Neurologic Dysfunction
1/20
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
21 Terms
Altered level of Consciousness (LOC): Causes, presentation
Level of responsiveness and consciousness is the most important indicator of the patient’s condition → based on patients baseline
LOC is a continuum from normal alertness and full cognition (consciousness) to coma
Altered LOC is not the disorder but the result of a pathology
Causes: neuro (head injury, stroke), toxic (drugs, ETOH), or metabolic (hepatic/kidney injury, DKA)
Coma: unconsciousness, unarousable unresponsiveness
Akinetic mutism: unresponsiveness to the environment, makes no movement or sound but sometimes opens eyes
Persistent vegetative state: devoid of cognitive function but has sleep–wake cycles
Locked-in syndrome: inability to move or respond except for eye movements due to a lesion affecting the pons
What are the components that are assessed with Altered Level of Consciousness?
Eye opening/response
Verbal response
Motor response (posturing)
Alertness
Respiratory status
Symmetry
Reflexes
Becomes restless, anxious initially if decreased state of consciousness
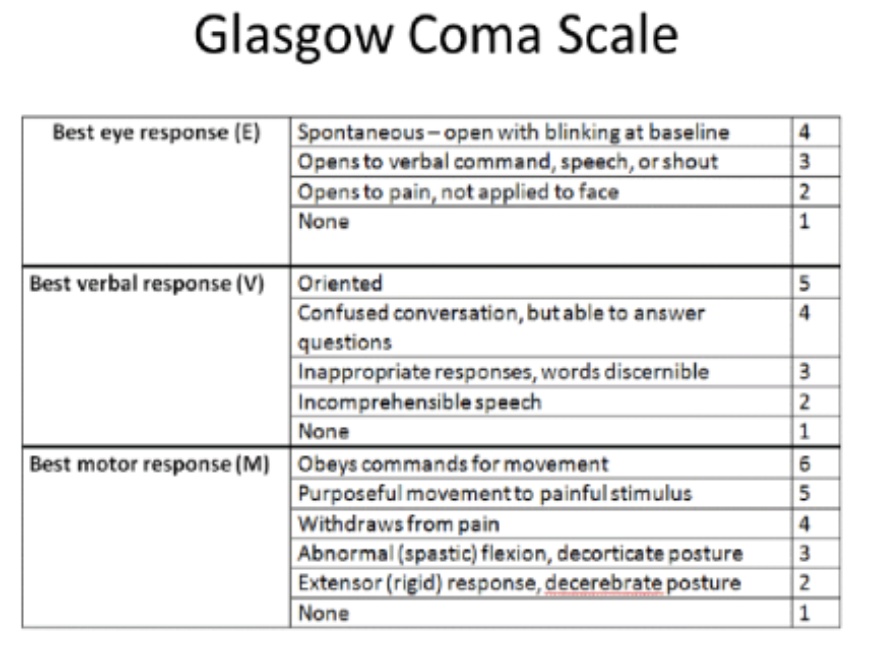
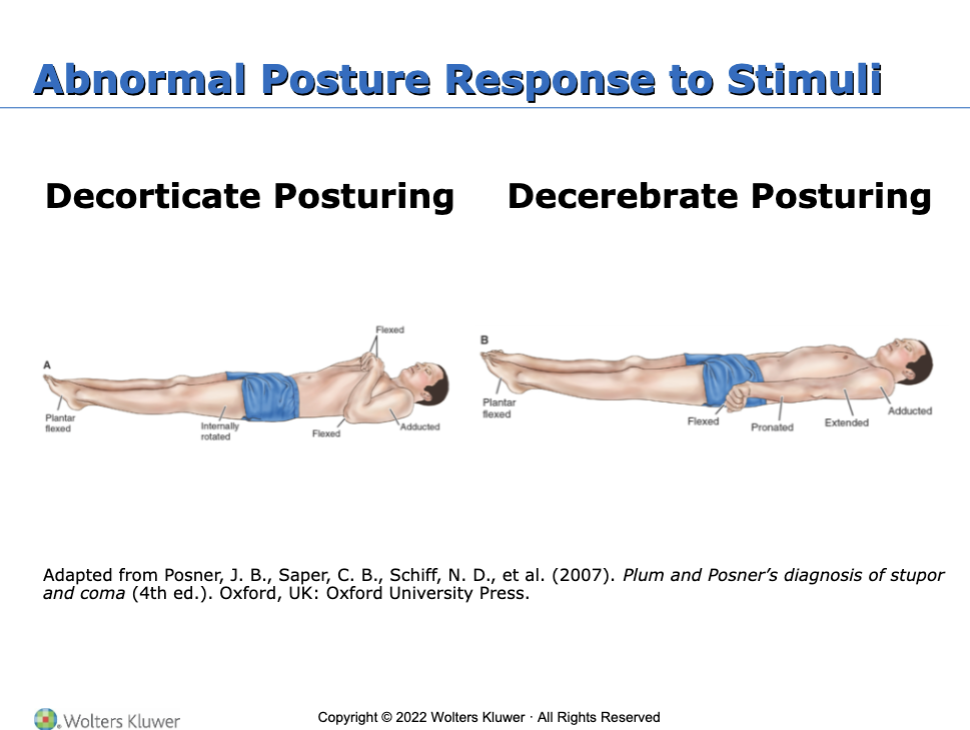
What are the two abnormal posture response to stimuli?
Planning and Goals for the patient with Altered Level of Consciousness
Goals may include:
Maintenance of clear airway
Protection from injury
Attainment of fluid volume balance
Maintenance of skin integrity
Absence of corneal irritation
Effective thermoregulation
Accute perception of environmental stimuli
Maintenance of intact family or support system
Absence of complications
What are the cerebral response to intercranial pressure (ICP)?
Cerebral perfusion pressure (CPP) is closely linked to ICP
CPP = MAP – ICP
Normal CCP is 70 to 100
A CCP of less than < 50 results in permanent neurologic damage
Increased Intracranial Pressure
Monro–Kellie hypothesis: because of limited space in the skull, an increase in any one of components of the skull (brain tissue, blood, CSF) will cause a change in the volume of the others
Compensation to maintain a normal ICP of 10 to 20 mm Hg is normally accomplished by shifting or displacing CSF
With disease or injury, ICP may increase
Increased ICP decreases cerebral perfusion and causes ischemia, cell death, and (further) edema
Brain tissues may shift through the dura and result in herniation
Autoregulation: refers to the brain’s ability to change the diameter of blood vessels to maintain cerebral blood flow
CO2 is decreased → vasoconstriction
CO2 is increased → vasodilatation
What are the early manifestations of increased ICP?
Changes in LOC
Any change in condition
Restlessness, confusion, increasing drowsiness, increased respiratory effort, purposeless movements
Pupillary changes and impaired ocular movements
Weakness in one extremity or one side
Headache: constant, increasing in intensity, or aggravated by movement or straining

What are the late manifestations of increased ICP?
Respiratory and vasomotor changes
VS: Increase in systolic blood pressure, widening of pulse pressure, and slowing of the heart rate; pulse may fluctuate apidly from tachycardia to bradycardia; temperature increase
Cushing triad: bradypnea, bradycardia, hypertension
Projectile vomiting
Further deterioration of LOC: stupor to coma
Hemiplegia, decortication, decerebration, or flaccidity
Respiratory pattern alterations including Cheyne–Stokes breathing and arrest
Loss of brainstem reflexes: pupil, gag, corneal, and swallowing

What is assessment of patient with increased intracranial pressure?
Obtain history of events leading to illness
Evaluate mental status, LOC
Assessment of selected cranial nerves
Assess cerebellar function, reflexes, motor and sensory function
Glasgow Coma Scale, pupil checks
Frequent vital signs
Assessment of intracranial pressure
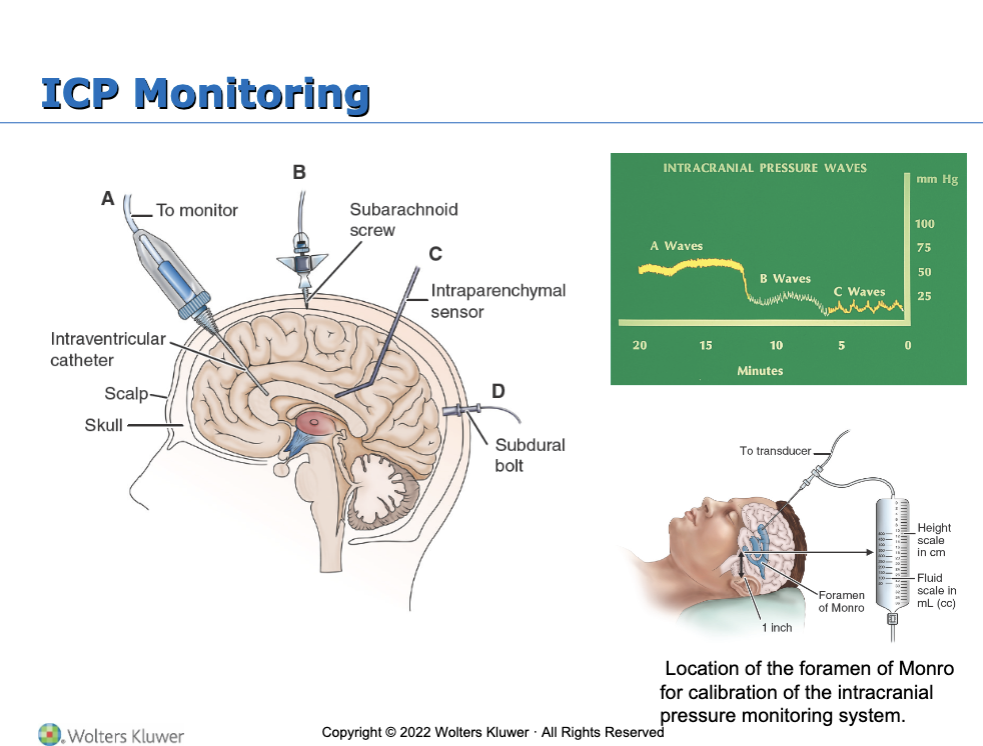
What are the nursing interventions for the patient with increased ICP?
Frequent monitoring of respiratory status and lung sounds and measures to maintain a patent airway
Position with head in neutral position and elevation of HOB 30 to 45 degrees to promote venous drainage unless contraindicated
Avoid hip flexion, Valsalva maneuver, abdominal distention, or other stimuli that may increase ICP
Maintain a calm, quiet atmosphere and protect patient from stress
Monitor fluid status carefully; every hour I&O during acute phase
Use strict aseptic technique for management of ICP monitoring system
Types of intracranial surgery
CraniOtomy: Opening of the skull
Purposes: remove tumor, relieve elevated ICP, evacuate a blood clot, control hemorrhage
Refer to Table 61-3
CraniECtomy: excision of portion of skill
Cranioplasty: repair of cranial defect using a plastic or metal plate
Burr holes: circular openings for exploration or diagnosis to provide access to ventricles or for shunting procedures, aspirate a hematoma or abscess, or make a bone flap
What is the preoperative care: medical management with intracranial surgery?
Preoperative diagnostic tests: CT scan, MRI, angiography, or transcranial Doppler flow studies
Medications are usually given to reduce risk of seizures
Corticosteroids, fluid restriction, hyperosmotic agent (mannitol), and diuretics may be used to reduce cerebral edema
Mannitol is used to decrease ICP(diuretic)
Antibiotics may be given to reduce potential infection
Diazepam may be used to alleviate anxiety
What is the postoperative care for intracranial surgery?
Postoperative care is aimed at
Detecting and reducing cerebral edema
Relieving pain
Preventing seizures
Monitoring ICP and neurologic status
The patient may be intubated and have arterial and central venous lines
What is the assessment of the pqtient undergoing intracranial surgery?
Careful, frequent monitoring of respiratory function, including ABGs
Monitor VS and LOC frequently; note any potential signs of increasing ICP
Assess dressing and for evidence of bleeding or CSF drainage
Monitor for potential seizures
Time seizure to know how long it lasted and possible damage
If seizures occur, carefully record and report
Monitor for signs and symptoms of complications
Monitor fluid status and laboratory data
What are the nursing interventions done for patients undergoing intracranial surgery?
Maintaining cerebral perfusion
Monitor respiratory status; even slight hypoxia or hypercapnia can affect cerebral perfusion
Assess VS and neurologic status every 15 minutes to every hour
Strategies to reduce cerebral edema; cerebral edema peaks 24 to 36 hours
Strategies to control factors that increase ICP
Avoid extreme head rotation
HOB may be flat or elevated 30 degrees according to needs related to the surgery and surgeon preference
Regulating temperature
Cover patient appropriately
Treat high temperature elevations vigorously; apply ice bags, use hypothermia blanket, administer prescribed acetaminophen
Improving gas exchange
Turn and reposition every 2 hours
Encourage deep breathing and incentive spirometry
Suction or encourage coughing cautiously as needed (suctioning and coughing increases ICP)
Humidification of oxygen may help loosen secretions
Sensory deprivation
Periorbital edema may impair vision, announce presence to avoid startling the patient; cool compresses over eyes and elevation of HOB may be used to reduce edema if not contraindicated
Enhancing self-image
Encourage verbalization
Encourage social interaction and social support
Attention to grooming
Cover head with turban and, later, a wig
Monitor I&O, weight, blood glucose, serum and urine electrolyte levels, and osmolality and urine specific gravity
Preventing infections
Assess incision for signs of hematoma or infection
Assess for potential CSF leak
Instruct patient to avoid coughing, sneezing, or nose blowing, which may increase the risk of CSF leakage
Use strict aseptic technique
Patient education for self-care
Seizures
Abnormal episodes of motor, sensory, autonomic, or psychic activity (or a combination of these) resulting from a sudden, abnormal, uncontrolled electrical discharge from cerebral neurons
Can be d/t light sounds or stress
Classification of seizures
Focal: originates in one hemisphere
Generalized: occur and engage bilaterally
Unknown: epilepsy spasms
“Provoked” related to acute, reversible condition
What are the specific causes of seizures?
Cerebrovascular disease
Hypoxemia
Fever (childhood)
Head injury
Hypertension
Central nervous system infections
Metabolic and toxic conditions
Brain tumor
Drug and alcohol withdrawal
Allergies
What is the plan of care for a patient experiencing a seizure?
Observation and documentation of patient signs and symptoms before, during, and after seizure
Nursing actions during seizure for patient safety and protection
After seizure care to prevent complications
Refer to Chart 61-4
Headache
Also known as cephalalgia
One of the most common physical complaints
Primary headache has no known organic cause and includes migraine, tension headache, and cluster headache
Secondary headache is a symptom with an organic cause such as a brain tumor or aneurysm
Headache may cause significant discomfort for the person and can interfere with activities and lifestyle
Assessment of headache
A detailed description of the headache is obtained
Include medication history and use
The types of headaches manifest differently in different persons and symptoms in one individual may also change over time
Although most headaches do not indicate serious disease, persistent headaches require investigation
Persons undergoing a headache evaluation require a detailed history and physical assessment with neurologic exam to rule out various physical and psychological causes
Diagnostic testing may be used to evaluate underlying cause if there are abnormalities on the neurologic exam
What is the nursing management of headache:pain and education?
Provide individualized care and treatment
Prophylactic medications may be used for recurrent migraines
Migraines and cluster headaches require abortive medications instituted as soon as possible with onset
Hydration, low stimulating environment, cold compress
Provide medications as prescribed
Provide comfort measures
Quiet, dark room
Massage
Local heat for tension