Pedi/OB Exam 3 Blueprint Part 1: Pedi
1/95
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
96 Terms
what is osteogenesis imperfecta?
an inherited connective tissue condition that results in bone fractures and deformity along with restricted growth
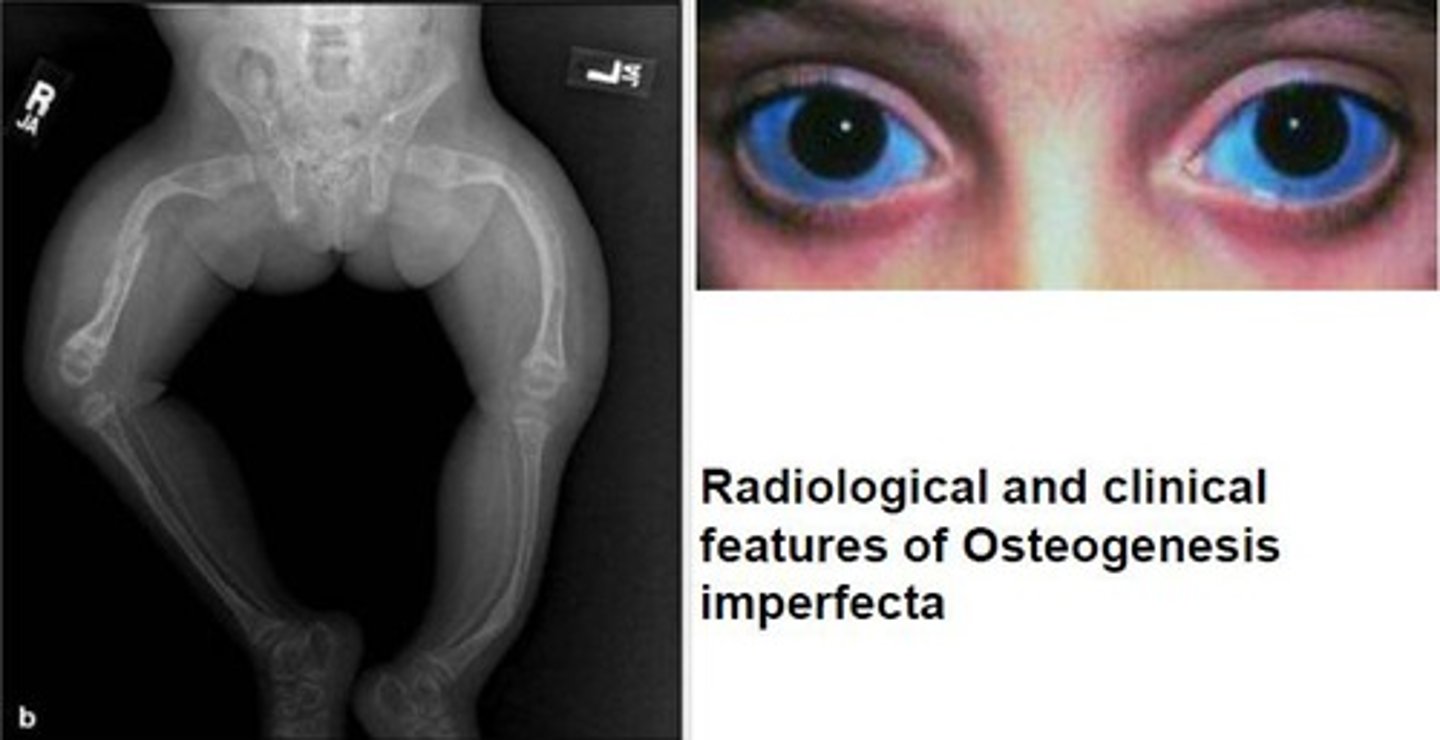
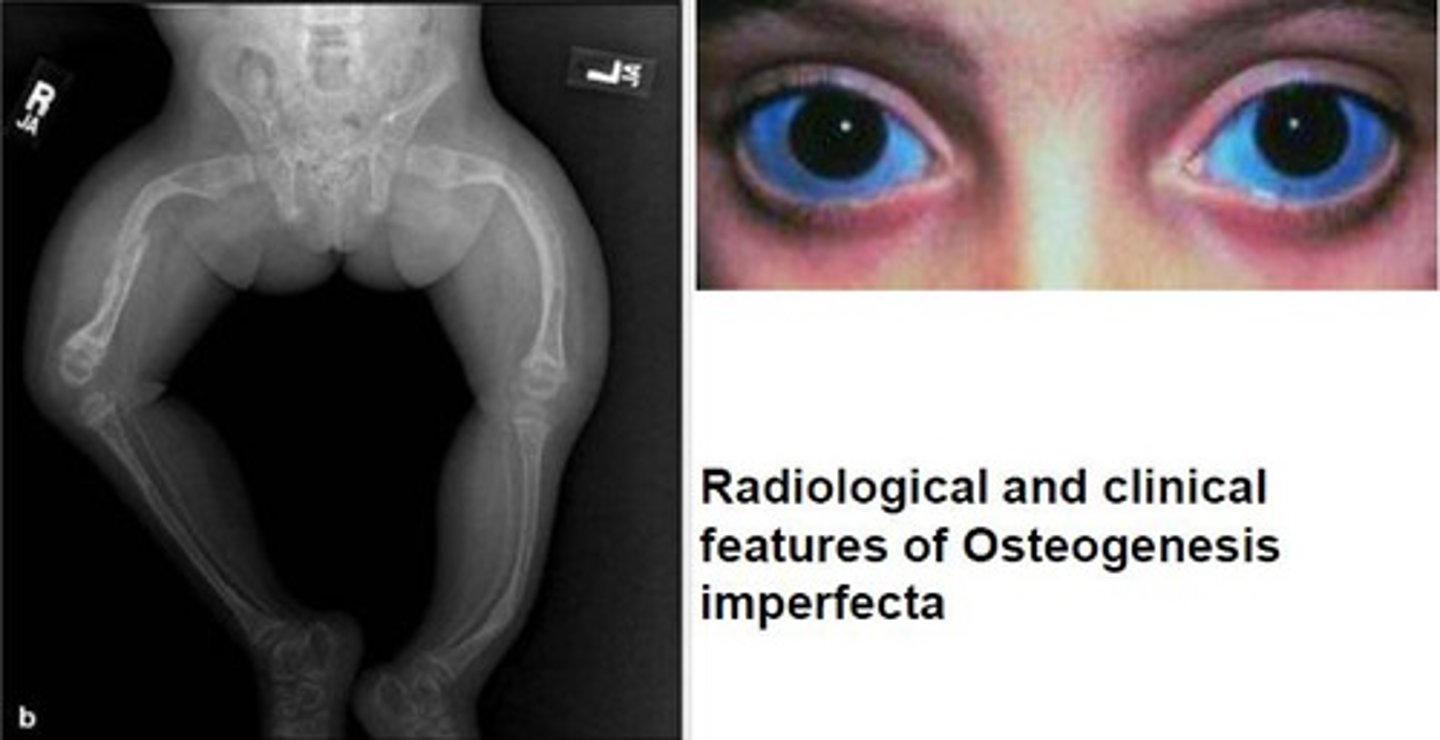
what are expected findings of osteogenesis imperfecta?
-multiple bone fractures (fragile bones and deformities)
-blue sclera
-early hearing loss
-small, discolored teeth
**multiple stages of bone healing can often be mistaken for abuse before diagnosed**
what is cerebral palsy?
a non-progressive impairment of motor function, especially that of muscle control, coordination, and posture
it can be either congenital (present at birth) or acquired (obtained after birth)
what are some expected findings in a child with cerebral palsy?
-gagging or choking with feeding, poor suck (swallowing issues, so aspiration risks!)
-asymmetric crawl
-toe walking
-hyperreflexia
-rigid/stiff posture and extremities; scissoring and extension of legs
-arching back
-trouble diapering child
-vision, speech, hearing impairments
-seizures
-cognitive impairments
-trouble reaching developmental milestones
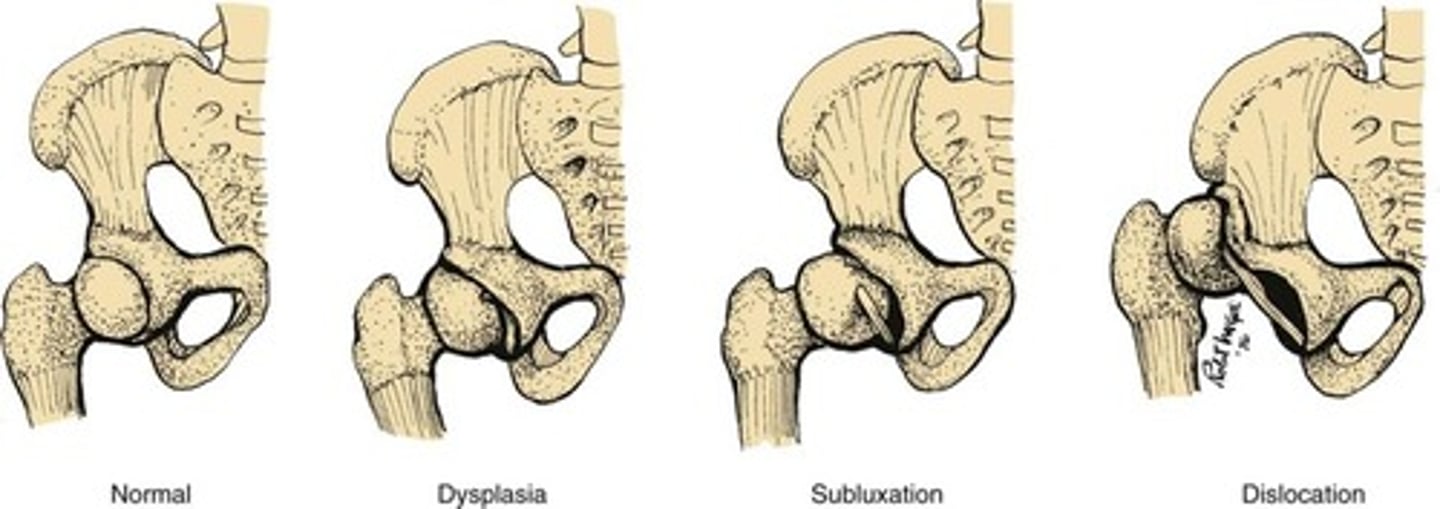
what is developmental dysplasia of the hip (DDH)?
abnormal development of the hip structures in infants and children
can be acetabular dysplasia, subluxation (incomplete dislocation), or dislocation (femur head not in proper position)
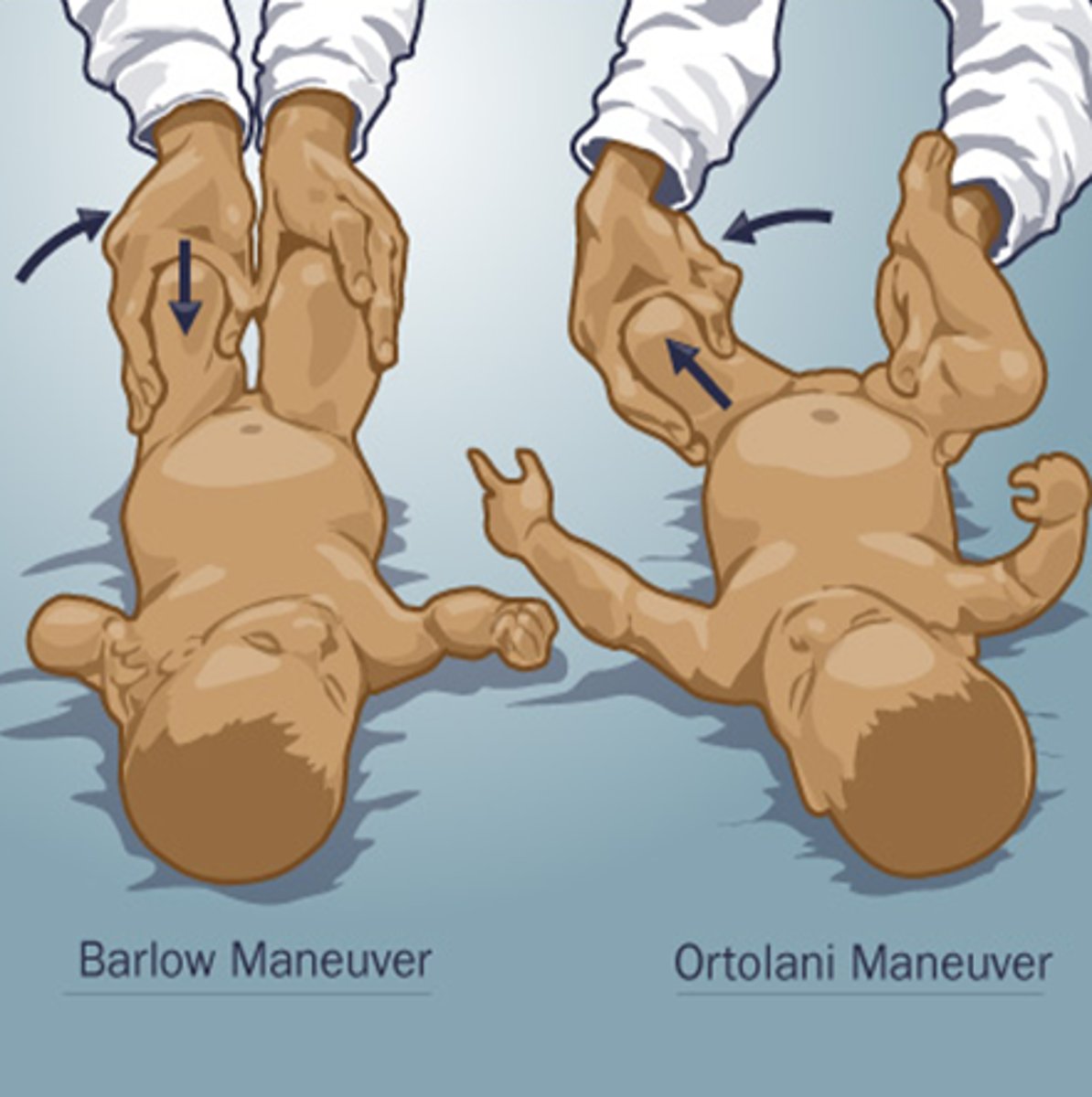
what screening/tests/diagnostics can a provider do to assess for developmental dysplasia of the hip?
ortolani test: hip is reduced by abduction
barlow test: hip is dislocated by adduction
also can do ultrasounds and x-rays
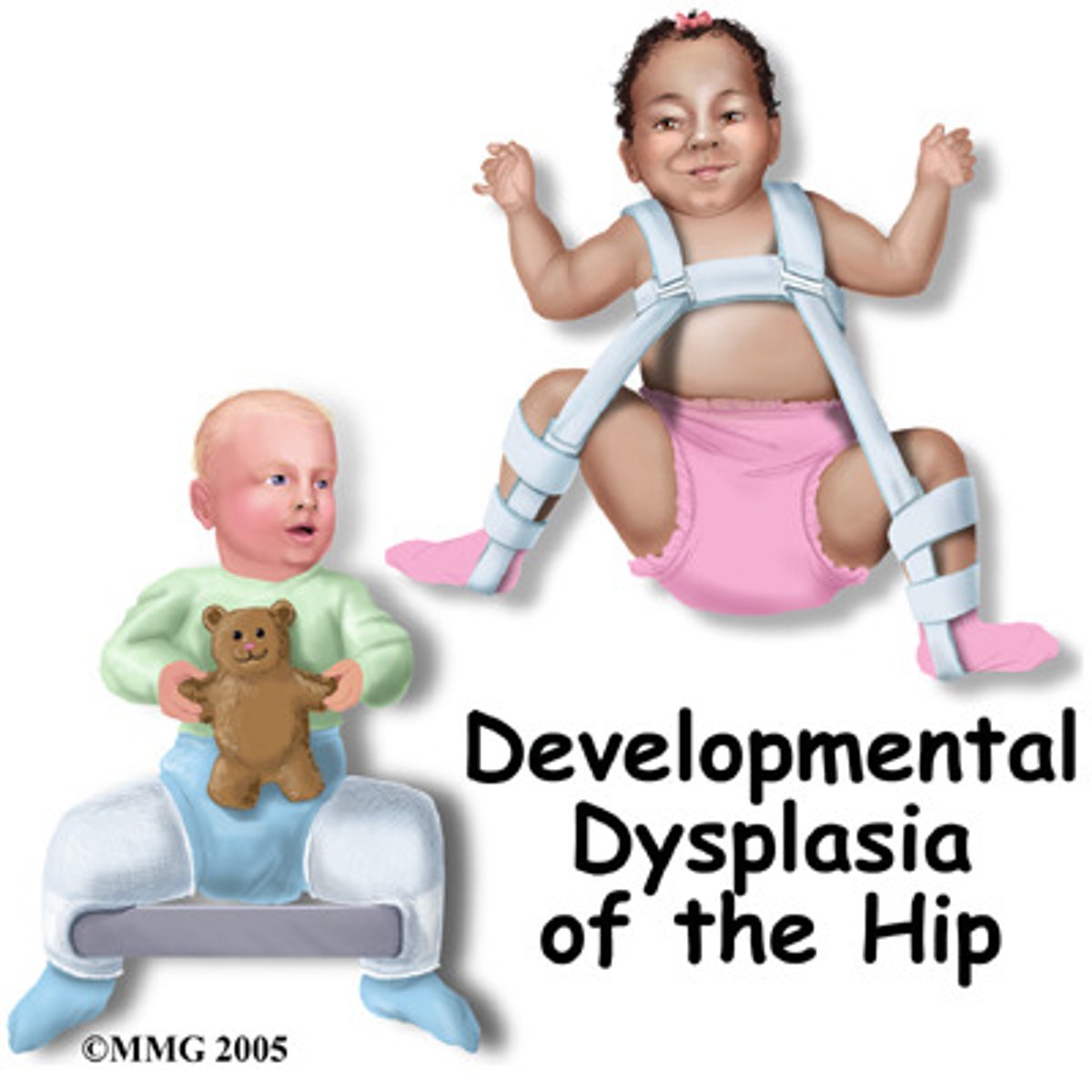
what is the treatment for developmental dysplasia of the hip (DDH)?
newborns to 6 months old:
-abduction splint (Pavlik harness)
-prevents hip flexion and adduction
-wear for 12 weeks, 23 hours/day
-want to check the straps and skin integrity
6 months to 2 years old (if Pavlik harness did not help):
-surgical reduction and hip spica cast
-maintains external rotation of the hip
-want to use a waterproof barrier around the cast to prevent soiling it
what are some physical manifestations of dying/death in a child?
-sensation of heat when the body feels cool
-decreased sensation and movement in legs
-loss of senses (hearing is last to go)
-confusion or loss of consciousness
-swallowing difficulties
-loss of bowel and bladder control
-bradycardia, hypotension
-Cheyne Stokes respirations
-secretions causing the "death rattle"
**encourage family to talk to the child all the way to the end since they can likely still hear if nothing else**
what is anticipatory grief?
when death is expected or a possible outcome
what is complicated grief?
extensive or prolonged grief
(intense, distressed yearning, unable to sleep or do normal life things, may need to see a mental health professional)
what is parental grief?
intense, long lasting grief
parents are also grieving the loss of hopes and dreams, family disruption, loss of identity as a parent)
parents can each grieve based on their role in their family
how do infants (birth to 3 years) perceive death and dying?
-no concept of death
-egocentric thinking
-mirror parents emotions
-react based on changes in their daily life or changes in routine
-regression possible
how do preschoolers (3-6 years) perceive death and dying?
-egocentric and magical thinking
-might think they are in trouble when they are separated from their parents
-think dying is temporary and don't understand due to their lack of concept of time and bc the dying person still sleeps, eats, and breathes
how do school aged kids (6-12 years) perceive death and dying?
-starting to have an adult concept of death
-have fear about death and the lack of control they feel about it
-might become uncooperative
-can be curious about funerals and what happens to the body
how do adolescents (12-20 years) perceive death and dying?
-understand what is happening
-have trouble accepting it
-can feel isolated
-become very stressed about what is happening
-may feel guilt and shame
when caring for a patient and family going through death and dying, what does the nurse need to assess for?
-knowledge of diagnosis, prognosis, and care
-what they think about and want regarding the diagnosis, prognosis, and care
-nutritional status and growth and development patterns
-activity and energy level of the child
-parents wishes regarding end of life care
-advanced directives?
-family coping and available support to them
-stage of grief the child and family are in
what are some adverse effects/complications caused by chemotherapy and radiation in kids?
-skin breakdown
-constipation
-foot drop
-pain
-loss of appetite
-hemorrhage cystitis
-bone marrow suppression causing anemia (Hgb < 12, Hct <36; low O2), neutropenia (WBC under 1500; easy infections), and/or thrombocytopenia (platelets <150,000; bleeding)
-anorexia, nausea, vomiting
-alteration in bowel elimination (either diarrhea from radiation or constipation from chemo)
-mucositis and dry mouth
-alopecia
what education and nursing interventions can you plan for with a child receiving chemotherapy regarding skin breakdown?
-inspect skin daily
-examine rectal mucosa for fissures & avoid rectal temps
-sitz baths as needed
-reposition often & use a pressure reduction system
what education and nursing interventions can you plan for with a child receiving chemotherapy regarding constipation?
-encourage fiber in diet
-give stool softeners and laxatives
-lots of fluids
what education and nursing interventions can you plan for with a child receiving chemotherapy regarding pain?
-frequently assess pain level
-give prescribed analgesics
-try multiple pain relief interventions pharm & non-pharm to see what helps/what doesn't
what education and nursing interventions can you plan for with a child receiving chemotherapy regarding loss of appetite?
-monitor fluid intake and hydration, as well as electrolytes
-daily weight on child
-provide small, frequent, well balanced meals with high protein and high calorie foods
-use supplements as needed
-include the child in meal planning
-use enteral nutrition as needed
-try to give chemo early in the day
-if n/v present, give antiemetics before or after chemo
what education and nursing interventions can you plan for with a child receiving chemotherapy regarding bone marrow suppression/anemia/neutropenia/thrombocytopenia?
-watch vitals closely and report a temp > 100 F
-watch for signs of infection and lesions in the mouth; watch any wounds closely
-give any antimicrobial, antivirals, or antifungal meds as prescribed
-protect the child from sources of infection (crowds, ppl who are known to be sick,
-use good hand hygiene
-avoid invasive procedures (injections, rectal temps, catheters)
-watch for signs of bleeding; no aspirin and NSAIDs
-watch for headaches, fevers, and bone pain
-use a soft toothbrush
-rest is important to make time for it
what education and nursing interventions can you plan for with a child receiving chemotherapy regarding anorexia/nausea/vomiting?
-avoid strong smells
-don't offer child' favorite food during chemo or they might develop an aversion to it!!
-provide small, frequent meals
-give antiemetics before meals
what education and nursing interventions can you plan for with a child receiving chemotherapy regarding mucositis and dry mouth?
-use soft toothbrush
-lip balm/vaseline child's lips
-give soft, non-acidic foods
-take analgesics as needed
-avoid hydrogen peroxide and lemon bc it can dry and worsen the irritated mouth; use chlorhexidine mouthwash instead
-use salt rinses for healing and soothing of the mouth
what education and nursing interventions can you plan for with a child receiving chemotherapy regarding alopecia and hair loss?
-monitor how the child feels about this
-talk about cutting long hair shorter
-use gentle shampoos and brush gently
-avoid blow dryers and curling irons/hot tools
-suggest a cotton hat or scarf; talk about wigs and hats
-take care of the scalp well
-educate about hair growing back in 3-6 months
what is leukemia?
group of malignancies that affect the bone marrow and lymphatic system
causes increase in immature WBCs that infiltrate organs and tissues and takes over healthy cells
most common childhood cancer
can be either acute lymphoid leukemia (ALL) or acute myelogenous leukemia (AML)
what are some expected findings in a child with leukemia?
-really high WBC (big increase in immature WBCs is more deadly), low RBCs, low platelets
-low grade fever
-pallor, bruising, petechiae
-enlarged liver, lymph nodes, joints, kidneys, and testicles
-abdominal, leg, and joint pain
-headaches
-vomiting and anorexia
-unsteady gait (due to bone pain)
-pain
-signs of increased ICP
what is osteosarcoma?
bone cancer usually at the metaphysis of a long bone (like the femur)
most common bone cancer in adolescents
usually peaks during adolescence and overlaps with growth spurts (around age 15)
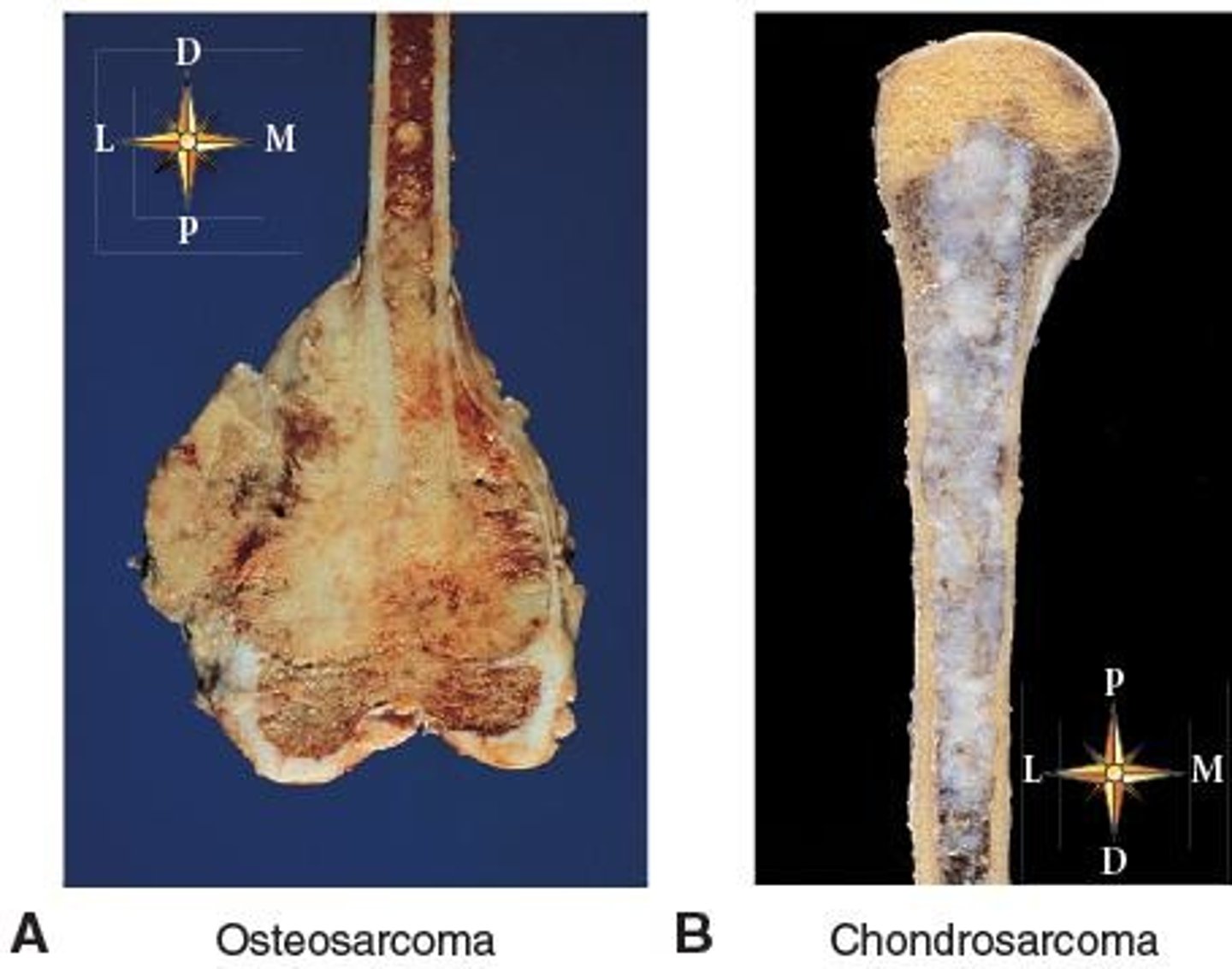
what are some common expected findings in bone cancer/tumors like osteosarcoma?
-nonspecific bone pain that is often mistaken for an injury or growing pains
-weakness, swelling, decreased movement, or limping
-anemia, fever, or unexplained weight loss
-inability to lift a heavy object
-temporary relief of pain when the extremity is flexed
-palpable lymph nodes near the tumor
what is rhabdomyosarcoma?
malignant tumor/cancer of skeletal muscle anywhere in the body
most common soft tissue malignancy in children
seen in kids younger than 5 most commonly
causes pain in local areas due to compression by the tumor
what are the expected findings with rhabdomyosarcoma?
symptoms depend on the area that the tumor is located; can be anywhere in the body there is skeletal muscle
pain and discomfort comes from the tumor pressing on the area or other organs/body parts
ex: in an extremity, there would be pain, a palpable mass, and lymph node enlargement. in the eye area, there would be redness of the eye, trouble seeing, and a visible mass in the area
what is the Epstein-Barr virus (Mononucleosis)?
aka the "kissing disease"
communicable disease that spreads through saliva
has an incubation time of 30-50 days and can be transmitted to others for weeks
what are the expected findings of the Epstein-Barr virus (mono)?
-fever
-lethargy
-sore throat
-swollen lymph glands
-loss of appetite
-headache
-increased WBCs
-atypical lymphocytes
-splenomegaly!
-hepatic involvement
what is the #1 complication that can come from Epstein-Barr virus (mono)?
ruptured spleen
*so no rough-housing or rough play or contact sports for several weeks to prevent rupture!*
what is conjunctivitis?
pink eye; inflammation of the conjunctiva
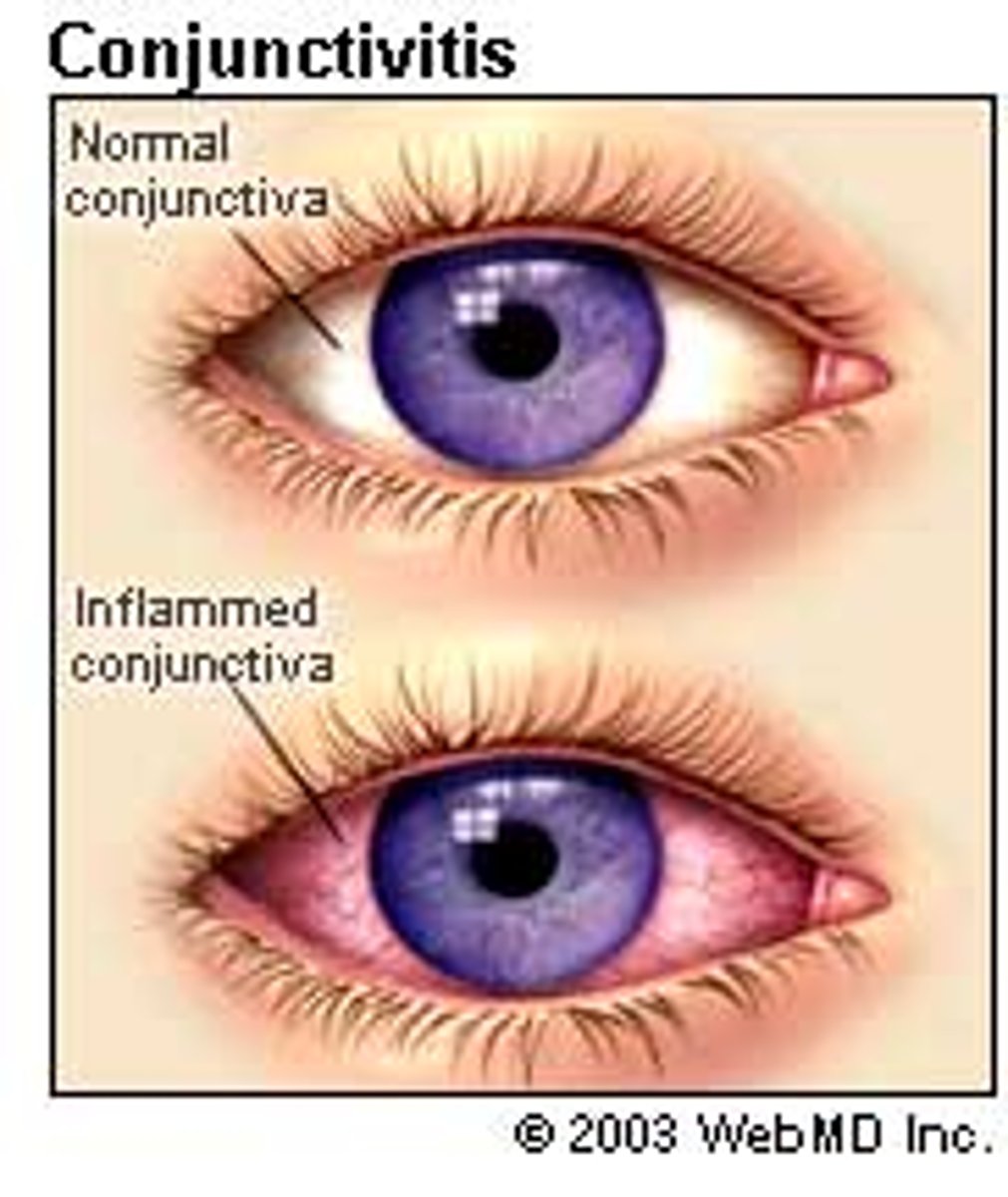
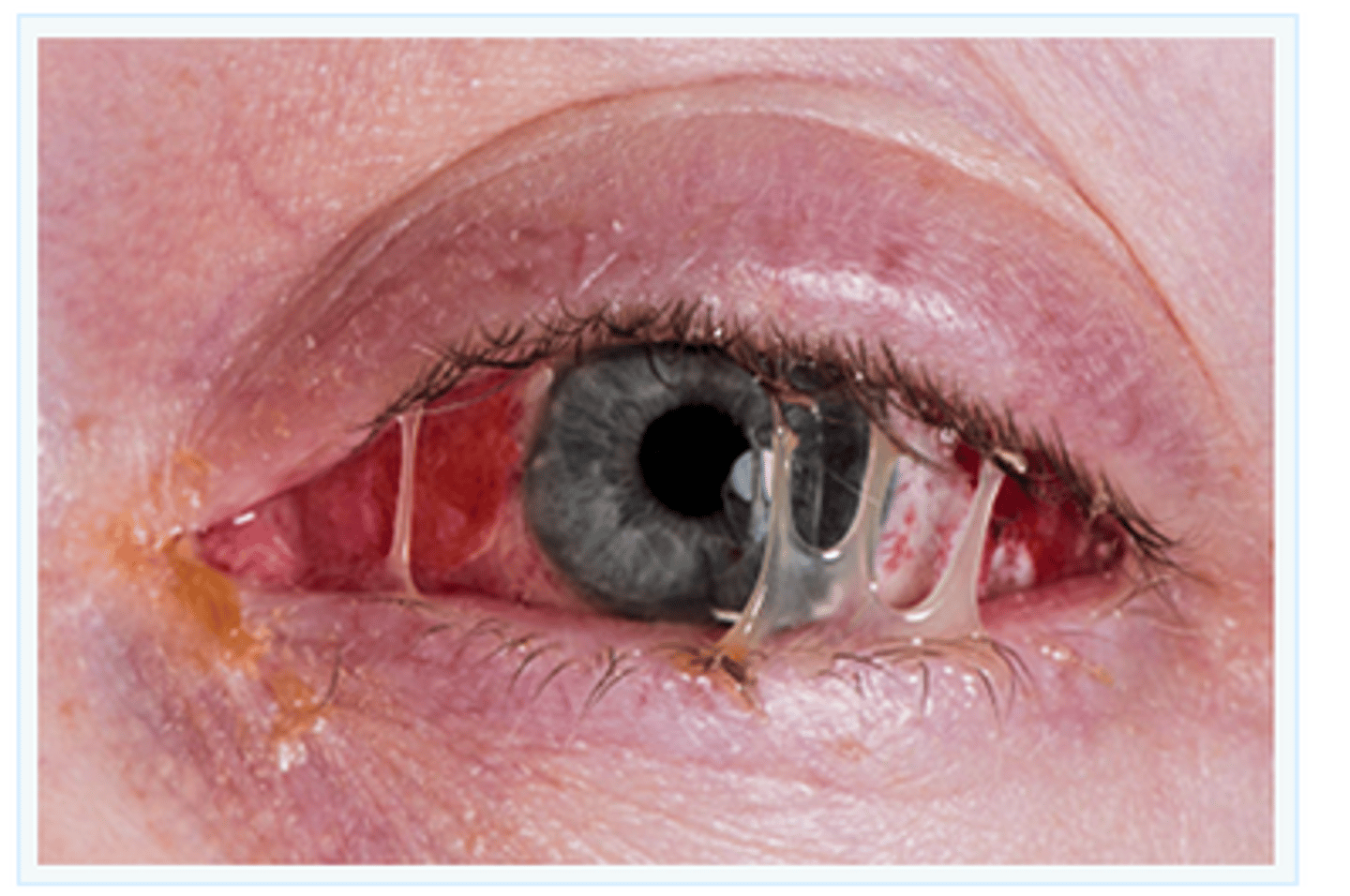
what are the expected findings of conjunctivitis (pink eye)?
-pink or red color in the sclera of the eyes
-swelling
-excessive tears
-yellow-green, purulent discharge (bacterial)
-crusting of the eyelids in the morning (bacterial)
-watery eye discharge (viral)
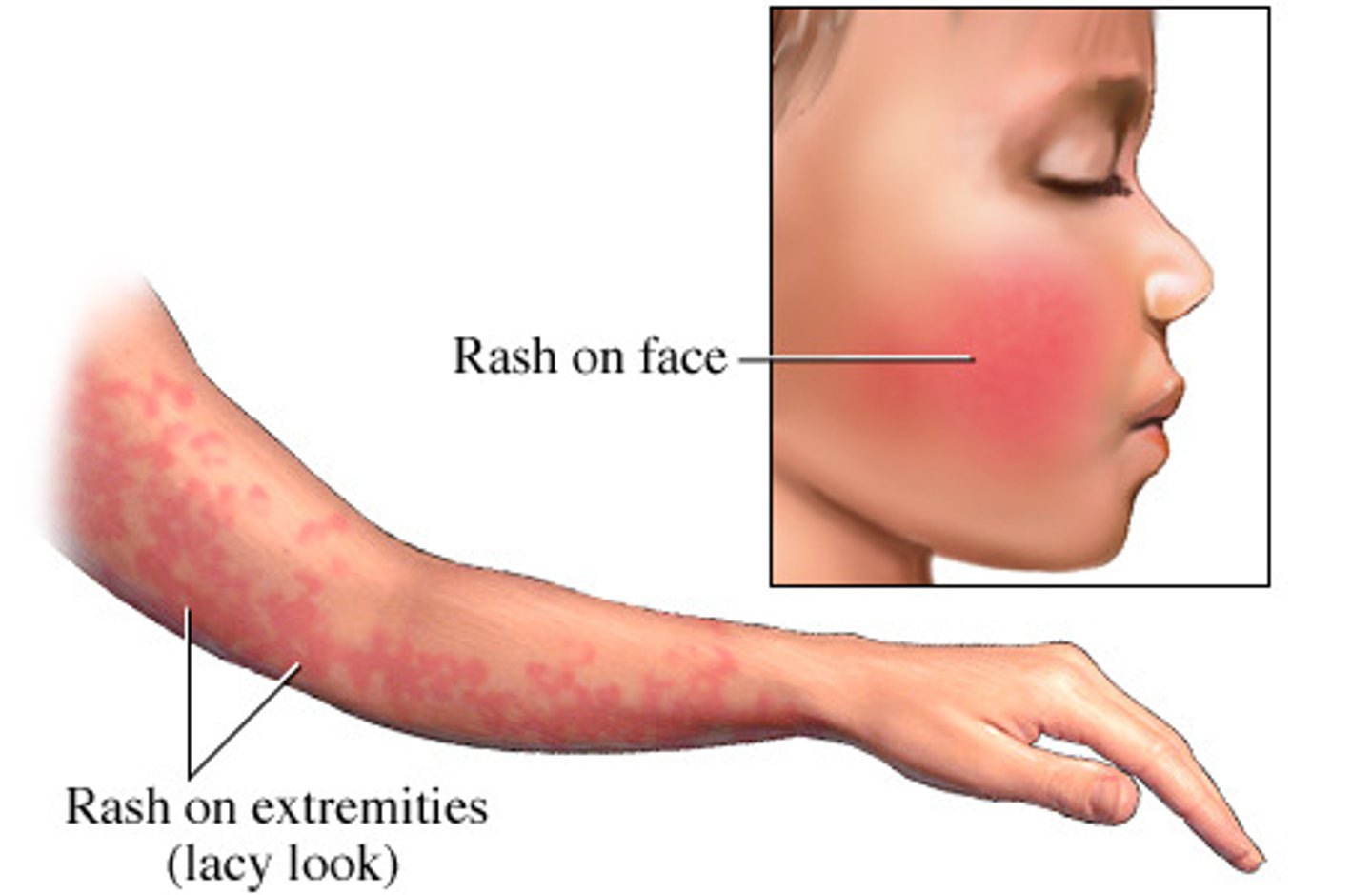
what are the expected findings of erythema infectiosum (Fifths Disease)?
-starts as fever, runny nose, headache
-turns into red, lacy rash on face (slapped cheek)
-maculopapular red spots symmetrically on upper and lower extremities
-itchy rash that can appear on rest of the body, especially soles of the feet
**check entire body for rash!!**
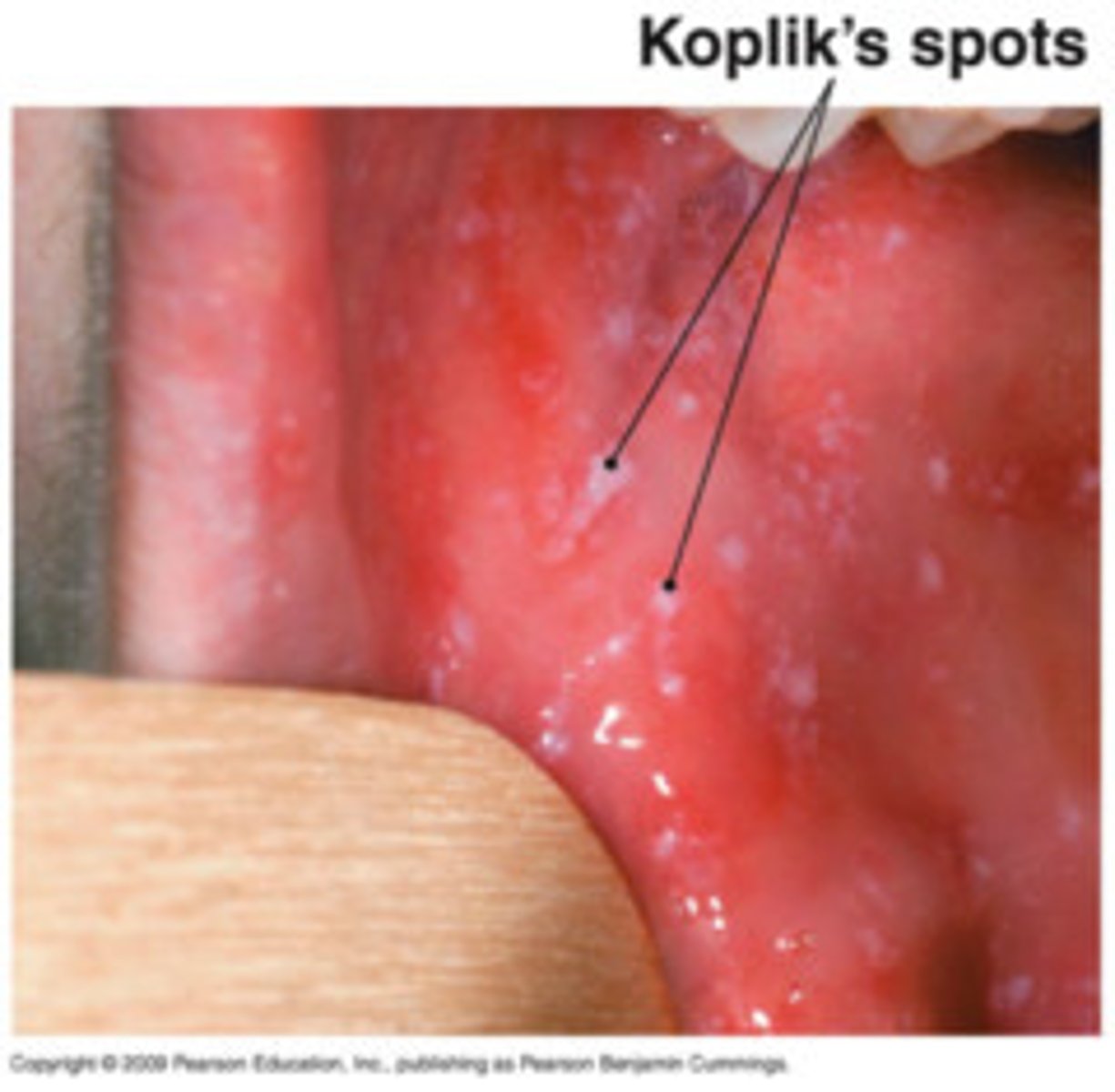
what are the expected findings of measles (rubeola)?
-starts with a fever, conjunctivitis, fatigue, cough, runny nose, red eyes, and a sort throat
-Koplik spots (tiny white spots) in the mouth before the rash starts
-red or reddish brown rash beginning on the face then spreads downwards
-spike in fever with rash
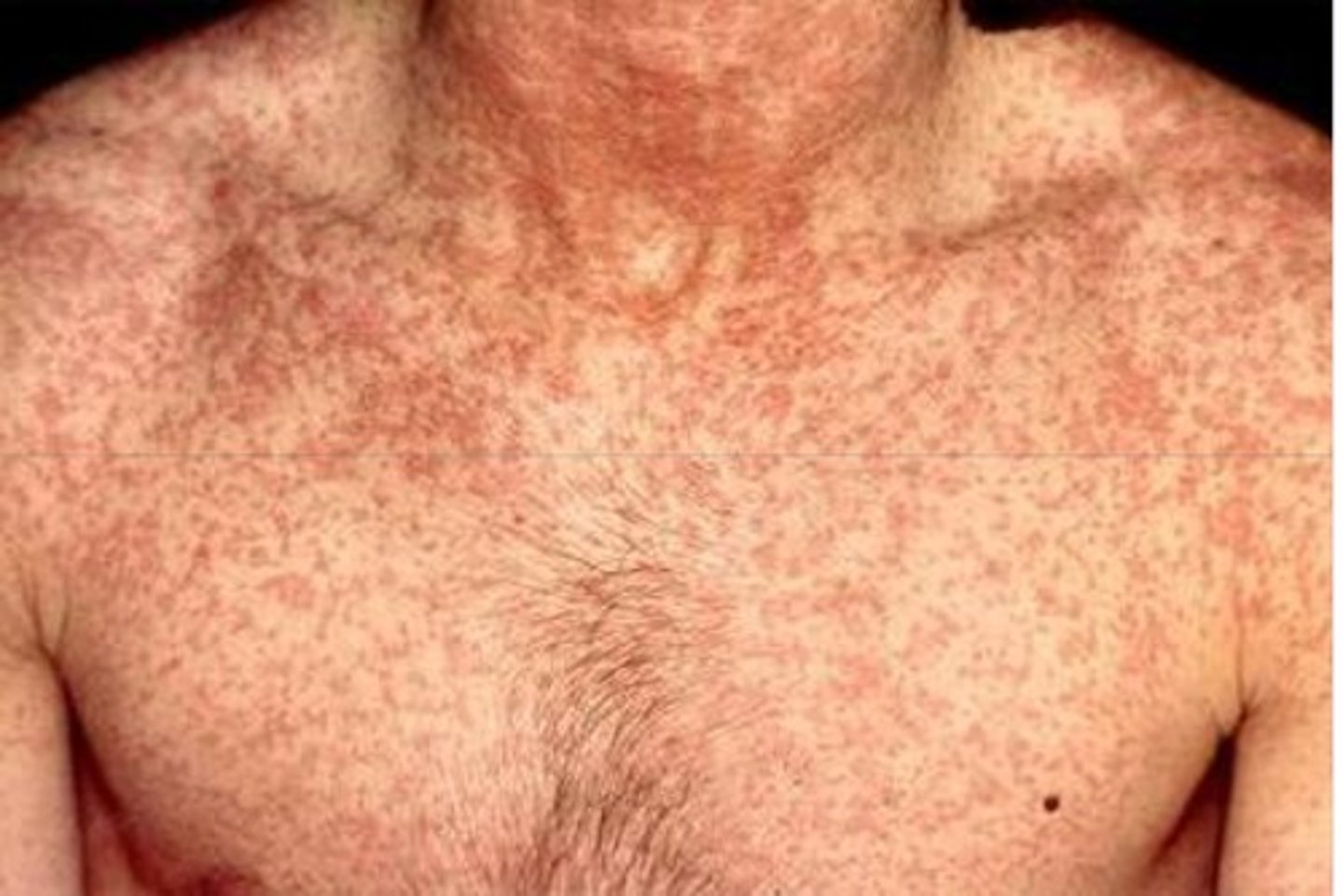
what are the expected findings of rubella (german measles)?
-low grade fever and sore throat
-headache
-malaise
-cough
-lymphadenopathy
-red rash on face then spreads to the rest of the body
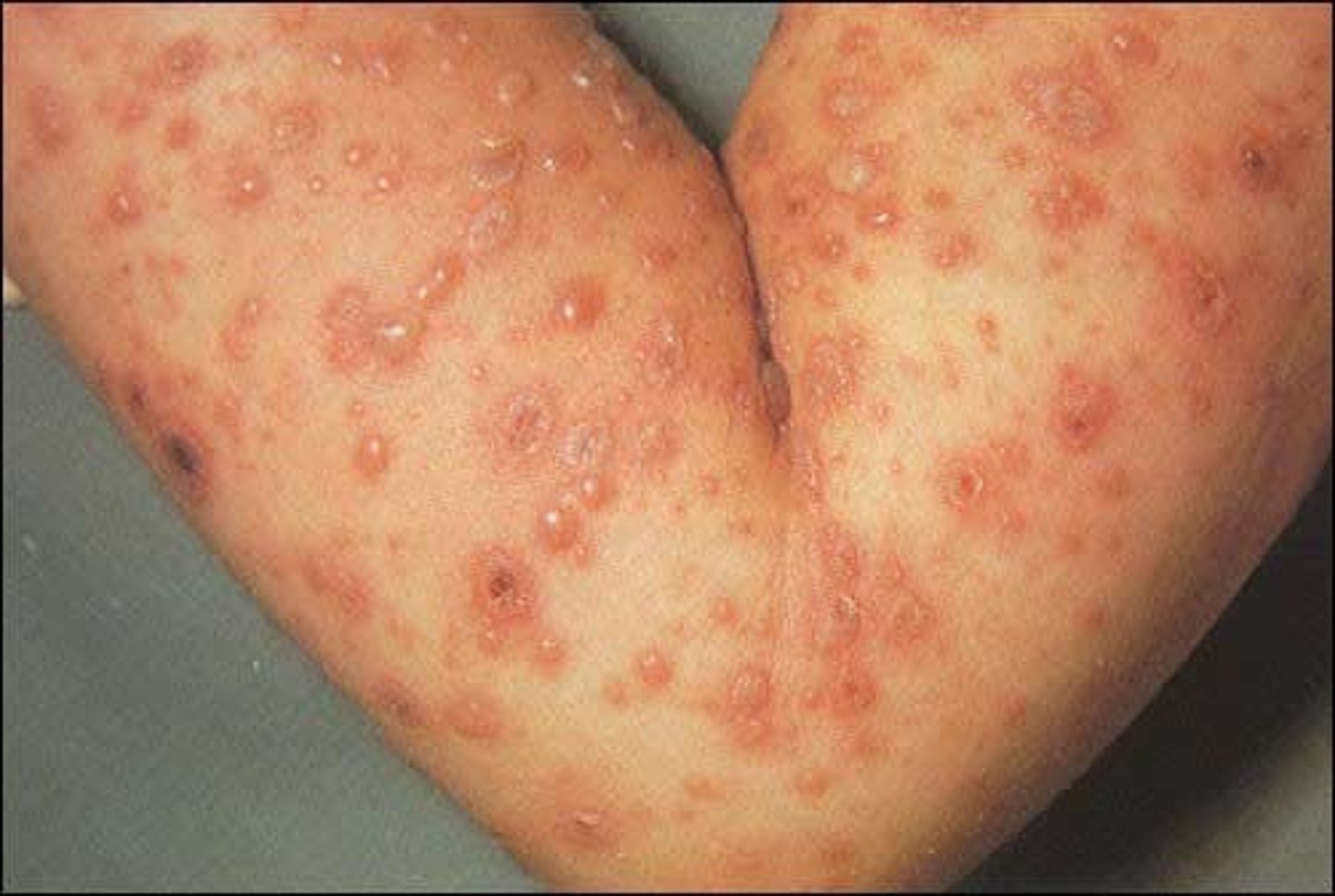
what are the expected findings of varicella (chickenpox)/ varicella-zoster virus?
-starts with fever, fatigue, loss of appetite, and headache before rash
-macules start in center of the trunk spreading to the face and proximal extremities
-macules turn into papules, then vesicles, and crust forms
-scabs appear in about a week
**very itchy**
what are the expected findings of mumps?
-painful, swollen parotid glands
-fever and muscle aches
-headache
-earache made worse by chewing
-fatigue and loss of appetite
what are the expected findings of pertussis (whooping cough)/bordetella pertussis?
-common cold manifestations at the start
-severe coughing after 1-2 wks
-coughing fits
-violent, rapid coughing
-loud whooping sound upon inspiration
what nursing care & education should the nurse plan for when caring for a pediatric patient with HIV/AIDS?
-balanced diet with calories and protein
-good oral care
-keep skin clean and dry
-pain control
-prevent infections; avoid sick people
-encourage immunizations (pneumococcal and flu); educate about when to avoid certain vaccines
-use standard precautions
-use safe practice when using needles, syringes, and giving any meds
-encourage turn, cough, deep breathing
-good hand hygiene
-psychosocial support; identify stressors and make referrals as needed
-educate about transmission and high-risk behaviors; talk to adolescents about transmission through sex and IV substance use!!!)
-educate about med adherence that will be lifelong antiretroviral therapy to reduce progression to AIDS, reduce viral load, and reduce infection risk
a child's lymphoid tissues reach adult size at what age?
6 weeks of age
when does the pediatric thymus reach peak mass?
before puberty
when does the pediatric spleen reach full size?
adulthood
why are infants and young children at risk for infections and getting sick compared to adults?
-not a lot of room for their body to initiate an antibody response
-immature inflammatory response (their symptoms are less severe and harder to diagnose)
-diminished nonspecific immune response (so infection spreads easy and fast)
-transplacental transfer of IgG from mom drops around 6-8 months
when do pediatric helper T cells reach adult levels?
by 6 years old
what precautions should be taken and kept in mind when giving immunizations to pediatric clients?
-watching for severe allergic reactions in response to a vaccine
-being cautious if a client has a moderate to severe illness with or without a fever before giving vaccine
-severe febrile illness IS a contraindication to all immunizations
**the common cold and other minor illnesses are NOT contraindications to vaccines**
who should NOT receive live virus vaccines (like varicella or MMR)?
1. severely immunocompromised (autoimmune, cancer, HIV, organ transplant pt on anti-rejection meds)
2. pregnant
3. pts who have received treatment that provides acquired passive immunity (like blood products or immunoglobulins) within last 3 months
what is acute otitis media?
infection of the middle ear
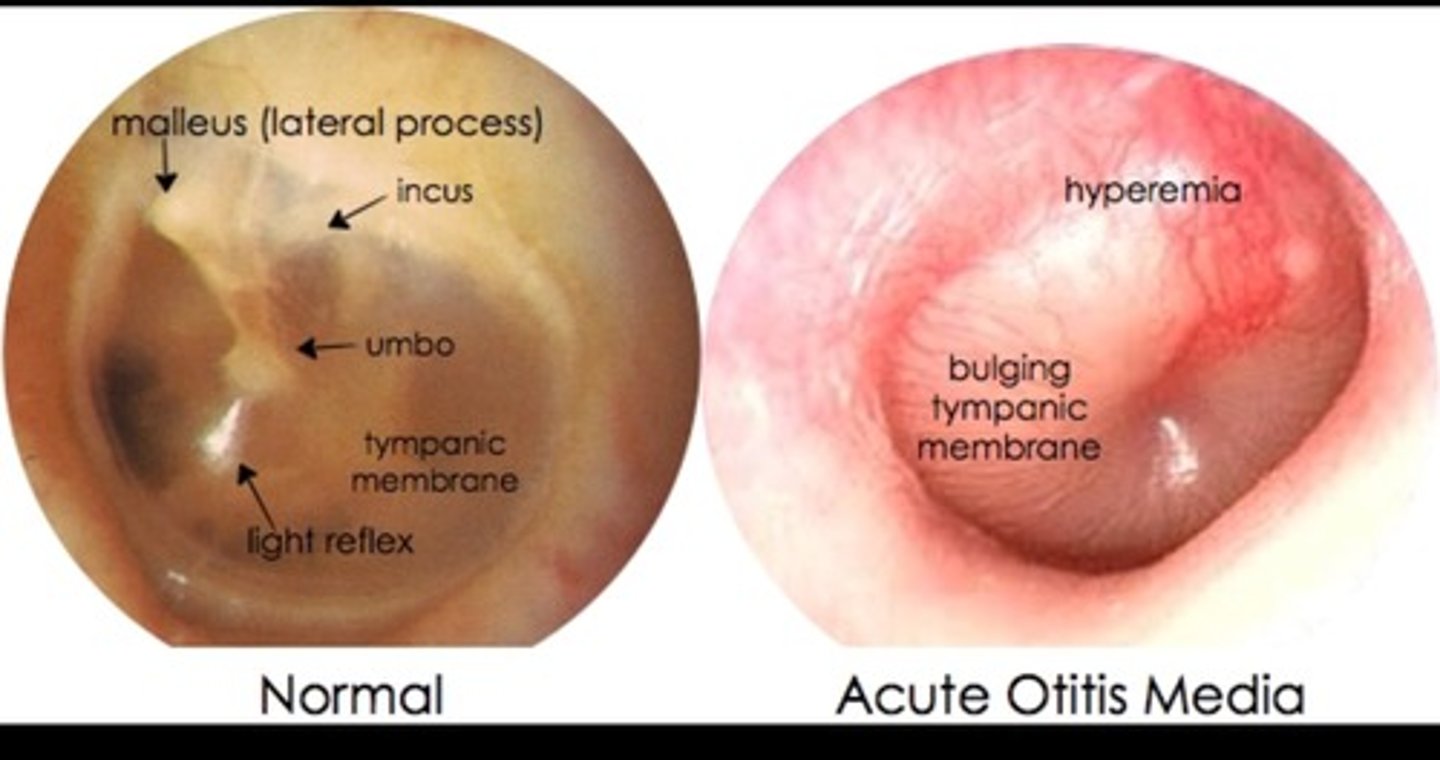
what nursing care can be planned for a child with acute otitis media?
-comfort measures
-manage/treat fevers
-provide analgesics (acetaminophen or ibuprofen); this is a priority action!!
-antibiotics
-possible myringotomy and placement of tympanoplasty tubes if recurrent AOM
-feed child in an upright position!!!
-watch for hearing loss and speech delays
what kind of antibiotics might be used to treat acute otitis media in a pediatric patient and what education should be provided about this?
amoxicillin (1st line), augmentin, or cefdinir PO in high doses usually over 10 days
education: need to finish all days of antibiotics; typically children start to feel better after 2-3 days
a child who just started insulin therapy for T1DM is in the "honeymoon" phase. what does this mean? what education should be given to parents about this?
there is decreased amounts of insulin being needed
education: some parents see this as there child is "cured". it can last 7-8 months and their parents need to know that they need to still be watching their child's insulin needs and sugars since it was increase over time.
how often should a child's blood sugar be checked when they are sick?
every 3 hours
what education should be provided to parents about when their diabetic child is sick and how to manage their diabetes/insulin needs?
-check sugar every 3 hours and adjust insulin as needed
-test urine for ketones
-call the provider if their sugar is greater than 240
-do not stop taking insulin when sick, especially if they are taking any kind of steroids bc this raises their blood sugar and T1DM kids cannot live without insulin
in a child with growth hormone deficiency, how should their weight and height compare?
they have delayed growth, but normal weight for that height (proportional)
how often do kids with growth hormone deficiency need to have their height/weight measured?
every 6 months before the age of 3 then once a year after the age of 3
what are the expected findings in a child with growth hormone deficiency?
SLOW KID
s: short stature (but proportional)
l: late epiphyseal closure
o: onset of delayed dentition
w: weak jaw development
k: kids have insulin deficiency
i: immature sexual development (delayed puberty)
d: dropping below 2 standard deviations on growth chart
where is growth hormone secreted from?
pituitary gland
a pediatric client has just come with diabetic ketoacidosis. what nursing interventions need to be done asap?
-rapid IV fluid resuscitation (0.9% NaCl)
-IV insulin
-monitor blood glucose hourly
-give sodium bicarb for severe acidosis
-monitor potassium levels (will be high initially with starting insulin but will then shift into cells)
-monitor I/Os
-put on continuous cardiac monitor
what medications might be used for pediatric ADHD?
methylphenidate (Ritalin) or dextroamphetamine (Adderall) -----> these are STIMULANTS
atomoxetine (Strattera) ----> SSRI
what nursing care and education can the nurse plan for in caring for a pediatric patient with ADHD?
-should use a calm, but firm approach with the child
-use checklists to stay organized
-provide safe environment
-encourage family therapy
-recommend behavioral strategies to parents (positive reinforcement, rewards for good behavior, age-appropriate consequences)
-educate and assist in modifying the environment for them (structure, charts, decreased stimuli, modeling positive behavior, steps when assigning chores, pastel colors)
-assist with appropriate classroom placement
what can the nurse plan to educate about regarding pediatric bullying and what to look for/do in the case that bullying is occuring?
-observe for signs and be inquisitive
-refer to counseling and bullying prevention programs
-listen to them first
-practice empowering ways to react
-add strong words
-shut down online bullying (cyberbullying is against the law in all 50 states)
-encourage friendships
-know when to get other adults involved
-refer to stopbullying.gov
what are pediatric risk factors for burns?
-abuse, neglect, or lack of supervision
-developmental growth of the child
why are burns worse in pediatric patients?
they have thinner skin (more extracellular fluid), so injury is usually more severe and they lose fluids faster
when a child has a large burn, what interventions need to be a priority after ABCs have been managed?
really need to treat their pain (IV morphine) and their temperature
how does the TBSA of a pediatric client compare to the TBSA of an adult when it comes to burns?
pediatric TBSA is greater than adults when they get burned
what are the 3 classification of burns and where is each of them treated?
minor: outpatient setting
moderate: treated in a hospital with expertise in burn care
major: requires medical services of a burn center
how deep does an epidermal burn go? expected findings?
burns through the epidermis
skin is red and painful but no blisters (sun burn)

how deep does a superficial partial thickness burn go? expected findings?
burns through the epidermis and upper layer of the dermis
skin is pale pink and painful with blisters; cap refill blanches and rapidly returns
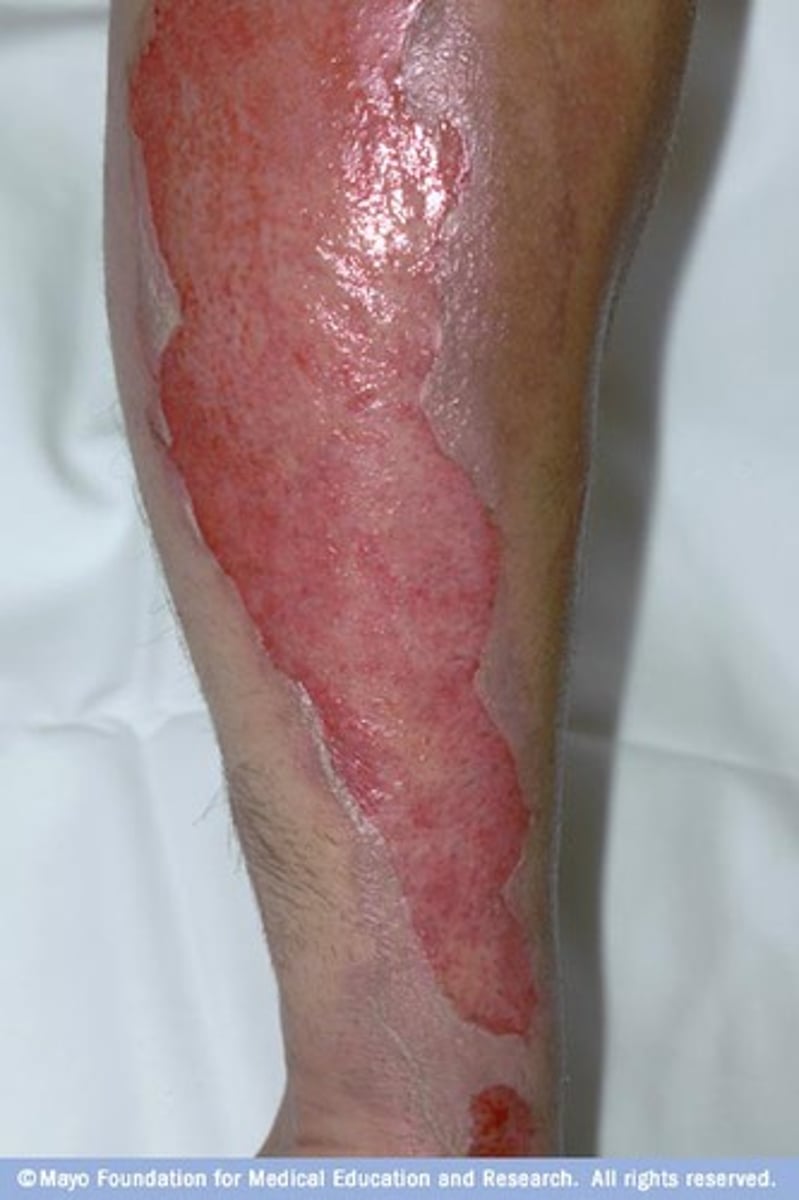
how deep does a deep partial thickness burn go? expected findings?
burns through the epidermis, upper, and deeper layers of the dermis
skin is dry or moist, blotchy, or cherry red and may be painful or painless. may be blisters. cap refill blanches with a sluggish return or does not blanch.
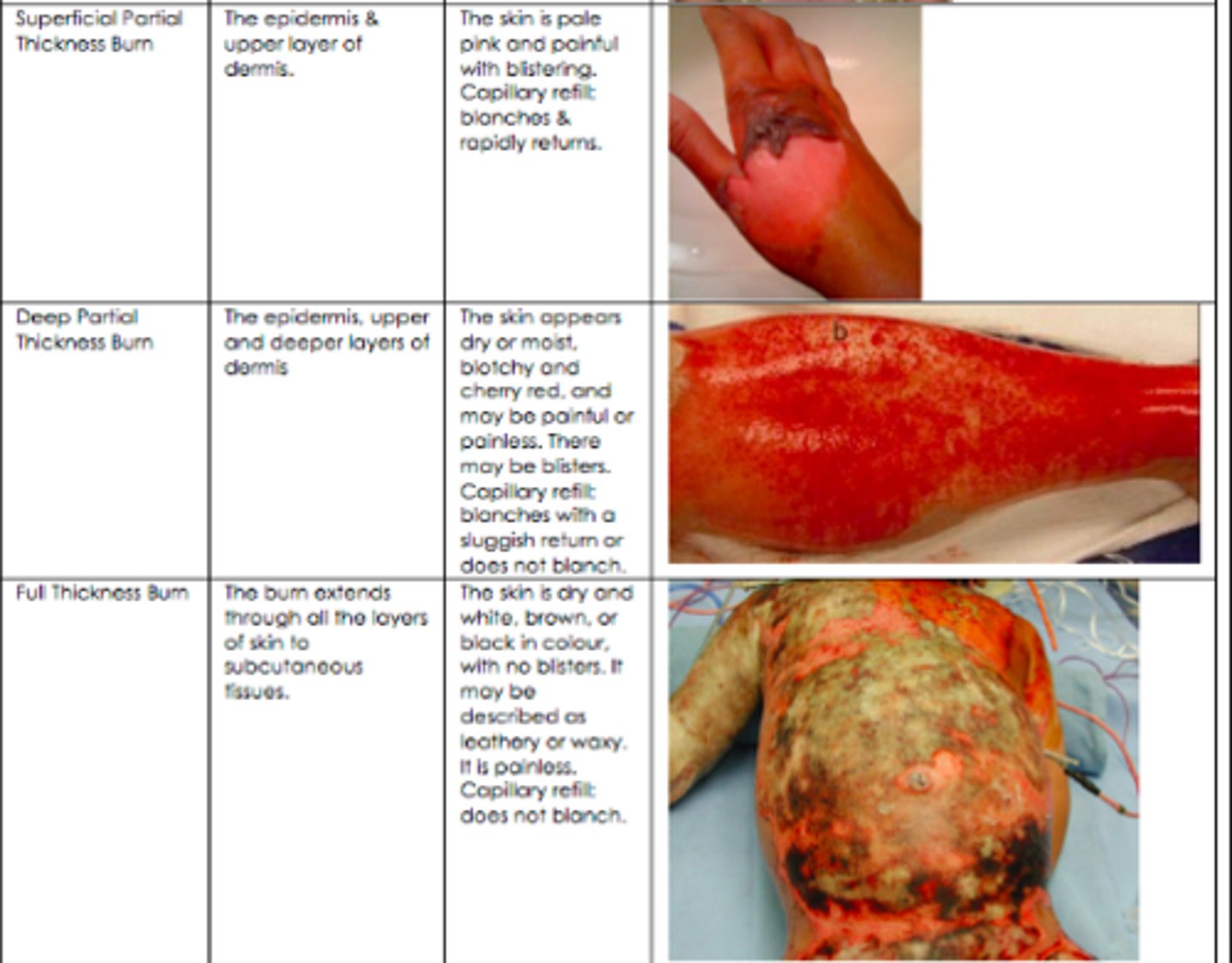
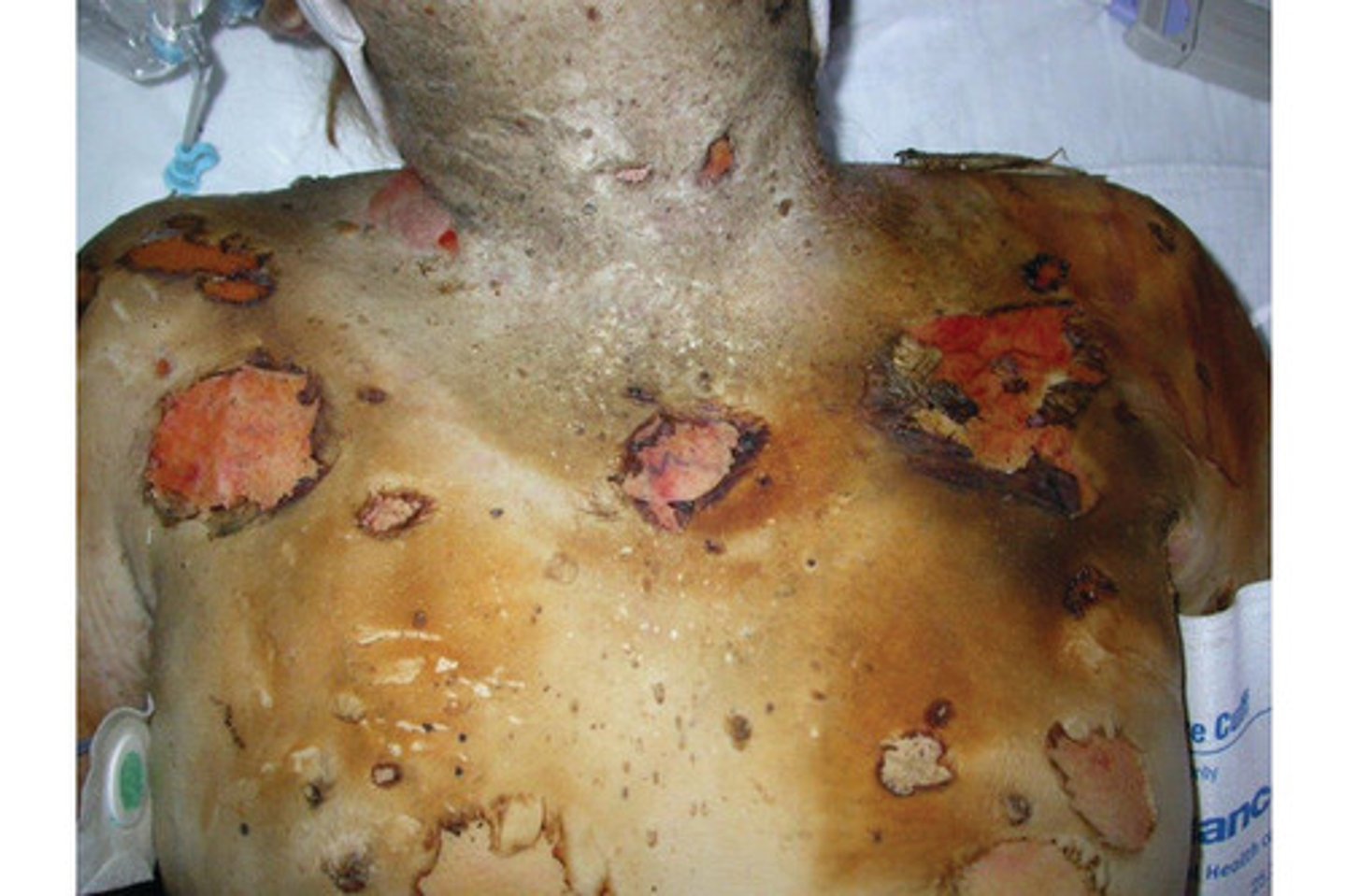
how deep does a full thickness burn go? expected findings?
burns through all layers of skin to the subcutaneous tissues
skin is white, brown, or black. no blisters. leathery or waxy and is painless. cap refill does not blanch.
how does the rule of nines break down TBSA for the pediatric client?
head and neck 9% (front) and 9% (back) = 18% total
each arm + hands each 4.5% (front) and 4.5% (back) = 9% total for each arm
torso 18% (front) and 18% (back) = 36% total
each leg + feet 7% (front) and 7% (back) = 14% total
what is the medical term for scabies?
sarcoptes scabiei
what is the medical term for lice?
pediculosis capitis
how does scabies spread?
by direct contact with an infected person
how does lice spread?
direct contact with an infected person, bedding and objects like hair brushes and clothing
what nursing interventions should the nurse plan for when caring for pediatric patients with scabies or lice?
-teach the child and parents about the medications
-assess for infestations
-if its scabies, look for pencil-like marks on the skin
-if its lice, look for small, grayish-tan bugs with no wings or nits, which look like dandruff on the hair shaft and are firmly attached
-assess for secondary skin infections
what patient education should the nurse give a child and their parents about caring for scabies or lice?
-avoid home remedies as it can worsen infections
-the correct laundering of potentially infected clothing and bedding (in hot water with detergent)
-bag items that cannot be laundered into tightly sealed bag for 14 days
-boil combs, brushes, and hair accessories for 10 min or soak in lice killing products for 1 hour
-avoid sharing personal items
how are school-aged kids developing psychosocially at their age?
-they care a lot about what adult figures think
-erikson: industry vs. inferiority
industry: learning skills an knowledge that allows them to start providing meaningful contributions to society
-a sense of accomplishment is gained through the ability to cooperate and compete with others
what can school-aged kids do/participate in to develop and support their psychosocial development of belonging and being a part of something with others?
organized sports
helps them develop psychosocial skills like resilience and confidence
a school-aged kid is dealing with chronic illness, putting them in the hospital often. how can this affect their psychosocial development?
leads to feelings of inferiority
what erikson stage of development are adolescents in (12-20 yrs)?
identity role vs. confusion
they try different roles and experiences to develop a sense of personal identity and come to view themselves as unique individuals
they may also become part of a group of peers that will greatly influence their behavior (peer pressure!!)
in adolescent females, in what order does their sexual maturation occur?
1. breasts buds
2. pubic hair
3. armpit hair
4. menstruation/periods
**boobs, pubes, pits, period**
in adolescent males, in what order does their sexual maturation occur?
1. testicular enlargement
2. pubic hair
3. penile enlargement
4. armpit hair
5. facial hair
6. voice changes
**balls, pubes, penis, pits, beard, voice**
how can we keep school-age children safe from bodily harm at this age in a way that applies to them and their current activities/hobbies with their friends?
teach kids to wear helmets, and or pads when roller skating, skateboarding, bicycling, riding scooters, skiing, and snowboarding
A nurse is caring for a child with Osteogenesis Imperfecta type 3. Which of the following
interventions should the nurse implement for this child? SATA
A) Administer bisphosphonate medications to increase bone density.
B) Encourage the use of assistive devices such as crutches or wheelchairs.
C) Apply heat to painful areas to relieve discomfort.
D) Encourage resistance band exercises
E) Provide a safe environment to prevent fractures
a. admin bisphosphonate meds to increase bone density
b. encourage use of assistive devices like crutches or wheelchairs
e. provide safe environment to prevent fractures
Which sport does the nurse recommend to the child with osteogenesis imperfecta who is interested in physical fitness?
A) Ice hockey
B) Gymnastics
C) Swimming
D) Judo
c. swimming
The parent of an infant asks the nurse what to watch for to determine whether the infant has cerebral palsy. Which is the nurse's best response?
A) If the infant cannot sit up without support before 8 months.
B) If the infant demonstrates tongue thrust before 4 months.
C) If the infant has poor head control after 2 months.
D) If the infant has clenched fists after 3 months.
d. the infant has clenched fists after 3 months
The nurse is developing a plan of care for a child recently diagnosed with cerebral palsy. Which should be the nurse's priority goal?
A) Ensure the ingestion of sufficient calories for growth.
B) Decrease intracranial pressure.
C) Teach appropriate parenting strategies for a special-needs child.
D) Ensure that the child reaches full potential.
c. teach appropriate parenting strategies for a special needs child
Which would the nurse expect a child with spastic cerebral palsy to demonstrate? SATA
A) Increased DTR
B) Decreased muscle tone.
C) Scoliosis
D) Contractures
E) Scissoring
F) Good control of posture
G) Good fine motor skills
a. increased DTR
c. scoliosis
d. contractures
e. scissoring
A nurse is providing teaching to a guardian about complicated grief. Which of the following statements should the nurse make?
A) Complicated grief occurs when little time is spent thinking about the loss
B) Personal activities are rarely affected when experiencing complicated grief
C) Guardians will experience complicated grief together
D) Counseling can be helpful in resolving complicated grief
d. counseling can be helpful in resolving complicated grief
The family of a 4yo client who has a new diagnosis of a terminal illness asks the nurse for the best ways to discuss the illness with the client. Which of the following things should the nurse ensure are considered when discussing a terminal illness with a child?
SATA
A) The parents should not include the child when discussing the client’s illness.
B) Prepare the child before hospital visits
C) Allow the child to ask questions
D) Because of the client’s age, they wouldn’t understand what a terminal illness is
E) Use biological concepts of life cycles
b. prepare the child before hospital visits
c. allow the child to ask questions
e. use biological concepts of life cycles
A nurse is caring for a 6yo male client. Which of the following should the nurse take into account when communicating with this client? SATA
A) They will tend to blame themselves for negative events
B) They can learn self-regulation techniques like meditation
C) They may be curious about their condition and prognosis
D) They are too young to participate in discussions about their care
E) A varied routine and environment will foster optimal cognitive function.
a. they will tend to blame themself for negative events
b. they can learn self regulation techniques like meditation
c. they may be curious about their condition and prognosis
A nurse is assessing a child who has leukemia. Which of the following should the nurse expect to find?
A) Hypothermia
B) Anorexia
C) Petechiae
D) Erythema
E) Unsteady gait
b. hypothermia
c. petechiae
e. unsteady gait