1.2-3 - age related tissue changes
1/111
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
112 Terms
a self for-filling prophecy… internalized stereotypes that become self definitions that directly influence older adults mental, physical and cognitive health
describe the stereotype embodiment theory
T (in fact, people that internalize ageist beliefs will die sooner)
T/F: people that hold more positive beliefs around aging live longer
internal
do internal or external views impact aging more
FACT - but exercise can counteract and limit the amount of loss. thus, someone who is 65 and exercises regularly may be in better shape
myth or fact: physical strength declines with age
MYTH - 2.3% are living in SNF
myth or fact: most olerder adults will end up in a nursing home
FACT - however they may need help with things like moving furniture
myth of fact: about 80% of older adults report they don't need extra assistance with daily activities
MYTH - typically they will under report, it is true that older individuals will feel more pain due to an illness but not the actual aging process itself
myth or fact: pain is a natural part of aging process
T
T/F: aging is not a disease
F
T/F: there is a universal accepted theory of biological aging
T (ex. OA, age may bring dec synovial fluid and articular cartilage but that isn’t OA, they are risk factors for OA)
T/F: no pathology is inevitable with age
psychological, social, environmental
biological aging is inextricable from ___________, _____________, and _______________ factors
T
T/F: aging may increase vulnerability to pathology
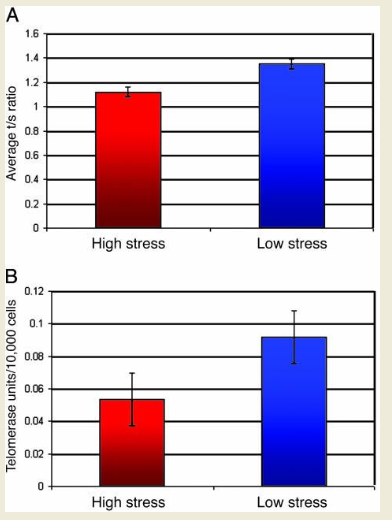
shorter
does the length of the telomere part of DNA get shorter or longer with increased stress
non-genetic
(genetic or non-genetic) factors account for up to 84% of the variance in human lifespan
heterogeneity
as humans progress across the lifespan, we become less alike and present with increasing variance which means _______________
longitudinal
what kind of study is best for representing age related changes
cross sectional (like a snap shot in time of multiple people)
what kind of study is best for representing age differences
plastic
lifespan development is (plastic or elastic)
myocardial infarction
the presentation of illness of ___________________:
may be no chest pain but present with diaphoresis, dyspnea, epigastric distress, syncope, weakness, vomiting, confusion or upper extremity pain.
pneumonia
the presentation of illness of ___________________:
malaise, anorexia, confusion, fever may be absent, cough without significant production.
urinary tract infection
the presentation of illness of ___________________:
confusion, dizziness, anorexia, fatigue, weakness possibly without fever.
F
T/F: the presentation of illness tends to not differ among older adults
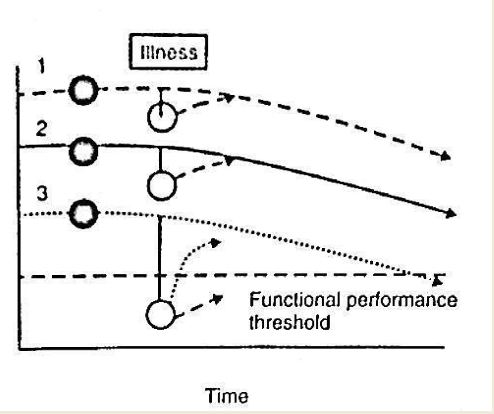
decrease (reserve capacity is the ability to maintain homeostasis in response to stress)
a major age-related change is a (dec or inc) in reserve capacity
0.5; 40
older adults experience a gradual loss of bone mass at about ____% per year starting around ________ years old
>
as we age the bone resorption rates (< or >) formation rates
>
as we age trabecular bone loss (< or >) cortical bone
bone mass; loss
bone mass in later life is related to peak ___________ achieved and rate of ____________
trabecular/cancellous
as we age we tend to lose more (trabecular or cortical) bone
females (mostly due to post menopause)
do females or males have greater loss of trabecular bone/bone density
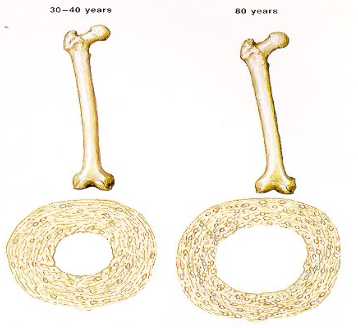
inc; inc; thin
as we age the total boe diameter (dec or inc) and the marrow cavity (dec or inc) which in turn makes the wall (thin or thick)
porosity
aging creates an increased diameter of the haversian canals means there will be an increase in _____________
primary = Exacerbated rates of expected age changes
secondary = Medical conditions, Medications, Immobilization, Nutrition disorders
what is the difference between primary and secondary osteoporosis
65
70
50
50
you would test for bone mineral density if:
female age ________ years and older
male age _________ years and older
anyone who has broken a bone after age _________ years
anyone over _________ years with risk factors present
DEXA scan
_____________ is the most common measurement for osteoporosis
>10 cm
>3 cm
>5 cm
<2 finger widths/about 3.6cm
the measurements of the postural assessment and vertebral fracture screening for osteoporosis:
Tragus to wall test =
Occiput to wall test =
Height loss =
Rib-pelvis distance =
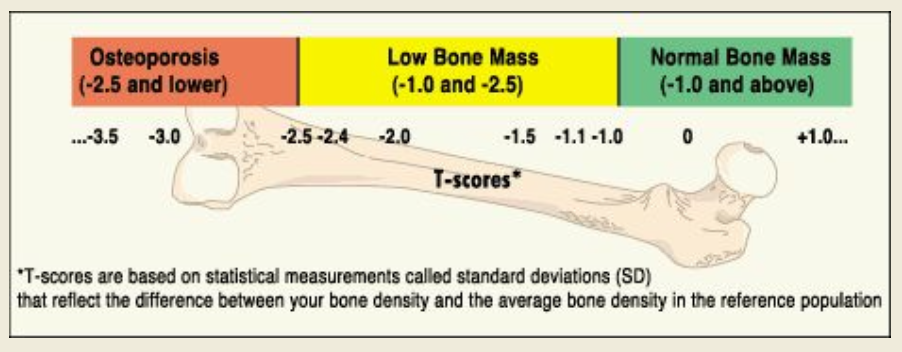
1.0; 1.0-2.5; >2.5
based of the DEXA scan, if a person falls _______ standard deviations below the yound adult female reference is considered normal, __________ standard deviations is considered low bone mass (osteopenia), and ___________ standard deviations is considered osteoporosis

nutritional support
hormonal support
nechanical stimulus
*need all three or the stool falls down
what is the 3 legged stool approach for osteoporosis care plan
vitamin D3
calcium
other viatmins with benefit: vitamin C, folic acid, B12, B6
what are some nutritional support/diet supplements for osteoporosis care plan
antiresorptives; anabolic agents
_______________ are hormonal medications that inhibit bone resorption and _______________ are hormonal medications that stimulate bone formation
antiresorptives
examples of _______________ hormonal medication:
Hormone Replacement Therapy (HRT), Bisphosphonates, Selective Estrogen Receptor Modulators, Calcitonin, RANK Ligand Inhibitor
anabolic agents
examples of _______________ hormonal medication:
Sclerostin Inhibitor, Parathyroid Hormone (PTH) Analog, Parathyroid Hormone-Related Protein (PTHrp) Analog
combo of impact exercise and resistance training
what is the exercise recommendation for osteoporosis
flexion; rotation; femur; overhead
what to avoid with osteoporosis exercise:
loaded trunk ________
end range trunk ________
end range _________ rotation
strenuous ___________ lifts
50-85%
50 jumps/session
the recommendation for older adults with resistance training is _____-____%
the recommendation for older adults with impact exercise is ____________
vertebral body
where is the compression on the spine in someone who is kyphotic or in a loaded trunk flexion position
F - brace is TEMPORARY
T/F: wearing a brace for an acute compression fracture is recommended for long term use
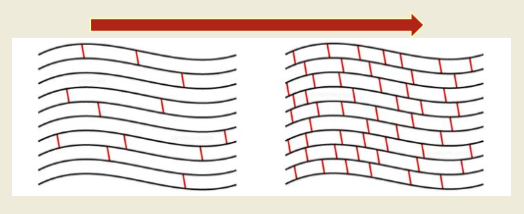
dec; inc; dec; dec
expected age-related change:
(dec or inc) water content
(dec or inc) cross-linking in collagen
(dec or inc) quantity of elastic fibers
(dec or inc) synovial fluid quantity and quality
inc; dec; dec
expected age-related change:
(dec or inc) stiffness and passive tension
(dec or inc) joint end range (still WFL)
(dec or inc) shock absorption
cervical - extension and lateral flexion
thoracic - extension
lumbar - extension, flexion, lateral flexion
hip - extension
ankle - dorsiflexion
shoulder - flexion, ER
the expected age-related decrease in ROM:
cervical -
thoracic -
lumbar -
hip -
ankle -
shoulder -
45; 2-4cm; >5cm
expected height loss starts at about age _________ and height has about a _____-_____ drop over life course, if height loss is more than ______ it could lead to potential compression fracture
postural changes
IV disc dehydration
what are 2 reasons why we see height loss
T
T/F: a decrease in articular cartilage water content and chondrocytes is expected with aging
F (it increases the RISK of OA)
T/F: older cartilage indicates osteoarthritis
inc
dec
inc (inc RISK, not causing OA)
expected age-related articular cartilage changes:
(dec or inc) resistance to joint surface gliding
(dec or inc) shock absorption across joint surface
(dec or inc) risk of developing OA
Subchondral bone
Joint capsule
Synovial membrane
Ligaments
Periarticular muscles
what other factors play into developing OA besides articular cartilage
F
T/F: imaging correlates with function/pain of an OA diagnosis
cytokines and catabolic enzymes
the pathological changes to chondrocytes cause an inflammatory response which creates an increase in ___________ and _____________
1 and 10 (leads to being unable to repair degraded AC matrix)
the pathological changes to chondrocytes cause an abnormal synthesis of type _____ and type _____ collagen
F (no nerve supply to cartilage, pain comes from the inflammation response to muscles, etc.)
T/F: joint pain comes from the degeneration of cartilage
early
in the (early or late) stage of OA, the cortical bone plate thins
late
in the (early or late) stage of OA, the cortical bone plate thickens
WOMAC; high
the __________ is a self reported outcome measure for OA looking at pain, stiffness, and physical function; a (low or high) score indicates a worse impairment
anti-inflammatory and pain reduction
to treat _____________ and ____________ take…
NSAIDs, Cox-2 inhibitors, intra articular corticoid injection
pain reduction
to treat _____________ take…
Tramadol, Acetaminophen
intra articular hyaluronic acid injections
to treat _____________ take…
lubrication, modification of cellular activity
T
T/F: there is NO FDA approved disease modifying drugs
inc
dec
dec
age expected responses in integumentary system:
(dec or inc) risk of skin tears and cracking
(dec or inc) protection from dehydration
(dec or inc) protection from infection
dec
dec
dec
dec
inc
inc
dec; inc
expected age-related changes: muscle tissue
(dec or inc) satellite cells
(dec or inc) mm tissue synthesis and repair capacity
(dec or inc) capillary density
(dec or inc) mitochondrial density
(dec or inc) inflammatory cytokines
(dec or inc) oxidative stress
(dec or inc) elastin and (dec or inc) collagen fibers
stiffness
decreased elastin and increased in collagen leads to an increase in ___________
dec
DEC
inc
dec
expected age-related changes:
muscle fibers:
(dec or inc) quantity, CSA, length
(dec or inc) Type II
(dec or inc) non-contractile CT and lipid infiltration
(dec or inc) total muscle CSA
dec
inc
dec
dec
inc
inc
Expected age-related changes: neuromuscular system
● (dec or inc) # motor units
● (dec or inc) size of motor units
● (dec or inc) # anterior horn cells/α motor neurons
● (dec or inc) motor nerve conduction velocity
● (dec or inc) contraction/relaxation time
● (dec or inc) antagonist co-activation
dec
dec
dec
dec; inc
inc
Expected age-related changes:
● (dec or inc) % lean muscle mass
● (dec or inc) force production
● (dec or inc) power
● (dec or inc) ROM end range / (dec or inc) susceptibility to contraction induced injury
● (dec or inc) movement stiffness
sex
between muscles
nutrition
physical activity
hormones
medications (ex . statins)
comorbidities
responsive to exercise
what 8 factors determine the degree in change and impact on function
sarcopenia
_______________ is an age-related condition of progressive loss of skeletal muscle mass, strength, and function
dec; inc; dec
age-related changes with sarcopenia:
(dec or inc) estrogen, testosterone, growth hormone
(dec or inc) inflammation and stress
(dec or inc) activity/sedentary lifestyle
osteosarcopenia
osteoporosis + sarcopenia = _____________
dec
inc
inc
dec
dec
dec (dec in baroreceptors means higher risk or orthostatic hypotension)
inc; inc
expected age-related changes: cardiovascular system
● (dec or inc) sinoatrial (SA) node cells
● (dec or inc) stiffness in myocardium
● (dec or inc) stiffness and thickness in mitral & aortic valves
● (dec or inc) capillary density
● (dec or inc) # myocytes (offset by hypertrophy)
● (dec or inc) baroreceptor sensitivity
● (dec or inc) LV fill time, (dec or inc) LV end diastolic volume
inc
dec
inc
inc (increased vascular tone due to prolonged vasoconstriction and limited vasodilation)
expected age-related changes: cardiovascular system
● (dec or inc) thickness/irregularity of capillary basement membrane
(dec or inc) oxygen extraction to working muscles
● (dec or inc) stiffness in vessel walls
● (dec or inc) vascular tone
dec
dec
dec
dec
inc
expected age-related changes: cardiovascular system
(dec or inc) VO2max
(dec or inc) MAX HR
(dec or inc) stroke volume*
(dec or inc) A-V O2 diff
(dec or inc) systolic BP
T
T/F: we would expect a decrease in VO2max with age
cardiovascular disease
what is the leading cause of death
< 120/80
130-139/80-89
optimal blood pressure =
medically controlled HTN =
>20 weeks
60-70% of VO2max
the following training factors to increase VO2max in previously sedentary older adults (age >60):
____________ duration
____________ intensity
T (training factors: mod to high intensity in aerobic ex)
T/F: older adults with chronic conditions can increase their VO2max
intensity
do not limit ___________ based on age
airways
inc
dec
dec (dec in cilia means inc risk of infection and expelling the lungs)
lung tissue
inc
dec (dec in elastic recoil means dec ventilation and gas exchange)
inc
alveoli
inc
dec
dec
dec
expected age-related changes: pulmonary system
airways
(dec or inc) rigidity of trachea and bronchi
(dec or inc) elasticity and contractility in bronchioles
(dec or inc) cilia
lung tissue
(dec or inc) compliance
(dec or inc) elastic recoil
(dec or inc) mucus layer
alveoli
(dec or inc) size
(dec or inc) surface area
(dec or inc) capillary interface
(dec or inc) gas exchange
dec
dec
dec
dec
inc
inc
expected age-related changes: pulmonary system
ribcage + respiratory muscles
(dec or inc) strength/contractile proteins
(dec or inc) diaphragm efficiency
(dec or inc) capillary density
(dec or inc) thoracic cage mobility
(dec or inc) connective tissue
(dec or inc) contraction/relaxation time
inc
dec
inc
dec
dec
expected age-related changes: pulmonary system
(dec or inc) work required
(dec or inc) V/P ratio
(dec or inc) respiratory rate
(dec or inc) O2 sats (>92% in absence of disease)
(dec or inc) Forced Exp. Volume (FEV1)
inc
inc
dec
dec
expected age-related changes: immune system
● (dec or inc) baseline systemic inflammation
● (dec or inc) risk of infection
● (dec or inc) ability to ID pathology
● (dec or inc) response to pathology
dec
dec
expected age-related changes: endocrine/metabolic systems
(dec or inc) hormone production
(dec or inc) target tissue response
dec
inc
dec
dec
dec
dec
expected age related brain changes: nervous system
● (dec or inc) volume + gyral thickness
● (dec or inc) ventricular size
● (dec or inc) sensory neurons
● (dec or inc) # of axons
● (dec or inc) Purkinje cells in cerebellum
● (dec or inc) myelin sheath and conduction velocity
inc
the rest of the bullet points are DECREASE
expected age related functional changes: nervous system
(dec or inc) reaction time
(dec or inc) short term memory
(dec or inc) memory retrieval (proper nouns)
(dec or inc) thermoregulation (ANS)
(dec or inc) movement speed
(dec or inc) reflexes
(dec or inc) perceptual acuity
(dec or inc) postural control and balance
F
T/F: you would expect the nervous system to impact task completion in older adults
proper nouns
older adults have a decreased memory retrieval especially with _____________
presbyopia
_____________ is age-related vision loss
inc
inc
dec
dec
dec
dec
dec
dec
expected age related changes: vision
(dec or inc) lens stiffness
(dec or inc) glare sensitivity
Pupillary aperture narrows
(dec or inc) contrast
(dec or inc) peripheral and visual field
(dec or inc) visual acuity
(dec or inc) light/dark adaptation
(dec or inc) depth perception
(dec or inc) tear production
>40
can expect presbyopia at age __________
inc; far
presbyopia (dec or inc) lens stiffness and is related to (near or far) sightedness

macular degeneration
________________ is when the central portion of the retina (macula) deteriorates causing central visual field loss

glaucoma
____________ is damage to the optic nerve causing peripheral vision loss