CH. 7 | The Control of Microbial Growth
1/13
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
14 Terms
Overview
Microbial control agents are physical or chemical methods used to inhibit, kill, or remove microorganisms to prevent infection, spoilage, and contamination.
Key types include chemical disinfectants (alcohols, phenolics, halogens), antiseptics, antibiotics, and physical methods like heat, radiation, and filtration. These agents target bacteria, viruses, and fungi on living tissue or surfaces.
Microbial Growth
The increase in the number of cells or total population mass of microorganisms
7 - 1 Define the following key terms related to microbial control: sterilization, disinfection, antisepsis, degerming, sanitization, biocide, germicide, bacteriostasis, and asepsis.
Bactericidal
Kills bacteria
Bacteriostatic
Inhibits/Prevents the growth of bacteria
Sterilization
Complete removal or destruction of all living microorganisms, including endospores
Methods include physical and chemical ways
The most common is autoclaving, or using aseptic technique (heating an inoculating loop/needle) — flaming the instruments / tubes through a bunsen burner flame
Complete sterilization is often not required in other settings
Commercial sterilization
→ A process of treating canned goods aimed at destroying microbes and endospores of C. botulinum
→ Limited heat treatment
Disinfection
Any treatment used on inanimate objects to kill or inhibit the growth of microorganisms
Destruction of vegetative pathogens (Non-endospore forming)
Makes use of chemicals, ultraviolet radiation, boiling water, or steam
Commonly applied as chemical agents to treat an inert surface or substance
→ i.e., alcohol, bleach, hydrogen peroxide
Antisepsis
→ A chemical method for disinfectation that is directed at living tissue and or skin
Degerming
The removal of microorganisms in an area / mechanical removal rather than the killing of microbes in a limited area
Usual target is on living tissue and or skin
→ i.e., when someone is about to receive an injection, the skin is swabbed with alcohol
Sanitization
Intended to lower microbial counts to safe public health levels and minimize the chances of disease transmission from one user to another
Accomplished by high-temperature washing, etc
Biocide + Germicide
A substance capable of killing microorganisms
Kills microorganisms (with certain exceptions)
i.e., a fungicide kills fungi, a virucide inactivates viruses, etc
Bacteriostasis
A treatment capable of inhibiting bacterial growth
Asepsis
Absence of significant contamination by unwanted organisms
Clean and sterile techniques
Involves washing hands
→ i.e., hand sanitizer, using alcohol wipes before injections
7 - 2 Describe the patterns of microbial death caused by treatments with microbial control agents.
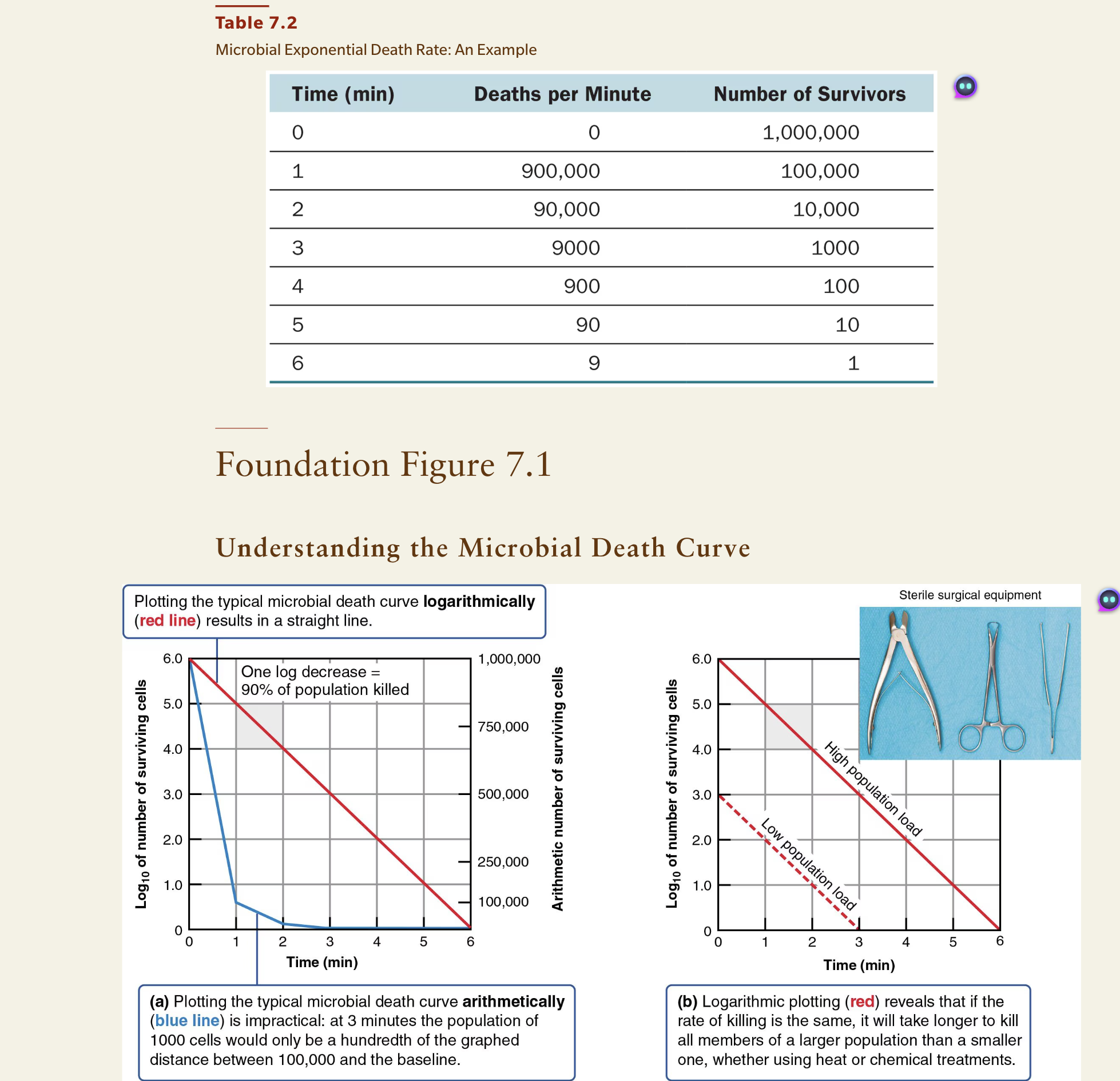
Pattern: Exponential (Constant Rate) Death
Microbes don’t die all at once, they die at a constant proportional rate. Each unit of time, the same percentage of whatever is left gets killed
Constant rate: The proportion being killed each minute, and it stays the same throughout the entire treatment
→ i.e., 90%
The number of deaths decreases by one each minute, but the rate (90% per minute) remains constant. This is known as exponential death
What affects this pattern?
Number of microbes — Bigger starting population = longer it takes to eliminate completely
Environmental conditions — Warmer temperatures and acidic conditions make treatments more effective
Organic matter — Blood, feces, and biofilms can shield microbes and slow killing (Usually protective of microorganisms)
Time of exposure — Longer exposure is needed for tough organisms or endospores
Microbial characteristics — Cell wall composition and endospore formation affect resistance
In other words…
Microbes die at a constant proportional rate (exponential death), meaning the same percentage dies each time interval, which appears as a straight line on a logarithmic graph. This rate is influenced by factors such as population size, environment, organic matter, exposure time, and microbial traits.
7 - 3 Describe the effects of microbial control agents on cellular structures.
3 Primary Ways —in which various agents can kill or inhibit microbes—
Plasma membrane — Actively regulates the passage of nutrients into the cell, and deals with the elimination of waste from it
→ Damage to the lipids or proteins by microbial control agents can cause cellular contents to leak into the surrounding medium and interfere with cell growth
Enzymes — Vital to all cellular activities = Destroying its enzymes destroys the cell
→ Damage / Breakage of the hydrogen bonds results in the denaturation of the protein
Nucleic Acids — Carrier of the cell’s genetic information
→ Damage to these nucleic acids is lethal for the cell, as it can no longer replicate or carry out metabolic functions (such as the synthesis of enzymes)
7 - 4 Compare the effectiveness of moist heat and dry heat.
Bacterial Heat Resistance
Thermal Death Point (TDP)
→ Lowest temperature at which all the microorganisms in a particular liquid suspension will be killed in 10 minutes
→ i.e., Salmonella, if you heated it to 59°C for 10 minutes, some cells might survive. But at 60°C for 10 minutes, every single cell is dead — that's the thermal death point
Thermal Death Time (TDT)
→ Minimal length of time for all bacteria in a particular liquid culture to be killed at a given temperature
Decimal Reduction Time (DRT)
→ Time in minutes, in which 90% (one log) of a population of bacteria at a given temperature will be killed
Moist Heat Sterilization
Boiling
→ Usual temperature: 100o c
→ Kills vegetative forms of bacterial pathogens
→ Endospores are not killed/destroyed by this
→ Does not result in sterilization
Autoclaving
→ Preferred method of sterilization (unless the material can get damaged by heat or moisture)
→ Higher the pressure, higher the temperature
→ 121o c for 15 minutes will kill all organisms and endospores
Pasteurization
→ Developed by Louie Pasteur
→ Mild heating — sufficient to kill organisms that cause spoilage, without damaging the taste of the product
→ Kills harmful/pathogenic microorganisms in food and beverages without completely sterilizing them
→ High-temperature short time pasteurization (HTST)
→ Ultra-high temperature treatments (UHT)
Dry Heat Sterilization
Flaming
→ The process of sterilizing an inoculating loop or needle by holding it in an open flame
→ Incineration
Hot Air Sterilization
→ Sterilization by the use of an oven at 170o c for approximately 2 hours
7 - 5 Describe how filtration, low temperatures, high pressure, desiccation, and osmotic pressure suppress microbial growth.
Filtration
Membrane filtration
Works by passing a liquid or gas through a screen-like material with pores small enough to trap and retain microorganisms physically — it doesn't kill them, it simply removes them from the substance
In other words, filtration physically removes microorganisms rather than suppressing or killing them
→ i.e., strainer
Low Temperatures
Refrigeration
→ Works by slowing down the metabolic rate of microorganisms, so much so that they can barely function (cannot reproduce or synthesize toxins)
→ Bacteriostatic effect — Inhibits / Prevents bacterial growth
Freezing
→ Rapid Freezing — Microbes are dormant, but not dead
→ Slow Freezing — Most harmful, ice crystals form and physically disrupt the cellular and molecular structure
→ Thawing — Most damaging, slow, but causes more ice crystal damage
Lyophilization / Freeze-drying
→ Laboratory process for preserving microbes by freezing, reducing pressure, and removing water
High Pressure
If the pressure is high enough, it can alter the molecular structures of proteins and carbohydrates, resulting in the rapid inactivation of vegetative bacterial cells
Endospores are highly resistant to high pressure
Desiccation (Dry)
Absence of water → microorganisms cannot grow or reproduce, but can remain viable
Prevents metabolism
Osmotic Pressure
High concentrations of salt or sugar create a hypertonic environment outside the microbial cell, causing water to rush out of the cell through osmosis
Dehydrates the cell, which starves the cell of moisture (which is needed for it to survive and reproduce)
Mostly bacteriostatic, but can become bactericidal if dehydration is severe enough
7 - 6 Explain how radiation kills cells.
Ionizing Radiation
Gamma rays
X-rays
High-energy electron beams
→ Shorter wavelength = carries more energy
→ Ionization of water makes it so that highly reactive hydroxyl radicals form, which can kill organisms by reacting with their organic cellular components (especially DNA), and damage them
→ Destruction of DNA
Nonionizing Radiation
UV light
→ Longer wavelength
→ Does not have enough energy to ionize atoms
→ UV light damages cells by being absorbed into their DNA. This absorption causes bonds to form between adjacent pyrimidine bases (usually thymines) in the chain, creating thymine dimers. These dimers block proper DNA replication during cell reproduction, ultimately preventing the cell from reproducing correctly and eventually leading to cell death
→ Damage to DNA
Physical Methods used to control Microbial Growth
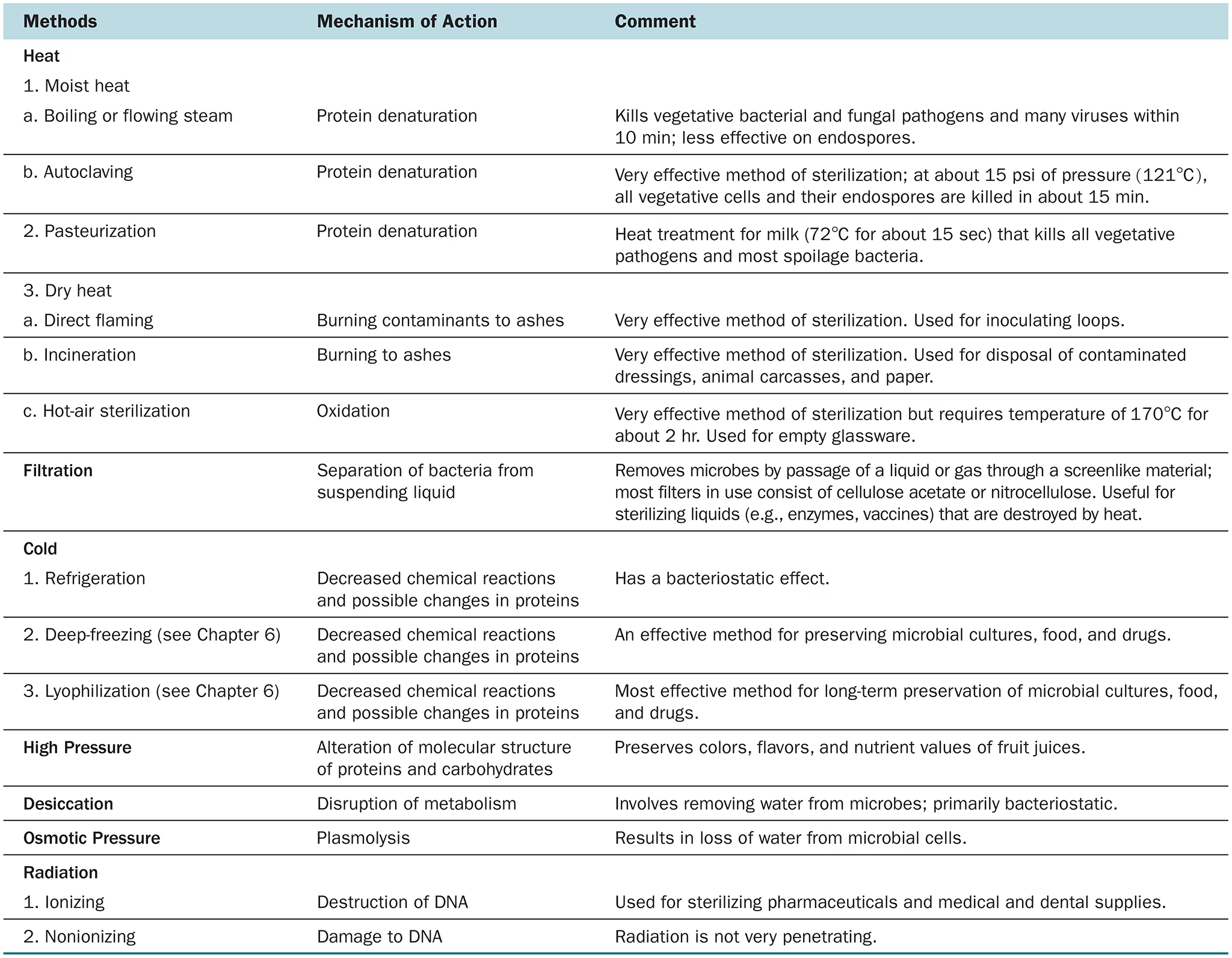
7 - 7 List the factors related to effective disinfection.
Concentration of the Disinfectant
→ Directly affects how well a disinfectant will work
→ Must always be diluted exactly as specified by the manufacturer
→ Too weak = Ineffective
→ Too strong = Potentially wasteful/harmful
Temperature
→ The activity of most disinfectants increases as the temperature rises
→ Too high a temperature can end up inactivating the disinfectant itself
pH of the Medium
Significantly affects pH activity
Chlorine is a good example; it is most effective at pH 6, but ineffective at pH > 8
Nature / Organic matter
Organic materials present on a surface can interfere with disinfectant action
This is why surfaces need to be scrubbed and rinsed before applying the disinfectant
Time
7 - 8 Interpret the results of use-dilution tests and the disk-diffusion method.
Use-Dilution Tests
A method of determining the effectiveness of a disinfectant using serial dilutions
Measures the presence and or absence of bacterial growth to determine the effectiveness of a disinfectant
How it works:Metal/glass cylinders are dipped into standardized bacterial cultures. Thereafter, they are removed and dried at 37o c for a short time. Afterwards, they are placed into the disinfectant solution at the recommended concentration and left for 10 minutes at 20o c, and then transferred over to a growth medium
To interpret results:
→ No bacterial growth = Disinfectant effectively killed all bacteria
→ Some bacterial growth = Disinfectant was partially effective, some survived, some died
→ Heavy bacterial growth = Disinfectant was ineffective
Disk-Diffusion Method (Kirby-Bauer Test)
An agar-diffusion test to determine microbial susceptibility to chemotherapeutic agents
Measures the diameter of the zone of inhibition surrounding the antimicrobial-soaked disk to determine the susceptibility of bacteria to drugs
How it works:A filter paper disk is soaked with the chemical agent, which is then placed on an agar plate that has been inoculated with the test organism. Afterwards, the plate gets incubated, and the results are up for discussion
To interpret results:
→ Clear zone of inhibition around disk = Chemical is effective, meaning that bacteria cannot grow in the zone
→ No clear zone = Chemical is ineffective, meaning that bacteria can growA zone of inhibition can be an irregular/crooked circle because it still represents that bacterial growth was inhibited due to an antimicrobial agent
7 - 9 Identify the methods of action and preferred uses of chemical disinfectants.
Antimicrobial action/activity
Inhibits the growth of or killing of microorganisms through mechanisms such as damaging their cell walls, disrupting membranes, inhibiting protein synthesis, or blocking DNA replication
The following examples are chemical antimicrobial agents and their specific mechanisms of antimicrobial activity
Phenolics
Suitable agents for disinfecting pus, saliva, and feces
Exerts antimicrobial activity by injuring plasma membranes, which results in leakage of cellular contents
Remain active in the presence of organic compounds → stable → persist for long periods of time
Bisphenols
Used to control infections in nurseries, and is an ingredient in soaps, toothpastes, and mouthwashes
Triclosan (Bisphenol used in s, t, and m)
→ Was eventually banned because it was not considered safe in healthcare settings. It would inhibit an enzyme needed for the biosynthesis of fatty acids, which affects the integrity of the plasma membrane
→ Effective against gram + bacteria
Biguanides
Affects bacterial cell membranes
Effective against gram + and gram - bacteria
Chlorhexidine
→ Common in microbial control on skin and mucous membranes
→ Often used for surgical hand scrubs & skin preparation in patients
Essential Oils
Mixture of hydrocarbons extracted from plants
Similar to phenolics, they can be used to disinfect hard surfaces like countertops, and can be used on skin
Halogens
Iodine and Chlorine are effective antimicrobial agents
→ Iodine: Impairs protein synthesis and alters membranes (their structure and ability to function)
→ Chlorine: Oxidizing agent, shuts down cellular enzyme systems
Alcohols
Effectively kill bacteria and fungi but not endospores and non-enveloped viruses
Denatures proteins and can disrupt membranes
Ethanol and Isopropanol
Heavy Metals
Can be biocidal or antiseptic
Oligodynamic action
→ The ability of small amounts of a heavy metal compound to exert antimicrobial activity
7 - 12 List the advantages of glutaraldehyde over other chemical disinfectants.
Glutaraldehyde
Superior high-level disinfectant and sterilant
An aldehyde (effective antimicrobial)
Less irritating, more effective than formaldehyde
Effective against bacteria, viruses, fungi, spores, etc
Used in hospital settings as a disinfectant
7 - 13 Identify chemical sterilizers.
Plasmas
Consists of an electrically excited gas
Free radicals destroy microbes
Advantage: Requires only low temperatures
Supercritical Fluids
CO2 with gaseous and liquid properties
Organisms exposed to this supercritical CO2 are inactivated (including most vegetative organisms that cause spoilage and foodborne illnesses)
Peroxygens
Oxidizing agents
Used for contaminated surfaces and food packaging
7 - 14 Explain how the type of microbe affects the control of microbial growth.
Ethylene Oxide
Kills all microbes and endospores, but requires a lengthy exposure time for several hours
1. Prions — MOST RESISTANT
Infectious proteins (not even living cells!)
Cause neurological diseases like mad cow disease
Normal autoclaving is inadequate
To destroy: incineration of infected carcasses
For surgical instruments: WHO/CDC recommend sodium hydroxide + autoclaving at 121°C for 1 hour OR 134°C for 18 minutes
Disposable instruments must be incinerated
2. Bacterial Endospores
Affected by relatively few biocides
Extremely tough protective coating makes them highly resistant
Require very harsh conditions to destroy (e.g. autoclaving at 121°C)
3. Mycobacteria
Non-endospore-forming but still greater-than-normal resistance
Example: Mycobacterium tuberculosis
Resistance due to waxy, lipid-rich cell wall
Special tuberculocidal tests developed specifically to test biocides against them
Disinfectant labels often indicate if they are tuberculocidal
4. Cysts & Oocysts of Protozoa
Relatively resistant to chemical disinfection
The cyst form is a protective stage making them harder to kill than vegetative forms
5. Vegetative Protozoa
Active, non-cyst form
More susceptible than cysts but still moderately resistant
6. Gram-Negative Bacteria
More resistant than Gram-positive due to:
External lipopolysaccharide (LPS) layer
Porins — highly selective structural openings that control what enters the cell, blocking many biocides
Pseudomonas and Burkholderia are especially resistant — can even grow actively in some disinfectants (e.g. quaternary ammonium compounds)
Also resistant to many antibiotics
7. Fungi (including most fungal spores)
Moderately resistant
More tolerant of osmotic pressure and acidic conditions than bacteria
Reason molds cause spoilage in fruits and grains
8. Viruses Without Envelopes (Nonenveloped)
Have only a protein coat
More resistant — fewer biocides are effective against them
9. Gram-Positive Bacteria
Generally more susceptible than Gram-negative
Lack the external LPS layer and selective porins
Most biocides work well against them
10. Viruses With Lipid Envelopes — LEAST RESISTANT
Most susceptible because their lipid envelope is easily disrupted
Lipid-soluble antimicrobials are very effective against them
Labels indicate effectiveness against lipophilic viruses
