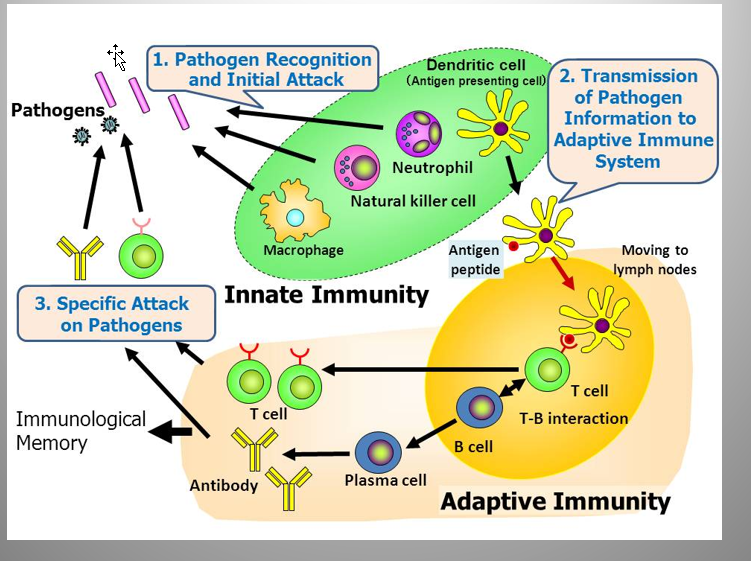
Cell-Mediated Immunity
1/15
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
What are the origins of Signal 3
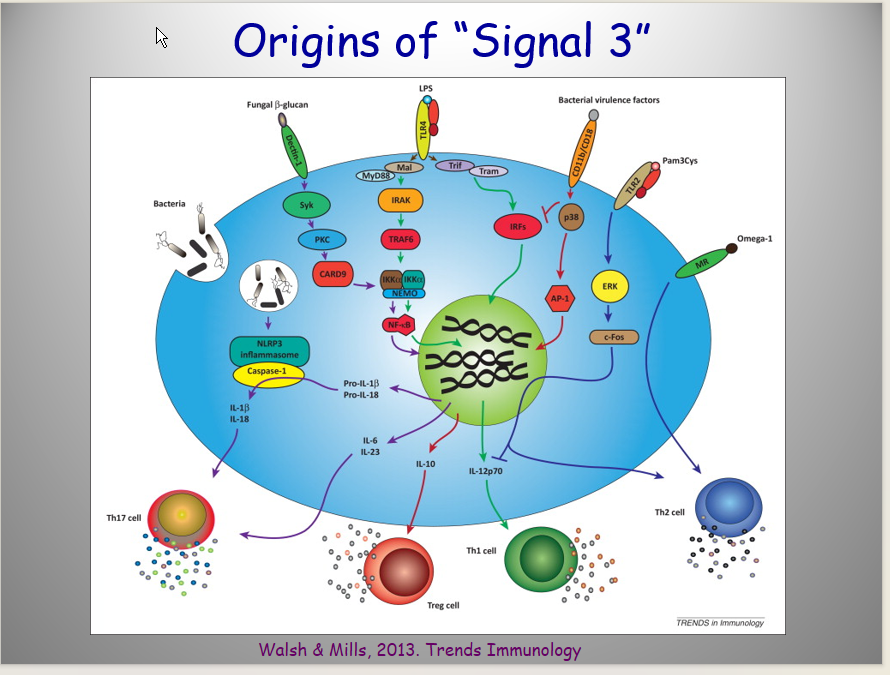
What are the factors influencing the polarization of Th cells
Factors:
Cytokine milieu determined by preceding innate immune response (signal 3).
Cytokines produced by APCs (signal 3).
The abundance of specific peptide:
The affinity of the peptide-MHC complex for the TCR.
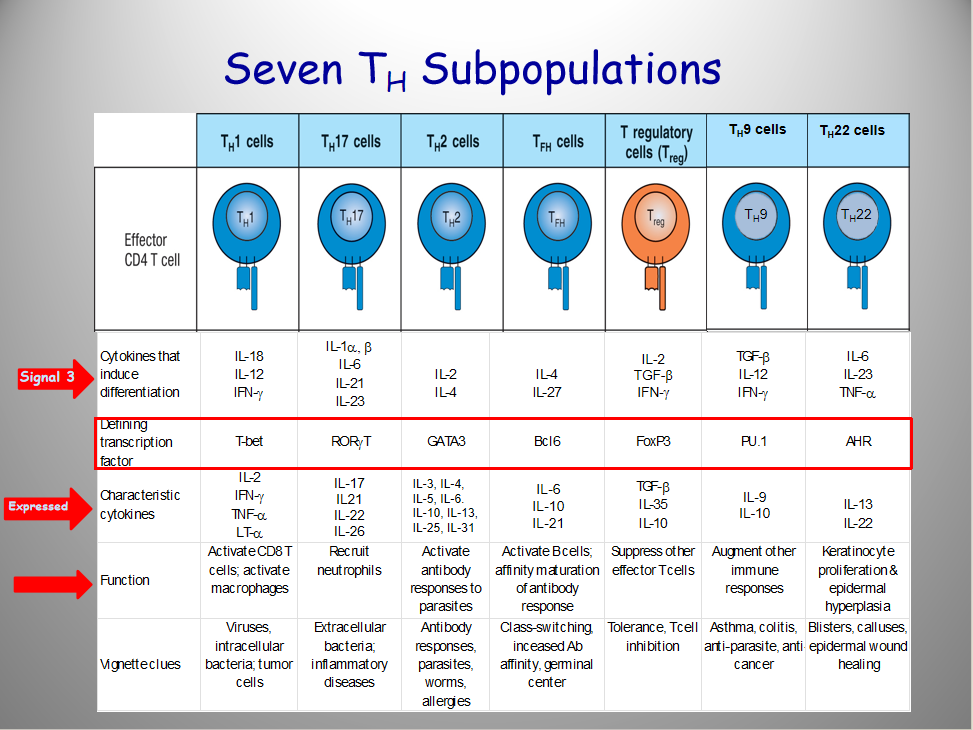

Describe TH1
Functions
Describe cross presentation
What is it?
Mech
Describe CD8+ T cells
Function
Mech
Describe Macrophages
Req. for act.
effect of act.
What happens if act. does not occur
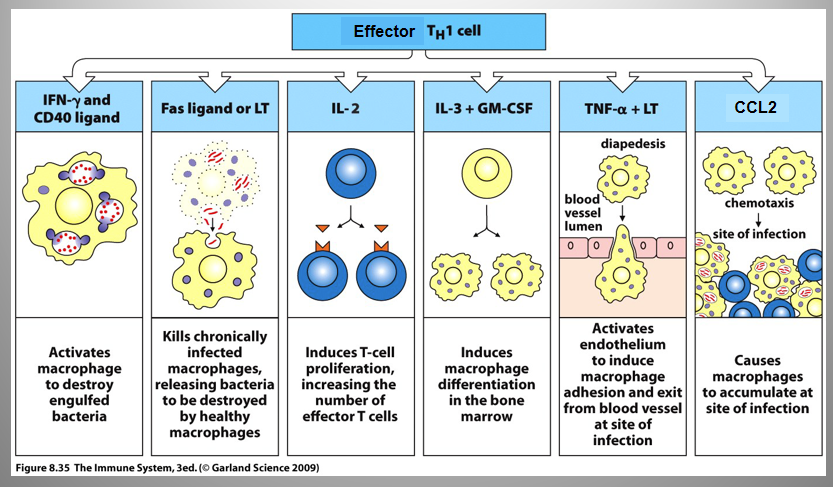
TH1
Functions:
Activate CD8+ T cells (AKA cytolytic T cells (CTLs)
Activate Macrophage killing functions
Cross Presentation
What is it
the process in which DC changes from MHC Class II to I to act. CTLs
Mech.
1. CD4+ T Cell is Activated
2. Activated CD4 T Cell “Gives DC License” to Activate CD8 T Cell
Binding of CD40L(T) - CD40(DC)
endocytosed pathogen → proteasome → endogenous processing pathway → MHC class 1
Cytotoxic CD8+ T Cells
Function:
Protection against viruses and tumors
Mechanism:
CTL Fas ligand (FasL) binds to Fas on target cell → apoptosis
releases cytotoxins → target dies by necrosis
Perforin:
form pores in membrane
Granulysin:
disrupt cell membrane integrity
Granzyme:
serine protease
enters via pores → chops up target cell proteins
Macrophages:
Mac Act. requirements (from Th1):
(IFNg)
CD40 ligand
Effects of Activation:
phago/lysosome fusion more efficiently
Increased expression of CD40
Secretion of TNFa
Highly reactive and microbicidal molecules are produced:
Oxygen radicals
Nitric Oxide
Proteases
Failure to Activate:
Granuloma formation,
when lymphocytes surrounds the macrophages w/ the antigen
EX: M. tuberculosis infections
Consequences:
Caseous Necrosis can occur @ center of tubercular granuloma,
bacilli can replicate → escape granuloma → disseminate.
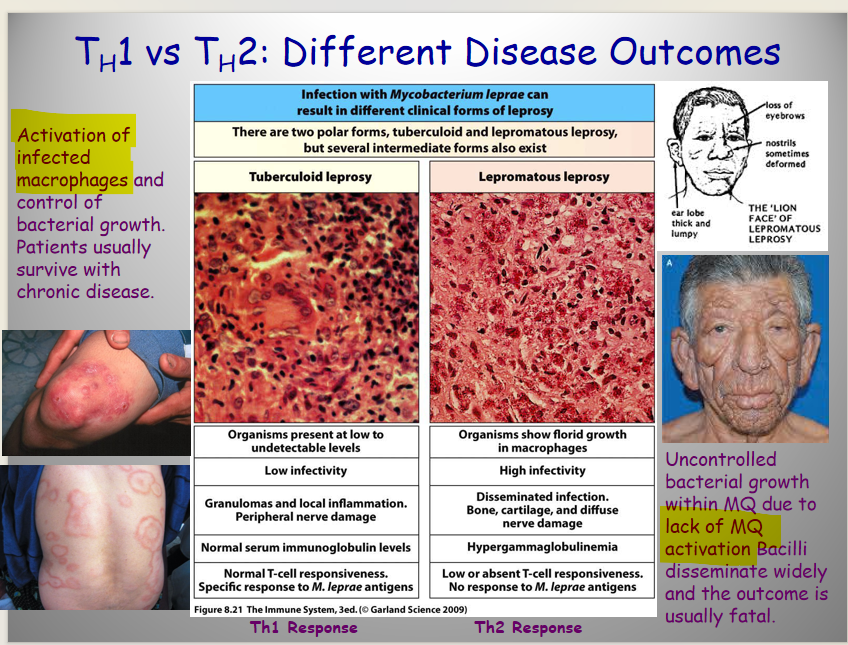
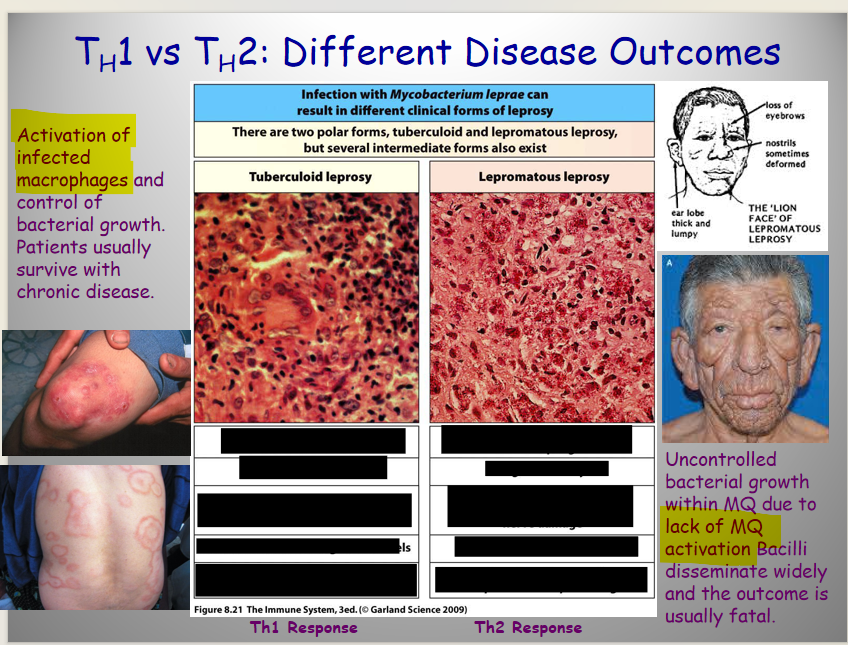
Describe Th2
Function
Mech
Function:
Act. B cell Dif. → Plasma Cells
often labeled “Humoral”
Th1 can also do this, but tend to induce human IgG2 isotype antibodies
very good at opsinization and complement activation.
Mech:
Th2 only act. B cells if BOTH recognize same specific antigen (cognate interaction)
specific epitopes can be dif. but the antigen must be the same
Th2 → upregulates CD40L + produce IL-4/5 → B cell clonal expansion
Il-5 → B cell dif. to plasma cells
Describe Th9
Function
Explain how Th9 is good and bad
Function:
Augment Immune Responses
Th9 = good and Bad
Bad:
enhances antibody production + increases immune cell activity in respiratory tract → asthma
increases intestinal permeability + enhance pro-inflammatory Th cell responses in colon
Good:
potent antiparasite activity
increases cell infiltration and enhances leukocyte functions.
augment anti-tumor immune activity.
Describe Th17’s function
Functions:
major role in autoimmunity
multiple sclerosis
inflammatory bowel diseases
activate tissue cells
recruit neutrophils.
important defense against extracellular bacteria
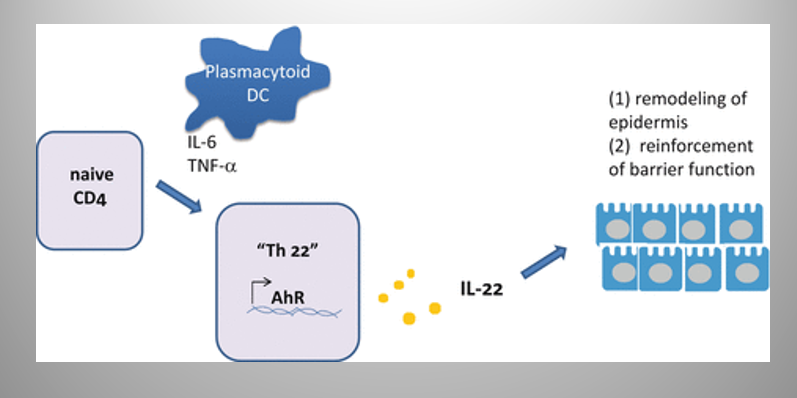
Describe Th22
Function
Mech
Function:
remodeling of epidermis
reinforcement Of barrier function
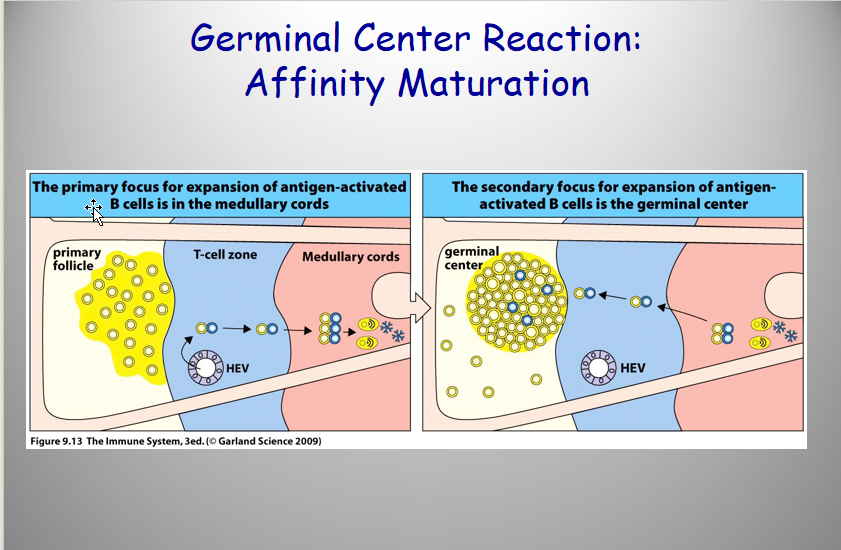
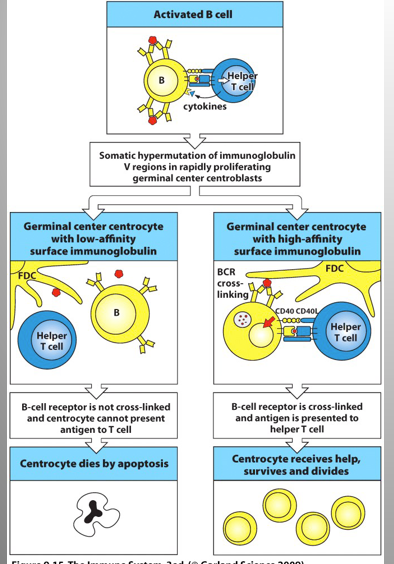
Describe Tfh
Function
Mech
Function:
helps in Selection of high affinity B cell clones after Somatic hypermutation
makes sure these mutations doesn’t produce a worst B Cell
Mech:
+ reaction:
BCR crosslinking → presentation to Thf cell → Thf sends signals to B cells → Proliferation + differentiation to plasma cells
- reaction:
low/no binding to ag; no presentation to Thf → dies
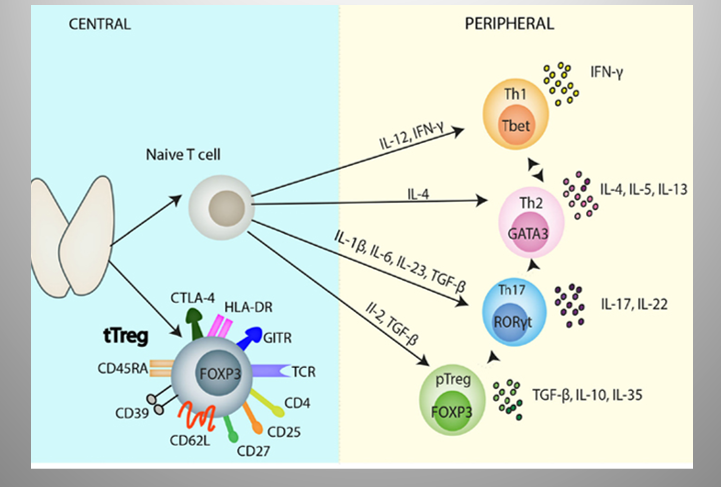
Describe Treg
Function
Creation
Mech.
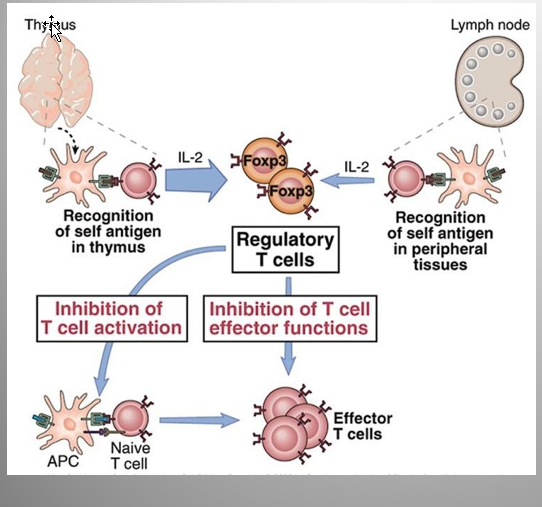
Function:
Block dendritic cell function
Suppress the responses of other effector T cells
Suppress autoreactive T cells
Treg binds to same APC → suppress the autoreactive T cell
Creation:
“Natural” or ”Thymic” tTreg : formed in thymus
“Induced” or “Peripheral” pTreg: differentiate in periphery from naïve CD4+ T cells
Mechanisms:
Targets DCs
Secrete inhibitory cytokines
Induce cytolysis
Compete for DCs against Teff
Metabolic disruption of Teff
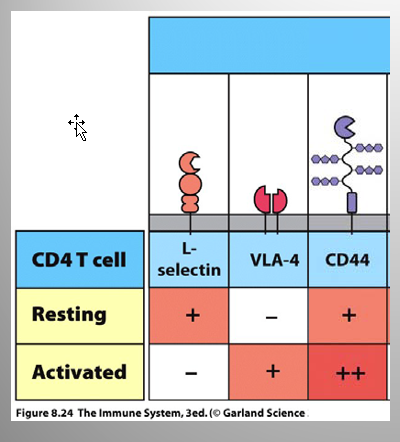
Describe the Mech. of improving Teff migration from Lymph node → infection/inflammation site
Mech. of improving Teff migration from Lymph node → infection/inflammation site
Upregulation of chemokine receptors
Downregulation of L-selectin
so that activated cells can exit lymphoid organ.
Upregulation of specific adhesion molecules
Ex: Integrin a4b1 - aka VLA-4
increases adhesion to endothelial cells in Blood vessel lumen
Upregulation of CD44
receptor for hyaluronic acid
tissues contain high levels of this
Allows Teff to be retained
Draw out how the innate and adaptive immunity work together