BSC 216- A and P Exam 4 (Hicks)
1/240
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
241 Terms
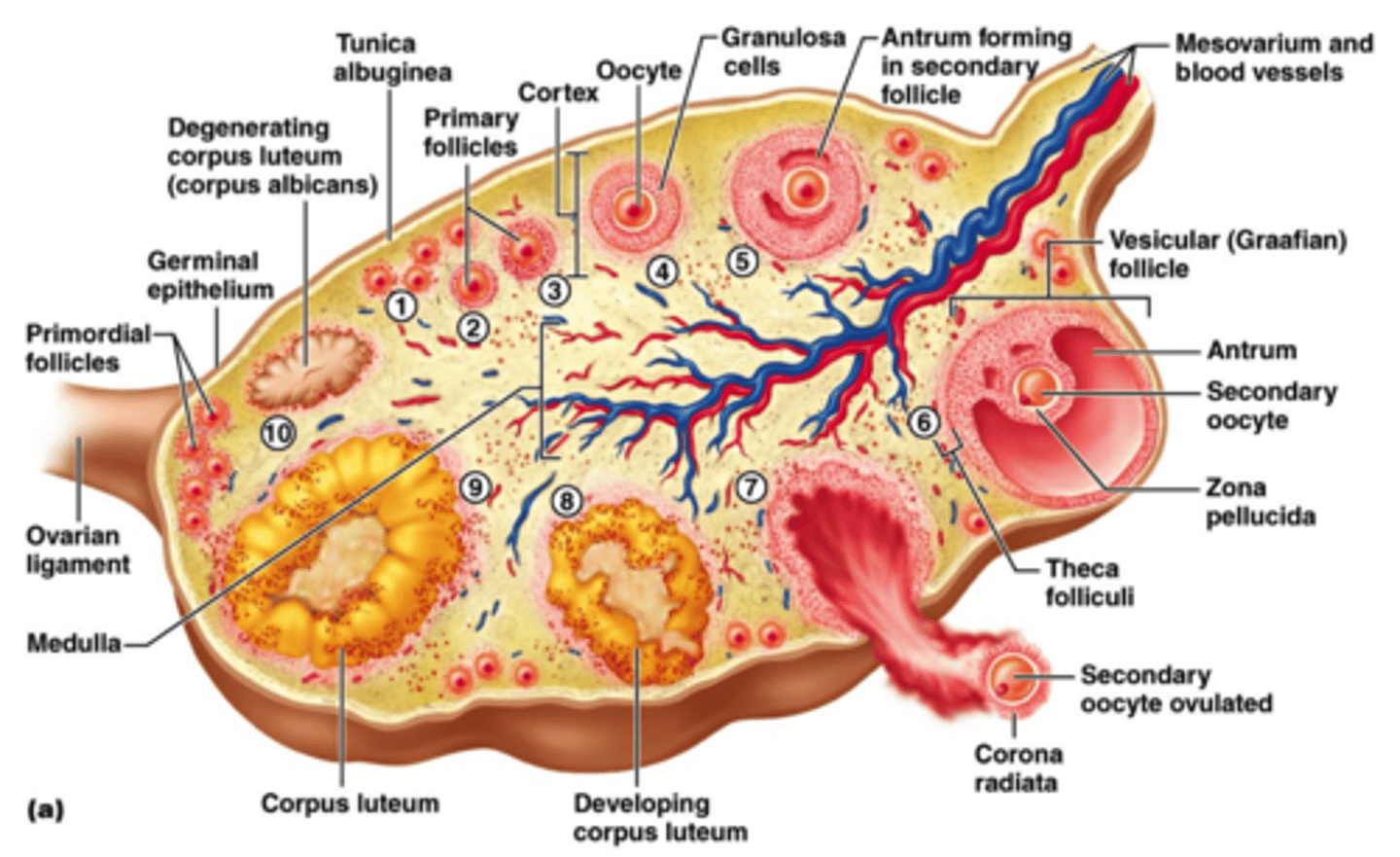
ovaries
female gonads that produce egg cells (ova) and sex hormones
-Almond-shaped and nestled in the ovarian fossa; Depression in the posterior pelvic wall
-Tunica albuginea capsule, like on testes
-Outer cortex where germ cells develop
-Inner medulla occupied by major arteries and veins
-Lacks ducts, instead each egg develops in its own fluid-filled follicle
ovulation
bursting of the follicle and releasing the egg
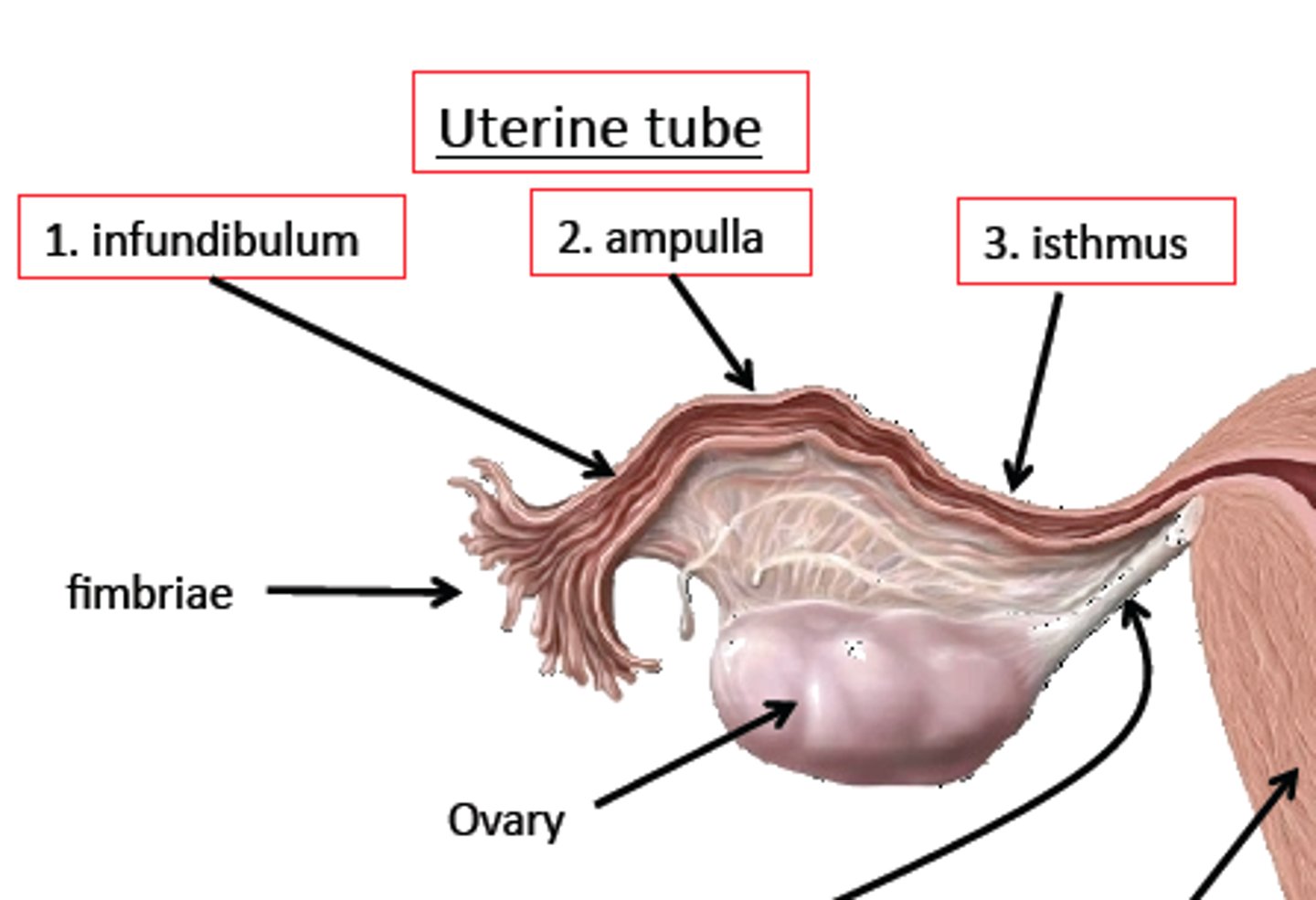
Uterine tube (oviduct) or (fallopian tube)
-Canal about 10 cm long from ovary to uterus
-Muscular tube lined with ciliated cells; Highly folded into longitudinal ridges
-epithelial lining of the uterine tube
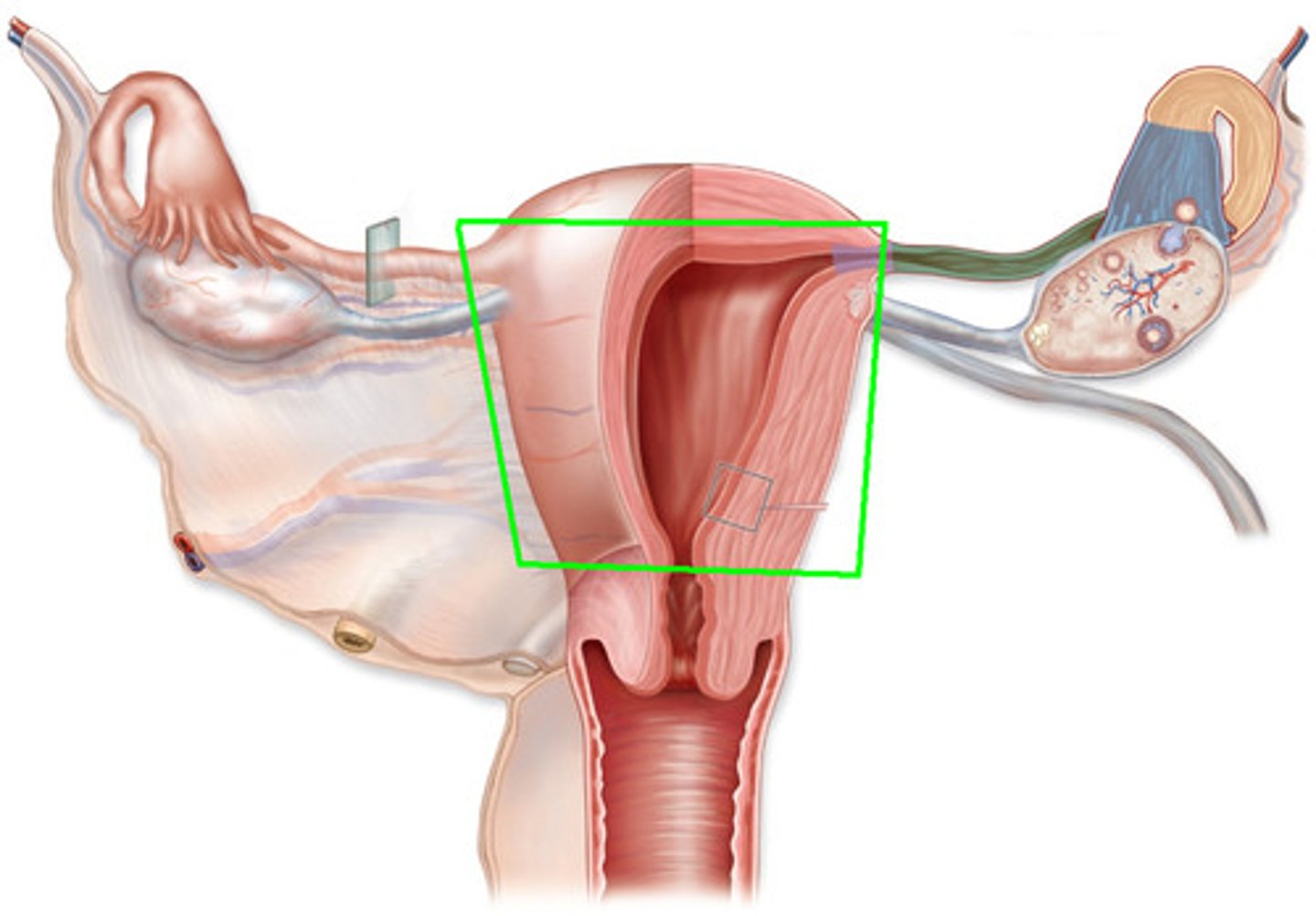
uterus
thick muscular chamber that opens into roof of the vagina
-Usually tilts forward over the urinary bladder
-Harbors fetus, provides a source of nutrition, and expels the fetus at the end of its development
-Pear-shaped organ
•Fundus—broad superior curvature
•Body (corpus)—middle portion
•Cervix—cylindrical inferior end
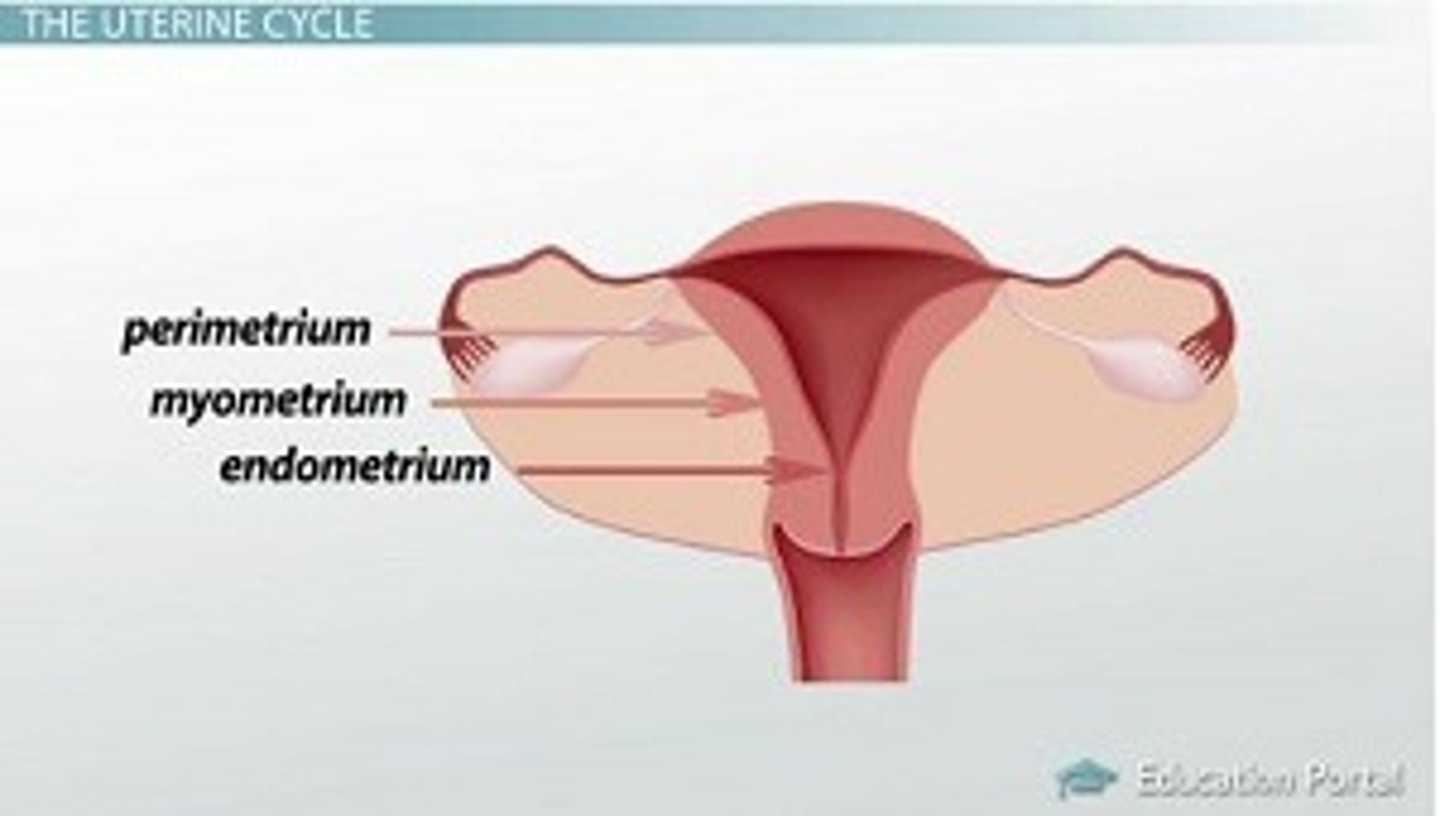
name the walls of the uterus
1. endometrium
2. myometrium
3. perimetrium
3. perimetrium
external serosa layer
2. myometrium
middle muscular layer
a. Constitutes most of the uterine wall
b. Composed mainly of smooth muscle
-Sweep downward from fundus; spiral around body
-Less muscular and more fibrous near cervix
-Produces labor contractions, expels fetus
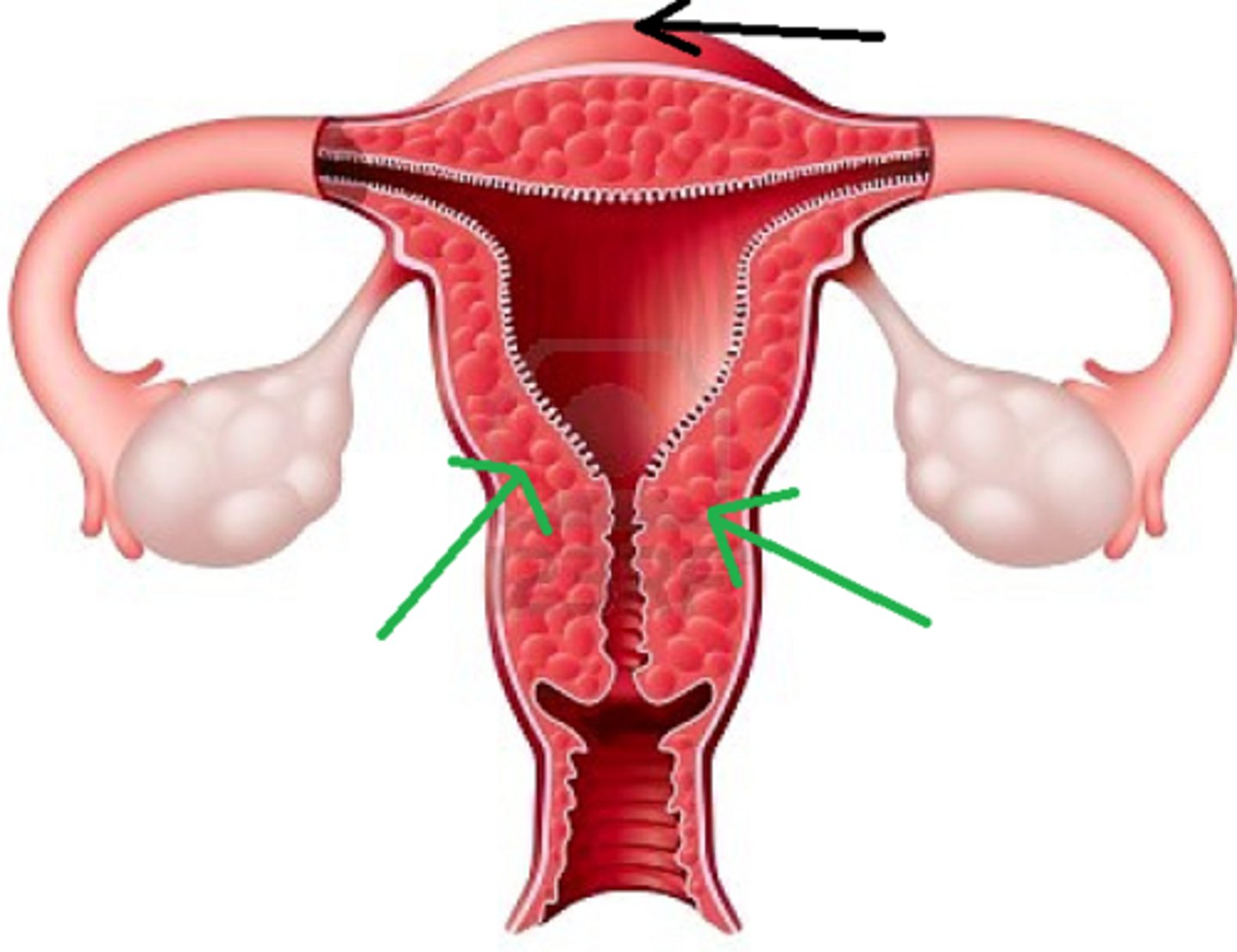
1. endometrium
inner mucosa
a. Simple columnar epithelium, compound tubular glands, and a stroma populated with leukocytes, macrophages, and other cells
-Stratum functionalis
-Stratum basalis
-During pregnancy, the endometrium is the site of attachment of the embryo and forms the maternal part of the placenta from which the fetus is nourished
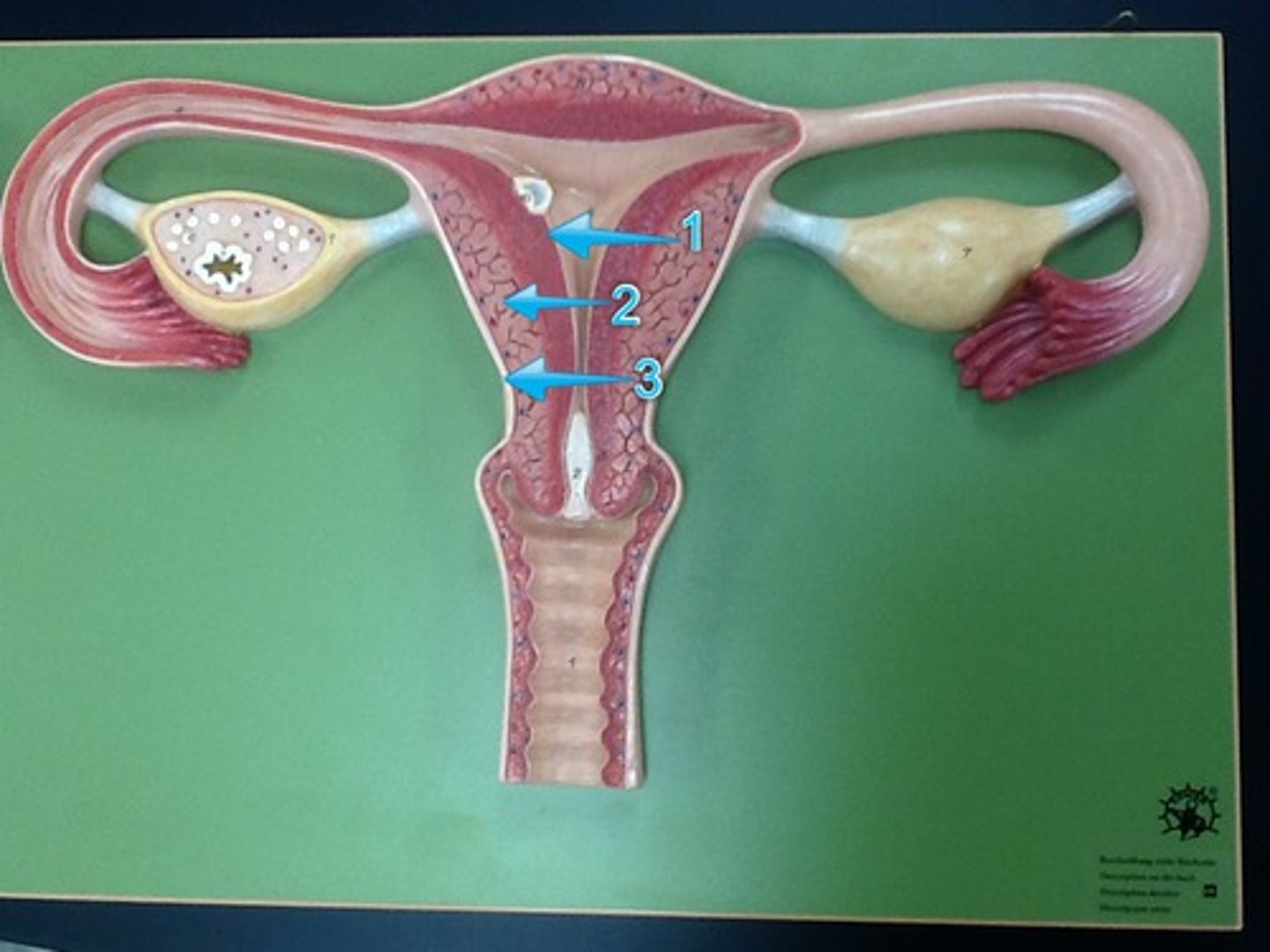
Stratum functionalis
superficial half, shed each menstrual period
Stratum basalis
deep layer, stays behind and regenerates a new stratum functionalis with each menstrual cycle
vagina (birth canal)
8 to 10 cm distensible muscular tube
a. Allows for discharge of menstrual fluid, receipt of penis and semen, and birth of baby
b. Vagina has no glands
-Transudation lubricates vagina: "vaginal sweating"
--Serous fluid through its walls and by mucus from the cervical gland above it
c. Transverse friction ridges (vaginal rugae) at lower end
d. Mucosal folds form hymen across vaginal opening
vaginal epithelium
a. Childhood: simple cuboidal
b. Puberty: estrogens transform to stratified squamous
-Bacteria ferment glycogen-rich cells producing acidic pH in vagina
c. An example of metaplasia: the transformation of one tissue type to another
d. Antigen-presenting dendritic cells: route by which HIV from infected semen invades the female body
Identify the external genitalia of the female
Clitoris, labia minora, and labia majora
-Occupy the perineum
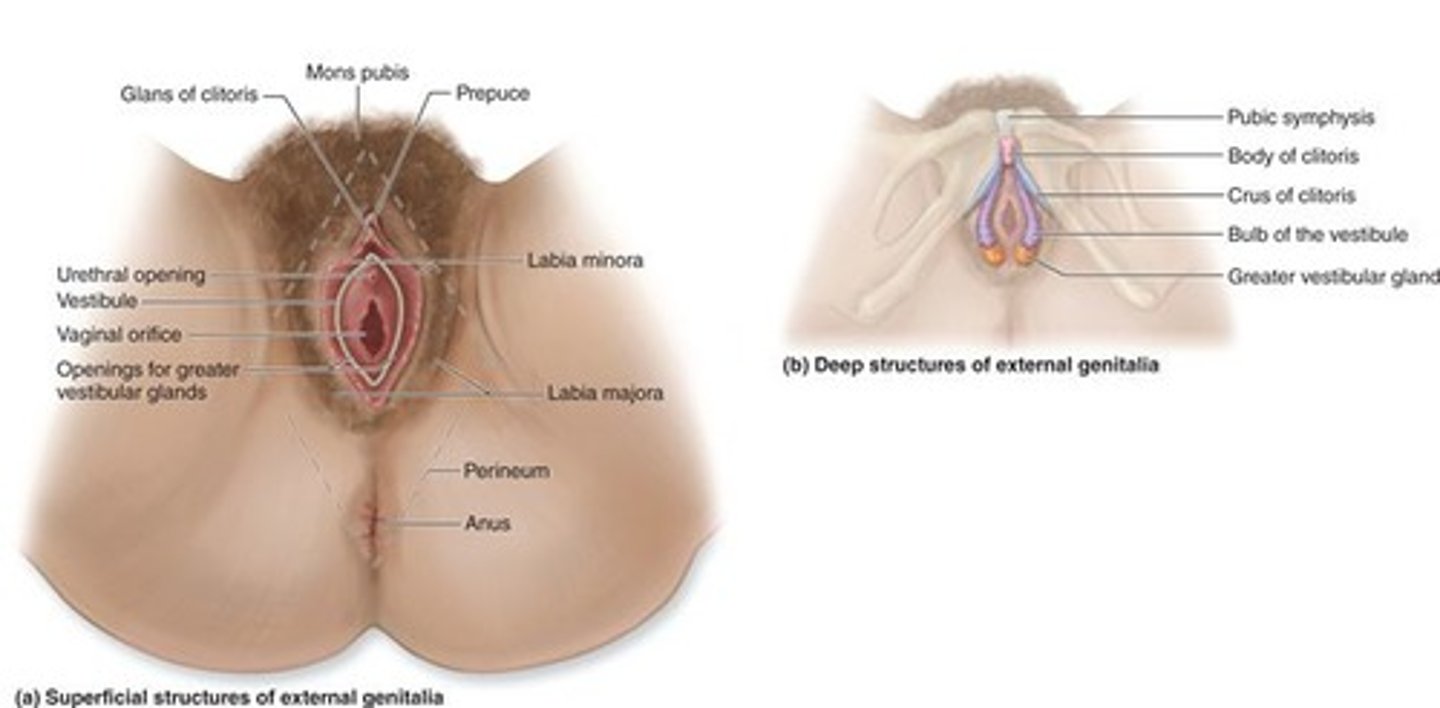
puberty begins at age 8 to 10 for most girls in US and is triggered by..
rising levels of GnRH (gonadotropin-releasing hormone)
-Stimulates anterior lobe of pituitary to produce:
•Follicle-stimulating hormone (FSH)
•Luteinizing hormone (LH)
follicle stimulation hormone (FSH) stimulates...
developing ovarian follicles and they begin to secrete estrogen, progesterone, inhibin, and a small amount of androgen
estrogens are...
feminizing hormones with widespread effects on the body
-most abundant is estradiol
what are the principal signs of puberty?
1. thelarche
2. pubarche
3. menarche
1. thelarche
onset of breast development is the earliest noticeable sign of puberty
-Estrogen, progesterone, and prolactin induce formation of ducts and lobules in the breast
-Completion of duct and lobule formation: glucocorticoids and growth hormone
-Adipose and fibrous tissue complete breast enlargement by age 20
2. pubarche
appearance of pubic and axillary hair, sebaceous glands, and axillary glands
-Androgens from ovaries and adrenal cortex stimulates pubarche and libido
3. menarche
first menstrual period
a. Requires at least 17% body fat in teenager, 22% in adult
-Improved nutrition has lowered age of onset to age 12 from about age 16 in 1860
-Leptin stimulates gonadotropin secretion
-If body fat and leptin levels drop too low, gonadotropin secretion declines and a female's menstrual cycle might cease
-First few menstrual cycles are anovulatory (no egg ovulated)
-Girls begin ovulating regularly about a year after they begin menstruating
estradiol/estrogen- puberty
-Stimulates vaginal metaplasia
-Stimulates growth of ovaries and secondary sex organs
-Stimulates growth hormone secretion; Increase in height and widening of the pelvis
-Responsible for feminine physique because it stimulates the deposition of fat
-Makes a girl's skin thicker; But remains thinner, softer, and warmer than males of the corresponding age
progesterone- puberty
Primarily acts on the uterus preparing it for possible pregnancy in the second half of the menstrual cycle
__________ and _____________ suppress FSH and LH secretion through negative feedback
estrogen and progesterone
•Inhibin selectively suppresses FSH secretion
•Hormone secretion is distinctly cyclic and the hormones are secreted in sequence
climacteric
midlife change in hormone secretion
climacteric is accompanied by ________________
menopause: cessation of menstruation
Female born with about 2 million eggs, climacteric begins when there are about 1,000 follicles left
-Follicles less responsive to gonadotropins
-Less estrogen and progesterone secretion
-Uterus, vagina, and breast atrophy
-Intercourse becomes uncomfortable as vagina becomes thinner, less distensible, and drier
-Vaginal infections more common
-Skin becomes thinner
-Cholesterol levels rise increasing the risk of cardiovascular disease
-Bone mass declines producing increased risk for osteoporosis
-Blood vessels constrict and dilate in response to shifting hormone balances
-Hot flashes: spreading sense of heat from the abdomen to the thorax, neck, and face
hormone replacement therapy (HRT)
low doses of estrogen and progesterone to relieve some of these symptoms
-Risks and benefits are still being debated
reproductive cycle- females
sequence of events from fertilization to giving birth
sexual cycle- females
events that recur every month when pregnancy does not intervene
a. Consists of two interrelated cycles controlled by shifting patterns of hormone secretion
-Ovarian cycle: events in ovaries
-Menstrual cycle: parallel changes in uterus
oogenesis
egg production
-Produces haploid gametes by means of meiosis
-Distinctly cyclic event that normally releases one egg each month
-Accompanied by cyclic changes in hormone secretion
-Cyclic changes in histological structure of the ovaries and uterus; Uterine changes result in monthly menstrual flow
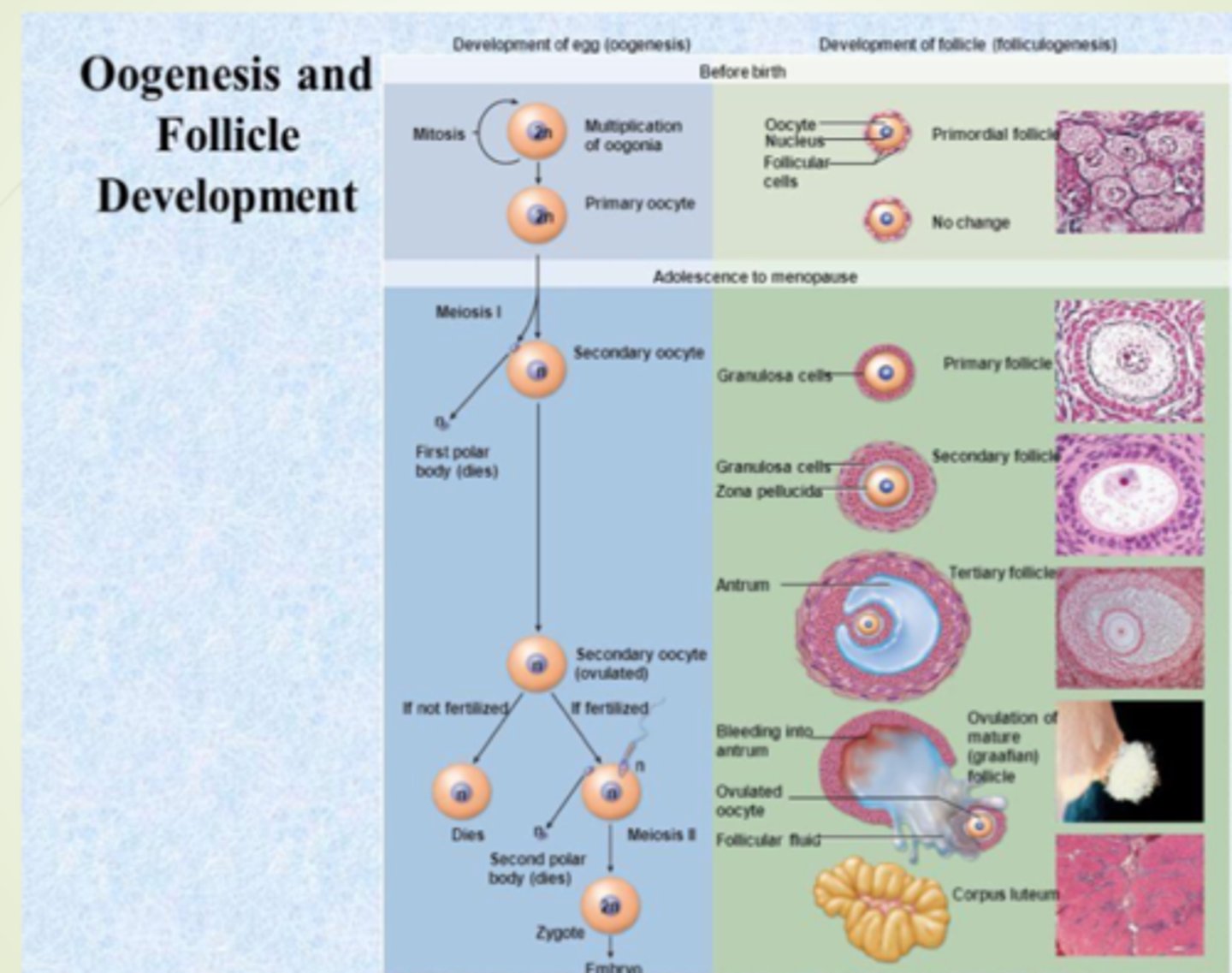
Oogenesis (embryonic development of ovary)
-Female germ cells arise from yolk sac
-Colonize gonadal ridges the first 5 to 6 weeks of development
-Differentiate into oogonia and multiply (by mitosis) until the fifth month; 5 to 6 million in number
-Transform into primary oocytes: early meiosis I
-Most degenerate (atresia) by the time the girl is born
-Egg, or ovum: any stage from the primary oocyte to the time of fertilization
-By puberty, 400,000 oocytes remain
•Lifetime supply—probably will only ovulate 480 times
Oogenesis (egg development resumes in adolescence)
-FSH stimulates monthly cohorts of oocytes to complete meiosis I
-Each oocyte divides into two haploid daughter cells of unequal size and different destinies
-Important to produce an egg with as much cytoplasm as possible
-If fertilized, it must divide repeatedly and produce numerous daughter cells
-Secondary oocyte: large daughter cell that is the product of meiosis I
first polar body- oogenesis
smaller one that sometimes undergoes meiosis II, but ultimately disintegrates
-Merely a means of discarding the extra set of haploid chromosomes
secondary oocyte- oogenesis
proceeds as far as metaphase II
-Arrests until after ovulation
-If not fertilized, it dies and never finishes meiosis
-If fertilized, it completes meiosis II and casts off a second polar body
-Chromosomes of the large remaining egg unite with those of the sperm
folliculogenesis
development of the follicles around the egg that undergoes oogenesis
1. primordial follicles
2. primary follicles
3. secondary follicles
4. tertiary follicles
5. Vesicular/ Graafian follicles
6. Corpus luteum
7. Corpus albicans
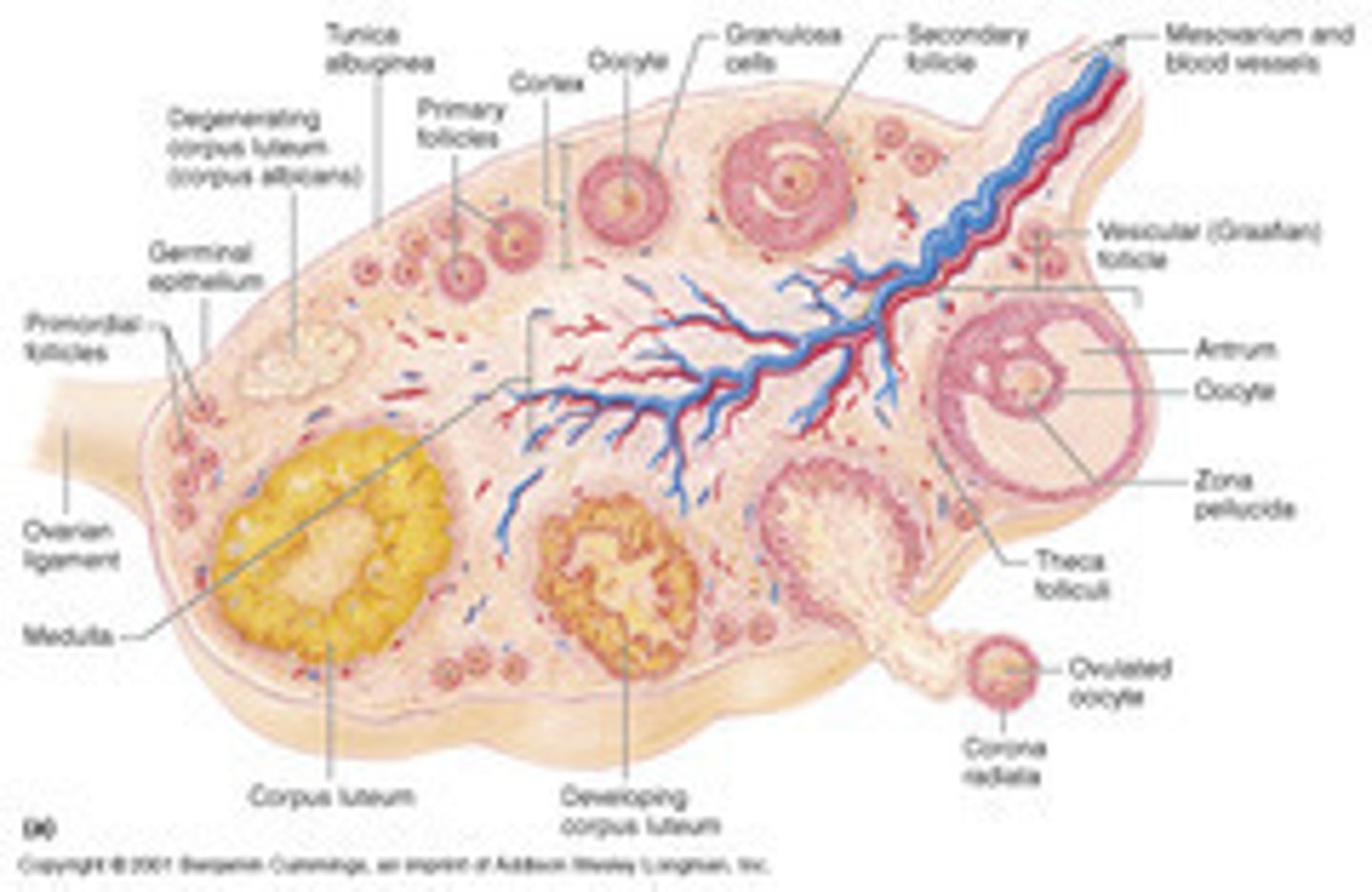
1. primordial follicles
•Consists of a primary oocyte in early meiosis (arrested in prophase 1 till puberty)
•Surrounded by a single layer of squamous follicular cells
•Concentrated in the cortex of the ovary
•Most wait 13 to 50 years before they develop further
•Adult ovary has 90% to 95% primordial follicles
2. primary follicles
•Have larger oocytes and follicular cells that still form a single layer
•Typically primary oocytes within
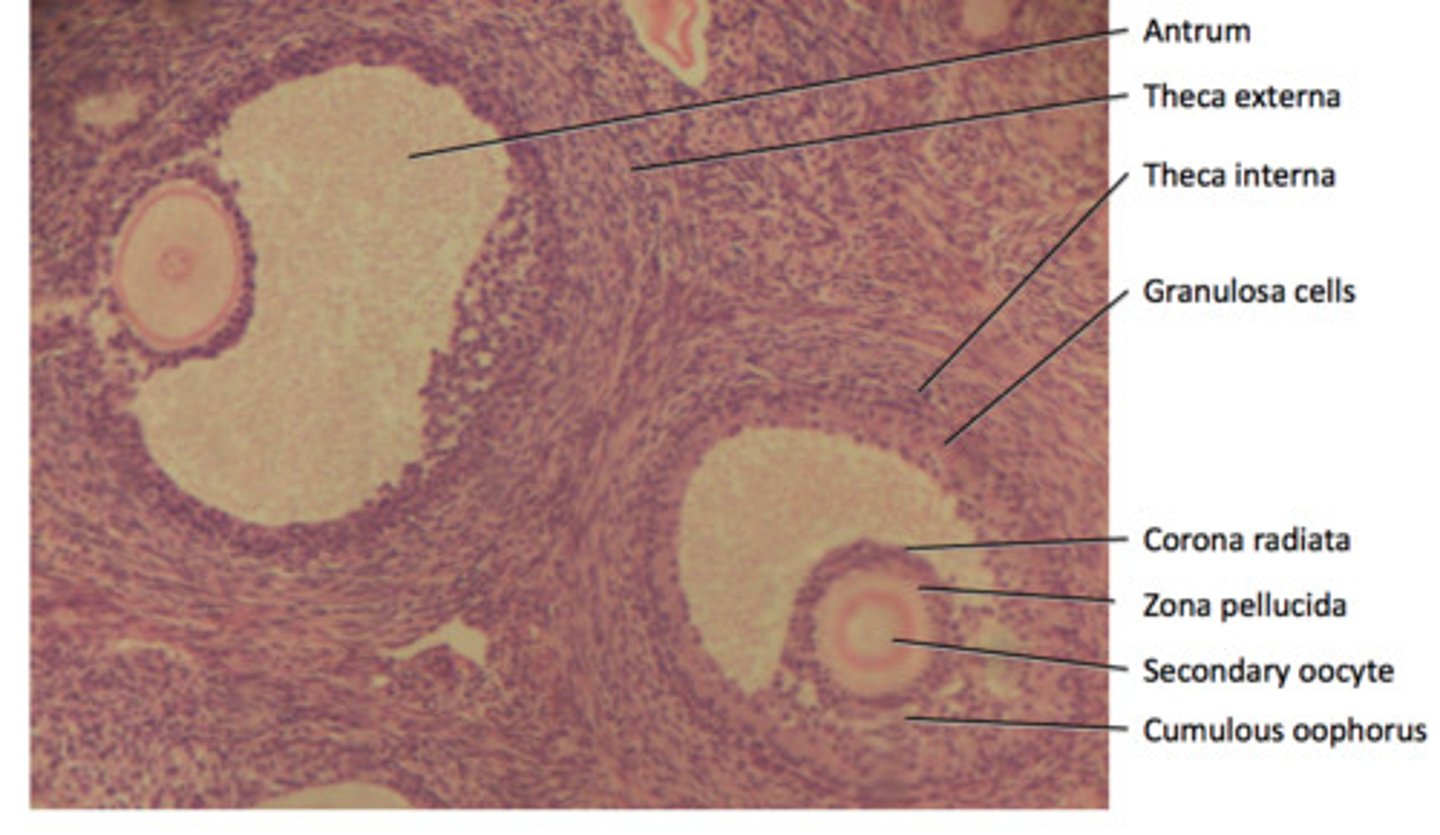
3. secondary follicles
•Still larger oocytes (typically secondary oocytes within)
•Follicular cells now stratified (granulosa cells)
•Zona pellucida—layer of glycoprotein gel secreted by granulosa cells around the oocyte
•Theca folliculi—connective tissue around the granulosa cells condenses to form a fibrous husk
4. tertiary follicles
•Granulosa cells begin secreting follicular fluid
•Accumulate in little pools in follicular wall—defines tertiary follicles
•As they enlarge, the pools merge forming a single fluid-filled cavity, the antrum
•Antral follicles—tertiary and mature follicles
•Preantral follicles—earlier stages of the follicles
•Cumulus oophorus—a mound of granulosa cells on one side of the antrum that covers the oocyte and secures it to the follicular wall
5. Vesicular/ Graafian follicles
•Normally only one follicle from each month's cohort becomes a mature follicle destined to ovulate
•Remainder degenerate
Sexual Cycle averages ______ days
28, varies from 20 to 45 days
a. basic hierarchy of hormonal control: -Hypothalamus to pituitary to ovaries to uterus
b. Ovaries exert feedback control over hypothalamus and pituitary
the sexual cycle begins with..
2 week follicular phase
-Menstruation occurs during first 3 to 5 days of cycle
-Uterus replaces lost tissue by mitosis and cohort of follicles grow
-Ovulation around day 14: remainder of follicle becomes corpus luteum
the last two weeks of the sexual cycle are...
luteal phase
-Corpus luteum stimulates endometrial secretion and thickening
-If pregnancy does not occur, endometrium breaks down in the last 2 days
-Menstruation begins and the cycle starts over
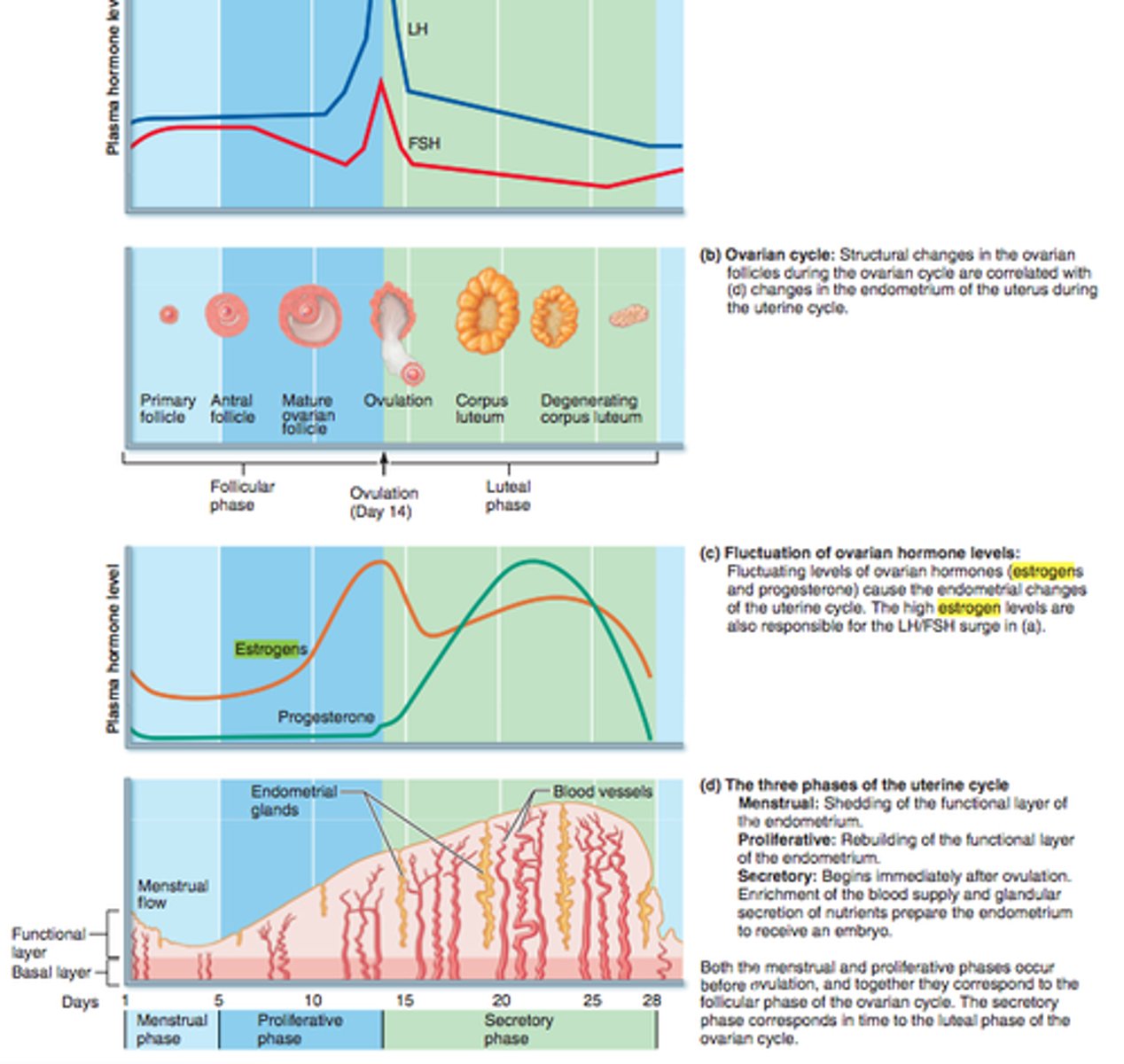
ovarian cycle
follicular phase, ovulation, luteal phase
-reflects what happens in the ovaries and their relationship to the hypothalamus and pituitary
1. follicular phase- ovarian cycle
extends from the beginning of menstruation until ovulation
a. Day 1 to day 14 of an average cycle
b. Preovulatory phase: from the end of menstruation until ovulation
c. Most variable part of the cycle; seldom possible to reliably predict the date of ovulation
d. Preparation for the follicular phase begins almost 2 months earlier
-Shortly after ovulation a new cohort of preantral follicles descends from the cortex deeper into the ovary
-Begins to grow and each develops an antrum
-Selection window of 5 days in which one of them is selected as the dominant follicle to mature and ultimately ovulate in the next cycle
-FSH stimulates continued growth of the cohort, but the dominant follicle above all
-FSH stimulates the granulosa cells of the antral follicles to secrete estradiol
-Dominant follicle becomes more sensitive to FSH and LH
-Grows and becomes mature (graafian) follicle while others degenerate
2. ovulation- ovarian cycle
the rupture of the mature follicle and the release of its egg and attendant cells
-Typically around day 14
a. Estradiol stimulates a surge of LH and a lesser spike of FSH by anterior pituitary
-LH induces several events
•Primary oocyte completes meiosis I
•Produces secondary oocyte and first polar body
•Follicular fluid builds rapidly and follicle swells
•Looks like a blister on the ovary surface
•Follicular wall weakened by inflammation and proteolytic enzymes
•Mature follicle approaches rupture
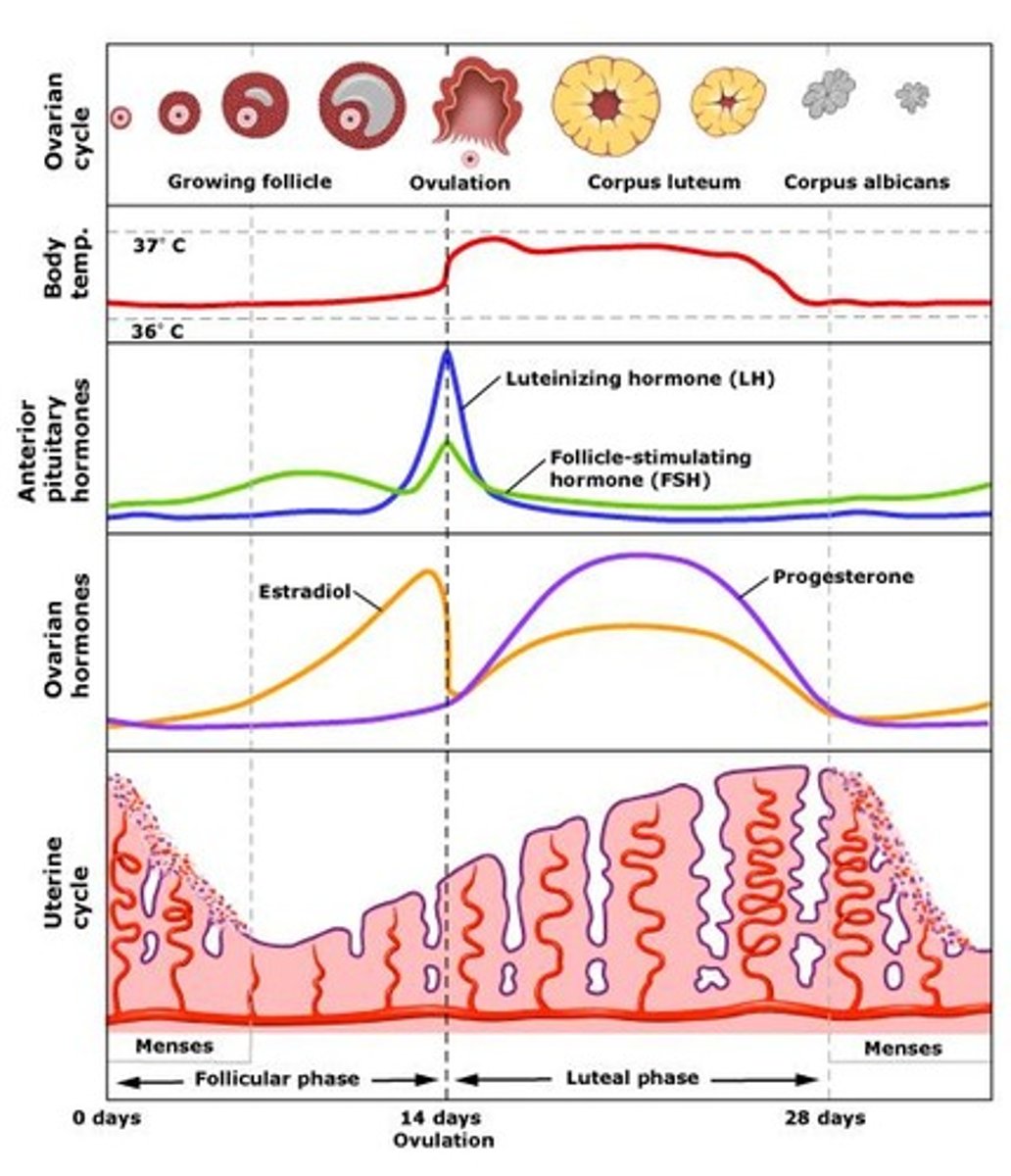
Control of Ovulation
also fig 26.16
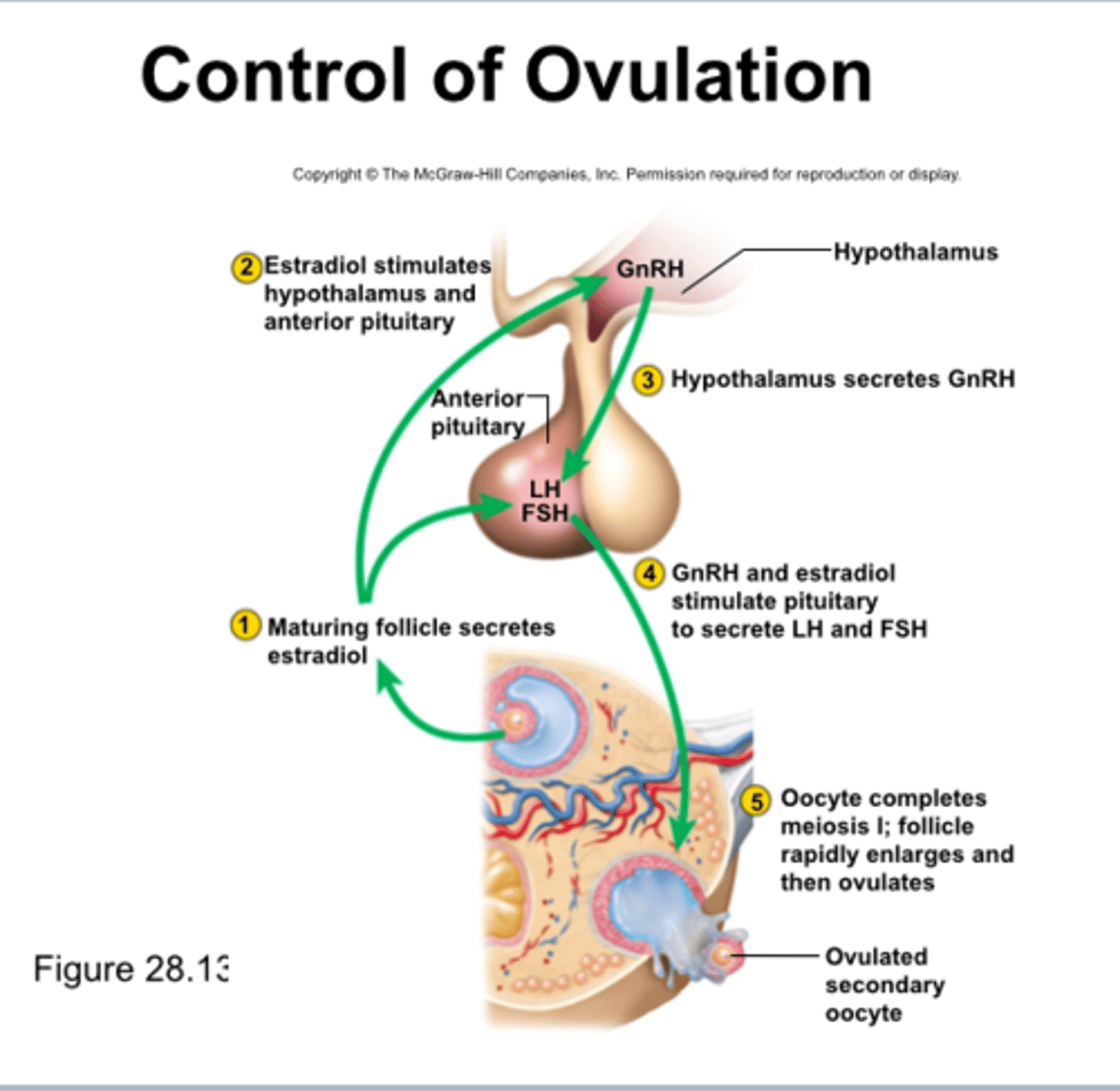
ovulation takes only _______ __________
-ovarian cycle
2 to 3 minutes
•Nipplelike stigma appears on ovary surface over follicle
•Seeps follicular fluid for 1 to 2 minutes
•Follicle bursts and remaining fluid oozes out carrying the secondary oocyte and cumulus oophorus
•Normally swept up by ciliary current and taken into uterine tube
________ _________ prepares to catch the oocyte when it emerges
uterine tube
•It swells with edema
•Its fimbriae envelop and caress the ovary in synchrony with the woman's heartbeat
•Cilia create gentle current in the nearby peritoneal fluid
Many oocytes fall into the pelvic cavity and die

3. Luteal (postovulatory) phase- ovarian cycle
day 15 to day 28, from just after ovulation to the onset of menstruation
a. If pregnancy does not occur, events happen as follows:
-Ovulated follicle becomes the corpus luteum
-Transformation from ruptured follicle to corpus luteum is regulated by LH
--- LH stimulates the corpus luteum to continue to grow and secrete rising levels of estradiol and progesterone
--- 10-fold increase in progesterone is the most important aspect of the luteal phase
-Progesterone has a crucial role in preparing the uterus for the possibility of pregnancy
-LH and FSH secretion declines over the rest of the cycle
-High levels of estradiol and progesterone, along with inhibin from the corpus luteum, have a negative feedback effect on the pituitary (too much estrogen and progesterone!!!)
-The corpus luteum begins the process of involution (shrinkage)
---Beginning about day 22 (8 days after ovulation)
---By day 26 involution is complete and becomes inactive bit of scar tissue, the corpus albicans
---With diminishing ovarian steroid secretion, FSH levels rise ripening a new cohort of follicles
-Ovaries usually alternate from month to month
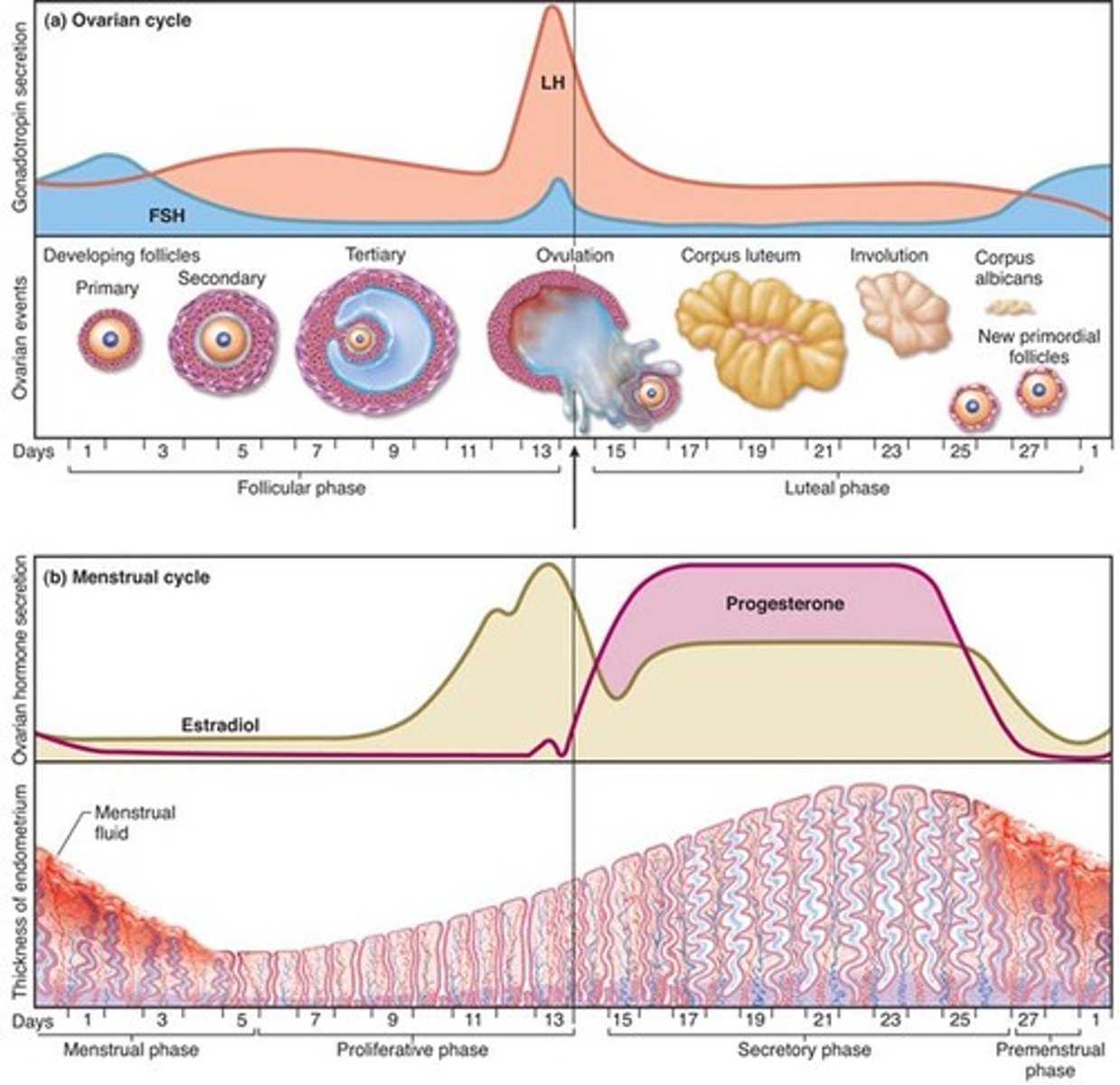
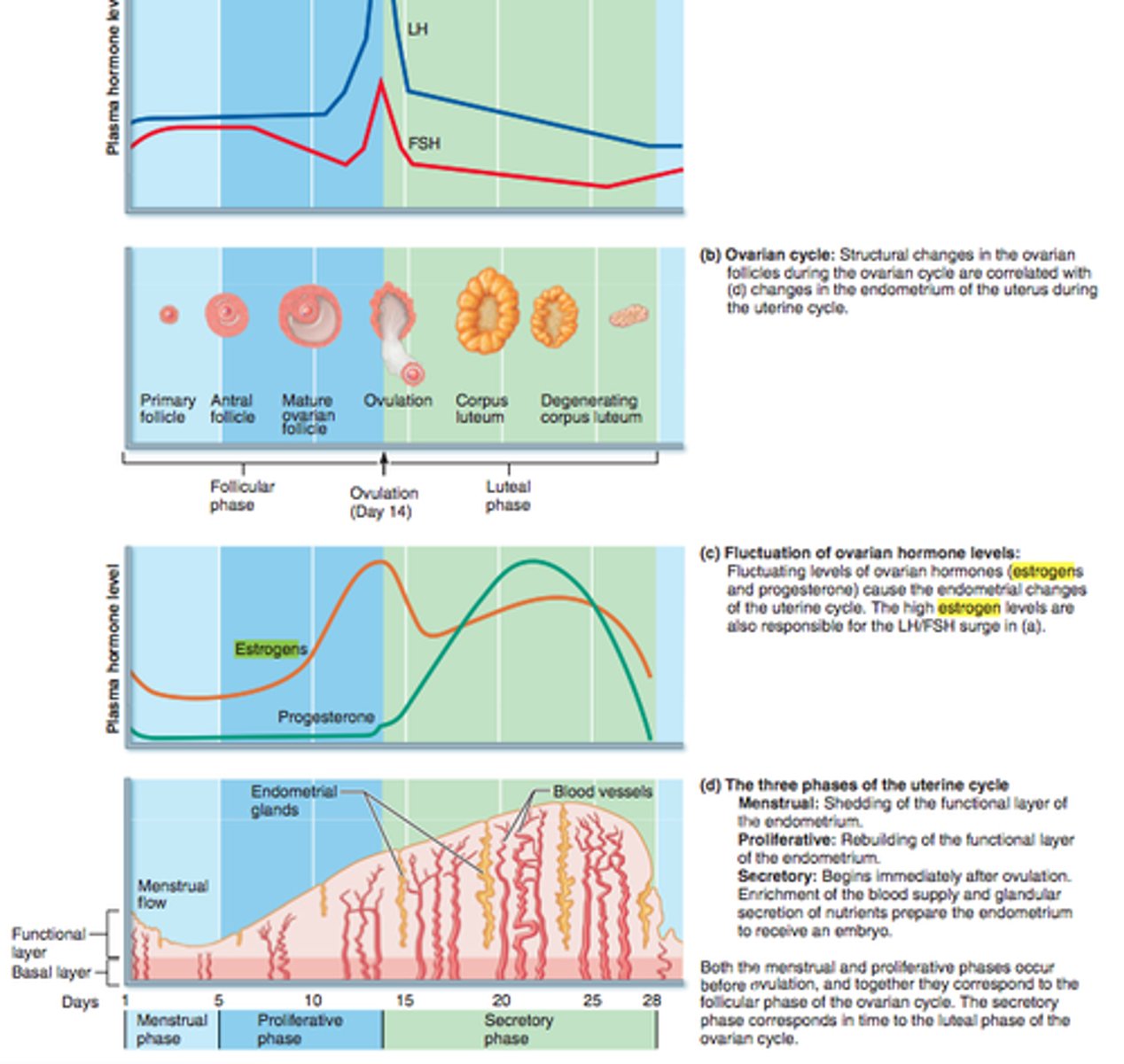
menstrual cycle
consists of a buildup of the endometrium during most of the sexual cycle, followed by its breakdown and vaginal discharge
-proliferative phase, secretory phase, premenstrual phase, and menstrual phase
-First day of noticeable vaginal discharge is defined as day 1 of the sexual cycle... Average: 5 days
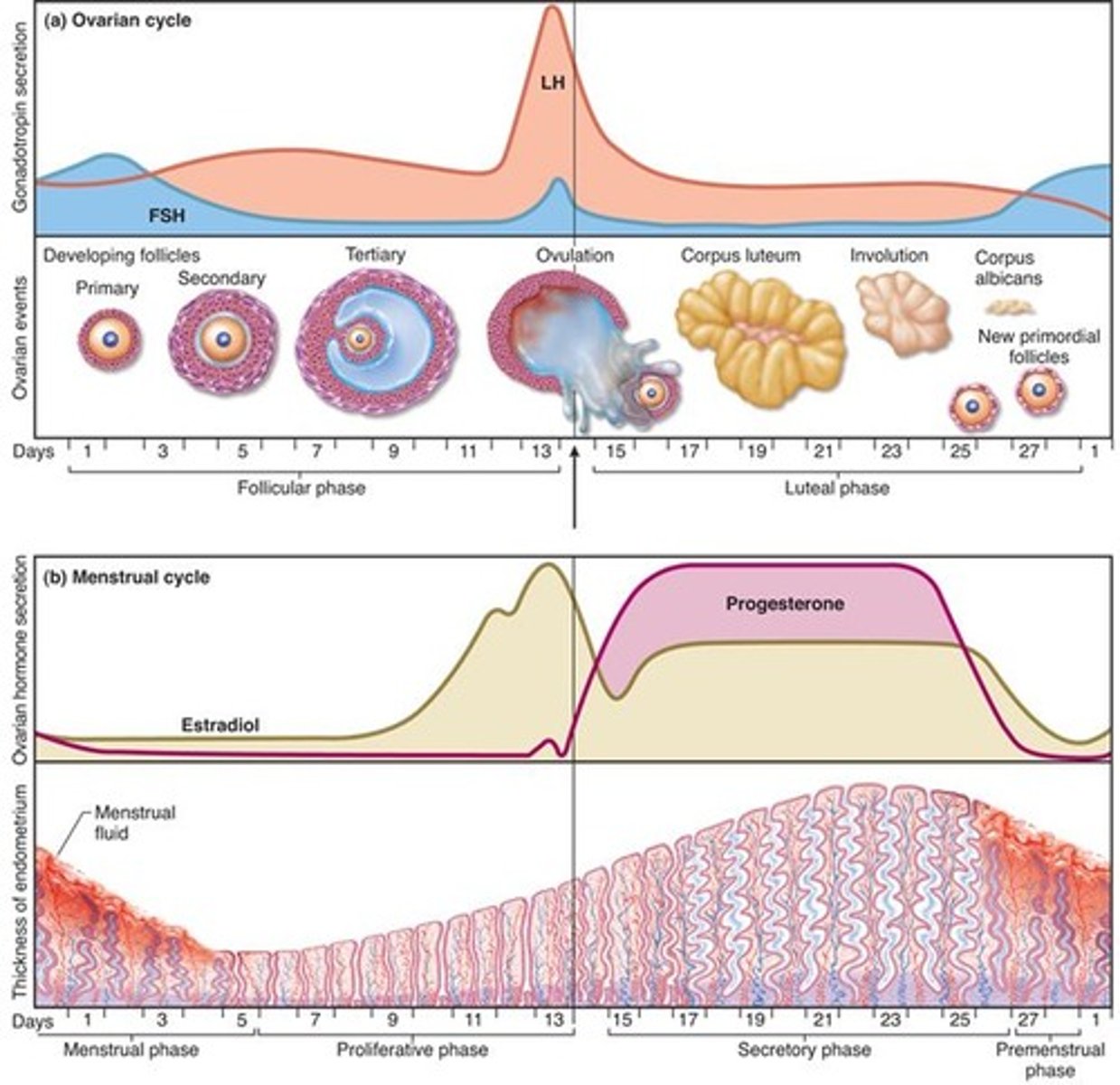
1. Proliferative phase
layer of endometrial tissue (stratum functionalis) lost in last menstruation is rebuilt
-At day 5 of menstruation, the endometrium is about 0.5 mm thick
-Consists only of stratum basalis
-As new cohort of follicles develops, they secrete more and more estrogen
-Estrogen stimulates mitosis in the stratum basalis and the prolific regrowth of blood vessels regenerating the functionalis
-By day 14, it is 2 to 3 mm thick
-Estrogen also stimulates endometrial cells to produce progesterone receptors (Get ready for progesterone!)
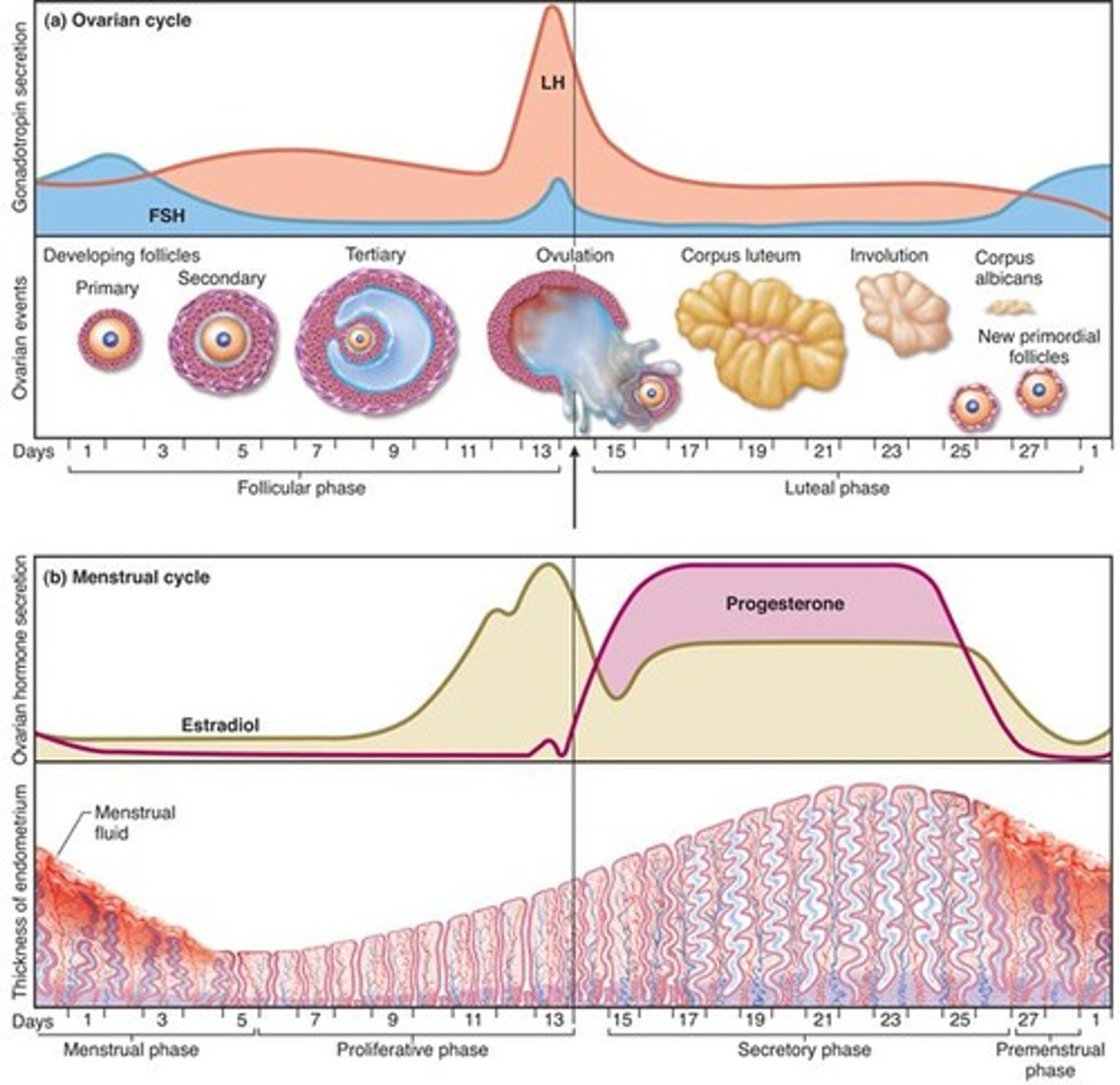
2. Secretory phase
endometrium thickens still more in response to progesterone from corpus luteum
-Day 15 to day 26
-Secretion and fluid accumulation rather than mitosis
-Progesterone stimulates endometrial glands to secrete glycogen
-Glands grow wider, longer, and more coiled
-Endometrium 5 to 6 mm thick
-Soft, nutritious bed available for embryonic development
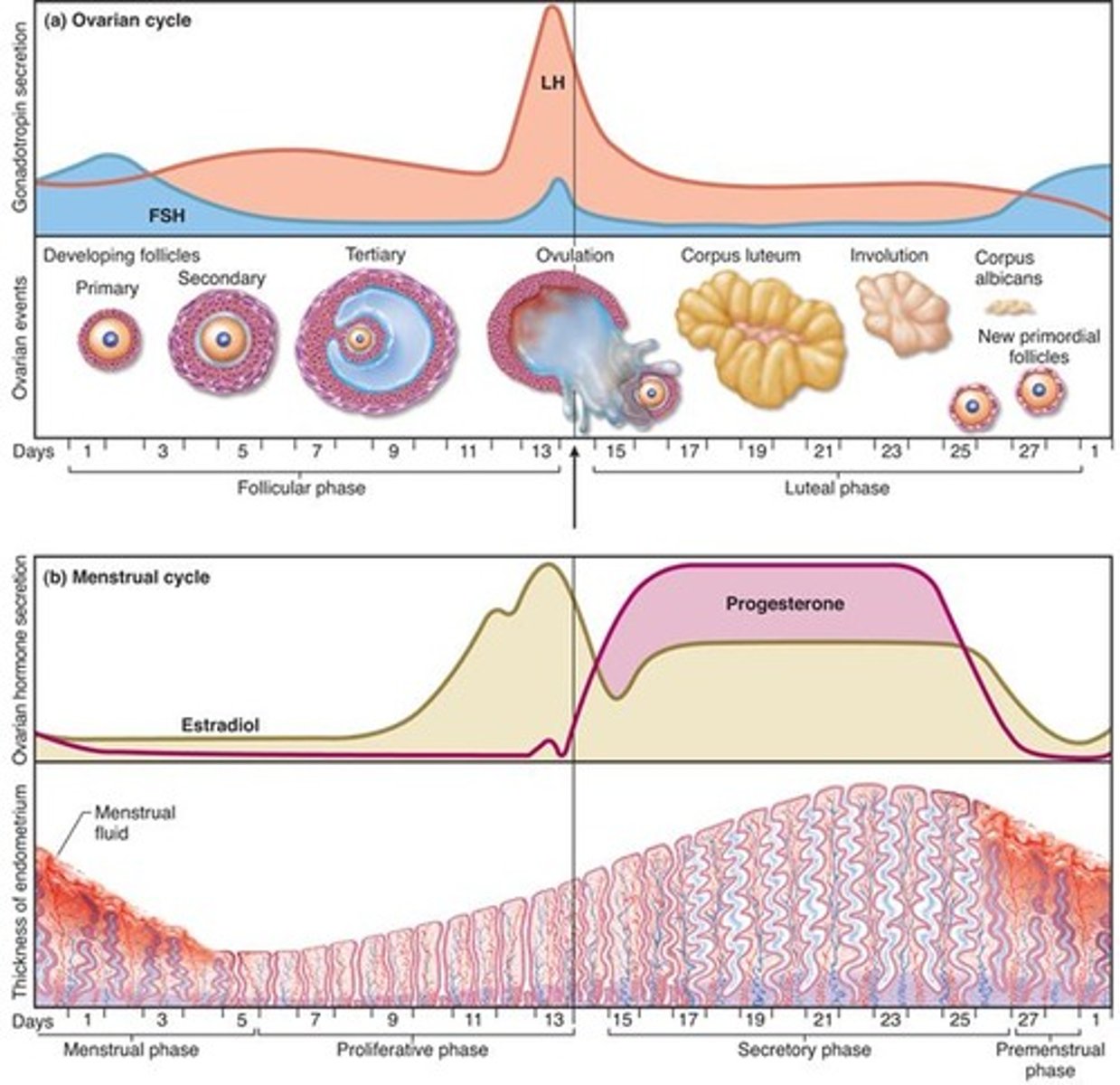
3. Premenstrual phase
period of endometrial degeneration
-Last 2 days of the cycle
-Corpus luteum atrophies and progesterone levels fall sharply
-Triggers spasmodic contractions of spiral arteries
-Causes endometrial ischemia (interrupted blood flow)
-Brings about tissue necrosis and menstrual cramps
-Pools of blood accumulate in stratum functionalis
-Necrotic endometrium mixes with blood and serous fluid: menstrual fluid
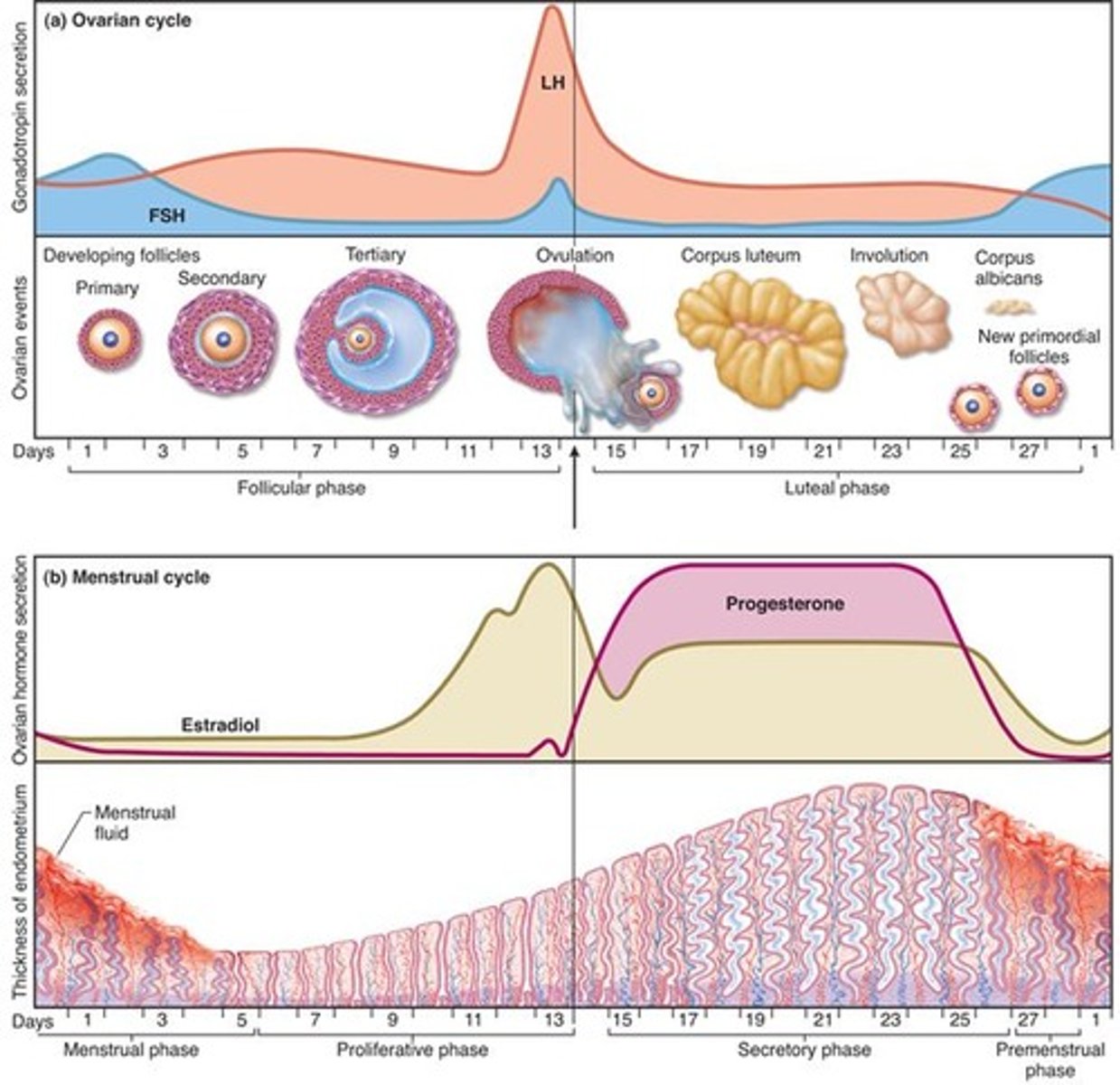
4. Menstrual phase
discharge of menstrual fluid from the vagina (menses)
First day of discharge is day 1 of the new cycle
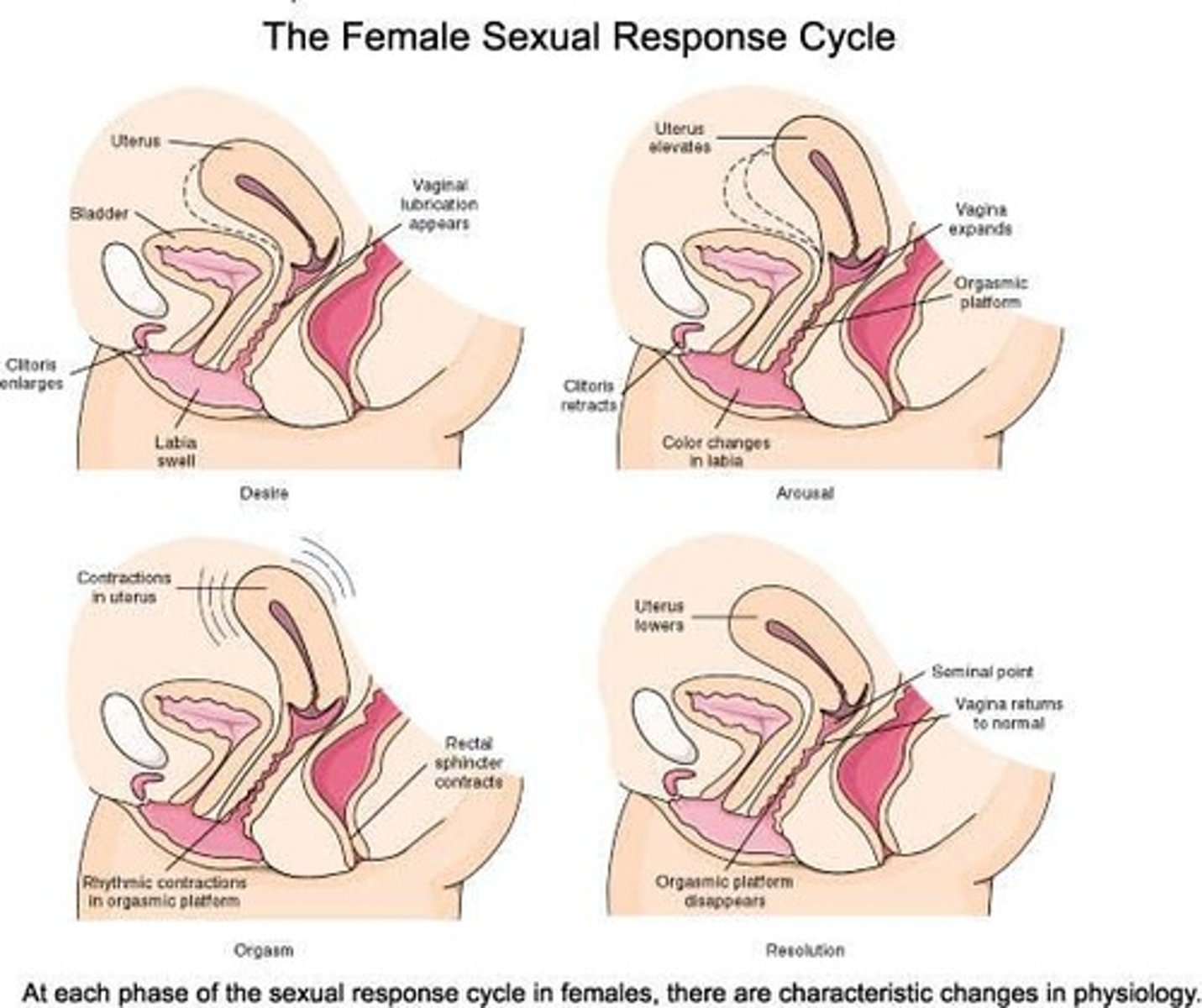
female sexual response
-slide 64
unstimulated, excitement, plateau, orgasm, resolution
-no refractory period
gestation
pregnancy
-Lasts an average of 266 days from conception to childbirth
-Gestational calendar measured from first day of the woman's last menstrual period (LMP)
a. Birth predicted 280 days (40 weeks) from LMP
-Term: the duration of pregnancy
-Trimester: the three 3-month intervals in the term
conceptus
all products of conception: the embryo or fetus, the placenta, and associated membranes
-Blastocyst: the developing individual is a hollow ball for the first 2 weeks
-Embryo: from day 16 through 8 weeks
-Fetus: from beginning of week 9 to birth
•Attached by way of an umbilical cord to a disc-shaped placenta
---Provides fetal nutrition and waste disposal, secretes hormones that regulate pregnancy, mammary development, and fetal development
-Neonate: newborn to 6 weeks
Hormones with strongest influence on pregnancy are:
-Estrogens
-Progesterone
-Human chorionic gonadotropin
-Human chorionic somatomammotropin
4 hormones primarily secreted by the placenta
-Corpus luteum is important source for first several weeks
-If corpus luteum removed before 7 weeks, abortion
-From week 7 to week 17, the corpus luteum degenerates and placenta takes over its endocrine function
1. Human chorionic gonadotropin (HCG)
a. Secreted by blastocyst and placenta
b. Detectable in urine 8 to 9 days after conception by home pregnancy test kits
c. Stimulates growth of corpus luteum
-Secretes increasing amounts of progesterone and estrogen
2. Estrogens
a. Increases to 30 times normal by the end of gestation
b. Corpus luteum is source for first 12 weeks until placenta takes over gradually during weeks 7 to 17
c. Causes tissue growth in the fetus and the mother
-Mother's uterus and external genitalia enlarge
-Mammary ducts grow, breasts increase to nearly twice normal size
-Relaxes pubic symphysis and widens pelvis
3. progesterone
-Secreted by placenta and corpus luteum
-Suppresses secretion of FSH and LH, preventing follicular development during pregnancy
-Suppresses uterine contractions
-Prevents menstruation, thickens endometrium; Promotes proliferation of decidual cells of the endometrium on which the blastocyst feeds
-Stimulates development of acini in breast in another step toward lactation
4. Human chorionic somatomammotropin (HCS)
a. Placenta begins its secretion about week 5
-Increases steadily until term in proportion to placental size
-Effects seem similar to growth hormone, but weaker
-Seems to reduce the mother's insulin sensitivity and glucose usage, leaving more for the fetus
A few other hormones of pregnancy: parathyroid, aldosterone, relaxin
1. Parathyroid glands enlarge and increase osteoclast activity
-Provides calcium from Mom's bones for fetal use
2. Aldosterone secretion rises, promoting fluid retention and increasing mother's blood volume
3. Relaxin, secreted by corpus luteum and placenta
-Synergizes progesterone in stimulating the multiplication of decidual cells
-Promotes growth of blood vessels in the pregnant uterus
Describe a woman's bodily adaptations to pregnancy.
Adjustments to Pregnancy- digestive system
a. Morning sickness: nausea especially arising from bed in first few months of gestation
-Unknown cause
b. Constipation and heartburn due to:
-Reduced intestinal motility
-Pressure on stomach causing reflux of gastric contents into esophagus
Adjustments to Pregnancy- metabolism
Basal metabolic rate (BMR): rises about 15% in second half of gestation
-Appetite may be strongly stimulated
-Healthy average weight gain: 24 lb
Adjustments to Pregnancy- circulatory system
a. By full term, placenta requires 625 mL of blood per minute from the mother
b. Mother's blood volume rises about 30% during pregnancy
-Due to fluid retention and hemopoiesis
-Mother has about 1 to 2 L of extra blood
c. Mother's cardiac output rises 30% to 40% above normal by week 27
-Falls almost to normal during the last 8 weeks
d. Pregnant uterus puts pressure on large pelvic blood vessels: interferes with venous return from legs
-Can result in hemorrhoids, varicose veins, and edema of the feet
Adjustments to Pregnancy- respiratory system
a. Respiratory rate remains constant
-But.....Tidal volume and minute ventilation increase about 40%
b. Two reasons:
1. Oxygen demand rises in proportion to the woman's increase in metabolic rate and the increasing needs of the fetus
2. Progesterone increases the sensitivity of the woman's chemoreceptors to carbon dioxide
-Ventilation is adjusted to keep her arterial Pco2 lower than normal
-Promotes CO2 diffusion from fetal bloodstream into maternal blood
-"Air hungry" from pressure on the diaphragm from growing uterus
-Breathes more easily in the last month due to pelvic expansion, causing the fetus to drop lower in the pelvic cavity, and thus taking pressure off diaphragm
Adjustments to Pregnancy- urinary system
a. Aldosterone and the steroids of pregnancy promote water and salt retention by the kidneys
b. Glomerular filtration rate increases 50% and urine output is slightly elevated
-Enables the woman to dispose of both her own and the fetus's metabolic wastes
c. Pregnant uterus compresses the bladder and reduces its capacity
-Frequent urination and uncontrollable leakage of urine (incontinence)
Adjustments to Pregnancy- integumentary system
a. Skin grows to accommodate expansion of abdomen and breasts
b. Added fat deposition in hips and thighs
c. Striae or stretch marks can result from tearing the stretched connective tissue
-Reddish at first, but fade after pregnancy
d. Melanocyte activity increases in some areas
-Darkening of the areolae and linea alba (linea nigra)
e. Temporary blotchy darkening of the skin over the nose and cheeks
-"Mask of pregnancy" or chloasma
-Disappears after pregnancy
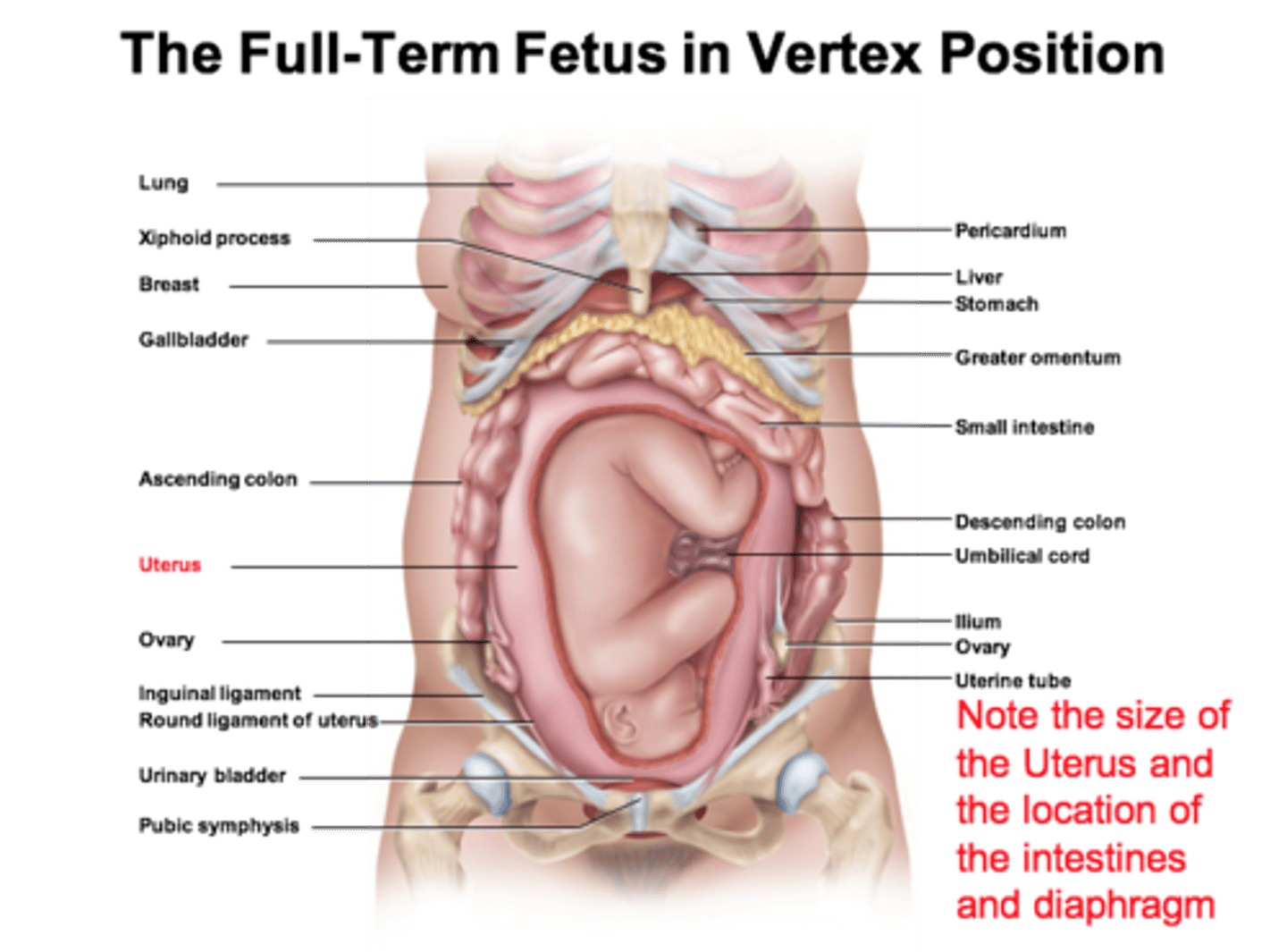
In the seventh month of gestation, the fetus normally turns into the head-down ________ __________
vertex position
fetus is a _________ ________ in its own birth
passive player
-Expulsion achieved by contractions of mother's uterine and abdominal muscles
-Fetus may play a role chemically by stimulating labor contractions
-Sending chemical messages that signify when it is developed enough to be born
Braxtion Hicks contractions
relatively weak contractions of the uterus over the course of gestation ("practice contractions")
-Strengthen late in pregnancy: false labor
-Contractions transform suddenly into more powerful labor contractions
parturition
the process of giving birth
-Marked by the onset of true labor contractions
Progesterone and estradiol/estrogen balance may be one factor in this pattern of increasing contractility
-which declines and which increases?
-Progesterone inhibits uterine contractions, but declines after 6 months
-Estradiol stimulates uterine contractions, and continues to rise
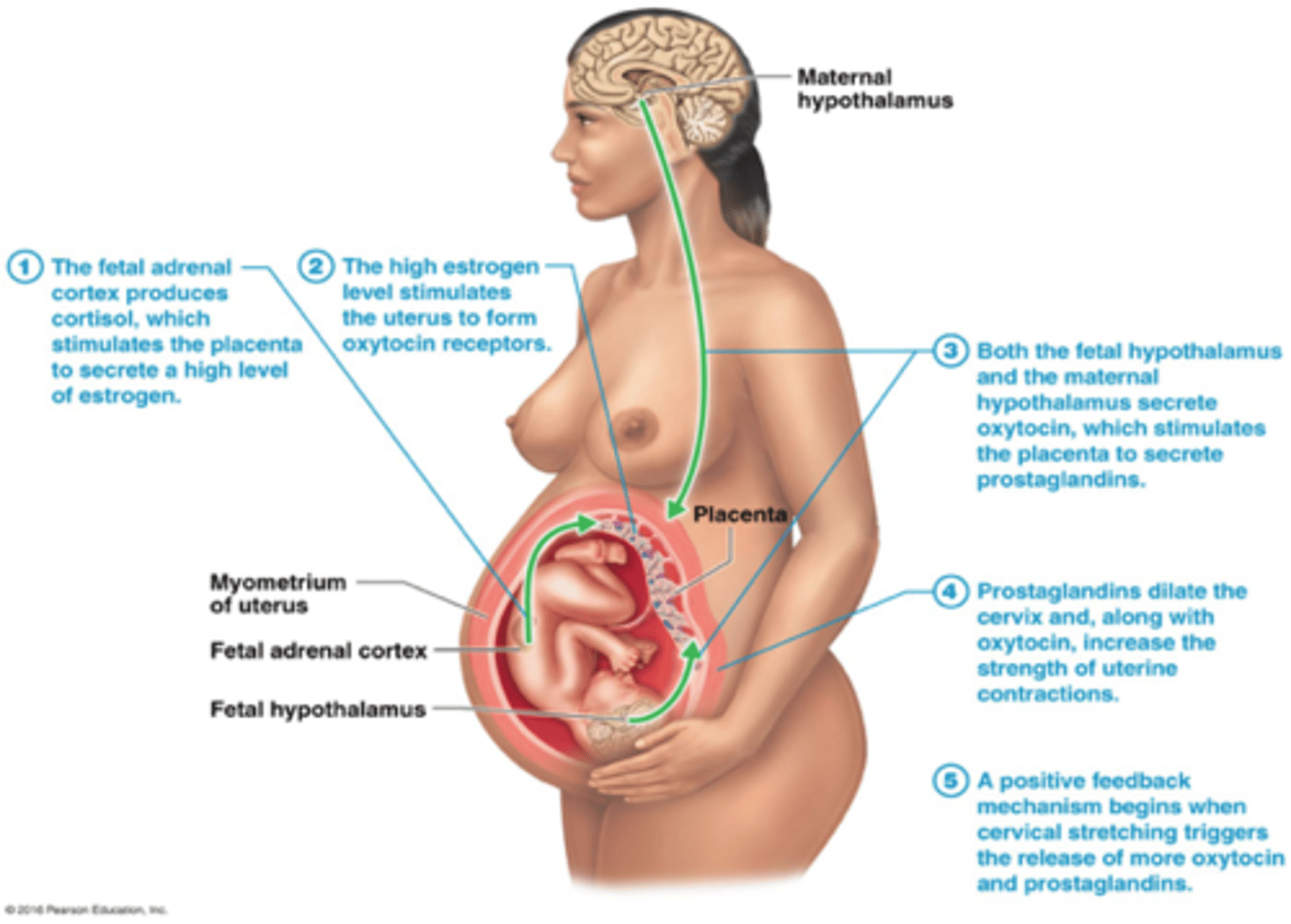
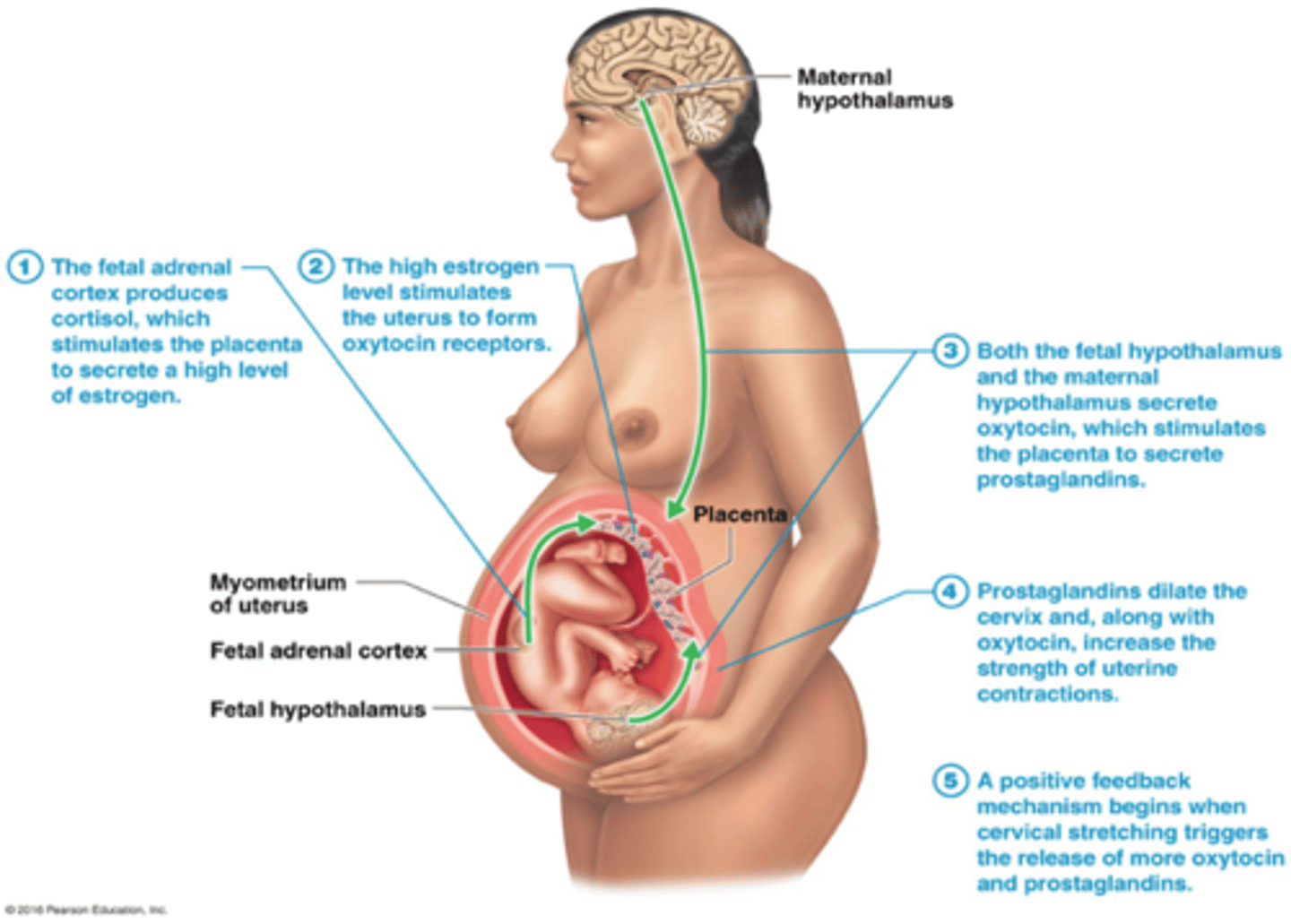
As pregnancy nears full term, posterior pituitary releases more _______________, uterus produces more OT receptors
oxytocin (OT)
-promotes labor in two ways:
1. Directly stimulates muscles of myometrium
2. Stimulates fetal membranes to produce prostaglandins, which are synergists of oxytocin in producing labor contractions
_______ ______________ begin about 30 minutes apart and eventually occur every 1 to 3 minutes
Labor contractions
a. Periodically relax to increase blood flow and oxygen delivery to placenta and fetus
b. Contractions strongest in fundus and body of uterus
-Weakest in the cervix
-Pushes fetus downward
with labor contractions woman feels need to "____ ______"
bear down
-Contraction of these muscles aids in expelling the fetus
-Especially when combined with the Valsalva maneuver for increasing intra-abdominal pressure
Pain of labor is due at first mainly to _________ __ ___ ________
ischemia of the myometrium
-Muscles hurt when they are deprived of blood
-Each contraction temporarily restricts uterine circulation
As fetus enters the vaginal canal, the pain becomes stronger
-Stretching of the cervix, vagina, and perineum
-Sometimes tearing of the vaginal tissue
-Episiotomy may be necessary: an incision in the vulva to widen the vaginal orifice to prevent random tearing
Labor occurs in three stages
1.Dilation
2.Expulsion
3.Placental stage
-can be longer in primipara (first timers)
-shorter in multipara (2nd+ timers)
1. Dilation stage
a. Dilation stage, longest stage—lasting 8 to 24 hours
b. Dilation of cervical canal and effacement (thinning) of cervix to reach 10 cm, the diameter of fetal head
c. Rupture of fetal membranes and loss of amniotic fluid
-"Breaking of the waters"
d. Late dilation—dilation reaches 10 cm in 24 hours or less in primipara (first baby) and in as little as a few minutes in multipara
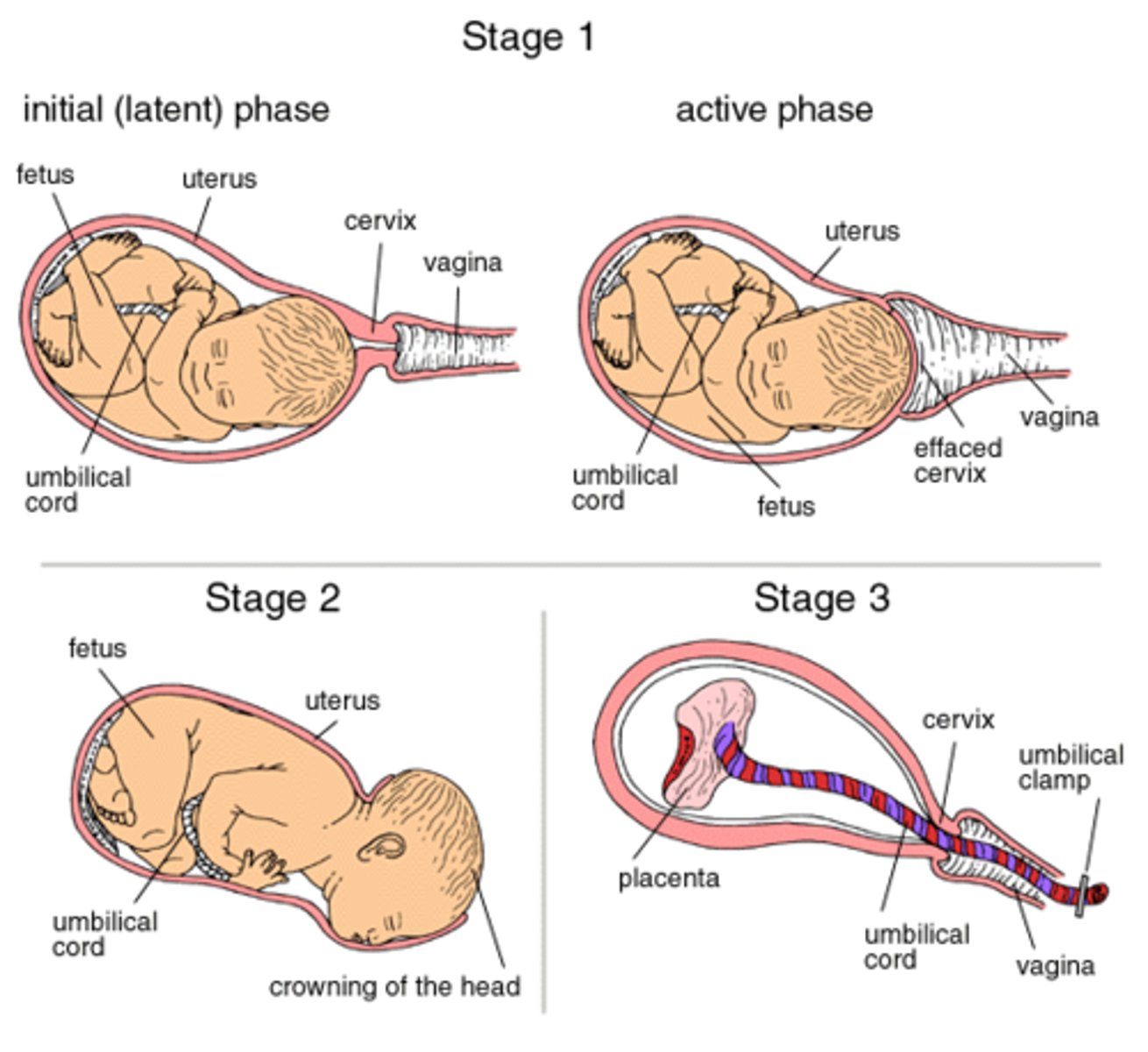
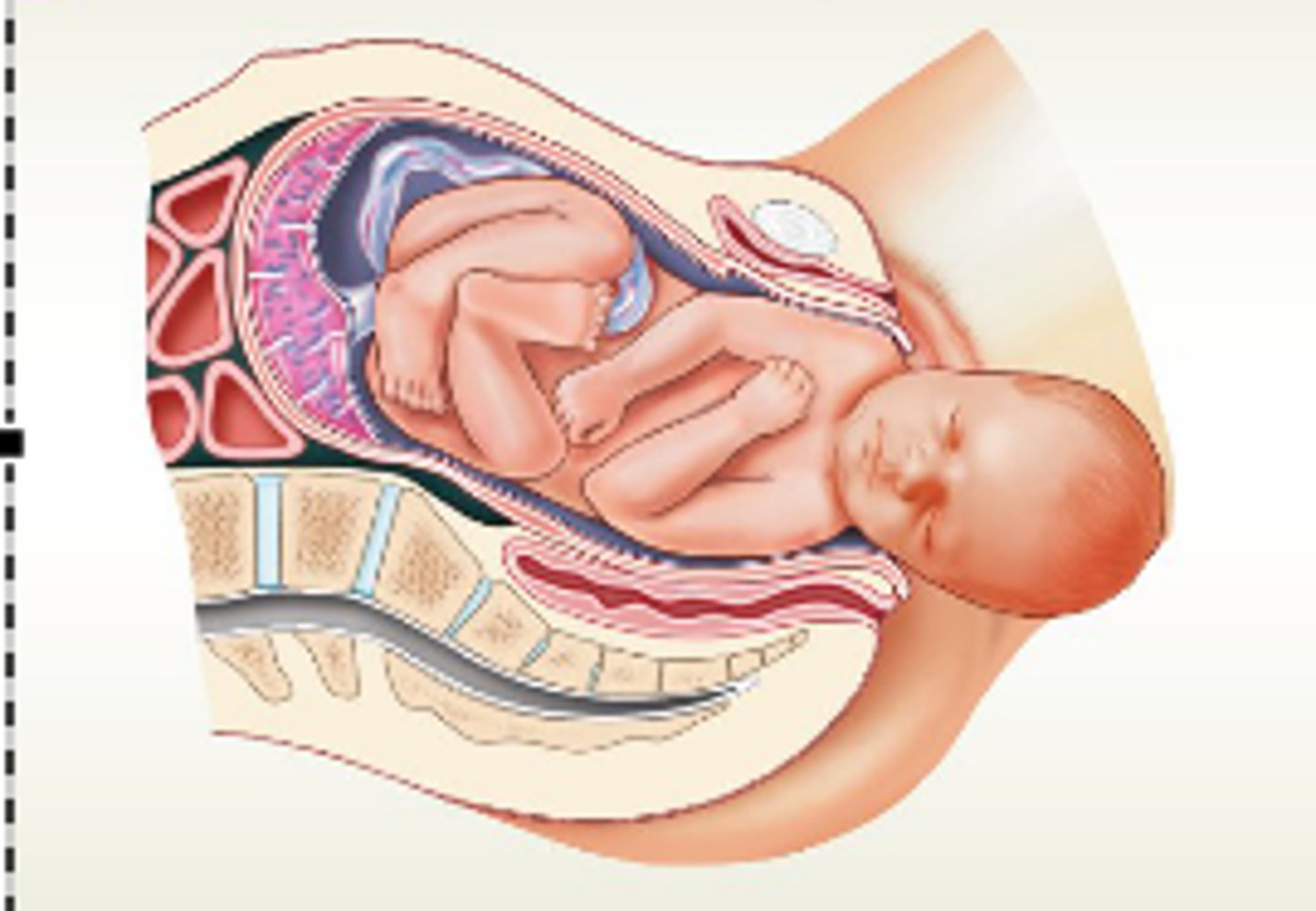
2. Expulsion stage
a. Expulsion begins when baby's head enters vagina and lasts until baby is expelled, up to 30 minutes
b. Crowning—when the baby's head is visible
-Delivery of the head is the most difficult part
-Nose and mouth suctioned before delivery to clear airway
c. After expulsion, attendant drains blood from umbilical vein into baby
-Clamps umbilical cord in two places; cuts cord between clamps
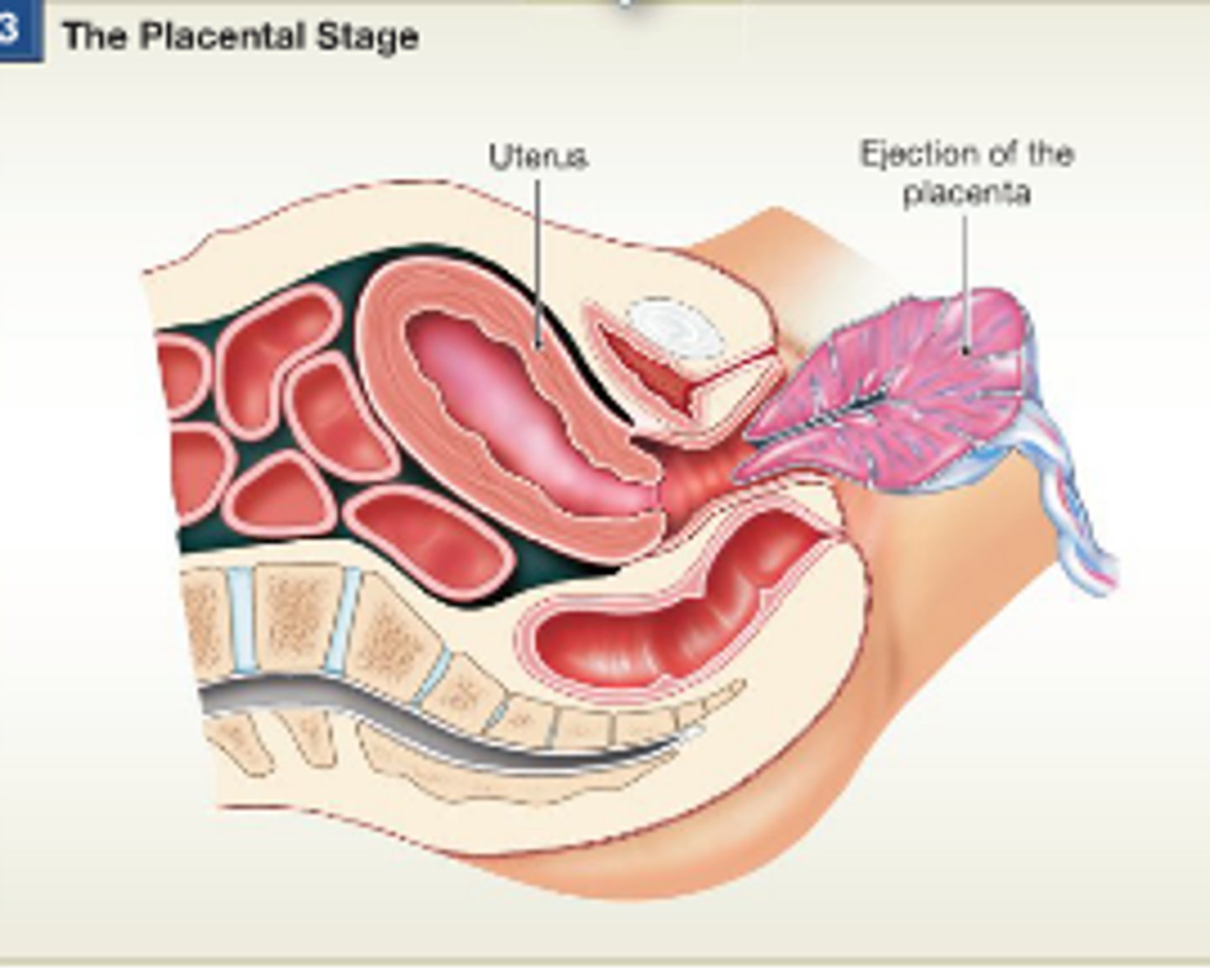
3. Placental stage
a. Uterine contractions continue causing placental separation
b. Membranes (afterbirth) inspected to be sure everything has been expelled
puerperium
First 6 weeks postpartum
-Period in which the mother's anatomy and physiology stabilize and the reproductive organs return nearly to the pregravid state (condition prior to pregnancy)
a. Involution—shrinkage of the uterus
-Loses 50% of its weight in the first week
-Involution is achieved by autolysis (self-digestion) of uterine cells by their own lysosomal enzymes
what promotes involution after birth?
Breast-feeding
-Suppresses estrogen secretion which would make the uterus more flaccid
-Stimulates oxytocin secretion which causes myometrium to contract and firm up the uterus sooner
lactation
the synthesis and ejection of milk from the mammary glands
-Lasts as little as 1 week in women who do not breast-feed their infants
-Can continue for many years as long as the breast is stimulated by a nursing infant or a mechanical device (breast pump)
-Women traditionally nurse their infants until a median age of about 2.8 years
__________ forms in late pregnancy
colostrum
-Similar to breast milk in protein and lactose, but contains 1/3 less fat
-First 1 to 3 days after birth
-Thin watery consistency and a cloudy yellow color
-Contains IgA to protect baby from gastroenteritis
what promotes milk synthesis?
prolactin (from anterior pituitary)
-Inhibited by dopamine when not pregnant
-Synthesis of hormone begins 5 weeks into pregnancy, by full term it is 10 to 20 times normal level; Little effect on mammary glands until after birth
-Steroid hormones from placenta oppose prolactin until birth
-Milk synthesis also requires growth hormone, cortisol, insulin, and parathyroid hormone to mobilize necessary amino acids, fatty acids, glucose, and calcium
prolactin levels are fluctuating
a. At birth, prolactin secretion drops to nonpregnancy levels
b. Every time the infant nurses prolactin levels jump to 10 to 20 times this level for the next hour
-Stimulates the synthesis of milk for the next feeding
-Without nursing, milk production stops in 1 week
c. Only 5% to 10% of women become pregnant while breast-feeding
-Inhibition of GnRH and reduced ovarian cycling
-Natural means of spacing births
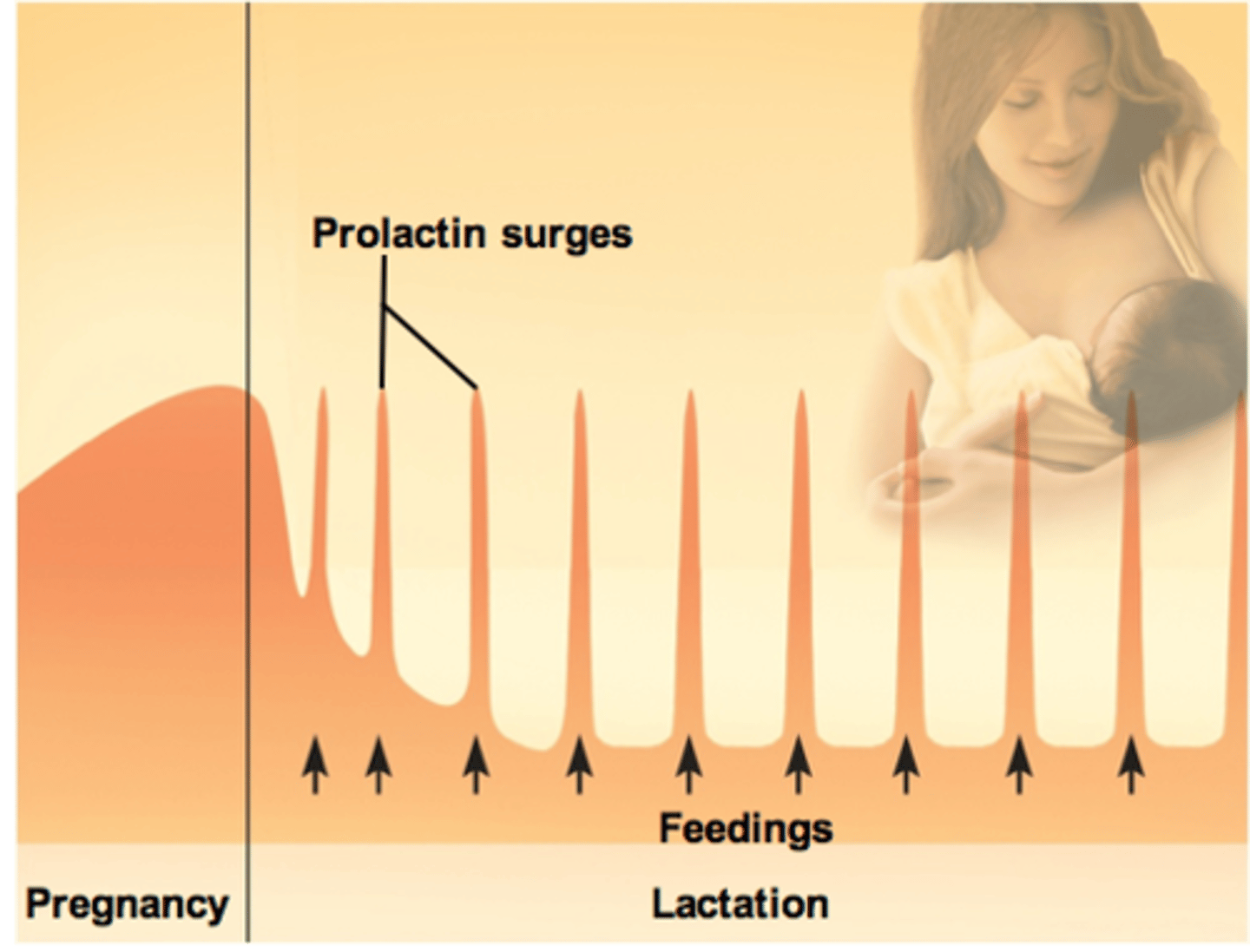
Breast milk changes composition over the first 2 weeks
-Varies from one time of day to another
-At the end of a feeding there is less lactose and protein, but six times the fat
______ _____ is not a good substitute for breast milk
cow's milk
-1/3 less lactose but three times as much protein
-Harder to digest and more nitrogenous waste (diaper rash)
-Not recommended until baby is 1 year old
Colostrum and milk have a laxative effect that clears intestine of ___________ (green, bile-filled fecal material in newborn)
meconium
breast milk supplies...
antibodies and colonizes intestine with beneficial bacteria
-nursing woman can produce 1.5 L per day
What is the female copulatory organ?
vagina
Which portion of the uterus is shed each month during menstruation?
stratum functionalis
What is one of the earliest noticeable signs of puberty in females?
thelarche
How many viable oocytes are produced at the end of meiosis in females?
1