HL Biology Unit 6.7: Reproduction
1/20
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
21 Terms
What causes intersex phenotypes in reproduction?
Minor adjustments in the complex series of genes + hormones that control the development of sex organs
How do male sex organs develop?
The SRY gene on the Y chromosome codes for the Teste Determining Factor (TDF) protein, which causes embryonic gonads to develop into testes.
Testes develop testosterone secreting glands around 8 weeks, increased testosterone in puberty signals development of sperm
How do female sex organs develop?
If the SRY gene is not present, gonads develop into ovaries from maternal estrogen and progesterone. Estrogen and progesterone increase during puberty, signalling development of the menstrual cycle
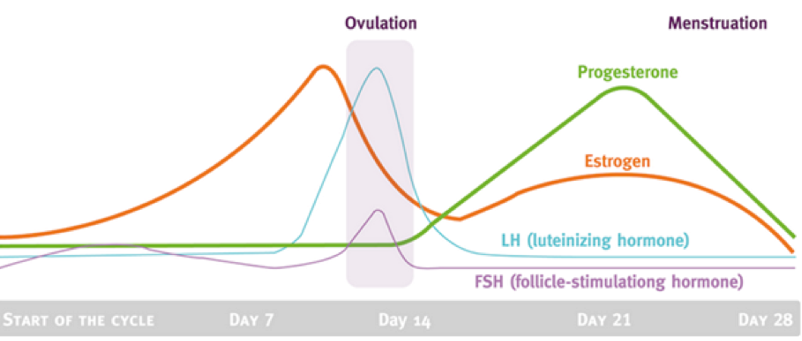
Using a graph, describe the presence of different hormones involved in the menstrual cycle
Estrogen spikes before ovulation
Right before day 14, Luteinizing hormones (LH) and Follicle Stimulating Hormone (FSH) spike, which is where ovulation occurs.
Near day 21, progesterone and estrogen spike
At which point of the menstrual cycle are females most fertile?
During ovulation when an egg is released into the oviduct (~days 10-17)
What are two examples of ovarian hormones? Pituitary hormones?
Ovarian: Estrogen, Progesterone
Pituitary Hormones: LH, FSH
Describe the follicular phase of the menstrual cycle
Occurs the first day right after menstruation
FSH signals estrogen increase → endometrium thickens
FSH present → increased follicle growth → more estrogen is released from follicles
Increased FSH → increased estrogen → increase in LH release
Increased LH → increased follicular wall size → even more estrogen releaseOVULATION: LH spikes, the most developed follicle grows and ruptures, releasing its ovum into the oviduct
When estrogen is highest, it inhibits LH and FSH , allowing progression to the luteal phase
Describe the luteal phase of the menstrual cycle
The endometrium continues to thicken
Ruptured follicle differentiates, becoming a corpus luteum that releases estrogen and progesterone → progesterone maintains the endometrium
New hormones inhibit LH and FSH until the next cycle
If no fertilization, the corpus luteum breaks down → decreased progesterone and estrogen → endometrium breaks down
The endometrium sheds during menstruation
What are characteristics of both spermatogenesis and oogenesis?
Mitosis, cell growth, 2 meiotic divisions, differentiation
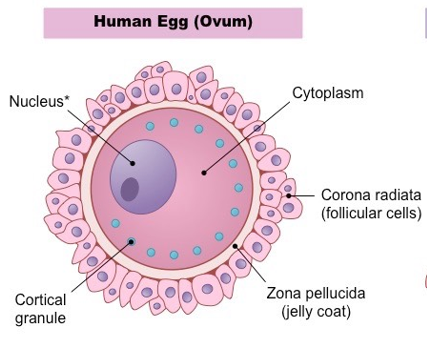
Describe the structure of an ovum
*note, condensed nucleus is not actually present because ovum development stops in metaphase II, only there to represent the presence of haploid genetic material
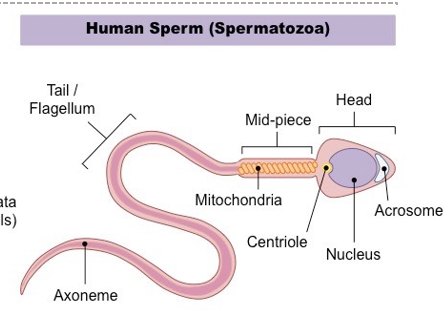
Describe the structure of a spermatozoa
Describe the structure of the seminiferous tubules
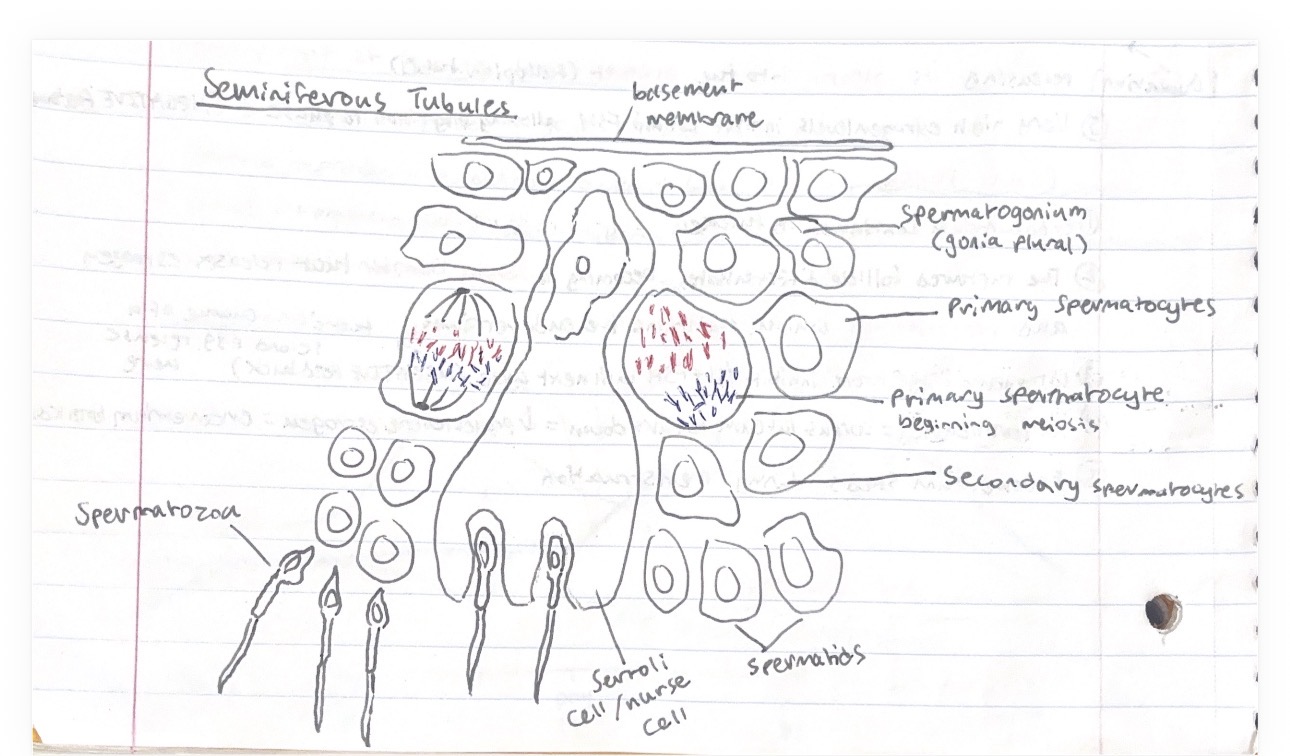
Describe the steps of spermatogenesis
Begins in the outer part of the seminiferous tubules and progresses inwards towards the lumen
Spermatogonia are diploid germinal epithelial cells beneath the basement membrane. These divide by mitosis into either more spermatogonia or primary spermatocytes
Formation of primary spermatocytes begins 1st meiosis, forming 2 haploid secondary spermatocytes
Secondary spermatocytes undergo 2nd meiosis, becoming 4 haploid spermatids
Spermatids are attached to sertoli cells which help them differentiate into mature spermatozoa
Once spermatozoa develop tails, they detach from sertoli cells and get carried down the lumen of the seminiferous tubules towards the epididymis
Describe the steps of oogenesis
Begins in utero by the developing female fetus. Diploid germinal cells in the fetal ovary divide by mitosis into oogonia, which are distributed throughout the ovaries
Oogonia develop into primary oocytes, beginning meiosis but stopping at prophase I. This cell is then surrounded by follicle cells, forming a primary follicle.
During menstrual cycle in puberty, a few follicles become oocytes as the first meiotic division produces 2 haploid cells by uneven cytoplasm division to create a secondary oocyte and a small polar body.
The polar body divides and degenerates, the secondary oocyte is protected by the follicle, starting the second meiotic division and stopping at prophase II. The follicle cells divide and produce a liquid that causes follicles to swell.
The follicle cell bursts during ovulation, releasing the secondary oocyte to the oviduct.
Describe the steps of fertilization
The sperm binds to the jelly coat of the ovum
Enzymes are released from the acrosome of the sperm to break down the jelly coat
The sperm nucleus enters the egg (end of the Acrosome Reaction)
The cortical granules in the ovum contain molecules that harden the zona pellucide, making it impermeable to prevent polyspermy (Cortical reaction)
What occurs in the embryo post-fertilization?
Human gonadotropin (hCG) is produced to continue the release of progesterone and estrogen
What hormone do pregnancy tests look for to confirm pregnancy?
Presence of human gonadotropin
What occurs in the placenta post-fertilization?
Allows the exchange of nutrients between mother and fetus, since maternal and fetal blood don’t mix. ALSO secretes progesterone and estrogen
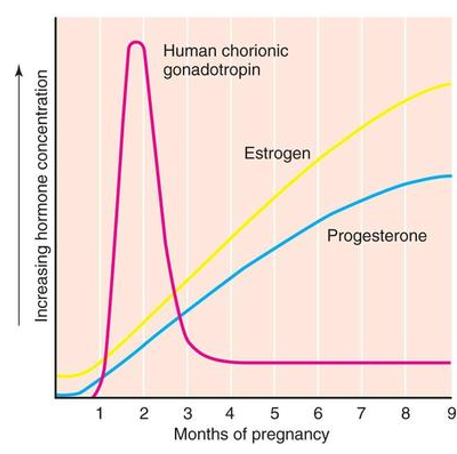
Using a graph, describe the levels of the hormones involved in pregnancy post-fertilization
hCG promotes initial increases of progesterone and estrogen
hCG declines as placenta becomes main secretor of progesterone and estrogen
Describe the positive feedback loop between estrogen and oxytocin during birth
Head of fetus pushes against cervix, transmitting a nerve impulse to the brain that stimulates the pituitary gland to secrete oxytocin
Oxytocin enters the bloodstream and into the uterus
Oxytocin promotes uterine contractions that continues the cycle by pushing the fetus closer to the cervix
What does prolactin do?
A hormone that stimulates milk production
Secreted during and after feed in order to produce the next feed
More is secreted at night
Suppresses ovulation (no more babies right now!)
Suckling promotes prolactin secretion