Chapter 12- Communicable diseases
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
What is a disease?
A condition that impairs the normal functioning of an organism. Both plants and animals can get diseases. These can be communicable (spread between organism) or non-communicable (non infectious)
What is a pathogen?
A pathogen is an organism that causes disease (communicable diseases). Types of pathogen include bacteria, viruses, fungi and protoctista (a type of single-celled eukaryotic organism).
What pathogens cause common diseases in animals?
Pathogen type | Disease | Method of transmission |
|---|---|---|
Bacterium | Tuberculosis | Airborne droplets |
Virus | HIV/AIDS | Body fluids |
Influenza | Airborne droplets | |
Protoctist | Malaria | Female mosquitoes |
Fungus | Athlete's foot | Skin-to-skin contact with an infected individual Contact with an item of clothing |
What pathogens cause common diseases in plants?
Pathogen type | Disease | Plant host | Method of transmission |
|---|---|---|---|
Bacterium | Ring rot | Potato, tomato | An infected tuber can lead to the growth of infected new plants Contaminated soil, water and equipment |
Virus | Tobacco mosaic | Tobacco | Leaf-to-leaf contact between plants Humans touching different plants |
Protoctist | Late blight | Potato, tomato | Spores are carried by wind from plant to plant |
Fungus | Black sigakota | Bananas | Leaf-to-leaf contact Spread of spores by humans or within infected plant matter |
How can pathogens be spread?
by droplet infection
by touching an infected organism
sexual intercourse
via an intermediate (e.g. air,water,food,vector)
How can spores be spread?
By the air and in water
How can malaria be spread?
It is spread via mosquitoes. The mosquitoes act as vectors - they don’t cause the malaria themselves, they just spread the protist that causes it. The mosquitoes feed on blood and pass the protists into the hosts bloodstream.
What factors can affect disease transmission?
living conditions
climate
social factors
How can living conditions affect the spread of pathogens?
Overcrowded living conditions increase the transmission of many communicable diseases.
E.g. TB is spread from one person to another via droplet infection. The bacteria can also remain in the air for long periods of time and infect new people, so the air acts as an intermediate for TB transmission. The risk of TB infection is increased when lots of people live crowded together in a small space.
How can climate affect the spread of pathogens?
Late blight is especially common in wet summers as the spores need water to spread
Malaria is most common in tropical countries which are humid and hot as there are the ideal conditions for mosquitoes
How can social factors affect the spread of pathogens?
In poorer areas diseases can often be spread more easily due to:
lack of good healthcare
lack of good health education
overcrowding in living areas
poor living conditions
What physical defences do plants have against pathogens?
a waxy cuticle - provides a physical barrier against pathogen entry and may also stop water collecting on the leaf, which could reduce the risk of infection by pathogens that are transferred between plants in water
Cell walls - physical barrier against pathogens that make it past the waxy cuticle
Bark
Casparian strip
What role does callose play in plant defences against pathogens?
Plants produce a polysaccharide called callose which gets deposited between plant cell walls and plasma membranes (sometimes with lignin) during times of stress. This makes it harder for pathogens to enter the cells. Callose deposition at the plasmodesmata can limit the spread of pathogens across cells
What chemical defences do plants have against pathogens?
Plants can produce antimicrobial chemicals (such as antibiotics)
e.g.
Some plants produce chemicals called saponins. These are thought to destroy the cell membranes of fungi and other pathogens.
Plants also produce chemicals called phytoalexins, which inhibit the growth of fungi and other pathogens.
Plants can also produce chemicals that are toxic to insects
What non-specific defences do animals have against pathogens?
skin - a physical barrier blocking pathogens from entering the body. Also acting as a chemical barrier by producing chemicals that are antimicrobial and can lower pH, inhibiting the growth of pathogens.
mucous membranes - line the gut, airways and reproductive system. Consists of epithelial cells and mucus-secreting cells like goblet cells. Mucous traps pathogens and contains antimicrobial enzymes
inflammation - It can be triggered by tissue damage (the damaged tissue releases molecules, which increase the permeability of the blood vessels, so they start to leak fluid into the surrounding area). This causes swelling and helps to isolate any pathogens that may have entered the damaged tissue. The molecules also cause vasodilation (widening of the blood vessels), which increases blood flow to the affected area. This makes the area hot and brings white blood cells to the area to fight off any pathogens that may be present.
Wound repair — the skin is able to repair itself in the event of injury and re-form a barrier against pathogen entry. The surface is repaired by the outer layer of skin cells dividing and migrating to the edges of the wound. The tissue below the wound then contracts to bring the edges of the wound closer together. It is repaired using collagen fibres
Expulsive reflexes — e.g. coughing and sneezing. A sneeze happens when the mucous membranes in the nostrils are irritated by things such as dust or dirt. A cough stems from irritation in the respiratory tract. Both coughing and sneezing are an attempt to expel foreign objects, including pathogens, from the body. They happen automatically.
blood clotting - when platelets are exposed to damaged blood vessels they release substances the result in the formation of fibrin via a cascade of events . Fibrin meshes together to form a network the traps platelets and forms a blood clot. Blood clots plug wound to prevent pathogen entery and blood loss
What are phagocytes? (and what are the types?)
Phagocytes are white blood cells that are produced continuously in the bone marrow. There are three main types of phagocyte, each with a specific mode of action. The three types are:
Neutrophils
Macrophages
Dendritic cells
What are neutrophils and what do they do?
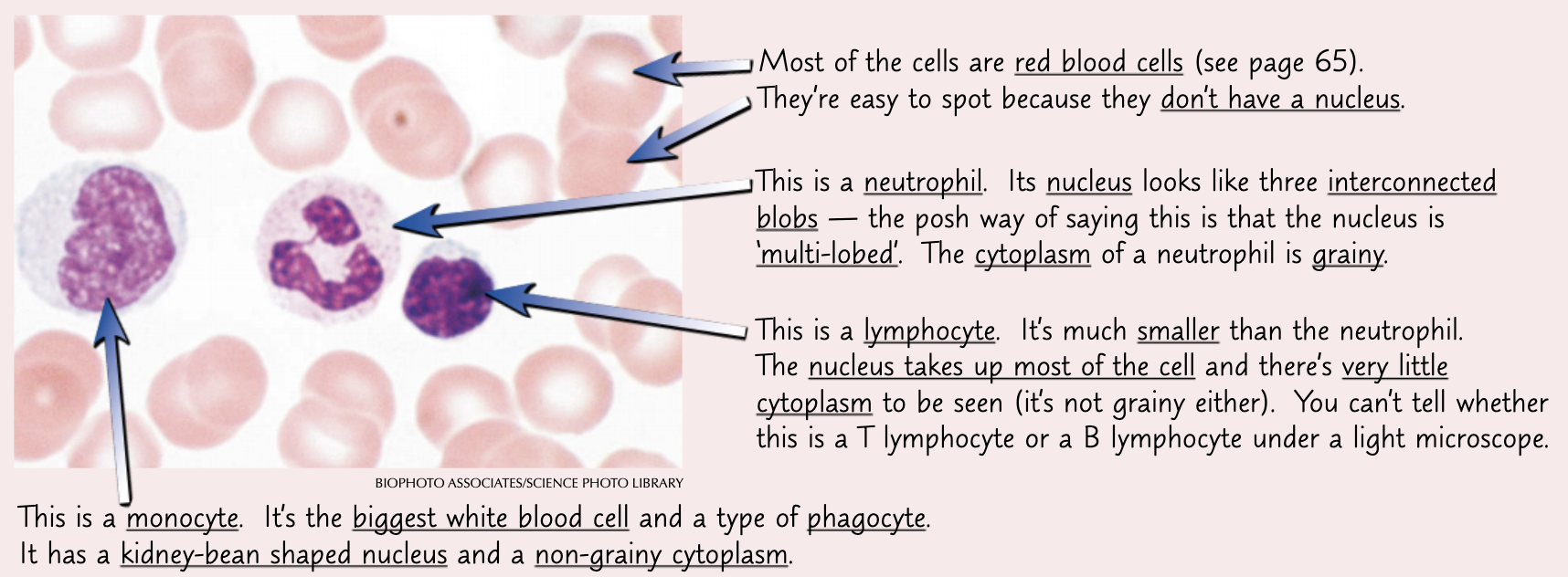
They are a type of phagocyte and they can carry out phagocytosis. They have a lobed nucleus and this allows for them to be identified in blood smears.
Neutrophils have receptor proteins on their surfaces that recognise antibody molecules and attach to them
Once attached to a pathogen the cell surface membrane of a neutrophil extends out and around the pathogen, engulfing it and trapping the pathogen within a phagocytic vacuole
The neutrophil then secretes digestive enzymes into the vacuole.The enzymes are released from lysosomes which fuse with the phagocytic vacuole
These digestive enzymes destroy the pathogen
After killing and digesting the pathogens, the neutrophils die
What is an antigen?
Molecules found on the surface of cells that lymphocytes (a type of white blood cell) can recognise as foreign. Different types of lymphocytes work together to co-ordinate the response against that pathogen.
What are the main stages in the immune response?
phagocytes engulf pathogens
phagocytes activate T-lymphocytes
T-lymphocytes activate B-lymphocytes
Plasma cells make more antibodies to a specific antigen
What happens in the first stage of the immune response?
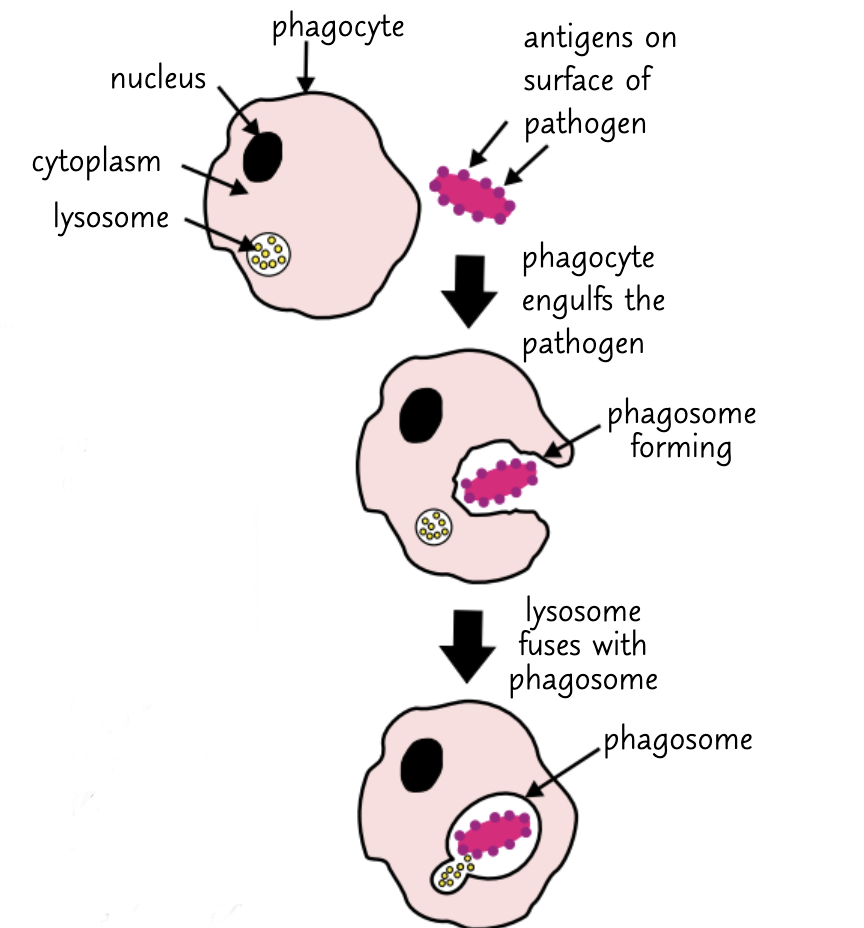
1) A phagocyte (usually a macrophage) recognises the antigens on a pathogen.
2) The membrane and cytoplasm of the phagocyte move round the pathogen, engulfing it. This may be made easier by the presence of opsonins
3) The pathogen is now contained in a phagosome (a type of vesicle) in the cytoplasm of the phagocyte.
4) A lysosome (an organelle that contains digestive enzymes) fuses with the phagosome. The enzymes break down the pathogen.
5) The phagocyte then presents the pathogen's antigens. It sticks the antigens on its surface to activate other immune system cells. When a phagocyte does this it is acting as an antigen-presenting cell.
What is an opsonin?
A type of antibody that attaches to the antigens. They help the phagocyte to bind with and engulf the pathogen. Opsonins work in different ways. Some hide the negative charges on the membrane of the pathogen, making it easier for the negatively-charged phagocyte to get closer to the pathogen.
What happens in stage 2 of the immune response
A T lymphocyte is another type of white blood cell.
Their surface is covered with receptors.
The receptors bind to antigens presented by APCs.
Each T lymphocyte has a different receptor on its surface.
When the receptor on the surface of a T lymphocyte meets a complementary antigen, it binds to it — so each T lymphocyte will bind to a different antigen.
This activates the T lymphocyte — the process is called clonal selection.
The T lymphocyte then undergoes clonal expansion - it divides to produce clones of itself.
The clones of that T cell produces interleukins = a type of cytokine which stimulate more T helper cells to divide.
What happens in stage 3 of the immune response?
1) B lymphocytes are another type of white blood cell. They're covered with proteins called antibodies. Each B lymphocyte has a different shaped antibody on its surface.
3) Antibodies bind to antigens to form an antigen-antibody complex.
4) When the antibody on the surface of a B lymphocyte meets a complementary shaped antigen, it binds to it — so each B lymphocyte will bind to a different antigen.
5) This, together with substances released from T helper cells, activates the B lymphocyte. This process is another example of clonal selection.
6) The activated B lymphocyte divides, by mitosis, into plasma cells and memory cells (this is another example of clonal expansion)
What happens in stage 4 of the immune response?
Plasma cells are clones of the B lymphocyte (they're identical to the B lymphocyte).
They secrete loads of the antibody, specific to the antigen, into the blood.
These antibodies will bind to the antigens on the surface of the pathogen to form lots of antigen-antibody complexes
What are lymphocytes?
Lymphocytes are a type of white blood cell that aer smaller than phagocytes. They ave a large nucleus that fills most of the cell. They are produced in the bone marrow before birth and they travel around the body in the blood.
There are two types of lymphocytes (with different modes of action)
T-lymphocytes (T cells)
Lymphocytes that mature in the thymus gland
B-lymphocytes (B cells)
Lymphocytes that mature in the bone marrow
What are the main types of T lymphocytes?
T helper cells - Have receptors which bind to antigens on antigen presenting cells and release interleukins which can activate B lymphocytes
T regulator cells - Regulates the immune response by suppressing the other T cells and maintaining a tolerance to self-antigens
T killer cells - attach to the foreign antigens on the cell membranes of infected cells and secrete toxic substances that kill the infected body cells, along with the pathogen inside They secrete perforin which punches a hole in the cell surface membrane of infected cells, allowing toxins to enter
T memory cells- remain in the blood, meaning that if the same antigen is encountered again the process of clonal selection will occur much more quickly
What are the main types of B lymphocytes?
B effector cells - divide to form plasma cells
B memory cells
What are antibodies?
Structure:
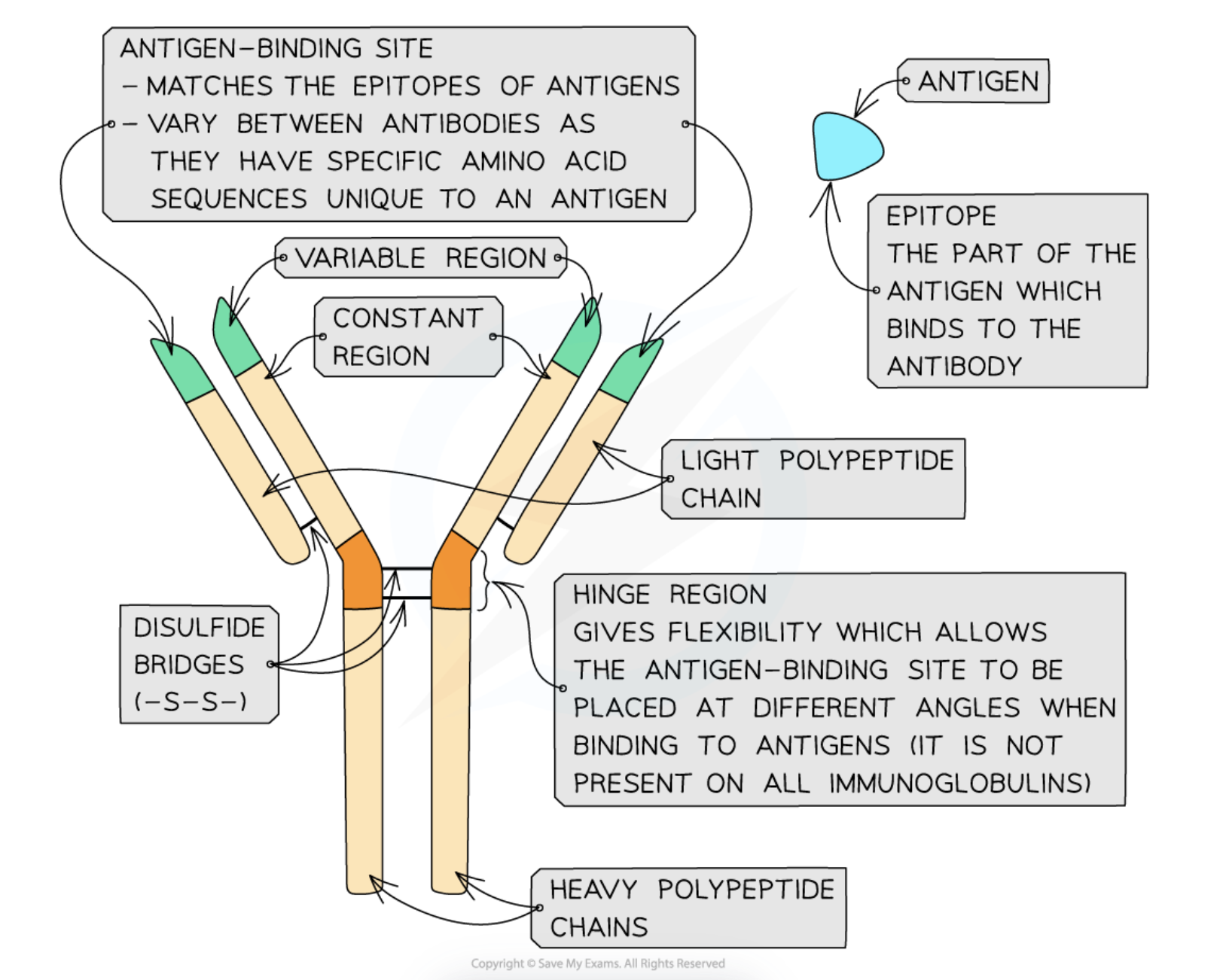
Antibodies are glycoproteins made of four polypeptide chains — two heavy chains and two light chains. Each chain has a variable region and a constant region.
The variable regions of the antibody form the antigen binding sites. The shape of the variable region is complementary to a particular antigen. The variable regions differ between antibodies.
The hinge region allows flexibility when the antibody binds to the antigen.
The constant regions allow binding to receptors on immune system cells, e.g. phagocytes. The constant region is the same (i.e. it has the same sequence of amino acids) in all antibodies.
Disulfide bridges (a type of bond) hold the polypeptide chains of the protein together.
Function:
Antibodies are produced by B-lymphocytes
Antibodies bind to specific antigens that trigger the specific immune response. Every antigen has one antibody
Antigens include pathogens and their toxins, pollen, blood cell surface molecules and the surface proteins found on transplanted tissues
The function of antibodies is to destroy pathogens within the body either directly, or by recruiting other immune cells
Antibodies can act as anti-toxins, opsonins and agglutinins
How can antibodies help to clear infection?
Agglutinating pathogens — each antibody has two binding sites, so an antibody can bind to two pathogens at the same time and the pathogens become clumped together. Phagocytes then bind to the antibodies and phagocytose a lot of pathogens all at once. Antibodies that behave in this way are known as agglutinins.
Neutralising toxins — like antigens, toxins have different shapes. Antibodies called anti-toxins can bind to the toxins produced by pathogens.This prevents the toxins from affecting human cells, so the toxins are neutralised (inactivated). The toxin-antibody complexes are also phagocytosed.
Preventing the pathogen binding to human cells — when antibodies bind to the antigens on pathogens, they may block the cell surface receptors that the pathogens need to bind to the host cells. This means the pathogen can't attach to or infect the host cells.
Opsonisation - Antibodies can attach to bacteria making them readily identifiable to phagocytes, this is called opsonisation. Once identified, the phagocyte has receptor proteins for the heavy polypeptide chains of the antibodies, which enables phagocytosis to occur
What is the cell mediated immune response?
Specialised T-cells target and destroy infected or abnormal cells. Targets intracellular pathogens
What is the humoral immune response?
B-cells produce antibodies that circulate the body in bodily fluids and attack and neutralise the extracellular pathogen?
Is the primary or the secondary immune response faster?
The secondary response is faster due to memory cells
What is the primary immune response?
responding to a newly encountered antigen
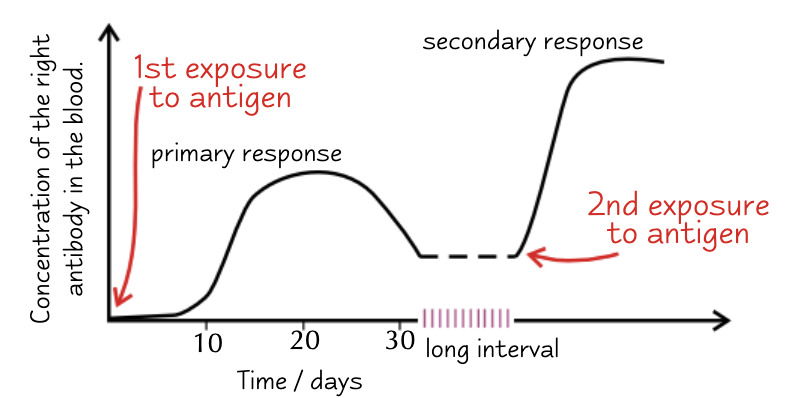
When a pathogen enters the body for the first time, the antigens on its surface activate the immune system. This is called the primary response.
The primary response is slow because there aren't many B lymphocytes that can make the antibody needed to bind to it.
Eventually the body will produce enough of the right antibody to overcome the infection. Meanwhile the infected person will show symptoms of the disease.
After being exposed to an antigen, both T and B lymphocytes produce memory cells. These memory cells remain in the body for a long time.
Memory T lymphocytes remember the specific antigen and will recognise it a second time round. Memory B lymphocytes record the specific antibodies needed to bind to the antigen.
The person is now immune - their immune system has the ability to respond quickly to a second infection.
Why is the secondary response faster?
If the same pathogen enters the body again, the immune system will produce a quicker, stronger immune response — the secondary response.
Clonal selection happens faster. Memory B lymphocytes are activated and divide into plasma cells that produce the right antibody to the antigen. Memory T lymphocytes are activated and divide into the correct type of T lymphocytes to kill the cell carrying the antigen.
The secondary response often gets rid of the pathogen before you begin to show any symptoms.
What is a blood smear?
A sample of blood smeared onto a microscope slide.
What are the different types of immunity?
active- When your immune system makes its own antibodies after being stimulated by an antigen
passive- You get this from being given antibodies made by a different organism
natural
artificial
What is passive natural immunity?
This is when a baby becomes immune due to the antibodies it receives from its mother, through the placenta and in breast milk.
What is natural active immunity?
When you become immune after catching a disease. E.g. if you have measles as a child, you shouldn't be able to catch it again in later life.
What is artificial active immunity?
This is when you become immune after you've been given a vaccination containing a harmless dose of antigen
What is artificial passive immunity?
When you become immune after being injected with antibodies from someone else. E.g. If you contract tetanus you can be injected with antibodies against the tetanus toxin, collected from blood donations.
Compare active and passive immunity
Feature | Active | Passive |
Production of antibodies | Are produced by the body | Not produced by the body |
Time before antibodies appear in blood Long term or short term protection | 1-2 weeks Long term | immediate Short term |
Presence of memory cells | yes | no |
Induced by: | ||
Natural | Exposure to pathogen | Antibodies received from another organism (e.g. via the placenta or colostrum / breast milk) |
Artificial | Vaccination | Antibodies manufactured and injected or transfused into organism (e.g. monoclonal antibodies delivered by blood transfusion) |
What is an autoimmune disease?
An abnormal immune response of your immune system to your body’s own cells. For example, rheumatoid arthritis is an autoimmune disease that solely affects the joints, symptoms include muscle spasms, inflamed tendons, lethargy and constant joint pain. This happens when an organism's immune system isn't able to recognise self-antigens. When this happens, the immune system treats the self-antigens as foreign antigens and launches an immune response against the organism's own tissues. Autoimmune diseases are usually chronic and can be treated but not cured.
What is a vaccination and how do they work?
The process of administering dead or inactive pathogen/antigens. This stimulates an immune response allowing memory cells to form so the individual can form an immunity without getting the illness. Vaccination is not the same as immunisation but it causes immunisation. They can help to prevent epidemics and outbreaks and this can help to reduce pressure on healthcare services.
What are some examples of routine vaccinations?
Routine vaccinations are offered to everybody to maintain herd immunity. Examples include:
The MMR - protects against measles, mumps and rubella. The MMR is usually given to children as an injection at around a year old, and again before they start school. It contains attenuated measles, mumps and rubella viruses.
The Meningitis C vaccine - protects against the bacteria that cause Meningitis C. It is first given as an injection to babies at 3 months. Boosters are then given to 1-year-olds and teenagers.
What is herd immunity?
Herd immunity arises when a sufficiently large proportion of the population has been vaccinated (and are therefore immune) which makes it difficult for a pathogen to spread within that population
Those who are not immunised are protected and unlikely to contract it as the levels of the disease are so low
It is very important as it allows for the individuals who are unable to be vaccinated (e.g. children and those with weak immune systems) to be protected from the disease
What is ring immunity?
People living or working near a vulnerable (or infected) person are vaccinated in order to prevent them from catching and transmitting the disease
The vaccinated individuals do not spread the pathogen onto others so those vulnerable individuals "within the ring" are protected as the people they interact with will not have the disease
Why are changes made to vaccines and global vaccination programs?
Because viruses can mutate and change often (e.g. the antigens on the influenza virus change regularly forming new strains that memory cells can’t recognise)
What are used as natural sources of medicine?
Microorganisms and plants
penicillin comes from a fungus
aspirin comes from willow bark
Digoxin comes from foxgloves
Rifamycins have been discovered in marine actinobacteria. These compounds kill bacteria by inhibiting bacterial transcription
This means that it is very important to protect biodiversity as there may be many other drugs out there with species which may die out before we get the chance to study them.
Discuss the potential for personalised medicine?
Your genes determine how your body responds to certain drugs. Different people respond to the same drug in different ways — which makes certain drugs more effective for some people than others.
Personalised medicines are medicines that are tailored to an individual's DNA. The idea is that if doctors have your genetic information, they can use it to predict how you will respond to different drugs and only prescribe the ones that will be most effective for you.
Scientists hope that by studying the relationship between someone's genetic make-up and their responsiveness to drugs, more effective drugs can be produced in the future.
What are antibiotics?
Chemicals that kill or inhibit the growth of bacteria. They are useful as they can usually target bacteria without harming body cells. Broad-spectrum antibiotics act on a wide range of bacteria while narrow-spectrum antibiotics act on a very small number of bacteria
What was the first antibiotic discovered?
The first antibiotic discovered was penicillin. It was discovered in 1928 by Alexander Flemming. Antibiotic use became widespread from the mid-twentieth century — partly thanks to the successful treatment of soldiers with penicillin in the Second World War. For the past few decades, we've been able to deal with bacterial infections pretty easily using antibiotics. As a result of this, the death rate from infectious bacterial disease has fallen dramatically.
What are some of the issues with antibiotics?
side effects
severe allergic reactions
antibiotic resistance
How can bacteria become resistant to antibiotics?
This is becoming far more common and is very dangerous
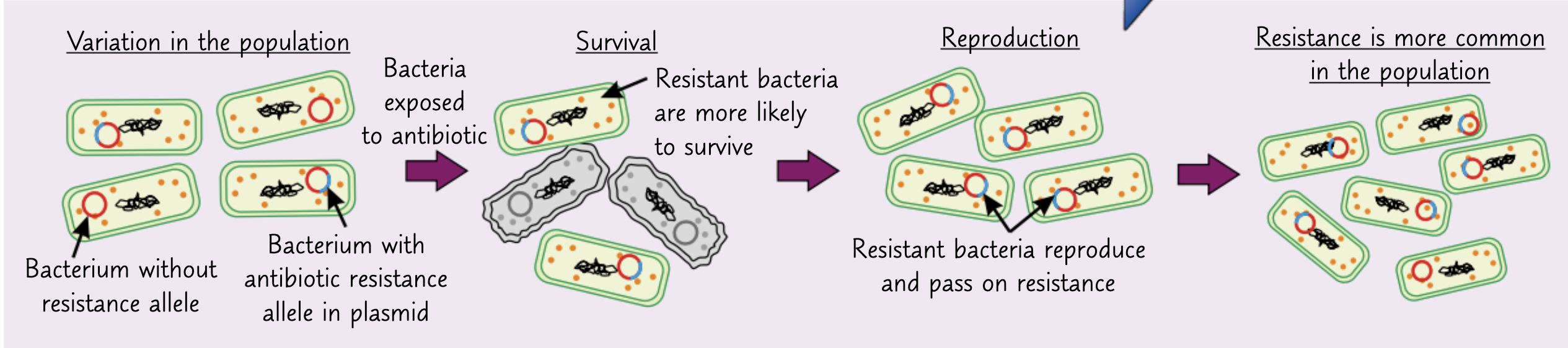
What are the implications of antibiotic resistance?
It is very hard to get rid if ‘superbugs’ which are resistant to most common antibiotics. This is very harmful to people who catch these illnesses and also can put lots of pressure on healthcare systems.
How can the implications of antibiotic resistance be reduced?
Developing new antibiotics and modifying existing ones are two ways of overcoming the current problem of antibiotic resistance. This isn't easy though.
To reduce the likelihood of antibiotic resistance developing in the first place, doctors are being encouraged to reduce their use of antibiotics
Patients are advised to take all of the antibiotics they're prescribed to make sure the infection is fully cleared and all the bacteria have been killed (which reduces the likelihood of a population of antibiotic-resistant bacteria developing).