
arterial tonometry measures the force that is needed to flatten a superficial artery. When this force is exerted with a piezo electric sensor, the recorded signal is representative for the arterial blood pressure contour. Theoretically, a tonometer yields correct absolute pressure values, but it is difficult to obtain steady long-term measurements in clinical practice
where are the most reliable tonometric measurements taken
radial artery as the vessel can be compressed against bone
(however provided the artery can be flattened, any superficial artery can be used, other sites are carotid, femoral, subclavian artery)
what is the tonometer used to measure
pressure wave morphology, and the signal is calibrated using blood pressure wave morphology, and the signal is calibrated using blood pressure values from a sphygmomanometer. As mean and diastolic blood pressure are almost identical throughout the arterial tree, the tonometric signal is best calibrated using these values
What can tonometers be designed as
fully automated devices and simpler systems in the form of a pen
What is an assumption can be made when using a tonometer
a measured sequence of raw tonometry data, and a pressure wave obtained after averaging and calibration of the raw data. One may assume a direct linear relation between theoretically the change in pressure inside the arterial lumen equals the change of force applied outside the artery (∆𝑃 = ∆𝐹)
What are the fundamental principles of tonometry
Placing a pressure sensor (tonometer) over a superficial artery
Pressing the sensor to partially flatten (applanate) the artery
at the point of applanation, the wall tension will not contribute, and the force applied to the sensor will equal the internal arterial pressure
the sensor will measure the changes in force caused by the blood pulse pressure extending the arterial wall. This is then converted into a continuous pressure waveform
Assumption while using a tonometer
The theoretical calculation assumes that the wall is elastic but the relationship between diameter and pressure is nonlinear. Also, the theory assumes a circular geometry. However, applying the force on the wall requires flatting part of the wall, changing the shape and the area
What is the effect of other layers when using a tonometer
The tonometer measures external wall force and not the true internal pressure alone. The true transmitted pressure is influenced by other layers, not just blood pressure
soft tissues
muscle compression
skin stiffness
All these layers are not taken into the theoretical consideration
Laplace’s Law Effect
During systole the radius increases and so does wall tension. This leads to the need for a larger force to flatten the artery. This amplifies the force change relative to pressure change. Also, wall tension absorbs some of the pressure change.
Wall tension equation
Wall tension is T=P x r
transfer function
using tonometry can also be used to estimate non-invasively, the central aortic pressure wave by measuring the arterial waveform
at a superficial artery close enough to the heart (subclavian, carotid artery) so that the effects of wave distortion may be neglected or
at a peripheral superficial artery (radial or carotid artery) and use a pressure transfer function (TF) to compute the pressure wave at the central aorta
How can central aortic pressure be reconstructed
from a peripheral artery pressure in the time or in the frequency domain (in the frequency domain, the peripheral pressure is decomposed in its Fourier harmonics)
What can the transfer function be used to calculate
The TF is used to calculate the harmonic at the central aorta, after which all harmonics are superimposed to yield the reconstructed wave
How in a time-domain relation is calculated in the time domain approach
time-domain relation is calculated between aortic pressure (Pao) at time t, and for instance radial artery pressure (Prad) at preceding points in time
Equation for time domain relation between aortic pressure
P𝑎𝑜(𝑡) = 𝑎1 𝑃𝑎𝑜(𝑡 −1) +⋯+𝑎𝑛 𝑃𝑎𝑜(𝑡−𝑛)+𝑏1 𝑃𝑟𝑎𝑑(𝑡−𝑘) +⋯𝑏𝑚 𝑃𝑟𝑎𝑑(𝑡 −𝑘 −𝑚+1)
Where k is the time delay between aortic and radial artery pressure while n and m are the number of a and b coefficients, which determine the order of the model (usually n and m are taken as = 10). This model type is overall superior to the frequency domain method

What does the transfer function describe
the relation between the pressure at 2 locations (e.g. the radial artery and the aorta).
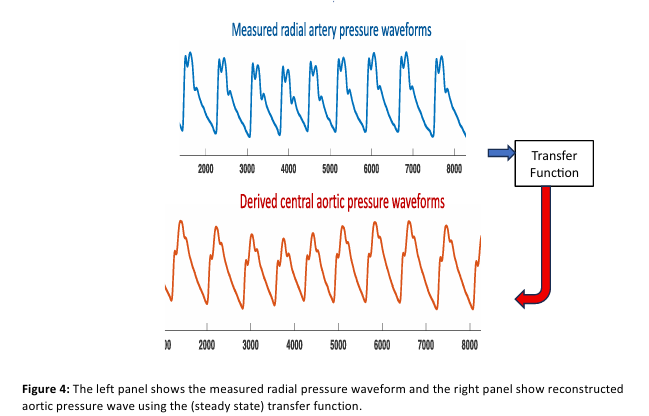
Can u describe this image
The transfer function method estimates central aortic pressure from radial artery pressure by decomposing the radial waveform into Fourier harmonics, modifying each harmonic according to the amplitude ratio and phase shift between the two sites, and reconstructing the aortic waveform.
Flow meter
The flow meter can measure the average velocity along the path of an emitted beam of ultrasound, by averaging the difference in measured transit time between the pulses of ultrasound propagating into and against the direction of the flow or by measuring the frequency shift from the Doppler effect.
What are ultrasonic flow meters affected by
acoustic properties of the fluid and can be impacted by temperature, density, viscosity and suspended particulates depending on the exact flow meter
measure for the average velocity of the fluid along the path of the ultrasonic beam
Ultrasonic flow meters measure the difference between the transit time of ultrasonic pulses propagating with (upstream, Tu) and against the flow direction (downstream, Td). This time difference is a measure for the average velocity of the fluid along the path of the ultrasonic beam. By using the absolute transit times, the average flow velocity, U, and the speed of sound, c, can be calculated, which require two other parameters are needed.
What is the derivation of the average velocity of the fluid along the path of the ultrasonic beam, speed of sounds
c=L/2 ((Tu-Td)/TuTd)

How is flow in the arterial system is measured
noninvasively mostly using ultrasound
How is blood flow velocity measured using
ultrasound echo-Doppler mode and movement (distance) of arterial or cardiac walls are measured using ultrasound M-Mode or B-mode
How can flow be measured
flow can be measured using magnetic resonant imaging (MRI) technology
What is flow the product of
Flow is the product of the aortic valve area and aortic flow velocity (assumed constant over the valve orifice) and both can be measured with ultrasound techniques (echo-Doppler). At present, ultrasound is still the cheapest and fastest technique. The aortic orifice can be imaged using 2D echo images from a parasternal long-axis view
how to measure velocity in the outflow tract
the doppler probe can be placed at the thorax, viewing the aortic valve from the cardiac apex, or at the suprasternal notch
where does measurement errors come from
Measurement errors arise from a poor estimation of aortic valve dimensions, or from the inclination of the Doppler beam with respect to the direction of flow. The error, made by assuming a flat velocity profile is expected to be small. The image was stored on-file as bitmap, and the aortic velocity manually traced in customize software. Multiplying an averaged velocity wave with (constant) valve area would yield the averaged flow rate
What yields the averaged flow rate
Multiplying an averaged velocity wave with (constant) valve area would yield the averaged flow rate.
what is an assumption you can make of air in lungs
Air can be considered as a perfect gas which for certain partial pressure values becomes liquid
The equation of state for both components in aeriform state
P =𝜌𝑅𝑇
where P, 𝜌 and R are partial pressure, density, and the constant R = 287.68 J/(kgK)), whereas T is the absolute mixture temperature (damp air). Water vapor quantity associated to one Kg of dry water is ~ 14.7 g in saturated air at 20 °C and 41.4 g in saturated air at 37 °C). Properties values of air flowing in the airways can be considered equal to that of dry air at the same temperature.
Properties values of air flowing in the airways can be considered equal to
that of dry air at the same temperature
What can air viscosity, air compressibility and max velocity be assumed to be
Neglecting temperature dependence, air viscosity can be considered constant, then humid air behaves as a Newtonian fluid. With regard to air compressibility, unless Mach number = (U/Us) is > 0.3, air can be considered as incompressible fluid whilst flowing in the lung. Maximum velocity in respiratory system is ~ 1 m/s and sound speed in air is ~ 350 m/s air in airways can be considered an incompressible fluid.
Is air compressible
No its incompressible
Neglecting temperature dependence, air viscosity can be considered constant, then humid air behaves as a Newtonian fluid. With regard to air compressibility, unless Mach number = (U/Us) is > 0.3, air can be considered as incompressible fluid whilst flowing in the lung. Maximum velocity in respiratory system is ~ 1 m/s and sound speed in air is ~ 350 m/s air in airways can be considered an incompressible fluid.
Functions of the respiratory system
The main functions of the respiratory system is to provides oxygen to the blood and eliminate carbon dioxide. Also, to forms speech sound (phonation). Other functions are to assist the body defends against microbes and Importantly traps and dissolves blood clots.
What do the lungs consist of
The lungs consist of tiny sacs called alveoli, which number ~150 million per lung and are the sites of gas exchange with the blood.
What do the lungs consist of
The lungs consist of tiny sacs called alveoli, which number ~150 million per lung and are the sites of gas exchange with the blood. The airways are all tubes through which air flows between the external environment and the alveoli.
Which side of the lung is larger
The two lungs although symmetrical in respect of their position to the spine, the right lung has 3 lopes where the left lung is slightly smaller with only 2 lopes, which has an implication to the distribution of air, gravitational effects and on particles and aerosol deposition
inspiration
Inspiration is the movement of air from the external environment through the airways into the alveoli during breathing. When inhaling, the diaphragm contracts and the lungs expand, pushing the chest upwards.
expiration
Expiration is the movement in the opposite direction. Air leaves the lungs to the external environment. When exhaling the diaphragm relaxes and the lungs contract, moving the chest back down.
what is the respiratory cycle
The respiratory cycle constitutes of one inspiration and one expiration.
can u write the table for The effect of breathing on the various parameters associated with inspiration and expiration in every breathing cycle.
see image
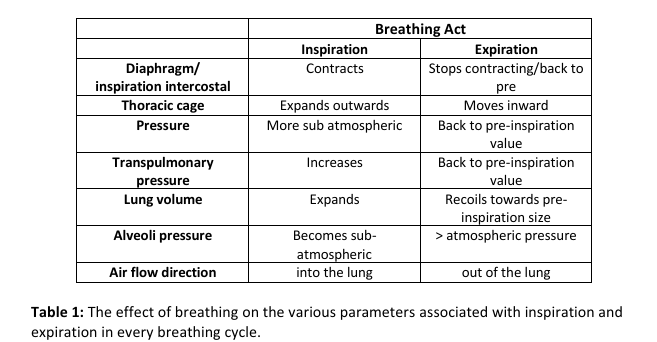
ventilation
the exchange of air between the atmosphere and alveoli
bulk flow equation
Q=PAtm-Palv/R=Δ𝑃/R
Where Q is the flow of air into lungs, and is proportional to the pressure difference (∆𝑃) between the atmospheric (Patm) and alveoli pressures (Palv). ∆𝑃 is inversely proportional to the resistance ( R ).

What are the two major determinants of lung compliance
stretchability of lung tissue
surface tension in the alveoli
what is the lung compliance at any instance is proportional to
The lung compliance at any instance is proportional to the trans-pulmonary pressure, that is, the difference between the alveolar pressure (Palv) and the intra pleural pressure (Pip).
Lung compliance
How much a given transpulmonary pressure expands the lung depends on the
lung compliance equation
L𝐶𝑠 = ∆𝑉𝐿 /∆ (𝑃𝑎𝑙𝑣 −𝑃𝑖𝑝)
𝑤ℎ𝑒𝑟𝑒 ∆𝑉𝐿 𝑖𝑠 𝑡ℎ𝑒 𝑙𝑢𝑚𝑔 𝑣𝑜𝑙𝑢𝑚𝑒 𝑑𝑖𝑓𝑓𝑒𝑟𝑒𝑛𝑐𝑒 𝑏𝑒𝑡𝑤𝑒𝑒𝑛 𝑖𝑛𝑠𝑝𝑖𝑟𝑎𝑡𝑖𝑜𝑛 𝑎𝑛𝑑 𝑒𝑥𝑝𝑖𝑟𝑎𝑡𝑖𝑜𝑛
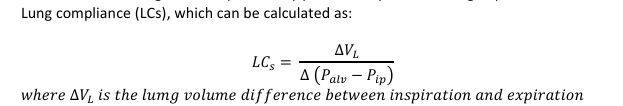
Alveolar ventilation
Alveolar ventilation (Va, mL) is a function of the tidal volume (Tv, mL), the dead space (ds, mL) and the frequency of breathing (Bf, breaths/min)
Alveolar ventilation equation
V𝑎 =(𝑇𝑣−𝑑𝑠)(𝑓)
Dead space
Dead space (ds) is defined as the volume of air that does not participate in the process of gas-exchange in the lung. The total dead space is composed of two main elements of anatomic dead space and alveolar dead space
anatomic dead space
Anatomic dead space: which is the space of the respiratory system that holds volume of air that does not contribute to gas-exchange (being outside the lungs) such as the volume of air in the nasal cavity, bronchi, trachea or larynx.
alveolar dead space
Alveolar dead space: which is the space that does not participate in gas exchange because there is no blood flow to that part of the lung, which increases significantly in lung diseases where blood flow to the alveoli is blocked or reduced
total physiological dead space equation
Anatomic dead space + Alveolar dead space = Total physiological dead space
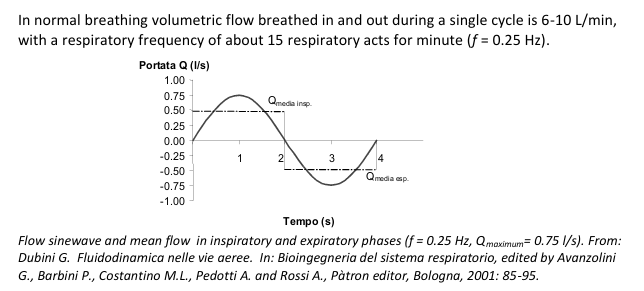
what is the normal volumetric flow and respiratory frequency
In normal breathing volumetric flow breathed in and out during a single cycle is 6-10 L/min, with a respiratory frequency of about 15 respiratory acts for minute (f = 0.25 Hz)
Turbulent Flow
Air flow characterized by disorganized movement of gas molecules and/or eddy formation; it occurs when velocity of flow exceeds a limiting value (judged by Reynolds number in the region of 2200) or when irregularities in the configuration of the tube preclude laminar flow.
Laminar Flow
Air flow in the lungs which is streamlined, low velocity, and obeys Poiseuille's Law; generally it is confined to the small peripheral airways.
Laminar Flow Equation
Q=Δp (𝜋𝑅^4 / 8uL)
Stokes flow
In this type of flow, the inertial forces are assumed to be negligible, and the Navier-Stokes equations simplify to give the Stokes equations; the Stokes flow assumption usually applies to the flow in the alveoli
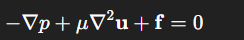
implications of dimensions in flow
The length of straight portion of the pipe between two consecutive bifurcation (mother tube) is short, so in airways, flows are never completely developed. Therefore, dissipation energy is always larger than energy that corresponds to a fully developed laminar flow i.e. a Poiseuille f low. Another consequence is that the relationship between drop pressure and mass flow rate in bifurcation is not linear.
Womersley number
a dimensionless parameter that describes the importance of inertial forces, due to the unsteady state of the flow (oscillatory in the case of breathing) with respect to the viscous one.
Womersley number equation
Wo=D/2 sqrt(w/v)=D/2 sqrt(2pi f p /u)
where D is the internal diameter, 𝜔 is the respiratory cycle pulsation, f is the respiratory frequency, whereas 𝜈,𝜇 are kinematic viscosity, dynamic viscosity and fluid volumetric mass respectively.
In oscillatory motions, transition between laminar and turbulent regimes is greatly affected by cyclical inversion of velocity profiles so what is considered
Therefore, two Reynolds numbers are considered, one corresponds to the mean and the other to the maximum flow rate:
Re-mean=pUmeanD/u=4Qmean/pi u D
Re-max = pUmaxD/u = 4Qmean / pi u D
where Umean and Upeak velocities are expressed in terms of volumetric flows Qmean and Qmax
For a pipe with circular section what following relation is valid
U=4Q/pi D²

What is one of the main functions of the upper airways
Finally, one of the main functions of the upper airways is warm and humidify inspired air which arrives at the first bifurcation after the windpipe at 37 °C and it has a relative humidity of 𝜙 =100%. Air has the same properties in pulmonary alveolus. For this reason, human beings can survive in artic as well as tropical climates and it can adapt rapidly to different climate without respiratory system damages. This condition takes place in the nasal cavity and the pharynx where heat and vapour exchange take place.