Edema/Lymphedema **come back to**
1/101
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
102 Terms
secondary lymphedema
Mary is a 56 y/o female who was diagnosed with cervical cancer 10 years ago. Lymph node biopsy came back positive. She had a total hysterectomy and was treated with chemo and radiation. 6 months after radiation, Mary noticed some swelling in her right leg. What type of lymphedema does she have?
the vascular system
what systemic system of the body does the lymphatic system parallel
- Compromised of lymph nodes and vessels
- very delicate superficial vessels
what is the lymphatic system made of
1. RECYCLE PROTEINS
2. Immune Surveillance
3. Transportation of Digested Fat
what are the primary roles of the lymphatic system
autonomic nervous system
what system controls the lymphatic system
- Contractions of smooth muscle within the lymph vessel wall that allows for transport of lymph
- Skeletal muscle contraction can aid this transport
how does lymph transport occur
Unidirectional flow occurs due to one-way valves
in what direction does lymph flow and why
- Exchange at capillary level
- Arteries bring oxygen/nutrients to cells
- Veins remove waste/CO2
- 80-90% of fluid
what occurs to lymphatic vessels at the capillary level
- Recycles protein
- Immune Surveillance
- Transport of digested fat (chyle)
what are the functions of the lymphatic system
both vascular and lymphatic systems intact
what is required for fluid hemeostasis to occur
- The lymphatic system becomes overloaded
- Resulting in fluid remaining in the interstitium
What happens when the venous system is not functioning properly
- Small proteins taken away first into the lymphatic system
- Leaves large, hydrophilic proteins in the interstitium
- These proteins pull more water into the interstitium causing increase in swelling
If the lymphatic system becomes overloaded, resulting in fluid remaining in the interstitium, what will the resulting process be?
Edema is a Symptom - Lymphedema is a Disease
what is the difference between edema and lymphedema
Lymphedema
Accumulation of protein-rich fluid in the tissue space of the affected area
Can cause chronic inflammation and reactive fibrosis of the affected tissues
what are the primary effects of lymphedema
in the extremities but can also be present in the face, neck, abdomen or genital
where does lymphedema typically occur
When it lasts beyond the inflammatory stage
When does edema become problematic?
- dysplasia
- damage to lymphatic system
- overload
what are the main causes of lymphatic disorders
Primary lymphedema
what is lymphatic disorder due to dysplasia
- Cancer treatment
- Tumor
- Crush injury
what are some causes of damage that would result in lymphedema
- Chronic venous insufficiency
- Morbid obesity
- Pregnancy
what conditions can result in overload causing lymphedema
- extremities
- trunk
- face
- head and neck
- abdomen
- genitalia
Where Does Lymphedema Occur?
- cellulitis
- chronic venous insufficiency
- compartment syndrome
- complex regional pain syndrome
- DVT
- lipedema
- lymphedema
- May-Thurner syndrome
what are localized causes of edema
DVT
if a patient presents with an acute case (< 72 hrs) of unilateral LE edema what is the first thing we should assess for to rule out
whether it is doe to venous, lymphatic or systemic problems such as history of cancer, pelvic surgery, or trauma
if a patient presents with a chronic case (> 72 hrs) of unilateral LE edema what is the first thing we should assess for to rule out
- Sudden Onset
- Painful
- Cyanosis
- + Homan's possible
- Risk of PE
- Wells Rule
- D-Dimer
- Dx by doppler US
- Venous Obstruction
what are signs/symptoms of acute DVT
- active cancer
- immobility > 3 days or major surgery < 4 weeks ago
- calf swelling > 3cm compared to other calf
- collateral superficial veins present
- entire leg swells
- localized tenderness along deep venous system
- pitting edema, greater in symptomatic leg
- paralysis, paresis, or recent plaster immobilization of LE
- previously documented DVT
- alternative diagnosis to DVT as likely or more likely
DVT- clinical prediction (ie Wells Rule) check list
can present with lower leg (particularly the calf) or UE swelling depending upon location
where does a DVT typically occur in the body
D-Dimer Blood Assay
- by-product of a blood clot
- levels are elevated in patients with acute DVT
- major surgery
- major bleeding
- trauma
- pregnancy
- cancer
- acute arterial thrombosis
what factors can increase the levels of a D-Dimer Blood Assay
does not mean a DVT. But you should Follow with an Ultrasound.
what does a positive D-dimer blood assay indicate
low likelihood of DVT
what does a negative D-dimer blood assay indicate
- Tumor
- Chronic venous insufficiency
- Lymphedema
if you have ruled out that LE edema is due to a DVT or is Trauma/post-surgical edema, then what should you consider for the cause of the edema
- Gaiter Distribution
- Brawny
- Hemosiderin Staining
- Fibrosis of tissue
- Atrophy of Skin
- Possible wounds
- Pain above medial malleolus
- DVT puts pt at higher risk for CVI
- Venous obstruction
what are the clinical presentations of Chronic Venous Insufficiency
rule out cardiac/hepatic/renal disease
with cases of bilateral LE edema what is the first thing that the patient should be screened for
cardiac/hepatic/renal disease
what are some systemic disease that can result in bilateral LE edema
medication
in a case of bilateral LE edema if the cause is not cardiac/hepatic/renal disease and it is an acute case of edema (less than 72 hours) then what is the likely cause of the edema
- chronic venous insufficiency
- lymphedema
- lipedema
- idiopathic
in a case of bilateral LE edema if the cause is not cardiac/hepatic/renal disease and it is a chronic case of edema (more than 72 hours) then what is the likely cause of the edema
1. Medication induced
2. Systemic
what are the two types of Bilateral Lower extremity edema
- Chronic venous insufficiency
- Lymphedema
- Lipedema
if bilateral Lower extremity edema is not due to medication or systemic, then what are some other possible causes of the edema
lipedema
- Not a result of fluid accumulation
- Adipose tissue expansion
- Typically, Bilateral LE but NO swelling of the feet
- Lower extremity adipose tissue is out of proportion to the upper body adipose tissue
- bruising easily
- hypersensitivity
- abnormal accumulation of adipose from pelvic girdle to the feet
what is the triad of signs/symptoms of lipedema
- Anything that damages the lymphatic system
- Cancer related lymphedema
- filariasis
- Obesity
- Infection
- Surgery
what are causes of secondary lymphedema
filariasis
- Tropical disease
- parasitic infection/transmitted by mosquito
- Treatment/prevention with chemotherapy
- DVT
- Secondary lymphedema Secondary to cancer (breast)
- Primary disease
- lymphedema/vascular malformation
- Thoracic outlet
what are some primary causes of UE edema
- Complex regional pain syndrome
- Sign of malignancy
- Infection
- Trauma
- Post surgical
what are some secondary causes of UE edema
Cancer related Lymphedema
- Can occur anytime lymph system is damaged
- By cancer or its treatment
- 80% who get lymphedema, get it within 3 years of surgery All others: rate of 1% per year
- patients with Lymph node dissection (More nodes removed = higher risk)
- Chemotherapy
- Radiation To chest wall
- Elevated BMI
Who is at risk for lymphedema?
- Rapid Onset
- Proximal
- Associated with recurrence
- Neurogenic pain
what are the clinical presentations of Malignant Lymphedema
Primary Lymphedema
- Due to abnormal development of the lymphatic system where the system cannot meet fluid demands
- Can occur at birth or develop over time (Typically during teenage years or after pregnancy)
- Some have a genetic component
Milroy's Disease
what is an example of primary lymphedema
- Detailed History
- Skin integrity, port wine staining, scars
- Limb function, mobility, age-appropriate activity
- Photos
- Volumetric measurement
- Current edema patterns
- Pitting, stemmer sign, signs of infection, shape of limb
what does the Assessment of Lymphedema entail
onset, swelling in AM vs PM, with activity, with mood
when documenting the patient's current pattern of edema what should be included
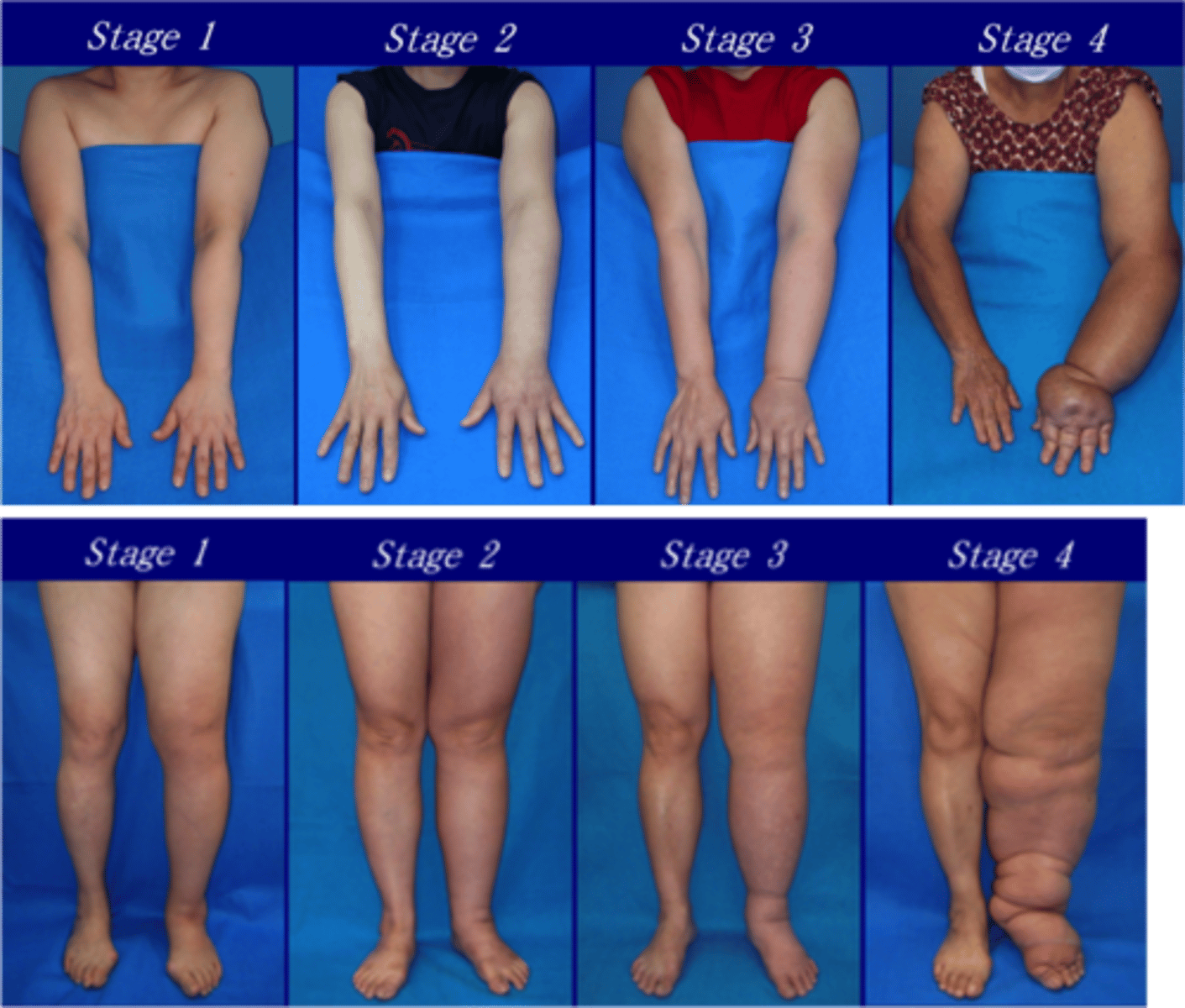
Stage 0- latency
stage 1 - reversible stage
stage 2 - spontaneously irreversible
stage 3 - lymphatic elephantiasis
what are the stages of lymphedema
- Not visible but tissue changes have begun
- Confirmed with bioimpedance
what is stage 0 lymphedema latency characterized by
what is stage 1 lymphedema spontaneous reversibility characterized by
- Swelling is palpable and visible but is intermittent
- treatment is indicated
what is stage 2 lymphedema spontaneous irreversibility characterized by
More severe; does not respond to elevation
what is stage 3 advanced stage elephantiasis characterized by
- Tissue fibrosis /local hypoxia in the tissues
- Significant risk of infection
Stages of Lymphedema
Axillary Web Syndrome
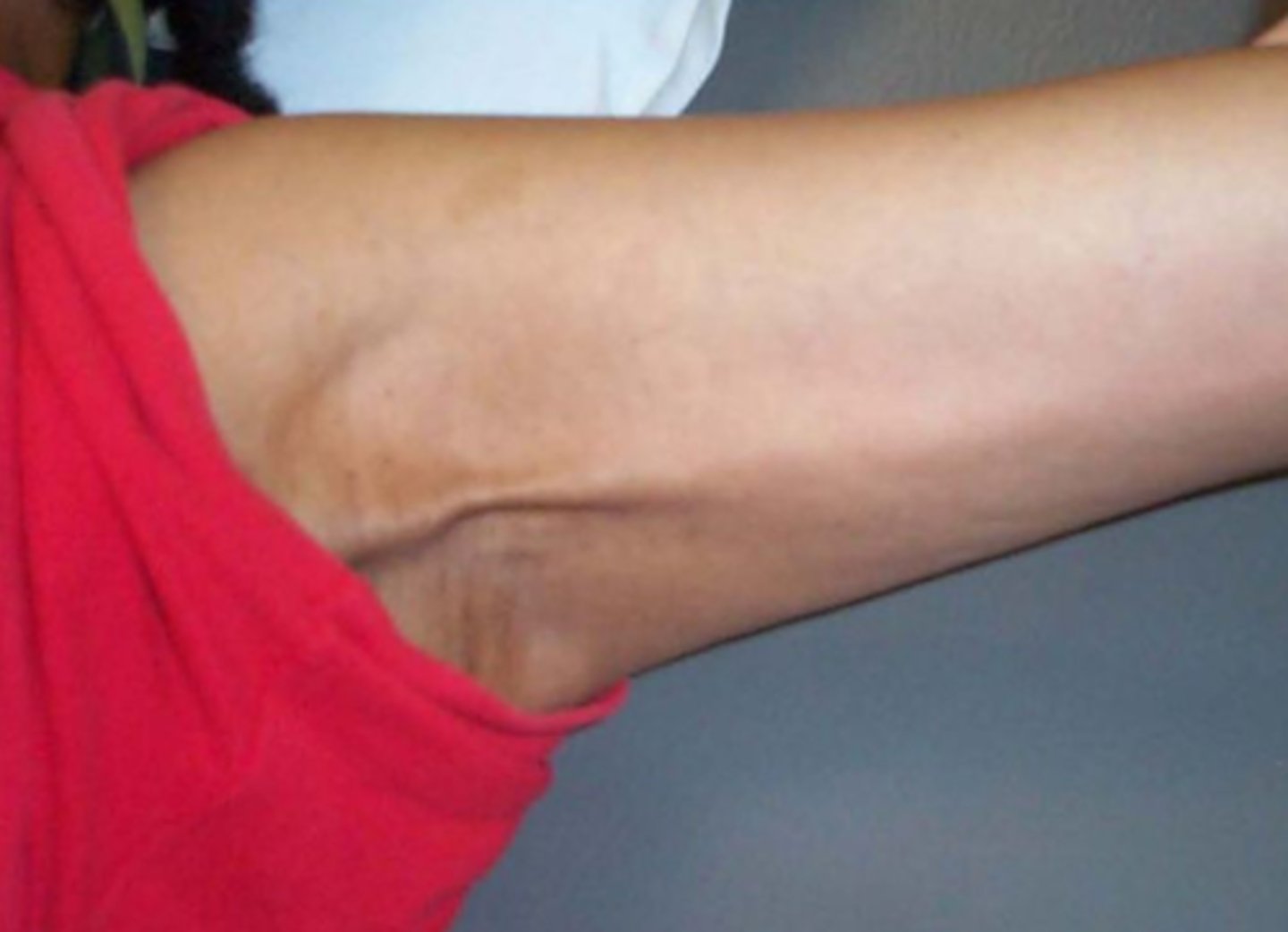
what is another name for axillary web syndrome
cording
what is Axillary Web Syndrome
- A cord or web of cords develops under the skin on the inside of your arm
- Side effect of having axillary lymph nodes removed or other breast cancer treatments
when might axillary web syndrome occur
Typically occurs days to weeks after surgery
what are the effects of axillary web syndrome
Limits range of motion of the UE and is painful
what does the treatment of axillar web syndrome entail
Often treated in PT with manual therapy and stretching
what should be considered about cellulitis
- Active infection (What signs and symptoms would you expect?)
- Should be treated with antibiotics
- CDT should not begin until the antibiotic course is completed
Reducing Risk of Developing Lymphedema
- Early detection
- Reducing overuse of untrained affected arm
- Avoid injury/trauma
- Avoid infection
- Avoid extreme temperatures
- Avoid prolonged inactivity
- Take care of the skin
what does early detection for Reducing Risk of Developing Lymphedema entail
- Prospective surveillance
- Identifying the edema before it progresses
- Patient report of heaviness
- Volumetric measurements
- Bioimpedence
- Garments when appropriate
Exercise to minimize risk of lymphedema
Twice weekly slowly progressive strength training is SAFE for breast cancer survivors who have had lymph node removal including Those WITH lymphedema and Those AT RISK FOR lymphedema
what are the benefits of Exercise to minimize risk of lymphedema
- Risk of lymphedema flare-ups decreased by HALF
- Among at-risk women with 5+ nodes removed, risk of ↑ arm swelling is reduced by 70%
- Substantive strength improvements
- core muscle mass increased
- Body image improvements
What are the Most Important Role as PT's for lymphedema/edema treatment
- Identify new edema
- Ensure that any PT treatment is SAFE
- Refer to a specialist
- Educate on risk reduction
Lymphatic Diagnostics tools/procedures
- Lymphoscintigraphy
- MR Lymphangiogram w/o contrast
- MRI/CT scan: reserved to rule in/out tumor
what are some Physical Exam Measures for edema/lymphedema
- Observation: skin inspection
- Palpation for pitting edema
- Stemmer sign
- ROM
- Sensory testing
- Functional testing
- Volumetric measurements
- Circumferential measurements
what is the Stemmer Sign
- Physical examination finding
- used to diagnose lymphedema.
- Examiner cannot pinch the skin of the dorsum of the foot or hand
what does a positive stemmers sign indicate
A positive Stemmer sign is a sensitive predictor for primary and secondary Lymphedema
Perometer for edema measurements
- Typically used only in the research setting
- High cost
- Uses light waves to estimate limb volume
- More accurate measurements
Bioimpedence Spectroscopy for edema measurements
- Reliable and accurate tool to detect the presence of lymphedema
- Able to detect Stage 0
- Uses how fast electrical current travels through the tissue
- CPG recommends using bioimpedance immediately after breast CA diagnosis and screening
what are the primary options for Medical Treatments for Lymphedema
surgery or medications
what are the two surgical options for treatment of lymphedema
- Lymph node transfer
- Liposuction/debulking
what are key points about Lymph node transfer surgical intervention of lymphedema
- Still in early stages/studies
- Patients will still require compression to maintain gains
what are key points about Liposuction/debulking surgical intervention of lymphedema
- Will remove lymphadematous tissue
- Ruins flow of lymphedema
- Long-term negative consequences
Only for Primary Lymphedema
what type of lymphedema is medication treatment able to be used on
what are 3 medications that can be used for treatment of lymphedema
- Sirolimus = Immunosuppressant; mTOR inhibitor
- Sildenafil = Treats pulmonary arterial hypertension
- Trametinib = Chemotherapy agent
what is the key point about Medical Treatments for Lymphedema
No viable treatment options. Conservative treatment is the best option
what is the conservative treatment method for lymphedema
Complete Decongestive Therapy
what is Complete Decongestive Therapy comprised of
- standard of care composed of 2 phases
- skin care and nail care
- manual lymph drainage
- compression therapy
- exercise
what does skin care and nail care as part of Complete Decongestive Therapy entail
prevent infections such as cellulitis
what does manual lymph drainage as part of Complete Decongestive Therapy entail
- gentle and superficial unless tissue is fibrotic
- often lasts approximately 30 minutes/session
what does compression therapy as part of Complete Decongestive Therapy entail
- short stretch bandages or alternative compression garments during phase 1
- compression garment or alternative compression garment phase 2
- use of foam
what does exercise as part of Complete Decongestive Therapy entail
pumping effect of muscle contractions to move lymph
Phase one of CDT (Complete Decongestive Therapy)
- Intensive decongestive phase carried out by a certified lymphedema therapist
- Treatment time for a session depends upon severity but typically 1 hour
- Recommended 5x/week 1 to 3 weeks;
- tapers down to 2-3 x/week until compression garment is received
Phase two of CDT (Complete Decongestive Therapy)
- Maintenance phase consisting of self care; not currently in PT
- Goal: maintain swelling reduction achieved in phase 1 of CDT
- Meticulous skin care
- Self MLD
- Exercise
- Daytime: Wear garment
- Nighttime: short stretch bandaging or alternative compression
Classes of Compression Garments
- class 1 = 18 -21 mmHg
- class 2 = 23 - 32 mmHg
- class 3 = 34 -46 mmHg
- class 4 = >49 mmHg
what is the typical wearing Schedule for Compression Garments for lymphedema
- Lymphedema: Some form of compression is recommended 23 hours/day
- Daytime: compression garment
- Nighttime: bandaging using short stretch bandaging
what is the typical wearing Schedule for Compression Garments for vascular edema
- Daytime: Worn while out of bed
- Nighttime: may or may not be required
Intermittent Pneumatic Compression for lymphedema treatment entails
- Goal is to reduce edema through mechanical stimulation of the lymph fluid
- Target pressure is 10 mmHg for UE and 30-40 mmHg for LE
- Patient is sedentary while the pump is in use
- Chambers sequentially fill from distal to proximal
what are contraindications for Intermittent Pneumatic Compression for lymphedema treatment
- DVT
- Acute infection
- malignancy
- anticoagulant therapy
Lymphatouch
- Modality used to treat edema, lymphedema, and scars
- Theorized to activate the lymphatic circulation through combination of negative pressure and vibration
- Cost: $8000+ for the Cadillac model
what does research say about K - tape for treatment of breast cancer related lymphedema
- Outcome of interest: UE limb edema/volume
- 7 included articles: risk of bias is high and study quality is low of included studies (Average PeDro 4.71 of possible 11
- All 7 articles found positive effect on reducing limb volume (pre vs. post tx)
what are the impacts of lymphedema/edema on patients
- Physical: mobility, limited ADL's/social participation
- Clothing challenges
- Psychosocial impact: physical appearance has changed and there is no cure
- Economic Burden