Unit 4 PLTW HBS
1/91
Earn XP
Description and Tags
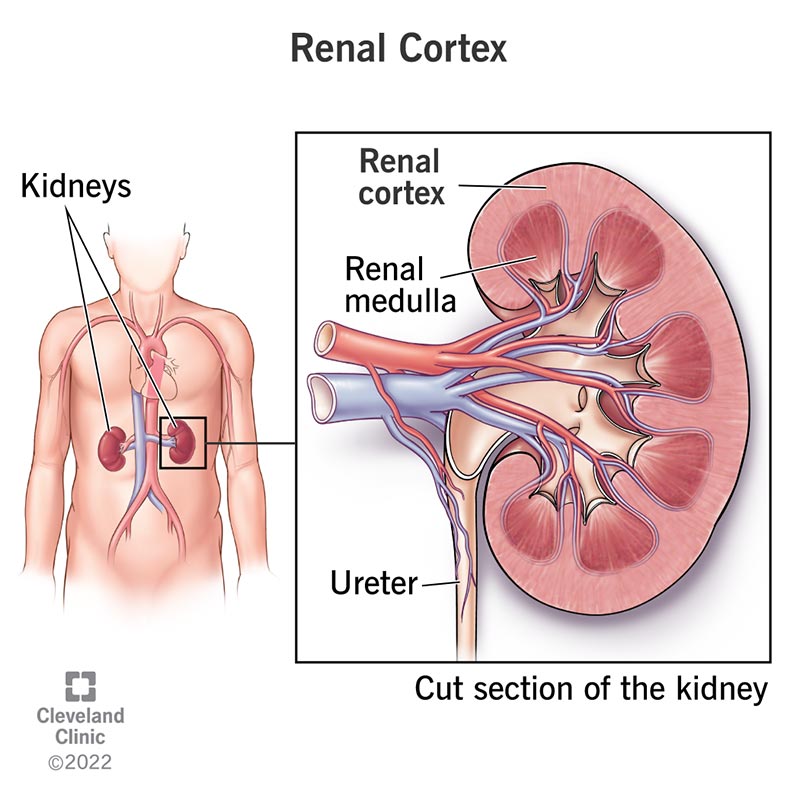
The Kidney
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
92 Terms
Function of renal artery
how the blood enters the kidney (unfiltered blood)
function of renal vein
how the blood returns to the body (filtered blood)
function of bladder
stores urine
function of kidney
filters blood, regulates fluid balance, and produces urine
function of ureter
tube that transports urine from the renal pelvis of the kidney to the bladder
function of urethra
carries urine from bladder to outside of body
function of renal pyramid
transports urine from the outer cortex to the calyxs
function of renal column
holds cortex in place, provides structural support, and seperates kidney into lobes (pyramids)
function of nephron
a tiny unit in the kidney that filters blood and makes urine through filtration, secretion, and reabsorption. (each kidney has over 1 million)
function of major calyx
collects urine from the smaller calyxs and sends it to the renal pelvis
function of renal capsule
protects the kidney from trauma and infections, maintain its structural shape, and manage internal pressure
function of renal pelvis
funnel shaped, acts as the primary collecting chamber for urine
what is the primary function of the excretory system
filters blood and gets rid of waste products as urine in the blood
what are 3 other functions of the excretory system
maintain fluid and electrolyte balance
regulate blood pressure (by maintaining sodium and water balance and releasing hormones that influence vessel contriction)
produces erythropoietin (EPO) - hormone that stimulates production of RBCs
what are 3 other roles of the excretory/urinary system
regulates water levels
balances electrolytes (chemicals)
maintains pH
describe the process of filtration and why it is important
blood is filtered in the kidney (in the glomerulus), small things like water, salts, and waste go into the nephron.
it is important because it starts urine formation and removes waste from blood
describe the process of reabsorption and why it is important
useful things (like water, glucose, and salts) are taken back into the blood
it is important because it keeps the body from losing needed nutrients and water
describe the process of secretion and why it is important
extra wastes and chemicals are added from the blood into the nephron
it is important because it helps remove toxins and balance pH and ions in the body
what are the 3 processes that occur in the nephron
filtration, reabsorption, secretion
where in the nephron does filtration occur
at the glomerulus (inside the bowmans capsule)
where in the nephron does secretion occur
proximal convulted tubule
distal convulted tubule
collecting duct
where in the nephron does reabsorption occur
proximal convulted tubule
distal convulted tubule
collecting duct
loop of Henle
what are some substances that are reabsorped in the nephron?
water
glucose
amino acids
ions (salts)
why are substances reabsorbed in the nephron
they’re reabsorbed bc your body still needs them to function. filtrations lets a lot of stuff leave the blood but reabsorption fixes that by taking back useful substances so you don’t lose them in urine
what is an algorithm
algorithms are a set of step by step instructions used for solving a problem or performing a calculation
what are some examples of algorithms
fever check
urinalysis
decision tree
what is a problem with using algorithms for medical purposes
some disadvantages are that they aren’t personalized for every patient, may become outdated, and they don’t work well for complex cases
what is the estimated glomerular filtration rate (eGFR), why is it important
eGFR is a number that shows how well the kidneys are working to filter your blood, (low numbers mean worse). They are important because it helps doctors measure kidney function and detect kidney disease early so they can treat it before it gets worse
at what point should a patient begin dialysis
if the eGFR is 15-29
at what point should a patient receive a kidney transplant
if the eGFR is lower than 15
what is a kidney transplant chain
a kidney transplant chain is a system where donors give kidneys to different people so everyone can get a match
how does a kidney transplant chain work
if you’re not a match for the person you want to help, you give your kidney to someone else, and another person gives to them. this creates a chain
what are the two factors doctors look at to determine if a donor kidney is a good match for a recipient
if the donor and recipient are a match for their blood type (compatible)
their HLA markers match closely
what should normal urine NOT contain
glucose, protein, blood
what is a urine analysis
a macroscopic, chemical, and microscopic analysis of urine
what are some conditions a urine analysis can diagnose
it can diagnose UTI, kidney dsease or kidney malfunction, diabetes, liver disease, kidney stones
what are some things that are specifically tested for in a urinalysis
glucose
protein
ketones
blood (RBCs)
WBC
pH
specific gravity
bacteria
what is the difference between macroscopic examination, chemical analysis, and microscopic examination of urine
macro:
looking at urine with the naked eye (color, clarity, odor)
chemical:
testing urine with dipsitcks/strips (glucose, protein, pH, ketones)
micro:
looking at urine under a microscope (cells, bacteria, crystals)
what are the main components of urine, in a healthy individual
water (abt 95%)
urea (waste from protein breakdown)
electrolytes (sodium, potassium)
creatinine (waste from muscle activity)
uric acid
what are electrolytes
minerals that when they dissolve in blood, take on a negative or positive charge
what are the 7 electrolytes needed for life
sodium
potassium
magnesium
calcium
chloride
bicarbonate
phosphate
describe substances that are needed in the body
substances that are needed by the body are returned to the capillaries, while wastes stay in the nephron until they make it to the ureter
how does the kidney maintain homeostasis regarding water
the kidneys maintain water balance by controlling how much water is reabsorbed
more water needed —> reabsorb more —> concentrated urine
less water needed —> reabsorb less —> diluted urine
what is PKD
PKD is a genetic disease where cysts grow in the kidneys and damage them
what are the symptoms of PKD
high blood pressure
pain
blood in urine
enlarged kidnets
what is the cause of PKD
passed down from parents (genetic mutation)
what is the treatment of PKD
no cure, you can manage symptoms, severe cases need dialysis or transplant
what is the typical prognosis for PKD
gets worse over time and can lead to kidney failure
prognosis definition
a prediction of how a disease or condition will progress and the likely outcome
what is the difference between a healthy kidney and a PKD kidney
a PKD kidney has cysts on it and the kidney is larger which affects the function of it negatively. a healthy kidney does not have this
how are restriction enzymes used in the lab to help diagnose PKD
they cut DNA at specific sites so scientists can analyze fragment patterns and detect PKD mutations
how are polymerase chain reactions used in the lab to help diagnose PKD
makes many copies (amplify) of target DNA so it can be tested for mutations linked to PKD
how is gel electrophoresis used in the lab to help diagnose PKD
seperates DNA fragments by size so scientists can compare band patterns and identify mutations linked to PKD
does blood flow in or out of the artery/vein in the kidney
artery: blood flows in
vein: blood flows out
where are the nephrons found in the kidney
renal medulla and renal cortex
who should begin dialysis and who indicates that they need an evaluation for a kidney transplant
patient equation 1 equation 2 equation 3 equation 4 equation 5
sophia 21 21 18.4 23 19
koa 69 68 64 53 59
maxwell 18 16 13 18 14
ella 132 118 96 122 130
sophia should begin dialysis
maxwell needs to evaluate for a kidney transplant
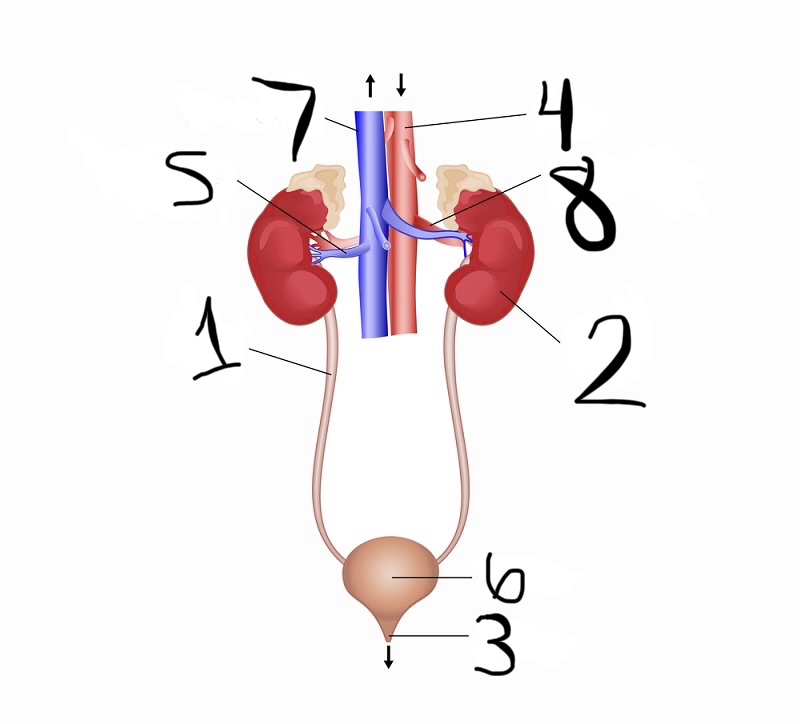
what is 1
ureter
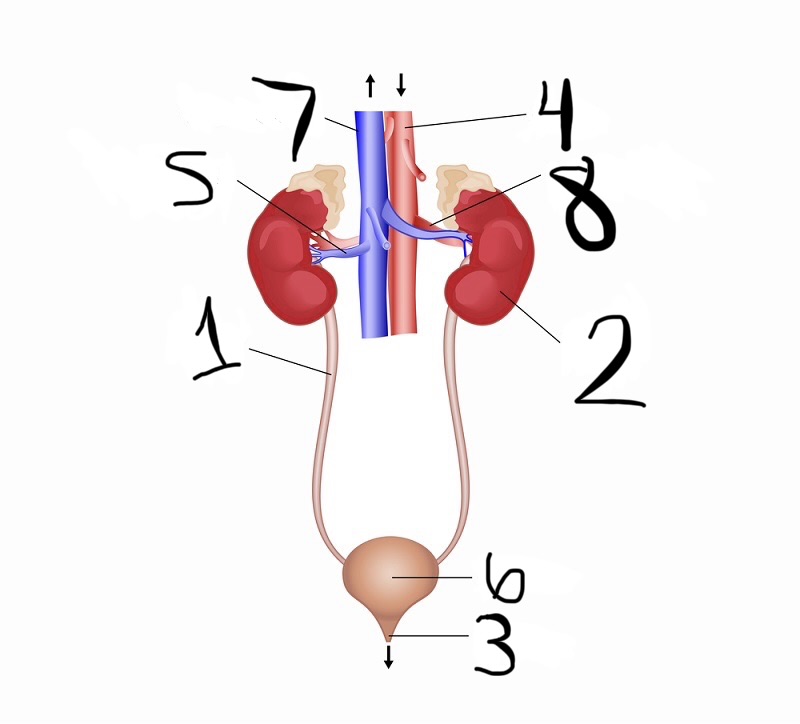
what is 2
kidney
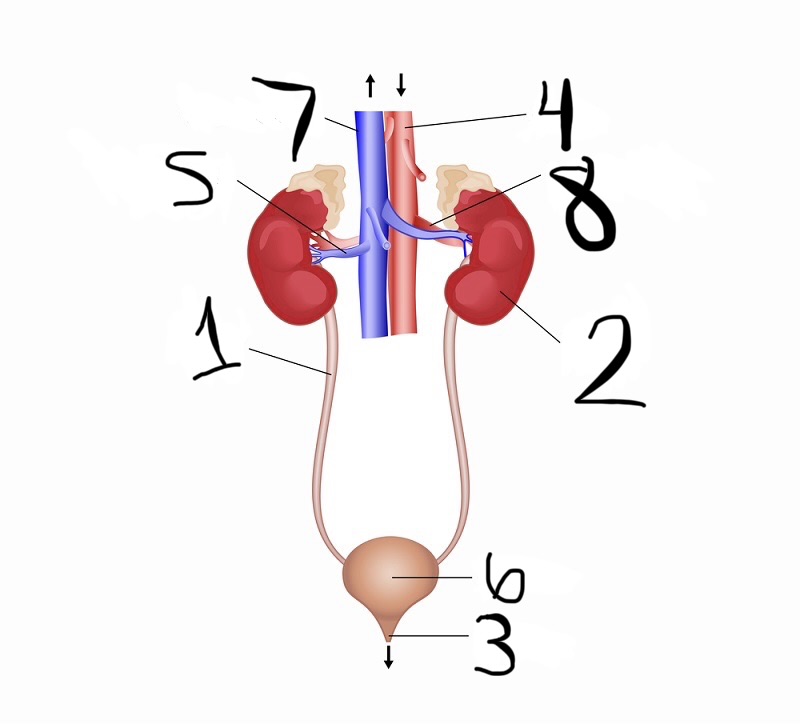
what is 3
urethra
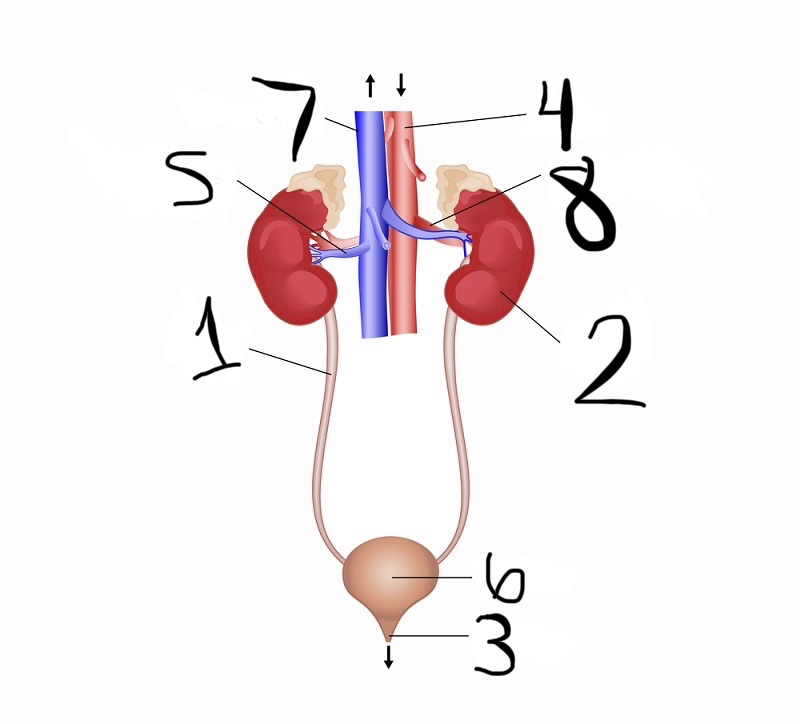
what is 4
aorta
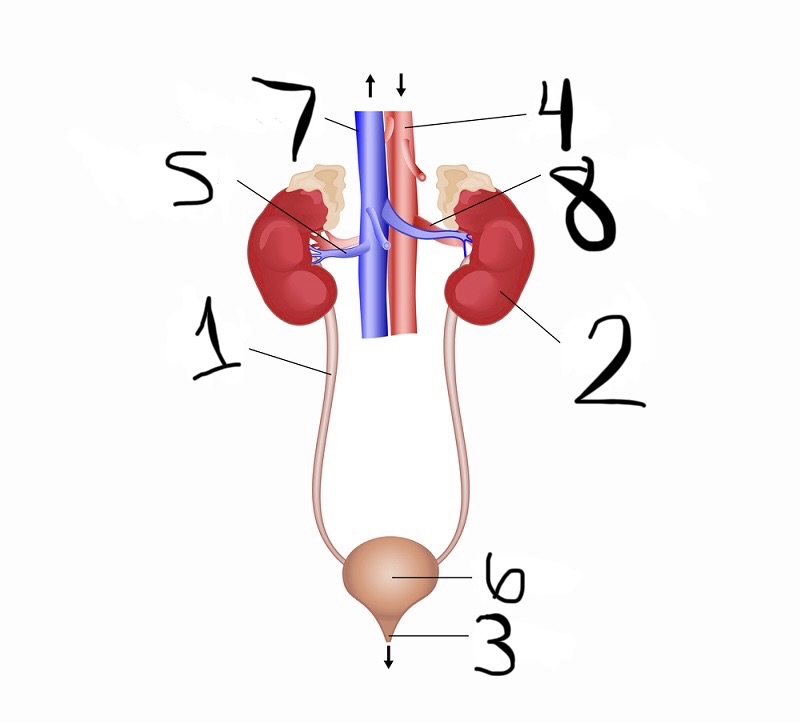
what is 5
renal vein
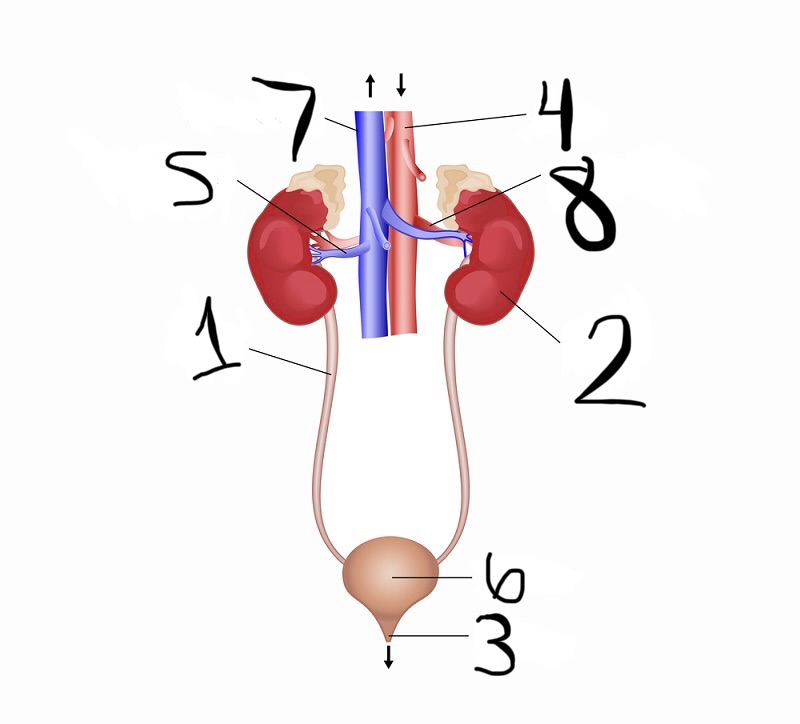
what is 6
bladder
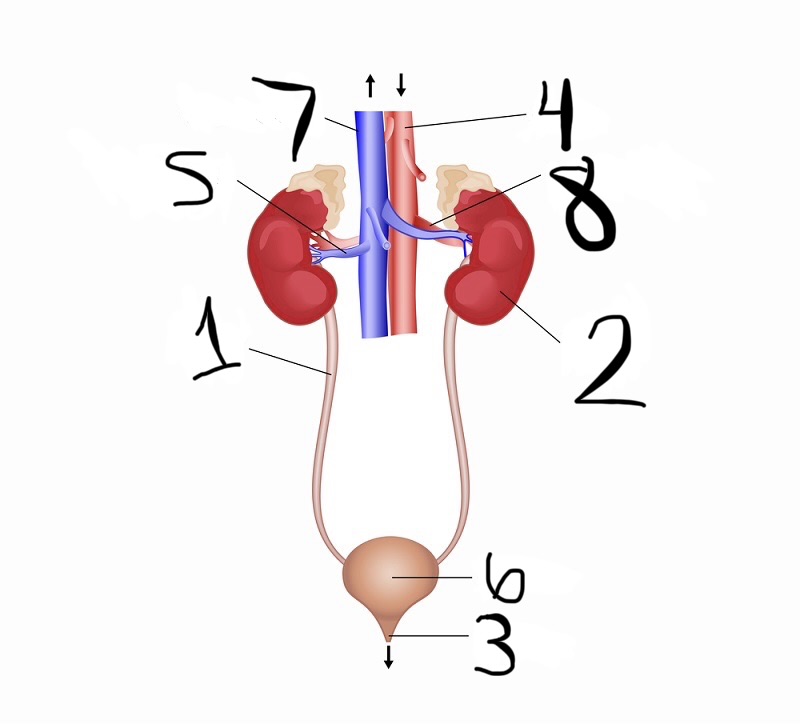
what is 7
vena cava
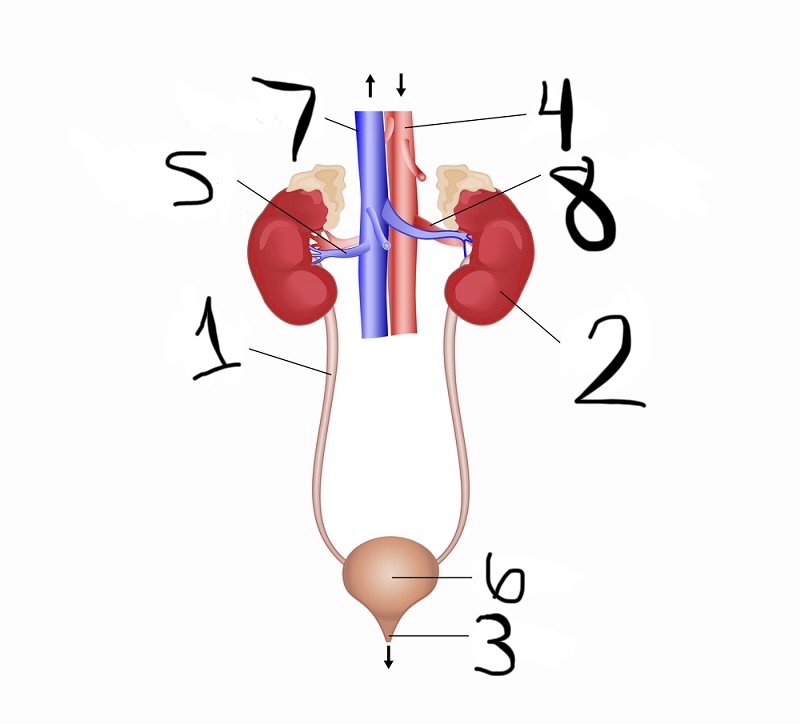
what is 8
renal artery
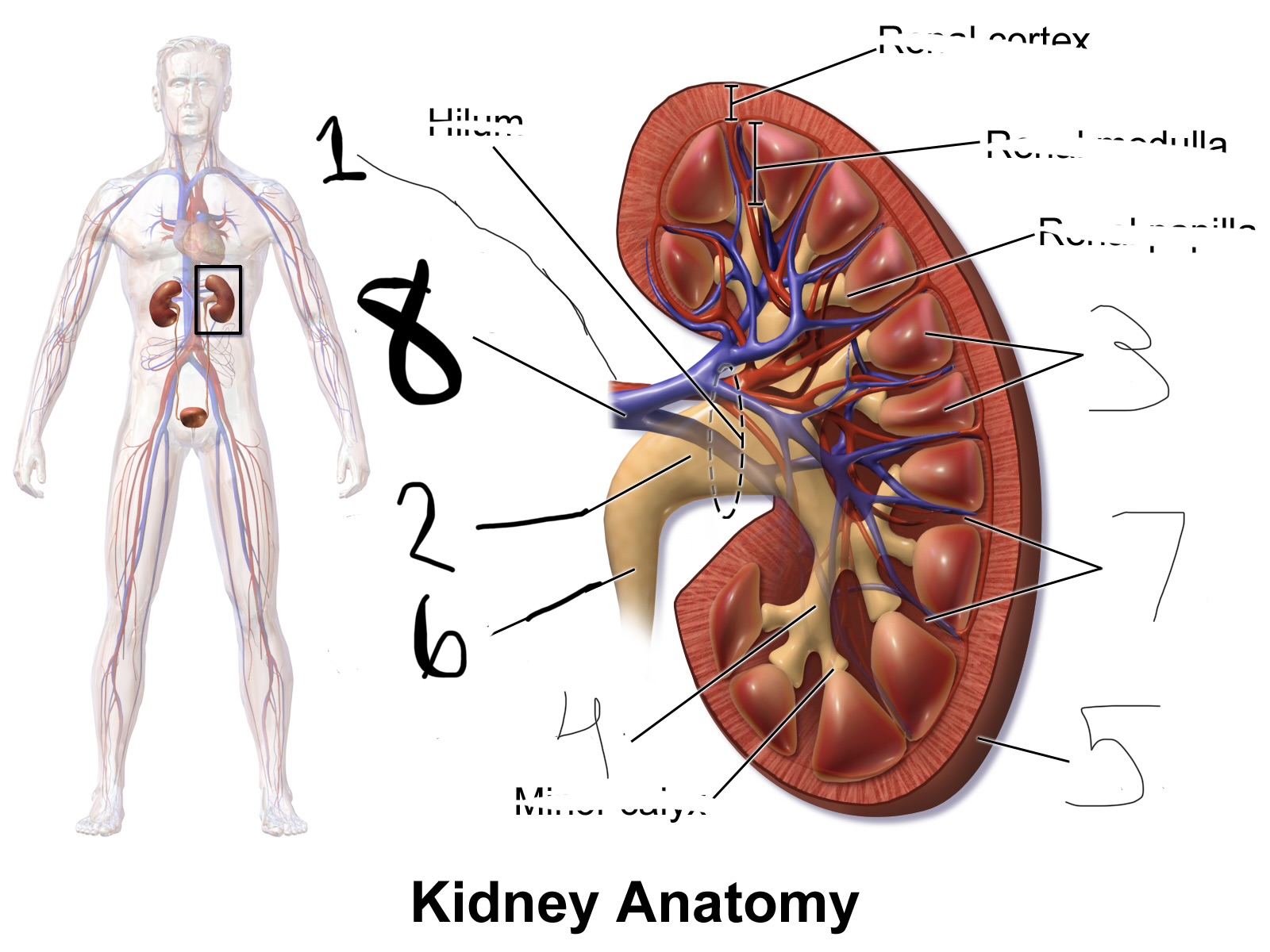
what is 1
renal artery
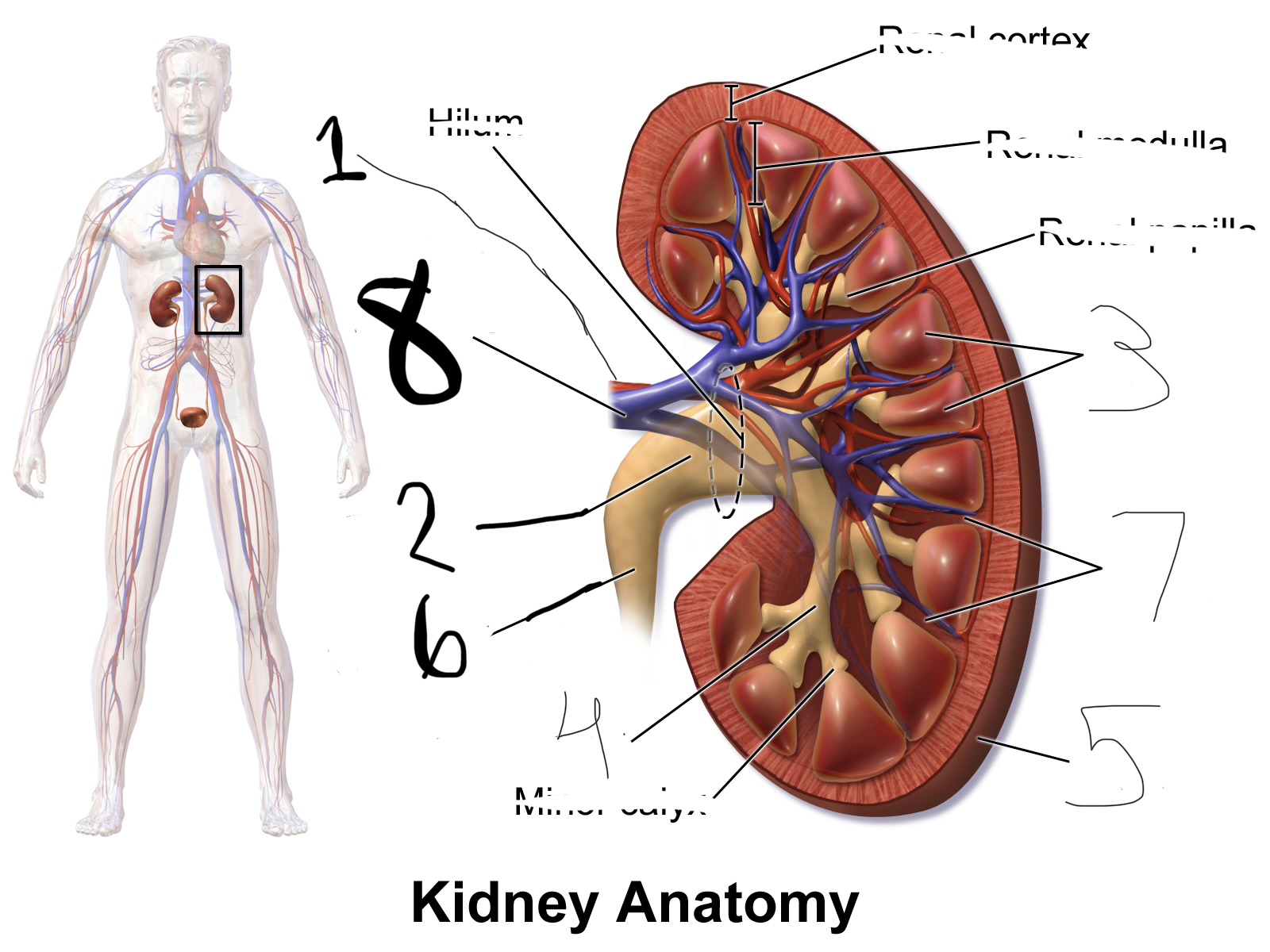
what is 2
renal pelvis
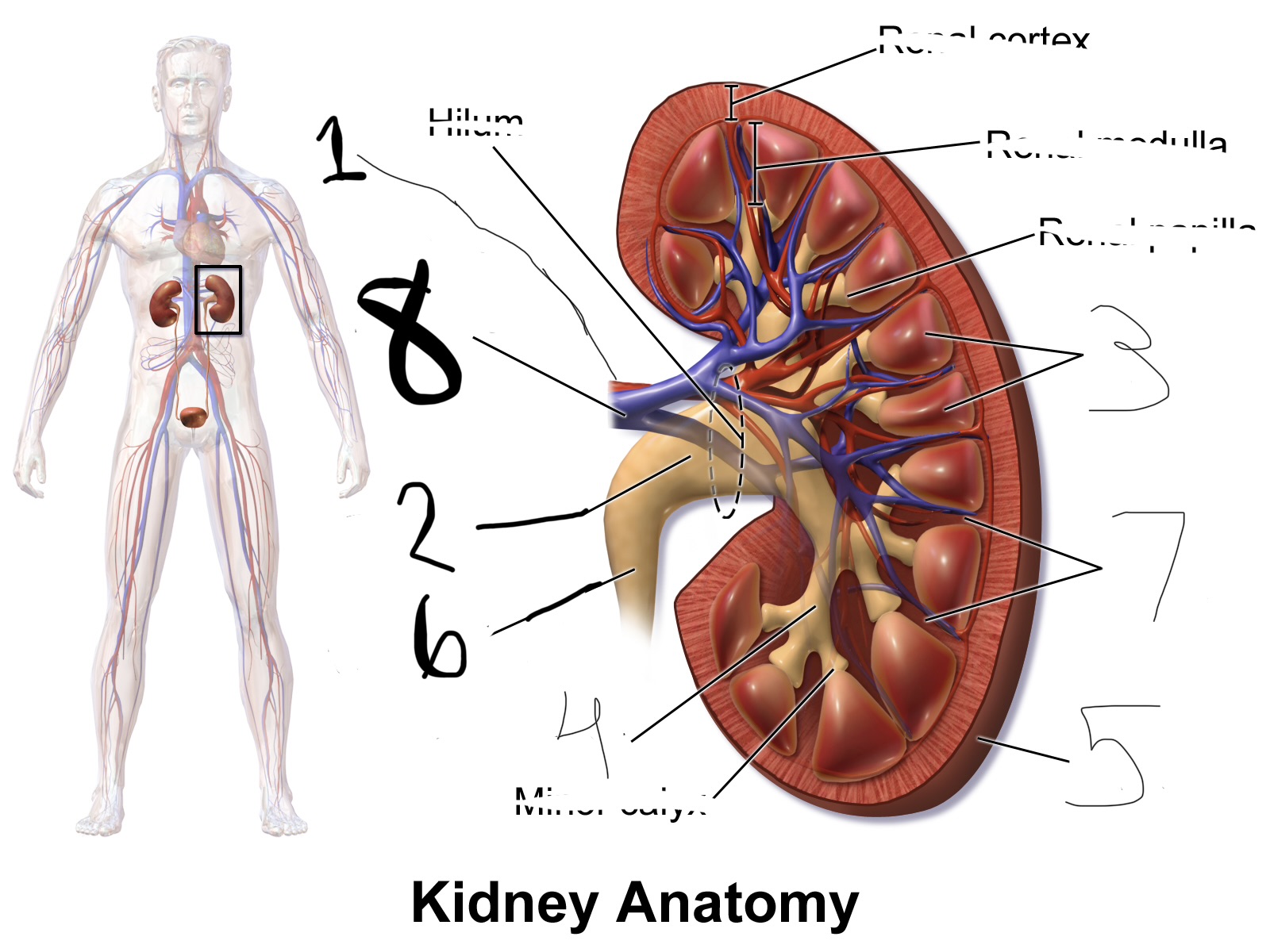
what is 3
renal pyramid
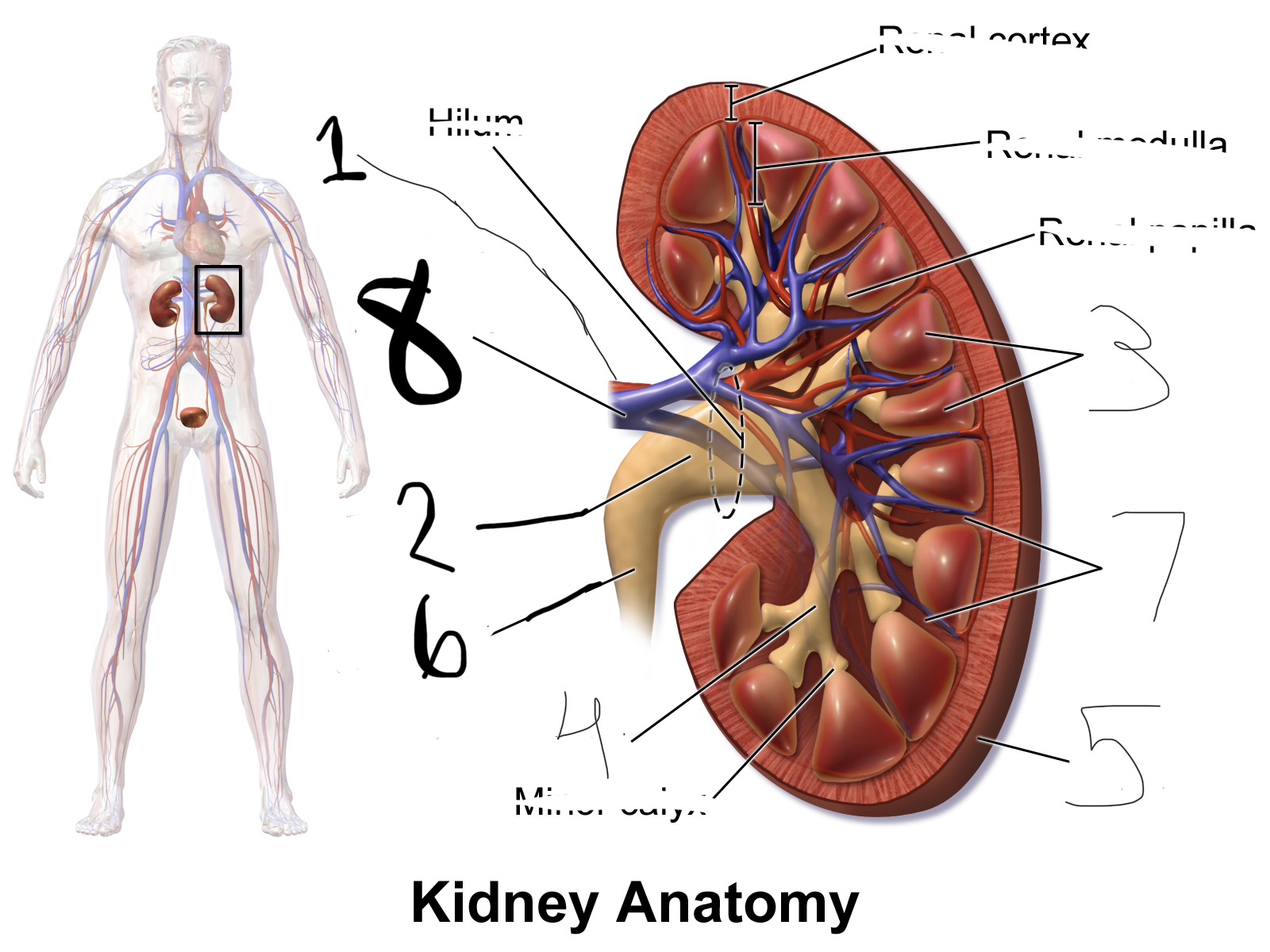
what is 4
major calyx
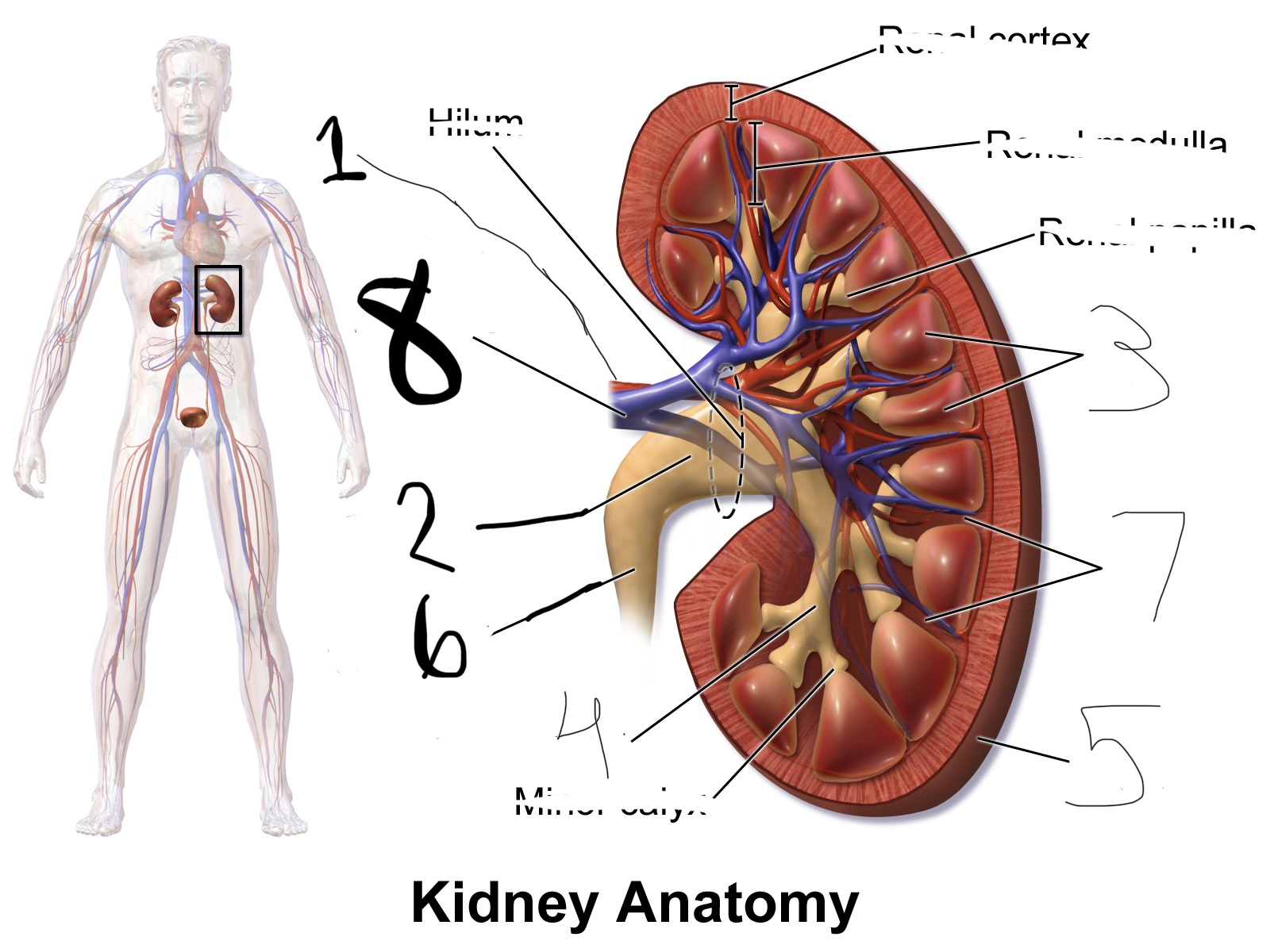
what is 5
renal capsule
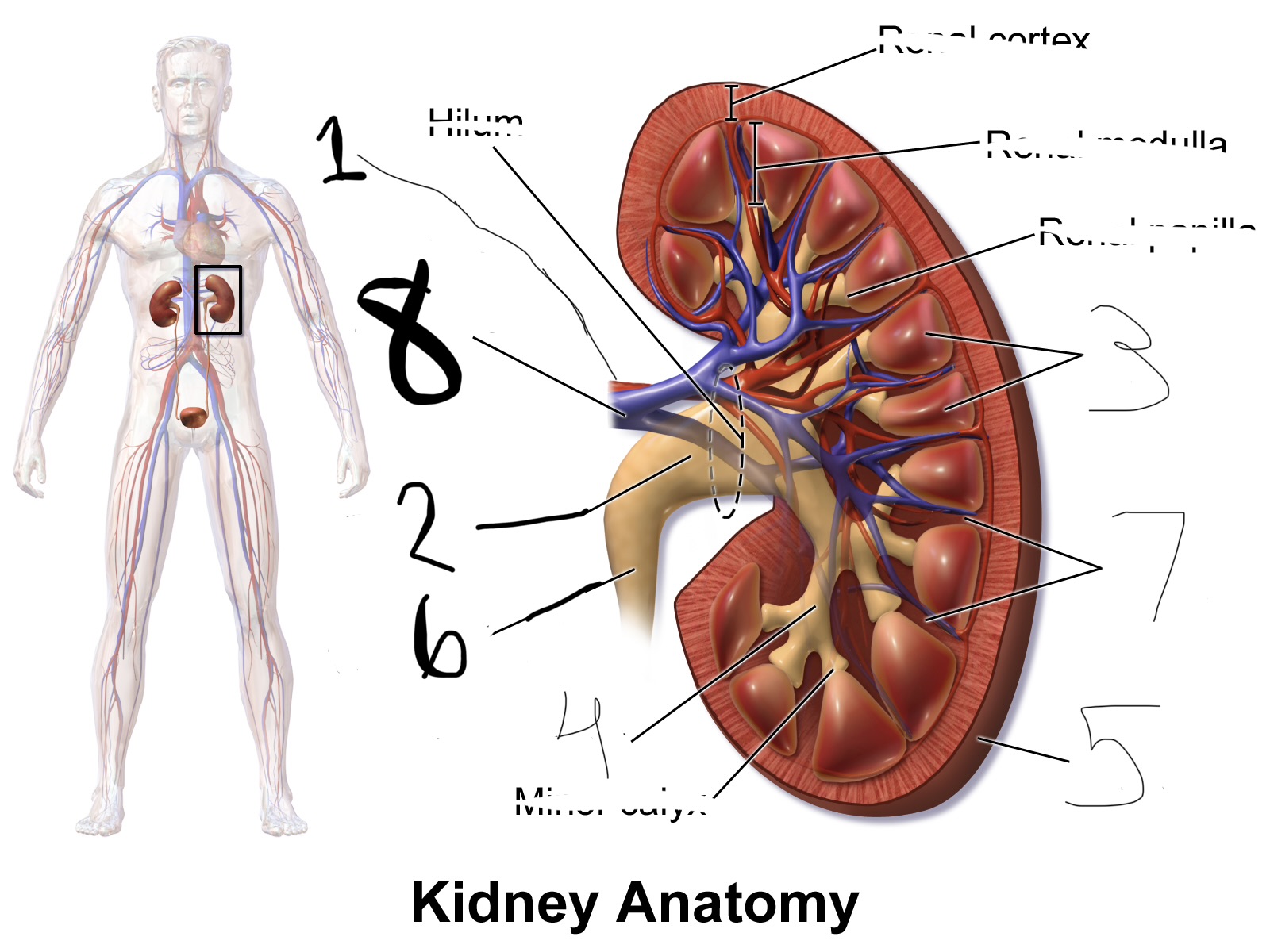
what is 6
ureter
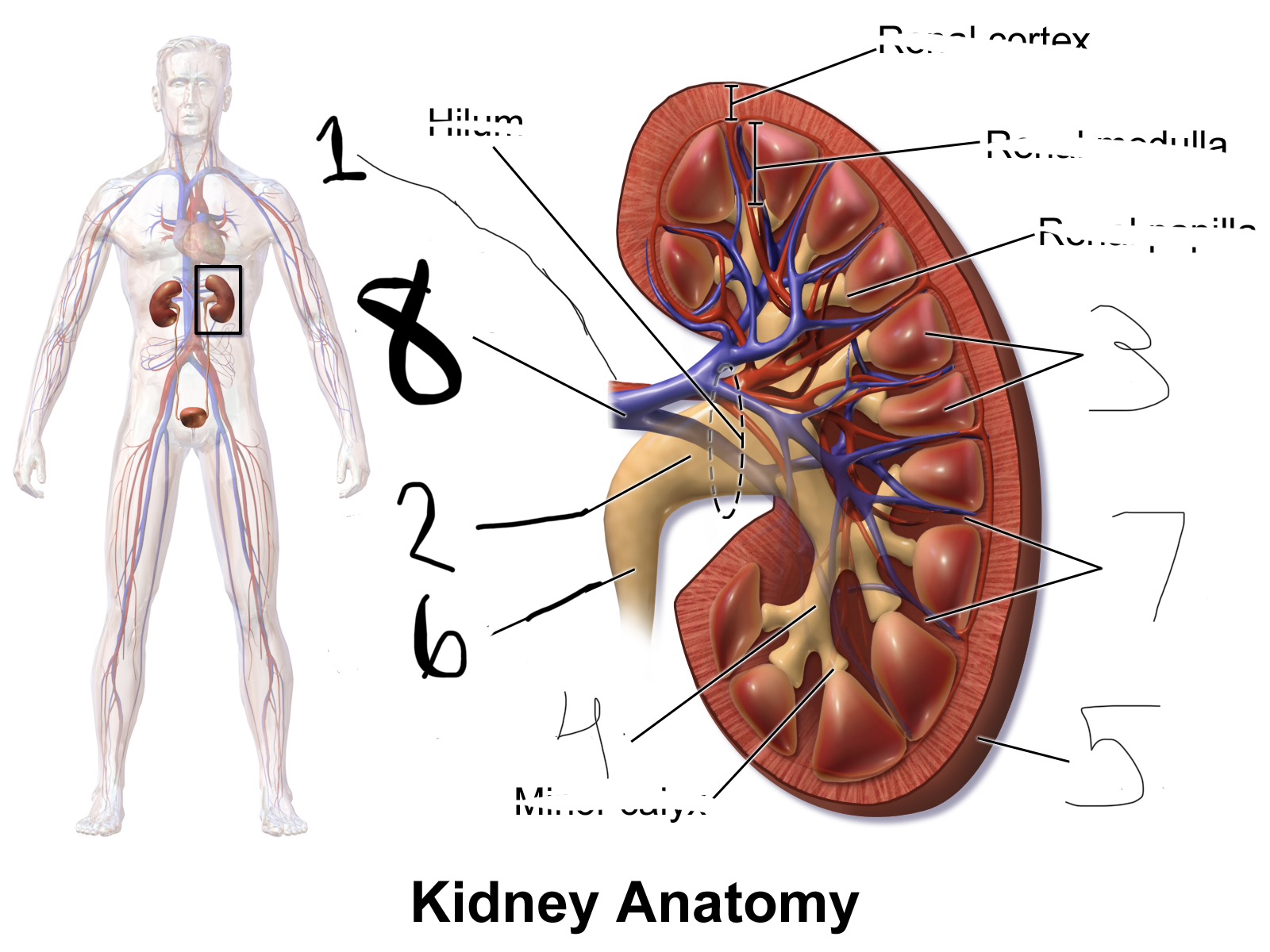
what is 7
renal column
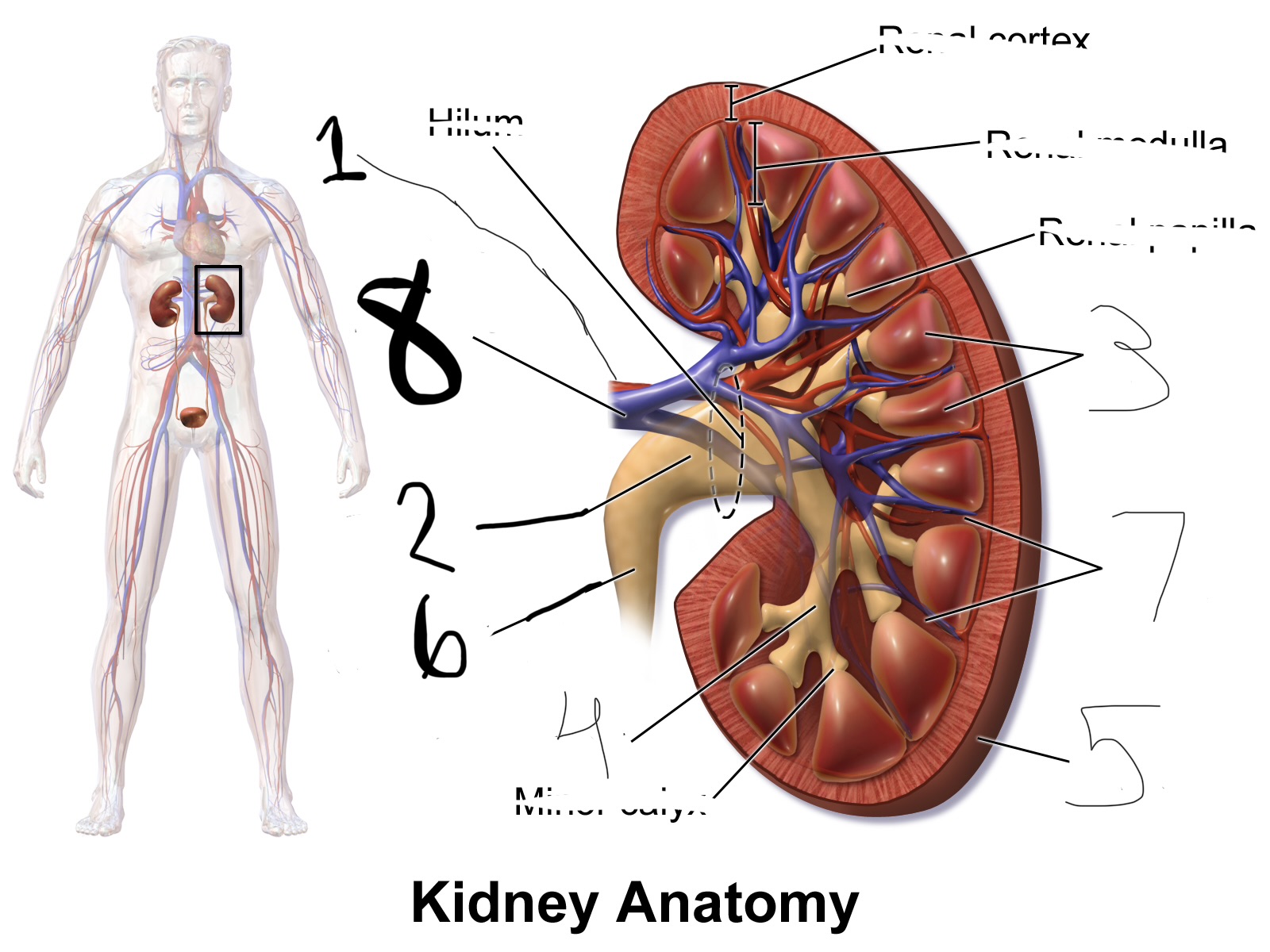
what is 8
renal vein
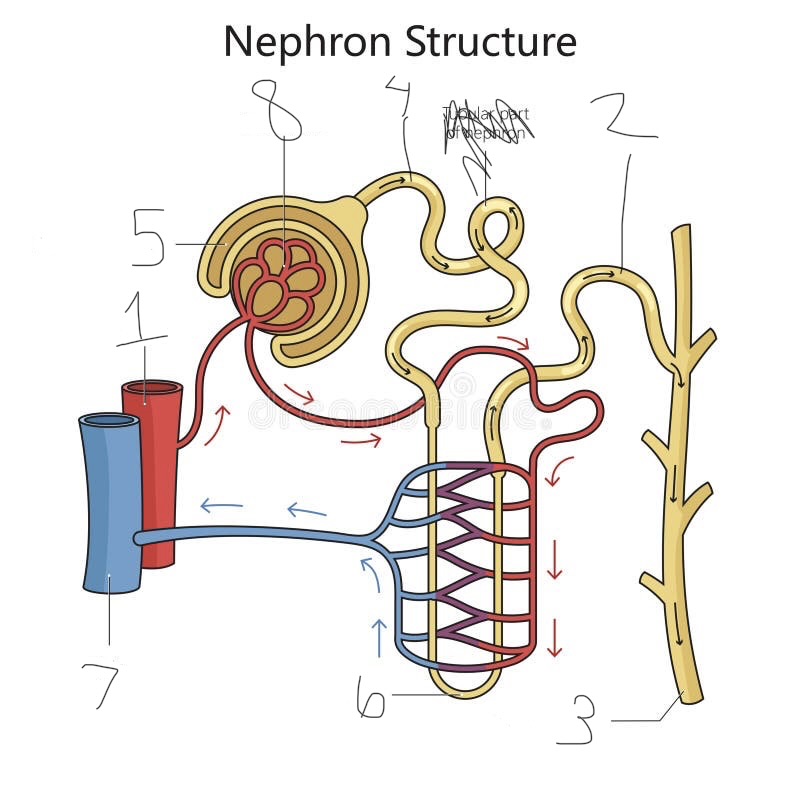
what is 1
renal artery
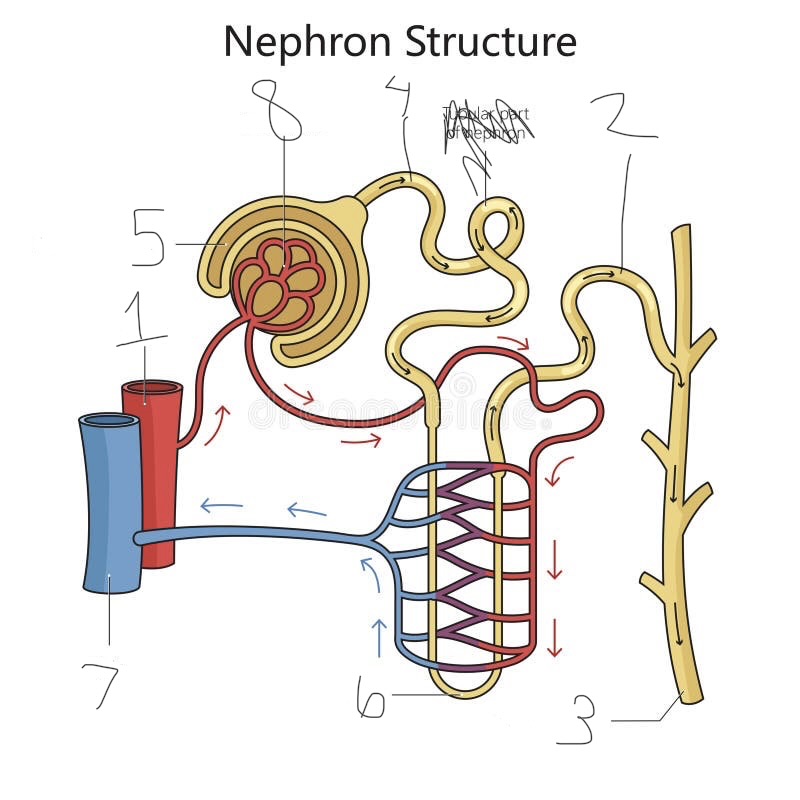
what is 2
distal convoluted tubule
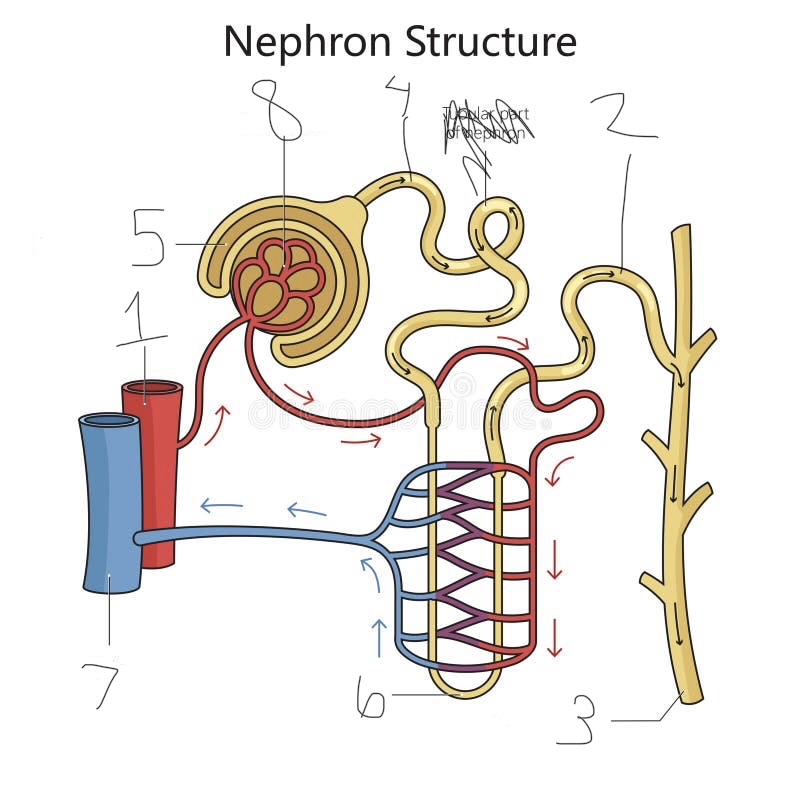
what is 3
collecting duct
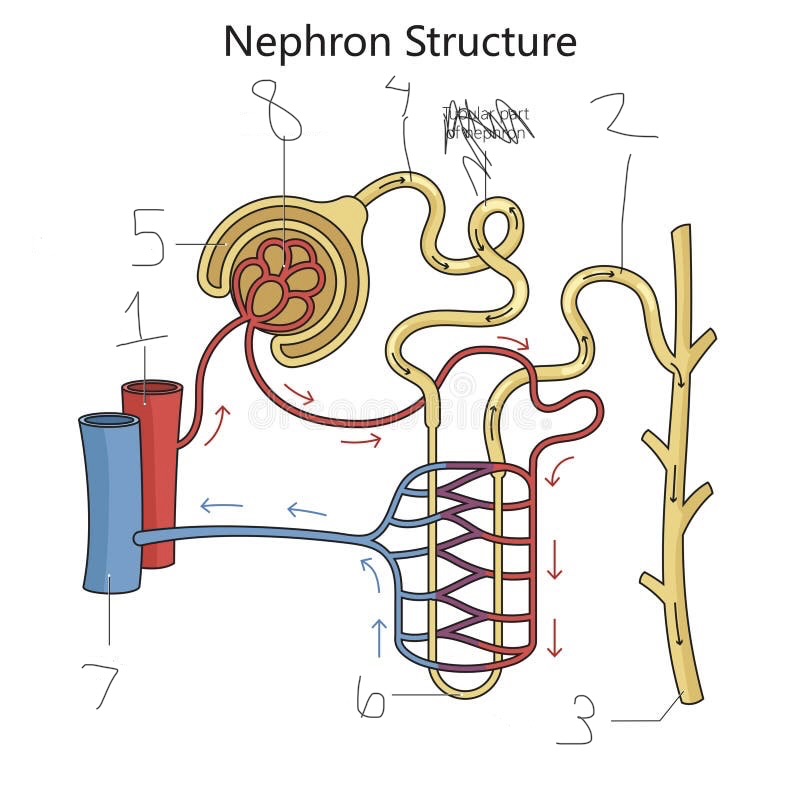
what is 4
proximal convoluted tubule
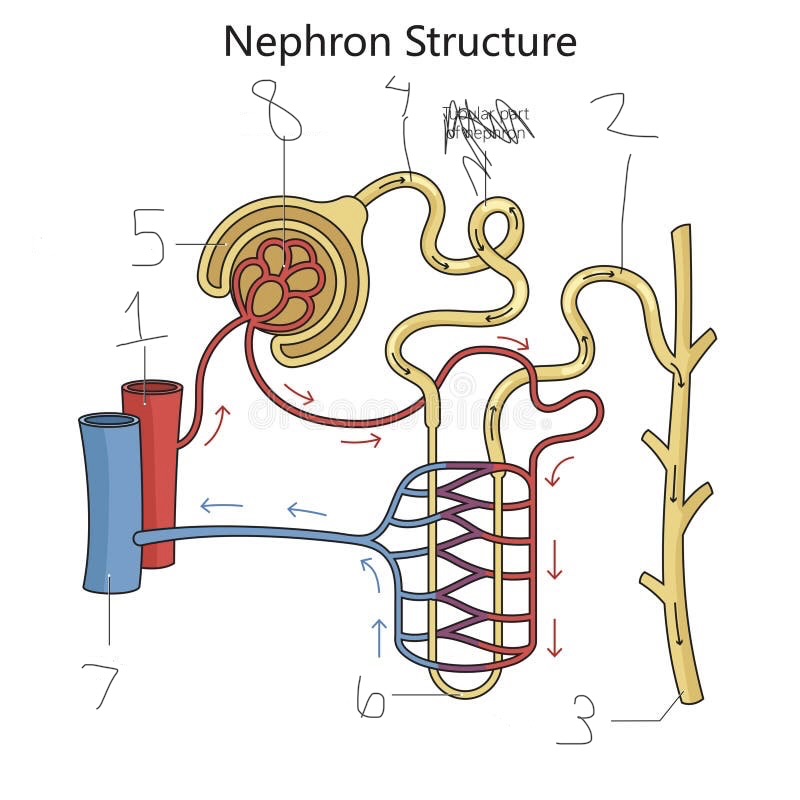
what is 5
Bowman’s capsule
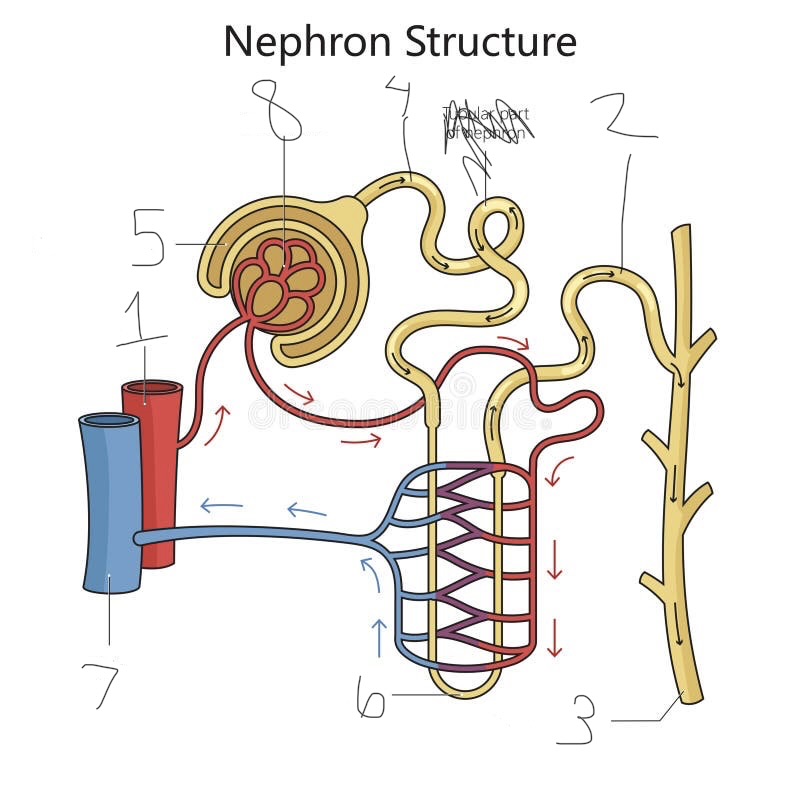
what is 6
loop of Henle
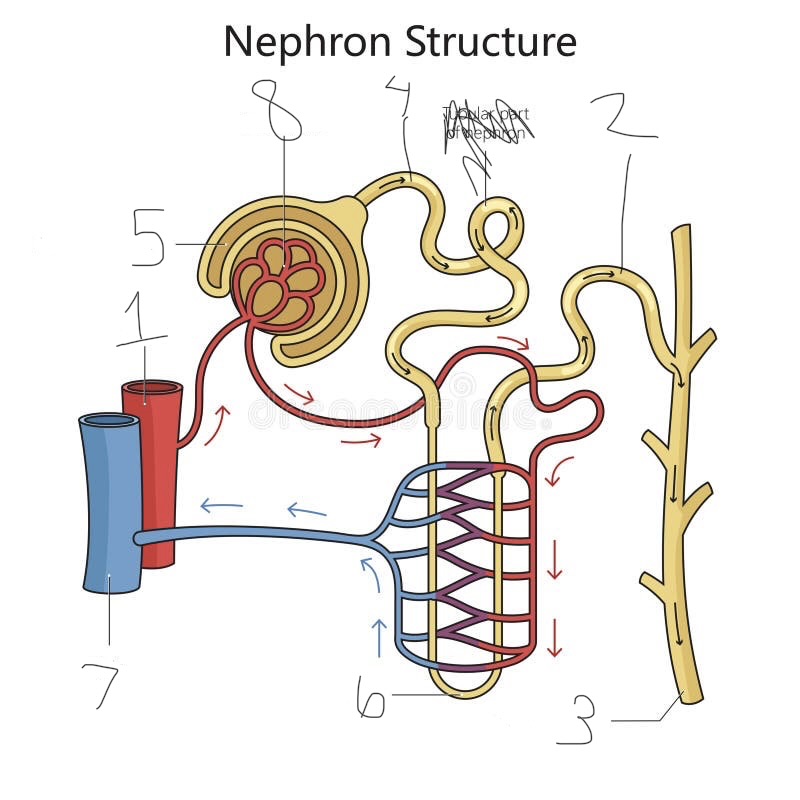
what is 7
renal vein
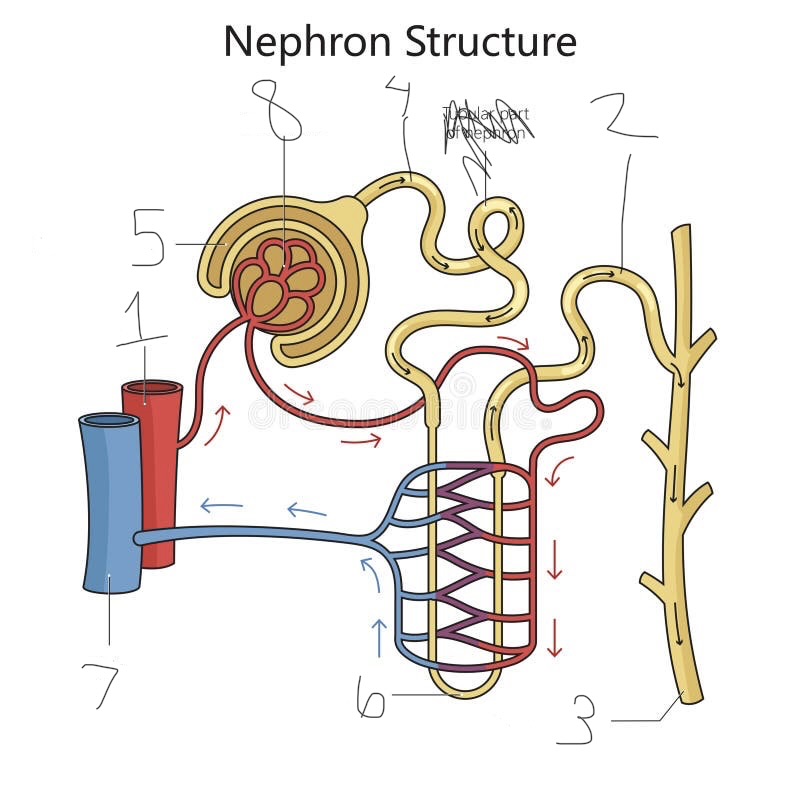
what is 8
Glomerulus
what does the proximal convoluted tubule do in the nephron
reabsorbs most water, glucose, and nutrients back into the blood, also does some secretion
what does the distal convoluted tubule do in the nephron
reabsorbs sodium and chloride
secretes ions to maintain blood pH and electrolyte balance
what does the Loop of Henle do in the nephron
helps concentrate urine by reabsorbing water and salts
what do the capillaries do in the nephron
allow exchange of substances between blood and nephron (reabsorption of materials)
what does the collecting duct do in the nephron
reabsorbs water and salts, secretes excess ions and wastes
what does the bowman’s capsule do in the nephron
surrounds the glomerulus and participates in filtering small solutes from the blood
what does the glomerulus do in the nephron
filters small solutes from the blood
why do we need to look at blood flow through the kidneys
the kidneys clean the blood so understanding blood flow helps explain how waste is removed and the body stays balanced
which structure is where urine is formed
nephron
which renal structure collects urine
collecting duct
dialysis tubing
a semipermeable membrane that allows only certain substances to pass through its pores
diagnosis of Alexis (patient from 4.1.5)
UTI