PIE- passive immunity and The Importance of Colostrum
1/29
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
30 Terms
what are the functions of colostrum?
- provision of energy (very energy dense, rich in fats, CHOs, and proteins) and fluid (hydrating)
- transfer of passive immunity → Protect until the neonates immune system develops
- development of the early gastrointestinal microflora (critical for digestion and immune function)
explain how colostrum allows the passive transfer of immunity
immunoglobulins (predominantly IgG which provides immediate humoral disease protection)
cell mediated immunity (maternal lymphocytes which are important to neonatal immunity- research has shown that antibody transfer alone both humoral and cellular immune components are required for adequate protection against protection)
what is the approx % of the following IGs in colostrum?
1. IgG
2. IgA
3. IgM
1. 85%-90%
2. 5%
3. 7%
what is not sufficient to protect calves from fatal disease in the neonatal period?
colostral leukocytes fed alone (humoral only- need cell mediated too)
what is the main Ig in colostrum
IgG
What factors influence neonatal microbiota development?
Neonatal microbiota development is influenced by maternal gut flora, amniotic fluid exposure, and colostrum ingestion.
How do bacterial populations in horses change in the first 72 hours after birth?
In horses, bacterial populations shift rapidly from milk-associated species to cellulose-digesting bacteria necessary for adulthood.
what is the benefit of maternal leukocytes in colostrum case study?
blood mononuclear cells from calves fed colostrum containing maternal leukocytes developed the ability to activate cell-mediated immune response by the time the calves were 1 week of age, compared with 3 weeks of age for calves fed leukocyte-free colostrum
describe the change in the gut microbiota
•Day 1-3
•Gradual acquisition of Enterococcus and Enterobacteriaceae (Colostrum/ milk derived)
•Day 3+
•Prevotella, Blautia, Ruminococcus
•Core gut microbiota of adult horses
what is the most important management in foals
Colostrum management is the single most important management factor in determining calf health and survival.
Positive blood cultures are associated with poor survival in hospitalised foals
Outcomes of failure of passive transfer of immunity to neonatal large animals (FPT)
link between colostrum intake with neonatal survival.
In large animal neonates, it is one of the most significant factors affecting health outcomes. Failure of passive transfer (FPT) is associated with:
Gastrointestinal Disease (e.g., diarrhea)
Septicemia (e.g., umbilical infections, pneumonia)
Higher Mortality Rates
describe the change in gut microbiota in neonates
- day 1-3 occurs
- gradual acquisition of enterococcus and enterobacteriaceae (colostrum/ milk derived)
- day 3+
- prevotella, Blautia, Ruminococcus
- core gut microbiota of adult horses
In small animals, passive immunity is partially transferred through the placenta, making immediate colostrum intake less critical than in large animals.
True or false?
True
what is good qual colostrum
has approprate Ig content
How do we assess colostrum quality?
- A colostrometer measures colostrum density: higher density indicates higher immunoglobulin content.
- A Brix refractometer provides a percentage reading, with values over 22% correlating with effective immunoglobulin levels (>50 mg/mL).
how much colostrum do we want young to have, what is the target IgG
3-4L in first 6 hours
Target IgG>10g/L at 4 hours of age
How can you quickly test foals for passive transfer failure (FPT)?
IgG SNAP test
What can you give a foal/calf that has evidence of passive transfer failure/FPT (IgG snap test levels were insufficient)?
Early intervention (within six hours) is key to preventing FPT:
- Two feeds of high-quality colostrum via a nasogastric tube (3-4L in first six hours then the target IgG should be over 10g/L at four hours of age)
- A plasma transfusion from hyperimmunized mares to elevate his IgG levels above the protective threshold (1L split into two and give one 500mls within the first six hours. The target IgG should be over 8g/L at 24 hours of age.

describe the OTUs (operation taxonomic units) shared between meconium, mares' gut microbiota and amniotic fluid
- 6 OTUs shared between all 3
- 75 between meconium and the mares gut
- 32 between meconium and amniotic fluid
what is the most important factor in determining calf health and survival?
colostrum management
what is associated with poor survival in hospitalised foals?
positive blood cultures
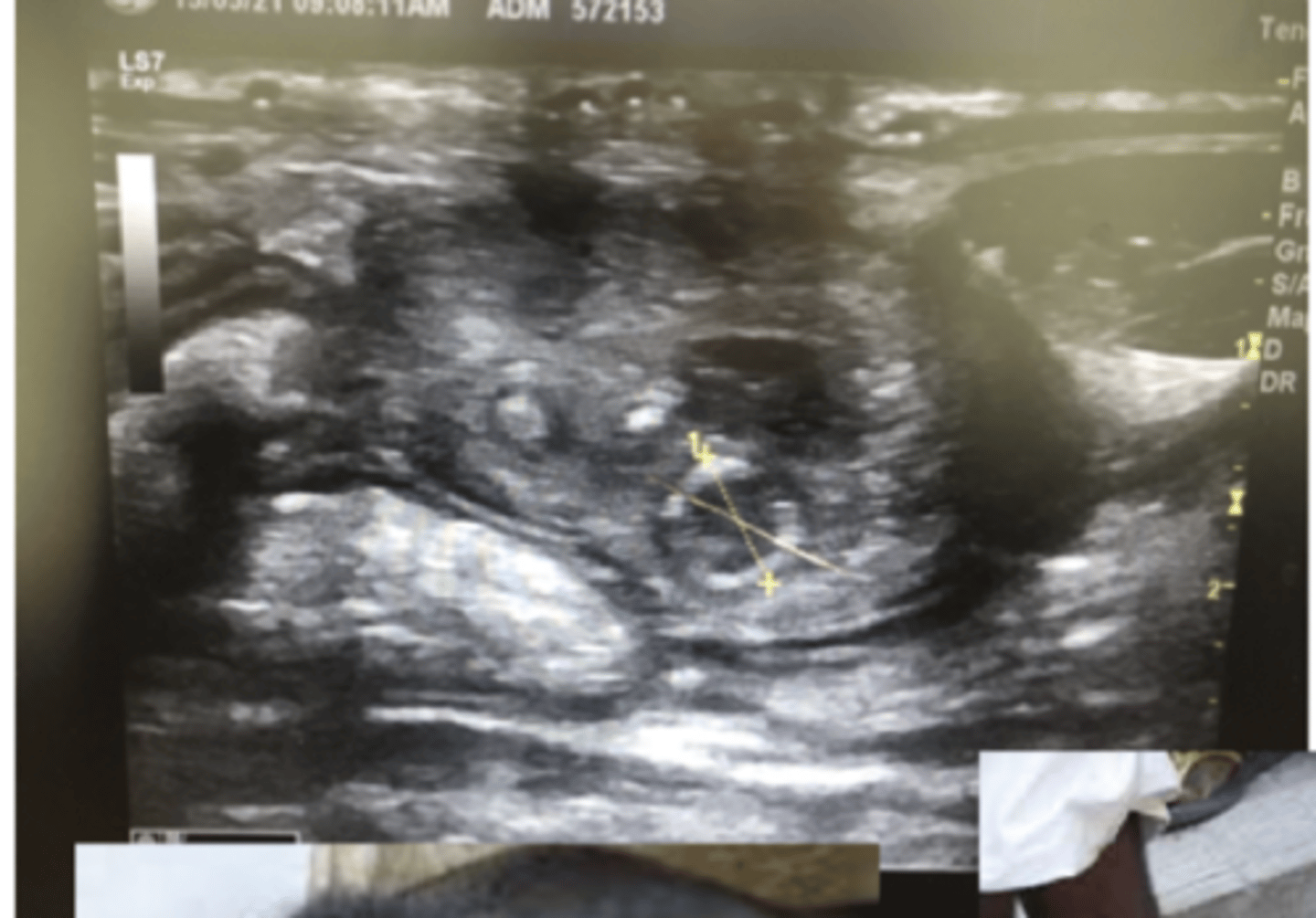
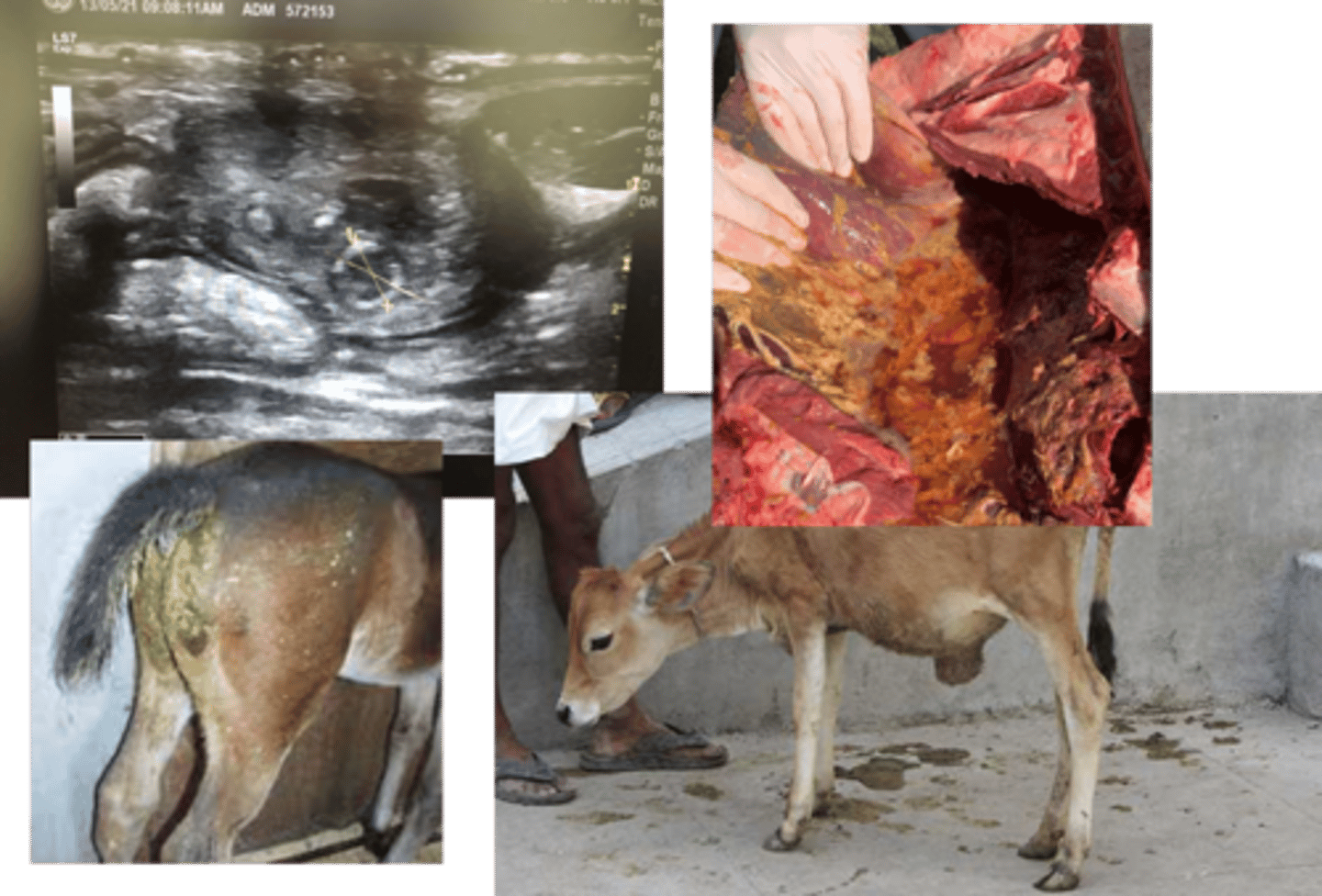
outcomes of failure of passive transfer of immunity 1
Internal umbilical remnant
enlarged right umbilical artery associated with infection

outcomes of failure of passive transfer of immunity 2
fibriosupprative ammonia, secondary to bacterial transfer after failure of passive transfer
what is the ideal Brix value for sheep colostrum?
over 22%
how much colostrum should be given in the first 6 hours of life of a neonate sheep?
3-4L
what is the IgG target at 4 hours of age for a neonate sheep?
target IgG>10g/L
if the mother has died or is recumbent what colostrum can we use?
we can use donor colostrum or powder colostrum (however not as good)
what can we also give to raise IgG concentration?
I.V. plasma transfusion
what is the target IgG for a foal at 24 hours of age?
target IgG>8g/L
how much colostrum should we aim for a foal within the first 6 hours of life?
1L split into two x 500 mls doses