All flashcards - unit 5
1/678
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
679 Terms
Lymphoid Organs and Tissues
Provide structural basis of immune system
House phagocytic cells and lymphocytes
Structures include spleen, thymus, tonsils, lymph nodes, other lymphoid tissues
Lymphoid Cells
Lymphocytes main warriors of immune system
Arise in red bone marrow
Mature into one of two main varieties
T cells (T lymphocytes)
B cells (B lymphocytes)
Lymphocytes
T cells and B cells protect against antigens
Anything body perceives as foreign
Bacteria and bacterial toxins, viruses, mismatched RBCs, cancer cells
T cells
Manage immune response
Attack and destroy infected cells
B cells
Produce plasma cells, which secrete antibodies
Antibodies mark antigens for destruction by phagocytosis or other means
Macrophages
phagocytize foreign substances; help activate T cells
Dendritic cells
capture antigens and deliver them to lymph nodes; activate T cells
Reticular cells
produce reticular fiber stroma that supports other cells in lymphoid organs
Spleen
Largest lymphoid organ
Served by splenic artery and vein, which enter and exit at the hilum
Functions
Site of lymphocyte proliferation and immune surveillance and response
Cleanses blood of aged cells and platelets, macrophages remove debris
Spleen: Additional Functions
Stores breakdown products of RBCs (e.g., iron) for later reuse
Stores blood platelets and monocytes
May be site of fetal erythrocyte production (normally ceases before birth)
Encased by fibrous capsule; has trabeculae
Contains lymphocytes, macrophages, and huge numbers of erythrocytes
Plasma
non-living fluid matrix
Formed elements
living blood "cells" suspended in plasma
Erythrocytes
red blood cells, or RBCs
Leukocytes
white blood cells, or WBCs
Platelets
Spun tube of blood yields three layers
Plasma on top (~55%)
Erythrocytes on bottom (~45%)
WBCs and platelets in Buffy coat (< 1%)
Cytoplasmic fragments
Normal = 150,000 – 400,000 platelets /ml of blood
Form temporary platelet plug that helps seal breaks in blood vessels
Circulating platelets kept inactive and mobile by nitric oxide (NO) and prostacyclin from endothelial cells lining blood vessels
Age quickly; degenerate in about 10 days
Hematocrit
Percent of blood volume that is RBCs
47% ± 5% for males; 42% ± 5% for females
Physical Characteristics and Volume
Sticky, opaque fluid with metallic taste
Color varies with O2 content
High O2 - scarlet; Low O2 - dark red
pH 7.35-7.45
~8% of body weight
Average volume
5-6 L for males; 4-5 L for females
Functions of Blood
Distributing substances
Regulating blood levels of substances
Protection
Distribution Function
Delivering O2 and nutrients to body cells
Transporting metabolic wastes to lungs and kidneys for elimination
Transporting hormones from endocrine organs to target organs
Regulation Functions
Maintaining body temperature by absorbing and distributing heat
Maintaining normal pH using buffers; alkaline reserve of bicarbonate ions
Maintaining adequate fluid volume in circulatory system
Protection Functions
Preventing blood loss
Plasma proteins and platelets initiate clot formation
Preventing infection
Antibodies
Complement proteins
WBCs
Blood Plasma
90% water
Over 100 dissolved solutes
Nutrients, gases, hormones, wastes, proteins, inorganic ions
Plasma proteins most abundant solutes
Remain in blood; not taken up by cells
Proteins produced mostly by liver
60% albumin; 36% globulins; 4% fibrinogen
Albumin
60% of plasma protein
Functions
Substance carrier
Blood buffer
Major contributor of plasma osmotic pressure
Erythrocytes
Biconcave discs, anucleate, essentially no organelles
Diameters larger than some capillaries
Filled with hemoglobin (Hb) for gas transport
Contain plasma membrane protein spectrin and other proteins
Spectrin provides flexibility to change shape
Major factor contributing to blood viscosity
Structural characteristics contribute to gas transport
Biconcave shape—huge surface area relative to volume
>97% hemoglobin (not counting water)
No mitochondria; ATP production anaerobic; do not consume O2 they transport
structure gives function
Eyrthrocyte Functions
RBCs dedicated to respiratory gas transport
Hemoglobin binds reversibly with oxygen
Normal values
Males - 13-18g/100ml; Females - 12-16 g/100ml
Hemoglobin (Hb)
O2 loading in lungs
Produces oxyhemoglobin (ruby red)
O2 unloading in tissues
Produces deoxyhemoglobin or reduced hemoglobin (dark red)
Blood is NEVER blue
CO2 loading in tissues
20% of CO2 in blood binds to Hb → carbaminohemoglobin
Hematopoiesis
Blood cell formation in red bone marrow
In adult, found in axial skeleton, girdles, and proximal epiphysis of humerus and femur
Hormone Erythropoietin (EPO)
Direct stimulus for erythropoiesis
Always small amount in blood to maintain basal rate
High RBC or O2 levels depress production
Released by kidneys (some from liver) in response to hypoxia
Dialysis patients have low RBC counts
Causes of hypoxia
Decreased RBC numbers due to hemorrhage or increased destruction
Insufficient hemoglobin per RBC (e.g., iron deficiency)
Reduced availability of O2 (e.g., high altitudes)
Effects of EPO
Rapid maturation of committed marrow cells
Increased circulating reticulocyte count in 1–2 days
Some athletes abuse artificial EPO
Dangerous consequences
More blood = heart has to work harder
Testosterone enhances EPO production, resulting in higher RBC counts in males
Fate and Destruction of Erythrocytes
Life span: 100–120 days
No protein synthesis, growth, division
Old RBCs become fragile; Hb begins to degenerate
Get trapped in smaller circulatory channels especially in spleen
Macrophages engulf dying RBCs in spleen
Heme and globin are separated
Iron salvaged for reuse
Heme degraded to yellow pigment bilirubin
Liver secretes bilirubin (in bile) into intestines
Degraded to pigment urobilinogen
Pigment leaves body in feces as stercobilin
Globin metabolized into amino acids
Released into circulation
Erythrocyte Disorders - Anemia
Anemia- deficiency in RBCs
Blood has abnormally low O2-carrying capacity
Sign rather than disease itself = symptom
Blood O2 levels cannot support normal metabolism
Accompanied by fatigue, pallor, shortness of breath, and chills
Causes of Hemorrhagic Anemia
Blood loss rapid (e.g., stab wound)
Treated by blood replacement
Causes of Chronic hemorrhagic anemia
Slight but persistent blood loss
Hemorrhoids, bleeding ulcer
Primary problem treated
Causes of Anemia: Low RBC Production - Iron Definciency Anemia
Caused by hemorrhagic anemia, low iron intake, or impaired absorption
Microcytic, hypochromic RBCs
Iron supplements to treat
Causes of Anemia: Low RBC Production - Renal Anemia
Lack of EPO hormone
Often accompanies kidney disease
Treated with synthetic EPO
*renal =kidney
Causes of Anemia: High RBC Destruction
Hemolytic anemias
Premature RBC lysis (lysis= cell membrane ruptures... cells dies)
Caused by
Hemoglobin abnormalities
Incompatible transfusions (you are A blood and are given B blood as a transfusion)
Infections
Causes of Anemia: High RBC Destruction (Sickle cell anemia)
Black people of African malarial belt and descendants
Malaria
Kills 1 million each year
Sickle-cell gene
Two copies → Sickle-cell anemia
One copy → Sickle-cell trait; milder disease; better chance to survive malaria
Sickle Cell Treatment
Acute crisis treated with transfusions; inhaled nitric oxide
Preventing sickling
Hydroxyurea induces fetal hemoglobin (which does not sickle) formation
Blocking RBC ion channels
Stem cell transplants
Gene therapy
Leukocytes
Make up <1% of total blood volume
4,800 - 10,800 WBCs/μl blood
Function in defense against disease
Leukocytosis:
WBC count over 11,000/mm3
Normal response to infection
Neutrophils
Most numerous WBCs
3-6 lobes in nucleus; twice size of RBCs
Very phagocytic—"bacteria slayers"
Lymphocytes
Second most numerous WBC
Large, dark-purple, circular nuclei with thin rim of blue cytoplasm
Mostly in lymphoid tissue (e.g., lymph nodes, spleen); few circulate in blood
Crucial to immunity
Two types
T lymphocytes (T cells) act against virus-infected cells and tumor cells
B lymphocytes (B cells) give rise to plasma cells, which produce antibodies
Leukocyte disorders
Leukopenia
Abnormally low WBC count—drug induced
Leukemias
all fatal if untreated
Cancer → overproduction of abnormal WBCs
Named according to abnormal WBC clone involved
Myeloid leukemia involves myeloblast descendants
Lymphocytic leukemia involves lymphocytes
Acute leukemia derives from stem cells; primarily affects children
Chronic leukemia more prevalent in older people
Leukemia
Cancerous leukocytes fill red bone marrow
Other lines crowded out → anemia; bleeding
Immature nonfunctional WBCs in bloodstream
Death from internal hemorrhage; overwhelming infections
Treatments
Irradiation, antileukemic drugs; stem cell transplants
Hemostasis
Fast series of reactions for stoppage of bleeding
Requires clotting factors, and substances released by platelets and injured tissues
Three steps
Vascular spasm
Platelet plug formation
Coagulation (blood clotting)
Hemostasis: Vascular Spasm
Vasoconstriction of damaged blood vessel
Triggers
Direct injury to vascular smooth muscle
Chemicals released by endothelial cells and platelets
Pain reflexes
Most effective in smaller blood vessels
Hemostasis: Platelet Plug Formation
Positive feedback cycle
Damaged endothelium exposes collagen fibers
Platelets stick to collagen fibers via plasma protein von Willebrand factor
Swell, become spiked and sticky, and release chemical messengers
ADP causes more platelets to stick and release their contents
Serotonin and thromboxane A2 enhance vascular spasm and platelet aggregation
Hemostasis: Coagulation
Blood transformed from liquid to gel
Series of reactions using clotting factors (procoagulants)
Factors Preventing Undesirable Clotting
Platelet adhesion is prevented by
Smooth endothelium of blood vessels prevents platelets from clinging
Antithrombic substances nitric oxide and prostacyclin secreted by endothelial cells
Disorders of Hemostasis
Thromboembolic disorders:
undesirable clot formation
Disorders of Hemostasis
Bleeding disorders
abnormalities that prevent normal clot formation
Disorders of Hemostasis
Disseminated Intravascular Coagulation (DIC)
abnormal blood clotting in small vessels throughout the body that cuts off the supply of oxygen to distal tissues, resulting in damage to body organs
Blood Clotting Conditions - Thrombus
clot that develops and persists in unbroken blood vessel
May block circulation leading to tissue death
Blood Clotting Conditions - Embolus
thrombus freely floating in bloodstream
Blood Clotting Conditions - Embolism
embolus obstructing a vessel
E.g., pulmonary and cerebral emboli
Risk factors - atherosclerosis, inflammation, slowly flowing blood or blood stasis from immobility
Anticoagulant Drugs
Aspirin
antiprostaglandin that inhibits thromboxane A2
Anticoagulant drugs - heparin
Anticoagulant used clinically for pre- and postoperative cardiac care
Anticoagulant drugs - Warfarin
Used for those prone to atrial fibrillation
Interferes with action of vitamin K
Anticoagulant Drugs - Dabigatran
directly inhibits thrombin
Hemophilia
includes several similar hereditary bleeding disorders
Hemophilia A: most common type (77% of all cases); factor VIII deficiency
Hemophilia B: factor IX deficiency
Hemophilia C: mild type; factor XI deficiency
Symptoms include prolonged bleeding, especially into joint cavities
Treated with plasma transfusions and injection of missing factors
Increased hepatitis and HIV risk
Blood Tranfusions
Whole-blood transfusions used when blood loss rapid and substantial
Packed red cells (plasma and WBCs removed) transfused to restore oxygen-carrying capacity
Transfusion of incompatible blood can be fatal
Human Blood Groups
RBC membranes bear 30 types of glycoprotein antigens
Anything perceived as foreign; generates an immune response
Promoters of agglutination; called agglutinogens
Mismatched transfused blood perceived as foreign
May be agglutinated and destroyed; can be fatal
Presence or absence of each antigen is used to classify blood cells into different groups
ABO blood groups
Types A, B, AB, and O
Based on presence or absence of two agglutinogens (A and B) on surface of RBCs
Blood may contain preformed anti-A or anti-B antibodies (agglutinins)
Act against transfused RBCs with ABO antigens not present on recipient's RBCs
Anti-A or anti-B form in blood at about 2 months of age; adult levels by 8-10
Transfusion Reactions
Occur if mismatched blood infused
Donor's cells
Attacked by recipient's plasma agglutinins
Agglutinate and clog small vessels
Rupture and release hemoglobin into bloodstream
Result in
Diminished oxygen-carrying capacity
Diminished blood flow beyond blocked vessels
Hemoglobin in kidney tubules → renal failure
Symptoms
Fever, chills, low blood pressure, rapid heartbeat, nausea, vomiting
Treatment
Preventing kidney damage
Fluids and diuretics to wash out hemoglobin
Tranfusions
Type O universal donor
No A or B antigens
Type AB universal recipient
No anti-A or anti-B antibodies
Misleading - other agglutinogens cause transfusion reactions
Autologous transfusions
Patient predonates
Blood Typing
Mixing RBCs with antibodies against its agglutinogen(s) causes clumping of RBCs
Done for ABO and for Rh factor
Cross Matching
Mix recipient's serum with donor RBCs
Mix recipient's RBCs with donor serum
Restoring Blood Volume
Death from shock may result from low blood volume
Volume must be replaced immediately with
Normal saline or multiple-electrolyte solution (Ringer's solution) that mimics plasma electrolyte composition
Plasma expanders (e.g., purified human serum albumin, hetastarch, and dextran)
Mimic osmotic properties of albumin
More expensive and may cause significant complications
Diagnostic Blood Tests
Hematocrit - test for anemia
Blood glucose tests - diabetes
Microscopic examination reveals variations in size and shape of RBCs, indications of anemias
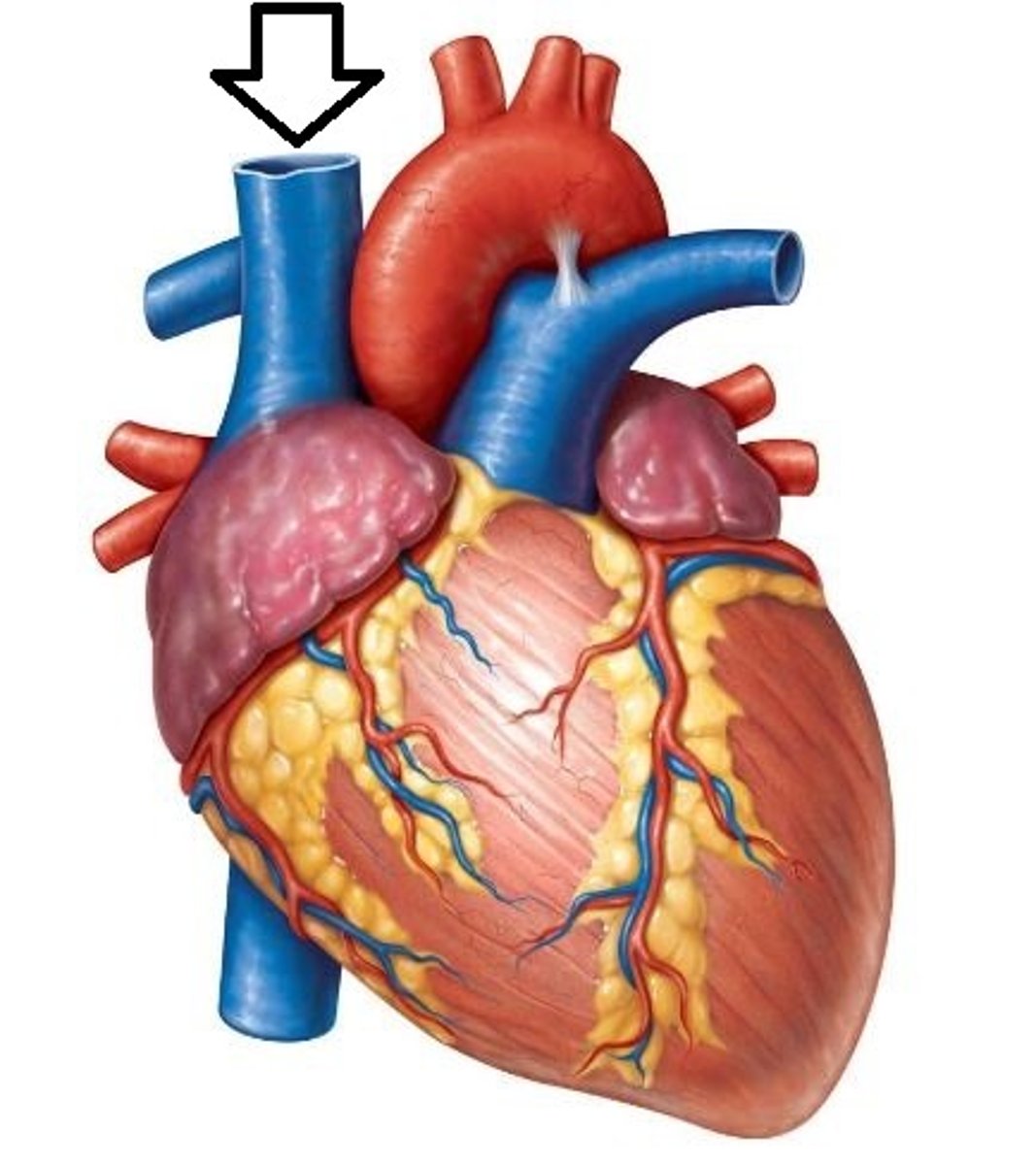
Superior Vena Cava
A vein that is the second largest vein in the human body and returns blood to the right atrium of the heart from the upper half of the body.
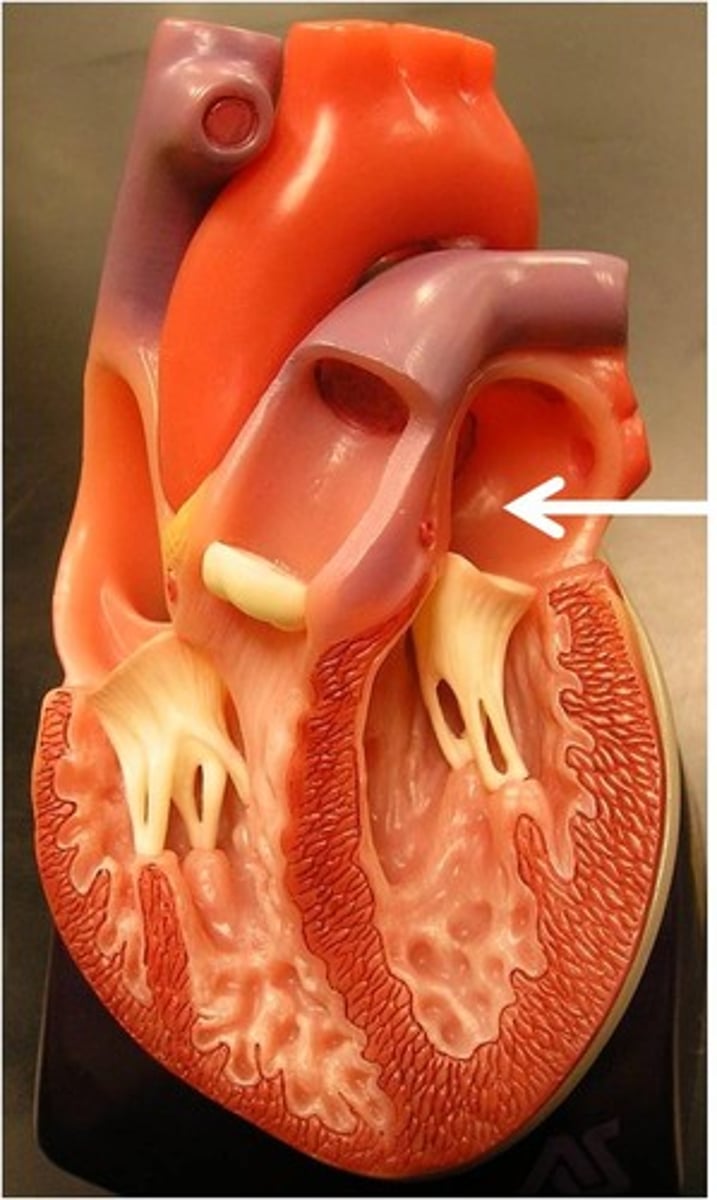
left atrium
receives oxygenated blood from the lungs
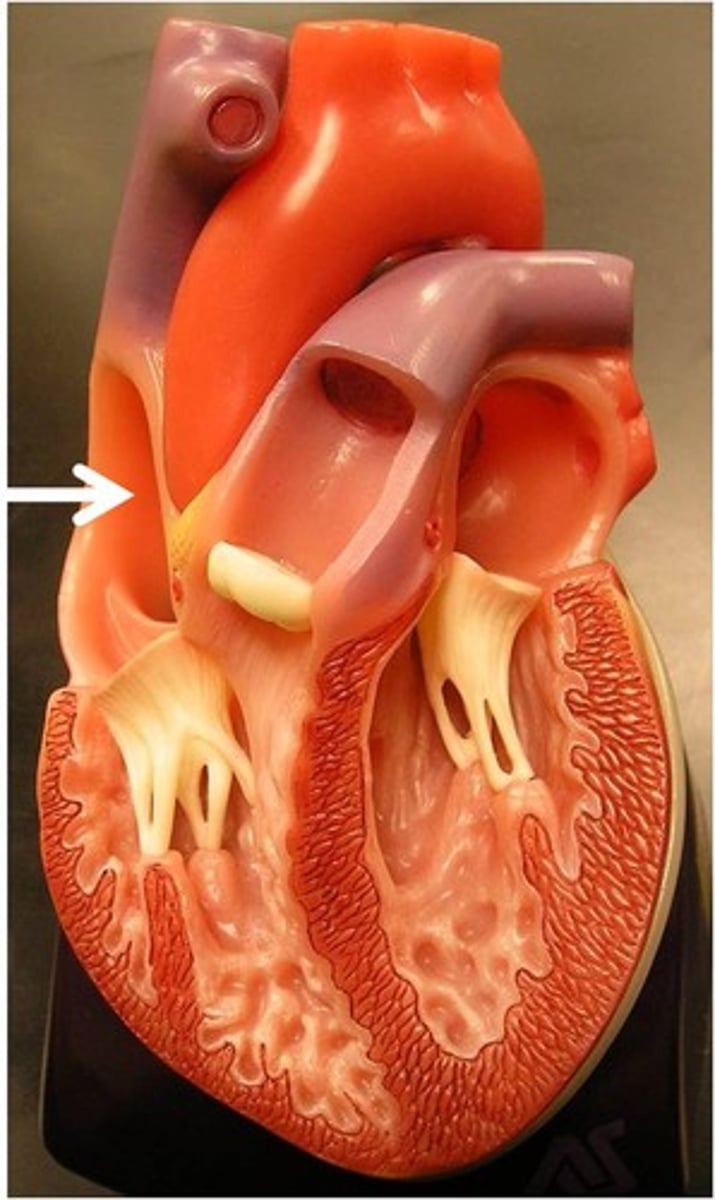
right atrium
Receives deoxygenated blood from the body
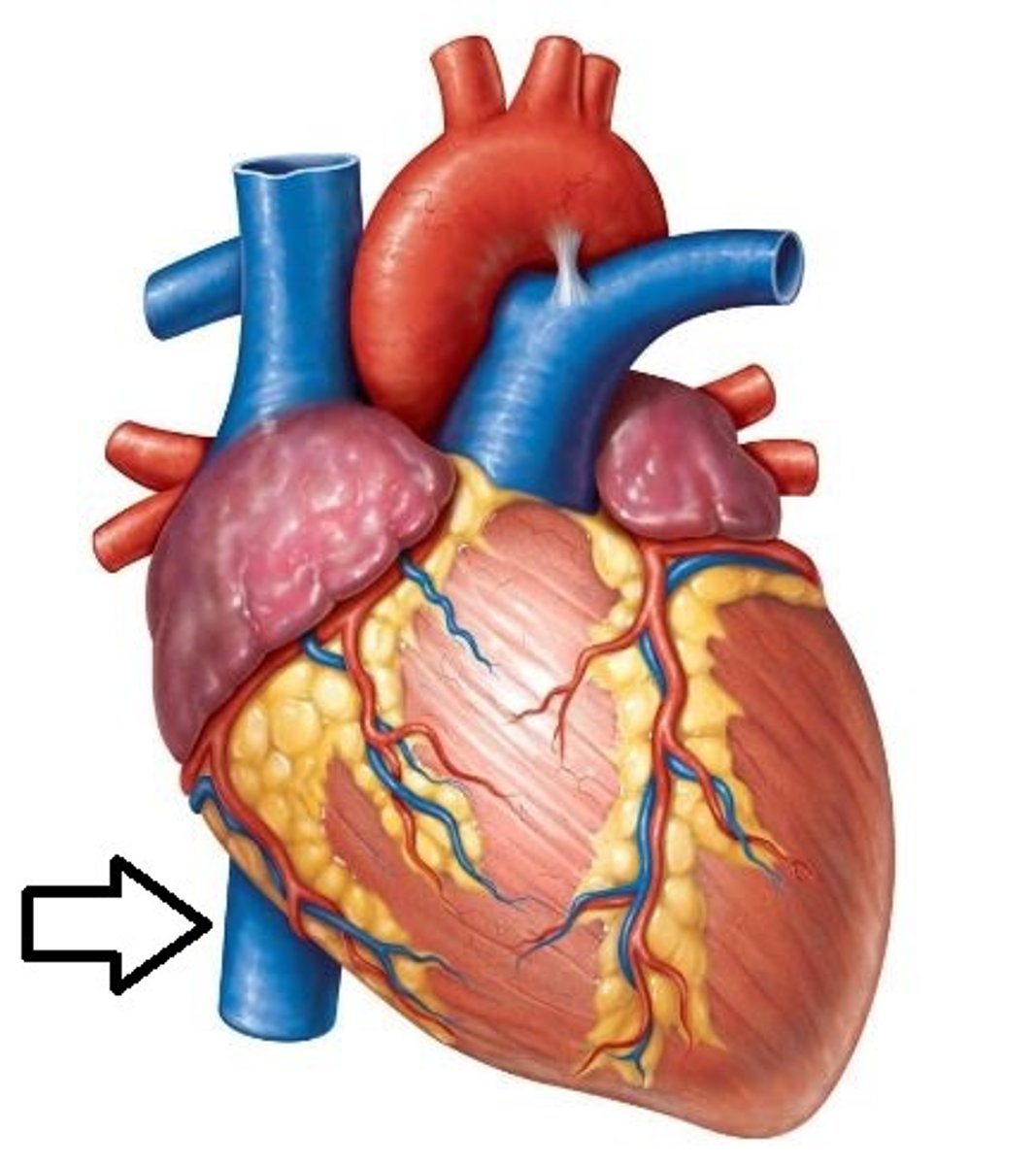
Inferior Vena Cava
A vein that is the largest vein in the human body and returns blood to the right atrium of the heart from bodily parts below the diaphragm.
Right Pulmonary Artery
takes blood from the right ventricle to the right lung
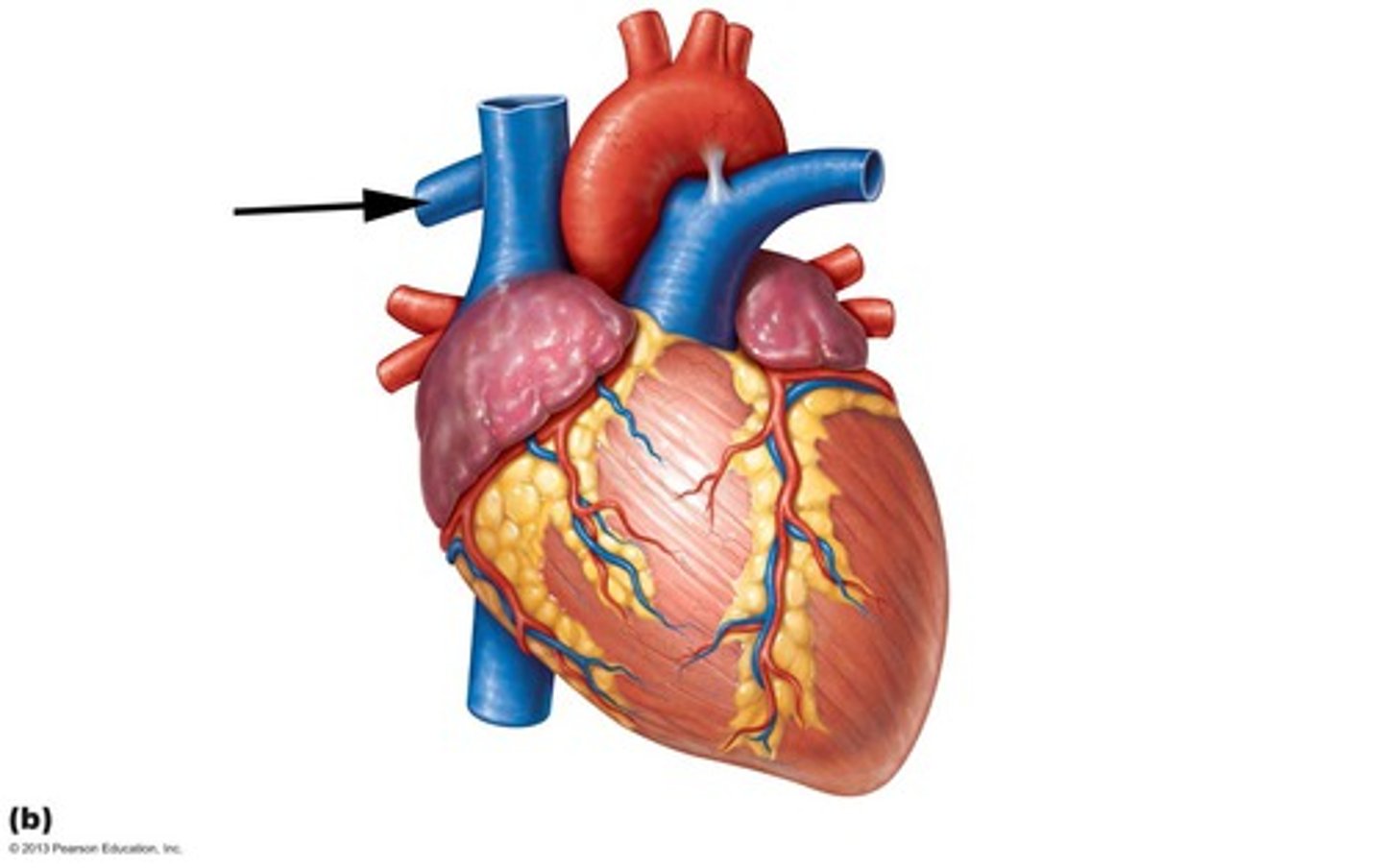
Left Pulmonary Artery
carries poor oxygenated blood from the right ventricle to the left lung.
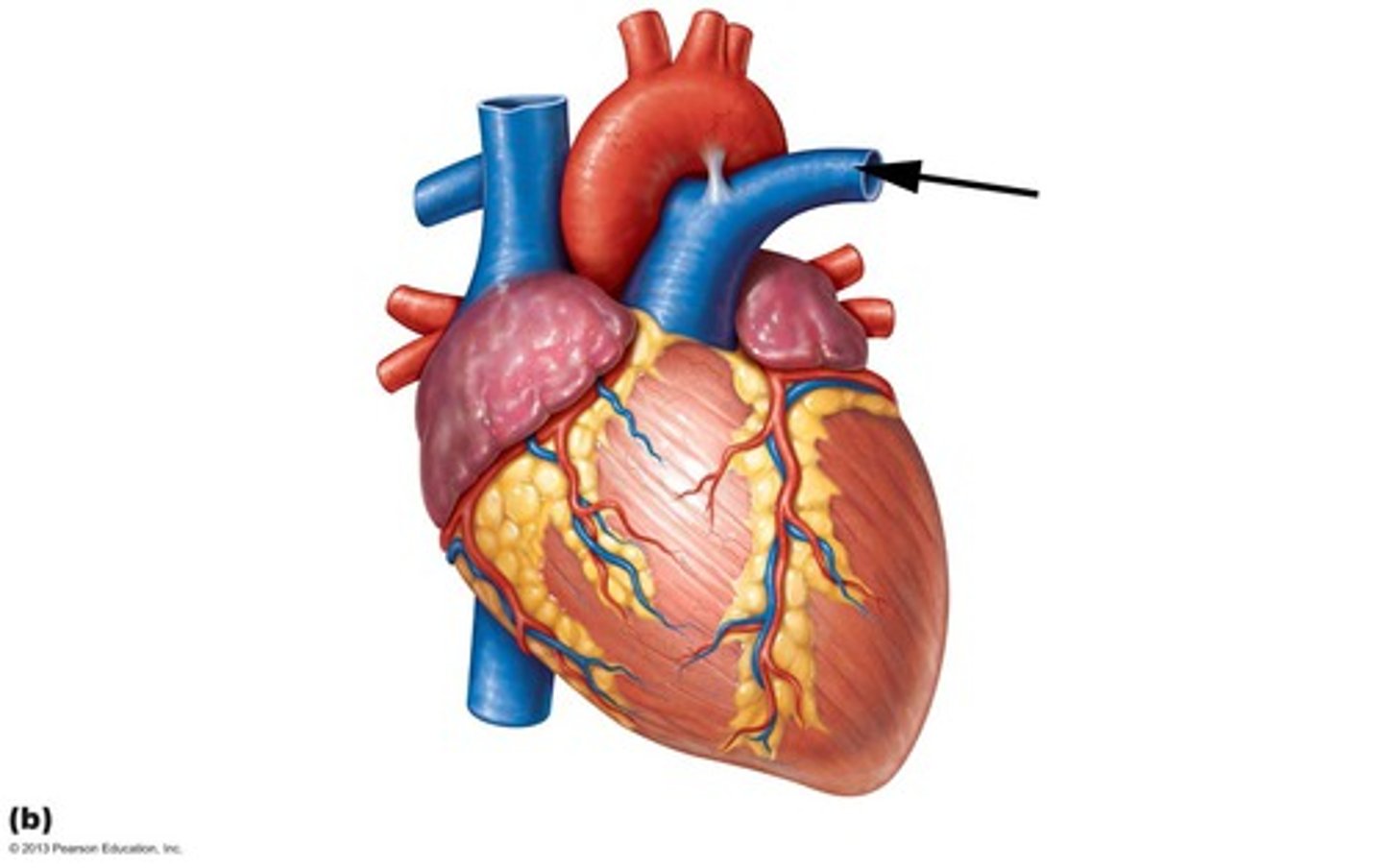
Tricuspid Valve
valve between the right atrium and the right ventricle
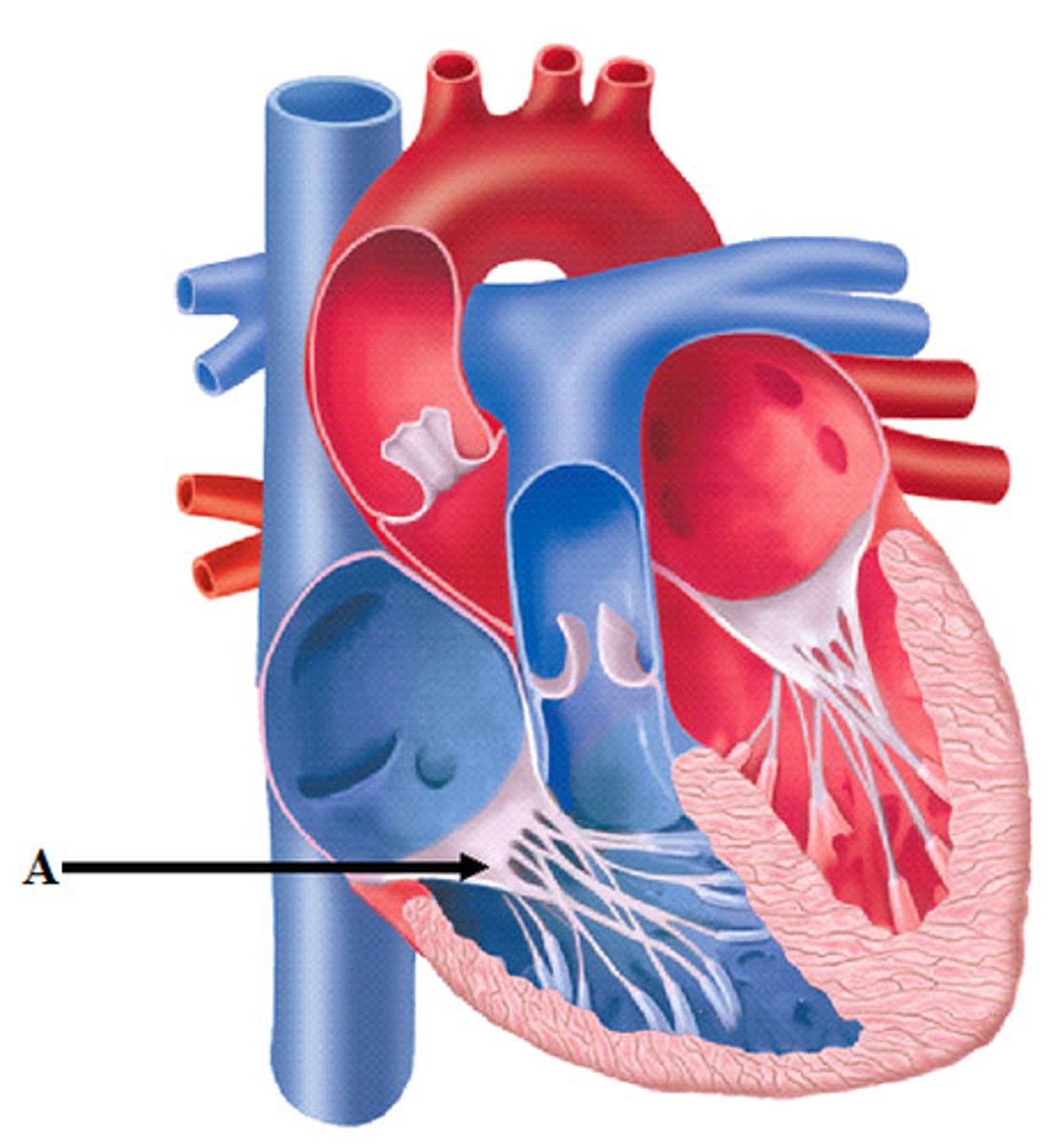
Bicuspid Valve
valve between the left atrium and the left ventricle.
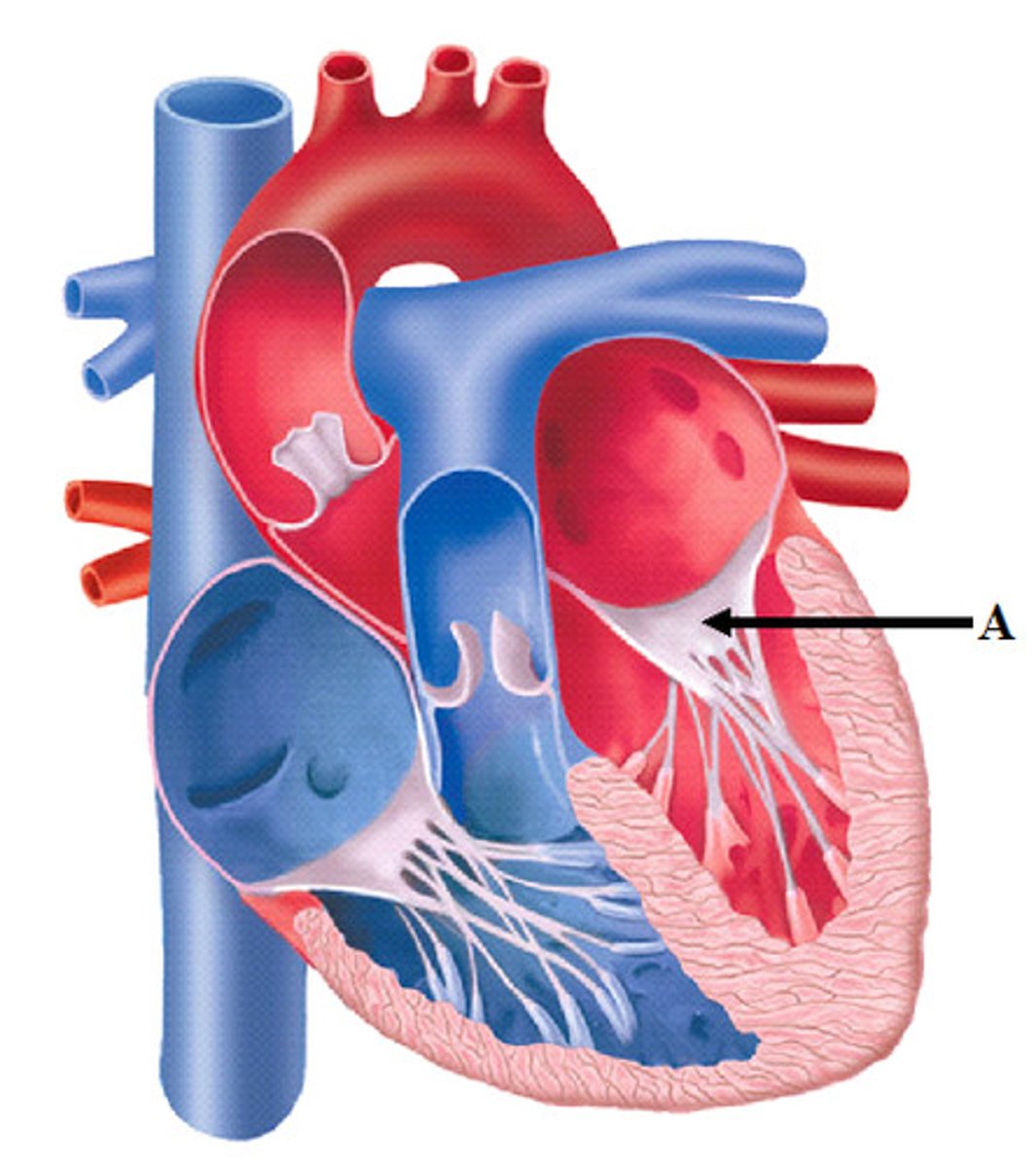
Aortic Valve
The semilunar valve separating the aorta from the left ventricle that prevents blood from flowing back into the left ventricle.
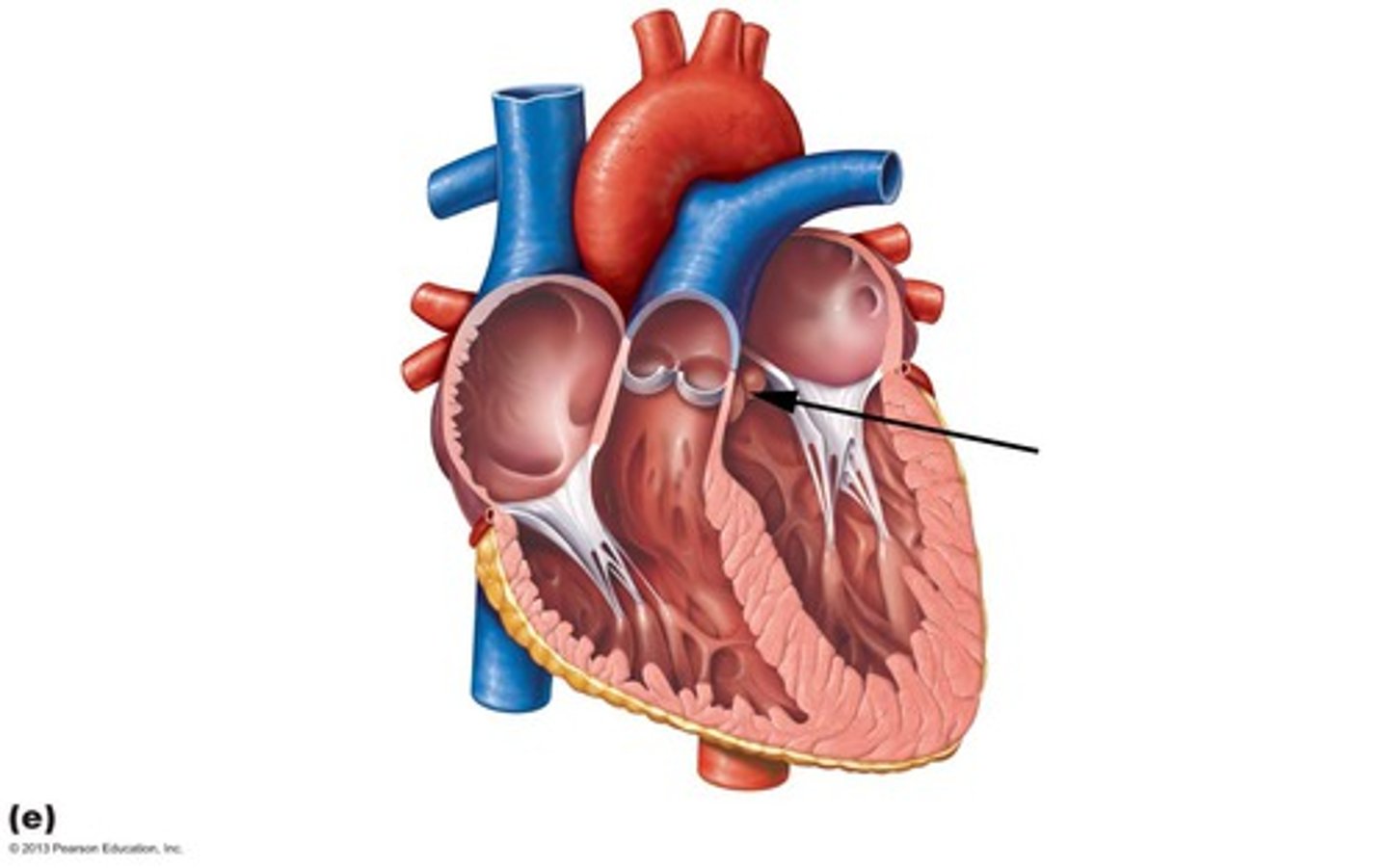
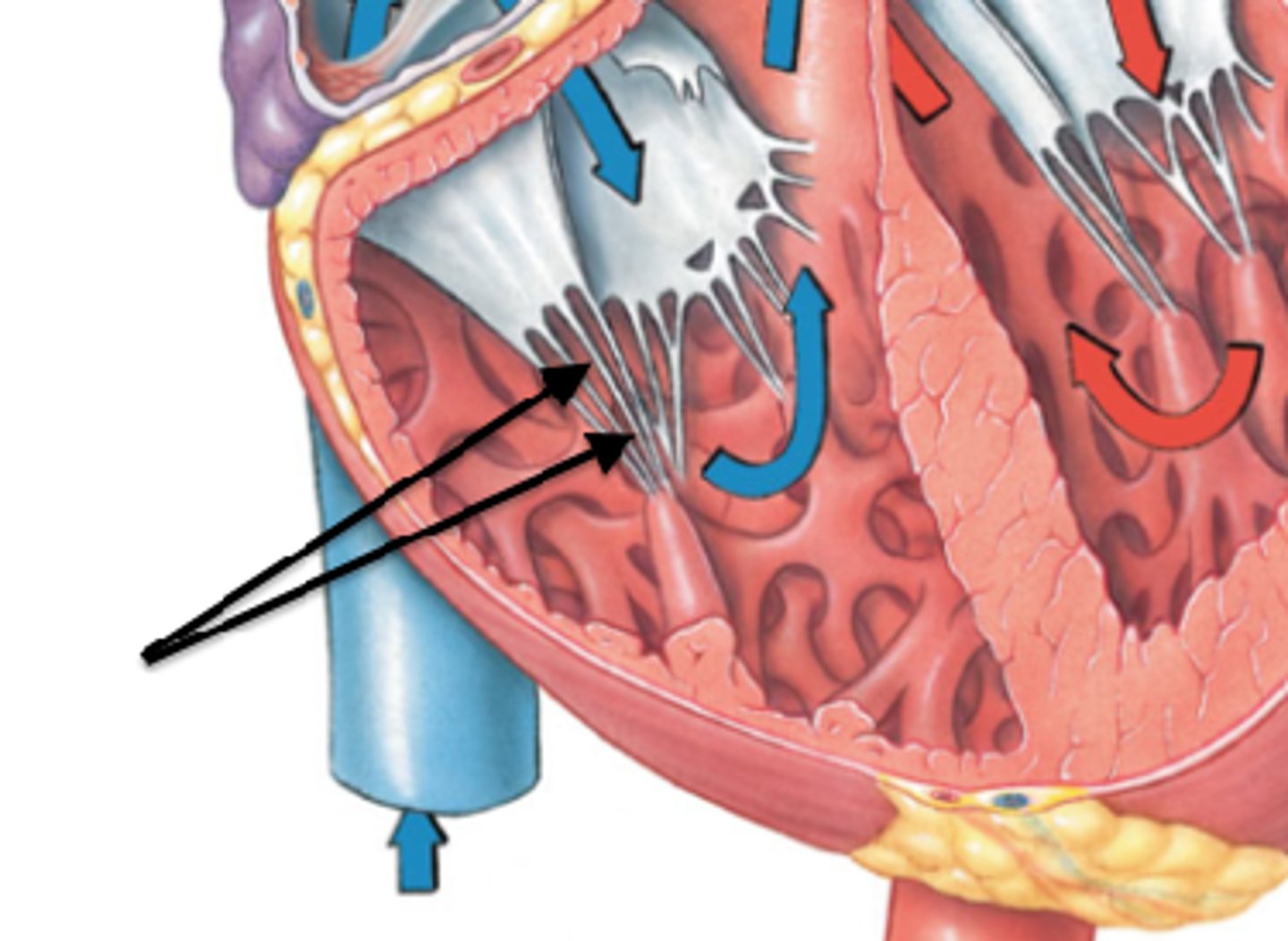
Chordae Tendineae
thin bands of fibrous tissue that attach to the valves in the heart and prevent them from inverting
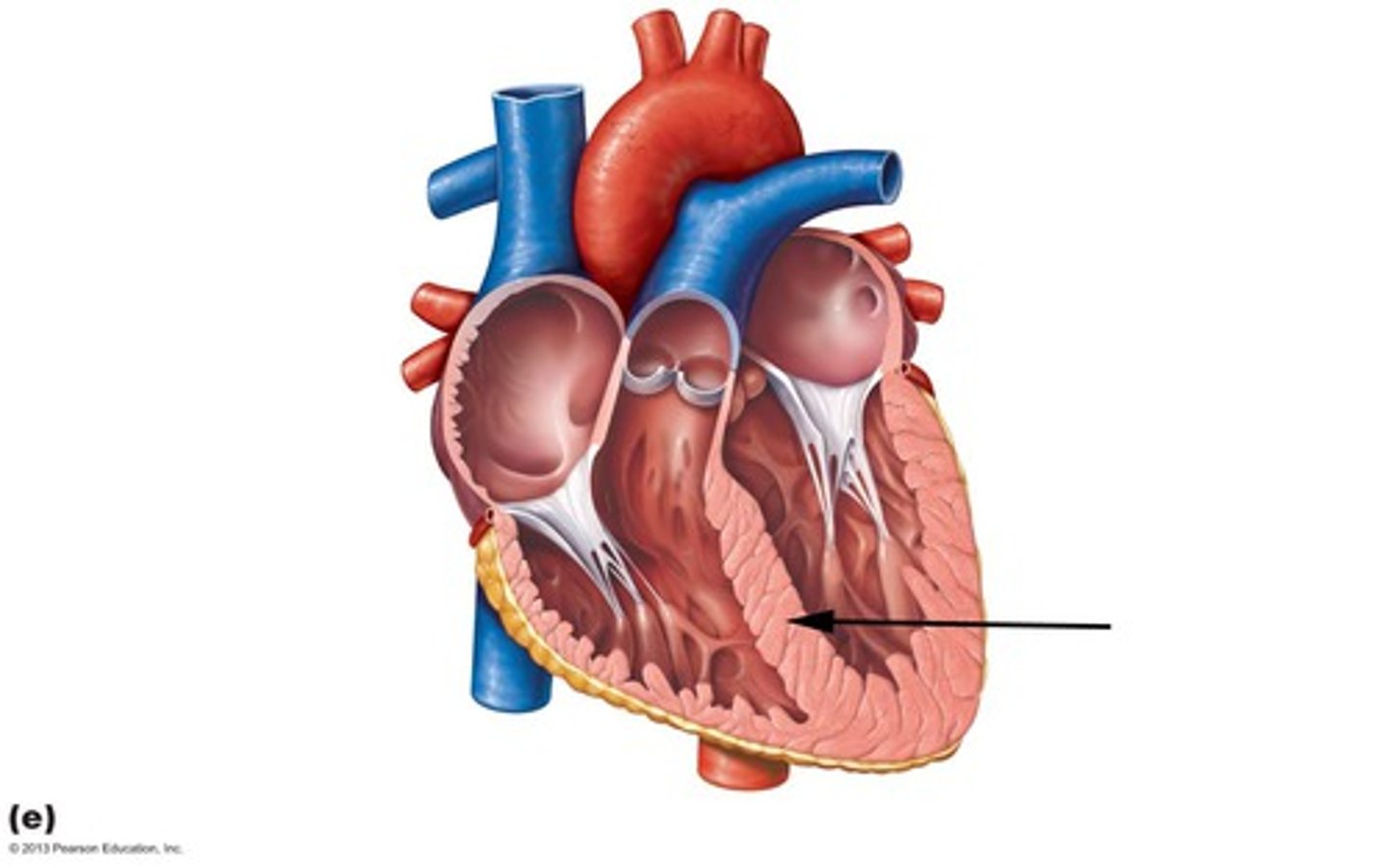
Interventricular Septum
separates the two ventricles
Epicardium
outer layer of the heart
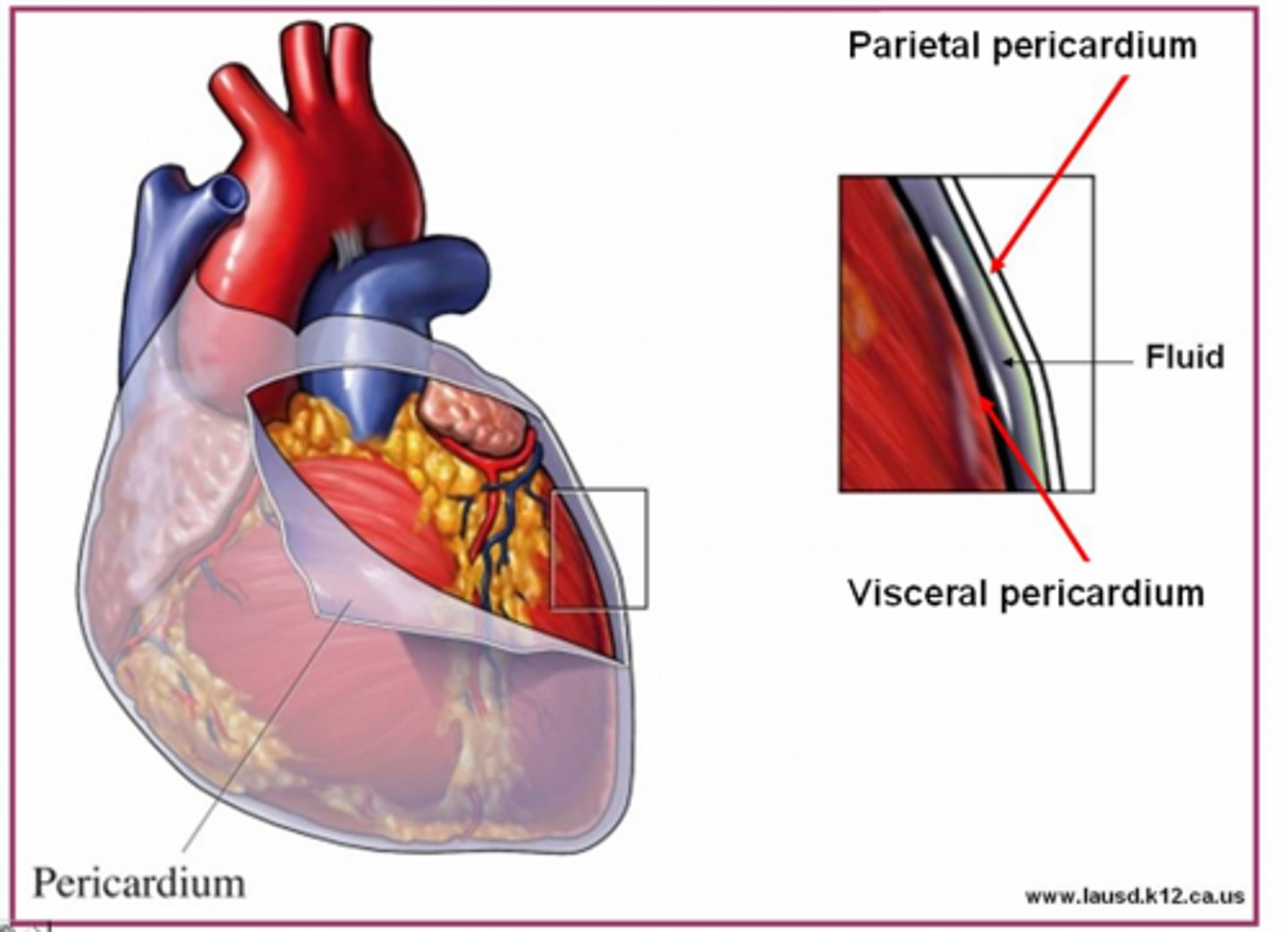
Myocardium
muscular, middle layer of the heart
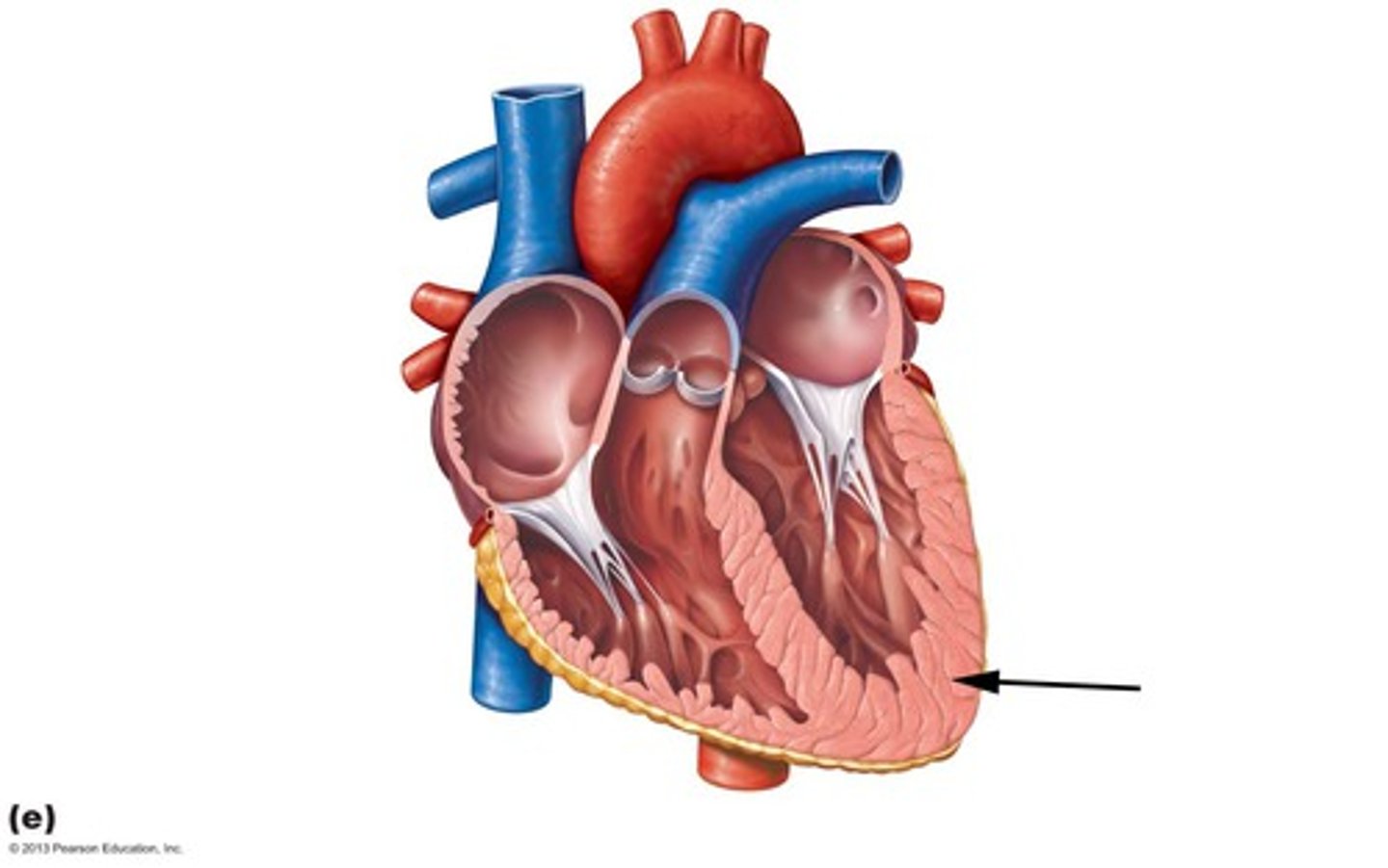
Endocardium
inner lining of the heart
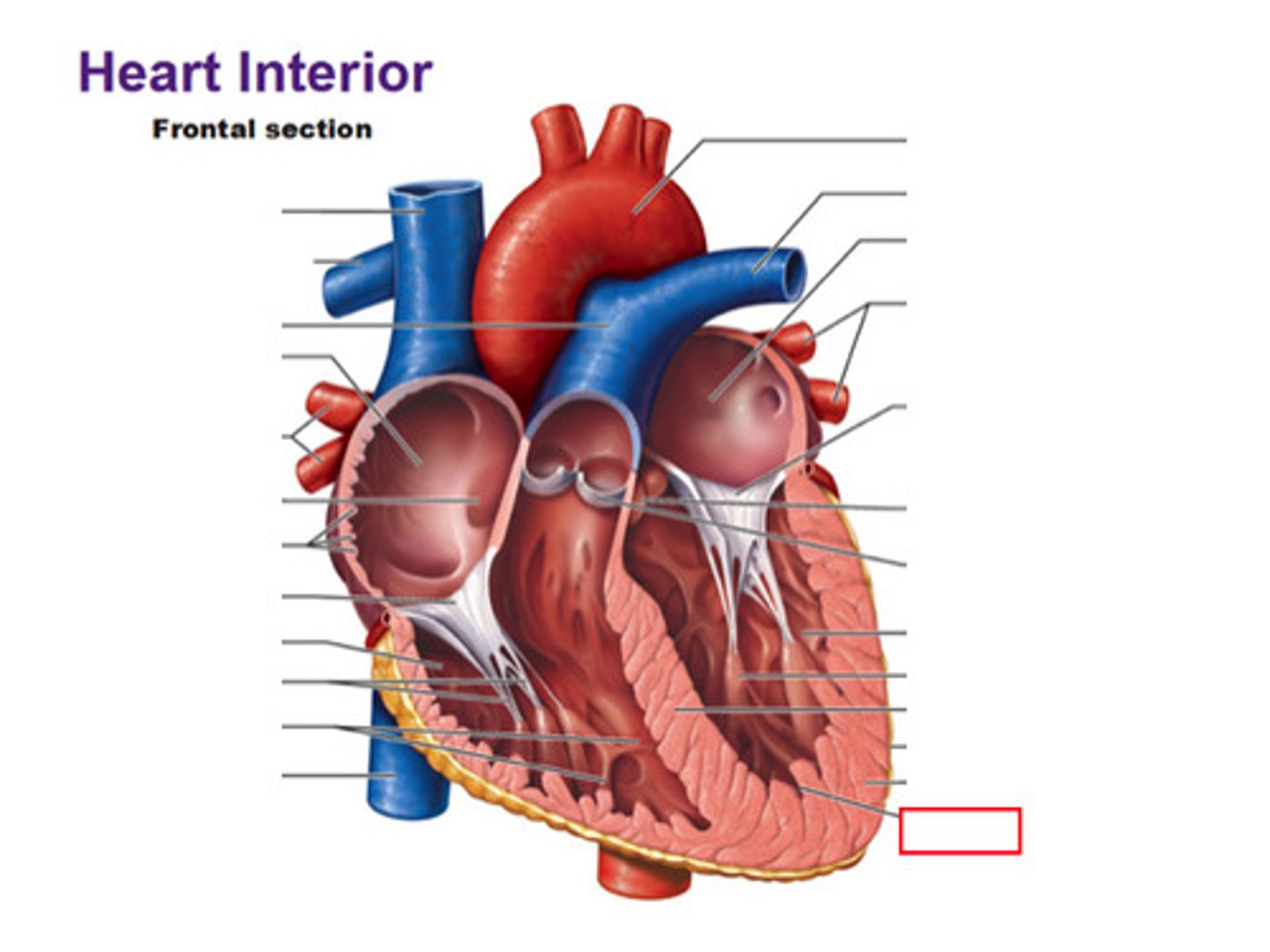
Coronary Arteries/Veins
Bring nutrients and blood to the heart; removes waste products
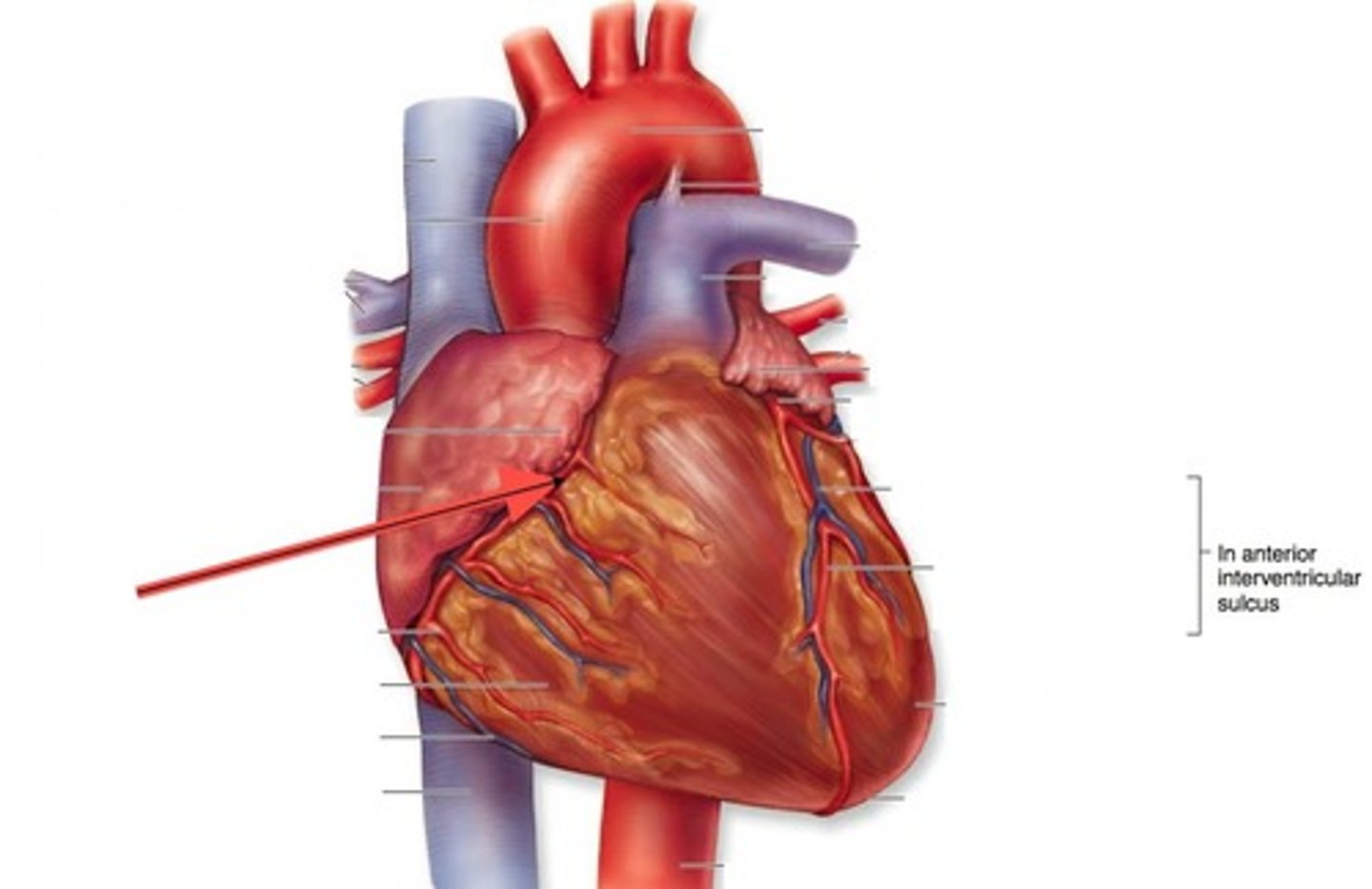
Aortic Arch
a curved blood vessel from which arteries branch to the head and neck.
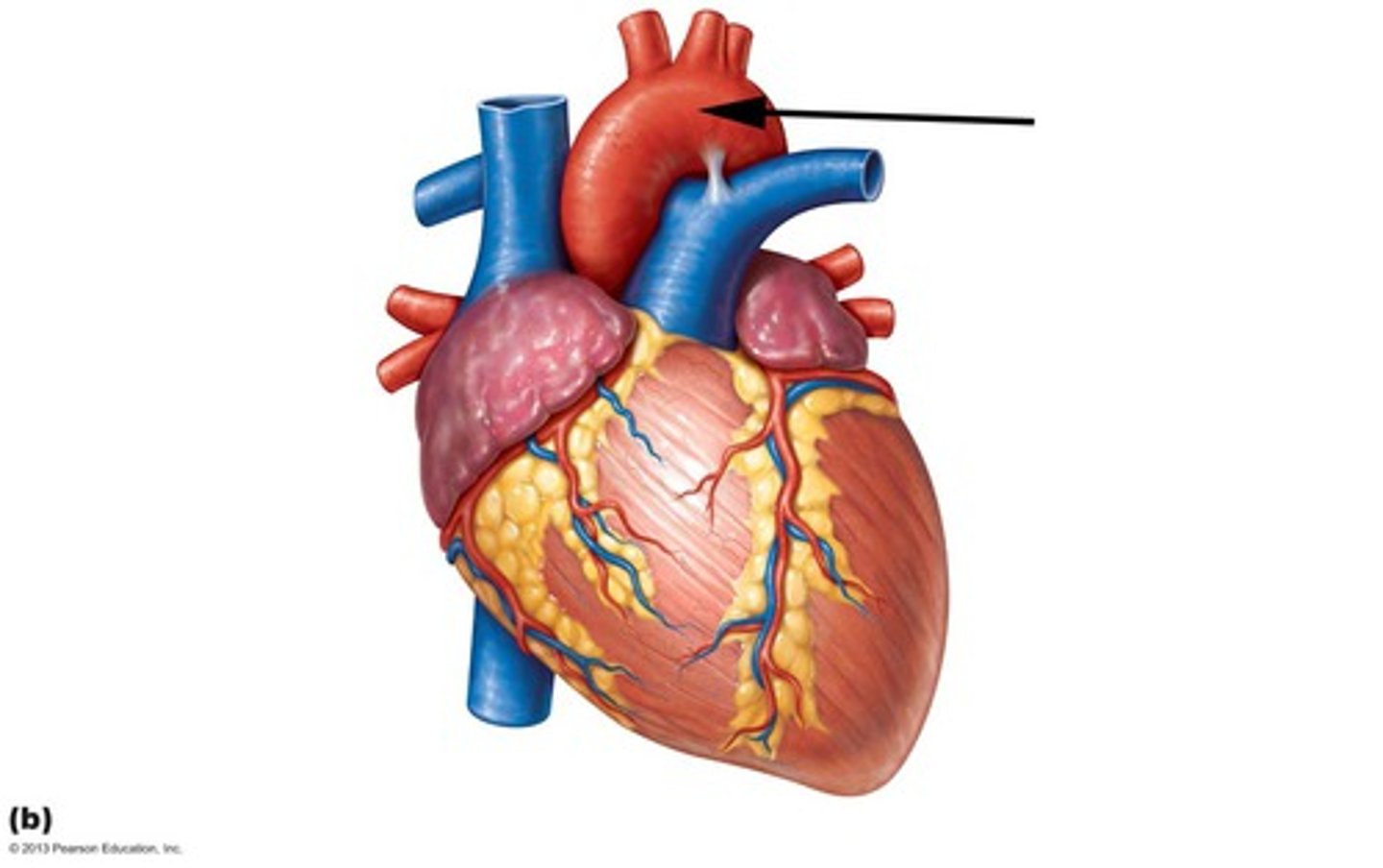
Aorta
The large arterial trunk that carries blood from the heart to be distributed by branch arteries through the body.
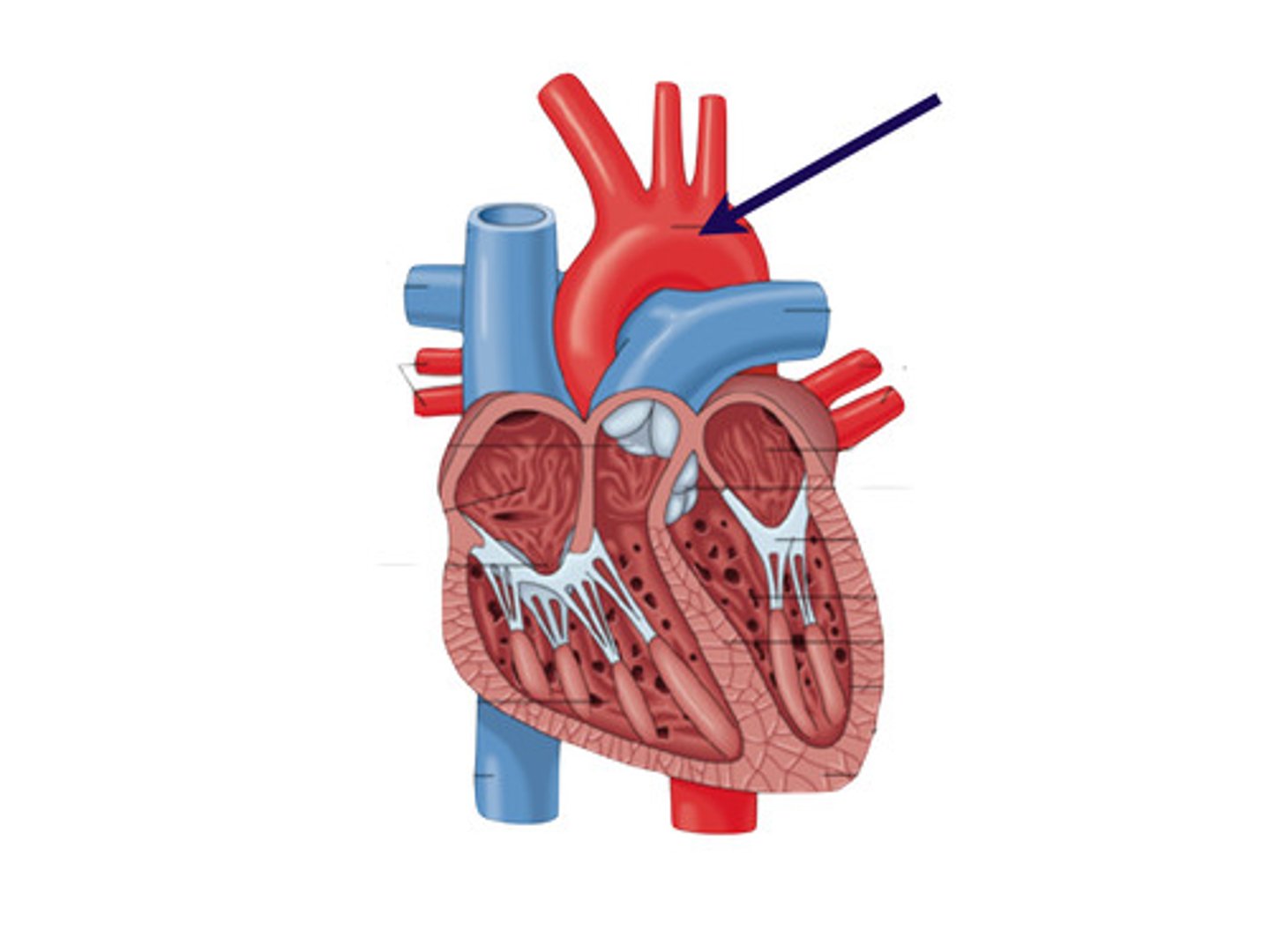
Right Pulmonary Vein
transports oxygenated blood from the right lung to the left atrium
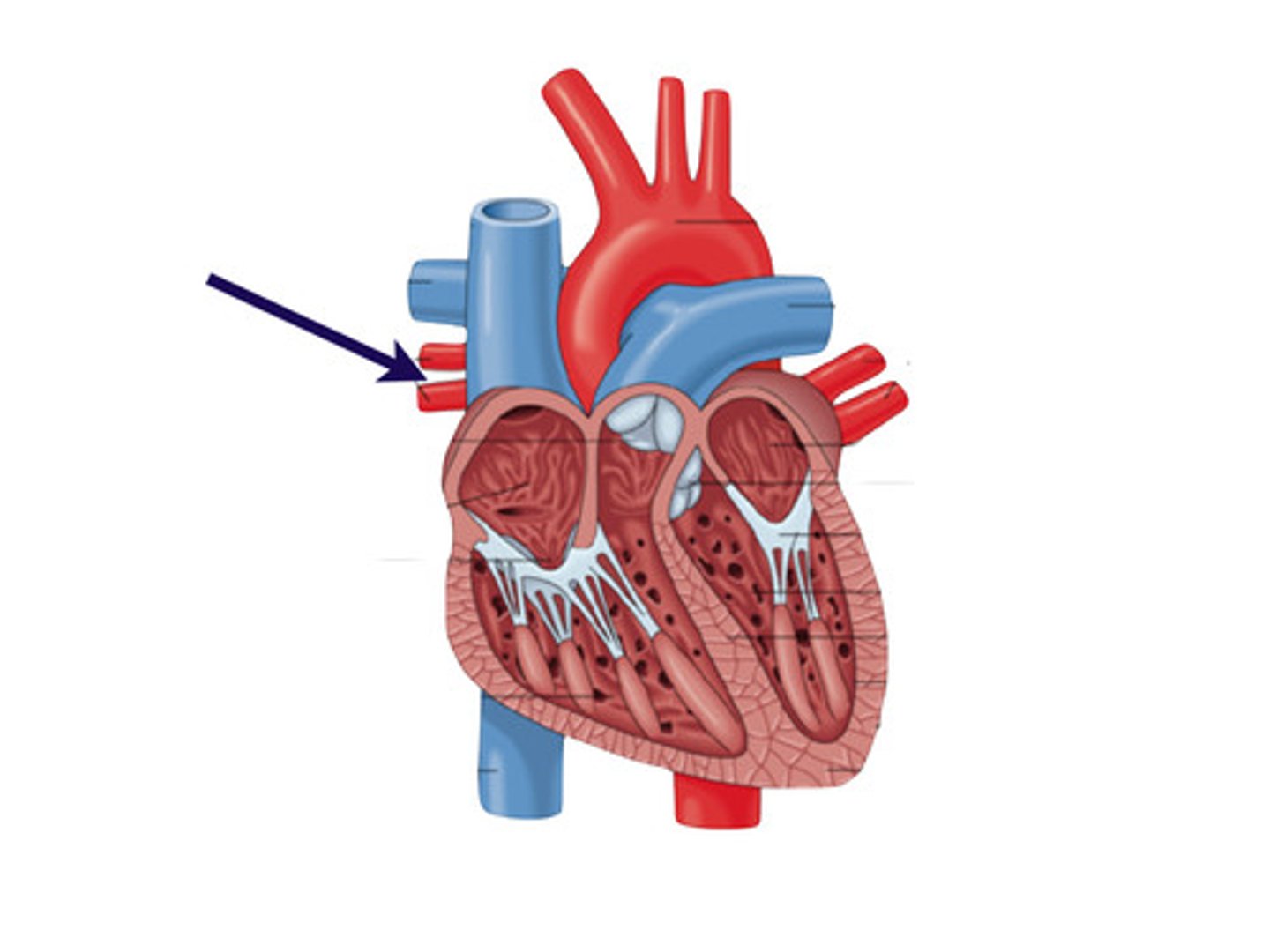
Left Pulmonary Vein
transports oxygenated blood from the left lung to the left atrium
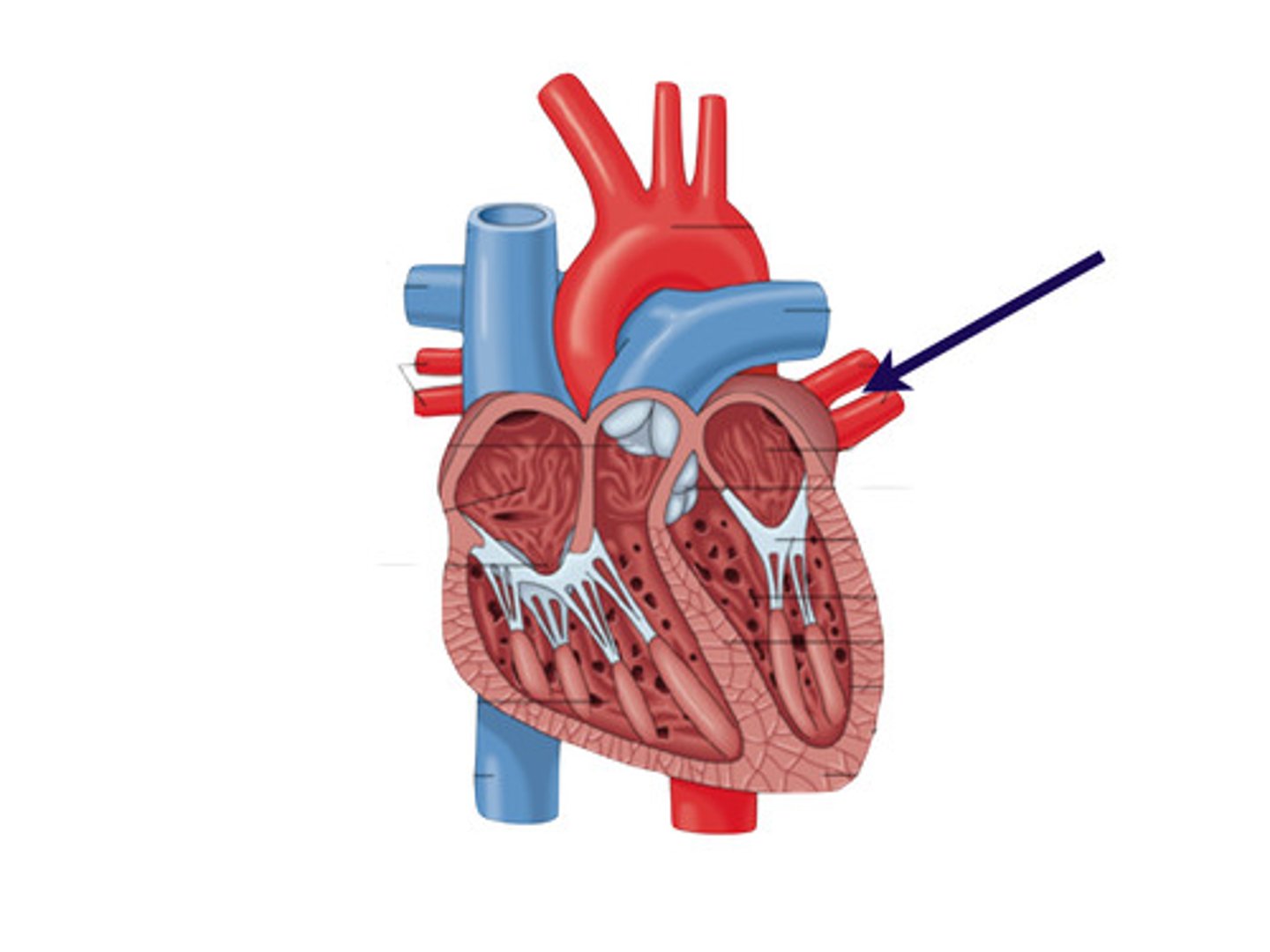
Right Ventricle
pumps deoxygenated blood to the lungs
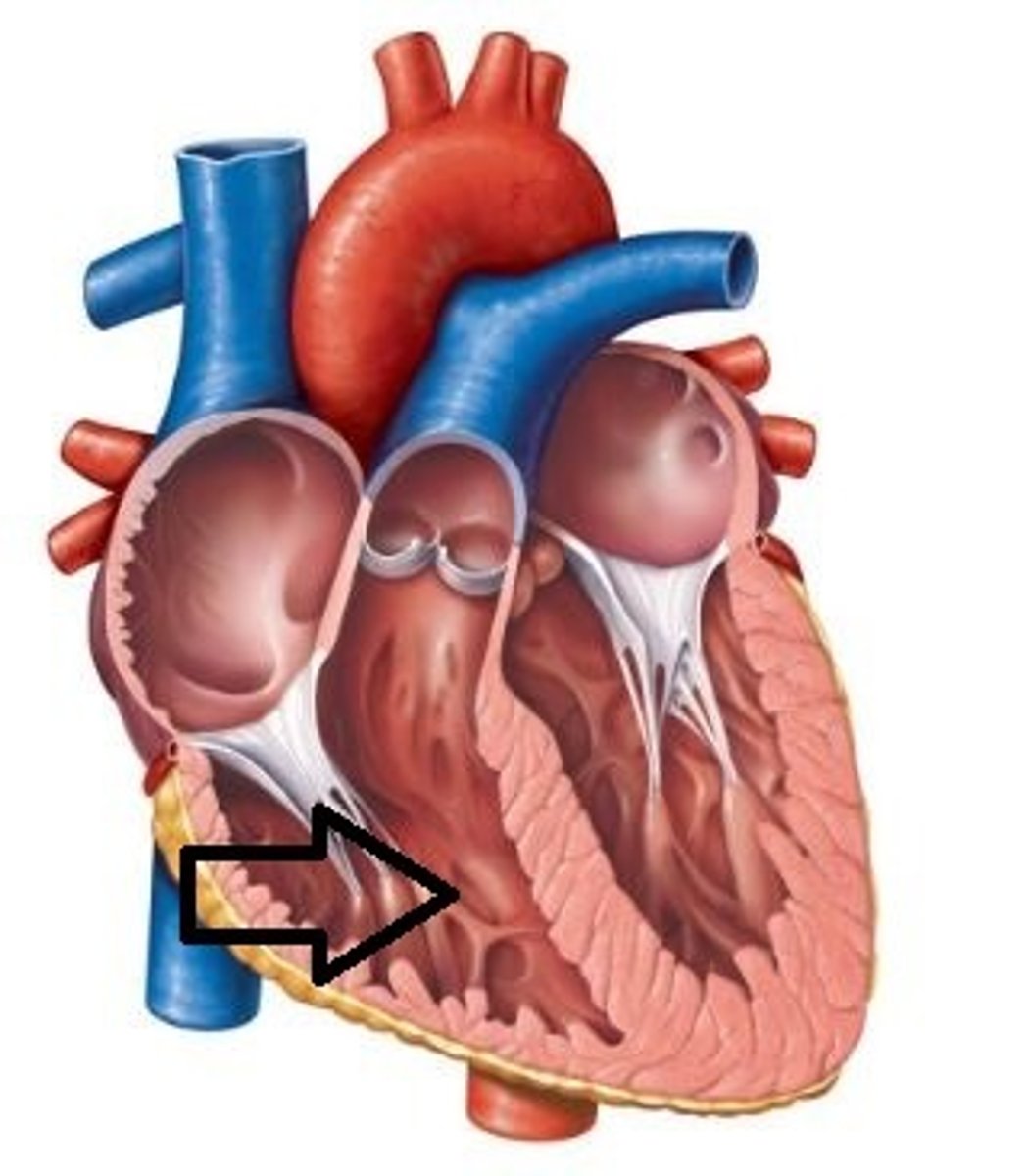
Left Ventricle
pumps oxygenated blood to the body
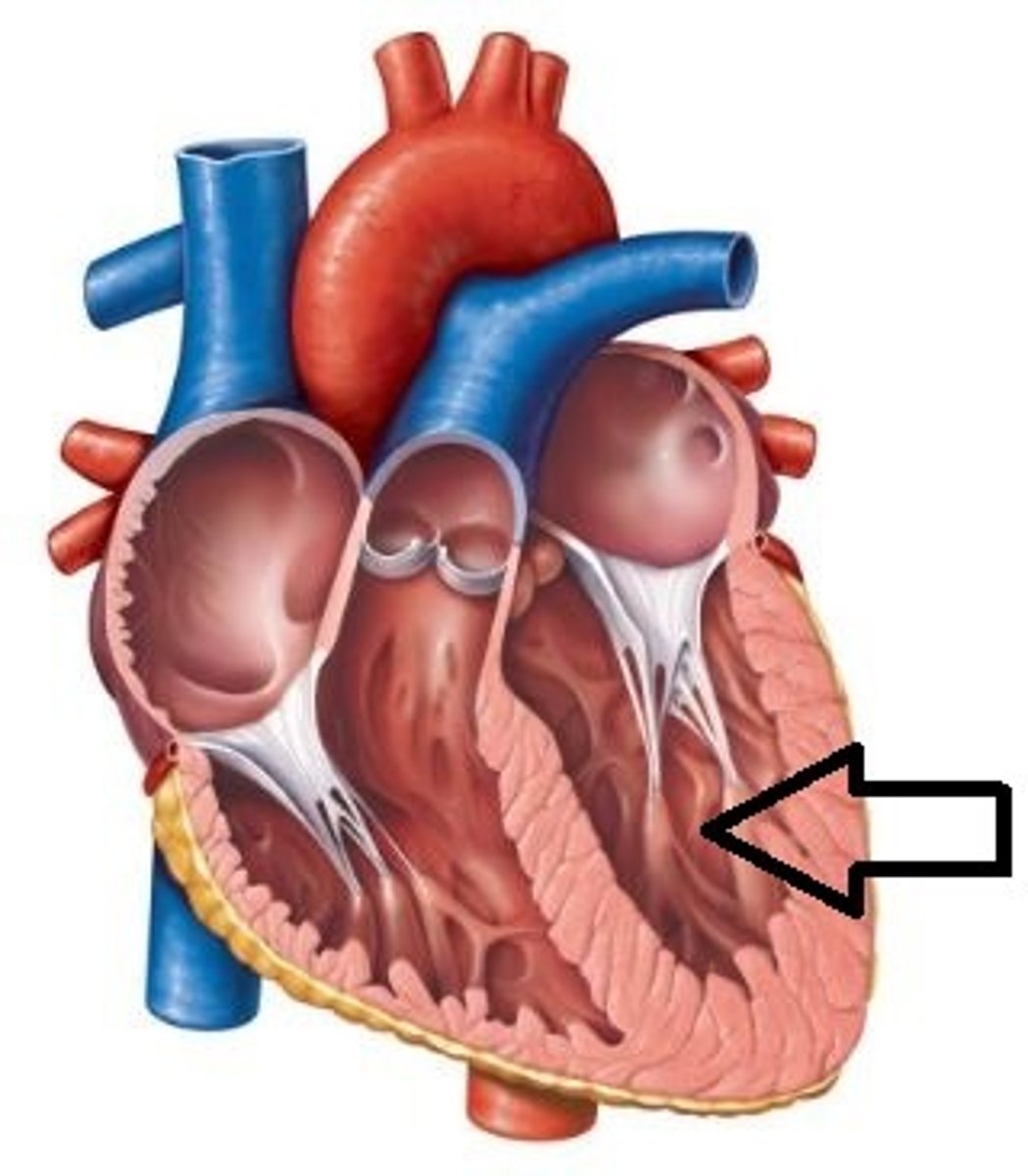
Apex
the highest point
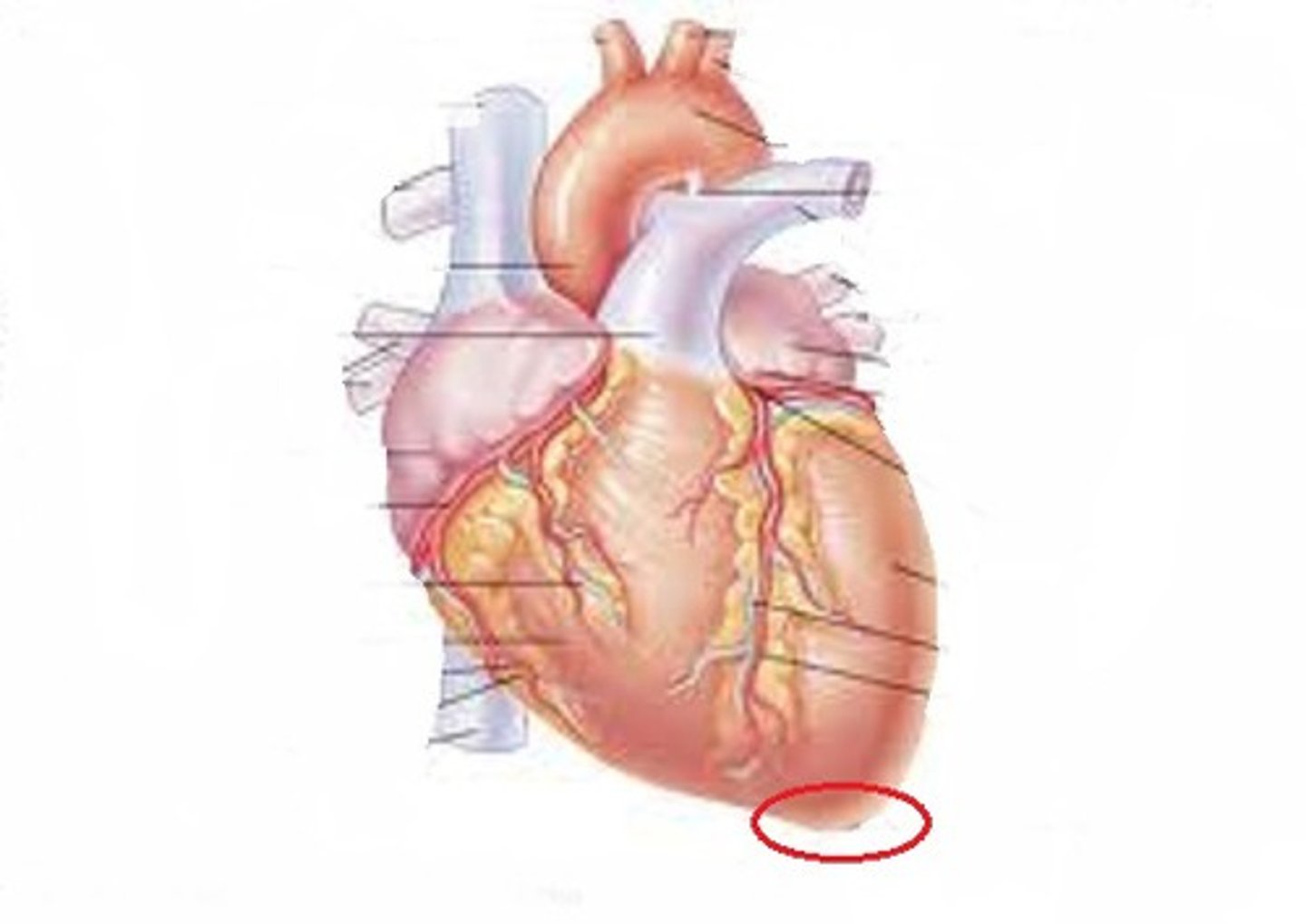
Pulmonary Valve
valve positioned between the right ventricle and the pulmonary artery
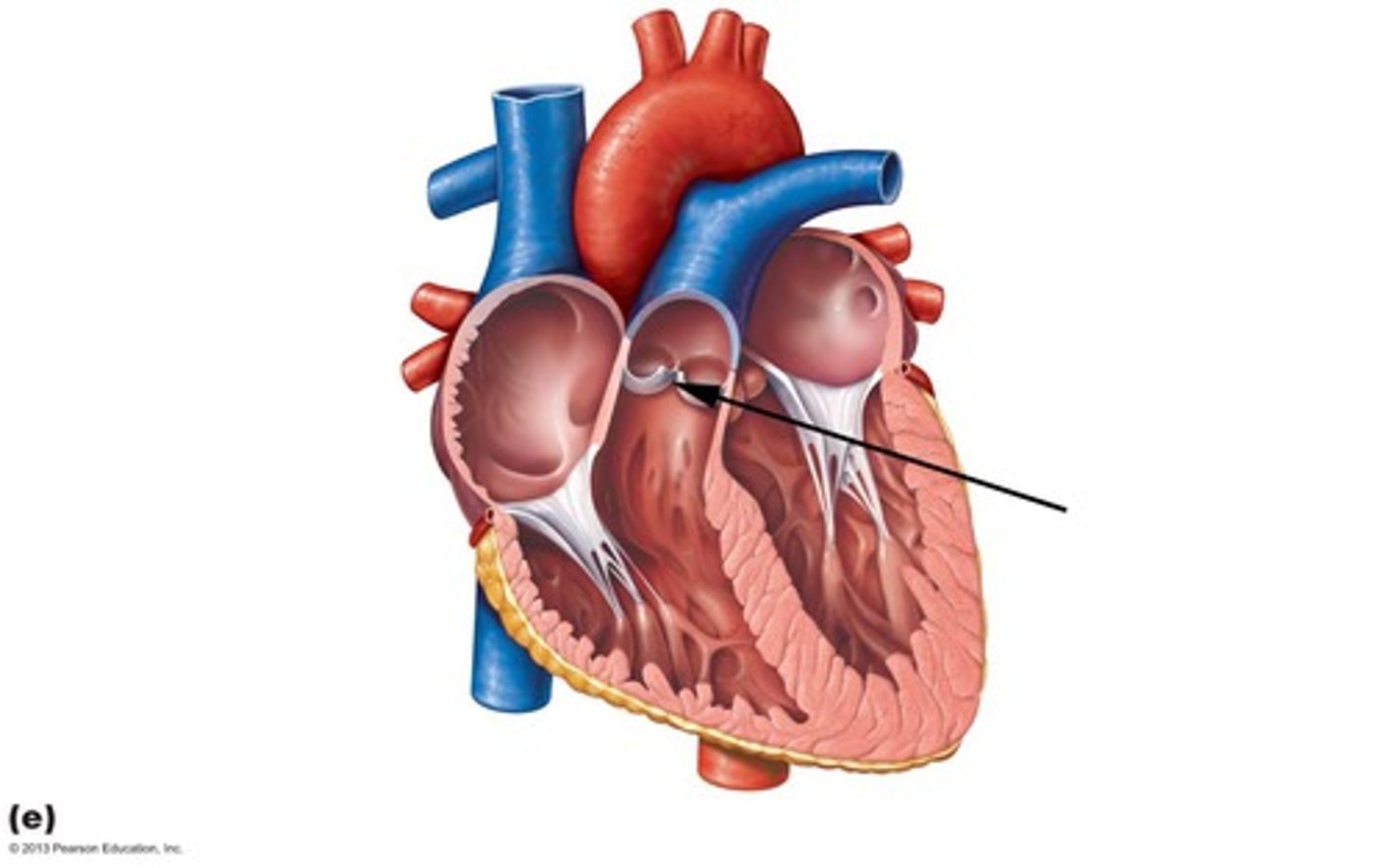
Trabeculae Carneae
muscular ridges on the internal surface of the ventricles
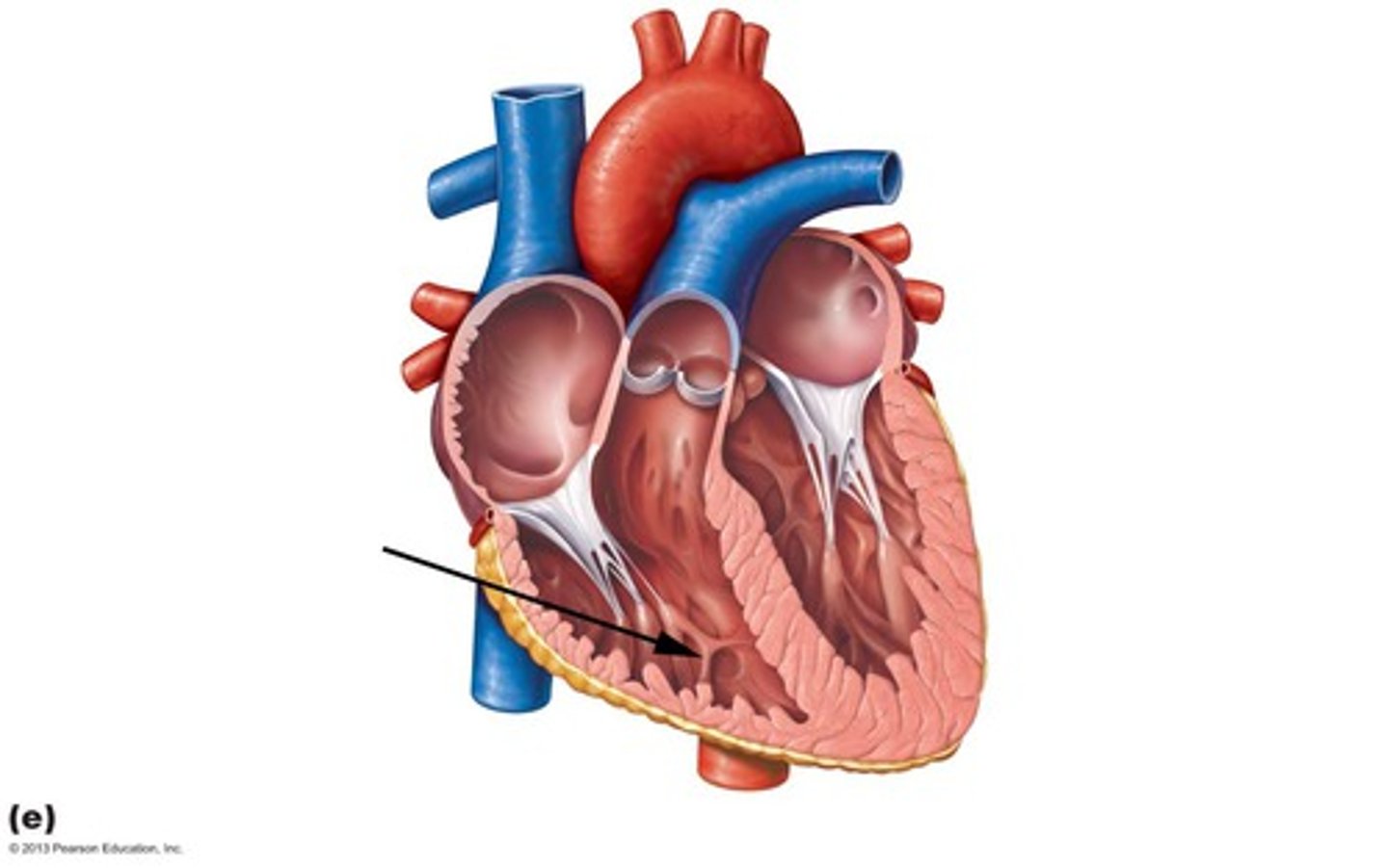
sinoatrial node
A small mass of tissue that is made up of Purkinje fibers, ganglion cells, and nerve fibers, that is embedded in the musculature of the right atrium, and that originates the impulses stimulating the heartbeat -- called also S-A node, sinus node.
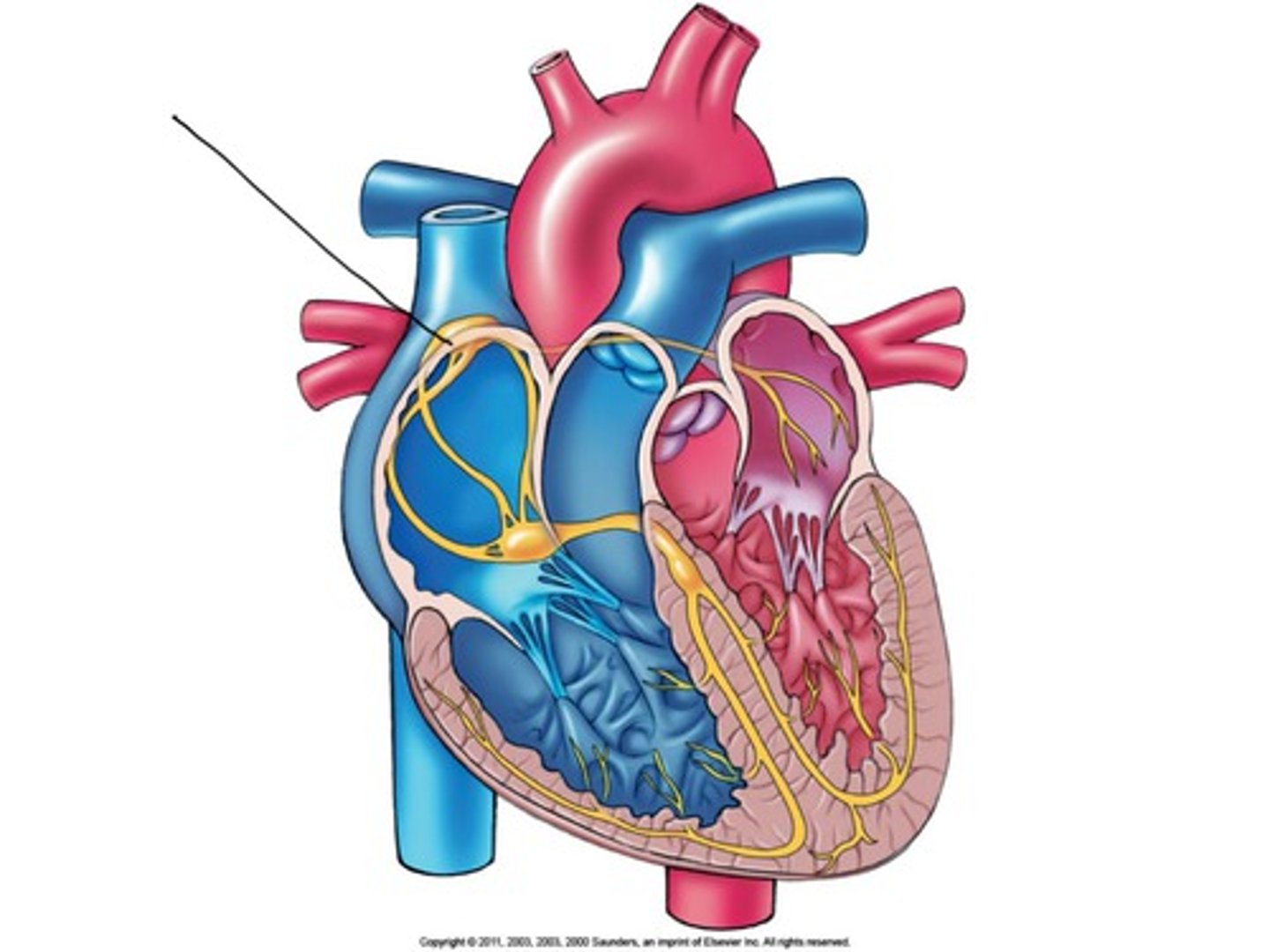
brachiocephalic artery delivers blood to
head, neck and upper extremities
Endocrinology
Study of hormones and endocrine organs; controls reproduction, growth, electrolyte balance, and more
Exocrine glands
Produce non-hormonal substances like sweat and saliva, have ducts
Endocrine glands
Produce hormones, lack ducts; include pituitary, thyroid, adrenal, and more
Chemical Messengers
Include hormones, autocrines, and paracrines; hormones travel in blood