E&P II final
1/118
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
119 Terms
orthopnea
dyspnea that is triggered when patient is reclining
platypnea
dyspnea triggered by assuming upright position
orthodeoxia
oxygen desaturation on assuming upright position
trepopnea
laying on one side relieves dyspnea
pedal enema
swelling of lower extremeties due to heart failure most often
pleuritic chest pain
located internally or posteriorly, sharp and increases with deep breathing
nonpleuritic chest pain
located in center of chest and may radiate to shoulder or arm
pectus carinatum
abnormal protrusion of sternum
pectus excavatum
depression of part or entire sternum, can cause restrictive lung effect
apneustic breathing
deep, gasping inspiration with brief, partial expiration
ataxic breathing
completely irregular breathing pattern with variable periods of apnea
biot respiration
clustering of rapid, shallow breaths couples with regular or irregular periods of apnea
cheyne stokes respirations
breaths increase and decrease in depth and rate with periods of apnea
kussmauls respirations
deep and fast respirations
paradoxical breathing
abdominal wall moves inward on inspiration and outward on expiration, typically due to chest trauma
crepitus
air leaks into subcutaneous tissues causing this, sign of subcutaneous emphysema
bronchovesicular breath sounds
heard around sternum, softer and lower in pitch
vesicular breath sounds
heard over lung parenchyma, very soft and low pitch
coarse crackles
airflow moves secretions or fluid into airways
fine crackles
sudden opening of small airways in lung deep breathing
acrocyanosis
occurs in newborns, usually disappears within 24-72hrs after birth
FEV1
force exhalation volume, healthy adults should be able to exhale 80% of their inahle volume in the first second of a breath
FVC
forced vital capacity, amount one can forcibly exhale after taking in a deep breath
COPD mechanism
inflammation and obstruction of small airways, loss of elasticity (elastic destruction in alveolar walls), active bronchospasm, alveoli collapse on themselves causing air trapping
COPD symptoms
productive cough, wheezing or diminished breath sounds, SOB particularly on exertion, progressive dyspnea, barrel chest, accessory muscle use, edema (cor pulmonale)
acute COPD management
reestablish the patient to baseline status as quickly as possible, inhaled bronchodilators, oral antibiotics if purulent, short systemic corticosteroid course, O2, NIV if hypercapnic
emphysema
characterized by abnormal, permanent enlargement of the airspaces beyond the terminal bornchiole accompanied by destruction of the walls of the airspaces without fibrosis, loss of chest recoil, mucus plugs due to not being able to exit past collapse
chronic bronchitis
chronic cough is present for at least 3 months per year for at least 2 years, infection or inflammation of the large airways or bronchi, caused by virus, treated with antitussives
centriacinar vs panacinar (emphysema)
centriacinar occurs usually in upper lobes, with septal destruction in bronchioles and alveolar ducts, panacinar involves the entire acinus, damage is more randomly distributed (alpha 1)
late asthmatic response
4-8hrs after early response, recruitment of lymphocytes, eosinophils, basophils and neutrophil, airway scarring, increased bronchial hyperresponsiveness, mucous accumulation, airway remodeling
pulsus paradoxus
exaggerated drop in systolic blood pressure during inspiration, can indicate athma/acute COPD
status asthmaticus
bronchospasm not reversed by usual measures, life threatening (death signs: silent chest (no air movement) and a PaCO2 >70mmHg)
leukotriene inhibitors
mediate inflammation and bronchospasm, mild to moderate asthma control
anticholinergics
can be used as adjunct to first line brochohodilators if there is inadequete response, addictive effect
anti IgE therapy
omalizumab (xolair) blocks IgE biologic effects, allergic asthma with corticosteroids
asthma emergency management
early and frequent B2 agonists, high dose parenteral corticosteroids, magnesium sulfate, oxygen (heliox), antibiotics
bronchiectasis
abnormal, irreversible dilation of bronchi caused by chronic airway inflammation and destruction (common in CF), persistent abnormal bronchi dilation, hallmark: persistent purulent secretions
bronchiectasis treatment
sputum culture (antibiotics), bronchodilators, humidification and hyperosmolar substances, DPI mannitol, anti inflammatories, chest physiotherapy, O2, surgery
respirable mass
portion of inhaled mass that can reach lower airways
inertial impaction
>5 micrometers, occurs when aerosol in motion collides with and are deposited on surface, occur in first 10 airway generations
sedimentations
occurs when aerosol particles settle out of suspension and are deposited due to gravity (1-5micrometers)
brownian diffusion
very small particles, >3 micrometers, diffuse into alveolus, 1-.5 micrometers the particles may remain suspended until exhaled
priming
pMDI, shake for at least 5 seconds prior than releasing one or more sprays into the air if it is new or has not been used in awhile, required to provide adequate dose
blow by technique
used if patient cannot tolerate mask treatment, directs aerosol from nebulizer towards patients nose or mouth several inches away
mucous blanket
consists of a gel layer and a sol layer, produced by the goblet cells and bronchial glands, sol layer allow cilia movement, gel layer traps particles
sol layer
can be replenished by drinking water, blank aerosol therapy, coughing
cough stages
inrritation (stimulating nerve endings), inspiration, compression, expulsion (high velocities pick up particle laden mucus)
chest PT contraindications
distended abdomen, recent esophageal surgery, uncontrolled airway risk for aspiration, subcutaneous emphysema, would, bronchospasm, osteoporosis, chest wall pain, lung contusion
vibration
stimulates the cilia and the cough mechanism, should be done on every site where percussion occurred, done on exhalation usually 3x at one site
active cycle of breathing technique
relaxation and breathing control, 3-4 thoracic expansion exercises, relax, repeat 3-4, relax, perform one or two FETs (huffs), relax
autogenic drainage
patient uses diaphragmatic breathing to mobilize secretions by varying lung volumes and expiratory airflow in three phases, should be sitting, coughing suppressed until complete (CF) can be done in place of. PDPV/CPT
mechical insufflation-exsufflation
apply positive pressure of 30-50cm H2O to airway for 1-3 seconds then abruptly reverses airway pressure to -30 to -50cm H2O for 2-3 seconds, five cycles of this followed by normal breathing, mimics a cough (neuromuscular disease patients)
positive airway pressure therapy
mimics pursed lip breathing (pursed lip prevents airway collapse on exhalation, increases expiratory flow) increases expiratory flow in large airways and collateral flow in smaller airways
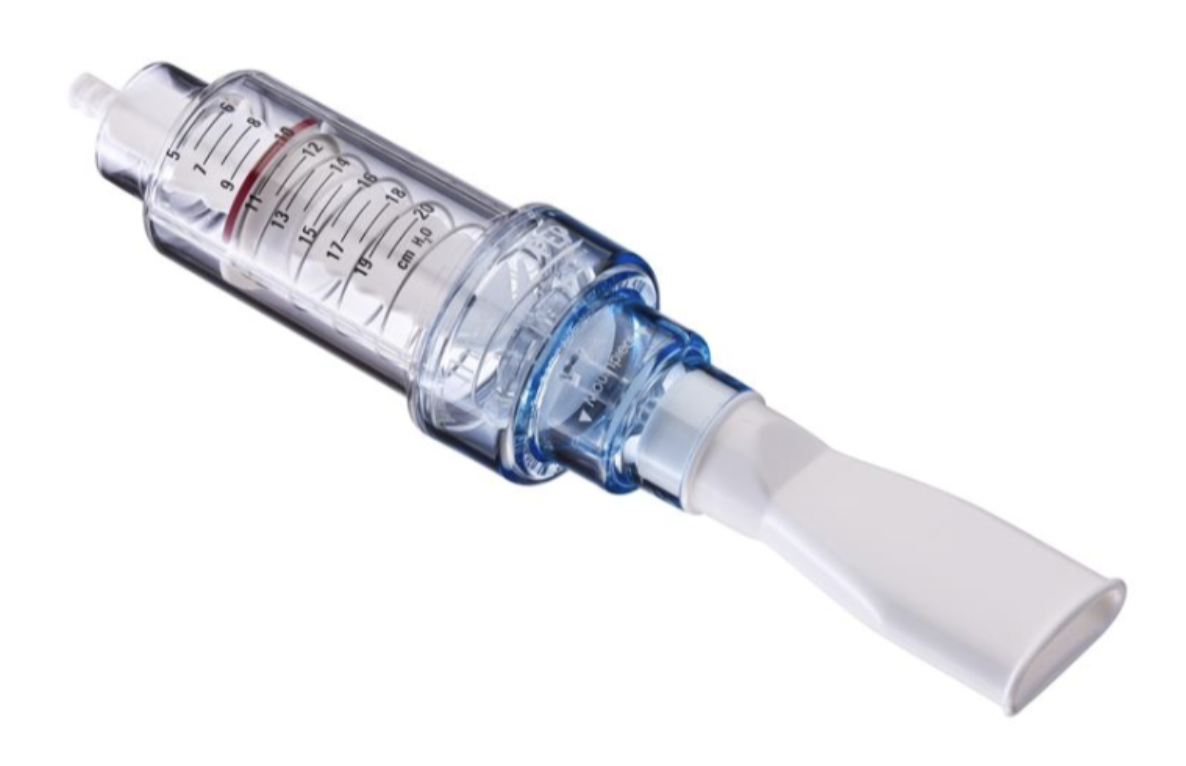
threshold PEP
mimics pursed lip breathing, numbers increase the pressure the device is putting back on the lungs, promotes bronchial hygiene, exhale into it
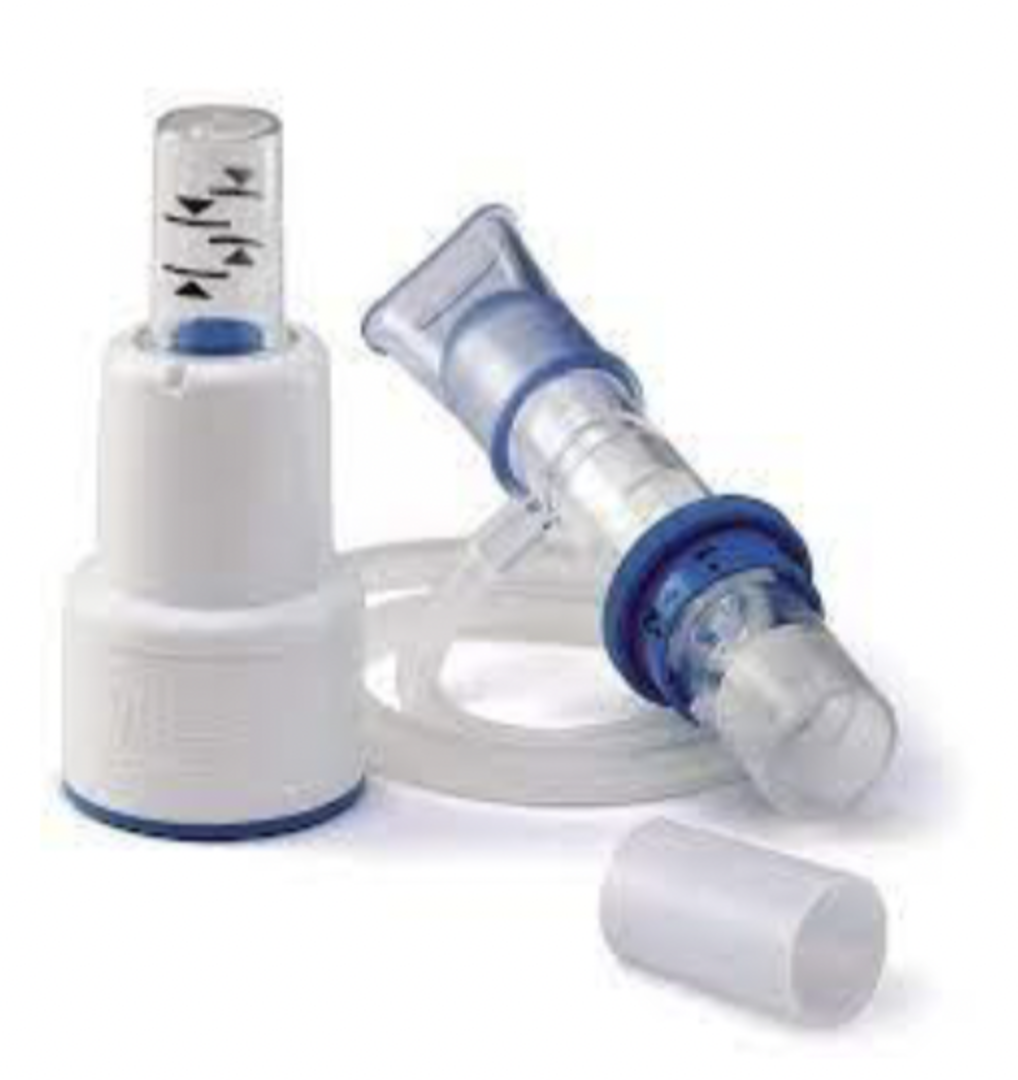
therapep
gives visual representation to keep blue dial between the arrows while exhaling, breathing treatment can be incorporated

aero pep
holding chamber, can do inhaler through it and PEP

aerobeca / acapella
increases expiratory flow and collateral flow, it creates oscillations which vibrate the airway walls and loosen mucus, shakes the airway
intra alveolar pressure
decreases on inspiration, increases on expiration
pulmonary surfactant
decreases surface tension which increases pulmonary compliance (reduces effort needed to expand lungs), reduces tendency for alveoli to collapse
adhesive atelectasis
from lack of surfactant, air exchanged is labored without surfactant resulting in collapse
gas absorption atelectasis
occurs when there is a complete interruption of ventilation to a section of lung or when there is significant shift in V/Q, also known as nitrogen washout
lobar atelectasis
can occur when ventilation is compromised in a larger airway or bronchus
compression atelectasis
when something presses against lungs to let out the air in the alveoli, this occurs. an obstruction in the area between the lungs and chest wall due to a mass, fluid or air
incentive spirometry
provides visual cues to patient when desired inspiratory volume of flow is reaches, provided to be effective in high risk patients, mimics sigh
IS indications
presence of pulmonary atelectasis, presence of conditions predisposing to atelectasis (abdominal/thoracic surgery, COPD pt surgery), presence of restrictive lung defect associated w/ quadriplegic or dysfunctional disphragm (10 breaths per hour)
intermittent positive pressure breathing
uses positive airway pressure to expand lung during inhalation, lasts 15=20min, useful in treatment of pulmonary complications or exacerbations of lung disease
IPPB indications
preventing or expanding atelectasis, atelectasis not responsive to other modalities such as IS, patient high risk for atelectasis and cannot perform IS
EzPAP
when IS alone wont open airways, connect device to flowmeter and adjust to 5-15lpm, patient exhales into it and breathes against a pressure on exhale
PAP effects
recruitment of collapsed alveoli via FRC increase, decreased WOB secondary to increased compliance elimination, improved ventilation distribution, secretion removal increase
PAP indications
atelectasis treatment/cardiogenic pulmonary edema (fluid in lungs secondary to R sided HF), contraindications → hemodynamic instability, hypoventilation
CPAP
continuous positive airway pressure, spontaneous ventilation with a positive airway pressure being maintained throughout the whole respiratory cycle
PEEP
positive end expiratory pressure, maintained airway pressure above atmospheric at the end of expiration and may be used with mechanical ventilation or spontaneous breathing
hilar region
great vessels and mediastinum
lateral neck x ray
helpful in differentiating between croup and cute epiglottitis
pleura
thin membrane surrounding the lung parenchyma, two thin membranes - outer parietal and inner visceral
pleural effusion
hydrothorax, accumulation of excess fluid within pleural space, best.x ray for detecting is lateral, blunted costophrenic angles
pneumothorax
collection of air in pleural space, may occur spontaneously (bled rupture), with trauma or invasive procedure or mechanical ventilation (barotrauma), causes lung margins to pull from chest wall
tension pneumothorax
occurs when air in the pleural space in under pressure, air accumulates in pleural space on inhalation but cannot exit on exhale, requires immediate decompression, pushes organs to the other side
pulmonary edema
alveoli are filled with a watery fluid that contains few cells, parenchymal disease, pink, frothy secretions, BIPAP indicated
bacterial pneumonia
alveoli are filled with an exudative fluid containing numerous white blood cells (pus), parenchymal disease
pulmonary hemorrhage
alveoli fill with blood, parenchymal disease, ICU patients mechanically ventilated → given heparin on high FiO2 breaking down alveolar capillary membrane → drank blood exits membranes into lungs
airspace opacity or infiltrates
indentical - appear patchy, increased density shadows that tend to coalesce over time on chest radiograph, infiltrates → fluid filling of alveolus (pneumonia, pus)
air bronchograms
lucent tubular structures that course through dense airspace opacities or infiltrates on both chest radiographs and chest CT images, air filled airways surrounded by infiltrates will cause these, hallmark of infiltrates that fill alveoli (air space disease)
pulmonary edema
due to left heart failure usually, kerly B lines (thin lines seen near pleural edge on chest film as a result of increased pulmonary capillary pressures) bat wing appearance (predominance of edema in hilar regions of lungs)
radiograph signs of cardiac decomp
(pulmonary edema) cardiac enlargement, pleural effusions - bilateral, resdistribution of blood flow to upper lobes, poor definition of the central blood vessels, kerley B lines, alveolar filling
interstitial lung disease
(idiopathic pulmonary fibrosis, sarcoidosis) radiograph shows diffuse, bitaletal infiltrates, opacities may resemble scattered, poorly defined nodules
plate atelectasis
when atelectasis is localized to subsegmental portion of lung, makes a plate shape where good lung function remains in center
volume loss (x-ray)
unilateral diaphragmatic elevation, mediastinal shift towards atelectasis, narrowing of the pace between ribs, hilar displacement towards atelectasis
hyperinflation (x-ray)
commonly seen with emphysema, more than sever anterior ribs are seen above the diaphragm, flattening of hemidiaphragms, large retrosternal airspace, narrowed mediastinum, increased AP diameter
solitary pulmonary nodules
seen via CT, smooth edge, malignant, star jagged edge, parenchymal opacity smaller than 3cm in diameter surrounded by aerated lung
pneumomediastinum
barotrauma, may result from movement of air into mediastinum, esophageal rupture - occurs in distal esophagus, chest trauma- may cause trachea / mainstem bornchus rupture
hypertension treatment
ACE inhibitors, ARBs, aldosterone agents, calcium channel blockers, thiazide diuretics and other antihypertensives
aneurysm
local dilation or outpouching of a vessel wall or cardiac chamber, true (fusiform-bilateral, fusiform-saccular one side, dissecting-saccular medical emergency) vs false
dilated cardiomyopathy
impaired systolic function (LV) leading to increases in intracardiac volume, ventricular dilation and systolic heart failure, caused by ischemic heart disease, hyperthyroidism, niacin deficiency, treatment involve reducing blood volume and increasing contractility
hypertrophic obstructive cardiomyopathy
inherited thick septal wall causing angine, syncope, palpitations, MI symptoms, L sided HF symptoms, treat w/ beta blockers/ACE inhibitors, surgery, septal ablation, implantable cardioverter-defibs
hypertensive/vavular hypertrophic cardiomyopathy
hypertrophy of the myocytes, attempts to compensate increased myocardial workload causing angina, syncope, dypnea on exertions & palpitations
restrictive cardiomyopathy
myocardium becomes rigid and noncompliant, impeding ventricular filling and raising filling pressures (diastole) causing R sided HF, venous congestion
acute HF
symptoms result from any structural or functional impairment of ventricular filling or ejection of blood (ischemic, MI, valvular heart disease, HTN)
ejection fraction
50-70% or less is HF, how much blood the left ventricle pushes out on exertion
AHF may result from…
impaired ventricular filling (preserved EF), impairment of ejection of blood (reduced EF), triggers a catecholaminergic response aimed to improve heart function by increased HR and muscle contractility