Intro. to Pharmacology
1/144
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
145 Terms
What are the 3 ways in which drugs can be classified?
chemical name, generic name, trade name
What is the chemical name of a drug?
the drug’s chemical composition (chemical make-up)
What is the generic name of a drug?
the drug’s short and simple name which lists the drug
What is the trade name of a drug?
the drug’s registered trademark
Is the trade name more simple than the generic name of a drug?
Yes
Define “therapeutic equivalence”
Drugs that are proven to have the same therapeutic effect on the body
What are the 3 phases of pharmacology?
pharmaceutics, pharmacokinetics, pharmacodynamics
What is pharmaceutics?
Dosage form and drug’s effect on the body
What is pharmacokinetics?
What body does to drug
What is pharmacodynamics?
What drug does to body
Define “drug dissolution”
Dissolving of solid dosage forms and their absorption from GI fluids
What determines the rate at which drug dissolution occurs?
Dosage form
Are oral liquids dissolved and absorbed more quickly than solids?
Yes
What kind of tablets result in slower dissolution and slower absorption?
Enteric-coated tablets
Do combination dosage forms contain multiple drugs in one dose?
Yes
What do oral dosage forms rely on to work?
gastric and intestinal and pH environments to break down the medication, which is then transported to site of action by blood or lymph
In terms of fastest to slowest dissolution and absorption rates, list all 7 oral dosage forms
liquids, suspension solutions, powders, capsules, tablets, coated tablets, enteric-coated tablets
What are topical drugs?
drugs act immediately, passing through skin barrier to site of action via circulation
Do parenteral dosage forms have a 100% absorption rate?
Yes, as long as the pH of injections is similar to that of blood
Define “parent drug”
The chemical form of a drug that is administered before it is metabolized into active or inactive metabolites
What are the 4 phases of pharmacokinetics?
Absorption, distribution, metabolism, excretion
What does “absorption” mean?
Site of administration to bloodstream
Define “bioavailability”
Extent of drug absorption
Does a drug absorbed from the intestine first pass through the liver before it reaches circulation?
Yes
TRUE or FALSE: If a large proportion of a drug is chemically changed into inactive metabolites in the liver, then a much smaller amount will be bioavailable
True
Define “first-pass effect”
The initial metabolism in the liver of a drug absorbed from the GI tract before the drug reaches blood circulation
When does a drug have a high first-pass effect?
When a large proportion of a drug is chemically changed into inactive metabolites in the liver, and so, a much smaller amount will be bioavailable
TRUE or FALSE? When the bioavailability of a drug is decreased, the first-pass effect of the drug is increased. When the first-pass effect of a drug is increased, the bioavailability of the drug is decreased.
True
First-pass effect reduces the bioavailability of oral drugs to…
less than 100%
Are drugs administered by the intravenous route 100% bioavailable? Why?
Yes, because 100% of the drug reaches the systemic circulation
Define “bioequivalent drugs”
Two medications that have the same bioavailability and same concentration of active ingredient
TRUE or FALSE: Parenteral dosages of drugs with a high first-pass effect are much smaller than enterally (orally) administered doses
True
TRUE or FALSE: The presence of food may enhance the absorption of some fat-soluble drugs that are more easily broken down in an acidic environment
True
TRUE or FALSE: Sublingual route = under the tongue
True
TRUE or FALSE: Buccal route = the oral mucosa between the gum and the cheek
True
Why are drugs administered by the sublingual and buccal route able to bypass the liver, becoming highly bioavailable?
They are absorbed rapidly into the tissue under the tongue with a large blood supply (the oral mucosa)
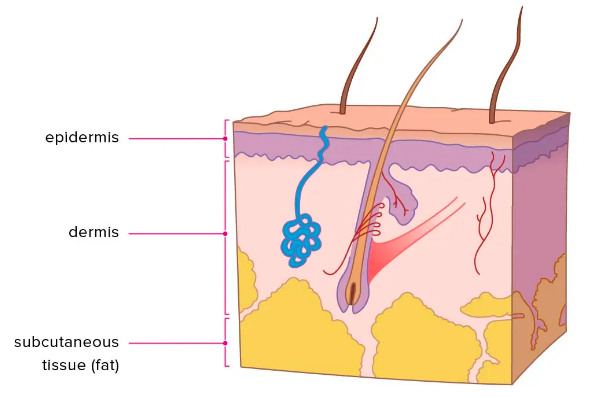
Define “subcutaneous injections”
Injections into the fatty subcutaneous tissues under the dermal layer of the skin
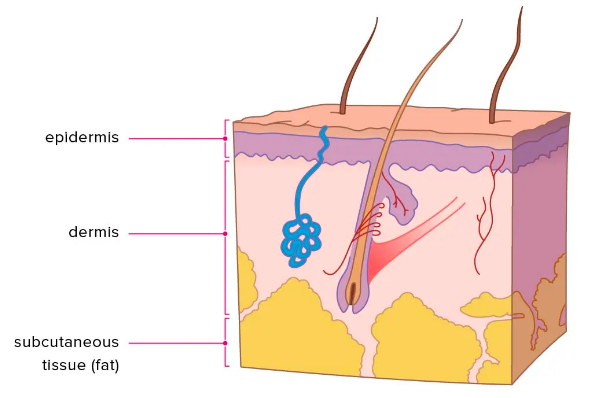
Define “intradermal injections”
Injections under the more superficial skin layers immediately underneath the epidermal layer of skin and into the dermal layer
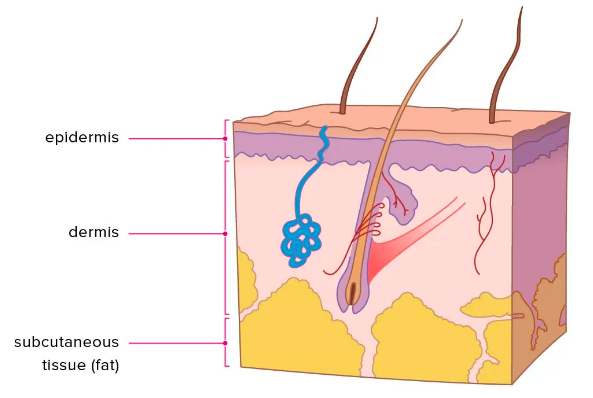
Define “intramuscular injections”
Injections given into the muscle beneath the subcutaneous fatty tissue
Why are drugs injected intramuscularly absorbed faster than drugs injected subcutaneously?
Muscles have a greater blood supply than the skin does
TRUE or FALSE: Topical application delivers a drug over a longer period of time, but the effects of the drug are usually slower in their onset and more prolonged in their duration of action
True
TRUE or FALSE: All topical routes of drug administration avoid first-pass effects of the liver, EXCEPT for rectal drug administration
True
Define “transdermal drug delivery”
delivery of a drug through drug patches, and an elaborate topical route of drug administration
Is inhalation another type of topical administration?
Yes
What does “distribution” mean?
The transport of a drug by the bloodstream to its site of action
Where are drugs first distributed to?
areas with extensive blood supply
TRUE or FALSE: Once a drug enters the circulating blood, it is distributed throughout the body. At this point, it is also starting to be eliminated by the liver and kidneys that metabolize and excrete drugs
True
Which drug molecules can freely distribute to extravascular tissue to reach their site of action?
Only drug molecules that are not bound to plasma proteins, such as Albumin
What is Albumin?
the most common blood protein and carries the majority of protein-bound (inactive) drug molecules
Define “drug-drug interaction”
Occurs when the presence of one drug decreases or increases the action of another drug administered concurrently
How does a drug-drug interaction work?
Two medications that are highly protein bound may compete for binding sites on the albumin protein, resulting in more free, unbound drug
What is Metabolism also called?
Biotransformation
What does “metabolism” mean?
The biochemical alteration of a drug into becoming active or inactive
What is the organ most responsible for the biotransformation/metabolism or drugs?
The Liver
Define “enzyme inhibitors”
Drugs that can inhibit (put a stop to) drug-metabolizing enzymes
TRUE or FALSE: Decreases or delays in drug metabolism result in the accumulation of the drug and prolongation of the effects of the drug, which can lead to drug toxicity
True
Define “enzyme inducers”
Drugs that can stimulate drug metabolism and cause decreased pharmacological effects
What does “excretion” mean?
The elimination of drugs from the body
All drugs must eventually be removed from the body. The primary organ responsible for this elimination is the…
Kidney
TRUE or FALSE: By the time most drugs reach the kidneys, they have undergone biotransformation, where it is converted to a less active form and only a small fraction of the original drug is excreted as the original compound
True
Drugs that have been metabolized by the liver become more…? Which makes their elimination easier because…?
polar and water-soluble. This makes their elimination by the kidney much easier because the urinary tract is water-based
Define “half-life”
The half-life of a drug is the time required for drug levels to be reduced by 50% during the elimination phase
After how many half-lives are most drugs removed from the body?
about 5 half-lives
At the time most drugs are removed from the body, what percentage of the drug has been eliminated?
97%
Why is the concept of half-life useful?
for determining when a steady state will be reached in a patient taking a drug
Define “steady state”
The physiological state in which the amount of drug removed via elimination is equal to the amount of drug absorbed with each dose
When does steady state typically occur?
after 4-5 half-lives of administration of a drug
TRUE or FALSE: if a drug has an extremely long half-life, it will take much longer for the drug to reach steady-state blood levels
True
TRUE or FALSE: Once steady-state blood levels have been reached, there are consistent levels of drug in the body that correlate with maximum therapeutic benefits
True
Define “drug actions”
The processes involved in the interaction between a drug and a cell
Define “drug effects”
The physiological reactions of the body to a drug
Can drug effects be toxic or therapeutic?
Both
Define “onset of action”
The time required for a drug to elicit a therapeutic response
Define “peak effect”
The time required for a drug to reach its maximal therapeutic response
Define “duration of action”
The length of time that a drug’s concentration is sufficient (without more doses) to elicit a therapeutic response
Define “peak level”
The maximum concentration of a drug in the body after administration
If the peak blood level is too high, can drug toxicity occur?
Yes
Define “trough level”
The lowest concentration of a drug reached in the body after it falls from its peak level
If the trough blood level is too low, will the drug be at therapeutic levels to produce a response?
No
Define “therapeutic drug monitoring”
The measuring of peak (highest) and trough (lowest) values in order to verify adequate drug exposure, maximize therapeutic effects, and minimize drug toxicity
Define “therapeutic effect”
A positive change in a faulty physiological system that is caused by a drug’s effects
What is the goal of drug therapy?
To reach the therapeutic effect of a drug
What do the effects of a drug depend on?
The cells or tissue targeted by the drug
TRUE or FALSE: Once the drug is at the site of action, it can increase/decrease the strength of that cell/tissue
True
In what 3 basic ways can drugs exert their actions on the body?
through receptors, through enzymes, through nonselective interactions
Define “receptor”
A reactive site on the surface or inside of a cell
Define “affinity”
The degree to which a drug attaches and binds with a receptor
TRUE or FALSE: The drug with the best “fit” and strongest affinity for the receptor will elicit the greatest response from the cell/tissue
True
How can drugs interact with receptors?
By either eliciting or blocking a physiological response
What is the action of the drug type, “Agonist?'“
The drug binds to the receptor and there is a response
What is the action of the drug type, “Partial agonist (agonist-antagonist)?”
The drug binds to the receptor and the response is diminished compared to the response elicited by an agonist
What is the action of the drug type, “Antagonist?”
The drug binds to the receptor and there is no response. The drug prevents the binding of agonists
What is the action of the drug type, “Competitive antagonist?”
The drug competes with the agonist for binding to the receptor. If it binds, there is no response
What is the action of the drug type, “Noncompetitive antagonist?”
Drug combines with different parts of the receptor and inactivates it. The agonist then has no effect
Define “enzymes”
Substances that activate nearly every biochemical reaction in a cell
Define “selective interaction”
For a drug to interact with enzyme systems and alter a physiological response, it may either inhibit (more common) or enhance the effects/actions of a specific enzyme on its normal target molecules in the body
TRUE or FALSE: Drugs with nonspecific mechanisms of action do not interact with receptors or enzymes, but rather their main targets are cell membranes and cellular processes
True
TRUE or FALSE: Before drug therapy is initiated, an end point or expected outcome of therapy should be established. This desired therapeutic outcome is patient specific
True
Define “contraindication”
Any patient condition, especially a disease state, that makes the use of a medication dangerous for the patient
What are the 7 types of therapies?
Acute, Maintenance, Supplemental (replacement), Palliative, Supportive, Prophylactic, Empirical