Male Reproductive System
1/33
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
34 Terms
what does male reproductive system do?
responsible for producing sperm cells and hormones
sperm cell is important to fertilize an egg cell
hormones are responsible for the development of adult male characteristics
male reproductive organs + urethra in the same place
bladder posterior to prostate gland
rectum is posterior to bladder
external parts & functions of male repro system
penis
external male organ
glans: tip
covered with foreskin that may be removed through circumcision
not removed = excess tissue around penis; not harmful but requires cleaning
acts as conduit for urine to leave body
scrotum
pair of pouch-like sacs that supports the testes
controls temperature
testes must be slightly cooler than the body to produce sperm cells
scrotum and testes are external to maintain a certain temperature for sperm
testes pulled closer = to warm up
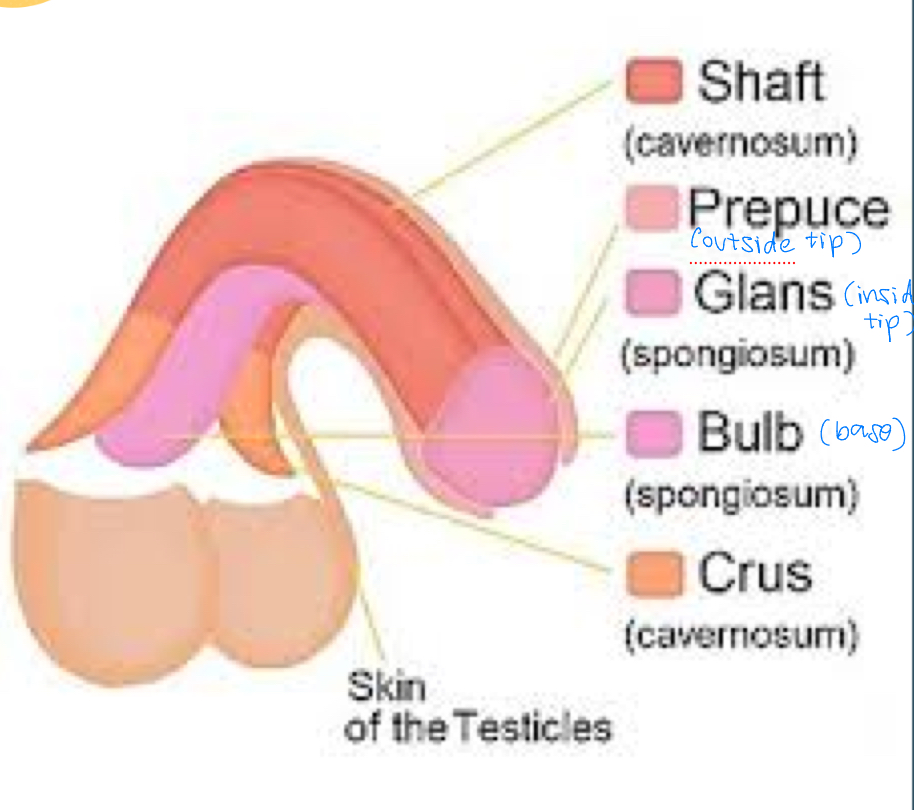
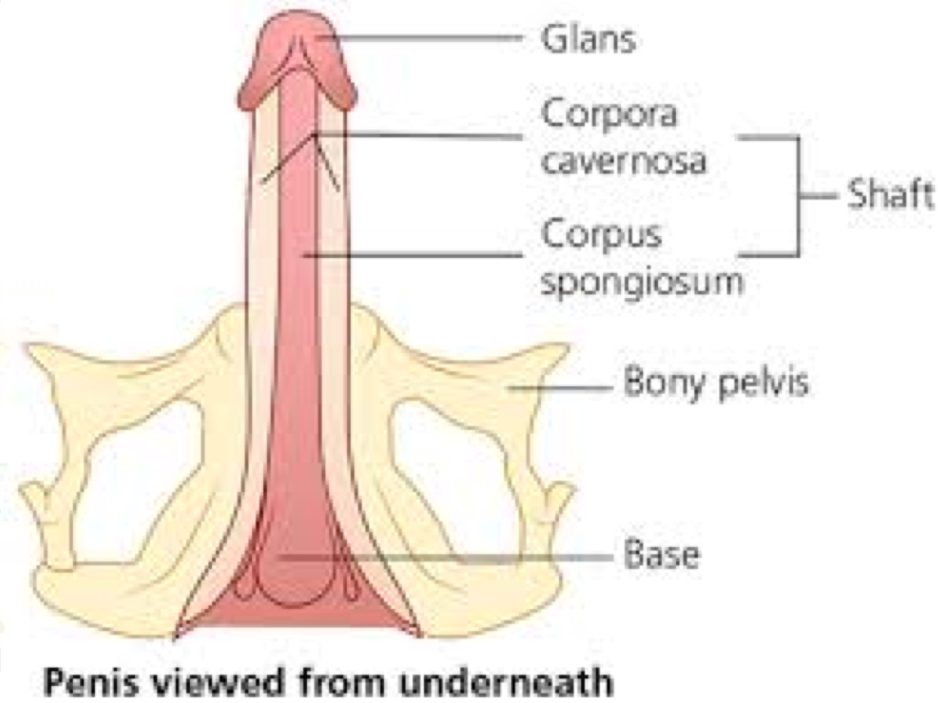
penis anatomy
shaft = corpus cavernosum, corpus spongiosum
prepuce = tip (external)
glans = tip; spongiosum (internal)
bulb = base; spongiosum
crus = toward the body
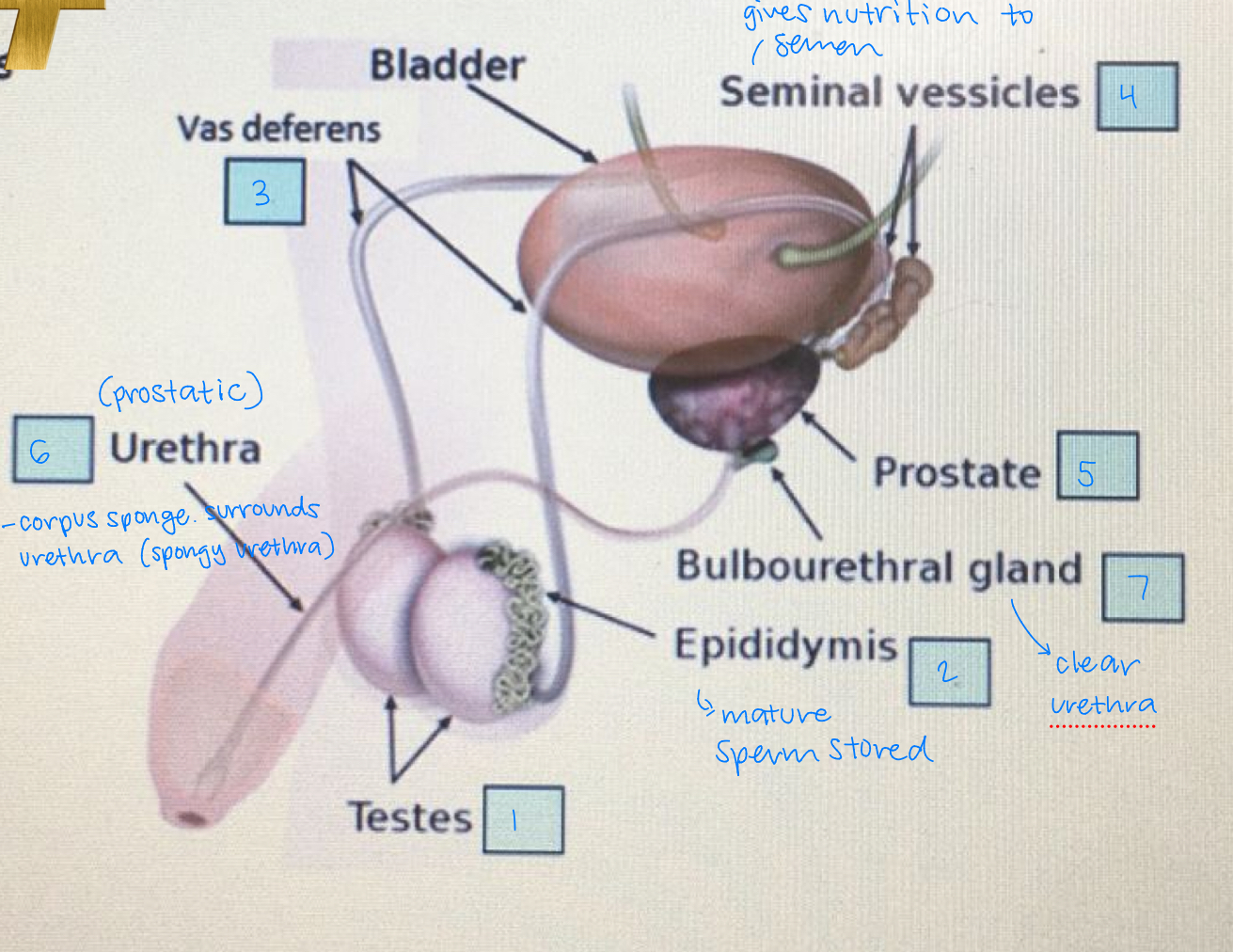
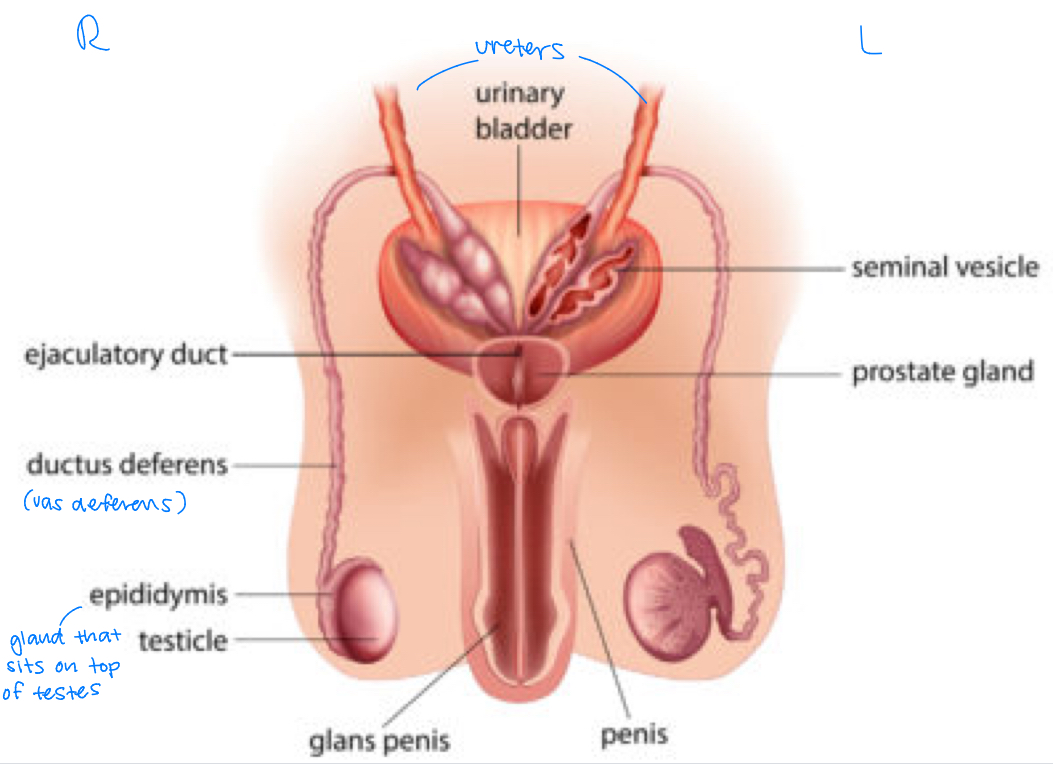
internal parts and functions of male repro system
anterior view
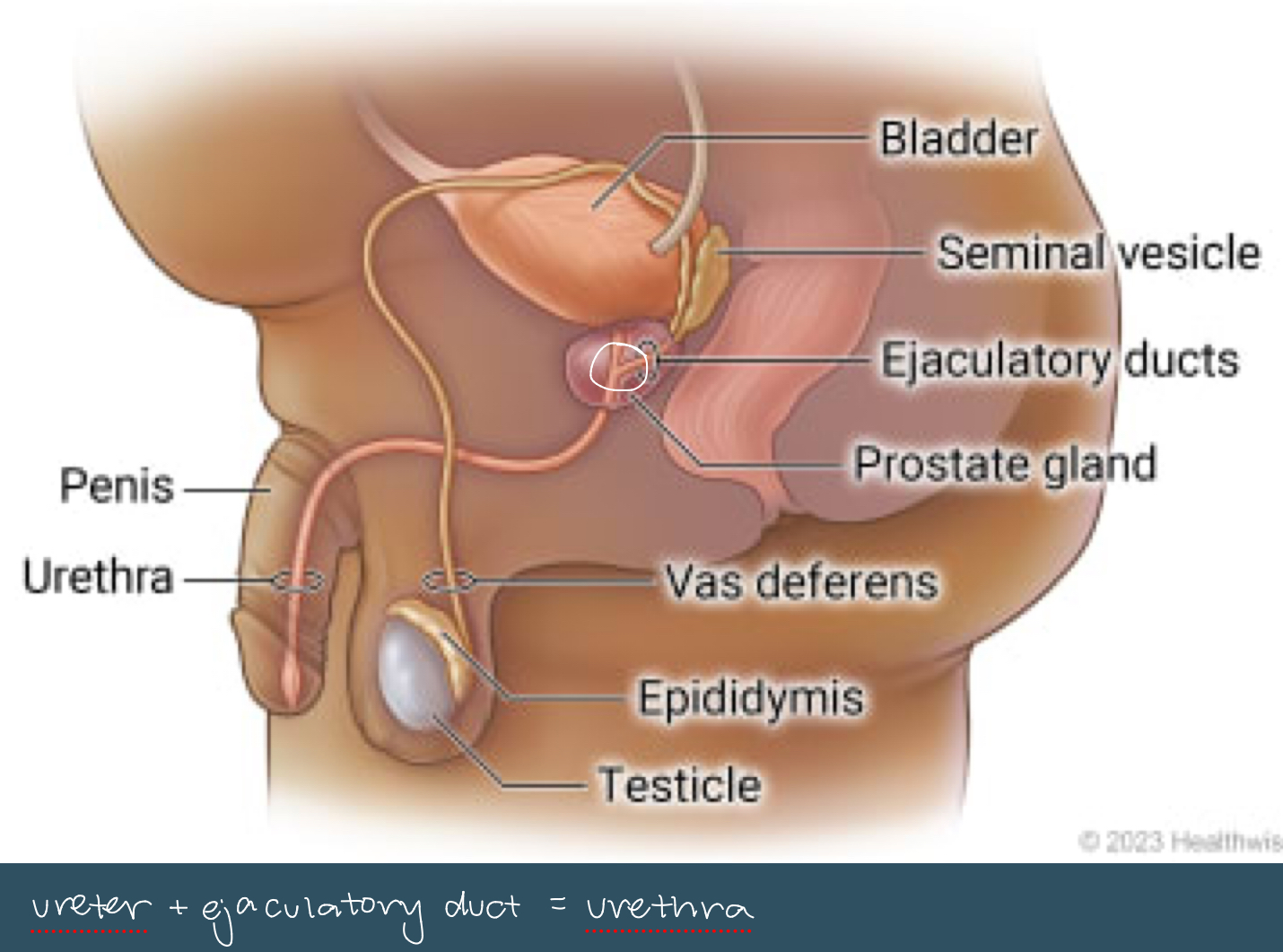
sagittal view
corpus cavernosa
spongey erectile tissue
smooth muscle
endothelial cell
“caverns” that fill with blood to create rigidity (stiffens) during an erection
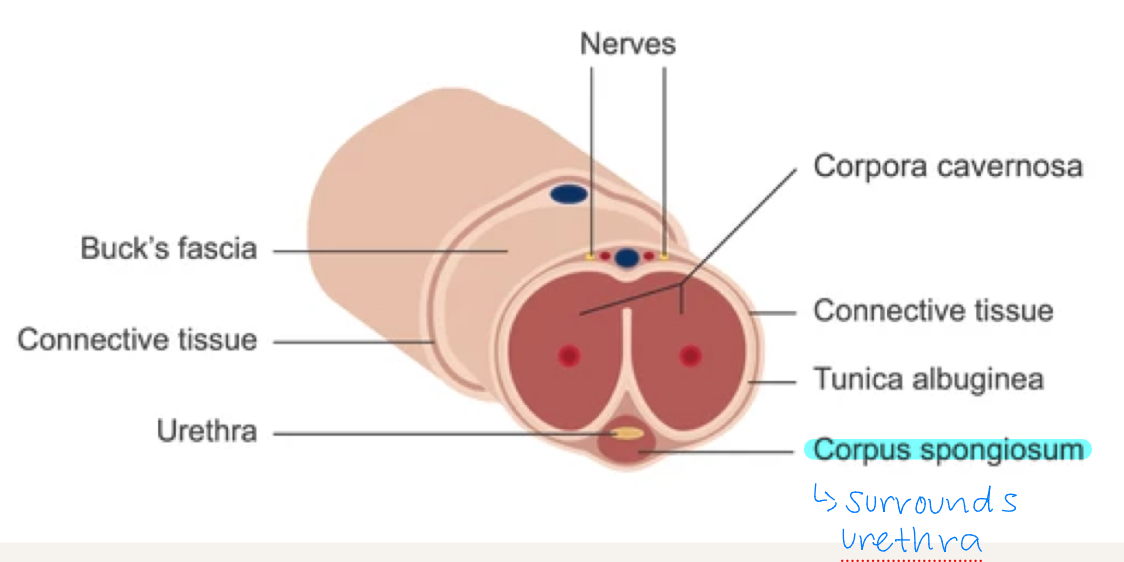
corpus spongiosum
anterior tube that surrounds the urethra and expands to form the glans
outer layer is thin and elastic which prevents urethra from being compressed and allows for passage of ejaculate
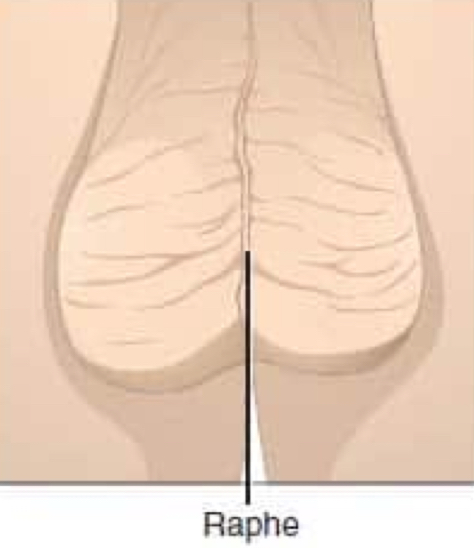
raphe
groove, ridge, or seam
divides the scrotum in half
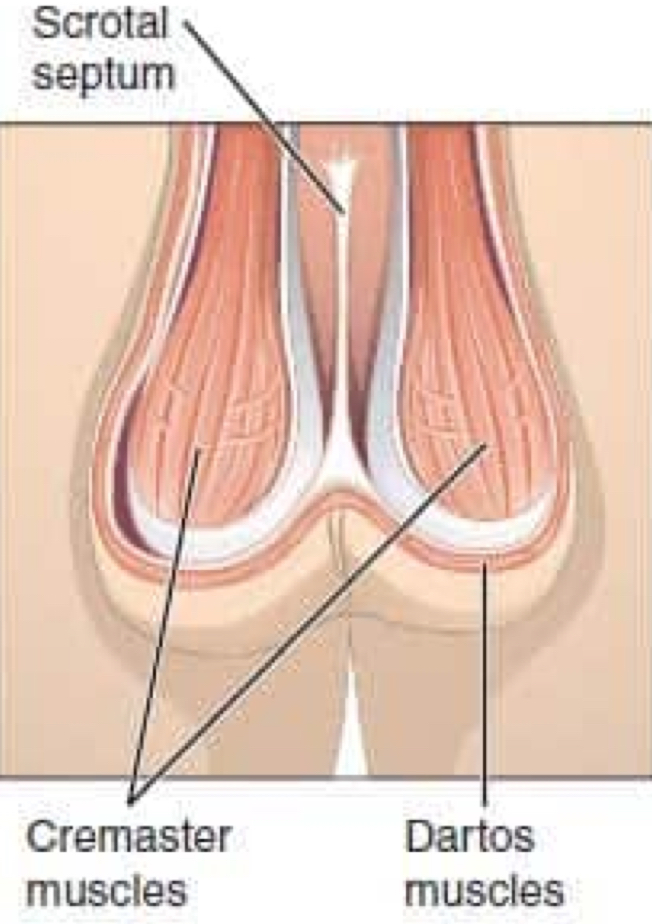
cremaster muscle
arises from the internal oblique muscle; vertical
contracts to lift the testes closer to body to conserve heat
surrounds the testicle and spermatic cords
job: elevate testicles for temperature regulation
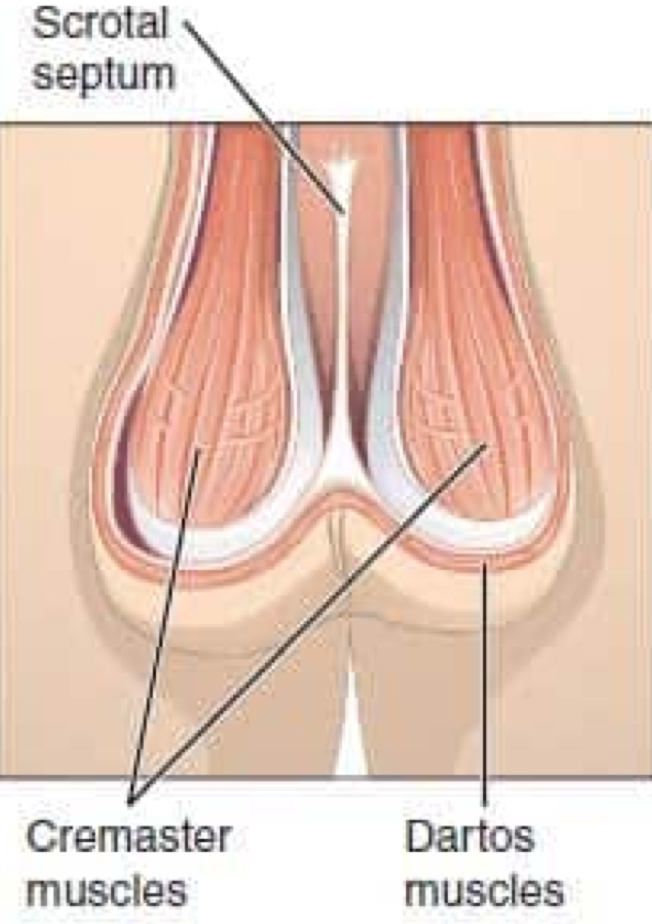
dartos muscle
contracts and causes wrinkling of the ipsilateral testicle to decrease its surface area and heat loss
needs elasticity to regulate temp
testicles
glands that produce sperm cells and male sex hormones called testosterone
testes protrude outside the body because the temperature inside the main body cavity is warmer and not suitable for the development of sperm cells
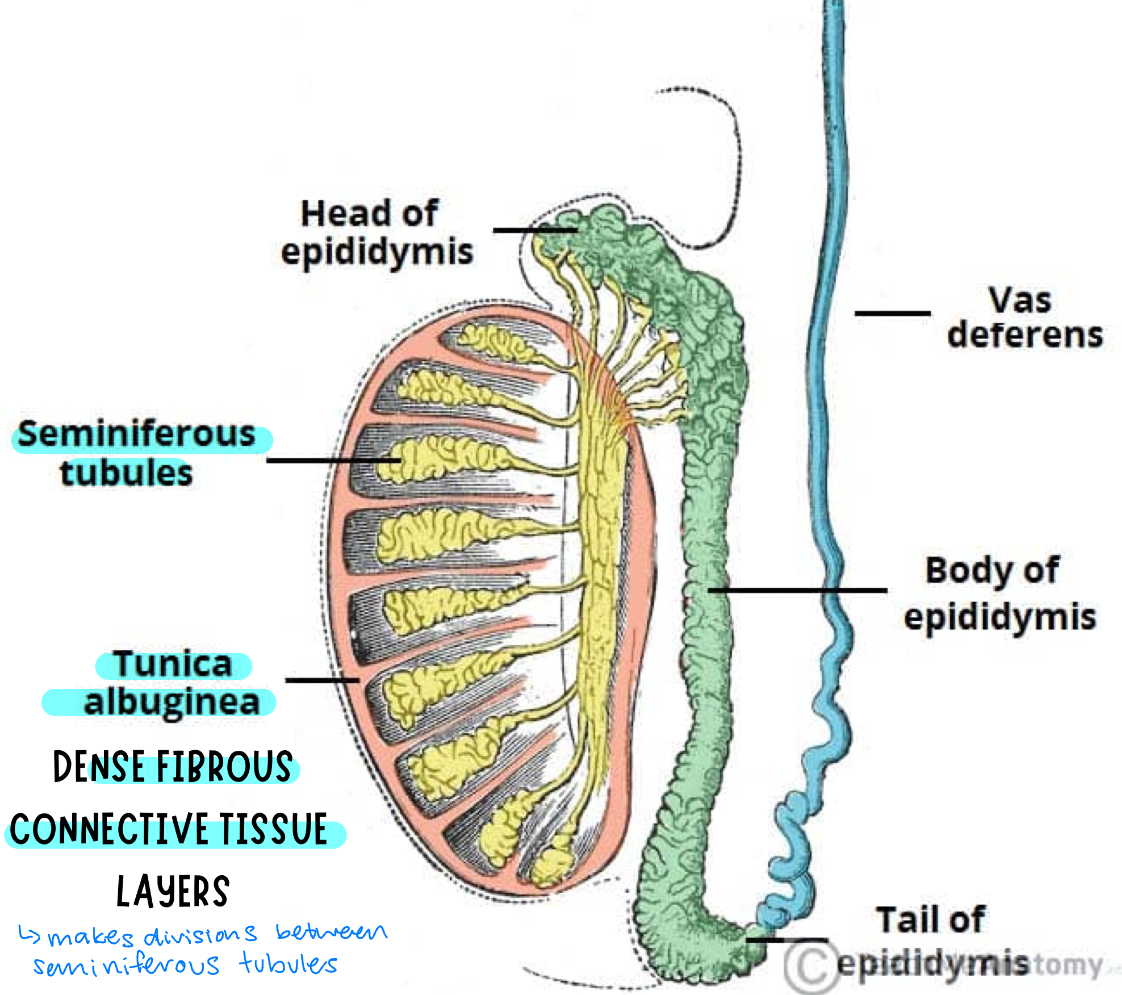
testes
leydig cells produce testosterone
seminiferous tubules: tightly coiled, microscopic tubes located within the testes responsible for producing, maintaining, and storing sperm, along with secreting testosterone
tunica albuginea: dense fibrous connective tissue layers that makes divisions between seminiferous tubules
spermatogenesis
sperm creation
takes place inside of seminiferous tubules
spermatogonium: potential sperm that could make mature sperm cells
meiosis
epididymis
narrow-coiled tube that stores immature sperm cells until they mature and temporarily stored before their release
sperm develops tails and get stronger
can store up to 30 days until ejaculated
sits on top of testes
epididymis structure
pseudostratified columnar epithelium
uncoiled = about 6 meters (19.65 ft)
produces a special fluid to maintain the maturing sperm
urethra
passageway of both urine from urinary bladder and semen from the glands
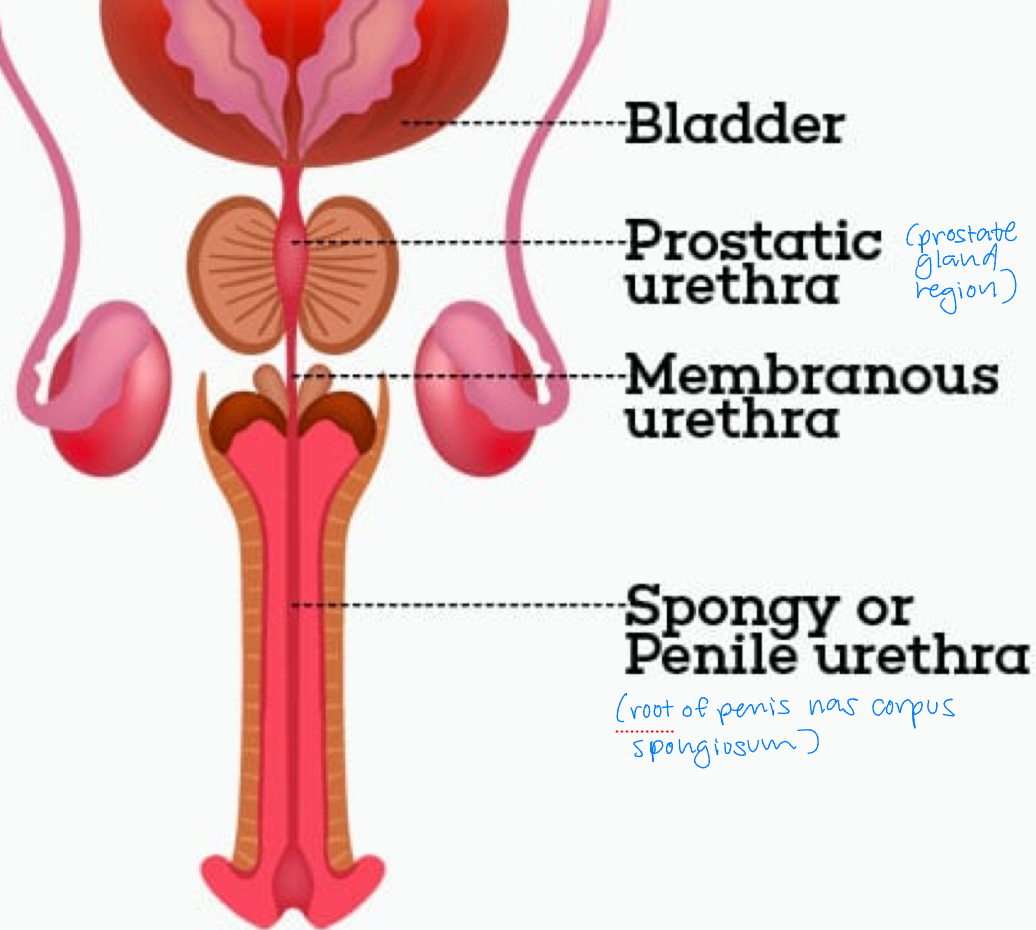
male urethra
divided into 3 sections
prostatic: prostate gland region
membranous: between prostate and root of penis
spongy/penile: root of penis; has corpus spongiosum
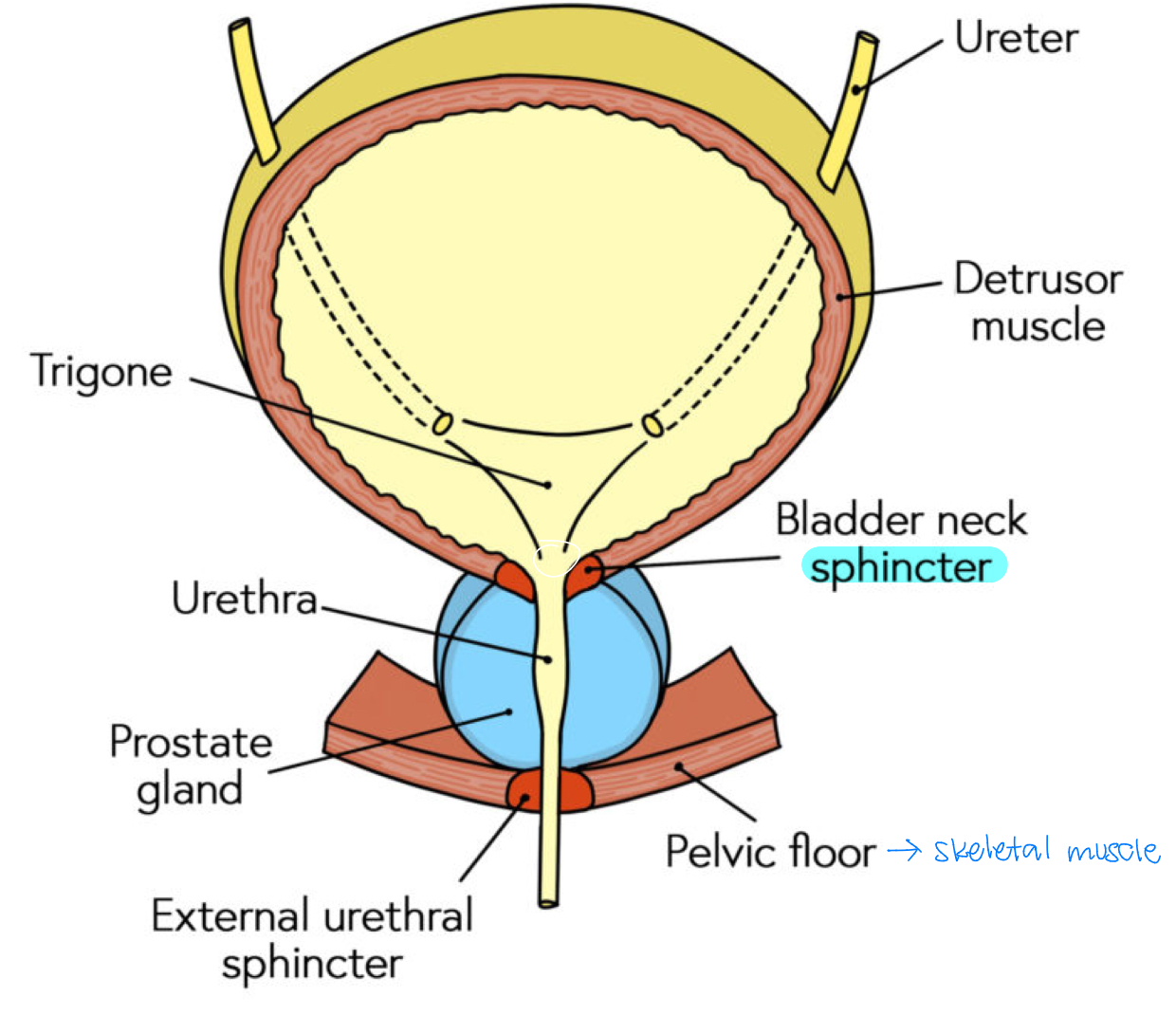
sphincters (internal and external)
internal sphincter: bladder neck
pelvic floor: skeletal muscle
external sphincter: urethra
reasons why a male could have urinary incontinence
urinary incontinence: involuntary loss of bladder control, ranging from occasional leaks to sudden, uncontrollable urges
sphincters can’t close completely due to weakening of pelvic floor muscle
prostate enlarges with age —> prostate presses on urethra
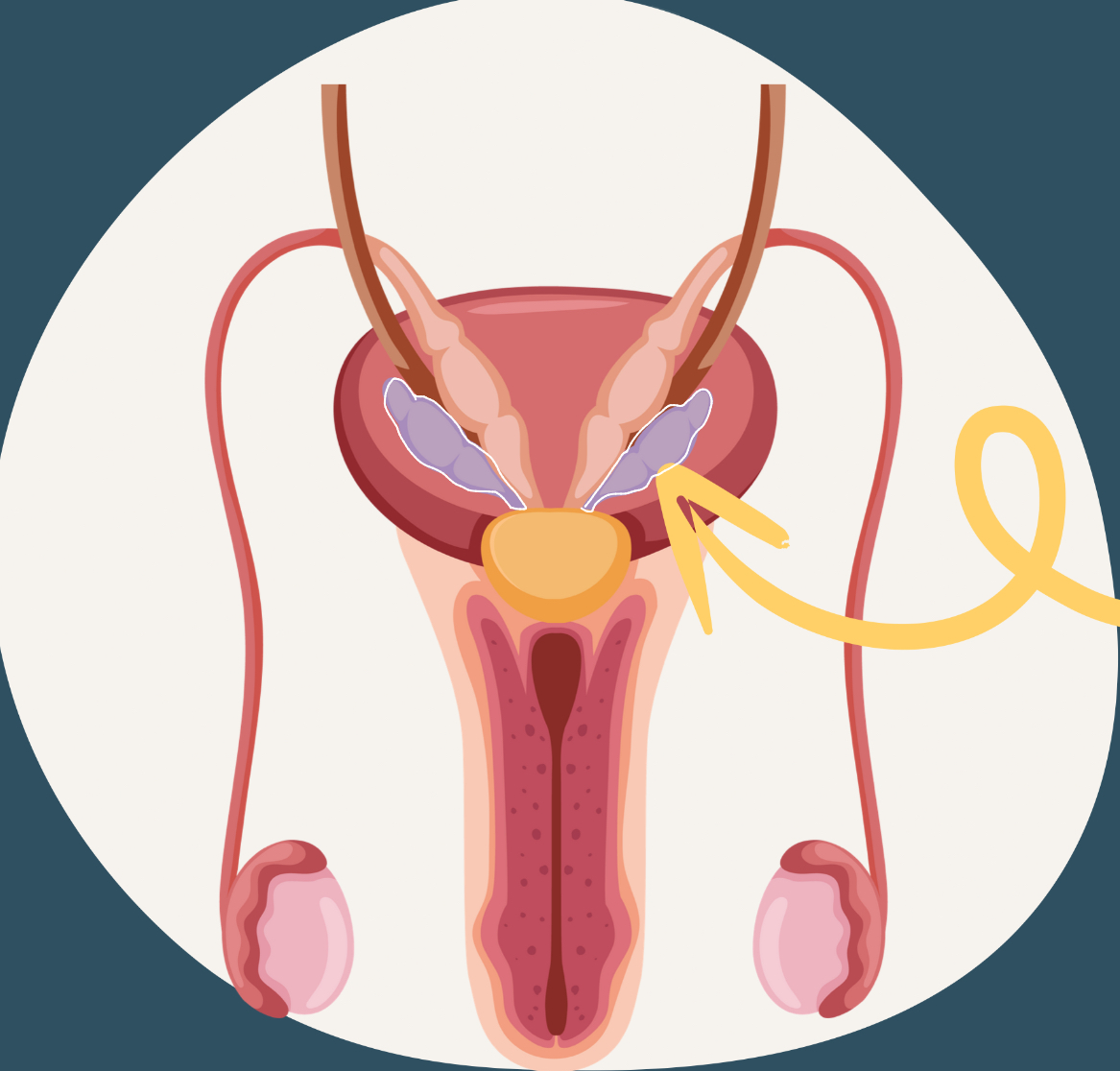
seminal vesicles
sac-like pouches attached to the vas/ductus deferens
produces a sugar-rich fluid that provides energy to sperm cells
sperm cell motility: swimming
sperm cells + sugar-rich fluid = semen
remains in females ~5 days
seminal vesicle (cont.)
can temporarily store sperm too
makes fluid that contains fructose, enzymes, and prostaglandins to keep sperm alive
contract during ejaculation and release fluid into ejaculatory duct
fluid makes up about 60% of semen
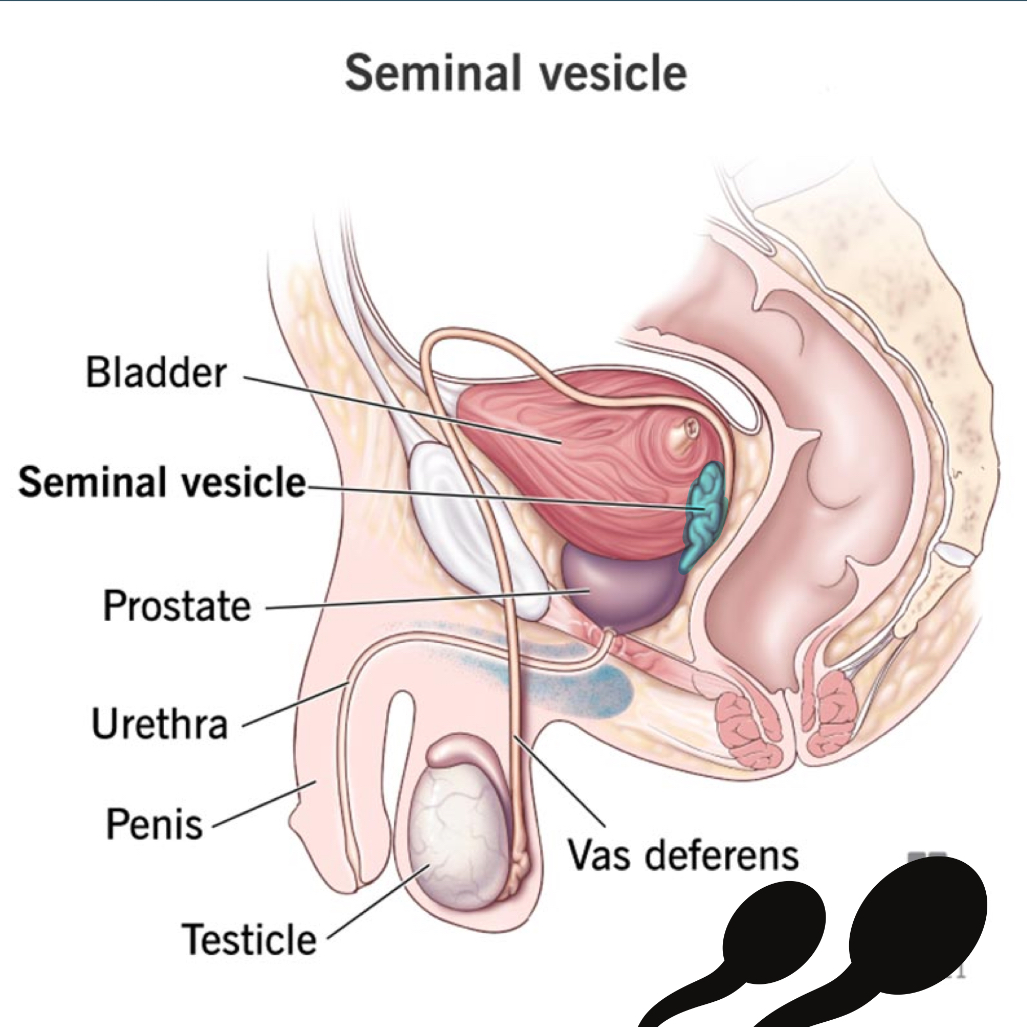
vas deferens
long, muscular tube that serves as passageway of the sperm cells released from the testes
connects testes to the seminal vesicle and urethra
smooth muscle
transports mature sperm to urethra for ejaculation
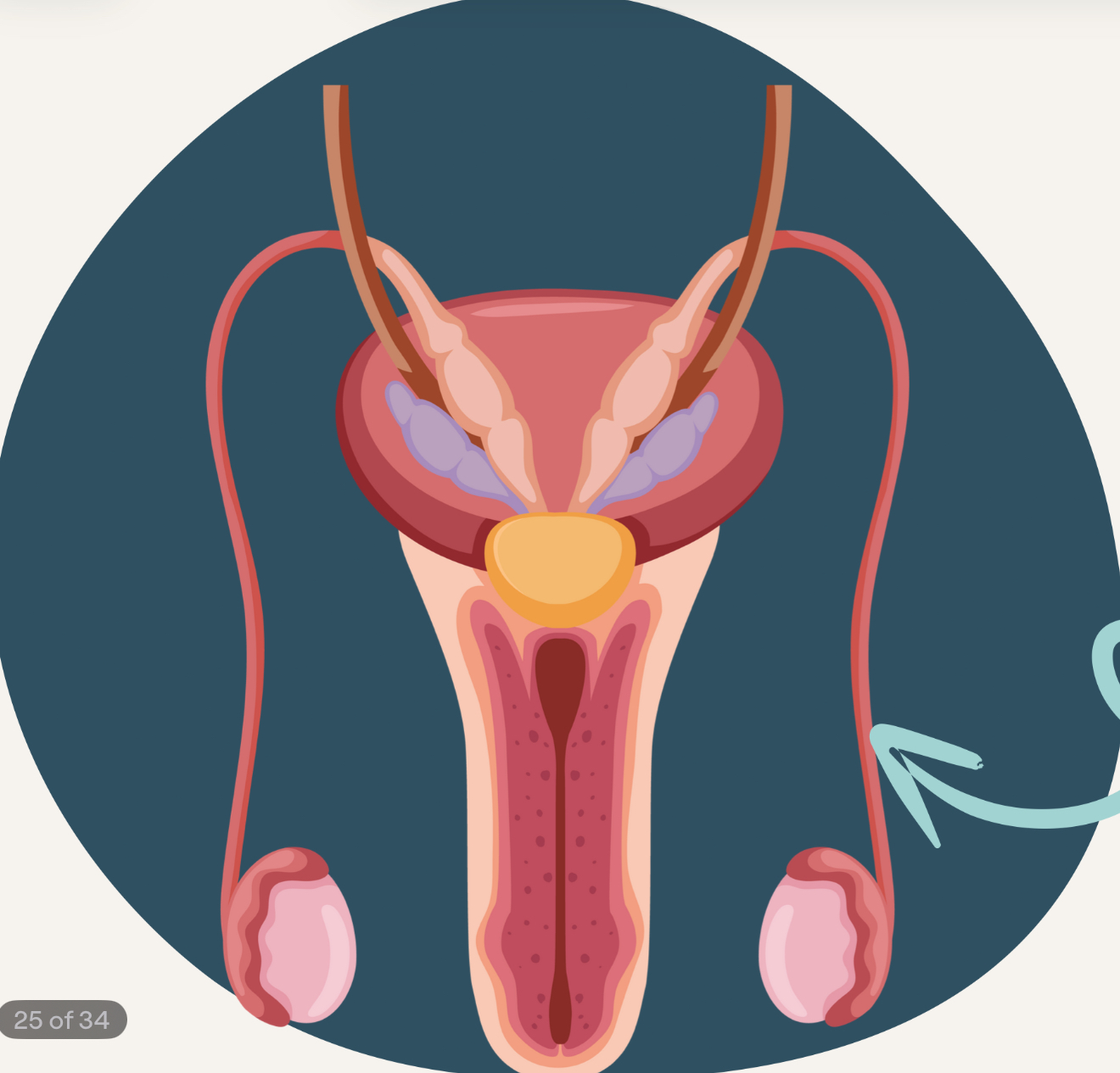
vasectomy
vas deferens are cut and sealed
mature sperm gets reabsorbed by the action of macrophages (WBCs)
the male needs 20-30 ejaculations until the sperm is cleared from the epididymis
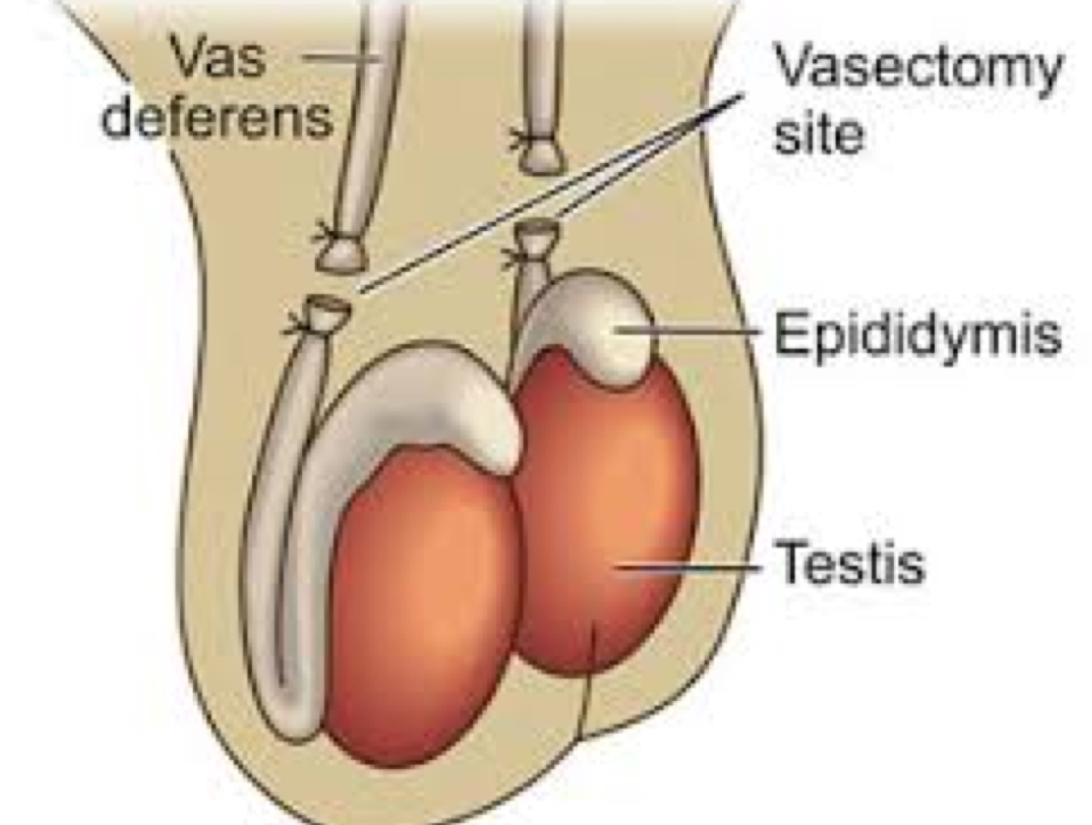
prostate gland
walnut-sized gland located between the bladder and the penis
secretes fluid that nourishes and protects the sperm
milky white color and is alkaline to help balance out the acidic environment of female vagina
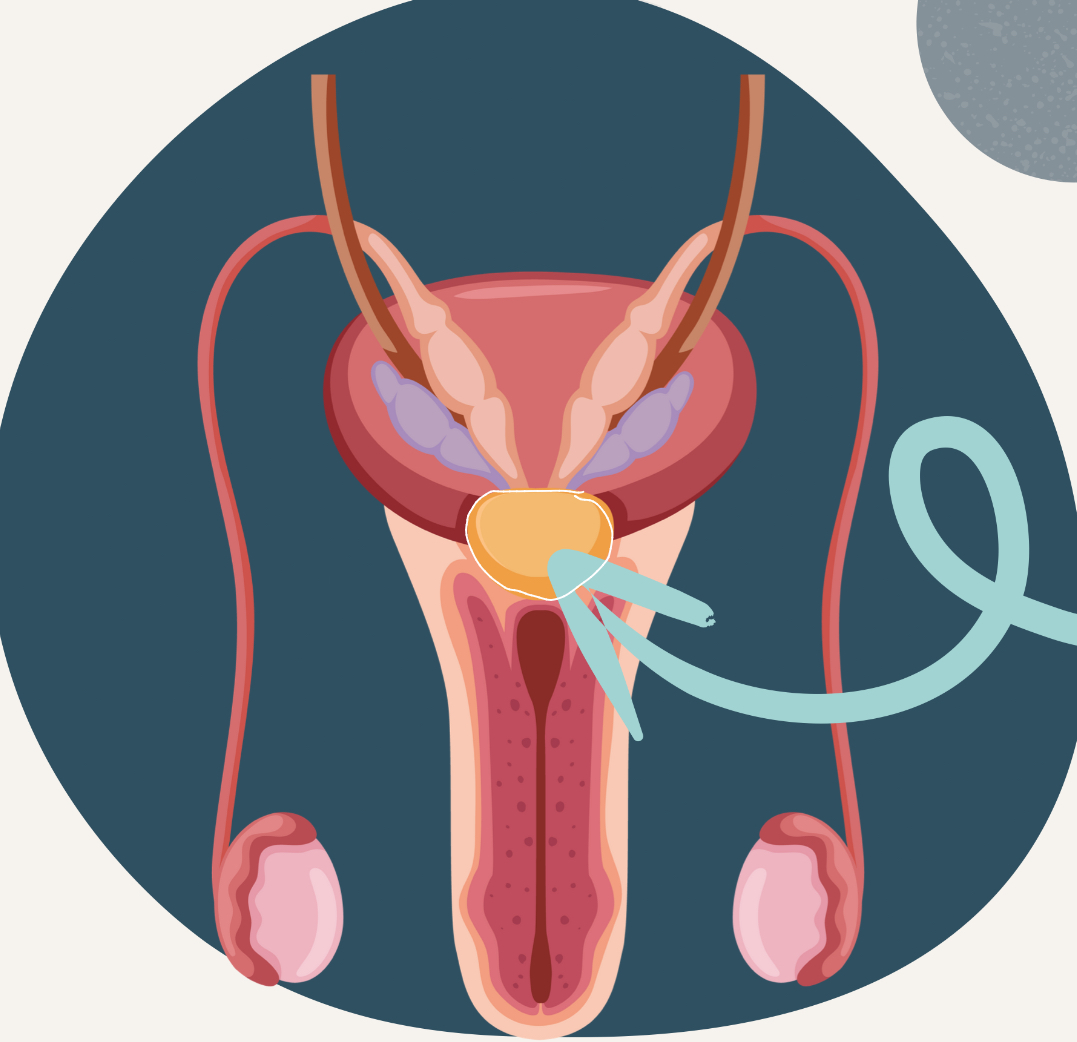
prostate (cont.)
like a switch to allow either urine or semen—not both
vas deferen + seminal vesicle come from prostate gland
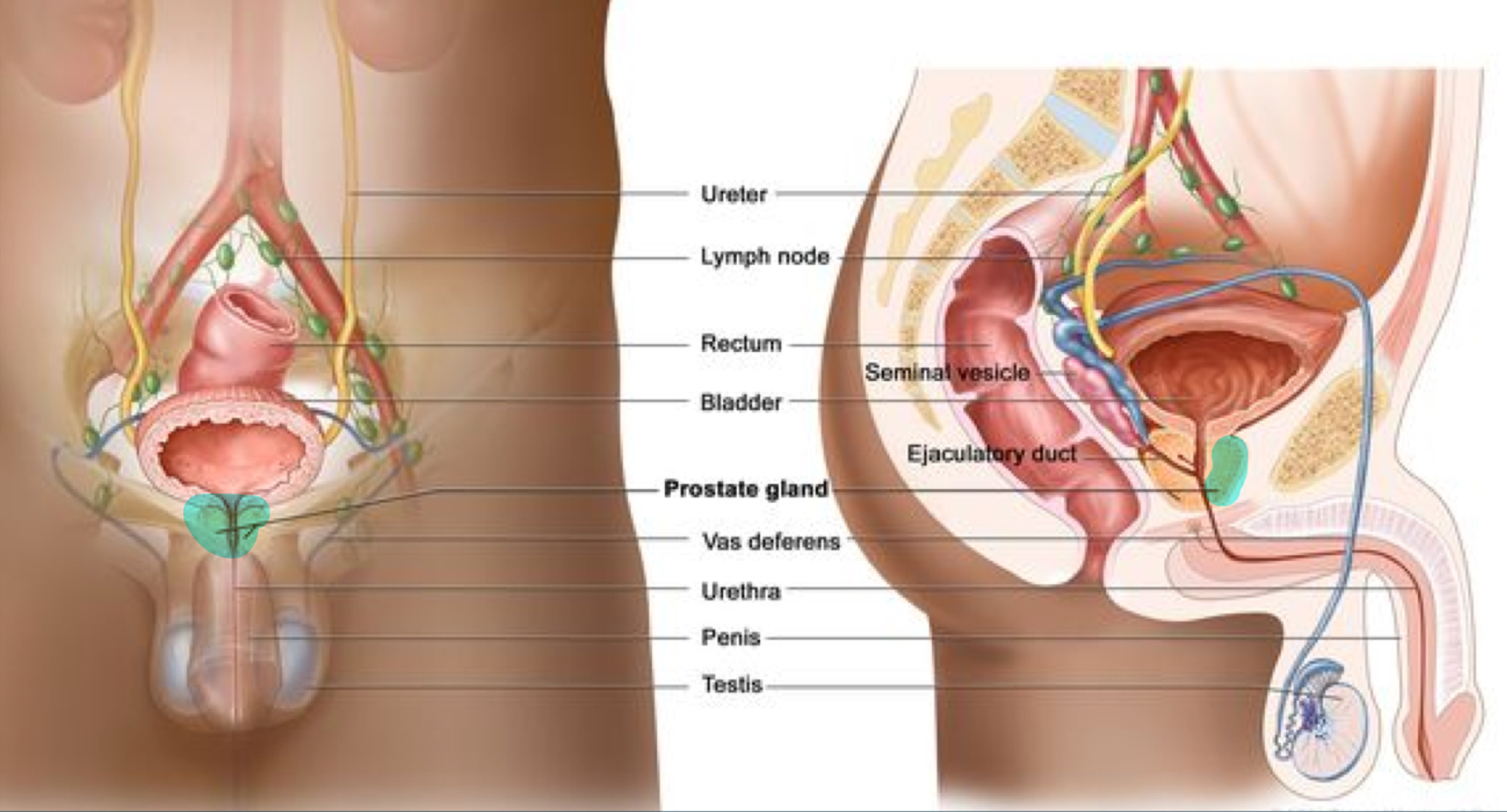
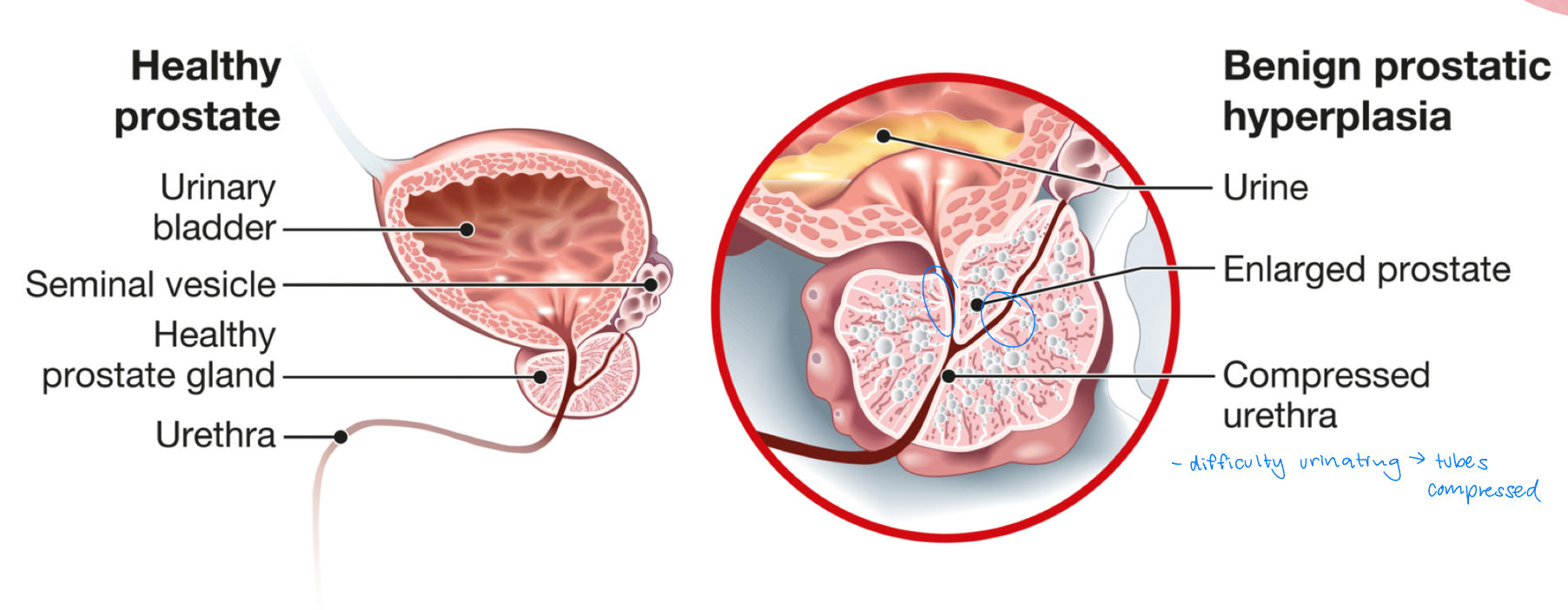
benign prostatic hypertrophy (BPH)
noncancerous enlargement of prostate gland
compresses urethra = difficulty urinating
etiology: unknown; most likely due to aging and hormone changes
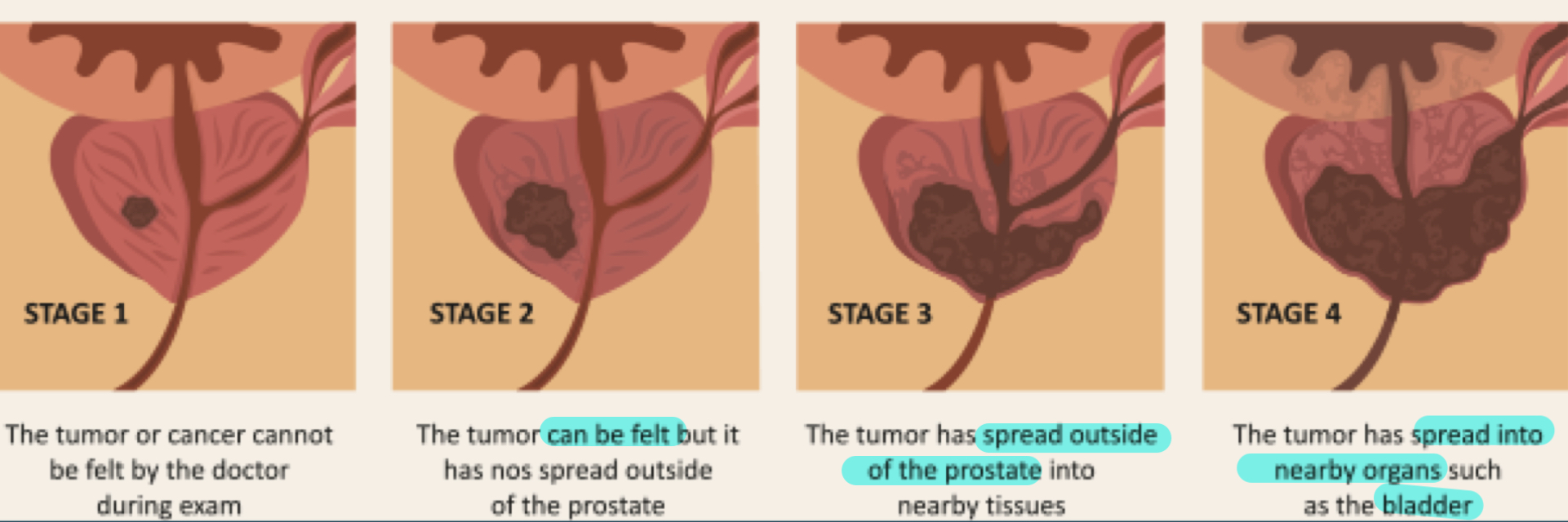
prostate cancer
(prostate lies directly anterior to rectum)
stage 1: tumor/cancer cannot be felt by doctor during exam
stage 2: tumor can be felt but it has not spread outside of prostate
stage 3: tumor has spread outside of prostate into nearby tissues
stage 4: tumor has spread into nearby organs such as bladder
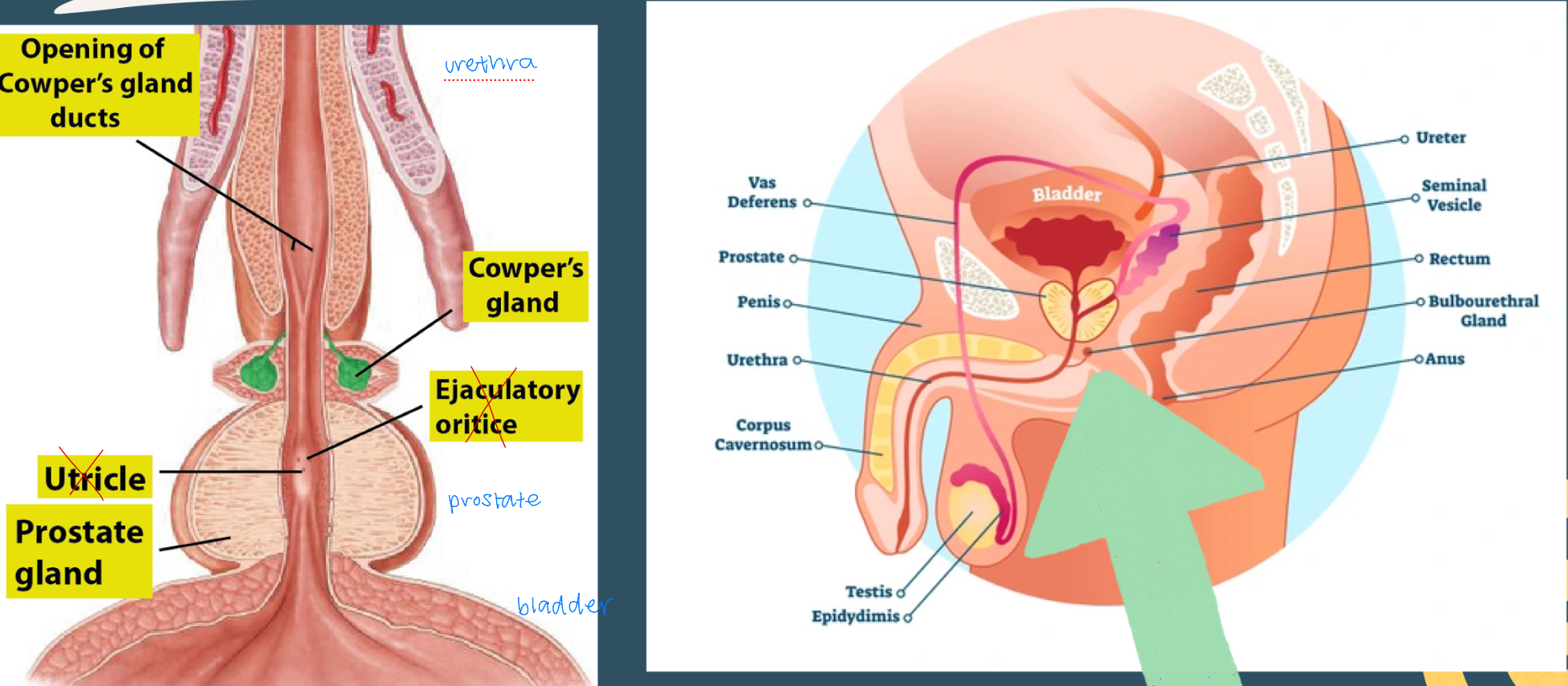
cowper’s gland
also called the bulbourethral gland, one of the two pea-sized organs found beneath the prostate gland
responsible for releasing fluid that flushes out foreign matter, lubricates, and neutralizes any acid in the urethra so the sperm will be safe and able to pass through freely
ensures sperm doesn’t mix with urine
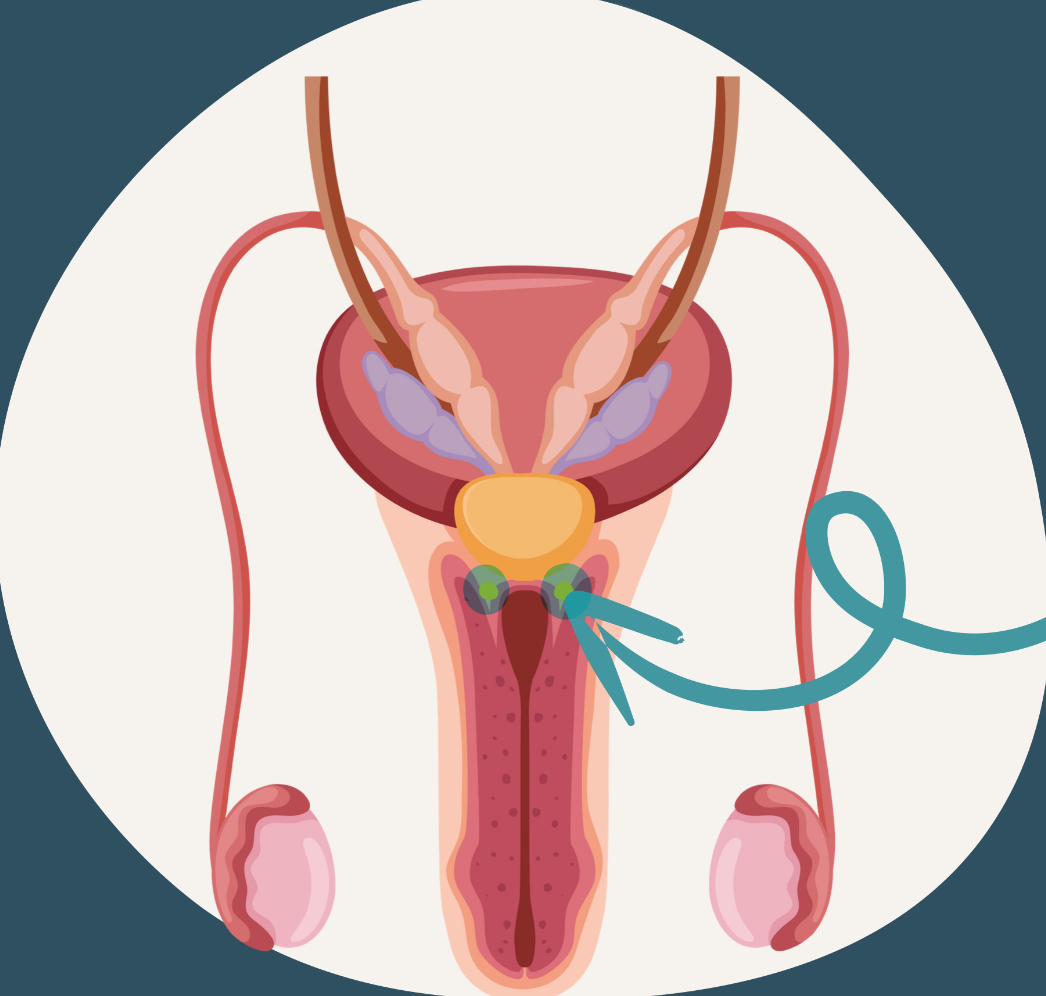
cowper’s/bulbourethral gland (different views)
sperm cell
head: where genetic info is
acrosome: most external; break through ovum’s outer layer
nucleus: genetic info
centriole
neck: connects head to body
body (mid piece): energy
mitochondria: gives energy for sperm to move
terminal disc
tail: propel/give motion
plasma membrane
axial filament
end piece
infertility can be due to genetic makeup of sperm
sperm pathway
testes: sperm, testosterone made
epididymis: mature sperm stored
vas deferens
seminal vesicles: gives nutrition (fructose/enzymes/prostaglandin) to semen
prostate
urethra: corpus spongiosum surrounds urethra (spongy urethra)
bulbouretheral gland: clears the urethra