HL Biology Anatomy Unit Review (Basically just LO3: Organisms)
1/149
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
150 Terms
What is quorum sensing?
The method that single-celled organisms used to communicate: each organism secretes their own chemical signals (auto-inducers), once enough organisms are gathered, these signals are detected and processes begin.
What is an example of quorum sensing?
Bioluminescence in the marine bacteria vibrio fischeri:
Once there is enough bacteria, more autoinducers are released
Once there are enough autoinducers, the expression of genes needed for luminescence are signaled (seen in squid).
What are receptors?
Proteins with binding sites for specific signaling chemicals (ligands, ex. hormones, neurotransmitters, drugs, antigens)
Example: Calcium can be a ligand of troponin in order to initiate muscle contraction
What are cytokines?
Ligands that start intracellular signaling to regulate cell function
What are 3 types of hormones?
Proteins, steroids, amines
What are 5 types of neurotransmitters?
Amines (ex. dopamine), peptides (ex. endorphins), nitrous oxide, acetylcholine, purines (ex. atp)
What are intracellular receptors?
Receptors that reside inside the cell membrane and usually affect gene expression
(ex. Sex hormones bind to intracellular receptors that initiate changes in gene expression - sex hormones are steroids (lipids) so they are hydrophobic, passing easily through the membrane)
What are transmembrane receptors?
Receptors that must have hydrophobic AND hydrophilic regions to stay embedded in the cell membrane.
What are signal transduction pathways?
The binding of a signaling chemical to a receptor that sets off a sequence of responses in the cell - the process that transmembrane receptors rely on, since they are stuck in place.
What are three examples of how transmembrane receptors work (signal transduction pathways)?
G protein-coupled receptors: G protein disassembles itself into 3 subunits after ligands bind to the receptors: alpha, beta, gamma. These subunits then initiate cellular responses.
Epinephrine binds to G protein-coupled receptors in liver cells. This pathway modifies ATP to make cylic AMP (cAMP) → glycogen break down activates → glucose released into blood → faster fight/flight response
Insulin binds to transmembrane receptors, whose tails located inside the cell are enzymes called tyrosine kinase. Binding initiates the formation of glucose transporters on the membrane to increase intake of glucose into cell.
What causes intersex phenotypes in reproduction?
Minor adjustments in the complex series of genes + hormones that control the development of sex organs
How do male sex organs develop?
The SRY gene on the Y chromosome codes for the Teste Determining Factor (TDF) protein, which causes embryonic gonads to develop into testes.
Testes develop testosterone secreting glands around 8 weeks, increased testosterone in puberty signals development of sperm
How do female sex organs develop?
If the SRY gene is not present, gonads develop into ovaries from maternal estrogen and progesterone. Estrogen and progesterone increase during puberty, signalling development of the menstrual cycle
Using a graph, describe the presence of different hormones involved in the menstrual cycle
Estrogen spikes before ovulation
Right before day 14, Luteinizing hormones (LH) and Follicle Stimulating Hormone (FSH) spike, which is where ovulation occurs.
Near day 21, progesterone and estrogen spike
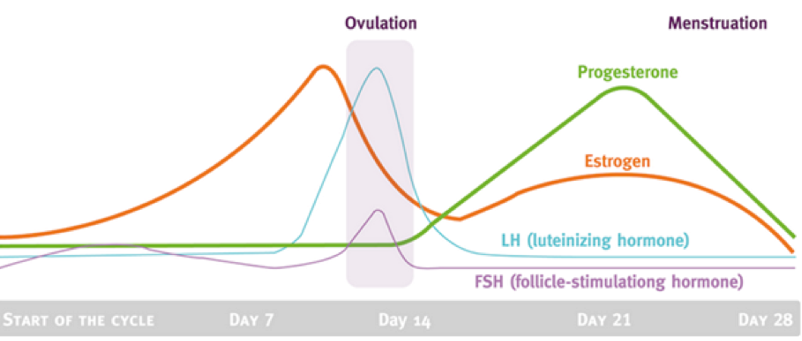
At which point of the menstrual cycle are females most fertile?
During ovulation when an egg is released into the oviduct (~days 10-17)
What are two examples of ovarian hormones? Pituitary hormones?
Ovarian: Estrogen, Progesterone
Pituitary Hormones: LH, FSH
Describe the follicular phase of the menstrual cycle
Occurs the first day right after menstruation
FSH signals estrogen increase → endometrium thickens
FSH present → increased follicle growth → more estrogen is released from follicles
Increased FSH → increased estrogen → increase in LH release
Increased LH → increased follicular wall size → even more estrogen releaseOVULATION: LH spikes, the most developed follicle grows and ruptures, releasing its ovum into the oviduct
When estrogen is highest, it inhibits LH and FSH , allowing progression to the luteal phase
Describe the luteal phase of the menstrual cycle
The endometrium continues to thicken
Ruptured follicle differentiates, becoming a corpus luteum that releases estrogen and progesterone → progesterone maintains the endometrium
New hormones inhibit LH and FSH until the next cycle
If no fertilization, the corpus luteum breaks down → decreased progesterone and estrogen → endometrium breaks down
The endometrium sheds during menstruation
What are characteristics of both spermatogenesis and oogenesis?
Mitosis, cell growth, 2 meiotic divisions, differentiation
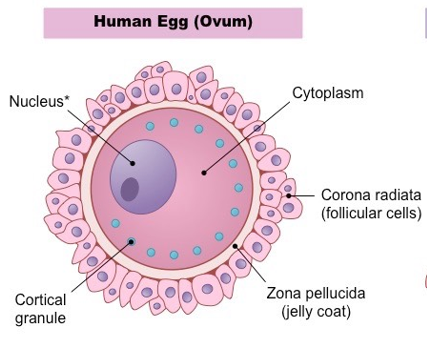
Describe the structure of an ovum
*note, condensed nucleus is not actually present because ovum development stops in metaphase II, only there to represent the presence of haploid genetic material
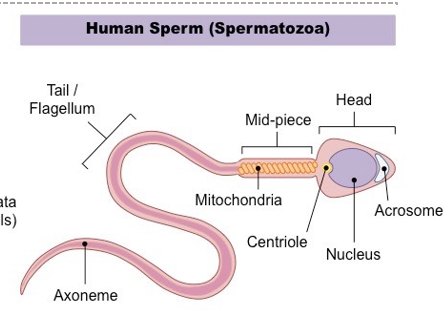
Describe the structure of a spermatozoa
Describe the structure of the seminiferous tubules
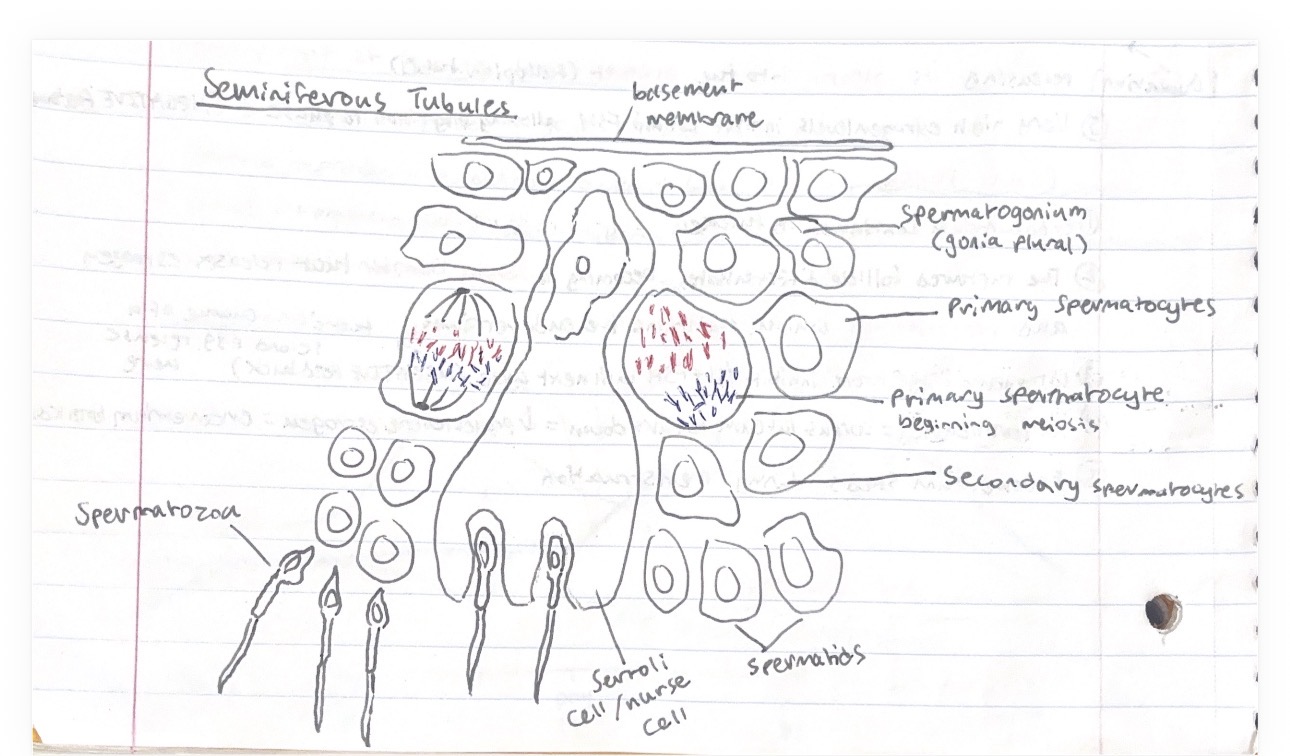
Describe the steps of spermatogenesis
Begins in the outer part of the seminiferous tubules and progresses inwards towards the lumen
Spermatogonia are diploid germinal epithelial cells beneath the basement membrane. These divide by mitosis into either more spermatogonia or primary spermatocytes
Formation of primary spermatocytes begins 1st meiosis, forming 2 haploid secondary spermatocytes
Secondary spermatocytes undergo 2nd meiosis, becoming 4 haploid spermatids
Spermatids are attached to sertoli cells which help them differentiate into mature spermatozoa
Once spermatozoa develop tails, they detach from sertoli cells and get carried down the lumen of the seminiferous tubules towards the epididymis
Describe the steps of oogenesis
Begins in utero by the developing female fetus. Diploid germinal cells in the fetal ovary divide by mitosis into oogonia, which are distributed throughout the ovaries
Oogonia develop into primary oocytes, beginning meiosis but stopping at prophase I. This cell is then surrounded by follicle cells, forming a primary follicle.
During menstrual cycle in puberty, a few follicles become oocytes as the first meiotic division produces 2 haploid cells by uneven cytoplasm division to create a secondary oocyte and a small polar body.
The polar body divides and degenerates, the secondary oocyte is protected by the follicle, starting the second meiotic division and stopping at prophase II. The follicle cells divide and produce a liquid that causes follicles to swell.
The follicle cell bursts during ovulation, releasing the secondary oocyte to the oviduct.
Describe the steps of fertilization
The sperm binds to the jelly coat of the ovum
Enzymes are released from the acrosome of the sperm to break down the jelly coat
The sperm nucleus enters the egg (end of the Acrosome Reaction)
The cortical granules in the ovum contain molecules that harden the zona pellucide, making it impermeable to prevent polyspermy (Cortical reaction)
What occurs in the embryo post-fertilization?
Human gonadotropin (hCG) is produced to continue the release of progesterone and estrogen
What hormone do pregnancy tests look for to confirm pregnancy?
Presence of human gonadotropin
What occurs in the placenta post-fertilization?
Allows the exchange of nutrients between mother and fetus, since maternal and fetal blood don’t mix. ALSO secretes progesterone and estrogen
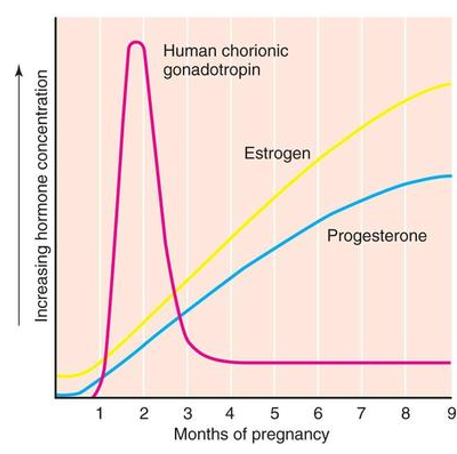
Using a graph, describe the levels of the hormones involved in pregnancy post-fertilization
hCG promotes initial increases of progesterone and estrogen
hCG declines as placenta becomes main secretor of progesterone and estrogen
Describe the positive feedback loop between estrogen and oxytocin during birth
Head of fetus pushes against cervix, transmitting a nerve impulse to the brain that stimulates the pituitary gland to secrete oxytocin
Oxytocin enters the bloodstream and into the uterus
Oxytocin promotes uterine contractions that continues the cycle by pushing the fetus closer to the cervix
What does prolactin do?
A hormone that stimulates milk production
Secreted during and after feed in order to produce the next feed
More is secreted at night
Suppresses ovulation (no more babies right now!)
Suckling promotes prolactin secretion
Central vs. Peripheral Nervous system
Brain + Spinal Cord vs. Everything else away from the brain
Resting Potential
When a neuron is not transmitting an impulse (~70 mV)
Action Potential
Rapid change in polarity on neuron membrane involving depolarization ( - → +) and repolarization ( + → - )
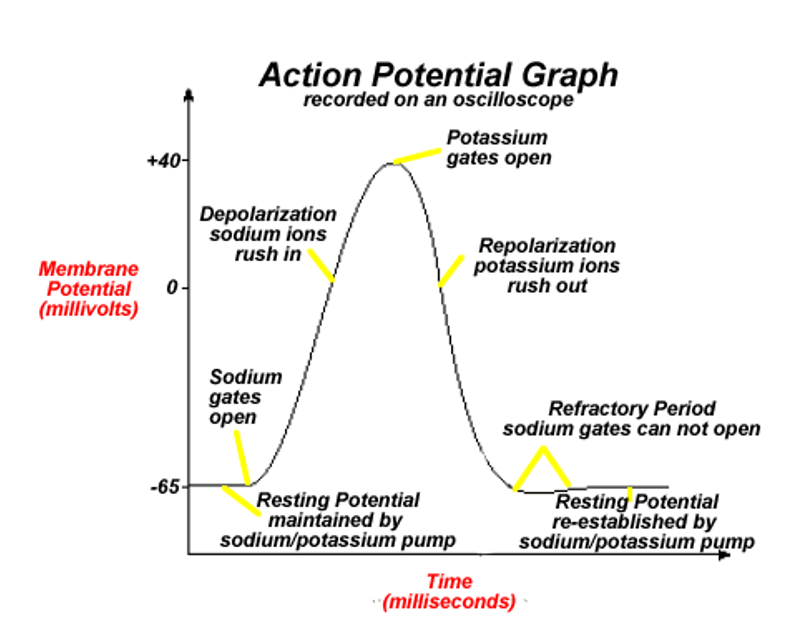
Describe what an action potential/nerve impulse transmission graph looks like at each stage and its shape
Resting potential ~70mV
After reaching threshold potential, Na+ gates open, allowing Na+ in and causing depolarization
K+ Gates open, allowing K+ out and causing repolarization
Neuron moves into refractory period below resting potential
How do charged ions make it past the neuron membrane?
Through facilitated diffusion using ion channels
Why does impulse transmission only occur in one direction?
Channels are voltage-gated, so they only open for certain charges. When the current of ion moves down the neuron, it causes channels to open along the way, through a process called self-propagation (depolarization → gates open → ions let in → more depolarization).
Nerve impulses are carried down the neuron by temporary shifts in electrical charge.
How does the neuron move out of the refractory period?
Na+/K+ pumps regenerate the concentration gradient required for the system to return to resting potential by pumping 3Na+ out and 2K+ back in. This is ACTIVE transport, which is why there are mitochondria in the neurons as well.
What adaptation do nerve fibers have to increase speed of tranmission?
They are myelinated - covered in a phospholipid membrane that insulates the axon, increasing transmission speed because ions can’t escape. Schwann cells form myelin, wrapping around the axon several times to insulate it.
What is saltatory conduction?
When impulses jump from gap to gap on the axon
What are the gaps on the axon called?
Nodes of Ranvier
What are synapses? What is a cholinergic synapse?
Junctions between cells in the nervous system, occurs between: neurons, neurons + receptor cells (forms sensory reception), neurons + effector cells (forms response to stimulus, ex. muscle cells).
Cholinergic synapse specifically involves Acetylcholine (Ach).
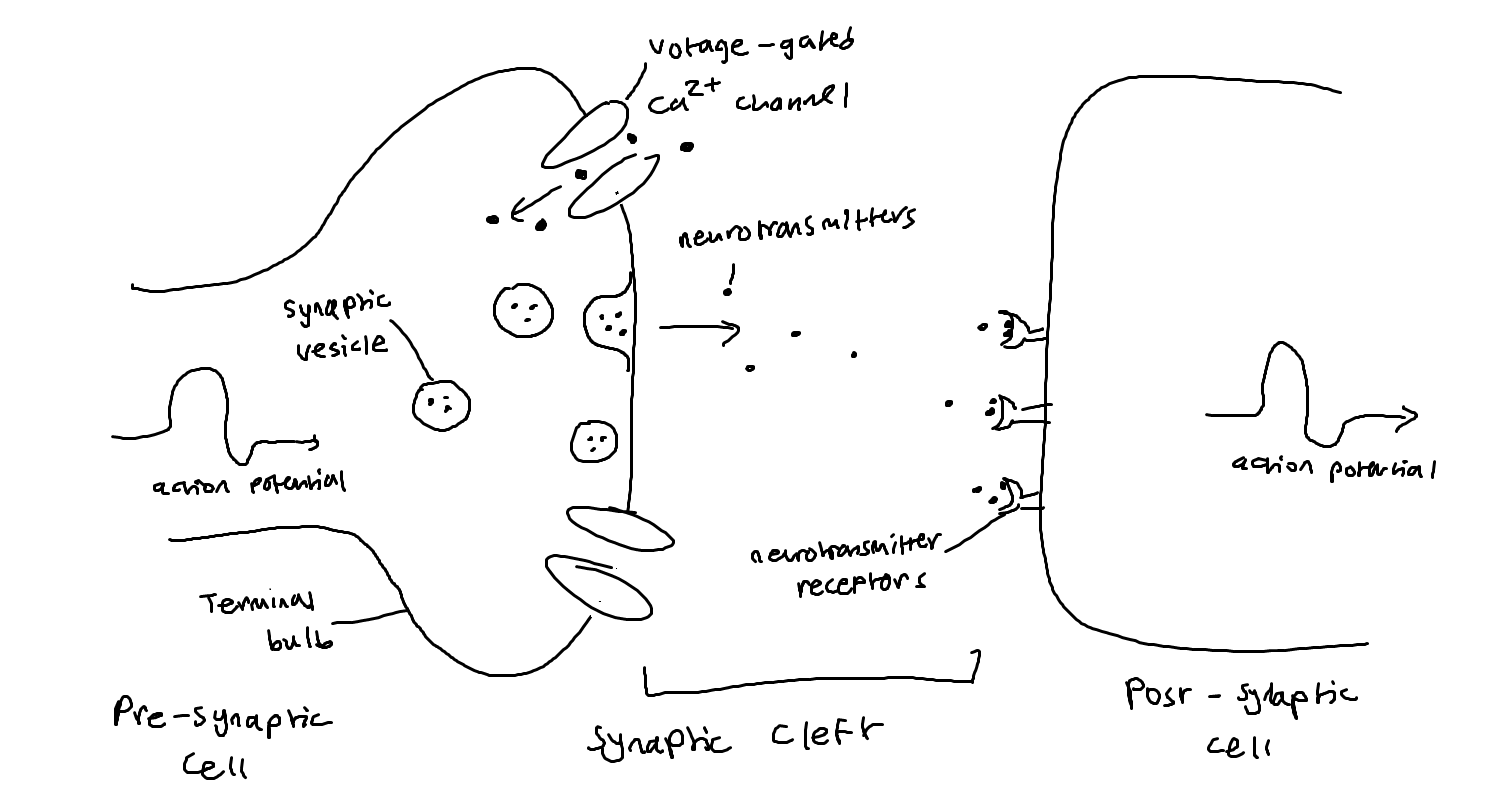
Describe the 6 steps of a synapse occurring between neurons
When pre-synaptic neurons are depolarized, they release a neurotransmitter into the synapse
Depolarization opens the voltage gated Ca+ channels on the presynaptic neuron
Ca+ influx signals synaptic vesicles to fuse with the pre-synaptic cell membrane, releasing neurotransmitters (ex. Ach) by exocytosis
Neurotransmitter diffuses across the synaptic cleft, binding to receptor proteins on the post-synaptic membrane
On the post-synaptic cell, this binding opens Na+ ion channels and an action potential is initiated on post-synaptic neuron
After the neurotransmitter binds, it is then rapidly broken down and reabsorbed by the pre-synaptic neuron (ex. Ach broken down into acetate + choline)
What are exogenous chemicals, and what are two named examples of them?
Substances originating outside an organism that can affect synapses (ex. neonicotinoids, cocaine)
How do neonicotinoids affect synapses?
Neonicotinoids bind to nicotinic acetylcholine receptors, so Ach can’t be binded to it and can’t be broken down by acetylcholinesterase (Ache), causing a buildup of Ach that causes the post-synaptic cell to become paralyzed/overstimulated
Neonicotinoids are used as pesticides because insects have a lot of Ach receptors. It doesn’t affect humans, but may unintendedly affect non-pests.
How does cocaine affect synapses?
Cocaine blocks the reuptake of dopamine into the pre-synaptic cell by blocking dopamine transporters. Since the dopamine remains in the synaptic cleft for longer, its effects are intensified.
True or false: neurons can only synapse with one other neuron, and can only release one type of neurotransmitter
False: multiple pre-synaptic neurons can synapse with another post-synaptic neuron at once, and pre-synaptic cells use two types of neurotransmitters - excitatory and inhibitory
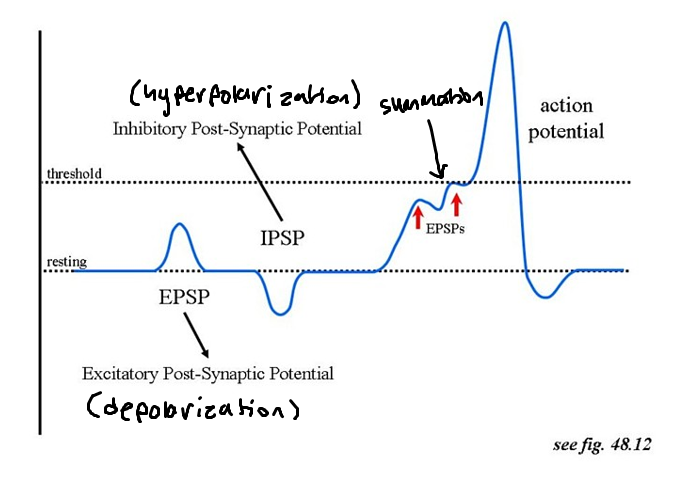
Excitatory vs. Inhibitory neurotransmitters
Excitatory neurotransmitters cause depolarization of the post-synaptic membrane, while inhibitory neurotransmitters cause hyperpolarization of the post-synaptic membrane (refractory period, going too far below charge)
What is summation?
Describes how nerve impulses only initiate if the sum of all inhibitory and excitatory neurotransmitters brings the post-synaptic cell to threshold potential
Describe a diagram of how synapses occur
Describe a graph of how excitatory and inhibitory neurotransmitters affect post-synaptic membrane potential
Describe the parts of a neuron
2
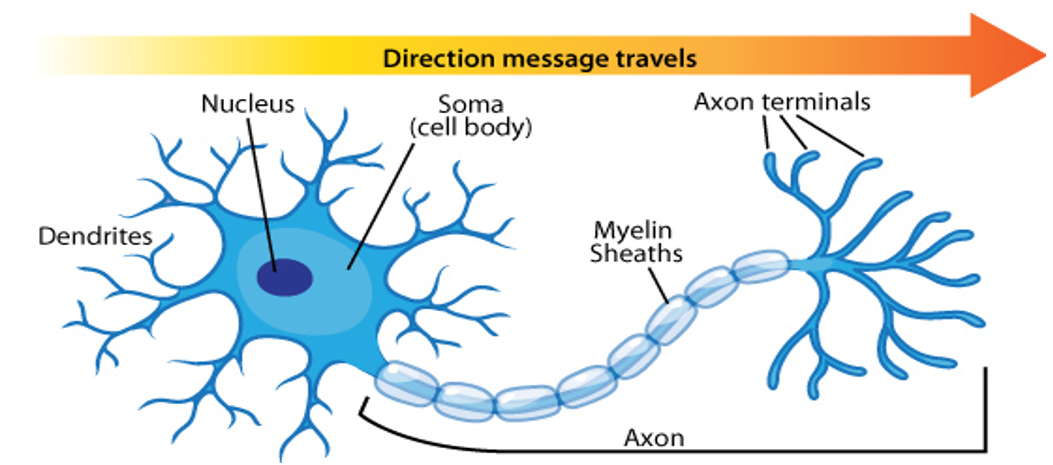
What is the difference between sessile and motile animals?
All animals move. Sessile animals are tethered to a spot while motile animals move freely.
How do muscles work to perform movement?
They attach to bones/exoskeletons to form levers, usually working in antagonistic pairs to perform opposite movements
What adaptations do joints have that reduce friction during movement?
Cartilage: protects areas of contact
Synovial fluid: Fluid held within a joint capsule (a membrane) that lubes joints to reduce friction
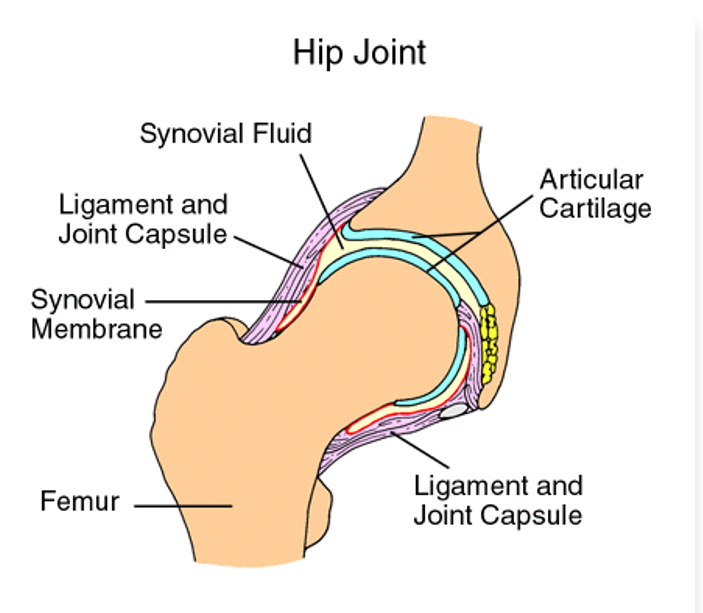
Name the parts of the hip joint
Ligaments: Connect bones
Tendons: Connect bones to muscle
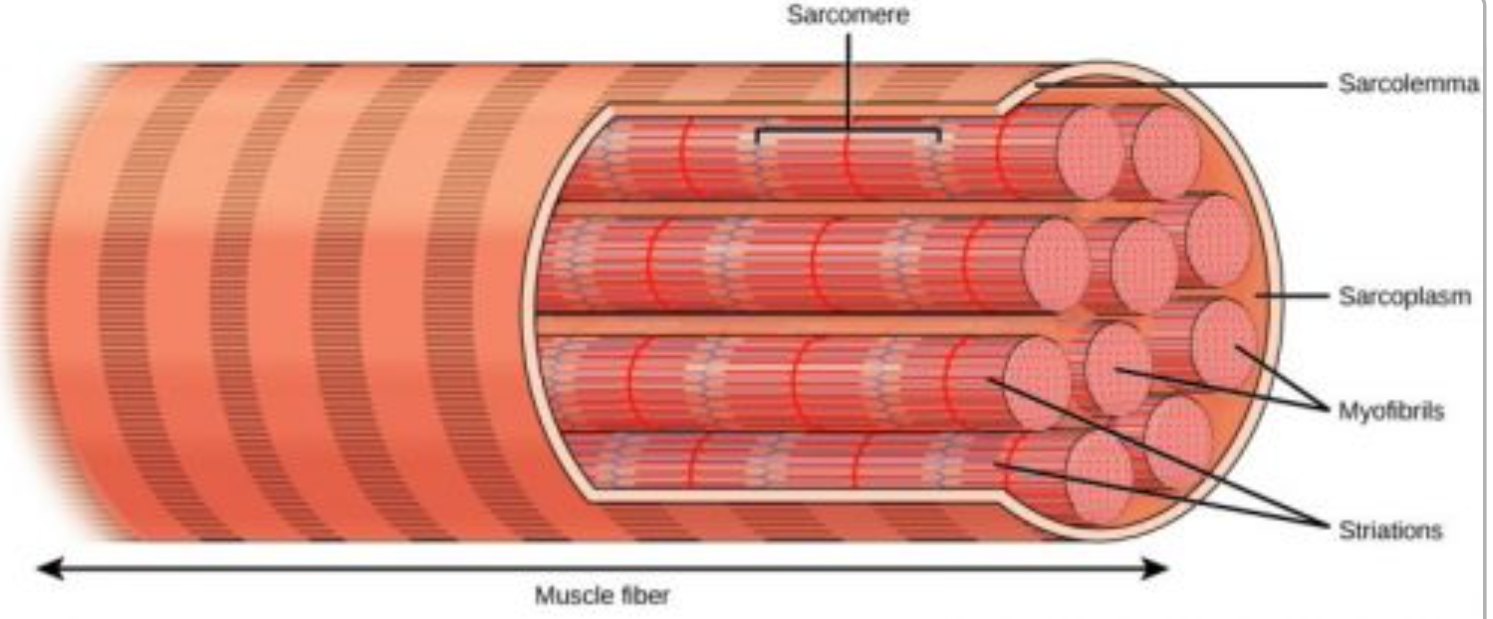
What are the parts of a muscle fiber?
Myofibrils: Smaller fibers that make up one muscle cell
Sarcolemma: Membrane that holds myofibrils together
Sarcoplasmic Reticulum: The endoplasmic reticulum of the muscles that stores calcium and coats every myofibril
Sarcomere: Packet of protein located on myofibrils
Many nuclei: part of the reason why it challenges cell theory because they are a fusion of many stem cells (myoblasts), they’re also very large
What are the parts of a sacromere?
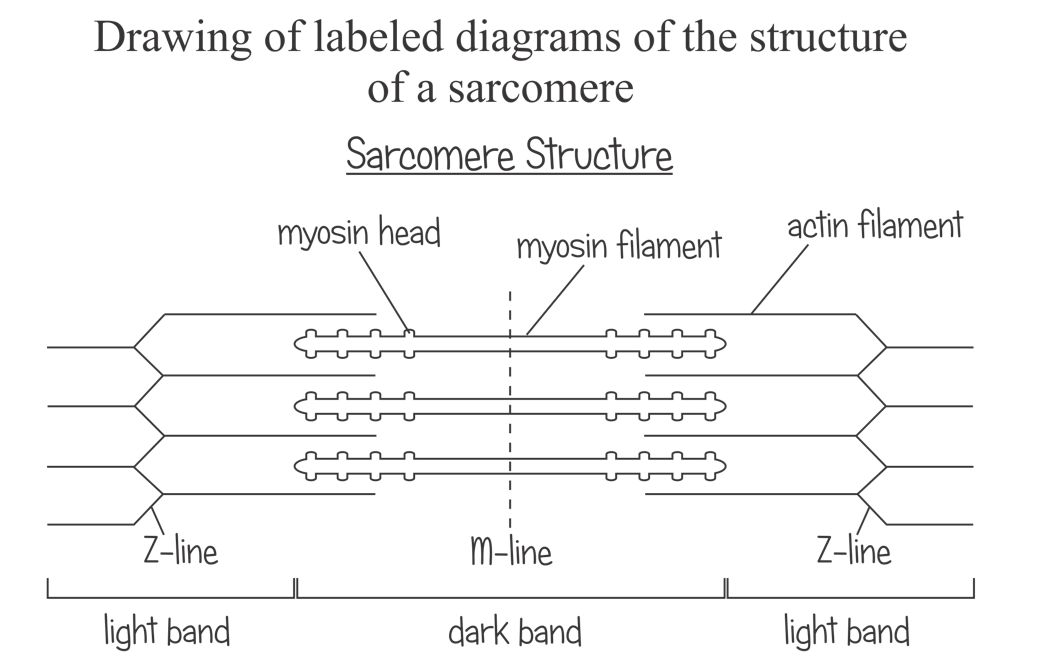
Describe what happens to the sarcomere when muscles move, and what it looks like
When muscles contract, Z-lines get closer together as the myosin heads move actin filaments closer to the M-line
During contraction: The light band will be less visible, and it will be darker around the M-line. The Z-lines will be closer together.
During relaxation: The light band will me more visible, there will be a lighter area around the M-line. Z-lines will be farther apart.
Remember that myosin FILAMENTS do not change shape. The dark bands will remain the same - only the myosin heads move to draw actin filaments in.
List the parts of the muscle fiber from smallest to largest
Actin filament < myosin filament < sarcomere < myofibril < muscle fiber < muscle tissue
What are motor neurons?
Nerves that synapse with organs to initiate responses
What are neurotransmitters?
Chemicals that are released from neurons to cause a response
What occurs when a neuromuscular junction is formed?
A motor neuron synapses with a muscle fiber
The neuron releases acetylcholine (Ach), a neurotransmitter that initiates muscle contraction
The Ach binds to a receptor on the muscle fiber, telling muscles to release calcium to begin contractions
What is the Sliding Filament theory, and what process does it suggest?
The Sliding Filament Theory attempts to explain how the sarcomere works to produce muscle movement.
Step 0: ATP binds to myosin head before any contractions occur
Myosin heads hydrolyze ATP → ADP, becoming reoriented and energized
Myosin head binds to actin, forming a crossbridge
Myosin heads rotate towards the cneter of the sarcomere, an action called the power stroke
As the myosin heads bind to more ATP, the crossbridges break, detaching them from actin
What is the role of calcium in muscle movement?
It binds to troponin, a protein that moves tropomyosin aside to expose binding sites on actin filaments, allowing crossbridge formation.
What is titin?
A massive protein in the sarcomere that recoils after contraction, preventing overstretching and supporting antagonistic movements.
What is the difference between cardiac and skeletal muscles?
Cardiac muscles are:
Shorter
Have fewer nuclei
Branched
Connected by intercalated disks
Both have sarcomeres, but they’re less pronounced in cardiac muscles
What is “Innate Immunity”
Non-specific immunity; barriers against infection that prevent entry of any pathogen
What role does skin play in immunity?
it provides non-specific immunity as a physical barrier against pathogens. It also has a chemical barrier: sebum is a waxy/oily substance that is slightly acidic to prevent infection (made in the sebaceous glands).
What are 4 types of pathogens and examples of each?
Viruses (coronavirus, flu), bacteria (e.coli, cholera), fungi (ringworm, athlete’s foot), protists (malaria, amoebas)
What is the role of mucus in immunity?
Mucus membranes line orifices to trap pathogens and contain lysozyme, an anti-bacterial enzyme
What are phagocytes?
White blood cells from the capillaries that find pathogens by amoeboid movement and engulf them
What is the process of blood clot formation?
When blood vessels are damaged, platelets bind to the exposed molecules and activate
Positive Feedback Loop: These activated platelets encourage activation/binding of more platelets and release clotting factors
Ex. of clotting factors:
prothrombin (inactive) → thrombin (active)
Thrombin facilitates: fibrinogen (soluble) → fibrin (insoluble), polymer fibers that hold cells together to form a mesh, stabilizing the clots
What are 4 things associated with specific/adaptive immunity?
Antigens, Antibodies, Macrophages, Lymphocytes
What are antigens?
Proteins (often glycoproteins) that elicit specific immune responses
What are Macrophages?
Phagocytes that begin “learned” immune responses
What are Lymphocytes?
White blood cells that make antibodies, used to target specific pathogens to gain learned immunity. Lymphocytes circulate through the blood and concentrate in the lymph nodes. (ex. T cells)
What are the steps of adaptive immunity?
Macrophage identifies and kills pathogen, but presents its antigens to a Helper T cell.
T cells produce antibodies and activate certain B cells - we have a lot of B cells, but each one only makes one type of antibody
Activated B cells clone by mitosis to form plasma cells that make specific antibodies for the infection
Plasma cells that remain in are called memory cells, which provide long-term immunity
Name 4 types of vaccines
antigen, live pathogen, attenuated/weakened pathogen, mRNA
What is Herd Immunity?
The threshold required to stop transmission of a pathogen (ex. Polio was eradicated in the U.S.)
What does gas exchange occur between?
The capillaries and lung tissue
What are characteristics of tissues/surfaces used in gas exchange?
moist, thin, permeable, large surface area
What are alveoli?
Thin sacs in the lungs (the ends of bronchioles) that facilitate gas exchange and hold type I and type II pneumocytes. They have branching chambers that increase surface area.
What do type I pneumocytes do?
Thin, flat cells used to facilitate quicker gas exchange in alveoli.
What do type II pneumocytes do?
Secrete fluid to make a moister environment for gas exchange and secretes a surfactant to prevent alveolar collapse by decreasing surface tension to alveoli don’t cohere to each other.
What is ventilation?
Expiration + Inspiration, moving air in/out of the lungs to maintain a concentration gradient of gases
What movements occur during Inspiration?
Diaphragm contracts
Abdominal muscles relax
External intercostal muscles contract, pulling ribcage up and out
Internal intercostal muscles relax, pulling back into their elongated state
What movements occur during Expiration?
Diaphragm relaxes
Abdominal muscles contract
External intercostal muscles relax, pulling back into their elongated state
Internal intercostal muscles relax, pulling ribcage inward and downward
What term describes the intercostal muscles?
Antagonistic - they work in pairs to perform opposite movements
What is hemoglobin?
An oxygen binding protein in red blood cells that helps transport oxygen
What is the structure of hemolglobin?
Made of 4 polypeptide chains, each with an iron-containing heme group that reversibly binds to oxygen - hemoglobin can bind to up to 4 oxygen molecules
What is cooperative binding?
When it gets easier for oxygen to bind to hemoglobin as more oxygen is binded because each molecule added alters that conformation of it, leading hemoglobin to also have a higher oxygen affinity in oxygen-rich areas (promotes oxygen loading) and not in oxygen-starved areas (promotes oxygen unloading)
What does a standard hemoglobin oxygen dissociation curve look like, and why?
It’ll have a Sigmoid “S” curve because cooperative binding alters oxygen affinity (which impacts %saturation, the y-axis) and causes it to be non-linear, and eventually heme groups become saturated and the graph plateaus
Compare the oxygen dissociation graphs of hemoglobin, fetal hemoglobin, and myoglobin
Fetal arteries have lower pressure, so their hemoglobin has a higher affinity at lower pressures, meaning the graph will increase faster and rest above a normal hemoglobin graph overall.
Myoglobin is an oxygen bonding molecule found in skeletal muscles that holds onto it for longer at lower concentrations AND is not capable of cooperative binding, so it very quickly builds a high saturation and retains it for longer at maximum capacity. It rests above both graphs and is more like an exponential curve.

What is the Bohr Shift?
Tissues with a higher metabolic rate will release more CO2. Since hemoglobin has an allosteric binding site for CO2, when it binds it lowers O2 affinity. Blood cells will also release O2 in the presence of high CO2.
This means when theres a lower pH (more CO2), the graph will lower, and a higher pH, the graph will rise.

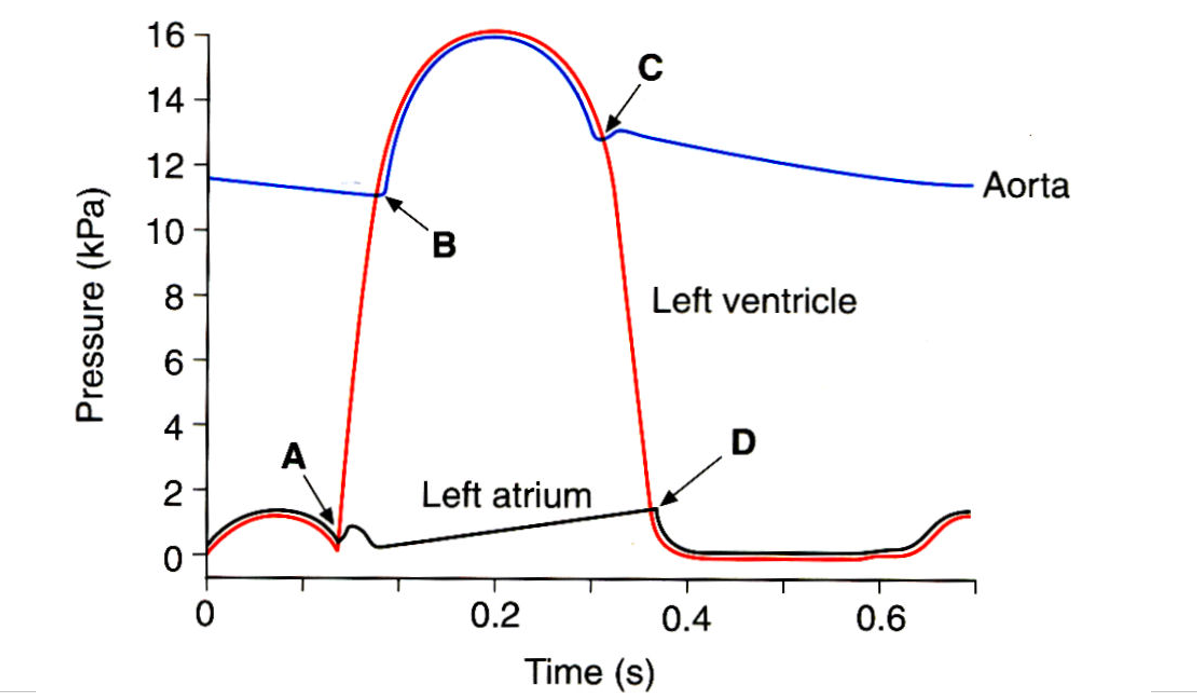
What occurs at each letter?
(Before A) AV Valves open
A) Ventricles contract, the SA valve is closed
B) Semilunar valve opens
C) Semilunar valve closes
D) AV Valve opens
What is blood comprised of?
55% Plasma, 45% Erythrocytes, <1% Leukocytes and Platelets
What is the blood’s Buffy Coat comprised of?
Leukocytes (white blood cells) and Platelets
Which two systems does circulation occur in?
Pulmonary (heart to/from lungs), and Systemic (heart to body)
Function of Arteries
Carries blood away from the heart an regulates blood flow by vasoconstriction/vasodilation