CS II 2.3: Fecal Analysis
1/23
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
24 Terms
What are some of the natural protective mechanisms of the GI tract against infection?
Increased acidity of the stomach
rapid transit time of the small bowel
ileocecal valve inhibits bacteria from the large intestine from moving backwards
normal flora (inhibit growth of new bacteria)
What are some osmotic causes of diarrhea? Does fasting improve sxs?
Lactose intolerance, increased sorbitol; yes - diarrhea volume will decrease if you stop consuming the items
What are some secretory causes of diarrhea? Does fasting improve sxs?
Endocrine disorders, Zollinger-Ellison syndrome, laxatives, bile salt malabsorption; no - diarrhea volume will not decrease if you stop consuming the items
What are some fast & slow motility disorder causes of diarrhea, respectively?
Fast: reduced contact (hyperthyroid, s/p gastrectomy, IBS)
Slow: bacterial overgrowth (hypothyroid, DM, scleroderma)
What are is the difference between the appearance/contents of inflammatory vs. noninflammatory diarrhea?
Inflammatory: outpouring of necrotic tissue, colloid, fluid, electrolytes, & blood
Noninflammatory: excessive secretion of electrolyte w/o blood or pus
How should stool samples be collected?
In a bed pan/hat & then transferred to sterile containers (cannot contain urine, toilet paper, or toilet water)
What is the difference between malabsorption and maldigestion?
Malabsorption: reduced absorptive capability & fast transit time (patient often has steatorrhea due to ↓ fat absorption)
Maldigestion: food cannot be digested usually due to secondary obstruction in the pancreatobiliary tree or small bowel (tumor, gallstones, etc.)
Overall, what is fecal fat testing used for?
Evaluate patients w/ steatorrhea by measuring fecal fat content over 3 days
What are some things that can cause increased & decreased fecal fat levels, respectively?
Increased: CF, malabsorption (Celiac, Crohn's, etc.), maldigestion (obstruction of some kind), short gut syndrome, enema use, laxative use (mineral oil)
Decreased: recent barium administration, fiber laxatives/supplements
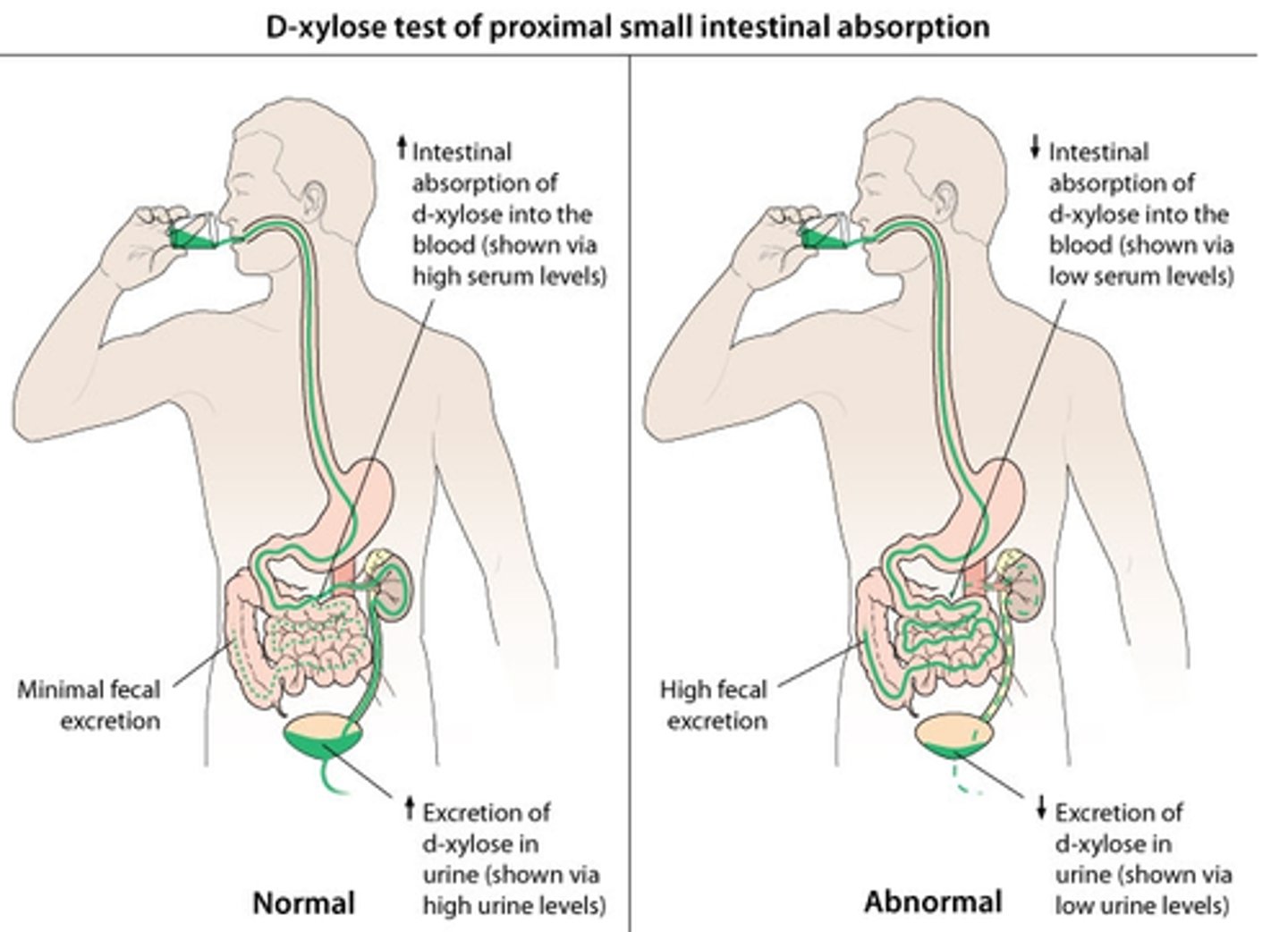
What does D-xylose absorption measure, & what is it useful for?
Evaluates the absorptive capability of the intestines - can d/dx malabsorption from maldigestion (D-xylose absorption diminished in malabsorption)
How are D-xylose levels measured?
Baseline serum & urine amounts are taken; serum levels collected again at 1 hr (peds) or 2 hrs (adults) while urine levels are collected again at 5 hrs
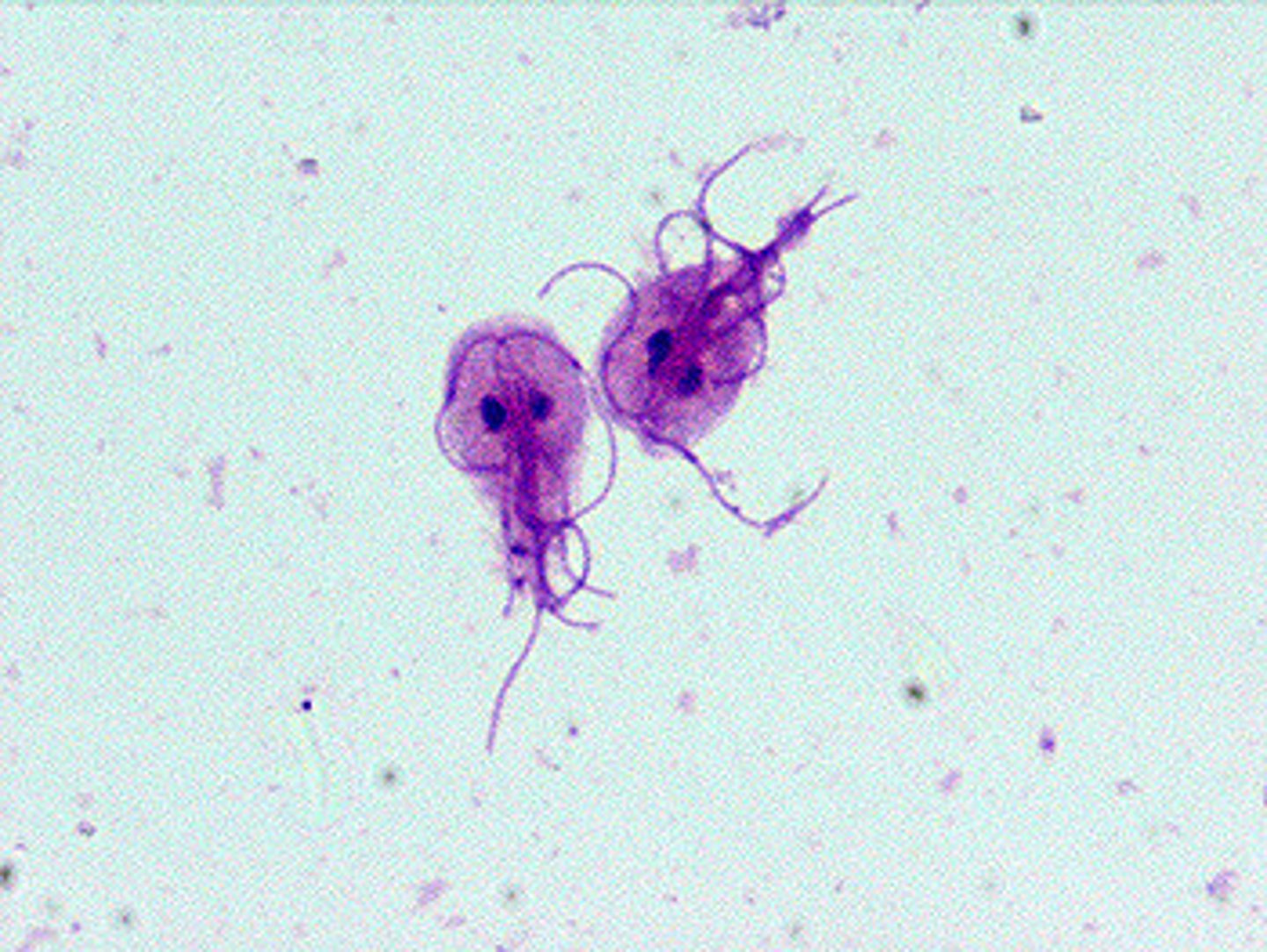
How many samples are required for a stool ova & parasite? What kinds of organisms can this test help ID?
Minimum of 3 over the course of ten days (every other day); worms & parasites
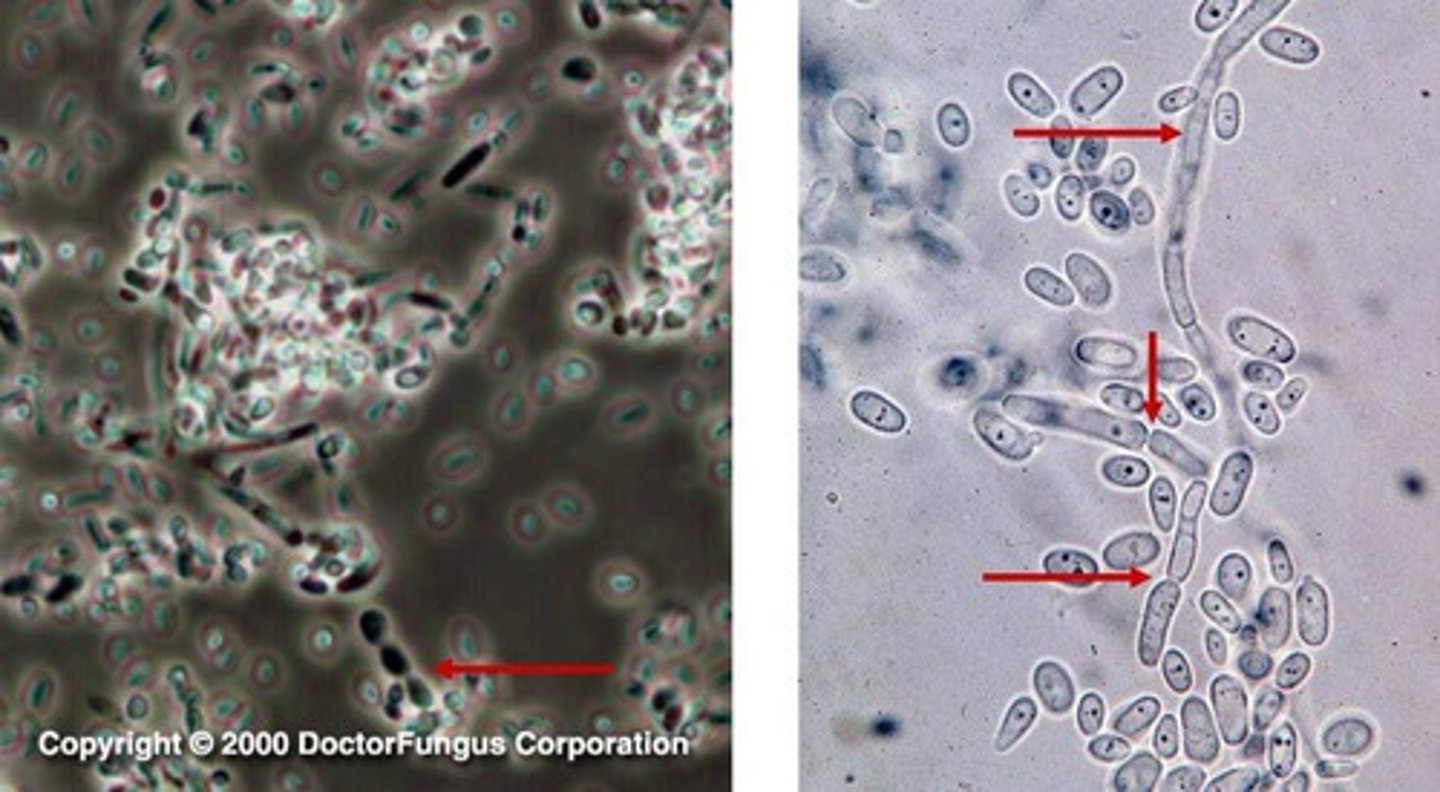
What kinds of organisms can a stool culture help ID? What else does this test do?
Common bacterial etiologies; isolation of the microbe for ID & antibiotic sensitivity
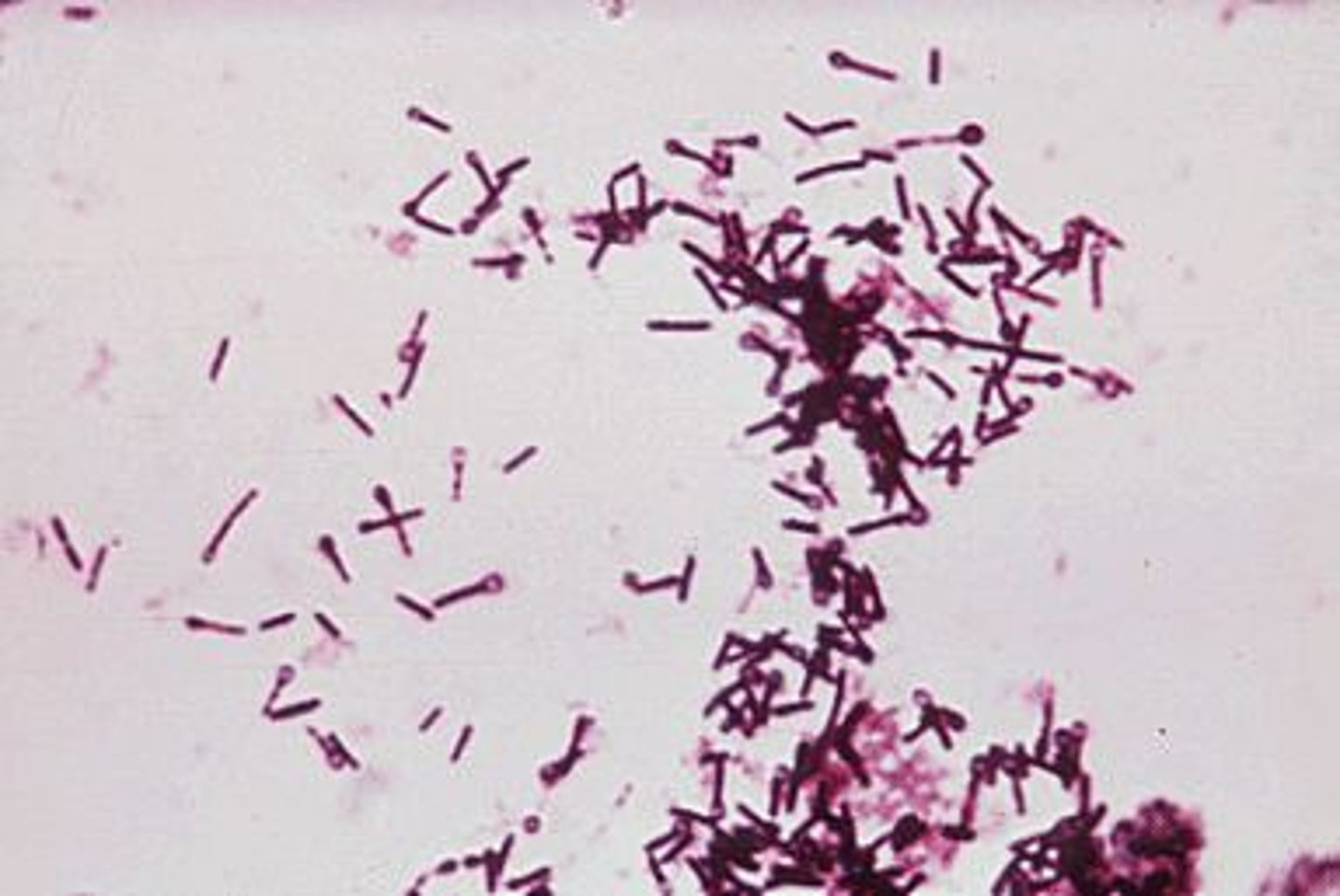
What is the gold-standard test for identifying C. difficile infection? What is an alternative we can do?
Gold-standard = toxigenic stool culture; alternative = stool EIA for toxin A & B (rapid but less sensitive)
What is the gold-standard test for identifying Salmonella?
Stool culture
What is the gold-standard test for identifying Shigella?
Stool culture
What is the significance of enterohemorrhagic E. coli?
This subtype produces a toxin called "Shiga toxin" that can cause bloody diarrhea & hemolytic uremic syndrome - this can be fatal
How are all subtypes of E. coli (enterohemorrhagic, enteropathogenic, & enterotoxigenic) diagnosed? What is something that can be specifically done to diagnose the enterohemorrhagic type?
Stool culture; Shiga toxin EIA
How is norovirus usually diagnosed?
Usually clinical (since sxs often self-resolve within a day), but if a test is needed PCR is used the most
How is rotavirus usually diagnosed?
Rapid antigen testing is most common
How is Giardia diagnosed?
Ova & parasite evaluation
How is Enterobius (pinworm) usually diagnosed?
Ova & parasite is the best test, but the tape test can also be done & usually works pretty well

Who does Cryptosporidium usually affect? How is this usually diagnosed?
Immunocompromised patients; ova & parasite w/ special stain (need to specifically indicate you are testing for crypto)
What is a great first-line test to diagnose Celiac disease? What is the gold-standard test that we need to follow this up with?
Serology in the form of an anti-tissue transglutaminase (anti-tTG) panel; small bowel biopsy = gold-standard