Lecture 23: Endocrine system
1/29
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
30 Terms
Anterior pituitary: FSH
Stimulates the growth and development of follicles in ovaries and thus the oogenesis (female gamete production)
Stimulates secretion of estrogens (female sex hormone) and stimulates spermatogenesis in males
Not making spermm/oocytes
Anterior pituitary: LH
Completes process of follicle development in ovary that was started by FSH
Once ovulation has occurred, high LH level stimulates cell left behind in the empty follicle to multiply and develop into another endocrine structure → corpus luteum
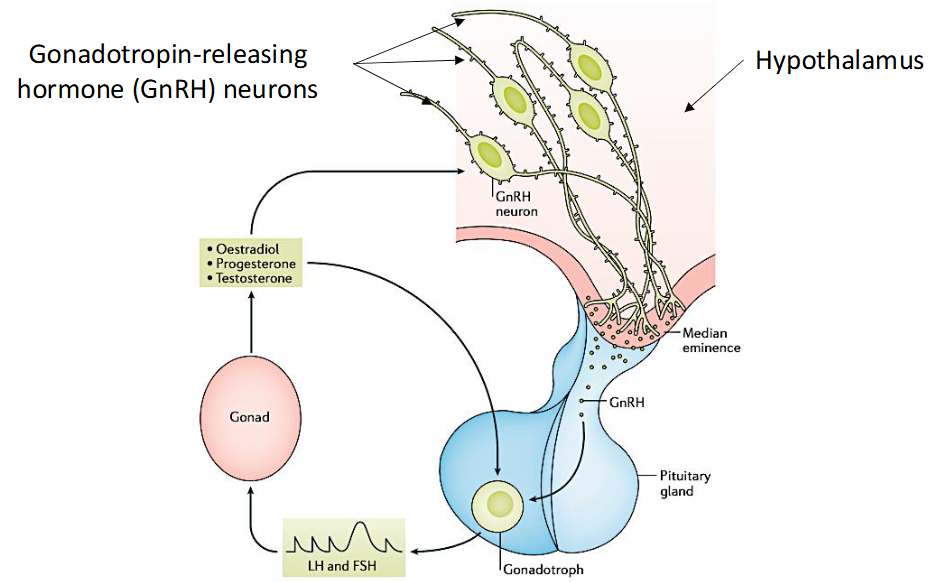
FSH and LH production → Hypothalamic pituitary gonadal axis
GnRH release in hypothalamus
Causes LH and FSH to be released from anterior pituitary gland
Targets testis and ovaries
Starts producing estrogen, progesterone and testosterone
New hormones produced affects gonadotrophs making LH and FSH higher
FSH in males
Stimulate sertoil cells
Increases spermatogenesis
LH in male
Stimulate Interstitial cells → Leydig cells
Increase release of testosterone
FSH in females
Stimulates Ovary
Increases folliculogenesis
Increases production of estrogen
LH in females
Stimulates ovary
Signals corpus luteum cells
Increases progesterone
Progesterone high to maintain pregnancy
Posterior pituitary
Does not produce any hormones
Stores two hormones produced by hypothalamus
Releases it periodically
Antidiuretic hormone
Oxytocin
Posterior pituitary glands and release of hormones
Hypothalamus sends nerve impulses to nerve endings of posterior pituitary
Releases Oxytocin or ADH into bloodstream
Anterior pituitary → hormones release from hypothalamus through portal vein
ADH
Help body conserve water when short supply in kidney
Causes kidney to reabsorb more water from urine
Goes back into blood stream
Oxytocin in Uterus
Induces contraction by myometrium
Breeding
Help movement of spermatozoa up to oviducts
Parturition
Aid delivery and expulsion of placenta
Can be injected to induce birth
Oxytocin in mammary glands
Movement of milk down to lower parts of gland
Circulates down mammary gland
Causes cells around alveoli and small ducts to contract
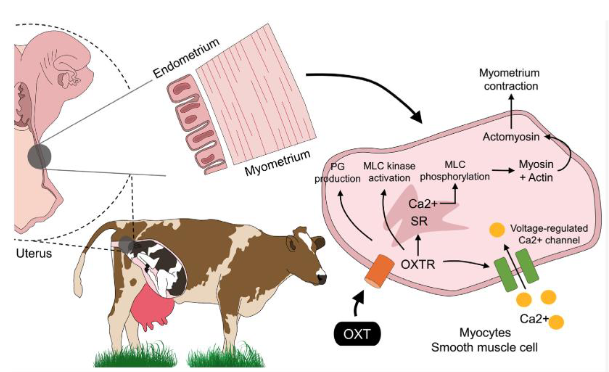
Oxytocin action on smooth muscle cells of myometrium
Endogenous and exogenous oxytocin promotes myometrium contraction
Activate receptor and its action on voltage regulated Ca2+ channels that facilitate Ca influx to cell
Oxytocin activate receptors and Ca receptors work
Prostaglandin (inflammatory mediators) produced
Actin and Myosin bind causing muscle contractions
Ca important to start contraction on smooth muscle
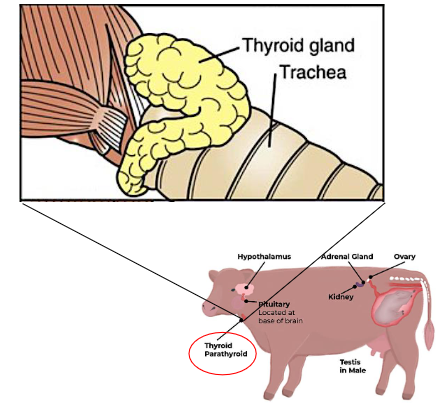
Major endocrine glands: Anterior pituitary → Thyroid gland
TSH from anterior pituitary → Affect thyroid gland
Two lobes on each side of larynx
Two different cells
Thyroid follicular epithelium
Medullary (C) cells
Thyroid gland: Medullary (C) cells
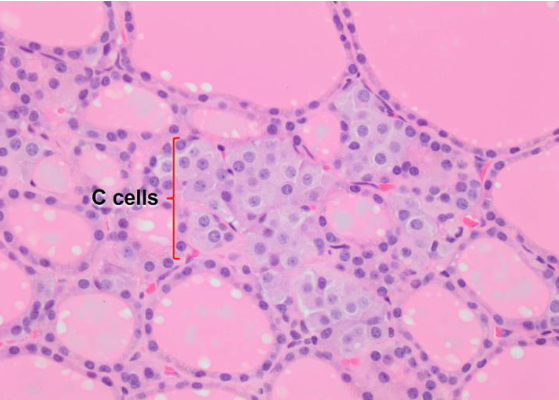
Thyroid gland: Epithelial cells
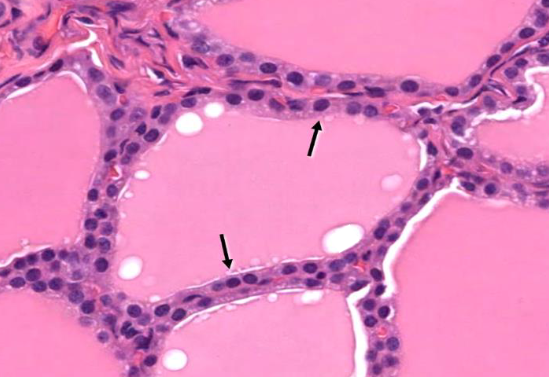
Thyroid gland producing Thyroid hormones
Anterior pituitary gland releases TSH
TSH activates Thyroid glands
Thyroid glands release T3 and T4
T4
Converted to T3 in peripheral tissues like liver, kidney, muscle when needed
Back up for T3
T3
Most biologically active form of thyroid hormone
T3 and T4: Calorigenic effects
Regulate metabolic rate of cells
Help generate heat and maintain body temperature
T3 and T4: Protein, Carbohydrate and Lipid metabolism
It may induce protein anabolism or catabolism
Depend on energy availability in diet
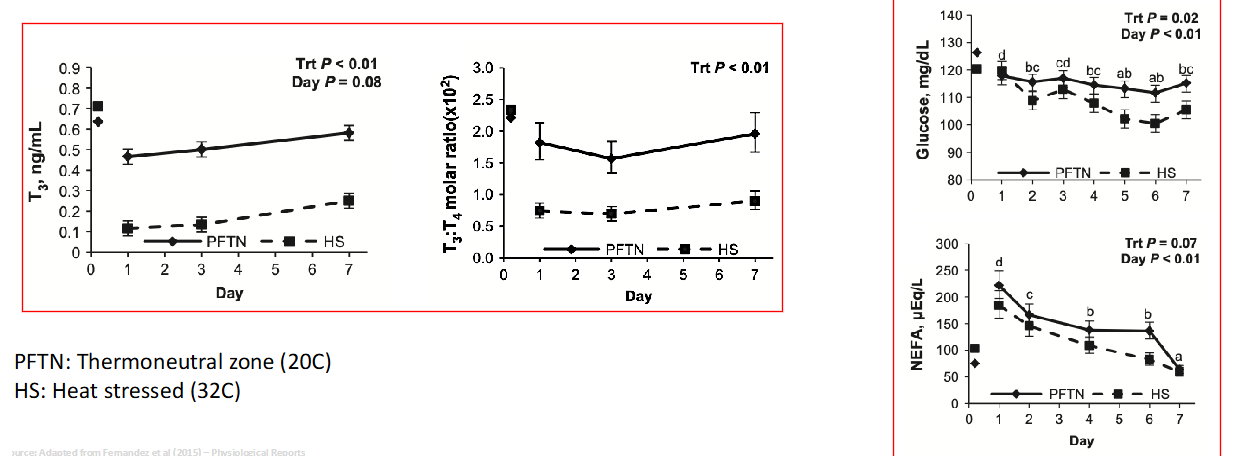
T3 and T4 levels with heat stress and glucose
Heat stress lower if T3 and T4 levels were normal
Lower glucose won’t make lots of protein
Not enough heat tolerance because low on glucose
Body now needs to break down muscles to make glucose
Lose lots of weight, negative economic effect
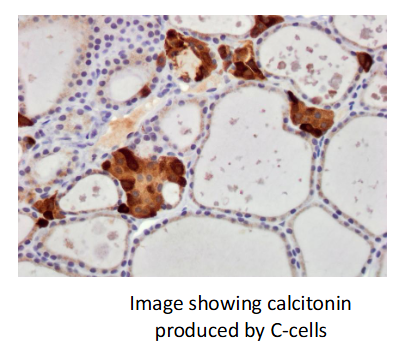
Thyroid gland: Calcitonin
Produced by C cells
Located between thyroid follicles
One of two hormones involved in maintaining homeostasis of blood Ca levels (other is parathyroid)
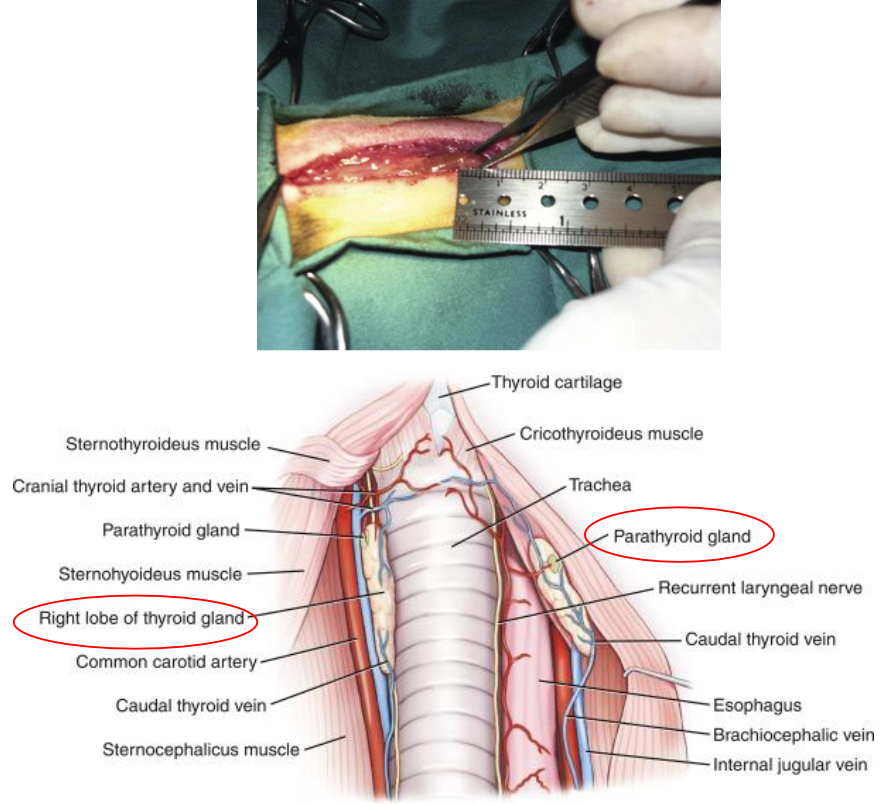
Thyroid gland: Parathyroid gland
Small pale nodules in/on/near thyroid glands
Produce parathyroid hormone (Parathormone)
Help maintain blood Ca homeostasis
Opposite effect of calcitonin
PTH homeostasis
Secreted by parathyroid gland
Increases renal Ca reabsorption (kidney)
Produces 1,25(OH)2D3 → Active form of vitamin D
Stimulates Ca absorption by intestinal epithelial
Positive feedback
Calcitonin homeostasis
Secreted by thyroid glands
Lower blood calcium if too high
Inhibit reabsorption of bone Ca
Increases urinary Ca loss
Aims to lower blood concentrations of Ca
Negative feedback
Calcium homeostasis in dairy cows
Parturient paresis (milk fever)
Common disease after calving in dairy cattle
Caused by high demand for Ca when lactating period begins
Result from inability to regulate calcemia
Use lots of Ca for uterus muscles
Lactation also uses lots of Ca for fetus
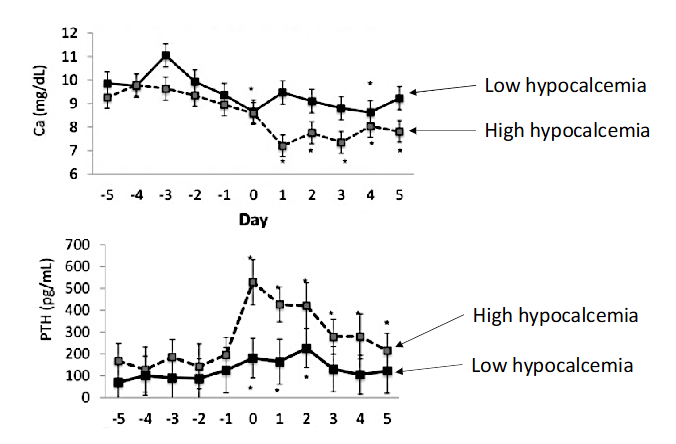
Calcium homeostasis in dairy cows
During milking
Have hypocaclemia
When Ca in blood is lower, calcitonin is lower
Doesn’t want to get rid of calcium
Low hypocalcemia
More PTH
Less Calcitonin
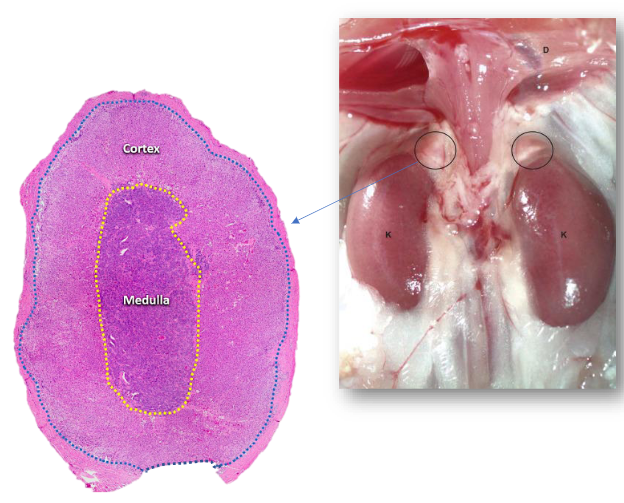
Adrenal glands
Named for their proximity to kidneys
Appears to be single structured, they are two glands
Outer adrenal cortex and inner adrenal medulla
Different structures and functions
Adrenal cortex
Stimulated and controlled by ACTH
Hormone produced by anterior pituitary
Produces three main groups of hormone
Glucocorticoid hormone
Mineralocorticoid hormones
Sex hormones (small amounts)
Adrenal cortex: Glucocorticoid hormones
Cortisol
Cortisone
Corticosterone
Increases blood glucose levels → Hyperglycemic effect
Glucose produced so you don’t faint when stressed
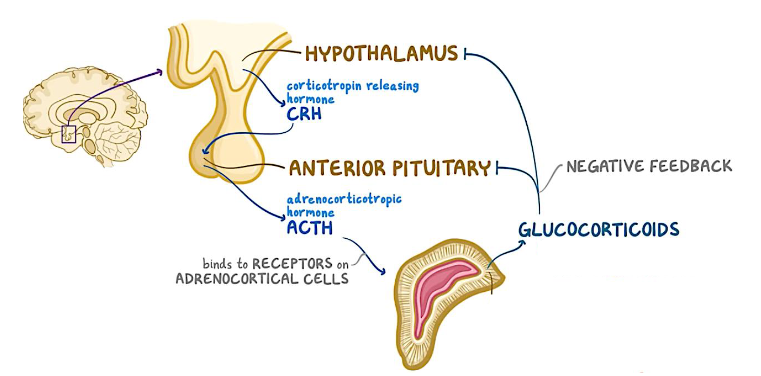
Adrenal cortex: Glucocorticoid hormones
Hypothalamus release CRH
Signals anterior pituitary to release ACTH
ACTH stimulates adrenal cortex
Releases glucocorticoids
Negative feedback
Cortisol inhibits hypothalamus and pituitary
Once cortisol is produced, it inhibits glands from releasing hormones