2. Lecture 2 - Anesthesia Exam 2: Lec 7 - Maxillary Anestheisa Part 2
1/83
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
84 Terms
palatal injections
What type of injection can be the most painful for a patient to experience?
-Use pressure anesthesia at the injection site before and during needle insertion
-Deposit the anesthetic solution slowly
What are 2 ways to reduce the amount of pain experienced by patients during a palatal injection?
Nasopalatine n.
this nerve travels across the roof of the nasal cavity, enters the incisive canal
-Provides sensory to the palatal mucosa in the pre-maxilla (canine - incisorscanines)
Greater Palatine n.
this nerve provides sensory fibers to the posterior 2/3 hard palate:
Lesser Palatine n.
this nerve provides sensory to the soft palate, tonsils, uvula:
Palatal hard and soft tissue anesthesia for > 2 teeth
What are the indications for a Greater Palatine Nerve Block?
-Infection/inflammation at injection site
-Smaller area of therapy (1 or 2 teeth)
What are some contraindications for a Greater Palatine Nerve Block?
Greater Palatine Nerve Block
ID the anesthesia technique:
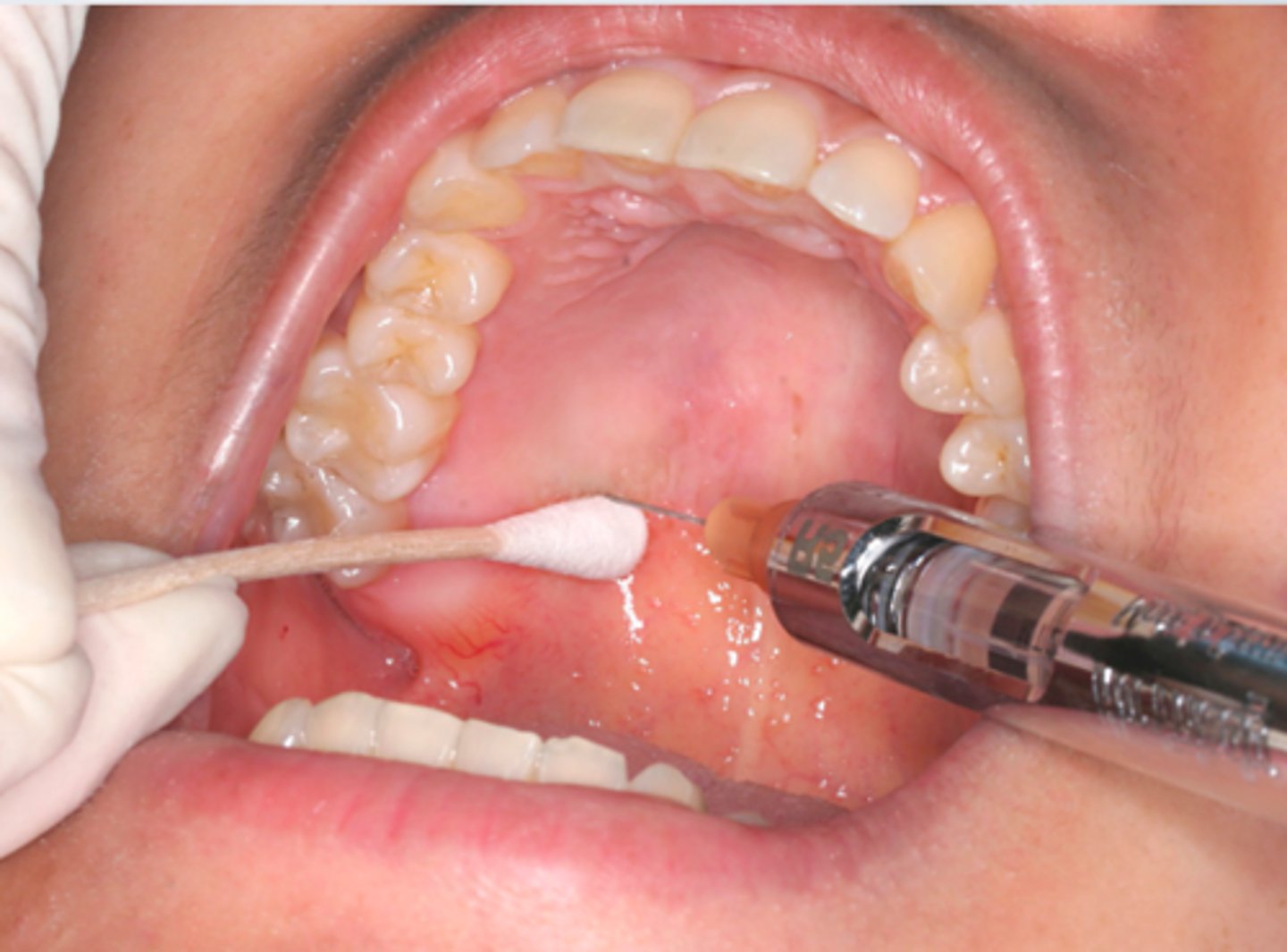
11 o'clock
what is the operators position for a Greater Palatine Nerve Block:
- 7 o'clock
- 8 o'clock
- 9 o'clock
- 9 or 10 o'clock
- 10 o'clock
- 10 or 11 o'clock
- 11 o'clock
27 short gauge
what size needle should you use for a Greater Palatine Nerve Block?
Greater Palatine n.
what is the needle target for a Greater Palatine Nerve Block?
Several mm anterior to the greater palatine foramen at the junction of the alveolar process and the lateral plate of the hard palate
what is the insertion point for a Greater Palatine Nerve Block?
Bevel towards bone. Laterally and superiorly through the mucosa until bone is gently contacted
what is the insertion path for a Greater Palatine Nerve Block?
4 - 6 mm
what is the depth for a Greater Palatine Nerve Block?
0.25 to 0.5 ml
what is the anesthetic volume for a Greater Palatine Nerve Block?
Greater Palatine Nerve Block
This type of nerve block will result in the anesthesia of the palatal gingiva of the molars and premolars and mucoperiosteum of the posterior two thirds of the ipsilateral hard palate to the mid-line:
Palatal hard and soft tissue anesthesia for > 2 teeth
What are the indications for a Nasopalatine Nerve Block?
-Infection/inflammation at injection site
-Smaller area of therapy (1 or 2 teeth)
What are some contraindications for a Nasopalatine Nerve Block?
Nasopalatine Nerve Block (single injection)
ID the anesthesia technique:
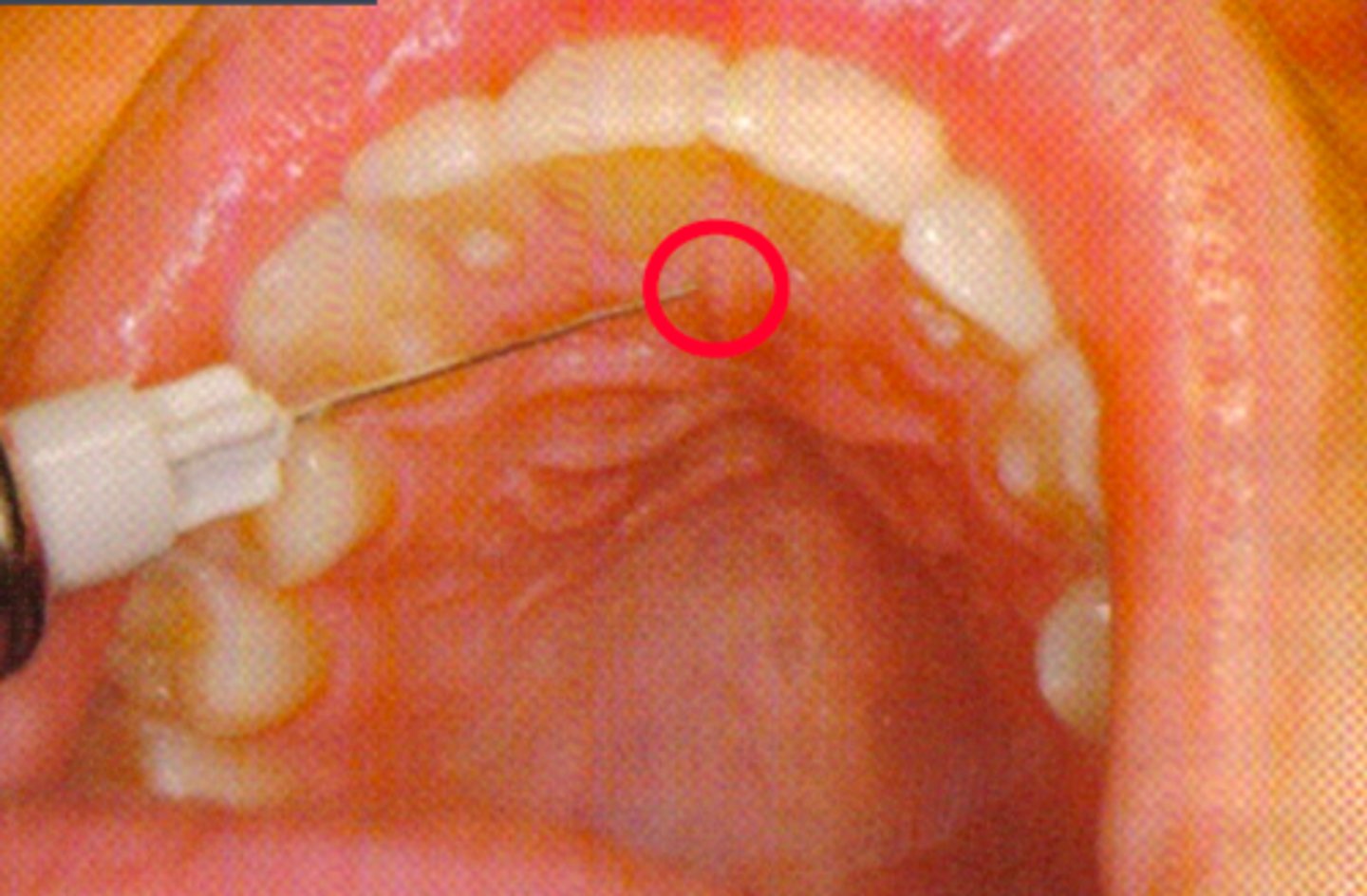
Nasopalatine Nerve Block (multiple injections)
ID the anesthesia technique:
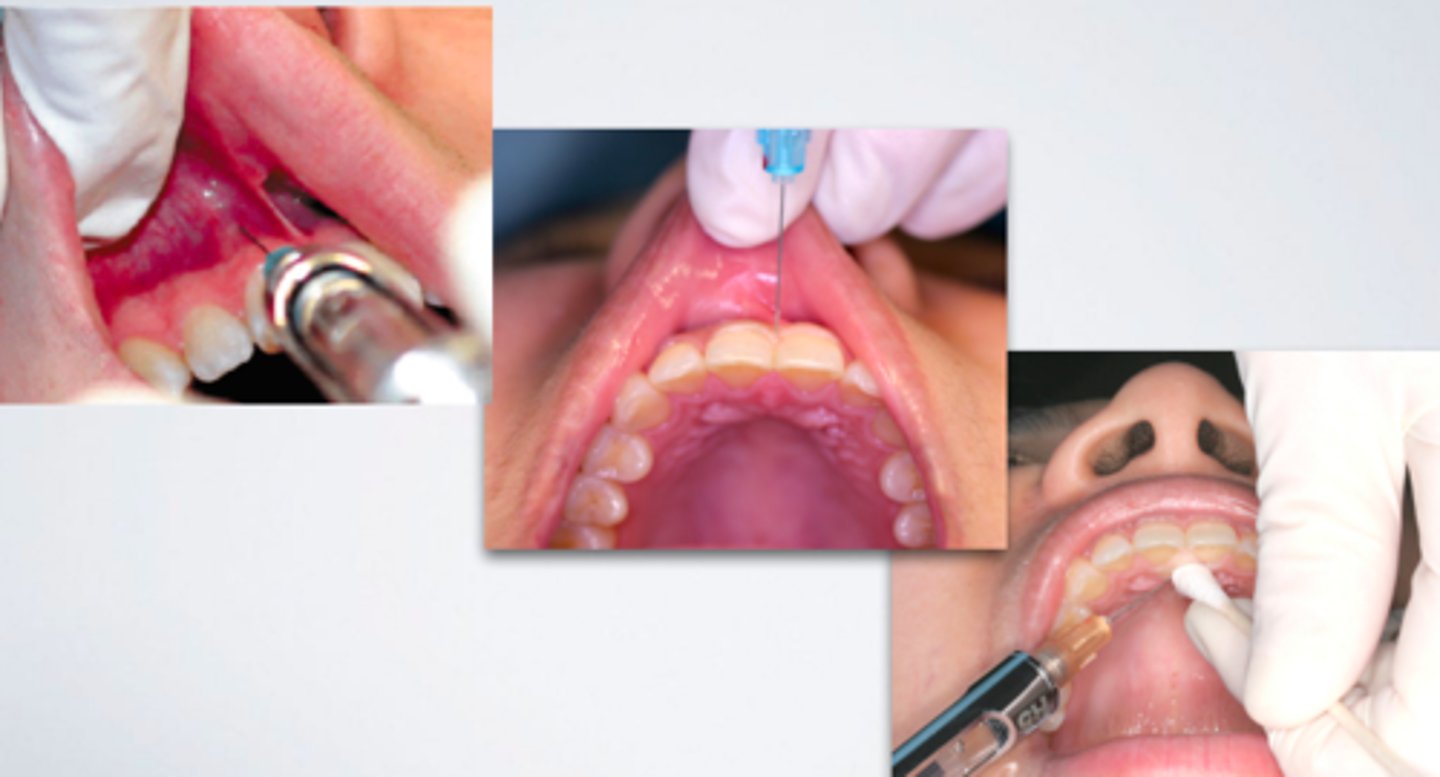
9 or 10 o'clock
what is the operators position for a Nasopalatine Nerve Block:
- 7 o'clock
- 8 o'clock
- 9 o'clock
- 9 or 10 o'clock
- 10 o'clock
- 10 or 11 o'clock
- 11 o'clock
27 short gauge
what size needle should you use for a Nasopalatine Nerve Block?
Incisive foramen on the anterior palate
what is the needle target for a Nasopalatine Nerve Block?
Palatal mucosa to the lateral border of the incisive papilla
what is the insertion point for a Nasopalatine Nerve Block (single injection technique)?
1st injection: labial frenum
2nd injection: interdental papilla between central incisors
3rd injection: incisive papilla (nasopalatine nerve block)
what is the insertion point for a Nasopalatine Nerve Block (multiple injection technique)?
Approach the injection site at a 45 degree angle toward the incisive papilla
what is the insertion path for a Nasopalatine Nerve Block?
3 to 5 mm
what is the depth for a Nasopalatine Nerve Block?
0.2 to 0.3 ml
what is the anesthetic volume for a Nasoalatine Nerve Block?
Nasopalatine Nerve Block (general)
This type of nerve block will result in the anesthesia of the palatal gingiva of the six anterior teeth and mucoperiosteum of the anterior third of the hard palate:
Palatogingival pain control for limited area (1-2 teeth) Achieving hemostasis during surgical procedure
What are the indications for a Palatal local infiltration?
-Infection/inflammation at injection site
-Smaller area of therapy (1 or 2 teeth)
What are some contraindications for a Palatal local infiltration?
Palatal Local Infiltration
ID the anesthesia technique:
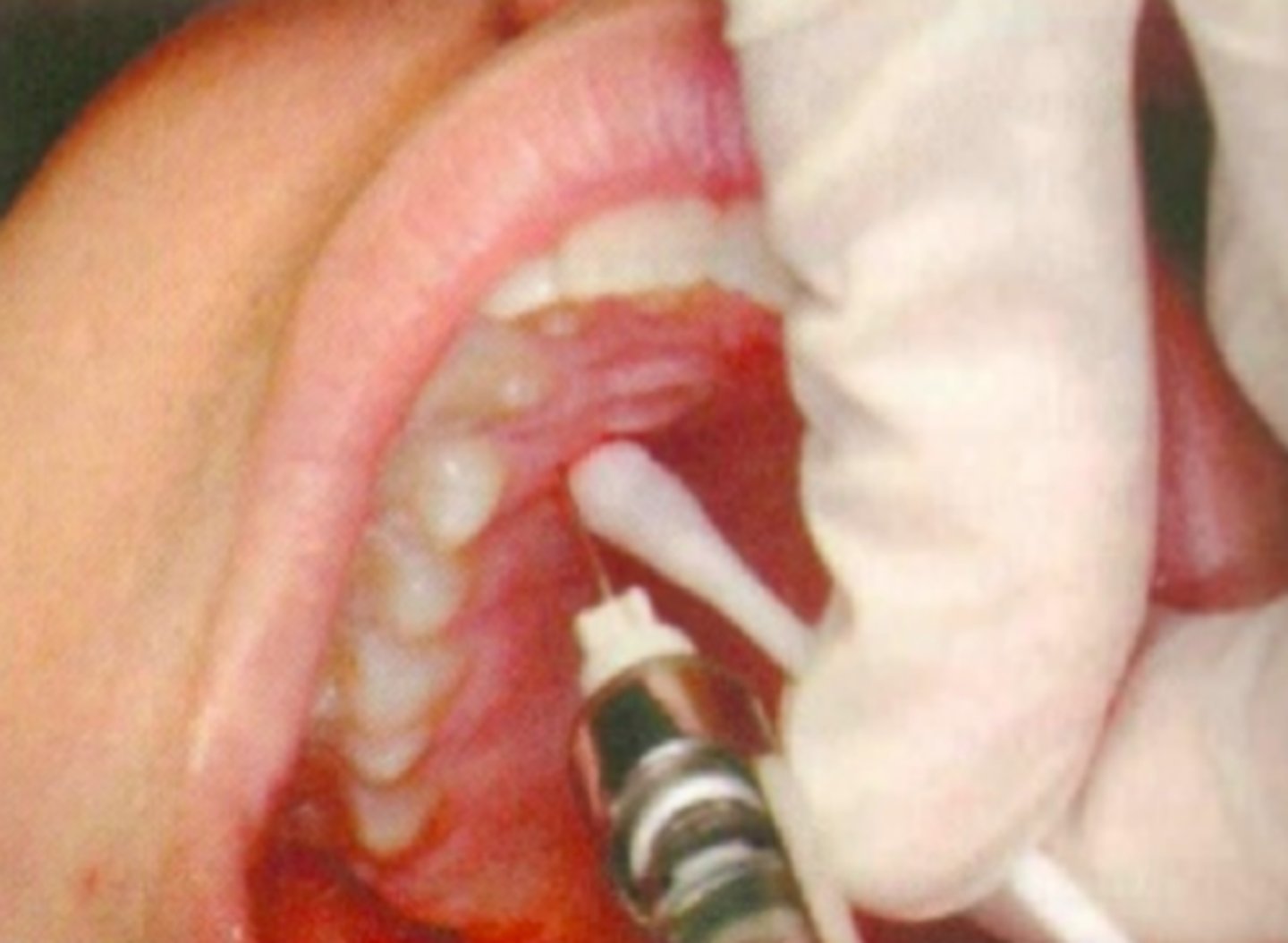
10 or 11 o'clock
what is the operators position for a Palatal Local Infiltration:
- 7 o'clock
- 8 o'clock
- 9 o'clock
- 9 or 10 o'clock
- 10 o'clock
- 10 or 11 o'clock
- 11 o'clock
27 short gauge
what size needle should you use for a Palatal Local Infiltration?
Palatal gingival tissue 5-10 mm from the free gingival margin
what is the needle target for a Palatal Local Infiltration?
Attached gingiva 5-10 mm from the free gingival margin
what is the insertion point for a Palatal Local Infiltration?
Approaching the injection site at 45 degree angle
what is the insertion path for a Palatal Local Infiltration?
3 to 5 mm
what is the insertion depth for a Palatal Local Infiltration?
0.2 to 0.3 ml
what is the anesthetic volume for a Palatal Local Infiltration?
Palatal Local Infiltration
This type of nerve block will result in the anesthesia of the palatal soft tissue in the immediate adjacent area of injection?
-Extensive oral surgical, periodontal, or restorative procedures requiring anesthesia of the entire maxillary division
-When tissue inflammation/infection precludes the use of other regional nerve blocks/supraperiosteal injections
-Diagnostic/therapeutic for neuralgias/tics of 2nd division of trigeminal nerve
What are the indications for a Maxillary Nerve Block?
-Pediatric patients
-Uncooperative patients
-Hemorrhage risk (hemophiliac)
-Inflammation or infection of tissue overlying the injection site
What are some contraindications for a Maxillary Nerve Block?
Maxillary Nerve Block (general)
this type of injection has the highest risk of hematoma of all maxillary LA injections:
-maxillary a.
-posteror superior alveolar a.
what two arteries are at high risk of hematoma when performing a Maxillary Nerve Block?
High Tuberosity Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has the advantage of being easier to perform:
High Tuberosity Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has the advantage of an atraumatic injection:
High Tuberosity Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has the advantage of being the least likely to cause discomfort:
High Tuberosity Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has the advantage of minimizing the number of needle penetration needed for successful anesthesia of the heme-maxilla:
High Tuberosity Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has a disadvantage of being more likely to cause clinically significant hematoma:
Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has the advantage of being less likely to cause hematoma:
Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has the advantage of ensuring accurate placement of the needle:
Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has a disadvantage of requiring separate palatal infiltration to minimize discomfort:
Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has a disadvantage because in 5-15% of population, bony obstruction may be present in the canal, which can prevent passage of the needle:
Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block)
this Maxillary Nerve Block technique has a disadvantage because over-insertion of the needle may result in anesthetizing nerve innervations to the orbit (very rare):
High Tuberosity Approach (for maxillary nerve block)
ID the anesthesia technique:
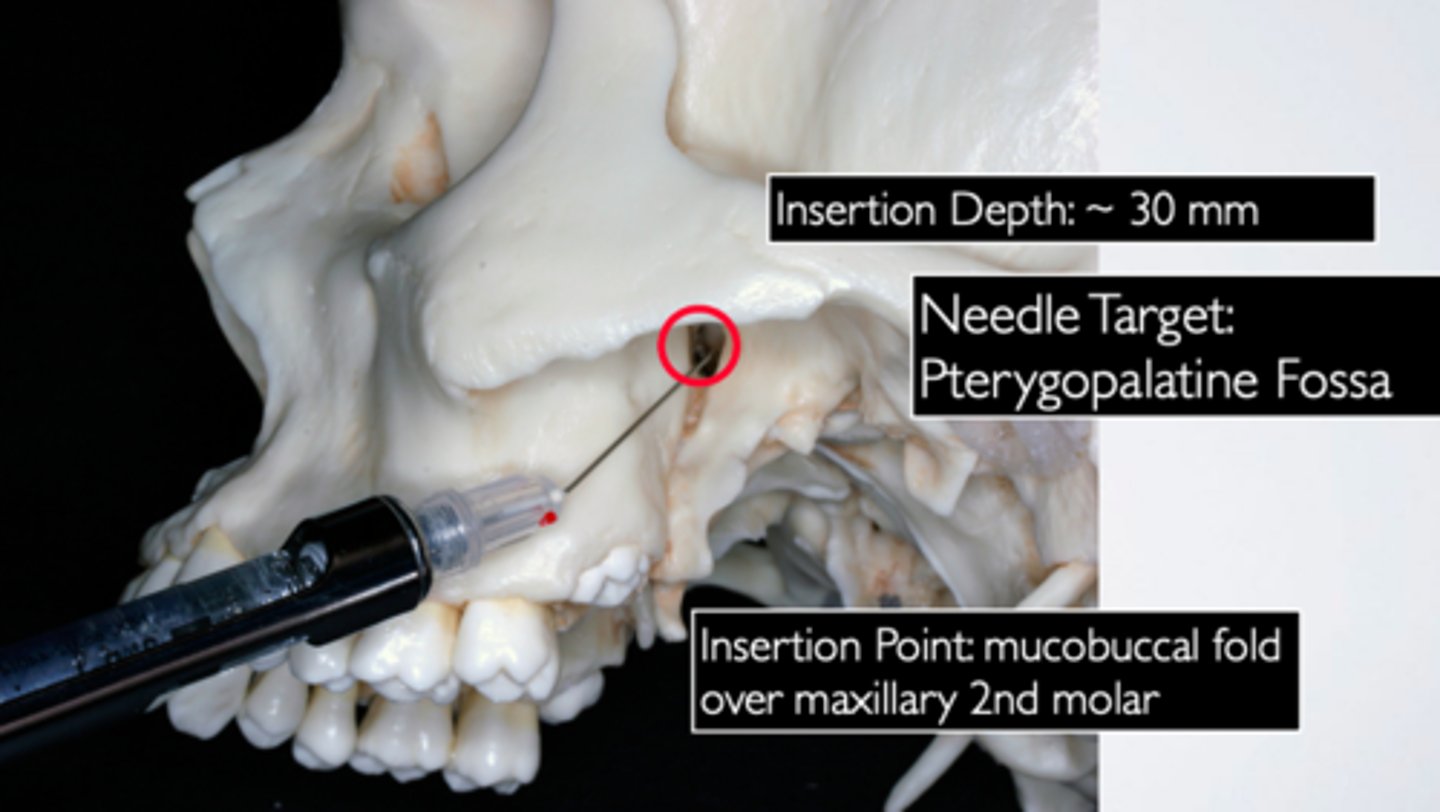
Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block)
ID the anesthesia technique:
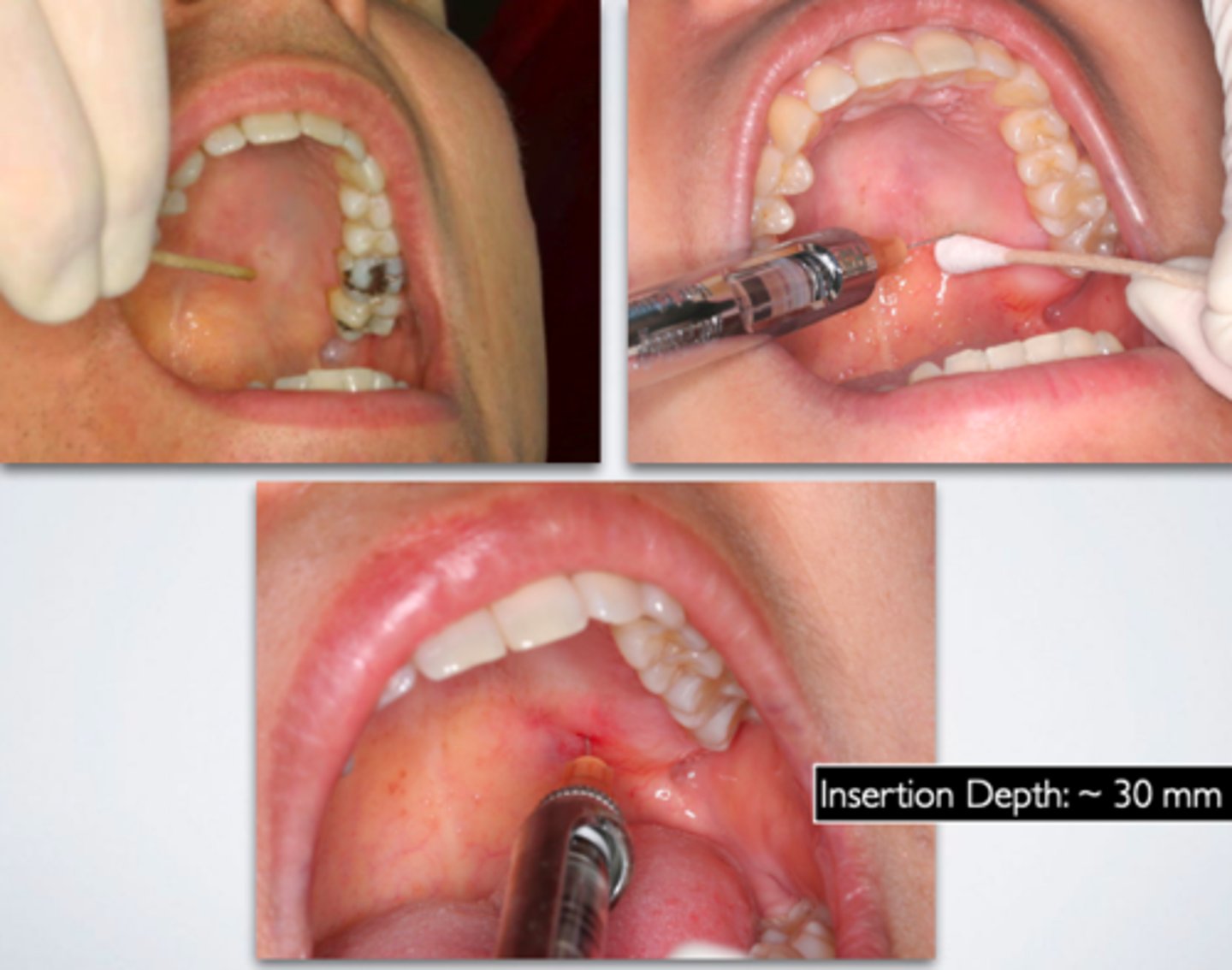
11 o'clock
what is the operators position for a High Tuberosity Approach (for maxillary nerve block):
- 7 o'clock
- 8 o'clock
- 9 o'clock
- 9 or 10 o'clock
- 10 o'clock
- 10 or 11 o'clock
- 11 o'clock
8 o'clock
what is the operators position for a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block) (for maxillary nerve block):
- 7 o'clock
- 8 o'clock
- 9 o'clock
- 9 or 10 o'clock
- 10 o'clock
- 10 or 11 o'clock
- 11 o'clock
25 gauge long with bevel facing down, may be bent once to 30 degrees at the hub
what size needle should you use for a High Tuberosity Approach (for maxillary nerve block):
27 gauge long with bevel facing down, may be bent once to 30 degrees at the hub
what size needle should you use for a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block) (for maxillary nerve block):
Pterygopalatine fossa 10 to 15 mm lateral and inferior to the maxillary nerve
what is the needle target for a High Tuberosity Approach (for maxillary nerve block):
Pterygopalatine fossa 10 mm below the maxillary nerve
what is the needle target for a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block):
Height of maxillary vestibule just posterior to zygomatic process, normally adjacent or slightly posterior to the DB root of maxillary second molar
what is the insertion point for a High Tuberosity Approach (for maxillary nerve block):
Greater palatine foramen
what is the insertion point for a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block):
Upward, backward, and inward through the mucosa, buccinator m, and pterygopalatine fossa
what is the insertion path for a High Tuberosity Approach (for maxillary nerve block):
Gently through the mucosa and greater palatine foramen and advanced up the canal in superior and posterior direction
what is the insertion path for a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block):
30 mm
what is the insertion depth for a High Tuberosity Approach (for maxillary nerve block):
30 mm
what is the insertion depth for a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block):
1.8 ml
what is the anesthetic volume for a High Tuberosity Approach (for maxillary nerve block):
1.8 ml
what is the anesthetic volume for a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block):
Maxillary Nerve Block (general)
This type of nerve block will result in the anesthesia of the Entire hemimaxilla (may be incomplete at midlline):
nasal cavity
during a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block), if the needle penetrates the medial wall, LA could be deposited into the _______
nasal cavity
during a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block), you aspirate and air fills the syringe. The needle is now in the _____
blockage of orbital contents
during a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block), if the needle is advanced too high in the pterygopalatine fossa, what could happen?
CN VI (abducens)
during a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block), if diplopia (double vision) occurs, what CN has been blocked?
diplopia (double vision)
What clinical sign would you observe if CN VI (abducens) was anesthetized?
CN III (oculomotor)
during a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block), if mydriasis in one eye occurs, what CN has been blocked?
mydriasis
What clinical sign would you observe if CN III (oculomotor) was anesthetized?
CN III, CN IV, CN VI
during a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block), if a Retrobulbar block occurs resulting in Mydriasis, Corneal anesthesia, Ophthalmoplegia , what CN has been blocked?
Mydriasis, Corneal anesthesia, Ophthalmoplegia
What clinical sign would you observe if CN III, IV, VI (Retrobulbar Block) were anesthetized?
CN II (optic)
during a Pterygopalatine/Greater Palatine Canal Approach (for maxillary nerve block), if loss or blurry vision occurs, what CN has been blocked?
transient loss of vision, blurry vision
What clinical sign would you observe if CN II (optic) was anesthetized?
CN II (optic)
Which CN provides the special sense of vision?
CN III, CN IV, CN VI
Which CNs provide motor innervation?