2
1/66
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
67 Terms
An unpleasant sensory and emotional experience associated with actual or potential tissue damage
Pain
The relatively objective characteristic of pain, including its location, duration and intensity
thermal v Mechanical v Chemical
Sensory Component
The aspects of pain associated with past experiences, fear, suffereing, anxiety and cultural difference
Motivational/Affective components
A drug that is used to decrease the sensation of pain
Analgesic
A drug that is used to abolish all sensation (blocking nociception is the primary goal)
Anesthetic
A drug causing a loss of sensation, whose action is limited to a specific area of the body, depending on which nerve was blocked and what area it innervates
Local anesthetic
An anesthetic agent whose action includes the entire body and all sensations
General anesthetic
Allodynia vs hyperalgesia
Allodynia: Pain caused by a stimulus that is normally innocuous (non-painful)
Hyperalgesia: Exaggerated pain response to a stimulus that is normally painful
sensitization of peripheral nociceptors in an area of tissue damage or due to the presence of algesic chemcials (bradykinin, substance P, etc)
Primary hyperalgesia
Increased pain response in the absence of local causes. Due to changes in the central nervous system (spinal cord and or higher centers) that result in a sensitization of nociceptors (eg referred pain and convergence)
Secondary hyperalgesia
Reffered pain and convergence
Nociceptors innervating deep structures often synapse with the same central neurons as the nociceptors from the superficial structures (they converge on the same neurons in the CNS)
A nociceptor is a peripheral neuron which is specialized to convey noxious (painful stimuli)
____ and ____ fibers
Adelta and C
- mechanical (pinch)
- Chemical (jalapeno peppers)
- Thermal
Anatomy:
Trigeminal nerve
Trigeminal ganglion
Pars oralis
Neurons:
- A-beta mechanoreceptors
- A-delta C
- Schwann cells/myelination
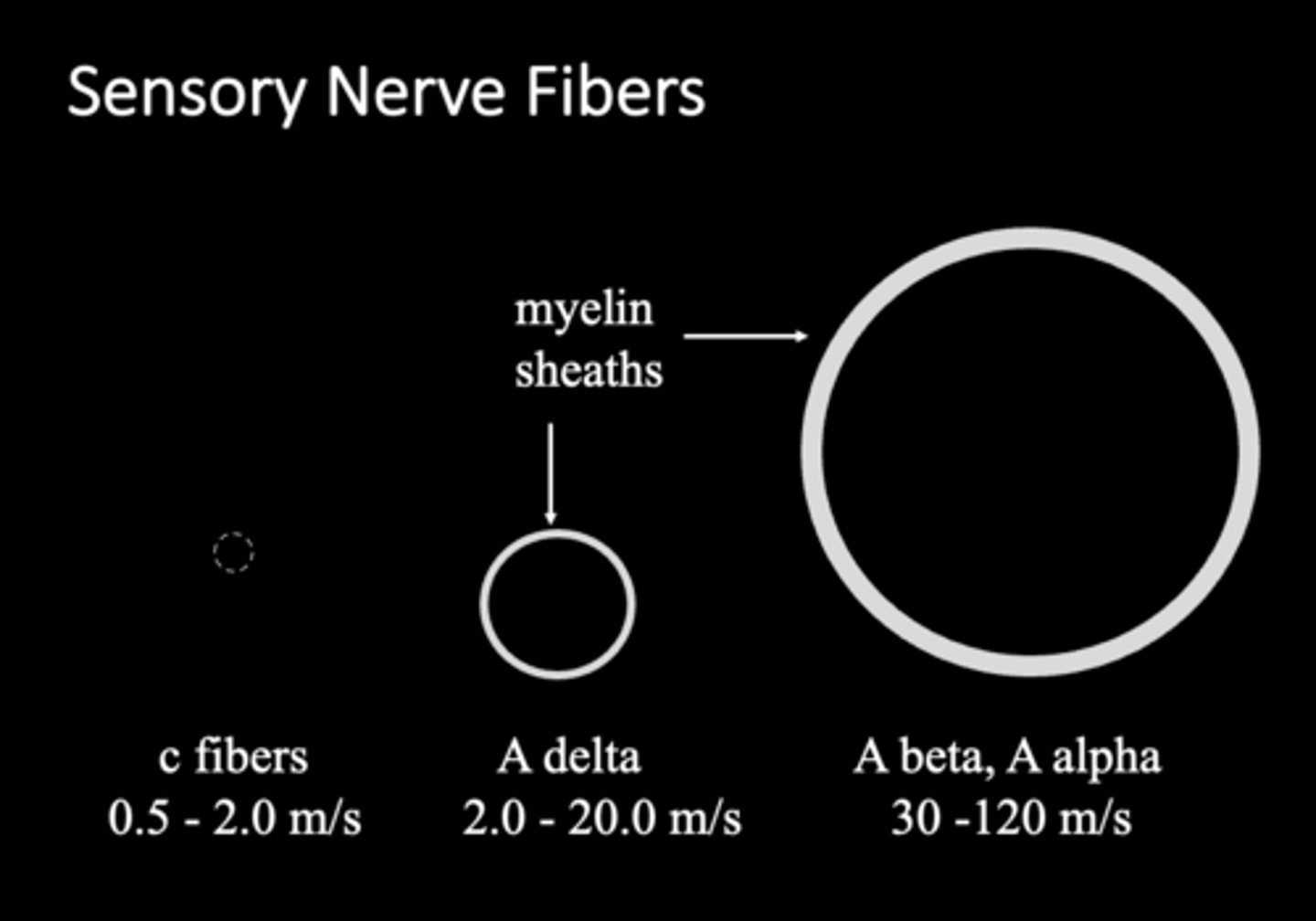
fyi
Impulse conduction
Resting membrane potential
Depolarization
Threshold stimulus
Refractory period
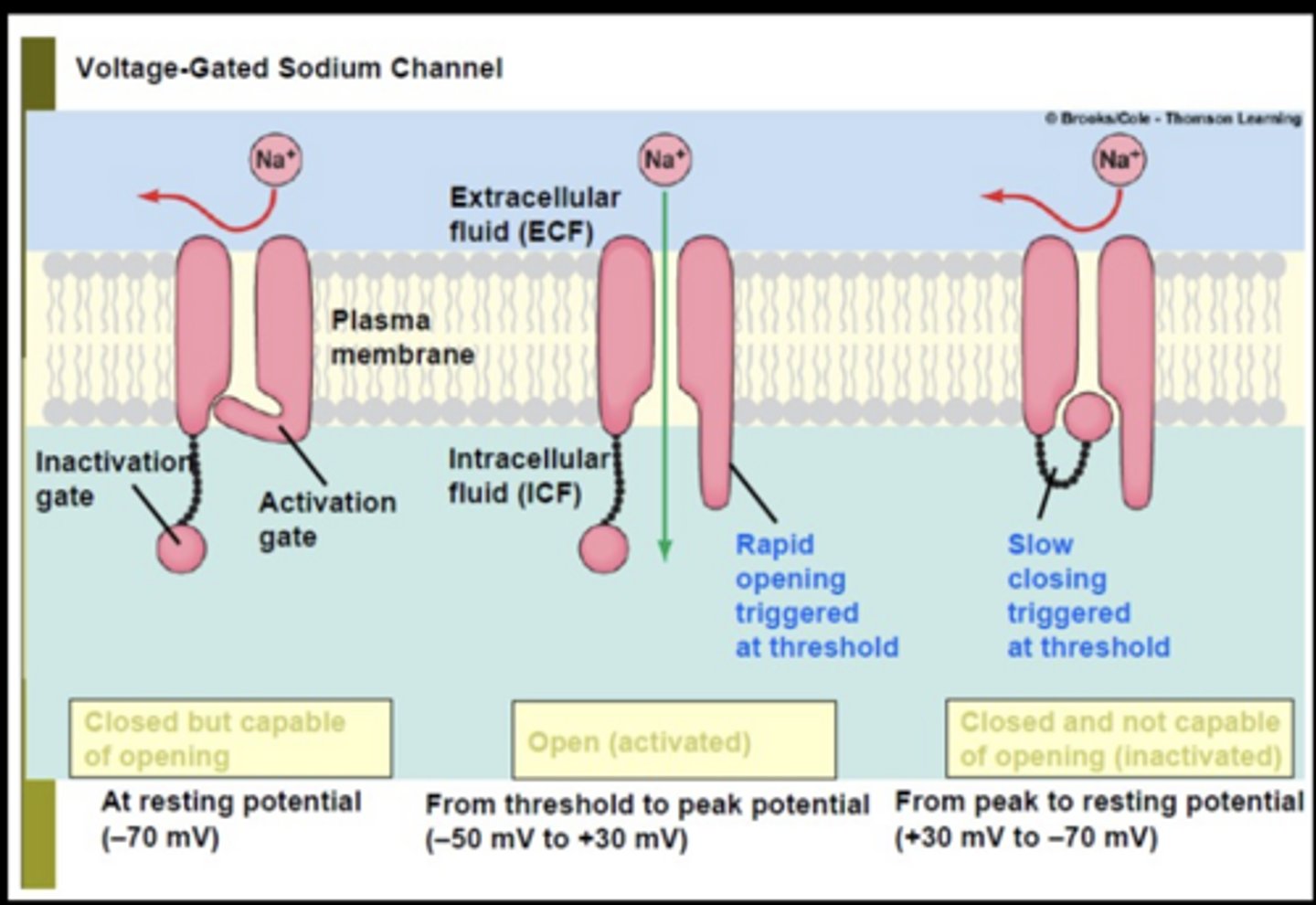
.
Immediately following an action potential, the neuron is unresponsive for a very brief period
absolute refractory period
This is followed by a period of time when a larger-than-normal depolarization is required to initiate a potential
relative refractory period
Two classes of LAs depending on their intermediate chain
Esters and amides
Esters and amides are ___ bases
weak
Equilibrium in solution based on _____ of LA and ____ of solution (H/H equation)
pka
Some LA disrupt the ____ ____
lipid bilayer
Mechanism of Action
Both uncharged and charged forms are required for action
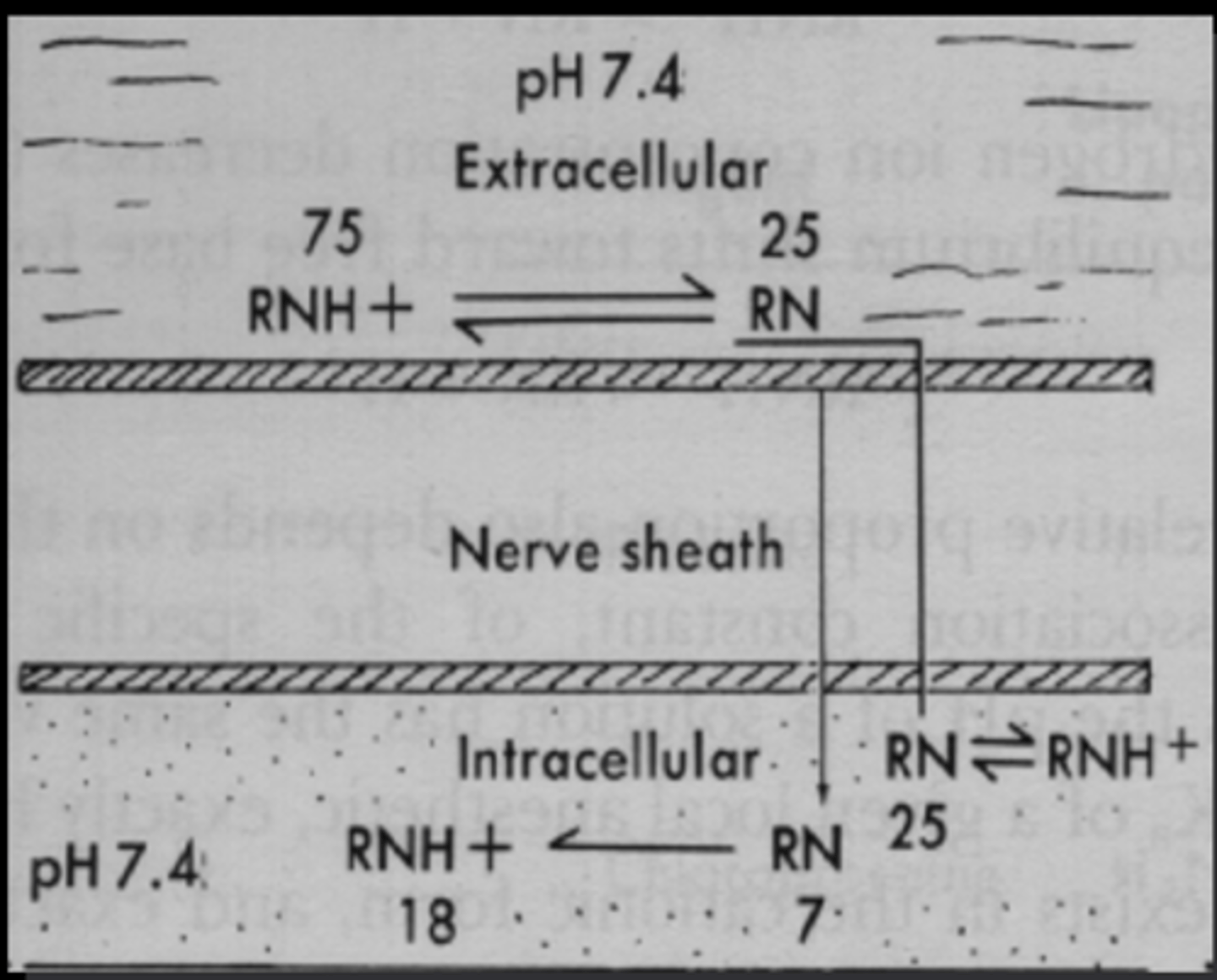
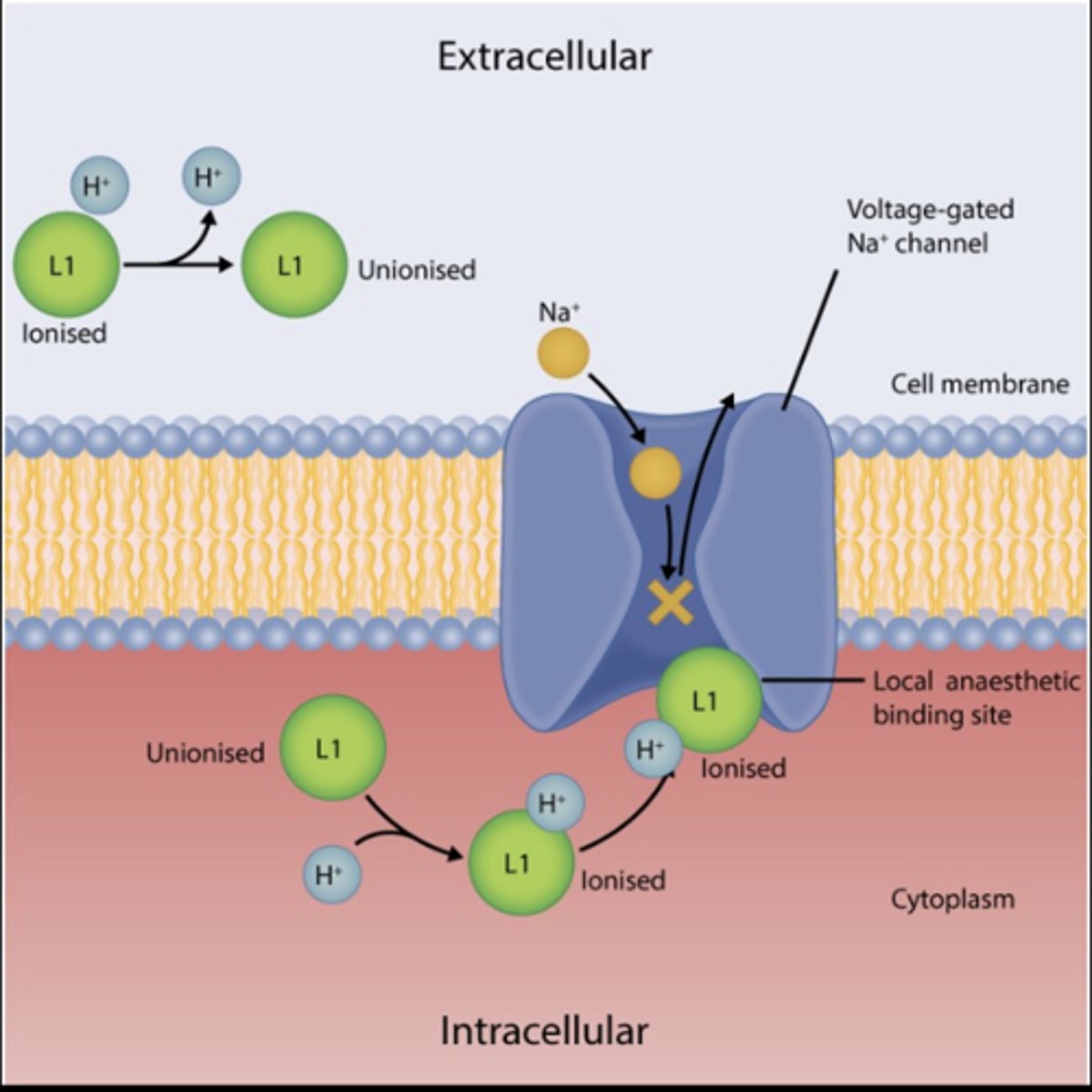
.
Less _______ (RN) LA will exist in an acidic environment
uncharged
When there is an acidic environment, this means that far fewer molecules can enter the axon, so the resulting blockade of AP's (numbness) will be ____ and possibly _____
poor inadequate
This is often a problem when treating areas with infection - inflammed tissue has a lower acidity
lower pka = more ____ onset of the LA
rapid
Faster onset of LA when pKa closest to ______ pH
physiologic (7.4)
More particles become de-ionized to diffuse through nerve sheath at _______ pH
physiological
Increased lipid solubility of the LA leads to increased _____
potency
When the LA has increased lipid solubility it has ____ ability to penetrate lipid membrane of nerves
increased
Pharmacokinetics
Uptake: Some diffusion into surrounding tissue occurs
Distribution: Distributed throughout the body and can pass the BBB and placenta
uptake of LA has some diffusion into ____ ____ occurs
surrounding tissues
diffusion of LA is distributed throughout the____ and can pass the ____ and _____
body
BBB
placenta
Ideal properties of LA
Reversible
Non-irritating
Rapid onset
Sufficient duration
Low systemic toxicity
Non-addicting
Effective at all sites
Stable in solution
History of LA
Cocaine in 1860s - topical and injection
Procaine developed in 1905
lidocaine synthesized in 1943
Articaine in 1969 - approved by FDA in 2000
Uses of LA
Topical anesthesia
Dental procedures
Minor surgical procedures
Spinal anesthesia
Epidural anesthesia
Useful for irregular heart rate
Ester LA are hydrolyzed in plasma by enzyme plasma __________-
pseudocholinesterase
Procaine (ester LA) is broken down into _____
PABA
Atypical pseudocholinesterase
ester LA is excreted into the ____
urine
Amides LA are metabolized in the ___
liver
amides are excreted in the _____-
urine
Methemoglobinemia
Some LAs can trigger methemoglobinemia
- prilocaine, articaine, and benzocaine
Altered state of hemoglobin
- Heme iron oxidized from Fe2+ to Fe 3+
- Ferric heme does not bind O2
- Remaining ferrous hemes in the tetramer have increased O2 affinity
Some LAs can trigger methemoglobinemia
methemoglobinemia
Altered state of hemoglobin
which LA can result in methemoglobinemia
prilocaine, articaine, and benzocaine
what happens in methemoglobinemia
Altered state of hemoglobin
- Heme iron oxidized from Fe2+ to Fe 3+
Ferric heme does not bind O2
Remaining ferrous hemes in the tetramer have increased ___ affinity
O2
Systemic actions of LAs
CNS
CVS
Minimize systemic actions HOW DO WE DO THAT EVEN
- Avoid intravascular injections
- Use vasoconstrictors
- Know and avoid maximum doses
CNS
Initially, ______ signs predominate but CNS ______ is the ultimate outcome
excitatory
depression
CNS side effects of LA
slurred Speech, Muscle tremors and twitches
Numbness, dizziness, drowsiness
The ____ is directly affected by LAs
heart
LA casues _____ electrical excitability, conduction rate, contraction force and eventual circulatory collapse occur with toxic doses
decreased
LAs also directly dilate _____ ______, adding to the hypotension
peripheral vasculature
Systemic toxicity
Avoid intravascular injections by aspirating the syringe
Add vasoconstrictors to slow absorption of LA into bloodstream
Know and avoid the maximum dosage
Avoid intravascular injections by ______ the syringe
aspirating
to avoid toxicity add ______ to slow absorption of LA into bloodstream
vasoconstrictors
Know and avoid the ____ ______
maximum dosage
Ideal properties
Reversible
Non-irritating
Rapid onset
Sufficient duration
Low systemic toxicity
non-addicting
Effective at all sites
Stable in solution
Summary: What is pain
Pain is an unpleasant sensory and emotional experience associated with actual or potential tissue damage. It has both sensory component (location, intensity, duration) and a motivational/affective component influences by emotions, past experiences, and culture
Summary: How does the structure of the nerve fiber contribute to conduction
Nerve fibers differ in diameter and myelination, which affects conduction speed. Larger, myelinated fibers (a-beta, a-delta) conduct impulses much faster than smaller unmyelinated C fibers
Summary: How is the impulse conducted
Impulse conduction occurs through changes in membrane potential, including depolarization once a threshold is reached. This propagates along the neuron as an action potential, followed by a refractory period before another signal can occur
Summary: What Ions are involved and at what points
Na are primarily responsible for depolarization as they enter the neuron through voltage-gated channels. Potassium ions (K) help restore the resting membrane potential during repolarization
Summary: What is the refractory period
The refractory period is the time after an action potential when a neuron cannot or is less likely to fire another impulse
Summary: What is the MOA of LA
Local anesthetics block Na channels in nerve membranes, preventing depolarization and stopping nerve impulse transmission. Both charged and uncharged forms are needed, and effectiveness is reduced in acidic environments
Summary: What are ideal properties for a local anesthetic
An ideal local anesthetic is reversible, non-irritating, and has rapid onset with sufficient duration. It should also have low toxicity, be stable, non-addicting, adn effective at all sites