Urinary System
1/23
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
24 Terms
Organs of the Urinary System
Kidneys - remove substances from the blood (filters blood)
ureters - transport urine from kidneys to bladder (muscular tubes)
urinary bladder - urine storage
urethra - conveys urine outside
Function of the Urinary SYstem
regulate aspects of homeostasis
water balance and electrolytes
acid-base balance in the blood
blood pressure (with the enzyme renin)
red blood cell production (with the hormone erythropoietin)
activation of vitamin D
Elimination of waste products
nitrogenous wastes, toxins, drugs
if urine has…
glucose→ diabetes
blood→ damaged tissue
proteins→ damaged kidneys
Location of the Kidneys
Against the dorsal body wall
In retroperitoneal cavity
at the level of T12 to L3 (spine)
The right kidney is slightly lower because of the liver
Lateral side is convex, medial is concave, kidneys sit in a depression called renal sinus (indentation)
Attached to the ureters, renal blood vessels, and nerves enter at renal hilus (opening w/ blood vessels)
Atop each kidney is an adrenal gland (produces cortisol)
Urinary Bladder
smooth, collapsible, muscular sac
temporarily stores urine
Holds 1L of urine
bladder can stretch
Trigone—three openings
two from the ureters
one to the urethra
Urinary Bladder wall
Three layers of smooth muscle (called detrusor muscle)
Walls are thick and folded in an empty bladder (2-3 inches)
Bladder can expand significantly without increasing internal pressure (more than 5 inches and more than 1L of urine)
Urethra
thin-walled tube that carries urine from the bladder to the outside of the body by peristalsis
Release of urine is controlled by two sphincters
internal urethral sphincter (involuntary)
external urethral sphincter (voluntary)
Urethra Gender Differences
Length
females - 3-4cm (1 inch)
males - 20cm (8 inches)
Location
females - along wall of the vagina
Males - through the prostate and penis
Function
females - only carries urine
Males - carries urine and is a passageway for sperm cells
UTI (Urinary Tract Infections)
An infection in any part of the urinary system, the kidneys, bladder, or urethra
Urinary tract infections are more common in women. They usually occur in the bladder or urethra, but more serious infections involve the kidney
A bladder infection may cause pelvic pain, increased urge to urinate, pain with urination, and blood in the urine. A kidney infection may cause back pain, nausea, vomiting, and fever
Women are at greater risk of developing a UTI than men are
Common treatment is with antibiotics
Regions of the kidney
Renal cortex—outer region
contains many cells that produce urine
Renal medulla—inside the cortex
Renal pelvis—inner collecting tube
collects urine produced by pyramids
Renal capsule—protects kidney
Medullary pyramids—triangular regions of tissue in the medulla
Renal columns—extensions of cortex-like material inward
Calyces—cup-shaped structures that funnel urine towards the renal pelvis
Nephrons
The structural and functional units of the kidneys
Responsible for forming urine
Each kidney has over 1 million nephrons
Main structures of the nephrons
Glomerulus
Renal tubule
made of 3 parts
Renal Tubule
About 3cm long
Proximal convoluted tubule (PCT)
Loop of Henle
Distal convoluted tubule (DCT)
Urine Formation Processes
glomerular filtration
tubular reabsorption
tubular secretion
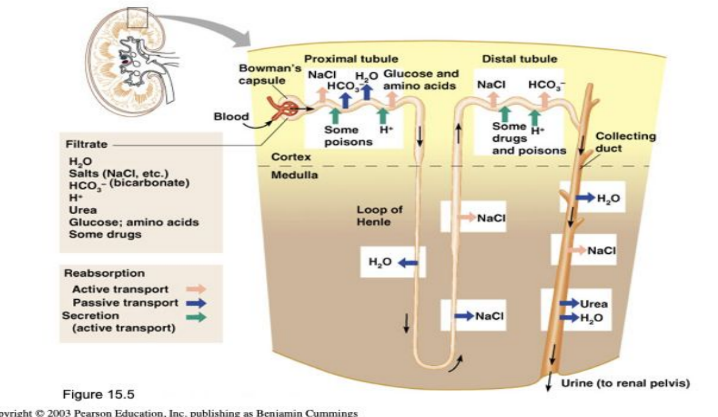
Filtration
nonselective passive transport
filtrate is collected in the glomerular capsule and leaves via the renal tubule
The glomerulus is the site of blood filtration where it filters water and other substances from the bloodstream into the Bowman’s capsule. As blood flows through the glomerulus, blood pressure pushes water and solutes from the capillaries into the capsule through a filtration membrane.
The filtration membrane keeps blood cells and large proteins in the bloodstream
Blood cells cannot pass out to the capillaries
blood should not be in urine
Reabsorption
The peritubular capillaries reabsorb several materials by moving nutrients and water back into the blood stream
Some water
glucose
amino acids
ions
Some reabsorption is passive, most is active
Most reabsorption occurs in the proximal convoluted tubule (PCT)
Materials that are not reabsorbed
nitrogenous waste products (this is what should be in your urine)
urea
uric acid
creatinine
Chemicals created through the breakdown of proteins
Excess water
Secretion — Reabsorption in reverse
Some materials move from the peritubular capillaries into the renal tubules
hydrogen and potassium ions
Creatinine
Drugs
Materials left in the renal tubule move toward the ureter
Waste ions and hydrogen ions are secreted from the blood to complete the formation of urine
Secretion primarily happens in the proximal convoluted tubule but also in smaller amounts in the DCT or distal convoluted tubule and collecting duct.
The secreted ions combine with the remaining filtrate and become urine.
The urine flows out of the nephron tubule into a collecting duct
It passes out of the kidney through the renal pelvis, into the ureter, and down to the bladder.
Characteristics of urine used for Medical Diagnosis
colored somewhat yellow due to the pigment of urochrome (from the destruction of hemoglobin—RBCs) and solutes
When RBCs die, they release a substance called bilirubin, which is then converted into uroschrome by gut bacteria to give its yellow color
sterile (no bacteria)
slightly aromatic
if you have diabetes, urine will smell fruity
Normal pH of around 6 (varies 4.5-8)
Specific density of 1.001 to 1.035 since 95% of urine is water
The typical urine volume for an adult is between 750-2000 mL a day
Solutes normally found in urine
sodium and potassium ions
chloride ions
small amounts of other ions, hormones, metabolites, and pigments
urea (waste product from liver breaking down proteins)
uric acid
creatinine
Solutes NOT normally found in urine
glucose (diabetes)
Blood proteins (pregnancy, HBP)
Red blood cells (bleeding—trauma, kidney stones)
Hemoglobin (anemia)
White blood cells (pus) (UTI)
Bile (liver disease, hepatitis)
Pregnancy Tests
urine may also contain other chemicals that can be detected that are produced by the placenta
hormones present in a pregnant woman are detectable in urine
Micturition (voiding)
The act of emptying the bladder
The detrusor muscle in the bladder wall contracts, causing the internal urethral sphincter to relax and allow urine to flow out.
Activation is from an impulse sent to the spinal cord and then back via the pelvic splanchnic nerves
The external urethral sphincter controlled by the pudendal nerve is the muscle that voluntarily controls the flow of urine by relaxing to allow urination.
Both sphincter muscles must open to allow voiding
Maintaining water balance
normal amount of water in the human body
Young adult females—50%
Young adult males—60%
Babies—75%
Old Age—45%
Water is necessary for many body functions and levels must be maintained
Water intake must equal water output
Sources for water intake
ingested foods and fluids
water produced from metabolic processes
Sources for water output
Vaporization out of the lungs
lost in perspiration
leaves the body in the feces
urine production
Coffee dehydrates or gets rid of water (diuretic)
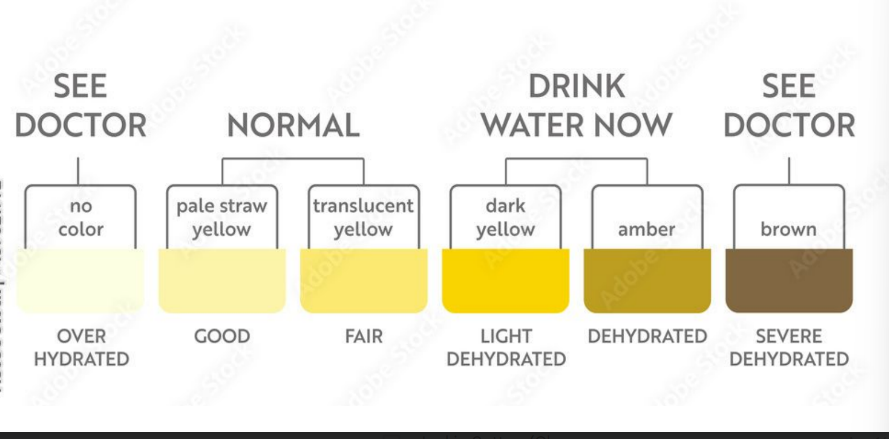
Dilute urine is produced if water intake is excessive
Less urine (concentrated/darker) is produced if large amounts of water are lost
Proper concentrations of various electrolytes must be present
Developmental Aspects of the Urinary System
Control of the voluntary urethral sphincter does not start until age 18 month (around 2 years old)
longer for males
Urinary infections are the only common problems before old age
Aging and the Urinary system
There is a progressive decline in urinary function
The bladder shrinks with aging
Urinary retention is common in males
frequent urinations even during the night.
Main function of urinary system
The main functions of the urinary system are to filter waste products from the blood, produce urine, remove excess water and salts from the body, maintain electrolyte balance, regulate blood pressure, and contribute to the body's overall fluid balance by excreting waste products like urea through urine.
Retroperitoneally meaning
"Retroperitoneally" means "behind the peritoneum," referring to a position in the abdomen located posterior to the peritoneal cavity, the lining of the abdominal cavity; essentially, situated behind the abdominal lining.
Hormone that regulates formation of urine
The hormone that regulates the formation of urine is Antidiuretic Hormone (ADH), also known as vasopressin
it is produced in the hypothalamus and released by the posterior pituitary gland.
ADH primarily controls the amount of water reabsorbed by the kidneys, thus regulating the concentration and volume of urine produced.
When ADH levels are high, more water is reabsorbed, leading to less urine production, and vice versa.