Eye Histology
1/23
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
24 Terms
Describe the three layers of the eye
3 concentric layers
outer supporting layer, the corneoscleral coat (colorless and blue) (aka fibrous layer)
middle vascular coat or uvea (pink)
inner photosensitive layer, the retina (yellow)
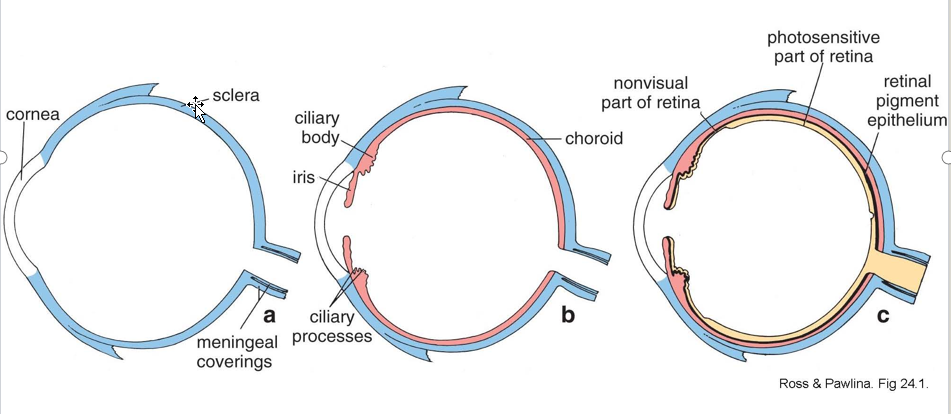
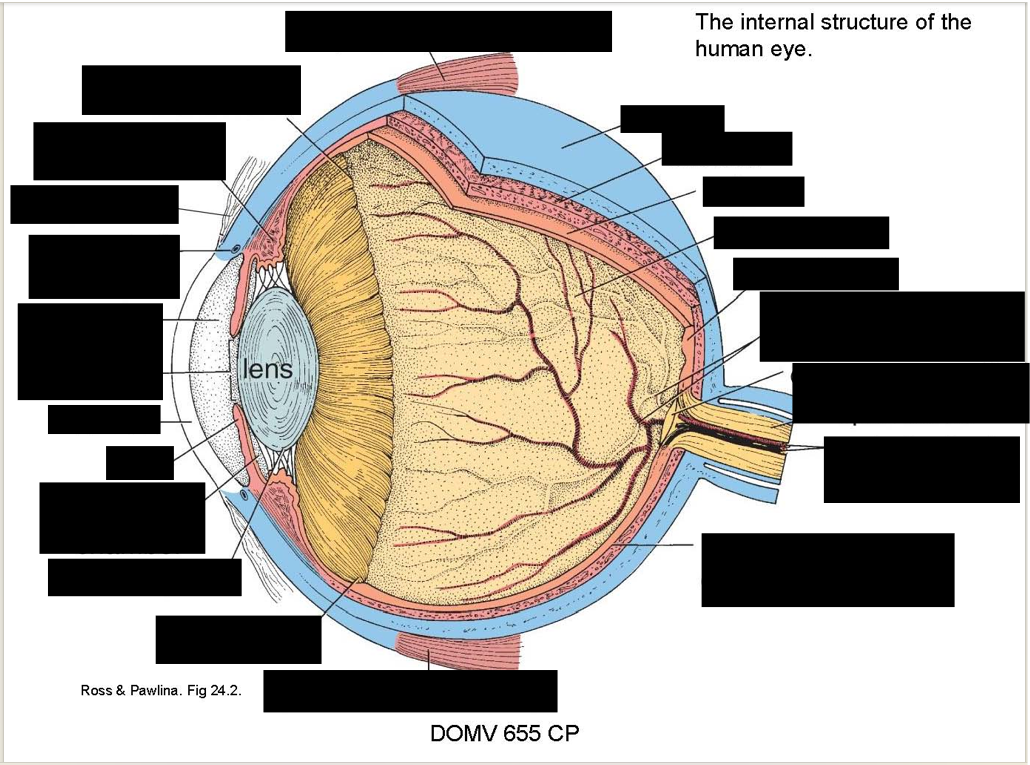
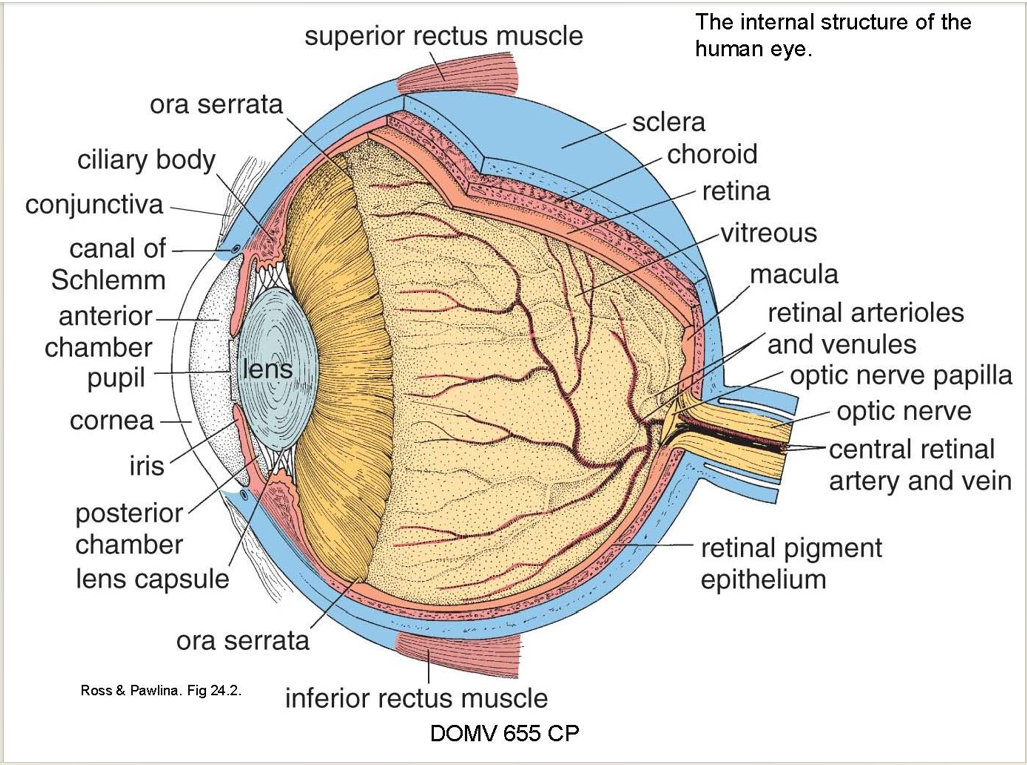
Describe the two parts of the fibrous layer
Location?
Function? (1);
Describe properties
What’s the limbus
Parts:
Sclera
posterior 5/6 of the eyeball
maintain eye shape
Dense, opaque fibrous coat
Cornea:
Ant. 1/6 of eye
Transparent part of fibrous coat
Limbus:
Corneoscleral Junction
Contains Scleral Venous Sinus (canal of Schlemm)
on internal surface of the sclera
Describe the Sclera
Episclera:
Stroma
Lamina Fusca
Lamina cribrosa
Collagen Arrangement:
Sclera Histological Features:
Episclera:
Loose connective tissue (vascular)
Stroma
irregularly arranged, thick collagen fiber bundles and many fibroblasts
Lamina Fusca
suprachoroid lamina w/ melanocytes.
Lamina cribrosa
specialization where optic nerve fascicles and vessels penetrates sclera
Collagen Arrangement:
circles or figure eight patterns spiraling around openings for central retinal artery and vein
Perforated disc appearance.
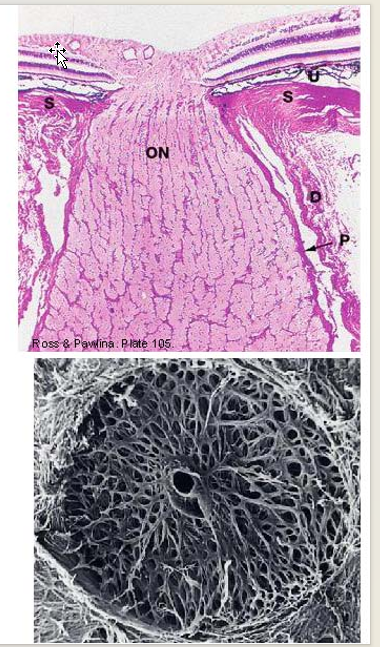
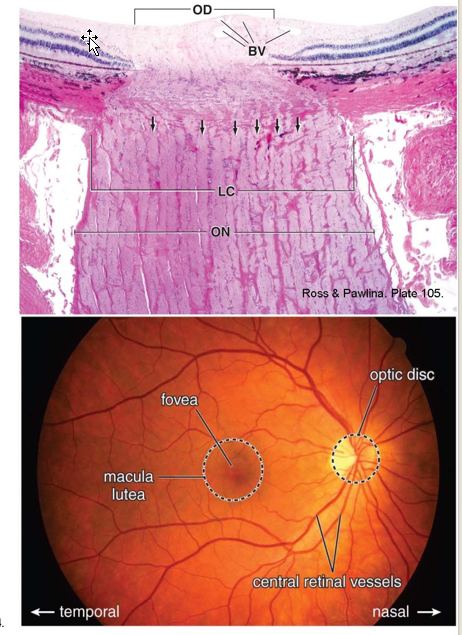
Describe the Limbus
CT present here
Describe blood vessels found here
Describe Contents of Internal Scleral Sulcus
What is the Scleral spur
Limbus:
CT:
Loose conjunctival subepithelial connective tissue
Blood Vessels:
conjunctival capillaries terminate here.
Contents of Internal Scleral Sulcus:
houses trabecular meshwork (with spaces of Fontana) and canal of Schlemm
Endothelium-lined channel
Pathway of aqueous humor outflow
thus, control of intraocular pressure
Scleral spur:
origin of corneoscleral trabecullae
Describe the Cornea
Properties
Function
list the 5 layers
Cornea:
Properties:
Transparent
regular epithelium
avascular
regular arrangement of stromal components
Function:
Major refractive element of eye
Curve irregularities = astigmatism
5 layers:
Epithelium
Bowman's membrane
Stroma (substantia propria)
Descemet's membrane
Endothelium
Describe the five layers of the Cornea
Epithelium: (5-6 layers)
Histology:
External surface contains/function:
Cont. w/:
Regenerative capacity:
Innervation:
Bowman’s Membrane:
Histology:
Function:
Location:
Regenerative Capacity:
Stroma (substantia propria):
Histology:
Transparency influenced by:
Cont. W/:
Descemet’s membrane
basement membrane for:
Extends into:
Corneal Endo:
Histology:
Function:
Damage →
Epithelium: (5-6 layers)
Histology:
Stratified squamous nonkeratinized epithelium
External surface contains/function:
microvilli
microplicae
help stabilize precorneal tear film
Cont. w/:
conjunctival epithelium
Regenerative capacity:
new cells generated in limbal region → migrate centrally
minor wounds heal rapidly
Innervation:
Numerous free nerve endings: touch, pain
Bowman’s Membrane:
Histology:
Acellular region
has Fine, randomly arranged collagen fibrils
Function:
helps anchor corneal epithelium
alongside basal lamina on external surface
forms barrier for infection
Location:
Ends @ limbus
Regenerative Capacity:
Does not regenerate well → corneal scarring
Stroma (substantia propria):
Histology:
collagen fibers and fibroblasts
flattened, collagenous lamellae
parallel to corneal surface
oriented at right angles
Flattened modified fibroblasts (keratocytes) between layers
Transparency influenced by:
regular diameter and spacing of collagen fibers
(maintained by glycosaminoglycans)
Cont. W/:
sclera at limbus
Descemet’s membrane
basement membrane for corneal endothelium
Extends into trabecular meshwork
Corneal Endo:
Histology: Simple squamous epithelium
Function:
Allows passage of nutrients from aqueous humor
critical for corneal hydration (stroma)
Damage →
swelling of stroma with loss of transparency
What are the 3 parts of the vascular layer
3 parts: choroid, ciliary body, iris
Describe the Choroid
Properties:
Location:
Consists of:
Function:
Attachment:
Bruch's membrane (lamina vitrea)
Function:
Clinical Significance:
Suprachoroid
Location:
Consisting of:
potential space?
Choroid:
Properties:
dark brown
highly vascularized
Location:
between the sclera and retina
(posterior 5/6 of eyeball)
Consists of:
choriocapillaris: net-like capillary beds
Fenestrated
Greatest density near macula
Bruch's membrane
a thin, amorphous hyaline membrane
Function:
choriocapillaris → supplies outer layers of retina
Attachment:
Firmly to pigmented layer of retina
Loosely to Sclera
Bruch's membrane (lamina vitrea)
acellular membrane
Function:
Acts as Basal Lamina for:
retinal pigment epithelium, collagenous and elastic layers,
Acts as basement membrane for:
endothelium of choriocapillaris
Clinical Significance:
Drusen: Areas of diffuse or discrete thickening
Suprachoroid
Location:
transition layer between choroid and lamina fusion of sclera
Consisting of:
interconnected layers
melanocytes,
fibroblasts,
connective tissue fibers
has surrounding potential (suprachoroidal) space
Describe the Ciliary Body
Structure:
Cont. W/:
Extends from? 2 Parts?
Function:
Annular smooth muscle fibers
3 parts:
Describe Ciliary Epithelium
Histology:
2 Layers? 1: Cont. of? 2. Function?:
Describe the Stroma
What is it?
Contains:
Cont. of:
Describe the Ciliary muscle
Innervation:
Mech (via radial/circular muscle fibers):
3 Groups:
Attached to?
function?
What is the function of ciliary processes?
Ciliary Body
Structure:
Ring Shaped; surrounds Lens
Cont. W/:
choroid behind and the iris in front
Extends from
scleral spur: ora serrata (irregular anterior border of retina)
Ant. 1/3 = (pars plicata)
contains: 70 radially arranged folds- ciliary processes
Post. 2/3: (pars Plana)
Function:
suspend lens → control thickness
via zonular fibers of suspensory ligament
Annular smooth muscle fibers
found w/in external part of ciliary body
3 parts:
ciliary epithelium
ciliary body stroma
ciliary muscle
Ciliary Epithelium
Histology:
Cuboidal, columnar epithelium
2 Layers:
Outer pigmented layer
Continuation of retinal pigment epithelium
Inner NON-pigmented layer:
Function
Secrete aqueous humor (ciliary process)
Produce vitreal collagen and hyaluronin
pars plana
Produces and anchors zonular fibers
pars plana
Stroma
What is it?
Vascular connective tissue layer extending into ciliary processes
Contains:
melanocytes and fibroblasts
Cont. of:
Choroid
Ciliary muscle
Innervation:
postganglionic parasympathetic from ciliary ganglion
Mech (via radial/circular muscle fibers):
Contraction (displaced towards optic axis) → suspensory ligament relaxed → lens thickens → near vision
Vice Versa for Far Vision
3 Groups:
Outer longitudinal muscle fibers
Attached to scleral spur
Function:
distends spaces of trabecular meshwork → aqueous outflow
Middle radial muscle fibers
Attached to circular fibers and scleral spur
Inner circular muscle fibers
Anteriorly located, sphincter arrangement
Ciliary processes
Function:
produce Aqueous Humor;
nourishes avascular lens and cornea
Describe the Iris
Location
Function
Base of Iris?
cont. w/?
Connected to?
Describe the substances that gives the iris pigments (2)
Describe the muscles of Iris:
Orientation?
Function?
Innervation?
Shape?
Describe the anterior zone: What separate what here?
List the four layers:
Iris:
Location:
Contractile diaphragm located in front of the lens
Surrounds pupil
Function:
Controls amount light entering eye
Base of Iris:
cont. w/ ciliary body
connected to inner border of cornea by trabecular meshwork.
Pigments:
Melanocytes and blood vessels in stroma
very dark posterior pigment epithelium
Muscles of Iris:
Sphincter pupillae:
annulus of smooth muscle;
contraction decreases pupil size (miosis);
supplied by parasympathetic fibers
Dilator pupillae:
radial smooth muscle;
increases pupil size (mydriasis);
supplied by sympathetic fibers
Shape:
Cone shaped
margin anterior to root Margin and root are thinnest
Anterior Surface:
ciliary zone and pupil zone separated by collarette
Radially-oriented collagenous trabeculae (elevations) in ciliary zone
some surround ovoid crypts
Layers:
Anterior border layer,
Stroma,
Dilator pupillae muscle,
Posterior pigment epithelium
Describe the four layers of the Iris
Anterior border layer
Histology:
Stroma:
Histology:
Communicates w/
Contains:
Dilator pupillae muscle (anterior epithelial layer)
Histology:
Orientation:
Basal vs apical portion:
Posterior pigment epithelium
Histology:
Extends:
Layers forms:
Anterior border layer
Histology:
No epithelial cells
Uneven discontinuous layer consisting of:
dense collection of fibroblasts + melanocytes + (few) collagen fibers
Stroma:
Histology:
Loose CT containing:
fibroblasts + melanocyte + collagen fibers,+ network of blood vessels.
Communicates w/
aqueous humor of anterior chamber
via openings in anterior border layer
Contains: sphincter pupillae
Dilator pupillae muscle (anterior epithelial layer)
Histology:
Layer of myoepithelial cells
derived from ant. layer of pig. epithelium
Orientation:
Radially Oriented
Basal vs apical portion:
Basal: Muscular
Apical: Epithelial
lightly pigmented
apposed to posterior pigment epithelial cell
Posterior pigment epithelium
Histology:
Large cuboidal epithelial cells that are densely pigmented.
Extends:
onto anterior surface at pupillary margin. (short distance)
Layers forms:
radial folds most apparent near pupil margin
Describe Aqueous Humor
Flow Pathway
Describe Glaucoma:
Pathophysiology
Types
Flow:
Post. → Ant. chamber (through zonule and pupil)
iridocorneal angle → trabecular meshwork
Drains into scleral venous sinus (canal of Schlemm)
Glaucoma:
Pathophysiology:
Increased resistance to aqueous humor outflow → increased intraocular pressure
Types:
Open angle
Obstruction of trabecular meshwork
Close Angle:
Iris physically blocks inner surface of anterior chamber angle
Note: Both forms may be primary or secondary.
Describe the Retina
Two Layers
contents of each
Two Divisions:
Location?
Extends?
Contains?
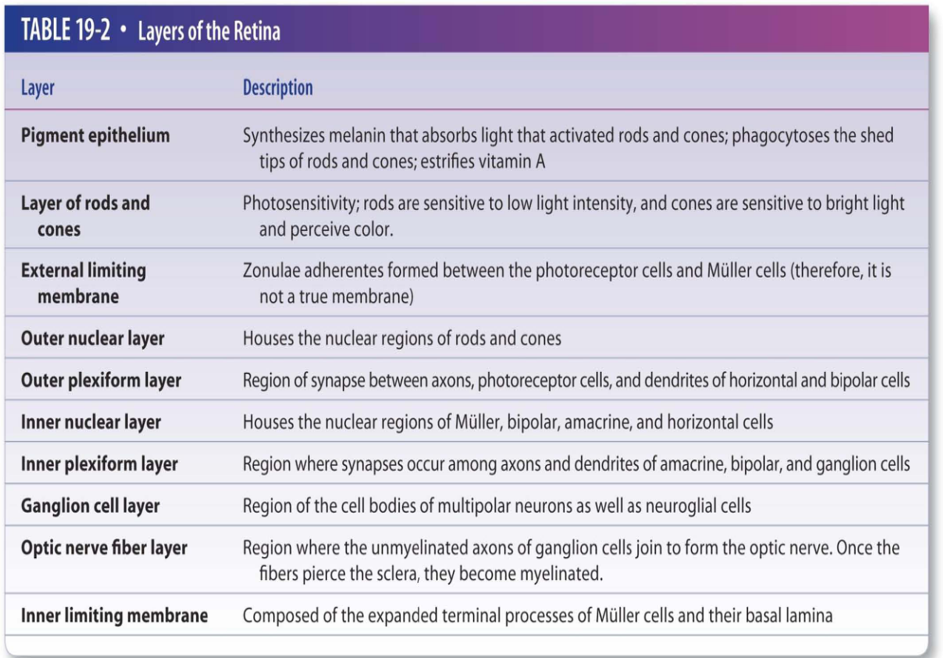
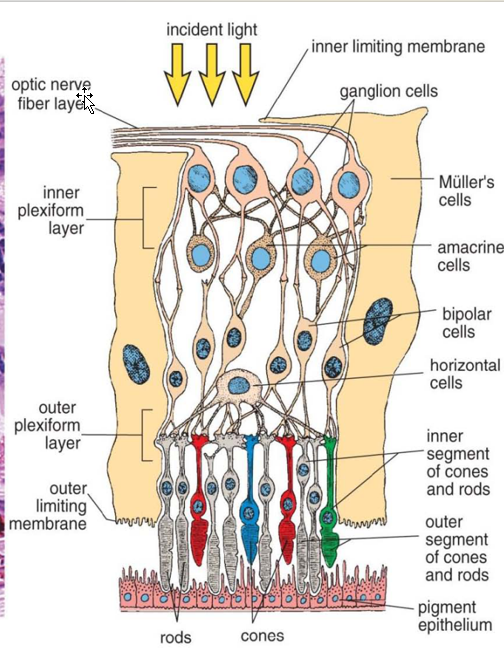
Two Layers:
Inner neural layer
Sensory and neural cells
Photoreceptors (rods/cones);
bipolar cells,
ganglion cells;
interneurons (horizontal and amacrine cells);
supporting cells (Müller cells)
Optic Disc (blind spot)
Macula Lutea — yellow elliptical area (1.5mm diameter) toward center of retina;
contains: Fovea Centralis (foveola)
central depression
area of most acute vision;
contains only cones
Outer pigmented layer
Retinal pigment epithelium
Fused with choroid
Divisions:
Optic part of retina (pars optica)
light sensitive;
extends from optic disc → Ora Serrata
irregular border slightly posterior to ciliary body.
Non-neural part of retina (pars caeca)
anterior to ora serrata
Extends:
forward over ciliary processes and posterior iris
Contains:
pigmented and columnar epithelium
Describe the two layers of the Retina
Outer Pig. Layer:
cont. w/
Function?
Hisgo. features:
Epithelium made up of?
Adherent to?
Function of Apical Microvillia?
Neurosensory Layer:
Overview
What is the first Layer?
What is the Second Layer?
Differentiate between Rods and cones
Outer Pigmented Layer:
Cont. w/:
pigment epithelium of pars plana
Function:
Absorb excess visible light and UV
Forms: blood-retinal barrier layer
via tight junctions
Adhesion to neurosensory retina
Phagocytosis
of shed photoreceptor membrane disks
Histological Features:
epithelium
Cuboidal, columnar epithelium
More columnar in central
flattened in periphery
Strongly adherent to Bruch's membrane
Apical microvillia
embrace photoreceptor cells;
increase SA for metabolic exchange,
aid in phagocytosis
maintain adhesion to neural retina
NOTE: Site of retinal detachment — a potential space, subretinal space, found here.
Neurosensory Layer:
Overview:
3 layers of cell bodies, 2 layers of synapses
ten layers in all
Layers:
Retinal pigment epithelium
Photoreceptor Layer
Rods:
120 million per eye
Function:
Highly Sensitive
Dim light Vision
no color differentiation
Histo Features:
Long slender cells
Membrane bound lamellae (disks) in outer segment containing rhodopsin
Cones:
7 million/eye
Function:
Less sensitive to light
sensitive to' colors
Highest Density: Fovea
Histo Features:
Conical shaped outer segments
Shorter than rods
Disks in outer segment containing iodopsin
free communication with interphotoreceptor space
Describe layers 3, 4, 5,6 of Retinal Layer
3:
Function
Formed by?
Describe Muller Cells?
4:
Contains?
5:
Layers of?
Composed of?
6:
Contains?
3: External limiting membrane
Function:
mechanical support
Formed by
adherens junctions between apical ends of Müller cells and photoreceptor inner segments
Müller cells
Principal supporting glial cells of retina
Radial orientation
Function:
Envelop blood vessels, neuronal cell bodies and processes
4: Outer nuclear layer
Contains nuclei of rods and cones
5: Outer plexiform layer
Layer of synapses
Composed of process of photoreceptors, bipolar cells, and horizontal cells.
6: Inner nuclear layer
Contains nuclei of bipolar, horizontal, amacrine and Müller cells.
Capillaries (outer plexus) from retinal arteries end in this layer
Describe Bipolar Cells
Function
Connectivity
Describe Horizontal Cells
Cell Process?
Synapses on?
Function?
Describe Amacrine Cells:
Dendritic Processes?
Function?
Bipolar Cells:
function:
Transmit signals from photoreceptor to ganglion cells (single axon passes inward to synapse)
Contributes to sensitivity of rod system
Connectivity:
Fovea: One Cone to One BP
Periphery: 50-100 rods to One BP
Horizontal cells
Cell processes project horizontally
Synapse on multiple photoreceptor pedicles
Function: Integrative
release inhibitory neurotransmitter (GABA)
Amacrine:
Many dendritic processes
Terminates on synaptic complex between BP and gang, cells
Function: Modulatory
(GABA, 5-HT, Ach, DOMV peptide) often inhibitory
Describe layer 7-10
7: Contains?
8: Function?
9: contains? Myelination?
10: Composed of? Separates?
7: Inner plexiform layer
Contains processes of bipolar, ganglion, and amacrine cells.
8: Ganglion cell layer
Output cells of neural retina
Axons coalesce → optic nerve
up to 7 layers of cells combined
9: Optic nerve fiber layer
Contains axons of ganglion cells coursing toward optic disc;
unmyelinated until enter optic nerve
10: Internal limiting membrane
Composed of basal lamina of Müller cells
Separates vitreous and retina
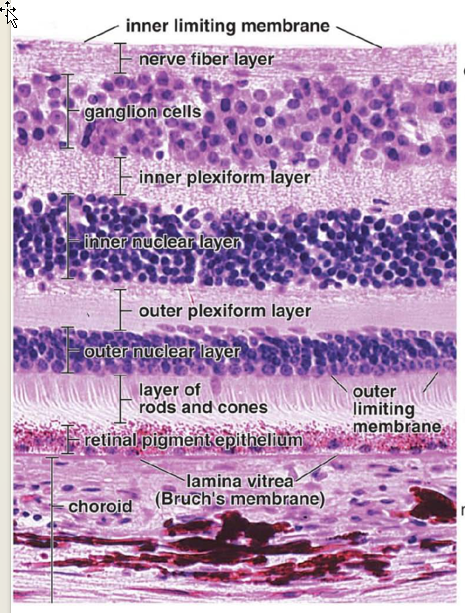
Describe the Chambers of the Eye:
Ocular:
Location?
Divides into
Vitreous:
Location
Contains
Composed of?
Function
Ocular chamber
Location:
anterior to the lens and suspensory ligament
Divided into: anterior and posterior chamber by iris
Vitreous Chamber
Location:
posterior 4/5 of eye between lens and retina
Contains:
transparent, avascular, gelatinous substance
vitreous body
Composed of:
water (-99%), collagen fibers, and hyaluronan
Function:
Holds retina in place,
supports lens,
transmits light
Describe the Lens
Prop.
relationship w/ ciliary
what happens w/ age
3 parts?
Lens:
Properties:
Avascular, biconvex ellipsoid structure
Normally Transparent
Ciliary Muscles Relationship:
alters shape of lens → change refractive power
W/ Age:
Loses elasticity
may lose transparency
Cataracts
3 parts:
Capsule
Anterior epithelium
Lens fibers
Describe the 3 parts of the lens
Capsule
what is it?
produced by
location?
Thickest @
Describe Peri-equatorial region
Function?
Histology?
Produced/maintained by?
Epithelium
Histo
Location
Transformation
fibers
Migration?
Deeper older cells?
Contains?
Lens Capsule
What is it?
Thickened, smooth basement membrane
Produced by
lens epithelium and lens fibers
Location:
Completely envelops lens
Thickest:
pre and post equatorially (17-28 prn)
Peri-equatorial region
Where zonules attach
Histo
Dense, glassy bundles
each contains series of fine fibers composed of microfibrils
Produced/maintained by:
pigmented epithelium of pars plana
Lens Epithelium
Histo:
Simple cuboidal epithelium
Location:
only on anterior surface of lens
Transformation:
Equatorial lens epithelial cells → elongate → transform into lens fibers throughout life
Lens fibers
Migration:
apical part of lens fiber → anteriorly and basal part posteriorly
Deeper (Older) cells
lose their nuclei
Contain: crystallins
specialized proteins