Immunology Fundamentals and Vaccination
1/48
Earn XP
Description and Tags
Adaptive & Innate Immunity, Antibodies, Vaccines
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
49 Terms
Immunosupression
Someone’s immune system has a reduced ability to fight infection
Ex) Someone has a genetic mutation that leads to cancer
1st Line of Defense
Innate Immunity
Constant, non-specific
Use of epithelial cells
Ex) Skin, mucus, saliva, microbiome,ciliary activity
2nd Line of Defense
Inflammatory Response
Generalized, rapid, non-specific
Immediately cccurs after physical barrier breach or cellular injury has occurred
Ex) Swelling and redness that occurs within minutes of spraining ankle
3rd Line of Defense
Adaptive Immunity/Acquired Immunity
Slow, specific
Has memory
Inflammatory Response - 2nd line of defense
Rapid, NON-SPECIFIC — same response regardless of pathogen type
Key microscopic changes: vasodilation, ↑ capillary permeability, WBC influx, hemostasis
Localized s/sx: erythema, warmth, swelling, pain, loss of function
Systemic s/sx: fever, leukocytosis (↑ WBC), ↑ ESR (liver makes acute-phase proteins)
Adaptive Immunity - 3rd Line of Defense
Initiated when innate immune system signals cells of adaptive immunity
Slow onset on first exposure, fast on re-exposure (memory)
Very specific to target antigen
T&B lymphocytes retain immunologic memory
Active molecules: antibodies, complement, cytokines
Protection includes:
Activated T and B lymphocytes
Cytokines
Antibodies
1st Line - Physical and Biochemical Barriers
Physical: epithelial cells (skin, GI lining) — minimize pathogen entry points
Chemicals: mucus, sweat, earwax, tears, saliva — trap microorganisms
Microbiome: 'good' bacteria on body surfaces (e.g., gut microbiome, yeast on skin)
Antigen
Molecular targets of antibodies and lymphocytes that evokes immune response
Can bind with antibodies or antigen receptors on lymphocytes
Includes exogenous antigens & endogenous antigens
Adaptive immunity recognizes and attacks these antigens to protect body
Antigen-Presenting Cell (APC)
Capture antigens, process them, and then display them through the MHC to immune system
Includes:
Dendritic cells:
Highly mobile due to unique structure
Located in tissues like the skin for easy access to potential exogenous antigens
Macrophages
B cells
Antigen Presentation Process
Antigen (protein) is present in cell
Antigen processed/broken down
Antigen fragments are presented on the surface of the cell by a MHC molecule
Antigen Presentation - Goal
Present foreign antigen in such a way that immune system knows exactly how to respond by drawing in the proper cells through the activation of the adaptive immune response
Major Histocompatibility Complex (MHC)
Presents antigen to immune system on surface of cell
Has two types
Type I MHC
Presents endogenous antigens (viruses, tumors)
Ex) Found on all nucleated cells and platelets
Type II MHC
Presents exogenous antigens
Ex) APCs
Cell-Mediated Immunity
Directly target and destroy infected cells
Key players:
Helper T Cells (CD4+)
Cytotoxic T Cells (CD8+)
Regulatory T Cells (Treg)
Natural Killer Cells (NK)
Cell-Mediated Immunity - Helper T Cells (CD4+)
Activate other immune cells to come to the site
Cell-Mediated Immunity - Cytotoxic T Cells (CD8+)
Kill infected cells directly
Cell-Mediated Immunity - Regulatory T Cells (Treg)
Stop an over-activation of immune system (so body does not attack itself)
Humoral Immunity (B-cells)
Immune response mediated by antibodies
B-CELLS PRODUCE ANTIBODIES
Antibodies are secreted into the bloodstream and they ciruclate to detect the invader
Key players:
Plasma Cells
Memory B Cells
Antibodies
Humoral Immunity (B-cells) - Plasma Cells
Produce antibodies
Humoral Immunity (B-cells) - Antibodies
Immunoglobulins
Specific class of proteins that bind to specific antigens to destroy them
Found in general circulation and lymph structures
Produced by B cells in response to an antigen
Immunoglobulins structure
2 identical heavy chains
2 identical light chains
Structure gives it the ability to bind to a certain antigen
Has 5 difference classes
Immunoglobulins function
Circulate through blood
Detect and bind directly to antigen
Tag antigen
Allows antigen to be recognized by immune system for targeted destruction
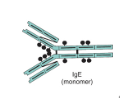
IgE
Allergic reactions
Binds mast cells → releases histamines (Type I hypersensitivity)→ inflammation
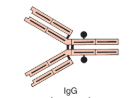
IgG
Most common antibody produced in the primary and secondary immune response
Most abundant in blood
Crosses placenta (neonatal immunity)
Enhances phagocytosis
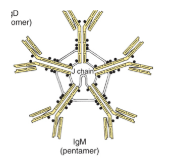
IgM
First antibody produces in response to an antigen
Fixes complement and promotes target cell-lysis
Present on the surface of mature B cells where it serves as a receptor for antigen recognition (along with IgD)
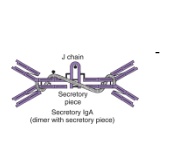
IgA
Mucous membranes
GI/respiratory tract
Breast milk → protects infant against microbes in GI tract
IgD
Found only on the surface of mature B cells, where it serves as a receptor for antigen recognition (along with IgM)
Attaches to B cells and activates them
Active Immunity
Formed thorough actual exposure to antigen
Body capable of producing its own antibodies
Acquired through infection or through vaccination
Takes longer to develop
Long-term protection
Memory Present → can mount secondary response to subsequent exposure
Passive Immunity
Occurs if antibodies outside of the body are transferred to the individual who needs them
Recipient of the antibodies cannot form them on their own
Commonly seen in newborns, who receive maternal antibodies from their mother through breast milk (offers immediate protection to baby)
Short-term protection (only persist if antibodies remain in the body)
Immediate onset
No memory
Vaccine - description
Preparation containing whole or fractionated microorganisms
Stimulates the recipient’s immune system to manufacture antibodies directed against the specific microbe from which the vaccines were made
Cannot cause disease itself in individuals with a healthy immune system
Vaccines produce active immunity
Directly expose recipient’s immune system to an antigen associated with the disease it may cause
Allows immune system to form memory against antigen
Inactivated vaccine
Contain a killed pathogen/microbe unable to cause an infection but can still trigger immune response by the immune system
Ex) Inactivated polio vaccine
Live, attenuated vaccine
Contain a weakened version of a live pathogen unable to cause an infection but can still signal immune response
Ex) MMR vaccine (Measles, mumps, rubella)
Avoid in those who are immunocompromised
Subunit vaccine
Non-viable or weakened fragments of microbe
Toxoid vaccine
Inactivated toxin (e.g., Td/Tdap)
mRNA vaccine
Codes for antigen; body produces it to trigger response (e.g., COVID-19)
Vaccination
Giving any vaccine to produce active immunity against particular microbe
Immunization
The process of becoming immune, includes both active and passive immunity
Natural immunization
Active immunity or an acquired response through infection and recovery
Artificial immunization
Active immunity from vaccinations
Vaccines - Mild Adverse Effects
Local reaction at injection site
Discomfort
Swelling
Erythema
Fever and flu-like symptoms
Immune system recognizes microbe as antigen -> activates inmune response (fever)
Vaccines - Severe (rare) Adverse Effects
Anaphylaxis
Acute encephalopathy
Seizures
Guillain-Barré Syndrome
Vaccine-associated paralytic poliomyelitis
Vaccines - Severe (rare) Adverse Effects - Anaphylaxis
severe, rapid allergic reaction -> shock, airway constriction, dramatic drop in blood pressure
Vaccines - Severe (rare) Adverse Effects - Acute encephalopathy
a rapid-onset, often reversible syndrome causing global brain dysfunction due to systemic issues like infections, toxins, or metabolic failure
Vaccines - Severe (rare) Adverse Effects - Guillain-Barré Syndrome
autoimmune disorder, immune system attacks peripheral nerves -> rapid onset muscle weakness, tingling, potential paralysis
Vaccines - Severe (rare) Adverse Effects - Vaccine-associated paralytic poliomyelitis
caused by live-attenuated virus in the Oral Poliovirus vaccine (OPV); occurs weakened vaccine virus reverts to a virulent form, causing paralysis in recipients or their contacts
True Contraindications for Vaccines
Anaphylactic reaction to a specific vaccine: Contraindicates further doses of that vaccine
Anaphylactic reaction to a vaccine component: Contraindicates use of all vaccines that contain that substance
Moderate or severe illnesses with or without a fever (places strain on immune system)
Live, attenuated vaccine should be avoided in those who are immunocompromised
False Contraindications for Vaccines
Mild to moderate local reaction (soreness, erythema, swelling) after a dose of an injectable vaccine
Mild acute illness with or without low-grade fever
Diarrhea
Current antimicrobial therapy
Convalescent phase of illnesses
Prematurity (same dosage and indicates as for normal, full-term infants)
Recent exposure to an infectious disease
Personal or family history of with penicillin allergy or nonspecific allergies