Anat - Unit 6
1/41
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
42 Terms
Digestion (Mechanical vs Chemical)
Mechanical - breaks food down physically (chewing, mixing)
Chemical - enzymes break large nutrient molecules (proteins, lipids, carbohydrates) into smaller ones
Absorption of digestive system
Movement of end product (nutrients) move from lumen of alimentary canal (GI tract) to blood/lymphatic system
Propulsion (motility) + Peristalsis
Propulsion - Movement of ingested food through the alimentary canal (RESULT OF PERISTALSIS)
Peristalsis - wave-like movement to push the food forward (THE PROCESS)
Secretion of digestive fluids
GI tract & accessory glands (salivary glands, pancreas, liver) secret digestive fluids
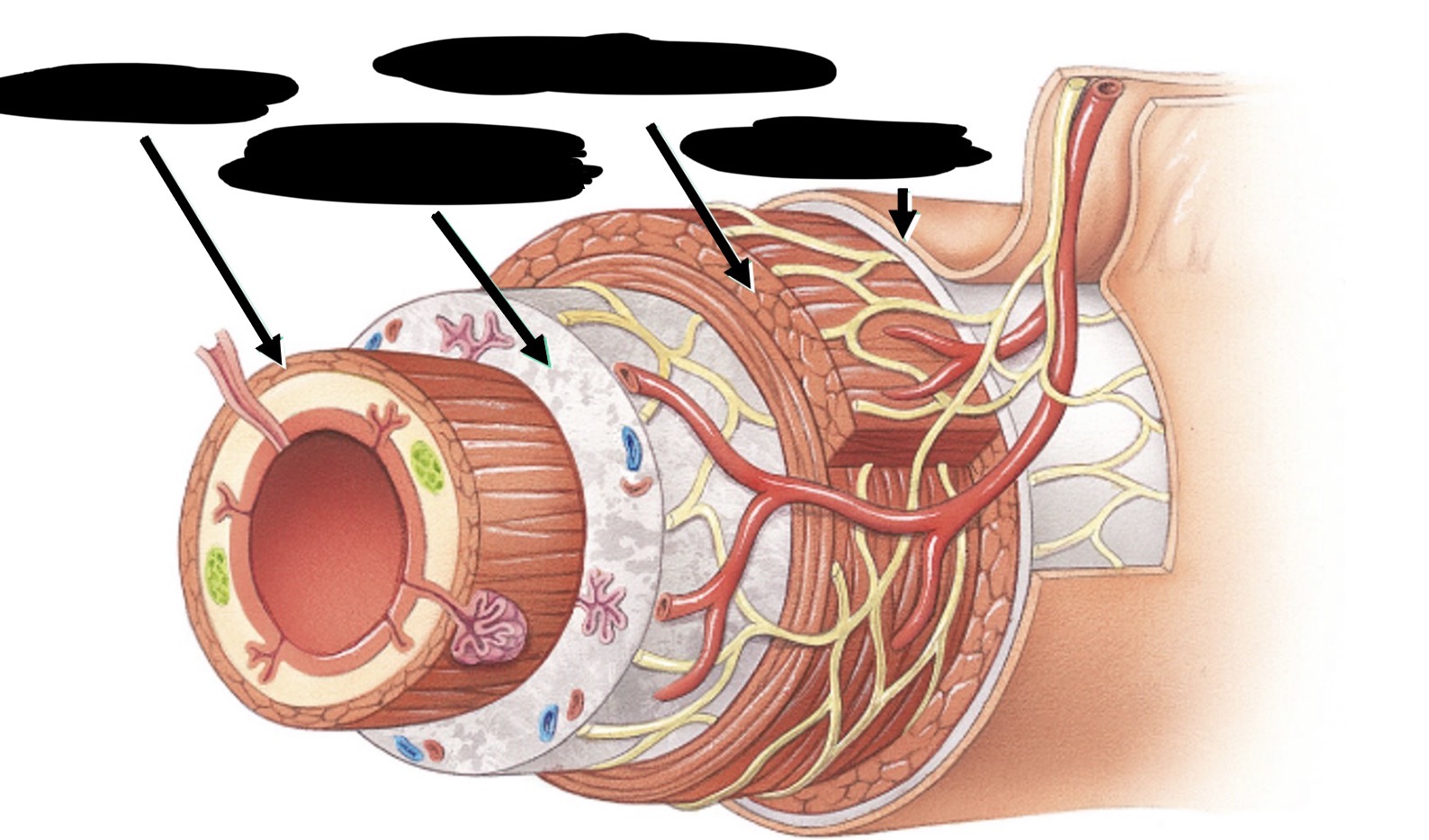
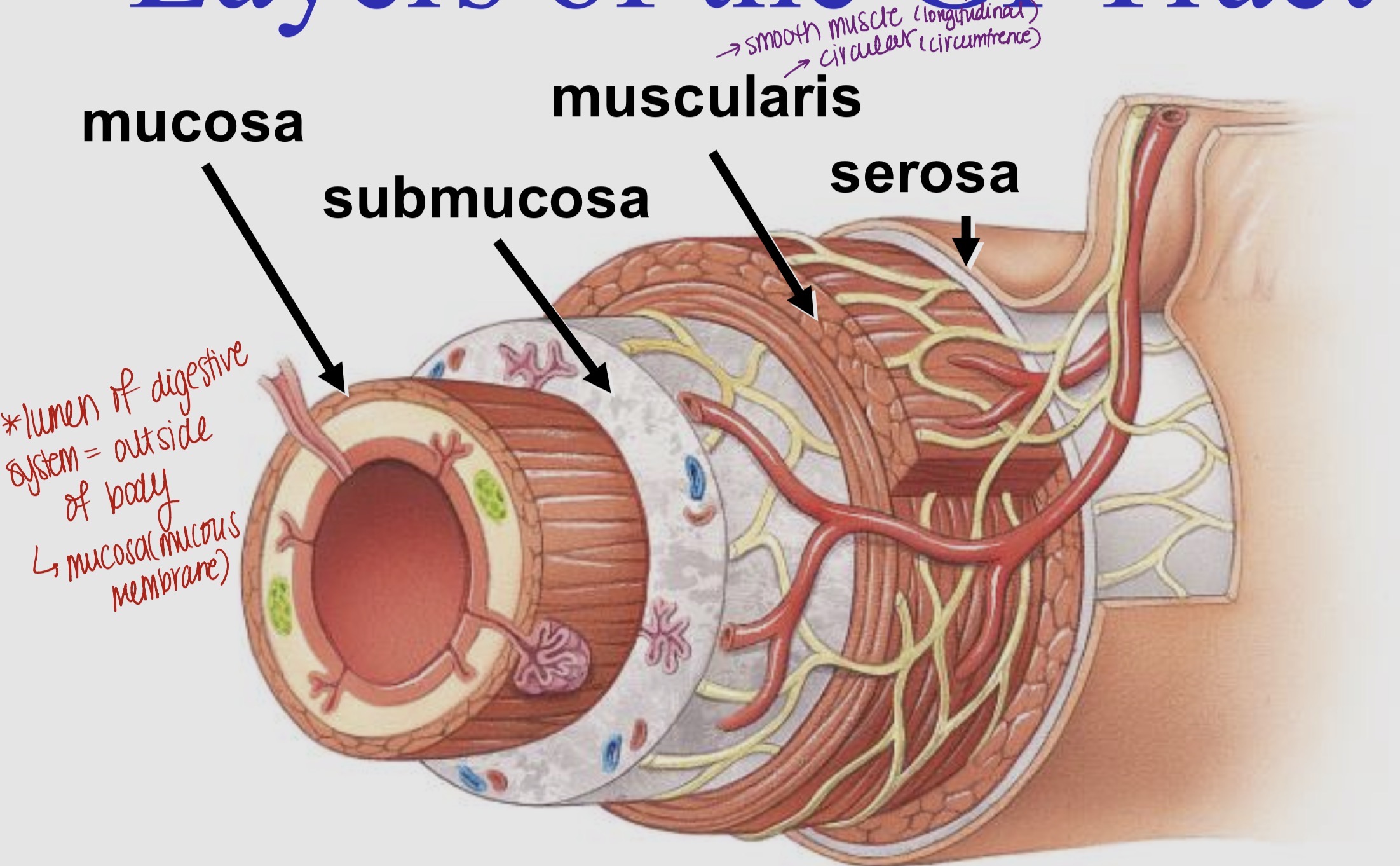
Label the layers of GI tract
Peritoneum (serous membrane)
Visceral Peritoneum - covers many abdominal organs
Parietal Peritoneum - lines walls of cavity (abdomen)
Peritoneal cavity - space between layers, contains little serous fluid (reduces friction)
Peritoneal Fold - Anatomy and Physiology (Part 1)
Two fused layers of serous membrane
Supports:
Organ nerves
Blood vessels
Lymphatic vessels
Extends from posterior abdominal wall to:
Liver
Stomach
Spleen
Most of small intestine
Transverse colon
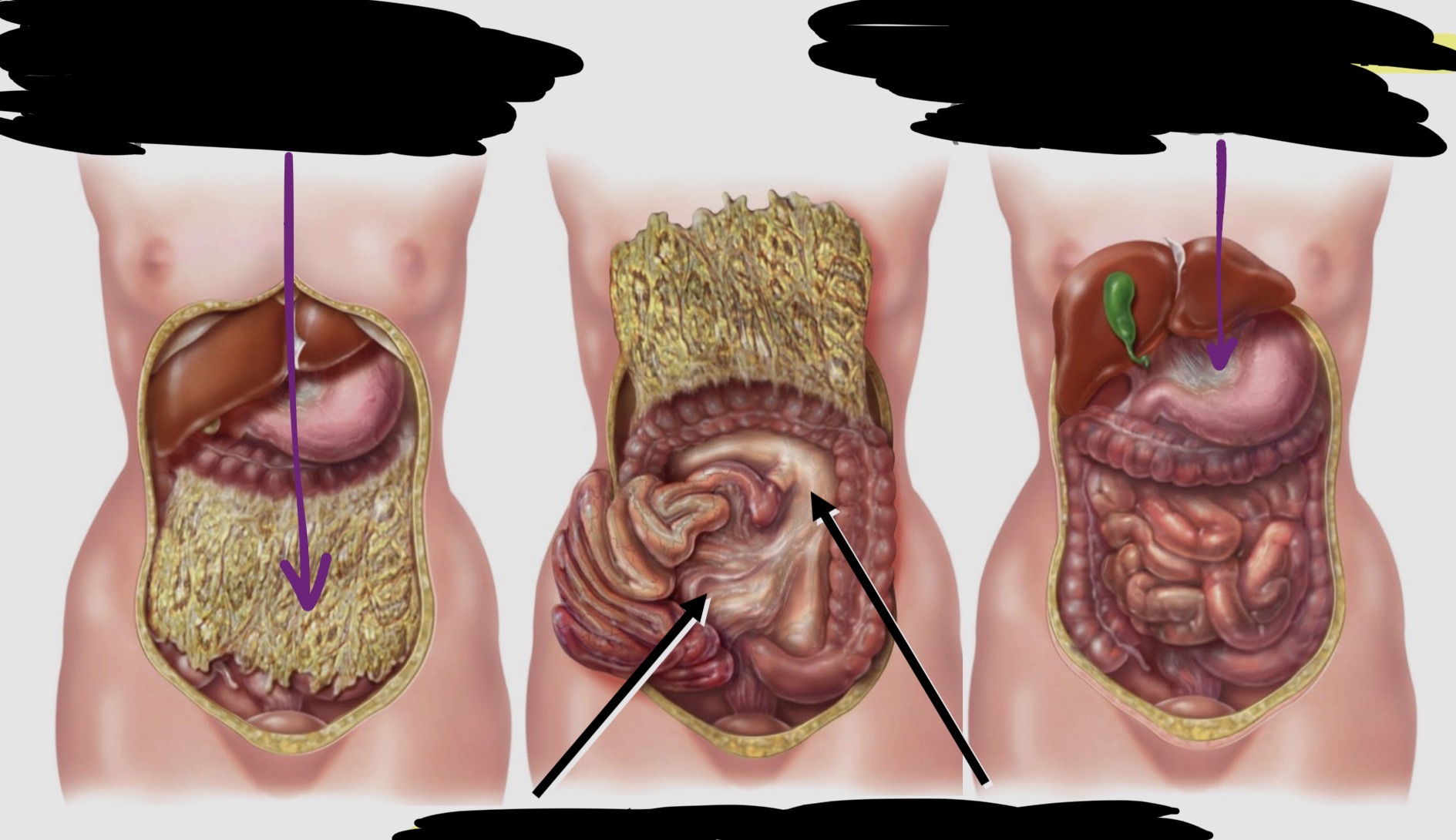
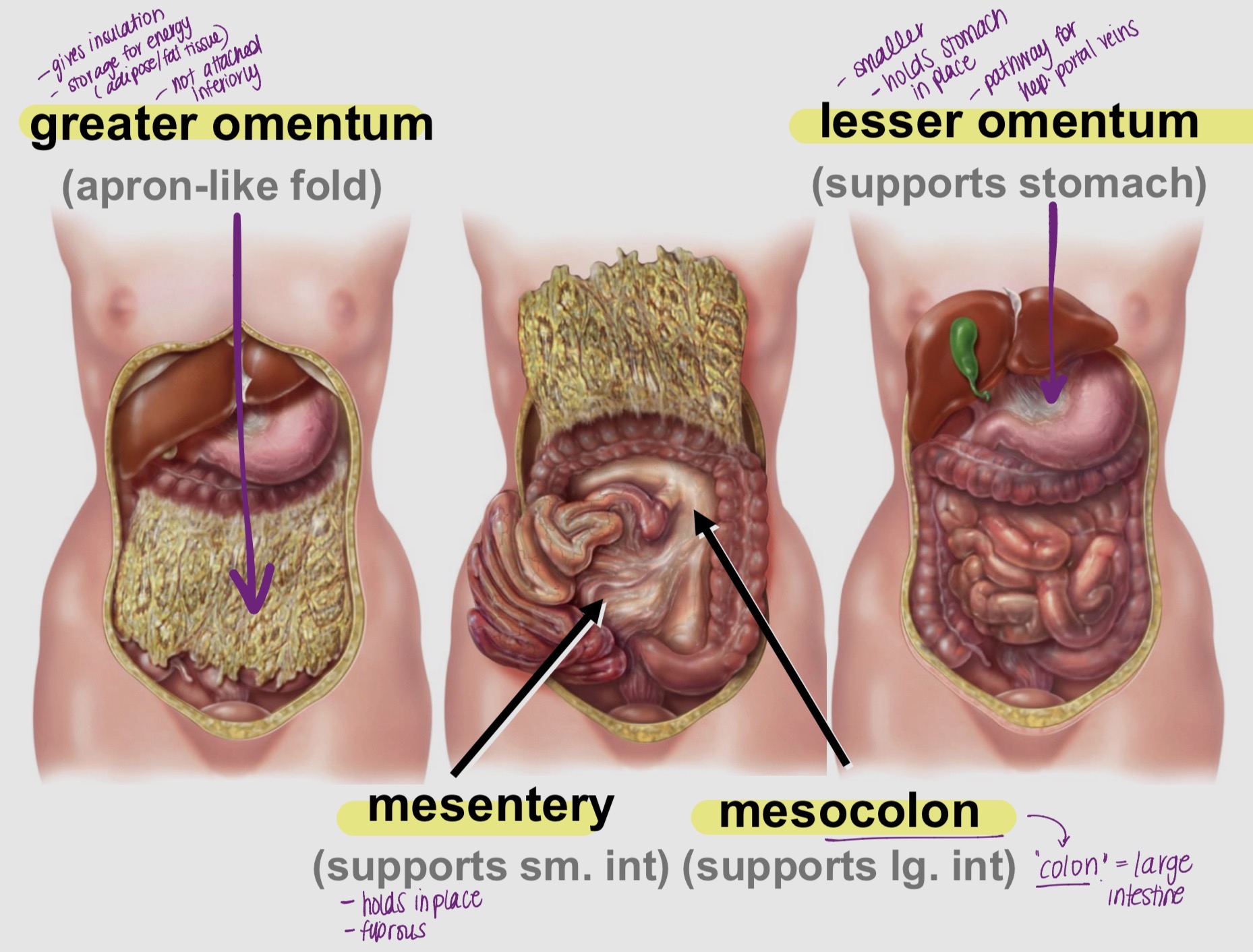
Types of Peritoneum Folds & function (Part 2)
Greater Omentum:
gives insulation, storage for energy (fat, adipose)
Mesentery:
supports sm intestines (holds in place)
Mesocolon:
supports lg intestines (colon= large)
Lesser Omentum:
supports stomach (smaller, pathway for hep.portal veins)
Major Divisions: Alimentary Canal vs Accessory Glands
Alimentary Canal - Digestive tract/ GI tract
pathway from oral to anal opening
Accessory Glands - everything else of GI tract
Chemical digestion helpers, no direct food contact
Mouth - Oral Cavity (Anatomy and Physiology)
Formed by: cheeks, tongue, hard & soft palate
Orbiculares oris in lips (changes shape for speech, closed mouth)
Buccinator mm in cheeks
Lined with stratified squamous epithelium (mucous membrane) for food
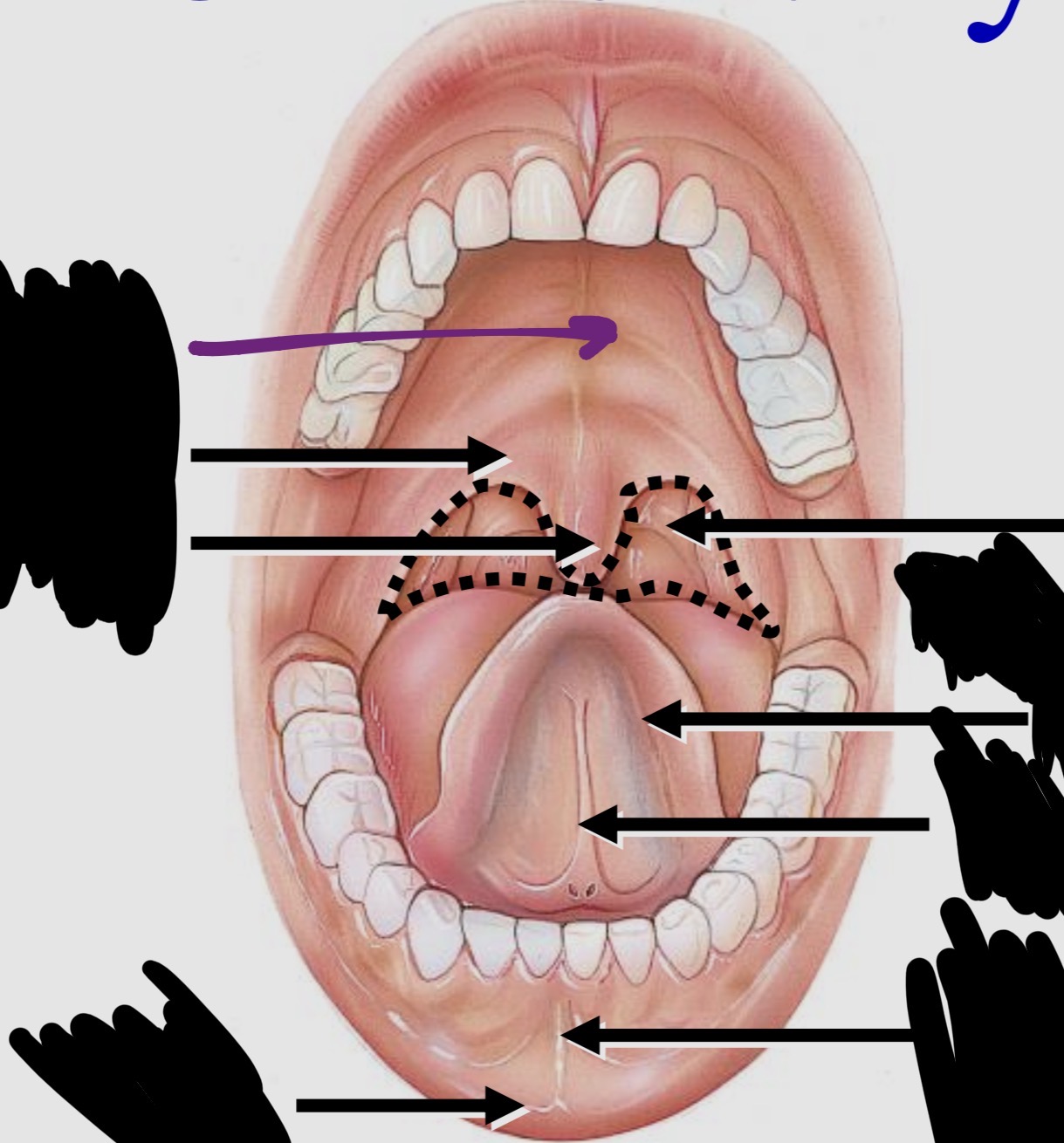
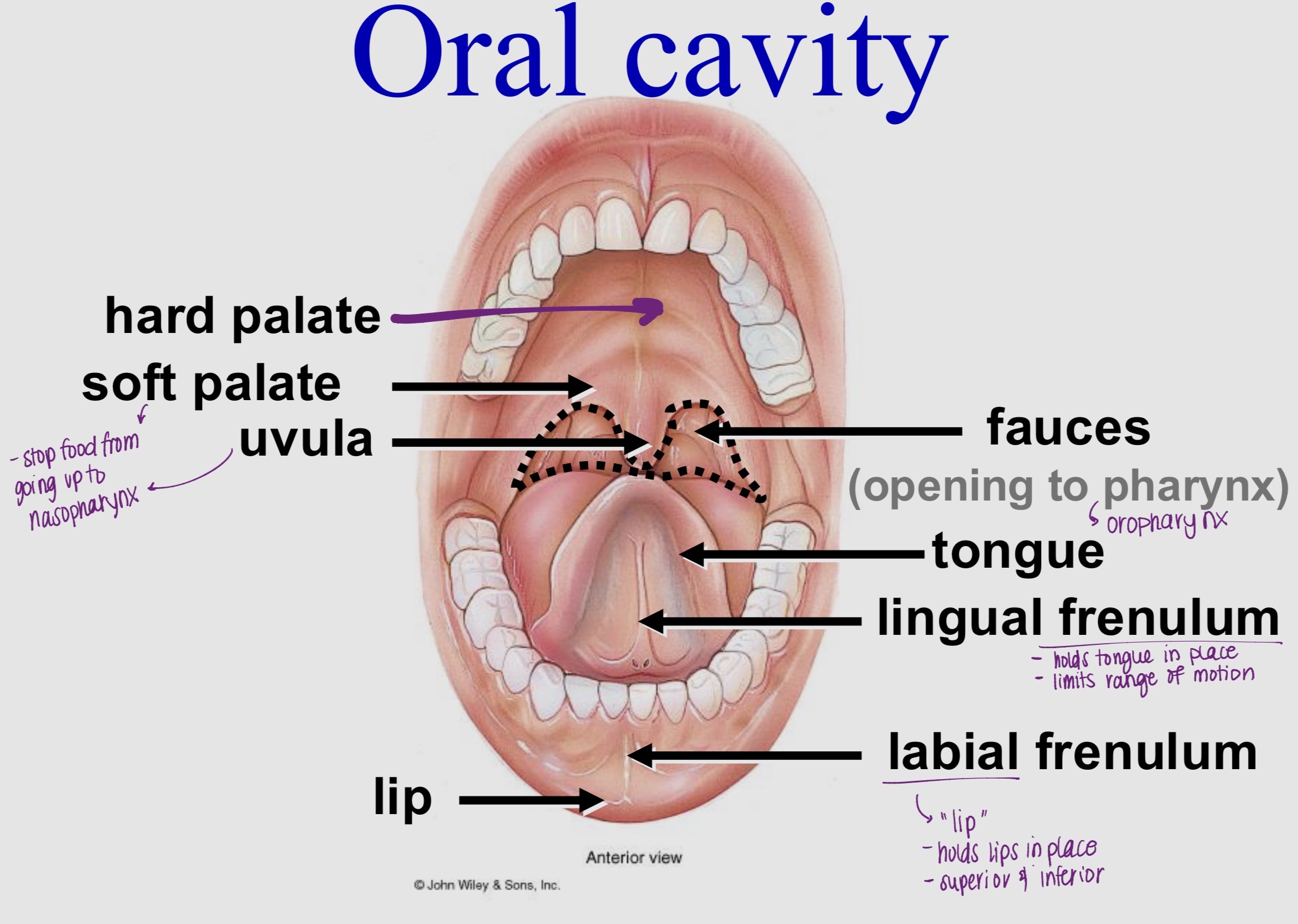
Oral Cavity - Label the Diagram
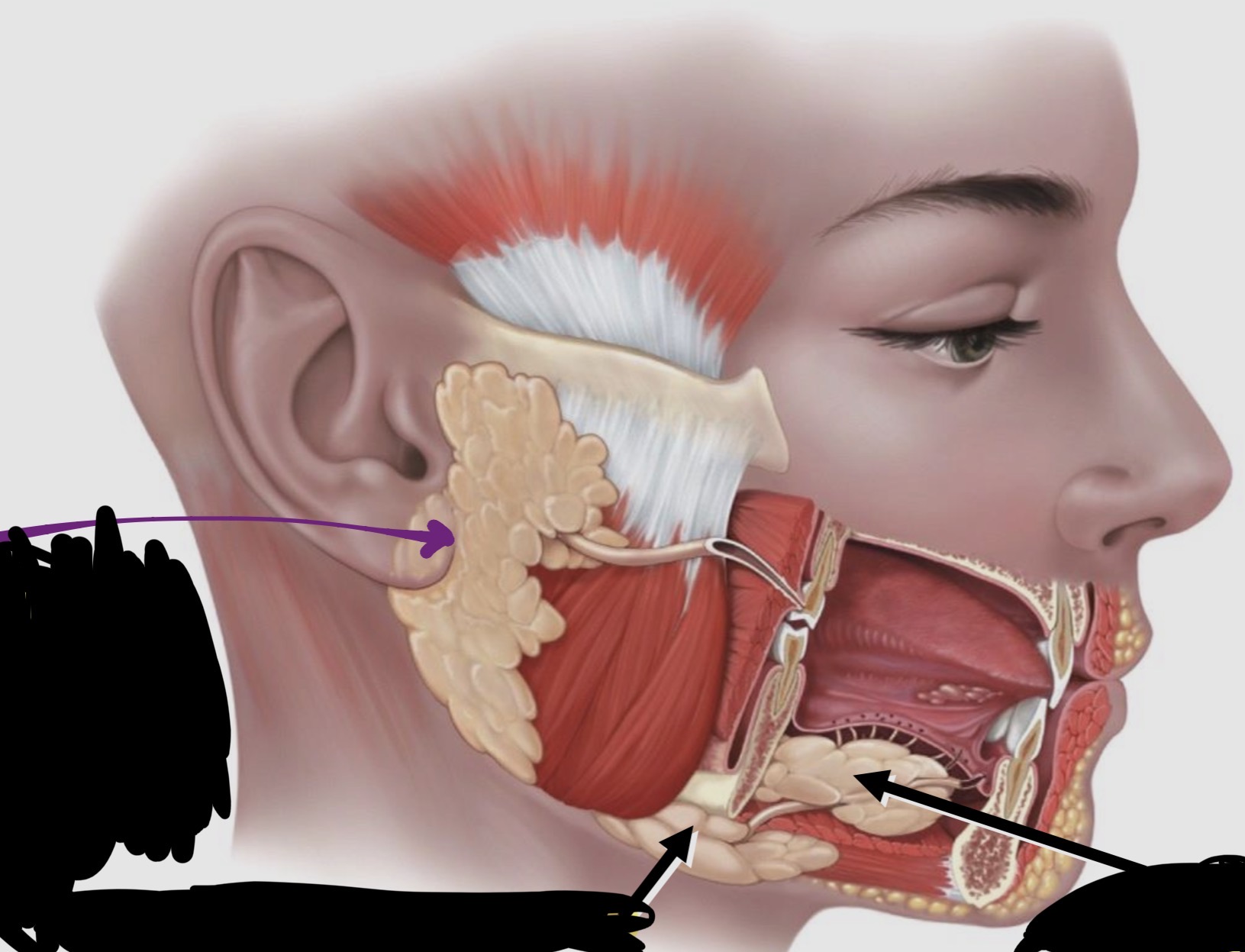
Salivary Glands - label the Diagram
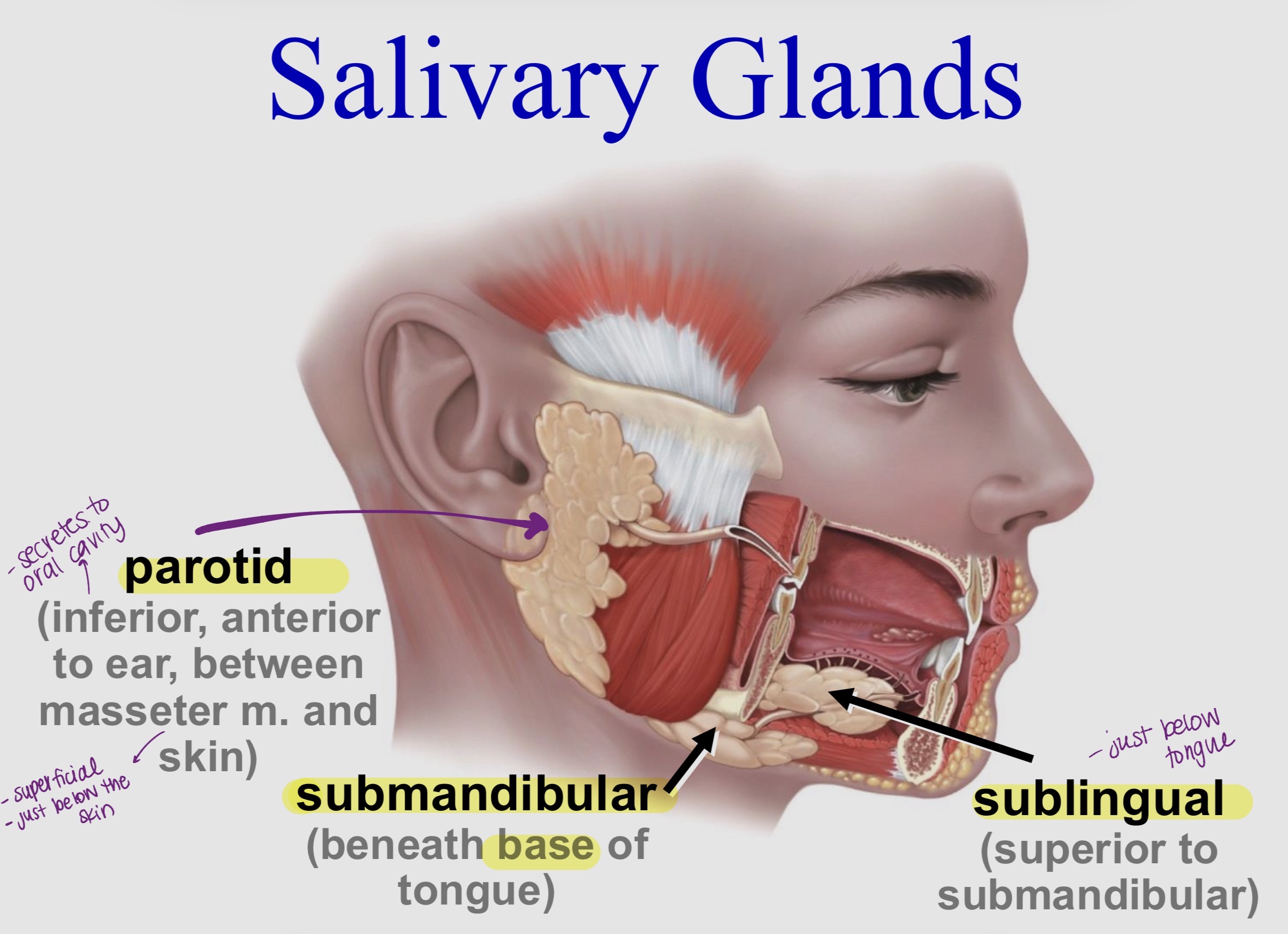
Saliva (Anatomy & Physiology)
Secreted from small glands in oral mucosa
1000 - 1500 ml secreted/day (most from the “big 3”)
Cleanses, moistens mouth & pharynx
Saliva Composition
•water - dissolves food, facilitates taste
•mucus - lubricates food
•urea, uric acid - metabolic wastes
•Ab’s - inhibits bacterial growth
•lysozyme - kills bacteria
•salivary amylase - acts on starch → carbohydrates
•lingual lipase - acts on triglycerides
Salivation Control - stimulation & inhabitation
Stimulated by: sight, smell, sound, memory of food, mechanical stimulation
Inhibited (reduced) by: fear, anxiety (SNS)
Tongue (General Anatomy)
Skeletal muscle
Covered with mucous membrane
Contains taste buds on surface
Has papillae
Tongue (extrinsic muscle)
Attach to:
Hyoid
Mandible
Hard palate
Styloid process
Function:
Move tongue:
In/out
Side-to-side
Help chewing and swallowing
Tongue (Intrinsic muscle)
Located within tongue (originate and insert to CT)
Function:
Change shape and size
Aid speech and swallowing
Digestion in mouth (in dept)
Mechanical digestion:
Mastication (breaksdown food)
Mixes with saliva to form bolus
Chemical digestion: (breakdowns)
Salivary amylase → starch digestion (carbs)
Lingual lipase → triglycerides (fats)
Deglutition - name the 3 phases
Beginning of the end of voluntary portion of digestive system.
Three phases:
Voluntary
Pharyngeal (involuntary)
Esophageal
Voluntary phase
Tongue pushes bolus to back of oral cavity (anterior to posterior)
Pharyngeal Phase
Bolus stimulates receptors in oropharynx
Signals to deglutition centre in brainstem
Uvula & soft palate blocks nasopharynx
Vocal cords close
Epiglottis blocks glottis (vocals closed)
Esophageal phase - Start
Upper esophageal sphincter relaxes
Bolus enters esophagus (No more voluntary control)
Esophageal phase - End
Lower esophageal/cardiac sphincter relaxes (prevents stomach acid from jumping to esophagus)
Bolus enters stomach
Esophagus
Moves ingested food by peristalsis
From pharynx → thoracic cavity → stomach
Histology of Esophagus
Mucosa
Submucosa
Muscularis:
Upper = skeletal
Lower = smooth
Sphincters at both ends
Adventitia
Stomach (Anatomy)
J-shaped sac
About 1.5 L capacity
Located in left upper quadrant of abdominal cavity
Inferior to diaphragm
Anterior to pancreas
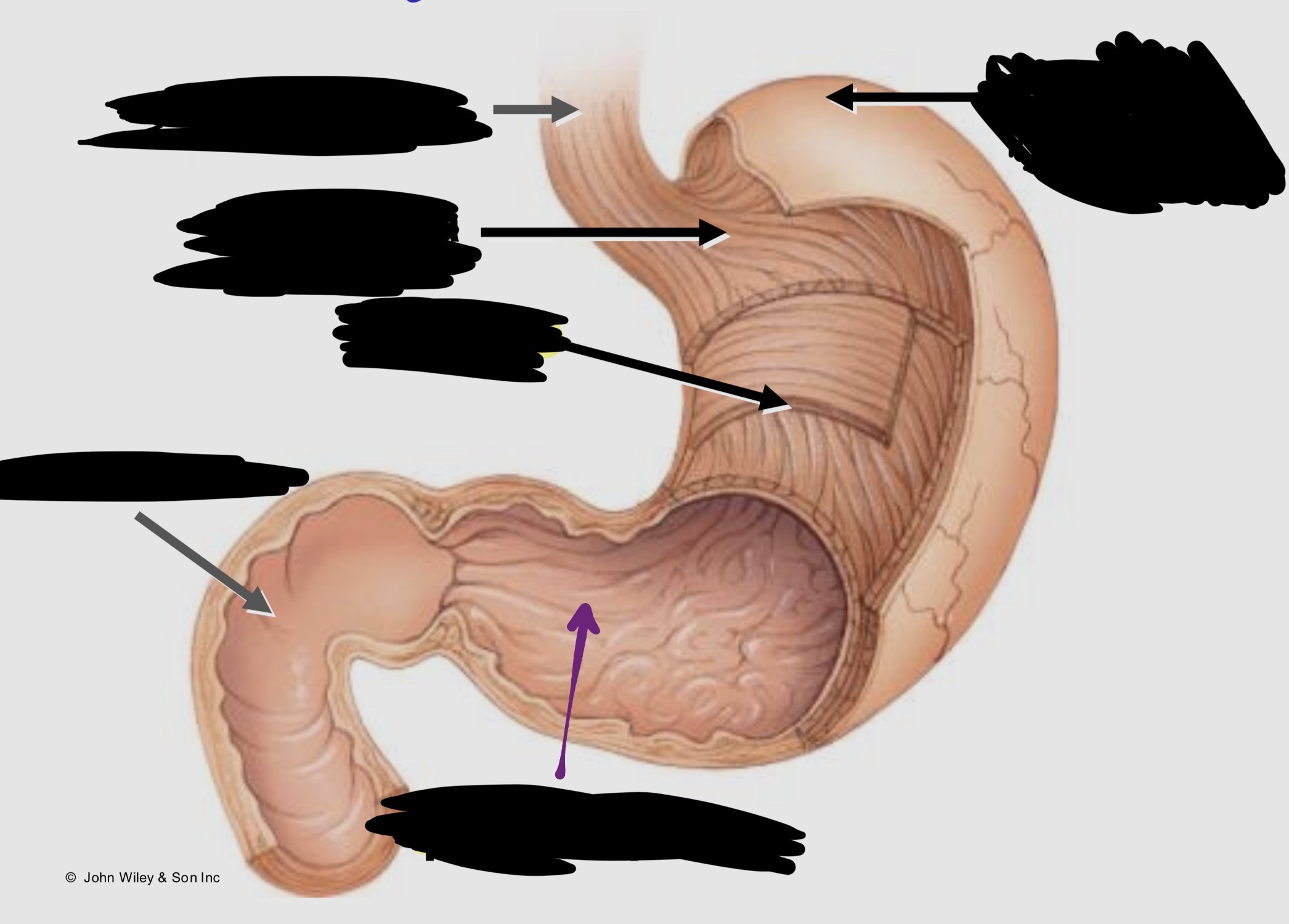
Label the stomach
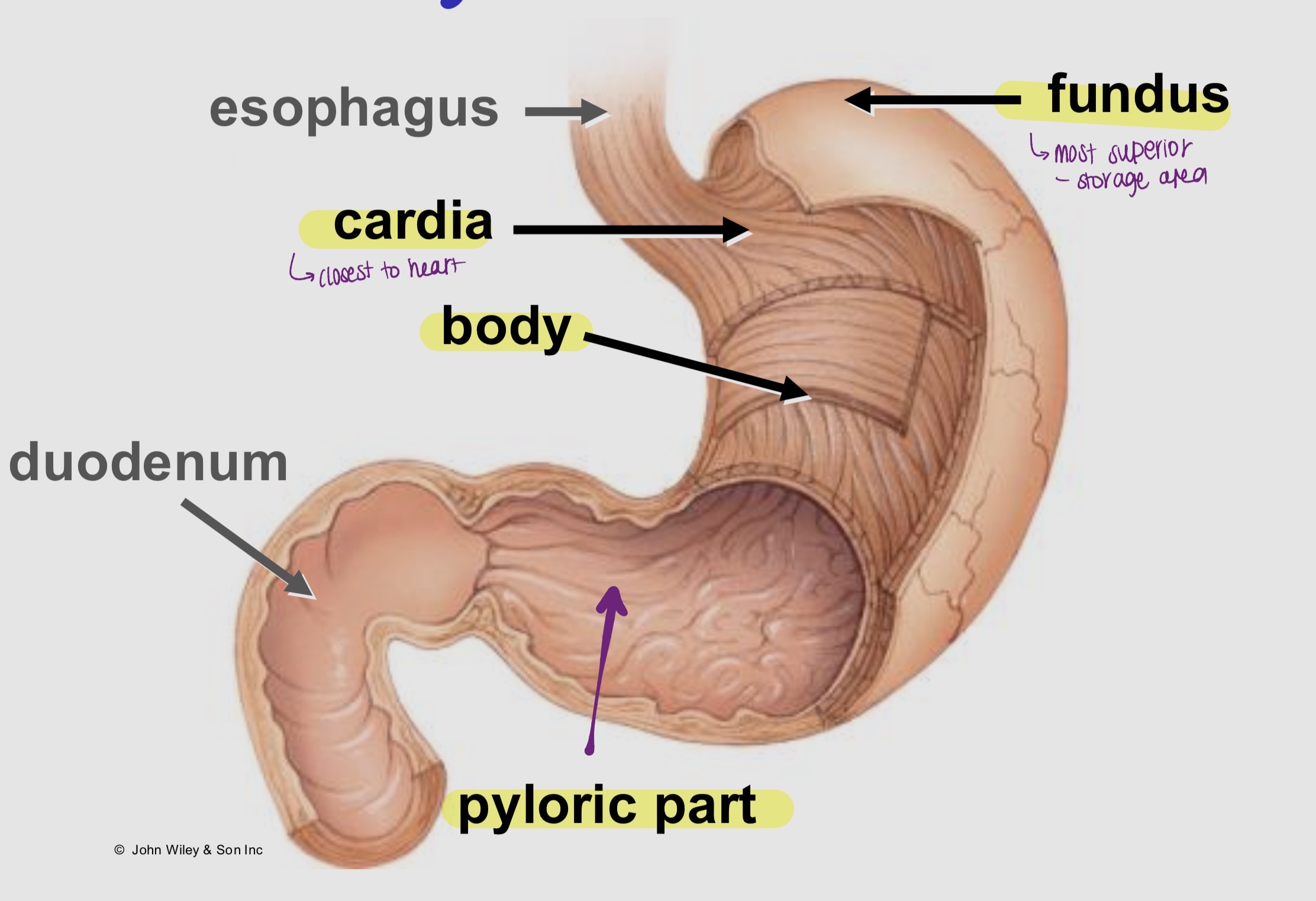
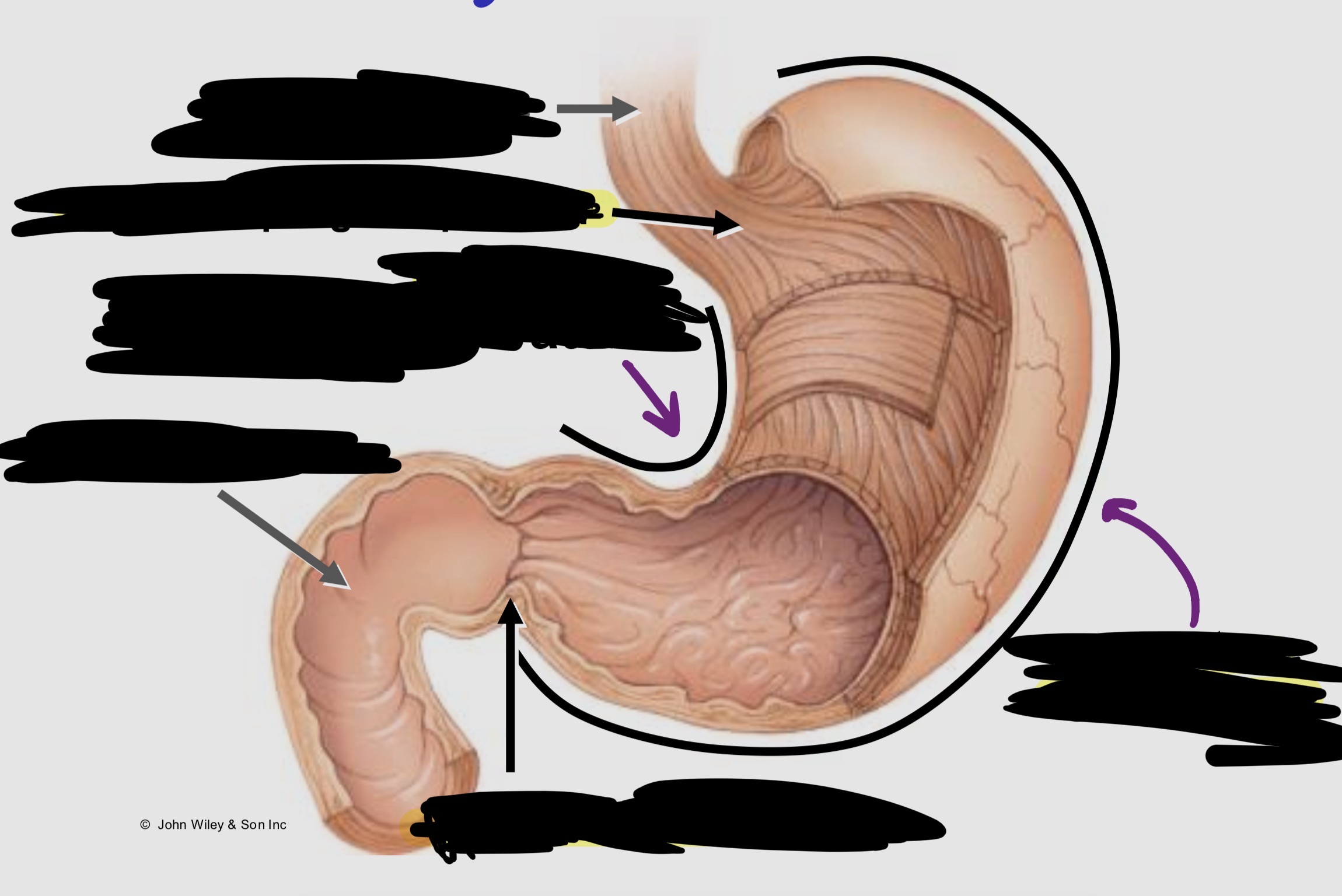
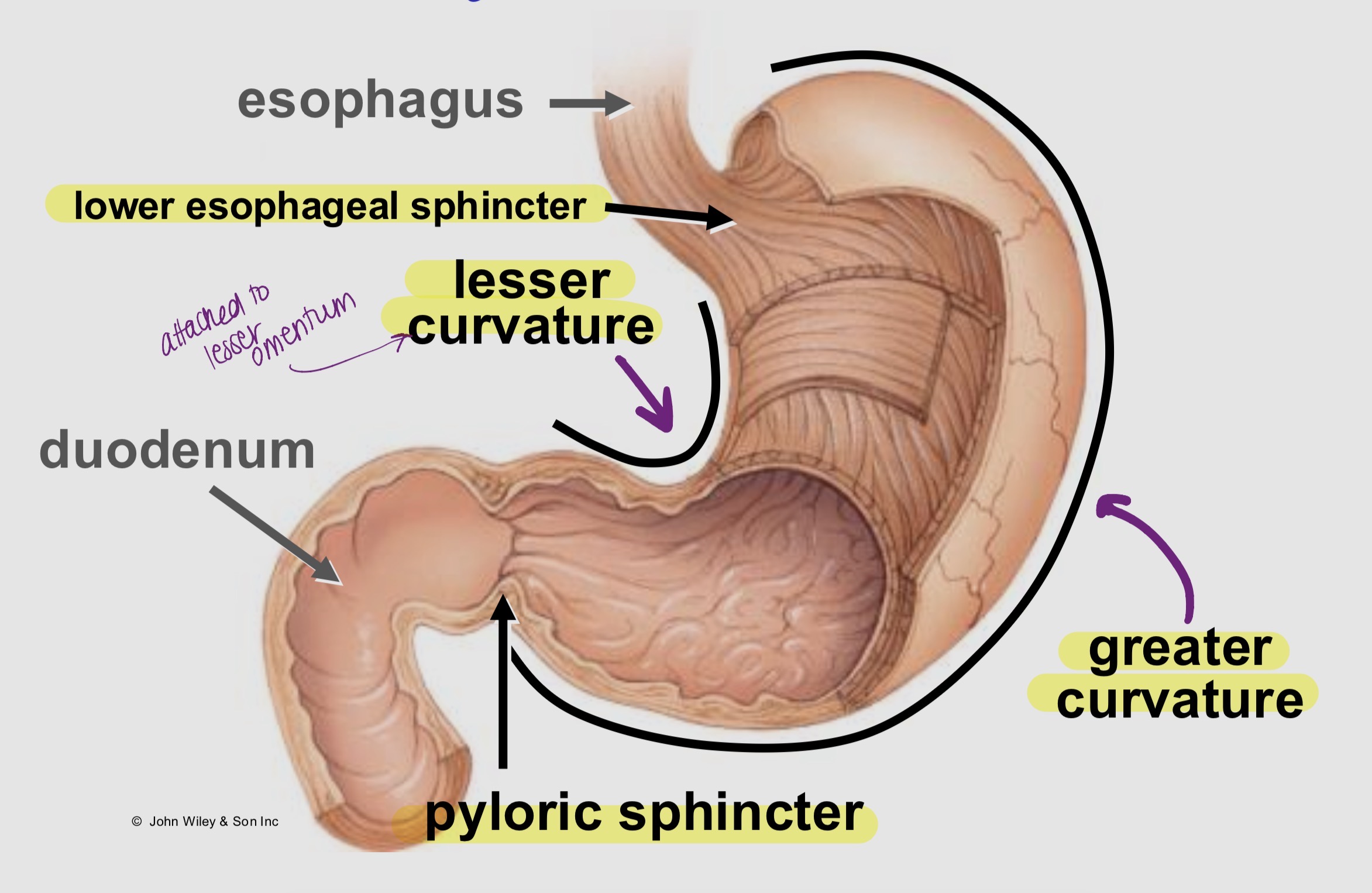
Label the stomach (curvatures and sphincters)
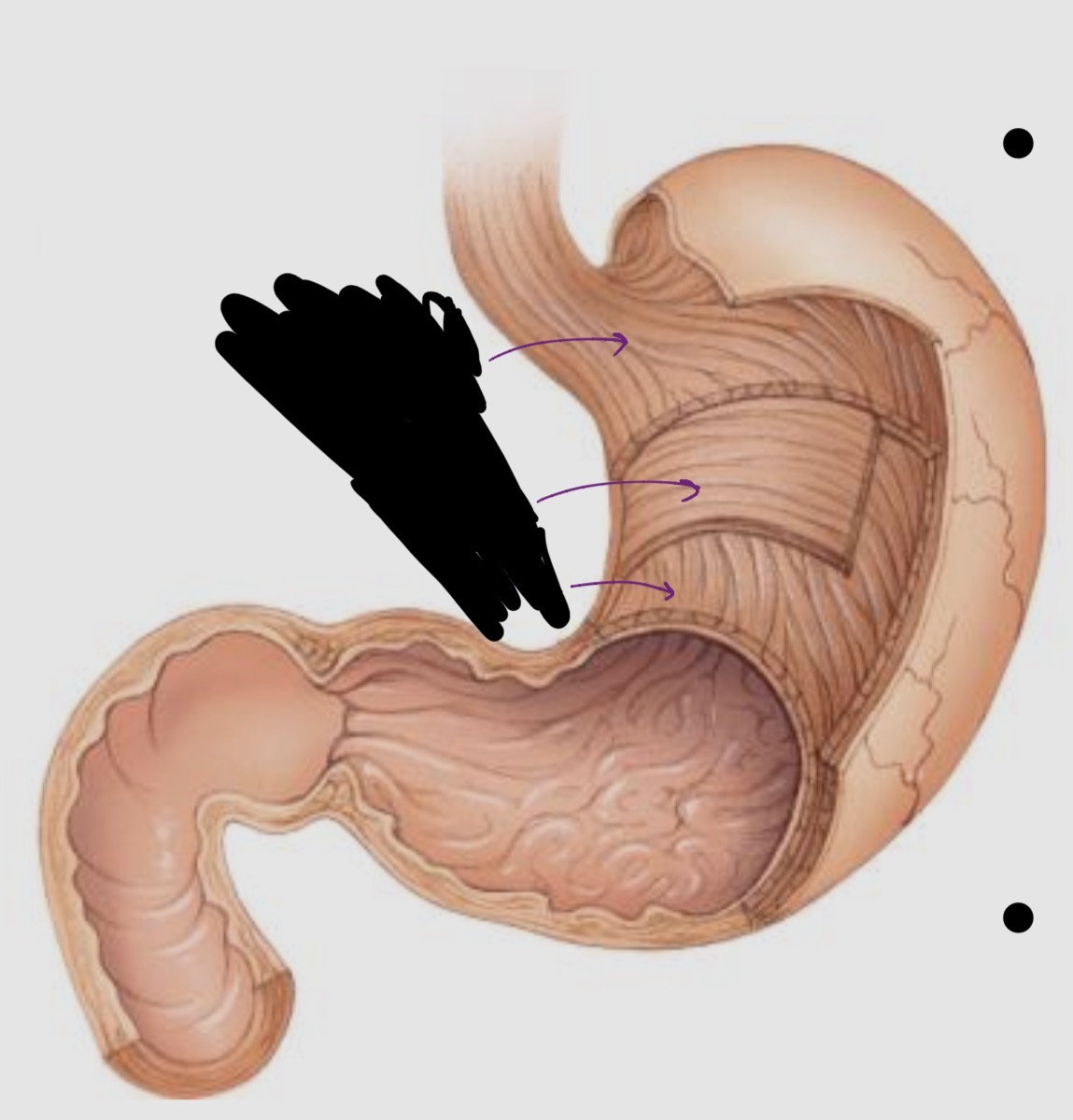
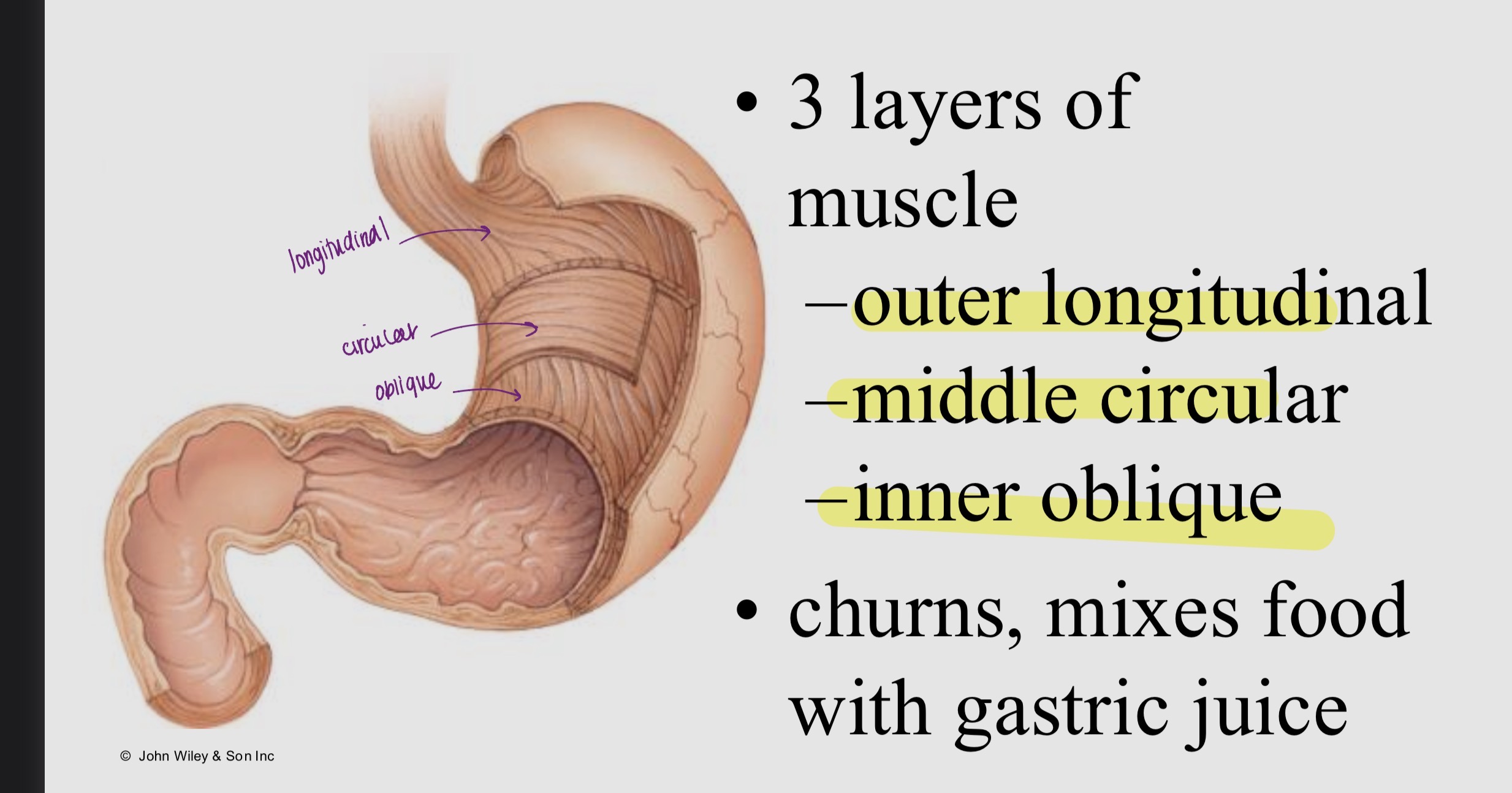
Label the muscularis and its function
Gastric secretions
Mucus:
Protects underlying tissue
Pepsinogen:
Inactive protease (enzyme)
Hydrochloric acid (HCl):
Activates pepsinogen → (converts to) pepsin
Together = gastric juice
Gastric Physiology - Mechanical Digestion Process
Bolus enters stomach
Gentle mixing waves every 15–25 seconds
Bolus + gastric juice → chyme (watery, acidic)
More vigorous waves in body
Intensify near pyloric part
Few waves in fundus
Each contraction:
Pushes 1–2 mL chyme to duodenum