Vascular Ultrasound: Abdomen, Aorta, and Portal System
1/134
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
135 Terms
Why is fasting recommended before a vascular ultrasound?
Fasting reduces abdominal gas that can block ultrasound waves and obscure anatomy.
What factors can affect blood flow during Doppler studies?
Eating, breathing pattern, and body position.
What is the typical scanning frequency for adult vascular imaging?
5 MHz or less.
What is the purpose of Color Doppler imaging?
To provide a quick overview of blood flow direction and speed.
What is the recommended patient position for vascular ultrasound?
Usually lying on their back (supine).
What are the three main layers of blood vessels?
Tunica Intima, Tunica Media, and Tunica Adventitia.
How do arteries differ from veins in terms of structure?
Arteries have thicker walls, especially the tunica media, and maintain their shape under low pressure.
What is the function of valves in veins?
To prevent backflow of blood, especially in the legs.
What is the main artery of the body?
The aorta.
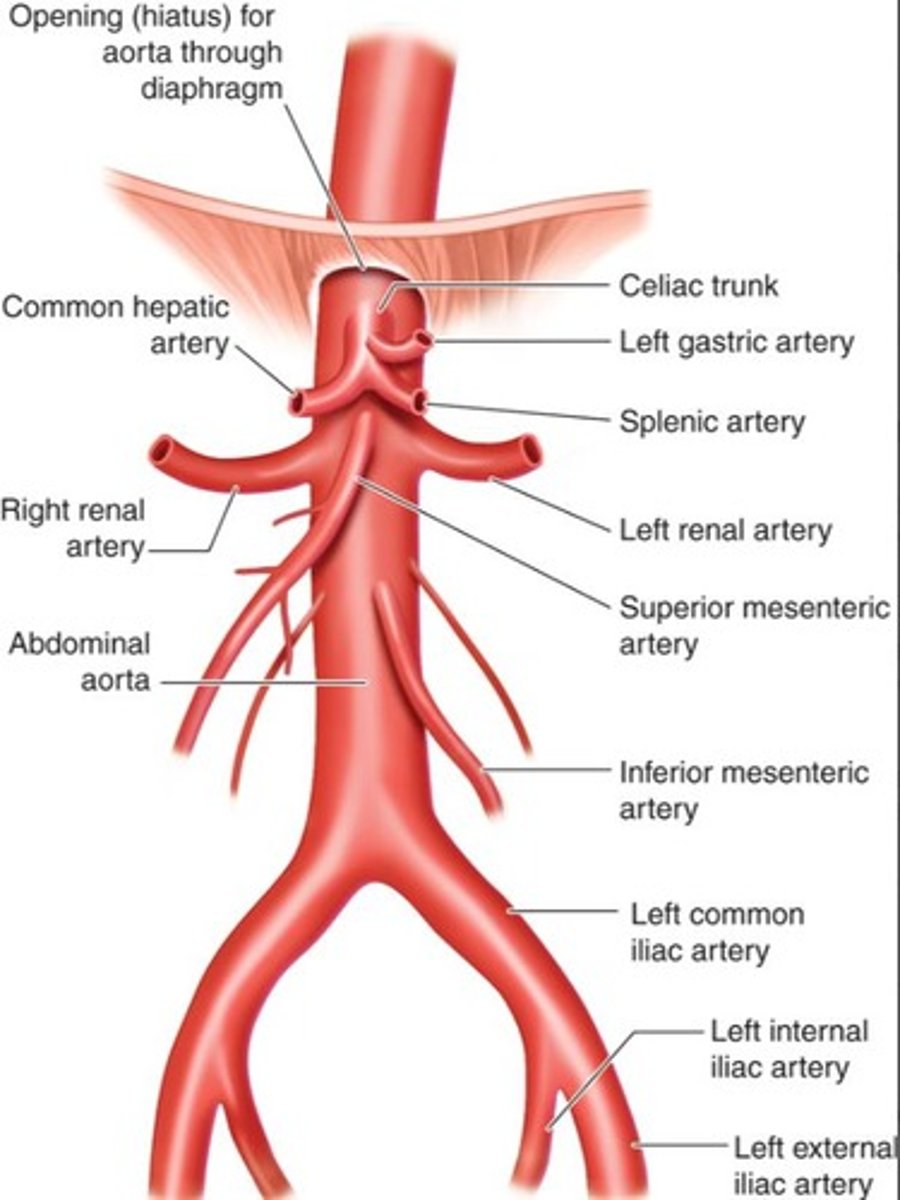
What is the celiac trunk?
The first major branch of the abdominal aorta, supplying blood to the liver, stomach, and pancreas.
What is the Nutcracker phenomenon?
Compression of the left renal vein between the superior mesenteric artery and the aorta.
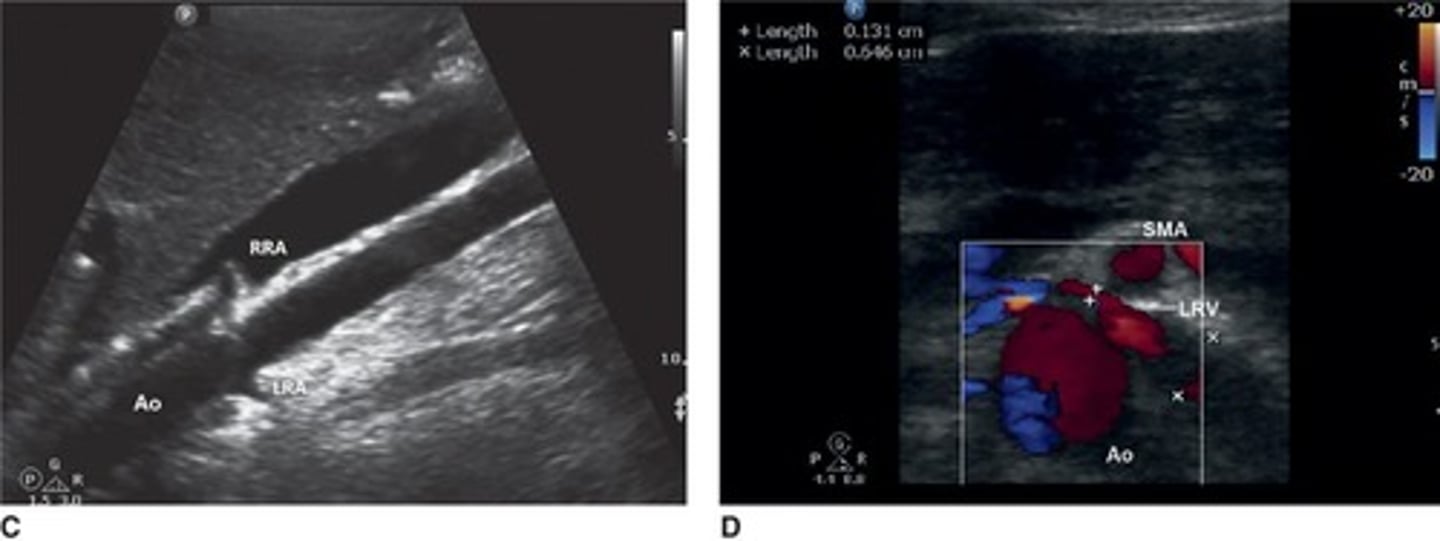
Where do the renal arteries arise from?
Just below the superior mesenteric artery.
What does the inferior mesenteric artery supply?
The distal colon.
What happens to the aorta at the level of the umbilicus?
It bifurcates into the right and left common iliac arteries.
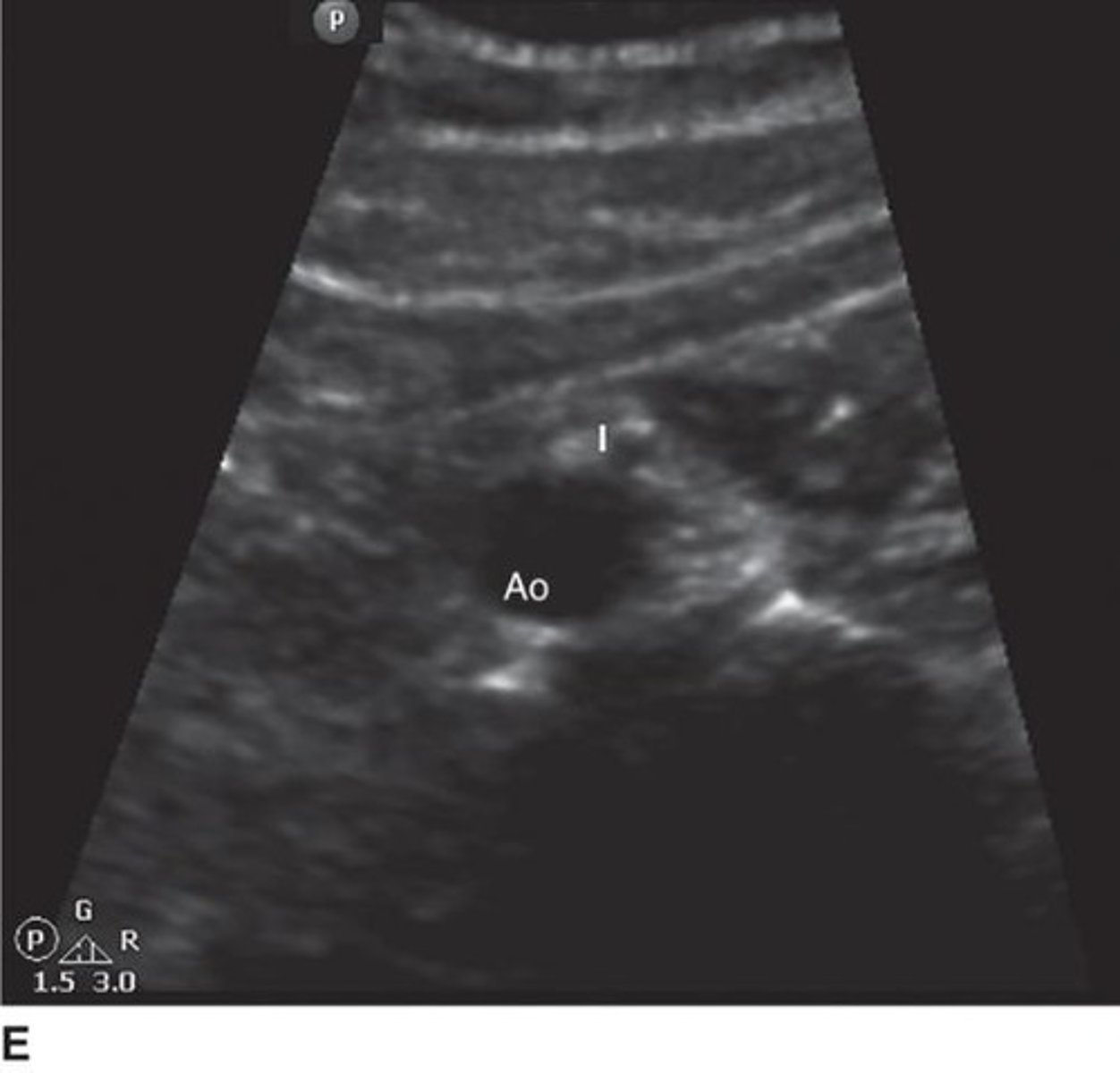
What is the sonographic appearance of the aorta?
Anechoic (black) due to its fluid-filled lumen.
What does the 'seagull sign' refer to in ultrasound imaging?
The appearance of the celiac axis and its branches in transverse view.
What is the role of the tunica media in blood vessels?
It provides strength and the ability to contract.
How can the common iliac arteries be visualized on ultrasound?
May require a full bladder or side position to see clearly.
What is the significance of the abdominal aorta's bifurcation?
It splits into the right and left common iliac arteries, supplying blood to the lower body.
What is the typical appearance of the superior mesenteric artery on ultrasound?
Round with a bright ring (echodense collar) of fat and mesentery.
What anatomical landmark is used to locate the renal artery?
Start at the aorta and look for it branching toward the kidney.
What is the function of the tunica adventitia?
It provides support and structure to blood vessels.
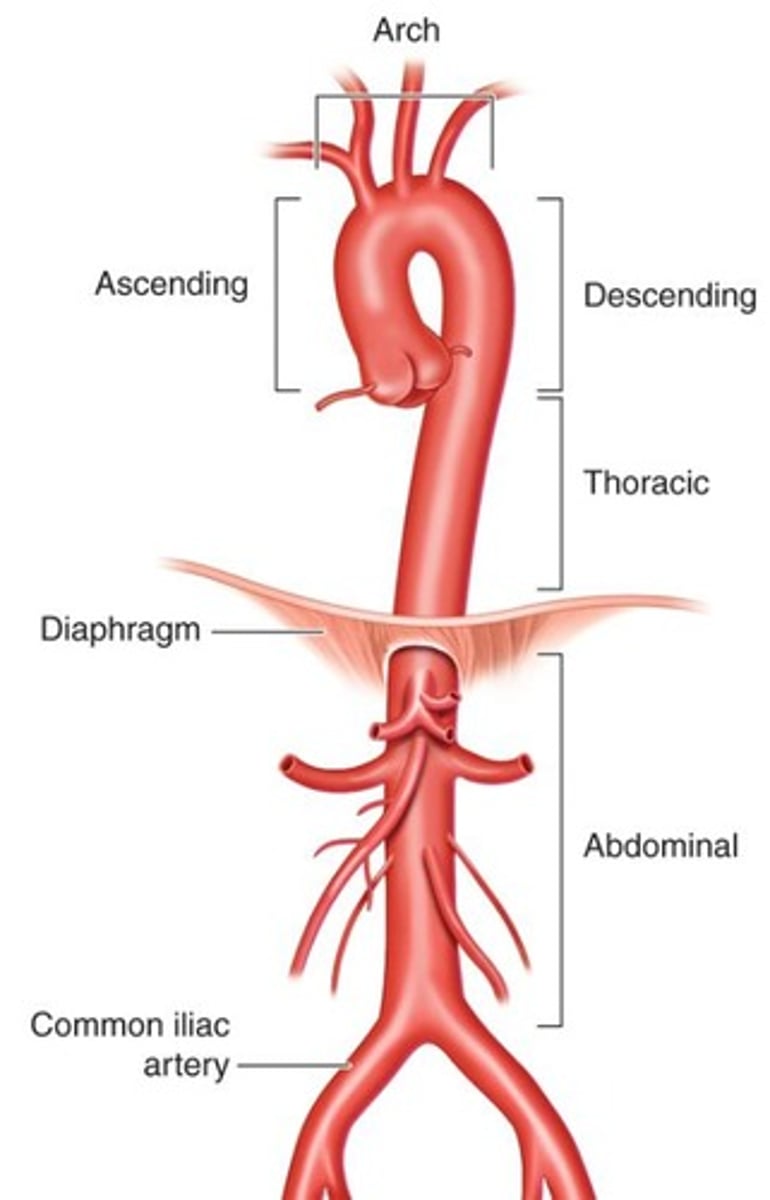
What happens to the aorta as it descends through the chest?
It continues downward as the descending thoracic aorta.
What is the primary role of arteries in the circulatory system?
To carry oxygen-rich blood from the heart to the body.
What is the primary role of veins in the circulatory system?
To carry oxygen-poor blood back to the heart.
What is the significance of the vasa vasorum?
It supplies blood to the walls of larger blood vessels.
What is the typical imaging technique for branch vessels?
Start near their origin and follow the path, recording images of the entire visible length.
What is the purpose of taking images every 1-2 cm during a scan?
To capture detailed images and identify any abnormalities.
What is the appearance of the celiac axis on ultrasound?
Appears as a short tube that splits into the hepatic artery (right) and splenic artery (left), forming the 'seagull sign' on transverse view.
How does the superior mesenteric artery (SMA) appear on ultrasound?
Appears round with a bright ring (echodense collar) of fat and mesentery, lying just below the celiac trunk.
What is the 'peeled banana' appearance in ultrasound imaging?
It refers to the view showing the renal arteries and aorta together in the coronal plane.
What does the nutcracker sign indicate?
It is seen when the left renal vein is compressed between the SMA and aorta, observed in transverse view.
Where does the inferior mesenteric artery (IMA) arise?
It arises midway between the renal arteries and the aortic bifurcation and is seen as a small vessel turning posteroinferiorly.
How do common iliac arteries appear on ultrasound?
In transverse view, they appear as two round black circles; in longitudinal view, they split into external and internal iliac arteries.
What is the best positioning for imaging the common iliac arteries?
Place the transducer in the iliac fossa and angle medially at 45 degrees, with a full bladder for better visibility.
What is the function of the inferior vena cava (IVC)?
The IVC returns deoxygenated blood to the right atrium of the heart, formed by the common iliac veins.
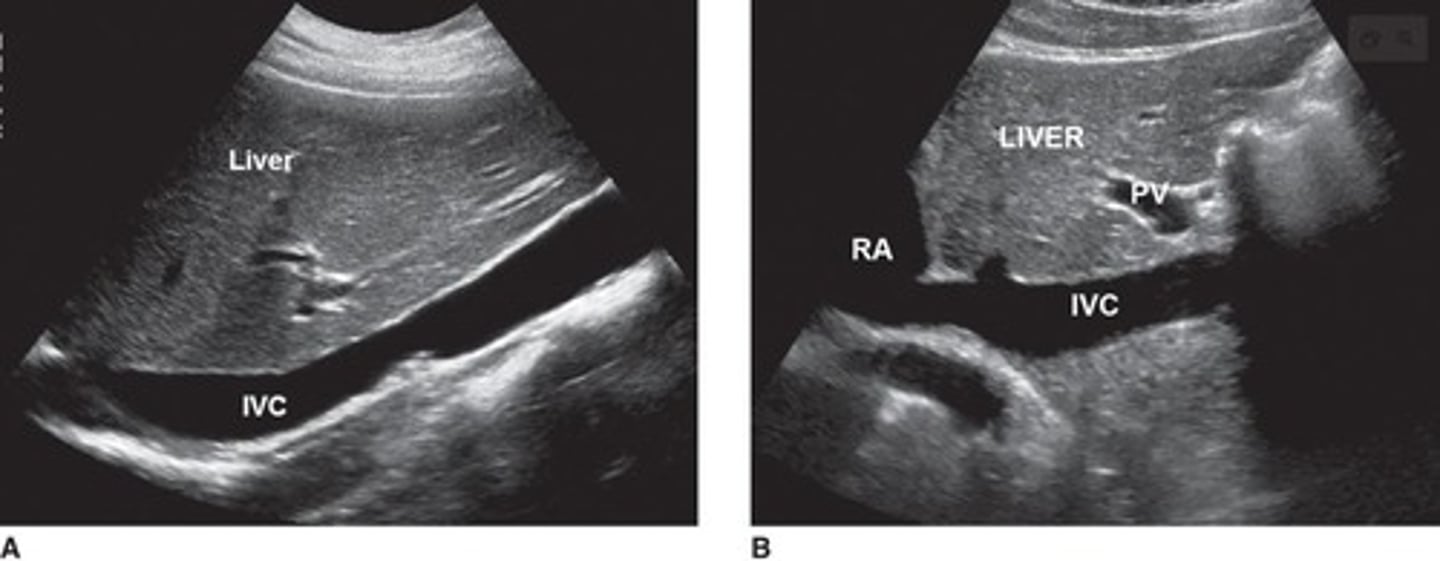
What shape does the IVC take as it nears the heart?
It takes on a slightly forward (anterior) curve, resembling a hockey stick.
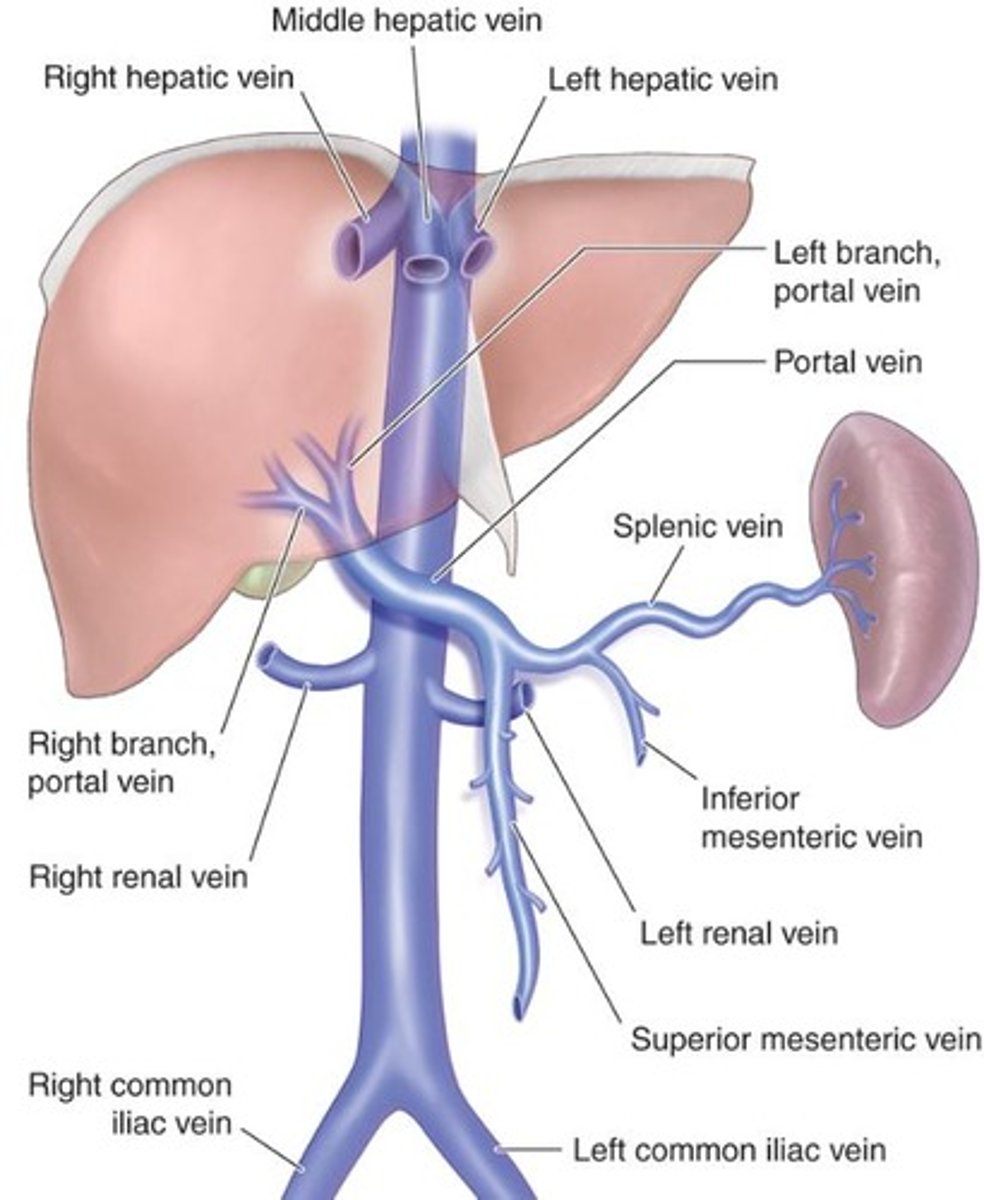
What are the three hepatic veins?
Right hepatic vein, middle hepatic vein, and left hepatic vein, which drain blood from the liver into the IVC.
What does the 'Playboy Bunny' sign refer to in ultrasound?
It describes the appearance of the three hepatic veins converging near the heart on ultrasound.
How does the IVC appear on ultrasound?
It appears anechoic (black) and oval-shaped, changing size with breathing.
What happens to the IVC during inspiration?
The IVC collapses as pressure drops and blood moves quickly to the heart.
What is the main portal vein (MPV) formed by?
It is formed at the portal confluence where the splenic vein and superior mesenteric vein (SMV) join together.
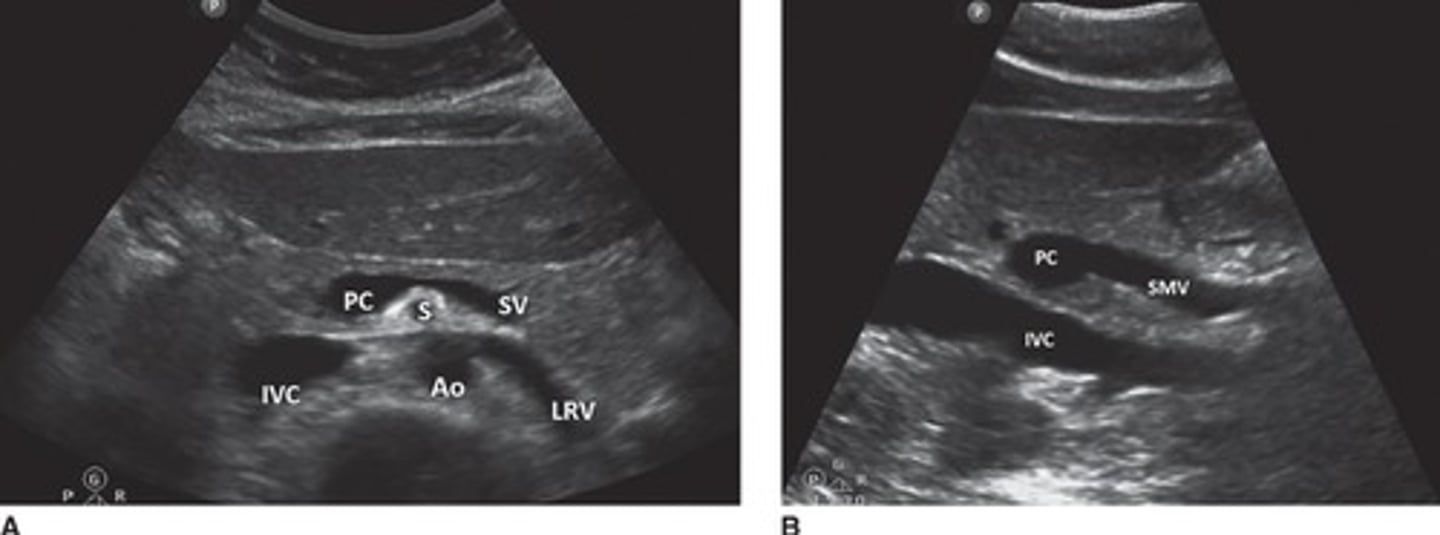
Where does the splenic vein travel?
It exits the spleen, travels across the back of the pancreas, and joins the SMV behind the neck of the pancreas.
How does the superior mesenteric vein (SMV) appear on ultrasound?
It runs parallel and to the right of the SMA and can be seen by rotating the probe 90° at the portal confluence.
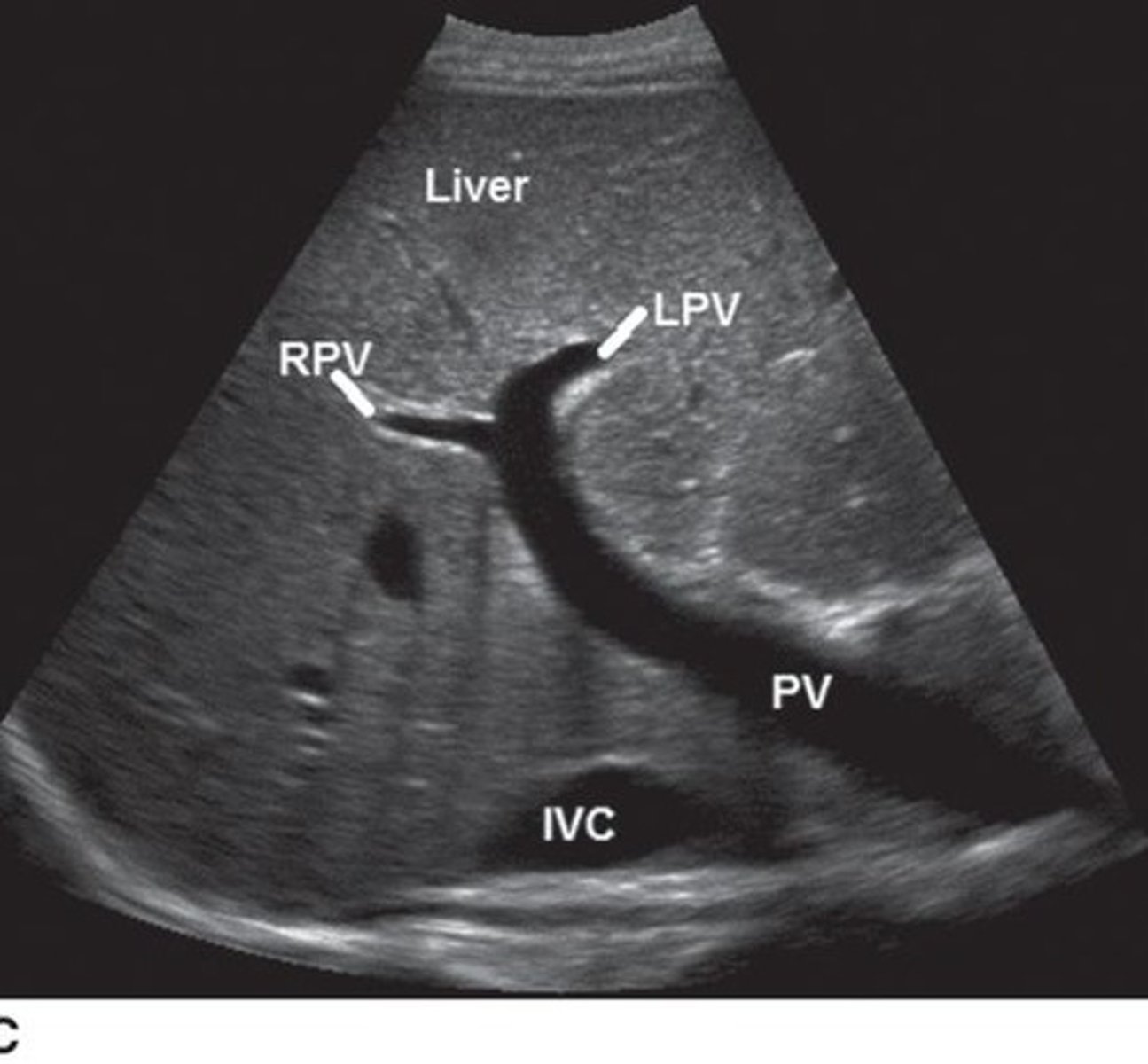
What pathway does the main portal vein (MPV) take?
The MPV travels obliquely and anteriorly to the liver hilum, where it divides into the left and right portal veins.
What is atherosclerosis?
A type of arterial disease where the inner lining of arteries thickens due to fatty deposits, carbohydrates, blood components, calcium, and fibrous tissue.
What are some risk factors for atherosclerosis?
High cholesterol (hyperlipidemia), high blood pressure (hypertension), smoking, and diabetes.
What are the clinical signs of atherosclerosis?
Often asymptomatic until arteries become significantly narrowed (stenotic).
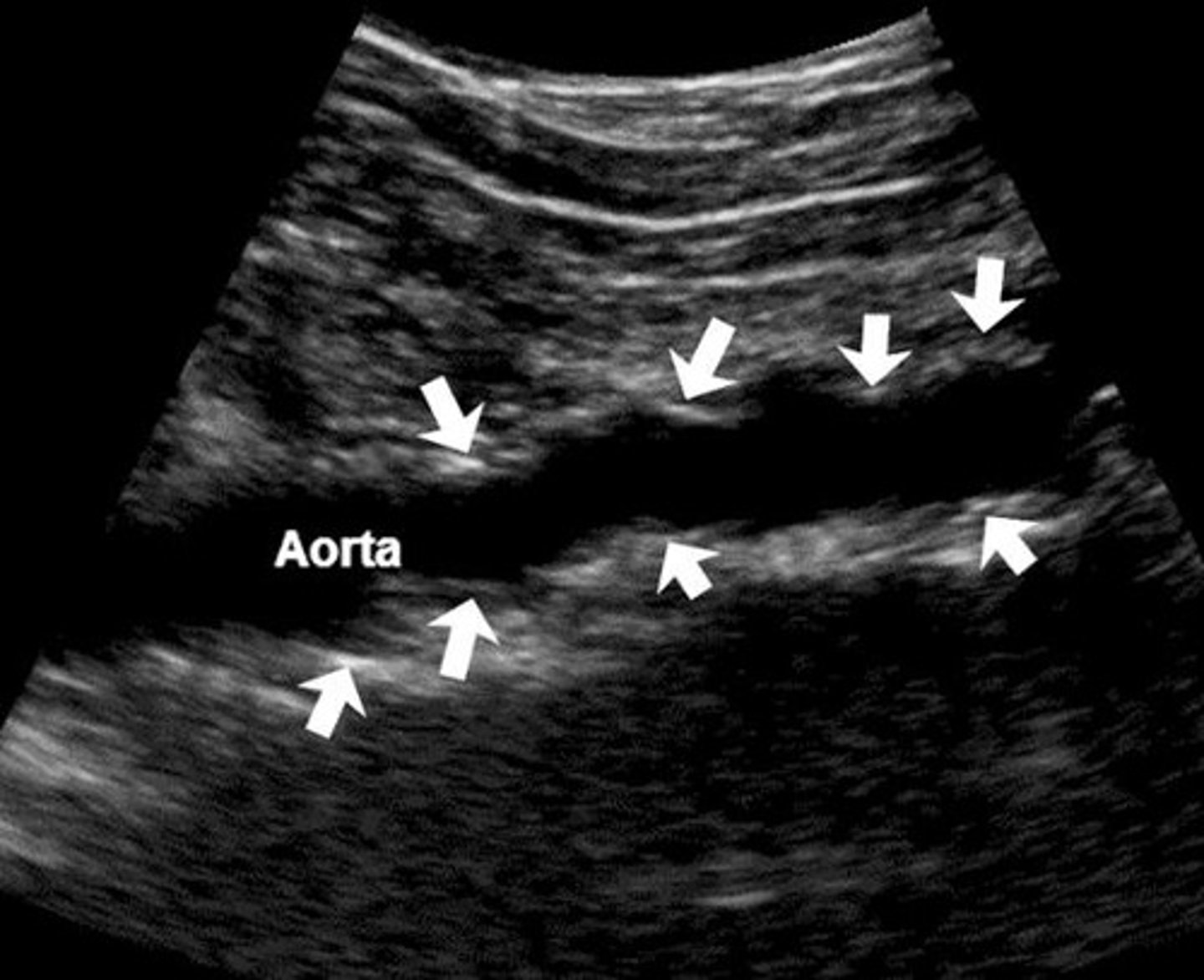
What is the appearance of the aorta in cases of arteriosclerosis?
Diffuse plaque with minimal acoustic shadowing can be seen in the longitudinal sonogram through the distal portion of the aorta.
What is the significance of relational anatomy in ultrasound imaging?
Understanding how arteries and veins relate to organs and ducts is essential for accurate ultrasound imaging.
How is the left renal vein positioned relative to the aorta and SMA?
The left renal vein passes between the aorta and the SMA.
What is the appearance of the IVC during the Valsalva maneuver?
The IVC collapses due to increased belly pressure.
What is the role of color Doppler in imaging the IMA?
High-frequency probes and color Doppler are needed for clear imaging of the IMA.
What is the significance of the 'banana peel' appearance?
It refers to the sonographic appearance of the renal arteries and aorta together in the coronal plane.
What can atherosclerosis lead to?
Reduced blood flow, aneurysms, organ ischemia.
What are the sonographic signs of atherosclerosis?
Irregular inner walls, plaque deposits, tortuosity, calcifications.
Where is atherosclerosis most commonly seen?
At bifurcations and near branching vessels.
What is an aneurysm?
A localized bulge/dilation in a blood vessel due to wall weakness.
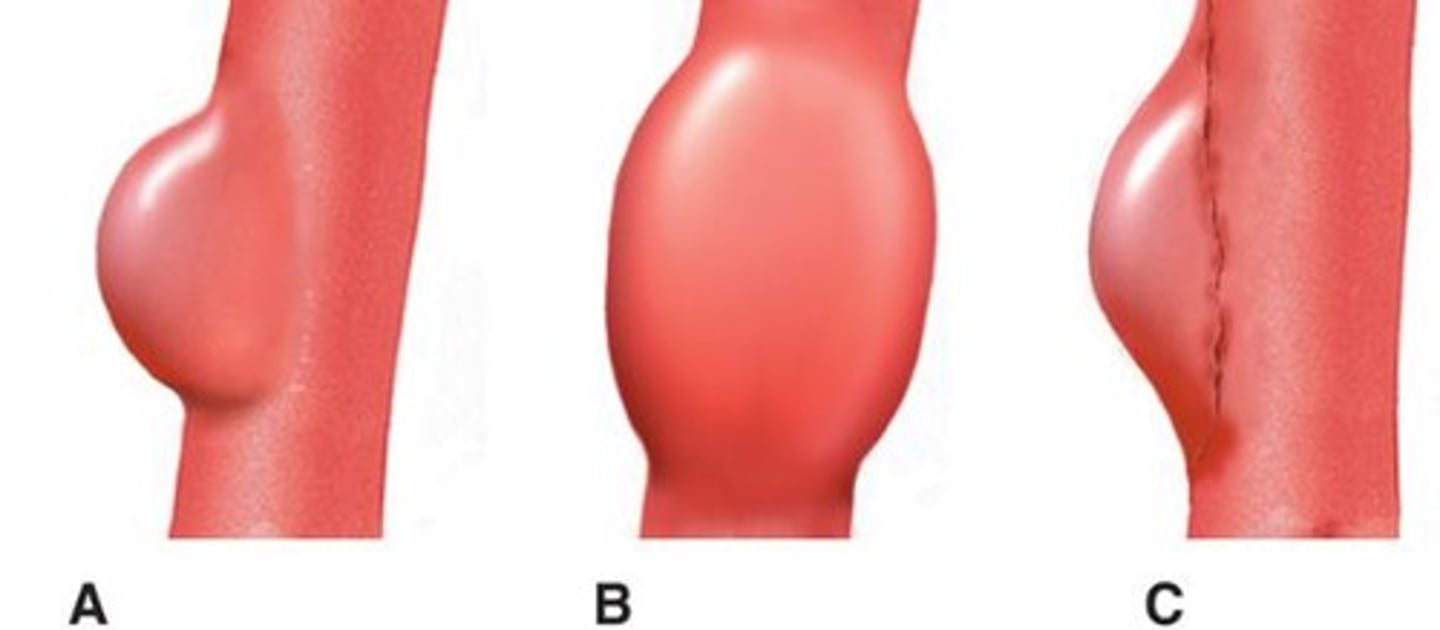
What is a true aneurysm?
An aneurysm that involves all three layers of the artery wall.
What is a false aneurysm (pseudoaneurysm)?
A blood-filled sac outside the vessel wall but still connected to the lumen.
What is a fusiform aneurysm?
Circumferential and gradual dilation of the entire artery wall.
What is a saccular aneurysm?
An aneurysm that bulges out on one side and is connected by a neck.
What is a dissecting aneurysm?
An aneurysm where blood enters a tear in the wall, splitting its layers.
Where do most abdominal aortic aneurysms (AAAs) occur?
Below the renal arteries.
What are the main risk factors for abdominal aortic aneurysms?
Smoking and atherosclerosis.
What symptoms may indicate an abdominal aortic aneurysm?
Usually asymptomatic; may feel a pulsating mass or vague abdominal pain.
What is the normal aorta diameter?
Approximately 2.5 cm at the diaphragm and 1.5-2.0 cm at the iliac bifurcation.
How is an aneurysm diagnosed?
If the diameter is ≥3.0 cm.
What is the significance of the 'anechoic crescent sign' in an aneurysm?
It indicates a dark fluid area inside the aneurysm, possibly liquefied clot.
What is an aortic dissection?
A tear in the inner lining of the aortic wall, forming a false lumen.
What are the types of aortic dissection according to Stanford classification?
Type A involves the ascending aorta; Type B starts after the left subclavian artery.
What are the main causes of aortic dissection?
Hypertension, connective tissue disorders, trauma, pregnancy.
What are common symptoms of aortic dissection?
Sudden severe chest pain, back pain, leg numbness, or neurological symptoms.
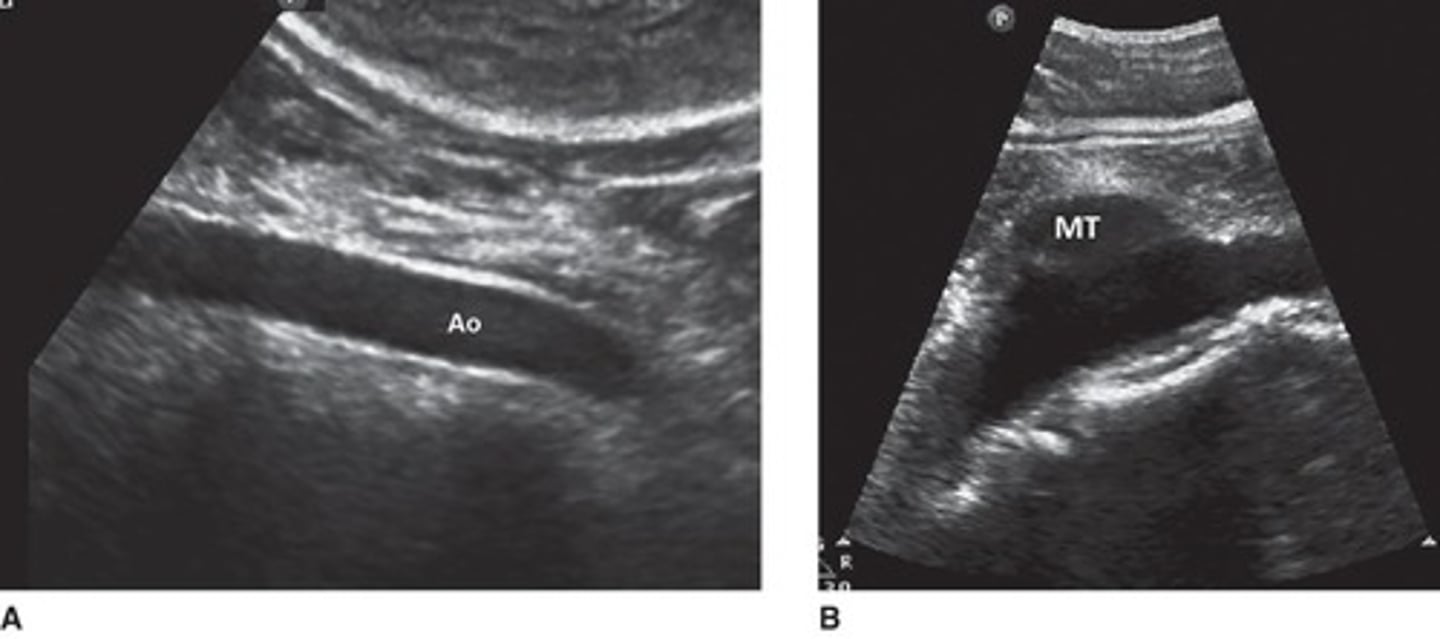
What is the sonographic appearance of aortic dissection?
A thin, fluttering flap inside the aortic lumen.
What is an aortic rupture?
A life-threatening tear in the vessel wall causing bleeding into the abdomen.
What symptoms indicate an aortic rupture?
Sudden back pain and low blood pressure.
What are inflammatory aneurysms characterized by?
Surrounded by fibrotic and inflamed tissue, can stick to nearby organs.
What is the most common splanchnic artery aneurysm?
Splenic artery aneurysm.
What are the symptoms of a splenic artery aneurysm?
Left upper quadrant pain, mass, or rupture.
What is the second most common splanchnic artery aneurysm?
Hepatic artery aneurysm.
What is the sonographic feature of renal artery aneurysms?
Anechoic mass along the renal artery, may show wall calcifications or thrombus.
What caution should be taken when diagnosing renal artery aneurysms?
A prominent left renal vein can be mistaken for a renal artery aneurysm.
What is a renal artery aneurysm?
An abnormal dilation of the renal artery, which may be right or left-sided.
What is the typical sonographic appearance of iliac artery aneurysms?
An anechoic mass in the pelvis, possibly showing pulsations, wall calcifications, and thrombus.
What is the relationship between iliac artery aneurysms and aortic aneurysms?
Iliac artery aneurysms usually occur with aortic aneurysms but can also be isolated and bilateral.
What are common symptoms of iliac artery aneurysms?
Often silent; may cause pelvic pressure, urologic or GI issues, or leg symptoms.
What materials are aortic grafts typically made from?
Teflon or Dacron.
What does the sonographic appearance of an aortic graft look like?
Brighter and straighter than the native aorta, may show ribbing.
What is a pseudoaneurysm?
A pulsating sac near a graft, characterized by turbulent Doppler flow and swirling.
What is an endoleak?
Continued flow outside the graft into the aneurysm sac, classified into types I-V based on cause.
What is vascular stenosis?
Narrowing of blood vessels due to plaque or other issues.
How can Doppler be used to detect vascular stenosis?
By identifying abnormal blood flow patterns, such as high-velocity jets and turbulence.
What are the causes of renal artery stenosis?
Atherosclerosis and fibromuscular dysplasia.
Who is at risk for renal artery stenosis?
Young women (<30 years) or older men (>50) with hypertension, kidney dysfunction, or known vascular disease.
What is the direct method for evaluating renal artery stenosis?
Evaluates the renal artery from aorta origin to kidney using color and spectral Doppler.
What indicates ≥60% stenosis in renal artery evaluation?
PSV > 180-200 cm/s or RAR > 3.5.
What is the indirect method for evaluating renal artery stenosis?
Evaluates segmental or interlobar intrarenal arteries looking for tardus-parvus waveforms.
What does a resistive index (RI) difference >5% between kidneys suggest?
Possible renal artery stenosis.
What does a stented renal artery typically look like on imaging?
Brighter and slightly wider, with increased PSV and turbulent flow at the stent end.
What is chronic mesenteric ischemia?
Poor blood flow to intestines, especially after meals, occurring if 2 of 3 main arteries are stenosed or blocked.